2
Transportation to Health-Related Destinations
To set the stage for discussion, Carolyn Flowers, the acting administrator of the Federal Transit Administration (FTA), provided a brief overview of FTA-supported efforts relating to transportation for accessing health care. Bruce Robinson, the acting associate administrator for program management at FTA, described the FTA Rides to Wellness initiative in more detail, and Oscar Gomez, the chief executive officer of Health Outreach Partners, discussed the Rides to Wellness Community Scan, a survey of the outcomes of missed appointments. Following the overview of FTA-supported efforts, Heidi Guenin, a senior associate at GridWorks, presented a synopsis of her findings from an environmental scan of health care and transportation partnerships around the nation, commissioned by the National Academies of Sciences, Engineering, and Medicine for this workshop.
The presentations were followed by comments from discussants Art Guzzetti, the vice president for policy at the American Public Transit Association (APTA); Heather MacLeod, the assistant director of physical infrastructure in the Seattle field office of the U.S. Government Accountability Office (GAO); and Judy Shanley, the vice president for education and youth transition at Easterseals, Inc. The session was moderated by Ysela Llort. (Highlights are presented in Box 2-1.)
FTA-SUPPORTED TRANSPORTATION EFFORTS
The fact that some patients lack reliable transportation is a serious health care challenge, Flowers began. Although many warnings about health threats garner prominent media attention (e.g., the Zika virus, opi-
oid abuse, obesity), most people are generally unaware of the considerable impact that lack of transportation has on health. Overcoming this challenge, Flowers added, will require education and involvement of the public and leaders at the local, state, and national levels.
In 2008, 48.6 million Americans, or nearly 16 percent of the U.S.
population, lacked health care insurance, Flowers said. Today the uninsured rate has dropped to 9.2 percent, which is the lowest it has been in the past 50 years. Current enrollment in the health care marketplace is 12.7 million, she continued, and roughly 20 million people total are enrolled through the marketplaces, Medicaid expansion, young adults remaining on their parents’ insurance, and other expanded coverage. The Patient Protection and Affordable Care Act (ACA) is built, in part, on the premise that regular, affordable access to primary care can lower costs and improve health outcomes over an individual’s lifetime. However, every year approximately 3.6 million Americans miss or delay nonemergency medical treatment despite having health care coverage because they lack transportation to care (Myers, 2015). The ACA will be unable to live up to its full promise if people cannot get to care, Flowers said, and she shared some of the ways in which FTA is leading the search for solutions.
FTA has been working closely with the U.S. Department of Health and Human Services (HHS), the Centers for Medicare & Medicaid Services (CMS), the U.S. Department of Agriculture, the U.S. Department of Veterans Affairs (VA), and others to start the Rides to Wellness initiative (discussed further below). With the help of the Fixing America’s Surface Transportation (FAST) Act,1 Flowers said, FTA will be funding innovative programs to help connect people to health care through public transportation. The need is great, she said, and during the first round funding opportunity, FTA received proposals for more than three times the available funding. FTA is working quickly to identify and fund those proposals with the best chance for success. FTA is also holding regional forums across the country to bring together stakeholders in the transportation and health care industries who often rely on one another but who have had few chances in the past to consider these challenges together. In addition, FTA is fostering cooperation among federal agencies through the Coordinating Council on Access and Mobility (CCAM). The council was created in 2004 by executive order, and its work has been given new energy and focus through the FAST Act, which charges the council with publishing a strategic plan within the next year.
Because solutions will ultimately be local, responding to local concerns and being carried out with local resources, Flower said, it is very important that stakeholders come together (such as at this National Academies of Sciences, Engineering, and Medicine workshop) to consider the fundamental questions and share their results. In closing, she reiterated the point by Behney that one of the most important questions is how to define and measure the success of investments in transportation and how to understand
___________________
1 More information on the FAST Act is available at http://www.fhwa.dot.gov/fastact (accessed August 4, 2016).
if improved access to health care facilities has made a difference in public health outcomes.
