|
Summary of Findings: Improving Birth Outcomes Within Health Care Systems
|
5
Improving Birth Outcomes Within Health Care Systems
The previous chapters have described a broad range of conditions that contribute to adverse birth outcomes. Most of these conditions can be addressed through affordable interventions that have been proven effective in clinical trials, and in some cases, in population-based studies. In order for these interventions to have the maximum impact on birth outcomes in large populations, however, they must be implemented within an effective health care system. As discussed in Chapters 2 and 3, the key requirements for reducing maternal, fetal, and neonatal mortality are skilled birth attendance and, for complicated deliveries, access to the appropriate level of essential obstetric and neonatal care (World Health Organization, 1999; Li et al., 1996). Building strong reproductive health care capacity both requires and contributes to a strong and equitable system for overall health care (Graham, 2002).
This chapter addresses the overall process of developing and strengthening a health care system. Countries meet their specific needs by tailoring that overall process. The chapter first reviews the evidence base for strengthening health care systems, then addresses primary care and referral by reviewing current models of care for labor and delivery, and considers the limitations in access to these health care services. The next section addresses the building of health care capacity, which involves staff development and training, the role of the private sector, financing, and health care reforms. This is followed by a section on management of health care systems, which includes the roles of surveillance and evaluation. The chapter concludes
with three recommendations and the research needed to develop health care systems that support sustained and future improvements in birth outcomes.
THE EVIDENCE BASE
Evidence concerning the effectiveness of specific interventions to prevent adverse birth outcomes has been reviewed in earlier chapters. This chapter addresses the implementation of these interventions within primary health care systems, a process that has not been evaluated with the same methodological rigor as the effects of the component services or activities. The clinical and cost-effectiveness of interventions within a health care system would ideally be determined through randomized, controlled trials (RCTs), since they provide the most reliable evidence. However, RCTs have not been used extensively in evaluating community interventions (Smith et al., 2000) because of the cost and complexity of very large trials or because denial of services to a control group when they are widely believed to be beneficial may be considered unethical. Because maternal mortality is a relatively rare event, very large populations need to be studied. Such trials are also complex owing to their multiple components and the involvement of several levels of government (Sorensen et al., 1998)
Clearly the evidence base for improving birth outcomes within the health care systems of diverse countries would be strengthened by conducting RCTs of interventions in the systems in question. It is important for future research to meet the challenges imposed by cost and complexity so that policies and programs can be based on a stronger scientific footing. For now, given the current lack of RCTs to evaluate the effectiveness of health care systems, and the urgent need to improve birth outcomes, the committee has examined less rigorous attempts to integrate interventions into health care systems and programs. This chapter therefore focuses on the feasibility of implementing systems and programs of maternal and infant care in different settings, the problems encountered, and the lessons learned. When published evidence on the overall effectiveness of these systems and programs is available, it has been reviewed. Since this evidence often consists of comparisons before and after interventions in the same geographic setting, participants versus nonparticipants in the same setting, or settings that have implemented a program versus those that have not, caution is advised in drawing inferences about the causal effects of the systems or programs of care.
PRIMARY CARE AND REFERRAL
The 1978 International Conference on Primary Health Care produced the Alma-Ata Declaration, a strategy promoting “health for all” that has
been broadly accepted. The main goal of this strategy is to make primary health care—defined as essential health care based on practical, scientifically sound, and socially acceptable methods and technology—accessible to people in every community and affordable to communities and countries at every stage of development. The Alma-Ata Declaration recognizes primary health care as the centerpiece of a country’s health system, and an important component of its overall social and economic development (World Health Organization, 1978).
More recently, “close-to-client” health care has been identified as the principal vehicle for addressing the small number of conditions, including maternal, fetal, and neonatal mortality, that account for much of the excess mortality in developing countries (Jha et al., 2002). In this model of primary care, relatively simple hospitals and health centers deliver effective interventions against major causes of death and disability in poor populations. Care in these settings, which can often be provided by nonphysicians (nurses, midwives, community or village health workers, and other paramedical staff) is complemented by a referral system that provides access when needed to higher-level care (World Health Organization, 1994, 1996a). The goal of referral is to assure that patients receive effective care in an appropriate facility at minimal cost (Murray et al., 2001). Box 5-1 lists the essential features of effective referral systems.
Several interventions recommended in this report, such as those for family planning, preconceptional care, and refocused antenatal care (Villar et al., 2001)—all primary care services—can be offered through community facilities linked to district hospitals. Antenatal care can be provided at a community health clinic. Skilled birth attendants can provide clean and safe deliveries and immediate postpartum care in homes or clinics. Postnatal
|
BOX 5-1
SOURCE: Murray et al., 2001. |
care for the infant can be provided by a midwife, nurse, or possibly a village health worker (Bang et al., 1999) (see Box 3-2). Trials are needed to test this approach in other settings and determine whether a similar approach can be effective for maternal postnatal care. Local services can easily be tailored to meet community needs and local participation in decisions on the delivery of health services increases the use of services, improves patient satisfaction and knowledge, and strengthens health care capacity.
Since the risks for adverse birth outcomes are so high at the time of labor and delivery and the immediate postpartum period, the quality of care at that time becomes the major focus. Reducing the significant burden of maternal, fetal, and neonatal mortality will require good-quality maternal and neonatal services along with effective referral systems (Jha et al., 2002; Murray et al., 2001; Ross et al., 2001; Kusiako et al., 2000; Fauveau et al., 1990). This can be accomplished in this “close to client” model by providing a skilled birth attendant—a midwife, doctor, or nurse—who can manage normal deliveries, recognize complications early, and promptly refer patients to the level of care needed. For complicated deliveries, referral to a basic or comprehensive essential obstetric care facility is critical. Patients who need care for complicated deliveries require a caregiver with a higher level of skill and a facility with the necessary equipment, drugs, and other materials. An enabling environment for labor and delivery includes specialized equipment, reliable supplies of drugs and other materials, and efficient transportation from the home or health facility to the referral facility (Ross et al., 2001; Graham et al., 2001). To be sustainable over time, it also requires ongoing staff development and training, adequate financing, supportive policies, and strong leadership.
Models of Care for Labor and Delivery
The essence of primary care and referral for labor and delivery is the presence of a skilled attendant backed up by good-quality, readily accessible emergency care. The wide range in services and settings in countries for labor and delivery can be described in terms of four models of care, based on the type of caregiver and the setting in which delivery takes place (Table 5-1) (Koblinsky et al., 1999). Each model is presented below along with examples of country programs. The models do not include one for home birth with a nonprofessional attendant and without referral for complicated cases. While this is the reality for many poor, rural populations, it is inevitably associated with high maternal, fetal, and neonatal mortality and is, therefore, in urgent need of being upgraded.
TABLE 5-1 Models of Health Care During Labor and Delivery
|
Model of Health Care |
Birth Attendant |
Location of Delivery |
Referral Capacity |
Country examples, each with its with Maternal Mortality Ratio (per 100,000) |
|
1 |
Nonprofessional: often a community member with little or no medical training |
Home |
Referral and transport needed for complicated cases |
Rural China (1994): 115 Fortaleza, Brazil (1984): 120 |
|
Many barriers and may involve long distances |
||||
|
2 |
Professional: often a midwife who can recognize complications and provide basic essential care |
Home |
Referral and transport needed for complicated cases |
Malaysia (1970s-1980s): 50 Netherlands (1983-1992): 7 |
|
Some barriers may involve long distances |
||||
|
3 |
Professional: often a physician, alternatively, a midwife |
Health clinic or hospital with basic essential care |
Referral and transport needed for complicated cases |
Malaysia (1980s-1990s): 43 Sri Lanka (1996): 30 |
|
4 |
Professional: most often a physician |
Hospital with comprehensive essential care |
No referral needed |
United Kingdom: 9 United States: 12 Mexico City (1988): 114 |
|
SOURCE: Adapted from Koblinsky et al., 1999. |
||||
Model 1: Home birth with nonprofessional attendant and referral for complicated cases
In countries with high rates of maternal and neonatal mortality, traditional birth attendants (TBAs) and relatives are the most common providers of care for mothers and infants during labor and delivery, especially in rural areas (Schaider et al., 1999; Itina, 1997; Eades et al., 1993). TBAs are typically older women who lack formal education, but are accorded social status in their communities due to their years of assisting women during childbirth (Eades et al., 1993; Itina, 1997; Abioye-Kuteyi EA et al., 2001). To begin to address the need in developing countries for skilled assistance during labor, delivery, and the postpartum period, several field projects have attempted to train TBAs in critical skills (Daga et al., 1997; Kwast, 1996; Miller et al., 1995; O’Rourke, 1995; Pratinidhi et al., 1986; Schaider et al., 1999; Smith et al., 2000). Some TBAs have learned to recognize complications and refer patients to medical facilities (Janowitz et al., 1985; Bailey et al., 2002); however, the training of TBAs has not been associated with reduced maternal and neonatal mortality rates (Jaffre and Prual, 1994; DeBrouwere et al., 1998; Graham, 2002; Smith et al., 2000).
China, in one of the rare successful large-scale scenarios for Model 1 care, achieved dramatic reductions in maternal and infant mortality in the 1960s to 1980s (see Box 5-2). Over this time, most births in rural China were attended by relatives or lay persons with some training (Goldstein, 1998; Hesketh and Zhu, 1997; Young, 1990). However, the Chinese experience stands as an exception to the generally high frequency of deaths during labor, delivery, and the first 24 hours postpartum that occur in Model 1 settings.
Model 2: Home birth with professional attendant and referral for complicated cases
Delivery at home and care of the newborn, usually by a midwife, is available in some developing countries, generally in rural areas (see Appendix C for a detailed definition of “skilled birth attendant”). In countries where skilled birth attendants manage at least half of all deliveries, such as Sri Lanka and South Africa, maternal and neonatal mortality rates are among the lowest in the developing world (see Figures 2-5 and 2-6).
