5
Overview of Health-Monitoring Activities: State and Federal Perspectives
In the context of human health, the state- and federal-level government responses to the Deepwater Horizon disaster include developing surveillance approaches based on the best available science, providing needed health services to affected communities as part of surveillance, and collecting the necessary data to ensure that responses to future disasters are based on an even stronger evidence base.
State agencies across the Gulf Coast and many federal agencies have been actively conducting environmental and public health monitoring in an effort to track the oil spill’s public health impact and to ensure that workers, residents, and other persons whose health could be affected by the spill are receiving the appropriate medical care. During this session, state health officials from Alabama, Florida, Louisiana, Mississippi, and Texas described the oil spill response from their respective states. Additionally, federal representatives from the Office of the U.S. Surgeon General, the Department of Health and Human Services (HHS), the Department of Homeland Security, and the Environmental Protection Agency (EPA) participated in this workshop session. This chapter summarizes their presentations and comments.
STATE RESPONSES
All five states reported two types of active public health surveillance: syndromic surveillance and reporting surveillance. Syndromic surveillance involves collecting data on sets of symptoms that may be exposure related (e.g., respiratory symptoms) and investigating case clusters. Data for syndromic surveillance come from the Department of Defense (DoD)
and Veterans Affairs (VA) treatment facilities as part of the Centers for Disease Control and Prevention’s (CDC’s) BioSense Program1 and from hospital emergency rooms and urgent care centers participating in other surveillance programs (e.g., Florida’s ESSENCE program [defined later in this chapter]). Reporting surveillance involves collecting data from poison control centers, physician clinics, and other sources, and investigating unusual clusters of symptoms that could be exposure related.
At the time of the workshop, only Alabama had detected an increase in illness through syndromic surveillance (29 exposure-related emergency room visits, mostly inhalation related). Additionally, Alabama had detected 66 exposure-related illnesses through reporting surveillance, with most being inhalation related. Louisiana had detected a total of 143 exposure-related illnesses through reporting surveillance. Most illnesses were inhalation-related illnesses among rig workers or clean-up workers, with the most commonly reported symptoms being headache, nausea, and throat irritation.
Alabama
Donald E. Williamson, State Health Officer
The entire Alabama coastline has been impacted by the Deepwater Horizon disaster, with all oyster reefs and coastal water closed for fishing at the time of the workshop, reported Donald Williamson. Although large amounts of oil were still rolling onshore, the swimming advisory that was at one point issued for all coastal waters has been lifted for some, but not all, beaches. As with the other states, Alabama has been conducting both syndromic and reporting surveillance.
Alabama’s hospital syndromic surveillance includes tracking visits to 8 hospital emergency rooms and 20 high-volume urgent care centers and Federally Qualified Health Centers in two spill-affected counties. Exposure-related data are collected daily and collated weekly. Of a total of 19,429 complaints between the middle of May and the time of the workshop, 29 were related to oil exposure (18 via inhalation, 8 via dermal contact, and 3 via ingestion). Syndromic surveillance of DoD and VA treatment facilities through the BioSense program had not detected any anomalies at the time of the workshop.
There were 66 oil-spill-related exposure calls to the Alabama Poison Center at the time of the workshop, including 57 describing minor symptoms (e.g., nausea, vomiting, diarrhea, skin rash) and 9 describing moderate symptoms. As with the syndromic surveillance data, most symptoms were inhalation related (50), followed by dermal contact (12) and ingestion (4).
Improving Surveillance
Alabama is continually refining its surveillance activities. Williamson identified several areas of surveillance that need improvement. Many of the areas identified were also mentioned by representatives from the other Gulf States:
-
Surveillance is voluntary with no validation of exposure reports. Williamson said that he suspected that most exposures are not from the oil itself, but from the oil spill response efforts (e.g., 10 days before the workshop, 17 people on a barge fell ill, not from exposure to oil, but from carbon monoxide that the generator had been pumping into the air intake).
-
Monitoring systems that capture relevant data for examining long-term health effects need to be developed (e.g., population-monitoring systems that can capture increases in hypertension, cardiovascular disease, and other chronic diseases).
-
Mental health surveillance needs improvement so that the necessary interventions are available.
-
The current syndromic surveillance system has yet to differentiate between resident and worker status, although efforts are under way.