Rides to Wellness Initiative
Transportation is a key factor in quality of life, Robinson said; it fosters healthy communities, promotes civil rights, and enables access to jobs, affordable housing, education, and training. As Flowers had explained, FTA launched the Rides to Wellness initiative to help address the important issue of transportation to health care. The initiative’s goals are to leverage public transportation assets and services to improve access to health care, improve outcomes, and reduce health care costs, Robinson said. The vision is that through Rides to Wellness, people and community health will thrive. As FTA administered its grants to state and local providers, it saw an opportunity to leverage its investments together with other federal investments to help reduce the gap between health care and transportation. This initiative was supported by the FAST Act, which established a new FTA grant program with funding over 5 years for services related to nonemergency medical transportation (NEMT) and also established requirements related to CCAM (described by Flowers, above). Robinson said that this issue has been around for a very long time and that GAO has produced several reports for FTA with recommendations related to NEMT and to the coordination of rules and requirements across federal partners that provide transportation services. He also noted that years ago FTA had established the United We Ride program, an interagency initiative through CCAM, to help coordinate between transportation and human services programs.
In establishing the Rides to Wellness initiative, Robinson said, FTA was particularly interested in understanding challenges and solutions at the community level. One of the first programs launched was the Healthcare Access Challenge Grants program, which has provided grants to 16 communities to consider ways to improve access to health care and to bring new community partners into the discussion. Another approach, as had been mentioned by Flowers, is a series of regional forums where community grantees and members of the public transportation sector can engage on the issues and challenges facing communities. A recent regional forum in Charlotte, for example, included speakers from the Raleigh–Durham area who described the challenges of residents who may have insurance but who also have other barriers that make it difficult for them to understand how to access public transit or even how to get to health care when transportation is provided. Input from the regional forums indicates that the relevant issues are not only access to care and the availability of transportation, Robinson emphasized, but also the need to help individuals understand
the options available to them and, in some cases, help them through the process.
The Rides to Wellness demonstration grant program has about $7 million available to fund promising projects and community solutions that are practicable. An important evaluation factor in reviewing programs, Robinson said, is how the partnerships among the transit agencies, health care organizations, and other nonprofit organizations are going to meet the transportation needs of stakeholders. Another important element of Rides to Wellness is the community scan project (described by Gomez, below). To be able to move forward and justify the need for these programs, he said, it will be important to collect data on the impact of missed appointments and the inability to get to care despite having insurance coverage.
Robinson shared several lessons learned thus far from the various discussions, regional forums, and initial grants process. A key lesson, he said, is the importance of coordinated planning and partnerships. He added that because both governments and health care organizations vary widely across the country, much of this work must be done at the community level. Challenges and solutions that are developed locally can then be adapted and be applied across the country. Another lesson is the need for people-first approaches, Robinson said. In many cases the solutions exist, but individuals do not necessarily know how to access those solutions; and technology offers promising approaches to help individuals navigate complex systems. One example could be for a person who is scheduling a health care appointment to also schedule his or her transportation at the same time, through some type of technology platform. Technology and research are central to helping develop the solutions for the challenge of transportation to health care, Robinson concluded.
Rides to Wellness Community Scan by Health Outreach Partners
The mission of Health Outreach Partners is to build strong, effective, and sustainable health outreach models by partnering with local community-based organizations in order to improve the quality of life of low-income, vulnerable, and underserved populations (e.g., homeless, low-income seniors, farmworkers, immigrants). Health Outreach Partners supports outreach programs by providing training, consultation, and timely resources, Gomez explained, and it works to demonstrate the value proposition of prioritizing marginalized communities. The Rides to Wellness Community Scan project supports this approach, he said. Health outreach is a patient-centered approach to providing services that support health care but that are not reimbursable under the current system of care. Such services include, for example, health promotion, health education, facilitating access to care, coordinating care, fostering community awareness of
underserved populations, and increasing the cultural competency of care providers. Measuring the impact or value of health outreach is challenging, Gomez said, because outreach programs are not transactional, but rather are based on building trust and relationships with individuals who have not previously accessed health care regularly, or at all.
