Health and Developmental Correlates of Child Food Insecurity from Pregnancy to Adolescence
The workshop’s sixth and seventh sessions examined the health and developmental correlates of child food insecurity from pregnancy to adolescence. Topics included the impacts of food insecurity on health, obesity, cognitive, and academic outcomes. The sessions addressed mechanisms/pathways (biological, psycho-emotional, via caregivers) and windows of vulnerability, as well as selected issues related to measurement. Both sessions are summarized in this chapter.
The moderator for the sessions was Deborah Frank, founder and principal investigator of Children’s HealthWatch, director of the Grow Clinic for Children at the Boston Medical Center, and professor of child health and well-being at Boston University School of Medicine. The first speaker in Session 6 was Barbara Laraia, School of Public Health, University of California, Berkeley, who focused her remarks on food insecurity and child outcomes. The second speaker, Rafael Pérez-Escamilla, Yale School of Public Health, spoke on household food insecurity and the impact on a child’s psycho-emotional, social, and academic condition. Their presentations were followed by a formal discussant, Alison Jacknowitz, of the American University School of Public Affairs.
The main speaker in Session 7 was John Cook, Boston University School of Medicine and one of the principal investigators for Children’s HealthWatch. The two formal discussants were Diane Whitmore Schanzenbach, Institute for Policy Research (IPR), Northwestern University, and Hilary Seligman, University of California, San Francisco.
A summary of the open discussion covering both sessions is included at the end of this chapter.
STATEMENT OF BARBARA LARAIA1
Laraia stated she would discuss food insecurity during pregnancy; the outcomes from food insecurity for children, including diet, weight status, and chronic disease; and suggestions for “next steps.”
Food Insecurity During Pregnancy
Laraia reported that food insecurity during pregnancy has been associated with the low birthweight of the child (Borders et al., 2007; Hobel, 2004), which in turn is associated with insulin-resistance and glucose intolerance later in that child’s life. Thus, food insecurity during pregnancy can set the fetus up for a trajectory to be more at risk for chronic disease later in life. Using data from the National Health and Nutrition Examination Study (NHANES), 1999–2010, she and her colleagues (Laraia et al., 2013a) estimated that 10.2 percent of pregnant women were low food secure, 4.4 percent were very low food secure, and an additional 8.8 percent were marginally food secure (unpublished data).
She said that food insecurity is a chronic stressor, and the effect of stress during pregnancy was summarized in Hobel, Goldstein, and Barrett (2008). In the hypothalamus-pituitary-adrenal (HPA) axis stress feedback system of a nonpregnant woman, the hypothalamus secretes corticotrophin releasing hormone that influences the pituitary. The pituitary secretes adrenocorticotropic hormone also known as corticotropin, which acts on the adrenal glands and the kidneys. The adrenal glands, in turn, secrete cortisol and the stress response is launched. In normal conditions, cortisol can provide feedback to the hypothalamus and stop the stress response. But under chronic stress conditions, cortisol levels stay high. In pregnancy, the process is altered. Cortisol levels during pregnancy are high anyway, but under stress the cortisol can cascade and also act on the placenta. The placenta can then launch its own stress attack, releasing more corticotrophin, which can then trigger delivery or influence fetal growth. Thus, food insecurity has a real role in metabolic disturbances during pregnancy.
Laraia illustrated a conceptual framework of household food insecurity on adiposity and health (see Figure 8-1). She hypothesized strong interactions with moderators such as acculturation, genetic factors, the life course stages critical for development, stress, and dietary restraint, and the food environment. She said that for all periods where growth is occurring rapidly and fat tissue is being laid down there is a strong interaction
________________
1Laraia and her colleagues, Cindy Leung and Amanda Murphy, prepared a commissioned paper on this topic for the workshop (Laraia et al., 2013a). Laraia acknowledged the assistance of her coauthors in developing her workshop presentation.
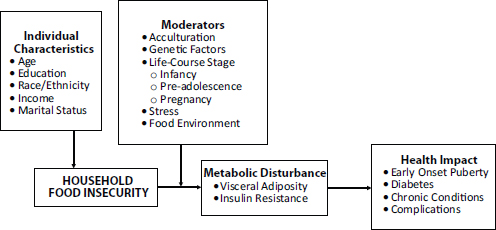
FIGURE 8-1 Conceptual framework of the effect of household food insecurity on adiposity and health.
SOURCE: Modified from Laraia (2013: Fig. 1) with permission.
with stress and dietary restraint and with the food environment. These periods include infancy, the first year of life, the adiposity rebound (ages 4–7), and pre-adolescence. Visceral adiposity and insulin resistance can all lead to negative health outcomes such as early pubertal onset, diabetes, chronic conditions, and other complications. Laraia stated that a focus on examining these interactions would help move research forward, looking specifically at the effects of food insecurity in the life course framework.
She noted Olson and Strawderman (2008) examined the relationship between food insecurity, pregnancy, and significant postpartum weight gain of the mother. They did not find that food insecurity was associated with developing obesity, but instead found a strong interaction between food insecurity and a woman who enters pregnancy already obese. This condition led to significant weight gain (4.55 kilograms, or 10–11 pounds) two years later.
Laraia presented results from the Pregnancy, Infection and Nutrition (PIN) Study2 with more than 2,000 women enrolled between 2001 and 2006. The survey asked questions related to socioeconomic status, eating behaviors, dietary intake, physical activity, and other health behaviors. It assessed household food insecurity status at 26–32 weeks gestation using the Household Food Security Survey Module (HFSSM) and included questions related to psychosocial factors such as perceived stress, trait anxiety,
________________
2The PIN Study was conducted by the Carolina Population Center, University of North Carolina; see http://www.cpc.unc.edu/projects/pin [August 13, 2013].
depression, locus of control, self-esteem, and mastery. When focusing on women whose income was under 400 percent of poverty, 15 percent were marginally food secure and another 10 percent were food insecure.
The study also showed associations with food insecurity and higher scores of stress, anxiety, depression, locus of control given to chance, and locus of control given to powerful others. Food insecurity was also associated with much lower scores of self-esteem and mastery. Thus, she said, food-insecure women are set up to possibly gain significant weight during pregnancy while having potentially lower coping skills (Laraia et al., 2006).
Returning to the topic of stress response, Laraia said that it has been well documented that chronic stress leads to either eating less (40 percent of animals and humans) or eating more (another 40 percent). In a food-abundant environment, more people overeat. In the stress response, high levels of cortisol are being produced, which activates metabolism, with an increase in insulin, leptin, and neuropeptide Y. These chemicals regulate not only metabolism and energy intake, but also, more importantly, where energy is stored. Eating under stress metabolizes food differently, and food and energy are shunted to visceral adiposity.
