WORKSHOP IN BRIEF ![]() JULY 2015
JULY 2015
![]() INSTITUTE OF MEDICINE
INSTITUTE OF MEDICINE
OF THE NATIONAL ACADEMIES
Advising the nation • Improving health
International Infectious Disease Emergencies and Domestic Implications for the Public Health and Health Care Sectors—Workshop in Brief
Emerging infectious disease events present a threat to U.S. national security, and we need improved efforts to coordinate a response both domestically and with global partners. The most recent outbreak of the Ebola virus disease in West Africa is the largest to date, affecting multiple countries simultaneously and once again bringing the challenges of global health security to the forefront of international preparedness discussions. The outbreak in the United States exposed health care system gaps and brought to a head the need for increased communication between hospitals and health departments and the need for clearer direction and coordination from state and federal agencies on operational standards and practices. SARS, MERS-CoV, and pandemic influenza are additional examples of why a global health security agenda is needed in the modern era of globalization. Some efforts in this area are already in progress, such as the 2005 World Health Organization’s (WHO’s) International Health Regulations (IHR), which include reporting compliance. Nevertheless, even when multiyear extensions were provided to implement these regulations, the percentage of countries meeting the requirements in 2014 was still less than 50 percent.
The Institute of Medicine’s (IOM’s) Forum on Medical and Public Health Preparedness for Catastrophic Events organized a session at the 2015 Preparedness Summit to discuss international public health emergencies, such as Ebola, and their corresponding impact on state and local public health and health care systems. After briefing the audience on the IHR and Global Health Security Agenda (GHSA) launched in 2014, speakers discussed their experiences during the Ebola outbreak in the United States and as it was unfolding in West Africa. They also discussed remaining challenges and explored ways to effectively respond the next time a public health emergency of international concern (PHEIC) arises. To put the session in context, Dan Hanfling, contributing scholar at the UPMC Center for Health Security and cochair of the IOM’s Preparedness Forum, highlighted the importance of coordinated and integrated global monitoring and awareness. Hanfling said, “In 2009, we weren’t looking to Mexico for the next infectious disease; we thought it would be Asia and were proved wrong. And in 2014, when the United States had mounting concerns that Ebola patients would appear in New York City or Washington, DC, we did not think to look at Dallas.” Ultimately, he stated, all global events start and end locally, and it is imperative that robust information sharing, monitoring, and regional response capabilities are created and maintained at the state and local level for the next time a disease crosses our border.
International Health Regulations and the Global Health Security Agenda
Rebecca Katz, associate professor of health policy and emergency medicine in the School of Public Health and Health Services at George Washington University, provided an overview of the IHR and how infectious disease reporting and U.S. compliance with these regulations fit within the global architecture. The IHR is a legal instrument, released in 2005 by the WHO, binding 196 countries across the globe to meet a set of standards with the goal of preventing, recognizing, and reporting local public health events that may become a PHEIC. As part of the IHR, national authorities have 24 hours from the time of identification to report an incident or information
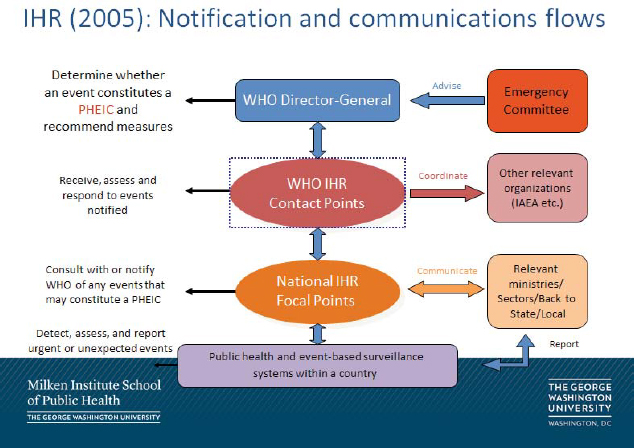
FIGURE 1 Information flow up to the WHO once a public health event has been deemed reportable through the IHR.
