8
Differences in Rates of Dementia Between Ethno-Racial Groups
Barry Guland, David Wilder, Rafael Lantigua, Richard Mayeux, Yaakov Stern, Jiming Chen, Peter Cross, Eloise Killeffer
Epidemiological Background
Dementia Rates and Subtypes
Dementia is the most common major mental disorder of very old age. This condition is characterized by a global and progressive decline in cognitive functions such as memory for recent events, learning, orientation, calculation, verbal ability, spatial manipulations, reasoning, planning, and competence in other complex tasks. Most noticeably, there is advancing impairment in the performance of the tasks of everyday living including managing personal business, shopping, cooking, dressing, feeding, and toileting. Extreme dependency on family and other care givers eventually supervenes, insight is lost, wandering and other disturbing behaviors emerge, frailty increases, and life is shortened.
The most common form of dementia is Alzheimer's disease, a slowly developing degenerative process of uncertain cause, affecting neural pathways, especially those serving memory functions, over large areas of the brain. Multiinfarct dementia arises from interruption of the blood supply to numerous small areas of the brain, with a cumulative effect over long periods of time. Neither condition can be reliably prevented or halted by treatment, though experimental long- and short-term interventions are being actively studied (Berg et al. 1992). Taken together, these two subtypes account for the great majority of dementias found in elderly populations.
Dementia is among the leading causes of disability and death in old age. Costs of care in the formal long-term care sector, including personal assistance
and residential services, are high for the individual and for Medicaid or other third-party payers; often dementia places a financial as well as an emotional burden on informal care givers (Brodaty and Hadzi, 1990; O'Connor et al., 1991a, 1991b). These are serious consequences of dementia for the victims, their families, and other care givers, and they raise concerns that can be informed by data on the frequency and distribution of rates of dementia, its precedents, and its outcomes.
For persons 65 years or older, community studies report prevalence rates of dementia generally around 4 percent to 6 percent, but as high as 10 percent; an additional 2 percent to 3 percent are found in surveys of nursing homes (Gurland and Cross, 1982; Gurland, 1996a, 1996b; Bland et al., 1988; Folstein et al., 1991; Livingston et al., 1990). The proportions of people with dementias who live in community dwellings rather than nursing homes will be influenced by the availability and affordability of nursing home residence and the willingness of care givers to continue supporting the person with dementia at home. In most nursing homes and in many home care programs, longer term clients are predominantly people with dementias.
Prevalence rates of dementia are low in the age group 65 to 74 but increase rapidly with age, roughly doubling with each decade and culminating in rates reported to be as high as 40 percent or more for those surviving beyond age 85. Incidence rates are below 1 percent for the young old (65 to 74 years) but rise to 4 percent or more for the very old, 85 years and older. Dementia can last 10 or more years, and duration averages around 5 to 7 years depending on the age of occurrence.
Subtypes of dementia in Western nations are mainly Alzheimer's disease (about 75%), with a modest proportion (about 15%) being purely multi-infarct dementia. Around 15 percent of people with dementia have both Alzheimer's and multi-infarct features. Some studies have found these proportions to be 50 percent, 40 percent and 10 percent, respectively (Folstein et al., 1991). A residual group of around 10 percent includes people with secondary dementias (e.g., stroke dementia, Parkinsonism, or Huntington's chorea) and potentially treatable causes such as increased intracranial pressure; metabolic, toxic, or anoxic conditions; and depression. Alcohol and drug dependence as possible causes of dementia are uncommon (1% to 2%) in most reports on community elders (Bland et al., 1988; Kramer et al., 1985; Weissman et al., 1985). Females are reported by some studies to have higher rates. Risk factors for Alzheimer's disease itself have been attributed to head injury, stroke, coronary artery disease, depression, age of mother at birth, Down's syndrome, family history, and (very recently) abnormalities of the apolipoprotein E genotype series.
In addition to the small proportion of people who present convincing signs of dementia but are found to have an initially reversible condition, there are people with such treatable conditions as major depressive disorder or delirium due to drug or other toxicity whose dementias are simply mislabeled as primary demen-
tia because the symptoms are not correctly evaluated. However, for the vast majority of properly diagnosed dementias, treatments to reverse the disease process are still experimental; there is no proven method of halting the progress of the condition. Nevertheless, health and social care management can provide invaluable relief to the patient through symptomatic approaches and attention to control of complications. It can also assist the care givers in maintaining the sufferer at home through psychological support and personal care services and, where necessary, can ease admission to a dignified, engaging, and nurturing sheltered environment.
Estimating Rates of Dementia
Almost all studies of prevalence and incidence of dementia rely upon two stages of assessment. The first stage is directed at maximizing the chances of finding cases in the population by use of screening techniques. Because these screens are brief and are reliable in the hands of interviewers from a wide variety of professional and nonprofessional backgrounds, it is feasible to administer them in the private homes of large numbers of the population under study. Simple threshold scores separate likely from unlikely cases of dementia, with a sensitivity and specificity that can be adjusted by raising or lowering the threshold score to suit the needs of the study.
In the second stage, concerned mainly with ascertaining the diagnosis, the study design may allow for an attempt to fully evaluate all likely cases or a representative selection of them. Typically this evaluation is carried out in a clinic equipped for conduct of an inquiry into presenting symptoms and signs, a history of the onset and course of the illness, a battery of psychological tests, general and neurological physical examination, and general and specific special investigations including brain imaging. Clinical judgment and/or algorithms are then applied to the accumulated information to make a diagnosis of dementia with reference to operational diagnostic criteria. A sample of unlikely cases, referred blind to the clinic personnel, is usually also fully evaluated in order to check on the efficiency of the screening procedure.
In some studies by design, and in some others by default, a greater or lesser proportion of likely cases may not be fully evaluated. In those circumstances, the rates of dementia may be projected from the findings on the cases fully evaluated. The projections take into account the fraction of subjects above and below the threshold of the screen who are expected to have dementia on the basis of the findings for the subjects who were fully evaluated.
Uncertainties enter into the case-finding and case ascertainment stages for the well-known reasons that confront surveys: nonresponding subjects, attrition between stages of evaluation, and unreliability of measures. Of particular importance for ethno-racial comparisons of rates and associations of dementia are the confounding effects of socioeconomic status on the validity of the two classificatory stages.
Ethno-Racial Differences in Rates of Dementia
Rates for indicators of dementia (cognitive impairment scores or diagnosis) have been reported to vary between ethno-racial groups. Among community residents aged 65 years and older, African Americans have been found to have a higher prevalence of a diagnosis of dementia, especially vascular dementias, than non-Hispanic whites (Heyman et al., 1991). Researchers have found concordant results using cognitive scores as an indicator of dementia, validated by diagnosis of a subsample (Folstein et al., 1991). The converse has been reported by researchers (de la Monte et al., 1989) drawing upon autopsy results; their rates were higher among non-Hispanic whites than among African Americans; non-Hispanic whites had more dementia associated with Parkinson's disease, and African Americans had more dementia associated with multi-infarct disease and alcoholism. Several other studies have reported higher rates of cognitive impairment and dementia among African Americans and Hispanics than among non-Hispanic whites (Escobar et al., 1986; Murden et al., 1991; Weissman et al., 1985).
Putative Effects of Education
Elders who have had low education are consistently reported as having unusually high rates of dementia (Gurland, 1981; Li et al., 1991; Folstein et al., 1991; Stern et al., 1994; Gurland et al., 1995b). Groups with lower education have been found to have a relatively greater proportion of multi-infarct dementia (Folstein et al., 1991) or increased rates of alcoholic dementia and unspecified types of dementia (Fratiglioni et al., 1991). However, the possibility of ethno-racial bias in assessment and diagnosis introduces ambiguity about the interpretation of study results that is mainly but not entirely attributable to educational influences (Salmon et al., 1989; Li et al., 1989; Murden et al., 1991).
Any substantial differences in rates of dementia between ethno-racial groups merit serious attention, given the personal and societal consequences of dementia; the related need to plan, finance, and deliver appropriate services; and the call for research to advance understanding and effective treatment of dementia. Moreover, valuable clues to etiology and treatment might emerge from the study of such ethno-racial variation. However, the inferences and action that should flow from findings of ethno-racial differences in rates of dementia continue to be inhibited by a critical uncertainty: namely, the possibility that case-finding and case ascertainment techniques might be biased towards overestimating dementia rates in socially disadvantaged ethno-racial groups (O'Connor et al., 1991b).
This issue is often expressed in terms of uncertainty about the distortions of educational bias. Educational achievement is not equally distributed among the various ethno-racial groups. Poorly educated people may make errors on the screening measures because they have less experience than better educated people
in answering these kinds of test questions. Furthermore, the questions are often directed at general knowledge (e.g., the name of the president of the United States), calculation, spelling, repetition of phrases, current dates, residential address, and the like. The same biases may enter the full evaluation through the psychological test battery. Furthermore, clinical judgments may be influenced to discount the profile of deficits of a poorly educated person or to add undue weight to deficits in a highly educated person.
One root source of these ambiguities is that information derived from screening and full evaluation is concentrated on a person's current status and little reliance can be placed on historical information. Yet dementia is essentially a longitudinal diagnosis; the diagnosis implies a progressive course of illness. Thus, a person who falls short of normal standards at the time of screening or full evaluation is assumed to be on a decline trajectory, whereas he or she might have been below standard throughout life.
