3
Global Obesity Prevention and Treatment Efforts
The charge to the three speakers in the workshop’s second session was to highlight efforts to identify, promote, and monitor global policy and systems initiatives that are designed to address the obesity problem, said session moderator James Sallis, distinguished professor emeritus of family
medicine and public health at the University of California, San Diego, and professorial fellow at Australian Catholic University, Melbourne.
MANAGEMENT AND ADVOCACY FOR PROVIDERS, PATIENTS, AND SYSTEMS
Olivia Barata Cavalcanti, director of health systems and professional education at the World Obesity Federation, discussed her organization’s Management Advocacy for Providers, Patients, and Systems (MAPPS) program. She described the program’s main goal as learning how national health care systems function regarding obesity policy, prevention, and treatment. The findings will be used to create a Health Systems for Obesity Index, she said, which will be added to the Federation’s Global Obesity Observatory, a repository of obesity prevalence and incidence data.
Barata Cavalcanti explained that the World Obesity Federation decided to focus on health systems because obesity is being tackled with multifactorial solutions. It is helpful to understand the clinical environment in different countries, she added, and whether and how individuals can access obesity treatment. She argued that identifying barriers and potential solutions to overcome them can lead to best practices that can be shared with other countries.
Barata Cavalcanti shared a brief description of the MAPPS methodology. The program began by convening a group of health systems experts to advise the process. Data collection commenced with an online literature review in PubMed, using selected search keywords in combination with the country’s name to learn more about its health systems in relation to obesity treatment and control strategies. The team implemented narrower search terms when results were too numerous, and used more location-specific terms as the search progressed. A website scoping review followed, Barata Cavalcanti continued, whereby the team explored, for example, the websites of ministries of health for different countries. The team also performed keyword searches to find information about health systems’ financial mechanisms for coverage of obesity treatment. According to Barata Cavalcanti, limitations included language barriers that made it difficult to extract materials not in English, as well as an overabundance of materials in English, which required limiting the depth of the research. She added that the quality and quantity of information varied among countries, and the team frequently had to conduct interviews with in-country informants to validate findings. These interviews contributed additional value, she remarked, because they provided on-the-ground perspectives on how the various health systems work.
Next, Barata Cavalcanti continued, the team sent questionnaires to key informants in each country of interest. The aim, she explained, was to collect information about such topics as whether the country defines obesity as
a disease, the operations and funding mechanisms for its health care system, and cultural and political influences on obesity. “We had some difficulty getting responses,” she disclosed, suggesting that this was likely because the questionnaire was lengthy. Furthermore, recipients included people in high-level positions, she observed, “which means that they are also very busy.”
The team then decided to develop two shorter, online questionnaires, Barata Cavalcanti reported, giving recipients the choice of participating in an in-depth interview. Since then, she said, in addition to the World Obesity Federation’s country members, more than 100 key informants have been invited to complete the online questionnaires. She added that respondents include a variety of medical and health care professionals, public health advisors, and researchers, to provide a “360-degree perspective.” The questionnaires have been translated into Italian, Portuguese, and Spanish, which she said is expected to improve the response rate.
Barata Cavalcanti shared the preliminary results of this work, remarking that they are constantly updated and refined as more countries and stakeholders are added. To gauge progress toward defining obesity as a disease, she explained, interviewees are asked to rate on a scale from 0 to 10 where their country’s government and health care providers are in that process. Every country is at a different place in this journey, she noted, and results are not consistent among high-income or low-income countries. What is consistent, she reported, is that health care providers are more likely than government officials to rate their country as being further along in the process. Some interviewees from the same country had completely different perspectives depending on their line of work and location within the country, she added, and outliers were removed from the results.
Barata Cavalcanti highlighted as one of the most valuable results of the study that interviewees identified their country’s five greatest barriers to obesity treatment. Lack of training for health care providers was the most commonly cited barrier, which was named by 50 percent of respondents, followed by lack of access to treatment and medications (especially subsidized medication) and lack of knowledge and awareness (among the public, health care providers, the government, and patients) about obesity’s causes and impact. Additional barriers identified are shown in Figure 3-1.
