Proceedings of a Workshop
| IN BRIEF | |
|
August 2019 |
Key Operational Characteristics and Functionalities of a State-of-the-Art Patient Scheduling System
Proceedings of a Workshop—in Brief
On May 16–17, 2019, the National Academies of Sciences, Engineering, and Medicine held a workshop1 focused on the key operational characteristics and functionalities of a state-of-the-art patient scheduling system. The workshop featured invited presentations and discussions on evolving technologies for patient scheduling; essential functions for timely and coordinated scheduling; how to phase in requirements and implementation; the unique aspects of scheduling patients within the U.S. Department of Veterans Affairs (VA) Healthcare System administered by the Veterans Health Administration (VHA); interoperability needs for scheduling interfaces with non-VA health care organizations and in different care settings; user experience, especially for a user population with diverse technology literacy and capabilities; lessons learned from designing and deploying scheduling systems currently used by large health care systems; and potential opportunities for optimizing scheduling technologies and procedures in the VHA.
Kenneth W. Kizer from UC Health (University of California, Davis) opened the workshop by explaining that the goal was to provide input for the VA’s implementation of a state-of-the-art patient scheduling system as part of a larger electronic health record (EHR) implementation initiative. While the workshop was specifically intended to meet the needs of the VA, Kizer pointed out that many large health systems struggle with similar challenges and may also benefit from the information presented at the workshop.
BACKGROUND AND CONTEXT
Steve Lieberman from the VA described the current status of VA health care and its patient scheduling system. The VHA has more than 9 million enrolled veterans and 6.34 million came to the VA for care in 2018. This translated into 58.2 million outpatient appointments across 1,244 medical facilities in fiscal year 2018. Priorities of the Secretary of the VA include improving services for patients and employees, implementing the MISSION Act of 2018,2 implementing new EHR systems, and transforming business systems. The VA uses the motto “One VA” to emphasize that veterans should receive the same quality of treatment and care management at all VHA locations. According to Lieberman, the VHA’s current scheduling system is “archaic” and promotes errors. A new commercial EHR system will be implemented in March 2020, beginning in Seattle and Spokane, Washington.
Mark Murray from Mark Murray & Associates, LLC, provided background on a 2015 Institute of Medicine (IOM) consensus study report3 that focused on timely scheduling within the VHA. The report included findings and recommendations regarding patterns, standards, challenges, and strategies for scheduling timely health care appointments; characterized the variability in patient needs and implications for scheduling protocols; and identified organizations with particular expertise in optimizing patient scheduling. The committee found that delays were ubiquitous and attributable to multiple factors. The report cited barriers to achieving timely health care scheduling and access, including limited evidence for decisions being made, substantial variability of implementation, a lack of systems engineering strategies, a need to reframe the concept of a “visit,” no clear
___________________
1 The workshop agenda and presentations are available at http://www.nationalacademies.org/hmd/Activities/HealthServices/KeyOperationalCharacteristicsandFunctionalitiesStateArtPatientSchedulingSystem/2019-MAY-16.aspx (accessed June 21, 2019).
2 Public Law Number 115-182.
3 Institute of Medicine. 2015. Transforming health care scheduling and access: Getting to now. Washington, DC: The National Academies Press. https://doi.org/10.17226/20220.
![]()
implementation to aid with continuity, no validated standards, and a paucity of leadership. The report emphasized patient- and family-centered care4 and a systems approach to balancing clinician supply with patient demand via data analysis, and integration of technologies to optimize system performance and outcomes for patients, clinicians, and the health care system.
Carolyn Clancy from the VA described specific scheduling needs for veterans’ health care. She said the goal for the new scheduling system is to address gaps within the current system; increase automation to reduce errors and save time; and allow patients to be seen either face to face, virtually, or by community care providers; all within one coordinated system. It is important for the system to accommodate VA-specific issues and requirements, including the service-connected disability status of veterans’ community care referrals; interoperability across VA medical centers and community-based outpatient clinics, U.S. Department of Defense (DoD) health care facilities, and community health care organizations; prioritization of urgent clinical needs; resource-based scheduling that leverages enterprise capacity; and scheduling for VA-specific programs such as spinal cord injury, residential treatment, telehealth, and home-based care.