Various corrections have been suggested for redressing ethno-racial bias in cognitive test items (Uhlmann and Larson, 1991; Teresi et al., 1995). However, a recent analysis of data (Gurland et al., 1995) from the reporting component of the North Manhattan Aging Project registry found the educational effects on rates of dementia were robust, persisting across 13 different methods of salient classifications, which ranged from criterion-based diagnosis to cognitive scores, stages of severity, and mathematical techniques for minimizing ethno-racial bias in assessment.
Methodological Issues
The North Manhattan Aging Project and the Active Life Expectancy Study
The study presented here was designed to examine rates of dementia in three ethno-racial groups: Hispanics, African Americans, and non-Hispanic whites, with due regard for potential ethno-racial biases. Data in this paper have been generated from work still in progress in a collaboration between the Columbia University Stroud Center/Center for Geriatrics, Sergievsky Center, and Department of Medicine.
The North Manhattan Aging Project and the Active Life Expectancy Study have jointly established a registry of people with dementia, stroke, and Parkinson's disease. The registry draws from a network of key informants (reporting component) and a cohort (survey component) of randomly selected people 65 years or older within a clearly bounded geographic area of north Manhattan. The analyses in this report are restricted to the survey component and the part of the reporting component that covered nursing home residents whose present or last location was in the target area.
Our Methods for Minimizing Biases in Ethno-Racial Comparisons of Dementia
We describe the strategies that we have developed or adopted for our ethno-racial comparisons of rates of dementia. The following description is abstracted and modified from three papers (Gurland, et al., 1992; Gurland et al., 1995b; Gurland, 1996a). Many of these strategies are shared with other studies in this field; some are innovative.
Case Findings
We adopted two contrasting routes for case finding: a network of key reporters and a house-to-house survey of a representative sample of elders. Both methods were aimed at the same target: a geographically delimited multicultural population. The target area is 13 adjacent census tracts in north Manhattan: census data indicated that there would be substantial numbers of elders in each of the groups: Hispanic, African American, and non-Hispanic white. Poverty, crime, and unemployment rates are high in the study target area. A single hospital (Columbia-Presbyterian Medical Center) provides almost all inpatient and emergency medical care and much of the ambulatory medical services to the study's target area. A large contingent of Hispanic physicians runs solo or small group practices in the neighborhood, supplemented by some multicultural large group practices. Social and community agencies are well organized and in close touch with each other.
In the reporting component, which began in 1989, study staff repeatedly scrutinize records of subjects reported to be living in or entering service sites that are known to have a high rate of dementia, such as nursing homes, home care programs, and certain neurological clinics; staff members also receive referrals according to specified criteria from key informants in a wide variety of health, social, and community sites. If a person is eligible by present or (in nursing homes) last location, the research team institutes a further examination, with a screen for cognitive impairment. A referral for a research diagnostic evaluation is made if the 90 percent sensitivity threshold on the cognitive screen is exceeded and in a subsample of the remainder of the subjects.
The survey component first interviewed people in 1993 and 1994; its sampling frame consists of all Medicare beneficiaries, 65 years or older, within the geographic target area. By the use of random methods in replicated subsamples, subjects in the survey are drawn equally from the three cultural groups until the number of elders in any group is exhausted or the total of elders interviewed exceeds 2,100. All who cooperate are given a subject interview. In selected representative survey subsamples, an informant, if one is available, is interviewed and a diagnostic evaluation is carried out on all subjects regardless of screen score. In all other subsamples, the subject interview is given to all subjects, but
an informant interview and a referral for a research diagnostic evaluation are made only if the 90 percent sensitivity threshold on the cognitive screen is exceeded and in one in four of the rest of the subjects. Trained raters administer the interviews using laptop computers for face-to-face interviews in the subject's home. Informant interviews are conducted by telephone.
The advantage of this two-pronged approach is that since all cases come from the same target area, researchers can compare the distribution of cases of dementia lodged on the registry through the two routes: key reporters and survey. The reported cases give a more complete representation of people with advanced dementia and people who are receiving services for dementia, whereas the survey cases offer better representation of mild and moderate cases and of people who are normal. The extent to which ethno-racial differences are constant across the two methods increases confidence in the findings.
The delimited nature of the target area makes it possible to superimpose the two methods of case finding. It also makes it possible for the researchers to conduct reevaluation over a long period of time, to track service utilization, and to maintain the cooperation of the community by facilitating services for those found to be in need. The other side of the coin is that the geographic generalizability of the findings must be tested through other studies, either previous or planned. Of course, were a nationally representative study of this kind achievable without sacrifice of the methodological refinement, its results would not be generalizable to the target area chosen for this study or to any other multicultural community in the nation. In our opinion, robust hypotheses worthy of further testing, especially with regard to etiological leads, are just as likely to emerge from a delimited sample as from a national one. Similar views could be expressed with respect to the public health significance of the findings or their significance for planning for service delivery.
In assembling the sample of subjects to represent elders in the target community for purposes of the survey, we added a frame for elders in nursing homes to that obtained from the Medicare list. There is no overlap between these frames: only the Medicare list was used for elders at home, and only the nursing home list was used for elders in nursing homes. This sampling procedure is more accurate than the alternative of tracing elders not found at home to a location in a nursing home (although this was done as a mutual check on the completeness of the frames). Any nursing home known to admit residents from the target area was repeatedly surveyed to capture new admissions during the course of the study.
Since this is a study of elder populations, not of nursing homes, the number of subjects in nursing homes is restricted to their appropriate contribution to the total sample of elders. We accomplished this by taking the number of elders who completed in-home interviews as the numerator and the total of all elders in the target area as the denominator, and applying the proportion this produced to all elders from the target area who completed interviews in the nursing homes over the same period as the in-home survey.
For purposes of calculating prevalence rates, the denominators are the number of persons interviewed in the first 27 subsamples of the in-home survey cohort and in the nursing home segment of the reporting component during the same period. The denominator numbers in the survey cohort (but not in the nursing home sample) were adjusted to fit the census age profile of the study target area. We have already described the adjustment of the total size of the nursing home sample. The numerators are the number of cases of dementia identified in the same samples with corresponding adjustments. The criterion diagnosis for dementia was used for those subjects who received a diagnostic evaluation (by a team designated as the clinical core), and it was projected from those subjects onto persons screened, but not diagnosed, by the use of the screen score probability of a diagnosis of dementia.
Screening and Field Classification Techniques
In both components of the study (i.e., reporting and survey components), efforts were made to render screening and field classification techniques as culture fair as possible. We conduct interviews in the subject's language of preference (English or Spanish). We prepared a Spanish translation of each assessment technique and checked it for comparability with the English version; in a few items, we chose a cultural equivalent rather than a literal translation.
We determined which subjects would be referred for full evaluation by analyzing the alternatives to show which was most consistent in operational characteristics (i.e., specificity and sensitivity) across ethno-racial groups (Wilder et al., 1995). We assembled a compendium instrument incorporating five widely used screens for cognitive impairment and dementia and tested it in the reporting component of the North Manhattan Aging Project. We obtained the best operating characteristics on this population from the Comprehensive Assessment and Referral Evaluation cognitive screen (Golden et al., 1984; Teresi et al., 1984) and therefore selected it as the benchmark screen for the survey component.
During the study, when we accumulated sufficient data we applied item bias statistical methods to construct a new relatively culture-fair scale. Although this new scale was not used for screening purposes, it helped to confirm or rebut findings from the other scales.
Criterion Diagnosis
In both components of the study, a criterion diagnosis is made after full evaluation by a research team (the clinical core). It is assumed (but arguable) that the resulting diagnostic classification has shed much of the potential ethno-racial biases, since the information at this evaluation is wide ranging, involves numerous internal checks on the diagnostic relevance of the information, and is guided by algorithms and operational criteria for integration of information from
psychometric tests (with educational norms) and from laboratory and clinical sources. This diagnosis is made independently of, and is blind to, the field assessments. Details of the diagnostic process are given elsewhere (Stern et al., 1992).
After all evaluations are completed, diagnoses are assigned at a diagnostic conference. The initial separation is between demented and nondemented patients. If a patient is demented, then the cause of dementia is specified further. The two main subtypes of dementia have suggestive clinical and brain imaging indicators, but neuropathology must ultimately be combined with the in vivo signs in order to reach a definitive diagnosis.
All subjects who screen positive and a proportion of subjects who fall below the critical threshold score on the screen, in both the reporting and the survey components of the registry, are referred blind for diagnostic evaluation by the research teams. In addition, in selected subsamples of the survey, all subjects are referred for diagnostic evaluation.
Biological Indicators
Indicators of biological status, in the form of brain imaging, molecular genetics (especially the role of apolipoprotein E genotypes), and autopsy material, are obtained where subjects permit it. There are established relationships between these objective indices and measures of cognitive impairment or diagnoses of dementia subtypes (Maestre et al., 1995; Mayeux et al., 1993). Consistency of these relationships among ethno-racial groups adds confidence to the ethno-racial comparisons of cognitive and diagnostic data. Inconsistencies raise questions about bias in screening techniques or diagnosis or suggest the need for reconsideration of the biological underpinnings of the dementing conditions in the various ethno-racial groups.
Longitudinal and Outcome Information
We follow subjects annually, in both components of the study, in order to gather longitudinal and outcome information. Diagnoses of dementia of the two common subtypes (which account for the great majority of cases in a population) carry with them a prediction that a progressive decline will be detectable at annual intervals. Diagnosis may have to be revised when a case does not follow the expected course. Concurrent corrections of this kind incrementally reduce misclassifications due to ethno-racial biases, since ethno-racial membership does not convey immunity from deterioration over a year or more.
