4
Improving Public Awareness and Training
Although the timely use of cardiopulmonary resuscitation (CPR) and automated external defibrillators (AEDs) following a cardiac arrest can improve chances of survival and outcomes, rates of bystander CPR and AED use in the United States are low (less than 3 percent annually) (Anderson et al., 2014; IOM, 2015). A coordinated public education campaign that is implemented at the state and local levels will be necessary to expand public CPR and AED training and improve the provision of bystander CPR and defibrillation (IOM, 2015) (see Box 4-1). As Tom Aufderheide noted during his opening remarks, and Marina Del Rios reiterated, cardiac arrest is not always the last event in a person’s life, and if the public is prepared and ready to act, individuals can make a difference and save lives.
CRYSTALLIZING MESSAGING TO PROMOTE PUBLIC AWARENESS
Robert M. Davis, U.S. Department of Homeland Security
In 2003, USA Today released an investigative series called Six Minutes to Live that was based on 18 months of research conducted by Robert Davis. During his investigation, Davis identified significant geographic disparities in survival rates associated with cardiac arrest and explored the root causes for these variations. The cities with the best survival rates held themselves accountable for outcomes and measured true response
times—the continuous time from collapse until the first responder arrived next to the patient and initiated treatment. These cities also measured true survival rates rather than just return of spontaneous circulation. Application of these types of benchmarks, said Davis, allows communities to reflect on the care being provided and determine where improvements should be made.
Beyond reporting on the geographic disparities, the USA Today series also included elements of public education. For example, it featured graphics that showed readers exactly how to do CPR and use an AED, encouraging them to act regardless of their level of prior CPR training. Davis emphasized the importance of messaging when educating the public and outlined six key messages about cardiac arrest and resuscitation that should be conveyed (see Box 4-2). Although the media can, and
do, play an essential role in educating the public, the media landscape is shifting. For example, social media are taking precedence, especially with younger audiences, over more traditional mechanisms, such as press conferences and desk-side briefings with medical reporters. The media are strained and stories are being segmented, which can lead to messages being diluted or lost, said Davis. Although mass media can still be used to reach millions of people, they require a lot of time and money. Davis indicated that a comprehensive outreach campaign that includes multimedia, social media, and viral messaging will be needed to effectively increase public awareness and promote bystander action in the face of cardiac arrest.
Unlike other public health campaigns (e.g., seat belts, drunk driving, smoking cessation, cancer screening), scare tactics cannot be used to induce behavior change when it comes to bystander response to cardiac arrest. In other words, said Davis, the message of other campaigns is often “if you do not take action—stop smoking, wear a seat belt, get a mammogram, etc.—you could die.” However, in the case of cardiac arrest, the potential victim is not the audience. The bystanders are the ones who need to be convinced to take action and overcome their fears in order to save someone else’s life. To overcome those fears, outreach efforts could focus on the public’s ability to participate and on how individuals can use their knowledge and skills to save a loved one or stranger who collapses, continued Davis.
Across the resuscitation field, the shared goal is to save lives, said Davis, and partnerships will be vital to success. To realize the goal of reduced mortality, the field could develop, synchronize, and consistently
use simple messages, regardless of whether they are applied to educating the public or discussing research funding and results. Davis urged all stakeholders to work together to develop consistent messaging. He said that one of the most powerful stories involves connecting a survivor with his or her rescuer. Whenever possible, these heroic stories need to be discussed publicly and used to promote awareness. Davis noted that the media could also be useful in encouraging accountability across communities and health care systems by reporting on performance and outcomes.
Furthermore, the role of the public should not be underestimated. Increasing public awareness can empower communities to demand accountability and higher standards of care from health care systems and providers. Increased awareness could also result in a larger role for the public in implementing the Institute of Medicine’s (IOM’s) recommendations. Although not everyone will survive a cardiac arrest, the field has an obligation to engage the public and create an environment of action, concluded Davis.
