Executive Summary
Disability is an issue that affects every individual, community, neighborhood, and family in the United States. It is more than a medical issue; it is a costly social, public health, and moral issue.
-
About 35 million Americans (one in every seven) have disabling conditions that interfere with their life activities.
-
More than 9 million people have physical or mental conditions that keep them from being able to work, attend school, or maintain a household.
-
More than half of the 4-year increase in life expectancy between 1970 and 1987 is accounted for by time spent with activity limitations.
-
Disabilities are disproportionately represented among minorities, the elderly, and lower socioeconomic populations.
-
Of the current 75-year life expectancy, a newborn can be expected to experience an average of 13 years with an activity limitation.
-
Annual disability-related costs to the nation total more than $170 billion.
Disability is the expression of a physical or mental limitation in a social context—the gap between a person's capabilities and the demands of the environment. People with such functional limitations are not inherently disabled, that is, incapable of carrying out their personal, familial, and social responsibilities. It is the interaction of their physical or mental limitations with social and environmental factors that determines whether they have a disability. Most disability is thus preventable, which will not only significantly improve the quality of life for millions of Americans but also could save many billions of dollars in costs resulting from dependence, lost productivity, and medical care.
The pattern of conditions that cause disability is complex and difficult to
summarize. For young adults, mobility limitations such as those caused by spinal cord injuries, orthopedic impairments, and paralysis are the most common causes. For middle-aged and older adults, chronic diseases, especially heart and circulatory problems, predominate as causes of limitation. Figure 1 shows the age-specific prevalence rates for activity limitation according to five groups of causes; Figure 2 shows the proportion in each age group ascribed to each of the groups of conditions.
Modern medicine's success in averting the death of many people who sustain life-threatening diseases and injuries often entails, as a consequence, the loss of at least some functional capacity. Indeed, the successful lifesaving techniques of modern medicine are adding to the population of people with disabilities. For example, in the 1950s, only people with low-level paraplegia were generally expected to survive; today, even people with high-level quadriplegia are surviving and living lives of high quality. Indeed, one commentator has characterized the growing numbers of people with chronic conditions as the ''failures of successes" achieved with medical technology. To help these individuals restore functional capacity, avert further deterioration in functioning, and maintain or improve their quality
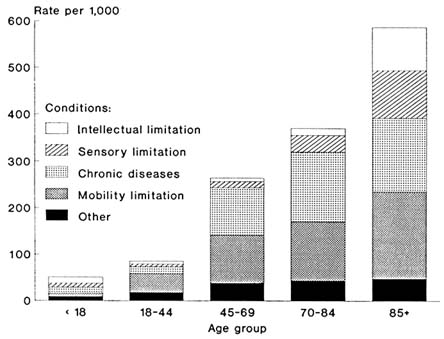
FIGURE 1 Prevalence of main causes of activity limitation, by age, 1983-1985.
Source: Calculated from LaPlante, 1988.
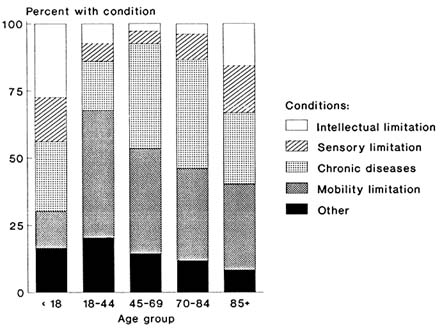
FIGURE 2 Percentage distribution of main causes of activity limitation, by age, 1983-1985. Source: Calculated from LaPlante, 1988.
of life, it is important to foster programs that emphasize rehabilitation and the prevention of secondary conditions. Partly for this reason the committee focused its report on prevention strategies for people who already have potentially disabling conditions, that is, on secondary and tertiary levels of prevention. In other words:
-
What can be done to prevent an impairment or functional limitation that results from injury, a birth defect, or chronic disease from becoming a disability?
-
What are the risks for developing a disability (or secondary condition), and how can they be controlled?
-
How is quality of life affected by disabling conditions, and what can be done to improve it?
Good disability prevention strategies must be built on strong basic knowledge of the relationships between risk factors, disabling conditions, quality of life, and secondary conditions. Until now, approaches to the prevention of disability have been significantly limited by the narrowness of conceptual views and inadequate data. This report gives special attention to issues
related to conceptual clarity and data needs and presents a model for studying the progression of conditions toward disability. The disability model described in this report should facilitate the development of improved surveillance systems, an epidemiology of disability, and more effective means of prevention.
Interfering with the development of effective prevention programs, however, is the lack of an effective public health surveillance network for monitoring the incidence and prevalence of disability, including predisposing risk factors. Without such a surveillance network, programs and policies intended to prevent disability will continue to be based on educated guesses rather than a solid data base that describes the sizable population of people that have either disabilities or a high risk of developing them. Furthermore, the fragmentation, gaps, and redundancies in the nation's disability-related programs—the focus of criticism in other quarters besides this report—will persist.
Although the current system for providing medical and social support to people with disabling conditions suffers from many inadequacies, most of the elements required for longitudinal care, as recommended by this committee, are likely to be in place. Additional financial resources may not be needed for many of the prevention measures noted here so much as a commitment to coordination, program planning, and service delivery to form a network that is readily accessible by consumer populations.
TOWARD A COMPREHENSIVE APPROACH TO DISABILITY PREVENTION
Despite an officially stated national goal of independence and equality of opportunity for people with disabilities, current approaches to preventing disability and improving the lives of people with disabling conditions lack conceptual clarity and unity of purpose. Reducing the prevalence and incidence of disability poses challenges on many fronts and requires coherent, comprehensive responses rather than the piecemeal actions that now characterize medical, rehabilitative, and social programs related to disability. In short, disability prevention requires new thinking, new collaborations among researchers, new relationships between agencies and organizations, both public and private, new approaches to delivering services, and new societal attitudes.
In developing its framework for a national disability prevention program, the committee sought to identify issues and needs that cut across the major categories of health conditions that can result in disability. It developed a model for disability and disability prevention (see Chapter 3) based on the work of Saad Nagi and the World Health Organization, and expanded it to include risk factors and quality of life. The committee then reviewed current knowledge in four major areas; developmental disabilities (Chapter 4);
injury-related disabilities, specifically those related to spinal cord injury and traumatic brain injury (Chapter 5); disabilities associated with chronic diseases and aging (Chapter 6); and secondary conditions associated with primary disabling conditions (Chapter 7). Needs and challenges specific to each category of disability are identified in the individual chapters.
Time and resources did not permit a review of all areas of disability. Mental health conditions, for example, are discussed only briefly as secondary conditions and, to a lesser extent, as primary conditions. Chapter 8 discusses the obstacles to and opportunities for a comprehensive approach to disability prevention, and Chapter 9 presents the committee's recommendations for a national agenda for the prevention of disability. A summary of Chapters 3-7 appears below, beginning with a discussion of the committee's model and followed by the committee's recommendations for a national agenda for the prevention of disability (Chapter 9 in its entirety).
