6
The Mission of Patient Care
This chapter focuses on dental schools' health-related service to individuals and communities. It calls for dental educators to affirm or reaffirm that patient care is a distinct mission that is related but not subservient to the missions of education and research. It argues further for major shifts in schools' patient care objectives and activities, shifts that cannot occur without the support of community dentists and dental organizations. The committee believes that such support will be forthcoming because educators and practitioners ultimately will agree that the best education occurs in a setting of exemplary patient care.
The committee found little in the dental education literature that examined patient care in the dental school from a patient's perspective. Even the discussions of comprehensive care cited in Chapter 4 focus primarily on how to educate students to be patient oriented. This chapter, thus, draws heavily on the committee's site visits and other activities, its broad understanding of the forces reshaping health care delivery and financing, and its judgments about the fit between patient care in the dental school and a restructured health care system.
Context
An examination of patient care activities in the dental school and academic health center must consider the patient as an indi-
vidual, as a member of a health insurance plan, and as a part of a community. This triple focus complicates the already intricate balancing act that characterizes patient care in the health professions schools. Not only do schools have to consider differences in individual patients' characteristics and manage possible conflicts between individual and community needs, they must also take into account differences in the objectives and policies of the health plans that increasingly manage or arrange for services for employer, governmental, or other sponsors. Sometimes the interests of these health plans closely parallel those of their individual members, but they may at other times conflict (e.g., when plans restrict member's choice of provider or impose bureaucratic hurdles before care can be provided). When they do, the health care provider can be caught in the middle. As discussed in this chapter, the provider's position is even more difficult if it is also an academic institution with educational and research missions.
Further confounding the patient care responsibilities of the dental school are the varied views of these responsibilities by different individuals and groups. To indigent patients, the student dental clinic may be the only source of care. Similarly, to politicians in a state with public or private state-related dental schools, the clinic may be a vehicle for meeting the needs of the underserved. The community dentist may view a faculty practice plan as a good place to refer complicated patients such as those with AIDS, infectious tuberculosis, or severe behavioral problems. The community dentist might also view the plan and the student clinic as competitors. To the administration of a university or academic health center, the outpatient clinics of a dental school may be a mystery—different from any component of the medical school and in chronic need of subsidy. These varied perspectives challenge dental schools to clearly articulate the value and requirements of their patient care mission.
Such an articulation of the contribution of dental schools to the parent institutions and communities is also important because, even if substantially restructured, patient care in dental schools will include some inefficiencies associated with the educational process. Student clinics are unlikely to be able to cover their full costs through patient fees. Moreover, many educators expect that dental schools' economic advantage—low cost or "free" care for patients without access to the private practice system— will diminish as dental insurers organize network health plans and demand price and other changes from community practitioners. Thus, dental educators with the help of others in the dental community must make the case for public support of the educa-
tional and community service aspects of patient care in the dental school. Support from national and local philanthropies and other private sources will also be necessary to help fund the demonstration projects and experiments that will assist schools in making the transition to new models of patient care and community service.
Who Provides Patient Care in Dental Schools?
In most dental schools, the majority of patient care activities are provided by students. Many schools delegate to predoctoral students responsibility for both managing and providing a patient's care; faculty assume responsibility for supervising a single visit or procedure at a time. Faculty may provide services incidentally as they oversee student care, and allied health personnel may provide care either as students themselves or as employees. In a few schools, the patient is the responsibility of a designated faculty member (usually a general dentist), although most of the care is still provided by the student. If a specialist faculty member is called in for consultation or procedural direction, the student and generalist faculty member retain responsibility for the patient.
Depending on the array of advanced education programs within a school, advanced education students also provide and oversee patient care in both predoctoral and graduate clinics. One dean has noted that although advanced education students accounted for only 10 percent of his school's enrollment, they generated 45 percent of clinic revenues both because they are more productive and because higher fees can be charged for their services (Hunt, 1993). Schools may let patients choose whether to receive care from a predoctoral student, postdoctoral student, or faculty member.
In the majority of schools, faculty also care for patients in separately housed and staffed faculty practice plans. As discussed further in Chapter 7, a major rationale for faculty practice plans is to supplement faculty salaries. Another rationale, described in Chapter 4, is that they help keep faculty clinically up to date and sensitive to the realities of practice. Involvement in these plans by predoctoral students appears to be limited.
Where Is Care Provided?
The location of patient care activities varies from school to school. All schools operate a dental school clinic on site, and the majority have separate facilities for faculty practice plans. Many
schools, but not all, provide care in off-site or extramural facilities, including community clinics, public schools, traveling clinic-vans, and temporary clinics for special populations such as migrant workers. Extramural facilities often provide sites for advanced general dentistry, dental public health, and other residencies. Because relatively few health maintenance organizations (HMOs) or other managed care organizations have significant dental care components, they rarely serve as extramural educational sites.
Student participation in on-site clinics is mandatory and fulfills graduation requirements as measured in procedures, hours, patients treated, or some combination of these. Some schools require student participation in extramural clinical activities and include them as rotations in the third and fourth years. Other schools provide only optional off-site activities because they lack convenient sites or the staff and faculty needed to manage the number of extramural clinics that the entire student population would require.
