Proceedings of a Workshop
| IN BRIEF | |
|
August 2021 |
Testing and Validating the Staffing Methodology for the Veterans Health Administration
Proceedings of a Workshop—in Brief
On June 21–22, 2021, the National Academies of Sciences, Engineering, and Medicine convened a virtual workshop on behalf of the Veterans Health Administration (VHA). This was the final in a series of workshops undertaken as part of a consensus study to prepare a resource planning and staffing methodology for VHA Facility Management (Engineering) Programs.1 In its consensus study report, the committee determined that the implementation of a staffing methodology is necessary for the VHA—both in response to congressional mandates for workforce projections and for the purpose of making better, data-informed staffing decisions; thus, the VHA began to develop an engineering staffing tool. The purpose of this workshop was to provide an update on the current status of and future opportunities for the VHA staffing tool, examine benchmarking for facilities, and discuss implementation. During the workshop, Co-Chairs James Smith, a former U.S. Ambassador, and Colin Drury, a Distinguished Professor Emeritus at the State University of New York (SUNY), expressed their satisfaction with the final consensus study report. Smith recognized how difficult it is to adopt changes in such a large and complex organization, and Drury looked forward to learning more about how the VHA is executing the report’s recommendations.
VHA ENGINEERING STAFFING TOOL OVERVIEW
Steven Broskey, a compliance engineer with VHA Healthcare Engineering, began by thanking the National Academies and the committee for its work on the study and for the preparation of this workshop. Broskey explained that the VHA needed a staffing tool that could support management and budgetary decisions related to the number and mix of engineering staffing as well as support staffing decisions to maintain building and utility systems that facilitate the delivery of patient care to veterans, help standardize the level of service and improve performance, and objectively assess staffing and the critical mission infrastructure they maintain. VHA designed the engineering staffing tool so that it would be adjustable for site-specific characteristics, easy for VHA facilities to understand and use, comprised of credible information, adaptable to changes, readily accessible without significant investment of local time and energy, and equipped with tools for facilities to validate and compare data.
Broskey remarked that a “drill down” tool allows facilities to review and validate current staffing cost assignments to confirm that existing staffing levels are represented accurately in a staffing analysis. It also provides ratios and comparisons to VHA averages. The engineering staffing tool is then used to calculate a predictive level of staffing
__________________
1 To read the final report of the consensus study committee, see National Academies of Sciences, Engineering, and Medicine, 2020, Facilities Staffing Requirements for the Veterans Health Administration—Resource Planning and Methodology for the Future, Washington, DC: The National Academies Press, https://doi.org/10.17226/25454.
![]()
compared to actual staffing (i.e., observed/expected [O/E] ratio). He explained that each facility receives an “expected” staffing level ranking based on a multivariate log-linear regression analysis. All rankings, including source data, are published on an internal website so as to broaden the understanding of the connections between staffing and performance. He noted that the staffing tool does not measure whether a facility has enough staff but rather provides a benchmark for comparison, based on patient workload, square footage, and facility size and age. Because VHA’s performance data are currently self-reported, it can be difficult to find meaningful correlations. He emphasized that it is important to view engineering as an enterprise-level business with standard measures for workload capture and performance. If a facility is understaffed, systems could fail—the VHA hopes to evolve to a risk-based analysis tool, with staffing as only one of its many components.
Smith asked for Broskey’s reflections on the consensus study report as well as on any areas that could benefit from further study. Broskey said that the report’s recommendations were well targeted in terms of determining strategic direction and creating a methodology. The challenge for VHA is creating an algorithm that leads to an understanding of the number of staff the organization should have in each facility. Broskey also noted that implementation of the recommendations is a larger undertaking than the committee or the VHA anticipated.