A Model of Disability
There are two major conceptual frameworks in the field of disability: the International Classification of Impairments, Disabilities, and Handicaps (ICIDH), and the "functional limitation," or Nagi, framework, which is not accompanied by a classification system. The ICIDH is a trial supplement to the World Health Organization's International Classification of Diseases; it has stimulated extensive discussions of disability concepts, received both positive and negative reviews in the literature, and is used widely around the world. Several European countries including France and the Netherlands have adopted the ICIDH and use it extensively in administrative systems and clinical settings. As a classification system that has received broad international sponsorship the ICIDH deserves considerable attention, and the WHO is to be commended for its efforts in developing a system that has met with such success. As has been pointed out in the literature, however, the ICIDH is neither a classification of persons nor a research tool.
The original intent of the ICIDH classification system was to provide a framework to organize information about the consequences of disease. As such, it has been considered by some as an intrusion of the medical profession into the social aspects of life—a "medicalization of disablement." The WHO is planning to revise the ICIDH in the near future, which will provide opportunities for significant improvements.
Both frameworks (i.e., the ICIDH and the Nagi or functional limitation framework) have four basic concepts. In the ICIDH the four concepts are disease, impairment, disability, and handicap. In the Nagi framework, the four concepts are pathology, impairment, functional limitation, and disability. Both frameworks recognize that whether a person performs a socially expected activity depends not simply on the characteristics of the person
but also on the larger context of social and physical environments. Conceptual clarity, however, seems to be a problem with some of the classifications in the ICIDH. As discussed in the literature, some of the ICIDH classifications are confusing; for example, certain social role limitations (e.g., family role, occupational role) are classified as "behavior disabilities," instead of "occupation handicaps" or "social integration handicaps." Another example cited is the distinction between "orientation handicaps" and disabilities associated with self-awareness, postural, or environmental problems.
In considering the options for a conceptual framework, the committee was faced with the fact that the ICIDH includes the term "handicap" in its classification. Traditionally, handicap has meant limitations in performance, placing an individual at a disadvantage. Handicap sometimes has been used to imply an absolute limitation that does not require for its actualization any interaction with external social circumstances. In recent years, the term has fallen into disuse in the United States, primarily because people with disabling conditions consider handicap to be a negative term. Yet the shadow of "handicap" as a commonly used term hovers behind the concept of quality of life, and has the effect of reducing quality of life even though impairment, functional limitation, and disability do not necessarily do so. Much as the term "cripple" has gone out of style, handicap seems to be approaching obsolescence, at least within the community of people with disabilities in the United States.
The committee concurs with those who have noted internal inconsistencies and a lack of clarity in the ICIDH concepts of disability and handicap, and it notes the need for its pending revision. It prefers not to use handicap in this report and offers an alternative framework that does not focus on the consequences of disease. The committee's alternative framework draws on the widespread acceptance and success of the ICIDH and the conceptual clarity and terminology of the Nagi framework, and then adds risk factors and quality of life into a model of the disabling process. Committee members found that this framework and model improved their understanding of the relationships among and between components of the disabling process and helped them identify strategic points for preventive intervention. It is hoped that this framework will be considered as a viable alternative in the revisions of the WHO ICIDH.
The conceptual framework used in this report is composed of four related but distinct stages: pathology, impairment, functional limitation, and disability. In the course of a chronic disorder, one stage can progress to the next. But depending on the circumstances, progressively greater loss of function need not occur, and the progression can be halted or reversed. Thus disability prevention efforts can be directed at any of the three stages that precede disability, as well as at the disability stage itself, where efforts can focus on reversal of disability, restoration of function, or prevention of
|
PATHOLOGY |
→ |
IMPAIRMENT |
→ |
FUNCTIONAL LIMITATION |
→ |
DISABILITY |
|
Interruption or interference of normal bodily processes or structures |
|
Loss and/or abnormality of mental, emotional, physiological, or anatomical structure or function; includes all losses or abnormalities, not just those attributable to active pathology; also includes pain |
|
Restriction or lack of ability to perform an action or activity in the manner or within the range considered normal that results from impairment |
|
Inability or limitation in performing socially defined activities and roles expected of individuals within a social and physical environment |
|
Level of reference |
||||||
|
Cells and tissues |
|
Organs and organ systems |
|
Organism— action or activity performance (consistent with the purpose or function of the organ or organ system) |
|
Society— task performance within the social and cultural context |
|
Example |
||||||
|
Denervated muscle in arm due to trauma |
|
Atrophy of muscle |
|
Cannot pull with arm |
|
Change of job; can no longer swim recreationally |
FIGURE 3 An overview of the concepts of pathology, impairment, functional limitation, and disability.
complication (secondary conditions) that can greatly exacerbate existing limitations or lead to new ones. Figure 3 summarizes the four stages of the framework.
As mentioned above, the committee's model for disability builds on the conceptual frameworks of Nagi and the WHO, placing disability within the appropriate context of health and social issues (Figure 4). It depicts the interactive effects of biological, environmental (physical and social), and lifestyle and behavioral risk factors that influence each stage of the disabling process; the relationship of the disabling process to quality of life; and the stages of the disabling process that often precede disability. A brief description of the components of the model follows.
Risk Factors
Risk factors are biological, environmental (social and physical), and lifestyle or behavioral characteristics that are causally associated with health-related conditions. Identifying such factors can be a first step toward determining a mechanism of action in the disabling process and then developing preventive interventions. The disability research and service communities have not yet adopted a systematic, comprehensive conceptual model for understanding disability risk factors. A model that incorporates biological, environmental (physical and social), and lifestyle and behavioral risk factor categories will help move the disability research and service communities nearer to a more unified understanding of disability and disability prevention.
Quality of Life
The quality of life concept subsumes many aspects of personal well-being that are not directly related to health. It is becoming increasingly clear, however, that health is the product of a complex array of factors, many of which fall outside the traditional province of health care. Similarly, the health of the nation's citizens has commercial, economic, and social importance. Thus quality of life is assuming greater importance and acceptance, and its enhancement, in addition to curing disease or improving survival, is becoming an accepted goal of the health-related professions.
As depicted in Figure 4, quality of life affects and is affected by the outcomes of each stage of the disabling process. Within the disabling process, each stage interacts with an individual's quality of life. There is no universal threshold—no particular level of impairment or functional limitation—at which people perceive themselves as having lost their personal autonomy and diminished the quality of their lives. Yet perceptions of personal independence and quality of life are clearly important in determining how individuals respond to challenges at each of the four stages of the disabling process. Similar theoretical models for health status and quality of life have been described by others.