Dementia and Quality of Life
Examining the impact of dementia on the quality of life is an innovative strategy (Gurland et al., 1992, 1993). It is an attempt to go beyond comparing conditions that merely meet diagnostic criteria to comparing conditions with defined consequences for the patient, the family, and society (Katz and Gurland, 1991). We use this strategy only in the survey component.
It would be tautological to accept as unbiased only results that showed no differences in rates of dementia between ethno-racial groups, yet it is difficult to be certain that emergent differences do not reflect some hidden biases, despite our efforts to find and eradicate them. There may also be a differing pattern of biological processes that account for dementia in the various ethno-racial groups. Therefore, an appeal to culture-fair methods and biological indices may still leave lingering doubts as to the meaning of ethno-racial differences in rates of dementia. To cut this Gordian knot, we examine the extent to which dementia, as classified by our methods, has comparable consequences for quality of life in the ethno-racial groups. We look for the quality-of-life consequences that are characteristic of dementia: decreases in functioning in the higher level, cognitively controlled tasks of daily living, such as using the telephone, handling cash, managing personal business, and following a medication regime (Reed et al., 1989; Reisberg et al., 1985). We also look for subjective complaints of memory lapses (O'Connor et al., 1990) and nonspecific impairments of quality of life such as affective suffering (Wands et al., 1990).
Introducing observations on the impact of dementia, as diagnosed, on quality of life moves the focus from a medical model, in which diagnosis carries an implicit association with disease, its prognosis, and its treatment, to a more holistic model, in which diagnosis is viewed as a means of connecting causes to an explicit set of consequences for the person. The assumption that real differences in rates are accompanied by real causes and real consequences drives concern about whether ethno-racial variation in these rates is real or an artifact of diagnostic bias. The holistic model reverses this line of reasoning: diagnosis is real if it has real consequences; real consequences have real causes. Ethno-racial differences in rates of diagnosis are important if they are accompanied by corresponding differences in real consequences for quality of life. A corollary of this premise is that diagnosis, or some surrogate category, can be usefully modified to act as a marker of a distinctive pattern of consequences.
The subject interview in the survey component includes a wide range of self-reported functioning in daily tasks of living and in acts of memory. The informant interview (again, in the survey component only) covers a similar range of information on the subject's current functioning and historical information on the course of the subject's symptoms; it is obtained independently and blind to the subject interview. In addition, at the time of the interview with the subject, a performance test, the Medication Management Test, is administered (Gurland et
al., 1994). Items from several standard measures of functioning have been imbedded in the subject and the informant interviews: Katz Index of Activities of Daily Living (Katz et al., 1963), Lawton Instrumental Activities of Daily Living (Lawton and Brody, 1969), and Comprehensive Assessment and Referral Evaluation (CARE) scales of activity limitation and mobility (Gurland et al., 1977; Golden et al., 1984). The items are directed at distinctive perspectives on functioning: self-report, informant report, and performance testing; cognitively and physically driven functions; and positive as well as negative functioning.
The full picture of quality of life includes at least these many aspects of functioning. For simplicity, we have selected a few important aspects, which will be sufficient for illustrative purposes. Each of these aspects has salience to quality of life. In this respect, it is worth noting that the self-perceptions reported by the subject with dementia (e.g., complaints about memory) are central to quality-of-life consequences and are not vitiated by presumed loss of insight. In fact, the subject's report correlates highly with the other measures of functioning, such as informant reports or performance testing, until late in the course of dementia (Chen, 1995).
Complaints of Memory Lapses. Subjective complaints of memory lapses are included because they are increased by the presence of dementia, although these complaints also occur at a lower rate in elders without dementia and may be missing in a substantial proportion of persons who do have dementia (O'Connor et al., 1990). This cluster of complaints is presented as a reflection of quality of life, not as a diagnostic indicator.
Affective Suffering. Items from a scale of depression in elders, the CARE Homogeneous Scale of Depression (Golden et al., 1984; Gurland et al., 1977; Teresi et al., 1984), have been reorganized to fit a quality-of-life perspective. Twenty of these items form a modified scale of affective suffering, which has a reliability coefficient alpha of .818. The content of the modified scale is free of items confounding mental and physical problems. Seven levels of severity of affective suffering are derived from references to intensity and extensity of distress. The extremes of intensity are defined at one pole by such expressions as ''life not worth living" and at the other pole by an absence of negative symptoms together with claims of being "very happy." The corresponding extremes of extensity bear upon the persistence of affective distress at one pole and the absence of symptoms at the other. The size and severity of the worst level were set to make possible useful comparisons with major depression (the most severe diagnostic category of clinical depression in the standard nomenclature), and the combined size and severity of the two worst levels (intolerable and desperate affective suffering) were designed to be comparable to the combined diagnostic categories of major depressions and dysthymia (a form of chronic depression) (American Psychiatric Association, 1994).
Dementia and Service Utilization
An examination of the impact of dementia on service utilization (in the survey component only) is in part justified for reasons analogous to those put forward on behalf of the quality-of-life consequences of dementia. If ethno-racial differences in the rate of dementia are seen as bearing upon the relative needs of the different populations for therapeutic interventions, then the current use of relevant services by these populations is germane to an estimation of the extent to which these needs are being fulfilled.
Convergence of Conclusions
Information accumulated from the survey and the full diagnostic evaluation offers several ways of classifying and analyzing the rates and consequences of dementia. Where all sources and pathways of analyses converge on the same inference regarding relative rates of dementia among ethno-racial groups, we can have greatest confidence in the conclusions.
Border-Zone Dementias and Nondementias
It can be expected that diagnostic misclassifications due to ethno-racial biases will rarely occur for people who are obviously demented (advanced dementia) or clearly normal. Rather, misclassifications will occur mainly for people who have early or ambiguous signs of dementia, whom we have designated as border-zone dementias, and for those who are not diagnosably demented but have evidence of cognitive impairment, whom we call border-zone nondementias. Thus, the designation of a border-zone range is expedient for the study of ethno-racial influences on the validity of diagnoses of dementia and for testing methods of reducing bias (Gurland et al., 1995a, 1995b; Wilder et al., 1994, 1995). For operational purposes, the border-zone range of cognitive impairment (including border-zone dementias and nondementias) is defined as impairment that, in the reporting component of the registry, predicted criterion diagnosis in about half the instances overall, with a probability between about 30 percent and 70 percent for the scores within this range.
Since rates depend in part on how broad a concept of dementia is used, we refer to both advanced dementias and border-zone dementias when comparing ethno-racial groups. Advanced dementia represents a narrow (conservative) view of dementia; a broad concept is represented by expanding the definition of a case to include the border-zone dementias.
Designation of Ethno-Racial Membership
Ethno-racial classification is recorded (in both components of the study) from self-designation of ethno-racial membership. Our comparison groups are
Hispanics, African Americans, and non-Hispanic whites. Study procedures were modeled on those adopted by the U.S. Census Bureau for self-identification of racial and ethnic membership. Elders were assigned to the three ethno-racial groups on the basis of their self-description as to whether they came from Spanish/Hispanic origin or descent and if they did not, whether they were white or "black/Negro." In cases of doubt about the validity of the information obtained from the subject, an informant was consulted.
This typology is not synonymous with race, ethnicity or culture.1 Nevertheless, the typology we used has the merit of replicating the census classification and contributing to informed decisions on allocation of health care resources based on census data. Moreover, this method of classification is the same as that usually underlying published reports on variation in rates of dementia among populations.
The study classification differed from the one that was initially available in the sampling frame, as Table 8-1 shows. Medicare lists made a distinction between black and white self-identification only. A match with 5,000 Spanish surnames was then superimposed. Table 8-1 shows discrepancies between the initial sampling frame and the ultimate study classifications. As many as 26 percent of the initial non-Hispanic white groups were reclassified as Hispanic; the other two groups were more stable. The study classification is validated by the preferred language of the interviewee: of those who preferred to be interviewed in Spanish, 98 percent were Hispanic in the final classification.
For purposes of collecting adequate numbers of the three ethno-racial groups in a community with unequal ethno-racial proportions, we stratified people by ethno-racial membership according to information on Medicare lists and the superimposed surname match. The result was a smaller non-Hispanic white group than we had intended in the ultimate study classification.
Most classifications of ethno-racial populations are reasonable entry points in the search for leads that might help us discover sociocultural, psychological, behavioral, or biological influences on the variation of rates of mental disorder. Refinement of the classification would have to be part and parcel of pursuing any such emergent leads. For example, variation tied to genetic differences might require subgroups with more homogeneous gene pools. Knowledge of the relationship of etiologies to styles of living (e.g., diet, smoking) would be advanced by analyses keyed to cultural subgroups. Service utilization and outcome differences might be best understood by issues of language, church affiliations, family constellations, neighborhood structures, and the matching ethno-racial health care arrangements.
TABLE 8-1 Ethno-Racial Classification: Contrasts Between Initial and Final Identification
Other Socioeconomic Information
We recorded this information (collected in both components of the study) from the most reliable informant; if the subject was judged unreliable, then a family member was consulted.
We gathered a history of educational achievement and condensed it into categories of 0 to 4 years, 5 to 11 years, and 12 or more years of education. The category of less than 5 years of schooling is of special interest in studies of dementia. Illiterate or marginally literate persons are disproportionately encountered in minority groups, but because they perform poorly on standardized screening instruments, they have been excluded from some studies or inadvisably combined with the next higher educational group.
We documented income by having the subject (or an informant) review a card displaying monthly income brackets. The card specifically mentioned all sources of income, including wages, salaries, Social Security or retirement benefits, help from relatives, and rent from property.