VHA ENGINEERING STAFFING TOOL: DEVELOPMENT AND IMPLEMENTATION OF STAFFING METHODS FOR VHA ENGINEERING PROGRAMS
Douglas Peterson, program analyst, VHA Office of Productivity, Efficiency, and Staffing (OPES), described the process of developing engineering staffing tools, based on the recommendations of the consensus study report and approaches that were successful for other groups. It was important to understand current staffing levels first; however, he noted that “engineering staffing” was not clearly defined, and engineering responsibilities varied by facility. To make better distinctions between VHA Healthcare Engineering and Other Healthcare Environment and Facilities Programs, and thus build a more accurate staffing tool, OPES relied on the three categories outlined in the report: Engineering Administration, Capital Projects, and Operations and Maintenance. Next, OPES developed a risk-adjusted staffing model to monitor the engineering full-time equivalent (FTE). After comparing data systems that could help describe current engineering staffing, the financial management system, which contains the official, annualized FTE counts based on data that are integrated with the payroll system, was selected as the platform. He explained that the FTE counts are summarized at the parent facility level, which corresponds to other VHA data sources, and contain a budget object code (BOC) and a Veterans Administration (VA) cost center. A staffing analysis was then conducted, which confirmed that different types of staff have different costs. To make fair staffing decisions, he continued, it was necessary to adjust for differences in average staff costs by BOC, which led to the final dependent variable, the total standardized health-care engineering FTE. The variation in staffing was monitored through the development of staffing tools and the creation of a continuous feedback loop.
Peterson mentioned that the fiscal year (FY) 2020 descriptive model included 137 facilities (those with <10 FTE were excluded). The variables that had a strong relationship with engineering staffing included patient population and facility size and age. The independent variables included VHA-owned and VHA-used square footage, allocation resource center pro-rated patients, percentage of facility patients covered by Medicare, long-term care average daily census, count of buildings, and count of rehab beds. (Three variables had an inverse relationship: drive time to specialty care, outleased gross square footage, and percentage of building areas 10–40 years old.) After adjusting for the variables, it was possible to account for 83 percent of the variation in engineering staffing. Peterson stressed that throughout the implementation of the model, data validity, reliability, and usability are key. For example, OPES changed the Capital Resource Survey (CAPRES) data by modifying the instructions to encourage editing of corporate financial and capital asset databases, resulting in a decrease in the number of facilities that reported changes in square footage without reporting changes in the building counts.
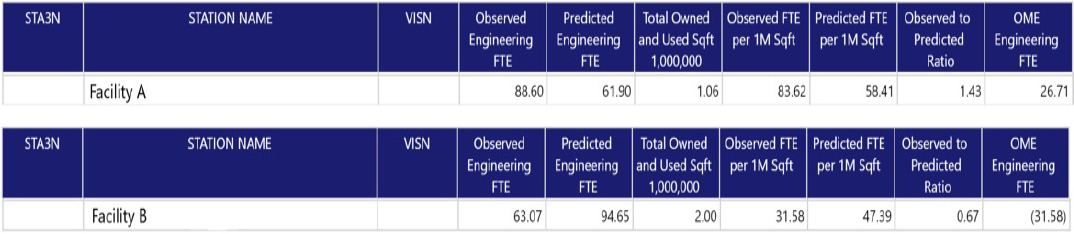
As an example of the model’s functionality, he compared Facility A, with an O/E ratio of 1.43, and Facility B, with an O/E ratio of 0.67. Sites with O/E values >1.0 have more engineering FTE than the VHA average; sites with O/E values <1.0 have fewer FTE than the VHA average (see Figure 1). The OPES Engineering Staffing Tool Detail Report reveals staffing groups by cost center and engineering staff type; the Engineering Staffing Facility Cost Center Detail Report identifies where staffing is relatively high or low; and the Engineering Staffing Name Detail Report includes staff name, occupation name, and paid FTE to understand staffing trends over time, whether any staff are mis-costed, and if there are staff deficiencies. “Drilling down” to this level of detail allows each facility to determine how best to address vacancies.
Peterson presented future opportunities, including comparing staffing to outcomes, workload-based modeling, examining workforce composition and developing management tools, understanding the impact of contract spending, specifying type of building space, and identifying industry-comparable non-VHA benchmarks. Possible
future outcome measures include key performance indicators (KPIs), a notional list of “never events,”2 critical systems maintenance, issue briefs, joint commission requirements, patient satisfaction, environment of care rounds data, closure and downtime data, and maintenance check data. In closing, he said that the VHA Engineering staffing tool is the first step in constructing a comprehensive model to investigate staffing needs and justifications, with internal benchmarking to prioritize facility resources and enhance data integrity and decision support.