Providing quality Model 2 care involves the training of competent birth attendants and provision of equipment. It also involves transportation and communication capacity for referrals. Provider and community attitudes that can be major barriers to the use of skilled birth attendants and other health care services need to be overcome (Mathur et al., 1979; The Prevention of Maternal Mortality Network, 1992). Whereas TBAs work in vil-
|
BOX 5-2 In 1949, the government of the newly founded People’s Republic of China launched a massive campaign to provide basic health care to all citizens, and particularly to its underserved rural population (Goldstein, 1998; Hesketh and Zhu, 1997; Young, 1990). As part of this effort, programs were developed to educate traditional birth attendants, midwives, and obstetric nurses in “modern birth methods,” and millions of village health workers known as “barefoot doctors” were trained. All of these health care providers were connected through a three-tiered referral system. Rural birth attendants were linked to township health centers and to county maternal and child health institutes or county hospitals; these in turn were linked to specialized municipal, provincial, and national maternal and child health services and research facilities. Over the next 30 years, the campaign was able to overturn centuries of tradition regarding birthing practices and sharply reduced both maternal and neonatal mortality rates. Maternal mortality fell from approximately 1,500 per 100,000 live births in 1950 to 61 per 100,000 in 1995. A strong family planning program, introduced in the early 1970s (abortion had been legal since 1957), appears to account for nearly two-thirds of the decline in maternal mortality (Koblinsky et al.,1999). Social campaigns such as those for late marriage and women’s literacy were also associated with mortality reductions for both women and children. Since about 1980, however, maternal and neonatal mortality rates in China have shown little improvement, and wide disparities continue in both the availability of care and in mortality rates between rural and urban areas. In the mid-1980s, for example, the maternal mortality rate in Shanghai was 18 per 100,000 births, compared with 108 per 100,000 in the central province of Ningxia (Young, 1990). Moreover, the proportions of beds and of physicians remain heavily weighted toward urban areas. This rural/urban disparity can be traced to the 1978 economic reforms, which caused a virtual collapse of the cooperative insurance scheme inaugurated in the villages at the start of the revolution (Young, 1990). As a result, the demand for and availability of primary health care has declined in rural areas. Some of China’s strategies to improve birth outcomes may be applicable in other countries. The national effort to reduce maternal and infant mortality had strong political guidance. The priorities of health care reform were determined by the need and potential impact, and strategies to achieve reform goals were adaptable to local needs. Access to skilled delivery and obstetric care at the time of complications was guaranteed through a referral network that reached into communities. These efforts were complemented by social campaigns that emphasized prevention and good health care practices. |
lages where they are known and respected, professional care providers begin their work as strangers to a village. Partnerships with TBAs can facilitate the transition of a new midwife, who will need to show understanding and respect for local birth traditions that are not harmful (Koblinsky et al., 1999; Sibley et al., 2002).
In some developing countries, birthing homes—places in the community where women can go to give birth with a skilled attendant—have been accepted as an alternative to deliveries at home or in a referral facility. Often built by community members, these homes are likely to attract skilled birth attendants by providing a central location for deliveries (Koblinsky et al., 2000). The homes can also foster partnerships between skilled birth attendants and TBAs or community health workers. In Honduras, the use of birthing homes has increased as they are relatively inexpensive and reduce overcrowding in referral hospitals (Danel and Rivera, 2002).
Model 3: Hospital/clinic birth with basic essential care
Deliveries attended by skilled, experienced birth attendants can be further supported when they take place in hospitals or clinics that provide basic essential obstetric and neonatal care. Model 3 services for the mother should include at least parenteral medications (antibiotics, oxytocic drugs, and anticonvulsants) and manual removal of the placenta and other retained products in basic essential obstetric care services. However, in comprehensive essential obstetric care services, provision for surgical procedures, anesthesia, and blood transfusion in addition to the above should be included (World Health Organization, 1996c). Model 3 services for the newborn include cardiopulmonary resuscitation (bag and mask ventilation, endotracheal intubation, cardiac massage), thermal management (using radiant warmers and incubations), supplemental oxygen, parenteral medications (e.g. antibiotics), nutrition management (use of feeding tubes), and fluid managment (Hesketh et al., 1994). Model 3 facilities are typically staffed by physicians, nurses, and midwives. Determining the availability of Model 3 care is difficult because documentation of coverage by health care facilities does not distinguish between basic (Model 3) and comprehensive (Model 4) care.
Increased access to hospital delivery and literate female populations has been associated with reduced maternal mortality in Sri Lanka (Gunaserera and Wijesinghe, 1996) and reduced neonatal mortality in Shunyi County, China (Yan et al., 1989). Similarly, there was a reduction in maternal and neonatal mortality in Malaysia (see Box 5-3). Where there is a demand for hospital delivery, maternity waiting homes—residences near hospitals where women who live far from the facility can stay near the time of delivery—can increase access for rural women (Koblinsky et al., 1999). Unlike birthing homes, maternal waiting homes are not used for deliveries. However, use of these facilities has been limited by their expense and the need for childcare when the mother is away from home (Fawcus et al., 1996). Their value in reducing maternal mortality has not been clearly established (Chandramohan et al., 1994).
|
BOX 5-3 When Malaysia became independent in 1957, the maternal mortality rate was 320 per 100,000 and the reported neonatal mortality rate was 75.5 per 1,000 births (Pathmanathan and Dhairiam, 1990). Free health services were made available to rural populations. Professional midwives and nurses were trained and assigned to villages, where they were supported by an expanding network of local health units (one for every 50,000 people) linked to regional clinics and, by referral, to district hospitals (Koblinsky et al., 1999). Between the mid-1970s and mid-1980s, most births still took place at home, but were attended by a professional midwife (Koblinsky et al., 1999). During this period, the maternal mortality rate dropped to 50 per 100,000. Midwives in Malaysia are salaried civil servants who provide maternal health care including home visits in the prenatal and postpartum periods, normal deliveries, risk screening, referrals with transport to a maternity home or hospital, family planning, and child health services (Koblinsky et al., 1999). They can administer certain drugs, including oxytocin, but rely on a nurse to provide antibiotics, sutures, or intravenous fluids. Midwives use checklists to recognize the signs and symptoms of complications and make timely referrals. In the mid-1990s, the formal training course of study for midwives was expanded to a two-and-a-half year program for high school graduates with hands-on learning in hospital and community settings. As the presence of and demand for professional midwives increased, the role of TBAs in Malaysia gradually moved from birth assistant to provider of family support (Koblinsky et al., 1999). This transition was encouraged by government initiatives to limit their role in labor and delivery, while training, registering, and supervising their provision of traditional massage and postpartum care. By 1996, 95 percent of all home births were assisted by midwives and less than 1 percent by TBAs (National Population and Family Development Board/Ministry of Health, 1998). Although Malaysia had achieved relatively low levels of maternal and neonatal mortality through home deliveries with a skilled midwife, the coverage of births was uneven. A survey at the end of the 1970s revealed many areas of underserved mothers, inadequate communication between rural maternal and child health services and obstetric and pediatric services, and too many inadequately attended high-risk pregnancies (Pathmanathan and Dhairiam, 1990). Concerned by these findings, the Malaysian government encouraged women to give birth in facilities providing basic essential obstetric care (includes all essential obstetric functions except surgery, anesthesia, and blood transfusion). The transition from home birthing to hospital birthing moved relatively rapidly, and by 1998, more than 90 percent of women with high-risk pregnancies, and 80 percent assigned moderate risk, delivered in a hospital. Deliveries by skilled personnel had risen from 51 percent in 1980 to 95 percent in 1996. By 1996, the maternal mortality rate had declined to 43, the perinatal mortality rate was 11, and neonatal mortality rate was 7 (National Population and Family Development Board/Ministry of Health, 1998). The goal of moving from home birthing to facility-based birthing was achieved in Malaysia by convincing women and their families that it is safer to deliver with skilled providers in a facility with backup support (Koblinsky et al., 1999). To further promote this goal, services and transport were provided at no cost for families, and significant improvements in the quality of hospital care were accomplished through quality assurance efforts. |
The transition from Model 2 to Model 3 care, which includes all obstetric services except surgery, anesthesia, and blood transfusion, is generally smoother than the transition from Model 1 to Model 2. In Malaysia, the transition from Model 1 to Model 3 began by evaluating the medical risks for all pregnant women rather than only those at high risk for complications. As a result, health care providers and families became increasingly concerned with safety measures that improve childbirth outcomes. Even women at low risk began to choose a hospital birth (see Box 5-3). Several countries now provide health education for pregnant women that emphasizes safety concerns during labor, delivery, and the postpartum period as well as during antenatal care (Yan et al., 1989).
Model 4: Hospital/clinic birth with comprehensive essential care
Model 4 care incorporates all of the services provided in Model 3, and also anesthesia, surgery (particularly cesarean section and repair of maternal birth injuries, such as vesico-vaginal tears), blood transfusion, and the ability to care for the sick or at-risk neonate. This most sophisticated model of care is available in some urban areas in developing countries and is the usual level of care in developed countries, where maternal and neonatal mortality rates are low. Use of Model 4 facilities is cost-effective for deliveries with complications requiring that level of care, but not for normal deliveries. Delivery in Model 4 facilities in developing countries does not necessarily guarantee low mortality (Koblinsky et al., 1999). The quality of care can be impaired by overuse of the facility, poor clinical judgment, use of inappropriate procedures, inadequate supplies, and poor attitudes on the part of providers toward patients (Bobadilla et al., 1996; Mbaruku and Bergstrom, 1995; Okonofua et al., 1992; Figueroa et al., 1989).
Which model is appropriate?
Determining the best model of labor and delivery care for a particular country or region, and the most effective and efficient steps to reach it, require future research (Graham et al., 2001). Each model, even Model 4, can be recommended only after establishing its clinical- and cost-effectiveness, feasibility, and family/patient acceptance in specific settings. Furthermore, countries must have the resources to successfully implement the changes needed. Variations on Models 2 and 3 care, as described above, are likely to be the most cost-effective facilities for uncomplicated deliveries in low resource settings. Basic and comprehensive EOC are clearly needed for complicated deliveries.
Recognition of pregnancy complications and their management is cen-
tral to reducing maternal, fetal, and neonatal deaths, yet success in doing so when most women deliver at home not attended by a professional attendant remains a challenge. Scarce health resources should therefore be managed with the primary goal of achieving skilled delivery at all births (i.e., Model 2 or 3). This can be accomplished by creating partnerships between midwives, with their medical skills, (and village health workers [VHWs] or) TBAs, with their knowledge of and access to individual patients, the community, and local birthing traditions. Where resources permit, identification of a specific target, such as the underserved, for improved quality of care and efficiency of referral can facilitate the transition from Model 2 to Model 3 care. Key needs can be identified and met using population-based surveys (Pathmanathan and Dhairiam, 1990), standard risk analysis (Yan et al., 1989), or death audits (Wilkinson, 1997).
In well-functioning health care systems, normal births are supported but not overmedicalized, limiting costs and reducing the risk of iatrogenic complications, while complicated births receive prompt, appropriate treatment (Jahn and De Brouwere, 2001). In Jamaica and Sri Lanka, developing countries in which physicians attend about 15 percent of deliveries—the approximate percentage of all births that involve potentially life-threatening complications (World Health Organization, 1994)—maternal mortality has been considerably reduced (Graham et al., 2001). In Chile, midwives and physicians typically work together to provide a high level of institution-based maternal and neonatal care (Segovia, 1998). Midwives attend 70 percent of all deliveries in that country; physicians handle the remainder. These take place in Model 3 or 4 facilities which also provide the vast majority of antenatal care. However, any country can develop a mix of models to suit local needs such as urban or rural. In places where women equate safe delivery with delivery in a facility, they may prefer a hospital that provides comprehensive care or a birthing facility affiliated with a referral hospital. Because of the higher cost of Model 4 deliveries, policy makers can decide where to provide quality Model 3 care for normal deliveries with links to referral services for pregnancies with complications that require Model 4 care (Koblinsky et al., 1999).
