7
Criterion 3: Outcomes of the Program
This chapter focuses on our third criterion for evaluating the outcomes of obesity treatments: the nature of the outcomes themselves. Obesity treatment typically includes short-term efforts to reduce weight or curb weight gain. But because most people regain lost weight over time, true success must be based on long-term weight loss or weight control (i.e., maintained over 1 or more years). The weight range (expressed in pounds or a percentage of initial weight) considered to represent successful weight loss is variable. Chapter 2 provides several sets of recommendations for desirable weights.
Characterizations of weight-loss outcomes also differ, depending, for example, on the amount of total weight loss relative to initial weight, weight goals, and the time when weight maintenance actually begins (see Figure 7-1). Further, defining what constitutes successful weight loss in particular cases involves specifying time frames, individual characteristics, and any special conditions under which treatment was conducted. Since most individuals in the United States become heavier with age, considerations regarding whether the common tendency to gain weight has been affected should not be overlooked. The question of whether individuals who regain some or all of the weight lost in treatment would be considerably heavier had they not lost weight in the first place is of critical interest. These issues influence the definition of what specifically constitutes successful weight maintenance, and to the extent that they need further study and refinement, our discussion of predictors of successful weight loss and maintenance is limited.
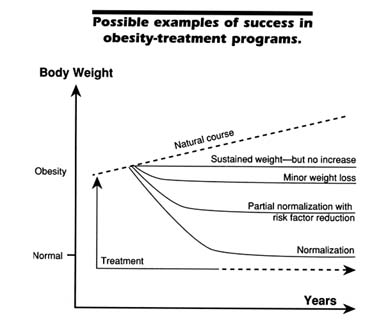
FIGURE 7-1 Adapted from Rössner, 1992.
This chapter summarizes the factors correlated with obesity-treatment outcomes. We discuss these factors in terms of providing recommendations for both obesity treatment and research, but for the reasons that follow, we have not incorporated them directly into our criteria for evaluating weight-management approaches.
Currently available obesity treatments are not producing the desired long-term outcomes for most dieters, so the predictors of favorable outcomes remain unknown. Most of the relevant information is based on results from clinical or research programs. Therefore, the available information on predictors of weight maintenance is most relevant to individuals who enroll in these programs, continue to attend the programs once enrolled (i.e., do not drop out after a few treatment sessions), and have follow-up assessments of weight change and associated variables. It is important to point out that such individuals probably do not represent those in the general population who are overweight or even those motivated to lose weight (Brownell, 1993), if only because they do not have access to such programs. More saliently, they may include a high proportion of persons who have failed on their own or in commercial programs and who thus may be less predisposed either physiologically or psychologically to achieve long-term weight maintenance (Brownell, 1993).
In addition to the limitation of using a database for a unique and poorly defined subset of the population, our understanding to date of successful weight management is further limited by its being based on studies in which the treatment approaches may have been less than ideal (e.g., separating weight management into discrete phases of weight loss and maintenance) and in which the outcomes used to evaluate success may not have been appropriate (e.g., reaching an ideal weight).
Predictors of successful weight management may differ in future studies that use different weight-management approaches, in particular, the components of the broader definition of success recommended toward the end of this chapter. The following review is limited by the existing literature, which has used the more narrow definition of success at weight management—simple weight loss.
PREDICTORS OF WEIGHT LOSS
Factors that predict weight loss are shown in Table 7-1; these include personal, process, and treatment factors. Personal and process factors pertain to an individual; treatment factors pertain to a program.
Personal Factors
Personal factors include initial weight or body mass index (BMI) and resting metabolic rate or resting energy expenditure (REE). The greater the initial BMI, the greater the initial weight loss. Additionally, although REE is most directly related to lean body mass, total weight affects REE as do age, gender, and height. Those with higher REE have higher energy requirements, facilitating more weight loss proportionate to intake. Adipose hypercellularity, usually associated with excessive deposition of fat cells in childhood, has been associated with greater weight loss. However, when the lower limit of adipose cell size is reached, further weight loss is difficult, often leaving the person still obese. Another problem is that the smaller fat cells may produce more lipoprotein lipase, which may stimulate hunger and facilitate increased fat deposition (Kern et al., 1990). Because it is difficult to measure fat cell number, estimates of percentage of total body fat and body-fat distribution are more useful measures for assessing progress (Perri et al., 1992). Although body-fat distribution is not a clear predictor of weight loss, women with upper-body obesity may be more likely to improve their waist-to-hip ratio (WHR) with weight loss, while the WHR for women with lower-body obesity tends to remain constant with weight loss (Wadden et al., 1988).
