
GOAL: Promote age-appropriate sleep durations among young children.
The obesity epidemic has been paralleled by a similar epidemic of sleep deprivation. Over the past 40 years, daily sleep duration among adults has decreased by 1–2 hours, and the proportion of adults getting less than 7 hours of sleep has more than doubled, from 15 percent to 39 percent (NSF, 2008). Evidence also suggests a decrease in sleep duration across infancy, childhood, and adolescence ranging from 30 to 60 minutes over the past 20 years, due largely to later bedtimes, with the most pronounced decreases seen among children under 3 years of age (Dollman et al., 2007; Iglowstein et al., 2003). Recent studies also suggest that the quality of sleep among young children is too often compromised (NSF, 2008) and that pediatric sleep disturbances frequently become chronic, with few children outgrowing the problem (Kataria et al., 1987; Pollock, 1994). As with obesity, racial/ethnic minority populations in particular experience insufficient sleep across their life span, starting in infancy (Nevarez et al., 2010) and continuing into childhood (Spilsbury et al., 2004) and adulthood (CDC, 2009; Lauderdale et al., 2006).
Mounting epidemiologic evidence indicates that short duration of sleep is a risk factor for obesity, type 2 diabetes, coronary heart disease, hyperten-
sion, and all-cause mortality in adults independently of other measured risk factors (Ayas et al., 2003; Gangwisch et al., 2006; King et al., 2008; Patel and Hu, 2008; Williams et al., 2007). A similar inverse association between sleep duration and obesity has been observed in cross-sectional studies of older children and adolescents (Chaput et al., 2006; Eisenmann et al., 2006; Kagamimori et al., 1999; Sekine et al., 2002; von Kries et al., 2002) and increasingly in longitudinal studies, including those of infants and children under age 5 (Agras et al., 2004; Bell and Zimmerman, 2010; Landhuis et al., 2008; Reilly et al., 2005; Snell et al., 2007; Taveras et al., 2008). Nonetheless, several aspects of the relationship between sleep and obesity are not yet sufficiently understood to inform clear policy recommendations beyond those that support the promotion of age-appropriate sleep durations. This chapter summarizes the evidence linking insufficient sleep to childhood obesity and provides recommendations to support the goal of promoting age-appropriate sleep durations for young children. To support and complement the first recommendation on requiring child care providers to adopt practices that promote age-appropriate sleep durations, the second recommendation addresses training for health and education professionals on how to counsel parents about this issue.
Recommendation 6-1: Child care regulatory agencies should require child care providers to adopt practices that promote age-appropriate sleep durations among young children.
Potential actions include
- creating environments that ensure restful sleep, such as no screen media in rooms where children sleep and low noise and light levels during napping;
- encouraging sleep-promoting behaviors and practices, such as calming nap routines;
- encouraging practices that promote child self-regulation of sleep, including putting infants to sleep drowsy but awake; and
- seeking consultation yearly from an expert on healthy sleep durations and practices.
Recommendation 6-2: Health and education professionals should be trained in how to counsel parents about their children’s age-appropriate sleep durations.
Rationale
Evidence suggests that among children under 2 years of age, 12 or more hours of sleep in a 24-hour period is protective of obesity at age 3. Among children aged 2–5, 11 or more hours of sleep has been found to be associated with lower obesity risk. Age-appropriate sleep durations from the National Sleep Foundation include (NSF, 2011)
- newborns, less than 3 months: 10.5–18 hours in a 24-hour period;
- infants, 3 months to <12 months: 9–12 hours during the night and 30-minute to 2 hour naps one to four times a day;
- toddlers, 1 year to <3 years: 12–14 hours in a 24-hour period; and
- preschoolers, 3 years to <5 years: 11–13 hours in a 24-hour period.
Evidence suggests an inverse association between sleep duration and obesity in children (Agras et al., 2004; Bell and Zimmerman, 2010; Landhuis et al., 2008; Reilly et al., 2005; Taveras et al., 2008). All published studies have reported an association between shorter sleep duration and increased obesity risk in children across the pediatric age range (Cappuccio et al., 2008; Chen et al., 2008; Patel and Hu, 2008).
