5 The Legal Environment
This chapter considers the effects on needle-sharing behavior among injection drug users that arise from various legal structures. We begin with a brief historical review of U.S. drug control policies to provide a better understanding of why various legislative bodies of government (federal, state, and local) have enacted laws that directly contribute to the scarcity of injection equipment.
U.S. DRUG CONTROL POLICY
The involvement of the U.S. government in matters of drug control policy has gone through various distinct phases during this century (Courtwright, 1992). As with other individual behaviors that deviate from the social norms of the time and are perceived by most as threatening the well-being of the majority, the breadth of government interventions has varied with the perceived magnitude of the problem. The perceived magnitude of the drug abuse problem in the United States is not driven exclusively by the incidence or prevalence of drug use, but is closely tied to the demographics and behavioral characteristics of the drug-using population.
Early in this century, the federal government became progressively more involved through a series of laws and judicial rulings that criminalized and regulated nonmedical drug use. The 1906 Pure Food and Drug Act helped slow the spread of medical addictions, which resulted mainly from the liberal narcotic prescription practices of physicians at the time. The Harrison
Narcotic Act of 1914, which regulated the sale, distribution, and possession of narcotics, was later strengthened by the Narcotic Drug Import and Export Act of 1922.
As discussed by Courtwright (1992), the period from the 1920s through the mid-1960s was characterized by a rigid, strict, and punitive approach toward dealers and users. The drug control policy of that era was, in many ways, a reflection of the drug addiction philosophy of Harry Jacob Anslinger, who was commissioner of the Bureau of Narcotics from its creation in 1930 until 1962. It was during this period that various states passed legislation to regulate the sale, distribution, and possession of drug paraphernalia (Pascal, 1988). These statutes generally prohibited the possession of any paraphernalia intended for the use of any narcotic drugs, and some required a prescription for the purchase of syringes. The primary difference between these two types of laws was that paraphernalia laws required a demonstration of criminal intent, whereas prescription laws did not—a distinction that still is reflected in the latest versions of those statutes.
The mid-1960s through late 1970s were characterized by a relaxation of the strict policing of the drug user and the pursuit of new treatment avenues (e.g., methadone maintenance). During the Reagan and Bush administrations, there was a resurgence of the strict law enforcement approach to drug control strategy, with a strong emphasis on supply reduction rather than demand reduction. The get-tough approach of the time is evident from the language contained in two antidrug bills (1986 and 1988) passed by Congress, which contained substantial civil penalties for personal use and possession. Public statements from Robert Martinez, President Bush's director of the Office of National Drug Control Policy, also reflect the strict and punitive approach of that administration (Office of National Drug Control Policy, 1992).
Although this nation has gone through different periods of government involvement and control over drug use, the dominant approach during the twentieth century clearly has been that of restrictive drug control policies, which has resulted in a substantial number of federal, state, and local laws that attempt to restrict the sale, distribution, and possession of drugs. Moreover, in their attempt to regulate and curtail illicit drug use, legislators have enacted statutes whose goals are to restrict indirectly the use of illicit drugs. That is, they have passed criminal laws restricting the sale, distribution, and possession of drug paraphernalia.
The primary intent of these criminal laws seems to have been to impact drug use by restricting and limiting the purchase of drug instrumentation and devices that facilitate drug use itself. For example, concerns regarding the sale of marijuana and other cannabinoids paraphernalia in ''head shops" led to the enactment of many local and state drug paraphernalia laws (American Civil Liberties Union, 1994). An obvious secondary intent was to prevent
merchants from profiting from the drug trade. It would seem that the underlying premise or rationale for the forceful involvement in drug control by governments is to protect the health and well-being of members of society by engaging police power to eliminate the drug trade and to free society from the negative health consequences and deviant behaviors that have been associated with drug abuse.
At the core of U.S. drug control policy is the belief that a scarcity of drugs and drug paraphernalia, coupled with harsh punishments for dealers and users, will cause a reduction in drug abuse and undesirable behaviors that are often tied to such drug abuse. (For a detailed treatment and analysis of the history of drug policy in the United States, the reader is referred to the following publications: Courtwright, 1982, 1992; Morgan, 1981; Musto, 1987, 1991; and Reuter, 1992.)
Legislative/Statutory Environment
Two categories of laws have been enacted that directly impact the availability of sterile syringes and other injection drug use paraphernalia: drug paraphernalia laws and prescription laws.
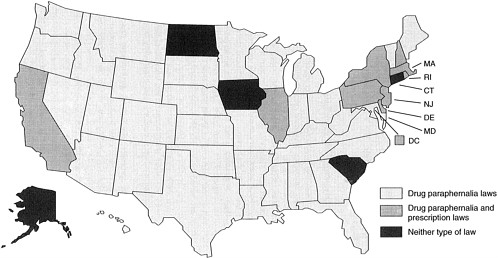
Drug paraphernalia laws prohibit the manufacture, sale, distribution, and possession of equipment and materials intended for use with narcotics (Gostin, 1993). Under these laws, over-the-counter sale of hypodermic syringes and needles is technically allowed. A valid medical prescription for the purchase of syringes or needles is not required. In 45 states and the District of Columbia (see Figure 5.1) such laws are in effect (Valleroy et al., in press). The most recent versions of these state and local laws (late 1970s and early 1980s) are based on the Model Drug Paraphernalia Act (art. 2), which was formulated by the Drug Enforcement Administration in 1979 as an amendment to the Uniform Controlled Substances Act (9 U.L.A., Part II, 1988). Under that model act, drug paraphernalia are broadly defined and specifically include hypodermic syringes, needles, and other objects used to inject controlled substances into the body.
