Proceedings of a Workshop
|
April 2017 |
IN BRIEF | |
Implementing Evidence-Based Prevention by Communities to Promote Cognitive, Affective, and Behavioral Health in Children
Proceedings of a Workshop—in Brief
Communities represent the front line in addressing many behavioral health conditions that children, adolescents, young adults, and their families have to face. These conditions are not rare: during their lifetimes, almost half of all Americans will meet one or more clinical criteria for behavioral health or substance abuse disorders. These disorders impose a tremendous personal burden on the affected individuals and their families, as well as substantial costs on the broader society. The first onset of such conditions is usually in childhood or adolescence, and communities can be a key opportunity for prevention, early intervention, and treatment.
Given the importance of communities in shaping the health and well-being of young people, the Forum on Promoting Children’s Cognitive, Affective, and Behavioral Health held a workshop in Washington, D.C., June 9-10, 2016, to examine the implementation of evidence-based prevention by communities. The workshop brought together researchers, program developers and implementers, state and local officials, community leaders, health care providers, patient advocates, and other stakeholders to examine how knowledge from researchers and practitioners can best be implemented in community settings.
KEYNOTE ADDRESS
Several key factors influence the use of evidence-based interventions by communities, said keynote speaker Velma McBride Murry, the Lois Autrey Betts chair in education and human development and Joe B. Wyatt distinguished university professor at Vanderbilt University. A particular intervention may offer an advantage over what is currently available. It may be more compatible with the existing values and practices of a community. It may be simple and easy to use or provide observable results. It may allow a user to do a trial run to experiment with innovation.
![]()
Regardless of the apparent benefits of an intervention, it is inevitable that it will be adapted in some way from its formal design or previous implementations to when it is implemented in a new community, Murry pointed out. Researchers and program developers can take steps to prepare for these adaptations. They can identify to adopters the core components of a program to provide guidance on how, what, and when to change or adapt a program. They can share available findings of mediational effects and information on all components of the program that may be contributing to change. They can conduct implementation assessments to capture adaptation effects.
Balancing program fidelity and adaptation requires that a program’s implementation reflects a true collaboration of researchers and program developers in which information flows both ways, Murry said. To gain acceptance of a particular intervention, researchers and program developers need to take the time to build a strong relationship and to learn from other communities, in part by watching how programs change as they are implemented. “If we see that the intervention or target changes, that’s good,” she said. “We need to be flexible in our process of moving these projects into the field.”
These considerations suggest a conceptual model for the development and implementation of family-centered prevention programs in communities: see Figure 1. In the model, community partners work with researchers and program developers and implementers to develop an understanding of the theory of change and then developing prescriptive theories about how the process or program should be implemented in their communities. This understanding informs the intervention, how to adapt it, and how best to disseminate information about it. The collaboration affects the program’s efficacy, adaptation, and dissemination.
BUILDING COMMUNITY CAPACITY
The first panel of the workshop examined five evidence-based programs as exemplars of how selection, implementation, and ad-
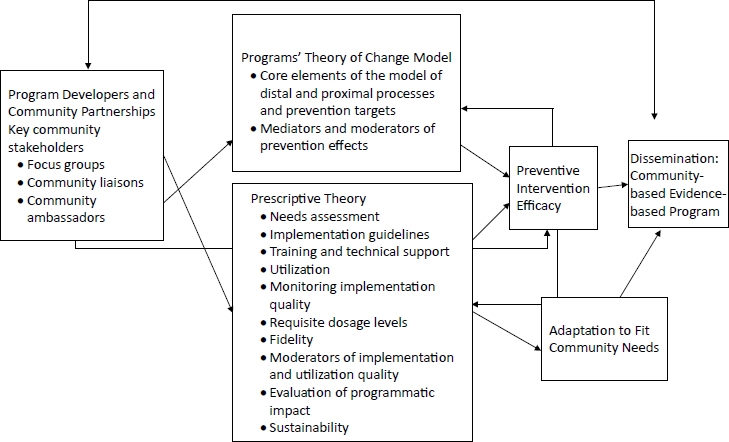
Source: Presentation at workshop by Velma McBride Murry.
aptation of evidence-based programs in communities can emerge from strong partnerships.