Self-referral for delivery care far outstrips emergency referrals in many hospitals in developing countries (Murray et al., 2001; Jahn and De Brouwere, 2001). Frequent self-referral for delivery without specific medical reason indicates that many women bypass community-level services, while the small percentage of emergency referrals indicates that many complicated births do not receive adequate care (Jahn and De Brouwere, 2001). Where resources are limited, maximum cost-effectiveness will be obtained when the majority of deliveries performed at higher-level facilities are complicated births. This requires strengthening the referral system, as described in the next section.
Improving Access to Referral Care for Labor and Delivery
Reducing maternal, fetal, and neonatal mortality requires broad access to the essential obstetric and neonatal services described in Chapters 2 and 3. The availability and quality of these services is inadequate in most countries. Also needed are referral structures to address major barriers to provision of referral care. The “four delays” in responding to maternal or neonatal complications were introduced in Chapter 2 (Lawn et al., 2001). These delays—in recognizing the problem; deciding to seek care; getting to a facility that can provide it; and receiving appropriate treatment—confront every medical emergency. Several determinants of the use of referral care may need to be addressed to increase referrals for complicated births, such as the ability of pregnant women and their families to recognize symptoms of complications (The Prevention of Maternal Mortality Network, 1992; Bloom et al., 1999); distance to the referral facility (The Prevention of Maternal Mortality Network, 1992) (see Figure 5-1), the availability and cost of transportation (Eades et al., 1993; Fraser and Meli, 1990; Fawcus et al., 1996; The Prevention of Maternal Mortality Network, 1992) and the cost of care (Bloom et al., 1999; Asowa-Omorodion, 1997).
Many women do not recognize the benefits of receiving higher-level care, are wary of the attitude of providers toward patients, and do not understand the medical causes of complications or the importance of specific treatments (Mathur et al., 1979; The Prevention of Maternal Mortality Network, 1992; Thaddeus and Maine, 1994; National Research Council, 1997). The signs of complications during pregnancy and labor and after delivery are not always recognized by women and their families as causes for concern. Recognizing complications and promptly seeking skilled care can be taught during antenatal care. Geographical and financial accessibility also present major barriers to referral care (Thaddeus and Maine, 1994; Bouillin et al., 1994; Haddad and Fournier, 1995). When deciding whether to seek referral care in an emergency, patients and their families tend to weigh the potential expense and effort involved against the perceived benefit of hospital care (Thaddeus and Maine, 1994; Oosterbaan and da Costa, 1995; Asowa-Omorodion, 1997). These decisions are often influenced by fears of discrimination, loss of privacy, and the lack of emotional and social support in a hospital setting.
Where access to referral care is less a problem than the quality of care available, improving provider skills and the availability of drugs and other medical supplies may increase the number of emergency referrals (Jahn and De Brouwere, 2001). However, in the more common situation, where skilled attendants are likely to remain scarce for the foreseeable future, improving referral mechanisms, communication capability, and transportation, so that those who need emergency care receive it, is an alternative means to reduc-
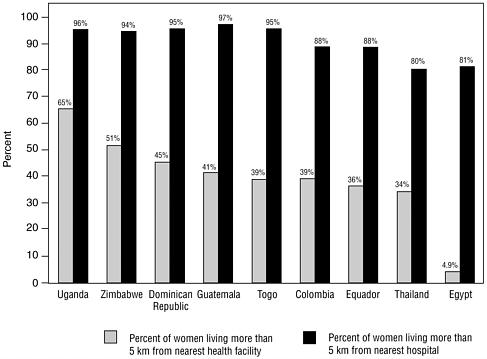
FIGURE 5-1 Percentage of rural women living more than 5 kilometers from a health facility or hospital in selected developing countries, 1990-1996.
SOURCE: World Health Organization, 1998.
ing maternal, fetal, and neonatal mortality (Graham et al., 2001). Community efforts toward this goal can be especially effective. These include coordination of communication with referral facilities, provision of transport, provision of emergency loans to cover transportation and treatment costs, and advocacy by community health staff to ensure that women and their families understand the potentially life-saving benefits of referral for complications (Jahn and De Brouwere, 2001).
In rural areas, providing transport to referral facilities for patients has been found cost-effective (Shehu et al., 1997). Emergency transportation has been organized in Nigeria through local car owners (Olaniran et al., 1997), in Mali with radio calls and ambulances (Maiga et al., 1999), and in Kenya with a hospital emergency vehicle and radio contact with several health centers (Macintyre and Hotchkiss, 1999). Transportation is needed for skilled birth attendants to deliver care to isolated populations. Loans for obstetric emergencies have been financed and managed by communities in Nigeria (Essien et al., 1997; Olaniran et al., 1997; Chiwuzie et al., 1997),
and Mali (De Brouwere 1997; Maiga et al., 1999), but whether these loans improve birth outcomes has yet to be established. For example, communities in Ethiopia (Poovan et al., 1990) and Zimbabwe (Chandramohan et al., 1994) have developed maternity waiting homes with easy access to the local hospital for women living in remote areas. Communities in Honduras (Danel and Rivera, 2002) and Guatemala (Bocaletti et al., 2000) have developed birthing centers where women can give birth with a skilled provider. These centers have been able to attract skilled birth attendants to communities and introduce them to local culture and birthing practices.
Guidelines for referral can reflect local epidemiological conditions, health service capacity, and community preferences (Jahn and De Brouwere, 2001). Initially it may be advantageous to focus on emergency referral for life-threatening maternal complications (Jahn and De Brouwere, 2001) such as prolonged or obstructed labor, hypertensive disease of pregnancy, antepartum hemorrhage, and neonatal sepsis. Once established, these procedures provide the foundation for effective referral for other emergency care needs and can lead, through the improved overall functioning of health care systems, to further improvement in birth outcomes (Ronsmans et al., 1997; Campbell, 2001; Jahn and De Brouwere, 2001).
BUILDING CAPACITY FOR REPRODUCTIVE HEALTH CARE
Access to quality reproductive health services is key to improving birth outcomes (Pittrof et al., 2002). In developing countries, this involves building health care capacity in the form of facilities, equipment, supplies, and—most important—personnel. An acute shortage of physicians, midwives, and nurses throughout much of the developing world is exacerbated by their unequal distribution. The vast majority of these professionals and nearly all obstetricians, pediatricians, and other specialists practice in urban areas (Kowalewski and Jahn, 2001). Midwives are more likely to work in rural settings, but their numbers are too small to fill the gap in care; according to a 1990 estimate, developing countries average about one midwife per 30,000-300,000 people (Kwast, 1991). Thus this section first describes several approaches to increasing the numbers of skilled assistants in public health services, the quality of care they provide, and their association with improved birth outcomes. These efforts can be further advanced through collaboration with private care providers, NGOs and other not-for-profit organizations, and professional organizations of health care providers.
An obvious barrier to achieving greater coverage for the most effective health interventions, including those that would reduce maternal and neonatal mortality, is the low level of total health expenditure in developing countries. With the average annual per capita health care expenditure in low-income countries at US$26 in 2002—and only half that amount in the
48 poorest countries—additional funds are clearly necessary to improve birth outcomes and health care worldwide (Jha et al., 2002). The third part of this section, on the financing of reproductive health services in developing countries, identifies potential sources of funding to begin to address this shortfall. The final part of this section discusses health system decentralization and sector-wide approaches to reproductive health. These reforms have been adopted by several countries in an effort to improve access to good quality health care.
Staff Development and Training
Several factors contribute to the lack of general physicians and specialists in most developing countries, including limited resources for health care, the inadequate capacity of medical schools, and the loss of physicians to opportunities abroad. The emigration of physicians can be stemmed by creating a more attractive career path with faster advancements, publicly acknowledging medical and other accomplishments, and providing more competitive salaries. Where the distribution of physicians is the major problem, strong national leadership is needed to establish rural coverage as a priority and provide incentives to physicians to work in rural areas before settling in cities. For example, physicians who agree to serve in rural areas might be forgiven the cost of their training; however, such agreements must be rigorously enforced to be effective (Kowalewski and Jahn, 2001). The need for specialized care in some underserved areas has been filled by general practitioners who have acquired the skills needed for operations such as cesarean delivery.
In order to increase the effectiveness of physicians, nurses and other health assistants can assume certain additional tasks under the supervision of a physician. In countries where it is permitted, nonphysician medical assistants have received further training to enable them to perform emergency surgery and administer anesthesia. In Burkina Faso, Malawi, Mozambique, Tanzania, and Zaire, nonphysician staff are trained to perform surgery and obstetric care in district hospitals or health centers where physicians are not available (Kowalewski and Jahn, 2001; Rosenfield, 1992; Adeloye, 1993; da Luz Vaz and Bergström, 1992; Pereira et al., 1996; Duale, 1992). In addition to increasing the coverage for emergency services, competent nonphysicians incur lower salary and training costs than do doctors, and some evidence suggests that they communicate more effectively with patients (World Bank, 1993). Follow-up costs must also be considered, however, as nonphysicians who provide specialized services may require a high level of supervision (Hopkins et al., 1996; Loutfi et al., 1995).
Skilled birth attendants—whether midwives, physicians, or nurses—
require ongoing training. Programs of instruction for skilled caregivers can be built on evidence-based, nationally approved standards, such as the skill base outlined in Appendix C, Essential Skills Required for Birth Attendants. While midwives need instruction in clean and safe delivery, field reports from Guatemala and Bolivia indicate that many physicians and nurses have not been sufficiently trained in partograph use, breech delivery, newborn resuscitation, and the control of postpartum hemorrhage (Koblinsky et al., 2000). A sound knowledge of procedures for a clean and safe delivery serves as a foundation for training in the treatment of complications. Expertise is gained through hands-on experience and maintained through caseload requirements, on-going training, and evaluation (McDermott et al., 2001; see Appendix C). The performance of skilled birth attendants should be monitored for the purpose of improving health care systems, as well as to ensure individual accountability (Gunathunga and Fernando, 2000).
Regular emergency drills or simulations can help health workers maintain a state of readiness to deal with emergencies. Courses in life-saving skills for midwives have been successful in addressing these needs, and could also be offered to nurses, clinical assistants, and general physicians. Several studies indicate that nonspecialists can be taught to perform life-saving obstetric techniques effectively (da Luz Vaz and Bergstrom, 1992).
Providing universal care during childbirth by training TBAs has not been shown to be effective. After receiving training in clean delivery practices and the recognition of complications, TBAs in the Gambia were initially found to have had a positive effect on maternal health, yet three years later, the maternal mortality ratio remained near 700 per 100,000 births (Greenwood et al., 1990). Training of TBAs—once thought to be an affordable way to reduce mortality during childbirth—is no longer considered an effective investment of limited funding resources.