In the midst of the AIDS epidemic, the federal government enacted a federal statute to further limit the sale, distribution, and possession of drug paraphernalia. In 1986, the federal government joined the regulation and control arena of drug paraphernalia by enacting the Mail Order Drug Paraphernalia Control Act (21 U.S.C. § 857, 1986) as section 1821-1823 of the Anti-Drug Paraphernalia Act (P.L. 99-570). This statute encompasses any activity involving drug paraphernalia (broadly defined) crossing interstate lines. The significance of this act is that it establishes federal jurisdiction over matters regulating drug paraphernalia that, until then, had been the territory of state and local governments.
Prescription laws are distinctly different from drug paraphernalia laws.
In contrast with paraphernalia laws, prescription laws do prohibit the sale, distribution, and possession of hypodermic syringes or needless without a valid medical prescription regardless of knowledge of intended use. Prescription laws are in effect in nine states (see Figure 5.1), the District of Columbia (Valleroy et al., in press), and Puerto Rico. (The nine states are California, Delaware, Illinois, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, and Rhode Island.) In those jurisdictions, it is a criminal offense to sell or possess syringes or needles without a valid medical prescription. Connecticut and Maine have recently modified their prescription laws to allow syringes and needles to be sold over the counter. Typical prescription statutes also attempt to set certain limitations on the physician's discretion to dispense such valid prescriptions. That is, not only do these statutes require a valid medical prescription, but they also place some legal constraints on physicians by requiring that prescriptions be issued only in cases with a legitimate medical purpose (Gostin, 1993). As depicted in Figure 5.1, all states with prescription laws also have paraphernalia laws, and only five states (i.e., Alaska, Connecticut, Iowa, North Dakota, and South Carolina) have laws permitting both the purchase and the possession of syringes without a medical prescription.
Judicial Rulings
Constitutionality
In examining legislation pertaining to the regulation of drug paraphernalia, an important consideration is the recognized broad authority of the states to regulate the manufacture, sale, prescription, and use of drugs by exercising their police powers. The constitutionality of this broad authority has been acknowledged by the Supreme Court as far back as 1921 (Minnesota ex re. Whipple v. Martinson, 256 U.S. 41) and was reiterated by the Court in more recent cases (Robinson v. State of California, 1962). Moreover, in subsequent years, unsuccessful challenges to the authority of state and local laws to regulate drug paraphernalia (in contrast to drug use itself) have been made (Wheeler v. United States, 276 A.2d 722, D.C.1971; Village of Hoffman Estates v. Flipside, Hoffman Estates, Inc., 455 U.S. 489, reh'g denied, 456 U.S. 950, 1982). In these cases, the Supreme Court has made it clear that state and local government authority to enact laws aimed at controlling drug use also extends to their authority to control the instruments of drug use. Thus, state and local government authority to restrict individuals from manufacturing, selling, or using drug paraphernalia appears to be on firm constitutional footing.
The prescription laws have also withstood constitutional challenges (People v. Bellfield, 33 Misc. 2d 712, 230 N.Y.S.2d 79 [1961], aff'd, 11 N.Y.2d
947, 183 N.E.2d 230 [1962]). Moreover, the Federal Mail Order Paraphernalia Act of 1986 has also survived constitutional scrutiny (United States v. Main Street Distributing Inc., 700 F. Supp. 655, E.D.N.Y., 1988).
State and Local Litigation
Needle exchange programs have operated in what may fairly be called ambiguous legal circumstances. Arrests are sometimes made. Most prosecutions to date have involved needle exchange workers arrested for violating state or local drug paraphernalia or prescription laws (see American Civil Liberties Union, 1994, for a list of recent cases). The necessity defense has been the strategy most frequently used by attorneys arguing these cases. This defense strategy rests on the legal doctrine that an individual should not be held liable for an offense if the individual has engaged in a criminal activity in order to avoid a greater imminent harm, that is, to save lives (i.e., by preventing HIV transmission). Although this defense has been used repeatedly and successfully to obtain acquittals in the courts, it has serious limitations. For example, such favorable decisions:
-
do not create any legal or judicial precedent for future cases—for example, an individual could be required to stand trial following an acquittal if he or she is arrested for repeating criminal actions subsequent to the earlier trial;
-
can be invoked only in situations that satisfy stringent criteria (e.g., no adequate alternative to avert the harm was available; see Gostin, 1993:53); and
-
may not be a viable defense for the clients of needle exchange programs, i.e., injection drug users.
The authority of public health officials to sanction needle exchange programs has sometimes been challenged. Many cities and states have provisions in their public health codes that may under certain circumstances allow public health laws to take precedence over criminal laws to protect community health. (In a critical judicial opinion, the Washington Supreme Court unanimously declared that in the narrow circumstances of the case, the State of Washington's needle exchange program was lawful.)
When legal exemptions are granted under the general public health authority, regulations and reporting requirements may be imposed, limiting the ability of program staff to adapt their services to the needs of their clients (e.g., spending time labeling needles, limiting the number of syringes exchanged per visit). Specific examples of regulations that may run counter to the intended service provisions of programs are provided in the
original New York City and Washington, D.C., case studies presented in Chapter 3.
For a more detailed discussion of the legal environment surrounding needle exchange programs, the reader is referred to the following publications: Gostin (1991a, 1991b, 1993) and Pascal (1988).