-
Worker health surveillance also needs improvement, with more information being communicated from BP to the state health departments.
-
Messages to the public need to clearly communicate uncertainty around potential adverse long-term health effects. For instance, noted Williamson, a lack of evidence for acute health effects does not mean that there are no adverse effects.
Florida
Ana M. Viamonte Ros, State Surgeon General
Although early indications suggest that the Gulf oil spill’s acute physical health effects may be minimal, Ana Viamonte Ros agreed with other panelists about the importance of monitoring behavioral health complications that may arise as a result of environmental devastation and growing economic losses stemming from the Gulf oil disaster. This is especially true of Florida, said Viamonte Ros, where both the tourism and seafood industries are experiencing severe economic downturns as a result of the Deepwater Horizon disaster. Tourism comprises a large sector of Florida’s economy. In 2008, tourism spending totaled more than $65 billion and brought in another $4 billion in sales-tax revenue, and more than 1 million people were employed in the tourism industry. Florida’s finfish and shellfish industry comprises another significant portion of the state economy, with a dockside value of more than $200 million.
Syndromic and Real-Time Reporting Surveillance
The Florida Department of Health has been collaborating with both the CDC and the National Institute for Occupational Safety and Health (NIOSH) to monitor potential adverse health effects in both the general public and clean-up workers. As in Louisiana and Alabama, the state has been conducting both syndromic and reporting surveillance, using similar data sources.
Hospital syndromic surveillance includes tracking visits to participating emergency rooms for illnesses that may be related to oil or smoke exposure. Tracking is done through a program called ESSENCE (Electronic Surveillance System for the Early Notification of Community-based Epidemics). Syndromic surveillance of DoD and VA treatment facilities is being carried out through the BioSense program. Additionally, real-time monitoring of electronic reports from the Florida Poison Information Center Network is ongoing.
At the time of the workshop, none of the surveillance activities had detected any oil-related clusters of illness, although there had been some reports of heat exhaustion and dehydration.
Environmental Monitoring
In addition to public health monitoring, Florida has initiated baseline environmental testing (e.g., water, sediment, and seafood-tissue sampling) and contingency planning for other future monitoring needs. For example, an air quality monitoring protocol is being developed in the event that near-shore oil burning becomes necessary, and a fisheries reopening protocol (e.g., seafood-tissue testing) is being developed for those fisheries that have been closed due to the presence of oil in the water.
Risk and Health Communication
Florida has also initiated a robust effort to manage public information, with health information being communicated to the public at the regional, county, and local levels in English, Spanish, and Creole. Additionally, the state government has enacted a rumor-control program to respond to health-related rumors; established an integrated Deepwater Horizon response website to serve as a single access point for information, with a real-time map showing places where oil-related health advisories have been issued; launched a toll-free, spill-related information hotline; and briefed the personnel at Florida’s four poison control centers about potential exposures and potential adverse health effects of exposure. The hotline and poison control center scripts are updated frequently as new health and safety information emerges.
Louisiana
Jimmy Guidry, State Health Officer
Louisiana has been conducting both syndromic and reporting surveillance of sickness complaints and exposure claims, as well as monitoring the environment (air, water, and seafood) with the goals of mitigating adverse effects related to exposure and ensuring that people do not become sick unnecessarily. As Jimmy Guidry explained, the state is also monitoring the health care provided to those who are potentially affected by exposure in order to ensure that people are receiving the right care.
Syndromic Surveillance
The state has been conducting syndromic surveillance among seven hospitals in impacted areas for increases in respiratory illness or asthma. At the time of the workshop, in comparison to trends over the past 3 years, there was no indication of spill-related increases in either outcome.
Reporting Surveillance
At the time of the workshop, Louisiana was in its third week of reporting surveillance. The state health department has been monitoring complaint data from the public and from health care providers about potential exposures (e.g., through odors, fumes, or dermal contact) and data on all illnesses and injuries potentially related to exposure (including heat stress). The health data include both objective (e.g., vomiting) and subjective (e.g., nausea) measures. Although not mandatory, Guidry said that the response has been robust and that people are often willing to share what is happening in their lives during tumultuous events or experiences. Details of the reported exposures and health effects are issued in weekly surveillance reports, and the state health department is using these reports to identify trends and to ensure that the necessary medical resources are available where needed. Additionally, the Occupational Safety and Health Administration (OSHA) is using the data to enhance worker surveillance, and the media are using the data to monitor health complaints.