One of the largest studies involved a Japanese birth cohort of 8,274 children. At ages 6 to 7, the odds ratios for obesity were 1.49, 1.89, and 2.87 for those sleeping 9–10, 8–9, and less than 8 hours, respectively, compared with those obtaining at least 10 hours of sleep and after adjusting for sex, parental obesity, and other lifestyle factors (Sekine et al., 2002). Similar findings have been reported from Portugal (Padez et al., 2005), Spain (Vioque et al., 2000), France (Locard et al., 1992), and Germany (von Kries et al., 2002). Prospectively, a UK study of 8,234 children showed that sleep duration at age 38 months predicted obesity at age 7, with odds ratios of 1.45, 1.35, and 1.04 for children sleeping less than 10.5, 10.5–10.9, and 11.0–11.9 hours, respectively, compared with those sleeping at least 12 hours (Reilly et al., 2005). In another study, 4-year-old children who slept less than 10.5 hours per weekday night had elevated odds of obesity compared with children who slept at least 10.5 hours (Anderson and Whitaker, 2010). Short sleep duration has been associated with increased television viewing and reduced participation in organized sports (Locard et al., 1992; Taveras et al., 2008; von Kries et al., 2002).
Poor sleep routines have also been associated with obesity in children. In one study, irregular sleeping habits between 2 and 4 years of age were associated
with elevated body mass index (BMI) and prevalence of obesity at age 21 (Mamun et al., 2007).
Three longitudinal studies have examined the relationship between insufficient sleep during infancy and early childhood and later weight gain. In a study of 915 children aged 0–3, infant sleep of less than 12 hours per day was associated with higher BMI Z-score, higher adiposity, and increased odds of obesity (Taveras et al., 2008). In a second study, parental reports of sleep duration were negatively correlated with weight for length at age 6 months (Tikotzky et al., 2010). Finally, Bell and Zimmerman (2010) found that for children younger than age 4 at baseline, short duration of nighttime sleep was strongly associated with increased risk of overweight or obesity at follow-up. Daytime napping was not a substitute for nighttime sleep and had little effect on obesity risk. Bell and Zimmerman also found that sleep duration was not associated with subsequent weight status among children who were older at baseline (e.g., aged 5–13). These studies among young children suggest that early childhood is a developmental period when sleep behaviors may particularly influence obesity risk.
Insufficient sleep may affect obesity and metabolic dysfunction through a variety of pathways. Short-term experimental studies in adults show that sleep restriction is associated with physiologic mechanisms that may increase the risk of adiposity and cardio-metabolic disorders (Patel and Hu, 2008). Basic laboratory studies of experimental sleep restriction have shown effects that include increases in hunger and appetite scores, increased snacking, reduced leptin, and insulin resistance (Nedeltcheva et al., 2009; Spiegel et al., 2004a,b). Sleep restriction also has been associated with elevated sympathovagal balance; hypercortisolemia (Spiegel et al., 2004a); elevated C-reactive protein; and increased secretion of pro-inflammatory cytokines (Vgontzas et al., 2004), which may relate to the association between short sleep duration and adverse cardio-metabolic outcomes, including hypertension (Gottlieb et al., 2006) and insulin resistance.
A few studies suggest that sleep curtailment may increase energy intake through influences on eating behavior and diet. In one study of normal-weight adults, for example, short sleep duration was found to be associated with increased hunger and greater desire to eat calorie-dense foods with high carbohydrate content (Spiegel et al., 2004b). Sleep restriction also may lead to increased time spent in sedentary activities, such as television viewing, when snacking is common (Sivak, 2006). In addition, chronic sleep deprivation can lead to feelings of fatigue, which may lead to reduced physical activity (Patel and Hu, 2008). Studies in humans suggest further that circadian misalignment can contribute to
metabolic dysfunction (Scheer et al., 2009). Molecular circadian clocks exist in almost all tissues and contribute to the coordination of gene transcription involved in a range of metabolic processes (Ko and Takahashi, 2006). Studies show that central and peripheral circadian molecular clocks interact to achieve appropriate internal alignment of metabolic signaling, as well as external alignment of cellular processes with the environment.
The existing literature on this subject has important limitations. Most of the studies examining mechanisms relating sleep and adverse outcomes have been conducted among adults, and most but not all (Chaput et al., 2008; Taheri et al., 2004) of them rely on short-term experimental work.
