Proceedings of a Workshop
| IN BRIEF | |
|
June 2021 |
Exploring the Role of Critical Health Literacy in Addressing the Social Determinants of Health
Proceedings of a Workshop—in Brief
On January 27, 2021, the Roundtable on Health Literacy of the Health and Medicine Division of the National Academies of Sciences, Engineering, and Medicine held a virtual public workshop titled The Role of Critical Health Literacy in Addressing the Social Determinants of Health. The workshop’s Statement of Task can be found in Box 1. The planning committee’s role was limited to planning the workshop and the Proceedings of a Workshop was prepared by the workshop rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants, and are not necessarily endorsed or verified by the National Academies, and they should not be construed as reflecting any group consensus.
To begin the virtual workshop, Lawrence Smith, member of the Roundtable on Health Literacy, executive vice president and physician in chief at Northwell Health, and dean of the Donald and Barbara Zucker School of Medicine at Hofstra/Northwell, welcomed attendees. Smith introduced the moderators for the panels: Olayinka Shiyanbola, associate professor in the Social and Administrative Sciences Division in the School of Pharmacy at the University
![]()
of Wisconsin–Madison; Amanda J. Wilson, chief of the Office of Engagement and Training at the National Library of Medicine; and Gem Daus, health policy analyst in the Office of Health Equity at the Health Resources and Services Administration in the U.S. Department of Health and Human Services and adjunct professor in Asian American studies at the University of Maryland, College Park.
The following sections of the Proceedings of a Workshop—in Brief present summaries of each of the workshop’s three presentations. The presentations examined the concept of critical health literacy, what critical health literacy can look like in action, and how it may be used in research and evaluation. The final section of the proceedings provides a summary of the panel discussion, facilitated by Shiyanbola, during which the panelists together explored facilitators, barriers, and future directions for the implementation of critical health literacy interventions.
APPLYING THE CRITICAL HEALTH LITERACY FRAMEWORK TO ACHIEVE HEALTH EQUITY
Shiyanbola introduced the first speaker, Linn Gould, executive director of Just Health Action (JHA) in Seattle, Washington.1 Gould developed and teaches a critical health literacy curriculum that can be used to take action on the social determinants of health (SDOH) to achieve health equity.2
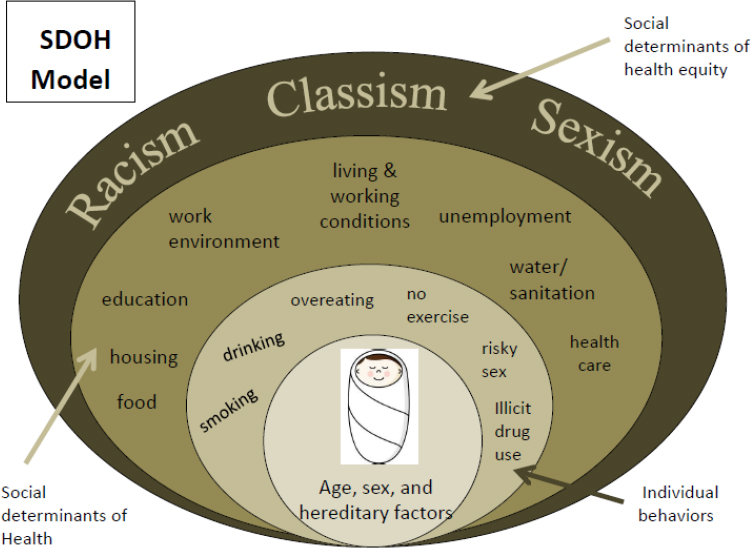
Gould began her presentation by first acknowledging that she lives and works on the traditional lands of the first people of Seattle and offered her gratitude to the Duwamish Tribe, past and present. Gould continued by presenting JHA’s SDOH model (see Figure 1), which is the basis for its work on critical health literacy. The first three layers of the model are adapted from Dahlgren and Whitehead’s (1991) SDOH model and the outer layer incorporates what Jones et al. (2009) refer to as the SDOH equity. This type of model is often referred to as the onion model.
Gould then shifted her discussion to the three levels of health literacy—functional, interactive, and critical (Nutbeam, 2000). She used safe sex as an example to describe each level. Functional literacy would entail providing individuals with facts about having safe sex. Interactive health literacy would be reached when people have learned how to communicate about having safe sex and are able to problem solve and independently make decisions about safe sex. Critical health literacy, which is not taught much in the United States today, she said, is about an individual’s understanding of the SDOH and their ability to take action at both the individual and the community level (Mogford et al., 2011). In the safe sex example, critical health literacy would come into play when a safe sex problem is identified in the community (e.g., high levels of sexually transmitted infections or unplanned pregnancies), and the question is asked: How can the community take action on the problem?
SOURCES: Gould presentation, January 27, 2021; adapted from Dahlgren and Whitehead, 1991; Jones et al., 2009.