Self-efficacy is a person's confidence in his or her ability to perform a given task or achieve a certain goal. Higher perceived self-efficacy in
TABLE 7-1 Predictors of Weight Loss
|
POSITIVE PREDICTORS |
|
Personal Factors High initial body weight or body mass index High resting metabolic rate or resting energy expenditure High perceived self-efficacy Process Factors Attendance at program Experiencing weight loss early in program Treatment Factors Increased length of treatment Having social support Engaging in physical activity Incorporation of behavior modification techniques Self-monitoring Goal setting Slowing rate of eating |
|
NEGATIVE PREDICTORS |
|
Repeated attempts at weight loss Experiencing perceived stress (Others include the opposites of the positive indicators) |
|
NONPREDICTORS |
|
Total body fat, fat distribution, and body composition Personality/psychopathology test results Dietary restraint Binge eating |
|
NOTE: With the exception of resting metabolic rate, the absence of metabolic and physiological factors as predictors of weight loss is not an oversight. The measurement of metabolic factors is beyond the practice of the vast majority of obesity-treatment programs, and it is not surprising that data are not available. It is likely that with additional research, some factors can be identified. For example, although adipose tissue lipoprotein lipase (LPL) activity is increased in obesity, there are no studies identifying LPL activity as a predictor of weight loss. Future studies are needed to identify metabolic and physiologic predictors of weight loss (see Chapter 10 ). SOURCES: Brownell and Wadden, 1992; Foreyt and Goodrick, 1991, 1994; O'Neil and Jarrell, 1992; Perri et al., 1992; and Wadden and Letizia, 1992. |
weight management has been found to predict greater weight loss (Oettingen and Wadden, 1991). Assessing self-efficacy before weight-loss treatment begins and applying cognitive-behavioral methods to increase low levels may increase overall response to treatment.
Further research is needed to determine how apparent self-regulatory
deficits in eating control and dieting behaviors affect success in weight management (Wilson, 1993). Although dietary restraint and binge eating have been reported as factors that reduce success in weight-loss programs, results are conflicting (Wadden and Letizia, 1992).
Process Factors
Process factors include attendance and early weight loss. Attending intervention classes has consistently been shown to be related to weight loss. Early weight loss in programs is related to final weight loss as well as to attendance (Wadden and Bell, 1990). However, some speculate that a higher level of early weight loss, especially if the final attained weight is too low, may increase the likelihood of relapse. Alternatively, smaller changes in weight reflecting gradual changes in eating and exercise habits may ensure better maintenance (Goodrick and Foreyt, 1991). Small initial weight losses have been related to early dropout for females in very-low-calorie programs (Wadden et al., 1991). A client may leave a program out of frustration, or leaving may reflect insufficient motivation. Counseling clients to accept a slower rate of weight loss may result in better treatment retention. Some believe that large changes in lifestyle lead to better success at long-term weight management (see, for example, Ornish, 1993), but there are no studies to support this view.
The correlation between attendance and weight loss seems obvious, but both factors may be influenced by a third one, such as increased motivation or fear. Table 7-2 lists those factors that have been reported to be correlated with attendance in weight-management programs. Age, weight, percentage of body fat, mood, and age of onset of obesity have not been linked with attendance. Excessive stress from life difficulties predicts early dropout and weight regain (Wadden and Letizia, 1992).