Patterns of care for women during pregnancy and childbirth in most developing countries, particularly in rural communities, are strongly influenced by cultural and traditional factors. In settings where TBAs are responsible for childbirth, few women receive antenatal care (Nylander and Adekunle, 1990). When obstetric problems arise, sociocultural factors (such as women’s social status and the use of traditional healing practices) frequently pose barriers to their seeking medical treatment (The Prevention of Maternal Mortality Network, 1992; Okolocha et al., 1998).
The Role of the Private Sector
Another strategy for increasing access to quality reproductive health care is the creation of alliances between governmental public health agencies and individuals or organizations that provide health services (World
Bank, 1993; United Nations Fund for Population Activities, 1999). Key players in the private sector include physicians and other providers of care for profit, as well as not-for-profit groups such as NGOs, universities and research institutions, charities and welfare organizations, and associations of health care professionals.
Private providers deliver a significant and growing share of health services (Hanson and Berman, 1998). According to a recent survey of 40 developing countries, more than half of all physicians were privately employed, and nearly one-third of all beds were in private institutions or reserved for private patients (Hanson and Berman, 1998). Where women have a choice of public or private health care providers, many seek private care due to its greater accessibility and convenience. Private clinics and practices may be open longer hours, have shorter waiting times, and (in some urban areas) be more accessible than public facilities (Ferrinho et al., 2001; Wyss et al., 1996). In many developing countries, labor and delivery services for significant numbers of births are provided by midwives in private practice (Gani, 1997; Schwartz et al., 1993).
In the rural areas of many African and other nations, NGOs and other private not-for-profit agencies are the main, if not the only, providers of health care. These providers vary widely in their missions and services, but often support government policies and programs (Ferrinho et al., 2001). In some areas, NGOs play a key role in administering family planning services and have significantly increased contraceptive uptake (Phillips et al., 1999). Organizations of health care professionals also contribute to the improvement of reproductive health care in developing countries. For example, the American College of Nurse Midwives has supported programs in South Kalimantan, Indonesia, to train midwives in safe delivery practices and the management of complications (McDermott et al., 2001). Groups such as the International Clinical Epidemiology Network (INCLEN) are well positioned to collaborate on the establishment or expansion of surveillance and evaluation of birth outcomes.
Government alliances with private health care providers—whether for-profit or not-for-profit—best serve the public interest when private providers offer a full range of priority services (e.g. antenatal care, skilled attendance at delivery, and early neonatal and maternal postpartum care), ensure access for all who need care, and are held accountable for the quality of the care they provide (Ferrinho et al., 2001). Few such alliances have been created (DFID Health Systems Resource Center, 2000), and only limited evidence suggests that that they improve health services in general and maternal and neonatal services in particular. In rural areas, there may not be enough providers to create a competitive market, and even if there are, evidence indicates that competition alone does not guarantee efficient services. In such settings, public-private alliances may need to be established
through long-term contracts with private health care providers (Palmer 2000).
Financing
Expenditures for reproductive health care in developing countries were projected to reach US$17 billion in 2000 and climb to nearly US$22 billion by 2015 (Borghi, 2001). The mechanisms for financing health care are unclear in many cases, particularly at the national level. Information on health care expenditures in developing countries is often incomplete, of questionable quality, or not internationally comparable. Further, it is often difficult to identify reproductive health expenditures because funds are allocated to broad health care categories such as maternal and child health and family planning (Borghi, 2001).
Governments raise funds to finance health care in a variety of ways. In Sri Lanka, public health care is funded largely through general taxation, with the private sector contributing almost half of the cost of primary care services (Hsaio, 2000). In Egypt a compulsory wage-based social insurance scheme is supplemented with additional government revenues (Borghi, 2001). The Bolivian government disburses funds to municipalities in a decentralized scheme; the municipalities, in turn, control reimbursement of health care providers and capital investment (Borghi, 2001).
Donors that fund reproductive health care in developing countries include international organizations, NGOs, governmental aid agencies, and private foundations. International organizations that fund reproductive health programs include WHO (the lead agency for technical health support), the United Nations Development Fund (through its support for poverty reduction programs), the United Nations Children’s Fund, and the United Nations Population Fund. The World Bank, the largest provider of international financial assistance for health care, has worked with governments on programs, financing, and strategies to support reproductive health. Bilateral agencies such as the Swedish International Development Authority and the U.S. Agency for International Development also finance reproductive health care. Projects with direct and indirect effects on maternal health—including family planning, primary health care, nutrition, training, and disease control—represent about 12 percent of bilateral financing. Several private foundations support reproductive health programs; in recent years, the Bill and Melinda Gates Foundation has provided significant funding for maternal and child health. In many developing countries, private voluntary organizations (PVOs) such as CARE and Save the Children support health care programs as part of broader development agendas. These programs are often directed toward low-income, rural populations.
Community-level programs in several developing countries provide
funding for reproductive health services through up-front charges for specific services (i.e., prepayment for delivery services in regular installments throughout antenatal care) or loans for referral services (Borghi, 2001; Fox-Rushby and Ford, 1996). Where they are affordable and result in improved care, user fees tend not to reduce the use of health services; however, fees for labor and delivery services do appear to discourage hospital deliveries (Stanton and Clemens, 1989; Hotchkiss, 1998). Where user fees are designed primarily to recover costs, the practice is likely to exacerbate inequities in care and inhibit the use of essential, and in some cases life-saving, services (Russell and Gilson, 1997). Some African communities offer loans for hospital transportation, treatment, and drugs and supplies required for emergency care during pregnancy. Access to these loans, which must be repaid as soon as possible, has increased referrals (Fofana et al., 1997). The effect on birth outcomes has yet to be established.
Health Care Reforms
Sustaining affordable improvements in birth outcomes depends upon improving the functioning of health systems as a whole (Goodburn and Campbell, 2001). Since the 1980s, many developing countries have undertaken health reforms in an effort to improve the accessibility, equity, quality, and efficiency of services. Key reform strategies that have been applied to reproductive health services in developing countries include the decentralization of health care management and sector-wide approaches to coordinate national and donor resources (McDonagh and Goodburn, 2001).
Through decentralization, resources and responsibilities are progressively transferred from the central government to local and provincial governments in order to give local managers greater responsibility and flexibility in meeting health needs. This process is more successful when the transfer of responsibility occurs in parallel with the development of local capacities (Langer et al., 2000; Hardee and Smith, 2000). A major objective of decentralized health systems is to encourage community participation in and responsibility for health services (Ramiro et al., 2001). Decentralization can lead to improvements in maternal and neonatal services. In Senegal, Zambia, and elsewhere, decentralization has improved delivery of general reproductive health services, but not those for more sensitive areas such as abortion, adolescent care, and HIV/AIDS prevention (Wilson, 2000; Population Council, 1998).
Sector-wide approaches focus on all components of health services, including maternal and neonatal health. They allow national health departments to coordinate national and donor resources and include donors as partners in developing a unified, equitable system of quality health services. Traditionally, donors have invested in separate, uncoordinated health ac-
tivities in different geographical regions, often attracting key staff from government health services and producing services of uneven quality and coverage (Foster et al., 2000a, 2000b; Johanson, 2000; World Health Organization, 1999). The essential services generally include immunization, pre- and post-natal care, oral rehydration, treatment for malaria and lower respiratory tract infections, and family planning. They may include clean and safe delivery, but comprehensive essential obstetric care, which requires a surgeon or other skilled assistant, is rarely covered. Donor agencies can also encourage governments to implement reforms on a realistic timetable, to monitor health and service outcomes, and to continue to identify and incorporate improvements in quality of and access to health services (Cassels and Janovsky, 1998; Johanson, 2000).
Maternal health has been ranked as a high priority for nationally coordinated services (World Bank, 1999; Jha et al., 2001). However, until this strategy is widely implemented, the effects of sector-wide approaches on the quality of maternal and neonatal health services and outcomes are unknown (Johanson, 2000; McDonagh and Goodburn, 2001). Some key activities (such as the training of midwives with the goal of increasing skilled attendance at childbirth) might not be covered by broad funding approaches, and will therefore require focused technical and financial support (Goodburn and Campbell, 2001).
MANAGING HEALTH CARE SYSTEMS
To improve birth outcomes in developing countries, health care leaders must identify the interventions, programs, and strategies likely to have the greatest impact on maternal, fetal, and neonatal mortality. They must then allocate the resources needed to achieve a successful result. An effective process for making such decisions involves the following steps: defining and prioritizing health problems, assessing the performance of current health services, selecting the best intervention, implementing it, and assessing its impact (Lawn et al., 2001). Health care leaders and providers and the community they serve must all participate in this process if it is to be successful.
The definition of key health problems is itself a process, which begins with the collection and analysis of data on health outcomes (in this case, adverse birth outcomes such as maternal, neonatal, or fetal mortality) in the community and comparison with standard populations. Key health problems revealed in this way are further defined in terms of the gaps in services they represent. Both criteria—the magnitude of the problem and the local availability of solutions—are weighed in the setting of priorities among health problems.
To assess the performance of current health services in addressing a priority problem (as defined by an adverse birth outcome), it must be deter-
mined whether the most effective services are provided, whether services reach the vast majority of the population, and whether the services are of good quality. Community input, in addition to that of health leaders and health care providers, is critical to obtaining an accurate assessment, and one that reveals opportunities for interventions to reduce adverse birth outcomes.
Selecting the best intervention to address a problem requires a strong evidence base that confirms the importance of the chosen problem in the local population. The promise of each potential intervention is assessed by examining evidence for its clinical-effectiveness, cost-effectiveness, feasibility and sustainability, and acceptability to the local community. In addition to the new interventions being considered, current interventions and the effect of no intervention should be assessed. Involving local leaders early in the assessment process helps ensure that a needed, wanted, and successful intervention is implemented.
The successful implementation of a chosen intervention requires a clear vision of the desired outcome and recognizes the need for community involvement and investment in the project. Plans for implementation must answer many specific questions. How will the intervention be introduced? Who will provide the services, and at what cost? How will the community be involved in making the intervention successful? These and other needs should be anticipated in the planning process. After implementation, health care providers must consider two questions. First, is the chosen intervention the best way to address the problem? Second, is the intervention being effectively carried out? That is, are the services of good quality and are they reaching most of the population? The answers to these questions can be determined through the surveillance of birth outcomes and evaluation of their change as a result of the intervention.
Experience in industrialized countries suggests that interventions must be tailored to local conditions and that continual monitoring and response is key to maximizing cost-effectiveness (Sorensen et al., 1998). Such fine-tuning of interventions and health care programs is achieved by repeating the steps in the decision-making process to solve increasingly well-defined problems. Surveillance of maternal, fetal, and neonatal mortality (and in some cases, proxy indicators for these outcomes) provides the foundation for identifying, prioritizing, and evaluating interventions to improve birth outcomes. Evaluation of services provides the basis for determining cost-effectiveness and establishes benchmarks for continuing improvement.