Results
General Results
Yields from the Survey Component
The response rates for completed survey interviews vary among subsamples but are 62 percent overall. Comparison of the age and gender distributions of the responders and nonresponders for each ethno-racial group shows no significant differences for gender. However, responders in all ethno-racial groups are younger than nonresponders, and the differences rise to statistical significance for Hispanics (p = .001) and non-Hispanic whites (p = .01). The proportions 75 years and over for nonresponders and responders, respectively, are for Hispanics, 51.5 percent versus 39.6 percent; for African Americans, 49.7 percent versus 44.1 percent; and for non-Hispanic whites, 51.9 percent versus 42.9 percent.
As Table 8-2 shows, 1,449 subjects in the community setting received a field interview in the first 27 representative subsamples. The proportionate number selected for nursing home residents is 40. This total is greater than the number with an informant interview or the number referred to diagnostic evaluation in the clinical core. Eighty-one percent of subjects referred to the clinical core completed the full diagnostic evaluation.
Overrepresentation
Sampling strategies led to overrepresentation of certain subgroups, those 75 years of age or older, non-Hispanic whites, and persons in nursing homes. Wherever appropriate, we have weighted the numbers in the cells formed by ethno-
TABLE 8-2 Sizes of Samples of Subjects Interviewed by Age and Ethno-Racial Groups
racial membership and age to match either the corresponding profile of characteristics evident in the original Medicare sampling frame or the census profile for the target area. The total number of nursing home subjects in the combined nursing home and in-home survey cohort has been adjusted to the proportion of target area elders who are in nursing homes. Stratification of ethno-racial groups in comparisons makes it unnecessary to adjust for this characteristic.
Differences in Prevalence Rates of Dementia
Rates of criterion dementias for the ethno-racial groups are found to be higher in Hispanics and African Americans and lowest in non-Hispanic whites as Figure 8-1 shows. The comparisons are made separately for age groups 65 to 74, 75 to 84, and 85 and older. In all age categories, Hispanic and African-American groups are comparable: if anything, the Hispanics have slightly higher rates, but
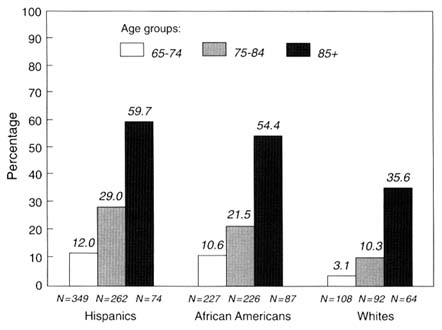
FIGURE 8-1 Rates of dementia by age and ethno-racial group. NOTE: The sample was restricted to 27 subsamples of community-residing elders, 65 years and older, N = 1,449, from the North Manhattan Aging Project target area; there was a proportionate group in nursing homes, N = 40. Diagnosis was made by research clinical evaluation or was generated from the probability of a diagnosis based on screen scores, which could be a decimal number.
there are no significant differences in any of the paired comparisons of these two ethno-racial groups within age categories. However, the non-Hispanic white group has dramatically lower rates of dementia in all age brackets compared with either of the other two ethnic groups. All of these paired comparisons are statistically significant: significance levels for the age groups 65 to 74, 75 to 84, and 85 and older are p < .01, p < .001, and p < .001, respectively, for Hispanics, and p < 0.05 for African Americans in all three comparisons.
All ethnic groups show a steep rise of rates of dementia with age. The graphic shape of the relationship between age and prevalence rates of dementia is close to linear for Hispanics and quadratic in non-Hispanic whites, with African Americans being intermediate in form.
Mislabeling
We compared the people with and without dementias in each ethno-racial group with an eye to the possibility that severe depression, presenting as a dementia-like syndrome (Larson et al. 1985; O'Connor and Roth, 1990), might be open to ethno-racial bias in assessment and classification of dementia. Depression rates are also raised in true dementia, especially in certain subtypes of dementia, such as those associated with multi-infarction or Parkinson's disease. Further complicating the meaning of concurrent depression and dementia is that more than half of the group with this combination later deteriorates cognitively (Kral 1983; Reding et al., 1985; McAllister and Price, 1982; O'Connor and Roth, 1990). As seen in Figure 8-2, severe depression is strikingly high among non-Hispanic whites with dementia, lower in Hispanics with dementia, and extremely low in the African-American dementia group. These findings are exactly opposite to what would be expected to support mislabeling of depression as an explanation for the excesses of dementia in the Hispanic and African-American groups.
Prevalence and Other Indices of Rates
Variation in prevalence rates among the ethno-racial or educational groups could be due to differences in incidence, duration, mortality, age of onset, or any combination of these. The incidence phase of our study began in the fall of 1994; neither new cases nor mortality rates are yet known. We have collected retrospective information from the informant on the duration and age of onset of functional and memory impairments of the subject, but we regard these data as unreliable. The age of onset was alleged to be earlier for Hispanic and African-American groups than for non-Hispanic whites: the onset of impairments after age 84 was 8 percent, 20 percent, and 40 percent, respectively. If this information is accurate, it might in part account for the relatively lower rates of dementia among the non-Hispanic whites since a later onset leaves a shorter duration of time for the condition to exist.
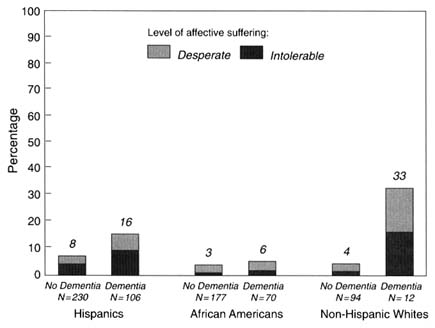
FIGURE 8-2 Affective suffering in subjects with and without dementia. NOTE: The sample was restricted to 27 subsamples of community-residing elders, 65 years and older, N = 1,449, from the North Manhattan Aging Project target area. Only those elders who have a research clinical evaluation are included.
Effect of the Breadth of the Concept of Dementia
The relatively higher rates of dementia among Hispanics and African Americans compared with non-Hispanic whites are consistently evident for concepts of dementia of varying breadth, as Figure 8-3 shows. For advanced dementias, rates for the Hispanics 10.0%) and African Americans (7.1%) are higher than for non-Hispanic whites (4.0%): compared with non-Hispanic whites, the Hispanic rates are significantly higher (p < .003), but not the African-American rates (p < .10, nonsignificant). The relative ethno-racial rates are similar if border-zone dementias are added: Hispanics, 20.8 percent; African Americans, 18.2 percent: and non-Hispanic whites, 7.2 percent. Now, however, compared with non-Hispanic whites, the Hispanic rates are significantly higher at the p < .001 level, and the African-American rates are also significantly higher (p < .001). Hispanic and African-American rates remain not significantly different. Even if people with-
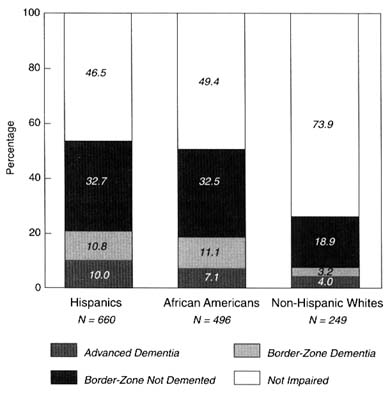
FIGURE 8-3 Rates of dementia by breadth of concept and ethno-racial group. NOTE: The sample was restricted to 27 subsamples of community-residing elders, 65 years and older, N = 1,449, from the North Manhattan Aging Project target area; there was a proportionate group in nursing homes, N = 40. Diagnosis was made by research clinical evaluation or was generated from the probability of a diagnosis based on screen scores. This excludes persons with paradoxical classifications: those who had normal cognitive levels but were diagnosed as demented, or who had severe cognitive impairment but were not diagnosed as demented, and 44 persons who were projected to be paradoxical.
out dementias but with cognitive impairment are taken into account, non-Hispanic whites have substantially lower prevalence rates (26%) than Hispanics (53.5%) or African Americans (50.6%), and the significance levels of differences are unchanged. The ethno-racial differences in the prevalence rate of dementia are apparently robust enough to withstand changes in the breadth of the concept of dementia.
Risk Factors
Some of the possible causes of variations of rates in dementia between subgroups within ethno-racial groups were mentioned in the introductory section; these causes include age, gender, education, head injury, hypertension, coronary artery disease, alcohol, malnutrition, and genetic predisposition. However, our current principal interest is in variation of rates of dementia between ethno-racial groups; previous studies (mentioned in the introduction) led us to expect that education might be a main association of this variation. Since educational achievement is related to level of income, immigration patterns, and age cohort, we also included reference to these characteristics in our examination of the associations between education and rates of dementia.
Educational Associations
There are pronounced distribution differences by education, age, income, and immigration among the three ethno-racial groups. Only 48.8 percent of Hispanics are aged 75 years or older, of whom 10.4 percent are 85 years or older, while African Americans have 57.6 percent aged 75 or older, including 15.5 percent who are 85 or older. The non-Hispanic whites are the oldest of the three groups, with 57.5 percent who are 75 years or older, including 23.0 percent aged 85 years or older. Differences between educational distributions among the three ethno-racial groups are even more marked. Over 40 percent of the Hispanics have completed less than 5 years of schooling, but almost 90 percent of African Americans and virtually all non-Hispanic whites have gone beyond this level. Just 12.3 percent of the Hispanics have completed 12 or more years of schooling, but over one-third of the African Americans and almost three-quarters of the non-Hispanic whites have reached this educational level. Income differences are equally striking: 59.3 percent of Hispanics, 34.1 percent of African Americans, and 16.7 percent of non-Hispanic whites have monthly income of less than $551. Respective percentages for income over $1,000 are 9.5 percent, 25.2 percent, and 46.0 percent.