DO PARAPHERNALIA AND PRESCRIPTION LAWS CONTRIBUTE TO HIV TRANSMISSION
Contaminated needles and syringes are a primary mechanism for transmitting HIV among injection drug users. According to some researchers, "it would be difficult to design a system better suited to promote the transmission of a blood-borne infection" (Friedland and Klein, 1987). The causal role of sharing1 used injection equipment in transmitting diseases has been well documented for some time (Brecher, 1941; Louria, 1967; Cherubin, 1967; Centers for Disease Control and Prevention, 1993) and for a variety of blood-borne diseases, such as hepatitis and bacterial endocarditis (Selwyn and Alcabes, 1994). Sharing contaminated injection equipment has also been shown to be the primary mechanism of HIV transmission among injection drug users (Chaisson et al., 1987; Chitwood et. al., 1990; Marmor et al., 1987; Schoenbaum et al., 1989; Friedland et al., 1985; Vlahov et al., 1990).
Given the clear risk of transmission of HIV infection when used drug equipment is shared, why do injection drug users engage in this activity? Various investigators have attempted to shed light on that important question. The sharing of drug paraphernalia is a dynamic behavioral process that is a function of multiple factors and their interactions:
-
demographic factors, such as age, gender, maturity of drug career, and treatment history;
-
paraphernalia availability, both in the community at large and at the time of injection;
-
perception of risk of arrest and of HIV infection and other diseases;
-
situational/contextual variables, such as the use of shooting galleries;
-
group norms and social networks, involving the cohesion of groups; and
-
drug of choice (e.g., cocaine, heroin, amphetamine, polydrug use), which is also related to intensity of use (i.e., frequency of injection).
Needle Scarcity and Sharing
Early reports focused on the psychological and cultural factors involved in sharing (e.g., Des Jarlais et al., 1986; Howard and Borges, 1972), often describing the sharing activity as a ritual engaged in by injection drug users to bond with each other. However, with the emergence of AIDS, several ethnographers have reexamined the relative importance of such factors in relation to other more pragmatic factors, such as needle scarcity (Carlson, 1991; Kane and Mason, 1992; Koester, 1992). For example, researchers have established that legal restrictions play an important role in the scarcity of needles and syringes within the injection drug user community (Des Jarlais and Friedman, 1992; Feldman and Biernacki, 1988; Koester, 1989; Murphy, 1987). These findings are consistent with empirical findings of a large-scale longitudinal study (Mandell et al., 1994). An analysis of baseline data on 2,524 injection drug users indicates that sharing behavior is related to economic and legal considerations as well as to the frequency of injection and drug class.
Koester (1994) recently provided a detailed description and explanation of how the scarcity of sterile needles caused by these legal constraints has contributed to the sizable amount of sharing among injection drug users. At first glance, it would appear that, given the misdemeanor offenses associated with conviction on paraphernalia possession in many states, such convictions would not constitute a serious deterrent to having injection drug users purchase sterile needles from pharmacies (it is legal to purchase them without a prescription in most states) to ensure that they have access to sterile equipment when they need to inject drugs. Koester's data indicate that most of his study participants did, in fact, frequently purchase needles from pharmacies. Nonetheless, these same individuals also stated that the imminent fear of arrest for possession of paraphernalia (which deterred them from carrying sterile needles) was greater than the distant threat of AIDS. Several researchers have reported that knowledge about the risk of infection associated with sharing is insufficient to affect behavior change (Inciardi, 1990; Friedman et al., 1992; Page et al., 1990a). In a study of out-of-treatment injection drug users (Celentano et al., 1991), 98 percent of active injection drug users reported that they were aware that HIV was transmitted through sharing contaminated needles and syringes, yet 70 percent reported sharing. Such findings were also observed with in-treatment injection drug users (Magura et al., 1989). These researchers reported that 40 percent of their sample reported sharing in the last month and that knowledge of AIDS risk was not empirically associated with that behavior.
Although fear of AIDS is often not a decisive motivation, it does bring about some meaningful behavioral changes among injection drug users. Since the early years of the AIDS epidemic, studies have reported significant risk
reduction among injection drug users (Des Jarlais and Hopkins, 1985; Des Jarlais et al., 1985, 1988; Hopkins, 1988; Kleinman et al., 1990; Selwyn et al., 1987). They reported an expansion of the street black market of injection equipment in New York City; the demand for sterile injection equipment was strong enough to lead to a noticeable increase in the illicit sales of such devices. An important point raised by Koester is that the fear of being caught carrying needles or syringes appears to vary across cities with similar prescription and paraphernalia laws, depending on the extent to which laws are enforced. Therefore, in cities in which these laws are consistently not enforced, injection drug users may be more likely to regularly carry sterile equipment, which reduces their need to share. Koester's findings show that drug paraphernalia laws, at least in Denver, play a significant role in explaining the high-risk sharing behaviors among certain segments of the injection drug user community. In addition to Koester's ethnographic data, empirically derived descriptive data from large-scale studies provide indirect support for the negative impact of these laws on sharing behaviors (Des Jarlais and Friedman, 1992; Nelson et al., 1991) as well as on HIV seroincidence among injection drug users (Friedman et al., 1994). For example, in a natural experiment in Baltimore, Nelson et al. (1991) were able to document lower transmission rates of HIV among injection drug users who are diabetic (i.e., with unrestricted legal access to sterile needles and syringes) compared with nondiabetic injection drug users.
Recent analyses (Metzger and DePhilippis, 1994) of data from a prospective study on the efficacy of methadone treatment in Philadelphia (Metzger et al., 1991) have elucidated the relationship between the difficulty of needle acquisition among injection drug users and their rate of needle sharing and drug use. A total of 12 months after the inception of this study, 202 of the original cohort of 325 study participants reported injection drug use in the last 6 months and formed the basis of the analyses. There was no significant difference between the needle-sharing rates of subjects who reported easier needle access at the 12-month follow-up and those who did not report easier needle access. Of those who reported increased difficulty of needle acquisition, 70 percent reported sharing needles at follow-up, compared with 8 percent of the subjects who did not report greater difficulty. Finally, these researchers found that changes in difficulty of needle acquisition were not associated with either increased or decreased use of any drugs (i.e., heroin, cocaine, amphetamines, benzodiazepines, marijuana).
