Over the past century the major causes of morbidity and mortality in the United States have shifted from those related to communicable diseases to those due to chronic diseases. Just as the major causes of morbidity and mortality have changed, so too has understanding of health and what makes people healthy or ill. Research has documented the importance of the social determinants of health (for example, socioeconomic status and education), which affect health directly as well as through their impact on other health determinants such as risk factors. Targeting interventions toward the conditions associated with today’s challenges to living a healthy life requires an increased emphasis on the factors that affect the current causes of morbidity and mortality, factors such as the social determinants of health. Many community-based prevention interventions target such conditions.
Community-based prevention interventions offer three distinct strengths. First, because the intervention is implemented population-wide it is inclusive and not dependent on access to the health care system. Second, by directing strategies at an entire population an intervention can reach individuals at all levels of risk. And finally, some lifestyle and behavioral risk factors are shaped by conditions not under an individual’s control. For example, encouraging an individual to eat healthy food when none is accessible undermines the potential for successful behavioral change. Community-based prevention interventions can be designed to affect environmental and social conditions that are out of the reach of clinical services.
When a person is ill, making a case for policies and programs to avoid further deterioration of health or death seems reasonable. However,
prevention requires that before someone becomes sick, society invest the financial and other resources necessary to make the required changes in individual and community life associated with preventing illness. Some of the persons who receive the intervention would never become sick, yet they share the costs of the intervention. These certain costs of improving health often outweigh the perceived benefits of community-based prevention, especially if individuals perceive their own risk of illness as low.
Four foundations—the California Endowment, the de Beaumont Foundation, the Robert Wood Johnson Foundation, and the W.K. Kellogg Foundation—asked the Institute of Medicine to convene an expert committee to develop a framework for assessing the value of community-based, non-clinical prevention policies and wellness strategies, especially those targeting the prevention of long-term, chronic diseases. The charge to the committee was further defined as follows:
- Define “community-based, non-clinical prevention policy and wellness strategies.”
- Define “value” for community-based, non-clinical prevention policy and wellness strategies.
- Analyze current frameworks used to assess the value of community-based, non-clinical prevention policies and wellness strategies, including
- the methodologies and measures used and
- the short- and long-term impacts of such prevention policy and wellness strategies on communities, including health care spending and public health.
- If warranted, propose a new framework or frameworks that capture the breadth and complexity of community-based, non-clinical prevention policies and wellness strategies, including interventions that target specific behaviors and health outcomes.
The framework should
- consider the sources of data that are needed and available;
- consider the concepts of generalization, scaling up, and sustainability of programs; and
- address national and state policy implications associated with implementing the framework.
DEFINITIONS
One of the first tasks facing the committee was defining the terms related to its charge. The phrase “community-based, non-clinical prevention
policy and wellness strategies” appears in the Statement of Task. This phrase has been shortened for purposes of this report to community-based prevention. The committee concluded that community-based prevention interventions are population-based interventions that are aimed at preventing the onset of disease, stopping or slowing the progress of disease, reducing or eliminating the negative consequences of disease, increasing healthful behaviors that result in improvements in health and well-being, or decreasing disparities that result in an inequitable distribution of health. The committee also concluded that, in addition to a focus on population health, community-based prevention interventions also may address changes in the social and physical environment, involve intersectoral action, highlight community participation and empowerment, emphasize context, or include a systems approach.
The committee uses the term community to mean any group of people who share geographic space, interests, goals, or history. A further discussion of community can be found in Chapter 2.
The value of an intervention, for purposes of this report, is defined as its benefits minus its harms and costs. There are expanded discussions of the concept of value at the end of Chapter 1 and in Chapter 4.
The committee concluded that a framework for assessing value is a structure for gathering and processing information to aid intelligent decision making and, more specifically, to help decide whether an activity or intervention is worthwhile. A framework for assessing value can aid decision making by
- requiring that goals be stated clearly;
- integrating incomplete and sometimes conflicting information and beliefs;
- avoiding decision making based on arbitrary impressions or self-interest;
- clarifying trade-offs;
- promoting transparency; and
- identifying and helping to work through legitimate sources of disagreement.