Complementing Davis’s conclusions, Edward Septimus, who spoke later in the workshop (see Chapter 6), noted that the Centers for Disease Control and Prevention has a website called Get Smart that has information and materials geared toward both health care providers and patients. One of the challenges in the context of antimicrobials, said Septimus, has been for health care providers to take the time to educate patients and persuade them that the antibiotic is unnecessary and that monitoring and waiting are appropriate options for certain conditions. Another challenge lies with the financing of these public education campaigns, he said. There are better ways to engage payers and other partners from across the continuum of care in funding joint efforts. There are significant, long-term societal costs associated with inaction, he emphasized. Working together can lead to better outcomes and lower health care costs.
INVESTING IN PATIENT ADVOCACY AND COMMUNITY EDUCATORS TO CHANGE POLICY
Joanne Howes, National Breast Cancer Coalition
A quarter of a century ago, a revitalized women’s health movement was under way in the United States and efforts were being made to involve more women in clinical trials and research studies, said Joanne Howes. This movement served, in part, as the impetus for the development of the National Breast Cancer Coalition, which was launched in 1991 with an overarching mission to end breast cancer. At the time, there were hundreds of survivor and advocacy groups across the country that offered
support, education, and care for women with breast cancer. A number of these organizations came together with a desire to change the system and build an effective advocacy coalition. Howes said the coalition was founded on three basic principles: (1) expanding research; (2) improving access to high-quality, evidence-based care; and (3) uniting and fortifying advocacy efforts.
Howes described a number of factors that she believes have contributed to the success of the National Breast Cancer Coalition over the years. For example, the coalition is somewhat unique in that it includes representatives from member organizations that each have a voice and a role to play within the coalition. Furthermore, the coalition’s leaders are all trained, volunteer advocates from across the United States who strive to support the coalition and advance its mission. Beyond training for its leadership, the coalition has recognized and understood the value of advocacy training from the beginning. It devised an annual multiday program called Project Lead, which provides survivors and advocates a basic understanding of the relevant science, research methods, statistics, and advocacy strategies before visiting Capitol Hill to meet with congressional leaders and staff. Howes also noted that over the course of its history the coalition has remained dedicated to its mission and only chooses to participate in activities that will ultimately fulfill the mission to end breast cancer.
Since its inception, the coalition has significantly expanded funding for breast cancer research and the role of advocates in research. The coalition’s most well-known effort is its partnership with the Department of Defense (DoD) to create the DoD Breast Cancer Research Program, said Howes. As part of this program, advocates from the National Breast Cancer Coalition serve on peer review panels and planning panels, actively interacting with researchers to provide survivor and advocacy perspectives. These advocates question the value and purpose of the research topics being presented and provide guidance to ensure that funding is being directed to studies that will work toward ending breast cancer. Although progress in research has been made, greater investment could help to ensure access to high-quality, evidence-based care, noted Howes. Reiterating a point from previous speakers, Howes said that the field often knows what the current research says to do. However, not all providers keep up with the guidelines and provide care supported by the best available evidence.
In response to an audience question about how to effectively engage the media and large national organizations (e.g., National Football League [NFL], National Basketball Association [NBA], and National Collegiate Athletics Association [NCAA]) to increase awareness about cardiac arrest and the importance of bystander CPR and AED use, Howes noted that
much of the demonstrated goodwill is political. Companies—and corporate America, more broadly—want to create and maintain a good public image. Therefore, they publicly support the fight against breast cancer by branding products with pink and participating in breast cancer awareness activities in October. To start this process for cardiac arrest, the resuscitation field could identify a spokesperson or an organization that can take the lead and represent the field as a whole. Specifically, Howes asked, who will be responsible for approaching the NBA and other organizations about this effort?
Del Rios noted that one of the challenges within the resuscitation field is that many of the organizations work in silos. In response, Howes urged the field and all of its disparate organizations to agree on messaging and strategies to move forward together and begin the necessary outreach work. Howes reiterated that the National Breast Cancer Coalition model could be quite useful to the resuscitation field, noting that a large organization with a big budget is not necessarily required to make sizable changes.
Howes also recommended that public messages be simple, straightforward, and empowering. For example, the message could be “there are actions that individuals can take to save a life, and everyone has a responsibility to know how to do that,” said Howes. Furthermore, a member of the audience highlighted the importance of engaging experts in behavior change, marketing, and advertising when developing messaging for the public to ensure that the messages will be effective. In closing, Howes noted that, while the resuscitation field has many complex challenges to overcome, it should convey a clear message of action to mobilize the public.