During its site visits, the committee learned that several schools have cut back or eliminated off-site community service activities due to financial pressures and cuts in state funding. Some schools have attempted to quantify the value of their extramural programs as a way to demonstrate their commitment to the community and underscore the value of state funding.
How Is Care Organized?
The site of care strongly shapes the organization of care. When dental students provide care in extramural facilities in which education is a distinctly secondary goal, their activities and supervision generally conform to the individual facility's scheme for patient care. That scheme will vary considerably from hospital to community clinic to private office.
Within the dental school, care provided by students may be organized around specialty clinics or comprehensive care clinics. Chapter 4 describes these alternatives primarily from an educational perspective but notes that a patient-oriented objective of comprehensive care is to put the patient-general practitioner relationship at the center of the clinic and to provide care in a setting as similar as possible to an efficient private practice or community clinic. Ideally, the student follows the patient through all procedures indicated by the diagnosis and treatment plan, perhaps supervised by a general dentist with involvement by specialists as necessary.
Who Pays for Care in Student Clinics?
Payment for services in dental school clinics typically comes from several sources. Some patients pay the fees from their own resources; some are covered by private insurance; and Medicaid reimburses care for others. States and communities may budget funds for care of indigent and other populations, and schools may also obtain funds from private foundations and alumni contributions or from internal university allocations.
In addition, dental students appear to ''subsidize'' patient care in two ways. First, if schools do not recover clinic operating costs from fees, appropriations for indigent care, or similar mechanisms, then student tuition may be higher than it otherwise would be. Second, if schools believe they cannot increase clinic operating costs by employing adequate numbers of allied dental and administrative personnel, students may subsidize the clinic by diverting time from their own clinical education to perform tasks that would normally be delegated to others. For example, students often serve as dental assistants, undertake housekeeping components of infection control, collect fees, schedule appointments, and perform other similar tasks that have minimal educational value after an early point. Although the contention is debatable, the income generated by student fees for equipment might also be regarded as a student subsidy of patient care rather than a way of financing education.
No clinic can break even on services provided to patients who cannot pay and whose costs are not reimbursed from other public or private sources. It is not, however, straightforward to determine what constitutes an appropriate "fee" or payment for student services provided to individuals outside the normal market for dental care (discounted or otherwise). To the extent that patient care within the dental school is restructured in the directions outlined in the rest of this chapter, patient or health plan "willingness to pay" may become a more commonplace determinant of prices.
Statistical Profile of Patient Care in Dental Schools
Detailed information on dental services is in relatively short supply, and dental schools are no exception. Because they are part of large organizations that routinely collect and report information, however, dental school utilization statistics may be more complete than data for private practices. Nonetheless, data may not be comparable across schools, and demographic, clinical, economic, and other information about patients is virtually nonexistent.
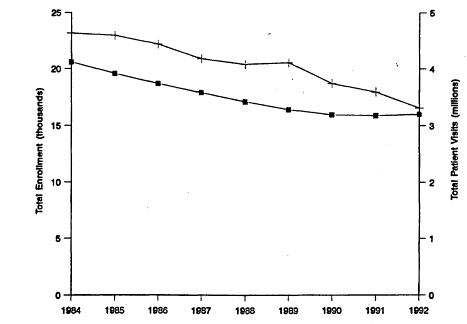
Figure 6.1
Trends in dental school enrollments ![]() and total patient visits (+), 1984-1992.
and total patient visits (+), 1984-1992.
Source: American Association of Dental Schools, 1993b.
Aggregate Data
From 1984 to 1992, dental school enrollments decreased 22 percent. With fewer students to provide patient care, patient visits in dental schools declined by 29 percent and the number of patients screened decreased by 13 percent (Figure 6.1). Numerically, patient visits fell from 4.63 million in 1984 to 3.31 million in 1992, and total patients screened dropped from a high of 396,000 in 1985 to 343.000 in 1992.
On a per D.D.S. student equivalent basis,1 patient visits de
creased from 216 in 1984 to 207 in 1992; at the same time, patients screened per student increased from 18 in 1984 to 21 in 1992. The ratio of visits to patients decreased from 12 per patient screened to 9.6. These changes appear to reflect increased efficiency (e.g., treatment plans completed with fewer visits) and more restrictive standards for accepting screened patients for comprehensive care. In addition, because oral health has improved even in the relatively disadvantaged populations served by most dental schools, dental schools today have to screen more patients to secure an adequate yield of clinical problems (numbers and types) for educational purposes.
From 1985 to 1992, clinic income increased from $104.9 million to $171.9 million (AADS, 1993b). In constant dollars, however, total clinic income during this period decreased from $104.9 million to $102.6 million, which is consistent with the decrease in numbers of patients and visits.2
As many dental educators and university administrators are all too aware, dental school clinics operate at a loss. In FY 1993, the total revenue of all U.S. dental school clinics was $188,182,280 and the total expense was $230,603,802. The overall net deficit is more than $42,000,000 (on average, more than $785,000 per dental school) (ADA, 1993b). (Unlike teaching hospitals, dental school clinics do not benefit from direct or indirect educational support under Medicare.)