The Second Decade Project—which operates in Region X of the U.S. Public Health Service (Alaska, Idaho, Oregon, and Washington)—integrates guidance on issues that affect the health and well-being of adolescents ages 10-19. It targets community leaders who are champions for adolescents and are in a position to build a broad coalition. Interviews with those leaders found that they want guidance that is simple and action oriented and incorporates multi-impact measures rather than a long list of separate programs. The overall concept is to develop “a broad community plan to develop a place . . . that is going to be healthy for adolescents,” said Patrick O’Carroll, health administrator for the region.
The Bronzeville Dream Center—under the Bright Star Community Outreach project in Chicago—is working with the Bronzeville community to provide counseling, mentoring, parenting, workforce development, and advocacy to counter the effects of violence and increase positive outcomes for residents. Using a model developed in Israel known as NATAL, it is identifying, training, and certifying faith leaders to do post-trauma counseling. Community leaders in Bronzeville trust the project as a partner and broker between researchers and the community, said Christopher Harris, pastor of Bright Star Church in Chicago and founder of the Bright Star Community Outreach project. “People don’t care how much you know until they know how much you care,” he said. “That’s why we’re having the success that we’re having.”
The PROmoting School-community-university Partnerships to Enhance Resilience (PROSPER) project is a delivery system of evidence-based programs that relies on fostering partnerships, explained Richard Spoth, the F. Wendell Miller senior prevention scientist and director of the Partnerships in Prevention Science Institute at Iowa State University. The project provides a menu of evidence-based programs to prevent substance misuse and other behavior problems among youth. It supports the use of community teams that work with schools to coordinate programs, monitor quality, and generate resources for ongoing programming. The community teams also engage in strategic communication to promote awareness of the program and to recognize and reward supporters and contributors. As a result of these efforts, youth who have participated in programs implemented through the PROSPER delivery system have scored significantly lower on a range of problem behavior outcomes, including substance misuse and conduct problems. Further, PROSPER has shown to be cost effective and cost beneficial.
ThriveNYC is a mental health plan in New York City that consists of an array of interventions based on six broad principles: changing the culture, acting early, closing treatment gaps, partnering with communities, using data better, and positioning government to lead. “These initiatives will touch, if we do it well, on the order of a million New Yorkers,” said Gary Belkin, executive deputy commissioner of mental hygiene in the New York City Department of Health and Mental Hygiene. By providing opportunities for hypothesis testing, the initiative has hardwired continuous quality improvement into the plan, according to Belkin. “The hypothesis testers are the communities, and we’re building their capacity to do that. If they aren’t partners, or leaders of testing in real time iteratively, then we can’t scale.”
The last exemplar was a decade-old policy of investing in evidence-based interventions in child welfare and juvenile justice systems in New York City has resulted in major declines in foster care placements and juvenile justice placements, according to Gladys Carrión, commissioner of the New York City Administration for Children’s Services. The focus has been on reducing the rate of maltreatment, reducing out-of-home placements, and improving well-being by embedding evidence-based models in the many community-based organizations that have city contracts and case management responsibility for foster care. “Communities know their families and their children best,” said Carrión. Challenges include the need for rigorous evaluations, the changing demographic characteristics of the city, and the fiscal constraints.
CUTTING-EDGE METHODOLOGIES
Because community interventions are generally complex and multilevel, evaluations of such programs often require innovative designs. Three presenters at the workshop described several of these methodologies as examples of what can be done.
The TimeWise and HealthWise curricula that have been implemented in the United States, South Africa, and Zambia, seek to reduce substance use, risky sexual behavior, and violence while promoting positive youth development among 8th and 9th graders. Linda Caldwell, distinguished professor of recreation, park, and tourism management and human development and family studies at The Pennsylvania State University, and her colleagues have developed a theory of action that relates different combinations of interventions through mediators to student outcomes. They also have developed an experimental design in which groups of seven schools each have different combinations of interventions, with classrooms being videotaped to study the effects of different independent variables.