Surveillance
National programs of birth and death registration provide the information needed to develop and evaluate interventions that reduce maternal, fetal, and neonatal mortality. In many countries the magnitude of mater-
nal—also neonatal and fetal—mortality is only beginning to be recognized after many years without accurate birth and death records. For much of the developing world, this lack of information on birth outcomes has obscured the depth of the need for skilled assistance during labor and delivery (Van Lerberghe and De Brouwere, 2001). Concern about the cost of obtaining data before, during, and after implementation of a new intervention is inevitable for communities with scarce resources. This cost is seen by many as competing with the need to deliver key health care services, yet this is an important investment in selecting and implementing the right interventions and tuning them to be effective. The goal is to collect data that are accurate enough to make the required decisions, but not more accurate than is required. For the implementation to be effective, community and health leaders must reach a consensus on the investment of resources. Such a consensus is facilitated by reliable data on the needs for specific interventions.
Surveillance of births
Birth registration provides a tangible acknowledgement of a child’s existence and establishes his or her identity. The United Nations Convention on the Rights of the Child, ratified by virtually every country,1 requires that “each child shall be registered immediately after birth,” yet only about one-quarter of the world’s births (and if China were excluded, less than 7 percent) are recorded by civil registration systems (AbouZhar and Wardlaw, 2001). Registration is nearly universal in much of the Americas, Europe, and East Asia; in many such countries, a child cannot receive medical services or enroll in school without being registered. Some countries have taken steps to increase registration by improving training, infrastructure, and technology. For example, in Argentina, Ecuador, Iran, Mozambique, Thailand, and Zimbabwe traveling registrars issue birth certificates. However, in several developing countries—particularly those with the highest neonatal and fetal mortality rates—few births are registered. Reasons for poor birth registration vary, but typically include the following:
-
shortages of trained personnel and inadequate technology
-
the expectation and acceptance of high mortality during pregnancy and the neonatal period
-
logistical difficulties for parents, including travel to registry offices
-
parental fear of the registration process
-
financial charges associated with registration
-
mismanagement of the registration system.
Surveillance of deaths
The reporting of maternal, fetal, and neonatal deaths is often neglected, even in countries where vital statistics are routinely recorded. For example, even the most widely accepted maternal mortality statistics—the revised WHO/UNICEF/UNFPA estimates based on 1995 levels (World Health Organization, United Nations Children’s Fund, United Nations Fund for Population Activities, 2001) which estimate 515,000 deaths per year worldwide—must estimate the total number of maternal deaths, because country data do not include mortality associated with indirect causes or related to abortions or ectopic pregnancies occurring earlier in gestation. Misclassification of maternal death can also occur when certifying offices fail to note that a woman has recently been pregnant (Walker et al., 1990). Accurate measurement of maternal and neonatal mortality is particularly difficult in many settings where the deaths occur in the home and go unrecorded.
Considerable underreporting of fetal and early neonatal deaths is a problem in most developing countries. International comparisons are further complicated by variations among countries in their definitions of live birth versus stillbirth and late fetal versus early neonatal mortality. In some regions, the births and deaths of children who die before a critical “age of acceptance”—which may be as long as 40 days after birth—are unlikely to be reported (Lawn et al., 2001). The births and deaths of low-birth-weight infants are also less likely to be registered than those of larger infants (World Health Organization, 1996b). As a result of all of these factors, estimates of pregnancy- and birth-related mortality in developing countries are almost certainly low.
Surveillance of pregnancy and birth outcomes
Where vital statistics are inaccurate or nonexistent, pregnancy-related data can be collected on a periodic basis in selected geographic areas to produce a “snapshot” of conditions and outcomes for those locations. Sentinel districts, selected as representative of larger areas, can be designated for ongoing surveillance when a universal system cannot be sustained. Surveillance can also monitor intermediate process data such as the use of specific maternal and neonatal services (see below). These measures do not adequately replace a universal system to plan and support health care services over the longer term.
Some regions have developed effective pregnancy-related surveillance
systems which, when linked to effective maternal and child health programs, have resulted in improvements in various birth outcomes. In Shunyi County, China, surveillance of late fetal and early neonatal deaths revealed five major causes of mortality: neonatal asphyxia, pregnancy-induced hypertension or eclampsia, breech presentation, neural tube defects, and low birth weight. To address these problems, public education and provider training programs were developed, as well as systems of patient screening and referral. Two years after these interventions were implemented, fetal and neonatal deaths due to eclampsia are reported to have been essentially eliminated, deaths due to asphyxia to have declined by 84 percent, breech home deliveries to have declined by more than 60 percent, and use of prenatal care to have increased significantly (Yan et al., 1989). The identification of neural tube defects as a major cause of mortality in this region prompted a study of periconceptional folic acid supplementation. It determined that supplementation significantly reduced the incidence of neural tube defects, prompting China to initiate a nationwide folic acid supplementation program (Berry et al., 1999).
Since 1988, a prospective surveillance system has monitored birth outcomes in the Gadchiroli district of Maharashtra State, India, a remote, underdeveloped area with a population of nearly 80,000 (Bang et al., 1994; 1999). Village-level workers collect data on pregnancies, live births, late fetal deaths, neonatal, and infant deaths from families and traditional birth attendants and assign a cause of death based on verbal autopsy. A retrospective population-based survey, performed every 6 months, indicates that 98 percent of births and childhood deaths are recorded. The data are compiled, organized into a usable format, and presented periodically to health care program managers, who use the information to identify and implement community-based interventions to reduce neonatal and childhood mortality (Bang et al., 1990, 1994, 1999).
These methods could be adapted to measure maternal, fetal, and neonatal mortality rates in other developing country settings. For example, pregnancies could be registered at 5 months’ gestation, and the mother’s age and place of residence recorded. A follow-up query would determine whether the mother survived childbirth, whether her infant was born alive or dead, and if born alive, whether the infant survived the neonatal period. If possible, the infant’s approximate weight at birth should be recorded; if the infant died, his or her age at death should also be noted. Additional information could include the type of birth attendant, location of delivery, procedures used, and the cause of maternal, fetal, and neonatal deaths.
Under an optimal system of surveillance, every pregnancy would be identified prospectively and every outcome ascertained. To obtain meaningful results, surveillance must be conducted in a standardized manner across broad geographic areas (e.g. nations), although the actual collection
of data is probably best accomplished and managed by local authorities. The potential benefits of such surveillance in developing countries must be weighed against the use of scarce resources for medical interventions.
Evaluation
Evaluating the impact of an intervention or health care program may involve measurements of key outcomes such as maternal, neonatal, or fetal mortality, or may be based on process indicators such as the proportion of births attended by a skilled caregiver or taking place in a health care facility. Comparisons based on mortality allow policy makers to track the impact of these services using relatively simple and affordable information systems (Graham, 2002). However, such measures depend on accurate determinations of maternal, fetal, and neonatal mortality, which are not available in most developing country settings. In these cases, process indicators can be used to estimate the large-scale impact of maternal and neonatal services (Ronsmans, 2001). Such process indicators must be shown to be strongly associated with key birth outcomes (Gelband et al., 2001), but causal relationships between process and mortality measures have yet to be established.
Cost of services
Ideally, the budgeting and planning of reproductive health services—and indeed, of health care in general—in a particular setting would reflect the most cost-effective means of meeting significant population needs. However, despite wide recognition of the need for quality, cost-effective maternal and neonatal health care, little comparable “cost per outcome” information exists to aid in identifying priority services. Studies to date have tended to address either the cost or the outcome of interventions (or packages of interventions) to reduce maternal or neonatal mortality in specific countries or regions, but rarely provide information on both cost and outcome (Borghi, 2001). In the absence of detailed data on the cost of implementing effective services, policy makers can use costing instruments to assemble key information on reproductive health care needs and service costs for specific populations. Two such instruments, the Mother-Baby Packaging Costing Spreadsheet and the Cost Estimate Strategy, are described in Box 5-4.
Researchers have examined the cost of packages of maternal health care interventions in terms of cost per death (maternal or neonatal) averted or cost per life-year saved (Gelband et al., 2001). Some of these estimates are cost projections for hypothetical care packages, including delivery with a skilled attendant; others are based on existing conditions in various devel-
|
BOX 5-4 The Mother-Baby Packaging Costing Spreadsheet (MB) from WHO is an easy-to-use, Microsoft Excel-based tool for estimating the cost of implementing recommended packages of interventions. It has been applied in Bolivia (Capra et al., 2000). MB can be obtained free of charge. Another such tool, the Cost Estimate Strategy (CES), provides a framework for incorporating commodity cost information into reproductive health care policy and program decisions. It has been used in Kenya and Zambia (Adams and Burn, 2000). MB and CES allow the costing of similar interventions and are based on similar assumptions about the level of health care facilities used for different activities. However, MB is more comprehensive and includes labor costs as part of the direct costs for each condition, while CES permits detailed analysis of equipment and consumable costs, but does not include labor costs. Thus MB can be used initially to estimate the cost of upgrading services to meet the requirements of the national Safe Motherhood program. Next, CES can be used to estimate the cost of supplies and equipment for these services and identify areas that impede efficient use of resources. Adapting both methods to the country standard can guide revision of national standard treatment guidelines by comparing them with the MB model. |
oping country settings and facilities. According to such calculations, the overall cost of averting a maternal or neonatal death through improved maternal health care varies from about US$1,000 to $3,000, depending on the setting (Gelband et al., 2001). Spread across entire populations of developing countries, a comprehensive package of maternal services that could avert 20 to 80 percent of maternal and neonatal deaths would cost an estimated US$1 to $4 per capita (Gelband et al., 2001).
Cost-effectiveness
Since commitments of money, time, and intellectual effort to one health priority inevitably deplete resources for other health priorities, the choice among interventions needs to be based on sound evidence. The purpose of cost-effectiveness analysis is to reconcile competing demands for finite health resources by systematically comparing public health interventions.
Assessment of the relative importance of a disease or the relative impact of a health intervention begins with an understanding of the magnitude of disease burden. Mortality has traditionally served as the basis for such comparisons; however, serious and long-term illness also contributes to the burden of disease. Both mortality and morbidity are incorporated into disability-adjusted years of life (DALY), an indicator that combines losses from premature death (the difference between the actual age at death and
life expectancy in a low mortality population) and loss of healthy life resulting from disability, (Murray and Lopez, 1996). Development of this indicator involved many judgments (such as the relative burdens of different conditions and of death at different ages) that continue to be refined as additional data become available. In recent years, comparisons based on the DALY have improved countries’ ability to assess health priorities, measure progress in health care delivery, and estimate the impact of conditions that, while they cause relatively few deaths, result in significant disability.