The Disabling Process
At the center of the model is the disabling process. Although it seems to indicate a unidirectional progression from pathology to impairment to functional limitation to disability, and although a stepwise progression often occurs, progression from one stage to another is not always the case. An individual with a disabling condition might skip over components of the model, for example, when the public's attitude toward a disfiguring impairment causes no functional limitation but imposes a disability by affecting
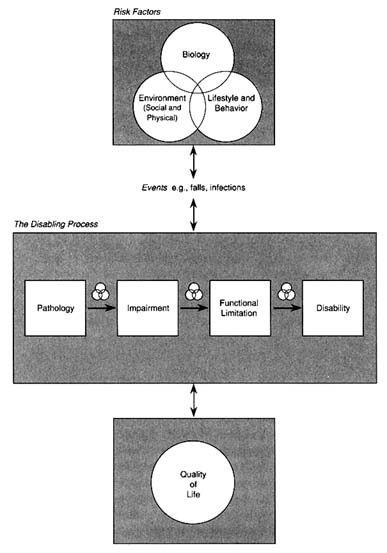
FIGURE 4 Model of disability showing the interaction of the disabling process, quality of life, and risk factors. Three types of risk factors are included: biological (e.g., Rh type); environmental (e.g., lead paint [physical environment], access to care [social environment]); and lifestyle and behavior (e.g., tobacco consumption). Bidirectional arrows indicate the potential for "feedback." The potential for additional risk factors to affect the progression toward disability is shown between the stages of the model. These additional risk factors might include, depending on the stage of the model, diagnosis, treatment, therapy, adequacy of rehabilitation, age of onset, financial resources, expectations, and environmental barriers.
social interaction. Also, the effects of specific stages in the model can be moderated by such interventions as assistive devices. Similarly, environmental modification (e.g., elimination of physical obstacles and barriers) is an important form of disability prevention, as is such landmark antidiscrimination legislation as the recently enacted Americans with Disabilities Act.
A variety of personal, societal, and environmental factors can influence the progression of a disabling condition from pathology to disability. They can also affect the degree of limitation or disability a person experiences and the occurrence of secondary conditions. A few of these factors are health status, psychological state, socioeconomic status, educational attainment and vocational training, climate, and the presence of multiple conditions and disabilities.
As indicated in the model, quality of life is an integral part of the disabling process. Research indicates that a person's perception of quality of life influences his or her responses to potentially disabling conditions and therefore outcomes. In turn, each successive stage in the disabling process poses an increasing threat of diminished quality of life. Measures that reduce this threat—for example, providing assistive technology that enables an individual to remain autonomous in at least some roles or modifying the work site to accommodate a person's limitations—can be effective interventions for preventing disability.
Thus disability is the product of a complex interactive process involving biological, behavioral, and environmental (social and physical) risk factors, and quality of life. Although disability always begins with a pathological condition, it is not inevitable even for people with incurable diseases or injury-caused conditions that carry the highest risks. There are usually, if not always, many points in the progression to disability at which to intervene and improve the quality of life for people with potentially disabling conditions.
The next four sections briefly discuss some of the information from each of the focus chapters. In the full report, these chapters each cover the magnitude of disability related to that category of disability, data needs, and prevention strategies. Although some primary prevention measures are described and discussed, the emphasis in the chapters and in these sections is on prevention for people who already have potentially disabling conditions (i.e., secondary and tertiary prevention).
Developmental Disabilities
Developmental disabilities affect about 4 percent of the population under age 21 and are caused by a variety of conditions, including cerebral palsy, seizure disorders, mental retardation, hearing and vision impairments, autism, structural birth defects (e.g., spina bifida) that cannot be corrected by
surgery, and social and intellectual deprivation. These conditions, which usually persist throughout an individual's lifetime, are diagnosed in an estimated 80,000 children each year. Because of their early onset, developmental disabilities account for a large percentage of the cumulative total of disability years1 for all age groups. In 1984, federal, state, and local governments spent an estimated $16.5 billion on programs and services for children with developmental disabilities. Not included in this cost estimate are programs and services for the additional 5-10 percent of all children who have learning disorders and require special education services.
Research has led to a number of important measures for preventing potentially disabling conditions that are acquired during childhood or that are the product of events during prenatal development. For example, lead screening followed by environmental lead abatement programs can reduce the incidence of lead toxicity. The removal of lead from gasoline has significantly reduced environmental exposure to lead. In the late 1970s an estimated 1.5 million children ages 6 months to 5 years had blood lead levels greater than or equal to 25 µmg/dl. It has also been estimated that, in 1984, 200,000 children (ages 6 months to 5 years) in standard metropolitan statistical areas (SMSA) had blood lead levels greater than or equal to 25 µg/dl. Recent studies indicate, however, that adverse effects on the fetus and child probably begin at blood lead levels of 15 µg/dl and below. A lower recommended threshold (currently 25 µg/dl) will probably be set, and more aggressive measures are being advocated for removing lead from the environment.
Interventions to prevent many birth defects and developmental disabilities have not yet been developed. Even when the means are known, they are often not adopted. For example, abstinence from alcohol during pregnancy prevents fetal alcohol syndrome, which can result in mental retardation, growth deficiency, facial abnormalities, and other conditions. The prevalence of fetal alcohol syndrome in the general population is estimated to be 1.7 cases per 1,000 births, but much higher rates have been reported for certain groups.
Injury-Related Disabilities
About 57 million Americans sustain injuries each year at a total lifetime cost of $158 billion. For every death caused by injuries—about 142,000 annually—16 people are hospitalized and 381 additional people incur injuries that do not require inpatient treatment. About $108 billion in economic costs, more than two-thirds of the total estimated lifetime cost of injuries, stem from nonfatal injuries.
In this report, the committee focused on head injuries and spinal cord injuries, which can cause significant physical, neurological, and psychosocial deficits and result in economic costs per person that are among the highest for injury-caused pathologies and impairments. Each year, about 1.3 million people suffer head injuries, and 70,000 to 90,000 of these individuals sustain moderate to severe traumatic brain injuries. Total annual medical costs for people who sustain head injuries were estimated to be $12.5 billion in 1982. At highest risk of sustaining traumatic brain injuries are people between the ages of 15 and 24, especially males. Demographic studies indicate that the incidence of traumatic brain injury is greatest for nonwhite urban populations and lowest for white populations living in suburban and rural areas. Motor vehicle collisions and falls are the leading causes of such injury. To the extent that they are discernible, trends over the past 10 years indicate that improvements in emergency medical services and acute management of head injuries have substantially increased the proportion of people who survive these injuries.
Each year, between 10,000 and 20,000 people sustain spinal cord injuries. Estimated lifetime costs for consequent medical treatment for such injuries range from $010,400 to $751,900, depending on the extent of injury. The most common major impairments are muscle paralysis and loss of sensation. Older adolescent males and young men are at greatest risk of spinal cord injury. Motor vehicle collisions and falls are the leading causes, followed by acts of violence, especially those involving firearms. In the 1950s, only people with low-level paraplegia were generally expected to survive; today, even people with high-level quadriplegia survive and live lives of high quality. A national study found that quadriplegia continues to be the outcome for half of all people who sustain spinal cord injuries; however, the proportion of people with quadriplegia who have neurologically incomplete lesions and therefore retain some motor control and sensation increased from 38 percent in 1973 to 54 percent in 1983.