A feeling of lethargy is associated with obesity (Sims, 1988; Thompson et al., 1982). This lack of energy is expected to be related to poorer attendance at, and adherence to, a weight-loss program, and this has been found in one study (Pekarik et al., 1984). Excessive use of caffeine to feel more energetic while on restrictive diets has been observed. Future research should evaluate the efficacy of monitoring perceived energy level while paying special attention to behaviors that affect energy expenditure (e.g., sleeping patterns, physical activity, and intake of specific foods and beverages). A gradual approach to exercise or increasing physical activity focused on boosting perceived energy could prove to be efficacious.
Most behavioral treatment programs use closed groups (i.e., groups that form at the beginning of a program and stay together throughout treatment without new members joining). Attrition rates in such programs
TABLE 7-2 Predictors of Attendance in Weight-Management Programs
|
POSITIVE PREDICTORS |
|
Closed-group classes Use of refundable deposits Perceived health improvement |
|
NEGATIVE PREDICTORS |
|
Stress Small initial loss Low perceived energy |
|
NONPREDICTORS |
|
Age Beginning weight Percentage of body fat Mood Age of onset of obesity Hunger susceptibility |
|
SOURCES: Foreyt and Goodrick, 1991, 1994; Perri et al., 1992; Rössner, 1992; and Wadden and Letizia, 1992. |
average about 13 percent, compared to dropout rates of up to 70 percent in some commercial programs using open groups (i.e., groups that allow participants to attend any time during treatment) (Volkmar et al., 1981). Closed groups may help build group cohesiveness and may allow for a scheduled treatment protocol. In addition, open groups tend to be larger than the 8- to 12-member classes in typical behavioral treatments.
Weight loss and attendance can be improved through the use of refundable deposits. Several studies evaluating the effectiveness of programs requiring strong monetary contracts for weight loss or dietary compliance have shown that these procedures enhance weight loss compared to programs that have similar educational content, but in which participants are encouraged to develop contracts on their own (Jeffery et al., 1978, 1983, 1984a). Similarly, attendance and attrition can be improved by having the participants deposit money that is refundable upon completing treatment. Use of such deposits can keep attrition rates below 10 percent (Wilson and Brownell, 1980).
As described in Chapter 2, small weight losses can lead to improvements in health risks. Perceived benefits of this type have been observed to improve the motivation and attendance of those whose rate of weight loss is not as fast as expected (Foreyt, 1987).
Treatment Factors
The numerous aspects of provider behavior and program content and process that may influence both the enrollment of clients (i.e., which kinds are attracted to the program) and the outcomes of treatment have not been well studied (Blackburn, 1993; Wadden, 1993). However, some program variables are consistently related to outcomes. Length of treatment predicts weight loss. This is shown, for example, in a study where increasing the treatment length from 20 to 40 weeks increased weight loss from 10.5 kg at week 20 to 13.5 kg at week 40 (Perri et al., 1989). Social influences from therapist contact and peer support may be partly responsible for this result, apart from the effect of the client's receiving extended training in behavioral self-management methods. Control over eating and exercise may be improved when individuals rely on peers to get them through situations involving temptations (Goodrick and Foreyt, 1991). Using peer-influence processes such as group problem solving and telephone contacts improves long-term weight management (Perri et al., 1992).
Studies investigating the effect of exercise on weight loss have reported mixed results (Wadden and Letizia, 1992). However, exercise has been shown to be one of the best predictors of maintenance, so it makes sense to emphasize its importance during treatment and follow-up. Exercise may improve body composition and blood lipid profiles (Blair, 1993a; Uchino et al., 1991) as well as reduce stress and improve well-being. These health factors should be further researched and promoted for successful weight management.
Self-monitoring (i.e., the recording of dietary intake and exercise) is the cornerstone of behavioral treatment and has been correlated with success (Perrri et al., 1989). While the information feedback from this process appears to be highly useful in treatment, it is difficult to determine whether self-monitoring is a cause or correlate of good results.
Goal setting in terms of eating, exercise, and weight goals has also been correlated with success at weight loss (Bandura and Simon, 1977; Dubbert and Wilson, 1938). This activity goes together with the concept of making gradual, incremental changes to ensure success. Slowing the rate of eating is also correlated with successful weight management (Speigel et al., 1991).