Variations Across Schools
In on-campus clinics, the number of patient visits during 1992-1993 varied from lows of 7,500 and 7,732 for two schools to highs of 139,000 and 261,975 for two others (ADA, 1993a). The mean for all schools was 54,890 and the median (which is not influenced by extreme outliers) was 48,169.
The number of patients screened varied from a low of 1,050 to a high of 28,930, with a mean of 5,245 (ADA, 1993a). The ratio of patient visits to patients screened was calculated to provide another measure of clinic activity on a per-school basis. This ratio showed wide variances as well. The highest ratios were 38.8 and 34.8, and the lowest was 1.1; the median was 12.9.
Clinic revenue on a per-student basis is also highly variable, ranging from highs of $15,905 and $14,042 per student to lows of $895 and $1,866 per student in 1992; the mean was $5,515 (median of $5,180) (ADA, 1993b). Private schools had a higher mean ($6,255), but also much greater variability as evidenced by a range of revenue ($895 to $15,905).
Similarly, clinic revenue as a percentage of total revenue varies from 2.5 to 36.4 percent, with a mean of 12.4 (ADA, 1993b). Again, the mean of 10 percent for public schools is lower than the mean of 16.5 percent for private institutions.3
Why do schools vary so much? One answer may be the scheduling practices of the dental school clinic. Differences in the faculty and staff ratios, which would allow more patients to be seen, are likely contributions to variation. Another factor may be the size of the surrounding community or the extent to which the clinic has a "captive" patient population, that is, those for whom private care is not an option. In addition, the ratio of patient visits to patients screened may not capture all of the complexities of dental school clinic operations. For example, a patient may be screened in one academic year but have visits that carry over into the next year. Patients at some schools may be more likely to decline the services recommended in the treatment plan based on the screening visit.
Issues and Challenges
The mixed missions of clinical education and patient care in the dental school make trade-offs almost inevitable regardless of the way that education is structured and overseen. Dental students must gain sufficient clinical experience in a variety of technical procedures to become competent entry-level practitioners, qualified to graduate and become licensed. A procedure-driven learning process does not necessarily translate into efficient, high-quality patient care, particularly when student care is further constrained by low budgets for clinical and administrative support. Thus, patients who can afford care elsewhere typically seek service in other settings, and health plans that contract with a limited set of providers do not look to dental school clinics first.
This discussion should not imply that schools and students regard patients merely as teaching material. In the committee's survey of dental school deans, only the education of general dentists rated higher than patient care in importance to deans. Schools educate students about the elements of high-quality, ethical patient care and about their responsibilities to provide such care as students not just as licensed practitioners. For a combination of educational, patient care, and economic reasons, educators are exploring simulations or other exercises that increase student proficiency but minimize patient exposure to inept learners.
Whether viewed from an individual patient or a health plan perspective, the patient care challenges for dental schools are significant. They include issues related to efficiency, quality, competitiveness, accountability, and informed consent. From a community perspective, service to disadvantaged or vulnerable populations is an important issue. On all fronts, shifting or addition of resources will compound the stress on educators.
The following discussion first reviews problems and then considers strategies for change. The focus is on-site predoctoral student clinics rather than faculty practice plans, clinics for advanced students, or off-site settings. For the student and the dental school, the changes discussed below reinforce the call in Chapter 4 for a postgraduate year of additional clinical experience. Likewise, they reinforce the emphasis in Chapter 8 on the need for greater agreement by dental educators and examiners on what constitutes competency and how it should be assessed.
Efficiency of Care
Compared with services provided by dental graduates, care provided by students may require more time and more visits.4 Students are generally slower in completing an individual service than are graduates. For example, a cavity preparation that would take an experienced dentist a few minutes will ordinarily take a beginning student much longer. This difference costs patients time and costs clinics money because students are less productive.
In addition, variations in educational strategies have time implications. One traditional approach emphasizes student completion of a few cases of a particular procedure from start to finish. The more inexperienced the student, the more likely are the patient, student, and teacher to stay in the clinic much longer than is reasonable, even in a learning context. This is not patient-centered care.
An alternative approach stresses student participation with faculty and postgraduate students in a much larger number of cases. The faculty member serves as a role model, with the student moving from limited to extensive responsibility based on increasing skill and speed. Although the focus of this strategy is broadly on patient care, not narrowly on procedures, and the learning process is structured differently, procedural competency is still an objective. For the patient, this strategy is likely to mean less time in the clinic.
Patients may also be delayed if faculty are not available in a timely fashion to review and approve student work. Moreover, students may not have allied personnel available to assist them and save time by laying out instruments or similar activities. In addition, students often perform nonclinical tasks such as collecting payments from patients and scheduling appointments, which is almost certainly less efficient than using paid office staff. The student's time is, however, typically regarded as "free" because no direct compensation costs are involved.
Student activities aside, efficient use of the patient's time may be a low priority in other respects. Appointments may not be scheduled individually throughout the day but simply set for the beginning of the morning or afternoon clinic, so waiting times may be long. Patients may have to return for multiple visits for procedures that crosscut departments and require separate appointments for each "subclinic" within the clinic. They may have to go elsewhere for specialized care not within the scope of predoctoral training. University personnel regulations may complicate efforts to establish convenient evening and weekend clinics or otherwise make services more patient-friendly. Investments in modern computer-based information and management systems lag.