At the time of the workshop, there had been a total of 143 reported exposure-related illnesses (108 workers, 35 general public), including 20 hospitalizations (17 workers, 3 general public). Poison control centers reported most of the data (73 reports), followed by physician clinics (33 reports), and the hotline (3 reports). The most commonly reported route of exposure was odor or inhalation, followed by skin contact. Again, most of the illnesses were among rig workers or clean-up workers, with the most commonly reported symptoms being headache, nausea, and throat irritation.
Improving Surveillance
An important limitation of the surveillance data being collected (at the time of the workshop) is that no attempts were made to confirm exact exposure. Confirming self-reported exposures is challenging. People’s perception of reality is often very different from reality, and people may perceive that they are exposed to things when they are not, said Guidry. For example, after receiving multiple reports of nausea, which many of the affected people attributed to oil-dispersant exposure, the state conducted air sampling in the cluster areas and concluded that the symptoms were more likely related to hydrogen sulfide coming from the swamps (and not to the oil spill). Additionally, given that many of the workers are working in 100°F conditions or hotter, it can be difficult to identify whether weakness, nausea, headache, or other illnesses due to chemical exposures or to heat.
In addition to the difficulties associated with validating exposure claims, another major surveillance challenge—not just for Louisiana but for all the Gulf states—is uncertainty around the oil spill’s long-term effects. Surveillance must separate oil spill related exposures from other factors that could adversely affect an individual’s health (e.g., genetics, lifestyle choices).
Mississippi
Mary Currier, State Health Officer
Although the oil spill has not hit Mississippi nearly as hard as it has hit Alabama, Florida, and Louisiana (at the time of the workshop), there is considerable monitoring already under way or planned, including of both the environment (e.g., air, water, fish) and of human health. The monitoring under way is very similar to what the other Gulf States are doing with respect to acute health effect surveillance, with both syndromic and reporting surveillance systems in operation. At the time of the workshop, none of the surveillance data indicated any increases in human illness related to the Deepwater Horizon oil spill.
Syndromic Surveillance
Mississippi has been conducting syndromic surveillance in five coastal and four inland hospital emergency rooms for four symptoms: (1) respiratory illness with fever, (2) respiratory illness without fever,
(3) rash, and (4) “other” (nausea, vomiting, headache). The inland hospitals serve as controls. The data are reported on a daily basis as a percentage of all non-trauma patients seen in a 24-hour period. Mary Currier emphasized the importance of gathering baseline data to get a sense of “normal” and “routine,” so that spikes can be readily identified and investigated. She showed a few examples of the types of spikes in data that prompted further investigation (see Figure 5-1).
In addition to hospital emergency department data, the state has also been using BioSense data from VA and DoD facilities to examine the same four syndromes.
Reporting Surveillance
The state has been collecting data from the Mississippi Poison Control Center on the number of calls related to the oil spill, differentiating between exposure and informational calls. At the time of the workshop, the poison control center had received a total of 13 calls on the oil spill, including 8 informational and 5 exposure-related calls. The Rocky Mountain Poison Control Center in Colorado was contracted to receive some of Mississippi’s calls, and those data had not been collected yet.
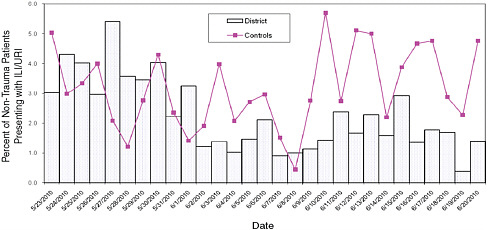
FIGURE 5-1 A comparison of coastal and inland (control) syndromic surveillance data for influenza-like illness (ILI) and upper respiratory infection (URI).
Improving Surveillance
In addition to determining how to transfer Rocky Mountain Poison Control Central calls to the Mississippi center, other immediate needs include improving mental health surveillance and care and monitoring long-term health effects. Currier remarked that the Department of Mental Health had already seen approximately a 10 to 15 percent increase in calls to its emergency phone lines and referrals to psychiatrists and psychologists.
