6
Conclusions and Recommendations
As the analysis and examples in this report have demonstrated, a wide array of factors influences a community's health, and many entities in the community share responsibility for maintaining and improving its health. Responsibility shared among many entities, however, can easily become responsibility ignored or abandoned. The community health improvement process (CHIP) described in this report offers one approach for a community to address this collective responsibility and to marshal resources of specific, accountable entities to improve the health of its members.
Contributing to the interest in health improvement and performance monitoring is a wider recognition that health embraces well-being as well as the absence of illness. For both individuals and populations, health can be seen to depend not only on medical care but also on other factors including individual behavior and genetic makeup and social and economic conditions. The health field model, as described by Evans and Stoddart (1994) and discussed in Chapter 2, presents these multiple determinants of health in a dynamic relationship. It also suggests that a variety of public and private entities in the community, many of whose roles are not within the traditional domain of health activities, have a stake in and an influence on a community's health (Patrick and Wickizer, 1995).
Performance monitoring has gained increasing attention as a
tool for evaluating the delivery of personal health care services and for examining population-based activities addressing the health of the public (see Chapter 4). Although many performance monitoring activities are focused on specific health care organizations, there is a growing appreciation of their importance from a population-based perspective. Only at the population level is it possible to examine the effectiveness of health promotion and disease prevention activities and to determine whether the needs of all segments of the community are being addressed.
A FRAMEWORK FOR COMMUNITY HEALTH IMPROVEMENT
If a community's resources are to be mobilized for a continuing effort to improve its own health, potential participants must know what values they have in common and develop a clear and shared vision of what can be achieved. Based on its review of the determinants of health, of the forces in the community that can influence them, and of community experience with performance monitoring, the committee finds that a community health improvement process that includes performance monitoring, as outlined in this report, can be an effective tool for developing a shared vision and supporting a planned and integrated approach to improve community health. The committee's recommendations for operationalizing a CHIP are based on a variety of theoretical and practical models for community health improvement, continuous quality improvement, quality assurance, and performance monitoring in health care, public health, and other settings. However, the specifies of the committee's proposal have never been tested, in toto, in community settings. Thus, the final section in this chapter identifies a number of ways in which the process that the committee proposes can be evaluated and developed.
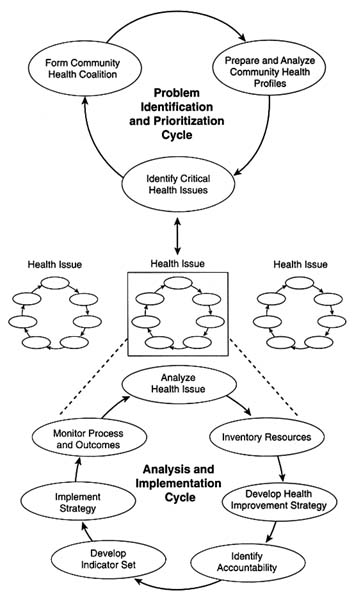
The committee suggests that a CHIP should include two principal interacting cycles based on analysis, action, and measurement. The problem identification and prioritization cycle focuses on identification and prioritization of health problems in the community, and the analysis and implementation cycle on a series of processes intended to devise, implement, and evaluate the impact of health improvement strategies to address the problems (see Figure 6-1).
OPERATIONALIZING THE CHIP CONCEPT
In developing a health improvement program, every commu-
nity will have to consider its own particular circumstances, including factors such as health concerns, resources, social and political perspectives, and other competing concerns. The committee cannot prescribe what actions individual communities should take to address their health concerns or who should be responsible for what, but it does believe that communities need to address these issues and that an organized approach to health improvement that makes use of performance monitoring tools will help them achieve their goals.
Given the different perspectives and activities of personal health service, public health, and other organizations that can contribute to the health of communities and given differing views of the meaning of "health" in the community context, the committee recommends that
-
communities should base a health improvement process on a broad definition of health and a comprehensive conceptual model of how health is produced within the community.
In the committee's view, the field model, as elaborated by Evans and Stoddart (1994), is a good starting point. They have drawn on evidence from social and behavioral as well as health sciences to construct a comprehensive model of the determinants of health, which provides a potential for engendering creative thinking about possible interventions to improve a community's health. The field model perspective makes it clear that most public and private organizational entities in a community, as well as individuals, share an interest in their community's health and are collectively responsible for it. Among these stakeholders in the community's health, those that can influence health outcomes can be thought of as "accountable entities." Although the field model's comprehensive approach to the determinants of health expands the list of stakeholders and the possibilities for interventions, the model's multifactorial nature also clarifies the need for careful analysis to specify (1) what individual entities can contribute and thus be held accountable for contributing, and (2) where collaborative action and shared responsibility are essential.