Barata Cavalcanti also shared data on the availability of specialized obesity training in 30 countries: approximately one-quarter of the countries have no such specialist training available; in another quarter, the availability of such training is unknown; and the remaining half of the countries reported specialist training for bariatric surgery, nutrition, counseling, or other broad-ranging specialist training. Barata Cavalcanti observed that the diversity of responses indicates the lack of a consistent plan of action for tackling obesity among different health systems. “That is one of the biggest problems that we have at the moment,” she maintained. She added that
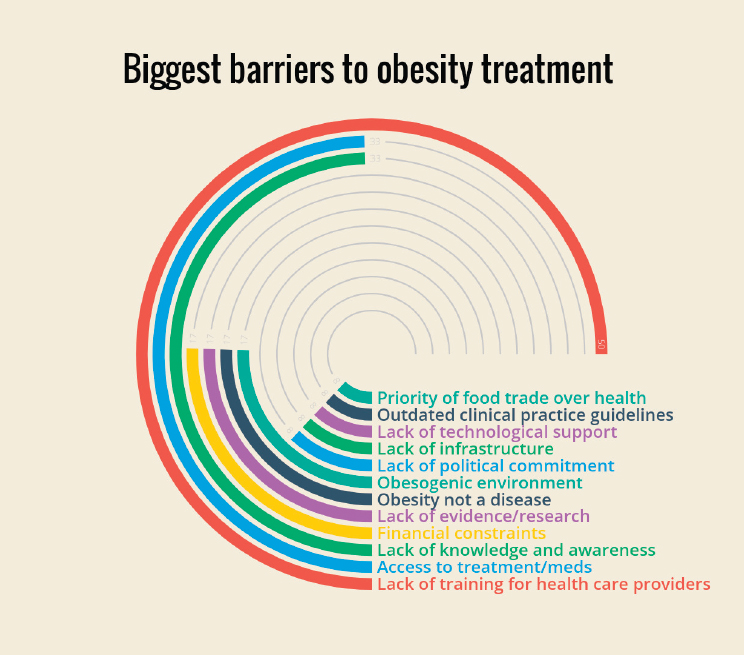
NOTE: Numbers at the end of each arc represent the percentage of respondents identifying that factor as a barrier.
SOURCE: Presented by Olivia Barata Cavalcanti, October 9, 2018.
lower availability of qualified obesity treatment professionals was reported in rural compared with urban areas.
Results of the data analyses are shared with country governments in the form of “traffic light report cards,” Barata Cavalcanti said (see Figure 3-2). The colors indicate areas in which a country is doing well and those in which it can improve, she explained, adding that there is wide variability among countries.
MORE ACTIVE PEOPLE FOR A HEALTHIER WORLD
Fiona Bull, program manager in the Department of Prevention of Noncommunicable Diseases at the World Health Organization (WHO),

NOTE: BMI = body mass index.
SOURCE: Presented by Olivia Barata Cavalcanti, October 9, 2018.
described the role of physical activity in obesity solutions and reviewed WHO’s global action plan for increasing physical activity (WHO, 2018a).
Bull began with a brief review of key milestones in physical activity, noncommunicable diseases (NCDs), and global health, noting that “it has been a patchy history.” A U.S. Surgeon General’s report in 1996 “really put the stamp on physical activity,” she asserted (HHS, 1996). The WHO Global Strategy on Diet, Physical Activity, and Health followed in 2004 (WHO, 2004), along with documents to help countries implement its guidance. As researchers and entities such as WHO made the case for physical activity’s contributions to promoting health and preventing NCDs and obesity, things started to change, Bull recalled.