SOURCE: Rebecca Katz presentation, April 15, 2015.
of concern to the WHO at the international level, she explained. She added that Annex 2 of the revised IHR agreement complements and updates fixed lists of specific notifiable diseases with a “decision algorithm” to determine reporting need. This algorithm determines if the WHO should be notified of a public health event under the IHR. When the event is determined a potential PHEIC, the National IHR Focal Point—a middle coordinator of information and assessments up to the international authorities and down to the impacted county or regional level—is activated. Once the National Focal Point level is activated, the information flow continues up to WHO IHR contact points and then to the WHO director-general, who receives advice and recommendations from the Emergency Committee as to the appropriate emergency measures to initiate (see Figure 1).
Katz reported that there have only been three declared PHEICs since the rollout of the IHR: H1N1 in 2009, polio in 2013, and Ebola in 2014. However, ongoing disease surveillance is occurring for H7N9, MERS-CoV, and other infectious diseases in the event a PHEIC needs to be initiated and a greater set of measures to curb international spread is required. Annex 1 of the IHR, she explained, defines the core capacity requirements at the national, intermediate, and local levels that each country should be working toward and master (see Figure 2). Katz pointed out that, as of 2012, only about 21 percent of countries said they could accomplish the IHR within the required timeline. As of 2014, and under an approved extension, the number of compliant countries has risen to only about 37 percent. With these low numbers in mind, several member countries saw the need for more support of these important monitoring and reporting capabilities in all countries, many whose current health system infrastructure is poor or fragile.
As a way to address this IHR compliance issue, Katz described the 2014 launch of the GHSA where, together with international partners, the United States seeks to prioritize coordinated action and specific measurable steps to prevent, detect, and respond quickly to emerging infectious diseases, either natural or man-made.1 Within the
____________________________
1 For more information on the GHSA, see http://www.globalhealth.gov/global-health-topics/global-health-security/ghsagenda.html.

FIGURE 2 Core capacity requirements as defined within the IHR, Annex 1.
SOURCE: Rebecca Katz presentation, April 15, 2015.
GHSA there are a series of “action packages” that provide guidance in areas ranging from prevention to detection to response. Included in these action packages are baseline assessment and planning activities, as well as monitoring and evaluation activities focused on breaking down the broader issues of global health security into measurable, attainable goals. As of this workshop in April 2015, 44 countries have signed on to at least 1 of the 11 action packages outlined within the GHSA with a 5-year target goal, either for themselves or another country in need of assistance. To help understand the similarities between these two initiatives, Katz discussed the overlapping elements between the IHR and the GHSA (see Figure 3).
The U.S. Ebola Response: Public Health and Health Care Perspectives
With these two global initiatives as context, the following section gives firsthand accounts from the Centers for Disease Control and Prevention (CDC) and a local public health department of the U.S. Ebola outbreak experience beginning in 2014.
Federal Agency Perspective
Rear Admiral Stephen Redd, director of the Office of Public Health Preparedness and Response at CDC, gave his federal perspective of the Ebola outbreak and how the actions of the federal agency partners changed as the emergency in West Africa worsened throughout 2014. He emphasized that throughout the spring and summer of 2014, they were monitoring the outbreak and maintaining communication with their partners and stakeholders. Hanfling added that, during that time period, as early as April 2014, the Department of Health and Human Services’ Office of the Assistant Secretary for Preparedness and Response, through its Hospital Preparedness Program, developed a two-page resource sheet of frequently asked questions for health care providers about the

FIGURE 3 Overlapping focus areas of the GHSA and the IHR.
NOTES: AMR = antimicrobial resistance; NFP = National Focal Point.
SOURCE: Rebecca Katz presentation, April 15, 2015.