To operationalize the concept of shared responsibility and individual accountability for community health, stakeholders need to know, jointly and as clearly as possible, how the actions of each potentially accountable entity can contribute to the community's health. Thus, the committee recommends that
-
a CHIP should develop its own set of specific, quantitative performance measures, linking accountable entities to the performance of specific activities expected to lead to the production of desired health outcomes in the community.
Developing community-level performance indicators through the lens of the field model leads to a multidimensional portrayal of the population's health—a highly desirable result, given the committee's working definition of health. To encourage full participation in the health improvement process, the selected performance measures should be balanced across the interests and contributions of the various accountable entities in the community, including those whose primary mission is not health specific. Selecting indicators also requires careful consideration of how to gain insight into progress achieved in the health improvement process. A set of indicators should balance population-based measures of risk factors and health outcomes and health systems-based measures of services performed. A balance is also needed among indicators that focus on short-term gains and those that target more fundamental changes in community health.
Knowing that stakeholder-level performance measures will, in many instances, be unique to a particular community and to the circumstances of stakeholders in that community, the committee devoted its energies to developing community-level performance indicators. Such performance measures would permit communities and their health coalitions to ask, "How are we, as a community, performing in assuring the health of our citizenry?" The prototype indicators also include measures specific to sectors in the community such as managed care organizations, schools, employers, and public health agencies. Depending on their circumstances, individual communities may want to go beyond this to include measures for specific managed care organizations, specific large employers, and so on.
Communities have to establish criteria that can guide the selection of indicators. In the committee's view, such criteria should include consistency with a conceptual framework, such as the field model, for understanding factors that contribute to the production of health, salience to community stakeholders, and support for the social change processes needed to achieve health improvements. Indicators should also be assessed against criteria of validity and reliability, evidence linking performance and health improvement, sensitivity to changes in community health status, and availability of timely data at a reasonable cost. It is also
essential to develop an operational definition for each measure to determine what data are needed and how (or if) they can be obtained. A review of existing indicator sets may suggest measures that could be adapted for community use and may be a source of tested operational definitions.
Many of the important influences on health that the field model helps identify are often not amenable to change in the short run. For example, interventions aimed at critical developmental periods, such as educational programs in early childhood, may have long-term health benefits but produce little measurable effect in the near term. A desire to make observable progress can lead a CHIP to focus on other more immediately measurable problems or on problems that may be high on the political agenda but of uncertain importance to the community's overall health (e.g., a new renal dialysis unit). Participants in a CHIP must also ensure that the process does not become paralyzed by focusing on the undoable. To maintain momentum for coalitions set up to foster community health improvement, it may be reasonable to select some problems that are amenable to change and success in the short term. Thus, the committee recommends that
-
a CHIP should seek a balance between strategic opportunities for long-term health improvement and goals that are achievable in the short term.
One way to achieve this balance is by including interim goals, such as risk reduction strategies, for major health problems. If a community were interested in reducing cancer mortality, for instance, reductions in smoking initiation among teenagers and the implementation of workplace smoking restrictions might be appropriate intermediate goals.
The proposed health improvement process and performance monitoring activities will require that communities have a sustainable organization or system that represents all major stakeholders and accountable entities. Thus, the committee recommends that
-
community coalitions guiding CHIPs should strive for strategic inclusiveness, incorporating individuals, groups, and organizations that have an interest in health outcomes, can take actions necessary to improve community health, or can contribute data and analytic capabilities needed for performance monitoring.
Participants should assume responsibility for contributing to the health of the community, not just furthering the goals of the organizations they represent.
As described in Chapters 3 and 4, a CHIP focuses on horizontal peer relationships in a community rather than vertical hierarchical relationships. Experience suggests that performance monitoring used as a basis for inspection and discipline of those not producing as expected is less effective in achieving improvements than is monitoring used as a tool for learning and process change (Berwick, 1989; Osborne and Gaebler, 1992). Rather, a CHIP should use performance monitoring to encourage productive action and collaboration from many sectors. Because the proposed community health improvement process is new, the groups that carry it out should be "learning organizations" in the sense that the people, agencies, and community involved are organized to learn from their own experience and improve their operations.