The early childhood period is a time when sleep problems are highly prevalent (Sadeh and Sivan, 2009), and are associated with multiple adverse outcomes for the child, including obesity (Taveras et al., 2008; Thunstrom, 1999, 2002), and with maternal depression and parenting stress (Wake et al., 2006). While much is known about the role of parental behavior and cognition in influencing infant sleep, less is known about the social and environmental context (Sadeh et al., 2010; Tikotzky and Sadeh, 2009). Poor sleep among children may be due to primary sleep disorders such as sleep apnea. Most commonly, however, poor sleep is due to a host of behavioral and environmental factors, collectively referred to as “poor sleep hygiene” (Mindell et al., 2009). These include sleep habits that reduce sleep quality and impair sleep duration, such as irregular bed and wake times, use of caffeine or other stimulating substances before bedtime, inappropriate napping habits, engagement in stimulating or stressful activities close to bedtime, and sleep environments that are uncomfortable or disruptive. Reduced childhood sleep also reflects differences in parental behavior (Acebo et al., 2005; Sadeh et al., 2007, 2009; Tikotzky and Sadeh, 2009) and environmental exposures, including the presence of a television in the bedroom (Mindell et al., 2009).
In addition to obesity, insufficient sleep and secondary daytime sleepiness may impact neurocognitive functioning; increase behavioral problems, including aggression; and affect mood (Cao and Guilleminault, 2008; Gregory et al., 2008). During the past 15 years, sleep researchers have shown that sleep disorders can lead to a clinical presentation that mimics attention-deficit/hyperactivity disorder (Chervin et al., 1997, 2003). In addition, Gregory and colleagues (2008) observed more than 2,000 children aged 4–16 and later at ages 18–32 and found a strong link between sleep problems and the development of behavioral difficulties later in life.
Box 6-1
Case Study: Sleeping and Intake Methods Taught to Infants and Mothers Early in Life (SLIMTIME)
SLIMTIME was a pilot study of 160 mother–infant dyads. With a 2 x 2 design, 160 dyads were randomized into one of four treatment cells to receive two, one, or no interventions delivered during two nurse home visits. The first intervention (“Soothe/Sleep”) was delivered by a research nurse at the first home visit, which occurred between 2 and 3 weeks after birth. Parents randomized to receive the “Soothe/Sleep” intervention were taught alternatives to feeding as an indiscriminate first response to infant distress. The use of alternative soothing techniques afforded nonhungry infants opportunities to experience being soothed without being fed and to learn to self-soothe and return to sleep without a feeding. In addition to one-on-one instruction, participating mothers were given an instructional handout and a commercially produced video, “The Happiest Baby on the Block.” The video details a process to help calm and soothe infants with strategies that can be applied during the day and at night when it is time for sleep. Briefly, the process includes instructions and demonstrations using five soothing techniques: (1) swaddling, (2) side or stomach position while awake, (3) shushing, (4) swinging, and (5) sucking. Other instructions included in the “Soothe/Sleep” intervention taught parents to emphasize day/night environmental differences and to respond to nocturnal awakenings with other soothing and care-taking responses, such as diaper changing before feeding. All study participants received a standard infant parenting book that included traditional advice on handling night awakenings, including feeding, rocking, and checking for a dirty diaper.
At 1 year, a significant effect of the intervention was seen on nocturnal sleep for predominantly breastfed infants, with breastfed dyads in the “Soothe/Sleep” groups showing significantly more sleep than controls (P = 0.04; see the figure on the next page). At 1 year, infants who had received both interventions had lower weight-for-length percentiles (P = 0.009) than the control group. This study suggests that a multicomponent behavioral intervention that includes sleep improvement may hold promise for long-term obesity prevention.
Despite the increasing evidence relating sleep duration and obesity, the urgent need to decrease the prevalence of childhood obesity, and the availability of efficacious behavioral interventions to prevent and treat childhood sleep problems (Mindell et al., 2006), few interventions have been undertaken to improve early childhood sleep to prevent obesity (Paul et al., 2011; Taveras
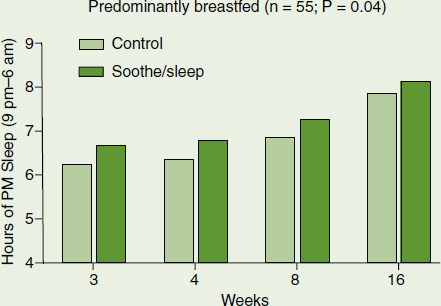
FIGURE 6-1 Effect of “Soothe/Sleep” intervention on nocturnal sleep duration among breastfed infants.