The Center for Personalized Prevention Research at the University of Minnesota has been experimenting with new delivery and evaluation systems. In one system, multiple and sequential randomizations have enabled researchers to test and optimize adaptive treatment strategies. In another system, preference-based interventions allow individuals to choose the intervention in which they will participate, and the program then gauges the effects on engagement and outcomes. Gerald August, professor in the Department of Family Social Science at the University of Minnesota, pointed out that these kinds of approaches can yield precision preventive interventions in behavioral health that are analogous to the kinds of interventions being developed through precision medicine.
The third presenter in the workshop session, Hendricks Brown, professor in the Departments of Psychiatry and Behavioral Sciences, Preventive Medicine, and Medical Social Sciences in the Northwestern University Feinberg School of Medicine, mentioned several innovative methodologies that have been used in the Bronzeville community in Chicago (mentioned earlier in the workshop). One example is a set of maps of neighborhood violence, youth exposure to programs, and adult networking and social processes that can be compared to examine alternative diffusion mechanisms that indicate how a program is working across and within a community.
PROGRAMS OR PRINCIPLES?
A major question in the prevention field has been whether it is possible to identify similar component elements in evidence-based programs and disseminate those elements—whether identified as principles, practices, or kernels—rather than the programs themselves. A panel of five presenters examined this question and came to mixed conclusions.
Stephen Gies, a senior researcher at Development Services Group, in Bethesda, Maryland, and Patrick Tolan, professor of education and of psychiatry and neurobehavioral sciences at the University of Virginia, offered somewhat different definitions for programs, practices, and principles. They agreed that programs are planned, coordinated, and prescribed groups of activities and processes designed to achieve a specific purpose. They also largely agreed that practices are seminal components that are extracted from multiple programs.
But Gies defined principles, which he equated with a component, kernel, or active ingredient, as behavior-influence procedures shown through experimental analysis to affect a specific behavior and that are indivisible in the sense that removing any of their components would render them inert. In contrast, Tolan defined principles as activities, processes, or relational orientations that underlie programs and are expressed by practices. Tolan also associated principles with the theories underlying a program. “What do you think you’re doing, and what is it about these programs that reflects similar theory?” he asked. In that sense, principles act as guiding ideas toward which practices and programs should be moving.
Programs based on different practices or principles can be evaluated to determine the effectiveness of either an entire program or its component parts, Gies noted. Tolan pointed out that principles, like programs, have both implementation requirements and engagement components, yet these attributes of principles have not received much scientific study.
Anthony Biglan, senior scientist at the Oregon Research Institute, described an evidence-based kernel as a simple behavior-influence technique that has been extensively validated, and he identified four types of kernels: antecedent, reinforcement, physiological, and relational. Antecedent kernels happen before the behavior, as when a classroom is structured so as to create a particular behavior. A reinforcement kernel happens after the behavior, such as a reward offered in a game. A physiological kernel changes the biochemistry of behavior, as some nutritional supplements do. A relational frame kernel creates verbal relations for a behavior, as when students are asked to describe an ideal classroom.
Biglan also noted two overarching or higher-level principles. The first is the need to minimize toxic social conditions. The second is the need to replace aversive means of control with more positively reinforcing practices. “The public health goal needs to be to increase the prevalence of nurturing families,” he said.
Amy Margolis, director of the Division of Program Development and Operations in the Office of Adolescent Health in the U.S. Department of Health and Human Services, observed that initiatives consisting of collections of programs also can provide insights into distinctions between programs and their components. In a cautionary note, Gilbert Botvin, professor emeritus of health care policy and research at Cornell University’s Weill Medical College, argued against disseminating interventions based solely on principles because there is limited research to determine what the active ingredients or core components would be for a particular program. “To unleash the power of prevention and capitalize on the past 35 years of research, it’s important at this point in time to stick to programs that have been tested and proven to be effective,” he said.
SUSTAINABLE FUNDING
Sustainable funding can ensure both continued implementation of evidence-based programs and continued support for those programs once they are implemented. Four presenters examined the question of how to sustain funding of evidence-based programs and systems, using both specific examples and broader rationales to support their views.