__________________
1 See http://justhealthaction.org (accessed April 13, 2021).
2 See http://justhealthaction.org/resources/jha-curriculum-material (accessed April 13, 2021).
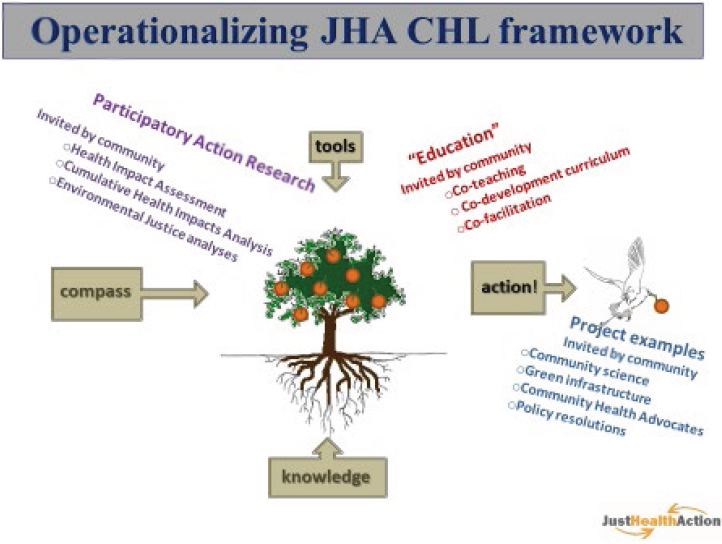
Gould then described a tree metaphor (pictured in Figure 2; Mogford et al., 2011) that is used in the curriculum and training that JHA developed to explain the critical health literacy framework to students and community members. The roots of the tree represent knowledge about equity, the SDOH, and health as a human right. In addition to the tree, the diagram includes a “compass” element. This dimension of the curriculum assists participants in finding a sense of direction as change agents, and exploring how participants want to be activists. An activist response to a problem, Gould explained, critically questions why the problem exists in the community and develops strategies to reduce or eliminate the problem on a structural level. Next, in order to move in the direction they identified in the compass stage, community members learn about tools and skills to take action; these are represented by the fruits of the tree. In the tree metaphor, the final stage of the process is represented by a bird flying away with a seed to take action and grow in the community.
JHA operationalizes the critical health literacy framework through several kinds of interventions. In any project that JHA engages in with a community, each stage of the framework (knowledge, compass, tools, and action) is incorporated. Gould also underscored that each intervention must be requested by the community, and that JHA does not enter a community without invitation. One type of intervention through which JHA operationalizes the critical health literacy framework is participatory action research. Together, the community and JHA conduct health impact assessments or cumulative health impact analyses. In the latter analyses, factors that contribute to negative health are considered together, rather than in isolation, to create a better assessment of a community’s cumulative health impacts and associated health risks. Additionally, JHA operationalizes the critical health literacy framework through a number of educational activities that are, again, invited by the community. These activities might include co-curriculum development, co-teaching, and co-facilitation with community members.
Having laid out the basic framework that underlies JHA’s work, Gould moved into describing critical health literacy projects undertaken by and with the Duwamish Valley community. She first noted that she collaborates with many organizations but her most important partner is the Duwamish River Cleanup Coalition, an alliance of 10 nonprofit organizations.3 She went on to describe the two communities with which the partnership has conducted critical health literacy and power-building activities: South Park and Georgetown in South Seattle’s Duwamish Valley. Gould explained that both communities, relative to other Seattle areas, have pronounced health inequities that compromise community health. For example, individuals living in the zip code that includes these communities (98108) have a life expectancy that is 13 years lower than that of individuals living in more affluent Laurelhurst (zip code 98105; Gould and Cummings, 2013). As additional context, Gould noted that the residents live adjacent to the Lower Duwamish
SOURCES: Gould presentation, January 27, 2021. Concept from Mogford et al., 2011.
__________________
3 See https://www.duwamishcleanup.org (accessed April 13, 2021).
Waterway Superfund Site. In the past, the Duwamish River had many meanders into a large estuary but in 1909, the Army Corps of Engineers straightened the river for industrial use. The valley represents 80 percent of Seattle’s industrial land base, but the river and surrounding area is heavily contaminated. She also noted that, though the industry in the Duwamish Valley supplies about 80 percent of the area’s family wage jobs, residents of the South Park and Georgetown communities do not necessarily have access to those jobs. Although the two communities face substantial health inequities, they have assets too; they are incredibly resilient areas, Gould said.
Gould said she often receives questions on how power building or empowerment and critical health literacy interact. During her presentation—and in discussion with Shiyanbola afterward—she emphasized that the concepts are inextricably linked; she noted that Nutbeam (1998), who originated the concept, says that empowerment cannot be achieved unless critical health literacy is developed and action is taken on the SDOH. To this end, JHA created a power-building model for its work in the Duwamish Valley (see Figure 3). This figure illustrates how the pieces of the critical health literacy framework come together, combined with power building, to enable community action, with the ultimate goal of achieving health equity. She highlighted that empowerment is recognized both as part of the process and as an outcome.
For the knowledge portion of the power-building model, JHA works with the communities to understand the SDOH through root-cause analysis exercises and storytelling. Community members also participate in root-cause analyses, an exercise used to understand the upstream, political determinants of health and to identify strategies to address those upstream factors.
In the compass and reflection portion of the work, JHA and community members conduct power analysis and advocacy mapping exercises. She described a health mapping exercise where youth and/or community members use pictures to depict the conditions that make a community healthy or unhealthy. This health mapping exercise contributes to decision making on the action areas that the community targets to improve health.
To build skills and capacity, Gould explained, JHA teaches whatever the community wants or needs. In terms of power building or empowerment, the goals are to understand and tackle inequitable distributions of power, improve daily living conditions, create health-promoting public policy, and conduct community action for health. Other exercises help community members define what equity means for the community and to design their own definitions for individual empowerment and community empowerment. They can measure their own progress on an empowerment pathway.