She said that food insecurity is a threat that can stimulate the HPA axis, triggering hunger and increasing the drive for feeding. The prefrontal cortex usually oversees decision making and reasoning, but under stress conditions, the limbic system overrides that prefrontal cortex. It taps into the reward system and influences the nucleus accumbens to help people reach for highly palatable foods (i.e., food dense with fat and sugar) to help dampen the stress response, which can lead to significant abdominal weight gain.
Laraia noted that in addition to activating the stress pathway and the reward pathway, the basal ganglia (the part of the brain that involves habit formation and memory) participates and a person learns quickly. The next time the person is under stress, he or she is biologically driven, even under a much lower level of stress, to reach for that non-nutritious food. Eating it in the presence of stress drives the store of fat tissues, specifically in the central abdominal region. Thus food insecurity can set people up for metabolic disturbances and chronic disease.
The PIN Study found that food insecurity was associated with greater weight gain, greater risk for gaining in excess of the Institute of Medicine (IOM) guidelines, and a much higher risk for developing gestational diabetes (Laraia et al., 2010). Gestational diabetes leads to insulin resistance and glucose intolerance later in life, so a fetus living in the environment of gestational diabetes is predisposed to childhood obesity, metabolic disturbances, and development of chronic disease later on in life. The study also found a strong interaction between food insecurity and dietary restraint.
The measure of dietary restraint focuses on weight cycling and dieting, so it is really a measure of failed past dieting. Women who scored low on dietary restraint but were food-secure gained significantly less weight than food-insecure women. The results were similar for women who scored high on dietary restraint: Women who were food insecure gained 10 or 11 pounds more than food-secure women, and they were more likely to gain in excess of the IOM guidelines (Laraia et al., 2013b). The mother was also more likely to retain that weight gain after pregnancy. Thus, the baby was more likely to be born with macrosomia or develop chronic diseases later.
Laraia reported that the PIN Study also found that food insecurity in the postpartum period was associated with a significant increase in stress beyond the baseline level of stress, which was already clinically significant. During the postpartum period, women in food-insecure households on average scored 7 points higher on Cohen’s perceived stress scale (Cohen et al., 1983). They scored higher on an eating attitudes test, which is a measure of eating behavior, and they ate 4 percent more calories from fat compared to their baseline intake. At 12 months, they retained almost a whole body mass index (BMI) unit higher. Thus, women who entered pregnancy overweight or obese and were food insecure were more likely to retain significant weight at 3 months (one BMI unit higher) and at 12 months (almost two BMI units higher) (unpublished data).
Food Insecurity and Outcomes for Children
Laraia observed the various methods and results in the literature presented age by gender-stratified results for intakes of different foods and nutrients, but results are mixed. Some models (8–20 percent) showed a significant association between food insecurity and nutrient intake, but results were not always significant in the same direction. There was not necessarily a decrease in fruit and vegetable intake or an increase in intake of highly palatable foods. Laraia suggested the research community form a priori hypotheses about how food insecurity is associated with dietary intake, and look at temporality as well. She also identified some data issues, such as that food insecurity may be measured over the past year (for example, in NHANES), but dietary intake is measured for the previous day. It would be useful to have a closer temporal association with those variables, she commented.
She characterized the research looking at Hispanic children as having done a good job with smaller convenience samples. The studies focused mostly on whole food intake and not necessarily on nutrients. The results showed more consistency in the measured association of food insecurity with lesser intake of meat, fruits, and vegetables. There was greater intake
of sweets and highly palatable foods. The various results still had inconsistencies, but at least food insecurity was associated with food intake in the hypothesized direction.
Laraia briefly discussed an animal study with the bonnet macaque monkey and variable foraging demands (Kaufman et al., 2007). The researchers’ results suggest that early life stress, characterized by the uncertainty of having enough food, during critical periods of neurodevelopment can result in the peripubertal emergence of obesity and insulin resistance.
Smith and Richards (2008) studied food insecurity among homeless youth in Minnesota and assessed different coping behaviors. Two of the most common coping behaviors were eating snacks (like chips, candy, and soft drinks) and overeating at mealtimes. If they were hungry, the youths said they would eat anything or they would find food somewhere else.
Laraia reported on an updated version of the marshmallow paradigm3 documented by Kidd et al. (2013) in a homeless shelter or food bank. They initially substituted poor art supplies for the marshmallows and children were told that they would get better supplies if they waited. Children were randomized into two groups. In the first group (reliable situation), children were given poor art supplies, and were told they would be given better art supplies and the art supplies were provided quickly. When they were subjected to the marshmallow test, being asked to wait and told they would be given a second marshmallow by the research assistant, the children waited 12 minutes on average. Children in the second group (unreliable situation) were also given poor art supplies in the beginning and were told that better art supplies would be provided. However, the investigator returned and told them there were no better art supplies available. When these children were subjected to the marshmallow paradigm, they waited an average of three minutes.
Laraia stated that cross-sectional studies have not shown a consistent relationship between food insecurity and child weight status, but said longitudinal studies will be the key to examining this issue, including the Early Childhood Longitudinal Study (ECLS). Existing research had mixed results. In children younger than age 2 in food-insecure households, there is no evidence of an associated weight change. When those children move into the adiposity rebound period (ages 4 to 7), the research begins to
________________
3This classic paradigm looked at delayed gratification and self-control among 4-year-olds. A child is given a marshmallow and said that if he/she waits to eat the marshmallow until the researcher returns, he/she will be given a second marshmallow. Results have associated a longer length of time a child is able to wait with higher confidence, higher academics, social and emotional scores, higher SAT scores, and a decreased likelihood of substance abuse. Poor delayed gratification was associated with being at risk of being overweight by age 11.
show some associations. Children subjected to food insecurity during infancy that persisted over time were associated with higher weight gain. She said additional research might try to identify for consistent outcomes.
Laraia provided an overview of several studies that looked at food insecurity in populations of children with chronic disease. Marjerrison et al. (2011) found that food insecurity is prevalent among children with diabetes and is associated with poor diabetes management in childhood. Mendoza et al. (2013), another small study, examined food insecurity and HIV among children. This study found household food insecurity associated with lower levels of CD-4 counts (immune system T helper cells) and higher levels of HIV viral loads. Laraia stated that future studies should consider the role of food security in chronic disease management.
Next Steps
In ending her presentation, Laraia posed several questions and provided her own views.