DALYs have been calculated for five major causes of maternal mortality and morbidity (hemorrhage, puerperal infection, eclampsia, obstructed labor, and abortion) and four major causes of neonatal mortality and morbidity (asphyxia, infection, preterm birth, and intrauterine growth retardation); DALYs do not include late fetal deaths. Based on these assessments, pregnancy-related death and disability account for about 18 percent of the total disease burden among women of reproductive age in developing countries (AbouZahr, 1999). Pregnancy-related care and family planning were ranked among the most cost-effective clinical services in the World Bank’s report Investing in Health (World Bank, 1993). Recent calculations estimate the cost of the mother-baby package at only $3-7 per mother-infant dyad depending on labor costs in the country, making this a cost-effective intervention (Tinker, 1997; Jowett and Ensor, 1999).
While DALY measures can be used to guide resource allocation and priority setting, few studies have evaluated interventions that reduce maternal or neonatal health in terms of cost per DALY averted (Mumford et al., 1998). Based on the outcomes of cost studies such as those described above, however, it is reasonable to expect that for women with uncomplicated pregnancies and deliveries, maternal and neonatal services will be more cost-effective when provided through primary care, rather than at referral facilities. Likewise, since prompt emergency care for complications of labor and delivery can significantly reduce maternal and neonatal mortality, providing access to a hospital and medical staff on an emergency basis is an obvious priority for maternal health services. At the referral level, the evidence-based use of surgical interventions such as cesarean section and episiotomy may substantially reduce costs associated with the overuse of these procedures.
RECOMMENDATIONS
The process of implementing the recommendations presented throughout this report begins with the recognition by health leaders and the general public that every pregnancy and birth is important and is at risk for complications. This risk can be reduced most effectively if every mother is assisted during childbirth by a skilled birth attendant and has timely access, in the
event of complications, to a facility where the appropriate level of essential obstetric and neonatal care can be obtained. Where resources for reproductive health care are limited, these goals should be given highest priority. Strong systems of referral will be necessary to overcome the many physical and financial barriers to obtaining good-quality essential obstetric and neonatal care in developing countries.
Establishing health services that reduce maternal, fetal, and neonatal mortality will require national leadership, support, and oversight. The Ministry of Health or another national health agency could coordinate the training of health staff, the organization and management of community health services, the surveillance and analysis of birth outcomes, the evaluation of established interventions, and the implementation of new and revised interventions to target priority outcomes. Support for maternal and neonatal health care policy and services should be sought through community participation, as well as through national, regional, and international collaborations.
Recommendation 5. Each country should develop a strategy to reduce maternal, fetal, and neonatal mortality, a framework of activities by which this can be accomplished, and the commitment of health leaders to accomplish these goals.
A crucial first step in improving health outcomes is the identification of priority outcomes. These must be measured with the precision needed to determine their present status and establish a basis for evaluating progress toward improvement. For health systems and maternal and child health programs, surveillance of maternal, fetal, and neonatal mortality provides the foundation for identifying, selecting, and evaluating interventions to improve birth outcomes. Fetal, early neonatal, and late neonatal, as well as maternal deaths must each be clearly defined to address the distinct causes of mortality for each of these populations. Where vital statistics are inaccurate or nonexistent, pregnancy-related data can be collected on a periodic basis or in sentinel districts or other representative areas and extrapolated to a larger time or geographic scale. Intermediate process data such as the use of specific maternal and neonatal services can also be monitored. However, priority should be given to improving vital statistics, while other data collection should be tailored to match specific conditions and resources.
Recommendation 6. To determine the true burden of disease associated with adverse birth outcomes and measure the effectiveness of interventions to address these problems, basic epidemiological and surveillance data must be collected, analyzed, interpreted, and acted upon. Each country should, as resources permit, incrementally develop complete
national demographic data and ongoing surveillance of maternal, fetal, and neonatal mortality and morbidity.
Once priority outcomes have been identified, interventions to address them must be selected and their impact assessed and improved through continuing surveillance and rigorous, evidence-based evaluation.
Recommendation 7. Each country should strengthen its public health capacity for recognizing and implementing interventions that have proven effective in reducing maternal, neonatal, and fetal mortality in similar populations. This also involves monitoring and tuning interventions for clinical- and cost-effectiveness in the local setting.
RESEARCH NEEDS
Rigorous research is needed to strengthen the evidence base on the effectiveness of interventions to reduce maternal, fetal, and neonatal mortality in the health care systems of developing-country populations. High-priority topics for study include:
-
Implement randomized controlled trials to measure, in a range of settings, the clinical- and cost-effectiveness of interventions likely to reduce maternal, fetal, and neonatal mortality.
-
Based on country needs (from surveillance) and resources and using rigorous evaluation, determine the optimal model of labor and delivery care for a particular country or a region of the country along with strategies to provide broad access to that level of care.
-
Identify appropriate mechanisms for financing reproductive care and measuring the impact of these financing methods on the use and effectiveness of maternal and neonatal services.
CONCLUSION
Health care systems vary widely among developing countries, but every system can be adapted or expanded to provide the fundamental services that reduce maternal, fetal, and neonatal mortality. These include a skilled attendant at every birth; access to essential obstetric and neonatal services for every complicated delivery; and preconceptional, antenatal, and postpartum care that is affordable and effective. Additional maternal and neonatal health services can be added to an effective basic program according to the priorities and resources of countries. Accurate information from population-based surveillance and from clinical and community-based studies is necessary to guide the identification and development of priority services and to improve the effectiveness of new and ongoing interventions.
Historically, governments have achieved significant reductions in maternal and neonatal mortality once they have recognized, through surveillance, the magnitude of the problem and the importance of skilled childbirth assistance in prevention. Policymakers can safeguard the success of such initiatives by monitoring the quality of care provided and ensuring professional accountability. Similar leadership is now needed in developing countries with high maternal and neonatal mortality. Mortality can be lowered most effectively by implementing the evidence-based interventions described in this report, addressing priority needs in underserved populations, and identifying and correcting inefficiencies in the delivery of maternal and neonatal health care services. Adverse birth outcomes cannot be eliminated, even in countries with large health budgets. However, experience in virtually all industrialized countries—and in many developing nations as well—indicates that maternal, fetal, and neonatal deaths can be reduced considerably.
REFERENCES
Abioye-Kuteyi EA, Elias SO, Familusi AF, Fakunle A, Akinolayan K. 2001. The role of traditional birth attendants in Atakumosa, Nigeria. Journal of Research in Social Health 121(2):119–124.
AbouZahr C. 1999. Disability adjusted life years and reproductive health: a critical analysis. Reproductíve Health Matters 7(14):118–119.
AbouZahr C, Wardlaw T. 2001. Maternal mortality at the end of a decade: signs of progress? Bulletin of the World Health Organization 79(6):751–758.
Adams I, Burn R. 2000. Optimizing health funds—planning for reproductive health services in Kenya and Zambia. MotherCare Matters 9(1):3–5.
Adeloye A. 1993. Surgical services and training in the context of national health care policy: the Malawi experience. Journal of Tropical Medicine and Hygiene 96:215–221.
Asowa-Omorodion FI. 1997. Women’s perceptions of the complications of pregnancy and childbirth in two Esian communities, Edo state, Nigeria. Social Science and Medicine 44(12):1817–1824.
Bailey PE, Szaszdi JA, Glover L. 2002. Obstetric complications: does training traditional birth attendants make a difference? Revista Panamericana de Salud Pública 11(1):15–23.
Bang AT, Bang RA, Tale O, Sontakke P, Solanki J, Wargantiwar R, Kelzarkar P. 1990. Reduction in pneumonia mortality and total childhood mortality by means of community-based intervention trial in Gadchiroli, India. Lancet 336(8709):201–206.
Bang AT, Bang RA, Sontakke PG. 1994. Management of childhood pneumonia by traditional birth attendants. The SEARCH Team. Bulletin of the World Health Organization 72(6):897–905.
Bang AT, Bang RA, Baitule SB, Reddy MH, Deshmukh MD. 1999. Effect of home-based neonatal care and management of sepsis on neonatal mortality: field trial in rural India. Lancet 354(9194):1955–61.
Berry RJ, Li Z, Erickson JD, Li S, Moore CA, Wang H, Mulinare J, Zhao P, Wong LY, Gindler J, Hong SX, Correa A. 1999. Prevention of neural-tube defects with folic acid in China. China-U.S. Collaborative Project for Neural Tube Defect Prevention. New England Journal of Medicine 341(20):1485–1490.
Bloom SS, Lippeveld T, Wypij D. 1999. Does antenatal care make a difference to safe delivery? A study in urban Uttar Pradesh, India. Health Policy and Planning 14(1):38–48.
Bobadilla JL, Reyes Frausto S, Karchmer S. 1996. Magnitude and causes of maternal mortality in the Federal District (1988-1989) [in Spanish]. Gneta de Medica de México 132(1):5–16.
Bocaletti E, Brat J, De Leon H. 2000. Comparative costs of normal delivery at a hospital and a community maternity center in Guatemala. MotherCare Matters 9(1):8–12
Borghi J. 2001. What is the cost of maternal health care and how can it be financed? In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 247–296.
Bouillin D, Fournier G, Gueye A, Diadhiou F, Cissé CT. 1994. Epidemiological surveillance and obstetrical dystocias surgery in Senegal [in French]. Cahiers Santé 4(6):399–406.
Campbell OMR. 2001. What are maternal health policies in developing countries and who drives them? A review of the last half-century. Studies in Health Services Organisation and Policy 17:415–448.
Capra K, Weissman, E, Lissner C, Seoane G. 2000. MotherCare Bolivia—cost study of the Mother-Baby Package in Bolivia. MotherCare Matters 9(1):5–8.
Cassels A, Janovsky K. 1998. Better health in developing countries: are sector wide approaches the way of the future? Lancet 352:1777–1779.
Chandramohan D, Cutts F, Chandra R. 1994. Effects of a maternity waiting home on adverse maternal outcomes and the validity of antenatal risk screening. International Journal of Gynaecology and Obstetrics 46:279–284
Chiwuzie J, Okojie O, Okolocha C, Omorogbe S, Oronsaye A, Akpala W, Ande B, Onoguwe B, Oikeh E. 1997. Emergency loan funds to improve access to obstetric care in Ekpoma, Nigeria. The Benin PMM Team. International Journal of Gynaecology and Obstetrics 59(suppl 2):S231–S236.
da Luz Vaz M, Bergström S. 1992. Mozambique–delegation of responsibility in the area of maternal care. International Journal of Gynaecology and Obstetrics 38(suppl):S37–S39.
Daga AS, Daga SR, Dighole RV, Patil RP, Patil MR. 1997. Evaluation of training programme for traditional birth attendants in newborn care. Indian Pediatrics 34(11):1021–1024.