SOURCE: Paul et al., 2010.
et al., 2010). One study reviewed 52 behavioral treatment programs for bedtime problems and night waking. Mindell and colleagues (2006) found that behavioral therapies and preventive parental education on healthy sleep habits for children were efficacious in demonstrating clinically significant improvements in child sleep. The authors also call for more research to examine various delivery methods for treatment, develop objective measures of sleep duration, and establish the long-term efficacy of existing interventions. Two recent pilot interventions among mother–infant dyads in the first year of life have attempted to improve early childhood sleep to promote healthy infant growth and prevent overweight (Paul et al., 2011; Taveras et al., 2010). These two interventions are described in Boxes 6-1 and 6-2.
Box 6-2
Case Study: First Steps for Mommy and Me: A Pilot Intervention to Improve Sleep Behaviors of Postpartum Mothers and Their Infants
First Steps for Mommy and Me was a pilot intervention to assess the feasibility of a pediatric primary care–based intervention aimed at promoting healthy sleep behaviors among infants aged 0–6 months and their mothers. Sixty mother–infant pairs were assigned to the intervention groups and 24 to the control group. Mothers in the intervention groups received (1) brief focused negotiation by pediatricians, (2) motivational counseling by a health educator, and (3) group parenting workshops. They received developmentally appropriate counseling from their pediatrician and the health educator on ways to promote infant self-regulation of sleep, including avoiding sleep associations (e.g., putting infants in their crib drowsy but awake, avoiding relying on an external cue such as nursing for the infant to fall asleep); using alternative soothing methods for crying infants; and implementing healthy sleep habits, such as a calming bedtime routine.
At 6 months, compared with control infants, intervention infants had greater increases in their nocturnal sleep duration from baseline to follow-up (mean increase 1.9 versus 1.3 hours/day; p = 0.05); greater reductions in settling time (mean reduction –0.70 versus –0.10 hours/day; p = 0.02); and greater reductions in hours/day of nighttime wakefulness (mean reduction –2.9 versus –1.5 hours/day; p = 0.08). In addition, fewer intervention infants were in the highest quartile of weight-for-length Z-score at age 6 months (22 percent versus 42 percent; p = 0.06). The study findings suggest that the program of brief focused negotiation by pediatricians, individual coaching by a health educator using motivational interviewing, and group parenting workshops tended to improve infant sleep behaviors and that such a program may prevent excess infant weight gain.
SOURCE: Taveras et al., 2010.
Acebo, C., A. Sadeh, R. Seifer, O. Tzischinsky, A. Hafer, and M. A. Carskadon. 2005. Sleep/wake patterns derived from activity monitoring and maternal report for healthy 1- to 5-year-old children. Sleep 28(12):1568-1577.
Agras, W. S., L. D. Hammer, F. McNicholas, and H. C. Kraemer. 2004. Risk factors for childhood overweight: A prospective study from birth to 9.5 years. Journal of Pediatrics 145(1):20-25.
Anderson, S. E., and R. C. Whitaker. 2010. Household routines and obesity in US preschool-aged children. Pediatrics 125(3):420-428.
Ayas, N. T., D. P. White, W. K. Al-Delaimy, J. E. Manson, M. J. Stampfer, F. E. Speizer, S. Patel, and F. B. Hu. 2003. A prospective study of self-reported sleep duration and incident diabetes in women. Diabetes Care 26(2):380-384.
Bell, J. F., and F. J. Zimmerman. 2010. Shortened nighttime sleep duration in early life and subsequent childhood obesity. Archives of Pediatrics and Adolescent Medicine 164(9):840-845.
Cao, M., and C. Guilleminault. 2008. Sleep difficulties and behavioral outcomes in children. Archives of Pediatrics and Adolescent Medicine 162(4):385-389.