A multivariate regression analysis of education on rates of dementia, with age, income, gender, and ethno-racial membership taken into account is shown in Table 8-3. In this regression analysis, income for certain nursing home residents could not be reliably ascertained. Uncertainty was encountered particularly because of the custom of spending down financial reserves and divesting oneself of assets and income prior to admission in order to qualify for Medicaid reimbursement. In order to include all subjects with missing information on income, mean values were substituted.
Age and education are the most significant and strongest associations of rates of dementia, with odds ratios of 6.1 and 4.3, respectively. With age and education controlled, ethno-racial membership loses its association with rates of
TABLE 8-3 Regression of Age, Education, Income, Gender, and Ethno-Racial Groups on Rates of Dementia
|
Variable |
Beta |
p |
Odds Ratio |
95% Confidence Interval |
|
Age |
1.81 |
.000 |
6.1 |
5.47, 6.82 |
|
Education |
-1.46 |
.000 |
4.3 |
3.42, 5.42 |
|
Income |
-0.35 |
N.S.a |
— |
— |
|
Sex (male = 1) |
-3.02 |
N.S. |
— |
— |
|
Ethnicity/race |
-2.56 |
N.S. |
— |
— |
|
a N.S. = nonsignificant. Note: The sample was restricted to 27 subsamples of community residents (65 year and older), N = 1,449, from the North Manhattan Aging Project target area. Diagnosis was made by research clinical evaluation or generated from the probability of a diagnosis on the basis of the screen score. Forty nursing home residents are included in this analysis. All missing values of income are substituted by mean values. Each ethno-racial group is treated as an individual category. |
||||
dementia, and neither income nor gender is significantly associated with rates of dementia. The variance in rates of dementia accounted for by age and education is 19.6 percent, and the variance accounted for by all these demographic variables taken together, 20.3 percent. Even when the regression is repeated combining the two disadvantaged groups (namely Hispanics and African Americans) for comparison with non-Hispanic whites, ethno-racial membership still does not attain a statistically significant level.
Subtypes of Dementia Among Ethno-Racial Groups
Nonspecific risk factors for dementia should affect rates regardless of subtypes, but there may be ethno-racial risks specific to subtypes. The distributions of subtypes of dementia (border-zone and advanced stages combined) are shown in Table 8-4 for each ethno-racial group. The great majority of dementias are diagnosed as Alzheimer's disease in Hispanics and African Americans, and this is the exclusive diagnosis in non-Hispanic whites.
Alzheimer's disease with stroke is particularly high among African Americans. However, if the subcategory of stroke-related Alzheimer's disease is combined with the category of Alzheimer's disease with stroke, then the ethnoracial rates are fairly similar: 18.2 percent for Hispanics, 28 percent for African-Americans, and 20 percent for non-Hispanic whites. Alcohol-related dementia is not prominent in any group. We note that although there are ethno-racial differences in subtypes, overall rates are accounted for largely by age and educational controls. This supports a view that the risks attached to age and education are for increased rates of dementia in general, rather than for specific subtypes of dementia, and is also in keeping with the possibility that Alzheimer's disease is
TABLE 8-4 Distributions of Subtypes of Dementia by Ethno-Racial Group
often the underlying disorder even when manifestations suggest diagnosis of another subtype.
Other Risk Factors: Income and Immigration
Income was shown in the regression analysis not to be a significant influence on rates of dementia when education and age are controlled, although this finding does not fully disentangle the effects of income and education. It is also difficult to separate the effects of immigration from those of ethno-racial membership and education. While Hispanics were almost never born in the United States, African Americans were almost never born in a foreign country. The percentages of foreign-born in these two subsamples are 98.2 and 9.6, respectively. Non-Hispanic whites are evenly divided between domestic and foreign birth, but have low rates of dementia.
Quality-of-Life Impairments
As long as a discussion about ethno-racial differences in rates of dementia does not go beyond counting the frequencies of diagnostic categories of dementia or cognitive scores, there is a risk that the clinical and policy implications of the findings will be obscured. Uncertainty about the appropriate techniques for assessment and classification that are unbiased by ethno-racial characteristics may inhibit the drawing of conclusions from findings. Therefore, the following
series of analyses details the impact on the quality of life of people with dementia in the three ethno-racial groups.
Memory Complaints
Complaints about memory are greatly increased in dementia within each ethno-racial group, as Figure 8-4 shows. Among Hispanics and non-Hispanic whites, there is a clear step-up of memory complaints in people with and without dementia, with people in the two dementia categories (border zone and advanced) being decidedly worse than those in the two nondementia groups (normal and border zone). This is also evident, although less consistently, for the African Americans. Among non-Hispanic whites, people with advanced dementias show fewer complaints than those with border-zone dementias, possibly as loss of insight supervenes.
These findings confirm that the condition of dementia is troubling to all three ethno-racial groups and support the value of employing the broader concept of dementia (i.e., including border-zone as well as advanced stages) for understanding the elder's sense of the difficulties accompanying dementia. Specifically, the border-zone dementia that occurs in relatively high rates in the Hispanic and African-American groups is as serious in the consequences for subjective distress, expressed by memory complaints, as is the advanced dementia that is more prevalent in the non-Hispanic white group.
The type of memory problem most prominently noticed by the sufferer varies among the ethno-racial groups. Certain tasks served by memory are probably either more important, or more of a challenge, for one ethno-racial group than another and are thus more likely to be singled out as problematic when memory fails. However, some complaints about memory are also offered by normal people, and those complaints are therefore weaker indicators of the effects of dementia.
Tasks of Daily Living
Dementias typically undermine independence in carrying out the tasks of daily living from an early stage onwards (Edwards et al., 1991; Davis et al., 1990; Warren et al., 1989), although factors other than dementia also govern the level of functioning observed (Reed et al., 1989). The relative distribution of functional impairments, reported by an informant, between people with and without dementia and the rank order of the frequencies of task impairments are similar among the ethno-racial groups, as Figure 8-5 shows. For all ethno-racial groups, the level of impairment increases regularly from people who are normal to those with border-zone nondementias to those with border-zone dementias. In Hispanic and African-American groups, people with advanced dementia continue this progression. In non-Hispanic whites with advanced dementia, the impairments decrease
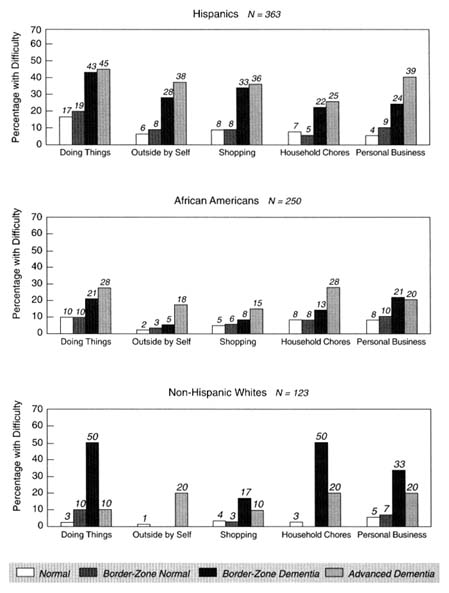
FIGURE 8-4 Memory complaints as reported by subject. NOTE: The sample was restricted to 27 subsamples of community-residing elders, 65 years and older, N = 1,449, from the North Manhattan Aging Project target area; there was a proportionate group in nursing homes, N = 40. Only the elderly who have a research clinical evaluation are included. This excludes 40 persons who had normal cognitive levels but were diagnosed as demented or who had severe cognitive impairment but were not diagnosed as demented.
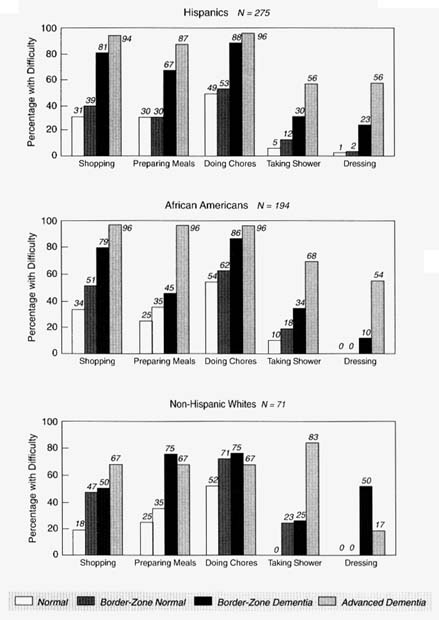
FIGURE 8-5 Task performance as reported by informant. NOTE: The sample was restricted to 27 subsamples of community-residing elders, 65 years and older, N = 1,449, from the North Manhattan Aging Project target area. Only the elderly who have a research clinical evaluation are included. This excludes 40 persons who had normal cognitive levels but were diagnosed as demented or who had severe cognitive impairment but were not diagnosed as demented.
somewhat; since these reports come from the informant, failure of insight due to dementia will not explain this finding.
Dementia appears to impair functioning to such an extent in the three ethno-racial groups as to overshadow reservations about the importance of the observed variation in rates among the ethno-racial groups, notwithstanding any possibility of ethno-racial bias in the assessment of cognitive status and in the criteria for diagnosis. These data again point to the pertinence, from the perspective of the dementia sufferer's quality of life, of including the broader concept of dementia (border-zone and advanced cases) in population studies. From these data, an argument might also be made for giving due attention to cases of border-zone nondementia on the grounds of their impact upon function in all three of the ethno-racial groups.