According to Bull, physical activity gained a “good foothold” with the 2013 release of WHO’s Global Action Plan for the Prevention and Control of NCDs 2013–2020 (WHO, 2013). That document, she elaborated, includes recommendations for policy actions to promote physical activity and sets a global target for a 10 percent relative reduction in the prevalence of insufficient physical activity by 2025. One of the report’s appendixes presents “best buys” and “good buys,” which she described as cost-effective interventions relevant for all countries, as determined by WHO-CHOICE (CHOosing Interventions that are Cost-Effective) cost-effective analysis methods, and which were updated in 2018. Bull explained that a “best buy” is public education campaigns combined with community-based education and environmental programs, and a “good
buy” is counseling and referral as part of routine primary health care services through the use of brief interventions. Other interventions have not undergone the WHO-CHOICE cost-effectiveness modeling but are recognized as necessary and valuable, she pointed out, citing the examples of efforts to promote physical activity in school settings and to improve urban designs so as to provide safe, easy access to public transport. Most recently and after much consultation, she said, WHO produced a Global Action Plan on Physical Activity 2018–2030 to accelerate implementation of the recommended policies (WHO, 2018a).
Bull paused to share the latest physical activity data released from WHO (Guthold et al., 2018), noting that these data “emphasize how countries were quite right in the urgent need to act.” She stressed that 28 percent of adults globally fail to achieve the levels of physical activity recommended for optimal health. This percentage has been relatively unchanged since 2001, she observed, and the trend has remained flat for both men and women, with approximately 25 percent and 31 percent, respectively, not meeting recommended levels. Turning to regional differences in the current prevalence of inactivity, she flagged the Latin American and Caribbean region for its overall high levels of inactivity and sizable difference between men and women (see Figure 3-3). There is even more concern within regions, she added, noting that as many as 70 percent of people in some regions do not meet the recommendations.
Bull also pointed out that the prevalence of inactivity is lowest in low-income countries, higher in middle-income countries, and highest in high-income countries (see Figure 3-4). The pattern, she elaborated, shows that sedentary time is positively associated with urbanization and globalization and the corresponding changes to work and travel patterns. “We see this very profoundly in these data,” she said.
Turning back to WHO’s global action plan on physical activity, Bull highlighted the extensive multisector stakeholder consultation that was part of its development. She stated that this collaboration to determine what is feasible, practical, and applicable is expected to pay off in the implementation phase. Now that the plan has reached the milestone of World Health Assembly endorsement, she remarked that “in some ways, it is the end of the beginning.”
Bull underscored the plan’s message that there are many ways to be active. She added that talking about specific ways, such as playing, dancing, cycling, or walking, resonates with nonhealth sectors that may be less accustomed to the term “physical activity.” She explained that the updated plan maintains the 2013 plan’s global target of a 10 percent relative reduction in the prevalence of insufficient physical activity by 2025, and also targets a 15 percent reduction by 2030. To achieve these goals, she suggested that all people have access to safe and enabling environments, as well as
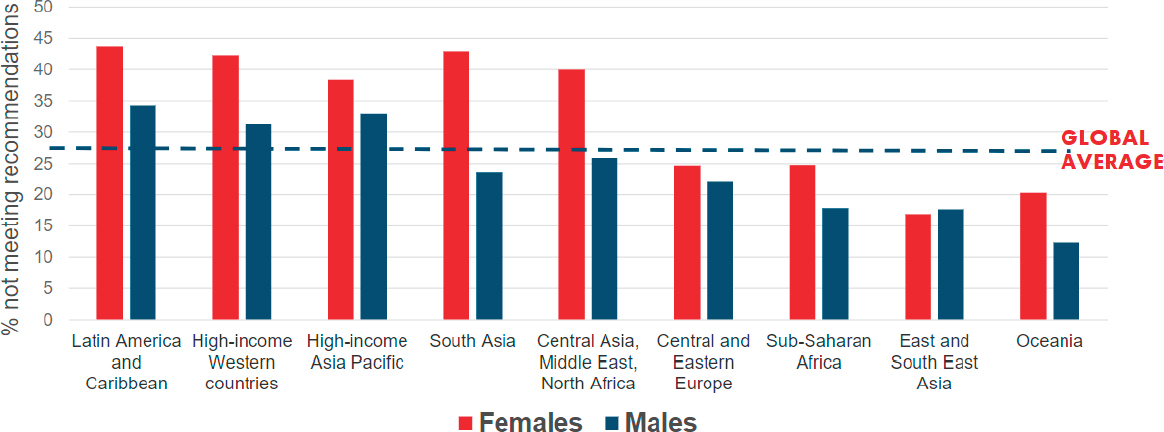
SOURCES: Adapted from Guthold et al., 2018. Presented by Fiona Bull on October 9, 2018. Reprinted with permission from Elsevier.