PREDICTORS OF WEIGHT-LOSS MAINTENANCE
Maintenance of reduced weight is the most difficult aspect of long-term treatment. Interventions that provide clients with a "maintenance" program produce better maintenance of weight loss than those without a
follow-up program (Björvell and Rössner, 1992; Perri et al., 1988). The expectation of the client, and often the claim of weight-loss programs, is that all excess weight will be lost and the new weight maintained. The reality is that most treated individuals gradually return to their original weight following treatment. Keesey (1989) has argued that just as a thermostat maintains room temperature, a person's metabolism maintains body weight at a set level. In this "set-point" theory, obesity is seen as a normal state for some individuals, and lowered weight gradually returns to its natural level through metabolic regulation. For persons with naturally high set-points, successful maintenance probably requires them to commit to a diet that supplies less than needed to satisfy hunger. We believe that goals for weight maintenance should also include delaying weight regain or maintenance of smaller weight losses.
Regain is a complex phenomenon and may be facilitated by biological factors causing a disorder of energy metabolism (Hirsch and Leibel, 1991), by psychological factors such as interpersonal problems leading to uncontrolled eating (Grilo et al., 1989; O'Neil and Jarrell, 1992), by family dysfunction (Fischman-Havstad and Marston, 1984), or by other problems (see Table 7-3). For many people, life in this country is conducive to obesity and to regain after treatment, given the abundance of food, wide availability of high-fat products, and limited opportunities for exercise (Brownell, 1991b; Brownell and Wadden, 1991; Rodin, 1993).
Physical activity is a strong predictor of maintenance of weight loss.
TABLE 7-3 Predictors of Maintenance of Weight Loss
|
POSITIVE PREDICTORS |
|
Physical activity Self-monitoring Positive coping style Continued contact Normalization of eating Reduction of comorbidities |
|
NEGATIVE PREDICTORS |
|
Negative life events Family dysfunction |
|
NOTE: As with Table 7-1, there are no physiological and metabolic factors listed as predictors of maintenance of weight loss. There are not sufficient data to include these factors, making this a future research need (see Chapter 10). SOURCES: Foreyt and Goodrick, 1991, 1994; Perri et al., 1992; and Wadden and Letizia, 1992. |
For example, one study of municipal employees in a supervised exercise program consisting of three weekly 90-minute aerobic sessions found that subjects who stopped exercising began to regain lost weight, while other subjects who had not been exercising began to lose weight when they joined the exercise program (Pavlou et al., 1989). Several positive psychological effects of exercise may have implications for long-term adherence and weight maintenance in the obese. Inferences drawn from clinical experience and data from several studies support the conclusion that the psychological effects of exercise may be the important mechanism, although physiological mechanisms linking exercise to weight control are certainly significant (Grilo et al., 1993a). Higher levels of physical fitness predict more positive mental health, with enhanced self-concept and general self-efficacy and reduced anxiety, stress, and depression (Grilo et al., 1993b). If subjects perceive that these benefits are caused by exercise, they may be more likely to continue physical activity and thus have better weight control. Research is needed to discover ways to increase exercise itself and adherence to physical activity in the obese, and to study how exercise and its psychological effects interact to promote a more physically active lifestyle. One promising approach that might appeal to the obese is home-based exercise programs that can generate adherence rates equal to or better than group exercise classes (King et al., 1993).
Individuals who confront life stressors with a positive, problem-solving attitude are more likely to have greater success in any endeavor, including weight management (Kayman et al., 1990). Self-monitoring and continued contact with therapists and peers are also correlated with successful maintenance (Perri, 1992).
POPULATION CHARACTERISTICS AS PREDICTORS OF WEIGHT MANAGEMENT
Many of the predictive factors in Tables 7-1, 7-2, and 7-3 vary by population characteristics. This variability can account for differences in rates of successful weight management across population subgroups. However, as pointed out earlier, data based on clinical or research programs may not describe the situation in the general population, because only a small percentage of the population enrolls in formal programs (Jeffery et al., 1984a; Levy and Heaton, 1993). Weight management in the general population may be better than one would expect on the basis of the obesity-treatment literature. The high and increasing prevalence of obesity, however, argues against the assertion that successful weight management is widespread in this country. In any case, the characteristics of individuals that identify groups having a higher- or lower-than-average
tendency to gain weight or a greater difficulty in losing weight may be useful for general guidance in designing programs for various population subgroups. These variables may also provide a basis for identifying the mechanisms that predispose individuals in these groups to a given weight-gain profile.