Gould provided a number of examples of community actions undertaken using the power-building model (see Figure 3). She described work with the Duwamish River Cleanup Coalition’s Clean Air Program.4 This program has
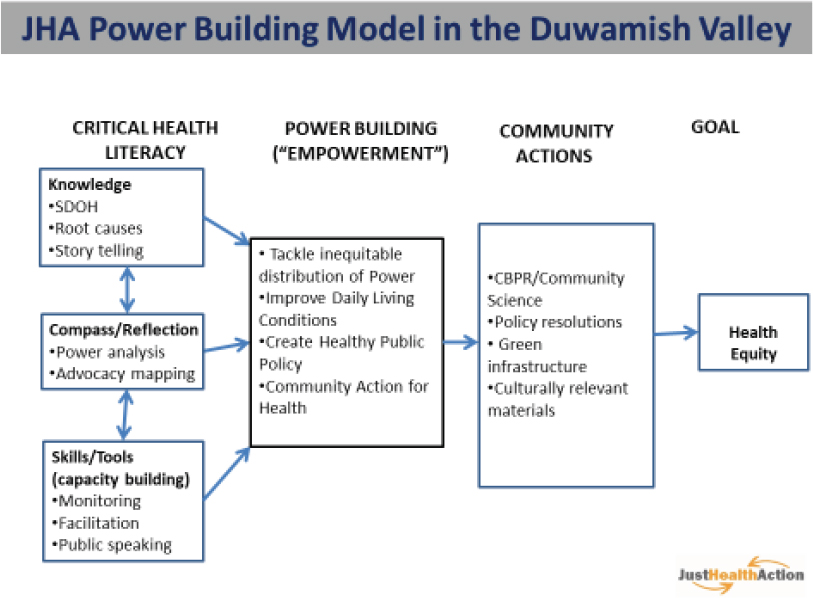
NOTE: CBPR = community-based participatory research.
SOURCE: Gould presentation, January 27, 2021.
__________________
4 See https://www.duwamishcleanup.org/clean-air-project-link (accessed April 13, 2021).
been in existence for several years, but was relaunched last year with a new model. A broad range of community clean air partners (government agencies, universities, nonprofit organizations, and community members) participates in the program. She explained that community members conducted a root-cause exercise of asthma to identify what action strategies could be taken. Based on the analysis, they identified poor indoor air quality in rental housing as a cause of asthma and poor landlord maintenance of housing units as a cause of the cause (or “root cause”). This understanding enabled community members to identify a policy action: advocacy to get landlords to improve housing conditions. One of the most interesting observations noted with this exercise, she said, was that the policy actions identified by the community members were much more upstream than those selected by other types of partners who underwent the same exercise.
Another action taken by community members is community science—what academicians refer to as community-based participatory research (CBPR). For example, as part of the Duwamish Valley Clean Air Program, community youth collected moss and analyzed metals in the samples in order to identify the source of air pollution in the Duwamish Valley. Throughout the process, Gould explained, the partnership’s intent is for the community to maintain ownership of the data and all other aspects of their work.
Gould ended her presentation with a brief summary of ongoing policy work around the Port of Seattle. She explained that, recently, the Port of Seattle admitted that it had been a partial contributor to the negative environmental and economic impacts in the Duwamish Valley over the past 100 years. For more than 3 years, JHA worked with the Port of Seattle Community Action Team, comprising about five members from Georgetown and five community members from South Park, to develop trust and to eventually co-write a policy resolution. Community members conducted policy advocacy and provided public testimony at the Port of Seattle meetings. On December 10, 2019, the Port of Seattle passed Resolution 3767, the Duwamish Valley Community Benefits Commitment Program. It was an exciting day for the Duwamish Valley, Gould said.5
CRITICAL HEALTH LITERACY AND COMMUNITY-BASED PARTICIPATORY RESEARCH
Wilson introduced the next speaker, Vanessa Simonds, associate professor at Montana State University. Simonds began her presentation by explaining that she conducts research in partnership with the Crow (or Apsáalooke) community in Montana. The research focuses on environmental health issues and uses the concept of critical health literacy to drive research activities, implementation, and evaluation efforts.
The community with which they work is an Indigenous, rural community. Like many other rural, low-income communities, this community faces a triple threat of a higher risk for exposure to chemicals or pathogens, a lack of access to resources to address and mitigate those exposures, and health literacy barriers (see Figure 4). Health literacy barriers, Simonds elaborated, arise when information on risks and resources is not communicated to the community in a way that aligns with the level of literacy skills in the community.
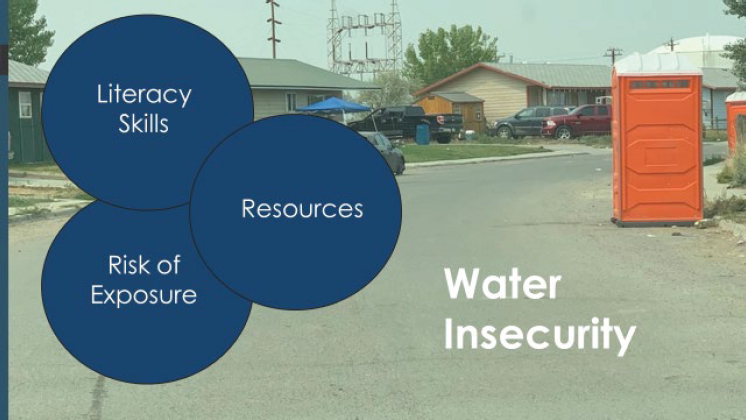
SOURCE: Simonds presentation, January 27, 2021.