Chad Ruoff from Cerner Government Services, the vendor for the VA’s new scheduling system, highlighted key features of the planned new system, including that it is resource-based; coordinates clinicians’ time, types of appointments, and resources; spans both the VA and DoD; integrates online portals and kiosks; and is interoperable and integrated with the VA’s new full EHR and population health platforms.
Kizer said that virtual visits are likely to become more common in the future, and there was a discussion about how to incorporate telehealth into the VA’s health care system. Don Goldmann of the Institute for Healthcare Improvement (IHI), Lisa Lehmann of the VA New England Healthcare System, and Leonie Heyworth of the VA’s Office of Connected Care (which oversees telehealth), pointed out challenges with telehealth, including that many rural veterans do not have access to the necessary technology. Also, telehealth cannot provide social support and connectedness to other veterans that VA facilities provide. Heyworth described one VA program that is addressing these challenges by establishing telehealth access sites at both Veterans of Foreign Wars and American Legion locations so that veterans can receive telehealth services in their home communities.
Another challenge raised by participants, including Lehmann, Kizer, and Mia Powers-Higgins from the VA Office of Veterans Access to Care (OVAC), is the increasing complexity of classifications for appointment types from a human resource perspective. This makes schedulers’ jobs more difficult and can exacerbate staff turnover, which is already high due to limited career pathways for medical support assistants (MSAs) who are responsible for scheduling at the VA.
EXPERIENCES OF OTHER INSTITUTIONS IN DEVELOPING AND DEPLOYING PATIENT SCHEDULING SYSTEMS
Eva Lee from the Georgia Institute of Technology summarized the ways technology can power a patient scheduling system and gave results from a review of commercial patient scheduling software products. She said the priorities for a system are to automate appointment processes; maximize the number of patient appointments; and minimize wait times, no-shows, and cancellations. Lee reviewed 18 commercial patient scheduling systems including cloud-based, stand-alone, and integrated solutions. She identified two key challenges: (1) data security and (2) the need for information from providers in real time regarding what is actually available for patients (e.g., staff checking to see if a bed is available). She said all scheduling systems ultimately rely on people to manage and use them and to address issues the system cannot.
Goldmann suggested that the VA use the “idealized design” approach in implementing its new scheduling system. This involves bringing together patients, clinicians, and other stakeholders to develop an idealized pathway that starts when a treatment need is identified and proceeds through appointment scheduling and follow-up. He also suggested using a systems-oriented approach that focuses on the patient holistically, measures patient safety and overall health rather than just the time to an appointment, utilizes smartphones and telehealth, incorporates knowledge from behavioral economics, and uses data analytics to manage supply and demand. He also challenged workshop participants to think beyond a traditional “scheduling system” in designing ways to connect patients and health care providers.
Chunhua Weng from Columbia University presented the Integrated Model for Patient Care and Clinical Trials (IMPACT) system that her institution uses for scheduling patient visits for clinical trials, which also could be relevant in a hospital care setting. IMPACT is a Web-based application operated by a coordinator that uses researcher and resource calendars, protocol constraints, process rules, and patient availability to identify appointments. Since launching in 2014, IMPACT has scheduled more than 15,000 patients for 154 clinical studies and has improved workflow by providing information on resource availability in real time; allowing for direct resource requests; reducing duplicate records; and more easily tracking patient scheduling, cancellations, and check-ins.
___________________
4 Per the IOM report, patient and family-centered care is designed, with patient involvement, to ensure timely, convenient, well-coordinated engagement of a person’s health and health care needs, preferences, and values; it includes explicit and partnered determination of patient goals and care options; and it requires ongoing assessment of the care match with patient goals.
Michele Samorani from Santa Clara University spoke about strategies for mitigating no-shows by using machine learning to optimize overbooking (scheduling more patients than slots available in case some patients do not show up). Overbooking can help reduce clinician idle time, but may sometimes result in long waits for patients or require clinicians to work overtime. Machine learning can be used to predict whether each patient will show up and optimally overbook patients based on their expected no-show rate, Samorani said. She emphasized the importance of setting the appropriate cost of patient waiting time, ensuring integration with existing scheduling systems, overcoming resistance to change, and effectively communicating with different patients depending on the probability of a no-show.