Gender
Gender is the population variable most strongly associated with weight maintenance. Women enter adulthood smaller than men but have a greater predisposition to weight gain and more variability in their adult weight status compared to men (Williamson, 1993; Williamson et al., 1993). Female reproductive variables are among the obvious potential candidates for causes of weight gain in young adult women. Menopause does not appear to be associated with weight gain independent of the age differences between pre- and postmenopausal women, although hormone replacement therapy may be linked to greater weight gain (Wing et al., 1991b).
Several lines of evidence indicate that weight-loss motivations for men and women differ in their nature and intensity. Dieting is more prevalent among women than among men, and more women enroll in obesity-treatment programs. Women are more motivated to diet to improve their appearance, while men are motivated more by health and fitness concerns. However, many studies find that success rates in weight-loss programs vary by gender, with women experiencing smaller weight losses than men (Adams et al., 1986; Kramer et al., 1989; Kumanyika et al., 1991; Lavery and Loewy, 1993; O'Neil et al., 1979; Stevens et al., 1993; Wing et al., 1987). National survey data suggest that men and women use different weight-loss strategies when dieting (Levy and Heaton, 1993), and abnormal-eating behaviors, which may be causes or consequences of unsuccessful dieting, are more prevalent in women (Connors and Johnson, 1987; Rand and Kuldau, 1992). Gender differences in exercise patterns may also affect success. Rössner (1992) suggests that the higher lean body mass of men, overall and at any given body weight, could be one factor in men's greater weight loss. The predominance of easier-to-mobilize abdominal, compared to gluteal-femoral, fat could be another factor. Men also have higher energy requirements and could, theoretically, undertake caloric restriction over a wide range of intakes. Overall, whether gender differences in obesity treatment outcomes can be explained by careful adjustment of known determinants of weight loss is unclear. This is an important area for future research.
Age
Several weight-loss predictors are associated with age or aging. Age, therefore, potentially confounds many associations of other population characteristics with weight-management variables. The average pattern of weight change shifts from a tendency to gain weight in youth and middle age to a net loss of weight after age 50 or 60 (Williamson et al., 1990). However, decreases in lean body mass and metabolic rate that occur with aging in most older adults may decrease their ability to lose weight when they attempt it (Tzankoff and Norris, 1977; Vaughn et al., 1991). The prevalence of dieting decreases as age increases (Piani and Schoenborn, 1993; Schoenborn, 1988), but at least two surveys indicate that the duration of dieting among persons trying to lose weight is longer in older persons (Levy and Heaton, 1993; Williamson et al., 1992). Sedentary behavior, health problems, and functional limitations increase with aging (King et al., 1992). Thus, older persons who enroll in treatment programs may be less likely to adopt or adhere to exercise regimens. Motivations for weight loss at older ages may shift more toward concerns for health instead of appearance (Hayes and Ross, 1987).
Race, Ethnicity, and Socioeconomic Status
Although obesity among whites varies with demographic categories and may be related to ethnic origins, the high prevalence of obesity in several racial/ethnic minority populations in the United States is striking, especially among women (Kumanyika, 1994). Obesity affects up to 80 percent of adults in some age groups among black, Hispanic, Native American, and Pacific Islander populations. The high prevalence of obesity in these populations, compared to less overweight populations, may reflect greater problems with avoiding weight gain or with losing weight. Associations of race/ethnicity with weight may include the effects of low socioeconomic status (which predisposes females to obesity) (Sobal and Stunkard, 1989), pregnancy-related weight gains (Dawson and Thompson, 1990), dieting motivations and practices, lower levels of leisure-time physical activity (King et al., 1992), and residence in the southern United States (Piani and Schoenborn, 1993; Schoenborn, 1988).
