1
Background and Introduction
Dental education has arrived at a crossroads. During the last 150 years, it has evolved from a prelude to apprenticeship into a comprehensive program of professional education. Advances in science, technology, and public health programs have greatly reduced tooth decay and tooth loss. Dentists are respected professionals, and dental schools are part of many of the nation's leading public and private universities.
This progress notwithstanding, the position of dental education within the university is being questioned as is its relationship to medicine and the larger health care system. Six dental schools—all private—have closed in the last decade (Table 1.1), and others among the 54 remaining schools are in jeopardy. The dental profession is at odds with itself on a number of issues including work force policies, licensure, and health care restructuring. Tensions between practitioners and educators can undercut the profession's position within the university.
The future of dental education will be shaped, in part, by scientific, technological, political, and economic factors that are largely beyond the profession's control. Nonetheless, dental educators—individually and collectively—have important choices to make. They may attempt to preserve the status quo—in effect, a path toward stagnation and eventual decline. Alternatively, they can choose a more difficult path of reassessing and renewing their missions of education, research, and patient care so that they
TABLE 1.1
Number of U.S. Dental Schools, 1970-1993
contribute more—and more visibly—to the university and the community. Taking this latter path will require more vigor in implementing long-standing recommendations for educational reform as well as attention to new issues and objectives. For dental educators to pursue change successfully, they will need the active cooperation of the larger dental community as well as support from university officials and state and national policymakers.
This Institute of Medicine (IOM) study was prompted by concerns that the challenges confronting dental education, although generally recognized, were not understood or appreciated adequately and that effective responses had yet to be identified or presented in a persuasive manner. The purpose of the study was "to assess dental education in the United States and make recommendations regarding its future." It was overseen by an 18-member committee that was appointed after extensive consultation with dental and related organizations. The group included members with expertise and experience in dental practice and education, oral health and health services research, other areas of health professions and higher education, health care delivery and financing, and public policy. The committee as a whole met six times between February 1993 and May 1994. As described in the Preface and summarized in Appendix 1.A, it undertook a wide range of activities to collect information and perspectives from all segments of the dental community and other relevant, interested groups. (The papers commissioned by the committee will be published in the Journal of Dental Education; they are listed in Appendix C.) This document, which was submitted for outside review in accordance with
IOM and National Research Council procedures and policies,* constitutes the committee's final report.
Dental Education in Context
The Broader Environment
The achievements of dental education and its current problems must be set against a larger societal backdrop. For the United States through most of this and the last century, that backdrop was generally one of growth and innovation. The nation's economy expanded and became vastly more complex. Scientific and technological development proceeded at a remarkable pace. The forms and purposes of government were reshaped and enlarged. The infrastructures of higher education and the health professions were greatly elaborated. Major improvements in personal health, wealth, and education accompanied these social and economic changes.
Today, growth and innovation continue, but they occur in an environment more generally characterized by reevaluation, reorganization, and retrenchment. Public confidence in government, education, and other basic social institutions has diminished. The aging of the population is reshaping the country's view of itself and stimulating debates about generational equity in social policies. Fiscal stress seems an almost routine state of affairs from the governmental to the individual level, and the gap between the more and the less advantaged segments of society threatens to become a gulf in some areas.
As this committee was deliberating, health care reforms that would extend health insurance to all or most Americans were once again on the national political agenda, but the prospect for meaningful action was in doubt. Even without federal legislation, concern about health care costs has already prompted major and sometimes traumatic restructuring in the way health care is delivered and financed. Increasingly, providers and consumers are finding their options limited by the growth of health plans characterized by capitated provider payment systems, closed panels of health care practitioners, limited access to specialists, and various other constraints.
Universities and their constituent parts are likewise under stress. Their stewardship in managing research funds has been questioned, and political controversies have raised public questions about the scholarly objectivity and merit on which such institutions pride themselves. Like private organizations, some have "downsized" by eliminating uneconomic or marginal programs. One consequence of the pressures on public and private institutions alike is an increased emphasis on accountability, performance measurement, and quality improvement.