Health Outreach Partners began to focus on transportation in 2011, with the Transportation Models that Work project, funded by The Kresge Foundation. Gomez said that in national needs assessments for health centers for the prior decade, transportation was always listed as the number one or number two barrier to care. That 3-year project identified and documented six successful case studies addressing transportation as a barrier to care; convened a National Policy Advisory Council, which produced a policy analysis and recommendations; launched a policy campaign to disseminate the findings; and incorporated lessons from the project into Health Outreach Partners’ training and technical assistance activities.2
In 2016, Health Outreach Partners launched its transportation initiative, which consists of the Not Just a Ride project, funded by the Health Resources and Services Administration, and the Rides to Wellness Community Scan, funded by FTA.3 Gomez reiterated the point made by others that for many individuals, gaining health care coverage under the ACA does not necessarily translate to having access to care. Certainly, relationship- and trust-building and overcoming fear of the system are key issues for first-time health system users, Gomez said, but at the core of the access issue is transportation. The Not Just a Ride project is designed to strengthen existing efforts at health centers. The project includes the development of transportation evaluation methodology for community health centers to assess the effectiveness and return on investment of their current transportation services for patients; cross-sector, peer-to-peer learning collaboratives to share case studies, strategies, and successes; and interactive online state transportation services and resource maps. Concurrently, the Rides to Wellness Community Scan will quantify the financial impacts of missed appointments. The first component of the project is a national survey of community health centers, VA medical centers, and private providers to identify the impact of the lack of transportation on health care costs. The second component is the development of profiles illustrating local communities that are adopting transportation solutions that show promising opportunities for return on investment.
___________________
2 The full report for the Transportation Models that Work project, including the case studies, analyses, and recommendations, is available at http://outreach-partners.org/2014/06/04/overcoming-obstacles-to-health-care-transportation-models-that-work (accessed August 4, 2016).
3 For more information, see http://outreach-partners.org/about-hop/transportation-initiative (accessed August 4, 2016).
Gomez closed with an anecdote from one of the case studies that emphasizes the challenges of capturing the value of transportation for health. In Hawaii, just outside of Honolulu, a community health center started a shuttle program that reaches seniors who live up on the mountainside and consequently have difficulty accessing care (Health Outreach Partners, 2014). The shuttle program, in partnership with other small businesses, stops at some of the senior homes to take residents to the health center, but the shuttle also stops at the pharmacy, a nutrition class, the grocery store, a Zumba exercise program, and other locations. Seniors are getting to their health care appointments and also meeting other personal and social needs that enhance health.
ENVIRONMENTAL SCAN OF OTHER TRANSPORTATION EFFORTS
As background for the discussions, the planning committee for this National Academies of Sciences, Engineering, and Medicine workshop, with support from FTA, commissioned a scan of the landscape of health care and transportation partnerships, including the data being collected and shared, and how return on investment or value is being measured. The scan was conducted by Guenin, who presented a brief overview of her findings (the full report is provided in Appendix C). Approximately 70 people were interviewed for the environmental scan, including individuals working in health care, human services, and transportation services; researchers; consultants; representatives from foundations and other funders; and consumers and consumer advocates.
Transportation Policies, Programs, and Services to Improve Access to Health Care and Health-Related Goods and Services
There are a variety of benefits of ensuring that individuals have transportation to health care and health-related services and destinations. Interviewees cited three types of benefits of investing in transportation in particular: reduced or avoided health care costs, social and personal benefits and avoided costs, and changes in health outcomes. Guenin developed a logic model for transportation access to health care in order to capture the relationships among resources, programs and policies, health factors, and outcomes (see Figure 2-1). She said that health factors can be a benefit in and of themselves in addition to leading to improved health outcomes, reduced health care costs, and other societal benefits. The challenge is how to define the return on investment and capture the relevant data for each of the interrelated elements relative to a given program’s goals. Guenin said that biology and genetics are not included as health factors in her model
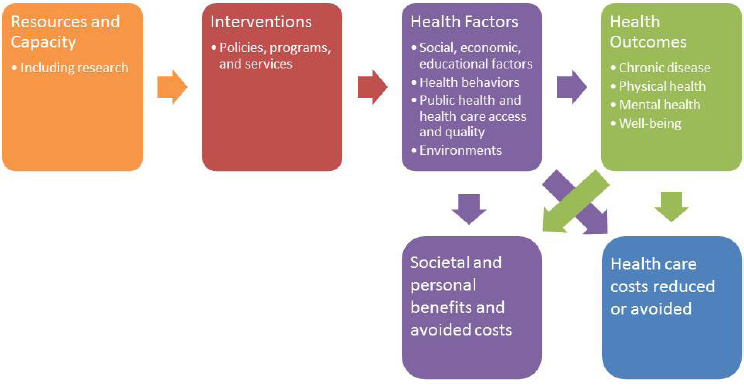
SOURCES: Guenin presentation, June 6, 2016. See Appendix C. Based on models from County Health Rankings (http://www.countyhealthrankings.org/our-approach, accessed October 25, 2016) and NASEM, 2016.
because the model and the scan focus on the influence of programs and policies on outcomes.