Is existing evidence sufficient to make causal claims? No, she said, there is not enough evidence to make causal claims. Many of the studies are cross-sectional, and there is evidence of a strong association. In pregnancy studies, there are temporality results that are not population based. There is consistency related to anemia. Regarding diet, there is significance in the expected direction but little consistency for the specific food or nutrient studied. There is considerable inconsistency with weight gain and disease management. Understanding causation is important, she said.
Does it matter how food insecurity is measured? Laraia stated that it depends on the research question. She referred to her comments about temporality issues in measurement between food insecurity and diet.
Are there important data gaps? Laraia said she favors fewer studies using cross-sectional data and more studies using longitudinal and linked administrative data. Big data may be a way to apply nonparametric models to understand interactions, she suggested. Laraia said that monitoring and surveillance beyond the prevalence of food insecurity will be important, as will be assessment of important modifiers of food security.
Are longitudinal, experimental, demonstrations, administrative, and qualitative data all valuable? She said these data are valuable, in her opinion, and are needed to identify causality. Experiments can show mechanisms. Interventions can show impact. She noted the efficiency in linking administrative data with survey data to monitor progress and show strong associations.
STATEMENT OF RAFAEL PÉREZ-ESCAMILLA
Pérez-Escamilla spoke on household food insecurity and the impact on children’s psycho-emotional and social development and on academic outcomes. He explained that the conceptual framework for his presentation posits that household food insecurity mediates the relationship of poverty, livelihood strategies, and suboptimal health among household members with maternal mental health and child psycho-emotional, social, and cognitive outcomes. The association between household food insecurity and poor maternal mental health and child development outcomes is, in turn, mediated by nutritional and non-nutritional stress-related pathways.
Household Food Insecurity and Child Psycho-Emotional, Social, and Cognitive Development
Pérez-Escamilla described a review of 26 studies examining household food insecurity and child development outcomes (Pérez-Escamilla and Pinheiro de Toledo Vianna, 2012). By design, all studies measured household food insecurity using an experience-based scale such as the HFSSM. With only one exception, all studies adjusted for socioeconomic and demographic confounders. He summarized the empirical evidence from these studies.
He said that cross-sectional studies conducted in the United States have consistently documented direct associations between household food insecurity and child development outcomes, including problem internalization and externalization and less ability to concentrate in the classroom. This evidence indicates that the relationship between household food insecurity and suboptimal child development can be detected from infancy and subsequently extends into the toddler, preschool, and school-aged periods. Cross-sectional data from the Children’s Sentinel Nutrition Assessment Program (C-SNAP; now Children’s HealthWatch) found a relationship between household food insecurity and poor child development outcomes among infants and toddlers. Likewise, studies have found negative psycho-emotional and behavioral outcomes among preschoolers associated with household food insecurity. A secondary analysis of NHANES data documents an association between household food insecurity and school-aged children’s hyperactivity, school absenteeism, or tardiness, as well as suboptimal academic performance, while further analysis of these data documents an association between household food insecurity and suicidal thoughts and attempts among adolescents. Likewise, a three-state study found that household food insecurity was associated with suboptimal psychosocial function among adolescents.
He reported that of five longitudinal studies, only one (Belsky et al., 2010) was conducted outside the United States, in the United Kingdom.
Analyses of ECLS-Birth Cohort (ECLS-B) data have found an association between household food insecurity exposure in infancy and suboptimal maternal attachment and parental attention at two years of age. Subsequent results from the ECLS-Kindergarten Cohort (ECLS-K) data found an association between household food insecurity exposure in kindergarten and suboptimal social and academic development in third grade. The remaining three longitudinal studies have found associations between exposure to household food insecurity at different ages after kindergarten on youth problem internalization and externalization, as well as lower IQ (in the case of the UK study when not adjusting for socioeconomic status).
Household Food Insecurity, Maternal Mental Health, and Parental Personality
Pérez-Escamilla reported that four cross-sectional studies have consistently documented associations between household food insecurity and maternal stress, anxiety, and depression, as well as problem internalization and externalization. He said a longitudinal study conducted in U.S. rural areas confirmed these associations.
Pérez-Escamilla stated another important question is whether parental personality mediates the relationship between household food insecurity and child development outcomes. Two longitudinal studies support this possible mediation. The analyses conducted by Huang et al. (2010), using data from the Panel Study of Income Dynamics (PSID), included the maternal personality traits of stress, warmth, distress, and self esteem. The E-Risk study conducted in the United Kingdom by Belsky et al. (2010) examined the maternal personality traits of openness to experience, conscientious, extraversion, agreeableness, and neuroticism.
Research Gaps and Policy Questions
To sum up, Pérez-Escamilla noted that different bodies of literature provide strong support for different segments or pathways in his conceptual framework (see Figure 8-2). Very few researchers attempted to test a framework such as this one using path analysis that allows for the identification of mediating factors based on sound conceptual models; however, he said, an exception is a study by Zaslow et al. (2009) based on ECLS-B longitudinal data. By following the approach of theory-based mediation analysis, they were able to discover that the relationship between exposure to household food insecurity at 9 months of age and insecure maternal-child attachment at 24 months of age was mediated by maternal depression and parenting practices. Similar findings were documented with regard to mental development at 2 years of age.
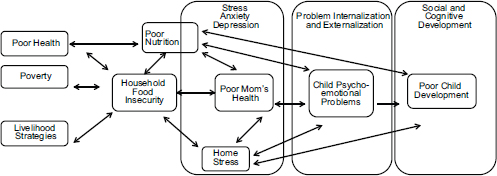
FIGURE 8-2 Conceptual framework of the effect of household food insecurity on child psycho-emotional, social, and cognitive development.
SOURCE: Modified from Pérez-Escamilla and Pinheiro de Toledo Vianna (2012) with permission. Figure 8-2
He reported that a major knowledge gap identified in his systematic review is the absence of mediation analysis studies via the dietary intake pathway of the framework. Decades of research have clearly documented the negative impact of malnutrition on child development. However, the vast majority of these studies have been conducted under conditions of protein calorie malnutrition and multiple micronutrient deficiencies, and the exposure was assessed with experience-based household food insecurity measures.
Pérez-Escamilla observed that another important gap is that studies have not been designed to find out if there is a critical period of initial exposure to household food insecurity in terms of child development outcomes. The answer to this question, he noted, has major relevance for policy decisions regarding how to better integrate food assistance and health care services, and how to design or improve existing programs across the life course. He said that an integration of findings from the literature clearly supports the policy research agenda to figure if and how parental mental health and child development remedial programs can be better linked with food assistance programs. A question concerns the importance of linking food assistance programs with parental mental health services or child development remedial programs, and whether a maternal child health care services screen might routinely also screen for household food insecurity, providing referrals for food assistance and child development evaluations.