DOMAINS OF VALUE
The committee was asked to develop a framework for assessing the value of community-based prevention. Clearly, a major outcome of community-based prevention is its impact on health. However, because of the way in which community-based prevention is designed and developed (e.g., often to address the social and environmental determinants of health), the impacts of these interventions can go beyond health effects. Therefore,
a framework for valuing community-based prevention needs to take into account not only the outcomes in the domain of health, but also outcomes in areas other than health. A framework that does not take into account and value non-health outcomes would be counting all the costs but not all the benefits, thereby providing an inaccurate and inadequate picture of the value of community-based prevention. Decision makers, funders, and stakeholders will all benefit from an approach that looks not just at health impacts, but at other impacts as well, and thus assesses the true value of community-based prevention.
The committee concluded that the outcomes of community-based prevention interventions can be divided into three distinct but interrelated categories, or domains of value: health, community well-being, and community process. The committee is aware that health is a component of well-being but for the purposes of this report the health component is separated from other elements of community well-being because health is a particular outcome of interest. By valuing these domains one can account for all of the potential harms and benefits of community-based prevention interventions as well as the possible savings and costs associated with the interventions. Chapter 3 provides an in-depth exploration of each of these domains of value; a brief summary is provided below. Many elements in each of the domains can be valued, and the ones selected will depend on the intervention of interest and on its implementation. The committee has identified one element—equity—that crosses all three domains.
The domain of health (both physical and mental) includes changes in the incidence and prevalence of disease, declines in mortality, and increases in health-related quality of life. More specifically, measures of physical health include mortality, morbidity, and functional capability. Measures of mental health include cognition, individual resilience or emotional reserves, mortality from such causes as suicide, morbidity (e.g., depression), and socio-emotional health-related quality of life (e.g., stress, behaviors, injuries, and perceptions of health).
Community well-being includes social norms, how people relate to each other and to their surroundings, and how much investment they are willing to make in themselves and in the people around them. Elements of community well-being include wealth and income, education, employment, crime, transportation, housing, worksites, food, social support and social networks, and health care, among others. These elements are produced, reproduced, and transformed by the practice of individuals in the community. Community well-being includes the physical as well as the social and economic environments that affect the health of individuals and populations, directly and indirectly.
The domain of community process includes local leadership development, skill building, civic engagement or participation, community
representation, and community history, among others. Community processes typically have a sequence of activities that incorporate learning about various options available for health improvement, deliberations associated with the selection of one or more options, consideration of the appropriate methods to implement the health improvement initiatives, and critical reflection on the entire process. Not only can the way that decisions are made and carried out be important to the success of a program or policy—and thus to community well-being—it can also have a direct impact on well-being through benefits of broad participation and buy-in to decisions.
FRAMEWORK FOR VALUING
The committee concluded that a framework for valuing community-based prevention programs and policies should meet at least three criteria. First, the framework should account for benefits and harms in the three domains of health, community well-being, and community process. Community-based prevention can create value not only through improvements in the health of individuals but also by increasing the investment that individuals are willing and able to make in themselves, in their family and neighbors, and in their environment. Furthermore, community-based prevention involves decisions among groups of people about how to live in society, how the physical environment is built, what food is served in schools, and so on. Thus, the process by which interventions are decided upon and undertaken needs to be treated as a valued outcome. If a community decides to tell people what they can or cannot do, or what they should or should not do, the decisions need to have the legitimacy—the added value—that comes from an open and inclusive group decision-making process.
Second, the framework should consider the resources used and compare benefits and harms with those resources. To make that comparison and to compare different interventions with each other, it is essential to know not just that some benefit is likely but also the magnitude of the benefits and of the associated costs for each intervention.
Finally, the framework needs to be sensitive to differences among communities and to take them into account in valuing community-based prevention. In part, this reflects the reality that, because communities vary so much in their characteristics, the causal links between interventions and valued outcomes may be different for different communities.
None of the frameworks analyzed by the committee meets the criteria described above. (For a detailed discussion of the analysis, see Chapter 4.) Therefore, the committee concluded that a new framework was needed to assess the value of community-based prevention interventions.