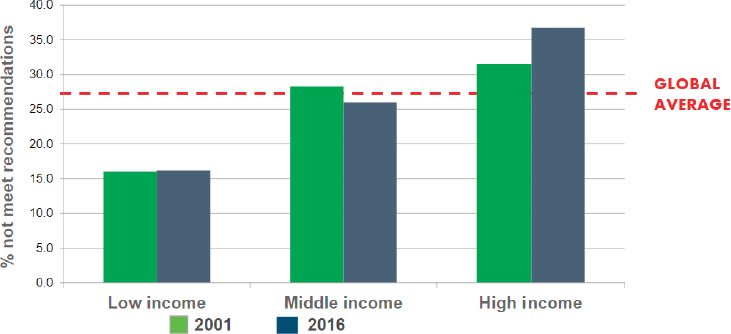
SOURCES: Adapted from Guthold et al., 2018. Presented by Fiona Bull on October 9, 2018. Reprinted with permission from Elsevier.
diverse opportunities to be physically active in their daily lives. She insisted that “one without the other will not be effective.”
Bull then outlined the plan’s four strategic objectives, each supported by policy recommendations:
- Create active societies. Create a paradigm shift in all of society by enhancing knowledge and understanding of, and appreciation for, the multiple benefits of regular physical activity, according to ability and at all ages, by changing social norms and attitudes around physical activity. “We won’t get the environmental changes and transport changes unless we get a shift in priority that walking and cycling is important, that green space is important.”
- Create active environments. Create and maintain environments that promote and safeguard the rights of all people, of all ages, to have equitable access to safe places and spaces, in their cities and communities, in which to engage in regular physical activity, according to ability. In cities and towns, there are differences in the opportunities for safe places for physical activity. Traffic congestion and road safety issues abound in some places where walking and cycling are promoted, and cross-sector partnerships can address some of these issues.
- Create active people. Create and promote access to opportunities and programs, across multiple settings, to help people of all ages
-
and abilities to engage in regular physical activity as individuals, families, and communities.
- Create active systems. Create and strengthen leadership, governance, multisectoral partnerships, workforce capabilities, and advocacy and information systems across sectors to achieve excellence in resource mobilization and implementation of coordinated international, national, and subnational action.
Taken together in a systems approach, Bull argued, these four objectives and their supporting strategies are interconnected and mutually supporting.
Bull went on to report that dissemination of WHO’s plan and its call for multisector commitment and action is occurring through a global launch, regional launches, webinars, national events, and stakeholder forums and conferences. She emphasized the importance of tailored, region-specific tools that combine evidence, rationale, and practice examples to make progress in implementation. She elaborated that countries need resources and “how to” guides for developing or updating their national action plans for physical activity, conducting communication and social marketing campaigns, integrating physical activity into the guidance patients receive from health and social care services, and promoting physical activity in schools. She stressed that countries also need help with capacity building for multisector collaboration, and noted the challenges of bringing government departments together to build a “whole-of-system” approach. She added that monitoring and evaluation are important for holding countries accountable for their progress in implementing their action plans. To that end, she explained, a global monitoring framework will track indicators and metrics with which to gauge success in achieving the WHO plan’s four strategic objectives.
Bull closed with a brief discussion of how physical activity policies can, both directly and indirectly, help achieve the United Nations’ 17 Sustainable Development Goals. She underscored that creating a more active society cannot be achieved by the health sector alone; rather, working together across sectors is imperative, from the national to the local level.