Cappuccio, F. P., F. M. Taggart, N. B. Kandala, A. Currie, E. Peile, S. Stranges, and M. A. Miller. 2008. Meta-analysis of short sleep duration and obesity in children and adults. Sleep 31(5):619-626.
CDC (Centers for Disease Control and Prevention). 2009. Perceived insufficient rest or sleep among adults—United States, 2008. Morbidity and Mortality Weekly Report 58(42):1175-1179.
Chaput, J. P., M. Brunet, and A. Tremblay. 2006. Relationship between short sleeping hours and childhood overweight/obesity: Results from the “Quebec en Forme” Project. International Journal of Obesity 30(7):1080-1085.
Chaput, J. P., J. P. Despres, C. Bouchard, and A. Tremblay. 2008. The association between sleep duration and weight gain in adults: A 6-year prospective study from the Quebec Family Study. Sleep 31(4):517-523.
Chen, X. L., M. A. Beydoun, and Y. F. Wang. 2008. Is sleep duration associated with childhood obesity? A systematic review and meta-analysis. Obesity 16(2):265-274.
Chervin, R. D., J. E. Dillon, C. Bassetti, D. A. Ganoczy, and K. J. Pituch. 1997. Symptoms of sleep disorders, inattention, and hyperactivity in children. Sleep 20(12):1185-1192.
Chervin, R. D., J. E. Dillon, K. H. Archbold, and D. L. Ruzicka. 2003. Conduct problems and symptoms of sleep disorders in children. Journal of the American Academy of Child and Adolescent Psychiatry 42(2):201-208.
Dollman, J., K. Ridley, T. Olds, and E. Lowe. 2007. Trends in the duration of school-day sleep among 10- to 15-year-old south Australians between 1985 and 2004. Acta Paediatrica 96(7):1011-1014.
Eisenmann, J. C., P. Ekkekakis, and M. Holmes. 2006. Sleep duration and overweight among Australian children and adolescents. Acta Paediatrica 95(8):956-963.
Gangwisch, J. E., S. B. Heymsfield, B. Boden-Albala, R. M. Buijs, F. Kreier, T. G. Pickering, A. G. Rundle, G. K. Zammit, and D. Malaspina. 2006. Short sleep duration as a risk factor for hypertension: Analyses of the first National Health and Nutrition Examination Survey. Hypertension 47(5):833-839.
Gottlieb, D. J., S. Redline, F. J. Nieto, C. M. Baldwin, A. B. Newman, H. E. Resnick, and N. M. Punjabi. 2006. Association of usual sleep duration with hypertension: The Sleep Heart Health Study. Sleep 29(8):1009-1014.
Gregory, A. M., J. Van der Ende, T. A. Willis, and F. C. Verhulst. 2008. Parent-reported sleep problems during development and self-reported anxiety/depression, attention problems, and aggressive behavior later in life. Archives of Pediatrics and Adolescent Medicine 162(4):330-335.
Iglowstein, I., O. G. Jenni, L. Molinari, and R. H. Largo. 2003. Sleep duration from infancy to adolescence: Reference values and generational trends. Pediatrics 111(2):302-307.
Kagamimori, S., T. Yamagami, S. Sokejima, N. Numata, K. Handa, S. Nanri, T. Saito, N. Tokui, T. Yoshimura, and K. Yoshida. 1999. The relationship between lifestyle, social characteristics and obesity in 3-year-old Japanese children. Child Care Health Development 25(3):235-247.
Kataria, S., M. S. Swanson, and G. E. Trevathan. 1987. Persistence of sleep disturbances in preschool children. Journal of Pediatrics 110(4):642-646.
King, C. R., K. L. Knutson, P. J. Rathouz, S. Sidney, K. Liu, and D. S. Lauderdale. 2008. Short sleep duration and incident coronary artery calcification. Journal of the American Medical Association 300(24):2859-2866.
Ko, C. H., and J. S. Takahashi. 2006. Molecular components of the mammalian circadian clock. Human Molecular Genetics 15(Spec. No. 2):R271-R277.
Landhuis, C. E., R. Poulton, D. Welch, and R. J. Hancox. 2008. Childhood sleep time and long-term risk for obesity: A 32-year prospective birth cohort study. Pediatrics 122(5):955-960.
