Proceedings of a Workshop
| IN BRIEF | |
|
October 2017 |
Strategies to Limit Sugar-Sweetened Beverage Consumption in Young Children
Proceedings of a Workshop—in Brief
On June 21–22, 2017, the National Academies of Sciences, Engineering, and Medicine’s Food and Nutrition Board convened a workshop in Washington, DC, to explore the range of policies and programs that exist at the federal, state, tribal, and local levels to limit sugar-sweetened beverage consumption in children birth to 5 years of age.1 Topics examined over the course of the 1.5-day workshop included prevalence and trends in beverage intake among young children; beverage intake guidelines applicable to the age range of interest; challenges and opportunities of influencing beverage consumption; the role of industry in beverage intake; and knowledge gaps and research needs. This Proceedings of a Workshop—in Brief is intended to highlight key points made by individual speakers during the presentations and discussions, but it is not intended to serve as a comprehensive summary.2
In her welcome to the audience, Karen Weber Cullen, professor of pediatrics-nutrition with the Children’s Nutrition Research Center at the Baylor College of Medicine, noted that a young child may interact with a number of caretakers in various locations over the course of a day, and that a variety of influences may affect decisions about what beverage is offered to and consumed by the child. As such, a range of strategies to limit sugar-sweetened beverages exist that target different caretakers, different settings, and different influences, stated Cullen.
Following Cullen’s comments, a speaker from each of the workshop’s three sponsors provided opening remarks. Tina Kauh of the Robert Wood Johnson Foundation (RWJF) explained that the high levels of consumption among young children and the disparities in intake, especially among population groups at risk for poor health outcomes, are factors that are motivating RWJF to identify policy opportunities to decrease sugar-sweetened beverage intake and to increase safe water consumption among children 5 years of age and younger. Building on this concept, Judi Larsen of The California Endowment suggested that an opportunity exists to create better alignment of efforts to increase water intake and initiatives to reduce sugar-sweetened beverage consumption. To create policies, practices, and environments that support such changes, Larsen underscored the importance of collective action, especially at the local level. Robert Post of the Chobani Foundation commented that policies and programs intended to improve the quality of dietary intake, such as replacing sugar-sweetened beverages with water and nutrient-dense options, will need to be pragmatic and actionable. He also emphasized the importance of considering the full context of the overall dietary pattern.
___________
1 A definition of sugar-sweetened beverages was not established for this workshop. Instead, speakers were asked to include in their presentations an explanation of which beverages they were referring to when using the phrase. Unless otherwise noted, speakers discussed 100 percent fruit juice as a category separate from sugar-sweetened beverages.
2 Full proceedings of the workshop will also be released. Materials from the workshop, including presentations and videos, can be found at http://nationalacademies.org/hmd/Activities/Nutrition/StategiesToLimitSSBConsumptioninYoungChildren/2017-JUN-21.aspx (accessed September 27, 2017).
![]()
SETTING THE STAGE
The period from birth to 5 years of age is filled with major developmental milestones, including learning how and what to eat, said session moderator Leann Birch, William P. Flatt professor at the University of Georgia. Children are born with an unlearned liking for sweet, Birch noted. In newborn infants, the sweet taste elicits pleasure, promotes intake, results in endogenous opioid release, and has analgesic effects. A liking for foods and drinks that are not sweet is acquired more gradually and only if children are given repeated opportunities for new foods and flavors to become familiar and preferred. The innate predisposition toward the taste of sweet, therefore, can make young children vulnerable to displacing “other foods in the diet, especially early on when other foods are unfamiliar and are not going to be liked,” explained Birch.
One of the first sweet beverages introduced to young children is 100 percent juice, presented Anna Maria Siega-Riz, professor at the University of Virginia School of Medicine, describing recent analyses of 2005–2012 National Health and Nutrition Examination Survey (NHANES) dietary intake data. Among children 6 to 23.9 months of age, 100 percent fruit juice contributes more to total sugar and total energy intake than sugar-sweetened beverages (Grimes et al., 2015). Intake of 100 percent juice among infants younger than 12 months of age has decreased in recent years, while overall sugar-sweetened beverage intake among children 6 to 23.9 months of age has remained stable (Miles and Siega-Riz, 2017). The prominence of both 100 percent juice and sugar-sweetened beverages in the diets of infants and toddlers increases with age, observed Siega-Riz.
