6
The National Prevention Council: Bringing Federal Agencies Together to Build Health and Resilience in Americans1
Highlights from the Presentations of Individual Speakers*
- Mandated by the Patient Protection and Affordable Care Act of 2010, the National Prevention Council (NPC) is coordinating health prevention activities across and within federal agencies that employ more than 4 million Americans. (Lushniak)
- The U.S. General Services Administration, an NPC member, has brought in farmers’ markets, promoted healthier food in its cafeterias, and supported bicycle share programs and walking paths around federal government buildings. (Damour)
- Major challenges in changing health behaviors within the federal government are a shortage of funding and the difficulty of sustaining momentum over time as administrations and political appointees change. (Levi)
- Leadership at the local level can unite a community and change its culture with respect to health issues. (Levi)
______________
*Highlights identified during the presentations and discussions; presenter(s) to whom statements are attributed are indicated in parentheses.
The second half of the workshop focused on five case studies of successful cross-sector initiatives aimed at fighting obesity. Speakers described the
____________________
1See Appendix B for additional information.
barriers and challenges faced by and lessons learned from their initiatives in the context of the four overarching considerations of health equity, sustainability, leadership, and measurement discussed in Chapters 2–5, respectively.
The first case study, discussed in this chapter, focused on the National Prevention Council (NPC), which was created under the Patient Protection and Affordable Care Act of 2010 to provide leadership and coordination across 20 federal agencies in working together on prevention, wellness, and health promotion activities.2 The member agencies represent sectors ranging from health and environment to education, housing, transportation, and defense.
Workshop attendees heard about the council’s efforts from the perspectives of three speakers: NPC chairman Rear Admiral Boris Lushniak, who is acting U.S. Surgeon General and oversees the U.S. Public Health Service Commissioned Corps; Susan Damour, regional administrator for the Rocky Mountain region of the U.S. General Services Administration (GSA), an NPC member; and Jeffrey Levi, executive director of the Trust for America’s Health, who chairs the NPC’s Advisory Group on Prevention, Health Promotion, and Integrative and Public Health. Melissa Lim Brodowski, acting senior advisor for policy and outreach with the Office of the Surgeon General at the U.S. Department of Health and Human Services, and Brigette Ulin, director of the Office of the National Prevention Strategy in the Centers for Disease Control and Prevention’s Office of the Associate Director for Policy, participated in the subsequent discussion.
DEVELOPMENT OF THE NATIONAL PREVENTION STRATEGY
Lushniak began by explaining that embedded among the hundreds of pages of the Affordable Care Act is a section emphasizing the importance of health prevention. “This is the law of the land,” he said. “This is really the first time that a major legislative piece told us, hey listen, it is not just about us treating illnesses and injuries—that we do have to get ahead of the curve.”
The NPC was formed within the U.S. Department of Health and Human Services and was initially chaired by former Surgeon General Regina Benjamin. Some of the 20 member agencies had to be convinced that they needed to be in the room, Lushniak recalled, because their department or office did not have the word “health” in its name, so they questioned what connection they had with health and wellness. “The learning curve, although at times rather steep, really pointed in that direction saying, ‘Guess what, we are all responsible for health and wellness by government
____________________
2For more information, see http://www.surgeongeneral.gov/initiatives/prevention/index.html.
policies, by the fact that we have . . . employees that we can influence,’” said Lushniak. Roughly 4.1 million people work for the federal government, all with family members, he noted. “What the feds do—this big elephant—in fact does leave an impact,” partly by setting a policy example for others to follow. “What we are asking people to do is stand in line with us because the prevention and health and wellness movement has to grab hold in this country,” said Lushniak.
In 2011, the NPC released the National Prevention Strategy (NPC, 2011), which focuses on seven priority areas for improving health and wellness among Americans (see Figure 6-1). Two of these priorities—active
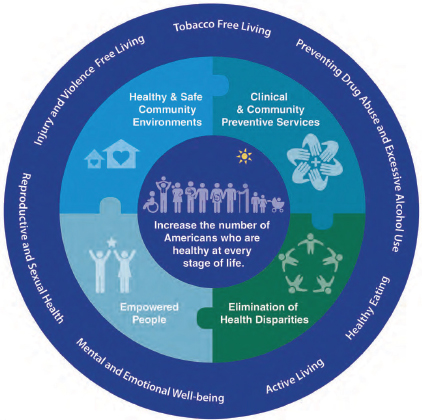
FIGURE 6-1 The National Prevention Strategy has four broad goals (inner circle) and seven priority areas (outer circle) for improving health and wellness among Americans.
SOURCE: NPC, 2011.
living and healthy eating—apply to the discussion at the workshop and are major parameters “that need to be altered in the formula of obesity in this country,” Lushniak said. “It is a complex world out there, but sometimes simplicity will bring us a step forward.”
The National Prevention Strategy lays out four strategic directions: healthy and safe community environments, clinical and community preventive services, empowered people, and the elimination of health disparities. The concept of “empowered people” is key, Lushniak observed, because Americans do not like to be told what to do. The job of public health officials is to get past health literacy barriers and provide people with correct information, whether it is about smoking or a nutritious diet, “so that ultimately, when it is decision time, they make the right decision.” With healthy eating, the goal is to provide the tools, the knowledge base, and the opportunity to access healthy food, including in “food desert” areas.
In 2012, moving toward implementation within its member agencies, the NPC created an action plan with three areas of focus (NPC, 2012): (1) introducing the concept of prevention into the lives of employees and staff, (2) tobacco-free workplaces, and (3) access to healthy foods within the “federal family.” “In public health, you cannot afford to be a pessimist,” Lushniak noted. “We have a new flag, and that new flag in the federal system is the National Prevention Strategy.” The Affordable Care Act “was not the most popular thing on this planet,” he pointed out, but it is the law and it is supported by the President. Lushniak’s personal view as acting surgeon general is that “we cannot drop the ball on this one. It has to continue with or without us in these leadership positions,” given that changes in administration will happen.