The social costs of such inefficiency—missed work hours or school days, excess transportation or child care costs—are rarely tallied. The tolerance of inefficiency may also give students a mixed message about the importance of each patient, especially the patient who cannot afford to go elsewhere.
Still, some patients, particularly older ones, may value clinic visits as a social experience more varied and interesting than a
private office visit. Evidence that patients value the relationship is provided every holiday season by the food and other gifts they bring to students and staff.
Although lower-income and retired patients now may be willing to trade time for low-cost care in student clinics, changes in the financing and organization of health care could alter this calculus. That is, newly insured patients may seek alternative sources of care, although required deductibles and other cost sharing may still make a low-cost student clinic attractive to some (Tunnicliff, 1994). Groups of patients covered by health plans may increasingly be directed to a restricted network of employed or contracting providers. It is unlikely that a health plan would include a traditional student clinic in this network.
Quality of Care
Quality of care has been defined by another Institute of Medicine committee as "the degree to which health services for individuals and populations increase the likelihood of desired health outcomes and are consistent with current professional knowledge" (IOM, 1990e, p. 21). Quality problems may arise from (1) overuse of care, which occurs when more services are used or provided than appropriate (e.g., unnecessary replacement of restorations); (2) underuse of care, which happens when clearly beneficial care is forgone (e.g., untreated caries, extraction of a tooth rather than feasible restoration); and (3) poor technical or interpersonal care (e.g., defective restorations, failure to explain treatment options and consequences).
Quality problems occur in all settings, but the dental school has some particular vulnerabilities. First, care provided by learners may be more physically uncomfortable or painful than care provided by the proficient. Also, slow performance may in and of itself produce emotional and physical distress.
Second, the initial technical quality of care may be inadequate. If the problem is apparent, corrective work must be performed by the student or supervising faculty, which involves additional time and perhaps physical discomfort. Other technical deficiencies, such as an imperfectly bonded restoration, may not be observable until some time has passed.
Third, graduation requirements and evaluation procedures are a potential threat to quality of care. At most schools, a student cannot graduate without completing a defined number of various procedures or acquiring a defined number of points calculated as
function of number and types of procedures and their difficulty. If a particular patient's (or group of patients') problems do not fit a student's requirements (e.g., for a crown), the student may be tempted to fit the patient to the service rather than vice versa. The result may be either undercare or overcare or both. In principle, faculty oversight—if not student ethics—should preclude such practices, but the oversight process is viewed by many of those interviewed for this study as uneven both within and across schools. Assessment based on competency levels, whether acquired after four or fourteen procedures, would not eliminate the potential for inappropriate treatment, but it would presumably reduce the risk of unnecessary care from those students who are able to demonstrate competency with fewer repetitions of a procedure.
Fourth, dental schools often serve patients who cannot afford to go elsewhere and whose economic status may lead to less than optimal treatment. For example, a poor patient may have a tooth extracted because indigent care programs do not cover root canals or expensive restorations that would save the tooth. Economic realities also mean that dental school clinics may leave some indigent or partially insured patients untreated or only partly treated. Both of these quality of care problems reflect social policies over which dental schools have little control, although dental schools may lobby for improved Medicaid coverage of dental services, for direct public and private support for their own clinic and outreach programs, and for other community-based programs to which they can refer some patients.
The above discussion emphasizes problems, but the dental school clinic also may have characteristics that are linked to higher-quality care including frequent faculty interaction with peers in the same or other disciplines and a systematic process and explicit criteria for evaluating individual treatments. Independently or in conjunction with efforts throughout an academic health center, student clinics can, in principle, draw on the management, research, and analytic capacities of administration and faculty to evaluate practice patterns, examine outcomes, and establish benchmarks for improving the processes and outcomes of care. The positive social benefits that accrue to some patients (as cited above) also may be attributed to a good interpersonal quality of care in a dental school clinic.
Unfortunately, systematic evidence about the quality of care in dental school clinics (and, for that matter, in private practice) is largely unavailable. Quality assurance programs are, for the most part, new and little tested in dental school clinics. As yet, such
programs have not provided valid and reliable information on the process and outcomes of care. A 1990 survey of quality assurance programs in dental schools indicated that barely half the responding schools were reviewing the outcomes of care (Butters et al., 1991). Only three-quarters of the schools reported a responsible individual or formal administrative program for quality assurance, and nearly all such programs had been established for less than six years. Less than 90 percent periodically reviewed infection control activities, a universal expectation of quality assurance programs in most settings. Although about two-thirds of the respondents indicated that they assessed patient satisfaction with services, only 19 percent had written criteria for this assessment.
In general, then, dental educators lack both the programs and the data needed to assess the quality of care in an individual school or to compare alternative models of patient care for differences in timeliness and appropriateness. Such assessments and comparisons could prompt changes in processes of care that would serve both the mission of patient care and the mission of education.