FOOD AND NUTRITION INITIATIVES IN LATIN AMERICA AND THE CARIBBEAN
Fabio da Silva Gomes, regional advisor on nutrition and physical activity for the Americas, Pan American Health Organization/WHO, discussed food and nutrition actions taken by Latin America and the Caribbean to support obesity solutions. He cited as a lesson learned from the region’s experience that it is common to jump from problems to solutions “without digging into the causes.” He emphasized, however, that “the causes
are probably where we can find most of the solutions,” and he invited the workshop participants to think through the causes that introduce and promote obesity and undermine its solutions. One way to learn from the causes and devise solutions, he suggested, is to “think on the opposite side” by identifying approaches to worsen diets and expand obesity.
Pointing out that eating ultraprocessed foods1 is associated with poorer dietary quality and higher obesity prevalence, da Silva Gomes emphasized that “there is no population that eats more ultraprocessed products and eats better.” He displayed a series of graphs showing that in various countries, a greater proportion of energy intake from ultraprocessed products is correlated with a higher intake of sugars and saturated fat and lower intake of fiber (Cediel et al., 2018; Cornwell et al., 2018; Costa Louzada et al., 2015; Julia et al., 2018; Juul and Hemmingsson, 2015; Martinez-Steel et al., 2016; Monteiro et al., 2018). He explained further that the non-nutrient profile of these foods is obesity promoting, with characteristics that encourage faster consumption (such as being easy to chew, crush, and cut), slower and weaker satiety, and less compensation from other energy sources (Fardet, 2016; Fardet et al., 2017, 2018; Gombi-Vaca et al., 2016). He pointed to ecological data indicating that greater annual per capita retail sales of ultraprocessed products (in kilograms) and greater household relative availability of these foods in the Americas and in Europe, respectively, are associated with higher obesity prevalence (Monteiro et al., 2018; PAHO, 2015).
On the other hand, da Silva Gomes continued, “real food” is not a good choice to promote obesity because its lower energy density means that people would need to eat much greater quantities. Such food also takes more time to prepare and eat, he observed, and requires sitting down to eat rather than eating while multitasking. The “Golden Rule,” he stated, is to always prefer natural or minimally processed foods and freshly made dishes and meals over ultraprocessed products (e.g., Ministry of Health of Brazil, 2015). He added that obesity will not be solved solely by promoting real food or by reducing the calories in ultraprocessed products. He argued for regulation of ultraprocessed products, and he again invited participants to take a counterapproach by asking, What are policies and practices that would promote excessive consumption of these foods?
In response to this question, da Silva Gomes stated that a solution to promote obesity is to use advertising and marketing to promote the consumption of ultraprocessed products. He briefly cited evidence demonstrat-
___________________
1 The Pan American Health Organization defines “ultraprocessed foods” as industrial formulations manufactured from substances derived from foods or synthesized from other organic sources. See http://iris.paho.org/xmlui/bitstream/handle/123456789/7699/9789275118641_eng.pdf (accessed December 27, 2018).
ing the positive effect of advertising and marketing on sales (Assmus et al., 1984; Davis and Carpenter, 2009; Kelly et al., 2010; Woodside and Waddle, 1975), including the use of licensed characters and other front-of-package labeling techniques. To illustrate this point, he cited the sensation transfer theory, according to which children rate products as better tasting when popular media characters are on the packaging (Lapierre et al., 2011). He added that ultraprocessed products may be advertised to suggest a particular way of eating. As an example, he pointed to a chocolate product with a name that translates to “nonstop,” remarking that this name suggests consuming the product compulsively. Thus, he asserted, regulation of advertising and marketing is necessary to help solve obesity. He referenced the example of Chile’s front-of-package warning labels that alert consumers to a high amount of saturated fat or added sugars. Products that carry the warning labels cannot use licensed characters, are banned from schools, and are restricted as to how they are advertised (e.g., using toys).
Stressing that the relative affordability of ultraprocessed products contributes to their displacement of “real foods,” da Silva Gomes advocated for correcting the distortion of prices so that real foods are more affordable, and ultraprocessed products are less affordable. He also encouraged clear, straightforward front-of-package labeling, citing data demonstrating that consumers try to minimize cognitive effort in repeat in-store purchasing decisions (Hoyer, 1984).
