2
Factors That Define the Pipeline
Major social forces and strong political leadership helped bring about the increases in minority enrollment in the health professions that began in 1968. At that time, the climate of the Civil Rights era and good economic times in the United States converged, and the nation seemed poised to commit itself to overcoming the barriers to full participation by minorities in the health professions (Epps et al., 1993).
The promise was not fulfilled, however. Progress in matriculating minorities came virtually to a halt in the mid-1970s, particularly in medicine, which had been at the forefront of efforts to educate minority students (AAMC, 1993a). Even with the recent upswing in applicants and new entrants, the proportion of minorities in all the health professions schools is still lower than the representation of these groups in the population at large.
No one can point to the sole reason for the persistent underrepresentation in minority enrollment and its subsequent impact on the number of minority health professionals in the United States. Some of the stalled progress in the late 1970s and through the 1980s has been attributed to a slower economy, a diminished domestic agenda, declining interest in providing educational opportunities to minorities, and the publication of the 1980 Medical Education National Advisory Committee report, which predicted a significant oversupply of physicians in most specialties by the year 2000. But minority students also report an insidious set of less tangible barriers—both academic and social—that have been strewn along their paths: denial of access to quality education; teachers who expect too little of students; anti-intellectual peer pressure; and a cultural gap between the world in which they study and that of their family and neighborhood (Epps et al., 1993; Ready and Nickens, 1993).
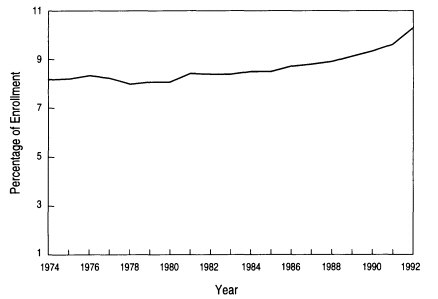
Figure 2-1. Underrepresented minorities as a percentage of total enrollment.
SOURCE: Minority Students in Medical Education: Facts and Figures VII, AAMC, 1993.
This is not to say there have not been successes in the last 25 years. The nation's historically black colleges and universities, which once educated three-quarters of all African-American doctors (Odegaard, 1977), have continued to play an important role in producing minority physicians. A number of other institutions, particularly some medical schools, and organizations such as the National Medical Fellowships, Inc., the National Urban Coalition, the Association of American Medical Colleges (AAMC), the National Medical Association, and a number of private foundations have put significant resources into efforts to increase the number of underrepresented minorities in the health care professions and other science-intensive disciplines.
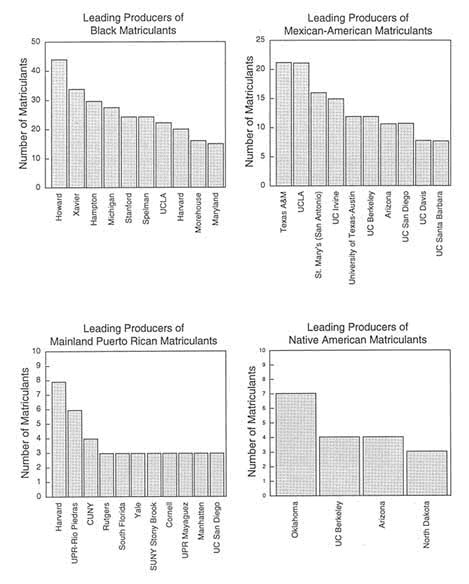
Figure 2-2 presents the colleges that provided the largest numbers of medical school matriculants in 1992. Such efforts alone, however, cannot overcome the disadvantages of an education obtained in the poorly funded and staffed schools that educate many minority students, or the lack of a concerted commitment by a broader spectrum of schools toward a larger minority presence (College Board, 1985; NRC [National Research Council], 1989).
Studies and other data tend to reinforce the notion that most minority students are not educated to the same level as their white counterparts (Action Council on Minority Education, 1990). And there is growing evidence that the failures of the students who slip off the various paths that lead to careers in the health professions must be shared by society and by the institutions responsible for educating young people (NRC, 1989). Among nonminority health professions schools, enrollment and performance statistics suggest that many institutions still have much to do to fully understand and address the problems confronting minority students. For example, minority students continue to be over represented among students repeating their first year of medical school or who do not complete their medical school training (AAMC, 1993a).
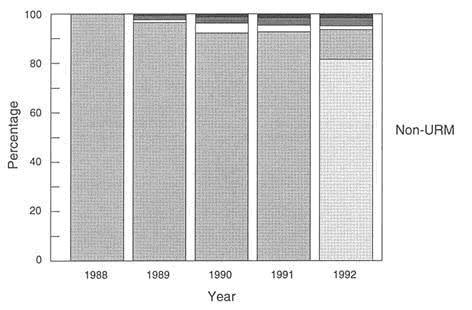
Figure 2-3a. Academic progression of 1988 non-URM matriculants.
SOURCE: Minority Students in Medical Education: Facts and Figures VII, AAMC, 1993.
This chapter focuses on the pipeline beginning with the early school years when students first turn away, or are directed away, from careers in the health professions. It then presents information about the enrollment and fate of minority students entering medical and health professions schools and discusses the factors associated with minority underrepresentation.
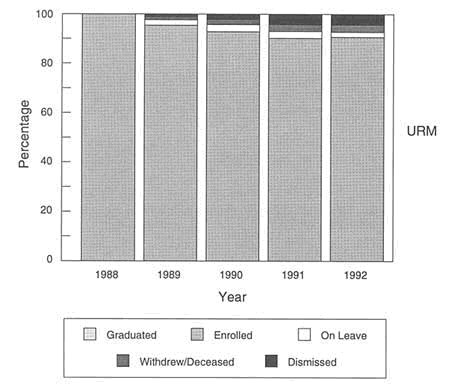
Figure 2-3b Academic progression of 1988 URM matriculants.