Disabilities Associated with Chronic Disease and Aging
The prevalence of chronic disease—incurable, long-lasting pathologies such as osteoarthritis, cancer, heart disease, and diabetes—has increased to near-epidemic proportions in the United States. Almost half of all working-age people have one or more chronic conditions. An estimated 80 percent of the elderly have a chronic condition, and about 40 percent have some form of activity limitation due to chronic conditions.
Chronic conditions increase a person's risk of disability, although the degree of risk varies among conditions. Indeed, the most prevalent conditions, such as sinusitis, hypertension, and hearing impairment, generally
pose low risks of activity limitation, whereas the least prevalent conditions, such as multiple sclerosis and lung or bronchial cancer, pose very high risks of disability. Thus conditions that frequently result in disability may be more appropriate targets for primary prevention strategies, and those that pose lower risks of developing into disability may be more appropriately addressed by secondary or tertiary prevention strategies.
Many chronic conditions are associated with the aging process, which contributes to the widely held stereotype that aging is synonymous with a decline in functional capacity. An increasing body of research contradicts this stereotype, demonstrating that the physical and mental health status of elderly people can improve as well as deteriorate. Studies show, for example, that the adoption of health-promoting practices even late in life is beneficial. Potentially debilitating problems such as those associated with incontinence and osteoporosis are amenable to skillful rehabilitation. Prospects are good for increasing the number of disability-free years in the average life span, but much more research on the aging process, on potentially effective interventions, and on the delivery and coordination of services is needed.
Secondary Conditions Associated with Disability
People with disabling conditions are often at risk of developing secondary conditions that can result in further deterioration in health status, functional capacity, and quality of life. Secondary conditions by definition are causally related to a primary disabling condition and include decubitus ulcers, contractures, physical deconditioning, cardiopulmonary conditions, and mental depression. Considerable research has been done on the etiology and prevention of certain secondary conditions (e.g., pressure sores); in general, however, secondary conditions have received very little attention from researchers and health care and social service providers, despite the causal relationship that makes many of them easily predictable.
Much of what is known about the prevention of many secondary conditions is incidental and often results from deduction based on individual or clinical experience. There is a clear need for systematic evaluations of currently used interventions, as well as for research devoted to developing treatment protocols for people with specific types of disabilities. Such protocols would list assessment and treatment strategies for patients whose conditions matched prespecified characteristics, addressing not only medical needs but also environmental (social and physical) and behavioral risk factors associated with secondary conditions. Implementation of the protocols, of course, will require the participation of a wide spectrum of professionals in medical and nonmedical fields, as well as the people with disabling conditions themselves, their families, personal attendants, and advocates.
Also requiring greater attention, in both research and service delivery, is the role of assistive technology. Such technology promotes personal independence, facilitates the performance of tasks related to personal, familial, and social roles, and helps prevent debilitating, costly secondary conditions. However, outmoded concepts held by public and private insurance programs of what is ''medically necessary" often result in restriction or denial of coverage for assistive technologies. This problem indicates the need for improved programs of research and services that focus on secondary and tertiary prevention of disability—in the committee's model, halting progress toward disability and preventing secondary conditions.
RECOMMENDATIONS
As described and discussed throughout the report, the social and environmental aspects of disability and disability prevention are of critical importance and help to define limitations in the role of medicine in disability prevention. Indeed, the major disability-related roles for the fields of public health and medicine involve the prevention, early detection, diagnosis, treatment, and rehabilitation of potentially disabling conditions. Once such a condition is identified, however, the means of disability prevention go beyond rehabilitative restoration of function to include important social and economic factors.
Increasing attention to and understanding of the broad range of issues related to disability in this country recently resulted in the Americans with Disabilities Act signed into law by President Bush on July 26, 1990. That same impetus, amplified by the desire for accessible, affordable quality health care for all, led to the committee's finding that there is an urgent need for a well-organized, coordinated national disability prevention program. An agenda for such a program is presented on the next page. The agenda includes the program's stated goal and five strategies for its achievement: organization and coordination of the national program, surveillance, research, access to care and preventive services, and professional and public education. The full set of recommended measures to support each strategy is presented in Chapter 9; some of them are listed below (their numbers correspond to the numbers in Chapter 9).
Organization and Coordination
There are a number of disability-related programs in the federal government, but currently no one agency has been charged with leadership responsibilities that focus on prevention. The committee's recommendations below suggest mechanisms to organize and coordinate a national disability prevention program and to provide input from the diverse groups affected by disability.
|
A NATIONAL AGENDA FOR THE PREVENTION OF DISABILITY GOAL To reduce the incidence and prevalence of disability in the United States, as well as the personal, social, and economic consequences of disability in order to improve the quality of life for individuals, families, and the population at large. STRATEGIES Organization and Coordination—Establish leadership and administrative responsibility for implementing and coordinating the National Agenda for the Prevention of Disability within a single unit of the federal government. Implementation of the agenda should be guided by a national advisory committee, and progress should be critically evaluated periodically. In addition to federal leadership, achieving the goals of the agenda will require the strong, sustained participation of the state, local, and private sectors. Surveillance—Develop a conceptual framework and standard definitions of disability and related concepts as the basis for a national disability surveillance system. Such a system should be designed to (1) characterize the nature, extent, and consequences of disability and antecedent conditions in the U.S. population; (2) elucidate the causal pathways of specific types of disability; (3) identify promising means of prevention; and (4) monitor the progress of prevention efforts. Research—Develop a comprehensive national research program on disability prevention. The research should emphasize longitudinal studies and should focus on preventive and therapeutic interventions. Special attention should be directed to the causal mechanisms whereby socioeconomic and psychosocial disadvantage lead to disability. Training young scientists for careers in research on disability prevention should become a high priority. Access to Care and Preventive Services—Eliminate the barriers to access to care, especially for women and children, to permit more effective primary prevention and prevent progression of disability and the development of secondary conditions. Existing programs of proven effectiveness should be expanded, and new service programs should be introduced. Returning persons with disabling conditions to productive, remunerative work is a high priority. Professional and Public Education—Educate health professionals in the prevention of disability. Foster a broad public understanding of the importance of eliminating social, attitudinal, and environmental barriers to the participation of people with functional limitations in society and to the fulfillment of their personal goals. Educate health professionals, people with disability, family members, and personal attendants in disability prevention and preventing the development of secondary conditions. |
Leadership of the National Disability Prevention Program
The congressionally mandated role of the National Council on Disability (NCD) is to provide advice and make recommendations to the President and to Congress with respect to disability policy. In keeping with its charter, the council has been and should continue to be an effective leader in developing disability policy in such areas as education, health care services, and civil rights.