These studies provide some evidence that existing statutes do affect the availability of sterile needles and syringes, are related to equipment sharing, and, as a consequence, can adversely affect the rate of transmission of HIV infection.
Changes in the Laws in Connecticut
Clearly, it is plausible that reducing legal strictures on the acquisition and possession of drug paraphernalia should result in less needle sharing, with attendant beneficial reduction in the risk of HIV infection. However, empirical checking of what actually occurs when such laws are changed gives a better reading on the effects of such changes.
The Centers for Disease Control and Prevention (CDC) recently conducted a study to investigate the impact of a new legislation in Connecticut (Valleroy et al., in press; Groseclose et al., in press), which was enacted in May 1992 and became effective in July 1992 (Connecticut General Statutes, Sections 21a-65, 21a-240, 21a-267, 1992). The intent of these new statutes was to increase the availability of sterile injection equipment in an attempt to reduce the use of contaminated needles and syringes among the injection drug user community and, consequently, the rate of HIV transmission in the state. Prior to passage of these new laws, it was illegal in Connecticut to purchase or possess needles or syringes without a valid medical prescription. The new laws permit, but do not require, pharmacists to sell up to 10 needles or syringes per visit to individuals without a prescription and allow individuals to possess up to 10 clean needles or syringes.
CDC's assessment (Centers for Disease Control and Prevention, 1993; Valleroy et al., 1993; Valleroy, 1993; Groseclose, 1993; Valleroy et al., in press; Groseclose et al., in press) of the impact of these new statutes focused on monitoring the pharmacies' sales of nonprescription and prescription needles and syringes, injection drug users' knowledge and behavioral changes, and law enforcement officers' behaviors.
Needle Sales
Pharmacy sales over a period of 1 following the effective date of the new laws (July 1, 1992, to June 30, 1993) were monitored for sentinel pharmacies (five) located in neighborhoods where there was a high prevalence of injection drug use (Hartford) and pharmacies (five) located in neighborhoods with low prevalence of injection drug use (Wethersfield). In addition to this prospective surveillance study in select pharmacies in two communities, the CDC research team also conducted a telephone survey of pharmacy managers using a statewide stratified random sample (stratified by type of location; five largest cities versus other locations) of pharmacies in November 1993. Of the 163 randomly selected pharmacies, 139 participated, with 64 (46 percent) located in the five largest cities and 75 (54 percent) in the other locations.
The results of the prospective surveillance study showed a steady increase in the number of nonprescription needles and syringes sold per month
for pharmacies located in Hartford (from 460 in July 1992 to 2,482 by June 1993) compared with a stable number of nonprescription needles and syringes being sold per month in Wethersfield (averaging 210 per month). The number of prescription needles and syringes sold by Hartford pharmacies during that same 1-year period remained stable with an average of 3,775 sold per month. Initial nonprescription sales (July 1992) in these pharmacies (i.e., in neighborhoods with high drug-use prevalence), represented 11 percent of total needles/prescription sales, and by June 1993 nonprescription sales represented 43 percent of total sales. Moreover, we should note that the average number of prescription needles and syringes sold per transaction was 63 (because most prescription sales in Hartford are to diabetics, who typically buy a supply of 100 needles and syringes per transaction at a cost of $25.00), compared with an average of 3 needles and syringes sold per nonprescription transaction (average cost of $0.51 per individual needle and syringe).
Only 10 of the 15 originally sampled pharmacies participated in this 1-year study. In neighborhoods with high drug-use prevalence, three participating pharmacies stopped selling nonprescription needles and syringes because of drug user-related incidents. The first pharmacy dropped out after a used syringe was found on a display shelf, the second stopped selling nonprescription needles and syringes after a drug user disrupted business a few hours after a robbery, and the third pharmacy dropped out after a transvestite drug user hustled an upper-middle-class customer for money to buy a syringe. Two of the original seven pharmacies in Wethersfield never sold nonprescription needles and syringes because they feared incidents with drug users.
Results of the telephone survey showed that pharmacy managers differed across the two strata (i.e., largest cities versus other locations) in terms of their reported estimated prevalence of injection drug use in their respective neighborhoods. That is, 75 percent of the managers in the largest cities reported that there were many injection drug users in their neighborhood, compared with 15 percent of all managers in other locations.
Findings from the survey also indicated that in the five largest cities stratum, 73 percent of the participating pharmacies sold nonprescription syringes in November 1993, compared with 85 percent in all other locations. Although a lower proportion of large-city pharmacies reported selling nonprescription syringes than pharmacies in other locations, a significantly larger number of syringes were sold in these five cities than in the other locations (i.e., 93 per pharmacy per week compared with 12 per pharmacy per week, respectively).
Of the participating pharmacy managers, 19 percent reported that they had experienced one or more negative incidents related to the sale of nonprescription syringes. A content analysis of these incidents revealed that 76
percent of the serious incidents (e.g., being attacked with a syringe by a drug user, a customer injecting drugs inside the pharmacy, used syringes found inside and outside the pharmacy) involved used syringe disposal issues. The authors (Valleroy et al., in press) estimated that by November 1993 (15 months after the laws were enacted), 83 percent of all Connecticut pharmacies were selling nonprescription syringes. These data suggest that the new Connecticut laws increased injection drug user access to sterile syringes, especially in areas with high prevalence of drug use.