__________________
5 See https://www.duwamishcleanup.org/port-of-seattle-community-equity (accessed April 13, 2021).
The environmental health problems that the Crow community is addressing, Simonds explained, are water insecurity and water safety. In the United States, rural tribal households are less likely to have access to safe water than non-tribal homes. Similar to other rural communities across the United States, many rural tribal residents rely on home wells as their primary water source. But home wells may be contaminated; for example, studies have documented uranium and arsenic contamination in wells on Navajo tribal lands.6 Well testing in Crow communities has also found that some homes have unsafe, contaminated well water (LaVeaux et al., 2018).
In addition to the problem of contaminated home well water, tribal members have raised concerns about the general deterioration of local water sources. Community members are losing access to safe and free water for basic household needs as river water quality declines. Water contamination and insecurity is troubling for all communities they affect, but for Crow people there are additional and significant dimensions to these problems, Simonds noted. First, the Crow people have a deep spiritual connection and relationship to water; water is deeply embedded within Crow cultural practices (Martin et al., 2021). Additionally, complex tribal jurisdictional issues, paired with a lack of financial resources in the community, make it difficult for the community to address water contamination (Simonds et al., 2019b).
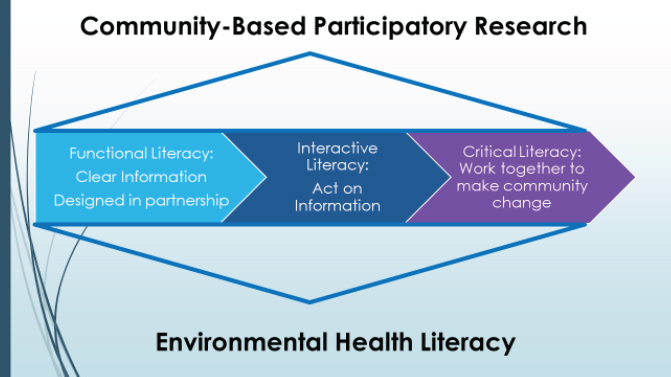
Simonds shared that the research team found that the health literacy framework (as described in Nutbeam, 2008) is compatible with CBPR to address environmental health issues (LaVeaux et al., 2018; see Figure 5). In other words, CBPR can be used to undertake interventions around the three components of environmental health literacy: functional literacy, interactive literacy, and critical literacy. To achieve functional literacy, the CBPR research team worked with the community to design information that is clear, based on community language rather than jargon, and culturally relevant. For example, because water is very important to Crow people (Martin et al., 2021), Simonds said it would be inappropriate to advise community members not to drink river water as part of a tribal ceremony, even though it may not be entirely safe. Once functional literacy is achieved, the CBPR research team and community co-created interventions around interactive literacy (where members act on and share the information they receive). Finally, by applying environmental critical health literacy, the CBPR team and the community worked together to achieve community-level change (LaVeaux et al., 2018).
Simonds next shifted to provide more specifics on how the research team integrated the environmental health literacy framework into its CBPR approach in order to promote critical health literacy among community adults. An important first step in CBPR research, she said, is to consider the skill level of community members and to identify which skills they believe need to be developed. She noted that in 2004, tribal members began to identify water quality and the impact poor water quality can have on human health as a community problem. These community members reached out to and developed a partnership with researchers so that they could work to understand and document the contaminants in local water sources.
Two challenges that proved to be critical were building trust between researchers and the community, and considering how the researchers could best provide data and information back to the community (LaVeaux et al., 2018). In the question-and-answer session that followed the presentation, Simonds reflected that the keys to building trust had been time and consistency. She highlighted the importance of the fact that the research team continued
SOURCE: Simonds presentation, January 27, 2021.
__________________
6 For example, Credo et al. (2019) and Hoover et al. (2017).
“showing up and doing what we said we would do.” With respect to the second challenge of communicating information back to the community, tribal members and the researchers determined that the co-creation of information materials would be the best method for communicating their findings (LaVeaux et al., 2018). They found that home visits served as another effective method for informing community members. Trusted members of the Crow Environmental Health Steering Committee, a group formed to address water issues, conducted the home visits.
In 2014, the tribal leadership invited Simonds and her team to assist in furthering critical health literacy around water insecurity. A community–academic partnership, Guardians of the Living Water, a project founded by the Crow Environmental Health Steering Committee, served as the vehicle for increasing environmental health literacy among youth (fifth- and sixth-grade students) and their families. Simonds explained that the goal of the project was to address water insecurity holistically by educating youth about water quality science, the cultural significance of water sources, and the Crow values of respecting rivers and springs. The project initiated new partnerships with the local public school, the college, and community members to pursue the goal of enhancing critical health literacy in youth and inspiring them to be agents of change. The project hosted summer camps and after-school activities for youth to learn about the relationship between water-related environmental issues and human health, and supported activities for youth to apply their knowledge and conduct dissemination tasks (Milakovich et al., 2018; Simonds et al., 2019a).
Simonds explained that the team employed the same health literacy framework used with the adult community members to achieve functional, interactive, and critical health literacy with the youth. With respect to functional literacy, an existing curriculum conveyed the basics on the science of water quality, and Crow elders engaged in storytelling with the youth to integrate cultural knowledge about the importance of water to the Crow people (LaVeaux et al., 2018).