William Hu from the Emory University School of Medicine described his experience in designing and implementing a novel machine learning–based scheduling system. He said the goal was to use previsit data to better assess case complexity and to ensure appropriate utilization and reduce clinician burnout. Previously, patients were required to complete and return a written questionnaire before their appointment could be scheduled, and it took up to 2 months for scheduling to take place. Under the revised process, patients complete a checklist online and patient visit complexity is assessed using machine learning. The complexity algorithm was developed with clinician input and is intended to model the dynamic between particular types of patients and care providers. Clinicians also retrospectively document appointment length to refine the algorithm. As a result of the revised process, schedules that require the clinician to see multiple highly complex patients in a row have been eliminated, clinician time spent waiting for the next patient has been reduced, and more low-complexity patients can be seen in a single day, reducing clinician overtime and burnout, patient backlogs, and wait times. Potential benefits to the health system include decreased time spent manually categorizing patients, increased ease of information flow, and a potential increase in revenue with an increased number of patients seen.
Seth Carlson from the National Institutes of Health (NIH), spoke about the experience in implementing the NIH Clinical Center’s Enterprise Scheduling System. The NIH Clinical Center has more than 100 research teams and 1,500 active research protocols, resulting in more than 100,000 outpatient appointments for 24,000 patients seen per year. The goal of the Enterprise Scheduling System was to realize the benefits of real-time access to appointment information for both clinical staff and patients. To achieve this, the Clinical Center developed custom tools to automate and streamline the process for requesting and scheduling appointments with standard workflows. Based on this experience, Carlson suggested obtaining leadership and stakeholder support early in the process; ensuring sustainability; considering both electronic and non-electronic solutions; partnering with the EHR vendor to build customizations into the scheduling system from the start; and devoting enough attention and resources to user training, communication with stakeholders, and a system rollout strategy.
Kizer asked speakers for suggestions on how to execute and implement scheduling tools within a large, complex system like the VA. Lee, Carlson, and Samorani suggested rolling out the new system in stages. Carlson suggested choosing at least one of the more complex and challenging areas for a pilot test. Hu emphasized building flexibility into the scheduling tools and ensuring adequate time for training.
PERSPECTIVES AND EXPERIENCES OF PATIENTS, CLINICIANS, AND SCHEDULERS
Susan Kirsh from the VA introduced four clinical scenarios, with the goal of illustrating the perspectives of patients, clinicians, and schedulers in primary and specialty care within the VA. Each scenario was followed by a panel discussion about the relevant characteristics and attributes of the scheduling system currently in place and its ideal future state. Panelists included Adrian Atizado, a veteran and patient advocate from Disabled American Veterans; Powers-Higgins, a scheduler from OVAC; Heyworth, a primary care physician and VA clinical lead in telehealth; Desiree Hill, a clinical profile manager at the VA; Clifford Smith, a psychologist in specialty care at the VA Office of Mental Health Operations and Mental Health Services; Lisa Arfons, an oncologist in specialty care at OVAC; David Au, a practicing pulmonologist and health services investigator at the Center of Innovation for Veteran-Centered and Value-Driven Care, VA Puget Sound Health Care System; and M. Christopher Saslo, Biloxi VA Medical Center, nurse executive and acting deputy for Dr. Teresa Boyd, Assistant Deputy Under Secretary for Health for Clinical Operations.