PUBLIC AWARENESS AND TRAINING: INNOVATIVE TECHNOLOGIES AS A TOOL TO IMPROVE ACTION
Raina Merchant, University of Pennsylvania
Innovative technologies offer significant promise for improving public awareness and can play a role in communication, marketing, messaging, and connectedness, all themes discussed by previous speakers, noted Raina Merchant. In the resuscitation field, innovative technologies are being developed to improve access to CPR-trained bystanders and AEDs. For example, a recent study evaluated an automated, mobile phone system in Sweden that notifies CPR-trained individuals of possible nearby cardiac arrests that are reported to a local emergency medical services system. These trained bystanders can then use mobile positioning technology to go to a scene and initiate bystander CPR. Although the researchers did
not identify an increase in survival rates, the rates of bystander CPR did increase (Ringh et al., 2015). In the United States, a similar mobile app-based initiative has been developed and is being implemented. The initiative, called PulsePoint, calls on volunteer citizens to respond to possible cardiac arrests and provides information on the location of the nearest AED, when available (Brooks et al., 2016) (see Figure 4-1). In a later presentation, Myron Weisfeldt echoed this point, highlighting PulsePoint as a resuscitation program that could lead to the next major national public policy shift. Merchant indicated that there has been sizable interest in the app, given the ubiquity of mobile phones and the potential to reduce the time from collapse to CPR and defibrillation.
Innovative technologies are also being used to expand access to AEDs. In Philadelphia, researchers developed a mobile app called MyHeartMap and are using crowdsourcing and gamification to engage the public and locate publicly available AEDs in the city. By the end of the contest, the public had reported more than 1,400 AEDs (852 unique entries) (Merchant et al., 2013). The data were made publicly available following the conclusion of the study, and more than 10,000 AEDs have been reported across the state of Pennsylvania since then (Merchant, 2016). Although this app is not connecting bystanders to AEDs when one is needed, said Merchant, just knowing where the AEDs are located is an important first step.
Merchant pointed out that knowing the locations of AEDs is not enough to save a life; the AED must also be noticeable and easily identifiable by a bystander. The Defibrillator Design Challenge used crowdsourcing and asked the public to submit designs that would make AEDs, and their location, stand out and be more memorable. Approximately 119 people submitted designs, such as one that showed Clark Kent open-
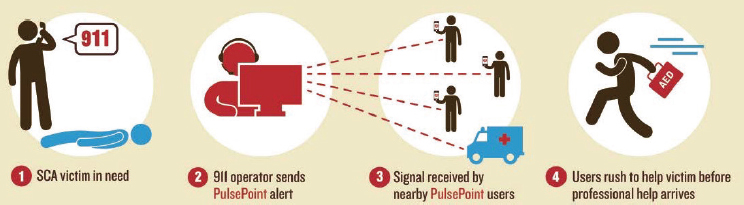
NOTE: AED = automated external defibrillator; SCA = sudden cardiac arrest.
SOURCE: Presented by Raina Merchant, July 11, 2016, A Dissemination Workshop on the Report Strategies to Improve Cardiac Arrest Survival: A Time to Act (citing PulsePoint, 2016).
ing his shirt to reveal an AED along with his Superman cape, and 2,140 people voted on these entries and provided demographic information (Merchant et al., 2014). Merchant pointed out that the designs offered yet another opportunity for messaging and increased public awareness. Another innovative technology that is being tested to expand access to AEDs is the use of drones for just-in-time AED delivery. Merchant noted that, although this is in the early phases, this approach could reduce the time to defibrillation by eliminating the need to search for and locate an AED.
One workshop participant noted that the NCAA recently released a consensus statement on cardiovascular care for athletes, including cardiac arrest care (Hainline et al., 2016). The participant said a large part of the statement deals with the availability of AEDs and ensuring that colleges and universities are complying with national AED recommendations. Merchant followed up on the participant’s comment, saying that just knowing where AEDs are located is not enough. AEDs must be accessible, visible, and functional, and perhaps most importantly, she said, people need to be willing to open the box and use them.