STATEMENT OF ALISON JACKNOWITZ
Jacknowitz stated that a relatively large literature exists that investigates whether food insecurity influences children’s well-being. Most
of this literature, however, focuses on food insecurity as measured by a binary variable: Does the child live in a household that experiences food insecurity or not?
Jacknowitz presented her ideas to help move the research forward. First, she explored five gaps in knowledge with a focus on moving beyond this binary variable of food insecurity: (1) differential effects of food insecurity on children’s well-being, (2) the duration of food insecurity, (3) transitions in and out of food insecurity, (4) the pathways through which food insecurity influences children’s well-being, and (5) causal relationships. Jacknowitz also discussed whether current data sources adequately address these research gaps.
Differential Effects
She posed a question about whether the effects of food insecurity on children’s well-being vary by child or household characteristics. Gender is one of the most-studied characteristics, and she suggested pushing forward with gender analysis but including other variables, such as age of the child, language spoken at home, and urban versus rural location. She noted the considerable discussion at the workshop concerning the uneven landscape of services across the country, with pockets of better and worse social services.
Duration of Food Insecurity
Jacknowitz asked about the effect of length of time that a child spends in food insecurity on the child’s well-being, stating that with one exception, a study by Hernandez and Jacknowitz (2009), most research ignores this temporal component. She proposed that researchers address this issue both within a single year and over multiple years. One hypothesis could be that there are cumulative effects of food insecurity, but Hernandez and Jacknowitz (2009) found evidence that this might not be the case. That study used the nine-month and two-year data from the ECLS-B noting the food insecurity measure at both time points.
Jacknowitz reported that the study looked at the outcomes of cognitive and motor development as measured by the Bayley scores, weight-for-age z-scores, and health status. Given the above hypothesis, one would expect that a child who resides in a household that is food insecure in both waves would exhibit worse outcomes, but the study found no negative effects of experiencing persistent food insecurity. It is possible that those who experience persistent food insecurity have developed coping strategies to address the situation. The children experiencing no food insecurity
at nine months, but who experienced food insecurity at two years, had lower cognitive scores and health status.
Transitions
She reported these results lead to questions regarding the transition in and out of food insecurity, and whether the number of spells of food insecurity that a child experiences affects that child’s well-being. Food insecurity is a transitory condition, with a sizeable movement in and out of food security among low-income children. In understanding how this movement in can influence children’s well-being, Jacknowitz suggested that research look not just at movements from one year to the next, but at movements within any year. The hypothesis that constant food insecurity is worse than transitioning in and out of that condition may not be correct, which, she said, is a reason why further research is important.
Identifying the Pathway
Jacknowitz stated that understanding the pathway through which food insecurity affects the outcome of interest provides policy-relevant information—for example, whether the academic or socioeconomic outcome of a child living in a household experiencing food insecurity is influenced by maternal depression or maternal stress. She said that these pathways vary in three ways: (1) who experienced the food insecurity in the household, adult or child; (2) age of the child; and (3) specific outcome of interest (such as academic performance or health).
Causal Relationships
Jacknowitz reported that within the large literature on the negative consequences of food insecurity on children, only a few studies establish causal relationships. As a result, it is not known whether there is either reverse causation or endogeneity that may be biasing results. She said establishing the causal effect of food insecurity on children’s well-being is an important current research gap.
Can Current Data Sources Address These Gaps?
She reminded the audience that several major data sources are typically used in food insecurity research. They include two early childhood panel studies: ECLS-B, which focuses on children from birth to kindergarten, and ECLS-K, which focuses on children from kindergarten
through the eighth grade. Other important sources of cross-sectional data include the NHANES, Survey of Income and Program Participation, and Current Population Survey (CPS).
Jacknowitz argued that these data sources cannot answer the questions she posed. The ECLS-B is based on a nationally representative sample of approximately 10,700 children born in 2001. Data were collected when children were nine months, two years, and at preschool, with two kindergarten waves in 2006 and 2007. It includes the 18-item HFSSM and a rich set of children’s well-being measures, such as birthweight, weight in each wave, height or length, cognitive test scores, and socioemotional outcomes.
Jacknowitz found that the length of time between waves of the ECLS-B creates information gaps. The timing of the administration of the HFSSM does not match timing of outcomes of interest or possible mechanisms. For example, with maternal depression, it is unclear which came first, the maternal depression or the food insecurity. This is important to understand if studying causation. The ECLS-B does not include the 30-day food insecurity questions or ask about past food insecurity experiences, nor does it specifically isolate whether the targeted child is experiencing food insecurity. There is a measure of child-level food insecurity, but it is unclear whether the targeted child or another child in the household is experiencing that insecurity. Finally, very few children in this age group experience very low food security or even low food security. Thus, the effective sample size is small, making high-quality statistical analysis difficult.
Jacknowitz called for more longitudinal data with more frequent collection that follows children from birth over a longer period of time. She said this would allow researchers to better establish the timing of food insecurity and other events. She also called for more questions that can capture the duration and transitions into or out of food insecurity. Additional questions similar to those asked in the Three City Study4 would provide information on which child in a household is experiencing food insecurity. Finally, she said, research would benefit from datasets with larger sample sizes to improve statistical power, especially for infants and toddlers.
STATEMENT OF JOHN COOK5
Cook noted that Children’s HealthWatch’s interest in measuring and studying child food insecurity and hunger, and their causes and consequences, derives from an urgent sense to treat and eliminate what the
________________
4See http://web.jhu.edu/threecitystudy [August 7, 2013].
5John Cook (2013b) prepared a commissioned paper for the workshop.
organization sees as a totally unnecessary and imminently solvable threat to public health, to the public good, and to the country’s future prosperity.
He said that Children’s HealthWatch research focuses on the early childhood period because the first three years of life are a very vulnerable developmental period for children, with active brain growth and development, and cognitive development. Centric pathways are being developed for hearing and vision; pathways for language and higher cognitive function also are developing rapidly. In this period, exposure to trauma and chronic stress can be very harmful to children’s cognitive development and can also harm their trajectory toward success in life, as discussed by Chilton (see Chapter 5).
Cook said that exposure to stress partly affects brain architecture. Brain architecture is a physical structure, which includes systems, subsystems, and networks. Many of the 100 billion cells or neurons in the brain are interconnected in neural networks that store information and are involved in memory and learning in ways that are not yet fully understood. There is an increase in understanding how stress and trauma can affect that process and reduce the complexity and effectiveness of the neural networks, which can, in turn, affect the trajectory of a child’s cognitive development, academic school readiness, academic achievement, and educational attainment. Children’s health, growth, and development during this period determine whether they might later be chronically unemployed at low incomes as working adults, or fully employed at livable wages and higher incomes, which has profound effects on U.S. society.