Eugene Hubbard, senior vice president for human capital at RiVidium, Inc., asked how the model captures data on purchased engineering services. Eileen Moran, director, VHA OPES, anticipated that low O/E medical centers may be filling workforce vacancies with contracts but noted that this remains a gap in the model, and OPES is developing methods for better measurement. Brian Norman, chief executive officer, Compass Manpower Experts, LLC, emphasized that it would be inappropriate to reward centers that appear lean (because they outsource work) or penalize centers that appear heavy (because they have a primarily in-house workforce). He suggested adopting a cost center methodology to better understand outsourced components. Robert Goodman, principal, The Innova Group, pointed out that engineering departments pay the cost of medical maintenance contracts; while there may not be FTEs involved, government contract managers have to be included. Smith asked if a staff loss in a Category 3 unit would be higher risk than a staff loss in a Category 1 unit. Vincent Rizzo, VHA, said that any facility that does not have enough staff is at risk, no matter how complex its medical services (e.g., when the heating system needs to be repaired, engineering staff are vital to all levels of clinical care). To avoid risk, Smith advised contextualizing data for decision making. Kimberley O’Keefe, Department of the Army (ret.), wondered about the role of climate resiliency in future work. Rizzo observed that climate resilience issues are most evident in design stages, but more information is needed on new energy and water efficiency requirements and new systems that could impact staff. In response to a follow-up question from Brian Yolitz, associate vice chancellor for facilities, Minnesota State College and University System, Rizzo noted that if resilient systems are too complicated to be maintained by current staff, an additional staffing problem emerges.
VHA ENGINEERING STAFFING TOOL: IMPLEMENTATION STRATEGIES AND FUTURE OPPORTUNITIES
Broskey explained that after the engineering staffing tool is published, an implementation team will develop performance standards for each of the three functional areas of engineering and integrate a VHA-wide computerized maintenance management system (CMMS). The VA decided to adopt the Defense Medical Logistics Standard Support (DMLSS) system, which has been used successfully in the Department of Defense (DoD). DMLSS will enable the VA to use DoD’s prime vendors and replace logistics and supply chain software as well as the legacy Automated Engineering Maintenance System. He shared future plans, including defining and implementing target performance levels, analyzing links between VHA Facility Management (Engineering) staffing and performance, reestablishing the Chief Engineer Advisory Council, deploying DMLSS VHA-wide and facilitating standardization and analysis of workload, revising staffing tools annually, and continuing to have VHA support for implementation and sustainment of this effort.
IMPLEMENTATION AND ANALYSIS
Jennifer Jackson, director of connectivity, Masimo, described her experience as director of Clinical Engineering and Device Integration (CEDI) at Cedars-Sinai Medical Center, where she managed medical device systems and related
__________________
2 “Never events,” also known as “serious reportable events,” are “unambiguous, largely preventable, and serious, as well as adverse, indicative of a problem in a healthcare setting’s safety systems, or important for public credibility or public accountability” (National Quality Forum [NQF], 2011, Serious Reportable Events in Healthcare: 2011 Update—A Consensus Report, Washington, DC).
staffing, including the integration of device systems with electronic health records (EHRs) and clinical communications. Although Cedars-Sinai is small in comparison to the VHA, both systems were tasked to set enterprise-wide expectations, break down siloes, and adopt cross-collaboration. When she arrived in 2011, Cedars-Sinai used a legacy CMMS, which maintained an inflated inventory (by ~10,000) of managed medical devices. She emphasized that an updated CMMS enables true interconnection among an institution’s systems. Another obstacle she faced was that clinical operations departments each controlled their own budget, procurement, implementation, and management of technical systems. To address these challenges, Jackson (1) centralized technology management, taking a more strategic role in enterprise-wide planning and the execution of a technology roadmap; (2) consolidated more than 400 clinical applications, replacing many with Epic modules, reducing financial commitment to several vendors, and eliminating redundancies in support and system administration staffing; and (3) upgraded or replaced obsolete medical device systems. She explained that integrating medical devices increases data sharing. For example, a multi-option remote replaced the 10-year-old nurse call system—much information could be taken from this device and aligned with patient history, comorbidities, and current state to improve the nurse call system and patient care in the future.