Stress, which was noted earlier in this chapter as a negative predictor of weight loss, may predispose susceptible individuals to abdominal obesity through negative health-related behaviors and neuroendocrine disturbances (Björntorp, 1993). Race, ethnicity, and low socioeconomic status are associated with numerous potential sources of stress (e.g., discrimination, living in substandard housing, and being unable to afford basic necessities). However, whether excess stress is a mediator of these
demographic factors on weight management is not known. The subjective elements of perceived stress (i.e., the threshold above which stress is perceived or the importance assigned to a given stress) are influenced by culture (Dohrenwend et al., 1978). This complicates cross-cultural comparisons of the prevalence of stress or of its effects.
Studies that provide a randomized, controlled comparison suggest that black women or black participants in the United States lose less weight than whites under the same conditions of behavioral treatment (Kumanyika et al., 1991; Wylie-Rosett et al., 1993). Observational follow-up data from a national survey also indicate that black women are less likely than white women to lose weight during adulthood (Kahn et al., 1991). Behavioral factors that could predispose black women and men to have a relatively greater difficulty with weight loss are easier to identify than metabolic variables that may be operating, although the latter are not precluded. Attitudes indicating a more multidimensional and less uniformly negative view of obesity among blacks than among whites have been documented as indirect evidence that the motivation for weight reduction is lower in black women (Allan et al., 1993; Kumanyika et al., 1992). Black women responding to a survey were more likely than white women to agree with the statement that there is little people can do to change their body weight (IBNMRR, 1993).
Survey data on self-reported weight-loss practices suggest that differences in weight management between black and white women are influenced primarily by factors relating to differences in the duration of adherence to weight-control regimens rather than to the level of adherence while on the regimen. Williamson et al. (1992) reported that black women were less likely than white women to be involved in long-duration weight-loss attempts (>1 year), but that race was not related to the rate of weight loss and to weight losses achieved among the subset of women who remained on diets. A report of a work-site lifestyle change program also provides evidence consistent with this finding (Brill et al., 1991). Blacks were significantly less likely to enroll in the program, and those who enrolled were significantly less likely to remain in the program. However, among those who did not drop out, weight losses among blacks were similar to those of whites.
The national survey data analyzed by Williamson et al. (1992) showed a higher starting weight for the current weight-loss attempts in blacks compared to whites. This may reflect the common finding that, compared to white women, fewer black women who are not overweight are dieting. A survey of weight-control practices of blacks and whites shows differences in dieting strategies, with black dieters reporting more practices defined as questionable (Levy and Heaton, 1993). One study has found that blacks lose less weight than whites from gastric surgery
(Sugerman et al., 1989). Although differences in response to surgery may imply biological differences, behavioral differences influence the ultimate weight loss following obesity surgery and may explain the racial difference (Sugerman et al., 1989).
Most potential associations between race/ethnicity and weight have been clearly documented for black women; relatively fewer data exist for black men or for men or women in other ethnic groups. Data on Hispanic men and women, often not subdivided by specific Hispanic ethnicity, in some cases show patterns that are intermediate between those of blacks and whites and in other cases more similar to those of whites (Brill et al., 1991; Piani and Schoenborn, 1993; Schoenborn, 1988; Serdula et al., 1993; Williamson et al., 1992). One older study indicated a lower level of concern about weight among Mexican-Americans compared to whites from the same region, although this difference was not present in the group with a higher socioeconomic status (Stern et al., 1982).
Education is strongly associated with several weight-management variables. The prevalence of dieting increases with education, even among those who are not overweight (Levy and Heaton, 1993; Piani and Schoenborn, 1993; Schoenborn, 1988). Education is positively related to level of leisure-time physical activity, although negatively associated with occupational activity (King et al., 1992). The work-site study reported by Brill et al. (1991) noted that persons with advanced degrees were more likely to enroll in and less likely to drop out of the program. It has been suggested that one mechanism for a favorable effect of education on weight management may be through increased self-efficacy (Leigh et al., 1992). Dieting prevalence also increases with income (Piani and Schoenborn, 1993; Schoenborn, 1988). Low social class has been associated with poor exercise program adherence in some studies (King et al., 1992).