The Measurement Framework
Cook provided some history about the development of the HSFFM (see also Chapter 2) and explained that the questionnaire and its associated scales were developed using item response theory (IRT). These methods can also be used to score responses to the scale items based on each item’s psychometric and statistical characteristics and the pattern of responses. IRT methods guide and inform decisions about thresholds and categories. The food security categories that are still used are human constructs, based on understanding and judgment.
Cook indicated that much has been learned since the food insecurity scales were developed, and he referred to reviews on this topic, including Cook and Frank (2008), Cook et al. (2013), Gundersen (2013a), Gundersen et al. (2011), Laraia (2013), and Nord (2009a).
Pathways
Cook categorized both nutritional and non-nutritional pathways through which food insecurity influences child health and development.
One example of a nutritional pathway is the perinatal nutrition of the mother and the child, including the internatal period for the mother. A very sensitive and vulnerable period follows (prenatally, and early in the first three years of a child’s life) for brain and cognitive development. Developmental events that usually happen during these periods either will not happen or will happen suboptimally in the absence of the necessary nutrients. Some of these deficits can be made up later on under the right conditions, but this is much more difficult and much more expensive than ensuring adequate nutrition during the prenatal period and early childhood.
Cook said adverse growth impacts from food insecurity and hunger persist in the United States, including stunting, wasting, structural system anomalies, endocrine system anomalies, obesity, and oral health issues, the latter of which he identified as an area that warrants more study. Food insecurity could also lead to a compromise in immune system functions, putting a child into what is referred to as an infection malnutrition cycle. When nutrition is suboptimal, it takes a child longer to recover from an illness, recovery is at a lower rate of health, and the cycle can repeat and lead to very strong effects on overall health.
He said energy deficits are relevant and can lead to compromised body temperature and regulation, particularly with regard to the “heat or eat” phenomenon. Babies cannot shiver and raise their body temperature so it is important to protect them and make sure they are well fed. Children who experience hunger are not as attentive to their environment—they want to find food, so they are not exploring other parts of their environment and learning.
Cook said examples of non-nutritional pathways include adverse impacts on the child’s and the mother’s mental health. Depression, as discussed throughout the workshop, leads to very strong effects on mother-child interactions and other adult-child interactions, one of the primary ways that young children learn. Depression impairs the responsiveness of both the mother and the child and interrupts the serve-and-return process of interaction. However, he said, depression is hard to understand in terms of its manifestation as well as in terms of policy, making it hard to conceive of policies that can address the issue with respect to food insecurity in an effective way, though Cook said that it is important to try.
Cook said that toxic stress (repetitive, persistent, or inescapable acute or chronic stress) includes acute stress like child abuse, domestic violence, and chronic stress such as recurrent or persistent hunger. He asked whether poverty and food insecurity might be a form of toxic stress, saying this is an open question to be clarified. A further example of a non-nutritional pathway involves delays in or deterrence of needed medical
care, and noncompliance with treatment. Over time, these pathways can have a profound effect on the child’s health, and both situations occur at significantly higher rates in food-insecure families.
Impact
Cook said that the impact of food insecurity on child health and development has been examined in a number of studies. Borders et al. (2007) found food insecurity positively associated with low birthweights. Laraia et al. (2006) examined psychosocial factors and socioeconomic indicators, finding food insecurity positively associated with psychosocial indicators of perceived stress, trait anxiety, and depression symptoms in pregnant women. There were indications of a dose-response relationship with greater effects at more severe levels of food insecurity. There have been a number of studies on breastfeeding; for example, Zubieta et al. (2006) found food insecurity negatively associated with both initiation and duration (if initiated) of breastfeeding.
Cook discussed two earlier scales that provided input and components for the HFSSM. Radimer, Olson, and Campbell (1990) and Wehler, Scott, and Anderson (1992) provided some of the earliest and most important information about relationships between food insecurity, hunger, and child health. Kaiser et al. (2002) studied food insecurity and nutritional outcomes of preschool-aged Mexican-American children using the Radimer/Cornell scale. They found that limited education, lack of English proficiency, and low income were all negatively correlated with food security, controlling for acculturation. Children in severely food-insecure households were less likely to meet the guidelines set out in the Food Pyramid. The percent of overweight tended to peak among children with household-level food insecurity, but the authors did not find significant differences with weight and height in the children.
He said Children’s HealthWatch conducted one of the earlier studies (Cook et al., 2004) that looked at the association between food insecurity and health in young children. They found that food insecurity is positively associated with fair to poor health and that receiving food stamps attenuated the effects of food insecurity on health status but did not eliminate them. Cook also referred to a study by Casey et al. (2004) on maternal depression, which found that maternal depressive symptoms were positively associated with household food insecurity, fair to poor child health, and child hospitalizations. Depression was also positively associated with reductions or loss of welfare and food stamps benefits. He said that Black et al. (2004) reported on a study on participation in the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) and infants’ growth and health, finding that infants under the age
of 12 months who did not receive WIC benefits because of access problems were more likely to be underweight, short, and perceived as having fair-to-poor health than WIC recipients. Infants receiving WIC and those eligible but not receiving WIC benefits because of access problems were more likely to be food insecure than infants whose caregivers perceived no need for WIC. Cook reported that Skalicky et al. (2006), working with the C-SNAP data, found child food insecurity positively associated with iron deficiency anemia in children 6–36 months of age. Neault et al. (2007) conducted a breastfeeding study on children of immigrant mothers and found that families of U.S.-born breastfed infants of immigrant mothers had greater odds of being food secure than those of nonbreastfed infants of immigrant mothers. The breastfed infants had lower odds of having fair-to-poor health versus excellent to good, of having a chronic health condition, and having been hospitalized less than nonbreastfed infants of immigrant mothers.
Cook said that Whitaker et al. (2006) used the food security scale to examine risk of depression and anxiety in early childhood. They found significant behavioral problems such as being aggressive, anxious/ depressed, and having inattention/hyperactivity in both the adults and children in households with food-insecure adults. Rose-Jacobs et al. (2008) looked at associations between food insecurity and at-risk infant and toddler development. Using the Parents’ Evaluations of Developmental Status (PEDS) scale, they found that food insecurity is positively associated with parental reports of developmental issues on the PEDS after controlling for confounders.