Ebola virus disease and that many health care systems and prehospital systems used this document to educate their employees.2
Recognizing that stopping patients prior to entering the health care system would be more successful in containing the disease spread, Redd said, the United States began the practice of screening travelers from affected countries at selected airports3 so those potentially exposed to the Ebola virus could be identified on entry into the country. Redd described the airport screening measures that, through strong partnerships with the Customs and Border Protection agency and the Transportation Security Administration, were subsequently put into place in mid-October 2014, following the diagnosis of the first domestic patient on September 30, 2014, who had traveled into the United States from Liberia. Through categorized risk assessments and follow-up with the local or state health department where the individual resided or was visiting (through prepaid cell phones that were given to high- and moderate-risk individuals), almost 13,000 travelers have been screened at U.S. airports; 350 of those travelers were identified to have some risk or high risk, and they received direct active monitoring.4
While the five enhanced screening airports and their partner health departments and hospitals seemed to have a higher likelihood of identifying a potential patient, it was still difficult to predict where other potential patients might present. Federal agencies disseminated information through all channels and all levels as part of their response. Nevertheless, it would not be practical or efficient for every hospital in the nation to prepare to treat and manage individuals suspected of having Ebola, as became apparent when the first domestic patient was
____________________________
2 For more details on the frequently asked questions, see http://www.aafp.org/dam/AAFP/documents/news/FAQs_Ebola_11_April_2014.pdf.
3 These included Atlanta (ATL), Chicago O’Hare (ORD), Newark Liberty (EWR), New York City (JFK), and Washington-Dulles (IAD).
4 For definitions on the different types of monitoring categories and other relevant guidance, see http://www.cdc.gov/vhf/ebola/pdf/monitoring-and-movement.pdf.
diagnosed and preparedness activities and corresponding needs and costs around the country skyrocketed. Many concerns arose regarding the acquisition and use of personal protective equipment. Two main questions were (1) how much and what types should health care facilities purchase and (2) how should facilities strike the balance between what was prudent and cost-effective. When two nurses became infected with the virus while treating a patient with Ebola at a Dallas hospital, many worried about the preparedness capabilities of local health care facilities that may be called on to treat future patients infected with Ebola. In response, CDC created a three-tiered system approach, Redd explained, comprising different levels of capability-based facilities throughout the country to form a national Ebola treatment center network. States were encouraged to adopt this approach, and acute health care facilities could choose to be a front-line health care facility, an Ebola assessment hospital, or an Ebola treatment center, with the latter two requiring more training and capabilities (see Figure 4). This way, not every hospital would need to spend precious time and resources building capabilities they might not need, knowing an Ebola treatment center was located within their region. Even more important, every hospital could focus on the capabilities and skills needed to be able to diagnose a patient under investigation (PUI), perform appropriate infection control practices, and provide care for them for up to 24 hours and until they were able to be transferred to the next level of care. As of this workshop in April 2015, Redd noted, there were 698 Ebola assessment hospitals throughout the country and 55 designated Ebola treatment centers.
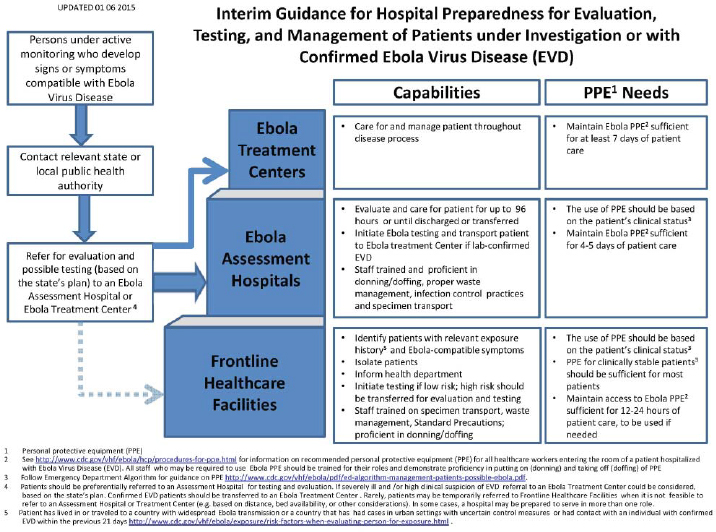
FIGURE 4 Interim guidance showing the breakdown in capabilities and personal protective equipment needs for the three levels of health care facilities: front line, Ebola assessment hospitals, and Ebola treatment centers.