Similar findings were reported by Mary Story, professor at Duke University, as she described analyses of data from the Feeding Infants and Toddlers Study (FITS) 2016 of children younger than 4 years of age. Story stated that within this age group, fruit-flavored drinks are the most commonly consumed sugar-sweetened beverages and are the primary source of sugar-sweetened beverage calories. She also highlighted that compared to their non-Hispanic white and Hispanic counterparts, a greater proportion of non-Hispanic black children (2 to 4 years of age) consume sugar-sweetened beverages, a difference primarily driven by more widespread intake of fruit-flavored drinks. Across the three cycles of FITS (2002, 2008, and 2016), 100 percent juice consumption has decreased in all age groups. Trends in sugar-sweetened beverage intake, however, are less consistent, noted Story.
Young children, 2 to 5 years of age, consume the majority of sugar-sweetened beverages at home and in the homes of others (Wang et al., 2008). As such, Steven Gortmaker, professor of the practice of health sociology at the Harvard T.H. Chan School of Public Health, suggested that interventions likely to have the greatest effect are those that would affect the home environment. Gortmaker’s team has created microsimulation models to project the 10-year cost-effectiveness and estimate the effect on population health of various strategies to improve nutrition and physical activity environments. His group has published modeled results for the effect of three strategies specifically related to reducing sugar-sweetened beverage intake in children: excise taxes, the Nutrition and Physical Activity Self-Assessment for Child Care (NAP SACC), and Smart Snacks in Schools. Each of these approaches is expected to prevent cases of childhood obesity over a 10-year period, albeit to various degrees because of differences in size and scope of the interventions. A sugar-sweetened beverage excise tax of one cent per ounce is projected to prevent approximately 580,000 cases of childhood obesity. Sugar-sweetened beverage excise taxes and Smart Snacks in Schools were each projected to result in health care cost savings for every $1 spent on the initiative (Gortmaker et al., 2015). With respect to modeling the effects of interventions limiting 100 percent juice consumption, Gortmaker pointed to challenges of existing data, including unreliable measurement of intake and few longitudinal studies evaluating the effect of change in intake on change in relative weight status in children.
Christina Hecht, senior policy advisor at the University of California Nutrition Policy Institute, echoed the need for better data, describing the information on young children’s hydration status and longitudinal changes in beverage intake profiles as “limited.” Nevertheless, evidence suggests that unhealthy beverage intake patterns begin early in life and are seen disproportionately in black, Hispanic, and low-income populations (Grimes et al., 2017; Watowicz et al., 2015). “We want to make plain water the normative beverage after age-appropriate amounts of milk in this age group,” said Hecht.
Because children younger than 7 years of age are particularly vulnerable to the toxic effects of lead, Hecht explained that an initial step in water promotion is to consider safety. She noted that while most communities have safe tap water, not all do. Hecht explained that even though most water utilities provide safe water, lead can leach into tap water from lead service lines and premise plumbing. Hecht described provisions for testing for lead in tap water in licensed child care centers, which presently exist in only a handful of states. She reported that a barrier to performing water testing is the fear of the cost of remedying any issue that is found.
Availability also plays a role in water consumption patterns, observed Hecht. She described studies in which improving water access and offering beverage selection education in the school setting increased water intake among students, but she added that little research has been done in the child care setting to date. Hecht outlined beverage standards
for child care programs operating under the Child and Adult Care Food Program (CACFP), noting that effective October 1, 2017, “water must be offered throughout the day with visual cues.” In considering the current status of beverage intake among young children, Hecht suggested that a need exists to provide clear guidance to parents and caregivers on what, how, and how much children should be drinking.