Atizado, who provided opening remarks on the patient and family perspective, said that one of the biggest challenges in reforming the VA health care system is ensuring quality and continuity of care when sending patients out to the private sector, which he described as fragmented and disconnected, with a different approach to patient care than that of the VA. There are also some important differences between the veteran population and the broader U.S. population. For example, the VA patient population has a higher prevalence of mental health conditions and homelessness, lower incomes, and more clinically complex conditions than the general population, on average. He noted that, like the general U.S. population, the veteran population includes various age groups and their preferences and predilections for using digital tools vary a great deal. He pointed to the VA Survey of Veteran Enrollees’ Health and Use of Health Care, which shows that the older a veteran is, the less inclined that veteran is to use technology in health care. He added that a lot of older veterans have complicated health care needs and face more barriers to care than the average patient in the private sector. Though technology is becoming more prevalent in health care (as can
be seen in the case scenarios), he emphasized the importance to the “silent generation” and to “baby boomers” of showing up in person and not relying too heavily on technology for health care delivery.
The clinical scenarios were as follows:
- A 64-year-old male veteran with a smoking history who underwent lung cancer screening had a video follow-up appointment to discuss the results, followed by a pulmonary consult with additional same-day diagnostic testing pre-appointment, and a warm handoff to the thoracic surgery team post-appointment. He used the VEText appointment reminder system to reschedule an appointment.
- A 54-year-old male veteran hospitalized for cardiac bypass surgery had a video discharge appointment and received a referral to community care for cardiac rehabilitation. Follow-up care was provided through telehealth and home visits with remote monitoring via the Annie app to provide daily weight and blood pressure measurements taken with devices loaned by the VA.
- A 32-year-old male veteran with type 1 diabetes and who was traveling the country asked his primary care provider (PCP) to place a Traveling Veteran Coordinator (TVC) request so that he could be seen at a VA health center near his destination. He requested communication via smartphone.
- A 32-year-old male veteran experiencing mental health challenges was given a warm handoff by his PCP to colocated Primary Care-Mental Health Integration (PCMHI), which identified a chronic mental health history. He was then referred to a psychotherapist and offered 12 weekly telehealth appointments with a psychiatrist.
Box 1 describes current characteristics of the VA’s scheduling system and suggestions from individual participants during the discussion of the four clinical scenarios.
INTEROPERABILITY AND INTEGRATION
Joe Kimura from Atrius Health moderated a session that featured presentations on functionalities, challenges, and care coordination strategies in commercial scheduling systems. Kimura provided an overview of a 2018 National Academy of Medicine special publication5 focused on the procurement of interoperable and integrated health information technology (IT) systems from the perspective of both the payer and the care provider. Kimura highlighted two concepts from the report: (1) four levels of interoperability of increasing complexity and integration and (2) three tiers of interoperability ranging from macro to micro. The first concept is the idea of four different levels of interoperability, which include technical, syntactic, semantic, and organizational interoperability. The second concept is about the setting, or different tiers of interoperability. The three tiers of interoperability are macro interoperability between different organizations; miso interoperability within an organization; and micro interoperability at the device, or point-of-care, level. Expanding on these different levels and tiers, he highlighted that interoperability is not just one single, colossal term, but a lot of different things.
Cris Ross from the Mayo Clinic said his institution works to provide service that is predictable, repeatable, affordable, and accessible to patients; to maintain joy in practice for clinicians so they can best help patients; and to achieve financial goals for the health care system. Algorithms are used to achieve two overarching scheduling principles of optimizing patient itinerary completion and managing clinician capacity. He said their principal goal is to put the needs of the patient first, so they strive to have every patient complete diagnostic tests, receive a diagnosis, and obtain treatment in 5–7 days using a flexible itinerary that allows for adding an additional test or appointment as needed. Decision trees are used by schedulers to identify the right appointments for each patient. To manage clinician capacity, the Mayo Clinic uses a “staff on floor” metric specifying the service each clinician provides on a given day, calendars with staff schedules and appointment types, and load/capacity balancing between and within specialties. Ross noted that future challenges include optimizing clinician time utilization, managing increasingly sophisticated and complex integration with other health care systems, and providing open access and self-scheduling.