Challenges for Dental Education
Developments in dentistry and dental education reflect the larger societal patterns of growth and realignment just discussed. In the decades after the founding of the first school in 1840, dozens of dental schools were established. Many eventually disappeared, but more than 50 schools became established within public and private universities. The fixtures of a profession also accumulated: associations, journals, licensure laws, educational standards, and specialization. Technical improvements in procedures and materials made dental services more effective and less painful and, thus, more acceptable to the public.
In addition to broader social, economic, and scientific changes that have altered expectations and opportunities, recent decades have brought pressures for change that are more specific to oral services and that will continue to reshape the profession in the next century. First, the oral health of the American people has improved substantially, thereby affecting the demand for many traditional dental services such as extractions, dentures, and restorations. As recently as World War II, the primary physical reason for rejection of military recruits and draftees was dental defects; nearly 9 percent of those examined were rejected because they did not meet the requirement for six opposing teeth in each jaw. Such rejections are now rare. Preventive strategies at the individual and community levels have reduced tooth decay dramatically in children, and the number of older Americans with no teeth has declined significantly in recent decades. Still, oral disease remains commonplace, although it is concentrated in a subset of the population. For example, one-quarter of U.S. children experience three-quarters of the tooth decay or caries found in children. In general, minority groups and families with low levels of income and education and with limited access to dental services suffer disproportionately from oral health problems.
Second, demographic changes are affecting dental practice. In the future, the number and proportion of elderly patients, who tend to have more complicating medical conditions and are retaining more of their teeth, will grow (Figure 1.1). In addition, the oral health care needs of other patients with complex medical problems such as cancer and AIDS are becoming better appreciated.
Third, scientific and technological advances are reinforcing the medical aspects of dental practice as new or improved preventive, diagnostic, and pharmacological interventions challenge procedure-oriented dental education. Computer-based technologies are changing the nature of dental practice and providing new opportunities for evaluating and improving the outcomes of care.
Fourth, health plans that restrict patient access to a selected panel of dentists are moving beyond their historically small base. However, because more than half the population is not insured for dental services compared to less than one-fifth with no health insurance, the impact of health care restructuring has, so far, been relatively limited for many practitioners and patients. Overall, about 6 percent of all expenditures for personal health services
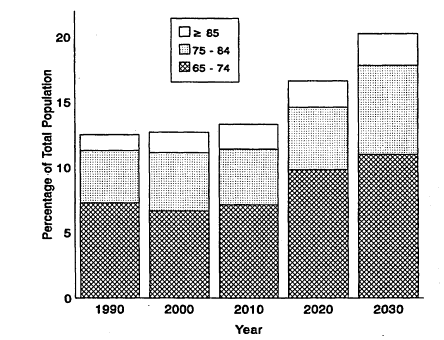
Figure 1.1
Trends in age distribution of U.S. population aged 65 and over, 1990-2030.
Source: U.S. Department of Commerce, 1993.
are accounted for by dental services, but the majority of this expense is not covered by insurance.
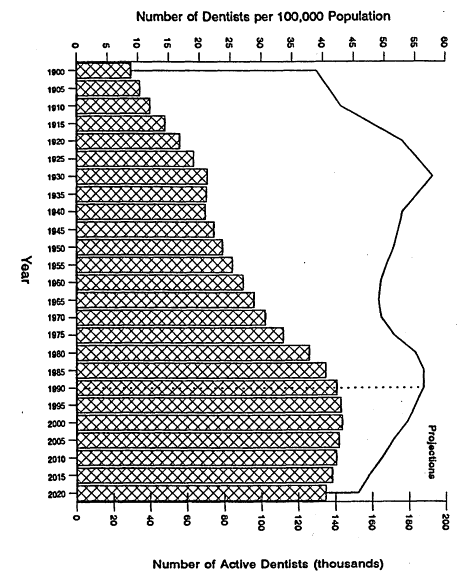
Fifth, although the number of dentists is still growing, projections suggest that the number will drop gradually after the turn of the century (Figure 1.2). This drop will reflect the decrease in dental school enrollments in the last decade, which has been equivalent to the closure of 20 average-sized dental schools. Because the U.S. population almost certainly will continue to grow, the ratio of dentists to the general population is expected to drop even more sharply—almost as sharply as it increased in the 1970s. How this downturn will affect future access to dental services and priorities for dental education depends on a number of economic, social, technological, and other factors. For example, the inclusion of dental benefits in a health care reform package would likely increase the demand for care because insured persons use more services than do those who are uninsured.