To be fair to dental schools, quality assurance mechanisms are generally less advanced in ambulatory care settings than in hospitals (IOM, 1990e). As quality has become an increasingly important issue to policymakers, providers, health plans, and patients, this is changing. More systems and requirements for quality assessment and assurance are developing. Since the early 1980s, accreditation standards for dental schools, for example, have included certain patient protection provisions (CDA, 1993a). These involve emergency services and training, diagnosis and treatment planning, preventive services, recall procedures, and patient rights (Table 6.1).
Whether a single accreditation process is satisfactory for both education and patient care in the dental school is an important question. Reflecting its traditional reliance on the hospital as an educational site, the medical model separates the roles. The Liaison Committee on Medical Education accredits medical schools, and a variety of independent organizations, notably the Joint Commission on the Accreditation of Health Care Organizations, accredit patient care facilities and programs. Although the Joint Commission has moved beyond its original focus on hospital care, the accreditation of ambulatory care settings is in the hands of multiple, often competing organizations that are still struggling with basic criteria and procedures. As the Joint Commission begins to review ambulatory care programs including hospital-associated dental clinics, the content and source of standards for patient care programs are likely to become a more pervasive issue in the academic health center.
TABLE 6.1
Standard 6—Patient Care and Clinic Management
|
6.1 Patients, students, faculty, and staff must be informed of the school's patient care policies. The school must have mechanisms to review and revise the procedures used in providing care to patients. |
|
|
6.1.1 |
Institutions must have mechanisms to ensure that patients are informed about and have the potential to receive comprehensive dental care. |
|
6.1.2 |
Each institution must develop and distribute to all students, faculty, appropriate staff, and to each patient a written statement of patients' rights. |
|
6.1.3 |
Each patient must receive an assessment and diagnosis consistent with the level of care being provided. |
|
6.1.4 |
An active recall program must be in operation for all active comprehensive care patients. An individualized prevention program should be an integral component of all comprehensive patient care activities. |
|
6.1.5 |
Each institution must provide for all registered patients a dental emergency service accessible at all times. |
|
6.1.6 |
A written protocol for the prevention and management of medical emergencies must be developed for all clinical programs; all students, faculty and support staff involved in the direct provision of patient care must be recognized (certified) in basic life support procedures, including cardiopulmonary resuscitation, at intervals not to exceed two years, and be able to manage other medical emergencies. |
|
6.1.7 |
Institutions must ensure the safe use of ionizing radiation in their clinics. |
|
6.2 Each institution must develop a system of clinic administration and ensure that appropriate authority is granted to those with the responsibility for clinic administration. |
|
|
6.2.1 |
Each institution must ensure that an appropriate level of direct faculty supervision is available at all times when students are providing patient care. |
|
6.2.2 |
Dental education institutions must ensure the availability of an adequate patient pool that permits students the opportunity to obtain clinical competency within a reasonable time. |
|
6.2.3 |
Each inception must develop mechanisms to ensure that all patients who enter into active treatment do so as soon as possible after first contact with the admissions process. Mechanisms must be in place to track each patient to ensure continuity of care as treatment progresses. |
|
6.2.4 |
Each institution must establish and enforce a mechanism to ensure adequate clinical/preclinical/laboratory asepsis, infection and hazard control and disposal of hazardous waste. |
|
6.2.5 |
The patient record must be available at each patient appointment and must be an orderly, standardized and legible document in which all necessary information is readily accessible. |
|
6.2.6 |
Each school must provide a formal system of quality assurance that includes a formal record review process and a post-operative patient review process. |
|
SOURCE: Commission on Dental Accreditation, 1993a. |
|
Accountability And Informed Consent
Accountability for individual patient care is a potential problem in most dental school clinics as is proper handling of informed consent by patients. In the traditional dental school clinic, no single student or faculty member may be responsible for comprehensive oversight of a patient. Instead, each department may have various faculty members supervising students whose patients arrive in the clinic for specific treatments. If one student or faculty member does not follow a patient from oral diagnosis through treatment, it may not be clear which student is responsible for patient follow-up or future dental work.
In comprehensive care clinics, a student is typically responsible for all basic services for a given patient, and most services are provided in a single general clinic overseen by faculty. Depending on how faculty are scheduled, however, the same combination of student, patient, and service may be overseen by different faculty members. This tends to dilute faculty accountability.
Concerns about informed consent permeate health care. Practitioners, administrators, and consumer advocates are struggling to devise strategies that permit truly informed consent to care from culturally and clinically diverse patients who receive remarkably varied services in different settings and circumstances. Within the dental school, informed consent collected at the screening stage is insufficient because a plan of treatment has yet to be devised to which a patient can consent. In addition, patients may not be properly informed about who will provide care—predoctoral student, resident, fellow, faculty, or some combination.
Competition
As noted earlier, restructuring of health care delivery and financing is challenging academic health centers.5 HMOs and other kinds of ''managed care'' plans generally emphasize primary care and compete heavily on price. The emphasis on price tends to
put academic health centers at a disadvantage because of their costly characteristics including clinical teaching and research, extensive tertiary services, and care for indigent patients turned away elsewhere. Many centers also have a dearth of primary care practitioners and facilities to serve the day-to-day needs of health plan members. To the extent that it favors mergers and multihospital systems, the competitive environment poses another problem because many academic health centers are constrained in their decisions by their university affiliations and public sponsorship. Proposals to revamp Medicare payments for graduate medical education—a major source of income for health centers—and to institute residency quotas also threaten the financial health and operating arrangements of academic health centers. (Some of these problems are discussed further in Chapter 7.)