Lastly, da Silva Gomes described how solutions are undermined in the region by the opposition’s efforts to weaken, delay, or impede them. “Part of the solution,” he asserted, “is exposing and studying these tactics that corporations are using to push back the solutions.” For instance, he said, these entities try to weaken or delay legislation, even resorting to legal tactics. Another tactic, he observed, is to shape the evidence base and frame the debate on diet- and public health–related issues. He shared a review paper comparing scientific studies funded by industry and nonindustry sources, noting that the industry-funded studies were more likely to report favorable conclusions, even if their results were unfavorable (Mandrioli et al., 2016). He cautioned that disclosure of conflict of interest is insufficient, declaring that “it actually can generate a sensation that you are now free to say whatever you want and to favor other results,” and noting that some researchers fail to declare industry ties (e.g., Serodio et al., 2018). Finally, he briefly mentioned a press article describing one large company’s efforts to monitor its reputation in social media (Thomasson, 2012), claiming that one of the company’s purposes is to curb the spread of content that may jeopardize its credibility.
In closing, da Silva Gomes emphasized that it is important not only to expose the problems, but also to show that it is possible to do things differently.
DISCUSSION
During a discussion period following the three presentations summarized above, speakers shared examples of strategies for reducing disparities related to obesity prevalence, dietary intake, and physical activity patterns. Speakers also elaborated on physical activity, discussing its incorporation into health care counseling and its relationship to obesity prevalence.
Barata Cavalcanti urged an attitude of humility in order to “understand that we have quite a few things to learn from low-income countries,” and called for increased sharing of data and information among countries. Bull asserted that disaggregated data, stratified beyond age and gender, could provide unique insights to help in crafting solutions. She described initiatives in Buenos Aires and London to collect suburb-level data on physical activity levels, as well as the environmental factors that affect physical activity. She pointed out that those data have helped these cities move from identifying the problem to developing tailored interventions to target the least active people in various suburbs. It was suggested by da Silva Gomes that school meals programs could improve students’ diet quality and leverage local economies and agrobiodiversity by sourcing 30 percent of foods from local sources. This approach, he added, would favor indigenous populations and other traditional people who produce fruits and vegetables.
Health Care
In response to a participant’s question about whether national health care systems are implementing physical activity counseling, Barata Cavalcanti responded that this intervention had not been highlighted by the MAPPS program’s key informants. “Physical activity was very much at the bottom of the priorities for countries, unfortunately,” she relayed. Bull concurred, saying that “it is a sad state,” and noting that patients do not consistently receive physical activity advice from health care systems or health care providers, despite this being a recommended intervention. “There are examples of countries doing things,” she acknowledged, “but we want to scale the very best practice and tailor it to all countries. It is a major priority for the health system.”
Another participant observed that obesity treatment is often overshadowed by a focus on prevention, and wondered whether this is because treatment is generally not as available. She asked Barata Cavalcanti what types of treatment countries offer and whether the World Obesity Federation recommends specific offerings for different health systems based on their capacities and resources. Barata Cavalcanti replied that treatment is usually a combination of access to surgery and standardized medication, along with nutritional counseling. However, she observed, the advertised
treatments are not always available in reality. As an example, she cited the availability of bariatric surgery in Brazil to individuals who meet prerequisites. But according to MAPPS key informants, she reported, “the waiting list is so long that you would have to wait around 100 years to get your surgery.” She added that the World Obesity Federation will try to clarify what treatments are actually available in practice, and noted that while it is not yet making recommendations to health care systems, any guidance would feature a multidisciplinary team approach.
Bull responded to a participant’s question about whether an association has been observed between physical inactivity and obesity across countries. She pointed to considerable variability in physical activity levels among, within, and across countries by gender. “The differences can reach up to 20 percent,” she added, “which is quite substantial.” She stated further that, although the data on the prevalence of physical inactivity and obesity could be graphed together, it is her belief that a positive association exists. She encouraged the workshop participants to keep in mind that physical activity can be integrated into the day in small ways, and encouraged framing activity as an enjoyable alternative to sedentary behaviors and entertainment. “We have to bring the fun back into it,” she urged.
This page intentionally left blank.