BEVERAGE INTAKE GUIDELINES FOR YOUNG CHILDREN
The Dietary Guidelines for Americans (DGA) shape the policies for nutrition education and food assistance programs and affect product formulation and reformulation by the food industry, said Rafael Pérez-Escamilla, professor of epidemiology and public health at the Yale School of Public Health. The DGA, which currently apply to children 2 years of age and older, are informed by the scientific report of the Dietary Guidelines Advisory Committee (DGAC). Pérez-Escamilla, a member of the 2015 DGAC, explained that the committee found higher intakes of refined grains and sugar-sweetened foods and beverages to be detrimental to health, citing relationships with obesity, dental caries, type 2 diabetes, and cardiovascular disease. In considering children’s overall diet, the 2015 DGAC identified sugar-sweetened beverages as one component of an unhealthy dietary pattern. For both findings, Pérez-Escamilla noted that the evidence specific to children, particularly cohort studies, was lacking.
In addition to evaluating dietary intake patterns, the 2015 DGAC also provided recommendations on evidence-based policies. Pérez-Escamilla highlighted a number of policies recommended by the 2015 DGAC relevant to limiting sugar-sweetened beverage intake, including implementing excise taxes on sugar-sweetened beverages, leveraging federal food assistance programs to encourage the purchase of healthier food options, developing and expanding programs within schools and early care and education (ECE) settings, and including added sugars on the Nutrition Facts label.
Providing nutrition guidance applicable to children and adolescents is a major area of focus for the American Academy of Pediatrics (AAP), noted Stephen Daniels, professor and chair of the Department of Pediatrics at the University of Colorado School of Medicine and chair of the AAP Committee on Nutrition. Although AAP does not currently have a specific policy statement regarding the sugar-sweetened beverage intake of young children, Daniels explained that efforts are currently under way to develop a statement with the American Heart Association regarding the health effects of added sugar. Based on AAP’s existing feeding and nutrition guidance for children birth to 5 years of age, Daniels suggested there is a hierarchy of beverages for young children. Breastfeeding and, when breastfeeding is not possible, formula make up the major nutrition for the first year of life. For children 12 months of age and older, milk serves as the primary beverage, followed by water. AAP has specified that soft drinks, sports drinks, and energy drinks are not appropriate for young children. Current AAP guidance, however, does allow for 100 percent fruit juice to be part of a child’s diet beginning at 12 months of age. While whole fruit is preferred, Daniels explained that 100 percent fruit juice can have a role in helping a child consume an appropriate number of fruit servings, but he emphasized the importance of portion size—up to 4 ounces per day for children 1 to 3 years of age and up to 6 ounces per day for children 4 to 6 years of age.
INFLUENCING BEVERAGE CONSUMPTION THROUGH FEDERAL, STATE, AND LOCAL POLICIES AND PROGRAMS
According to Sara Bleich, professor of public health policy at the Harvard T.H. Chan School of Public Health, approximately one-quarter of the U.S. population make use of at least 1 of the 15 federal nutrition assistance programs each year. Programs that serve children in the birth to 5 years age range include the Supplemental Nutrition Assistance Program (SNAP), CACFP, the National School Lunch Program, the School Breakfast Program, the Summer Food Service Program, the Special Milk Program, and the Special Supplemental Nutrition Program for Women, Infants, and Children. The beverage policies within these seven programs are relatively similar, with nuanced differences (e.g., specifications of allowable milks), noted Bleich. SNAP, however, is the only program that allows for reimbursement of sugar-sweetened beverages. With respect to consumption, Bleich described the evidence as “mixed” regarding whether participants enrolled in SNAP consume more sugar-sweetened beverages than their low-income, nonparticipant counterparts. “The overarching point here is that we in the United States drink a lot of sugary beverages,” she said, and indicated that higher consumption among participants enrolled in SNAP may be driven more by socioeconomic status than by program participation. Bleich suggested that empirical data are needed to determine whether restricting sugar-sweetened beverages in SNAP would ultimately affect the consumption levels of program participants.