The position of the dental school needs, however, to be distinguished from that of the university hospital or the medical school in certain respects. Rather than relying on a separate hospital as medical schools do, each school operates its own outpatient dental "hospital" in the form of a student clinic. These outpatient clinics do not receive the kind of direct and indirect educational payments from Medicare that teaching hospitals receive. Within the dental school, the imbalance between general and specialist care and faculty is substantially less than in the medical school and medical center hospital. In addition, although the spread of dental insurance has allowed more patients to pay for care from private practitioners, the high cost-sharing requirements of many dental plans continue to make the dental school clinic attractive to lower-income patients.
Today, some dental schools have a backlog of patients, and patients may wait weeks for an appointment (Tunnicliff, 1994). At the same time, these schools and others may worry about a shortage of certain types of patients for their student clinics. One consequence of the reduction in caries among children has, for some schools, been an insufficient number of patients with simple caries. Students may thus face complex patients earlier than they would have in the past, another argument for more faculty involvement in patient care.
Where schools face shortages of "teaching" patients, they may try to be more patient oriented to attract those in need of care. This may be difficult. The efficiency, quality, and accountability deficiencies described in this chapter are not easily overcome, especially when the resources constraints make it difficult to upgrade facilities and staffing. In addition, efforts by dental schools
to expand the patient base for student clinics—and faculty practice plans—may encounter opposition from community practitioners. For both dental schools and private dentists, the future may bring more significant competitive threats as those health plans that cover dental services extend selective contracting or employment arrangements to dental care (Bradford, 1992; Keefe, 1994).
As noted above, academic health centers face major challenges from health care restructuring, challenges that differ from community to community depending on the specifics of state policies and local health care markets. Individually and collectively, they are still developing strategies to deal with ongoing and anticipated changes in health system organization and financing. Some are likely to fare better than others, either because their environment is less hostile or because their adaptive strategies are superior.
Not surprisingly, the committee's site visits made clear that dental schools face different environments that relate in part to the size, competitiveness, and other characteristics of their community and in part to the directions being set by university or academic health center leaders. Some institutions have indicated that all components of the academic health center, including the dental school, must become more patient oriented and efficient to survive in a more competitive health care system. This may put additional pressure on dental schools to adopt the comprehensive, faculty-based models of clinical education described in Chapter 4. Faculty practice plans that incorporate care by predoctoral students may, however, not be attractive to health plans that include only a limited set of health care providers.
Community Service
During the 1970s, many dental schools developed community dentistry departments or programs that provided clinical experiences in community health settings for most dental students. Funding for these programs came from federal government initiatives such as the Model Cities program and Public Health Service grants. The elimination of these federal programs coupled with reductions in other sources of dental school revenues led many schools to discontinue or limit off-site clinical opportunities for students. Another disincentive is that schools forgo fee income when students are off-site rather than providing services in the dental school clinic. Reduced student and faculty involvement in the larger community increases the isolation of the dental school.
If coverage of basic dental services does not become more widespread through either private or public initiative, student clinics are likely to remain significant sources of care for low-income people. Even if dental insurance should become near universal, cost-sharing requirements, low reimbursement rates, and other restrictions might still encourage poor or even middle-class patients to seek lower-cost sources of care.
Financial barriers are, however, not the only obstacles to adequate dental care. As noted in Chapter 3, geographic, educational, and other factors also affect access. What this implies for the role of student-provided dental services will probably vary depending on the characteristics of the service area, the school's physical location, and other factors.
Rethinking the Mission of Patient Care
General Precepts
More than missions of education and research, the mission of patient care in the dental school is undergoing necessary and fundamental rethinking. This rethinking is necessary because the environment is changing. It is fundamental because it places patient care in a broader social context, one that extends well beyond the dental school and its current patients or patient care activities. The rethinking process will highlight the relationship of the dental school to the academic health center and the relationship of both to a changing health care delivery and financing system.
Because the health care system is a complex mixture of national, state, and community influences and institutions and because each dental school's situation has its own special characteristics, each school's own reassessment and restructuring process will be different. For example, some schools exist within universities that have no academic health center or that have located the center's components across distant campuses or communities. Even when an academic health center exists, it may or may not welcome stronger ties to the dental school. Other centers may see faculty and student dental clinics as assets. To cite another difference, some schools are located in small communities in which prospects for a "managed care revolution" are uncertain. These differences, although they require strategic consideration, should not be used to rationalize inaction.
Starting Points
In the committee's view, the starting point for dental schools is an affirmation or reaffirmation that patient care is a distinct mission that is related but not subservient to the educational and research missions. Dental educators and students must be as conscious as the private practitioner of patient needs, preferences, motivations, and limitations.