Cook noted some older studies used the questions and scale from the Community Childhood Hunger Identification Project (C-CHIP), as reported in Wehler et al. (1992), that was specifically designed to identify hunger in early school-aged children. Kleinman et al. (1998) used the C-CHIP scale to study hunger in children in the United States with a focus on behavioral and emotional correlates. Children who were categorized as hungry by the C-CHIP scale were more likely to have clinical levels of psychosocial dysfunction on the pediatric checklist then either at-risk or nonhungry children. The analysis of individual checklist items found that most behavioral, emotional, and academic problems were more prevalent in hungry children. Aggression and anxiety had the strongest degree of association with hunger. Murphy et al. (1998) used data from the same scale to look at relationships between hunger and psychosocial functioning in low-income children. They also found significant associations.
Cook reported that Weinreb et al. (2002), also using the C-CHIP scale, looked at hunger and its impacts on children’s health and mental health. They found that severe hunger was a statistically significant predictor of chronic illness in preschool-aged and school-aged children. It
was also significantly associated with internalizing behavior problems. Moderate hunger was a statistically significant predictor of health conditions in preschool-aged children, and severe hunger was associated with higher reported anxiety/depression among school-aged children. He also pointed to three important studies that Alaimo et al. conducted using NHANES data and the HFSSM (Alaimo et al., 2001a,b, 2002). Those studies provided important information that conditioned and guided later research on associating food insecurity with child health.
Cook said that Jyoti et al. (2005) was one of the most influential and important recent studies because using longitudinal data, it showed a priori and subsequent relationships between food insecurity and adverse outcomes, including some associated with both learning and health. Cook said this study may serve as a model for research in the future.
Cook pointed to four studies that address children’s experience of food insecurity. Connell et al. (2005) found that children in Mississippi ages 11–16 could describe food insecurity in terms of quantity: that is, eating less than usual or eating fast when food is available. They also described quality (having only a few low-cost foods) and food insecurity’s effect on psychosocial states, such as worry, anxiety, or sadness about the family’s food situation and shame/fear of being labeled poor. These children reported feelings of having no choice about what they had to eat, and also expressed an understanding that adults were trying to shield children from food insecurity. They described food insecurity in terms of social dynamics of using social networks to get food or being socially excluded. The study indicates that children have their own understanding of food insecurity. Fram et al. (2011) in South Carolina found that children 9–16 years of age experienced food insecurity distinct from their parents’ experience, and that adults were not always aware of their children’s experience of food insecurity. A study by Bernal et al. (2012) looked at children in Venezuela with very similar outcomes, while Fairbrother et al. (2012) reported that children in the United Kingdom incorporated media information in their expressions about food insecurity and about eating healthy. These children (ages 9–10) prioritized state and corporate responsibility in ensuring that eating healthy is affordable.
Cook stated that most Children’s HealthWatch studies make sure of their sentinel sample of more than 40,000 mother-child dyads with the dichotomous variable, household food security status as a predictor. In their studies, they found that food insecurity status was highly predictive of a number of adverse child health outcomes in children and caregivers. Children’s HealthWatch is currently engaged in a study funded by the University of Kentucky Center for Poverty Research and the U.S. Department of Agriculture (USDA) to test how foreign-born mothers’ status, together with risk and protective factors, are related to very low food
security in children. Very low food security was measured in 1.4 percent of the children in the Children’s HealthWatch data compared to 1.1 percent in the CPS data.
In a review of studies addressing marginal food security, Cook said he found that several studies presented evidence that marginal food security is more like food insecurity than it is like food security. All studies found that marginal food security is a significant predictor of adverse health outcomes in children or their mothers, compared to food security. New research shows that marginal food security is associated with the same negative health outcomes as food insecurity, but the magnitude of associations is intermediate between food security and food insecurity (dose response). Cook commented that marginal food security is a separate adverse category.
Closing Remarks
As wrap-up, Cook posed the question of how living in households where adults, but not children, have very low food security affects those children. He reported that in 2011, based on the official food security data from the CPS, his analysis indicates that there were nearly four million children who were not food insecure but lived in households where adults had very low food security. Because of time constraints during the workshop session, Cook pointed to his suggestions for proposed research topics in the background paper he prepared for the workshop (Cook, 2013b).
STATEMENT OF DIANE SCHANZENBACH
Schanzenbach began by commenting on the importance of he Supplemental Nutrition Assistance Program (SNAP) as the largest cash or near-cash antipoverty program in the United States. A large proportion of the U.S. population, 1 out of 6.5 people, is receiving food stamps, and she characterized it as the only universal safety net program in effect in the country. She said that the landscape for providing assistance to low-income families with children has changed since 1980, observing the United States has moved from a system of cash assistance to one with in-kind transfers. She also presented data that shows SNAP has become the fundamental safety net program compared to the Temporary Assistance for Needy Families (TANF).
Schanzenbach referred to a study by Almond et al. (2011), which looked at the initial rollout of the Food Stamp Program (1961–1975) to examine effects on infant health. Researchers have had difficulty separating cause and effect of the program because of its little variation
over time, but, by examining the rollout years, the authors could compare births in counties that received the program earlier with those that received it later. They found that the availability of food stamps in a county in the 1960s and 1970s increased overall birthweight and reduced the incidences of low-birthweight births, particularly concentrated at the bottom end of the birthweight distribution. There was a 2 percent decline in the number of infants born under 1,500 grams, a 2 percent decline in the number of births under 2,000 grams, and no change in the percent of birthweights that were under 4,000 grams.
These infants are now 40 and 50 years old. An important research question is whether this access to the safety net in utero and during early life led to longer term impacts in adulthood. Two theories could guide that question. First, Heckman (2006) argued that investment during early childhood leads to higher returns to human capital than investments later in life. In this hypothesis, access to the safety net, food stamps, will improve the acquisition of human capital during childhood. The second theory is based on a large literature (for example, Barker, 1992) on “fetal origins” that argues that there is a connection between fetal development and early “critical” periods and chronic conditions in adulthood. The hypothesis is that better early life health will improve adult health outcomes, such as potentially better overall health and reduced metabolic syndrome and obesity.
She said that Almond et al. (2011) also used data from the PSID, which provides information on economic and health outcomes. They categorized cohorts by county of birth to include the introduction of the Food Stamp Program in their analysis. With these data, the authors calculated two indexes. First was a metabolic syndrome index, based on health effects, such as whether a person in adulthood is obese, has high blood pressure, has diabetes, has had a heart attack, or has heart disease. The second is an economic self-sufficiency index, based on whether a person graduated from high school, is currently employed, is poor, or participates in TANF or food stamp programs, and his or her earnings and family income.