SOURCE: Centers for Disease Control and Prevention, http://www.cdc.gov/vhf/ebola/pdf/evaluation-testingmanagement-of-patients.pdf.
Local Public Health Perspective
To view the challenges of the U.S. Ebola response through a different lens, Umair Shah, executive director of Harris County Public Health and Environmental Services (HCPHES) in Houston, Texas, discussed that agency’s local response. Highlighting again the need for international surveillance to be constant and embedded in domestic local health activities, he pointed to other responses they have activated—namely for Dengue fever and more recently Chikungunya—both previously only found outside the United States. To ensure that HCPHES is ready to respond should an international disease be identified in its jurisdiction, he said, the staff maintain ongoing surveillance of other countries and diseases. He stressed, however, that the indicators and triggers of such circumstances are not always clear and may be different from state to state and local jurisdiction to local jurisdiction.
Although Harris County did not experience any Ebola cases, it is just 240 miles from Dallas, Shah said, and many residents expressed concerns. These ranged from fear of attending the Super Bowl in Dallas to avoiding members within the community who had West African heritage. In particular, Shah described one compelling story where a community member of West African descent shared that no one had shaken his hand in months out of fear of contracting Ebola—illustrating the need for strong education and awareness in the United States of these sometimes poorly understood foreign diseases.
To be sure it was being proactive—to both effectively manage its surveillance activities and address community concerns—his agency created an “Ebola Readiness Team” (pointing out the importance of the word “readiness” versus “response” to show that there were no cases to respond to). Some of this team’s internal activities included monitoring global intelligence to gain domestic situational awareness; establishing potential triggers and indicators, such as increased disease activity in Africa, the United States, or Texas that would point to the need to expand the community response; and reviewing legal considerations and contracts to ensure capabilities were present to respond if needed. For example, the staff prepared template health authority orders and modified procedures so legal documents could be served safely and quickly. The team also worked with law enforcement to prepare to prosecute persons who falsely claimed to have Ebola. In addition, they reviewed ambulance contracts to determine which services were available if a patient suspected of having Ebola needed transport. On the public information side, Shah described community meetings the staff organized with community members from the affected West African countries to educate them on the disease spread and to make connections with populations who might not have had previous relationships with the health department. They also developed a publicly available Ebola web page containing a variety of outreach materials so partners, stakeholders, and associations representing some of the affected countries and populations could stay informed.
Further emphasizing the fact that a response to an infectious disease such as Ebola takes strong partnerships between the health care and public health communities, Shah discussed a recent exercise to test some of the HCPHES capabilities and those of its partners. In February 2015, a regional Ebola transportation ambulance exercise was held in conjunction with the local health care system, hospital preparedness program partners, and the regional coordinating body, the Southeast Texas Regional Advisory Council. Hospitals wanted to know who was in charge, which guidance to follow, who might be showing up on their doorsteps, and how public health could support them. He added that this exercise was a validation of the critical partnership between the federal hospital preparedness program and Public Health Emergency Preparedness funding streams and stakeholders.
In closing, Shah noted that even without any cases of the Ebola virus identified in the community, the cost in time, human resources, and direct financial support of the Ebola readiness activities was a large burden on the agency. In just this short period of time, less than 1 year, the agency accounted for more than 500 hours of readiness activities and more than $150,000 in labor costs, and even these were conservative estimates. He added that a timely and responsive communications platform such as a real-time video link system, on-demand teleconference capabilities, and necessary logistical support especially for outreach activities were all critical to the agency’s success. A question to consider is how all of these activities are being paid for and what other programs are suffering because so many labor hours are being redirected to these “readiness” efforts across the country.