A NEW PERSPECTIVE ON WEIGHT-MANAGEMENT OUTCOMES
The signs are clear that a different perspective on obesity-treatment outcomes is needed. The prevalence of obesity in this country is increasing despite the spending of more than $33 billion per year on weight-loss products and services (U.S. Congress, 1990). Although some evidence shows improvements in several risk factors for chronic degenerative diseases related in part to obesity, the economic, medical, and social costs of obesity in this country are still enormous. Many people are obsessed with their weight in a culture that encourages one both subtly and overtly to equate thinness with beauty and obesity with sloth.
We recommend that the definition of success that is applied in evaluating
weight-loss programs be broadened and made more realistic based on the research summarized in Chapter 2 documenting that small weight losses can reduce the risks of developing chronic diseases. Specifically, the goal of obesity treatment should be refocused from weight loss alone to weight management, achieving the best weight possible in the context of overall health. In contrast to weight loss, the primary purpose of weight management is to achieve and maintain good health. This concept includes weight loss but is not limited to it. We recommend that weight loss programs be judged more by their effects on the overall health of participants than by their effects on weight alone. The criteria set forth in this report are framed around weight management.
We have identified four components of successful weight management: (1) long-term weight loss, (2) improvement in obesity-related comorbidities, (3) improved health practices, and (4) monitoring of adverse effects that might result from the program. To assess objectively whether successful weight management has been achieved, it is necessary to provide guidance on assessing each component.
Long-Term Weight Loss
Long-term weight loss is often referred to as maintenance, as in maintenance of lost weight. As described earlier in this chapter, most people in weight-loss programs lose weight but fail to maintain the loss. The amount of weight lost is, of course, easy to measure objectively. However, defining what is meant by long-term weight loss is a subjective matter. For practical purposes, we will define long-term as meaning 1 year or more, and weight loss of any significance as the loss of ≥ 5 percent of body weight and/or a reduction in BMI by 1 or more units. Successful long-term weight loss by our definition means losing at least 5 percent of body weight (or reducing BMI) by the completion of a weight-loss program or the weight-loss portion of a weight-management program, and keeping it below our definition of significant weight loss for at least 1 year. It can still be achieved even though some weight is regained, as long as the net weight loss stays significant as defined.
Improvement in Obesity-Related Comorbidities
As described in Chapter 2, comorbidities associated with obesity include high blood pressure (>140/90), elevated lipid concentrations (cholesterol >200 mg/dl or triglycerides >225 mg/dl), and the presence of non-insulin-dependent diabetes mellitus, osteoarthritis of weight-bearing joints, and sleep apnea. Each comorbidity can be objectively determined or evaluated by a health-care provider. Successful weight management
should include improvement in one or more of these comorbidities if present to a degree considered clinically significant by a health-care provider.
Improved Health Practices
Improved health practices include obtaining health-related knowledge; engaging in good eating habits and regular physical activity; obtaining regular medical attention, particularly regular screening if one has not achieved a healthy weight (to identify as early as possible the presence of comorbid conditions); and improving self-esteem and attitudes about self-care. Such practices help to maximize one's chances for successful weight management, decrease the risks of developing a variety of degenerative chronic diseases, and enable many major medical problems to be caught at an early stage.
Obese individuals, as they go through treatment, should develop a reasonable understanding of the disease, including its causes and treatments, the benefits of diet and exercise, the effects of excess weight on the body over time, and the benefits to health from weight loss. Short of giving individuals tests as they begin and complete a program to see if knowledge of obesity has increased, this component can be assessed indirectly by evaluating whether basic information about obesity is presented by the option (e.g., discussed prominently in a diet book or as part of the classes and counseling sessions in a commercial program) and whether the individual reads or hears it (e.g., reads the book in its entirety or attends most of the classes and counseling sessions of the program).