In an effort to optimize processes, Jackson created four teams within CEDI: Clinical Technology Services, OR Technology Services, Integrated Device Systems Services, and Research and Development. While each of the four teams “owned” particular projects, she continued, these projects often overlapped with one another. Centralizing technology services reduced the risk of system downtime, because the right people were readily available to make repairs, and reduced total cost of ownership with fewer service contracts. Centralizing device integration, which was an area comprised of only one individual, made it possible to create a succession plan. Success of the implementation was evident in that technicians were focusing more on preventative maintenance and less on device repairs or troubleshooting. Centralizing technology management also led to the creation of new job descriptions such as project managers and clinical systems engineers. Other successful CEDI medical device connectivity endeavors included integrating infusions pumps with EHRs, replacing the patient monitoring platform, and sending nurse calls to smartphones. Jackson concluded that sharing information via integrated care models allows clinicians to be more effective, saves hospitals money, and leads to more lives saved.
Smith wondered about the security risks of decentralized acquisition processes. Jackson indicated that her team discovered a magnetic resonance imaging machine running Windows95 while connected to the hospital’s network as well as epilepsy monitoring systems that allowed Internet use without malware detectors. She underscored that decentralized procurement and decentralized device monitoring created this unsecured environment; clinical technology management was needed, including a team dedicated to mitigating cybersecurity risks. Jackson was asked how users perceived the transition from decentralized to centralized systems. She noticed a connection between departments with high revenue opportunity and their resistance to centralization and added that user buy-in is critical, and trust had to be gained. Smith inquired about the role of sustainment in CEDI. Jackson noted that planning and implementation, as well as application management and some day-to-day tasks, fell under Integrated Device Systems. Part of the implementation strategy involved understanding the 5- to 7-year total cost of ownership, based on maintaining systems at existing staffing levels. Broskey asked how Cedars-Sinai determined staffing requirements. Jackson commented that there was one person maintaining the nurse call system for every 200–250 beds. Owing to a dearth of benchmarking on hybrid jobs, estimations based on organizational knowledge had to be made, with the flexibility to change staffing levels over time (e.g., after 5 years of new functionalities and related troubleshooting and optimization requests).
FIRST DAY WRAP-UP DISCUSSION
At the end of the first day of the workshop, participants had an opportunity to discuss what they had heard throughout the day. Drury commended the VHA for its tremendous progress, and Smith expressed his appreciation for the VHA’s “passionate and positive” approach to staffing, which will improve veterans’ health care. Fred Switzer, professor in the College of Behavioral, Social, and Health Sciences, Clemson University, pointed out that continuous data quality monitoring will be a strength of the VHA’s endeavors. Cheryl Paullin, vice president, Talent Management & Analytics Division, HumRRO, wondered about the facility complexity model that the committee proposed, and O’Keefe agreed that facility complexity could be an important consideration for the staffing model. Broskey said that for certain areas, such as a boiler plant, staffing is straightforward; setting a baseline for the trades is more difficult. The VHA will review benchmarks and cover a bare-minimum baseline in-house for certain functions. Broskey referenced the drill down tool as a way to understand current and future baselines. O’Keefe remarked that replacing CMMS with DMLSS creates a new perspective for workload and staffing. Peterson said that the differences will be monitored over time, and he added that this transition will occur alongside modernization of the human resources (HR), financial management, and EHR systems.
FACILITY BENCHMARKING WHITE PAPER
Jake Smithwick, assistant professor, civil engineering technology and construction management, University of North Carolina, Charlotte, pointed out that all organizations are challenged by how to identify and leverage talent. He revealed that 70 percent of organizations rate facility employees that have received formal training as having significantly higher performance. And for every $2,000 that a company spends on an employee’s training, it experiences ~12 percent increase in employee performance. Ninety-four percent of organizations agree that more facilities management (FM) training is needed; yet, only 30 percent of organizations have internal FM training, he continued. Steven Call, assistant professor, construction management, Washington State University, described a current effort working with a large hospital network over six states, a group with similar staffing and training challenges to the VHA. Call’s team is creating internal training for facilities professionals, specific to the hospital network and its internal trades.
Smithwick summarized the Simplar Institute’s 2020 white paper for the consensus study committee, “Facilities Staffing Benchmark Summary Assessment,” which compared facilities staffing benchmarks as a point of reference for the VHA staffing model.3 Call explained that they reviewed presentations and transcripts from National Academies meetings as well as CAPRES facilities data; publicly available sources from academic and trade journals and professional and private organizations; and other health-care facility staffing benchmarks. He noted that VHA medical centers (on average) are ~1.2 million gross square feet, with 112 managed acres and annual planned construction of $13.5 million, and he estimated that 54 percent of VHA-owned square footage is more than 50 years old. To make better comparisons, Simplar considered infrastructure factors that the committee deemed important—department size by space use, facility condition index, average facility age, managed acres, planned construction, and unique requirements such as water purification and water treatment plants.