Danel I, Rivera A. 2002. Honduras Case Study, 1990–1997: Shifting from Model 1 to Model 4.
De Brouwere V, Tonglet R, Van Lerberghe W. 1998. Strategies for reducing maternal mortality in developing countries: what can we learn from the history of the industrialized West? Tropical Medicine and International Health 3(10):771–782.
DFID Health Systems Resource Center. 2000. Making the most of the private sector. Report of workshop organized on behalf of the UK Department for International Development in May, 2000. London, England.
Duale S. 1992. Delegation of responsibility in maternity care in Karawa Rural Health Zone, Zaire. International Journal of Gynaecology and Obstetrics 38(suppl):33–35.
Eades CA, Brace C, Osei L, LaGuardia KD. 1993. Traditional birth attendants and maternal mortality in Ghana. Social Science and Medicine 36(11):1503–1507.
Essien E, Ifenne D, Sabitu K, Musa A, Alti-Mu’azu M, Adidu V, Golji N, Mukaddas M. 1997. Community loans funds and transport services for obstetric emergencies in northern Nigeria. International Journal of Gynaecology and Obstetrics 59(suppl 2):S237– S234.
Fauveau V, Wojtyniak B, Mostafa G, Sarder AM, Chakraborty J. 1990. Perinatal mortality in Matlab, Bangladesh: a community-based study. International Journal of Epidemiology 19(3):606–612.
Fawcus S, Mbizvo M, Lindmark G, Nystrom L. 1996. A community-based investigation of avoidable factors for maternal mortality in Zimbabwe. Studies of Family Planning 27(6):319–327.
Ferrinho P, Bughalo AM, Van Lerberghe W. 2001. Is there a case for privatising reproductive health? Patchy evidence and much wishful thinking. Studies in Health Services Organization and Policy 17:343–370.
Figueroa JP, Ashley D, McCaw-Binns A. 1989. An evaluation of perinatal services in institutions in Jamaica. In: The Perinatal Mortality and Morbidity Study, Jamaica: Final Report. Kingston: Department of Child Health, University of the West Indies.
Fofana P, Samai O, Kebbie A, Sengeh P. 1997. Promoting the use of obstetric services through community loan funds, Bo, Sierra Leone. International Journal of Gynaecology and Obstetrics 59(suppl 2):S225–S230.
Foster M, Brown A, Conway T. 2000a. Current Issues in Swap to Health Sector Development: A Synthesis of 6 Case Studies. Geneva: WHO.
Foster M, Norton A, Brown A, Naschold F. 2000b. The status of sector wide approaches: a framework paper for the meeting of the Like-minded Donor Working Group on Sector Wide Approaches, Seminar on Sector Wide Approaches with a focus on Partnership. Dublin, Ireland, February 8–10, 2000. Available online at http://www.odi.org.uk/pppg/publications/papers_reports/other/ira01.pdf.
Fox-Rushby J, Ford F. 1996. Costs, effects and cost-effectiveness analysis of a mobile maternal health care service in West Kiang, The Gambia. Health Policy 35(2):123–143.
Fraser W, Meli J. 1990. Maternal health services—the developing world. Canadian Journal of Public Health 81(6):436–438.
Gani A. 1997. Improving quality in public sector hospitals in Indonesia. In: Newbrander W (ed). Private Health Sector Growth in Asia. Issues and Implications. New York: Wiley. Pp. 197–217
Gelband H, Liljestrand J, Nemer L, Islam M, Zupan J, Jha P. 2001. CMH Working Paper #5: The Evidence Base for Interventions to Reduce Maternal and Neonatal Mortality in Low and Middle-Income Countries. Geneva: WHO.
Goldstein J. 1998. Scissors, surveys, and psycho-prophylactics: prenatal health care campaigns and state building in China, 1949–1954. Journal of Historical Sociology 11(2):153–184.
Goodburn E, Campbell O. 2001. Reducing maternal mortality in the developing world: sector-wide approaches may be the key. British Medical Journal 322(7291):917–920.
Graham W. 2002. Now or never: the case for measuring maternal mortality. Lancet 359(9307):701–704.
Graham WJ, Bell JS, Bullough C. 2001. Can skilled attendance at delivery reduce maternal mortality in developing countries? In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 97–130.
Greenwood AM, Bradley AK, Byass P, Greenwood BM, Snow RW, Bennett S, Hatib-N’Jie AB. 1990. Evaluation of a primary health care programme in The Gambia. I. The impact of trained traditional birth attendants on the outcome of pregnancy. Journal of Tropical Medicine and Hygiene 93(1):58–66.
Gunaserera PC, Wijesinghe PS. 1996. Maternal health in Sri Lanka. Lancet 347(9003):769.
Gunathunga W, Fernando DN. 2000. Assessment of community maternal care performance of public health midwives of a province in Sri Lanka: a multi-method approach. Southeast Asian Journal Tropical Medicine and Public Health 31(2):310–318.
Haddad S, Fournier P. 1995. Quality, cost and utilization of health services in developing countries: a longitudinal study in Zaire. Social Science and Medicine 40(6):743–753.
Hanson K, Berman P. 1998. Private health care provision in developing countries: a preliminary analysis of levels and composition. Health Policy and Planning 13(3):195–211.
Hardee K, Smith. 2000. Implementing Reproductive Health Services in an Era of Health Sector Reform. Washington, DC: Policy Project, Futures Group.
Hesketh T, Zhu WX. 1997. Maternal and child health in China. British Medical Journal 314(7098):1898–1900.
Hesketh TM, Zhu WX, Zheng KH. 1994. Improvement of neonatal care in Zhejiang Province, China through a self-instructional continuing education programme. Medical Education 28(3):252–259.
Hopkins A, Solmon J, Abelson J. 1996. Shifting boundaries in professional care. Journal of the Royal Society of Medicine 89:364–371.
Hotchkiss DR. 1998. The tradeoff between price and quality of services in the Philippines. Social Science and Medicine 46(2):227–242.
Hsiao W. 2000. A Preliminary Assessment of Sri Lanka’s Health Sector and Steps Forward. In conjunction with the Institute of Policy Studies Health Policy Programme, Sri Lanka. Cambridge, MA.
Itina SM. 1997. Characteristics of traditional birth attendants and their beliefs and practices in the Offot Clan, Nigeria. Bulletin of the World Health Organization 75(6):563–567.
Jaffre Y, Prual A. 1994. Midwives in Niger: an uncomfortable position between social behaviours and health care constraints. Social Science and Medicine 38(8):1069–1073.
Jahn A, De Brouwere V. 2001. Referral in pregnancy and childbirth: concepts and strategies. In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 229–246.
Janowitz B, Wallace S, Araujo G, Araujo L. 1985. Referrals by traditional birth attendants in northeast Brazil. American Journal of Public Health 75(7):745–748.
Jha P, Mills A, Hanson K, Kumaranayake L, Conteh L, Kurowski C, Nguyen SN, Oliviera-Cruz V, Ranson K, Vaz LME, Yu S, Morton O, Sachs JD. 2002. Improving the health of the global poor. Science 295:2036–2039.
Johanson R. 2000. Sector Wide Approaches: Education and Health in Sub Saharan Africa. Washington, DC: World Bank.
Jowett M, Ensor T. 1999. Investing in safe motherhood: evidence of cost-effectiveness in developing countries, with specific reference to Kenya. Prepared for United Kingdom, Department for International Development (DFID), East Africa. 396/98/DFID.
Koblinsky MA, Campbell O, Heichelheim J. 1999. Organizing delivery care: what works for safe motherhood? Bulletin of the World Health Organization 77(5):399–406.
Koblinsky MA, Conroy C, Kureshy N, Stanton ME. 2000. Issues in Programming for Safe Motherhood. Arlington, VA: MotherCare/John Sow International.
Kowalewski M, Jahn A. 2001. Health professionals for maternity services: experiences on covering the population with quality maternity care. In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 131–150.
Kusiako T, Ronsmans C, Van der Paal L. 2000. Perinatal mortality attributable to complications of childbirth in Matlab, Bangladesh. Bulletin of the World Health Organization 78:621–627.
Kwast BE. 1991. Shortage of midwives—the effect on family planning. IPPF Medical Bulletin 25(3):1–3.
Kwast BE. 1996. Reduction of maternal and perinatal mortality in rural and peri-urban settings: what works? Euopean Journal of Obstetrics and Gynecology and Reproductive Biology 69(1):47–53.
Langer A, Nigenda G, Catino J. 2000. Health sector reform and reproductive health in Latin America and the Caribbean: strengthening the links. Bulletin of the World Health Organization 78(5):667–668.
Lawn J, McCarthy BJ, Ross S. 2001. The Healthy Newborn: A Reference Manual for Program Managers. Atlanta, GA: CDC, CARE.
Li XF, Fortney JA, Kotelchuk M, Glover LH. 1996. The postpartum period: the key to maternal mortality. International Journal of Gynaecology and Obstetrics 54(1):1–10.
Loutfi A, McLean A, Pickering J. 1995. Training general practitioners in surgical and obstetrical emergencies in Ethiopia. Tropical Doctor 25(suppl 1):22–26.
Macintyre K, Hotchkiss DR. 1999. Referral revisited: community financing schemes and emergency transport in rural Africa. Social Science and Medicine 49(11):1473-1487.
Maiga Z, Traoré Nafo F, El Abassi A. 1999. La réforme du secteur santé au Mali, (1989–1996). [The reform of the health sector in Mali]. Studies in Health Services Origination and Policy. Vol. 12. Antwerp: ITG Press.
Mathur HN, Damodar, Sharma PN, Jain TP. 1979. The impact of training traditional birth attendants on the utilisation of maternal health services. Journal of Epidemiology and Community Health 33(2):142–144.
Mbaruku G, Bergstrom S. 1995. Reducing maternal mortality in Kigoma, Tanzania. Health Policy and Planning 10(1):71–78.
McDermott J, Beck D, Buffington ST, Annas J, Supratikto G, Prenggono D, Ekonomi S, Achadi E. 2001. Two models of in service training to improve midwifery skills: how well do they work? Journal of Midwifery and Women’s Health 46(4):217–225.
McDonagh, M, Goodburn E. 2001. Maternal health and health sector reform: opportunities and challenges. In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 371–385.
Miller LC, Jami-Imam F, Timouri M, Wijnker J. 1995. Trained traditional birth attendants as educators of refugee mothers. World Health Forum 16(2):151–156.
Mumford E, Dayaratna V, Winfrey W, Sine J, McGreevey W. 1998. Reproductive Health Cost: Literature Review. Working Paper Series, No. 3. Washington, DC: Policy Project. Available online at http://www.policyproject.com/pubs/workingpapers/wps-03.pdf.
Murray CJL, Lopez AD (eds). 1996. The Global Burden of Disease. Boston: Harvard School of Public Health.