Eating habits can be assessed by using one of the dietary assessment tools in Appendix A. For practical purposes, we define a good dietary pattern as one where the individual meets the recommendations of the Food Guide Pyramid on at least 4 of 7 days. (Such a dietary pattern might be inappropriate during the treatment phase of a clinical program where specially formulated products are used. During this period, the standard of nutritional adequacy should be meeting the Recommended Dietary Allowances for all nutrients except energy over the course of a week.) Again for practical purposes, we define regular physical activity as the accumulation of one-half hour or more of moderate-intensity activity (such as brisk walking) four or more times a week, and preferably daily. We believe it prudent for an obese individual to see a physician at yearly intervals for a physical examination and appropriate follow-up. Individuals who have not achieved a healthy weight (such as a BMI of less than 25 through age 34 and less than 27 beyond age 34; see Chapter 2) either have obesity-related comorbidities or are at risk of developing them at some
future point. Regular screening of these individuals by a health-care provider will help to identify as early as possible the presence of comorbid conditions and lead to the initiation of appropriate treatment or continuation of it. Dietary patterns and physical activity are difficult to measure objectively since they usually depend on the individual's own characterization of these factors. In contrast, medical visits can be documented with the individual's physician.
Improved well-being is a positive subjective feeling by the individual that includes feeling good about oneself (positive self-esteem) and a healthy attitudes about self-care with a desire to practice it. These feelings can be assessed by available questionnaires (see Appendix A), but most of these tools are best used by health-care providers trained in their use and interpretation. We recommend that all programs administer a test such as the Dieting Readiness Test to assess how well equipped a person is to undertake a weight-management program; individuals in a do-it-yourself program will need to self-administer and score the test. Clinical programs, in addition to using the Dieting Readiness Test or a similar test, should administer a test such as the General Well-Being Schedule, which provides a useful evaluation of the psychological health of the client and can help uncover potential psychological pathologies. Both of these tests are provided in Appendix B.
Monitoring of Adverse Effects That Might Result from Program
As described in Chapter 6, weight loss poses potential risks to health. The more restrictive the diet, the greater are the risks of adverse effects. All clinical and nonclinical programs should periodically question their clients about any changes in health while on the program and should encourage them to volunteer such information if changes in health, particularly negative ones, occur. Consumers undertaking a do-it-yourself program should be particularly aware of the fact that their efforts may have adverse effects and should pay attention to any changes in their health. Experiencing an adverse effect while on a weight-management program may or may not be related to the program (it may be a worsening of health as a result of the obesity), but it should be evaluated. Depending on the nature of the problem, in some cases the program will need to be modified for the individual and in other cases it should be discontinued.
We believe that weight-loss programs should be judged by how well individuals do in these four areas, and potential clients should expect that a high-quality program will attend to, or urge attention be paid to (since most of these components are not under the direct control of the
program), each of these areas. In Chapter 8, we provide recommendations on how these components might be addressed by programs.
CONCLUDING REMARKS
Life in the United States is conducive to obesity. Easy availability of an energy-rich diet and limited opportunities for exercise set the stage for a nation of overweight ''couch potatoes." Available data suggest that most obese individuals who try to lose weight in intervention programs do not maintain the losses they achieve during treatment. For the small numbers of people who do maintain their losses without drugs or surgery, the most important factors associated with long-term success include a regular habit of exercise, continued contact with the treatment program, normalization of eating patterns with continued control of energy intake, continued self-monitoring of diet and exercise, and a positive, problem-solving attitude toward life's stressors. Family dysfunction and negative life events are associated strongly with weight rebound.
Given the experiences of dieters and the research demonstrating that relatively small weight losses can reduce the prevalence and severity of comorbid conditions associated with obesity, we recommend that obesity-treatment programs focus more on weight management than on weight loss and broaden the definition of success to include, for example, better health, improved health practices, more and better health-related knowledge, and improved well-being. The next chapter suggests how this broader definition of success and the current knowledge of predictors of success can be used along with recommendations in Chapters 5 and 6 to facilitate the process of decisionmaking about program appropriateness, soundness, safety, and outcomes.

















