3
Workforce Health, Performance, Readiness, Resilience: The Case for Change
This chapter outlines the evolution of and evidence for a new vision and approach to optimizing employee health and performance.
INTRODUCTION AND BACKGROUND
Definition and Significance of “Healthy Workforce”
Like other large U.S. agencies and corporations, NASA is challenged with both increasing productivity demands and a changing American workforce. Just as the agency’s scientific and engineering breakthroughs have improved everyday life for Americans, so too can NASA’s pioneering effort in other aspects of its mission be harnessed as an opportunity to improve the health and performance of its own workforce and serve as a model for other “knowledge worker” employers whose workers are highly educated and whose work products are complex problem solving and solutions rather than service delivery or product manufacture.
The twenty-first-century American workforce is characterized by increasing demographic diversity, a greater number of multidisciplinary jobs, higher degrees of collaborative work and reliance on technology, “knowledge workers,” and highly skilled technicians, as well as around-the-clock or so-called “24/7” operations, an accelerated workpace, and more flexible work patterns (IOM, 2003a). In addition, significant changes are occurring in the organization of work.
U.S. workplaces now rely more heavily on information technology, have more distributed work arrangements, and engage teams composed
of members from different employers or from the same employer but with different terms of employment. They also create and dissolve work groups and employment around specific projects and employ global work teams using technology to perform work in “virtual” environments of electronic team rooms and web-hosted meetings. Within the workforce itself, there is greater uncertainty about employment, as evinced by people having many more employers over their working careers, being required to become continuous learners to enhance or expand their skills, and experiencing the movement of work and jobs to other countries (IOM, 2003a).
These changes within the workforce and at the workplace create greater psychological demands on workers as well as demands for higher levels of productivity. To succeed in a work environment of rapid change requires workers to be mentally and physically prepared, adaptable, and resilient—in a word, healthy.
A “healthy worker” can be characterized as one who is physically fit and demonstrates positive health-related behaviors such as not using tobacco, alcohol to excess, or illicit drugs, maintaining body weight in the ideal range, regularly performing appropriate levels of physical activity, and complying with recommended preventive health practices; who has psychological skills that enable success in work environments of high demand, collaborative work, and short cycle times; and who works within a safe and healthy work environment. An integrated occupational health and safety program can help improve worker health through worksite strategies aimed at strengthening psychological skills, changing health behaviors, and reinforcing social norms supportive of these health goals (Sorensen and Barbeau, 2004).
Integrated worksite health and safety programs have both individual and organizational applications that can be developed to promote personal and organizational health-related productivity. A “healthy workforce” is characterized by four key attributes, consistent with the World Health Organization (WHO) definition of health, that can be analyzed and improved to promote personal and organizational “well-being.” Specifically, for both individuals and organizations to achieve optimal performance, they must be
-
healthy—demonstrating optimal health status as defined by positive health behaviors; minimal modifiable risk factors; and minimal preventable illnesses, diseases, and injuries;
-
productive—functioning to produce the maximum contribution to achievement of personal goals and the organizational mission;
-
ready—possessing an ability to respond to changing demands given the increasing pace and unpredictable nature of work; and
-
resilient—adjusting to setbacks, increased demands, or unusual challenges by bouncing back to optimal “well-being” and performance without incurring severe functional decrement.
The traditional “occupational” and “nonoccupational” dichotomy that has been defined by predictable shifts and the 40-hour workweek is increasingly blurred by the changing demands of the contemporary American workplace (IOM, 2003a). Employers that have traditionally been responsible for safety, environmental, and occupational health concerns will, of necessity, become more involved with worklife issues, health behaviors, and social interactions. Adverse effects on employers of high health care costs and tight labor markets, particularly in engineering, create employer imperatives for engaging health beyond traditional occupational health and safety. Employers, including NASA, who must support a mission-directed, healthy, and optimally productive workforce will have to articulate a new vision, develop new strategies, and employ new tactics.
Effectiveness of Health and Health Care
The health and safety of NASA’s diverse and geographically widespread employees are the concern of the Office of the Chief Health and Medical Officer (OCHMO). The goal of this office, in collaboration with the NASA vision, is to ensure that employees who join NASA should end their careers healthier than employees in other organizations as a result of their experience with NASA occupational and preventive health programs. NASA draws its workforce from the general population, and thus the American working population serves as a point of comparison.
Understanding important occupationally related health issues and trends among Americans is critical to understanding the health needs of NASA employees. Previous federal and Institute of Medicine (IOM) reports addressing relevant health, health care, occupational health, and American workforce issues provide important information that can illuminate and guide NASA’s efforts to achieve its broad goal of creating a comparatively healthier NASA workforce.
Healthy People 2010
The Healthy People series, begun in 1979, was developed to address disparities in health status and outcomes between diverse population groups, and to improve the overall health of the nation (U.S. Public Health Service, 1979; USDHHS, 2000; www.healthypeople.gov/Publications).
The goals put forward in the original document and its subsequent editions embrace the concept of quality of life and protective, proactive health behaviors, rather than just disease prevention. The two overarching goals identified in Healthy People 2010 are to increase quality and years of healthy life and to eliminate health disparities.
The health goals that were established for the nation in the Healthy People series serve as a framework for NASA’s Occupational Health programs; however, as the focus of occupational health at NASA is its workforce, the agency’s focuses for action and the benchmarks are necessarily somewhat different from those established for the entire American population. Specific application of these goals to an integrated preventive health care program is discussed further in Chapter 5.
In the implementation of Healthy People 2010, health goals are monitored through a set of 467 objectives in 28 focus areas (USDHHS, 2000). The objectives are linked to targets for health improvement to be achieved by the year 2010 and are intended to facilitate the two overarching health goals described above.
An array of factors including individual (biology, behavior, and physical and social environment), policies and interventions, and access to quality health care directly influence morbidity and mortality in the United States. Understanding these determinants of health is a key component in the effort to achieve the Healthy People goals. Further, monitoring and measuring health determinants are necessary activities to understand and improve the population’s health status. This approach—understanding and monitoring health behaviors, environmental factors, and community health systems—has been applied to the development of Leading Health Indicators for Healthy People 2010 (USDHHS, 2000; www.healthypeople.gov/LHI).