The goals of the framework (Figure S-1) proposed by the committee are (1) to incorporate the full scope of benefits into the value of interventions,
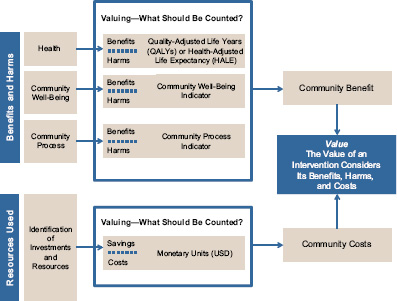
FIGURE S-1 Conceptual framework for valuing community-based prevention interventions.
so that in addition to health benefits and harms, the benefits and harms from community well-being and community process are included; (2) to emphasize that value requires a comparison of the benefits and harms of an intervention in relation to the resources used for the intervention; (3) to allow the specific characteristics and context of individual communities to be reflected in the valuation of community-based prevention; (4) to promote the quantification of value in terms of projected or actual changes due to the intervention; and (5) to encourage the development of evidence in order to make understanding the effects of interventions easier and more reliable. The valuation of community-based prevention interventions should be done with a comprehensive perspective; that is, the measurement of benefits, harms, and resources should include impacts on all members of the community as well as on stakeholders who may be outside the community. As illustrated in the framework, the measurement of benefits and harms should occur in the domains of health, community well-being, and community process. Resources used are a fourth major category to be considered in valuing community-based prevention. A further discussion of costs appears in Chapter 3 and in Box 5-1.
Recommendation 1: The committee recommends that those seeking to assign value to community-based prevention interventions take a comprehensive view that includes the benefits and harms in the three major domains of health, community well-being, and community process as well as the resource use associated with such interventions.
There are a variety of sources of data on health, including surveys (e.g., the National Health Interview Survey and the Behavioral Risk Factor Surveillance System), cohort studies (e.g., the Framingham Heart Study), registries, health services data, and vital statistics. Unfortunately, there are several limitations when attempting to use these data for local, community-based measurement. Identifying measures and sources of information for community well-being and community process elements is even more challenging than identifying these items for health. Such efforts will require an increased focus on identifying appropriate information gaps and data sources.
Recommendation 2: The committee recommends that the CDC
a. develop an inventory of existing data sources for health, community well-being, and community process;
b. identify gaps in data sources; and
c. develop data sources to fill those gaps.
Choosing among community-based prevention policies and programs can be difficult when programs have so many effects and those effects take so many different forms (see Chapter 3 for further discussion). The larger the menu of interventions and the larger the number of valued outcomes, the more difficult the choices become.
The committee proposes four indicators to assess the value of community-based prevention: changes in health, changes in community well-being, changes in community process, and changes in resources used. Health outcomes in the population can be valued with the well developed and widely used quality-adjusted life years (QALYs) or health-adjusted life expectancy (HALE). However, metrics for valuing community well-being and community process are yet to be developed. The committee is aware that the Centers for Disease Control and Prevention (CDC) has initiated efforts in these areas. Measures of community well-being (e.g., the Urban Hardship Index, Community Well-Being Indices, and county health rankings) have been developed and could serve as a starting point, but they have significant limitations in scope.
The committee views the development of a single indicator of community benefit comparable to QALYs or HALE for health as a long-term goal. The committee recognizes that developing this single indicator is a complex
task that will require expertise from many different fields. The National Prevention, Health Promotion, and Public Health Council (Prevention Council), an interagency group established by the Patient Protection and Affordable Care Act and chaired by the Surgeon General, recognizes that the health of a community is influenced by a number of factors outside of the health care and public health sectors, including education, housing, and transportation. Such a group is well positioned to encourage the research needed by the many different sectors that need to be involved in developing a community benefit indicator.
Recommendation 3: The committee recommends that the National Prevention, Health Promotion, and Public Health Council and other public and private sponsors support research aimed at developing
a. a single metric for appraising a community’s well-being,
b. a single metric for appraising community processes, and
c. a single metric for combining indicators of community well-being and community process with health into a single indicator of community benefit that can be considered in the context of costs and used to determine the value of a community-based prevention intervention.
Given that the outcomes in the four domains are—or will be, once they are developed—measured in different units, a single indicator of the value of community-based prevention is currently not possible. However, in the framework depicted in Figure S-1, if the indicator of community benefit is considered alongside the community cost indicator (which is suggested to be expressed in dollars or other currency), then value may be expressed as units of community benefit per dollar. The proposed indicators are a first step toward a possible future overall summary measure.
The value of a community-based prevention intervention reflects its impact in relation to what would have happened in its absence or in relation to an alternative community-based prevention intervention. It is therefore important to assess the actual changes that are projected to occur as a result of an intervention.
Recommendation 4: The committee recommends that those assessing value should include in their assessments the expected or demonstrated changes, both positive and negative, that result from the intervention.
Understanding what the community cares about is critical for designing and proposing interventions that address areas of importance to the community. Such an assessment will not only identify important health (and non-health) factors in the community but also those factors where
improvement is preferred by community members. What is important for one community may not be important for another.