Affective Suffering
The relative distributions of affective suffering between people with and without dementia suggest that a shift to the intolerable and desperate levels of affective suffering takes place between the border-zone nondementia and the border-zone dementia stages. The longitudinal phase of the North Manhattan Aging Project is needed to confirm this inference. The frequency of the worst levels of affective suffering in dementia is much greater in the non-Hispanic whites and is least in the African Americans, as Figure 8-6 shows. Nevertheless, the increase of suffering appears to be marked for each ethno-racial group. These data strengthen the case for including the broader as well as the narrower definition of dementia in ethno-racial population studies.
Service Utilization
Among the more expensive long-term care services delivered to the elder population are nursing home placement, home health care, and hospitalization for acute episodes in chronic conditions. Use of these services is in part conditioned by type of health insurance coverage, as Table 8-5 shows. Since the frame for the sampling was drawn from Medicare lists, all subjects in the North Manhattan Aging Project and the Active Life Expectancy Study samples have Medicare insurance. It is estimated that more than 95 percent of the population 65 years or older resident in the target area, and more than 90 percent of any of the ethno-racial groups, are enrolled in Medicare. Among all three ethno-racial groups, the majority of people have either Medicaid or other health insurance in addition to Medicare. In general, people with dementia have an increased chance of being on Medicaid as opposed to other insurance coverage. However, while the majority of Hispanics and of African Americans with dementia have Medicaid and only a small minority of each group have other insurance, over 60 percent of the non-
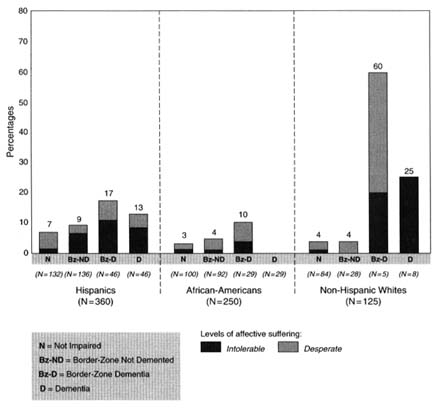
FIGURE 8-6 Affective suffering in stages of cognitive impairment. NOTE: The sample was restricted to 27 subsamples of community-residing elders, 65 years and older, N = 1,449, from the North Manhattan Aging Project target area. Only the elderly who have a research clinical evaluation are included here. This excludes 40 persons who had normal cognitive levels but were diagnosed as demented or who had severe cognitive impairment but were not diagnosed as demented.
Hispanic whites with dementia have other insurance, but less than 20 percent are covered by Medicaid.
Nursing Homes
Dementias account for the great majority of the use of nursing homes by residents from this target area. Utilization rates of nursing homes by people with dementia are vastly different between ethno-racial groups. Use by people with dementia among Hispanics (4.6%) and African Americans (9.9%) is very low compared with non-Hispanic whites (36.4%).
TABLE 8-5 Use of Health Insurance Coverage in Addition to Medicare (Part A) by Dementia in the Community
Home Care
To some extent, the neglect of nursing home admission as a resource for care of people with dementia in the African-American and Hispanic groups is made up for by a high volume of home care provision. This is particularly evident for African Americans with dementia in the community, who have a home care utilization rate of 45.7 percent. The corresponding rate for Hispanics is 31.6 percent, and for non-Hispanic whites 30 percent.
Emergency Clinics
Primary medical care is available in the target area in hospital-based, hospital-linked, and group and solo private practice. Emergency clinic visits can be taken as a rough guide to the degree to which a person is inadequately connected to the primary care system. Overall, emergency clinic attendance is reported for 37.7 percent of Hispanics with dementia and 38.8 percent of African Americans with dementia; for non-Hispanic whites with dementia it is 25 percent. Regard-
less of health insurance arrangements, there is a remarkably high use of emergency clinic services by people with dementia in the Hispanic and African-American groups. The utilization rate by non-Hispanic whites appears to be lower than for the other two ethno-racial groups, but the small size of the non-Hispanic white sample makes interpretation of this comparison uncertain.
Hospitalization
Admission to hospital inpatient status is increased by dementia for African Americans and non-Hispanic whites but not for Hispanics. Admissions are highest among African Americans with dementia (29.4%), next highest among non-Hispanic whites with dementia (23.5%), and lowest (19.6%) among Hispanics with dementia.
Discussion
Limitations of the Findings and Potential of the Methods
The methods of this study provide further opportunities for testing the robustness of the findings on ethno-racial variation in rates of dementia. Additional representative subsamples, amounting to almost 700 elders from the target area, have been surveyed; these supplementary data will be especially useful for checking those findings so far reported here on the relatively small sample of non-Hispanic whites with dementia. Enlargement of the database will also allow analyses to be linked to more homogeneous ethno-racial groups, such as Hispanic groups of distinctive national origin.
Epidemiological studies of ethno-racial variation in health conditions benefit from the collection of stratification of sampling to equalize sizes of ethno-racial groups. In this study, equalization was attempted through ''gerrymandering" of the target area on the basis of 1985 census data and stratification of recruitment based on the Medicare ethno-racial designation. However, non-Hispanic whites proved to have moved out of area more rapidly than expected; moreover, 26 percent of those designated non-Hispanic whites on Medicare lists were reassigned to the Hispanic group after interview. These situations resulted in a smaller group of non-Hispanic whites with dementia than planned.
In this presentation, the reporting component of the registry for Alzheimer's disease and related disorders has been combined with the survey component in order to amass a representative sample of elders from both community settings and nursing homes. Moreover, insight into possible selection biases can be pursued through the process of contrasting findings from the survey component and the reporting component. In economically disadvantaged neighborhoods, surveys typically fall short of desirable levels of response rates: resorting to information from a network of key informants can be a useful window into
selective biases arising from the loss of information on nonresponders. Analysis of response bias, so far, shows that there is a skewing of age distributions; this is further discussed later.
Study methods incorporate molecular genetics, neuroimaging, and autopsy material. These methods have not yet been applied to the interpretation of the observed ethno-racial variations in rates of dementia. Of key importance will be the relationships within each ethno-racial group between, on the one hand, these markers of the biological processes of dementia and, on the other hand, the classifications of dementia employed to compare rates of dementia in ethno-racial groups. Biological markers will assist in the evaluation of the ethno-racial consistency in diagnosis of dementia and can either support or conflict with the relative rates of dementia diagnosed in the three ethno-racial groups.
Also yet to be exploited is the longitudinal element of this study's methods, which will clarify the contribution of incidence, duration, and mortality to the relative prevalence rates in ethno-racial groups. Course and outcome data will also better define the extent and causal pathways of the impact of dementia on function and quality of life in the various ethno-racial groups and will allow distinctive patterns of service use to be discerned.
Self-designation of ethno-racial membership was found to be a satisfactory method of classification for purposes of making ethno-racial comparisons of rates of dementia and was found to be better than reliance on assignments based on surnames. We do not at this stage have a hypothesis that would require a more refined classification of ethno-racial groups, but it is likely that more demanding hypotheses will arise.
Ethno-Racial Variation in Prevalence Rates
Non-Hispanic whites have dramatically lower rates of dementia than the other two ethno-racial groups. These relative rates remain consistent for concepts of dementia of varying breadth: for advanced dementia taken alone, when border-zone dementia is also included, and even if nondementia with cognitive impairment is taken into account. Age and education are the most significant and strongest demographic associations of rates of dementia.
Skewing of the responding sample of elders towards a younger age would lead to an underestimate of the absolute prevalence rates of dementia, especially among Hispanics and non-Hispanic whites. However, the analyses of this paper are directed at relative (not absolute) rates of dementia among the ethno-racial groups: in this respect, rates in the African-American group would be overestimated relative to the other two ethno-racial groups. This bias is controlled by the regression analysis, by age stratification of comparisons groups, by adjustment of age profiles of all the ethno-racial groups to that found in the non-Hispanic white group, and by weighting ethno-racial age categories to match the original Medicare sampling frame or that of the census profile.
With age and education controlled, there appears to be little influence on variation among ethno-racial groups that is explained by reference to the selected other potential associations. Differences in subtypes of dementia do not account for the ethno-racial variation in dementia. Neither could income or immigration status be shown to contribute to this ethno-racial variation. Mislabeling of depression as dementia also could not be implicated. A later age of onset could produce a tendency towards the relatively lower rates of dementia noted among the non-Hispanic whites, but the evidence in favor of this hypothesis is built on an informant's retrospective report which is viewed with reservations about reliability and which must defer to the relevant data that the longitudinal phase of the study will generate. Nevertheless, if the Hispanic and African-American groups are adjusted to match the age-education profile of the non-Hispanic whites, significant differences in the rate of dementia remain between non-Hispanic whites and each of the other two ethno-racial groups.
Note that in referring to the results of analyses of relationships between dementia and education or income, we use the neutral term associations rather than terms suggesting causality. Nevertheless, it is clear that the processes that result in educational level are completed many decades before the onset of evidence of dementia resulting from either Alzheimer's disease or multi-infarctions. Moreover, the great majority of cases of dementia have an onset at 75 years or older, 10 or more years after the average age of retirement, making it unlikely that the level of income could be influenced by the dementia. There does remain the possibility of the existence of a pre-dementia condition (e.g., prodrome or state of vulnerability), so far undetected, that could intervene in the educational and income-producing years of life.