Interviewees stressed that access to health care is not just about clinical care, and Guenin showed that, of the health factors listed, clinical care accounts for about 20 percent of the impact that policies and programs have on health outcomes. Social, economic, and educational factors have the largest impact, accounting for about 40 percent, with health behaviors accounting for another 30 percent, and environments for 10 percent (see Figure 2-2). In other words, clinical care is a relatively small part of what people consider to be very important when considering the investment made in transportation.
Based on the literature and the interviews, Guenin identified some of the main health outcomes that seem most affected by transportation access to health care (McClintock et al., 2016; Stiefel et al., 2016). For chronic disease these included asthma, cancer, cardiovascular disease, child oral health, child vision health, diabetes, disability, and obesity. For physical health the main outcomes affected by transportation access to care included exercise capacity, mobility, mortality, pain, sensory ability, and low birth weight. Outcomes related to mental health included depression, anxiety, and suicide. Overall well-being was also an outcome.
Guenin explained that the scan does not directly measure the impact of investments in transportation on health outcomes. Instead, proxy mea-

SOURCES: Guenin presentation, June 6, 2016. See Appendix C. Revised from County Health Rankings model (http://www.countyhealthrankings.org/our-approach, accessed October 25, 2016) and 100 Million Healthier Lives Measurement System: Progress to Date (http://www.100mlives.org/measure/framework, accessed October 25, 2016).
sures are used, such as primary care utilization, emergency department utilization, missed appointments, transportation trips provided, and other data reflecting the provision of transportation and care. She said that interviewees were very interested in connecting the health and transportation datasets in order to better understand the impact of transportation on access to care and health outcomes.
With regard to transportation, Guenin said that there is a continuum of providers, modes of transportation, and entities that plan, design, and maintain the different transportation systems. Examples of these include public providers (e.g., fixed-route transit, fixed flexible route, demand responsive/Americans with Disabilities Act paratransit), commercial providers (e.g., wheelchair accessible, ambulatory with assistance, taxi-style service, stretcher service, ridesharing service), county-sponsored services (e.g., county-owned vehicles and drivers paid to transport Medicaid clients), first/last-mile connections (e.g., office/industrial park, neighborhood, military base, and university circulators), tribal transit, human services providers, veterans’ affairs services, volunteer transportation, and personal transportation (with mileage reimbursement). Many of the transportation programs
included in the scan are providers of NEMT for Medicaid clients accessing Medicaid-covered services. Other populations with which transportation providers worked included veterans, people experiencing multiple chronic conditions, pregnant women, children, individuals accessing drug treatment programs, older adults, people with disabilities, and rural residents.
Themes from the Interviews4
Barriers
Interviewees were asked about the barriers and challenges they faced in creating health and transportation partnerships and in measuring the return on investment of transportation efforts. Guenin reported that responses fell into seven core theme areas:
- Defining return on investment. Three main concerns were emphasized by interviewees: the value or return on investment outside of health care costs (returns may be nonfinancial, and actual costs may increase as more people access care or as currently unmet needs are met); the time-scale over which a return is being measured (e.g., some returns may be long term); and for whom a return is being measured (e.g., for insurers, patients, caregivers, the community).
- Funding. Interviewees discussed the need to “go slow” and “start small” in the face of limited resources.
- Missing information and data. Subthemes in this area included the need to ask the right questions (e.g., Why are patients missing appointments? How can one identify which patients are at risk for not having transportation options?); the impact of the ACA on access to insurance (which may result in increased costs in the short term); same-sector information gaps (i.e., not just between the transportation and health care sectors, but within each sector across providers, payers, services, etc.); and the impact of the Health Insurance Portability and Accountability Act (HIPAA)5 on data sharing (leading to workarounds, e.g., embedding transportation staff in the health system, using non-health proxy data).
- Technology. Recurring subthemes related to technology were the need for standardized data and open-source technology to support
___________________
4 See Appendix C for more details.
5 “The Health Insurance Portability and Accountability Act of 1996 (HIPAA) is a federal law that sets national standards for how health care plans, health care clearinghouses, and most health care providers protect the privacy of a patient’s health information” (Source: CMS, at https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-MLN/MLNProducts/downloads/SE0726FactSheet.pdf [accessed September 1, 2016]).