SOURCE: Same as Figure 2-3a.
African Americans, Hispanics, and Native Americans comprise about 20 percent of the U.S. population and 19 percent of its workforce, yet underrepresented minorities make up only 5 percent of the science and engineering workforce (U.S. Bureau of the Census, 1990; National Science Foundation [NSF], 1992). They have hardly fared better in the health professions. For example, little more than 8 percent of the nation's physicians and 11 percent of the nation's registered nurses are non-Asian minorities (U.S. Bureau of the Census, 1990).
WHERE THE LEAK BEGINS
The failure to stop the leaks in the pipeline starts early. Children begin their schooling with much curiosity about how the natural world works, but studies have shown that the school environment quickly erodes that interest (Gibbons, 1992a). Minorities start to fall behind in science and math by the fourth grade, and sometimes as early as second grade (Gibbons, 1992a). African-American students start school with test scores that fall within the same range as those of whites their age, but by the sixth grade, African Americans in many school districts are two full grade levels behind whites in achievement (Steele, 1992).
In recent years it has become clear that the quality and quantity of mathematical instruction given to students throughout their academic lives determine how prepared they will be for science-based careers. A study by the College Board, which administers the Scholastic Aptitude Test (SAT), found that high school students who took 1 or more years of algebra in high school were 2 to 3.5 times more likely to go to college than students who did not take algebra. Although white high school graduates are more likely to attend college than are African Americans, African-American students who studied algebra in high school are as likely to attend college as white students (Pelavin and Kane, 1990). According to the National Science Foundation, however, many minority students lack proper guidance and often enroll in algebra in 10th or 11th grade, too late to prepare them for college entrance exams (Selvin, 1992).
Numerous studies and surveys suggest a high degree of interest in science studies among high school students. But that interest does not seem to be exploited in a way that increases the numbers of students who go on to careers in the health professions (Mullis and Jenkins, 1988; NSF, 1992).
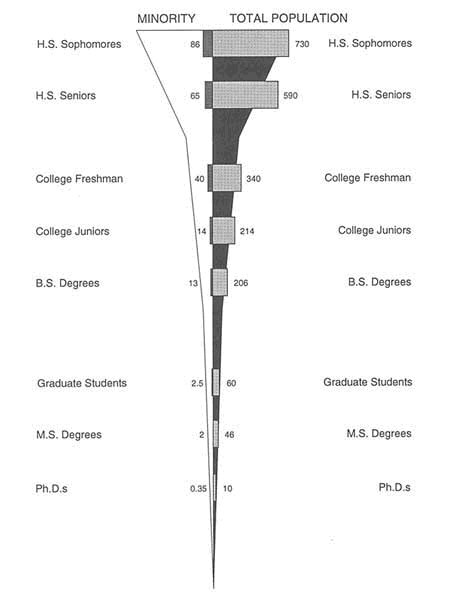
Figure 2-4 shows that an average of 86,000 minority students are interested in pursuing studies in the natural sciences and engineering in their sophomore year of high school. By the senior year of high school, that number has fallen to 65,000. In the freshman year of college, only 40,000 are still studying mathematics and science. This number falls to 14,000 by the junior year. Finally, 13,000 minority students earn B.S. degrees in science or engineering, 2,500 enter graduate studies, and 2,000 earn M.S. degrees (NSF, 1992). Difficult and impersonal introductory science courses are often cited as the specific reason many high school and beginning college students leak out of the medical school pipeline (Petersdorf, 1991).
Even as the number of students attending college increased in the 1980s, African Americans, Hispanics, and Native Americans continued to be underrepresented (NRC, 1989; Carter and Wilson, 1993). According to a recent American Council on Education report, whites are far more likely to participate in higher education than African Americans or Hispanics. In 1991, for example, of white 18- to 24-year-olds, 34.1 percent were in college, compared with 18
percent of Hispanics in that age group and 23.6 percent of all African Americans in that age group (U.S. Department of Education, 1991; Carter and Wilson, 1992). Underrepresented minorities showed a 9.1 percent enrollment gain from 1990 to 1991, most of it at 2-year institutions (U.S. Department of Education, 1991). However, college participation rates, which show how many students in the 18- to 24-year-old range have ''ever enrolled in college," declined for African Americans from 48 percent in 1990 to 46.1 percent in 1991, while the percentage of Hispanics increased 3 percentage points to 47.6 percent (U.S. Department of Education, 1991). Schools in some states recruited greater numbers and percentages of minority students at 2- and 4-year institutions, but in fact, enrollment gains lagged far behind actual population increases for some ethnic minorities (Carter and Wilson, 1993). The American Council on Education report on the status of minorities in higher education cited a study that estimated the disparities would grow in the coming decade (Carter and Wilson, 1993). By 1995, according to projections from 22 states, the number of African-American public high school graduates will drop, creating another potential barrier to progress for this group and its representation in college (Western Interstate Commission for Higher Education and the College Board, 1991).
It is clear that in addition to learning what steps to take to retain students in courses of study that lead to the health professions, educators and policymakers must consider how to increase the number of students who take those courses, as well as the number of teachers who encourage them to do so. Statistics show that students of all races become too discouraged, or fail to receive the encouragement they need, to continue their studies in the sciences and engineering. Only a fraction of interested high school students—1.4 percent—go on to earn Ph.D. degrees. Only 0.4 percent of minority students emerge with Ph.D. degrees in science and engineering (NSF, 1992). It is from this small group that the health professions schools draw, and compete, for their applicants.