Texas
Bruce Clements, Director of the Community Preparedness Section, Texas Department of State Health Services
At the time of the workshop, Bruce Clements reported that Texas had been spared direct damage from the Gulf oil spill. Nonetheless, the state had been preparing itself in the event that a response to direct impact would become necessary. Specifically, Texas has been conducting potential exposure-related syndromic surveillance among 28 hospitals (14 nonfederal and 14 military or VA treatment facilities). No anomalies in either mental or physical health had been detected.
Improving Surveillance
One of the challenges with surveillance is the large number of Texas residents who have left Texas to work on the oil spill response and the lack of clarity about how data on those workers will be tracked. As reported by other states, mental health surveillance poses yet another challenge. However, the greatest challenge, Clements said, is the reactionary nature of the political agenda. He observed that federal funding for public health preparedness has decreased every year since 2001 (i.e., after 9/11 and the anthrax mailings). As just one example, 2006 saw a 13 percent decrease in funding for public health preparedness; yet that same year, there was an infusion of targeted federal funding for avian influenza preparedness and response. Clements described the 8-year research and development process for developing a new grenade or other weapon as “very thoughtful” and “very strategic.” By contrast, he said, “We don’t put that kind of thought into our surveillance systems in public
health.” The way that funds are redirected from one topic to another, year by year, means that “we can’t be strategic in our approach. We are truly not building the infrastructure that we need to carry out the surveillance that is being described here.” Rather than focusing on individual events or outbreaks, efforts need to be directed toward putting systems in place that can address all public health threats.
PANEL DISCUSSION
The Need for a Sustained Federal Commitment to Building Surveillance Capacity
Although mental health and chronic health surveillance were both identified as major areas for improvement, Clements’ remark about the challenge posed by the reactionary nature of the political agenda prompted some heated discussion. Some panelists agreed that directing federal funds toward specific public health threats weakens the overall public health preparedness infrastructure, which affects all disaster response efforts. The surveillance systems needed for the Gulf oil spill are no different than the surveillance systems needed for other public health emergencies. As Currier said, “Surveillance for oil spill illness is surveillance for everything.” Viamonte Ros echoed Clements’ call for more sustained federal funding so that state-level efforts can be directed toward developing long-term surveillance systems. Williamson agreed that state-level capacity to build the necessary surveillance systems will be uncertain without sustained support. Additionally, Williamson pointed to the lack of surge capacity for “unusual” laboratory testing (e.g., polyaromatic hydrocarbon testing) as another example of activities needing sustained federal commitment.
The Need for Answers: The Importance of Collaboration in Research
There was some discussion about the importance of research collaboration among states, federal agencies, private industry, and the affected communities. Guidry pointed out that, even though a great deal of money was put into health research following the Exxon Valdez spill, “We still don’t have the answers.” He emphasized the importance of collective
thinking around how best to design a strategic research program so that the affected communities do not feel like “guinea pigs.” Guidry also commented on the added challenge created when messages are sent to the public about the potential chronic health consequences of exposure, such as cancer, despite insufficient scientific evidence to support those claims. He opined that sharing conjecture with the public may add to emerging mental health problems. Those messages can be difficult to hear when people are already worried about what they should and should not do in the face of a disaster. Williamson agreed with Guidry about the need to not let “half-science create unnecessary fear.” He said that part of the problem is that the longitudinal follow-up studies necessary to address some of the remaining questions about the potential long-term, human health consequences of exposure to oil spills were not conducted after the Exxon Valdez spill. He cautioned that the Deepwater Horizon disaster “won’t be the last spill” and said he hoped that the public health community is not faced with the same unanswered questions in the future.
FEDERAL RESPONSE
The Specific Goals and Activities of the U.S. Federal Government Health Response2
John Howard, National Institute for Occupational Safety and Health
As John Howard explained, the Department of Homeland Security is in charge of the overall Deepwater Horizon response (under Homeland Security Presidential Directive 5). At the operational level, the federal response to the Gulf oil spill is under the direction of Coast Guard Admiral Thad Allen, with the White House Domestic Policy Council coordinating the federal-level, human health response (i.e., health-related activities of all federal agencies and cabinet-level departments). Within
|
2 |
This section summarizes panel remarks that pertained to the federal response. See Chapter 1 for a summary of Howard’s remarks on populations of concern. |
HHS,3 the various spill-related public and mental health activities are coordinated by the Assistant Secretary for Preparedness and Response, Nicole Lurie, who spoke during the opening session of the workshop (see Chapter 1 for a summary of her comments). The EPA is in charge of most environmental monitoring of the Deepwater Horizon disaster, with some assistance from the National Oceanic and Atmospheric Administration (NOAA), with real-time monitoring data being posted on the EPA website.