In preceding sections of this chapter, some specific options for dental schools to improve their patient care mission are proposed or implied. They include
- strategic planning that anticipates continued restructuring of the health care system;
- adoption of a formal, comprehensive quality assurance and improvement program;
- increased faculty accountability for patient care and more reliance on residents (for schools that have relevant graduate programs);
- more efficient administration of nonclinical activities;
- improvement of information systems to support outcomes research, quality improvement, and effective management;
- possible separation of accreditation programs for education and patient care; and
- integration with the patient care activities of the entire academic health center.
Strategic Planning
Strategic planning considers alternative futures and approaches for dealing with both more and less likely contingencies. For most dental schools, the planning process occurs within the broader framework and constraints of strategic planning for the university or academic health center. Chapter 7 recommends that dental schools, as part of their strategic planning process, undertake a very explicit assessment of their position—assets, deficits, opportunities, constraints—within this larger environment and identify objectives and steps to strengthen their position. Patient care will figure significantly in any such effort.
Almost any future for a dental school will involve most of the elements discussed below, including more patient-oriented care, formal quality assurance processes, and improved information systems. Some schools will see integration in a larger system as a feasible
and desirable objective, and some may have such integration essentially dictated by their parent institutions. Other schools may determine that their patient care mission will be best served and sustained if they concentrate on market niches such as selected specialty services. Integration may not be a significant option for schools in more rural communities.
Quality Assurance and Improvement
Quality assurance is a very broad subject that, to some degree, encompasses most of the areas discussed later in this section, for example, accreditation and faculty accountability. It also overlaps with topics such as practice guidelines and outcomes research that have been discussed in other chapters. Patient care within dental schools needs, however, an overarching model of quality assurance and improvement as a reference point. One such model, continuous quality improvement (CQI), has gained wide currency elsewhere in the health care system. Its principles emphasize the following (IOM, 1992, p. 103):
- close relationships between so-called customers and suppliers (that is, the partners in any given health care transaction);
- errors being more often the result of defects in systems (e.g., those for reporting test results or scheduling operating rooms) than the consequence of individual deficiencies ("bad apples");
- planning, control, assessment, and improvement activities grounded in statistical and scientific precepts and techniques;
- reliance on internal (self-) monitoring—as opposed to external (regulatory) inspection—with mistakes viewed as "treasures" that should be used for learning and for resolving problems rather than as an occasion for punishment;
- standardization of processes (decreasing their variability) to reduce the opportunity for error and to link specific care processes to health outcomes;
- feedback to practitioners of statistical information on how their practices may differ from those of their peers or depart from evidence-based standards for practice;
- visible commitment to quality by the top leadership of the organization and involvement by all parts of the organization in processes of quality improvement; and
- a striving for continuous improvement in contrast to simply achieving preset goals.
Intricate mechanisms for applying these principles have been set forth and, subsequently, questioned for their costs and impact. Experimentation with implementation strategies continues (see, for example, Batalden et al., 1994; Horn and Hopkins, 1994; and Kibbe et al., 1994). This experimentation generally includes steps to improve information systems and analytic capacity at the institutional and systems levels. In the systems category falls research on the outcomes of patient care and the impact of guidelines for care in improving performance. (Chapter 3 discusses outcomes and guidelines.) Generally, institutions have applied CQI first to administrative processes, moving more slowly into clinical applications. The latter are, however, becoming increasingly important.
The precepts of continuous quality improvement appear to be diffusing among dental schools, albeit at an uneven rate. Fortunately, dental schools have the opportunity to learn from the experience of other institutions in implementing these precepts. For dental schools, an additional attraction of patient-oriented quality improvement strategies is that it presents research opportunities for dental school faculty, for example, in assessing patient priorities, measuring satisfaction with care, and evaluating methods for modifying patient behavior and improving compliance with oral hygiene regimens.
Faculty Accountability
Some dental schools are already moving to increase faculty accountability for patient care. The most definitive step is to assign responsibility for each patient to a faculty member who works with students, other generalist and specialty faculty, allied dental personnel, and administrative staff to match patient problems to student needs and capacities and who ensures comprehensive patient care by providing, overseeing, and coordinating services. This definitive step is by no means simple. It demands more of clinical faculty and typically involves administrative, personnel, and or facility adjustments that are neither quickly nor inexpensively implemented. Serving more fully as role models for students should, however, prove stimulating to those faculty who find satisfaction in both patient care and clinical education.
Greater faculty accountability may be accompanied by another change that could improve patient satisfaction and clinic efficiency. As described earlier, the current model in most schools is for students to learn procedures by doing a few of them perfectly
from start to finish. An alternative model is for students to participate in the care of a great many patients, undertaking a few elements of a procedure initially and adding steps as they gain proficiency. Under such a model, time demands for many patients should be significantly less.
For the student, the alternative model brings exposure to a wider array of patients with a broader array of clinical problems—some simple, some complex. As a result, students learn more about the acceptable range of practice in areas such as diagnosis, treatment planning, procedural treatments, teamwork with allied dental personnel, and referral to specialists.
Administrative Efficiency and Information
Better patient care means more efficient clinical care, which, in turn, requires more efficient administrative support. The restructuring of the health care system is reinforcing the pressure on practitioners and institutions to upgrade their information systems, patient records, quality assurance and improvement programs, and ability to report their performance to public and private purchasers. Although dentistry and office-based medical care more generally have been slow to experience some of these pressures, this chapter has argued that this relative exemption will not last.
