1
INTRODUCTION
At the request of several federal agencies, the Board on Environmental Studies and Toxicology in the National Research Council's Commission on Life Sciences convened the Committee on Biological Markers to examine the use of biologic markers in environmental health research. Biologic markers indicate events in biologic systems and are variations in the number, structure, or function of cellular or biochemical components of tissues and organs. Biologic markers afford a means to identify early stages of disease and to understand the basic mechanisms of the biologic responses to substances found in the environment (Committee on Biological Markers of the National Research Council, 1987). Four specific biologic systems were chosen for study: the reproductive system (NRC, 1989a), the respiratory system (NRC, 1989b), the immune system (NRC, 1992), and the urinary system. This is the report of the Subcommittee on Biologic Markers in Urinary Toxicology, which considered the kidney, bladder, and prostate to be within the scope of its charge.
The kidney's main function is excretion of waste products in the urine, but it has other functions. It plays an important role in homeostasis and is the predominant organ in the control of extracellular fluid volume and electrolyte composition. The kidney also produces hormones, including erythropoietin, renin, 1,25-dihydroxyvitamin D3, and several vasoactive prostanoids and kinins. The very processes by which the kidney maintains internal homeostasis make it highly susceptible to toxic damage; that is, because of the mechanisms by which large amounts of blood are filtered and waste products are concentrated within the kidney, its exposure to some toxic material can exceed that of other organs. In addition, the kidney is metabolically active and has the capacity to metabolize some materials to toxicants. The bladder is exposed to the waste products collected by the kidney, which at times reach high concentrations in the urine. Depending on the frequency of voiding, the bladder can have a longer exposure to toxic waste products than the kidney itself. Empty-
ing of the bladder can be influenced by various diseases of the prostate. These organs can also be exposed to bacterial and viral infectious processes that modify the normal milieu and act as confounding variables. All the characteristics just enumerated help to explain why the urinary tract—in both laboratory animals and human beings—is a site of xenobiotic-induced cancer.
BIOLOGIC MARKERS
Humans are often and unavoidably exposed to hazardous environmental chemicals. Biologic markers can be useful in confirming such exposures, estimating their magnitude, and identifying persons adversely affected or most likely to be adversely affected if exposures continue. Biologic markers are indicators of events or conditions in biologic systems or samples. It is hoped that they will clarify the relationship between environmental exposures and human diseases and help to prevent such exposures and diseases. Interest in the use of biologic markers to study the health effects of exposure to environmental toxicants is growing among researchers in clinical medicine, epidemiology, toxicology, and related biomedical fields. Specifically, clinicians can use markers for early detection of disease; epidemiologists can use them as indicators of exposure to determine internal dose or health effects; and toxicologists can use them to estimate dose-response relationships and to facilitate assessment of risk associated with exposures. Biologic markers also can be helpful in clarifying the underlying mechanisms of specific diseases.
New developments in molecular genetic and biochemical approaches to medicine have yielded sensitive markers for assessing toxicant exposures (NRC, 1991). They have also increased our knowledge of disease, improved our ability to predict the outcome of disease, and helped to direct courses of treatment. Many diseases are defined not only by clinical signs and symptoms but also by the assessment of biologic markers at the subcellular and molecular levels. Diseases of the liver and kidney, for example, are often detected by measurement of enzymes in blood, proteins, or cells in urine; diabetes can be suspected if glucose is found in urine; and inborn errors of metabolism, such as phenylketonuria, are found early by biochemical analysis, rather than later as a result of clinical dysfunction. Concentrations of material in the urine are often used to determine the degree of exposure in an occupational setting, in monitoring therapeutic regimens, and in forensic medicine.
Biologic markers are indicators of exposure, effect, or susceptibility. That classification is a useful theoretical scheme by which to characterize biologic markers of any organ system; however, it must be qualified somewhat for practical application. A strict classification with respect to any of the three categories (exposure, effect, or susceptibility) is difficult, for the three categories often are related and can be thought of as elements in a continuum
from environmental exposure to clinical disease.