Leading Health Indicators for Healthy People 2010
The Leading Health Indicators for Healthy People 2010 developed out of a collaborative effort led by an interagency working group within the Department of Health and Human Services (USDHHS). In addition, the report from the Institute of Medicine (IOM), Leading Health Indicators for Healthy People 2010 (IOM, 1999), provided models to support the indicator sets. The indicators represent major concerns in public health that stem from individual behaviors, physical and social environmental factors, and important health system issues affecting both individuals and communities.
The leading health indicators—physical activity, overweight and obesity, tobacco use, substance abuse, responsible sexual behavior, mental health, injury and violence, environmental quality, immunization, and
access to health care—are linked to specific objectives from Healthy People 2010 that are used to track progress. They are also linked to the 467 objectives in Healthy People 2010 in that they can serve as a starting point for community health initiatives. These indicators are anticipated to facilitate health promotion and disease prevention, encourage participation in health improvement efforts, and increase the effect of Healthy People on improving quality and length of life and eliminating health disparities (USDHHS, 2000).
The Future of the Public’s Health
The primary objective of the report on The Future of the Public’s Health (IOM, 2003b) was to develop a framework for action to assure the public’s health in the new century. The guiding vision for this framework is based on the goals of Healthy People 2010. The action areas reviewed in this report and its findings are consistent with Healthy People 2010 and support the case for change by addressing occupational health and productivity issues in federal agencies such as NASA, as well as the private sector. The Future of the Public’s Health study committee envisioned six areas of action and change to accomplish the objectives of the framework:
-
Adopt a population health approach that builds on evidence of the multiple determinants of health;
-
Strengthen the governmental public health infrastructure—the backbone of any public health system;
-
Create a new generation of partnerships to build consensus on health priorities and to support community and individual health actions;
-
Develop appropriate systems of accountability at all levels to ensure that population health goals are met;
-
Ensure that action is based on evidence; and
-
Acknowledge communication as the key to forging partnerships, ensuring accountability, and using evidence for decision making and action.
The findings of the report emphasize the challenge of achieving these goals at the community level and the need for action at the societal level that is broadly supported by the community and its agencies. The recommendations of the committee support the need for commitment to the action areas on the part of government, including national, state, and local levels, and engagement of citizens, nongovernmental organizations, health-care providers, businesses, academia, the media, and others to achieve the goal of a healthier U.S. population.
Safe Work in the 21st Century
The IOM report Safe Work in the 21st Century reviewed numerous programs for training and education of workers and identified needs in worker and employer training for workplace safety and health (IOM, 2003a). The report identified a need for more emphasis on workplace injury prevention as well as easier access for Occupational Safety and Health (OSH) workers to more comprehensive and alternative learning experiences. Another important finding of this report was that worker training and education in workplace safety and health was not considered a prime responsibility of most OSH professionals. Thus, recommendations from the report focus on OSH workforces and training programs, including urging that federal agencies such as the National Institute for Occupational Safety and Health (NIOSH), the Occupational Safety and Health Administration (OSHA), and the National Institute of Environmental Health and Safety (NIEHS) work together with employers, unions, and industry representatives to evaluate the effectiveness of worker training programs and better define minimum training requirements (IOM, 2003a).
Although training efforts are now in place at NASA, this report may serve as a useful guide to inform future training and education efforts. It may also serve as a guide to integration of training and education for worksite health professionals into agency-wide occupational health and safety programs.
Guide to Community Preventive Services
Employers can exercise many environmental and population-based interventions to improve the health and productivity of employees and their families. Evidence- and population-based strategies and programs to improve health and prevent disease, whether in states, communities, local organizations, health care organizations, worksites, or schools, have been analyzed and recommended by the Task Force on Community Preventive Services.
The Guide to Community Preventive Services (http://www.thecommunityguide.org/) is a federally sponsored initiative that is a component of a larger group of federal public health initiatives that includes documents such as Healthy People 2010. It was developed by the nonfederal Task Force on Community Preventive Services, which was appointed by the director of the Centers for Disease Control and Prevention (CDC). The Task Force was convened in 1996 by the USDHHS as an independent decision-making body that would provide leadership in the evaluation of community, population, and health care system strategies to address a variety of public health and health promotion topics (see
below). Support is provided by staff from CDC as well as various public and private partners.
The guide was developed for employers who controlled many population-targeted programs and environmental factors that have been demonstrated to be effective in improving or supporting health behaviors that reduce morbidity, mortality, and loss of productivity. The guide provides communities and health care systems with recommendations for population-based interventions to promote health and prevent disease, injury, disability, and premature death. The recommendations are provided through systematic reviews of three general topic areas: changing risk behaviors; reducing diseases, injuries, and impairments; and addressing environmental and ecosystem challenges. Specific topics covered in the recommendations are:
-
Alcohol
-
Cancer
-
Diabetes
-
Mental Health
-
Motor Vehicle Safety
-
Nutrition
-
Oral Health
-
Physical Activity
-
Pregnancy
-
Sexual Behavior
-
Social Environment
-
Substance Abuse
-
Tobacco
-
Vaccines
-
Violence
The various topics are covered in an ongoing series of publications (CDC, 2004; Zaza et al., 2005) and are also published in supplements to the American Journal of Preventive Medicine.
Quality Chasm
NASA is both a purchaser of health care insurance and a provider of health care services for its employees and their families. NASA, as other major U.S. employers, has an important role in promoting and ensuring effective and efficient health care systems and delivery. The IOM report from the Committee on the Quality of Health Care in America (IOM, 2001) addressed issues of quality care in the American health care system and
|
BOX 3-1 safe – avoiding injury from intended therapy; effective – providing evidence-based service to all who can benefit and not to those for whom no benefit can be derived; patient-centered – providing respectful and responsive care guided by the preferences, needs, and values of the recipient; timely – reducing waiting time and other delays to both recipients and providers; efficient – avoiding waste of equipment, supplies, ideas, and energy; and equitable – providing care of consistent quality to all recipients SOURCE: Committee on the Quality of Health Care in America (IOM, 2001). |
made recommendations for a wide variety of key stakeholders to improve the effectiveness and efficiency of health care.