In 2013, the International Facility Management Association (IFMA) provided benchmarks for facility expenses; age, size, and acres managed; and staff levels and job-type mix for trade and management. In 2018, the Washington State Department of Health issued benchmarks on facility expenses and facility staff levels. The Washington State Department of Health’s benchmark of 6.7 FTE was compared to the VHA’s benchmark of 7.3 FTE (both per 100,000 gross square feet). Although the VHA’s average appears higher, he cautioned that this is not a perfect comparison when put into context—for example, the average facility size was far less for Washington State than for the VHA. Furthermore, FTE averages for the VHA vary when broken into facility complexity level—for example, FTE is often a bit higher in lower-complexity VHA medical centers. Paullin and O’Keefe cautioned that facility complexity (i.e., clinical complexity) does not necessarily equate to infrastructure complexity. Call agreed that such a distinction is important and confirmed that he considered this for the benchmarking exercise.
Call highlighted that the most important part of Simplar’s benchmarking effort was to make comparisons of equivalent work units. An IFMA benchmark (3.3 FTE) of only operations and maintenance staff included specific job types, and Simplar found that the VHA (3.7 FTE) had more tradespeople and fewer generalists in-house compared to private industry. Call added that these benchmarks are “apples-to-oranges comparisons” because the true content of FTEs is hidden in private medical facilities that outsource significant amounts of work. Smith and Drury, committee co-chairs, emphasized that if any of the benchmarking information is taken out of context, focusing only on the fact that the VHA appears to be out of line with IFMA, an ill-informed staffing decision could be made. Call reiterated that having the right context prevents quick assumptions; there are many factors to consider, and the VHA is likely understaffed. VHA’s medical centers are older and larger, which might justify the need for additional staff to address related challenges, he continued. He said that future actions for the VHA include identifying staff training needs to support a sustainable and competent workforce, evaluating facility cost benchmarks to better understand staffing-level comparisons with private medical centers, and conducting further benchmarking.
In response to a question from Smith about the trade versus generalist models of staffing, Smithwick said that although staff are highly skilled in the trade model, relying on the availability of internal experts can be difficult and expensive. The generalist model can reduce headcount and better maintain connections to external experts in emerging technologies. Call suggested that budgetary pressures and the desire for better patient satisfaction with quicker responses to less technical calls influenced the private sector to move away from the trade model. The key question for a facility is to determine whether it has enough work volume to justify the cost of a licensed electrician, for example, on staff. Drury highlighted the need to balance flexibility to quickly diagnose many kinds of problems (a generalist) with depth of expertise to solve distinct problems (e.g., plumbing, electrical, and HVAC). Call commented that many organizations use a hybrid model with both generalists and tradespeople on staff. Smithwick pointed out that in a
__________________
3 Simplar Institute, 2020, “Facilities Staffing Benchmark Summary Assessment,” white paper submitted to the Committee on Facilities Staffing Requirements for Veterans Health Administration, September 14, https://www.nap.edu/resource/25454/White%20Paper%20on%20Facilities%20Staffing%20Benchmark%20Summary.pdf.
difficult economy, it is easier to eliminate contracts than to release employees, and the ability to adapt quickly to evolving marketplace conditions is crucial. Yolitz asked how the VHA could identify and prioritize training gaps. Call suggested conducting a workforce assessment: Which workgroup is facing the most retirements, and which is the most critical? He advised working with HR to modify recruitment strategies and to develop a training program for the highest-risk units. Smith wondered about succession plans when positions cannot be advertised pre-vacancy. Call responded that job descriptions that specify required years of experience are a barrier; given the trend that people are entering the industry with less technical experience and more education, competency should determine a candidate’s eligibility instead. He advocated for new processes that recognize this trend and for an investment in training for new employees (before staff retire) to avoid outsourcing managerial roles. A participant added that it is important to determine whether the skillsets of retirees will still be needed or if new skillsets would be more useful.