Sixth, dental education faces serious financial problems that, in many respects, constrain its ability to respond to the changes identified above. Within the university, dental education is viewed as relatively expensive, and as dental schools have reduced enrollments, many essentially fixed costs remain to be spread over a smaller number of students. During site visits and other discussions, the committee learned that discontinuation of several schools (in addition to the six that have already closed) is a serious—although not necessarily publicly acknowledged—possibility.
Dental education and dentistry are made vulnerable by their relative isolation from the broader university, from other health professions, and from the restructuring of health care delivery and financing that characterizes most of the health care system. This vulnerability is further increased by tensions between the practitioner and education communities. These tensions are most visible in the two areas, professional licensure and work force policy, both of which involve professional economic interest in the supply of dentists and allied dental practitioners and the conditions for entry into the profession. Other tensions have arisen from dental school efforts to increase revenues by creating faculty practice plans, to restructure departments, and to conduct research on such issues as access to dental care and the effectiveness of specific dental treatments. Failure to resolve or reduce these tensions will undermine the efforts of dental educators to improve their performance and solidify their positions within their parent universities and communities. This could jeopardize the future of the profession.
Envisioning the Future
To respond to the challenges just outlined and to move successfully into a new century, dental educators and the larger dental community need some agreement on common purposes and directions. Formulating such agreement, in turn, requires an understanding of how well current modes of thinking and operation equip dental education and dentistry in general to face a future that is likely to be quite different from the past.
This report is intended to help build understanding and agreement. It combines a set of policy and strategic principles with an extensive analysis of dental education's present and future to form a broad picture of dental education in the twenty-first century. This picture is not a vision of an ideal world. Rather, it distills the committee's general view of what the future will bring, combined with its conclusions about how dental educators and others can reasonably, if not easily, prepare the profession for a constructive role in improving oral health in the twenty-first century.
Principles
To guide its deliberations about the future of dental education and practice, the committee adopted eight general policy and strategic principles. These principles, which are woven throughout the text of this report, include those that follow.
Oral health is an integral part of total health, and oral health care is an integral part of comprehensive health care, including primary care. For oral health problems to be appropriately addressed, these connections need to be better understood and strengthened by dentists and other health professionals, educators, policymakers, and the public in general.
The long-standing commitment of dentists and dental hygienists to prevention and primary care should remain vigorous. This commitment has served the public well in the past and is consistent with demands that the broader health system—including health professions education—focus more on primary care in the future.
A focus on health outcomes is essential for dental professionals and dental schools. The effectiveness of dental services in achieving desired health outcomes for individuals and communities cannot simply be assumed but must be demonstrated to patients, other purchasers of dental services, and policymakers.
Dental education must be scientifically based and undertaken in an environment in which the creation and acquisition of new
scientific and clinical knowledge are valued and actively pursued. Research and scholarship are essential elements of university-based education and are critical to continued improvements in oral health.
Learning is a lifelong enterprise for dental professionals that cannot stop with the awarding of a degree or the completion of a residency program. Preparing dental professionals to continue to learn and to critically appraise new and traditional technologies is a critical function of dental education.
A qualified dental work force is a valuable national resource, and support for the education of this work force must continue to come from both public and private sources. Although industry, alumni, and students each have a contribution to make, government must play a strong role because a well-prepared oral health work force is a public good. Further, its future is too important to be determined solely by the isolated decisions of individual universities and states.