“Establishing healthy behaviors and eating patterns early in life can have long-lasting impacts,” stated Heidi Blanck, chief of the Obesity Prevention and Control Branch at the Centers for Disease Control and Prevention (CDC). Given this, Blanck explained that CDC’s Division of Nutrition, Physical Activity, and Obesity takes a life course approach to the state, territory, tribal, and local community efforts it funds and supports. Accordingly, one area of focus is breastfeeding
support. She noted that CDC’s efforts have included helping to expand the number of baby-friendly hospitals, providing support to employed women, and creating support at the community level, especially for African American and low-income women. Another component of the life course approach Blanck highlighted is fostering healthy growth through ECE settings and child obesity management. Blanck presented a spectrum of possible obesity prevention opportunities within ECE settings actionable at the state and local levels (see Figure 1). Blanck also shared that CDC has been working toward improving free and low-cost professional development for ECE providers, noting that nearly 2,000 providers have taken a recently available, on-demand module on healthy beverages. Blanck touched on a third component of the life course concept—maintaining good nutrition. To that end, CDC has created several guidelines, toolkits, frameworks, and other resources to help create healthy food environments in various community settings, including schools, hospitals, parks and recreation venues, worksites, and ECE settings.
With more than half of children 5 years of age and younger spending a considerable portion of their time in non-parental care, opportunities exist to leverage child care policies to improve young children’s access to nutritious food and active play, suggested Natasha Frost, senior staff attorney at the Public Health Law Center. She explained that ECE settings are primarily regulated at the state level, which has led to a highly decentralized and heterogeneous landscape across the United States. States differ with respect to funding streams, quality measures, licensing and administrative regulations, and definitions for what qualifies as a child care center or family child care home. Frost noted that provisions about sugar-sweetened beverages in the ECE setting typically reside within state licensing regulations, rather than in other regulatory requirements or quality measures. Few states, however, currently have such a provision. In working toward policy changes in ECE settings, she noted the importance of including child care providers in the discussion to provide insight, especially with respect to potential implementation barriers. Based on her experience in Minnesota, Frost also indicated that an opportunity exists to better coordinate across the broad array of advocates for the birth to 5 years age range. She
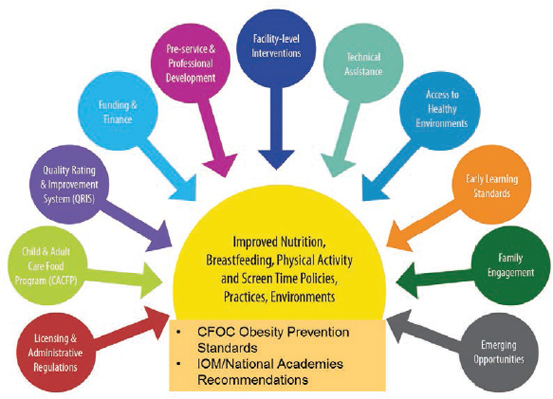
FIGURE 1 Spectrum of opportunities for obesity prevention in early care and education settings.
NOTES: CFOC = Caring for Our Children; IOM = Institute of Medicine; National Academies = National Academies of Sciences, Engineering, and Medicine. This figure has been modified from what the speaker presented to reflect that as of March 15, 2016, the Health and Medicine Division of the National Academies of Sciences, Engineering, and Medicine continues the consensus stud-ies and convening activities previously undertaken by the Institute of Medicine.
SOURCES: CDC, n.d. (modified). Presented by Heidi Blanck, June 21, 2017.
cautioned that few states have expressly given local jurisdictions the authority to implement their own nutrition and physical activity standards. For that reason, Frost suggested consideration be given to whether local changes can be enacted through law or implemented through programmatic interventions.
In making health equity a priority, New York City’s local health department takes into account the larger societal context and structural factors that contribute to the disparities, began Kim Kessler, assistant commissioner for the Bureau of Chronic Disease Prevention and Tobacco Control at the New York City Department of Health and Mental Hygiene (NYC Health). Recognizing that it is challenging to make healthy selections in environments that are not conducive to such choices, NYC Health uses a multi-pronged and comprehensive approach to increase access to and awareness of healthy foods and to decrease the availability and overconsumption of unhealthy foods, explained Kessler. For example, she shared that in 2006, the Board of Health amended the health code to include requirements for child care centers that prohibit provision of sugar-sweetened beverages, require appropriate juice portion sizes (which were further modified in 2015), and increase the availability of drinking water. Standards have also been established for meals and snacks and vending machines in city spaces. Kessler acknowledged that some efforts that were attempted by NYC Health but not implemented—such as proposing a sugar-sweetened beverage tax, making sugar-sweetened beverages ineligible for purchase with SNAP benefits, and introducing a portion cap on sugar-sweetened beverages at food service establishments—have played a significant role in raising awareness about the health effects of sugar-sweetened beverages.