The study panel proposed a broad agenda for improving and redesigning the current health care system in the United States, which included the following: all health-care constituencies, including policy makers, purchasers, regulators, health professionals, health-care trustees and management, and consumers, should commit to a national statement of purpose for the health care system as a whole and to a shared agenda of six aims (see Box 3-1) for improvement that can raise the quality of care to unprecedented levels; clinicians and patients, and the health care organizations that support care delivery, adopt a new set of principles to guide the redesign of care processes; the USDHHS identifies a set of priority conditions on which to focus initial efforts, provides resources to stimulate innovation, and initiates the change process; health care organizations design and implement more effective organizational support processes to make change in the delivery of care possible; and purchasers, regulators, health professionals, educational institutions, and the USDHHS creates an environment that fosters and rewards improvement by creating an infrastructure to support evidence-based practice, facilitating the use of information technology, aligning payment incentives, and preparing the workforce to better serve patients in a world of expanding knowledge and rapid change.
Although this report is focused on acute and critical care systems, the principles proposed apply as well to preventive health care. Preventive and health promotion programs and activities should provide services
that are evidence-based, patient- or participant-centered, and systems-oriented, and thus are applicable to improving the quality of care provided to employees of organizations such as NASA.
NIOSH Steps to a Healthier U.S. Workforce
Interest in worksite initiatives integrating occupational health and safety with health promotion and disease prevention efforts is on the rise among the business community, labor groups, and the research community, as evidenced by the recent NIOSH Steps to a Healthier United States Workforce Symposium (Goetzel, 2004; Seabury et al., 2004; Sorensen and Barbeau, 2004 [http://www.cdc.gov/niosh/steps/2004/whitepapers.html]). Additional evidence supporting the potential effect of an integrated approach is emerging in a growing literature reporting results of studies that have systematically assessed the efficacy of integrated interventions (Sorensen and Barbeau, 2004). For example, one randomized controlled study asked the question, “Does the addition of worksite occupational health and safety increase the effectiveness of worksite health promotion only?” (Sorensen et al., 2002). From a survey of 15 manufacturing worksites, randomly assigned to receive either worksite health promotion only or worksite health promotion plus occupational safety and health, the study found that among blue-collar workers who were more likely to be exposed to hazards on the job, smoking cessation rates for those in the integrated intervention were double those in the traditional health promotion-only program. This study also found that worksites receiving the integrated intervention made significantly greater improvements in their health and safety programs than the health program-only sites.
The Steps to a Healthier U.S. Workforce Initiative (STEPS) was developed by NIOSH from an initiative in the USDHHS called Steps to a Healthier U.S. (NIOSH, 2004; www.healthierus.gov/steps/). Concordant with this committee’s study charge to evaluate options for preventive health programs, incentives to encourage employee participation, and methodologies to longitudinally track employee health at NASA, the STEPS initiative seeks to improve the dissemination, effectiveness, and acceptance of activities directed at improving worker health through integrated approaches to health protection and health promotion.
The vision of the STEPS initiative is to combine occupational safety and health protection with health promotion activities into integrated health management programs that address both workplace and worker health. STEPS strongly supports the view that all illness and injury should be prevented when possible, controlled when necessary, and treated
where appropriate, and an integrated approach serves to enhance the effectiveness of programs designed to promote and protect worker health.
The STEPS initiative has created an opportunity for the occupational safety, occupational health, and health promotion communities to develop and implement a comprehensive set of programs aimed at improving integrated health and productivity in the workplace. Further, the STEPS project is pertinent to meeting the needs of public–private partnerships such as NASA, which include a mixed workforce of civil servant and private-sector employees, highly directed products with specific outcomes, and major research needs.
ENVISIONING THE FUTURE
Current Trends in the United States to Create a Healthy, Productive Workforce
Health and productivity of the U.S. workforce are affected and predicted by many and various factors, including individual health status (e.g., disease incidence and prevalence), health care access and quality, occupational health and safety efforts, employer-specific culture and organizational factors, and community-wide (demographic or geographic) influences (Evans and Stoddart, 1994). Figure 3-1 illustrates the Evans and
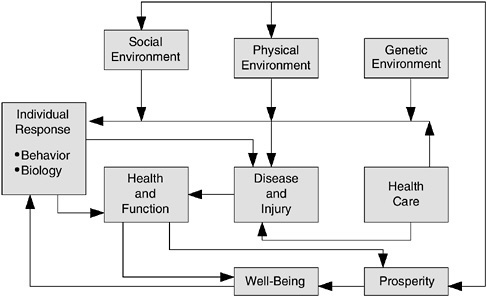
FIGURE 3-1 Determinants of health; Evans and Stoddart Model.
SOURCE: IOM, 2003b. Adapted from Evans and Stoddart, 1994.
Stoddart (1994) model of health, the determinants of health, and the health care system. Employers, through their policies, benefits, culture, and community influences, can affect numerous health determinants that have an effect on employees and their families.
The ability of health promotion programs to affect employee health has been the subject of hundreds of published research manuscripts and reviews (Wilson et al., 1996; Chapman and Pelletier et al., 2004). Health promotion programs are designed to promote health by maintaining healthy behaviors and by reducing health risks and actively preventing the onset of disease. The risk-reduction programs typically include interventions and programs designed to reduce stress; increase physical activity and fitness; reduce high blood pressure and cholesterol; reduce excess body weight; improve nutrition; reduce tobacco, alcohol, and substance abuse; and even increase seatbelt use. Some programs offer cancer screening, health risk appraisals, cooking classes, and a variety of health education activities. Reviews of the effectiveness of many of these interventions have shown promising results (Sorensen et al., 1998; Aldana and Pronk, 2001). The low-risk-maintenance programs are a more recent strategy and are designed to help maintain already healthy behaviors. It has been estimated that this strategy may be the most effective in influencing the health of a workplace population (Edington, 2001).
Improving Productivity and Reducing Labor Cost for Employers
Employers are increasingly concerned about the effect of poor health on the cost of health benefits as well as the cost of lost productivity. Interventions to improve employee health have been shown to improve financial outcomes for employers. Aldana and Pronk (2001) found a strong correlation between high levels of stress, excessive body weight, and multiple risk factors, and increased health care costs and illness-related absenteeism. Lower physical fitness and activity levels were also found to be associated with increased health care costs, although not with absenteeism.