According to Howard, the federal government health response to the Deepwater Horizon disaster has four primary goals:
-
Prevent injury, illness, and disability as a result of the spill and its consequences.
-
Monitor short- and long-term health consequences within affected populations.
-
Ensure care for those who need it, including behavioral health care, for spill-related problems.
-
Anticipate and mitigate problems that could arise.
To achieve these goals, federal agencies have been actively involved in a number of activities.
Disseminating Information on Health Risks
All federal agencies participating in the human health response have been disseminating information on the potential health risks associated with exposures to the oil spill.
Protecting Workers, Volunteers, and Residents
Several federal agencies are involved with worker, volunteer, and resident safety and protection, including the Coast Guard, OSHA, the
FDA, NOAA, NIOSH, and the Substance Abuse and Mental Health Services Administration (SAMHSA). For example, the Coast Guard is responsible for protecting Coast Guard personnel by monitoring exposures through established occupational safety and health programs; providing senior safety officials to assist other local, state, and federal clean-up efforts; ensuring port and tanker safety; monitoring the safe operation of all U.S. flag vessels and offshore facilities; and other activities. NIOSH has been providing interim guidance for protecting workers and volunteers. Additionally, the FDA and NOAA have been working together to test fish caught outside the closed fishing areas to ensure that the closed areas are sufficiently broad. The FDA also has increased its testing and inspection activities to ensure the safety of seafood harvested from the area.
Training Workers to Maximize Their Safety During Response Activities
Both the National Institutes of Health (NIH)’s National Institute of Environmental Health Sciences (NIEHS) and OSHA have been training workers. NIEHS has been providing recommendations on worker education and developing and translating training materials into relevant languages (e.g., Spanish and Vietnamese). OSHA has been distributing worker safety materials in multiple languages and auditing training sessions, as well as working with safety officials to protect workers from hazards such as chemical exposures, heat stress, and injuries.
Monitoring Exposures of Workers and the Public
In addition to exposure monitoring that the Coast Guard conducts as a regular part of its occupational health and safety program (see above), the EPA, OSHA, CDC’s National Center for Environmental Health (NCEH), and NIOSH have all been monitoring exposures. Most ongoing, federal-level environmental monitoring has been conducted through the EPA, with some assistance from NOAA. This includes monitoring air, water, sediment, and waste-streams samples along the shoreline and beyond for chemicals related to oil and dispersants in the air, water, and sediment (e.g., NOAA has been conducting aerial monitoring with NOAA P-3 aircraft), and monitoring the effects of dispersants in the sub-surface environment. The EPA regularly posts these data on its website. Additionally, OSHA has been monitoring worker exposures and posting
worker monitoring data on its website. NCEH has been working with the EPA to review air-monitoring data and identify potential health impacts on residents. NIOSH has been conducting health-hazard evaluations (worker health assessments and exposure characterizations).
Monitoring Public Health
The NIOSH, NCEH, the FDA, and SAMHSA are all involved with public health monitoring. NIOSH has been compiling worker rosters (i.e., administering surveys to 15,000 workers involved in the response); monitoring worker illness and injury (capturing all health symptoms that could be related to oil response work and ensuring that those reports are being evaluated by safety and health professionals); and collaborating with states, OSHA, and BP to identify acute and potential chronic health effects. NCEH has been helping the Gulf States collect surveillance data from health facilities and poison control centers (see the earlier summaries in this chapter of state-level surveillance activities). In the context of behavioral health-monitoring activities, SAMHSA is collecting baseline health data from impacted states, consulting nongovernmental partners about mental health and cultural issues, working with other federal agencies to ensure that behavioral needs are considered, and collaborating with states to facilitate access to behavioral health services.
Providing Medical Care
At the request of states, the Assistant Secretary for Preparedness and Response (ASPR)’s National Disaster Medical System (NDMS) has been providing medical care in needed areas. For example, at the time of the workshop, ASPR was providing sick-call/primary care support to responders and the local community in Venice, Louisiana.
Preparing for Long-Term Follow-Up
The NIH and the CDC are helping states prepare for long-term follow-up. For example, on June 15, 2010, NIH Director Francis Collins announced plans for a long-term cohort study of exposed workers and residents.