Schanzenbach reported that the authors found that exposure to the Food Stamp Program in early life reduced the incidence of metabolic syndrome by a highly statistically significant 0.3 standard deviations in adulthood. In looking at the component pieces of the index, only obesity was individually statistically significant, but all components changed in the expected direction. The authors examined other health outcomes (in good health, disabled, height below fifth percentile, ever smoked, drinking of alcoholic beverages). The only one of these outcomes that was individually statistically significant was that exposure to the food stamp program reduced stunting (height less than the fifth percentile). Other outcomes
changed in the expected direction, indicating that better health in early life leads to better health in adulthood.
She went on to say that the authors found that access to food stamps in early life increased economic self-sufficiency by a statistically insignificant 0.2 standard deviations. Looking at the component pieces, high school graduation or higher education was statistically significant. One important observation was that the indicators of receipt of welfare as an adult were negative. This may indicate that access to the safety net during childhood reduces dependency on the safety net in adulthood. Another important and puzzling result, she said, was that the authors found striking gender effects, with a strong statistically significant positive impact of early life access to the safety net on the economic self-sufficiency among women but not among men.
Thus, Schanzenbach said, the exogeneous shock to resources during early life (receipt of food stamps) improved adult health and, for women, improved economic outcomes. The study provided new evidence that the benefits of the safety net are broader than previously thought, with positive external benefits to taxpayers.
Schanzenbach provided several overview suggestions on research. First, she cautioned against focusing research too narrowly, saying that understanding how low-income families cope with different shocks will be beneficial. She went on to say that the measurement of food insecurity is vastly different in the PSID, CPS, and ECLS-K. A first-order question would be to understand and assess these differences. She noted policy-relevant research is important. She said she is not suggesting program evaluation, but a broad agreement to keep an eye on policy. She said that the Department of Education’s Institute for Education Sciences Initiative during the Bush Administration would be a good case study of the use of the federal “carrot or stick.” Finally, she said that funding of graduate students is important.
STATEMENT OF HILARY SELIGMAN
Seligman first discussed the hypotheses around the relationship between food insecurity and obesity. She explained that food affordability effects changes in nutritional outcomes because healthy foods cost more per calorie. Affordability changes dietary intake, which she said is the easiest way to conceptualize the increased risk of obesity. Researchers also see disordered eating practices (such as hoarding, binging, and preferences for calorically dense foods) in adults related to childhood food insecurity experiences in children, and it is important to look at this issue as it relates to the transition to adulthood. Food insecurity can be a major stressor during the adolescent period. Inflammatory mediators are par-
ticularly important in this discussion because they focus on physiological changes due to stress.
A pregnant mother may also transmit this risk of obesity to the next generation by making her developing fetus avid for nutrients. The unborn baby needs more nutrients if there is evidence that it may be born into a famine environment, thus predisposing children later in life to obesity risk because of the environment they experienced in utero. Seligman said this is very important because the risk of transmitting poverty to the next generation is even stronger than the risk of transmitting other diseases.
Seligman reviewed several studies looking at the association between food insecurity and BMI, extracting results for adolescents from these studies.
Parker et al. (2010) used NHANES data (1999–2006) categorizing boys and girls, 12–19 years, into four groups (food secure, marginal food security, low food security, and very low food security) and found the average BMI was highest for the marginal food security group. This result mimics what researchers see among adult women, she noted, and echoes earlier comments made by Laraia and Cook.
Theall and Dunaway (2013) conducted a study that used NHANES data, with results for 12- to 17-year-olds. The unadjusted association in this study showed the odds of having a BMI in the category of BMI 25 to 30 (overweight) was about 45 percent higher for individuals in a highly food-insecure family, a statistically significant increase. The measured odds were higher in the category of BMI greater than 30 (obese) but were not statistically significant.
Seligman briefly summarized other studies that used cross-sectional data from NHANES: Alaimo et al. (2001a); Bhattacharya et al. (2004); Casey et al. (2001, 2006); Gundersen and Kreider (2009); Gundersen et al. (2008); Lohman et al. (2009); and Smith and Richards (2008). She noted that except for Casey et al. (2001), these studies consistently found no relationship between food insecurity and BMI during adolescence.
Seligman said she views these results as limited, both because researchers were not always limiting analysis to a low-income cohort and because the data were cross-sectional. She said this highlights two weaknesses in using existing data for this type of analysis on adolescents: there is a lack of longitudinal data measuring food insecurity available for this age group, and food insecurity in these data is generally defined at the household level rather than at the child level, although the Lohman et al. (2009) and Gundersen et al. (2008) studies used the child food security status.
Seligman said food insecurity and obesity among adolescents may be associated with each other. The association is seen in unadjusted models, but it is probable that food insecurity is a marker for something else in the
adolescent period that is increasing obesity risk, including poverty in general, stress, or eating behaviors.
She argued that looking for obesity and other cardiometabolic risk factors among adolescents is the wrong question because the concern is the development of these long-term outcomes in adults. Obesity, diabetes, high blood pressure, high cholesterol, and metabolic syndrome do not generally develop over the course of a week, a month, or a year. They develop over decades and the failure to see them in adolescence does not mean that they are not there. Potentially, she suggested, the substrate is not detected early enough. To her, a more relevant research question is whether food insecurity during adolescence, childhood, or in utero is associated with cardiometabolic risk factors when the individual is 40, 50, and 60 years old. She said this outcome is important to understand not only because of the nutritional outcomes associated with food insecurity that could drive some of these cardiometabolic diseases, but also because coping strategies are laid down in childhood. It may be that coping strategies are leading to adverse health outcomes over time, and eating patterns established during childhood are resulting in cardiometabolic diseases many decades later.
Seligman read a quotation cited in Olson et al. (2007:203). A mother said, “I have this phobia about food and remembering that experience of having no food, now I constantly have to have food in the house, we start getting low and I start freaking.” The mother’s comment, Seligman says, raises a number of important points. First, the mother’s eating patterns were established when she was food insecure as a child. Second, she developed coping strategies that might increase her risk of chronic disease as an adult. Thus, even if her food insecurity when she was age two or four had no direct impact on her risk of diabetes as an adult, the way she is responding now probably does have an impact.
Seligman next provided a review of adult cardiometabolic risk factors and their association with food insecurity, saying that food insecurity, at least mild food insecurity, is consistently associated with obesity among women. Among women and men, there are associations with diabetes, high blood pressure, increased risk of some inflammatory markers, and metabolic syndrome. There probably is not an association with high cholesterol, she said, although a number of articles have found substratifications of cholesterol that are associated with food insecurity.
Seligman stated that a very important association is between food insecurity and tobacco, an association that does not get enough attention by researchers. Tobacco absorbs disposable income and, even more importantly, many smokers indicate that smoking makes them less hungry. This phenomenon is very important as a risk factor for poor health outcomes.