Health Care and Hospitals Perspective
Alicia Schulhof, senior vice president of Continuous Process Improvement at Indiana University Health, explained the experiences of their health care system in Indianapolis during the second half of 2014, as they endeavored to prepare for any patient with Ebola virus to walk into one of their facilities. Consistent with the other speakers, Schulhof also reiterated that emergencies are local, and should a patient present at any of their facilities, that hospital is the one in control and responsible for managing the operations with system support. With so many different facilities within their system, she emphasized the importance of ensuring local readiness, but through coordination and learning together with a standard framework and consistent incident command structures (ICSs). On the external side, she said, they liaised with outside health, government, and emergency response agencies, but added that there were opportunities for improvement regarding funding and logistics, so they are establishing better coordination and communication channels with local, state, and federal partners.
In addition to the strong ICS framework throughout their system, Schulhof added, it was important to be sure that everyone was following the same procedures and was receiving the same level of training to ensure that standard protocols were adhered to throughout the care system. They developed a system process flow map for any patients presenting to one of their facilities, which would direct the care provider to take a standard set of actions on the basis of patient answers. Furthermore, they developed an Ebola readiness checklist to help facilities identify critical gaps and gain an overall understanding of the different facilities’ readiness levels.
From a “lessons learned” perspective, Schulhof said, across the board she thought their use of “lean methodology” was extremely helpful in quickly examining their systems and protocols and identifying gaps. Lean methodology is a set of operating philosophies and methods that help create maximum value for patients by reducing waste and waits. It aims to fundamentally change organization thinking and value, which ultimately leads to the transformation of organization behavior and culture over time (Lawal et al., 2014). They created a “Vertical Value Stream Application,” which helped identify value steps as well as wasteful steps in the process by charting the actions of each employee in vertical streams and each task (and the relevant personnel and resources needed to complete it) in horizontal streams. Their lean methodology approach also encourages the input and knowledge of front-line staff, as they can be the first caregivers to recognize where waste can be eliminated and how to better standardize such processes. In addition, including the “appreciative inquiry” to the standard After Action Report process was key to their overall assessment, she thought. Appreciative inquiry is strategic change to increase sustainable growth for organizations through the engagement of all stakeholder groups in a collaborative approach to decision making (Cooperrider et al., 2005). But instead of solely focusing on the negative problems within their process, they also looked for strengths and accomplishments, which allowed them to have a more positive outcome and staff engagement during a chaotic and stressful time within health care.
Transposing International Emergencies to the Domestic Front
An emergency in another country can quickly become an emergency in this country, noted Katz, reiterating the motivation behind much of the GHSA. This is no longer just altruism, she said, but truly a matter of national security. Schulhof highlighted an important question: “How can we be most effective and efficient with the preparedness funding that public health and health care does receive to make global health security a sustainable effort?” Schulhof added that in addition to the lack of funding available to maintain preparations and systems that have been built in between disasters, there is a need for standards and measurements so that the limited funding can be distributed in an evaluative, standard way. Her hospital declined being an Ebola treatment center because it did not think it was prepared to treat such cases, but it found out afterward that other facilities, which she perceived as less prepared than her hospital was, had said yes. Without having measures and standards to compare to, each organization relies on using its own subjective benchmarks for measurement, making for a potentially haphazard compilation of Ebola treatment units that should ideally have the same standards.
Confusion in Response Leads—Nationally and Internationally
A participant from Florida noted that differing and sometimes conflicting guidance was coming from CDC, the state health departments, and the Occupational Safety and Health Administration. There was also often pressure from labor unions to go further than the recommended guidance proposed by these agencies in terms of worker safety, and without a single voice, he said, it was difficult to decide how to proceed. Eventually, his group simply made a decision to follow CDC guidance, but still was uncertain if this was the right choice. Acknowledging the differences in health care system relationships across states, he noted that public health and hospital systems are not always well connected. Hanfling highlighted this as a clear need to focus on interagency coordination and clarity of discussion. Schulhof also agreed, noting that there were multiple e-mails and webinars and guidance and instructions coming from a variety of sources. The overwhelming amount of information that was being disseminated added to the already present chaos, and many participants commented that one coordinated source of guidance would have made the synthesis of information much easier.