In 1986 the NCD identified the need for a national program for disability prevention and recommended to the President and Congress that such a program be established in the Centers for Disease Control (CDC). In 1988 CDC initiated the Disabilities Prevention Program to build capacity in disability prevention at the state and local levels, establish systems of surveillance for disabilities, use epidemiological approaches to identify risks and target interventions, and provide states with technical assistance. It is the only federal program that has been charged specifically with disability prevention. Its initial focus has been prevention of the more readily identifiable injuries and developmental disabilities, and the secondary conditions that are often associated with them.
The committee endorses the emerging federal leadership in disability prevention at CDC. The agency's traditional strengths—epidemiology, surveillance, technology transfer, disease prevention, and communication and coordination with state, local, and community-based public health activities—are consonant with the needs of a national program. Moreover, CDC has demonstrated its leadership in the development and effective implementation of interventions in numerous specific public health situations, in quality control for screening programs and their implementation, in the development of school and other public health curricula, and in the evaluation of public health service delivery programs.
Given the magnitude of the public health problem disability presents and the large number of various types of disability-related public and private programs, there is a need for expansion and coordination of disability prevention activities. The committee's recommendations, which appear below, have been formulated to address that need and provide a framework for future program development.
The CDC Disabilities Prevention Program is a good first step in the development of such a framework. In addition, the informal relationship that currently exists between it and the National Council on Disability appears to be a mutually beneficial one that has strengthened federal disability prevention activity during its infancy. To the extent that such a relationship remains beneficial to developing a national program for disability prevention, it should continue.
RECOMMENDATION 1: Develop leadership of a National Disability Prevention Program at CDC
To advance the goal and carry out the strategies of the national agenda, the committee recommends that the CDC Disabilities Prevention Program be expanded to serve as the focus of a National Disability Prevention Program (NDPP). In assuming the lead responsibility for implementing the national agenda for the prevention of disability over the life course, the NDPP should coordinate activities with other relevant agencies, emphasizing comprehensive surveillance, applied research, professional and public education, and preventive intervention with balanced attention to developmental disabilities, injuries, chronic diseases, and secondary conditions.
As the national program develops, with its emphasis on prevention of disability throughout the life course, it should focus on identifying and modifying the biological, behavioral, and environmental (physical and social) risk factors associated with potentially disabling conditions, as well as monitoring the incidence and prevalence of the conditions themselves. The program should be conducted in cooperation and in partnership with state health agencies and other public agencies. A major component of the program should be the development at the state level of a sharply increased capacity to prevent disability.
A disability prevention program of the scope and ambition envisioned by the committee will require much more than can be accomplished by governments acting alone. The active participation of all segments of society is required.
RECOMMENDATION 2: Develop an enhanced role for the private sector
The NDPP should recognize the key role of the private sector in disability prevention, including advocacy groups, persons with disabilities, business and other employers, the insurance industry, academia, the media, voluntary agencies, and philanthropies. Indeed, the potential contributions of the private sector in achieving the program's goals cannot be emphasized too strongly. Its role encompasses the provision of employment opportunities, modification of the workplace, research in and development of assistive technology, provision of appropriate insurance, and development of a national awareness program.
One way to involve the private sector might be to establish an independent forum on disability policy for the promotion, coordination, and resolution of disability-related issues that would facilitate prevention. Addressing many of these issues requires the collaborative support and involvement of
a broad array of scientists and informed leaders from both the private and public sectors. The purpose of the forum would be to improve policymaking through a continuing dialogue among individuals and groups that play a significant role in shaping policy and public opinion. Areas for consideration might include access to assistive technology and personal assistance services, gaps in health insurance coverage, family leave policies, and implementation issues related to the Americans with Disabilities Act.
Advisory Committee
As stated throughout the full report, disability is a public health and social issue. Thus a national disability prevention program will be centrally dependent on public attitudes toward people with disabilities and on the way community activities are organized, which includes access to housing, public transportation, and the workplace. Equally important is the reduction of prejudice and discrimination toward people with disabilities. An agenda for disability prevention will require cooperation among all levels of government; the health, social services, and research professions; business; educational institutions; churches; and citizens' organizations throughout the country.
RECOMMENDATION 3: Establish a national advisory committee
An advisory committee for the NDPP should be established to help ensure that its efforts are broadly representative of the diverse interests in the field. The advisory group should include persons with disabilities and their advocates; public health, medical, social service, and research professionals; and representatives of business, insurance, educational, and philanthropic organizations, including churches. The role of the advisory committee would be to advise CDC on priorities in disability prevention research and the nationwide implementation of prevention strategies, as well as to assess progress toward the goal of the national agenda for the prevention of disability. The advisory committee should be appointed by the Department of Health and Human Services and meet at least three times a year. In keeping with its role in regard to disability policy, the National Council on Disability should be a permanent member of this committee.
Interagency Coordination and Periodic Review
The fragmentation of disability-related activities and the lack of continuity of care are highly disruptive to preventive efforts. Part of the problem derives from the fact that essential services are funded and provided by various agencies and by different levels of government without a clear focus of authority and responsibility, leading to gaps in services. The lack of
coordination of health and medically related rehabilitation activities and social services is a long-standing problem that is not easily rectified. Improvements will require energy and direction, a focus on prevention, and a clear strategy for coordination, cooperation, and integration among several federal programs as they are administered at the local level. These federal programs include those concerned with health care (Health Care Financing Administration), disability benefits (Social Security Administration and the Department of Veterans Affairs), vocational rehabilitation (Department of Education), community support (National Institute of Mental Health), and housing (Department of Housing and Urban Development). Thus responsibility for planning, coordination, and evaluation of these activities should be highly placed in the federal government (e.g., in the Office of the Secretary of the Department of Health and Human Services) to facilitate the type of coordinated leadership at the federal level necessary to ensure cooperation at the local level.
RECOMMENDATION 4: Establish a federal interagency council
A standing Interagency Council on Disability Prevention should be established by the Secretary of Health and Human Services. The interagency council should be charged with examining and developing conjoint activities in disability prevention and with identifying existing policies that inhibit disability prevention and rehabilitation. More specifically, the interagency council should be convened semiannually to identify, examine, and foster enhanced disability prevention strategies by (1) recommending the elimination of conflicting public policies and coordinating and integrating programs, (2) developing new policy initiatives, (3) improving service delivery, and (4) setting research priorities. The interagency council should have a permanent staff and issue public reports to the Secretary of Health and Human Services, Congress, and the National Council on Disability.
The members of the interagency council should be high-level administrators drawn from the major agencies involved in the various aspects of disability, which include the following: Centers for Disease Control; Health Care Financing Administration; Alcohol, Drug Abuse, and Mental Health Administration; National Institute on Disability and Rehabilitation Research; Health Resources and Services Administration (HRSA), including the Maternal and Child Health Bureau; Agency for Health Care Policy and Research; Social Security Administration; National Institutes of Health; Consumer Product Safety Commission; Bureau of the Census; and other agencies within the Departments of Health and Human Services, Housing and Urban Development, Education, Transportation, Labor, Defense, Veterans Affairs, and others as appropriate.