Tooele City, Utah, is an example of a city that decided to support the Communities That Care Program after its initial grant ended because of the passion the program had inspired and the solid evidence base it had generated. The mayor asked for $160,000, which is “enough to pay for a lot of other city services,” noted Heidi Peterson, community coordinator at Tooele City, UT, but the mayor “was able to sell that, because we had an evidence-based system in place and there were data showing that it would do what it said it would do.”
On a larger scale, in the Chicago area, Marc Atkins, professor of psychiatry and psychology at the University of Illinois at Chicago, has been working with colleagues to redesign community mental health services for urban children in poverty. He particularly advocated working through social networks, which are a key source of information and advice for community residents. For example, he and his colleagues have been identifying teachers who are influential with other teachers and asking them what parts of programs are interesting and important: this approach puts the teachers in a position to share that information with other teachers. But reaching sustainability takes time, “because people have to see other people in the social setting who are in a similar situation,” he said.
On a national level, the Community Benefit Program provides support for a wide range of health-related activities, including physical improvements and housing, economic development, community support, leadership development and training for community members, coalition building, com-
munity health improvement advocacy, and workforce development, said Sue Thau, a policy consultant for Community Anti-Drug Coalitions of America. The program requires nonprofit hospitals to invest in the health and health care of their communities in exchange for their tax-exempt status, in part by doing a Community Health Needs Assessment every 3 years. Thau urged that community coalitions get data into the assessments; share the value of multisector, data-driven strategies; demonstrate population-level outcomes that are a result of the implementation of coalition strategies; and package the entire process into a turnkey approach to solve problems for both hospitals and communities.
Ellen-Marie Whelan, chief population health officer for the Center for Medicaid and CHIP Services of the Centers for Medicare & Medicaid Services (CMS) at the U.S. Department of Health and Human Services, argued for state and local officials to take advantage of the flexibility that states have in implementing and funding innovative programs under Medicare and Medicaid. Working with CMS can be a major investment for states, since they need to provide some of the funding themselves. But “it’s worth the investment,” she said. “These things that we’re piecing together now . . . will lay some groundwork for how we’re going to move forward.”
BEING RESPONSIVE TO COMMUNITIES
Communities have both needs and wants in considering the implementation of evidence-based interventions. Distinguishing the two and addressing them appropriately require that researchers and program developers and implementers be responsive to communities. The final panel of the workshop considered this issue in the context of the challenges and opportunities that confront communities.
Responsiveness to the needs of a community can involve showing communities the best way to adapt a program rather than assuming that a program will be implemented and conducted exactly as designed or implemented elsewhere, said William Hansen, the recently retired president of Tanglewood Research. For example, his research shows that infrequent adaptations that have a positive fit with a program tend to produce better outcomes than do frequent adaptations that have either a positive or a negative fit. “You have to deliver [a program] well, and deliver it in a way that’s engaging,” he said.
Similarly, integration of behavioral health services has many potential advantages in meeting the needs of families and communities, said David Kolko, professor of psychiatry, psychology, pediatrics, and clinical and translational science at the University of Pittsburgh School of Medicine. It can engage families, provide holistic care, improve the quality of care, and reduce costs. For example, patients are more likely to attend behavioral health care sessions if when it is provided in a primary care setting rather than a specialty care setting. But far more work is needed to establish, train, and support behavioral health partnerships in primary care settings to ensure quality care that can be sustained, Kolko said.
Kaiser Permanente Northern California is an example of an integrated health care delivery system with a great deal of ethnic, cultural, and socioeconomic diversity. A study of a screening and referral to treatment program found that families, teenagers, and providers all wanted more brief intervention services in pediatric primary care and more parent and family engagement in these programs. In general, Kaiser Permanente is dedicated to prevention, said Stacy Sterling, a scientist with the company’s drug and alcohol research team. It offers population health management programs in hypertension, diabetes, weight, and exercise; and it is also doing innovative work in addressing the social determinants of health. Sterling noted that Kaiser Permanente is beginning to work on adverse childhood experiences. “These are all tied together,” she said.
The Community Anti-Drug Coalitions of America (CADCA) is another example of an organization that bases its work squarely in communities. Coalitions receive training, technical assistance, and support so they can pursue comprehensive strategies to improve population-level outcomes, explained Albert Terrillion, deputy director for evaluation and research in CADCA’s National Coalition Institute.