In recruiting students and faculty, designing and implementing the curriculum, conducting research, and providing clinical services, dental schools have a responsibility to serve all Americans, not just those who are economically advantaged and relatively healthy. Efforts by some dental schools to serve disadvantaged individuals and communities—and to provide students and faculty with direct understanding of their needs—are challenged by reductions in public support for both education and patient care. The creation of a dental work force and faculty that reflect the nation's diversity is a goal only partially achieved at this time.
More generally, efforts to reduce the Wide disparities in oral health status and access to care should be a high priority for policymakers, practitioners, and educators. With its traditional emphasis on prevention and primary care at the individual and the community levels, dentistry has a good foundation on which to build.
Prospects
As the twentieth century ends, dental education faces many challenges—financial, intellectual, organizational, and technological. In the future as envisioned in this report, four elements stand out.
First, dentistry will and should become more closely integrated with medicine and the health care system on all levels: research, education, and patient care. The march of science and technology
in fields such as molecular biology, immunology, and genetics will, in particular, continue to forge links between dentistry and medicine as will the needs of an aging population with more complex health problems. These links combined with the financial strains on the university and academic health center will encourage these institutions to consolidate or otherwise link programs in related areas such as dentistry and medicine. Government and private purchasers of health services can be expected to maintain and indeed increase the pressure on health care practitioners and institutions to develop more highly integrated and constrained systems of care that stress cost containment, primary rather than specialty care, and services provided by teams of professional and other personnel. Although dentistry may experience a less rapid restructuring of its place in health care compared to other health professions, any such respite should be used not as a time to reinforce resistance to these developments but as an opportunity to achieve a smoother transition for patients, practitioners, and educators.
Second, to prepare both their students and their schools for Change, dental educators will need to teach and display desirable models of clinical practice. Such education will be scientifically and technologically up to date, focused on outcomes, interdisciplinary, efficient, patient and community oriented, and team based. For most schools, this will require substantial departures from current practices. These practices fall short for various reasons including incomplete implementation of long-standing and still valid proposals for reforming the curriculum, relatively slow recognition of new emphases on health outcomes and sophisticated information capabilities, and increasingly constrained resources.
Third, securing the resources essential for educational improvement and, indeed, survival will require that dental schools demonstrate their contributions to their parent universities, academic health centers, and communities through achievements not only in education but also in research, technology transfer, and community and patient service. Said differently, dentistry cannot pursue isolation. The process of change may exacerbate tensions with dental practitioners, for example, as dental schools experiment with new models of patient care and extend their outcomes research agenda. Thus, efforts to manage and resolve conflicts must have a high priority.
Fourth, the dental community—educators, practitioners, regulators, and policymakers—will benefit from continued testing Of alternative models of education, practice, and performance assess-
ment for both dentists and allied dental professionals. Experimentation and learning will also help dentistry face one its major uncertainties, namely, whether the future Supply of dental practitioners and services will match, exceed, or fall below population requirements for dental care. That uncertainty is, in large measure, a function of the unpredictability of scientific and technological advances and of social policies affecting access to oral health services. Under these circumstances, contingency planning is stressful but essential.
The committee's specific recommendations are not, in general, highly prescriptive statements about what individual schools should do and how they should do it. Likewise, although concerned about the sources and some of the consequences of the variation across schools, the committee views variation as inevitable and often desirable. Recommendations are not directed at dental educators alone but call upon the entire dental community to work collectively toward improved oral health through more effective education, research, and practice.
Missions of Dental Education and Organization of Report
The central chapters of this report are organized around the three basic missions of dental education: educating practitioners (Chapter 4), conducting research (Chapter 5), and providing patient care (Chapter 6). This organization reflects both the development of the American university and the emergence of the academic health center as a major part of the university.
The European university historically emphasized two missions—education and scholarship. The twentieth century vision of American universities as centers for scientific and technological progress has led the second mission to be widely relabeled—and in some ways profoundly redefined—as research. Service was incorporated as a third mission as the nation successfully harnessed higher education in the service of economic and social development, most visibly through the system of land-grant institutions initiated in the 1860s. With the post-World War II increase in university-based medical research, private and public health insurance, and demand for sophisticated hospital care, the position of the academic health center and the health professions schools rose relative to the rest of the university. Patient care became a distinct mission, one without a clear equivalent in other professional schools such as law and architecture. Thus, although universities speak
of the missions of education, research, and service, many academic health centers summarize their missions as education, research, and patient care.