Recommendation 5: The committee recommends that those involved in decision making ensure that the elements included in valuing community-based prevention interventions reflect the preferences of an inclusive range of stakeholders.
One dimension of the health outcomes that affects value is the possible conflict between equity and improving aggregate health for a population. Sometimes these two goals of health policy pull in the same direction, and sometimes they conflict. A community-based prevention intervention may be good at improving aggregate health, but it may have a bigger effect on those already better off in some important way, e.g., by income, residential location, or occupational status, and this may increase health disparities. The degree to which people are willing to trade off increased inequality for aggregate improvement may vary significantly. Reasonable disagreement about how to weigh these two values may persist, and the framework can make the source of that disagreement more visible.
The persistence of such disagreement around values suggests there may be a legitimacy problem for decision makers; even if they are the appropriate authorities for making such decisions, they must make them in the “right” way if legitimacy is to be obtained. Their process should search for rationales that take the relevant values into consideration, and the rationales must explain the basis for giving them the weight that the decision reflects. The framework emphasizes the importance of transparency, and one reason is that transparency improves the deliberative process. A transparent search for the value of an intervention is one key aspect of a process that arguably enhances legitimacy.
Recommendation 6: The committee recommends that, to assure transparency,
a. analysts make publicly available the evidence used for valuation and provide estimates of the uncertainty of their results, and
b. decision makers make publicly available the rationale for their decisions.
IMPLICATIONS FOR POLICY
As with the frameworks discussed in Chapter 4, the committee’s framework has limitations. The framework presented in this report is in its very early stages, and so its near-term impact on policy making is likely to be limited. Because of the importance of contextual factors and the limited
scope and generalizability of evidence on the effects of community-based prevention, the framework does not yet provide a detailed roadmap for valuation. The comprehensive data necessary to measure tangible benefits adequately are often not available, and the measurement of the many intangible benefits is not yet well developed. Such a broadly inclusive framework may seem overly abstract or unreliable to some observers. As the framework is applied, new measures and data sources will need to be developed, as will an appropriate methodology for creating valid single indicators for community well-being and community process. Old measures and data sources will need to be applied in new ways, a process that will take time to establish validity and gain acceptance. The committee has recommended several steps that can be taken to promote progress on these fronts. Although much work remains, the committee’s proposed framework is designed to capture the value of community-based prevention by taking a comprehensive approach, comparing benefits, harms, and resources used in three domains, and taking into account community context.
Additional efforts will be required to build consensus that the outcomes on which the framework focuses (health, community well-being, community process, and resources used) are broadly important, and not just the narrow interest of a specific group. It will also be important to validate the framework by showing repeatedly that it correctly distinguishes between interventions that improve community well-being and those that do not. This process of validation will almost certainly entail refinement of the framework as well as an expansion of the underlying base of evidence.
Formal incorporation of the framework into the policy-making process could consist of a requirement that legislative or grant proposals be accompanied by an objective impact assessment based on the framework or a requirement that executive-branch agencies use the framework in evaluating the output of their programs. Another way to give the framework a formal role would be to require that discretionary funding be distributed according to valuations that use the framework. Although that type of role may be many years off, the existing frameworks described in Chapter 4 provide clear precedents for such a progression.
The chapters of the report expand on the issues and findings discussed in this summary. Chapter 1 reviews the committee charge and definitions, explores why community-based prevention is important, examines how community-based prevention differs from clinical prevention efforts, and discusses issues associated with attempting to assign value. Chapter 2 expands on the discussion of community, provides a brief historical perspective of community interventions, discusses four approaches to community-based prevention, reviews models for implementation that represent the current state of the field, identifies important features of community-based prevention, and examines issues associated with evaluating the effectiveness of
such programs. In Chapter 3, the committee examines how methods from systems science can be applied to community-based prevention, discusses how such methods can be used to clarify and quantify the relationships among variables, identifies domains of value for community-based prevention, and discusses costs to consider in valuing. Chapter 4 provides a list of elements that a framework for assessing value should possess, examines how a framework for valuing resides within a decision-making context, reviews eight frameworks currently used to assess community-based prevention, and discusses the strengths and limitations of each for addressing the special characteristics of community-based prevention. In Chapter 5, the committee lays out its vision for the future of valuing community-based prevention.