The identification of a chemical or its metabolite in a biologic specimen is a marker of exposure. Cellular or molecular changes within an organism are biologic markers of effect. Biologic markers often are demonstrated by clinical laboratory measurements or clinical tests used in the differential diagnosis of various diseases. They can serve as surrogates for other methods of detection in determining the molecular and cellular events in the development of health problems. If such markers could be detected before exposed persons became obviously ill, a disease process might be reversed in those affected or prevented in others. Finally, some cellular or molecular measurements can identify groups of people or individuals who are more vulnerable than others to the effects of toxic exposure; the results of these measurements are markers of susceptibility.
Markers of Exposure
A biologic marker of exposure is a xenobiotic chemical or its metabolite or a product of an interaction between the chemical and some target cell. Markers of exposure most commonly are the concentrations of materials in urine, blood, or other body tissue, including hair and nails.
Several problems limit the usefulness of specific markers of exposure. For example, many environmental xenobiotics have similar metabolites, and this makes identification of the parent chemical difficult. Also, large doses of a substance, by inducing anatomic or physiologic change, can alter the retention or excretion of the marker and in this way decrease its utility as a marker of exposure. The body burden of a substance reflected by biologic markers might result from more than one route of exposure. It can be difficult to identify persons exposed to hazardous concentrations of substances commonly found in the body in lower concentrations. Such is the case in excessive exposure to essential minerals, such as copper and cobalt. Markers of exposure decay after exposure ceases; measurement soon after exposure is required for materials that are metabolized rapidly, such as trichloroethylene, but not after materials with long half-lives, such as cadmium. Markers of exposure alone give no indication whether an exposure has produced a biologically significant result. The same dose in persons who are susceptible and resistant to a given xenobiotic can have different results. Urine is one source of markers of exposure. High exposures to a material can result in increased concentrations of it or its metabolites in urine. When sufficient pharmacokinetic information is available, urinary markers of exposure can be used to estimate the total exposure of a person to a substance.
Markers of Effect
A marker of effect is a measurable cellular, physiologic, or biochemical al-
teration within an organism. Markers of adverse effect can be biochemical or cellular signals of tissue dysfunction, increased enzyme activity, the appearance of excessive waste products in the urine or other sampling compartments, and physiologic signs of abnormal function, such as increased blood pressure or blood in the urine. The effects themselves might not be directly adverse, but rather might indicate a potential for health impairment (e.g., DNA adducts). Biologic markers of effect include changes in the components of urine itself (such as an increase in urinary protein excretion or cellularity) and changes in the volume or composition of other body fluids caused by kidney dysfunction.
With impaired renal function, excretion products, such as creatinine and urea, can accumulate in the blood. Increased blood concentrations of these products can be markers of renal damage, although they are not particularly useful except in cases of severe damage as discussed in Chapters 2 and 4. Other markers of renal toxicity can be present in urine because of altered renal function or damage to the kidney. Many of these can be detected in examination of the urine, including color, volume, pH, specific gravity, albumin, electrolytes, enzymes, and elements in the urinary sediment. Markers that could show up include white and red blood cells, kidney epithelial cells, casts, and crystals.
Markers of Susceptibility
A marker of susceptibility is an indicator of an inherent or acquired limitation of an organism's ability to resist the effects of exposure to a specific xenobiotic substance. A biologic marker of susceptibility can be an intrinsic genetic or other characteristic or a pre-existing disease that results in an increase in the amount of a material absorbed, an alteration in its metabolism, or an increase in the target-tissue response. It can be difficult to distinguish between susceptible and nonsusceptible persons, either because of multiple interactive influences and genetic polymorphisms or because of difficulties in measuring markers of susceptibility.
Potential sources of normal variability in markers of susceptibility can be the result of concurrent disease or genetic, environmental, or biorhythmic influences other than the specified events that are the object of study. Such influences can cause differences between populations, differences between individuals, and differences within individuals over time. Decreased detoxification or excretory function are commonly involved in susceptibility. Thus, elderly persons with declining organ function and young persons with immature and developing organs are likely to be more vulnerable to toxic substances than healthy adults (Figure 1-1).