All community initiatives require leadership, which may come from the public or the private sector. To institutionalize the health improvement process as a multiparty effort, the committee recommends that
-
a CHIP should be centered in a community health coalition or similar entity.
Some communities will have appropriate coalitions in place, but others will need to expand existing groups or establish a workable forum for collective action for the first time. Strategies for improving the effectiveness of community coalitions for health improvement are discussed in Chapter 3.
ENABLING POLICY AND RESOURCES
Federal, state, and local public health agencies and boards of health are all stakeholders in a community's health and capable of taking action to improve it. Indeed, The Future of Public Health (IOM, 1988) implies that public health agencies have a responsibility to assure that something like a CHIP is in place.
In general, the roles of federal, state, and local public health agencies might be described as follows:
-
At the federal level, the Public Health Service can provide leadership and resources (e.g., research funding, technical assis-
-
tance, data and data collection) that promote the implementation of community-level activities and especially the development of measures and measurement tools.
-
At the state level, health departments should promote community-based activities and, in the committee's view, have a particular responsibility to facilitate community access to data such as that needed for the proposed community health profile. The experience in states such as Illinois, Massachusetts, and Washington (see Appendixes C and D) suggests that leadership from the state health department can promote activities at the local level.
-
At the local level, the health department must be a part of the community coalition that is addressing health issues and must be prepared, as one of the community's accountable entities, to perform functions consistent with the needs of the community; these will vary widely.
In particular, the committee recommends that
-
state and local public health agencies should assure that an effective community health improvement process is in place in all communities. These agencies should at a minimum participate in CHIP activities and, in some communities, should provide its leadership and/or organizational home.
For the CHIP to be effective, communities need certain resources, especially data for community health profiles and performance measures. Since all parties share in the goal of improving community health, it is reasonable that public and private resources be combined to support the data collection and analysis needed for communities to obtain health profile information, to conduct health status assessments and communicate results, and to sustain performance monitoring programs. Such resources could include funding, personnel, data, and data processing and analysis.
Both public and private sectors can contribute critical data for performance monitoring. Public health agencies, as part of the public health assessment function called for in The Future of Public Health , should promote, facilitate—and where necessary and appropriate—perform community health assessments and monitor changes in key performance measures. Much of the necessary
data and expertise exist at the state health department. Thus, the committee recommends that
-
in support of community-level health improvement processes, state health agencies, in cooperation and collaboration with local health departments, should assure the availability of community-level data needed for health profiles.
Currently, most of the data for these profiles are aggregated by standard geopolitical units such as counties, municipalities, and so on. To the extent possible, community health data should be made available in a form that allows communities to prepare health profiles and performance measures according to their own definitions (e.g., geographic, socioeconomic, cultural) of the community. Geocoding of health data gathered for other purposes would be an important step toward improving the data for performance monitoring. For data available only at the community level, state health departments should provide models and technical assistance that communities can use in their own data collection activities.
Because data on and from all accountable entities are essential for effective performance monitoring, states and the federal government (in their policy development and regulatory roles) can assist communities by facilitating access to relevant data held by the private sector. In particular, the committee recommends that
-
states and the federal government, through health departments or other appropriate channels, should require that health plans, indemnity insurers, and other private entities report standard data on the characteristics and health status of their enrolled populations, on services provided, and on outcomes of those services, as necessary for performance monitoring in the community health improvement process.
Providing these data should be seen as part of the responsibility that these private-sector organizations have to the community (IOM, 1996; Showstack et al., 1996). Adequate safeguards for privacy and confidentiality will be necessary for all CHIP data (IOM, 1994).
The relationship between the CHIP and public or private community organizations should be reciprocal. In addition to data that these organizations can provide to a CHIP, the organizations can use other community data that are gathered, and this in turn
should reinforce CHIP goals. For instance, health policymakers at the federal and state levels could consider community-level performance indicators when planning and evaluating publicly funded health services programs such as managed care for Medicaid populations. State agencies designing these programs can specify what performance measures will be used in evaluating the contractors and what data the contractors must report. Similarly, state-level licensure and accreditation of health systems could be tied to performance monitoring systems that stipulate measurable targets for performance and hold systems accountable for achieving targets during the term of licensure. Private health service organizations could use CHIP data in assessing their own contributions to the community's health under ''community benefit" guidelines and regulations or in their own service planning and resource allocation decisions. Community performance measures could also contribute to the management of federal block grants and the proposed federal Performance Partnership Grants (USDHHS, no date).
