Executive Summary
On August 2, 1990, Iraq invaded Kuwait and the Persian Gulf War began. The United States deployed almost 700,000 military personnel to the Gulf in Operations Desert Shield and Desert Storm. Following a brief war, most troops returned home and resumed their normal activities. Some, however, began to report various health problems that they believed were related to their deployment in the Persian Gulf. As reports of a purported "Persian Gulf Illness" circulated, public concern grew. In response, the Department of Veterans Affairs (VA) and the Department of Defense (DoD) developed a registry and clinical programs to track the health of Persian Gulf veterans.
The Comprehensive Clinical Evaluation Program (CCEP) was developed by the DoD to provide a systematic clinical evaluation program for the diagnosis and treatment of active-duty military personnel who have medical complaints they believe could be related to their service in the Persian Gulf. Since the program began, about 28,600 active duty Persian Gulf veterans have requested clinical examinations. By December 31, 1996, 24,400 veterans had received completed evaluations; an additional 4,180 are currently involved in some phase of the examination process.
In 1994, the DoD asked the Institute of Medicine to convene a committee to evaluate the adequacy of the CCEP. This committee reached the conclusion that the CCEP is a comprehensive effort to address the clinical needs of the thousands of active-duty personnel who served in the Gulf War. In addition, the committee found that, although the CCEP is not appropriate as a research tool, the results could and should be used to: educate Persian Gulf veterans and the physicians caring for them; improve the medical protocol itself; and evaluate patient outcomes.
The DoD asked the Institute to continue its evaluation of the CCEP with special attention to three issues: (1) approaches to addressing difficult-to-diagnose individuals and those with ill-defined conditions; (2) the diagnosis and treatment of stress and psychiatric conditions; and (3) the assessment of health problems of those who may have been exposed to low levels of nerve agents. This new committee (CCEP 2) was also asked to consider whether there are medical tests or consultations that should be added to the CCEP to increase its diagnostic yield. The following diagram describes the output of the two CCEP committees.
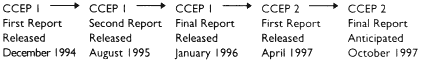
Because of growing concern about the health problems of those veterans who may have been exposed to low levels of nerve agents, the DoD asked the committee to address this issue first. A 1-day workshop was held during which leading researchers and clinicians presented the latest scientific and clinical information regarding possible health effects of low-level exposure to nerve agents and chemically related compounds, as well as the tests available to measure the potential health effects of such exposures. Because there is little available research documenting long-term health effects of low-level exposure to nerve agents, speakers were asked to address the kinds of effects that might exist. These potential effects included neurological problems such as peripheral sensory neuropathies and psychiatric effects such as alterations in mood, cognition, or behavior.
The committee concluded that, overall, the CCEP provides an appropriate screening approach to the diagnosis of a wide spectrum of neurological diseases and conditions. The issue of psychological and psychiatric problems will be addressed in greater detail in the upcoming workshops and the final committee report.
The committee agreed that, given the possibility of low-level exposure to nerve agents, certain refinements in the CCEP would enhance its value. Although these refinements need not be applied retrospectively, the committee hopes implementation will be rapid so that as many new enrollees as possible will benefit from the improved system. Refinements include:
- improved documentation of the screening used during Phase I for patients with psychological conditions such as depression and posttraumatic stress disorder (PTSD);
- improved documentation of neurological screening used during both Phase I and Phase II of the CCEP;
- ensuring that Phase I primary physicians have ready access to a referral neurologist and a referral psychiatrist;
- ensuring that more complete histories are taken, particularly regarding personal and family histories, the onset of health problems, and the occupational and environmental exposures for each patient;
- standardization—to the extent possible—of predeployment physical examinations given members of the armed forces across the services;
- increased uniformity of CCEP forms and reporting procedures across sites;
- for each patient, the physician should provide written evidence that all organ systems were evaluated; and
- DoD should offer group education and counseling to soldiers and their families concerned about exposure to toxic agents.
The committee emphasizes that the CCEP is not an appropriate vehicle for addressing questions about the possible long-term health effects of low-level exposure to nerve agents. Those questions must be addressed through rigorous scientific research. The CCEP is a treatment program. Therefore, it is important not to attempt to use the findings of the CCEP to answer research questions. The committee believes strongly that although data from the CCEP cannot be used to test for potential associations between exposures and health effects, it can, combined with other information, be used to identify promising directions for separate research studies.