Studies indicate that most of the qualified minority students in this country are already applying to medical school. In 1990, there were 2,709 African Americans, 1,637 Hispanics, and 207 Native Americans awarded bachelor's degrees in the life sciences and physical sciences in the United States. Among students applying to medical school that year, 2,349 were African American, 1,338 were Hispanic, and 132 were Native American (Ready and Nickens, 1993). It is clear from these numbers that medical schools are attracting almost all the nation's Hispanic and African-American science graduates. This finding suggests that more intensive recruiting efforts among science graduates would not significantly increase the number of minority applicants, and that there may be a dearth of minority science graduates to enter other science-based careers (Ready and Nickens, 1993; Ready and Nickens, forthcoming).
Medical School
With the exception of the historically black medical schools, most medical schools began recruiting minority students during the late 1960s and early 1970s. Until the mid-1960s, medical schools such as Meharry College School of Medicine and Howard University College of Medicine educated three-quarters of the nation's African-American physicians (Odegaard, 1977).
Many of the early gains in admissions came with the establishment of new medical schools and the expansion of class size in other schools. Student ferment, the rise of Dr. Martin Luther King, Jr., and the riots that followed his assassination also played a powerful role in nudging policymakers and educators toward establishing new reinforcement and enrichment programs together with scholarship money to help minority students obtain medical degrees. Many of these positive endeavors were made possible through federal funding sponsored by the Health Careers Opportunity Program (HCOP) of the Division of Disadvantaged Assistance, Bureau of Health Professions. since 1972, HCOP has been dedicated to increasing the number of minority disadvantaged individuals in health careers. By 1972, according to one survey, most medical schools had initiated programs to increase minority enrollment: two-thirds of the surveyed schools had altered admissions procedures and three-fourths had altered their admissions criteria (Epps et al., 1993). These factors pushed the first-year enrollment of underrepresented minorities from 4 percent in 1970 to 10 percent in 1974 (Petersdorf, 1991).
In the 15 years that followed, however, there was little change in the percentage of minority students enrolled in medical schools (Figure 2-5). Among the reasons was a declining interest in using affirmative action to right past wrongs (Epps et al., 1993; Ready and Nickens, 1993). Speaking in 1991, Robert Petersdorf, president of the Association of American Medical Colleges, observed, "The chances for an underrepresented student to be admitted to medical school have actually become more remote as their proportion of the total U.S. population continues to rise" (Petersdorf, 1991).
In its most recent data release, the AAMC reports that the number of minority medical school matriculants reached 1,827, or 11.2 percent, the highest ever (AAMC, 1993a). This parallels an upsurge in overall applications to medical school. The total enrollment of minorities in medical school was 6,787, or 10.3 percent, also the highest in many years (AAMC, 1993a).
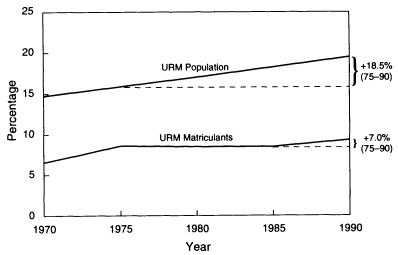
Figure 2-5. Underrepresented minorities as a percentage of the U.S. population and medical school matriculants: 1970-1990. SOURCE: Ready, T.P., and Nickens, H.W. Inventory and Analysis of the Effectiveness of Strategies and Programs for Increasing Minority Participation in Medicine. Paper prepared for the Institute of Medicine's Study to Increase Minority Participation in the Health Professions, 1993.
In its report, the AAMC describes the average 1992 underrepresented minority medical school matriculant as female; from a family in which the parents are either professionals or in sales, with some post-high school education, and earning a combined income of $56,661 (AAMC, 1993a). Women were 57 percent of underrepresented applicants, compared to 42 percent among all applicants. This profile indicates that the pool of applicants may be limited to an elite spectrum of the minority population, particularly in terms of education and income. The AAMC report supports the finding that post-high school education among parents is one of the few consistent predictors of whether a student goes to medical school, providing more reason for raising the educational level of all minority students (Robert Wood Johnson Foundation, 1987; AAMC, 1993a).
The Admissions Process
The use of quantitative measures, such as the Medical College Admissions Test (MCAT) and grade point averages (GPAs), cannot predict or guarantee a student's success in medical school. Although many schools have not studied this matter, most medical school admissions officers have a sense of what combination of MCAT scores and GPAs in college is required to minimize the
risk of academic failure. In a 1987 study, admissions officers were asked what score on the 15-point MCAT they would find acceptable in an applicant to medical school. Eleven was cited as the mean exemplary score; seven was the mean acceptable score. Some admissions officers found four an acceptable score; others would not accept less than ten (Mitchell, 1987).
Medical school admissions committees, under a mandate to increase the percentage of minority students, admit underrepresented minorities with lower MCAT scores and GPAs than their white counterparts. These scores have improved in recent years, particularly among African Americans, but African Americans are still being accepted at much lower rates than whites (Ready and Nickens, 1993). No studies have been done to explain this disparity, or to explain why minority medical students continue to repeat the first year of medical school far more often than do white students. Of the 790 students who repeated their first year of medical school or were taking a decelerated course load in the 1992-1993 school year, for example, 294 were underrepresented minorities (AAMC, 1993a).
In comparison to other medical students, underrepresented minorities are somewhat less likely to complete medical school, although their chances of doing so are improving. Surveys conducted by the AAMC show that by the fourth year of medical school, for the entering class of 1988, the percentage of underrepresented minorities retained was 92.2 percent, compared to 96.4 for all students (AAMC, 1993a).
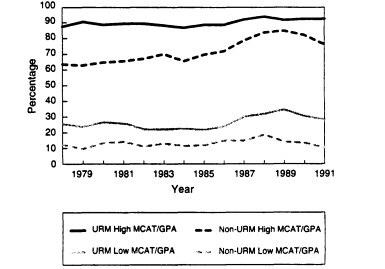
Figure 2-6. Acceptance rates by MCAT and GPA for underrepresented minorities and all other applicants, 1978-1991. SOURCE: Minority Students in Medical Education: Facts and Figures VII, AAMC, 1993.