Social media is yet another mechanism that could be used to increase public awareness. Merchant described how researchers have used Twitter to assess public knowledge related to cardiac arrest and to understand how information is shared via tweets (Bosley et al., 2013). In their analysis of tweets, Bosley and colleagues (2013) found that many questions were being posted about cardiac arrest and CPR. The resuscitation field needs to determine how to use messaging effectively to answer the public’s questions and to better educate individuals about cardiac arrest symptoms and treatment, said Merchant. In considering how the resuscitation field and researchers can harness the billions of bits of data available through social media and crowdsourcing along with the public enthusiasm, Merchant pointed out that the American Heart Association recently released a scientific statement titled Use of Mobile Devices, Social Media, and Crowdsourcing as Digital Strategies to Improve Emergency Cardiovascular Care (Rumsfeld et al., 2016). The statement outlines potential research questions to guide further investigations related to the use of these tools to improve the timely response and treatment of cardiovascular emergencies, including cardiac arrest. Merchant noted that this statement could be used as a starting point for progress in adopting innovative technologies to improve public awareness and response to cardiac arrest.
In response to a question about the state of the science for using cell phones to instruct people in hands-only CPR techniques, Merchant said there are several good apps available that provide instruction and sometimes a metronome to assist with compression rates. For people who have taken CPR training, the apps serve as a great refresher. Merchant said a
number of studies have also demonstrated that these apps can provide increased confidence in doing CPR—a serious barrier for many individuals. Despite the widespread availability of these apps, the uptake rates are not as high as they could be, representing an opportunity for the resuscitation field. However, determining how to encourage the public to download and regularly use the training apps is a challenge, said Merchant.
BREAKOUT SESSION REPORT: ESTABLISHING A PUBLIC AWARENESS CAMPAIGN
Paul Pepe, Planning Committee Member1
Paul Pepe moderated the breakout session on strategies to establish a public awareness campaign and advance the second recommendation from the IOM’s report (see Appendix A). In his opening remarks, Pepe noted that increasing public awareness is an intermediate step for achieving the overarching goal of creating a culture of action in which bystanders are prepared and motivated to immediately respond to a cardiac arrest and save a life.
As described in the IOM’s report, a number of barriers impede action from the public. For example, individual participants in the group identified barriers such as the public not recognizing cardiac arrest as a major public health concern, fear of injuring someone when doing CPR or using an AED, and a lack of confidence in skills and training. To overcome these barriers, individual breakout group participants brainstormed a number of possible strategies to consider when developing messaging:
- Use a singular, simple, concise, easy-to-communicate, and compelling message. Participants identified some examples to follow, including “Only you can prevent wildfires” and “Stop, drop, and roll.”
- Emphasize that individuals can save a life today, that training is simple and easy, and that CPR and AEDs are safe and effective tools that anyone can use.
- Help the public differentiate between cardiac arrest and a heart attack, and underscore that all loved ones are at risk.
___________________
1 Breakout session presenters were asked to summarize the major ideas and opinions proposed by individual participants during their respective breakout sessions. Individual statements described below are not necessarily the position of the presenter and should not be interpreted as consensus statements from the breakout group as a whole or of the National Academies of Sciences, Engineering, and Medicine.
- Remind people that the majority of cardiac arrests occur in homes and offices. Therefore, everyone needs to be ready to act.
Pepe urged the field to engage professional communication experts and focus groups, come to a consensus, and use the agreed-upon messaging consistently. Conveying the persuasive messages and motivating action will likely require a multifaceted outreach strategy, said Pepe. He noted that, although a mass media campaign could reach a large audience, resource limitations may be a challenge and sustainability is not guaranteed. Social media offer a lot of potential. However, Pepe said that marketing experts should carefully plan outreach through these channels, and more broadly, ensure the use of fully tested and validated messages that reach all audiences, including vulnerable populations.
Effective outreach will also necessitate collaboration across a range of stakeholder groups in a variety of settings, said Pepe. For example, some individuals in the breakout groups noted that health care providers and health care settings could play a role in public education efforts. For example, pediatricians could ask parents about CPR training, and posters in waiting rooms could be used to show how to identify cardiac arrest and what to do. Furthermore, schools, employers, businesses, community groups (e.g., faith-based organizations, youth groups), and advocacy organizations (e.g., AARP) should be engaged as valuable local partners, said Pepe. The resuscitation field should also consider developing a network or uniting and fortifying existing groups that include survivors, individuals who have lost a loved one to cardiac arrest, and patient advocates who can be called on to share their powerful stories, some breakout group members suggested. Whenever possible, these individuals should receive advocacy training and be actively involved in outreach initiatives, although outreach endeavors may be resource intensive, Pepe said.