Lauderdale, D. S., K. L. Knutson, L. L. Yan, P. J. Rathouz, S. B. Hulley, S. Sidney, and K. Liu. 2006. Objectively measured sleep characteristics among early-middle-aged adults: The Cardia Study. American Journal of Epidemiology 164(1):5-16.
Locard, E., N. Mamelle, A. Billette, M. Miginiac, F. Munoz, and S. Rey. 1992. Risk factors of obesity in a five year old population. Parental versus environmental factors. International Journal of Obesity and Related Metabolic Disorders 16(10):721-729.
Mamun, A. A., D. A. Lawlor, S. Cramb, M. O’Callaghan, G. Williams, and J. Najman. 2007. Do childhood sleeping problems predict obesity in young adulthood? Evidence from a prospective birth cohort study. American Journal of Epidemiology 166(12):1368-1373.
Mindell, J. A., B. Kuhn, D. S. Lewin, L. J. Meltzer, and A. Sadeh. 2006. Behavioral treatment of bedtime problems and night wakings in infants and young children. Sleep 29(10):1263-1276.
Mindell, J. A., L. J. Meltzer, M. A. Carskadon, and R. D. Chervin. 2009. Developmental aspects of sleep hygiene: Findings from the 2004 National Sleep Foundation Sleep in America Poll. Sleep Medicine 10(7):771-779.
Nedeltcheva, A. V., L. Kessler, J. Imperial, and P. D. Penev. 2009. Exposure to recurrent sleep restriction in the setting of high caloric intake and physical inactivity results in increased insulin resistance and reduced glucose tolerance. Journal of Clinical Endocrinology and Metabolism 94(9):3242-3250.
Nevarez, M. D., S. L. Rifas-Shiman, K. P. Kleinman, M. W. Gillman, and E. M. Taveras. 2010. Associations of early life risk factors with infant sleep duration. Academic Pediatrics 10(3):187-193.
NSF (National Sleep Foundation). 2008. Sleep in America. http://www.sleepfoundation.org/sites/default/files/2008%20POLL%20SOF.PDF (accessed May 13, 2011).
NSF. 2011. Children and Sleep. http://www.sleepfoundation.org/article/sleep-topics/children-and-sleep (accessed May 13, 2011).
Padez, C., I. Mourao, P. Moreira, and V. Rosado. 2005. Prevalence and risk factors for overweight and obesity in Portuguese children. Acta Paediatrica 94(11):1550-1557.
Patel, S. R., and F. B. Hu. 2008. Short sleep duration and weight gain: A systematic review. Obesity 16(3):643-653.
Paul, I. M., J. S. Savage, S. L. Anzman, J. S. Beiler, M. E. Marini, J. L. Stokes, and L. L. Birch. 2011. Preventing obesity during infancy: A pilot study. Obesity (Silver Spring, Md.) 19(2):353-361.
Pollock, J. I. 1994. Night-waking at five years of age: Predictors and prognosis. Journal of Child Psychology and Psychiatry and Allied Disciplines 35(4):699-708.
Reilly, J. J., J. Armstrong, A. R. Dorosty, P. M. Emmett, A. Ness, I. Rogers, C. Steer, and A. Sherriff. 2005. Early life risk factors for obesity in childhood: Cohort study. British Medical Journal 330(7504):1357-1359.
Sadeh, A., and Y. Sivan. 2009. Clinical practice: Sleep problems during infancy. European Journal of Pediatrics 168(10):1159-1164.
Sadeh, A., E. Flint-Ofir, T. Tirosh, and L. Tikotzky. 2007. Infant sleep and parental sleep-related cognitions. Journal of Family Psychology 21(1):74-87.
Sadeh, A., L. Tikotzky, and A. Scher. 2010. Parenting and infant sleep. Sleep Medicine Reviews 14(2):89-96.
Scheer, F. A., M. F. Hilton, C. S. Mantzoros, and S. A. Shea. 2009. Adverse metabolic and cardiovascular consequences of circadian misalignment. Proceeding of the National Academy of Sciences 106(11):4453-4458.
Sekine, M., T. Yamagami, K. Handa, T. Saito, S. Nanri, K. Kawaminami, N. Tokui, K. Yoshida, and S. Kagamimori. 2002. A dose-response relationship between short sleeping hours and childhood obesity: Results of the Toyama Birth Cohort Study. Child: Care, Health and Development 28(2):163-170.