The next step, according to Simonds, was to help the youth apply that knowledge and demonstrate interactive health literacy. Similar to activities conducted by the Crow Environmental Health Steering Committee, the youth chose to apply what they learned through water testing. They identified specific water sources of interest to them and conducted the tests themselves (Milakovich et al., 2018; see Figure 6).
Another dimension of the project that supported functional and interactive health literacy was the use of a cross-mentoring model. Under the model, Simonds explained, tribal college or tribal high school students who had achieved functional health literacy served as mentors to middle school students. They assisted the younger students in developing their own questions and research, thinking about applying what they learned, and conducting water testing. In this way, older youth also demonstrated interactive health literacy.
Simonds shared that a number of questions arose with respect to developing critical health literacy among youth. These included “What is it that youth can do about this issue? How can they address water insecurity? What are the steps they can take? What do they need to learn so that they can act?” Students brainstormed a number of ideas, including adopting areas where trash tended to accumulate. They set out, monitored, and cared for trash cans in these areas in order to discourage trash dumping. The youth also thought up research questions related to water testing, including comparing water quality at different sites and determining how best to protect the water springs over time.

SOURCE: Simonds presentation, January 27, 2021.
Finally, the youth chose to develop a movie to educate others about what they had been learning (interactive health literacy). Indigenous filmmakers assisted the youth in creating the film, which ultimately received an award at an Indigenous film festival.
Simonds then commented on the success of their work in achieving its main goal: to develop youth as change agents through the application of critical health literacy. She reported that the research team conducted surveys and interviews with participants, parents, and the larger community in order to evaluate change. She noted that the youth talked about their increased sense of environmental responsibility, actions they had taken, and actions they wanted to take in the future (Milakovich et al., 2018; Simonds et al., 2019a). Photovoice, a qualitative method utilized in CBPR, was also part of the evaluation. Youth used photography and stories associated with their photographs as a medium to share their new knowledge and inform and educate the community. Simonds noted that the youth’s experience led to the development of a new logic model (see Figure 7) that tells the story of how the project works to integrate Indigenous science and Western science, and to transmit that knowledge through youth to the broader community.
Simonds next reflected on lessons learned from the CBPR project. The overarching takeaway is that CBPR and critical health literacy can be beneficial in addressing the SDOH. The first lesson she offered is that environmental health issues related to water insecurity are complex and need to draw on science literacy, health literacy, and legal literacy. Second, she observed that the complexity of the issues necessitates cross collaboration, especially between community and academic–scientific partners. Scientists and academicians can provide guidance on what to research and how to address the identified problems; community partners can help researchers make their research more impactful and more effective. The third lesson relates to balancing what she describes as the need to provide youth with guidance versus the need to direct youth to be change agents. Ultimately, Simonds believes that youth need to be in charge of the ideas and the process. The fourth lesson Simonds stressed is the importance of integrating Indigenous knowledge and culture with Western science.
IMPLEMENTING CRITICAL HEALTH LITERACY TO BUILD RESILIENCY
Daus introduced the final panelist, Gabriel Maldonado. Maldonado is founder and chief executive officer of TruEvolution, a community-based organization that advocates for health equity and racial justice to advance the quality of life and human dignity of LGBTQ+ people. The organization also provides HIV, mental health, and housing services.
Maldonado opened by providing some background to his presentation, titled Leading with Resiliency. He explained that his lived experiences as a member of the LGBTQ+ community, an individual living with HIV, and a former resident of an urban community of low socioeconomic status, led him to focus much of his work on stigma as an SDOH, and the role it plays in creating health disparities and health inequities. He noted that the organization he directs witnesses the impact of stigma on the health of the clients it serves, and it recognizes the role critical health literacy can play in promoting resiliency and addressing stigma in community settings.
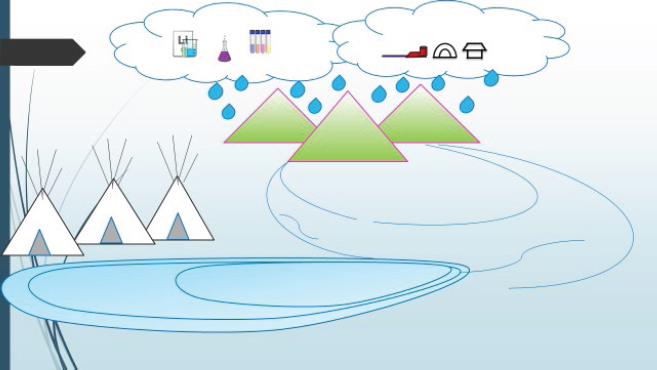
SOURCE: Simonds presentation, January 27, 2021.
Stigma has been identified as an SDOH, as it has been demonstrated to impact health outcomes and risks for a variety of conditions (Craig et al., 2017; Hatzenbuehler et al., 2013, 2014; Turan et al., 2017). Maldonado went on to describe the concept of stigma and how it operates in society. He explained that stigma broadly refers to assumptions made about a group of people, and how those assumptions affect the experiences of individuals. He said that stigma consists of three pieces. Stereotypes are characteristics generally assumed about a group of people. These stereotypes can lead to prejudice, when people assume that those stereotypes about a group are valid and confirmed. This, in turn, results in discrimination, which occurs when actions are taken based on those stereotypes and prejudices. These actions, he said, manifest in stigmatizing assumptions, stigmatizing experiences, and stigmatizing systems that affect individuals. As an example, he noted that systemic racism and systemic bias and prejudice exist in the health care system toward individuals with HIV. The systemic racism and bias often begin when individuals in positions of power, who hold stereotypes about people with HIV, create discriminatory experiences for the people they serve.