Injection Drug Users' Behaviors
The CDC project (Groseclose et al., in press) assessed injecting drug users' knowledge of the new laws, their needle and syringe purchasing practices, and their needle-sharing behaviors, both before and after the new laws were in effect. To do so, the investigators conducted two cross-sectional surveys of active injection drug users employing a structured interview format. The first survey (n = 124) occurred shortly after the new laws were in effect (between August and November 1992) and the second cross-sectional survey (n = 134) was carried out between March and June 1993. In the initial survey, injection drug users were asked to describe their practices and behaviors in June 1992 (30 days before the laws were enacted). The second cross-sectional survey assessed injection drug user practices and behaviors after the new laws were implemented by asking participants to describe their behaviors during the 30 days preceding the interview. Findings concerning injection drug users' knowledge of the new laws (i.e., that it is legal to purchase and possess up to 10 needles and syringes) show that the percentage of active injectors who said they knew that they could both buy and possess clean needles and syringes increased significantly from 55 to 68 percent between the two time periods. At the second survey period, fewer than 8 percent did not know that either purchase or possession of needles was newly legally authorized, down from 22 percent interviewed during the baseline survey. These results reflect that drug users became aware of the changes in the laws.
In investigating active injectors' supply sources, the study compared purchasing sources during the month preceding the new laws with purchasing sources at the time of the second survey (9 to 12 months after the laws were enacted). Results clearly show a shift in most frequently reported source of needles and syringes from the street before the laws were enacted to pharmacies 9 to 12 months after the laws were enacted. That is, 74 percent of the injection drug users interviewed reported they had purchased syringes on the street before the new laws, compared with 28 percent after the laws were enacted. Moreover, 78 percent of the study participants
reported they had purchased syringes from a pharmacy after the new laws compared with 19 percent before the laws were enacted.
The study also found a decline in sharing between the first and second surveys. In the earlier survey, which was done before the law went into effect, 52 percent of those active injectors who had ever shared reported some sharing in the previous month; in the later survey, this dropped to 31 percent. This finding reinforces the expectation that eased legal access to syringes results in less sharing.
One finding that appeared peculiar at first was that there was no significant increase observed in the percentage of active injectors who reported that they always carried needles and syringes with them on the street after the new laws were enacted (26 percent before compared with 34 percent after the new laws). The research team compared the percentage of active injectors who reported having been harassed by police at least once during the 6-month period before (13 percent) and the 6-month period after the new laws were in effect (14 percent). They found that approximately the same percentage of participants in both cross-sectional surveys (13 and 14 percent, respectively) reported having been harassed at least once in both of these periods. Therefore, the unchanged level of always carrying needles corresponds to the unchanged level of de facto police activity rather than the de jure legal change.
In an attempt to assess whether police officers were at higher risk of needlesticks due to the increase in needles in circulation resulting from these new laws, researchers reviewed Occupational Safety and Health Administration records for reported needlestick incidents and found no significant changes in the number of needlestick injuries among Hartford police (i.e., six injuries in 1,007 drug-related arrests for the 6-month period before the new laws, compared with two in 1,032 arrests for the 6-month period after the new laws were enacted).
SHOULD THE LAWS BE CHANGED
CDC's evaluation of the Connecticut experience indicates that needle scarcity can be reduced by repealing existing legal hurdles (paraphernalia and prescription laws) as they relate to injection equipment. Moreover, CDC's monitoring of police harassment of injection drug users for possession of paraphernalia seems to reinforce the concern, voiced by participants at the panel's workshop (see Chapter 4), that law enforcement officers need to be educated about the health effects and other ramifications of the laws. Pharmacists and law enforcement officers can play a pivotal role in increasing the availability of sterile needles and syringes. Street officers need to be made aware of the severe health consequences associated with needle scarcity and of the significant role they can play in reducing the spread of
HIV in the general population. Merely changing the laws and obtaining the approval and endorsement of police department heads may not be sufficient.
A similar principle applies to pharmacists (Koester, 1994; Compton et al., 1992). Although it is legal to purchase needles and syringes in most states in this country, many pharmacists refuse to sell to injection drug users. There is a clear need to address the concerns of pharmacists and pharmacy owners and law enforcement officers, as well as to make them realize how critical their collaboration is in the nation's fight against AIDS. Furthermore, CDC's study disclosed the importance of educating injection drug users about any changes in laws that impact their ability to purchase or carry injection equipment.
Changing the Laws
As briefly discussed above, in their attempt to curtail the use and sale of illicit drugs and the harmful consequences that often accompany drug abuse, legislators have enacted statutes that indirectly address drug use (paraphernalia and prescription laws). Moreover, the judicial system appears to have recognized the timebound merit of drug paraphernalia and prescription laws as they pertain to injection equipment (Gostin, 1993). However, the fact remains that this is a matter that the legislature—not the courts—must address and resolve. As the epidemiologic data on HIV presented in Chapter 1 suggest, the prominent—and increasingly critical—role of injection drug use in transmitting HIV, within both the injecting drug user and, subsequently, the general population (heterosexual and perinatal), requires immediate action to protect public health.
In view of the hindering effects of paraphernalia and prescription laws on the prevention of HIV transmission, the panel urges that state prescription laws be repealed and that all paraphernalia laws be amended to allow for the possession of drug injection equipment. It should be noted that this recommendation has already been made in major policy reports by other groups (Institute of Medicine of the National Academy of Sciences, 1986; National Commission on Acquired Immune Deficiency Syndrome, 1991).
The panel is cognizant that any legislative changes would inevitably require some form of government regulation (Des Jarlais et al., 1994) and proposes that public health agencies and the research community (i.e., National Institutes of Health, Centers for Disease Control and Prevention) appoint a task force to delineate the details of these regulations—for example, eligibility requirements for program participation, type of exchange of needles allowable (one-for-one or otherwise), maximum number of needles a participant is allowed to exchange per visit—to ensure that they meet health needs and concerns regarding the spread of HIV. Regulatory guidelines must address such issues as the disposal of used needles and syringes,
who can distribute injection equipment, the maximum number of needles and syringes an individual can purchase or possess, and many other issues.