Examining this issue from a different angle, Tim Stephens, executive director of the MESH Coalition in Indianapolis, said that more information does not always mean better outcomes. He further commented that more than $1 billion was spent by agencies to provide health care during this outbreak, except they did not need to provide any care, just engage in significant preparedness efforts in the event they did receive a PUI. Currently, there is no mechanism to recover the money that was spent simply preparing or, as Shah described in HCPHES, working on readiness activities, but not response. Stephens concluded by saying there is no command and control for providing health care in our country, which makes a strong, coordinated national response to an infectious disease extremely challenging.
Leveraging an Existing Knowledge Base
Understanding that the last worldwide infectious disease outbreak was more than 5 years ago, it can be difficult to keep health care staff well educated and trained on appropriate infection control procedures. In addition, with so many potentially emerging diseases with different transmission routes and infectivity, it is impractical to have all health care staff trained on every possible pathogen. However, as a participant from Minnesota pointed out, there are existing knowledge bases that can be leveraged in these different areas. Organizations such as the American Refugee Committee and the International Rescue Committee have travel medicine and tropical medicine experts who often have this detailed knowledge to share. Some participants asked about having a “global medical reserve corps” similar to the U.S. Medical Reserve Corps, where units are trained in ICSs and respond in their communities and region following disasters. Though, in these types of infectious disease epidemics an additional level of specific training relevant to the outbreak may be necessary. Hanfling commented that broadening coalitions to include groups such as these speaks to the validity of having a regional capability.
In addition, another participant spoke about volunteers who are coming back from affected countries into their home communities. How can we do a better job of making sure they return safely and healthy, he asked, but also work to incorporate them into coalition or training practices happening domestically that they have the knowledge to inform?
Sustainability in Infectious Disease Response
“Sustainability has been one of our biggest challenges,” voiced a participant from California. Since October 2014, she said, her team at the state level has had daily meetings and weekly calls, which have since shifted to weekly meetings and monthly calls, still taking up a significant portion of staff time. And while they are trying to set up the regional network to satisfy the three-tier approach, she noted that they struggled to get buy-in from the local hospital system level. There are 58 health care coalitions in California, she said, but they cannot have 58 Ebola assessment hospitals across the state. To add to the complexity, the participant said, 80 percent of the counties in California are rural, so it is not sustainable to have one prepared ambulance sitting out of rotation all the time just in case an Ebola PUI presents. Another participant suggested connecting health care–associated infection, infectious disease, and emergency preparedness programs to better promote sustainability with these similar and sometimes
overlapping issues. If these representatives can meet every single day and be fully aware of what is happening across different programs, they can be informed of the corresponding implications for their own programs. Instead of emergency events demanding staff coordination and leaving other duties behind, having ongoing meetings and communication could produce a more streamlined response without leaving nonemergency responsibilities from being completed.
Agreeing with the need for sustainability, Schulhof asked whether it was plausible to create a stand-alone biocontainment unit by combining resources across sectors and partners, which has been done and was used successfully during the Ebola outbreak in Nebraska. Many questions accompany that idea, however, such as the following: Who is responsible for licensing? Who owns the facility? Who is responsible for staffing? In the case of the Nebraska Biocontainment Unit, the facility is a collaboration among the University of Nebraska Medical Center, Nebraska Medicine, and Nebraska Health and Human Services and initially cost $750,000 to build in 2005.5 Although it is a 10-bed unit, the maximum number of patients the 40-member staff could handle would be no more than three at a time, depending on acuity. Schulhof also offered the idea of partnering with the National Guard—which has a sustainable model for responding to emergencies that comes complete with training. Regardless of which option is chosen, she emphasized that just because the worldwide Ebola outbreak has diminished, the important work and recent advancements cannot wind down and disintegrate before the next emergency.
Another participant also voiced concern around the sustainability of this work because there was never a guarantee that “something” would happen in a particular jurisdiction or community. Some counties might show interest or have “one-off” meetings, but then would lose interest just as quickly. Hanfling asked whether coordination and consistency at a health care coalition level would be enough to achieve the integration of coordination and consistency overall at a city or county level. Many participants said that would be helpful, but there is a need for a systems perspective that offers transparency when it comes to making important decisions regarding the public’s health and safety. The higher profile the incident, the higher level at which decisions are made (e.g., school closings, mandated quarantines), and because of that, a participant said, there can be unintended consequences that trickle down from higher levels.