Edington et al. (2001) showed that reductions in health risk factors including stress resulted in decreased medical care costs. Analyses of health risk and medical claims over a period of years indicated a correlation between decreased health risks and declines in cost of care. Additional evidence from Ozminkowski et al. (2002) demonstrated that after a period of 4 years, following introduction of programs to reduce health risk factors; a savings of $244.66 per employee was realized, compared to a traditional medical plan.
Workplace health strategies and programs today are progressing beyond the traditional health promotion approach toward integrating all
TABLE 3-1 Current Trends in America for a Healthy and Productive Workforce
|
Perspective |
Current State |
Desired State |
|
Function |
Absenteeism |
Performance |
|
Cost Metrics |
Medical Costs |
Economic Outcomes |
|
Care Model |
Treatment Focused |
Prevention and Behavior Change Focused |
|
Medical Model |
Individual |
Population |
|
Health Metrics |
Disease Status |
Health Status |
|
Interventions |
Single-Risk Focused |
Multiple-Risk Focused |
|
Health Framework |
Employer-, Condition-, and Program-Centric |
Employee-Centric |
|
Management Systems |
Segregated Programs |
Integrated Systems |
aspects of health to look fully at health-related productivity. Employers are finding that not only is it important to affect the overall health of a population to manage health care costs and sustain productivity (e.g., by minimizing the effect of absenteeism) but that advancing health also reduces presenteeism (the effect of diminished health on an employee’s ability to engage and function to full capacity while at work), reflecting the realization that not all employees present are fully engaged and optimally productive. Isolating the components of absenteeism, disability, workers’ compensation, and presenteeism has enabled employers to more closely examine the effect of health risks on overall productivity (Edington, 2001).
In recent years, employers and relevant federal agencies have demonstrated that multifactor determinants of health and productivity must be addressed using new perspectives, metrics, and models. Table 3-1 outlines current trends toward achieving a healthy and productive workforce based on determinants of health and productivity.
Function: From “Absenteeism” to “Performance”
Global competition and systems analyses of productivity of the workforce has led to more holistic thinking about productivity at the workplace. Whereas absenteeism was the metric of choice for many years, the current metric has been expanded and evolved into the measurement of performance or presenteeism. Productivity at the workplace now includes two components: time away from work (absenteeism and disability) and presenteeism (job performance).
Presenteeism, a term first mentioned in the literature by Smith (1970), has been defined as being the exact opposite of absenteeism: being at work when you should be at home, either because you are ill or because you are too tired to be effective. Presenteeism recognizes that work was done, but at a level of performance below optimal (see Chapter 5 for further discussion).
The more recent application of this concept was first published by Burton et al. (1999), when actual work performance of call center operators was measured in relation to health risks and disease states. Because most jobs do not have an easily accessed metric for performance, a series of self-reported work effectiveness scales has been developed and incorporated into the more general Health Risk Appraisal (HRA). The establishment of a relationship between health risk indicators and disease incidence using self-reported performance skills while on the job has been recently described (Boles et al., 2004; Mayne et al., 2004).
A healthy work ecosystem is an enabler for improving and maintaining performance-based measures of productivity. Although “time away from work” measurements are relatively standard, presenteeism is very job- and organization-specific and must be defined within the context of each center. It may not be captured by civil service or contractor classifications and could be manager defined, in the case of NASA, either by organizational leaders or by NASA contractors who are familiar with the capabilities of a healthy worker.
If presenteeism cannot be defined and measured by job classifications, then more general self-report questionnaires may be used. A serious limitation to the measurement of presenteeism, however, is the absence of a gauge of quality of work. That is, an employee may be present each day and may be productive, but if that employee makes numerous mistakes, the total productivity is diminished.
Cost Metrics: From “Medical Costs” to “Economic Outcomes”
Employers’ health-related concerns are dominated by rapidly increasing medical costs, but in general, there is little appreciation for the underlying and mitigable factors that drive medical care expenditures. NASA, like all federal agencies, obtains civil service employee health care through the Federal Health Employee Benefits Program (FEHBP), centrally administered through the Office of Personnel Management (OPM). Unlike private and non federal government sector employers, however, NASA does not receive information on health care expenditures to monitor for quality and health improvement purposes. Such data typically include utilization costs and data for hospitalizations, outpatient care, surgical procedures, medications, diseases, and nonoccupationally related injuries. This lack
of information on health care costs as a “starting point” to detect the risk factor- and disease-related costs is a significant disadvantage for NASA, compared to non federal employers, in trying to understand and improve the health and productivity of its workforce.
Employers have traditionally viewed “medical costs” as largely separate from productivity or “indirect costs” such as absenteeism, disability, and presenteeism. However, there is little question that non-occupational illness and injury has a significantly greater impact on productivity, morbidity, mortality, and health-related costs than occupational injury and illness. For example, in 2002, death from all occupational causes was 4.0 per 100,000 employed workers overall (BLS, 2003), a reflection of the “healthy worker” effect. In contrast, mortality per 100,000 population was 240.8 for heart disease, 193.5 for cancer, 25.4 for diabetes, and 36.9 for unintentional injuries. Even death from suicide and homicide exceeded all occupational cause mortality (NCHS, 2004). Cost data specific to employed populations was reported by Goetzel et al. (2001) in their analysis of health and productivity impacts for forty-three employers in 1998. Categories of cost and utilization examined included non-occupational health benefits and disability, workers’ compensation, absenteeism and worker turnover rates.
The employers studied were from eight different industry sectors: communications (n=5), government and education (n=10), finance and insurance (n=4), manufacturing (n=8), and employed nearly a million workers. Data for 1998 showed the impact of non-occupational sources of morbidity and cost far exceeded that of occupational causes as reflected in workers’ compensation costs. Goetzel et al. (2001) reported the range of per capita costs for these corporations related to non-occupational health benefits as $3,127 to $6,421; for non-occupational disability, $225 to $1084; and for workers’ compensation, $93 to $863. While it is unclear from these data whether the non-occupational health benefits data are for the employee only or the employee plus dependents, even at one third the cost reported, assuming the reported costs reflect a conservative allocation of cost at one third employee/one third spouse/one third children, the conclusion is unchanged.