Surveillance
Although information on the incidence and prevalence of disability is available, it is organized in so many different ways that accurate, useful analysis is impeded. Estimates of the prevalence of disability vary by more than 100 percent. One difficulty is the conceptual confusion surrounding disability and its antecedent conditions. Until there is a consistently applied, widely accepted definition of disability and related concepts, the focus for preventive action and rehabilitation will remain uncertain.
Conceptual Framework
Conceptual confusion regarding disability is not limited to the United States, as indicated by the World Health Organization's development of the International Classification of Impairments, Disabilities, and Handicaps. The WHO classification scheme, which seeks to establish uniformity in the use of important concepts, is an important step toward international comparative studies of disability. The committee, however, saw a need to develop its own system and in this report presents a conceptual framework and model derived from the works of Nagi and the WHO that differs from both primarily in that it incorporates risk factors and quality of life. What is needed now is international agreement on a logical, conceptual system that would result in comparable disability statistics across nations. Existing frameworks represent only the initial steps in a process of conceptual refinement and evaluation.
RECOMMENDATION 6: Develop a conceptual framework and standard measures of disability
The CDC, which is responsible for surveillance of the nation's health, should design and implement a process for the development and review of conceptual frameworks, classifications, and measures of disability with respect to their utility for surveillance. This effort should involve components of the private sector that collect disability data, as well as federal agencies including the National Institutes of Health; Alcohol, Drug Abuse, and Mental Health Administration; National Council on Disability; Office of Human Development Services (a component of the Department of Health and Human Services); Agency for Health Care Policy and Research; Health Care Financing Administration; Bureau of the Census; Department of Veterans Affairs; Social Security Administration; and HRSA's Maternal and Child Health Bureau. The objective should be consensus on definitions, measures, and a classification and coding system of disability and related concepts. These elements should then be adopted by all local, state, federal, and private agencies that gather data and assemble statistics on disability. Collaboration
with the WHO and other international agencies should be encouraged in developing a classification system to obtain comparable disability data across nations.
A National Disability Surveillance System
Despite its significance as a public health and social issue, disability has received little attention from epidemiologists and statisticians; consequently, surveillance of disabling conditions is inadequate in many ways. When disability is a focus of attention, surveillance is more often concerned with counting the number of people affected than with investigating its causes and secondary conditions. Without knowledge of the conditions and circumstances that can lead to disability, the problem in its many manifestations cannot be fully understood, nor can effective prevention strategies be systematically developed.
Disability prevention will require expanded epidemiological studies and surveillance to identify risk factors, the magnitude of risk, and the degree to which risk can be controlled. Because disability is the product of a complex interaction among behavioral, biological, and environmental (social and physical) factors, epidemiological investigations must encompass a broad range of variables that influence the outcomes of mental and physical impairment. Current surveillance systems are condition specific, permitting identification, for example, of the risk factors associated with injuries. None of them, however, track the risk factors associated with the progression from pathology to impairment to functional limitation to disability. Nor is there sufficient research on the range of consequences associated with specific behaviors and circumstances.
Congenital and developmental conditions, injuries, and chronic diseases that limit human activity do not occur randomly within the general population. Epidemiological principles can be used to identify high-risk groups, to study the etiology, or causal pathways, of functional limitations and disabilities, and to evaluate preventive interventions. More specifically, epidemiology and surveillance could play an increased role in the prevention of disability by (1) accurately determining the dimensions of the populations of people with disabilities, (2) identifying the causes of disabilities, (3) guiding the development and selection of preventive interventions, and (4) evaluating the implementation of interventions.
RECOMMENDATION 7: Develop a national disability surveillance system
A national disability surveillance system should be developed to monitor over the life course the incidence and prevalence of (1) functional limitations and disabilities; (2) specific developmental disabilities, injuries,
and diseases that cause functional limitations and disability; and (3) secondary conditions resulting from the primary disability. The system should also monitor causal phenomena, risk factors, functional status, and quality of life, and provide state-specific data for program planning and evaluation of interventions. This system should be developed in cooperation with a broad range of federal agencies and private organizations and be implemented as part of the National Disability Prevention Program.
Research
A wide variety of disability risk factors are associated with the spectrum of diseases and injuries that can lead to disability. These risk factors affect not only the occurrence of the initial event but also the progression of pathologies to impairments, functional limitations, and disabilities. To the extent that risk factors can be eliminated or moderated, the incidence of initial disabling conditions and the progression toward disability can be limited. Much more needs to be known, however, and such knowledge can be acquired only through a broad range of research activities.
Coordinated Research Program
RECOMMENDATION 11: Develop a comprehensive research program
A coordinated, balanced program of research on the prevention of disability associated with developmental disabilities, injury, chronic disease, and secondary conditions should be an essential component of the National Disability Prevention Program. Emphasis should be placed on identifying biological, behavioral, and environmental (physical and social) risk factors over the life course that are associated with disability and secondary conditions and on developing effective intervention strategies. A continuing effort should be made to incorporate functional assessment and quality of life indicators into the research agenda and surveillance measures.
Longitudinal Studies
The process of developing a disabling condition, as well as the associated potential for secondary conditions, is complex and longitudinal. Yet most available data on disability are cross-sectional, making it impossible to accurately gauge the course of disability in relation to varying risk factors or the impact of timely interventions on the development of disability. There is thus a great need for longitudinal studies that effectively describe
the course of disability and identify the most strategic points for effective intervention.
RECOMMENDATION 12: Emphasize longitudinal research
A research program of longitudinal studies should be developed to determine the course of conditions and impairments that lead to disability and to identify the strategic points of preventive intervention. The research should emphasize the prevention of secondary conditions, improved functional status, and improved quality of life. In addition, because rapid changes are occurring for people with disabling conditions in terms of health services, public attitudes, and opportunities for social participation, cohort studies are needed to assess the effects of these changes over the life course.
Relationship of Socioeconomic Status
Deeper understanding of the biological underpinnings of pathologies, impairments, and functional limitations is an obvious need, and this knowledge is being pursued in a variety of biomedical research programs, such as those sponsored by the National Institutes of Health and the Alcohol, Drug Abuse, and Mental Health Administration. Far less effort has been devoted to the influence of behavioral, physical and social environmental, and social factors on the development of disability. One transcendent problem, for example, is the high rate of disability among people of low socioeconomic status. Most studies of disability attempt to control statistically for socioeconomic status because it is a powerful risk factor. Moreover, because socioeconomic status has sometimes been considered to be incidental to research investigations, the relationship between disability and socioeconomic status has rarely been addressed directly.