Department of Homeland Security
Alexander G. Garza, Office of Health Affairs
One of the main missions of the Office of Health Affairs is to work across federal agencies to ensure that Secretary of Homeland Security Janet Napolitano is aware of all health issues that affect national security. The Office of Health Affairs is also involved with workforce health protection and has been working closely with Rear Admiral Mark Tedesco.4 As Alexander Garza explained, Secretary Napolitano recently convened a meeting with all the various federal agency stakeholders (e.g., the CDC, OSHA, the EPA) to ensure that she understood how the Gulf oil spill’s potential effects on human health could impact national security. However, the Office of Health Affairs “owns” neither the medical response nor environmental monitoring. Rather, it views itself as a facilitator and a collaborator for the multiple agencies working on medical and health issues—an umbrella agency to bring all information together.
Environmental Protection Agency
Mathy V. Stanislaus, Office of Solid Waste and Emergency Response
As Mathy Stanislaus explained, the EPA has an extensive air-monitoring system in place, including mobile monitors circulating around the Gulf, to measure levels of various oil products (e.g., hydrocarbons) and dispersant constituents, (e.g., airplane monitors). Within a few days of the initial Deepwater Horizon explosion, the agency had gathered baseline data and has been conducting ongoing monitoring since then. At the time of the workshop, the EPA had no evidence of inhalational hazards either on the shore or at sea. The EPA has also been monitoring waste disposal. None of the waste being disposed in landfills had been identified as hazardous, although oil products were being sent to separate facilities. Additionally, the agency has been conducting dispersant toxicity tests to identify whether equally effective but less toxic dispersants could be used. The results of those tests were not available at the time of the workshop.
Finally, the EPA has been in regular communication with state and local governments, as well as nongovernmental organizations involved in the response, to ensure that the information gathered—including not just
what is known but also what is not known—is effectively communicated. Indeed, several times during the course of the workshop, participants commented on the usefulness of the EPA’s real-time air-monitoring information (www.epa.gov/BPSpill). The agency also worked with HHS to develop a fact sheet about odors that is also available on the EPA website.
Seeking a Public Health Approach Based on the Best Available Science: Remarks from the Surgeon General
Regina M. Benjamin, Surgeon General of the U.S. Public Health Service
Regina Benjamin elaborated on how the federal government is taking a public health approach toward the Deepwater Horizon disaster. By identifying the issues, the federal government can better treat and mitigate existing health problems and prevent similar conditions in the future. In addition to a multitude of public health experts, veterinarians, engineers, and other professionals working throughout other government agencies (e.g., the CDC, the FDA, the Health Resources and Services Administration [HRSA], the NIH, and SAMSHA) to address the public health problems at hand, U.S. Public Health Service Commission Corps officers were deployed to the Gulf region on May 27, 2010. Local Medical Research Corps volunteers also are working with the affected communities and achieving a comfort level that would take outside groups months to achieve.
Like many other participants, Benjamin recognized the needs of people who are not only just losing their jobs, but also their livelihoods and ways of life that have been part of the Gulf region for generations. She referred to the central role that the seafood industry, water sports industry, and subsistence fishing play in Gulf residents’ lives. Having grown up in the Gulf region, Benjamin stated, “The water is really a part of our lives ... it’s really in our blood.” She described her personal connection to the Gulf region, including her childhood in Daphne Bay, Alabama, where her family’s homestead has been since the early 1800s; her education at Xavier and Tulane Universities; and her 23-year private family practice in Bayou La Batre, Alabama. She echoed other participants’ comments about how the Gulf oil disaster is delivering a “new blow” to Bayou La Batre, which is only just recovering from Hurricane Katrina.
Finally, Benjamin remarked that her job as U.S. Surgeon General is to provide trustworthy information that is based on the best available science and to clearly communicate how the disaster is going to affect both short- and long-term health. However, the current scientific literature is inconclusive with regard to the potential hazards resulting from the oil spill, with some scientists predicting little to no toxic effect and others expressing serious concerns about the potential short- and long-term effects on responders’ and residents’ health. She ended with a quote from President Barack Obama: “Science is more essential for our prosperity, our security, our health, our environment, and our quality of life than it has ever been before.”


