He went on to describe three types of stigma: community, institutional, and self- or internalized stigma. During this discussion, Maldonado provided examples of the mechanisms through which stigma can act as an SDOH and deepen health inequities. Community stigma refers to stigma that is encountered among family and friends, in the workplace, and in faith spaces. Faith spaces, he emphasized, may need special consideration. He shared that that there is a precarious relationship between the LBGTQ+ community and religious and faith spaces. On one hand, it is important to acknowledge that Black and Brown communities have found faith places to be spaces of safety and refuge, which can be beneficial for health. However, the Black and Brown LGBTQ+ communities have also experienced very real traumatizing effects of stigma perpetrated in faith spaces, he said.
He then discussed institutional stigma, which is the stigma encountered in a range of places that provide needed resources, such as the health care system, clinics, schools, universities, and the legal system. He emphasized the special situation of the large number of marginalized young people who are involved in the criminal justice system. Members of the LGBTQ+ community and individuals living with HIV, who already experience marginalization, encounter additional marginalization while in prison or jail. Such institutional stigma may act as an SDOH because it may prevent these individuals from accessing needed medications and services to address co-occurring conditions such as mental health problems and trauma, he said.
Last, Maldonado explained internalized stigma, held toward the self. This form of stigma is often characterized by sexual shaming, guilt, depression, retraumatization, avoidance, unprocessed anger and sadness, and fatalism. Fatalism, he said, finds its way into the souls of clients; internalized stigma acts as an SDOH because it affects their ability to engage in services, disclose information, trust, and be willing to go to multiple agencies to seek services.
Having established that stigma operates as an SDOH, Maldonado then transitioned to describe how critical health literacy could be used to address internalized stigma. Specifically, critical health literacy interventions can be used to build resiliency, which Maldonado said is the key to empowering individuals to combat stigma. Maldonado used the framework for resilience described by Harper et al. (2014). Maldonado explained that building resiliency requires an individual to engage in health-promoting cognitive processing (functional health literacy), enact healthy behavioral practices or choices, enlist social support from others (interactive health literacy), and empower other young LGBTQ+ individuals (critical health literacy). Empowering the client to have a perspective beyond themselves is important, he said. Otherwise, the focus might remain on the tragedy and trauma of the individual’s life experiences, rather than on what is possible.
Maldonado suggested that critical health literacy could be used to help build resiliency and combat stigma, as illustrated through the previous examples. Maldonado said his understanding of critical health literacy is based on a definition by Sykes et al. (2013). It describes critical health literacy as “a set of characteristics of advanced personal skills, health knowledge, information skills, effective interaction between service providers and users, informed decision making and empowerment, including political action.” The potential consequences of critical health literacy, under this definition, are “improving health outcomes, creating more effective use of health services, and reducing inequalities in health” (Sykes et al., 2013).
Maldonado offered eight suggestions to implement health literacy in health agencies and institutions (see Box 2). He suggested that the interventions described can help build toward critical health literacy, in part by improving functional and interactive health literacy in a community. These steps toward critical health literacy may also be regarded as, ultimately, steps toward building resiliency and combatting stigma.
After the presentation, Daus led a brief discussion. He asked Maldonado what data his service organization collects in order to identify what social determinants may be affecting clients. In reply, Maldonado explained that because providers at community-based organizations interact with clients every day they are able to provide crucial insight. For example, at his organization, check-ins and screenings are conducted regularly; this form of data allows the providers to identify themes and obstacles across clients (e.g., transportation barriers to accessing care). Those conver-
sations, in turn, inform what social determinants the organization might target in the future. The interventions identified to address these SDOH could include approaches based in critical health literacy.
DISCUSSION
Following the final presentation, Shiyanbola facilitated a discussion with all of the panelists. Beginning with a question submitted by a member of the public, she asked what advice the speakers would give to health departments seeking to promote critical health literacy around the COVID-19 vaccine. Maldonado responded first to this question, and emphasized the importance of empowering and building the infrastructure of community-based organizations. Simonds concurred. She stressed that the Crow reservation and other tribal nonprofits have played a crucial role in delivering needed
resources (such as food and masks) to the community during the COVID-19 pandemic. Gould shared that South King County has faced large disparities in the COVID-19 crisis, and that, though it took some time, she feels that the health departments have recognized a need to redirect their messaging and address the most impacted communities.
The next question came from roundtable member Wilson. Noting that all of the webinar’s presentations shared the theme of working with youth, she asked the panelists whether there are certain populations, like youth, that are more amenable to critical health literacy projects than others. Simonds responded first, immediately explaining that the impetus for focusing on youth came from the urging of her partners in the Crow community. The community leaders felt that the youth would be the most effective change agents. In light of the fact that many of the partnership’s leaders are elders, they felt it would also help sustain the work in future generations. Simonds added that it has proven to be a fruitful approach. Additionally, Gould noted that in immigrant communities, youth are an important audience for critical health literacy because they often have the highest levels of English fluency and are able to communicate information to other members of their communities.
Roundtable member Daus then asked the panelists about their experiences working with those who have had the opportunity to receive a professional education, such as nurses or doctors, and how they receive these concepts of health literacy. Gould responded that in her personal experiences teaching these concepts at medical schools and health departments, she has found that nurses have often been the most receptive to concepts of the SDOH and health equity. On the other hand, she states that she has encountered more resistance in her experiences with medical schools, where some individuals expressed that these concepts were “for social workers.” She suggested that community clinics tend to be more open to critical health literacy. Maldonado shared that he has felt encouraged that newer medical schools seem to be incorporating the SDOH, community health, and equity into their work. As an example, he noted that the University of California, Riverside, incorporated a commitment to these concepts as part of its entrance process and loan forgiveness programs.