RECOMMENDATION 13: Conduct research on socioeconomic and psychosocial disadvantage
Research should be conducted to elucidate the relationship between socioeconomic and psychosocial disadvantage and the disabling process. Research that links the social and biological determinants of disability should result in improved understanding of the complex interactions leading to disability, an understanding that would help in developing new prevention strategies.
Interventions
There is a clear need to incorporate existing knowledge more efficiently into disability prevention. A concomitant need is to ascertain the effectiveness
of current approaches in the wide variety of situations in which disability occurs. All areas of prevention require critical evaluations of the effectiveness of the tools and methods used in the prevention of disability and secondary conditions.
The federal government spends about $60 billion annually for medical coverage and to supplement the incomes of people with disabilities; it spends a relatively small amount on research to identify practices and technologies that can prevent the initial occurrence of disability or limit complications among people with disabilities to help them lead more productive lives. Moreover, the federal funding agencies that support biomedical research have not made prevention a high priority, and there has been little effort devoted to developing research programs on the prevention of disability and secondary conditions.
RECOMMENDATION 14: Expand research on preventive and therapeutic interventions
Research on the costs, effectiveness, and outcomes of preventive and therapeutic interventions should be expanded. The expanded research program should also include acute care services, rehabilitative and habilitative services and technologies, and longitudinal programs of care and interventions to prevent secondary conditions. The National Institute on Disability and Rehabilitation Research, the Department of Veterans Affairs, the National Institutes of Health, the Alcohol, Drug Abuse, and Mental Health Administration, and the Agency for Health Care Policy and Research should join with CDC to develop cooperative and collaborative research programs in the biological, behavioral, and social sciences as they relate to disability prevention. These programs should also emphasize the translation of new findings into national prevention efforts that inform and educate people with disabilities, their families, personal attendants, and advocates, as well as clinical practitioners. Consideration should be given to approaches used in other countries (e.g., the Netherlands, Sweden, England, and France), where disability prevention is viewed from a broad perspective that includes social and ethical implications and socioeconomic costs.
Access to Care and Preventive Services
Many persons with disabilities are not covered by Medicare or Medicaid and have little access to private coverage because they either are unemployed or have been rejected for insurance because of their disabilities. Thus the problem of access to care is even greater for people with disabilities than for the general American population. Moreover, persons with disabilities and those at risk of disability are disproportionately poor, making
it difficult for them to purchase insurance, make required copayments, or purchase essential services and equipment for their rehabilitation. In addition, poverty compounds the difficulties faced by those with disabilities in gaining recognition of their needs (which are often complicated by the social circumstances associated with poverty) and in developing satisfactory relationships with health providers.
Accessible, Affordable Quality Care
The committee recognizes that the problems of access to health care are deeply embedded in the organization of the U.S. health insurance system and its relationship to employment and other issues. The committee is also aware that resolution of many of the problems identified in this report will require a fundamental restructuring of the financing and organization of the nation's health services. This committee was not charged with addressing these larger issues; nevertheless, its members feel strongly that the gaps in the nation's present system contribute to an unnecessary burden of disability, loss of productivity, and lowered quality of life, and that the United States must make basic health services accessible to all.
Thirty to forty million Americans, including millions of mothers and children, do not have health care insurance or access to adequate health services. Even those Americans who have health care insurance are rarely covered for (and have access to) adequate preventive and long-term medical care, rehabilitation, and assistive technologies. These factors demonstrably contribute to the incidence, prevalence, and severity of primary and secondary disabling conditions and, tragically, avoidable disability.
Recently, the U.S. Bipartisan Commission on Comprehensive Health Care (the Pepper Commission) recommended a universal insurance plan that emphasizes preventive care and identifies children and pregnant women as the groups whose needs should be addressed first. In addition, the American Academy of Pediatrics (AAP) has developed a specific proposal to provide health insurance for all children and pregnant women. The AAP proposal presents several principles relative to ensuring access to health care, as well as estimates of program costs and a package of basic benefits. Many aspects of the proposal could have favorable effects on the cost of health care (e.g., prenatal care should lower expenditures for intensive care of newborns and subsequent disabling conditions).
The committee believes that a system that provided accessible, affordable quality health care for all would have an enormous beneficial effect on the prevention of disability. Yet the economic and political hurdles to that end are formidable, and a near-term solution is not in sight. A first step that has been proposed is to provide quality health care services for all mothers and children (up to age 18). These services have a high probability of
preventing disability; however, assessing or evaluating their cost implications was not part of the charge to this committee.
RECOMMENDATION 16: Provide comprehensive health services to all mothers and children
Preventing disability will require access by all Americans to quality health care. An immediate step that could be taken would be to ensure the availability of comprehensive medical services to all children up to the age of 18 and to their mothers who are within 200 percent of the poverty level; in addition, every pregnant woman should be assured access to prenatal care. When provided, these services should include continuous, comprehensive preventive and acute health services for every child who has, or is at risk of developing, a developmental disability. In certain circumstances—for example, providing prenatal care for the prevention of low birthweight—the economic consequences have been shown to be favorable, but they need to be explored further in other areas of health care delivery.
Research on prenatal care has demonstrated that comprehensive obstetric care for pregnant women, beginning in the first trimester, reduces the risk of infant mortality and morbidity, including congenital and developmental disability. Researchers also have documented that women who have the greatest risk of complications during pregnancy—teenagers and women who are poor—are also the least likely to obtain comprehensive prenatal care. Furthermore, in its 1985 report, Preventing Low Birthweight , the IOM showed conclusively that, for each dollar spent on providing prenatal care to low-income, poorly educated women, total expenditures for direct medical care of their low-birthweight infants were reduced by more than $3 during the first year of life.
RECOMMENDATION 17: Provide effective family planning and prenatal services
Educational efforts should be undertaken to provide women in high-risk groups with the opportunity to learn the importance of family planning services and prenatal care. Access to prenatal diagnosis and associated services, including pregnancy termination, currently varies according to socioeconomic status. The committee respects the diversity of viewpoints relative to those services but believes they should be available to all pregnant women for their individual consideration as part of accessible, affordable quality care.
Even among privately or publicly insured people with disabilities, access to needed services is often a problem. Coverage may be limited by an
arbitrarily defined ''medical necessity" requirement that does not permit reimbursement for many types of preventive and rehabilitative services and assistive technologies. Insurance policies tend to mirror the acute care orientation of the U.S. medical system and generally fail to recognize the importance and value of longitudinal care and of secondary and tertiary prevention in slowing, halting, or reversing deterioration in function. The presumption, which has never been thoroughly evaluated, is that rehabilitative and attendant services, assistive technology, and other components of longitudinal care are too costly or not cost-effective.
Access to health care, particularly primary care, is a major problem for persons with disabilities. Many report that they have great difficulty finding a physician who is knowledgeable about their ongoing health care needs. They also have problems obtaining timely medical care and assistive technology that can help prevent minor health problems from becoming significant complications. National data indicate that, relative to the general population, person with disabilities, regardless of age, have high rates of use of health care services such as hospital care.