She said that studies, such as by Theall and Dunaway (2013), increasingly show that food insecurity increases the risk of inflammatory markers, and these inflammatory markers increase risk of many diseases. There are little data on most of these diseases in adolescence because, although possibly changing, people for the most part do not have these diseases in adolescence. Parker et al. (2010) used NHANES data for 12- to 17-year-olds to look at the components of the metabolic syndrome. The only difference in anthropomorphic measurements was in waist circumference for the marginal food insecurity group, a pattern that mimics what is seen in adults. There were no other differences in other components of the metabolic syndrome. An article by Theall and Dunaway (2013) looked at food insecurity and C-reactive proteins (CRPs), which researchers use to predict a person’s cardiovascular risk in 20–30 years. The study found no association between food insecurity and CRP levels among adolescents, although research has found the association with younger children.
In closing, Seligman addressed the research gap in terms of the long-term health implications of childhood food insecurity. She suggested longitudinal studies, starting with adolescents or younger, with follow-up into adulthood; a primary focus on understanding the health implications of food insecurity; repeated measures of food insecurity to develop a better understanding of what it is about food insecurity over time that confers the greatest risk, and whether there is a way to quantify the “dose” of food insecurity over time; robust measurement of health data, rather than relying on self-reported data; and robust measurement of coping strategies, public program participation, tobacco/drug use, dietary intake, geographic food access, and parental feeding behaviors.
OPEN DISCUSSION
Craig Gundersen (University of Illinois at Urbana-Champaign) began the discussion with two comments. First, he said, economists use cross-sectional data to establish causality. Conversely, even longitudinal data may or may not establish causality, so he said he would not dismiss the possibility of looking at causal issues using cross-sectional data. He stated some of the methods that can be used in this type of analysis have not been exhausted. Longitudinal data definitely provide advantages. Schanzenbach’s work illustrates how one can do more analysis if there is cross-sectional variation, and variation over time. Second, he urged a focus on what it is about food insecurity that really matters. Figuring out ways to isolate the effect of food insecurity (apart from other things) is important in terms of causality.
Laraia responded that she doubts that the causality of food insecurity in a life course framework can be identified with cross-sectional data
because there is a baseline issue. If an analyst observes a cross-sectional relationship, there is no way to know what came first. She said she considers it challenging to examine the health effects of food insecurity using cross-sectional data.
Ronette Briefel (Mathematica Policy Research) commented about the blurring of household-level versus individual-level measures. She stated the HFSSM is great for assessing food security at the household level (and by household characteristic or all adults/all children in the household). Its purpose was to provide a good population-based scale that could be measured and tracked over time. It is now widely used, but in ways that she said are inappropriate when trying to link individual-level food security to individual-level health and nutrition outcome data. She asked researchers to clearly think about the conceptual framework and their choice of a variable, as she said she sees a lot of blurring because a household-level indicator is being used as an individual-level variable. She also suggested that future research look at an exposure variable in terms of severity and duration. Even for studies that are appropriately using the 30-day measure to answer research questions, there is no good indication of the experience in the past, how well a 30-day measure tracks to longer periods (e.g., an annual measure), and whether survey respondents’ perceptions of food security change depending on severity and duration over time.
Seligman responded that she thinks that Briefel’s points are well taken and important. However, she said, if living in a household that is food insecure, an individual’s risk of being food insecure is very high whether every member in that household is food insecure or not. She said current measures are probably sufficient, because the children in the household are probably being underreported in terms of their individual food insecurity status. Briefel agreed, but something beyond the current four-category classification scheme would help, perhaps an intervention study or a small study to compare across subgroups. In particular, severity and duration measures would be important to assess variability within and across food security categories.
Deborah Frank (Boston University) observed that the technical problem with young children is that they cannot talk about the impact of living in a food-insecure household, although they show it physiologically. Cook said that a periodic census of the household members, in which all the people in the households are interviewed to collect food security information from each individual in the household instead of just the household respondent, or alternatively all adults and all children as groups could be done easily with the child scale. Although a little more expensive, the main cost is associated with having the household interview. James Weill (Food Research and Action Center) said that Seligman’s quotation from the woman who kept food in the house reminded him of people who grew
up during the Depression and who keep food in their homes many years later. It raised the question to him whether people in the current recession will change their long-term coping strategies and whether researchers are measuring that change. He noted data from a robust longitudinal study of adolescents, as advocated by Seligman, would support an analysis of whether interventions are reducing the use of coping strategies.
David Ribar (University of North Carolina at Greensboro) said that other countries routinely collect information from all members of the household, including sensitive measures on hardships. He said the difference is that these countries pay for high-quality surveys, but, he asserted, the United States underfunds its survey operations.
Edward Frongillo (University of South Carolina) referred to Schanzenbach’s remarks, noting the people who are the most disadvantaged are often most responsive to intervention. He also observed that the major gain researchers derive from longitudinal data is the elimination of unmeasured confounders, and not from getting to causality through a chronology of events. He agreed with Gundersen that sometimes cross-sectional data are very helpful. He highlighted Schlüssel et al. (2013) that, with coauthor Pérez-Escamilla, showed that different points in the life course reveal a different picture of how food insecurity is related to obesity. Referring to Laraia’s research, Frongillo pointed out other measures to be concerned about. BMI in children is particularly problematic because it does not get at fatness at all. Laraia responded that she agreed, but is concerned about using cross-sectional data to ask individuals about their food insecurity experiences in childhood. She said bias is associated with the way a family copes with a food insecurity experience. Longitudinal data are critical, she said, because she does not like asking adults whether they were food insecure as a child and using that to determine health outcomes.
Lara Shore-Sheppard (Williams College) said that she wanted to reiterate a comment from Seligman. Neither cross-sectional nor longitudinal data will do a good job if the correct thing is not being measured. She said she worries that the cause of the problem is not really known: food insecurity, whatever is triggering food insecurity, or some other kind of a shock. The current system does not measure the cause of the problem well and this matters for policy. She said food insecurity may suggest a wide set of policies. However, if the real problem is economic insecurity or another family issue, then food stamps may not be the best response. Considering the accurate targeting of policy to a problem, it is important to observe other things in addition to food insecurity.
Jay Hirschman (USDA) commented that it is helpful to focus on the measurement question. He noted that most researchers have used the HFSSM or variations of it, but the concept of existence and duration
are both important, as is the frequency of bouts of food insecurity. One of the measurement challenges is to devise a way for cross-sectional surveys to ask questions retrospectively over some period of time, which can be validated in some simple way and fed into the research process.



