The final panelist at this workshop session, Manuel Ángel Oscós-Sánchez, professor of medicine in the Department of Family and Community Medicine at the University of Texas Health Science Center at San Antonio, described Familias en Acción, a community-academic research partnership to develop, implement, and evaluate youth violence prevention programs in an urban Latino community. It has demonstrated the bottom-line requirement for community involvement, he said. Communities “want to have a voice. But that’s not enough. They want to be heard.”
SMALL-GROUP DISCUSSIONS AND CONCLUDING REMARKS
Before the final plenary session of the workshop, participants divided into three groups to discuss critical issues associated with implementing evidence-based prevention programs in communities.
The first group summarized its discussion with the observation that a systems approach to public health that is focused on populations and equity can engage all levels of communities in collaborative decision making and shared accountability for actions and change.
The second group observed that healthy child development could be promoted by prevention and wellness funds for needs-based community implementation of efforts that support functioning in communities. It also observed that consideration of healthy child development in all public policies could facilitate sustainable funding for services.
The third group said that prevention efforts would benefit from consistent definitions for the terms programs, practices, principles, and kernels, along with criteria regarding when to scale up and disseminate a program, practice, principle, or kernel. It also noted that implementation of the Affordable Care Act and improved community monitoring and program evaluation provide opportunities for prevention.
In their concluding remarks, Leslie Walker and José Szapocznik both called attention to the gradual broadening of the discussions over the day and a half workshop. To move the needle in a major way, it may be necessary to transition from a strict focus on programs toward the social context and the social determinants of health, Szapocznik said. “We’re at the edge of a change here,” added Walker. “We need to begin to think differently.”
PLANNING COMMITTEE FOR THE WORKSHOP ON FUNDING OPPORTUNITIES FOR EVIDENCE-BASED PREVENTION AND INTERVENTIONS TO PROMOTE CHILDRENS COGNITIVE, AFFECTIVE, AND BEHAVIORAL HEALTH
JOSÉ SZAPOCZNIK (Cochair), Professor and Chair, Department of Public Health Sciences; Director, Miami Clinical Translational Science Institute; Director, Center for Family Studies, University of Miami; LESLIE R. WALKER (Cochair), Professor and Chief, Adolescent Medicine Division, Department of Pediatrics, Seattle Children’s Hospital and University of Washington; KAREEMAH ABDULLAH, Director, National Community Anti-Drug Coalitions of America; WILMA P. CROSS, Deputy Director, Office of Disease Prevention, National Institutes of Health; ALEXA EGGLESTON, Senior Program Officer, Conrad N. Hilton Foundation; AMY GOLDSTEIN, Associate Director for Prevention, National Institute of Mental Health, National Insitutes of Health; AMY LEFFLER, Executive Fellow, National Institute of Justice; EVE E. REIDER, Health Scientist Administrator, National Center for Complementary and Integrative Health, National Institutes of Health; BELINDA SIMS, Health Scientist Administrator, Prevention Research Branch, Division of Epidemiology, Services, and Prevention Research, National Institute on Drug Abuse, National Institutes of Health; DEBORAH KLEIN WALKER, President, American Orthopsychiatric Association; Senior Fellow, Abt Associates; and NOAM KEREN, Study Director.
DISCLAIMER: This Proceedings of a Workshop in Brief has been prepared by Steve Olson, rapporteur, as a factual summary of the presentations and discussion at the workshop. The statements made are those of the individual speakers and do not necessarily represent the views of all participants, the planning committee, or the National Academies of Sciences, Engineering, and Medicine. The planning committee was responsible only for organizing the workshop, identifying the topics, and choosing speakers.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop in Brief was reviewed by David J. Kolko, Psychiatry, Psychology, Pediatrics, and Clinical Translational Science, University of Pittsburgh School of Medicine and Wilma Peterman Cross, Office of Disease Prevention, National Institutes of Health. Patricia L. Morison, Division of Behavioral and Social Sciences and Education, served as review coordinator. The review comments and draft manuscript remain confidential to protect the integrity of the process.