CHALLENGES AND OPPORTUNITIES OF EMERGING AND INNOVATIVE STRATEGIES
Henrietta Sandoval-Soland, food access director for the Community Outreach and Patient Empowerment (COPE) Program, said the organization was founded in 2009 to eliminate health disparities and improve the well-being of American Indian and Alaska Natives on Navajo land. COPE is one of the nine tribes and organizations participating in the Notah Begay III Foundation’s Water First! Learning Community. Over the next 2.5 years, the nine awardees will assess sugar-sweetened beverage consumption, safe drinking water access, and breastfeeding promotion practices to establish priority areas in forming policies and system changes within their respective communities, explained Sandoval-Soland. Preliminary results from COPE’s initial needs assessment indicate tradition and family are two key factors that affect the food and beverage selections of Navajo Nation residents. Emphasizing these influences, Sandoval-Soland presented the following comment from one of COPE’s survey participants: “Water is my clan. We are water—we come from water. There are water beings we pray to.” As COPE begins work on the next stage of the project, it will gather and integrate ideas from community members to ensure the messages about reducing sugar-sweetened beverage consumption are culturally appropriate.
Marlene Schwartz, director of the Rudd Center for Food Policy and Obesity, provided an overview of Howard County Unsweetened, a multifaceted, community-based initiative designed to improve beverage environments in Howard County, Maryland. She characterized the campaign as the “social ecological model in practice” (see Figure 2). One component of the campaign Schwartz highlighted was the Better Beverage Finder, a website that provides users with options for alternatives to sugar-sweetened beverages and maps of where those products can be purchased in the county (Horizon Foundation, 2014). She also explained that through another element of the campaign, the Healthy Howard program, child care centers had an opportunity to evaluate their policies and practices and set goals related to beverages, screen time, and breastfeeding support. A media campaign primarily targeting mothers was also carried out and included advertisements on local cable television, digital media, and social media, along with direct mail to county households. Although sugar-sweetened beverages are still prevalent in the county, analyses suggest that the campaign has made inroads, with sales of sugar-sweetened soda, fruit-flavored beverages, and 100 percent juice falling to a greater degree in Howard County than in stores in a nearby state that were matched for sales of sugar-sweetened beverages at baseline.
“We know that defaults help to set people’s expectation for what they should do,” said Margo Wootan, director of nutrition policy at the Center for Science in the Public Interest. She explained that restaurant children’s meals, which bundle items and offer them together at a reduced cost, serve as an example of a default. Evidence suggests that changing the defaults in children’s meals to healthier options affects the average calories of meals that are chosen and consumed (Peters et al., 2016). Advocacy is one approach being taken to create such changes. Through a variety of modes of action, including partnerships and campaigns, the proportion of top chain restaurants offering sugar-sweetened beverages on their children’s menus has decreased from more than 90 percent in 2008 to approximately 75 percent in 2016, noted Wootan. Children’s meals are also being changed though public policy. In California, Santa Clara County and the cities of Davis, Stockton, and Perris, for example, each have policies that require the default beverages in children’s meals to be healthy options. Wootan acknowledged that removing sugar-sweetened beverages as the default beverage for children’s meals is not the single antidote to the obesity epidemic, but she suggested it is a means to changing social norms.
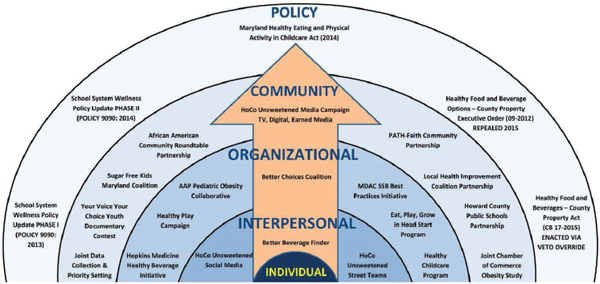
FIGURE 2 Social ecological model of the Howard County Unsweetened campaign.