Isaac Vetter from Epic described what he considers to be the three properties of a state-of-the-art scheduling system: (1) scheduling and clinical systems that are tightly integrated from the perspectives of schedulers, clinicians, and veterans; (2) multimodal communication systems that allow patients to send and receive messages using their preferred method; and (3) interoperability, both between scheduling applications and across the enterprise, using HL7-Fast Healthcare Interoperability Resources (FHIR) technology, a modern interoperability standard used by many health care systems. The Argonaut project of HL7 International is focused on advancing interoperability using application programming interfaces (APIs) by creating, refining, implementing, testing, and releasing FHIR profiles. In 2017, the project released a FHIR scheduling implementation guide, which allows for cross-enterprise scheduling using FHIR. Ross added that the Centers for Medicare & Medicaid Services (CMS) has proposed requiring HL7-FHIR interoperability standards.6 He suggested that this standard will be “disruptive” and will make health care more efficient, but that changes to business processes are needed to facilitate use that is patient centric and health focused. Kimura said that the reduction in information silos that may result from increased integration and interoperability provides additional opportunities for schedulers and clinical staff to improve patient access.
Sagnik Bhattacharya from PatientPing described how a patient scheduling system could help to accelerate care coordination, noting that failures in care coordination often occur during transitions from acute to outpatient settings and from primary to specialty care. PatientPing is a platform that leverages existing widely deployed technology, such as HL7 admission, discharge, and transfer notifications, to improve care transitions by connecting clinicians across parts of the health care system. Participating clinicians and health care systems receive a “ping” in real time whenever their patients receive care. For example, when a patient arrives in the emergency department (ED), a notification alerts a patient coordinator so he or she can coordinate care in real time. He said that an event like an ED visit or a hospital discharge should serve as an automated trigger for proactively scheduling an appointment because transitional care gaps are a big driver of poor-quality care. Bhattacharya provided several examples of how PatientPing has improved outcomes, including maternal mortality prevention, reductions in hospital readmissions, improved specialty referral handoffs, and reductions in no-shows for dialysis or chemotherapy treatments.
Robert Cothren from the California Association of Health Information Exchanges (CAHIE) also emphasized that sophisticated scheduling technology does not necessarily lead to service coordination. He said that the 21st Century Cures Act has the potential to inform activity on interoperability. The law defines interoperability as “complete . . . secure . . . access, exchange, and use of all electronically accessible health information . . . without special effort on the part of the user . . . in a way in which . . . HIT developers, exchanges, networks, and providers . . . do not discourage . . . or restrict authorized access, . . . or impede
___________________
5 Pronovost, P., M.M.E. Johns, S. Palmer, R.C.Bono, D.B. Fridsma, A.Gettinger, J.Goldman, W.Johnson, M.Karney, C.Samitt, R.D. Sriram, A.Zenooz, and Y.C. Wang, Editors. 2018. Procuring interoperability: Achieving high-quality, connected, and person-centered care. Washington, DC: National Academy of Medicine.
6 Centers for Medicare & Medicaid Services. 2019. Proposed Rule: Medicare and Medicaid Programs; Patient Protection and Affordable Care Act; Interoperability and Patient Access for Medicare Advantage Organization and Medicaid Managed Care Plans, State Medicaid Agencies, CHIP Agencies and CHIP Managed Care Entities, Issuers of Qualified Health Plans in the Federally Facilitated Exchanges and Health Care Providers. 45 CFR Part 156. RIN 0938-AT79. Federal Register 84(42): 7610–7680.
innovations and advancements. . . .”7 In California, regional HIEs serve as trusted forums for convening stakeholders in order to develop consensus approaches to solving health care problems through interoperability and data sharing among participants, including public health departments, payers, patients, and clinicians. He said HIEs provide value to veterans in allowing different specialties, care settings, and organizations to access, exchange, and use data; expanding data types; and translating between disparate standards and core capabilities and functions. However, he noted that data exchanges are only useful if they support the desired workflow. Cothren also noted that laws and regulations address data security and privacy issues in the context of health IT. In California, most health care systems now require patients to “opt out” rather than “opt in” to the exchange and use of their data.