Emergencies Begin and End Locally
As stated during Hanfling’s remarks, as well as during statements by other members of the panel, location truly matters because all events start and end locally. Nonetheless, Schulhof commented, sometimes “local” is not well defined. Even the different players and reporting structures at the local level should be well understood so that in times of crisis important time and resources are not lost to inefficiencies and confusion. In closing, Hanfling offered that there is value in making sure there is an awareness of the IHR and the GHSA within the United States and in recognizing where the gaps are—both globally and domestically—whether they are found in surveillance, detection, or elsewhere. After this experience with Ebola, he said, it is clear that many people better understand and recognize that the risk of international incidents arriving in the United States is as simple as one plane ride away. As discussed previously, however, sustaining that important understanding will be imperative to support the work and progress that have been achieved in the past year. Forgetting these lessons and the reality of emerging infectious disease threats before the next incident occurs outside of our borders would be a disservice to all those who have worked and suffered through this worldwide event. ![]()
References
Cooperrider, D., D. Whitney, and J. Stavros. 2005. Appreciative inquiry handbook. San Francisco, CA: Berrett-Koehler.
Lawal, A. K., et al. 2014. Lean management in health care: Definition, concepts, methodology and effects reported (systematic review protocol). Systematic Reviews 3:103.
____________________________
5 Nebraska’s Biocontainment Unit became operational in 2014, but because of its structure and strict training, it was able to receive and successfully treat several patients with Ebola. For more on the Nebraska Biocontainment Unit, see http://www.nebraskamed.com/biocontainment-unit.
Forum on Medical and Public Health Preparedness for Catastrophic Events
Dan Hanfling (Co-Chair)
Consultant, Bethesda, MD
Lynne R. Kidder (Co-Chair)
Consultant, Boulder, CO
Alex J. Adams
National Association of Chain Drug Stores, Alexandria, VA
Roy L. Alson
American College of Emergency Physicians, Winston-Salem, NC
Kathryn Brinsfield
Office of Health Affairs, U.S. Department of Homeland Security, Washington, DC
Susan Cooper
Regional Medical Center, Memphis, TN
Brooke Courtney
Office of Counterterrorism and Emerging Threats, U.S. Food and Drug Administration, Washington, DC
David T. Dyjack
National Association of County and City Health Officials, Washington, DC
Bruce Evans
National Association of Emergency Medical Technicians, Upper Pine River Fire Protection District, Bayfield, CO
Julie L. Gerberding
Merck Vaccines, Merck & Co., Inc., West Point, PA
Lewis R. Goldfrank
New York University School of Medicine, New York
John L. Hick
Hennepin County Medical Center, Minneapolis, MN
James J. James
Disaster Medicine and Public Health Preparedness, Onancock, VA
Paul E. Jarris
Association of State and Territorial Health Officials, Arlington, VA
Lisa G. Kaplowitz
Office of the Assistant Secretary for Preparedness and Response, U.S. Department of Health and Human Services, Washington, DC
Michael G. Kurilla
National Institute of Allergy and Infectious Diseases, Washington, DC
Donald M. Lumpkins
Federal Emergency Management Agency, U.S. Department of Homeland Security, Washington, DC
Jayne Lux
National Business Group on Health, Washington, DC
Linda M. MacIntyre
American Red Cross, San Rafael, CA
Monique K. Mansoura
Novartis Vaccines and Diagnostics, Inc., Cambridge, MA
Suzet M. McKinney
Chicago Department of Public Health, IL
Nicole McKoin
Target Corporation Furlong PA
Aubrey K. Miller
National Institute of Environmental Health Sciences, Bethesda, MD
Matthew Minson
Texas A&M University, College Station
Erin Mullen
Pharmaceutical Research and Manufacturers of America, Washington, DC
John Osborn
Mayo Clinic, Rochester, MN
Tara O’Toole
In-Q-Tel, Arlington, VA
Andrew T. Pavia