NOTE: AAP = American Academy of Pediatrics; HoCo = Howard County; MDAC = Maryland Dental Action Coalition; PATH = People Acting Together in Howard; SSB = sugar-sweetened beverages.
SOURCES: Presented by Marlene Schwartz, June 21, 2017. Printed with permission from the Horizon Foundation.
Taxation and warning labels are two strategies that fit in the context of a broad range of options for local communities, noted Lynn Silver, senior advisor at the Public Health Institute. Since 2014, nine U.S. jurisdictions have approved sugar-sweetened beverage taxes. The level of taxation, the products taxed, and the uses of the generated revenue differ across jurisdictions, explained Silver. Evidence from the first year of a penny-per-ounce excise tax on sugar-sweetened beverages in Berkeley, California, suggests “taxes may be effective in shifting consumers to healthier beverages without undue economic hardship and while raising revenue,” she said. As for warning labels, Silver described two models that have been proposed as local laws in the United States— labeling on the product and labeling on print advertisements. The former has yet to be passed as legislation. The latter, which would primarily affect point-of-sale advertisements in stores and on coolers, has passed in San Francisco, but is currently being challenged.
A subset of local polices to limit sugar-sweetened beverages has been subject to litigation, stated Michelle Mello, professor of law at the Stanford Law School and professor of health research and policy at the Stanford University School of Medicine. She noted that judicial protection of commercial speech has made regulating advertising difficult from a legal perspective. Two ordinances in San Francisco—one, an ordinance banning advertising on certain city properties, the other, a sugar-sweetened beverage warning label ordinance—serve as examples, as they are currently being challenged in court as restriction on speech and compelled speech (the companies assert that they are being forced to express the government’s viewpoint). In cases of compelled speech, Mello explained that the government fares best in court when it can establish that the information it is requiring to be disclosed is factual and uncontroversial. “These cases really turn critically on how the court is going to review it, what standard is going to apply, and that is really still being worked out,” she said. Mello also observed that technical and sometimes arcane provisions in local and state laws have been used to challenge strategies. For instance, the New York City soda portion cap put forth by the Board of Health was not upheld because the City Charter gave the City Council the authority to impose such a rule, not the Board of Health. Mello ended her remarks by suggesting legal challenges to local public policy can be overcome with careful program design decisions and guidance from lawyers early in the process.
THE ROLE OF INDUSTRY IN SUGAR-SWEETENED BEVERAGE CONSUMPTION
Young children are particularly vulnerable to the persuasive intent of advertising, stated Jennifer Harris, director of marketing initiatives at the Rudd Center for Food Policy and Obesity. In a step toward providing extra protection to this age
group, Harris noted that most major food companies participate in the voluntary Children’s Food and Beverage Advertising Initiative (CFBAI), which sets nutrition standards for products that can be advertised to children younger than 12 years of age. She added that most companies also have policies that they do not advertise in media primarily directed toward children younger than 6 years of age. Harris acknowledged companies participating in CFBAI eliminated advertisements of full-sugar beverages on child-oriented television programming in 2016, but indicated that young children watch other types of programming and are still being exposed to advertisements for sugar-sweetened beverages.
Harris explained that children’s beverages are also marketed to parents, often through nutrient content claims (e.g., “no high-fructose corn syrup”) and structure/function claims (e.g., “probiotics to help support digestive health”). She highlighted that toddler drinks (also called toddler milks or toddler formulas) are a fairly new beverage category, with the intended consumer being young children who have reached the point of no longer consuming infant formula. Harris described such products as “sweetened milk,” and she identified these products as an emerging issue.
Richard Black, a principal at Quadrant D Consulting, framed the first portion of his presentation around the concept of establishing trust across all stakeholders, including industry. “We have to recognize and deal with our own biases and recognize that everyone brings something worthwhile to the table,” he said. Related to the concept of biases, Black highlighted the importance of careful interpretation of data and being mindful “of interpreting things in a way that we would like to see them interpreted.” He then noted that industry has engaged in voluntary efforts that have had evidence of effect, such as removing more than 6 trillion calories per year from the marketplace through the Healthy Weight Commitment Foundation and placing caloric information on the front of packages. Black also emphasized the importance of leveraging digital media in efforts to limit sugar-sweetened beverage consumption. Black concluded his presentation by saying that accountability is a key aspect of partnerships, including developing and tracking measurable and interpretable outcomes and keeping partners actively supportive of such efforts.