Consequences
The experiences of other industrialized countries (Porter and Gostin, 1991) that have no paraphernalia or prescription laws (e.g., Netherlands, Italy) point out that merely amending these statutes to alleviate the scarcity of sterile injection equipment should not be expected to eliminate syringes and needles as a important route of HIV transmission. In that regard, it seems important to distinguish between two levels of syringe and needle availability (T. Stephen Jones, Centers for Disease Control and Prevention, February 1994, personal communication): the first, community availability, is a necessary condition for the second level, time of injection availability, to be met. However, it is not a sufficient condition for ensuring that the second level will be attained. That is, amending paraphernalia and prescription laws would increase the availability of syringes and needles within a community but would not necessarily ensure that injection drug users have a sufficient supply of sterile equipment for each injection. Availability at the time of injection is more difficult to achieve (Bruneau, 1994).
Countries in which community availability is no longer a problem (e.g., Netherlands, Australia, Canada, France) still observe the sharing of syringes and needles at the time of injection. This is in part due to the fact that time of injection availability is a function of multiple factors, including drug purchasing, preparing, and distributing norms and practices among injectors and environmental factors (e.g., police harassment and community availability). It is important to realize that increasing community availability will not completely eliminate sharing behavior.
In the United States, nine states have prescription laws. These nine states are located in a region with high concentrations of injection drug users (the Northeast). In these states, injection drug users (who typically have limited contact with medical services) have to visit a physician to obtain a prescription. Elimination of this barrier would increase the availability of sterile injection equipment to injection drug users whose access is currently quite limited. Finally, repeal of the prescription laws in the nine states that have them would increase availability.
Although needle exchange programs tend to reduce the discarding of used syringes (for they are assets, when exchangeable), augmenting the pharmacy sales of needles will tend to increase the number of needles that reach users and pose a potential increase in the total number of discarded needles. Alternatives for dealing with these issues have already been put forth in the United States and other countries. For example, in an attempt to minimize the improper disposal of used needles, some countries (e.g.,
Australia) make available special containers that allow for proper disposal of used syringes in the needle exchange programs and pharmacies. Systematic evaluation of this issue should begin promptly and must take into account the concerns of community groups presented in Chapter 4 of this report.
CONCLUSIONS
The panel concludes that:
-
Any marked increase in the supply of sterile needles to injection drug users above current levels through pharmacy sales is likely to call for new measures to ensure the safe disposal of used needles. Whereas this problem has been solved in other countries (e.g., Australia provides special containers in public places that allow for proper disposal of used syringes, as well as individual returnable containers for used syringes), it is important to design good solutions to the disposal issue in the United States now.
-
Laws that make it a criminal offense to possess injection equipment (paraphernalia laws) were designed to decrease the prevalence of injection drug abuse, but they also inhibit users from carrying their own supply of needles and syringes and thus unwittingly contribute to the sharing of contaminated ones.
-
Laws requiring a prescription for the purchase of new needles and syringes (prescription laws) constrain the availability of sterile injection equipment and thus promote the sharing of contaminated equipment.
RECOMMENDATIONS
The panel recommends that:
-
The Assistant Secretary for Health should cause the disposal issue to be studied and appropriate means of needle disposal to be developed. A task force should be appointed and should include health safety specialists, infectious disease specialists, injection drug use researchers, and community representatives/civic leaders.
-
Legislative bodies should remove legal sanctions for the possession of injection paraphernalia.
-
Appropriate legislative bodies should repeal laws in the nine states that require a prescription in order to purchase injection equipment.
NOTE
REFERENCES
American Civil Liberties Union 1994 Briefing Book: Needle Exchange, Harm Reduction, and HIV Prevention in the Second Decade, R. Harlow and R. Sorge, eds. New York, NY: ACLU AIDS Project.
Brecher, E.M. 1941 The case of the missing mosquitoes. Reader's Digest February.
Bruneau, J. 1994 Presentation at informal workshop convened by Panel on Needle Exchange and Bleach Distribution Programs, National Research Council and Institute of Medicine. January 5.
Carlson, R.G. 1991 HIV Needle Risk Behavior Among IDUs in West Central Ohio: An Ethnographic Overview. Invited paper presented at the Conference on AIDS and Anthropology in the United States, Atlanta, Georgia, October 16-17.
Celentano, D.D., D. Vlahov, S. Cohn, J.C. Anthony, L. Solomon, and K.E. Nelson 1991 Risk factors for shooting gallery use and cessation among intravenous drug users. American Journal of Public Health 81(10):1291-1295.
Centers for Disease Control and Prevention 1993 Morbidity and Mortality Weekly Report, March 5, Vol. 42, No. 8.
Chaisson, R.E., A.R. Moss, R. Onishi, D. Osmond, and J.R. Carlson 1987 Human immunodeficiency virus infection in heterosexual intravenous drug users in San Francisco. American Journal of Public Health 77(2):169-172.
Cherubin, C. 1967 The medical sequelae of narcotic addiction. Annals of Internal Medicine 67:23-33.
Chitwood, D.D., C.B. McCoy, J.A. Inciardi, D.C. McBride, M. Comerford, E. Trapido, H.V. McCoy, J.B. Page, J. Griffin, M.A. Fletcher, et al. 1990 HIV seropositivity of needles from shooting galleries in South Florida. American Journal of Public Health 80:150-152.
Compton III, W.M., L.B. Cottler, and S.H. Decker 1992 Legal needle buying in St. Louis. American Journal of Public Health 82:595-596.
Courtwright, D. 1982 Dark Paradise: Opiate Addiction in America Before 1940. Boston, MA: Harvard University Press.