BREAKOUT SESSION REPORT: FOSTERING A CULTURE OF ACTION IN COMMUNITIES THROUGH POLICY
Marina Del Rios, Planning Committee Member2
Marina Del Rios moderated the breakout session that focused on fostering a culture of action in communities through policy. Similar to the breakout session led by Pepe, the discussion from this session was also
___________________
2 Breakout session presenters were asked to summarize the major ideas and opinions proposed by individual participants during their respective breakout sessions. Individual statements described below are not necessarily the position of the presenter and should
linked to the second recommendation from the IOM’s report. In its discussion, this group considered potential partners, barriers to creating cultural changes, and policy changes at the national, state, and local levels. The individual breakout group participants identified a plethora of possible public and private organizations that could be involved in community-based action initiatives (see Box 4-3). Del Rios noted that the resuscitation field could look to successful state lobbying coalitions for lessons related to developing partnerships and implementing policy change. The group also discussed partnering with existing state and national networks that are dedicated to other time-sensitive health conditions, said Del Rios. For example, stroke, trauma, and acute myocardial infarction offer potential partnerships. Whenever possible, the cultural changes need to be driven from a grassroots level, said Del Rios. Additionally, some breakout group members suggested that community-centered initiatives to improve
___________________
not be interpreted as consensus statements from the breakout group as a whole or of the National Academies of Sciences, Engineering, and Medicine.
response to cardiac arrest should include factors related to motivation, ability, influence of others, and influence of physical surroundings.
This breakout group discussed numerous barriers to establishing a culture of action in communities across the United States. The primary barriers that Del Rios highlighted included the following:
- As discussed in previous breakout and plenary sessions, the lack of unified messaging creates a mixed media narrative and potential confusion among the public, especially in the context of how to recognize and respond to cardiac arrest versus heart attack.
- There is a lack of local, state, and national mandates for accessible, visible AEDs located near the entrance of public buildings.
- Good Samaritan laws are inadequate and the public has misperceptions about what those laws entail. Del Rios said there needs to be a national template that can be used to promote legislative consistency across states.
- There is a lack of an organized, independent, and active national survivors and family network (including family and friends of non-survivors) with strong leadership that can serve as a voice for cardiac arrest on the national level. Del Rios noted that current survivor organizations are disjointed and primarily operate at local and state levels.
- The public has misperceptions about the complexity and length of CPR and AED training.
- Psychological barriers prevent certain individuals, some of whom have had CPR training, from helping when confronted with a cardiac arrest. Del Rios said that inaction following a cardiac arrest needs to become socially unacceptable.
When asked about possible barriers to requiring CPR and AED training as a high school graduation requirement, Del Rios said that school systems and teacher associations have voiced concerns about unfunded mandates and having to restructure curricula that are already strained by time limitations. The potential costs of developing and maintaining a CPR and AED training program are particularly problematic for low-income schools. However, one workshop participant pointed out that there are organizations that can provide free mannequins and support for these programs. Therefore, building sustainable, low-cost programs is a possibility, said the participant, if this is defined as a policy priority at state and local levels. Del Rios also noted that the Department of Education could be asked to develop guidance on school-based CPR programs and possibly provide funding to support these programs.
In considering opportunities to expand access to bystander CPR and
AED use, the group highlighted policy changes at the national, state, and local levels that could have an impact. At the national level, some participants in the group suggested that the Food and Drug Administration consider updating its AED regulations to require that all new AEDs include a standardized geolocation technology, making AEDs easier to locate and increasing public access. At the state and local levels, Del Rios said that dispatcher-assisted CPR should be required. This type of policy change could significantly increase the availability of bystander CPR. Furthermore, leveraging existing state and local policies, such as fire alarm testing and building inspections, could be useful in ensuring that AEDs are available, prominently displayed, and functional. Del Rios also noted that hospitals and health care systems could include CPR training as part of their community health needs assessments to identify areas for improvement and develop strategies to fill training gaps.