By organizing central chapters around the missions of education, research, and patient care, this report highlights the purposes that justify the existence of dental schools. This structure, however, inevitably sharpens distinctions that frequently—and usefully—blur in the operating reality of any given school. The missions of dental schools and academic health centers are clearly intertwined. Patient care is essential in predoctoral and postdoctoral clinical education, and patients also serve as subjects in clinical trials and other research activities. Education itself provides the focus for faculty research on the effectiveness of different instructional strategies. Ideally, both clinical and educational research, in turn, provide findings that help improve patient care and instruction. For many institutions, patient care includes provision of care for the disadvantaged, a crucial community service.
Although this report focuses on education, research, and patient care, it also considers activities more conventionally described as part of the service mission of the university. These include continuing education, support for public health services, and participation in mentoring, tutoring, and other programs for precollegiate minority youths that benefit the community as well as the young people themselves.
To understand dental education today and put current issues in perspective, the committee believed that it needed to understand something of dentistry's past. Chapter 2, therefore, presents a brief review of the evolution of dental practice and dental education. This history underscores issues that dentistry has wrestled with for a very long time such as standard setting, work force size and composition, and scientific foundations.
Chapter 3 examines oral health status and services, suggests basic objectives and directions for oral health, and discusses their implications for dental education. Chapters 7, 8, and 9 examine in more detail how dental education relates to the university, the profession, and the larger society. These chapters consider such controversial topics as dental school closures, educational financing, licensure, accreditation, and size of the dental work force. Several chapters, in particular Chapter 7, discuss leadership challenges and skills. In Chapter 10, the committee reconsiders the challenges facing dental education, presents its views on the strengths and weaknesses of dental education in facing these challenges, and recapitulates its findings and recommendations.
Although the discussion that follows includes many references to the relationship between the dental school and its parent university or academic health center, this overstates reality. Some dental schools are not part of academic health centers, and some are part of academic health center campuses that are not part of a university (although they may be part of a state university system). Some schools are formally part of a university or academic health center but are physically isolated and, in some cases, fairly independent organizationally. For the sake of simplicity and emphasis, this report's discussion of the dental school within the university or academic health center is generally not accompanied by references to the special circumstances just cited.
Summary
The future of dental education is inextricably linked to its contributions to improving the effectiveness and efficiency of oral health services through education, research, and patient care. It must not only contribute but also be perceived as contributing—by society generally, by the dental profession, and by other relevant social institutions, in particular, the university. For dental education to meet the challenges ahead will require the support and involvement of the practitioner community as well as researchers and policymakers. The intent of this report is to provide guidance for each of these important groups.
APPENDIX 1.A Information Collection Activities of the Committee on the Future of Dental Education
Dental School Visits
11 schools—May to November 1993
6 states—California, District of Columbia, Illinois, New York, North Carolina, Texas
>600 participants—students, faculty, administrators, alumni, dental society leaders
Liaison Panels
Regional practitioner-leader panel, 16 members, met June 1993
Faculty panel, 17 members, met September 1993
Specialty panel, 9 members, met November 1993
Public Hearing and Panels at Committee Meetings
Testimony invited from more than 80 organizations
Oral testimony from 24 organizations, September 1993
Written testimony submitted by 30 additional organizations
Panel on Predicting Supply, Demand, and Need for Dental Personnel and Services (May 1993)
Panel on Financing Dental Education (September 1993)
Leaders of Dental and Allied Dental Organizations (various meetings)
Commissioned Papers, Surveys, Other
Oral health status*
Effectiveness and outcomes for dental care*
Issues in dental curriculum development and change*
Research, technology transfer, and the dental school*
Research frontiers in oral health*
Projecting supply, demand, and need for dental services and practitioners*
Financing dental education*
Licensure and accreditation*
Telephone survey of officials at 12 universities
Mail survey of 54 deans of dental schools
Literature reviews