Lushniak hopes to elevate the public discussion of health to a level where people understand that “health is the most important thing for the future of our nation,” he said. “It runs the economy. It runs the defense of our country.” But the change in attitude has to begin at the individual level, starting with public health experts and health care officials “walking the walk,” Lushniak said. “We all need to be examples for everybody else.”
OBESITY PREVENTION IN THE GENERAL SERVICES ADMINISTRATION
Damour next described how prevention-related work is playing out within GSA and the “federal family” in the Rocky Mountain region. She is not a health expert but rather a “dealmaker” who oversees GSA operations in Denver and the five surrounding states.
GSA has child care centers, and 97 percent of all the child care centers across the United States sponsored by GSA are certified by the “Let’s Move! Child Care” campaign as promoting exercise and healthy food. Damour’s
agency also coordinated 19 farmers’ markets across the federal government, is working to ban e-cigarettes in its buildings, and is promoting healthier food and sustainable practices in its cafeteria and vending machine operations. The latter is an uphill battle, though, because “many of the people who are vendors in our areas are very frightened that the revenue will go down if they shift what they are doing,” she noted. GSA also supports bicycle share programs, walking paths, and fitness centers.
Damour’s favorite program is Feds Feed Families, in which all the federal agencies give food to community food banks. In her region, “we donated healthy food,” she said. “We bought food from our farmers’ market all summer long that was fresh fruits and vegetables—the only donations like that going into our food bank.”
On the federal level, the Rocky Mountain region is one of two regions in which regional surgeons general have brought U.S. agencies in their area together to form an active National Prevention Strategy team. Team members share best practices on, for example, making their buildings smoke-free and healthier for greater employee productivity.
Damour also has been building partnerships with communities, state health departments, and nonprofit organizations. In collaboration with the Boston-based literacy-promoting nonprofit Reach Out and Read, she created bookmarks in Spanish and English to hand out to families at child care and health centers as “a way to talk to parents, not only about good reading, but about good eating and good exercise.” Another exciting project she is developing is with Denver International Airport, which is a waystation for travel to states with limited services such as Montana, North Dakota, South Dakota, Utah, and Wyoming. Damour’s idea is to get the airport to partner with the NPC on creating walking paths in and out of the building and offering healthier food options or gifts, such as jump ropes, for children.
The strategies and projects Damour highlighted are about behavior change, but the challenge of bringing change to the federal government is “we don’t have the money,” she said. In addition, Damour noted that with people like herself being political appointees who come and go, a big question is how to sustain prevention and wellness champions when administrations change.
While there is consensus that multisector collaborations are needed to address the obesity epidemic, the question is whether the National Prevention Strategy can inspire broader federal leadership on this issue. Levi suggested that the NPC can be a model for how to proceed. The very process of writing the National Prevention Strategy helped shift the thinking of some
agency representatives who initially did not understand why they were part of the council, Levi pointed out. “That is the kind of culture change we need to be replicating,” he said
The Advisory Group’s mission is to think about the NPC’s potential for leading cross-sector approaches. That potential is important because Damour’s examples of bringing people together to collaborate are unfortunately the exception rather than the rule, Levi said. “Even with the obesity-related goals of the Prevention Strategy, the agencies have really been focused on interventions that can be achieved within their own silos,” he noted. The real success of the NPC and its National Prevention Strategy “will be measured when and if we see much more work across jurisdictions,” he said, and if federal agencies inspire common action among their employee constituencies and grantees.
To demonstrate the value of the cross-sector approach, the Advisory Group recommends that the future incoming surgeon general develop one or more focused community health initiatives designed to engage several Cabinet-level agencies in collaboratively addressing obesity or some of the social determinants of health. The Advisory Group also suggests that NPC agencies use a collective impact framework for assessing the initiative, including the use of common data-gathering mechanisms and outcome measures (Advisory Group on Prevention, Health Promotion, and Public Health, 2014).
Such an effort will encounter significant practical challenges, such as how different collaborating agencies will “braid and blend” funding streams on the ground, Levi noted. “If we really believe in these multisector collaborations, if we really believe that these things ought to come together, the federal government shouldn’t just be inspiring,” he said. “It needs to create the mechanisms that allow this to happen in an easier way at the local level.”
One new opportunity that has emerged from the Advisory Group’s work is a national collaborative on education and health that it established with support from the Kellogg Foundation, the Robert Wood Johnson Foundation, and Kaiser Permanente. The project is bringing people from the health and education sectors together to develop common health metrics that could be integrated into school report cards, and to work on integrating schools as key players in the health reform system. The Advisory Group also sees an opportunity for addressing obesity through the ongoing work on population health initiatives supported by the Centers for Medicare & Medicaid Services, which appears to be increasingly interested in addressing social determinants of health, Levi said.
Levi added that a particularly critical element for success is leadership at the local level that changes the culture in a community and brings it together. At the federal policy-making level, the fact that obesity is a major
driver of health care costs, which could diminish the nation’s economic competitiveness, helps in getting people to pay more attention to the problem. But workable solutions also are needed, and “we are now at the stage where we actually have some of those viable solutions,” Levi said.
“To me, cross-sector is the alignment of resources to meet common goals. . . . Obesity is one of those issues that we really need to address as parents, within the schools, within the community.”
—Lisa Gable of the Healthy Weight Commitment Foundation
This page intentionally left blank.