Ethno-Racial Consistency in the Associations of Dementia
For all ethno-racial groups, the level of independently (i.e., informant) reported functional impairment increases regularly from normal people to those with border-zone nondementia to those with border-zone dementia. Correspondingly, memory complaints are greatly increased in the two dementia categories (border-zone and advanced) within each ethno-racial group, although more clearly among Hispanics and non-Hispanic whites than for African Americans. Although there are ethno-racial differences in the types of memory problems that are the content of complaints, the increase of memory complaints in dementia is consistent for all ethno-racial groups. An excess frequency of intolerable and desperate levels of affective suffering was also found in the two dementia categories: this excess is much greater in the non-Hispanic whites and is least in the African Americans.
It appears that the concepts of dementia applied in this study are associated with considerable impairment of subjective and objective aspects of functioning
and qualities of life in the three ethno-racial groups. For these reasons, the findings on ethno-racial variation warrant attention. These findings also strengthen the argument for applying the broader concept (i.e., border-zone and advanced cases) of dementia in the investigation of ethno-racial variation in rates and effects of dementia. By extension, an argument can be made for investigating also the border-zone nondementias. All these categories have associations with impairments in the quality of life.
Working Hypotheses for the Effects of Education
Evidence is mounting that the educational effects on rates of dementia are real and not a methodological artifact, although it is supposed that education acts on a biologically predisposed substrate. Added to other brain insults and vulnerabilities, these educational factors raise the rates of Alzheimer's disease, multi-infarct dementia, and other subtypes of dementia. An account of the pathways by which education could appear to affect, or could actually affect, rates of dementia has been addressed in a recent paper (Gurland et al., 1995a, 1995b) by these investigators. The following summary is adapted from that paper:
- Selective hypothesis: Persons who will develop dementia in late life already have reduced cognitive reserve from early childhood. They therefore have difficulty in coping with the challenges of the schooling process. Consequently, they drop out of school and thus produce a relationship between lower educational achievement and later development of dementia. Barriers to continuing schooling come at distinctive educational levels depending on the inadequacies of a particular educational system.
- Associational hypothesis: Poor education goes hand in hand with many other potential mechanisms for inducing or precipitating dementia, including malnutrition, exposure to trauma, alcohol abuse, and inadequate health care.
- Educational hypothesis: Good, lifelong education builds and maintains a robust neurobiological structure and cognitive reserves that compensate for any deteriorative forces that might come to bear upon the brain. Beneficial effects earlier in life might be extended through continuing intellectual stimulation.
Ethno-Racial Differences in Service Utilization
Given the ethno-racial equivalencies in the quality-of-life associations of dementia, the inequalities in service utilization take on added importance. Hispanics and African Americans with dementia are much less likely than non-Hispanic whites with dementia to be admitted to a nursing home. Preference for, and reliance on, home care of people with dementia rather than nursing home admission is stronger for Hispanics and African Americans than for non-Hispanic whites. The high use of emergency clinic services by Hispanics and
African Americans could indicate that their preference for home care is not supported by the adequate availability of primary medical care. Less consistent with this pattern of service use are that admissions to hospitals are highest among African Americans and non-Hispanic whites with dementia and lowest among Hispanics with dementia. Analyses of the service impacts have been presented elsewhere, with suggestions for policy and planning efforts (Chen and Gurland, 1995).
Conclusion
Age and education account for a substantial part of the variance in rates of dementia among the three ethno-racial groups under study. Other demographic variables that were tested do not appear to make a significant contribution to this variance. The methods of the study were directed at reducing ethno-racial (including educational) bias in making diagnostic comparison and support the inference that the findings are related to a process of dementia and not to mislabeling.
Given the profiles of demographic and other variables occurring in these ethno-racial groups, rates of dementia in Hispanic and African-American groups are dramatically in excess of that found in non-Hispanic whites. In all ethnoracial groups the presence of dementia is accompanied by a deterioration in the quality of life: functional limitations in the tasks of daily living, self-report of memory problems, and affective suffering. This reinforces the view that the diagnosis of dementia reflects a process that carries serious consequences for each of the ethno-racial groups.
The findings identify several useful lines of inquiry. Further investigation of the associations between education and rates of dementia could lead to preventive interventions: three working hypotheses have been proposed here. Distinctive ethno-racial service utilization patterns by people with dementia point to the value of examining the needs and need fulfillment of people with dementia in these groups more closely, with special reference to the impact these needs and their fulfillment have on the quality of life of people with dementia and of their family.
Methodological advances demonstrated in this study could allow the issues in ethno-racial variation in dementia to be approached with some confidence that ethno-racial bias will not confound the interpretation of findings unduly. Perhaps, the most important contribution of these methods is to clarify the associations of this health disorder with impairments in the quality of life. This step changes the focus of inquiry from diagnostic labels to conditions with serious consequences for those afflicted and their families.
Acknowledgment
This work was supported by the following grants: (1) North Manhattan Aging Project, National Institute on Aging (principal investigator Barry Gurland, co-principal investigator David Wilder), Project 5 P01 AG7232-04. (2) Epidemiol-
ogy of Dementia in an Urban Community, National Institute on Aging (principal investigator Richard Mayeux, co-principal investigator Barry Gurland, and Yaakov Stern), Project P01 AG07232. (3) Active Life Expectancy Among Urban Minority Elderly, National Institute on Aging (principal investigator Rafael Lantigua, co-principal investigator David Wilder, co-investigators Barry Gurland, Sidney Katz) Project 5 R01AG10489-02. (4) A Transcultural Screen for Alzheimer's Disease and Related Disorders, New York Community Trust Foundation (principal investigator Barry Gurland), Project *NYCT CU 50404701. (5) The Morris W. Stroud, III, Program on Scientific Approaches to Quality of Life in Health and Aging, Endowment Fund (co-directors Barry Gurland and Sidney Katz).
Other staff members of the North Manhattan Aging Project were Virginia Barrett, Betty Barsa, Mabel Bolivar, Harold Browne, Jean Denaro, Priscilla Encarnacion, Maria Gonzalez, Lucia McBee, and Jeanne Teresi. Interviewers who completed over 100 interviews were Raul Almanzar, Carlomagno Baldi, Carlos Garcia, Consuelo McLaughlin, Annie Nuñez, Argentina Peralta, and Joseph Romero.
W. Edwards Deming designed the sampling plan for the North Manhattan Aging Project.
We thank the Bureau of Data Management and Strategy of the Health Care Financing Administration for providing the tape files of Medicare beneficiaries.
Assistants in formatting, illustrating, and compiling the bibliography for this paper were María Fernández and Aline Ratau.
References
American Psychiatric Association 1994 Diagnostic and Statistical Manual of Mental Disorders, 4th ed. Washington, DC: American Psychiatric Association.
Berg, L., J.P. Miller, J. Baty, and E.H. Rubin 1992 Mild senile dementia of the Alzheimer type: IV. Evaluation of intervention. Annals of Neurology 31:242 (abstract).
Bland, R.C., S.C. Newman, and H. Om 1988 Prevalence of psychiatric disorders in the elderly in Edmonton. Acta Psychiatrica Scandinavica 77(suppl. 338):57-63.
Brodaty, H., and P.D. Hadzi 1990 Psychosocial effects on carers of living with persons with dementia. Australian and New Zealand Journal of Psychiatry 24:351-361.
Chen, J. 1995 Insight in dementia: Increasing cognitive impairment and the strength of the relationship between self-report of function, informant report, and depression. Stroud Center publications 120. New York: Columbia University.
Chen, J., and B. Gurland 1995 Bird's Eye Reports. Issues 1-7. Stroud Center publications 110-117. New York: Columbia University.
Davis, P.B., J.C. Morris, and E. Grant 1990 Brief screening tests versus clinical staging in senile dementia of the Alzheimer type. Journal of the American Geriatrics Society 38:129-135.
de la Monte, S.M., G.M. Hutchins, and G.W. Moore 1989 Racial differences in the etiology of dementia and frequency of Alzheimer lesions in the brain. Journal of the National Medical Association 81:644-652.
Edwards, D.F., C.M. Baum, and R.K. Deuel 1991 Constructional apraxia in Alzheimer's disease: Contributions to functional loss. Physical and Occupational Therapy in Geriatrics 9(3-4):53-68.
Escobar, J.I., A. Burnam, M. Karno, A. Forsythe, J. Landsverk, and J.M. Golding 1986 Use of the Mini-Mental State Examination (MMSE) in a community population of mixed ethnicity. Journal of Nervous and Mental Disease 174:607-614.
Folstein, M.F., S.S. Bassett, J.C. Anthony, A.J. Romanoski, and G.R. Nestadt 1991 Dementia: Case ascertainment in a community survey. Journal of Gerontology 46:132-138.
Fratiglioni, L., M. Grut, Y. Forsell, M. Viitanen, M. Grafstrom, K. Holmen, K. Ericsson, L. Backman, and A. Ahlbom 1991 Prevalence of Alzheimer's disease and other dementias in an elderly urban population: Relationship with age, sex, and education. Neurology 41:1886-1892.
Golden, R.R., J.A. Teresi, and B.J. Gurland 1984 Development of indicator scales for the Comprehensive Assessment and Referral Evaluation (CARE) interview schedule. Journal of Gerontology 39(2):138-146.
Gurland, B.J. 1981 The borderlands of dementia: The influence of sociocultural characteristics on rates of dementia occurring in the senium. Pp. 61-84 in Clinical Aspects of Alzheimer's Disease and Senile Dementia, N.E. Miller and G.D. Cohen, eds. New York: Raven Press.
1996a Epidemiology of psychiatric disorders among elders. In Comprehensive Review of Geriatric Psychiatry (CRGP-II), J. Sadavoy, J. Foster, et al., eds. Washington, DC: American Psychiatric Press.