-
partnerships, client-side barriers to accessing available technology (e.g., a lack of awareness or understanding, technological limitations), and the difficulty of tracking trips on public transit.
- Geography. Interviewees highlighted the transportation, health care, and measurement challenges that are specific to rural areas (e.g., an effective or efficient transportation system in a rural area may be different from that in an urban area, and different metrics are needed). Respondents also noted the barriers faced when crossing jurisdictional and service boundaries.
- NEMT destination and service gaps. Interviewees emphasized issues specific to Medicaid, Medicare, and VA transportation, noting that some necessary destinations are not included (e.g., pharmacy, grocery store, support group) and that patients are unable to have caregivers or children ride along.
- Cross-sector collaboration. The subthemes raised included issues concerning cross-sector knowledge (e.g., a lack of understanding of other sectors’ language, operations, funding, programs, key contacts, etc.); different motivations and measures of success for different programs; coordination; and acknowledging that the implementation of solutions takes time (e.g., a too-rapid scale-up or trying to solve too many problems at once can lead to sustainability issues).
Opportunities
Interviewees also identified opportunities and potential solutions. Topics raised by individuals were organized by Guenin into eight main theme areas:
- Grants. Interviewees emphasized the importance of grants in catalyzing partnerships.
- Spaces for shared learning. Those interviewed highlighted the need for more opportunities and better ways to share knowledge and obtain guidance.
- Start small and go slow. One of the most common themes, Guenin said, was that partnerships take time and resources to build. As mentioned above, interviewees emphasized the reasons for and benefits of starting small and going slowly, working within the available resources, and not attempting to solve too many issues at once.
- Let patients tell the story. Interviewees noted the importance of listening to the end-users of services to understand their needs and
-
to determine if those needs are being met. The patient perspective also helps to make the case for funding and partnerships.
- Bring the care to the patients. One transportation solution raised by several interviewees was the option of bringing the care to the patients (e.g., mobile care units, mobile pharmacy).
- Customer service. Interviewees noted the value of providing good customer service and establishing relationships between service providers (i.e., drivers) and clients (i.e., patients).
- Sharing resources and increasing revenue. Although some interviewees mentioned the challenges of cost sharing, Guenin said that some partnerships were able to find win–win solutions so that both the transportation and health care sides benefited.
- Sharing data and analyzing solutions. Interviewees described various new tools and strategies for facilitating data sharing while maintaining compliance with HIPAA (e.g., cost allocation, proxies for health data, adding questions about transportation to community health needs assessments).
DISCUSSION
Following the presentations, the panelists, discussants, and participants considered a variety of issues related to efforts to facilitate transportation to health-related destinations. Topics discussed included the lessons learned from recent mobility demonstration projects; transportation as a component of prevention; and the challenges of geography (e.g., the location of care, rural transit barriers), data availability, and funding gaps.
Bridging Health Care and Transportation Issues
Over the past 6 or 7 years, at congressional request, GAO has conducted a series of studies looking at transportation-disadvantaged populations from the transportation perspective and has issued recommendations to FTA, MacLeod said. One study, for example, looked at the role of FTA in coordination, and another reviewed NEMT. Over the course of this work, GAO initially identified 80 federal programs that provide transportation services to transportation-disadvantaged populations and 42 federal programs that provide NEMT. MacLeod highlighted the challenge of obtaining data on programs, noting that, outside of FTA and a small number of other federal programs, federal agencies were unable to identify which of their programs provided these services or to provide any funding information. GAO was subsequently asked to review the transportation issues from a health care perspective and to make recommendations to HHS. This pro-
gression—and the workshop discussions thus far—illustrate the evolution of bringing the health care and transportation issues together, she said.
Lessons Learned from Demonstration Projects
The National Center for Mobility Management is a national technical assistance center that disseminates information on mobility management and coordination and assists local communities in adopting proven transportation strategies to build community capacity, Shanley said. The center is supported though a cooperative agreement with FTA, and it operates in partnership with Easterseals, the Community Transportation Association of America, and APTA. The center has been involved in administering the FTA Rides to Wellness demonstration projects and providing technical assistance support to the grantees.