In response to Shiyanbola’s question about what the future looks like for health literacy in the space of the SDOH, Maldonado responded that it is unavoidable, and that “we are at the door.” He argued that the COVID-19 pandemic has revealed to the public that inaction around factors such as congregate housing and mental health has created a strain on the U.S. health care system. He suggested that continued avoidance of these topics by institutions is likely to result in poor health outcomes in the future. Gould stated that she envisions the end of poverty. She underscored the importance of “root-cause” exercises, such as those used in JHA’s program, as a tool to help individuals understand the upstream policies that might affect change. She also expressed that focusing on individual behavioral change amounts to victim blaming. Simonds concurred with the statements of the other two panelists, and added that, when it comes to research, community partners want researchers to take action (as critical health literacy requires) rather than simply measuring and leaving.
In response to Simonds’s comment, Wilson asked what researchers and scientists need to learn in order to effectively engage in CBPR. Simonds noted that her research team benefited from the fact that the Crow community was experienced in communicating its priorities to researchers. Additionally, the community had existing advisory boards that would consider researchers’ proposals or that would initiate proposals themselves and bring them to researchers. She again underscored the importance of building trust between the research team and the community and said that researchers should maintain flexibility to pivot their approach if the community feels that it is not working.
Daus, sharing a question from the webinar chat, asked the panelists how they navigate balancing the important work of building resiliency with maintaining a focus on a systemic approach to the SDOH. In particular, he asked how they avoid reinforcing the narrative that individuals are responsible for disparate outcomes. Maldonado responded by noting that these are not mutually exclusive. Institutions and providers, he suggested, should focus on reducing the burdens placed on clients. At the same time, he clarified, it may be necessary to figure out how an individual with marginalized identities can navigate and overcome the barriers that they encounter on a day-to-day basis. He provided an example of working with an individual who has just relapsed during their recovery process with methamphetamine. His approach in that moment, he said, is to work with the client to identify what tools and resiliency they may need to be able to recover in that moment.
Shiyanbola then asked the panelists to turn to the challenges they have encountered in creating community-level, systemic change through critical health literacy work. Simonds shared that her team has encountered many challenges in its work around water insecurity in tribal communities. For instance, she shared that it can be difficult to navigate the overlapping jurisdictions of state and tribal entities. In the short term, her team addressed these challenges by focusing on well water testing, which goes unregulated by the government. The tribal colleges, she added, have responded by creating more courses related to water quality, as a longer-term solution to the gaps faced in these rural communities.
While Smith noted that trust is likely the biggest barrier to effective interventions in critical health literacy, he asked if the panelists have encountered misinformation, whether intentionally or unintentionally spread, as another
barrier. He also asked how they approach addressing misinformation. In response, Gould noted that contamination and its causes can be complex, and that sometimes genuine confusion can result in the spreading of misinformation. She reiterated that addressing misinformation goes back to building trust. She shared a story about the impact that a meeting between U.S. Fish & Wildlife enforcement officers and community health advocates had on decreasing misinformation around fishing practices. Maldonado agreed that misinformation, and the unlearning of that misinformation, often present a serious challenge.
Lastly, the panelists responded to a question from Wilson, who asked what resources they recommend for people seeking to understand the difference between critical health literacy and health literacy. Maldonado stressed the importance of beginning with understanding the SDOH; if someone understands basic health literacy, and understands the SDOH, he suggested it is easier to bridge the gap. Gould noted that she and her team have shared educational materials on the JHA website and have published an article that can serve as a useful jumping off point (Mogford et al., 2011). ◆◆◆
REFERENCES
Craig, G. M., A. Daftary, N. Engel, S. O’Driscoll, and A. Ioannaki. 2017. Tuberculosis stigma as a social determinant of health: A systematic mapping review of research in low incidence countries. International Journal of Infectious Diseases 56:90–100. doi: 10.1016/j. ijid.2016.10.011.
Credo, J., J. Torkelson, T. Rock, and J. C. Ingram. 2019. Quantification of elemental contaminants in unregulated water across Western Navajo Nation. International Journal of Environmental Research and Public Health 16(15):2727. doi: 10.3390/ijerph16152727.
Dahlgren, G., and M. Whitehead. 1991. Policies and strategies to promote social equity in health. Background document to WHO—Strategy paper for Europe. Stockholm, Sweden: Stockholm Institute for Futures Studies.
Gould, L., and B. Cummings. 2013. Duwamish Valley cumulative health impacts analysis. Seattle, WA: Just Health Action and Duwamish River Cleanup Coalition/Technical Advisory Group.
Harper, G. W., D. Bruce, S. G. Hosek, M. I. Fernandez, B. A. Rood, and the Adolescent Medicine Trials Network for HIV/AIDS Interventions. 2014. Resilience processes demonstrated by young gay and bisexual men living with HIV: Implications for intervention. AIDS Patient Care and STDs 28(12):666–676. doi: 10.1089/apc.2013.0330.
Hatzenbuehler, M. L., J. C. Phelan, and B. G. Link. 2013. Stigma as a fundamental cause of population health inequalities. American Journal of Public Health 103(5):813–821. doi: 10.2105/AJPH.2012.301069.