Sivak, M. 2006. Sleeping more as a way to lose weight. Obesity Reviews 7(3):295-296.
Snell, E. K., E. K. Adam, and G. J. Duncan. 2007. Sleep and the body mass index and overweight status of children and adolescents. Child Development 78(1):309-323.
Spiegel, K., R. Leproult, M. L’Hermite-Baleriaux, G. Copinschi, P. D. Penev, and E. Van Cauter. 2004a. Leptin levels are dependent on sleep duration: Relationships with sympathovagal balance, carbohydrate regulation, cortisol, and thyrotropin. Journal of Clinical Endocrinology and Metabolism 89(11):5762-5771.
Spiegel, K., E. Tasali, P. Penev, and E. Van Cauter. 2004b. Brief communication: Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite. Annals of Internal Medicine 141(11): 846-850.
Spilsbury, J. C., A. Storfer-Isser, D. Drotar, C. L. Rosen, L. H. Kirchner, H. Benham, and S. Redline. 2004. Sleep behavior in an urban US sample of school-aged children. Archives of Pediatrics and Adolescent Medicine 158(10):988-994.
Taheri, S., L. Lin, D. Austin, T. Young, and E. Mignot. 2004. Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS Medicine 1(3):e62.
Taveras, E. M., S. L. Rifas-Shiman, E. Oken, E. P. Gunderson, and M. W. Gillman. 2008. Short sleep duration in infancy and risk of childhood overweight. Archives of Pediatrics and Adolescent Medicine 162(4):305-311.
Taveras, E. M., K. Blackburn, M. W. Gillman, J. Haines, J. McDonald, S. Price, and E. Oken. 2010. First steps for mommy and me: A pilot intervention to improve nutrition and physical activity behaviors of postpartum mothers and their infants. Maternal and Child Health Journal October 19 [Epub ahead of print].
Thunstrom, M. 1999. Severe sleep problems among infants in a normal population in Sweden: Prevalence, severity and correlates. Acta Paediatrica 88(12):1356-1363.
Thunstrom, M. 2002. Severe sleep problems in infancy associated with subsequent development of attention-deficit/hyperactivity disorder at 5.5 years of age. Acta Paediatrica 91(5):584-592.
Tikotzky, L., and A. Sadeh. 2009. Maternal sleep-related cognitions and infant sleep: A longitudinal study from pregnancy through the 1st year. Child Development 80(3):860-874.
Tikotzky, L., G. de Marcas, J. Har-Toov, S. Dollberg, Y. Bar-Haim, and A. Sadeh. 2010. Sleep and physical growth in infants during the first 6 months. Journal of Sleep Research 19(1 Pt. 1):103-110.
Vgontzas, A. N., E. Zoumakis, E. O. Bixler, H. M. Lin, H. Follett, A. Kales, and G. P. Chrousos. 2004. Adverse effects of modest sleep restriction on sleepiness, performance, and inflammatory cytokines. Journal of Clinical Endocrinology and Metabolism 89(5):2119-2126.
Vioque, J., A. Torres, and J. Quiles. 2000. Time spent watching television, sleep duration and obesity in adults living in Valencia, Spain. International Journal of Obesity and Related Metabolic Disorders 24(12):1683-1688.
von Kries, R., A. M. Toschke, H. Wurmser, T. Sauerwald, and B. Koletzko. 2002. Reduced risk for overweight and obesity in 5- and 6-y-old children by duration of sleep—a cross-sectional study. International Journal of Obesity and Related Metabolic Disorders 26(5):710-716.
Wake, M., E. Morton-Allen, Z. Poulakis, H. Hiscock, S. Gallagher, and F. Oberklaid. 2006. Prevalence, stability, and outcomes of cry-fuss and sleep problems in the first 2 years of life: Prospective community-based study. Pediatrics 117(3):836-842.
Williams, C. J., F. B. Hu, S. R. Patel, and C. S. Mantzoros. 2007. Sleep duration and snoring in relation to biomarkers of cardiovascular disease risk among women with type 2 diabetes. Diabetes Care 30(5):1233-1240.