VALIDITY OF BIOLOGIC MARKERS
In the course of developing this document, the subcommittee noted that var
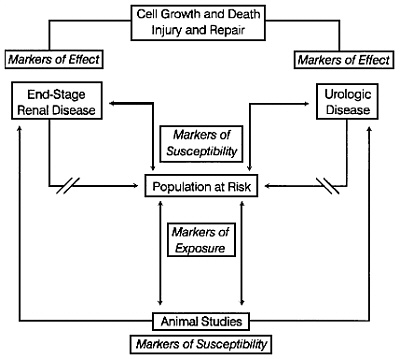
Figure 1-1. Flow diagram depicting the relationship between markers of exposure, effect and susceptibility for patients with either ESRD or UD. The central focus is on identification of the population at risk, that is, those most likely to be exposed to xenobiotics and susceptible to their adverse effects. The most devastating clinical outcomes are the development of chronic renal disease or urogenital cancer. Identification of the population at risk can be facilitated by retrospective analysis of those with ESRD or UD and by prospective use of animal studies. In both cases, the utility of markers of exposure and susceptibility can be established. Markers of susceptibility can vary between humans and animals, whereas markers of exposure must be shared if they are to be used to extrapolate between populations at risk and laboratory investigations. The aim is to provide insight into disease mechanisms and allow testing for prevention or modification. Before changes in organ function, adverse response to xenobiotics might be detected by understanding the mechanisms of cell growth, injury, repair, and death. It is anticipated that this will lead to identification of highly sensitive and specific markers of effect.
ious disciplines use validity, sensitivity, and specificity in different ways. The oversight committee discussed the validation of biologic markers for use in assessments of human health, particularly in epidemiologic studies. To validate the use of a biologic measurement as a marker, it is necessary to understand its relationship to the event or condition of interest, such as the potential for health impairment or susceptibility to disease. Sensitivity and specificity are critical in the process of validation (MacMahon and Pugh, 1970). In epidemiology, sensitivity is the ability of a test to identify correctly persons who have the disease, condition, or exposure of interest; specificity is the ability to identify correctly persons who do not have the disease, condition, or exposure of interest. The sensitivity and specificity of markers of exposure must be validated.
The use of the terms sensitivity and specficity in epidemiology must be distinguished from their use with respect to laboratory methods. Laboratory sensitivity refers to the lowest concentration of a substance that can be measured reliably, and laboratory specificity refers to the ability of an analytic technique to measure only the substance in question.
Predictive value is a measure of the potential usefulness of a test in identifying an exposed member of a population (positive predictive value) or identifying an unexposed member of a population (negative predictive value). For rare conditions (those with low prevalence in the population), even very good tests can have low positive predictive value. When there is high prevalence in a population, even substantially poorer tests can have high positive predictive value.
Sensitivity and specificity are determined by both intrinsic and extrinsic factors. Intrinsic factors include differences in the distribution of the marker between the unexposed population and the exposed population. An ideal biologic marker is absent in all unexposed persons and easily detectable in all exposed persons. No such marker is known to exist for any organ system, and, because of the variability of responses within and between individuals, the distributions of most markers are likely to show considerable overlap in unexposed and exposed individuals.
Extrinsic factors also influence specificity and sensitivity. For example, people who have not been exposed to a toxicant could have other conditions that cause the appearance of the biologic marker that is seen in people who have been exposed. In addition, errors in measurement also influence specificity and sensitivity. Analytic imprecision blurs the difference in distribution of a marker between exposed and unexposed populations, and analytic inaccuracy can lead to misclassification of individuals.
The criteria used to define an event or condition (especially a health effect) can affect the fraction of the population that is found to have it. If, for example, the event is a disease, the finding of a ''case'' is often based on a subjectively determined collection of signs and symptoms. Adding or excluding a particular symptom can result in finding a
larger or smaller number of cases. This will influence estimates of the sensitivity and specificity of the method used to find cases.