Hatzenbuehler, M. L., A. Bellatorre, Y. Lee, B. K. Finch, P. Muennig, and K. Fiscella. 2014. Structural stigma and all-cause mortality in sexual minority populations. Social Science and Medicine 103:33–41. doi: 10.1016/j.socscimed.2013.06.005.
Hoover, J., M. Gonzales, C. Shuey, Y. Barney, and J. Lewis. 2017. Elevated arsenic and uranium concentrations in unregulated water sources on the Navajo Nation, USA. Exposure and Health 9(2):113–124. doi: 10.1007/s12403-016-0226-6.
Jones, C. P, C. Y. Jones, G. S. Perry, G. Barclay, and C. A. Jones. 2009. Addressing the social determinants of children’s health. Journal of Health Care for the Poor and Underserved 20(4 Suppl):1–12. doi: 10.1353/hpu.0.0228.
LaVeaux, D., V. W. Simonds, V. Picket, J. Cummins, and E. Calkins. 2018. Developing a curriculum for change: Water and environmental health literacy in a Native American community. Progress in Community Health Partnerships 12(4):441–449.
Martin, C., V. W. Simonds, S. L. Young, J. Doyle, M. Lefthand, and M. J. Eggers. 2021. Our relationship to water and experience of water insecurity among Apsáalooke (Crow Indian) people, Montana. International Journal of Environmental Research and Public Health 18(2):582. doi: 10.3390/ijerph18020582.
Milakovich, J., V. W. Simonds, S. Held, V. Picket, D. LaVeaux, J. Cummins, C. Martin, and L. Kelting-Gibson. 2018. Children as agents of change: Parent perceptions of child-driven environmental health communication in the Crow community. Journal of Health Disparities Research and Practice 11(3):115–127.
Mogford, E., L. Gould, and A. DeVoght. 2011. Teaching critical health literacy in the U.S. as a means to action on the social determinants of health. Health Promotion International 26(1):4–13. doi: 10.1093/heapro/daq049.
Nutbeam, D. 1998. Health Promotion Glossary. Health Promotion International 13(4):349–364. doi: 10.1093/heapro/13.4.349.
Nutbeam, D. 2000. Health literacy as a public health goal: A challenge for contemporary health education and communication strategies into the 21st century. Health Promotion International 15(3):259–267. doi: 10.1093/heapro/15.3.259.
Nutbeam, D. 2008. The evolving concept of health literacy. Social Science & Medicine 67(12):2072–2078. doi: 10.1016/j.socs-cimed.2008.09.050.
Simonds, V. W., F. L. Kim, D. LaVeaux, V. Pickett, J. Milakovich, and J. Cummins. 2019a. Guardians of the living water: Using a health literacy framework to evaluate a child as change agent intervention. Health Education Behavior 46(2):349–359. doi: 10.1177/1090198118798676.
Simonds, V. W., M. Margetts, and R. E. Rudd. 2019b. Expanding environmental health literacy—a focus on water quality and tribal lands. Journal of Health Communication 24(3):236–243. doi: 10.1080/10810730.2019.1597948.
Sykes, S., J. Wills, G. Rowlands, and K. Popple. 2013. Understanding critical health literacy: A concept analysis. BMC Public Health 13(1):150. doi: 10.1186/1471-2458-13-150.
Turan, B., A. M. Hatcher, S. D. Weiser, M. O. Johnson, W. S. Rice, and J. M. Turan. 2017. Framing mechanisms linking HIV-related stigma, adherence to treatment, and health outcomes. American Journal of Public Health 107(6):863–869. doi: 10.2105/ajph.2017.303744.
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Rose Marie Martinez and Kelly McHugh as a factual summary of what occurred at the workshop. The statements made are those of the rapporteurs or individual workshop participants and do not necessarily represent the views of all workshop participants; the planning committee; or the National Academies of Sciences, Engineering, and Medicine.
*The National Academies of Sciences, Engineering, and Medicine’s planning committees are solely responsible for organizing the workshop, identifying topics, and choosing speakers. The responsibility for the published Proceedings of a Workshop—in Brief rests with the rapporteurs and the institution. The members of the planning committee were Annlouise Assaf, Pfizer Worldwide Medical and Safety; Gem Daus, Health Resources and Services Administration; Laurie Myers, Merck Sharp & Dohme Corp.; Olayinka O. Shiyanbola, University of Wisconsin–Madison School of Pharmacy; and Amanda J. Wilson, National Library of Medicine.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Ruth Parker, Emory University School of Medicine; Christopher R. Trudeau, University of Arkansas at Little Rock William H. Bowen School of Law; and Amanda J. Wilson, National Library of Medicine. Hugh Tilson, University of North Carolina Gillings School of Global Public Health, served as the review coordinator.
SPONSORS: This workshop was partially supported by AbbVie Inc.; California Dental Association; Eli Lilly and Company; Health Resources and Services Administration (HHSH25034011T); Merck Sharp & Dohme Corp.; National Institutes of Health (HHSN263201800029I); and Pfizer Inc.
For additional information regarding the workshop, visit www.nationalacademies.org/HealthLiteracyRT.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2021. Exploring the role of critical health literacy in addressing the social determinants of health: Proceedings of a workshop—in brief. Washington, DC: The National Academies Press. https://doi.org/10.17226/26214.
Health and Medicine Division

Copyright 2021 by the National Academy of Sciences. All rights reserved.