It has been argued that medical schools could solve the problem of underrepresentation if they accepted all or most of the underrepresented minorities who applied to medical school, and if the institutions took whatever steps necessary to produce board-certified physicians (Ready and Nickens, 1993). To implement such a strategy, medical schools would have to provide expensive programs of academic support and would have to allow students to spend 5 or 6 years in medical school. For a number of reasons, including political considerations, such a strategy is unlikely to be pursued by medical schools (Ready and Nickens, 1993).
Other Health Professions Schools
The best reported data on minorities entering the health professions come from the field of medicine. Comparable data for other specialties are difficult to obtain. Definitive racial and ethnic categories have not been universally established or accepted, and professional associations have adopted and adapted classifications to correspond to their needs and ability to ascertain racial and ethnic identity.
Nevertheless, since 1974, the U.S. Department of Health and Human Services' Bureau of Health Professions has published Minorities and Women in the Health Fields, which provides data on the representation of minorities and women in health occupations and in education programs leading to health careers. Data from the most recent edition, published in 1990, and additional data from the 1991-1992 academic year provided by the Bureau show some modest upward trends in the proportional representation in first-year and total enrollment across the other professions, but these increases remain well below population parity (Tables 2-1 and 2-2).
In 1991-1992, the latest year for which the Bureau of Health Professions has comprehensive data, the racial and ethnic minority representation in first year classes of health professions schools ranges from lows of 5.8 percent for veterinary medicine and 7.1 percent for osteopathic medicine, to highs of 17.8 percent for podiatry, 13.5 percent for all types of registered nursing programs, and 12.5 percent for dentistry (HRSA [Health Resources and Services Administration], personal communication, 1993).
In terms of total enrollment, minorities remain least well represented in veterinary medicine (6.9 percent) and osteopathic medicine (7.8 percent), while best represented in podiatric medicine (17.9 percent), dentistry (13.4 percent), and allopathic medicine (10.3 percent).
Table 2-1. Underrepresented Minorities (African Americans, Hispanics, Native Americans): Representation in U.S. Population and in 1st year classes (selected health professions), 1971-1992.
|
|
'70-'71 |
'71-'72 |
'72-'73 |
'73-'74 |
'74-'75 |
'75-'76 |
'76-'77 |
'77-'78 |
'78-'79 |
'79-'80 |
|
% of Total U.S. Population |
15.8 |
16.0 |
16.3 |
16.6 |
16.8 |
17.1 |
17.4 |
17.7 |
18.0 |
18.3 |
|
Allopathic Medicine |
7.1 |
8.6 |
8.7 |
9.1 |
10.0 |
9.1 |
9.0 |
9.0 |
8.7 |
9.1 |
|
Osteopathy |
— |
2.4 |
2.8 |
1.8 |
3.4 |
3.9 |
4.0 |
4.0 |
4.4 |
4.5 |
|
Dentistry |
— |
6.1 |
6.2 |
6.6 |
6.6 |
6.9 |
6.9 |
7.1 |
6.7 |
7.5 |
|
Optometrya |
— |
2.1 |
2.5 |
3.1 |
3.4 |
3.7 |
3.5 |
3.3 |
3.1 |
3.0 |
|
Pharmacy |
— |
— |
— |
4.9 |
5.2 |
7.0 |
6.3 |
6.4 |
6.4 |
7.2 |
|
Podiatric Medicine |
— |
3.3 |
— |
2.5 |
— |
— |
5.5 |
— |
— |
7.1 |
|
Veterinary Medicineb |
— |
2.6 |
2.6 |
3.0 |
2.9 |
3.3 |
3.8. |
3.8 |
4.1 |
4.0 |
|
Nursingc |
||||||||||
|
R.N. Program |
— |
10.8 |
— |
— |
12.6 |
— |
— |
11.2 |
— |
— |
|
L.P.N. Program |
— |
19.4 |
— |
— |
17.9 |
— |
— |
15.6 |
— |
— |
|
a Based upon total enrollment data for underrepresented minorities. b Based upon total enrollment data for all minorities prior to academic year 1982-1983. c Based upon first year enrollment data for all minorities. SOURCE: Minorities and Women in the Health Fields, 1990 Edition; DHHS/PHS/HRSA personal communication, October 6, 1993. |
||||||||||
|
|
'80-'81 |
'81-'82 |
'82-'83 |
'83-'84 |
'84-'85 |
'85-'86 |
'86-'87 |
'87-'88 |
'88-'89 |
'91-'92 |
|
% of Total U.S. Population |
18.6 |
18.9 |
19.2 |
19.5 |
19.9 |
20.2 |
20.5 |
20.9 |
21.2 |
22.2 |
|
Allopathic Medicine |
9.0 |
9.7 |
9.4 |
9.7 |
9.8 |
10.6 |
10.0 |
11.1 |
11.8 |
11.0 |
|
Osteopathy |
4.4 |
4.5 |
4.8 |
5.7 |
6.5 |
5.2 |
6.5 |
6.2 |
— |
7.1 |
|
Dentistry |
7.6 |
8.7 |
8.9 |
9.0 |
10.4 |
11.4 |
13.6 |
15.2 |
15.1 |
12.5 |
|
Optometrya |
3.3 |
3.6 |
4.4 |
5.0 |
5.2 |
5.8 |
— |
6.2 |
— |
9.4 |
|
Pharmacy |
8.0 |
8.3 |
9.1 |
9.3 |
9.4 |
9.6 |
— |
9.9 |
— |
12.2 |
|
Podiatric Medicine |
8.1 |
9.1 |
9.7 |
11.0 |
12.9 |
14.7 |
13.4 |
15.8 |
17.1 |
17.8 |
|
Veterinary Medicineb |
4.6 |
4.8 |
4.7 |
4.7 |
4.5 |
5.4 |
5.6 |
5.4 |
6.3 |
5.8 |
|
Nursingc |
||||||||||
|
R.N. Program |
13.5 |
— |
— |
12.9 |
12.7 |
14.6 |
— |
— |
— |
13.5 |
|
L.P.N. Program |
17.5 |
— |
— |
17.7 |
22.2 |
— |
— |
— |
— |
— |
|
