5
Criterion 1: The Match Between Program and Consumer
Our first criterion for evaluating the outcomes of obesity treatments focuses on the issue of the match between person and treatment. That is, in seeking to establish criteria, we are faced with two questions: (1) How can we predict with any degree of precision which individuals will succeed in a given treatment program? (2) Are some programs suitable only for certain people, where suitability includes both the probability of success and the level of risk associated with undertaking the program? Answering these questions requires examining how individuals and treatments are matched, which is the subject of this chapter. We have deferred the issue of program safety, a critical component of matching, to the following chapter on the soundness and safety of weight loss programs.
The issue of matching patients to treatment has long been a key aspect of medical treatment. This matching has traditionally been carried out by the practitioner, who follows his or her diagnosis with the treatment that he or she has found to be most specific and efficacious for the disorder under consideration and to have the fewest adverse effects. With the rise of specialization and the increase in available treatment options, the issue of matching has moved from the intuitions of the individual practitioner to systematic efforts at the level of theory and research to match disorders to treatments.
The field of alcoholism provides useful examples of matching patients to treatments (IOM, 1990). Recognizing that one uniform treatment program was unlikely to be appropriate for all patients, Bowman and
Jellinek as far back as 1941 advocated the matching of patients and treatment; by 1950, an experiment in matching patients to four treatment programs had been carried out (Wallerstein, 1956). Since then, research in treatment matching in alcoholism has accelerated, and several reports have defined many of the relevant matching variables (IOM, 1990). The field of obesity has lagged behind that of alcoholism in considering the matching of patients to treatments, probably as a reflection of the fact that self-treatment (i.e., voluntary dieting and exercise) is widely practiced and thought to be generally applicable to most obese people.
SCHEMES FOR MATCHING IN THE OBESITY FIELD
It was not until the early 1980s that the first efforts at matching in obesity were reported. In 1981, Garrow proposed a system of classification of obesity as the necessary precondition for matching, together with treatments appropriate for the different ''grades" of obesity. Garrow's classification was based on the body mass index (BMI) and divided obese persons into four groups: (1) Grade III, BMI > 40; (2) Grade II, BMI 30–40; (3) Grade I, BMI 25–29.9; and (4) Grade 0, BMI 20–24.9. Treatments were prescribed according to the grade of obesity, from surgery for Grade III, through dietary measures of greater or lesser stringency and the possible use of medication for intermediate grades, to reassurance about body weight for Grade 0.
Independent of Garrow, Stunkard (1984) proposed a similar matching scheme. His classification also divided obese persons on the basis of their weight, defining mild obesity as a percentage of overweight of less than 40, moderate obesity as 40–99 percent overweight, and severe obesity as 100 percent or more overweight. He matched these levels of obesity with treatment, recommending that severe obesity be treated with surgery, moderate obesity with diet and behavior modification under medical supervision, and mild obesity with behavior modification under lay auspices, as carried out by some commercial organizations.
A third effort at matching in obesity was published by Brownell and Wadden (1991). In this model, the authors divided obesity into four levels, once again assessed only in terms of percentage of overweight. The authors provided a greater number of treatment options, however, divided into five "steps" moving from self-directed diet programs and self-help groups for the thinnest persons (5–20 percent overweight) to, as in the earlier schemes, surgery for the most obese (at least 100 percent overweight). Furthermore, they provided a list of individual factors and program factors to be used in the matching decision. The model is shown in Figure 5-1.
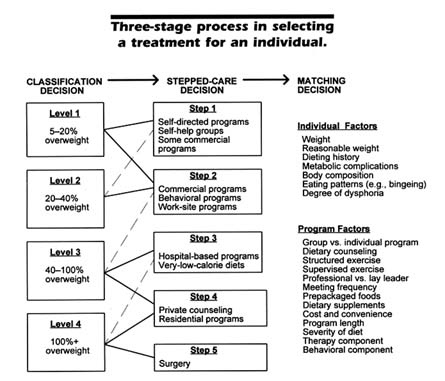
FIGURE 5-1 The classification decision divides individuals into four levels according to percentage of overweight. These levels dictate which of the five steps would be reasonable in the second stage, the stepped-care decision, on the principle that the least intensive, costly, and risky approach will be used from among alternative treatments. The third stage, the matching decision, is used to make the final selection of a program and is based on a combination of client and program variables. The dashed lines between the classification and stepped-care stages show the lowest level of treatment that may be beneficial, although more intensive treatment is usually necessary for people at the specified weight level.