Care Model: From “Treatment-Focused” to “Prevention and Behavior Change-Focused”
The leading causes of premature morbidity and mortality in the United States have consistently been shown to be modifiable health behaviors (McGinnis et al., 2002; McGinnis and Foege, 1993). Recent large cohort studies of Asian and Mediterranean populations have further supported the finding of an unnecessary U.S. burden of risk factor-related disease. It is estimated that 65-85 percent of heart disease, 60 percent of
cancers, and 91 percent of diabetes among Americans are caused by modifiable personal health behaviors that, if adapted, would result in a likely 50 percent reduction in all-cause mortality (Knoops et al., 2004; Rimm and Stampfer, 2004). Both the U.S. Preventive Services Task Force and the U.S. Community Preventive Services Task Force provide evidence-based recommendations for the prevention of risk factors, illnesses, and injuries (see above).
The medical and short-term disability costs of preventable medical conditions are substantial (Edington and Musich, 2004). In at least two studies, excess risks were clearly related to excess costs in workers’ compensation and short-term disability costs (Musich et al., 2001; Wright et al., 2002). Thus, the outcome of controlling costs through the process of controlling risks becomes obvious, and risk-reduction and low-risk maintenance programs should become a major business strategy in moderating disability costs.
Medical Model: From “Individual” to “Population”
The traditional medical model focuses on treating individuals after a series of symptoms are identified and associated with a known disease. It has been useful for the diagnosis and treatment of disease in individuals; however, a population-based public health framework (“agent-host environment” causation of diseases or conditions) is more suitable to address both the health of the general population and workforce health issues (Rose, 1985; McKinlay, 1995; Berkman and Kawachi, 2000; Wilkinson and Marmot, 2003; Goetzel, 2004). Occupational health and safety models, closely aligned with a public health perspective, emphasize a systems-based approach to preventing illnesses and injuries and sustaining good health. A similar population health-based approach to effectively alter individual health behaviors is needed to address large preventable burdens such as disease and lost productivity. Employers are more likely to improve their employees’ health and productivity using multiple strategies and tactics at the population level than by focusing on individual medical or clinical programs to address risk factors, disease, and injuries as they occur.
Most employers continue to focus on postevent medical claims, although heart disease, cancer, diabetes, and musculoskeletal disorders are major threats to performance and mission accomplishment (Wang et al., 2003; BLS, 2002). However, as discussed in Chapter 2, health care costs, costs resulting from the centralization of occupational preventive medicine, and data on prevalence of conditions are not visible at NASA, and are thus not seen as a mission threat or as a predictor of disease, injury, or death.
Health Metrics: From “Disease Status” to “Health Status”
Employers have monitored health care costs that reflect medical expenditures for existing diseases or conditions but have not been able to track either the actual prevalence of disease or the prevalence of important health risk factors. Numerous studies have shown that risk factor identification and early disease detection have beneficial effects on associated health care and productivity costs (Edington et al., 1997; Edington and Musich, 2004; Martinson et al., 2003). Some employers, therefore, are attempting to monitor both individual and population “health status,” as expressed by the presence or absence of risk factors and other indicators shown to be associated with workplace performance such as cardiorespiratory endurance (VO-2 max) (Pronk et al., 2004a).
Although disease status is often the metric of choice as the “driver” of health care and lost productivity costs, the more important factor is actually health status (Yen et al., 1991; Edington, 2001). Overall health status might be thought of as the sum, among others, of risk factors and disease state, and it is influenced by lifestyle choices, genetics, and workplace environmental factors. Monitoring of health status for a population of employees is the preferred metric to document improved health and productivity (Edington, 2001).
Interventions: From “Single-Risk Focused” to “Multiple-Risk Focused”
Tobacco use, unhealthy diet, physical inactivity, overweight, and obesity remain the leading causes of morbidity and mortality in the U.S. today, and some factors are continuing to increase in prevalence (McGinnis and Foege, 1993; Mokdad et al., 2001; Orleans, 2004). Effective interventions have been described for many specific health behaviors, and the U.S. Preventive Services Task Force supports the assertion that implementing these is among the most effective approaches to reduce the incidence as well as the frequency and severity of the leading causes of morbidity and mortality (Nigg et al., 2002; Orleans et al., 1999; http://www.ahrq.gov/clinic/gcpspu.htm). Unfortunately, rates of screening and implementation of brief interventions to address these risk factors remain low in a variety of settings, including primary care (Pronk et al., 2004b; Whitlock et al., 2002).
Many of these health risk factors tend to cluster within individuals (Coups et al., 2004; Fine et al., 2004; Pronk et al., 2004c). Using 2001 National Health Interview Survey data, Fine and colleagues (2004) examined the prevalence and clustering of four risk factors—smoking, alcohol consumption, low levels of physical activity, and overweight—among adults in the United States. They provided point prevalence estimates for each
risk factor singly and in combination with others (see Chapter 5 discussion of Prevention Programs for examples). On the basis of their estimates, only 10 percent of the adult population had none of the four risk factors, whereas one, two, three, and four risk factors were noted among 33 percent, 41 percent, 14 percent, and 3 percent of the population respectively. Hence, multiple risk factors (two or more of these four) occurred in the majority of the U.S. population. Other studies by Coups and colleagues (2004) and Pronk et al. (2004c) have confirmed these results.
A small proportion of working-age adults and seniors meet recommended guidelines for multiple behavioral risk factors that are associated with health benefits (Pronk et al., 2004c). In fact, the majority of the U.S. population has two or more risk factors at the same time (Coups et al., 2004; Fine et al., 2004; Pronk et al., 2004c). Because multiple behavioral risks are present simultaneously among most people, addressing these risk factors in combination rather than singly is warranted, but requires more effective models, tools, strategies, and systemic support for integrated health behavior change efforts (Orleans, 2004).