Murray SF, Davies S, Kumwenda P, Ahmed Y. 2001. Tools for monitoring the effectiveness of district maternity referral systems. Health Policy and Planning 16(4):353–361.
National Population and Family Development Board Malaysia and Ministry of Health Malaysia. 1998. Developing Initiatives for SAFE MOTHERHOOD. In: Kuala Lumpur: NPRDBN/MOH.
National Research Council (NRC). 1997. Reproductive Health in Developing Countries: Expanding Dimensions, Building Solutions. Washington, DC: National Academy Press.
Nylander PP, Adekunle AO. 1990. Antenatal care in developing countries. Bailliere’s Clinical Obstetrics and Gynaecology 4(1):169–186.
Okolocha C, Chiwuzie J, Braimoh S, Unuigbe J, Olumeko P. 1998. Socio-cultural factors in maternal morbidity and mortality: a study of a semi-urban community in southern Nigeria. Journal of Epidemiology and Community Health 52(5):293–297.
Okonofua FE, Abejide A, Makanjuola RA. 1992. Maternal mortality in Ile-Ife, Nigeria: a study of risk factors. Studies in Family Planning 23(5):319–324.
Olaniran N, Offiong S, Ottong J, Asuquo E, Duke F. 1997. Mobilizing the community to utilize obstetric services, Cross River State, Nigeria. The Calabar PMM Team. International Journal of Gynaecology and Obstetrics 59(suppl 2):S181–S189.
Oosterbaan MM, da Costa MV. 1995. Guinea-Bissau: what women know about the risks—an anthropological study. World Health Statistics Quarterly 48(1):39–43.
O’Rourke K. 1995. The effect of hospital staff training on management of obstetrical patients referred by traditional birth attendants. International Journal of Gynaecology and Obstetrics 48(suppl):S95–S102.
Palmer N. 2000. The use of private-sector contracts for primary health care: theory, evidence and lessons for low-income and middle-income countries. Bulletin of the World Health Organization 78(6):821–829.
Pathmanathan I, Dhairiam S. 1990. Malaysia: Moving from Infectious to Chronic Diseases. In: Tarrimo E, Creese A (eds). Achieving Health for All by the Year 2000: Midway Reports of Country Experiences. Geneva: WHO.
Pereira C, Bugalho A, Bergstrom S, Vaz F, Cotira M. 1996. A comparative study of caesarean deliveries by assistant medical officers and obstetricians in Mozambique. British Journal of Obstetrics and Gynaecology 103:508–512.
Phillips JF, Greene WL, Jackson EF. 1999. Lessons from community-based distribution of family planning in Africa. Research Division Working paper no. 121. New York: Population Council. Available online at http://www.popcouncil.org/pdfs/wp/121.pdf.
Pittrof R, Campbell OMR, Filipii VGA. 2002. What is quality in maternity care? An international perspective. Acta Obstetricia et Gynecologica Scandinavica 81:277–83.
Poovan P, Kifle F, Kwast BE. 1990. A maternity waiting home reduces obstetric catastrophes. World Health Forum 11(4):440–445.
Population Council. 1998. Report of the Meeting on the Implications of Health Sector Reform of Reproductive Health and Rights, December 14–15, 1998, Washington DC. Washington, DC: Population Council. Available online at http://www.genderhealth.org/pubs/HSRreport.pdf.
Pratinidhi A, Shah U, Shrotri A, Bodhani N. 1986. Risk-approach strategy in neonatal care. Bulletin of the World Health Organization 64(2):291–297.
Ramiro LS, Castillo FA, Tan-Torres T, Torres CE, Tayag JG, Talampas RG, Hawken L. 2001. Community participation in local health boards in a decentralized setting: cases from the Philippines. Health Policy and Planning 16(suppl 2):61–69.
Ronsmans C. 2001. How can we monitor progress toward improved maternal health? In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 317–342.
Ronsmans C, Vanneste AM, Chakraborty J, van Ginneken J. 1997. Decline in maternal mortality in Matlab, Bangladesh: a cautionary tale. Lancet 350(9094):1810–1814.
Rosenfield A. 1992. Maternal mortality: community-based interventions. International Journal of Gynaecology and Obstetrics 38(suppl):17–22.
Ross JA, Campbell OMR, Bulatao R. 2001. The maternal and neonatal programme effort index (MNPI). Tropical Medicine and International Health 6(10):787–798.
Russell S, Gilson L. 1997. User fee policies to promote health service access for the poor: a wolf in sheep’s clothing. International Journal of Health Services 27(2):359–379.
Schaider J, Ngonyani S, Tomlin S, Rydman R, Roberts R. 1999. International maternal mortality reduction: outcome of traditional birth attendant education and intervention in Angola. Journal of Medical Systems 23(2):99–105.
Schwartz JB, Akin JS, Popkin BM. 1993. Economic determinants of demand for modern infant-delivery in low-income countries: the case of the Philippines. In: Mills A, Lee K (eds). Health Economics Research in Developing Countries. Oxford: Oxford University Press. Pp. 165–192.
Segovia I. 1998. The midwife and her functions by level of care. International Journal of Gynaecology and Obstetrics 63(suppl 1):S61–S66.
Shehu D, Ikeh AT, Kuna MJ. 1997. Mobilizing transport for obstetric emergencies in Northwest Nigeria. The Sokota PMM Team. International Journal of Gynaecology and Obstetrics 59(suppl 2):S173–S180.
Sibley LM, Sipe TA, et al. 2002. Traditional Birth Attendant Training Effectiveness: A Meta-analysis. Washington, DC: Academy for Educational Development.
Smith JB, Coleman NA, Fortney JA, Johnson JD, Blumhagen DW, Grey TW. 2000. The impact of traditional birth attendant training on delivery complications in Ghana. Health Policy and Planning 15(3):326–331.
Sorensen G, Emmons K, Hunt MK, Johnston D. 1998. Implications of the results of community intervention trials. Annual Review of Public Health 19:379–416.
Stanton B, Clemens J. 1989. User fees for health care in developing countries: a case study of Bangladesh. Social Science and Medicine 29(10):1199–1205.
Thaddeus S, Maine D. 1994. Too far to walk: maternal mortality in context. Social Science and Medicine 38(8):1091–1110.
The Prevention of Maternal Mortality Network. 1992. Barriers to treatment of obstetric emergencies in rural communities of West Africa. Studies in Family Planning 23(5):279–291.
Tinker A. 1997. Safe motherhood as a social and economic investment. Presentation at Safe Motherhood Technical Consultation, Inter-Agency Group for Safe Motherhood, October 18–23, Colombo, Sri Lanka.
United Nations Fund for Population Activities (UNFPA). 1999. The UNFPA private-sector initiative. Exploring ways to facilitate co-operation between governments and the commercial sector to expand access to reproductive health commodities. A project of the UNFPA Global Initiative on Reproductive Commodity Management. United National Population Fund, Technical and Policy Division, Technical Branch. New York: UNFPA. Available online at http://www.unfpa.org/tpd/globalinitiative/pdf/privatesector99.doc.
Van Lerberghe W, De Brouwere V. 2001. Reducing maternal morality in a context of poverty. In: De Brouwere V, Van Lerberghe W (eds). Safe Motherhood Strategies: A Review of the Evidence. Studies in Health Services Organization and Policy, 17. Antwerp: ITG Press. Pp. 1–6.
Villar J, Ba’aqeel H, Piaggio G, Lumbiganon P, Miguel Belizan J, Farnot U, Al-Mazrou Y, Carroli G, Pinol A, Donner A, Langer A, Nigenda G, Mugford M, Fox-Rushby J, Hutton G, Bergsjo P, Bakketeig L, Berendes H, Garcia J, WHO Antenatal Care Trial Research Group. 2001. WHO antenatal care randomised trial for the evaluation of a new model of routine antenatal care. Lancet 357(9268):1551–1564.
Walker GJ, McCaw-Binns A, Ashley DE, Bernard GW. 1990. Identifying maternal deaths in developing countries: experience in Jamaica. International Journal of Epidemiology 19(3):599–605.
Wilkinson D. 1997. Reducing perinatal mortality in developing countries. Health Policy and Planning 12(2):161–165.
Wilson E. 2000. Implications of decentralization in reproductive health in Senegal. Policy Matters 30:1–4.
World Bank. 1993. World Development Report 1993. Investing in Health. New York: Oxford University Press.
World Bank. 1999. Safe Motherhood and the World Bank: Lessons From Ten Years Of Experience. Washington, DC: World Bank.
World Health Organization (WHO). 1978. Alma-Ata Declaration. International Conference on Primary Health Care. Geneva: WHO. Available online at http://www.who.int/hpr/archive/docs/almaata.html.
World Health Organization (WHO). 1994. WHO Mother-Baby Package: Implementing Safe Motherhood in Countries. Geneva: WHO. Available online at http://www.who.int/reproductive-health/publications/MSM_94_11/MSM_94_11_table_of_contents.en.html.
World Health Organization (WHO). 1996a. Care in Normal Birth: A Practical Guide. Geneva: WHO. Available online at http://www.who.int/reproductive-health/publications/MSM_96_24/MSM_96_24_table_of_contents.en.html.
World Health Organization (WHO), Division of Family and Reproductive Health. 1996b. Perinatal Mortality a Listing of Available Information. Geneva: WHO.
World Health Organization (WHO), Division of Health Situation and Trend Assessment. 1996c. Catalogue of Health Indicators. A Selection of Important Health Indicators Recommended by WHO Programmes. Geneva: WHO.
World Health Organization (WHO). 1998. Improve Access to Maternal Health Services. Geneva: WHO. Available online at http://www.who.int/archives/whday/en/pages1998/whd98-07.html.
World Health Organization (WHO). 1999. Reduction of Maternal Mortality: A Joint WHO/ UNFPA/UNICEF/World Bank Statement. Geneva: WHO. Available online at http://www.who.int/reproductive-health/publications/reduction_of_maternal_mortality/reduction_of_maternal_mortality_contents.htm.
World Health Organization (WHO), United Nations Children’s Fund (UNICEF), United Nations Population Fund (UNFPA). 2001. Maternal Mortality in 1995: Estimates Developed by WHO, UNICEF, UNFPA. Geneva: WHO
Wyss K, Whiting D, Kilima P, McLarty DG, Mtasiwa D, Tanner M, Lorenz N. 1996. Utilisation of government and private health services in Dar Es Salaam. East African Medical Journal 73(6):357–363.
Yan RY, McCarthy B. 1989. The Risk Approach in Perinatal Health. Shunyi County, People’s Republic of China, U.S. Department of Health and Human Services (DHHS), Public Health Service, Centers for Disease, Control. DHHS Publication No. 890-8412. Washington, DC: U.S. Government Printing Office.
Young ME. 1990. Maternal health in China: challenges of the next decade. Health Policy and Planning 14:87–125.








