BREAKOUT SESSION REPORT: INNOVATIVE TECHNOLOGIES AS A PUBLIC HEALTH TOOL
Raina Merchant, Planning Committee Member3
Raina Merchant facilitated the breakout session on how innovative technologies can be used as public health tools. Merchant first noted that technology is not a replacement for current tools, but rather a mechanism to better integrate and optimize existing systems. During the breakout session, the group discussed the possible benefits and detriments of several technologies that could be broadly implemented for three primary purposes: data collection and research, training and prompting (e.g., guided CPR), and connecting individuals with necessary resources. Some members of the group identified privacy as a unifying challenge relevant to each of the technologies discussed during the session.
First, the group considered the potential of mobile technologies, such as cell phones, to help overcome public inaction. As discussed previously, there are many benefits associated with mobile technology—for example high per-capita cell phone ownership, geolocation and navigation features for locating AEDs and potential rescuers, and availability of just-in-time instruction. However, there are also challenges associated with fully integrating cell phones into 911 processes. Merchant pointed out that many
___________________
3 Breakout session presenters were asked to summarize the major ideas and opinions proposed by individual participants during their respective breakout sessions. Individual statements described below are not necessarily the position of the presenter and should not be interpreted as consensus statements from the breakout group as a whole or of the National Academies of Sciences, Engineering, and Medicine.
911 localities are unable to accept or send text messages, limiting communication opportunities. Some members of the breakout group identified 911 improvements as low-hanging fruit, indicating that the capability to send and receive text messages, images, and videos combined with the use of built-in geolocation technologies could greatly expand information transfer possibilities and promote further public response to cardiac arrests. As with other applications of mobile technologies, privacy concerns would be applicable. There are also questions regarding the limitations of the technologies and the quality of the data provided, such as the accuracy of geolocation in high-rise buildings.
Merchant described sensors and wearable technologies as opportunities to harness the data that these devices collect to identify cardiac arrests in real time and alert rescuers. Although early detection is a significant benefit, the value of these devices is currently limited given the modest adoption rates among the public, she stated. Additional studies would be required to assess the quality and accuracy of the data from these devices and manage potential privacy concerns. In thinking about the development of new technologies and apps, the group discussed the use of hack-a-thons, gamification, and innovation challenges. These types of initiatives often include varying levels of prize money and may call for the participation of interdisciplinary teams in order to inspire the generation of new ideas, unconventional designs, and creative solutions to existing problems. For example, Merchant said the resuscitation field could convene a hack-a-thon to optimize app-based CPR instruction. The challenges with these approaches include additional testing requirements, assurance that the ideas produced are indeed novel and better than existing options, and determining which products will be implemented broadly, some individuals noted.
The breakout group also considered the intersection between technology and public engagement and training. Many technologies are available that could be leveraged to increase public awareness, involvement, and training, said Merchant. Social media, videos, games, apps, and simulation were discussed as possibilities, especially as mechanisms to reach younger audiences. One workshop participant asked Merchant about the potential for using social media and other technologies to study cardiac arrest risk factors. Merchant noted that the data available through social media and mobile technologies, including sensors and wearable technologies, offer incredible research potential to explore complex questions, such as risk for cardiac arrest. The possibility of two-way communication with social media also opens up new educational opportunities to share accurate messages about cardiac arrest, CPR, and AEDs, thus enhancing public communication and connectedness. Although the promise of new technologies can be appealing, developing, testing, and implementing
these technologies can require large investments and time-consuming research, Merchant commented. On the other hand, optimizing existing low-tech tools could offer equal or greater returns. For example, removing signs on AEDs indicating that only trained professionals should use them or educating the public about hands-only CPR guidelines could remove barriers to public action and response to cardiac arrest.
REFERENCES
Anderson, M. L., M. Cox, S. M. Al-Khatib, G. Nichol, K. L. Thomas, P. S. Chan, P. Saha-Chaudhuri, E. L. Fosbol, B. Eigel, B. Clendenen, and E. D. Peterson. 2014. Cardiopulmonary resuscitation training rates in the United States. JAMA Internal Medicine 174(2):194–201.