a Based upon total enrollment data for underrepresented minorities. b Based upon total enrollment data for all minorities prior to academic year 1982-1983. c Based upon first year enrollment data for all minorities. SOURCE: Minorities and Women in the Health Fields, 1990 Edition; DHHS/PHS/HRSA personal communication, October 6, 1993. |
||||||||||
Table 2-2. Minority Total Enrollments in Selected Health Professions Schools: Academic Year 1991-1992
|
|
|
Number of Students |
||||
|
Selected Health Professions School |
TOTAL |
Under-represented Minorities |
African American |
Hispanic |
Native American |
Asian |
|
Allopathic Medicinea |
66,142 |
6,787 |
4,638 |
1,665 |
333 |
9,994 |
|
Osteopathic Medicine |
7,012 |
549 |
236 |
276 |
37 |
685 |
|
Dentistrya |
15,980 |
2,143 |
943 |
1,152 |
48 |
2,650 |
|
Pharmacy |
23,482 |
2,485 |
1,531 |
867 |
87 |
2,755 |
|
Podiatric Medicine |
2,247 |
402 |
233 |
161 |
8 |
201 |
|
Optometry |
4,864 |
458 |
141 |
295 |
22 |
652 |
|
Nursing (RN) |
237,598 |
30,578 |
21,529 |
7,349 |
1,700 |
6,947 |
|
Veterinary Medicine |
8,440 |
495 |
192 |
257 |
46 |
141 |
|
Allied Healthb |
92,520 |
16,349 |
10,251 |
5,590 |
508 |
3,453 |
|
|
Percent Distribution |
|
||||
|
Allopathic Medicinea |
100.0 |
10.3 |
7.0 |
5.8 |
0.5 |
15.1 |
|
Osteopathic Medicine |
100.0 |
7.8 |
3.4 |
3.9 |
0.5 |
9.8 |
|
Dentistrya |
100.0 |
13.4 |
5.9 |
7.2 |
0.3 |
16.6 |
|
Pharmacy |
100.0 |
10.6 |
6.5 |
3.7 |
0.4 |
11.7 |
|
Podiatric Medicine |
100.0 |
17.9 |
10.4 |
7.2 |
0.4 |
8.9 |
|
Optometry |
100.0 |
9.4 |
2.9 |
6.1 |
0.5 |
13.4 |
|
Nursing (RN) |
100.0 |
12.9 |
9.1 |
3.1 |
0.7 |
2.9 |
|
Veterinary Medicine |
100.0 |
5.9 |
2.3 |
3.0 |
0.5 |
1.7 |
|
Allied Healthb |
100.0 |
17.7 |
11.1 |
6.0 |
0.5 |
3.7 |
|
a Data are for 1992-1993. b Data are for 1990-1991 as reported by 2,882 CAHEA Accredited Programs. These data include 26 allied health occupations. SOURCE: Bureau of the Health Professions, DHHS, 1993; AAMC, 1993. |
||||||
The Bureau of Health Professions data gives some further analysis on the type of progress being made from the early 1970s through the mid/late 1980s, the last years for which comprehensive analysis was made available (HRSA, 1990). For example:
-
While overall first-year enrollment in schools of osteopathic medicine almost tripled between 1971-1972 and 1987-1988, minority first-year enrollment increased tenfold during that time, from 2.4 percent to 6.2 percent of total first-year enrollment. Although all underrepresented groups remain well below parity, Hispanics have the largest proportional presence. However, the racial and ethnic enrollments in individual schools vary widely.
-
In dentistry, as in medicine, the representation of minority women has been increasing at a faster rate than minority men. On a population parity basis, Hispanics and Native Americans are better represented than African Americans.
Even in dental schools where enrollment rates have increased among all minority groups, whites still have the highest enrollment rate and African Americans the lowest. African Americans have attrition rates 2.5 times higher than whites and Hispanics (American Dental Association, 1992). Nearly, three-quarters of African-American first-year students who withdraw say they do so for academic reasons; 57 percent of Hispanics and 47 percent of whites who withdraw also cite academic reasons (American Dental Association, 1992).
Dentistry consistently has one of the highest proportions of underrepresented minorities among all health professions. Given this fact, further study of ways to enhance dental programs may prove helpful not only to dentistry, but to the other health professions' efforts. The Institute of Medicine is currently undertaking an intensive study on dental education and oral health. Upon its release in 1994, the study will give recommendations as to how dental education might better respond to current problems and future challenges, including issues of racial and ethnic representation.
-
The presence of underrepresented minorities in veterinary schools increased significantly between the years 1978-1979 and 1988-1989. While the overall increase in student enrollment was 5.2 percent, the minority matriculation rate increased by 77 percent. Tuskegee, a historically black institution, graduated 38 percent of all minority veterinary graduates in 1985-1986; only two schools, excluding Tuskegee, had more than 6 percent minority graduates.
-
In optometry, minority students are further from reaching parity than in medicine or dentistry. Native Americans are well represented in optometry, but their total numbers are small.
-
All minorities have made significant enrollment gains in schools of pharmacy. Minority enrollment has continued to rise steadily. As a percentage of the total, minority students have increased from 5.1 percent to 13.3 percent.