DEVELOPING THE COMMUNITY HEALTH IMPROVEMENT PROCESS
The community health improvement process and its use of performance monitoring, as laid out in this report, are a work in progress. In preparing this report, the committee reviewed existing efforts at the national, state, and community levels and found much of value. The committee also found, however, that a conceptual framework for using performance monitoring concepts to improve community health as a whole (as opposed to monitoring the performance of specific entities such as managed care organizations or public health agencies) was lacking. The development of such a conceptual framework, and the illustration of its application through sets of prototype indicators, is the major contribution of this report, but this framework remains largely untested. The overall community health improvement process, its performance monitoring component, and the indicator sets should be tested and improved over time. Thus, the committee recommends that
-
the CHIP concept developed in this report should be implemented in a variety of communities across the country, and these efforts should be carefully documented and independently assessed.
The assessment process should strive to include sites that vary both in the nature of the community (size and political jurisdiction, socioeconomic and racial composition, region of the country, specific health issues addressed) and in the structures and processes used for performance monitoring (composition of the group responsible for identifying and monitoring performance measures, leadership role of state and local health departments, and so on). The assessment should also include estimates of the full range of public and private costs of carrying out the CHIP and should explore ways to achieve efficiencies in these efforts. The goals of these "natural experiments" would be to learn how local circumstances, including opportunities and barriers experienced, affect the way the CHIP is adapted by different communities; to identify the "necessary and desirable conditions" for implementation of the CHIP; and to assess whether or not the CHIP indeed results in a refocusing of attention on root causes of health problems and, ultimately, in important improvements in community health.
The current evaluations of community health interventions ought to inform this field through their findings on specific interventions to address health problems, on the community intervention process itself, and on the analytic techniques to apply to community studies. Among the programs being evaluated are interventions to reduce coronary heart disease sponsored by the National Heart Lung and Blood Institute in California (Fortmann et al., 1995), Minnesota (Murray, 1995), and Rhode Island (Elder et al., 1993); the Community Intervention Trial for Smoking Cessation (COMMIT, 1995a,b) sponsored by the National Cancer Institute; and the Kaiser Family Foundation's Community Health Promotion Grant Program (Wagner et al., 1991; Wickizer et al., 1993). The work of the recently established Task Force on Community Preventive Services, organized by the Centers for Disease Control and Prevention, will be compiling evidence on the effectiveness of a variety of community-level activities. The CHIP in its entirety can also be thought of as a "comprehensive community initiative," and many of the ideas regarding the evaluation of such initiatives can be applied (see Connell et al., 1995).
For the proposed community health improvement process to be effective, performance measurement tools for community health must be developed further. Thus, the committee recommends that
-
the Public Health Service, in conjunction with state and
-
local health agencies, national professional organizations, and foundations, should develop standard measures for community health profiles and topic-specific model indicator sets that perform well in individual communities and are suitable for cross-community comparison.
These standard measures would be a resource available to communities, not a set of prescribed measures. The prototype indicator sets described in Appendix A of this report should be viewed as a starting point. Particular attention should be given to issues for which valid measures are not currently available, but the refinement of existing measures should also be addressed. The development of measures of "quality of life" and consumer satisfaction for use in community surveys is particularly important. Research to develop and improve techniques of measurement and analysis (e.g., small area analysis) that can be applied to community-level performance monitoring should also be supported. Noack and McQueen (1988) have observed that the development of health promotion indicators has often been approached as a technical matter, ignoring the need to clarify basic concepts of health and the purpose of such indicators. To further indicator development, they encourage a dialogue between health researchers and policymakers.
More generally, technical expertise based on experience with the CHIP must be developed and shared. Although a wide variety of excellent resources on community health assessment and CQI currently exist, those materials generally do not link assessment and CQI concepts and techniques in the way that is envisioned for a CHIP. Thus, the committee recommends that
-
the Public Health Service, in conjunction with state and local health agencies, national professional organizations, and foundations, should develop workbooks, seminars, and other forms of technical assistance to catalog and convey to communities information on best CHIP practices, specific model performance measures for a variety of health issues and ways to interpret changes in these measures, and available data resources.
Universities can, in a variety of activities and through a variety of disciplines, play an important role in helping communities implement a CHIP and in developing and sharing technical expertise. Schools of public health, which have been urged to turn
their attention to public health practice issues (IOM, 1988; Sorensen and Bialek, 1991), could begin by working with their local communities as part of a CHIP. CDC's university-based health promotion and disease prevention research centers (CDC, 1996) are another vehicle through which universities might contribute.