Shanley shared some of the lessons learned from the community demonstration projects, especially with regard to sustainability and replicability. Affirming the points made by Guenin, Shanley said that having the voices of riders at the planning table is critical. She mentioned a project funded by the HHS Administration for Community Living that is studying how to better engage people with disabilities and older adults in coordinated planning activities. Important elements of the demonstration projects included an educational component that helps patients navigate the transportation and transit services in the community; systemic data collection and evaluation processes built in during project design and development; multiple levels of data collection (e.g., individual/rider, organization/agency, and systems/community levels); technical assistance to support communities and partnerships; and peer-to-peer learning opportunities for grantees to share challenges and success. Shanley also noted the need for grantees to learn to use data to communicate and market their transportation solutions to the regional transition authorities and other stakeholders (e.g., potential funders and partners).
Shanley said that the lack of transportation to care has a ripple effect that is important to keep in mind. For example, transportation to care has implications for caregivers, Shanley said, and she added that the patient may also be a caregiver for a spouse or other family member. If that patient cannot regularly get to his or her chronic care appointments and ends up hospitalized, the family member for whom he or she cares might need to be placed in an institution.
Prevention
Guzzetti raised the prevention aspect of transportation to health care and asked about any efforts to quantify the contribution of prevention to
health outcomes. Guenin responded that current efforts measuring value and return on investment mostly consider primary care and the use of primary care versus emergency department visits and hospitalizations. At the county level, public health and medical health are having more collaborative conversations about their shared role in improving health, she said, and are starting to consider better ways to measure the impact of access and environments on such aspects as prevention. MacLeod added that prevention was considered briefly in a recent GAO study of NEMT service under the Medicaid expansion provision of the ACA. She reported that some states were applying to Medicaid for waivers so that they would not have to provide NEMT service for newly eligible populations. GAO was able to gather data on the states applying for or planning to apply for waivers and also on the reasons. In terms of the potential impacts, however, there was little information, and MacLeod expressed frustration at not being able to provide that information to congressional decision makers.
Challenges
The Geography of Health Care
Guzzetti said that health care has become consolidated and centralized over the past couple of decades. Neighborhood clinics, for example, are much less common, and people must travel farther to access care. Guenin said that in many cases primary care is still locally available, even in rural areas, but specialty services are often regional. She reiterated the added barrier of crossing jurisdictional boundaries for care. A patient seeking care at a regional facility may need to travel to the service border of one transit agency and then exit that transportation and wait for different transportation.
Martin Ornelas of the Rural Economic Assistance League, Inc., stressed the importance of developing rural models based on rural realities and not simply applying urban models to rural areas and assuming they will work. In addition to health professional and health facility shortage areas, rural areas have transportation shortage areas. Llort said that many medical centers are providing distance services through the Internet or other mechanisms. She acknowledged that many people have challenges engaging with technology, particularly the elderly, but she noted the need for more discussion on providing medical services in rural areas to individuals in their homes or other local bases.
Kate Lawson of the State University of New York at Albany raised the issue of coordination with partners in land use, and she asked whether anyone has been encouraging the health industry to consider developing facilities in empty shopping center spaces since they are most likely already
on the transit system. Guenin replied that this was not raised by any of the interviewees.
Data and Metrics
Guzzetti called on the panelists to discuss what data and metrics are needed to advance the conversation and make progress on transportation and health care. MacLeod raised the topic of states using Medicaid transportation brokers to handle NEMT. About 5 years ago, she said, GAO asked states about coordination among their transportation programs and heard a lot of negativity around the Medicaid brokerages that were in place in some states. More recent surveys, however, show that some states are feeling more positive about the Medicaid brokerages and are even finding ways to coordinate and collect data through those brokerages. Unfortunately, she continued, GAO has been unable to determine how many states have brokerage systems or whether they are statewide brokerage systems or another model. Medicaid programs are state by state and can be complex, and even CMS does not have data on how many states have brokerages. Some of the brokerages are for-profit companies and could provide context concerning their riders and finances, she suggested.
Funding Gaps
Gomez said that funding for outreach and enabling services can be episodic or disease specific, making it very difficult to evaluate the program or demonstrate impact and value. Guenin agreed and added that interviewees reported that they would get funding and implement a program, and then the program would disappear when the funding ended. Patients who had become reliant on that program were left potentially in a worse situation. She mentioned that Oregon has a special transportation fund that is flexible, and this has helped to fill the gap when other funding for transit providers has ended.
This page intentionally left blank.
