To be more specific about what could be done to translate current scientific knowledge into practical applications, Glasgow et al. (2004) enumerated five principles and fifteen hypotheses for consideration and testing in the context of addressing multiple risk factors in the primary care setting. Three of the five principles of program design related to the patient–clinician interaction and included greater use of the “5As” model of self-management—assess, advise, agree, assist, and arrange (Goldstein et al., 2004)—collaborative goal-setting and shared decision-making, and recognition that the primary care setting is only a component of the patients’ larger social framework. The other two principles included the notion that individual-level behavior change should also apply to practice and health system levels, and that redesign of the practice office environment through inclusion of more proactive and planned actions will produce better outcomes. These principles can easily be applied to the employer/worksite setting. In addition, the associated fifteen hypotheses can be used for guidance in creating testable and manageable processes that apply to NASA specifically.
Health Framework: From “Employer-, Condition-, and Program-Centric” to “Employee-Centric”
A condition- or program-centric framework inadequately addresses determinants of poor health, increased costs, and decreased economic outcomes. Condition- and program-centric approaches artificially segment human populations, ignore interactions, suboptimize worker en-
counters, and can become static and unresponsive to changes in an employee’s dynamic ecology.
Golaszewski et al. (1998) showed that environmental (employer) interventions can be effective in supporting employee efforts to maintain and improve health. Just as the medical care system is “provider-centric,” a change to an employee-centric focus can ease employee engagement and improve their personal health and medical care outcomes. A parallel argument can also be made to all employer policies and programs.
The transition away from a model that measured “indicators of health” as a consequence of mortality and disease rates began in the mid-twentieth century with the World Health Organization’s broader view of health as complete physical, mental, and social well-being rather than the absence of disease (WHO, 1948). Subsequent work contributed to the evolution in thinking about health and the effect of a variety of biological and social determinants on physical, mental, and social well-being. (See Figure 3-1 for illustration of the Evans and Stoddart model of health, the determinants of health, and the health care system.)
The effect of the social and physical environments on health and health-related quality of life was further developed in a model proposed in the IOM report The Future of the Public’s Health in the 21st Century (IOM, 2003b). This model, shown in Figure 3-2, illustrates how the characteristics of these environmental factors affect physical, mental, and social well-being.
Management Systems: From “Segregated Programs” to “Integrated Systems”
As discussed previously and in Chapter 2, the current state of occupational health at NASA reflects a traditional work organization and division of responsibility with centralization of policy, compliance and audit, and decentralized program planning, funding, resource management, and service delivery (see Figures 1-2 and 2-1). Further, at the local level, NASA occupational health activities are managed on a program-by-program basis. This method of service delivery is highly vulnerable to program segregation, and it tends to diminish opportunities for cross-program synergy and reinforcement of health objectives which occur at each encounter, irrespective of the specific program triggering the encounter. Outsourced occupational health programs under very large site-wide contracts, for which the occupational health team at NASA has little direct oversight, create obstacles to vendor collaboration and efficient integration of interventions.
To pursue additional individual and organizational benefits associated with a more holistic view of health and work, Occupational Health at NASA requires a service construct oriented toward human performance;
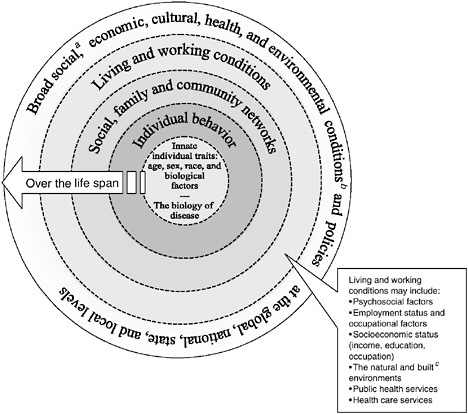
FIGURE 3-2 A guide to thinking about the determinants of population health.
aSocial conditions include, but are not limited to: economic inequality, urbanization, mobility, cultural values, attitudes and policies related to discrimination and intolerance on the basis of race, gender, and other differences.
bOther conditions at the national level might include major sociopolitical shifts, such as recession, war, or governmental collapse.
cThe built environment includes transportation, water and sanitation, housing, and other dimensions of urban planning.
SOURCE: The Future of the Public’s Health in the 21st Century, IOM, 2003b. Adapted from Dahlgren and Whitehead, 1991. The dotted lines between levels of the model denote interaction effects between and among the various levels of health determinants (Worthman, 1999).
a health model focused on population, rather than individual goals and objectives; and a measurement system oriented toward health status and outcomes (Table 3-1). A systems approach rather than a programs approach better supports this paradigm because systems are constructed of linkages and seek synergy. Systems operations require thinking, work processes, and resource utilization which emphasize integration, collaboration, and optimizing overall performance rather than stand-alone components or programs.
Integration Across Program Components
Goetzel et al. (2001) have made the case for an integrated health approach. In their report, data from 43 employers with an annual median total health and productivity management cost per employee of $9,992, included costs in five core areas: group health, turnover, unscheduled absence, nonoccupational disability, and workers’ compensation. When other program areas were considered, the figure increased to $10,365 per employee per year. A savings of 26 percent per employee per year was shown to be possible by using an integrated approach in the five core areas.
FINDINGS
Occupational health, safety, and wellness programs at NASA, as at the majority of U.S. employers, are currently organized as a program-centric model with a focus on disease status rather than health status; treatment and traditional physical health risk factor modification, with relatively less emphasis on mental health and behavior change; an individual- rather than population-based medical model; and a program-by-program approach to risk factor remediation rather than an integrated multiple-risk approach (see Table 3-1). These traditional approaches to occupational health and health promotion are not well adapted to the needs of the modern knowledge workforce and represent a significant opportunity for reengineering and improvement.
RECOMMENDATION
The committee recommends that the administrator of NASA adopt a new vision for worker health, readiness, and resilience that directly links to NASA’s mission and includes health as a core NASA value that is implemented through an integrated health and systems approach. This vision should extend and apply to the entire NASA workforce and should:
-
clearly articulate a broader perspective of health and how it advances NASA’s core mission;
-
be adopted and adapted by each center’s director to maximize the alignment with each center’s mission and workforce composition; and
-
be promoted and implemented vertically and horizontally within NASA, using participatory strategies to ensure sustained senior management and organizational commitment and total workforce engagement.