PHASING IMPLEMENTATION OF KEY FUNCTIONALITIES
Rachel Weber from HealthcareIE LLC illustrated three primary goals of scheduling care for veterans: (1) access to, (2) coordination of, and (3) continuity of care (see Figure 1). She described foundational elements of a patient scheduling system in primary and specialty care, stating that the best scheduling system matches a patient’s need for an appointment to the right care provider with minimal delay. For primary care, she said a scheduling system should be able to search for the next available appointment with the patient’s PCP across all scheduling grids, with only one queue for each clinician, and it should not schedule new patients with a clinician whose panel is closed. For specialty care, Weber suggested that each clinician have their own caseload and queue for return appointments, with a separate queue for distributing new patients to all available specialists. Caseload data can be used to optimize the allocation of clinician time between new and return patients. For referrals from primary to specialty care, Weber suggested building service agreements into the scheduling workflow, through which a specialist determines how to properly prepare patients for their first visit and the PCP agrees to meet the requirements. These can be in the form of a checklist that the scheduler can use to sequence tests required for a patient with a specific condition in advance of a specialist appointment. Specialist return visits may be minimized when patients are fully prepared for their initial appointment, she said. Weber said it is important to ensure that the implementation of scheduling rules can allow flexibility when needed.
Eva Lee from the Georgia Institute of Technology, said a limitation of the current scheduling software is that it frequently
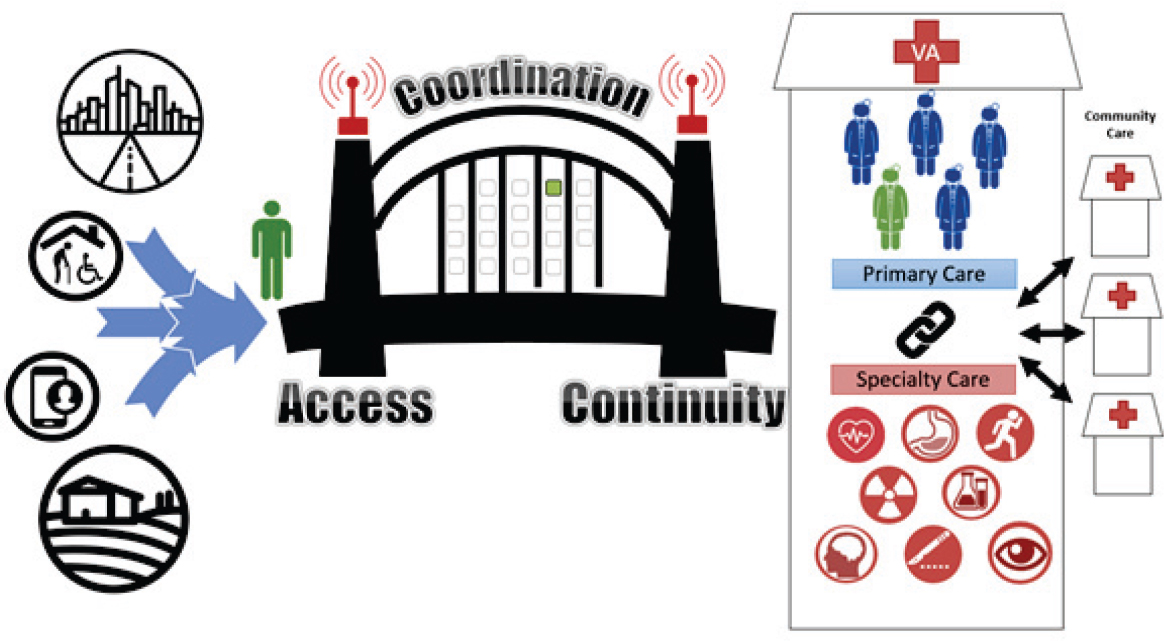
SOURCE: Presented by Rachel Weber, May 16, 2019.
___________________
7 21st Century Cures Act. Public Law 114-255. Title IV, Sec. 4003.
relies on humans rather than algorithms. The patient scheduling process might be more optimally powered by methods such as mathematical modeling, discrete event simulation, and machine learning. A machine learning framework could be used to classify patients in multiple ways, with a group for whom judgment is reserved and the patient is scheduled manually. Such a system could predict a type of appointment for a patient, based on both disease-related and resource-oriented needs. As an example demonstrating the clinical benefits of machine learning, Lee described an ED that experienced a 30 percent increase in workflow efficiency with reduced wait times and an increase in the number of trauma patients seen.