-
First-year enrollments in schools of podiatry increased by more than 100
-
percent between 1971-1972 and 1986-1987. The overall percentage of minority first-year enrollment increased from 3.3 percent in 1971-1972 to 17.9 percent in 1991-1992. African-American and Hispanic enrollment increased at mainly steady rates; Native American representation was more erratic and small. In 1988-1989, African-American representation was closest to parity. Hispanics are not as well represented in podiatry as in other health professions.
-
Total enrollment in education programs for registered nurses declined by 15.6 percent between academic years 1971-1972 and 1987-1988. During this same period, minority enrollment decreased 7.6 percent, but the proportion of minorities enrolled increased to 15.8 percent from 10.4 percent according to schools reporting the racial and ethnic composition of their students. Total enrollment for practical nurse programs, after a drop in the mid- 1970s, remained consistently around the 21 percent level during this time. All minority groups remain significantly underrepresented in registered nurse programs. Among health careers, practical nurse programs continue to have the highest minority representation (HRSA, 1990).
As enrollment in nursing schools has declined along with financial resources, there have been increased efforts to recruit and retain students once deemed academically ''high risk" into baccalaureate programs (Epps et al., 1993). But statistics compiled by the National League of Nursing illustrate the importance of developing adequate prematriculation and retention programs. By 1984, according to the League, 13 percent of those accepted into college nursing programs in the South were African American, but African Americans made up only 8 percent of the graduates of those programs (Epps et al., 1993).
Published programs in nursing schools, primarily those implemented and evaluated in the 1970s, are few and statistical evaluations are almost nonexistent; data consist usually of a qualitative review of questionnaire responses. A number of these evaluations, while limited, show some improvement in student retention and graduation rates as a result of various support programs. The presence or absence of a real faculty commitment toward enhancing minority participation has been shown to be closely related with achieving more positive results (Epps et al., 1993).
Some nursing schools have now begun more innovative and concerted programs to increase minority participation and retention in the health professions. Early evaluations of this strategy in nursing have been favorable, but there are as yet few published studies of their impact (Epps et al., 1993). Recently, there has been more of an effort on the part of nursing programs to bring so-called high-risk students along. These endeavors should be more closely examined.
Allied Health
The ethnic mix of students enrolled in schools of allied health generally reflects the ethnic mix of the U.S. population. In 1991-1992, African Americans represented 11 percent of total enrollments; Hispanics, 6 percent; and Native Americans, 0.5 percent. Among allied health personnel, which make up between I million and 4 million people (depending on how the field is defined), there are both highly educated people and people who have been trained on the job (for example, occupational therapists and home health aides) (IOM [Institute of Medicine], 1989). It is important to note that minorities are underrepresented in allied health fields that require more education (IOM, 1989).
Like other health professions schools, allied health schools have received federal funds under the Health Careers Opportunity Program, and these schools have often succeeded in recruiting enough minorities to double their minority enrollment (Epps et al., 1993). Belatedly, the schools have discovered that many of the new students are ill-prepared because of inadequate high school and college training in biology, chemistry, and physics (Epps et al., 1993). One survey, in 1992, found that more than one-half of the Hispanic and one-third of the African-American students were high risk because they had C or D grade point averages in the college courses they took before beginning their allied health studies (Epps et al., 1993).
Few data are available on programs to increase minority enrollment because school administrators have only recently begun collecting data for programs that were begun in the 1980s. There have been, however, recent increases in the number of minority students at schools receiving HCOP funds to both recruit and retain minorities in the schools of allied health (Epps et al., 1993).
FACTORS ASSOCIATED WITH MINORITY UNDERREPRESENTATION
A number of factors have been associated with minority underrepresentation in the health professions, particularly medicine. They include racism, lack of sustained funding for programs, lack of institutional commitment, and the effects of a significant legal ruling. These factors are examined in this section.
Overt Racism or Lack of Concern?
In surveys, students have said they faced little overt racism, but others found racism in medical school and said it had an influence on their careers (Reitzes and Elkhanialy, 1976; Wolkon and Yamamoto, 1978; Fullilove et al.,
1988). Why would these feelings persist even in schools working hard to admit and retain minority students? Jennings, in an article in the Trotter Institute Review, argues that the academic environment is no less hostile today to African-American students than it was in 1926, when W.E.B. Dubois described the attitude of the "northern institution toward the negro student [as] one which varies from tolerance to active hostility" (Jennings, 1989). The nation's educational leaders pay "lip service" to the idea of opening institutions of higher education to more minorities and deplore racial violence and harassment. But they may tolerate racism and racial insensitivity at their own institutions (Jennings, 1989). Others concede that a less-than-hospitable climate for minorities on many college campuses has played a role in diverting minority students from careers in the health professions (Petersdorf, 1991; Richardson and Skinner, 1991). Petersdorf points to "poor academic preparation prior to college" as the primary reason minority students drop out of the medical school pipeline (Petersdorf, 1991).
A study at the University of Rochester offers clues to why some academics view overt racism as "much less common" (Petersdorf, 1991), while others call such a perspective an example of a phenomenon noted by Martin Luther King, Jr.—"America fantasizes racial harmony" (King, 1967; Jennings, 1989).
The University of Rochester study of a year-long tutorial examined the interactions between minority medical students, staff, and faculty (Fullilove et al., 1988). Tutoring began only after students had failed their first year, months after they had begun to have academic problems. By the time the target students joined in a group tutorial specifically created for minority students, they distrusted the school (Geertsma, 1977).
Students in the program who had been told that their academic work was not up to par believed they were the objects of racially motivated put-downs. As a result, they did not respond to helpful suggestions for improving their academic performance. In their account of the study, Fullilove et al. suggested that faculty members had indirectly implied that the students lacked the intellectual resources to learn. The authors warned that this message is passed on to minority students from nursery school to graduate school (Fullilove et al., 1988). At all levels, most programs for minority students are remedial. Instead of learning to define and overcome what is holding them back in their studies, students often learn they are inferior and cannot succeed (Fullilove et al., 1988).