1996b Methods of screening for survey research on Alzheimer's disease and related dementias. In Alzheimer's Disease, Z.S. Khachaturian and T.S. Radebaugh, eds. Boca Raton, FL: CRC Press.
Gurland, B.J., and P.S. Cross 1982 Epidemiology of psychopathology in old age: Some clinical implications. Psychiatric Clinics of North America 5(1):11-26.
Gurland, B.J., P. Cross, J. Chen, D.E. Wilder, Z.M. Pine, R.A. Lantigua, and R. Fulmer 1994 A new performance test of adaptive cognitive functioning: The Medication Management (MM) Test. International Journal of Geriatric Psychiatry 9:875-885.
Gurland, B.J., S. Katz, R.A. Lantigua, and D. Wilder 1993 Cognitive function and the elderly. Pp. 21-26 in Proceedings of the 1991 International Symposium on Data on Aging, National Center for Health Statistics. Series 5(7). Washington, DC: U.S. Department of Health and Human Services.
Gurland, B., J. Kuriansky, L. Sharpe, R. Simon, P. Stiller, and P. Birkett 1977 The Comprehensive Assessment and Referral Evaluation (CARE): Rationale, development and reliability. International Journal of Aging and Human Development 8(1):9-14.
Gurland, B.J., D.E. Wilder, J. Chen, R. Lantigua, R. Mayeux, and J. Van Nostrand 1995a A flexible system of detection for Alzheimer's disease and related dementias. Aging: Clinical and Experiential Research 7:165-172.
Gurland, B.J., D.E. Wilder, P. Cross, R.A. Lantigua, J. Teresi, V.Barrett , Y. Stern, and R. Mayeux 1995b Relative rates of dementia by multiple case definitions, over two prevalence periods, in three cultural groups. American Journal of Geriatric Psychiatry 3:6-20.
Gurland, B.J., D.E. Wilder, P. Cross, J. Teresi, and V.W. Barrett 1992 Screening scales for dementia: Toward reconciliation of conflicting cross-cultural findings. International Journal of Geriatric Psychiatry 7:105-113.
Heyman, A., G. Fillenbaum, B. Prosnitz, and K. Raiford 1991 Estimated prevalence of dementia among elderly black and white community residents. Archives of Neurology 48:594 (abstract).
Katz, S., A.B. Ford, R.W. Moskowitz, B.A. Jackson, and M.W. Jaffe 1963 Studies of illness in the aged. The index of ADL: A standardized measure of biological and psychosocial function. Journal of the American Medical Association 185:914-919.
Katz, S., and B.J. Gurland 1991 Science of quality of life of elders: Challenges and opportunity. Pp. 335-343 in The Concept and Measurement of Quality of Life in the Frail Elderly, J. Birren, J.E. Lubben, J.C. Rowe, and D.E. Deutchman, eds. Los Angeles: Academic Press.
Kral, V. 1983 The relationship between senile dementia (Alzheimer type) and depression. Canadian Journal of Psychiatry 28:304-306.
Kramer, M., P.S. German, J.C. Anthony, M. Von-Korff, and E.A. Skinner 1985 Patterns of mental disorders among the elderly residents of eastern Baltimore. Journal of the American Geriatric Society 33:236-245.
Larson, E., B. Reifler, S.M. Sumi, C.G. Canfield, and N.M. Chinn 1985 Diagnostic evaluation of 200 elderly outpatients with suspected dementia. Journal of Gerontology 40:536-543.
Lawton, M.P., and E.M. Brody 1969 Assessment of older people: Self-maintaining and instrumental activities of daily living. Gerontologist 9:179-186.
Li, G., Y.C. Shen, C.H. Chen, Y.W. Zhau, S.R. Li, and M. Lu 1989 An epidemiological survey of age-related dementia in an urban area of Beijing. Acta Psychiatrica Scandinavica 79:557-563.
1991 A three-year follow-up study of age-related dementia in an urban area of Beijing. Acta Psychiatrica Scandinavica 83:99-104.
Livingston, G., A. Hawkins, N. Graham, B. Blizard, and A. Mann 1990 The Gospel Oak Study: Prevalence rates of dementia, depression and activity limitation among elderly residents in inner London. Psychological Medicine 20:137-146.
Maestre, G., R. Ottman, Y. Stern, B. Gurland, M. Chun, M.X. Tang, M. Shelanski, B. Tycko, and R. Mayeux 1995 Apolipoprotein E and Alzheimer's disease: Ethnic variation in genotypic risks. Annals of Neurology 37:254-259.
Mayeux, R., R. Ottman, M.X. Tang, L. Noboa-Bauza, K. Marder, B. Gurland, and Y. Stern 1993 Genetic susceptibility and head injury as risk factors for Alzheimer's disease among community-dwelling elderly persons and their first-degree relatives. Annals of Neurology 33(5):494-501.
McAllister, T.W., and T.R. Price 1982 Severe depressive pseudodementia with and without dementia. American Journal of Psychiatry 139:626-629.
Murden, R.A., T.D. McRae, S. Kaner, and M.E. Bucknam 1991 Mini-Mental State Exam scores vary with education in blacks and whites. Journal of the American Geriatric Society 39(2):149-155.
O'Connor, D.W., P.A. Pollitt, M. Roth, P.B. Brook, and B.B. Reiss 1990 Memory complaints and impairment in normal, depressed, and demented elderly persons identified in a community survey. Archives of General Psychiatry 47(3):224-227.
O'Connor, D.W., P.A. Pollitt, M. Roth, C.P. Brook, and B.B. Reiss 1991a Problems reported by relatives in a community study of dementia. British Journal of Psychiatry 156:835-841.
O'Connor, D.W., P.A. Pollitt, and F.P. Treasure 1991b The influence of education and social class on the diagnosis of dementia in a community population. Psychological Medicine 21(1):219-224.
O'Connor, D.W., and M. Roth 1990 Coexisting depression and dementia in a community survey of the elderly. International Psychogeriatrics 2:45-53.
Reding, M., J. Haycox, and J. Blass 1985 Depression in patients referred to a dementia clinic: A three year prospective study. Archives of Neurology 42:894-896.
Reed, B.R., W.J. Jagust, and J.P. Seab 1989 Mental status as a predictor of daily function in progressive dementia. Gerontologist 29:804-807.
Reisberg, B., S.H. Ferris, and E. Franssen 1985 An ordinal functional assessment tool for Alzheimer's-type dementia. Hospital Community Psychiatry 36(6):593-595.
Salmon, D.P., P.J. Riekkinen, R. Katzman, M.Y. Zhang, H. Jin, and E. Yu 1989 Cross-cultural studies of dementia: A comparison of Mini-Mental State Examination performance in Finland and China. Archives of Neurology 46(7):769-772.
Stern, Y., H. Andrews, J. Pittman, M. Sano, T. Tatemichi, R. Lantigua, and R. Mayeux 1992 Diagnosis of dementia in a heterogeneous population: Development of a neurophysiological paradigm-based diagnosis of dementia and quantified correction for the effects of education. Archives of Neurology 49:453-460.
Stern, Y., B. Gurland, T.T. Tatemichi, M. Xin Tan, D. Wilder, and R. Mayeux 1994 Influence of education and occupation on the incidence of Alzheimer's disease. Journal of the American Medical Association.
Teresi, J., R. Golden, P. Cross, B. Gurland, M. Kleinman, and D. Wilder 1995 Item bias in cognitive screening measures: Comparisons of elderly white, Afro-American, Hispanic and high and low educational subgroups. Journal of Clinical Epidemiology 48:473-483.
Teresi, J.A., R.R. Golden, B.J. Gurland, D.E. Wilder, and R.G. Bennett 1984 Construct validity of indicator-scales developed from the Comprehensive Assessment and Referral Evaluation interview schedule. Journal of Gerontology 39(2):147-157.
Uhlmann, R.F., and E.B. Larson 1991 Effect of education on the Mini-Mental State Examination as a screening test for dementia. Journal of the American Geriatrics Society 39(9):876-880.
Wands, K., H. Merskey, V.C. Hachinski, M. Fisman, H. Fox, M. Boniferro 1990 A questionnaire investigation of anxiety and depression in early dementia. Journal of the American Geriatrics Society 38:535-538.
Warren, E.J., A. Grek, D. Conn, N. Herrmann, E. Icyk, J. Kohl, and M. Silberfeld 1989 A correlation between cognitive performance and daily functioning in elderly people. Journal of Geriatric Psychiatry and Neurology 2(2):96-100.
Weissmann, N.M., J.K. Myers, G.L. Tischler, C.E. Holzer III, P.J. Leaf, H. Orvaschel, and J.A. Brody 1985 Psychiatric disorders (DSM-III) and cognitive impairment among the elderly in a U.S. urban community. Acta Psychiatrica Scandinavica 71:366-379.
Wilder, D.E., P. Cross, J. Chen, B.J. Gurland, R.A. Lantigua, J. Teresi, M. Bolivar, and P. Encarnación 1995 Operating characteristics of brief screens for dementia in a multicultural population. American Journal of Geriatric Psychiatry 3(2):96-107.
Wilder, D.E., B.J. Gurland, J. Chen, R.A. Lantigua, E.H.P. Killeffer, S. Katz, and P. Encarnación 1994 Interpreting subject and informant reports of function in screening for dementia. International Journal of Geriatric Psychiatry 9:887-896.





