In the long run, effective dissemination of the CHIP concept will depend on the development of a workforce whose attitudes, values, and skills support its implementation. Thus, the committee recommends that
-
educational programs for professionals in public health, medicine, nursing, health administration, public management, and related fields should include CHIP concepts and practices in their curriculum for preservice and midcareer students.
These programs should introduce the concept of CHIP as a way of thinking about the application of a group of academic disciplines (epidemiology, biostatistics, environmental health, health behavior, and so on) to the practice of community health improvement. Among the other fields in which CHIP might be addressed are maternal and child health, behavioral sciences, and mental health and substance abuse counseling and program administration.
REFERENCES
Berwick, D.M. 1989. Continuous Improvement as an Ideal in Health Care. New England Journal of Medicine 320:53–56.
CDC (Centers for Disease Control and Prevention). 1996. Health Promotion and Disease Prevention Research Center Program: Annual Report 1996. Atlanta, Ga.: CDC, National Center for Chronic Disease Prevention and Health Promotion.
COMMIT (Community Intervention Trial for Smoking Cessation). 1995a. I. Cohort Results from a Four-Year Community Intervention. American Journal of Public Health 85:183–192.
COMMIT. 1995b. II. Changes in Adult Cigarette Smoking Prevalence. American Journal of Public Health 85:193–200.
Connell, J.P. Kubisch, A.C., Schorr, L.B., and Weiss, C.H., eds. 1995. New Approaches to Evaluating Community Initiatives: Concepts, Methods, and Contexts. Washington, D.C.: Aspen Institute.
Elder, J.P., Schmid, T.L., Dower, P., and Hedlund, S. 1993. Community Heart Health Programs: Components, Rationale, and Strategies for Effective Interventions. Journal of Public Health Policy 14:463–479.
Evans, R.G., and Stoddart, G.L. 1994. Producing Health, Consuming Health Care. In Why Are Some People Healthy and Others Not? The Determinants of Health of Populations. R.G. Evans, M.L. Barer, and T.R. Marmor, eds. New York: Aldine De Gruyter.
Fortmann, S.P., Flora, J.A., Winkleby, M.A., Schooler, C., Taylor, C.B., and Farquhar, J.W. 1995. Community Intervention Trials: Reflections on the Stanford Five-City Project Experience. American Journal of Epidemiology 142:576–586.
IOM (Institute of Medicine). 1988. The Future of Public Health. Washington, D.C.: National Academy Press.
IOM. 1994. Health Data in the Information Age: Use, Disclosure, and Privacy. M.S. Donaldson and K.N. Lohr, eds. Washington, D.C.: National Academy Press.
IOM. 1996. Healthy Communities: New Partnerships for the Future of Public Health. M.A. Stoto, C. Abel, and A. Dievler, eds. Washington, D.C.: National Academy Press.
Murray, D. 1995. Design and Analysis of Community Trials: Lessons from the Minnesota Heart Health Program. American Journal of Epidemiology 142:569–575.
Noack, H., and McQueen, D. 1988. Toward Health Promotion Indicators. Health Promotion 3(1):73–78.
Osborne, D., and Gaebler, T. 1992. Reinventing Government: How the Entrepreneurial Spirit is Transforming the Public Sector. Reading, Mass.: Addison-Wesley.
Patrick, D.L., and Wickizer, T.M. Community and Health. 1995. In Society and Health. B.C. Amick, S. Levine, A.R. Tarlov, and D.C. Walsh, eds. New York: Oxford University Press.
Showstack, J., Lurie, N., Leatherman, S., Fisher, E., and Inui, T. 1996. Health of the Public: The Private Sector Challenge. Journal of the American Medical Association 276:1071–1074.
Sorensen, A.A., and Bialek, R.G., eds. 1991. The Public Health Faculty/Agency Forum: Linking Graduate Education and Practice. Final Report. Gainesville: University Press of Florida.
USDHHS (U.S. Department of Health and Human Services). No date. Performance Measurement in Selected Public Health Programs: 1995–1996 Regional Meetings. Washington, D.C.: Office of the Assistant Secretary for Health.
Wagner, E.H., Koepsell, T.D., Anderman, C., et al. 1991. The Evaluation of the Henry J. Kaiser Family Foundation's Community Health Promotion Program: Design. Journal of Clinical Epidemiology 44:685–699.
Wickizer, T.M., Von Korff, M., Cheadle, A., et al. 1993. Activating Communities for Health Promotion: A Process Evaluation Method. American Journal of Public Health 83:561–567.