In her remarks about the Alliance for a Healthier Generation’s broad range of partnerships across different sectors, Anne Ferree, leader of the organization’s engagement with the business sector, echoed several of Black’s sentiments about the value of working collaboratively with companies. As an example, Ferree described the 2006 Alliance School Beverage Guidelines in which companies agreed to phase out the sale of full-calorie carbonated soft drinks, shift product mix toward low- and no-calorie beverages, and reduce the portion sizes available in schools. This agreement led to a 90 percent reduction in beverage calories shipped to schools between 2004 and the 2009–2010 school year (Wescott et al., 2012).
Ferree shared several lessons the Alliance for a Healthier Generation has learned in its experience with partnerships. She emphasized the importance of sustaining relationships and continuing to set new goals to work toward together. One key to the Alliance for a Healthier Generation’s long-term partnerships has been establishing top-down support from “high-level champions” at the companies. Ferree also highlighted the importance of having an understanding of the company’s business, and to “speak their language and challenge their thinking.” Pointing to the complexities of the interconnected elements of the food system, she expressed that a systems approach is needed to think through an issue, identify gaps, and consider solutions. Finally, Ferree underscored the value of being transparent and maintaining integrity throughout the life course of a partnership.
REFLECTIONS AND FUTURE OPPORTUNITIES
Virginia Stallings, professor of pediatrics at the University of Pennsylvania Perelman School of Medicine and director of the Nutrition Center at the Children’s Hospital of Philadelphia, was charged with providing her reflections on the presentations and discussion that took place over the course of the workshop. She began by emphasizing that the age group of interest, children birth to 5 years of age, is completely dependent on what is served or offered to them. Stallings described this dependency as a strength of focusing on young children and something that could be leveraged. She thought that opportunities exist to turn the goal of limiting sugar-sweetened beverage consumption in young children into a “public health step and message that all parents and communities and even the government can be proud of.” Stallings challenged the audience to consider what the messages could be and how to build the evidence, create cultural awareness, be relevant to populations across income strata, and make use of local, state, and federal government.
Following her remarks, Stallings moderated a panel discussion with Black, Daniels, Schwartz, and Story. Speakers and audience members considered various topic areas, with particular attention paid to addressing fruit drinks, filling gaps in existing data, and creating a message for parents, specific population groups, and the community at large.
One of the challenges the panel addressed was the terminology used to describe fruit drinks that are not 100 percent juice. Schwartz indicated that using the term fruit drinks to describe such products can lead to confusion because it contains the word fruit, a sentiment also shared by Story. Daniels wondered if the word fruit could be reserved only for products that are 100 percent juice. One issue that could arise with such a proposition, Black suggested, is with the
legitimate descriptive terms of flavor, which are not considered content claims in the United States (e.g., “fruity”). Recognizing the complexities related to fruit drinks, Story put forth the idea of convening a meeting or a taskforce to specifically consider how to define such products and how to limit their consumption in young children.
Various limitations of existing data were touched on during the panel discussion. Schwartz suggested that there is “an empirical question about what would happen if we really recommended that [children] not drink 100 percent fruit juice up until age five,” and acknowledged that there are concerns about the dietary substitutions that would occur. Black questioned whether it was necessary to collect data on children birth to 6 months of age, as it would be assumed that this age group would not be consuming sugar-sweetened beverages. Stallings responded that such data would be needed, and expressed that “sometimes the prioritization or the imperative nature of change comes out of finding out something we [did not] believe was happening is happening.” Daniels also countered, suggesting that longitudinal data are needed to understand the interplay of taste preference and parental feeding practices on long-term beverage preferences.
The panel also explored the concept of developing effective messages. Schwartz noted that messages about growth, health, and development are important to parents of young children. When asked about how to promote change among specific population groups, Story offered that a key to promoting change is tailoring the message. Black thought it would be important to communicate a message that allows people to identify what products they want, rather than focusing on the products they are not supposed to have. He also thought that cutting-edge approaches with social media could be used more effectively. A member of the audience commented that there may be learnings and evidence from tobacco prevention campaigns (e.g., The Real Cost, Fresh Empire, Truth) that could potentially be applied to sugar-sweetened beverage strategies.