REFERENCES
Aldana SG, Pronk NP. 2001. Health promotion programs, modifiable health risks, and employee absenteeism. Journal of Occupational and Environmental Medicine 43(1):36–46.
Berkman LF, Kawachi I, eds. 2000. Social Epidemiology. New York: Oxford University Press.
BLS (Bureau of Labor Statistics), USDL. 2002. Lost-Worktime Injuries and Illnesses: Characteristics and Resulting Days Away from Work. [Online]. Available: ftp://ftp.bls.gov/pub/news.release/History/osh2.04102002.news [accessed May 12, 2005].
BLS, USDL. 2003. BLS News, USDL 03-488. Washington, DC: United States Department of Labor. [Online]. Available: http://www.bls.gov/iif/oshwc/cfoi/cfnr0009.pdf [accessed May 18, 2005].
Boles M, Pelletier B, Lynch W. 2004. The relationship between health risks and work productivity. Journal of Occupational and Environmental Medicine 46(7):737–745.
Burton WN, Conti DJ, Chen C-Y, Schultz AB, Edington DW. 1999. The role of health risk factors and disease on worker productivity. Journal of Occupational and Environmental Health 41(10):863–877.
CDC (Centers for Disease Control and Prevention) Community Guide Branch. 2004. Guide to Community Preventive Services: Systematic Reviews and Evidence-Based Recommendations. Atlanta, GA: Oxford University Press.
Chapman LS, Pelletier KR. 2004. Population health management as a strategy for creation of optimal healing environments in worksite and corporate settings. Journal of Alternative and Complementary Medicine 10(Suppl 1):S127–S140.
Coups EJ, Gaba A, Orleans CT. 2004. Physician screening for multiple behavioral health risk factors. American Journal of Preventive Medicine 27(Suppl 2):34–41.
Edington DW. 2001. Emerging research: A view from one research center. American Journal of Health Promotion 15(5):341–349.
Edington DW, Musich S. 2004. Associating changes in health risk levels with changes in medical and short-term disability costs. Health and Productivity Management 3(1):12–15.
Edington DW, Yen LT, Witting P. 1997. The financial impact of changes in personal health practices. Journal of Occupational and Environmental Medicine 39(11):1037–1046.
Evans RG, Stoddart GL. 1994. Producing health, consuming health care. In: Evans RG, Barer ML, Marmor TR, eds. Why Are Some People Healthy and Others Not? The Determinants of Health of Populations. New York: Aldine DeGruter.
Fine LJ, Philogene GS, Gramling R, Coups EJ, Sinha S. 2004. Prevalence of multiple chronic disease risk factors; 2001 National Health Interview Survey. American Journal of Preventive Medicine 27(Suppl 2):18–24.
Glasgow RE, Bull SS, Piette JD, Steiner JF. 2004. Interactive behavior change technology; A partial solution to the competing demands of primary care. American Journal of Preventive Medicine 27(Suppl 2):80–87.
Goetzel RZ. 2004 (October 26-28). Examining the Value of Integrating Occupational Health and Safety and Health Promotion Programs in the Workplace. Paper presented at the National Institute of Occupational Safety and Health (NIOSH) Steps to a Healthier U.S. Workforce Symposium, Washington, DC. [Online]. Available: http://www.cdc.gov/niosh/steps/2004/whitepapers.html [accessed May 12, 2005].
Goetzel RZ, Guindon AM, Turshen IJ, Ozminkowski RJ. 2001. Health and productivity management: Establishing key performance measures, benchmarks, and best practices. Journal of Occupational and Environmental Medicine 43(1):10–17.
Golaszewski T, Barr D, Cochran S. 1998. An organization-based intervention to improve support for employee heart health. American Journal of Health Promotion 13(1):26–35.
Goldstein MG, Whitlock EP, DePue J. 2004. Multiple behavioral risk factor interventions in primary care; Summary of research evidence. American Journal of Preventive Medicine 27(Suppl 2):61–79.
IOM (Institute of Medicine). 1999. Leading Health Indicators for Healthy People 2010. Washington, DC: National Academy Press.
IOM. 2001. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press.
IOM. 2003a. Safe Work in the 21st Century. Washington, DC: The National Academies Press.
IOM. 2003b. The Future of the Public’s Health in the 21st Century. Washington, DC: The National Academies Press.
Knoops KT, de Groot LC, Kromhout D, Perrin AE, Moreiras-Varela O, Menotti A, van Staveren WA. 2004. Mediterranean diet, lifestyle factors, and 10-year mortality in elderly European men and women: The HALE project. Journal of the American Medical Association 292(12):1433–1439.
Martinson BC, Crain AL, Pronk NP, O’Connor PJ, Maciosek MV. 2003. Changes in physical activity and short-term changes in health care charges: A prospective study of older adults. Preventive Medicine 37(4):319–326.
Mayne TJ, Howard K, Brandt-Rauf, PW. 2004. Measuring and evaluating the effects of disease on workplace productivity. Journal of Occupational and Environmental Medicine 46(Suppl 6):S1–S2.
McGinnis JM, Foege WH. 1993. Actual causes of death in the United States. Journal of the American Medical Association 270(18):2207–2212.
McGinnis JM, Williams-Russo P, Knickman JR. 2002. The case for more active policy attention to health promotion. Health Affairs 21:78–93.
McKinlay MJ. 1995. The new public health approach to improving physical activity and autonomy in older populations. In: Heikkinon E, ed. Preparation for Aging. New York: Plenum Press. Pp. 87–103.
Mokdad AH, Bowman BA, Ford ES, Vinicor F, Marks JS, Koplan JP. 2001. The continuing epidemics of obesity and diabetes in the United States. Journal of the American Medical Association 286(10):1195–1200.
Musich SA, Napier D, Edington DW. 2001. The association of health risks with workers’ compensation costs. Journal of Occupational and Environmental Medicine 43(6):534–541.
NCHS (National Center for Health Statistics). 2004. Health, United States, 2004 with Chartbook on Trends in the Health of Americans. Hyattsville, MD: U.S. Government Printing Office. [Online]. Available: http://www.cdc.gov/nchs/data/hus/hus04.pdf [accessed May 18, 2005].