Infectious Disease Society of America, Salt Lake City, UT
Steven J. Phillips
National Library of Medicine, Bethesda, MD
Alonzo L. Plough
Robert Wood Johnson Foundation, Princeton, NJ
Lewis J. Radonovich
U.S. Department of Veterans Affairs, Washington, DC
Stephen C. Redd
Centers for Disease Control and Prevention, Atlanta, GA
Mary J. Riley
Administration for Children and Families, U.S. Department of Health and Human Services, Washington, DC
Kenneth W. Schor
Uniformed Services University of the Health Sciences, Bethesda, MD
Roslyne Schulman
American Hospital Association, Washington, DC
Richard Serino
Senior Advisor, Harvard University, Boston, MA
David Smith
U.S. Department of Defense, Washington, DC
Margaret Vanamringe
The Joint Commission, Washington, DC
W. Craig Vanderwagen
Martin, Blanck & Associates, Alexandria, VA
Jennifer Ward
Trauma Center Association of America, Las Cruces, NM
John M. Wiesman
Washington State Department of Health, Tumwater
Gamunu Wijetunge
National Highway Traffic Safety Administration, Washington, DC
Matthew K. Wynia
Center for Bioethics and Humanities, University of Colorado, Denver
DISCLAIMER: This workshop in brief has been prepared by Megan Reeve, Jack Hermann, and Ashley Ottewell, rapporteurs, as a factual summary of what occurred at the meeting. The statements made are those of the authors or individual meeting participants and do not necessarily represent the views of all meeting participants, the planning committee, or the National Academies.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this workshop in brief was reviewed by Gio Baracco, Veterans Health Administration; Veronica Rodriguez, Wayne County Department of Public Health; and Ali Khan, University of Nebraska Medical Center. Chelsea Frakes, Institute of Medicine, served as review coordinator.
SPONSORS: This workshop was partially supported by contracts between the National Academy of Sciences and the American College of Emergency Physicians; American Hospital Association; Association of State and Territorial Health Officials; Centers for Disease Control and Prevention (Contract No. 200-2011-38807, TO #30); Infectious Diseases Society of America; Martin, Blanck & Associates; Mayo Clinic; Merck Research Laboratories (Contract No. APA-2014-1666); National Association of Chain Drug Stores; National Association of County and City Health Officials; National Association of Emergency Medical Technicians; Novartis Vaccines and Diagnostics, Inc.; Pharmaceutical Research and Manufacturers of America; Robert Wood Johnson Foundation; Society for Disaster Medicine and Public Health; Target Corporation; Trauma Center Association of America; United Health Foundation; U.S. Department of Defense (Contract No. HT0011-11-P-0186); U.S. Department of Defense, Uniformed Services University of the Health Sciences (Contract No. HT9404-12-1-0022); U.S. Department of Health and Human Services’ Administration for Children and Families (Contract No. HHSP2332014001533P); U.S. Department of Health and Human Services’ National Institutes of Health: National Institute of Allergy and Infectious Diseases, National Institute of Environmental Sciences, National Library of Medicine (Contract No. HHSN26300007 [Under Base 1 #HHSN263201200074I]); U.S. Department of Health and Human Services’ Office of the Assistant Secretary for Preparedness and Response (Contract No. HHSO100201000021P); U.S. Department of Homeland Security’s Federal Emergency Management Agency (Contract No. HSFE2013-P-0212); U.S. Department of Homeland Security, Office of Health Affairs (Contract No. HSHQDC-13-J-00384 [Under Base 1 #HSHQDC11-D-00009]); U.S. Department of Transportation’s National Highway Traffic Safety Administration (Contract No. DTNH22-10-H-00287); U.S. Department of Veterans Affairs (Contract No. 101-G09041); and U.S. Food and Drug Administration (Contract No. HHSF22301027T [Under Base Contract DHHS-8598]). The views presented in this publication do not necessarily reflect the views of the organizations or agencies that provided support for the activity.