1992 A century of American narcotic policy. Pp. 1-61 in D.R. Gerstein and H.J. Harwood, eds., Treating Drug Problems (Volume 2). Institute of Medicine. Washington, DC: National Academy Press.
Des Jarlais, D.C., and S.R. Friedman 1992 AIDS and legal access to sterile drug injection equipment. Drug Abuse: Linking
Policy and Research, E.D. Wish, ed. Annals, American Academy of Political and Social Science 521:42-65.
Des Jarlais, D.C., and W. Hopkins 1985 ''Free" needles for intravenous drug users at risk for AIDS: Current developments in New York City. New England Journal of Medicine 313(23):1476.
Des Jarlais, D.C., S. Friedman, and W. Hopkins 1985 Risk reduction for acquired immune deficiency syndrome among intravenous drug users. Annals of Internal Medicine 103:755.
Des Jarlais, D.C., S. Friedman, and D. Strug 1986 AIDS and needle sharing within the IV drug use subculture. Pp. 141-160 in The Social Dimensions of AIDS: Methods and Theory, D. Feldman and T. Johnson, eds. New York, NY: Praeger.
Des Jarlais, D.C., S.R. Friedman, and R. Stoneburner 1988 HIV infection and intravenous drug use: Critical issues in transmission dynamics, infection outcomes, and prevention. Review of Infectious Diseases 10(1):151-158.
Des Jarlais, D.C., D. Paone, S.R.Friedman, N. Peyser, and R.G. Newman 1994 Regulating syringe exchange programs: A cautionary note. Journal of the American Medical Association 272(6):431-432.
Feldman, H.W., and P. Biernacki 1988 The ethnography of needle sharing among intravenous drug users and implications for public policies and intervention strategies. Pp. 28-39 in Sharing Among Intravenous Drug Abusers: National and International Perspectives, R.J. Battjes and R.W. Pickens, eds. Research Monograph 80, National Institute on Drug Abuse.
Friedland, G., and R. Klein 1987 Transmission of human immunodeficiency virus. New England Journal of Medicine 317:1125-1135.
Friedland, G.H., C. Harris, C. Butkus-Small, D. Shine, B. Moll, W. Darrow, and R.S. Klein 1985 Intravenous drug abusers and the acquired immune deficiency syndrome (AIDS): Demographic, drug use, and needle-sharing patterns. Annals of Internal Medicine 145(8):1413-1417.
Friedman, S., A. Neaigus, D.C. Des Jarlais, J.L. Sotheran, J. Woods, M. Sufian, B. Stepherson, and C. Sterk 1992 Social intervention against AIDS among injecting drug users. British Journal of Addiction 87(3):393-404.
Friedman, S.R., M.C. Doherty, D. Paone, and B. Jose 1994 Notes on Research on the Etiology of Drug Injection. Paper commissioned by the Panel on Needle Exchange and Bleach Distribution Programs, National Research Council and Institute of Medicine.
Gostin, L. 1991a The interconnected epidemics of drug dependency and AIDS. Harvard Civil Rights-Civil Liberties Law Review 26:113-184.
1991b The needle-borne HIV epidemic: Causes and public health responses. Behavioral Sciences and the Law 9:287-304.
1993 Law and policy. Pp. 35-61 in Dimensions of HIV Prevention: Needle Exchange, J. Stryker and M.D. Smith, eds. Menlo Park, CA: The Henry J. Kaiser Family Foundation .
Groseclose, S.L. 1993 Legislative Changes, The Connecticut Experience: Survey of Injecting Drug Users. Presentation at Workshop on Needle Exchange and Bleach Distribution Programs, Panel on Needle Exchange and Bleach Distribution Programs, National Research Council and Institute of Medicine. Baltimore, MD, September 28.
Groseclose, S.L., B. Weinstein, T. S. Jones, L.A. Valleroy, L.J. Fehrs, and W.J. Kassler in press Impact of increased legal access to needles and syringes on practices of injecting drug users and police officers—Connecticut, 1992-1993. Journal of Acquired Immune Deficiency Syndromes.
Hopkins, W. 1988 Needle sharing and street behavior in response to AIDS in New York City. In Needle Sharing Among Intravenous Drug Abusers: National and International Perspectives, R. Battjes and R. Pickens, eds. Rockville, MD: National Institute on Drug Abuse.
Howard, J., and P. Borges 1972 Needle sharing in the Haight: Some social and psychological functions. Pp. 125-136 in It's So Good, Don't Even Try It Once, D. Smith and G. Gay, eds. New Jersey: Prentice Hall.
Inciardi, J. 1990 HIV, AIDS and intravenous drug use: Some considerations. Journal of Drug Issues 20(2):181-194.
Institute of Medicine and National Academy of Sciences 1986 Confronting AIDS: Directions for Public Health, Health Care, and Research. Washington, DC: National Academy Press.
Kane, S., and T. Mason 1992 The limits of epidemiological categories and the ethnography of risk. Pp. 199-224 in The Time of AIDS, G. Herdt and S. Lindenbaum, eds. Newbury Park, CA: Sage Publications.
Kleinman, P.H., D.S. Goldsmith, S.R. Friedman, W. Hopkins, and D.C. Des Jarlais 1990 Knowledge about and behaviors affecting the spread of AIDS: A street survey of intravenous drug users and their associates in New York City. International Journal of the Addictions 25(4):345-361.
Koester, S.K. 1989 When Push Comes to Shove: Poverty, Law Enforcement and High Risk Behavior. Paper presented at the Annual Meeting of the Society for Applied Anthropology, Santa Fe, New Mexico.
1992 Ethnography and High Risk Drug Use. Paper presented at the Fifty Fourth Annual Meeting of the College on the Problems of Drug Dependence, Keystone, Colorado, June 23.