Bosley, J. C., N. W. Zhao, S. Hill, F. S. Shofer, D. A. Asch, L. B. Becker, and R. M. Merchant. 2013. Decoding Twitter: Surveillance and trends for cardiac arrest and resuscitation communication. Resuscitation 84(2):206–212.
Brooks, S. C., G. Simmons, J. Worthington, B. J. Bobrow, and L. J. Morrison. 2016. The PulsePoint Respond mobile device application to crowdsource basic life support for patients with out-of-hospital cardiac arrest: Challenges for optimal implementation. Resuscitation 98:20–26.
Davis, R. 2016. Synchronizing messages: Promoting public awareness to save more lives. Presentation at the Dissemination Workshop on the Report Strategies to Improve Cardiac Arrest Survival: A Time to Act, Washington, DC. http://www.nationalacademies.org/hmd/~/media/Files/Activity%20Files/PublicHealth/TreatmentofCardiacArrest/JULY%202016%20Workshop/Davis.pdf (accessed October 30, 2106).
Hainline, B., J. A. Drezner, A. Baggish, K. G. Harmon, M. S. Emery, R. J. Myerburg, E. Sanchez, S. Molossi, J. T. Parsons, and P. D. Thompson. 2016. Interassociation consensus statement on cardiovascular care of college student-athletes. Journal of the American College of Cardiology 67(2):2981–2995.
IOM (Institute of Medicine). 2015. Strategies to improve cardiac arrest survival: A time to act. Washington, DC: The National Academies Press.
Leung, A. C., D. A. Asch, K. N. Lozada, O. B. Saynisch, J. M. Asch, N. Becker, H. M. Griffis, F. Shofer, J. C. Hershey, S. Hill, C. C. Branas, G. Nichol, L. B. Becker, and R. M. Merchant. 2013. Where are lifesaving automated external defibrillators located and how hard is it to find them in a large urban city? Resuscitation 84(7):910–914.
Merchant, M. 2016. Public awareness and training: Innovative technologies as a tool to improve public awareness and action. Presentation at the Dissemination Workshop on the Report Strategies to Improve Cardiac Arrest Survival: A Time to Act, Washington, DC. http://www.nationalacademies.org/hmd/~/media/Files/Activity%20Files/PublicHealth/TreatmentofCardiacArrest/JULY%202016%20Workshop/Merchant.pdf (accessed October 30, 2016).
Merchant, R. M., D. A. Asch, J. C. Hershey, H. M. Griffis, S. Hill, O. Saynisch, A. C. Leung, J. M. Asch, K. Lozada, L. D. Nadkarni, A. Kilaru, C. C. Branas, E. M. Stone, L. Starr, F. Shofer, G. Nichol, and L. B. Becker. 2013. Innovations in Care: A crowdsourcing innovation challenge to locate and map automated external defibrillators. Circulation: Cardiovascular Quality and Outcomes 6:229–236.
Merchant, R. M., H. M. Griffis, Y. P. Ha, A. S. Kilaru, A. M. Sellers, J. C. Hershey, S. S. Hill, E. Kramer-Golinkoff, L. Nadkarni, M. M. Debski, K. A. Padrez, L. B. Becker, and D. A. Asch. 2014. Hidden in plain sight: A crowdsourcing public art contest to make automated external defibrillators more visible. American Journal of Public Health 104(12):2306–2312.
PulsePoint. 2016. Community engagement. http://www.pulsepoint.org/resources (accessed November 11, 2016).
Ringh, M., M. Rosenqvist, J. Hollenberg, M. Jonsson, D. Fredman, P. Nordberg, H. Järnbert-Pettersson, I. Hasselqvist-Ax, G. Riva, L. Svensson. 2015. Mobile-phone dispatch of laypersons for CPR in out-of-hospital cardiac arrest. New England Journal of Medicine 372:2316–2325.
Rumsfeld, J. S., S. C. Brooks, t. P. Aufderheide, M. Leary, S. M. Bradley, C. Nkonde-Price, L. H. Schwamm, M. Jessup, J. M. E. Ferrer, and R. M. Merchant. 2016. Use of mobile devices, social media, and crowdsourcing as digital strategies to improve emergency cardiovascular care. Circulation 134(14):1–18.
