Nigg CR, Allegrante JP, Ory M. 2002. Theory-comparison and multiple-behavior research: Common themes advancing health behavior research. Health Education Research 17(5):670–679.
NIOSH (National Institute of Occupational Safety and Health). 2004. Steps to a Healthier U.S. Workforce. [Online]. Available: http://www.cdc.gov/niosh/steps/ [accessed December 9, 2004].
Orleans CT. 2004. Addressing multiple behavioral health risks in primary care; Broadening the focus of health behavior change research and practice. American Journal of Preventive Medicine 27(Suppl 2):1–3.
Orleans CT, Gruman J, Ulmer C, Emont SL, Hollendonner JK. 1999. Rating our progress in population health promotion: Report card on six behaviors. American Journal of Health Promotion 14(2):75–82.
Ozminkowski RJ, Ling D, Goetzel RZ, Bruno JA, Rutter KR, Isaac F, Wang S. 2002. Long-term impact of Johnson & Johnson’s Health & Wellness Program on health care utilization and expenditures. Journal of Occupational and Environmental Medicine 44(1):21–29.
Pronk NP, Martinson B, Kessler RC, Beck AL, Simon GE, Wang P. 2004a. The association between work performance and physical activity, cardiorespiratory fitness, and obesity. Journal of Occupational and Environmental Medicine 46(1):19–25.
Pronk NP, Peek CJ, Goldstein MG. 2004b. Addressing multiple behavioral risk factors in primary care; A synthesis of current knowledge and stakeholder dialogue sessions. American Journal of Preventive Medicine 27(Suppl 2):4–17.
Pronk NP, Anderson LH, Crain AL, Martinson BC, O’Connor PJ, Sherwood NE, Whitebird RR. 2004c. Meeting recommendations for multiple healthy lifestyle factors; Prevalence, clustering, and predictors among adolescent, adult, and senior health plan members. American Journal of Preventive Medicine 27(Suppl 2):25–33.
Rimm EB, Stampfer MJ. 2004. Diet, lifestyle, and longevity—The next step? Journal of the American Medical Association 292(12):1490–1492.
Rose G. 1985. Sick individuals and sick populations. International Journal of Epidemiology 14(1):32–38.
Seabury SA, Lakdawall D, Reville RT. 2004 (October 26–28). The Economics of Integrating Injury Prevention and Health Promotion Programs. Paper presented at the National Institute of Occupational Safety and Health (NIOSH) Steps to a Healthier U.S. Workforce Symposium, Washington, DC. [Online]. Available: http://www.cdc.gov/niosh/steps/2004/whitepapers.html [accessed May 12, 2005].
Smith DJ. 1970. Absenteeism and “presenteeism” in industry. Archives of Environmental Health 21(5):670–677.
Sorensen G, Barbeau E. 2004 (October 26–28). Integrating Occupational Health and Safety and Worksite Health Promotion: State of the Science. Paper presented at the National Institute of Occupational Safety and Health (NIOSH) Steps to a Healthier US Workforce Symposium, Washington, DC. [Online]. Available: http://www.cdc.gov/niosh/steps/2004/whitepapers.html [accessed May 12, 2005].
Sorensen G, Emmons K, Hunt MK, Johnston D. 1998. Implications of the results of community intervention trials. Annual Review of Public Health 19:379–416.
Sorensen G, Stoddard A, LaMontagne A, Emmons K, Hunt MK, Youngstrom R, McLellan D, Christiani D. 2002. A comprehensive worksite cancer prevention intervention: Behavior change results from a randomized controlled trial (United States). Cancer Causes and Control 13(6):493–502.
USDHHS (U.S. Department of Health and Human Services). 2000. Healthy People 2010. Washington, DC: U.S. Government Printing Office. [Online]. Available: http://www.healthypeople.gov/Publications [accessed May 12, 2005].
U.S. Public Health Service. 1979. Healthy People: The Surgeon General’s Report on Health Promotion and Disease Prevention. Publication PHS 79-55071. Washington, DC: U.S. Government Printing Office.
Wang SP, Beck A, Bergland P. 2003. Chronic medical conditions and work performance in the health and work performance questionnaire calibration surveys. Journal of Occupational and Environmental Medicine 45(12):1303–1311.
Whitlock EP, Orleans CT, Pender N, Allan J. 2002. Evaluating primary care behavioral counseling interventions: An evidence-based approach. American Journal of Preventive Medicine 22(4):267–284.
WHO (World Health Organization). 1948. Preamble to the Constitution of the World Health Organization. As adopted by the International Health Conference, New York, June 19–22, 1946.
Wilkinson R, Marmot M, eds. 2003. Social Determinants of Health: The Solid Facts. Copenhagen, Denmark: World Health Organization, Regional Office for Europe.
Wilson MG, Holman PB, Hammock A. 1996. A comprehensive review of the effects of worksite health promotion on health-related outcomes. American Journal of Health Promotion 10(6):429–435.
Worthman CM. 1999. Epidemiology of human development. In: Panter-Brick C, Worthman CM, eds. Hormones, Health, and Behavior: A Socio-Ecological and Lifespan Perspective. Cambridge, UK: Cambridge University Press.
Wright DW, Beard MJ, Edington DW. 2002. The association of health risks with the cost of time away from work. Journal of Occupational and Environmental Medicine 44(12):1126–1134.
Yen LT, Edington DW, Witting P. 1991. Associations between employee health-related measures and prospective medical insurance costs in a manufacturing company. American Journal of Health Promotion 6(1):46–54.
Zaza S, Briss PA, Harris KW, eds. 2005. The Guide to Community Preventive Services: What Works to Promote Health? (Task Force on Community Preventive Services). New York, NY: Oxford University Press.
Websites:
www.ahrq.gov/clinic/gcpspu.htm
www.bls.gov/iif/oshwc/cfoi/cfnr0009.pdf
www.cdc.gov/nchs/data/hus/hus04.pdf
www.cdc.gov/niosh/steps/2004/whitepapers.html
