1994 Copping, running and paraphernalia laws: Contextual variables and needle risk behavior among injection drug users in Denver. Forthcoming in Human Organization 53(3).
Koester, S.K., and L. Hoffer 1994 Indirect sharing: Additional HIV risks associated with drug injection. AIDS & Public Policy Journal Summer:100-105.
Louria, D.B., T. Hensle, and J. Rose 1967 The major medical complications of narcotic addiction. Annals of Internal Medicine 67:1-32.
Magura, S.J., I. Grossman, D.S. Lipton, et al. 1989 Determinants of needle sharing among intravenous drug users. American Journal of Public Health 79(4):459-462.
Mandell, W., D. Vlahov, C. Latkin, M. Oziemkwska, and S. Cohn 1994 Correlates of needle sharing among injection drug users. American Journal of Public Health 84(6):920-923.
Marmor, M., D.C. Des Jarlais, H. Cohen, S.R. Friedman, S.T. Beatrice, N. Dubin, W. el-Sadr, D. Mildvan, S. Yancovitz, U. Mathur, et al. 1987 Risk factors for infection with human immunodeficiency virus among intravenous drug abusers in New York City. AIDS 1(1):39-44.
Metzger, D., G. Woody, D. DePhilippis, T. McLellan, C.P. O'Brien, and J.J. Platt 1991 Risk factors for needle sharing among methadone treated patients. American Journal of Psychiatry 148:636-640.
Morgan, H.W. 1981 Drugs in America: A Social History, 1800-1980. Syracuse, NY: Syracuse University Press.
Murphy, S. 1987 Intravenous drug use and AIDS: Notes on the social economy of needle sharing. Contemporary Drug Problems Fall:373-395.
Musto, D.F. 1987 The American Disease: Origins of Narcotic Control. Expanded Edition. Oxford, Eng.: Oxford University Press.
1991 Opium, cocaine and marijuana in American history. Scientific American July:40-47.
National Commission on Acquired Immune Deficiency Syndrome 1991 Report: The Twin Epidemics of Substance Use and HIV. Washington, DC: National Commission on Acquired Immune Deficiency Syndrome.
Nelson, K.E., D. Vlahov, S. Cohn, A. Lindsay, L. Solomon, and J.C. Anthony 1991 Human immunodeficiency virus infection in diabetic intravenous drug users. Journal of the American Medical Association 266:2259-2261.
Office of National Drug Control Policy 1992 Needle exchange programs: Are they effective? ONDCP Bulletin No. 7. Washington, DC: Executive Office of the President.
Page, J.B., P.C. Smith, and N. Kane 1990a Shooting galleries, their proprietors, and implications for prevention of AIDS. Drugs and Society 51(1):69-85.
Page, J.B., D. Chitwood, P. Smith, N. Kane, and D. McBride 1990b Intravenous drug use and HIV infection in Miami. Medical Anthropology Quarterly 4(4):56-71.
Pascal, C.B. 1988 Intravenous drug abuse and AIDS transmission: Federal and state laws regulating needle availability. Pp. 119-136 in Needle Sharing Among Intravenous Drug Abusers: National and International Perspectives , R.J. Battjes and R. Pickens, eds. Research Monograph 80, National Institute on Drug Abuse.
Porter, L., and L. Gostin 1991 Legal Environment Surrounding the Availability of Sterile Needles and Syringes to Injecting Drug Users. Unpublished manuscript.
Reuter, P. 1992 Hawks ascendant: The punitive trend of American drug policy. Daedalus: Journal of the American Academy of Arts and Sciences 121(3):15-52.
Schoenbaum, E.E., D. Hartel, P.A. Selwyn, R.S. Klein, K. Davenny, M. Rogers, C. Feiner, and G. Friedland 1989 Risk factors for human immunodeficiency virus infection in intravenous drug users. New England Journal of Medicine 321(13):874-879.
Selwyn, P.A., and P. Alcabes 1994 The Potential Impact of Needle Exchange Programs on Health Outcomes Other Than HIV and Drug Use. Paper prepared for the Panel on Needle Exchange and
Bleach Distribution Programs, National Research Council and Institute of Medicine.
Selwyn, P.A., C. Feiner, C.P. Cox, C. Lipshutz, and R.L. Cohen 1987 Knowledge about AIDS and high-risk behavior among intravenous drug users in New York City. AIDS 1(4):247-254.
Valleroy, L.A. 1993 Legislative Changes, The Connecticut Experience, Pharmacies. Presentation at Workshop on Needle Exchange and Bleach Distribution Programs, Baltimore, MD, September 28. Panel on Needle Exchange and Bleach Distribution Programs, National Research Council and Institute of Medicine.
Valleroy, L.A., B. Weinstein, S. Groseclose, W. Kassler, T.S. Jones, and R. Rolfs 1993 Evaluating the Impact of a New Needle/Syringe Law: Surveillance of Needle/Syringe Sales at Connecticut Pharmacies. Poster C24-3189. IXth International Conference on AIDS, Berlin, Germany, June 6-11.
Valleroy, L.A., B. Weinstein, T.S. Jones, S.L. Groseclose, R.T. Rolfs, and W.J. Kassler in press Impact of increased legal access to needles and syringes on community pharmacies' needle and syringe sales—Connecticut, 1992-1993. Journal of Acquired Immune Deficiency Syndromes.
Vlahov, D., A. Muñoz, S. Cohn, D.D. Celentano, J.C. Anthony, and K.E. Nelson 1990 Association of drug injection patterns with antibody to human immunodeficiency virus type 1(HIV-1) among intravenous drug users in Baltimore. American Journal of Epidemiology 132:847-856.