SOURCE: Adapted from Brownell and Wadden, 1991. Reprinted with permission of the Association for Advancement of Behavior Therapy.
Another approach to model construction was that of Bray, who added comorbidities to the degree of overweight in assessing the risks of obesity. In this model, an individual is placed in a risk category based on BMI and the presence or absence of "complicating factors," which include obesity-related comorbidities such as hypertension and hyperlipidemia as well as other factors indicating risk, such as a high waist-to-hip ratio and onset of obesity before 40 years of age. For example,
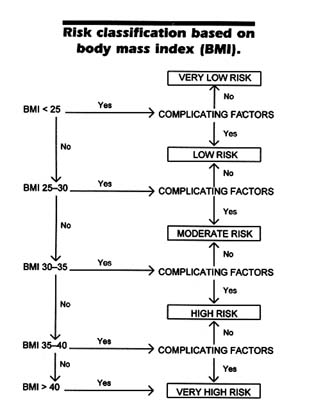
FIGURE 5-2 The presence or absence of complicating factors determines the degree of health risk. Complicating factors include an elevated waist-hip ratio, non-insulin-dependent diabetes mellitus, hypertension, hyperlipidemia, male sex, and age younger than 40 years. Copyright 1987 by George A. Bray. Used with permission.
an individual with a BMI of 34 is at "moderate risk" from his or her obesity without any complicating factors, and at "high risk" if one or more such factors are present. The Bray model is shown in Figure 5-2.
The evolution of matching schemes in the field of obesity has moved from the so-called static ones of Garrow, Stunkard, Brownell and Wadden, and Bray toward a more dynamic stepped-care model that prescribes the steps to be undertaken in arriving at a treatment decision. Stepped-care models are used in the treatment of hypertension (NHBPEP, 1993) and hypercholesterolemia (NCEP, 1993). They are based on the premise that the least invasive and costly treatments are applied during the earliest manifestations of progressive chronic conditions, especially when these conditions are not yet associated with any medical complications.
Stepped care also assumes that treatment is cumulative or incremental—in other words, that nothing is lost by instituting a less aggressive or intensive treatment at an early stage and that, even if not sufficient, this treatment (e.g., diet therapy) can provide a foundation for therapies (e.g., use of drugs) that are added subsequently.
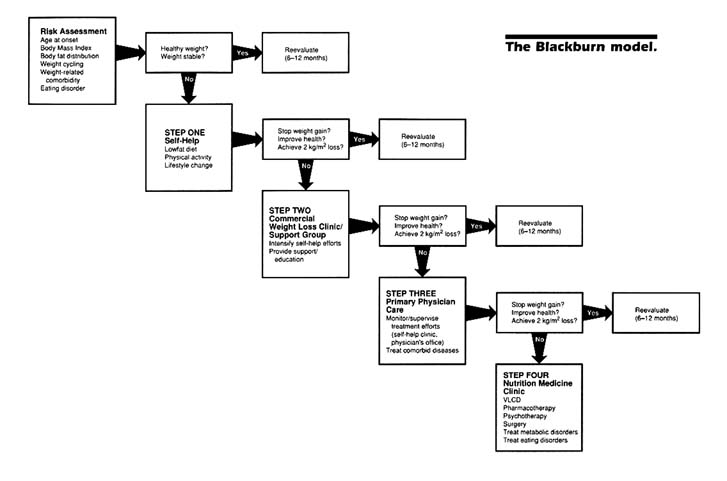
At our request, Dr. George Blackburn prepared a stepped-care model for obesity treatment that we hoped would help us in developing our criteria for the evaluation of weight-management programs. His model, shown in Figure 5-3, is based on one developed in 1978 (NAS, IOM Ad Hoc Advisory Group on Preventive Sciences, 1978) and includes a four-step treatment. In the model, all individuals assessed to be at risk participate in Step One over a 3- to 6-month treatment phase. Risk assessment involves identification of characteristics known to place individuals at increased risk for obesity-related morbidity and mortality. The goals in the Blackburn model include stopping weight gain and/or effecting a weight loss of 2 BMI units (approximately 10 pounds), while at the same time incorporating healthful lifestyle changes and improving the quality of life. This can be done largely through a self-help approach. Provisions are made for adjunctive therapy with "step-down" protocols to comply with a long-term program of nonpharmacologic, lifestyle treatment.