Problems in Funding
Against the backdrop of rising tuition, an unhealthy economy, and the declining public interest in providing minorities with equal rights to an education, students have had to rely on loans rather than scholarships to fund their education (Ready and Nickens, 1993). Several studies indicate that rising
tuition and the decline in scholarship money have been decisive factors in the decreasing minority enrollment in higher education, including the health professions schools (Jennings, 1989; NRC, 1989; Petersdorf, 1991). According to data collected by the National Medical Fellowships, Inc., the annual cost of a medical education in academic years 1981-1982 and 1987-1988 rose 80.3 percent at public schools and 55.5 percent at private schools (Johnson, 1990). Despite the daunting costs, however, many minority students are willing to shoulder the debt necessary to obtain an education in the health professions. However, medical students in particular too often make uninformed decisions about the medical schools they choose to attend and the manner in which they will pay for medical education (Johnson, 1990).
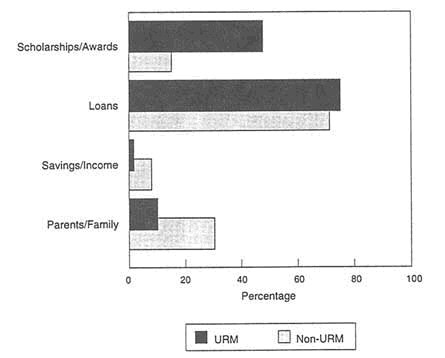
Figure 2-7. How matriculants will finance at least 25 percent of their medical school costs.
SOURCE: Minority Students in Medical Education: Facts and Figures VII, AAMC, 1993.
As tuitions have risen, private philanthropy has cut back on its support for preparing minority students for careers in the health professions. During the 1970s and 1980s, the private foundations that funded efforts to enhance minority participation focused primarily on increasing the applicant pool (Epps et al.,
1993). Those programs had little impact, however, on the shortage of minorities in the health professions, and the foundations looked elsewhere for proved interventions, committed institutions, and careful selection of students (Robert Wood Johnson Foundation, 1987). Meanwhile, the federal government has shifted its financial aid resources into providing high-interest loans and programs that subsidize tuition costs in return for promises of public service after graduation, such as the National Health Service Corps (Epps et al., 1993; Ready and Nickens, 1993). It has been argued that in cutting back on its financial aid programs for students in higher education, the federal government has undermined racial diversity and access (Jennings, 1989).
In 1992, the average debt of minority students in medical school was $58,737, compared to $55,497 for other medical students (AAMC, 1993a). While this difference may not seem great, the size of the debt is much more likely to discourage a minority student whose family has little experience with earning enough to repay such large sums of money (Johnson, 1990; Cregler et al., 1993). Furthermore, current data show that 40 percent of underrepresented minority students have to rely on high-cost, unsubsidized loans, compared with 35 percent of all students (AAMC, 1993a).
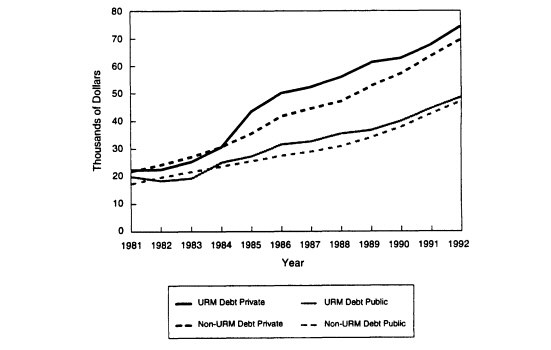
Figure 2-8. Average debt for indebted medical school graduates, 1981-1992.
SOURCE: Minority Students in Medical Education: Facts and Figures VII, AAMC, 1993.
Lack of Institutional Commitment
There have been other reasons why well-intentioned efforts have failed to increase the number of underrepresented minorities in the sciences. Some key reasons most often cited by educators, government officials, researchers, and others are presented below (Sims, 1992).
-
Lack of real commitment from the top or from most faculty.
Institutions often fail to integrate into their missions the goals of their minority programs. The programs are also often run by faculty members who have no real leadership role at their institutions and, thus, lack credibility and adequate resources to address the problems faced by minority students (Sims, 1992; Cregler et al., 1993; Ready and Nickens, 1993). There may indeed be a correlation between the way a medical school staffs its minority affairs office and how successful the school is at attracting minority students (Ready and Nickens, 1993). For example, medical schools that have no minority staff working on minority affairs issues tend to have low minority enrollment (Ready and Nickens, 1993). Furthermore, medical schools often show a lack of commitment to increasing minority enrollment by failing to include on admissions committees women and underrepresented minorities who might be sensitive to cultural differences (Edwards et al., 1990; Cregler et al., 1993).
Table 2-3. Staff Time Devoted to Minority Programs as Related to Underrepresented Minority Enrollment, 1991
|
FTE |
Number of Schools |
Average URM Matriculants (%) |
Matriculant Representation Factor |
|
<1 |
37 |
5.8 |
.36 |
|
1-1.9 |
25 |
8.7 |
.41 |
|
2-2.9 |
25 |
8.6 |
.58 |
|
≥3 |
25 |
11.3 |
.80 |
|
SOURCE: Ready, T.P., and Nickens, H.W. Inventory and Analysis of the Effectiveness of Strategies and Programs for Increasing Minority Participation in the Health Professions, 1993. |
|||
Despite improvements in the academic credentials of African-American applicants to medical school, African Americans have had substantially lower acceptance rates in recent years (Ready and Nickens, 1993). All three of the background papers prepared for the IOM committee called for further study of the falling matriculation rate for minorities, even when the recent upward trend in medical school enrollment for 1992 and 1993 is considered (Cregler et al.,
1993; Epps et al., 1993; Ready and Nickens, 1993). The major barrier for underrepresented minorities is getting accepted to medical school, and the greatest barrier to acceptance is the lack of academic preparation.