As noted earlier, dental school clinics are, in principle, in a good position to draw on their faculty and on other components of the academic health center for the knowledge and analytic capacities needed to assess and improve their performance. Steps that schools take to improve information and administrative systems should bring diverse benefits, for example, improving feedback of performance information to students and reducing the clerical and other noneducational components of clinic work. They should also reinforce some of the research strategies proposed in the preceding chapter.
Accreditation
The dental community, most notably the Commission on Dental Accreditation and the American Association of Dental Schools, must address the collective processes for overseeing the quality of dental education and the quality of patient care within the dental school. If dental school clinics follow the path of competition and integration outlined elsewhere in this chapter, the develop-
ment of a separate organization and process for accrediting or certifying clinics in dental schools may be advisable at some point. That process would best be structured as part of a more comprehensive effort to assess and ensure the quality of dental care including community-based and hospital-affiliated services.
The path toward certification for outpatient care programs has not been a smooth one in either medicine or dentistry, and the design and implementation of quality assurance and improvement programs for ambulatory care encounter particular problems. Difficulties include the number and diversity of ambulatory care settings and services, their traditionally fragmented and incomplete data systems, and the relative scarcity of agreed-upon quality indicators, especially outcomes measures (IOM, 1990e). Improvements in data systems and outcome measures should be priorities for dental school clinics regardless of how external review programs are structured.
Integration With the Academic Health Center
To the extent that the health care system of the future is based on organizations that integrate different types and settings of care, most academic health centers will need to develop a more coherent relationship among their constituent patient care units. Where a center can call upon its dental school, it may be able to develop an advantage over competitors without dental programs if the school's patient care activities become more patient oriented and able to attract patients independently or through referrals. Not only could the school offer services, it could be a productive source of referrals for other parts of the academic health center. Thus, academic health centers may indeed welcome participation by dental educators in reorganizing patient care activities to make them more competitive. Where such participation does not exist or is limited, dental school deans and faculty should take the initiative in exploring closer relationships.
Dental schools that are not part of an academic health center could, in principle, seek integration or involvement with other institutions. Whether they would be attractive partners absent some preexisting connection probably would depend on how attractive patient care within the dental school could be made.
Findings And Recommendations
Dental schools' perceptions of their patient care mission are still evolving, as are their strategies for fulfilling this mission. The
typical dental school clinic, put simply, is not patient-friendly. The focus is still very much on procedures rather than on patients, and sufficient emphasis has not been placed on efficiency, quality, and accountability for care from the patient's perspective. Problems it these areas are serious in their own right and will become more acute if current trends in health care delivery and financing continue. Academic health centers are having to compete for patients and for participation in managed care plans of various sorts. Whether a dental school clinic adds or subtracts from the overall institution's market position is likely to be an issue in its future. As currently structured, few dental schools—even when they charge lower fees— are attractive to insured patients.
Over the long-term, the committee believes that dental schools have no ethical or practical alternative but to make their programs more patient-centered and more economically viable. This will involve very significant changes in the way many dental educators and practitioners view the roles and operation of dental schools. Such changes will not be achieved painlessly or immediately or without the support of community dentists and dental organizations. Financing will be a major challenge.
To affirm that patient care is a distinct mission, each dental school should support a strategic planning process to
- develop objectives for patient-centered care in areas such as appointment scheduling, completeness and timeliness of treatment, and definition of faculty and student responsibilities;
- identify current deficiencies in patient care processes and outcomes, along with physical, financial, legal, and other barriers to their correction; and
- design specific actions—including demonstration projects or experiments—to improve the quality, efficiency, and attractiveness of its patient services.
To respond to changes in roles and expectations for providers of outpatient health services including dental school clinics, the Commission on Dental Accreditation and the American Association of Dental Schools should
- reexamine processes for assessing patient care activities in dental schools and ensuring the quality of care, and
- begin to evaluate new options such as eventual participation by dental schools in separate accreditation programs for their ambulatory care facilities.
To increase access to care and improve the oral health
status of underserved populations, dental educators, practitioners, researchers, and public health officials should work together to
- secure more adequate public and private funding for personal dental services, public health and prevention programs, and community outreach activities, including those undertaken by dental school students and faculty; and
- address the special needs of underserved populations through health services research, curriculum content, and patient services, including more productive use of allied dental personnel.
Summary
This chapter has examined the clinical services of dental schools primarily from the patient and health care system perspective rather than from an educational perspective. Such a perspective has not been typical among dental schools, and most schools' views of their patient care mission are still evolving as are their strategies for fulfilling this mission. Changes in the role of health professions schools and academic health centers both in the university and in the larger health care system will put pressure on dental schools to improve the efficiency and quality of their patient services.
Reshaping the provision of patient care in the average dental school will not be easy or quick because it will require change in long-standing attitudes and administrative practices. In addition, it may require that funds be found to upgrade facilities and staffing. These difficulties will be compounded by broad alterations in health care delivery and financing that are proving difficult for academic health centers, private practitioners, patients, and governments alike. Turmoil and uncertainty may be the most stable features of the next decade.

