Participation in Step Two requires screening by the patient's primary-care physician. Patients are then referred to certified commercial weight-loss clinics (as defined by the New York City Division of Consumer Affairs in Winner [1991]) or support groups. Again, the goal is to stop weight gain and/or achieve a weight loss of 2 BMI units while incorporating healthy lifestyle changes and improving overall quality of life.
Step Three includes monitoring and supervision if the patient is at high risk for comorbid disease. Intervention is still via self-help, a commercial weight-loss clinic, or a primary-care physician. Additional goals include ameliorating obesity-related disease, achieving a 2–4-BMI-unit weight loss, and continuing weight loss until a healthy body weight is achieved.
Step Four is the most aggressive of the interventions. Intensive therapy can include the use of very-low-calorie diets (VLCDs), medication, surgery, and psychotherapy as necessary and appropriate. In addition to goals for Steps One through Four, an added goal is a 30–50 percent reduction of excess body fat with concomitant achievement of metabolic fitness.
THE INDIVIDUAL BASIS FOR MAKING DECISIONS
Another way to approach the matching of individuals with treatments is to identify important factors that may influence decisionmaking. We have identified three sets of such factors: (1) personal, situational, and global factors; (2) health status and weight-related risk factors; and (3) information and guidance.
Personal factors include demographic ones, such as age and gender, that cannot be changed, as well as psychosocial ones, such as motivation and readiness to change, that one can alter. Situational factors can be changed by the individual's actions; an example is using the stairs whenever appropriate rather than the elevator. Finally, global factors are those that influence the environment in which an individual lives, such as culture and views about weight; they typically change slowly over time from the efforts of large numbers of people. The ready availability and cost of a weight-loss program are two global factors that often influence a person's decision about whether or not to undertake a particular weight-loss program.
Health status and weight-related risk factors are factors that, as they worsen, may become an individual's primary motivation for losing weight. However, concerns about appearance are usually given by individuals seeking a weight-loss program, and these may conflict with actions taken on the basis of health-related considerations. For example, health considerations generally support small incremental weight losses to a level likely to be maintained over the long term, while appearance considerations predispose many to try repeatedly to achieve large weight losses at a rate requiring an unhealthy and ultimately unsustainable level of caloric restriction. Health considerations will argue against weight loss by those who consider themselves to be overweight but are not so by standards described in Chapter 2. There are strong reasons why health status should take precedence, especially in those at risk for comorbid conditions by family history or prior morbidity or those in whom comorbid conditions (e.g., diabetes, dyslipidemias, hypertension, sleep apnea, and osteoarthritis) are already present (see Chapter 2). Individuals should pay particular attention to their weight if they have a family history of premature comorbidities, increased visceral fat as indicated by waist-to-hip ratios in men of >1.0 and in women of >0.8, or BMIs associated with increased risk (>25 with one or more comorbid conditions and >27 without a comorbid condition).
Information and guidance come from a variety of sources, including the media (information and advertising); family, friends, and acquaintances
(who relay their opinions and experiences with the various options); and health-care providers. The information and guidance may be sound or unsound, well intentioned or intended to deceive, and empowering or provoking inaction. They may also be incomplete or biased toward a particular program or approach that may not be suitable. Our recommendations for program disclosure presented in Chapter 8 are designed to increase the chances that individuals will receive a balanced and complete picture of the potential benefits and risks of each weight-loss option.
CONCLUDING REMARKS
In some cases, it is possible to identify mismatches of individuals with weight-loss programs, at least in the sense of excluding people from particular options. For example, a healthy young woman with a BMI of 28 is no candidate for gastric surgery, while a very obese male with a BMI of 40 and hypertension—who has not lost weight despite many attempts—is not likely to be helped by a do-it-yourself diet book or exercise video. However, for most people who wish to lose weight, there is general agreement that it is not yet possible to match people with programs to significantly improve their chances of success. There has yet to be an empirical demonstration of the effectiveness of matching individuals with obesity treatments (Wilson, 1994b).
As the matching approaches described in this chapter indicate, we have some knowledge about components of the match and their association with successful weight management to make prudent recommendations. An individual with weight-related comorbidities, for example, should be encouraged either to choose a program with medical management or to be monitored by a physician throughout the program chosen. (See also Chapter 7 in which predictors for successful weight loss and maintenance are identified.) However, matching people to programs successfully will require a much better understanding of how individuals come to choose from among the options available and the characteristics of programs. This is a very important area for future research.