-
Colleges recruit unprepared minority students and then leave them to sink or swim.
In the early 1970s, as the result of a second-rate education (particularly in math and sciences), underrepresented minorities on average had weaker academic credentials than other students accepted to college and health professions schools as they began their studies in what had been nearly all-white institutions (Johnson et al., 1975). This factor, combined with the psychological barriers noted below, contributed to the relatively high attrition rates among minority students (Ready and Nickens, 1993).
Health professions schools and other institutions all along the pipeline have struggled with helping students make up for gaps in their preparation, with varying degrees of success. Some schools, as discussed above, have tried remedial programs that may carry with them a stigma and a message that the student is destined to fail (Fullilove et al., 1988). Even today, students with little mathematics or science background are aggressively recruited to study science or engineering in college, then left to make their own way (Sims, 1992).
-
Programs ignore subtle psychological issues, such as low expectations on the part of teachers and counselors.
High school and college teachers and guidance counselors often discourage their minority students from taking challenging courses in mathematics and science. There is a general assumption that minorities are not smart enough to handle the work (Sims, 1992).
Once minority students have succeeded in gaining admission to a health professions school, they must still handle cultural differences and biases and learn how to accommodate their cultures with the prevailing one at the majority institution. In many cases, when minority students experience difficulty during medical school, it is due to nonacademic reasons (Shea and Fullilove, 1985; Sedlacek, 1987).
Medical schools also have been slow to provide students with the mentors who can help guide career choices and help make the academic environment a more hospitable one. The failure of medical schools to increase the number of underrepresented minorities among their faculty has deprived minority students of role models and created another barrier to increasing the number of minority physicians (Cregler et al., 1993; Wilson and Kaczmarek, 1993). In 1992, minority faculty made up 3.5 percent of the 70,187 medical school faculty in the United States, compared to the 2.6 percent in 1982 (Jolley and Hudley, 1993). However, more than one-third of these faculty members either are teaching at minority medical schools or are on staff at minority medical centers (Wilson and Kaczmarek, 1993). Consequently, in 1992, underrepresented minorities
comprised only 2.6 percent of full-time faculty at nonminority institutions (AAMC, 1993a).
-
Programs target college-age or older students Instead of also going to the root of the problem in elementary and high schools.
As far back as 1978, an AAMC task force recommended that medical schools establish "meaningful relationships with the colleges and senior high schools in their region to encourage, motivate and prepare students from racial minority groups for careers in medicine" (AAMC, 1978). Despite these recommendations, medical schools have made little effort to change their strategies for increasing minority enrollment (Ready and Nickens, forthcoming).
The schools had perhaps hoped that the pool of applicants would grow if minority college graduates could be encouraged to pursue careers in medicine. However, rapid growth in minority enrollment in bachelor's degree programs ended in the mid-1970s, and so did the expansion in the number of minorities in medical schools (Ready and Nickens, forthcoming).
-
Programs had vague or unrealistic goals.
Even when they were implemented, programs to increase minority enrollment in the sciences at the undergraduate and graduate levels suffered from unrealistic expectations and lack of accountability (Sims, 1992). The programs expected too much from too many students in too short a period of time. Also, many of the programs failed to understand the complexity of the situation. Students from disadvantaged backgrounds had a lot of catching up to do, and the academic challenges they faced were complicated by the economic and environmental circumstances in which they found themselves. Had these programs been carefully evaluated, later initiatives could have anticipated and overcome previous failings more readily.
In the early days of federal funding under HCOP, evidence of success appeared because the numbers of minority students were increasing in the health professions schools funded under the program. But during the 1980s, program reports began to suggest that students were shown to have attained the objectives of the funded programs (Epps et al., 1993). More recently, attrition rates and the failure of programs to actually increase the number of minority health professionals have led private foundations into "making sure the program sponsor is truly committed to the recruitment and retention of minority students" (Robert Wood Johnson Foundation, 1987).
Regents of California v. Bakke
In the early 1970s, 16 percent of medical schools maintained separate admissions committees, and many also set aside a specified number of seats for minority applicants. In 1974, these practices at the University of California at
Davis were challenged in the state courts by an unsuccessful white applicant to that school. Four years later, the U.S. Supreme Court said such practices were unconstitutional. Race, the court said, could be considered as only one factor in admissions decisions. This decision, taken against the backdrop of declining societal interest and commitment to opening up opportunities for minorities, is thought to have contributed to the stagnation in minority enrollment in health professions schools (Cregler et al., 1993).
Individual and Community Responsibilities
Minority families, communities, and institutions must share the responsibility for changing the system, working with nonminority policymakers and educators (Action Council on Minority Education, 1990). All students have a major responsibility for their education and the level of effort put forth to learn even in the poorest of circumstances. Minority students, in particular, must set their sights high. In so doing they will need the support of family and community. Such support may not always be possible because of the family's own limited educational opportunities or other societal deprivations. Especially in such cases, support must be available from an extended family in the form of a teacher, or mentor, or the larger community (Epps et al., 1993).
CONCLUSION
The current stagnation in minority enrollment in the health professions exists despite a significant commitment to minority recruitment on the part of many institutions and individuals. In some cases, their efforts have been successful, showing that the problem is not insurmountable. There are still some schools, however, whose failure to increase the number of minority graduates shows a lack of commitment. It is to those institutions that Chapter 3 is addressed. In Petersdorf's words, "It is fair to say that the schools that have been successful in producing a relatively large number of underrepresented minority graduates have benefitted from strong commitment to minority recruitment by their leadership" (Petersdorf, 1991).