If being above (or below) some index value or threshold on a test is what determines whether a finding is "positive," the sensitivity of the test can sometimes be increased by adjusting the threshold. However, because sensitivity and specificity are linked for a given test, increasing one will inevitably result in decreasing the other. There are circumstances, however, in which adding another test (or tests) can be of value. For example, a test with poor specificity (that is, one that incorrectly identifies persons as having the condition of interest) can sometimes be followed by a test with greater specificity that will eliminate many (if not all) false-positive results.
In developing a test, sensitivity and specificity are usually estimated as a result of a trial on a known or (often) an easily acquired population, such as medical students or nurses. The sensitivity and specificity often shift with the population tested, so persons using the test need to be aware that the first published sensitivities and specificities are almost certain to change when different populations are used.
Specificity of markers is important in the consideration of validity. For example, urinary concentrations of trichloroethanol and trichloroacetic acid, which are metabolites of trichloroethylene, are used as indicators of occupational exposure to trichloroethylene. But, they are not specific for trichloroethylene, inasmuch as metabolism of tetrachloroethylene and chloral hydrate also produces these metabolites; in addition, their half-lives are relatively short, so the ability to detect them decays over time.
The variability between individuals in the factors that affect sensitivity greatly influences the ability of markers to detect exposure. Some markers that are validated generally have been established only for obvious clinical events. A major purpose of markers in environmental health research is to identify exposed persons, so that risk can be predicted and disease prevented. Validation involves both forward and backward processes of association—from the marker back to exposure and from the marker forward to effect.
ETHICAL ISSUES
The availability of highly sensitive assays that can identify effects resulting from the interplay between small exposures and genetic or acquired susceptibility raises several ethical questions. The National Research Council's Committee on Biological Markers (NRC, 1987), Schulte (1987), and Weiss (1989) have discussed these issues. Primary among them is the use made of information derived from biologic markers. Consider the hypothetical case of a biologic marker known to reflect susceptibility to the effects of a chemical. Should a worker in a workplace that contains the chemical who tests positive for that marker or has an increased measurement of it in his or her blood be removed from the workplace? If so,
should the worker be offered an equivalent job in the same industry? Or should the workplace be cleaned up to protect even the most sensitive worker?
The relationship of group and individual risk to biologic markers is crucial. It is important, therefore, to inform research-study participants in advance of the degree to which the results will be interpretable at the group level as opposed to the individual level. Participants in such studies should be given test results that are presented and discussed in the context of variability within and between people in the normal (nonexposed) population and the study group. Participants in epidemiologic studies might resist or refuse invasive techniques for obtaining markers or resist providing markers obtained by techniques perceived to be not fully safe. Although the use of urine samples for marker detection might be universally accepted, attention should not be directed away from blood, other body fluids, or tissue as reliable sources of markers; accuracy and not convenience should be the driving force. Whatever the choice, it must be economically feasible.
It is anticipated that some characteristics or markers of susceptibility will define a population at high risk for developing renal or urologic disease in response to environmental or occupational nephrotoxicants. Identification of the susceptible populations and appropriate markers may be greatly facilitated by comparative studies in animals with the understanding that in both cases it is necessary to consider precise definitions of markers of exposure, because susceptibility and exposure can be closely associated. In many cases before renal or urologic disease is clinically apparent, various markers of effect are present. These markers—which reflect cell injury, repair, growth, differentiation, or death—facilitate early intervention with the hope that disease progression can be slowed, halted, or reversed.
STRUCTURE OF THE REPORT
Chapter 2 provides information on the structure and function of the urinary tract, the diseases associated with the urinary tract, and their risk factors. In Chapter 3, relationships among exposure, susceptibility, and the associated markers are developed. The usefulness of markers in monitoring urinary diseases is discussed in Chapter 4. Chapter 5 develops a rationale based on epidemiologic studies for the use of biologic markers in protection of human health and extrapolation of data from animals to humans. New technologies and related issues are reviewed in light of research needs in Chapter 6. Chapter 7 summarizes the subcommittee's findings and recommendations.