In her closing remarks, Cullen revisited the idea that over the course of a day, a young child may encounter different caretakers, in different settings, with different influences, and thought the strategies presented throughout the workshop highlighted the spectrum of approaches that currently exist. While she acknowledged the range of opportunities for action, Cullen emphasized that the family and home environment are key in efforts to limit sugar-sweetened beverage consumption in young children.♦♦♦
REFERENCES
CDC (Centers for Disease Control and Prevention). n.d. Spectrum of opportunities for obesity prevention in the early care and education setting. https://www.cdc.gov/obesity/downloads/spectrum-of-opportunities-for-obesity-prevention-inearly-care-and-education-setting_tabriefing.pdf (accessed August 1, 2017).
Gortmaker, S. L., Y. C. Wang, M. W. Long, C. M. Giles, Z. J. Ward, J. L. Barrett, E. L. Kenney, K. R. Sonneville, A. S. Afzal, S. C. Resch, and A. L. Cradock. 2015. Three interventions that reduce childhood obesity are projected to save more than they cost to implement. Health Affairs (Millwood)34(11):1932–1939.
Grimes, C. A., E. A. Szymlek-Gay, K. J. Campbell, and T. A. Nicklas. 2015. Food sources of total energy and nutrients among U.S. infants and toddlers: National Health and Nutrition Examination Survey 2005–2012. Nutrients7(8):6797–6836.
Grimes, C. A., E. A. Szymlek-Gay, and T. A. Nicklas. 2017. Beverage consumption among U.S. children aged 0–24 months: National Health and Nutrition Examination Survey (NHANES). Nutrients9(3):E264.
Horizon Foundation. 2014. Better beverage finder. http://www.betterbeveragefinder.org (accessed August 1, 2017).
Miles, G., and A. M. Siega-Riz. 2017. Trends in food and beverage consumption among infants and toddlers: 2005–2012. Pediatrics139(6):e20163290.
Peters, J., J. Beck, J. Lande, X. Pan, M. Cardel, K. Ayoob, and J. O. Hill. 2016. Using healthy defaults in Walt Disney World restaurants to improve nutritional choices. Journal of the Association for Consumer Research1(1):92–103.
Wang, Y. C., S. N. Bleich, and S. L. Gortmaker. 2008. Increasing caloric contribution from sugar-sweetened beverages and 100% fruit juices among U.S. children and adolescents, 1988–2004. Pediatrics121(6):e1604–e1614.
Watowicz, R. P., S. E. Anderson, G. L. Kaye, and C. A. Taylor. 2015. Energy contribution of beverages in U.S. children by age, weight, and consumer status. Childhood Obesity11(4):475–483.
Wescott, R. F., B. M. Fitzpatrick, and E. Phillips. 2012. Industry self-regulation to improve student health: Quantifying changes in beverage shipments to schools. American Journal of Public Health102(10):1928–1935.
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Nancy Konopasek and Meghan Quirk as a factual summary of what occurred at the workshop. The statements made are those of the rapporteurs or individual workshop participants and do not necessarily represent the views of all workshop participants; the planning committee; or the National Academies of Sciences, Engineering, and Medicine.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Sylvia Rowe, SR Strategy, LLC, and Jennifer Weber, American Heart Association. Lauren Shern, National Academies of Sciences, Engineering, and Medicine, served as the review coordinator.
SPONSORS: This workshop was partially supported by The California Endowment, the Chobani Foundation, and the Robert Wood Johnson Foundation.
For additional information regarding the workshop, visit http://nationalacademies.org/hmd/Activities/Nutrition/StategiesToLimitSSBConsumptioninYoungChildren/2017-JUN-21.aspx.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2017. Strategies to limit sugar-sweetened beverage consumption in young children: Proceedings of a workshop—in brief. Washington, DC: The National Academies Press. doi: https://doi.org/10.17226/24897.
Health and Medicine Division

Copyright 2017 by the National Academy of Sciences. All rights reserved.