STAFFING METRIC JOURNEY AT KAISER PERMANENTE NORTHERN CALIFORNIA CLINICAL TECHNOLOGY
Chris Ewing, chief operating officer, Paradigm Leaders, LLC, described the development of a staffing model for clinical technology at Kaiser Permanente Northern California (KPNCAL), which was motivated by a concern about excessive overtime (OT). He presented similarities between KP and the VA: both are large organizations with satellite locations, among which the clinical complexity varies. He said that prior to 2013, KPNCAL’s health-care technology management practices were inadequate and not standardized, and metrics were not communicated well. To understand manpower distribution across the enterprise and determine whether a perceived lack of manpower represented an actual deficit, Ewing’s team worked to identify a manning metric and establish a communication plan. Studying CMMS activity codes, Ewing’s team was disappointed to discover that of the 65.5 percent of true OT, 25 percent was expected. He highlighted the costs of improper staffing, such as equipment building up in hallways or malfunctioning equipment, and surgical procedures being compromised by heating, ventilation, and air conditioning (HVAC) issues. Addressing technician manning levels prevents poor patient outcomes, meets organizational goals, and avoids critical joint commission outcomes.
To create a staffing model, Ewing’s team worked backward from ideal outcomes to determine the staffing level needed to achieve them. Model performance measures included preventative and scheduled maintenance, customer-generated service calls, ratio of preventative maintenance to repair work orders, system downtime, cost per metric, and customer and employee satisfaction. He mentioned that self-report and observations were the only valid way to measure productivity, but some of the CMMS modules were not cataloging those data appropriately (e.g., travel time was not always included). He emphasized that the model has to take non-productive work time (e.g., meetings or leave) into account and that KPIs and never events were a means to measure the effectiveness of the model. Understanding factors such as equipment age and age of hospitals was key, but, ultimately, the cost-to-service ratio (COSR) figured most prominently into the calculation of the overall staffing metric because it presented a “uniform metric for comparison” among a broad range of hospitals. If the capital expenditure and project cost are combined, and then staffing is added, one better understands the available amount of money that can be spent—with a goal to maintain a moderate annual spend on equipment services. Ewing remarked that although staffing cannot be changed rapidly, the model helps to predict what staffing is needed. He added that it is important to consider variances (e.g., pieces of equipment used more in some locations than others) and account for outliers without losing validity.
Once the model was implemented, Ewing’s team focused on management and communication to ensure that it was understood, embraced, and sustained. Patients noticed that the hospital was quieter, technicians were not working in the hallways, and equipment was not broken as often. Rerouting staff and reducing OT increased productivity ~14 percent (averaged across modalities) and led to significant cost savings. While some service contracts were eliminated, he continued, it was more cost effective to keep others, and this staffing model is now fairly standard across KP’s network. In closing, he noted that all of the staff affected were Local 39 engineers. Despite initial resistance, with trust-building, communication, and evidence of a more fair and equitable distribution of work, the engineers accepted the project.
In response to a question from Yolitz about the Local 39’s involvement, Ewing said that he did not involve the union until he had a specific plan; then he fostered relationships and identified champions. Wesley Harris, the Charles Stark Draper Professor and Head of the Department of Aeronautics and Astronautics, Massachusetts Institute of Technology, asked about future machine learning (ML) and artificial intelligence (AI) opportunities as more high-quality data become available. Ewing replied that ML/AI allow for real-time monitoring through CMMS (e.g., dashboards with 17-second refresh rates). The combination of predictive modeling and AI provides a rapid understanding of both staff deficiencies and ideal staffing. In a data-rich environment, he cautioned against extracting performance management—productive hours do not necessarily indicate high performance. Drury asked if Ewing’s team connected modeling to
never events. Ewing noted that the downtime for critical systems decreased more than 50 percent as a result of appropriate staffing levels. In response to a question from Broskey about the relationship between COSR and staffing, Ewing explained that most practices were between 2.8 and 6 percent COSR.
PLANNING FOR SKILLED TRADES DURING IMPLEMENTATION
Cameron Oskvig, director of the Board on Infrastructure and the Constructed Environment, National Academies, described the Federal Facilities Council (FFC) as a cooperative association of federal agencies that helps to improve the planning, design, and management of federal facilities throughout their life cycle. The FFC Workforce and Organizational Performance standing committee is exploring the supply chain of skilled trades and opportunities for recruiting, retaining, and training this high-demand workforce. Responses to a 2020 survey of FFC sponsors on federal wage-grade staff training revealed a recognition of the need for wage-grade skilled trade staff (especially HVAC technicians, electricians, building automation solutions operators, and plumbers); reliance on federal job websites for recruiting; increased use of contracted services; reliance on informal upskilling and reskilling for in-house staff; balanced use of in-house and outsourced training; and perception that retirements and low wages lead to shortages.