The problem of access to care for persons with disabilities transcends the availability of insurance of a regular relationship with a health professional (although for many large gaps exist in both these areas). More important is that the person have access to appropriate care during the full course of a disabling condition. Such care should be provided in a way that prevents secondary conditions and maximizes the person's ability to function in everyday social roles. It must have continuity and not be restricted by arbitrary rules that limit services necessary for effective rehabilitation and participation in society. Persons with disabilities often face enormous impediments to obtaining the coordinated services they need to prevent secondary conditions and improve their opportunity for successful lives. Such impediments include (1) lack of support from insurance and other funding agencies, (2) lack of locally available services, and (3) absence of local coordinating mechanisms.
RECOMMENDATION 18: Develop new health service delivery strategies for people with disabilities
New health service delivery strategies should be developed that will facilitate access to services and meet the primary health care, health education, and health promotion needs of people with disabling conditions. These strategies should include assistive technologies and attendant services that facilitate independent living.
Access to Vocational Services
Vocational services are crucial to ensure that return-to-work goals are achieved. These services may include counseling and work readiness evaluations,
job training, job placement, work-site modification, and postemployment services (e.g., Projects with Industry) to ensure satisfactory adjustment and assistance in sustaining employment.
RECOMMENDATION 22: Provide comprehensive vocational services
Vocational services aimed at reintegrating persons with disabilities into the community and enabling them to return to work should be made financially and geographically accessible.
Professional and Public Education
The prevention of disability requires not only access to care and restructuring of services but also a radically different mind-set among many health and other professionals (e.g., psychologists, sociologists, educational specialists) and the general public. As the committee observes throughout its report, the attitudes and behavior of health professionals and the public could either facilitate effective coping and productive lives for persons with disabilities or erect obstacles in their path. For example, many secondary conditions are preventable, but health professionals often are not familiar with the intervention strategies that can be used, and may provide inappropriate care as a result.
Education of Professionals
The committee notes that the field of physical medicine and rehabilitation is one of only a few medical specialties with a shortage of physicians. This situation is not surprising because rehabilitation has had a low priority in medical schools and residency training programs, and many do not even offer courses on disability and rehabilitation. Similarly, personnel shortages exist in physical therapy, speech therapy, occupational therapy, and all allied health and nursing disciplines dealing with disability. Yet the problem goes well beyond these shortages. Even if the numbers of practitioners in these specialties were substantially increased, many problems would remain (e.g., there are few incentives for practicing the types of longitudinal care this committee advocates, and health professionals who follow these careers historically have had little recognition and prestige within their professional groups). In addition, longitudinal care, which has its own special appeal, is also "patient intensive" and requires complex teamwork, two factors that may outweigh its rewards in the minds of many health professionals.
Steps must be taken to ease the current shortage of knowledgeable physicians, allied health professionals, and others (e.g., psychologists, sociologists, educational specialists) working in disability prevention. In fact, all specialties should have a better understanding of the process of disability and
appropriate modes of preventive intervention. The longitudinal care described in this report is sometimes provided by specialists in physical medicine and rehabilitation, but most typically it will be provided by general internists, family physicians, psychiatrists, psychologists, social workers, and others. Any long-term strategy must address the education of a broad range of these professionals as part of a national agenda for the prevention of disability.
RECOMMENDATION 23: Upgrade medical education and training of physicians
Medical school curricula and pediatric, general internal medicine, geriatric, and family medicine residency training for medical professionals should include curricular material in physical medicine, rehabilitation, and mental health. In addition, such curricula should address physiatric principles and practices appropriate to the identification of potentially disabling conditions of acute illness and injury. Appropriate interventions, including consultation and collaboration with mental health and allied health professionals, social workers, and educational specialists, and the application of effective clinical protocols should also be included.
RECOMMENDATION 24: Upgrade the training of allied professionals
Allied health, public health, and other professionals interested in disability issues (e.g., social workers, educational specialists) should be trained in the principles and practices of disability prevention, treatment planning, and rehabilitation, including psychosocial and vocational rehabilitation.
Education of Persons with Disabilities and Their Families, Personal Attendants, and Advocates
People with disabilities and their families, personal attendants, and advocates should be better informed about the principles of disability prevention. Such education would contribute significantly to the prevention of disability and secondary conditions—those brought about by poor self-care as well as those induced by a lack of needed social and other support services, architectural inaccessibility, unequal educational and employment opportunities, negative attitudes toward disability, changes in living environments, and greater exposure to disruptive, frustrating events.
Independent living centers, which are controlled and staffed by persons with disabilities, are designed to deal with the prevention of secondary conditions and to be a source of information on the practical aspects of daily living with a disability. Because these centers are usually staffed by persons with disabilities who are living independently, they offer advice based on first-hand experience of the motivation and ingenuity needed to
pursue an independent lifestyle. Being able to share experiences with peers who are independent brings to light those coping mechanisms that aid in preventing secondary conditions. Independent living centers are also effective advocates for attitudinal and architectural changes in society that would improve accessibility, stimulate social interaction and productivity, and facilitate an active, quality lifestyle.
RECOMMENDATION 27: Provide more training opportunities for family members and personal attendants of people with disabling conditions
Persons with disabilities, their families, personal attendants, and advocates should have access to information and training relative to disability prevention with particular emphasis on the prevention of secondary conditions. Independent living centers and other community-based support groups provide a foundation for such training programs and offer a source of peer counseling.
A list of the committee's recommendations for a national agenda for the prevention of disabilities follows.
|
LIST OF RECOMMENDATIONS A NATIONAL AGENDA FOR THE PREVENTION OF DISABILITY ORGANIZATION AND COORDINATION Develop leadership of National Disability Prevention Program at CDC Develop an enhanced role for the private sector Establish a national advisory committee Establish a federal interagency council Critically assess progress periodically SURVEILLANCE Develop a conceptual framework and standard measures of disability Develop a national disability surveillance system Revise the National Health Interview Survey Conduct a comprehensive longitudinal survey of disability Develop disability indexes RESEARCH Develop a comprehensive research program Emphasize longitudinal research Conduct research on socioeconomic and psychosocial disadvantage Expand research on preventive and therapeutic interventions Upgrade training for research on disability prevention ACCESS TO CARE AND PREVENTIVE SERVICES Provide comprehensive health services to all mothers and children Provide effective family planning and prenatal services Develop new health service delivery strategies for people with disabilities Develop new health promotion models for people with disabilities Foster local capacity building and demonstration projects Continue effective prevention programs Provide comprehensive vocational services PROFESSIONAL AND PUBLIC EDUCATION Upgrade medical education and training of physicians Upgrade the training of allied professionals Establish a program of grants for education and training Provide more public education on the prevention of disability Provide more training opportunities for family members and personal attendants of people with disabling conditions |