SPONSORS: The Forum on Promoting Children’s Cognitive Affective and Behavioral Health is partially supported by the American Academy of Pediatrics; the American Board of Pediatrics; the American Orthopsychiatric Association; the American Psychological Association; Autism Speaks; the Centers for Disease Control and Prevention; Community Anti-Drug Coalitions of America; the Conrad N. Hilton Foundation; the Hogg Foundation for Mental Health; the National Institutes of Health; the Robert Wood Johnson Foundation; the Society for Child and Family Policy and Practice; the Society of Clinical Child and Adolescent Psychology; the Society of Pediatric Psychology; Substance Abuse and Mental Health Services Administration; U.S. Department of Health and Human Services, Assistant Secretary for Planning and Evaluation; U.S. Department of Justice.
For additional information regarding the meeting, visit http://nas.edu/communityprevention.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. (2017). Implementing Evidence-Based Prevention by Communities to Promote Cognitive, Affective, and Behavioral Health in Children: Proceedings of a Workshop—in Brief. Washington, DC: The National Academies Press. doi: https://doi.org/10.17226/24762.
FORUM ON PROMOTING CHILDREN’S COGNITIVE, AFFECTIVE, AND BEHAVIORAL HEALTH
WILLIAM R. BEARDSLEE (Cochair)
Boston Children’s Hospital and Harvard Medical School
C. HENDRICKS BROWN (Cochair)
Feinberg School of Medicine, Northwestern University
KAREEMAH ABDULLAH
Community Anti-Drug Coalitions of America
DARA BLACHMAN-DEMNER
National Institute of Justice, U.S. Department of Justice
THOMAS F. BOAT
Cincinnati Children’s Hospital Medical Center
FELESIA R. BOWEN
School of Nursing, Rutgers University
DAVID A. BRENT
School of Medicine, University of Pittsburgh
LAUREN CALDWELL
American Psychological Association
WILMA P. CROSS
Office of Disease Prevention, National Institutes of Health
ALEXA EGGLESTON
Conrad N. Hilton Foundation
RICHARD G. FRANK
U.S. Department of Health and Human Services
AMY GOLDSTEIN
National Institute of Mental Health, National Institutes of Health
COSTELLA GREEN
Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Services
RICK HARWOOD
National Association of State Alcohol and Drug Abuse Directors
J. DAVID HAWKINS
School of Social Work, University of Washington
KIMBERLY E. HOAGWOOD
Society of Clinical Child and Adolescent Psychology and New York University
COLLEEN HORTON
Hogg Foundation for Mental Health, University of Texas at Austin
JENNIFER W. KAMINSKI
U.S. Centers for Disease Control and Prevention
KELLY J. KELLEHER
Nationwide Children’s Hospital
UMA KOTAGAL
Cincinnati Children’s Hospital Medical Center
LAUREL K. LESLIE
American Board of Pediatrics and Tufts University School of Medicine
MARY ANN MCCABE
Society of Pediatric Psychology, Society for Child and Family Policy and Practice, George Washington University, and George Mason University
JENNIFER NG’ANDU
Robert Wood Johnson Foundation
LAWRENCE A. PALINKAS
School of Social Work, University of Southern California
EVE E. REIDER
National Center for Complementary and Integrative Health, National Institutes of Health
MARY JANE ROTHERAM-BORUS
University of California, Los Angeles
JOYCE SEBIAN
Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Service
PAT SHEA
National Association of State Mental Health Program Directors
ANDY SHIH
Autism Speaks
BELINDA SIMS
National Institute on Drug Abuse, National Institutes of Health
JOSÉ SZAPOCZNIK
University of Miami
VERA FRANCIS “FAN” TAIT
American Academy of Pediatrics
JENNIFER TYSON
Office of Juvenile Justice and Delinquency Prevention, U.S. Department of Justice
DEBORAH KLEIN WALKER
American Orthopsychiatric Association and Abt Associates
For additional information about the Forum, visit http://nas.edu/ccab.
Division of Behavioral and Social Sciences and Education

Copyright 2017 by the National Academy of Sciences. All rights reserved.