Judie Cooper, associate director for Organizational Development, Office of Facilities Management and Reliability (OFMR), Smithsonian Institution (SI), explained that SI enables employees, through various training programs, to become experts in their current roles or to cultivate the skillsets needed for the future of SI. She noted that for every three skilled maintenance people who retire, only one person is ready to fill that role, resulting in the loss of institutional knowledge, efficiency, and stakeholder satisfaction. Yet the United States spends only $0.06 per dollar on technical education, so education in maintenance skilled trades, construction and architecture, engineering technologies and repair, and transportation is declining. To address these shortages, SI has created an independent learning organization, the Facility Management Academy (FMA). She noted that FMA vetted more than 400 learning opportunities with third-party-certified training providers to ensure that learning outcomes correspond to SI’s expectations, and all training is aligned to the Federal Buildings Personnel Training Act of 2010. Some of the training programs focus on upskilling (improving skills for a current role), while others focus on reskilling (learning skills for a new role).
Cooper described three of SI’s training programs: (1) The Bridge Program is targeted toward high-performing custodial staff with an interest and aptitude to shift to a maintenance position. SI created a general maintenance worker position through HR and identified the needed training. The first part of the program includes courses in construction orientation, math for engineers, National Association of Power Engineers “Ready to Work” training, plant equipment/operations, and schematics. After a promotion, participants take courses in AC, low-pressure boilers, plumbing, carpentry, and electric. (2) The Maintenance Multi-Skilled Training Program is for maintenance employees who are successful in their current role and wish to learn a new skill. Employees’ supervisors help to select participants, based on performance ratings, willingness to learn and teach, technical proficiency and potential, and attitude. Participants then receive an overview of the trades and choose a specialty (e.g., mechanical, electrical, and plumbing, welding, or carpentry). (3) The Apprenticeship Training Program, offered by Associated Builders and Contractors, is for current OFMR staff and includes programs for electricians, plumbers, building engineers, and cement masons—positions likely to have shortages in the next 4–7 years. The HR aspects of this program were especially challenging, she explained, because SI had to work through the Department of Labor to receive national certification. This program also requires working closely with supervisors to ensure that work assignments are consistent with learning. Post-course evaluations are collected for all three programs from students, instructors, and supervisors; each program improved morale, employee engagement, retention, maintenance, and recruitment. In closing, Cooper highlighted several other approaches to recruit skilled maintenance staff: industrial staffing agencies; programs such as the VA’s Compensated Work Therapy; technical internships for trade students; and career fairs at training programs, high schools, and trade schools, the latter of which has been the least successful.
In response to a question from Switzer about the lack of interest from trade schools, Cooper said that trade schools often focus on larger companies and students’ familial associations for employment opportunities. She tries to promote the “professional portability” of SI’s program and added that institutions that do not invest in training for employees because they do not want them to leave are making a mistake: employees might stay in one position too long and not preform quality work, and the institution will suffer. Sharon Harrington, IFMA fellow and member of the FM Pipeline National Team, explained that the FM Pipeline and SkillsUSA created a competition to raise awareness among SkillsUSA students of the breadth of FM careers available and offer small scholarships for FM-related education. In response to a question from Yolitz about training providers, Cooper shared that she has begun working on a large request for proposals for a learning management system that will accommodate all third-party certifications.
Scott Davis, managing director, Government Integrated Facility Management (IFM)–Public Institutions, JLL, oversees state, federal, and local IFM contracts, which have diverse geographic locations, trades, and construction
activities. Most of the contracts endure from one period to the next, adding stability within the FM-skilled workforce. His organization maintains military, university, and federal campuses and often works with unions—the source of a well-trained, skilled, and readily available workforce. When his organization has a vacancy, it coordinates with the union to write the job description and identify the right candidate. He explained that it is often easier to recruit a workforce in cities, which are densely populated and have public transportation near union halls and training programs; what is more difficult is recruitment near remote military bases, where there is limited access to skilled labor. Statewide contracts present challenges as well, because skilled workers rarely relocate for work. However, the most pressing obstacle is when a government employer has lower wages than the local market standards. He suggested offering slightly more than the prevailing wage to avoid labor shortages.
Davis pointed out that the COVID-19 pandemic has impacted the industry, as former hospitality staff have been hired, for example, in the commercial real estate industry. As hospitality firms raise wages to re-attract this workforce, he continued, the commercial real estate industry will have to increase wages to compete. Other industry trends include technical high school students pursuing work in the computer industry rather than in the trades. Davis described this as a systemic problem and noted that better recruiting efforts before these students make decisions about postsecondary education would allow them to see all of the trade opportunities available. However, he asserted that trade schools are not teaching modern equipment skills (e.g., high-end sensor technology), so it may be difficult for those people to find jobs. The carpentry, painting, plumbing, and flooring workforce remains prevalent; the greatest shortage is for high-end HVAC and elevator maintenance.
Harrington asked where people are learning modern technology skills. Davis replied that they join companies at a lower skill level, leave for a higher-paid job that offers a training program, and return as specialty subcontractors. However, because modern technologies dominate facilities, he said that it would be preferable (although more costly) to keep this workforce in-house. William Marras, the Honda Chair Professor in the Department of Integrated Systems Engineering, Ohio State University, wondered if database maintenance would be considered a trade skill in the next 5–10 years. Davis remarked that as organizations invest more in data management strategies, the candidate pool will shift accordingly. The skilled workforce has to understand both the equipment it maintains and the CMMS. He added that those who are not tech-savvy and are competing against a younger generation can be trained to use the technology and become more efficient. He advocated for the allocation of resources to address this “infusion of new technologies.” Drury questioned whether there is federal or state support to recruit skilled workers. Davis indicated that the United States has more than 100 Job Corps centers, organized by the Department of Labor. These centers have multiple skilled trade schools at each location; however, they are not well advertised and are thus not well connected to the marketplace. Goodman asked about advice for staffing amidst the reluctance to travel. Davis suggested recruiting people leaving the military, who are accustomed to moving and have strong job skills. He noted successful engagements with Hiring Our Heroes and the Wounded Warriors Project.
DISCUSSION OF MODEL AND IMPLEMENTATION AND KEY THEMES
Smith asked Broskey about VHA’s plans for its future technical workforce. Broskey described an existing program that certifies construction managers as well as the Technical Career Field Intern Program for engineers, safety professionals, and boiler plant operators. He recognized an opportunity for the VHA to expand its training opportunities. Smith suggested creating a task force to review this issue but noted unique challenges, given that VHA’s workforce is spread across the country. In closing, Smith described three themes emerging from the workshop: the value of accurate and actionable data, the significance of benchmarking, and the importance of change management systems. He reiterated the value of capturing service contract spending in future modeling efforts but emphasized VHA’s remarkable progress in implementing the consensus study report’s findings and recommendations. Broskey acknowledged that many challenges lie ahead and that a sustained effort will be needed, but he noted that the VHA is beginning to achieve its vision with the creation of these tools.
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Linda Casola as a factual summary of what occurred at the meeting. She was assisted by Daniel Talmage and Heather Kreidler. The committee’s role was limited to planning the event. The statements made are those of the individual workshop participants and do not necessarily represent the views of all participants, the planning committee, or the the National Academies of Sciences, Engineering, and Medicine.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed in draft form by David Nash, Dave Nash & Associates International, LLC; Brian Norman, Compass Manpower Experts, LLC; and Fred Switzer, Clemson University. The review comments and draft manuscript remain confidential to protect the integrity of the process.
PLANNING COMMITTEE: Co-Chairs James B. Smith, U.S. Ambassador (retired), and Colin Drury, SUNY Distinguished Professor Emeritus; Brian Yolitz, Associate Vice Chancellor for Facilities, Minnesota State College and University System; and Cheryl Paullin, Vice President, Talent Management & Analytics Division, HumRRO.
STAFF: Cameron Oskvig, Director, Board on Infrastructure and the Constructed Environment; Daniel Talmage, Program Officer, Board on Human-Systems Integration; and Joe Palmer, Senior Program Assistant, National Materials and Manufacturing Board.
SPONSOR: This workshop was supported by the Veterans Health Administration.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2021. Testing and Validating the Staffing Methodology for the Veterans Health Administration: Proceedings of a Workshop—in Brief. Washington, DC: The National Academies Press. https://doi.org/10.17226/26300.
Division on Engineering and Physical Sciences

Copyright 2021 by the National Academy of Sciences. All rights reserved.