Desiree Hill from the VA shared her perspective as a scheduler using the current scheduling system and described gaps that need to be addressed. She suggested that an updated scheduling system should help schedulers do their jobs without errors, be veteran-centric, utilize a resource-based model, improve clinician and scheduler productivity, integrate community care, and have one place for schedulers to receive and respond to patient requests. Hill suggested that both schedulers and veterans be involved in testing during a pilot phase and that a help desk should be established to address problems. She also emphasized the need for communication among schedulers and other stakeholders about upcoming changes. A specific challenge for schedulers making an initial PCP appointment is that they can see PCP panel availability but not the PCP’s next available appointment or how many new versus existing patients are scheduled for that day. Clinicians may also have multiple scheduling queues. Hill also suggested that the VA could do a better job of incorporating the preferences of veterans, a point on which Heyworth elaborated by noting that clinician information and metrics could be better utilized in matching patients to care providers.
Sean Bina from Epic described the potential for EHR features to meet scheduling system requirements and address gaps. He suggested implementing a standard system nationally with system updates implemented on an ongoing basis, noting that VA-specific and site-specific customizations do not allow the VA to take advantage of work done by others and that these also have ongoing costs. He also suggested that the VA allow self-scheduling, noting that patients who schedule their own appointments are less likely to miss an appointment. Bina also suggested using symptom-based scheduling, a point with which Heyworth agreed.
Jane Fogg and Kellianne Thayer from Atrius Health spoke about their health system’s recent scheduling optimization project, which is aimed at maximizing staff efficiency and increasing access and outcomes for patients. Fogg explained that the process used a data-driven approach with clinicians as the primary stakeholders. System changes included standardizing schedule templates based on service line standards, integrating scheduling expectations of individual clinicians, reducing the burden from maintaining scheduling templates, and leveraging existing tools within their EHR system. Thayer explained that the health system implemented the changes by initially focusing on standardization and the operational changes needed to improve workflow. A steering committee that included end users provided governance, but she said a shortcoming of their approach was that patients were not represented on the steering committee. Data analysis was used to inform the choice of template options for session structures and appointment types. When the new system was piloted at one site, there was ongoing communication with stakeholders, one-on-one meetings with clinicians to identify their individual needs and modify templates as needed, and on-site support. Additional features of the new system include automatic notifications when appointments become available for wait-listed patients, which has resulted in the scheduling of more than 2,000 appointments without human involvement, and a 37 percent increase in online self-scheduling, with a lower no-show rate. According to Thayer, key elements of success include communication about the reasons for change, incorporating feedback from stakeholders throughout the process, evaluating impacts at pilot sites, and providing multipronged training support. Fogg also emphasized that people are still needed, as there will always be issues that technology cannot address.
Mike Davies from the VA highlighted the importance of considering questions such as how far in advance to open a schedule, when the ideal time is to schedule a future appointment, whether to allow self-scheduling, how to manage multiple scheduling queues, and what instructions schedulers should provide to patients on preparing for their appointment.
EMERGING TECHNOLOGIES AND PRACTICES
John Halamka from the Harvard Medical School provided an analogy for scheduling, noting that shipping containers were invented to increase efficiency in loading ships; however, they were only helpful after there were ships to fit them and cranes to lift them. This is like interoperability in health care, which is technically feasible, but there has been a deficiency in corresponding changes in skillsets, infrastructure, and workflow. Halamka provided highlights from the past 30 years of health IT standards. The HL7 version 2 system, invented in 1989, was an important advance but proved too hard to extend. The subsequent adoption of eXtensible Markup Language (XML) addressed the problem by providing the same information in a more modern format. However, because it was easy to extend and add options to, vendors implemented the HL7 standard in different ways. In 2014, the federal government wanted to ensure that standards would lead to better interoperability and it commissioned a JASON Report Task Force, which built on a 2013 JASON report on the integration of health data.8 The task force interviewed
___________________
8 JASON. A Robust Health Data Infrastructure. AHRQ Publication No. 14-0041-EF April 2014.
technology companies to learn how they share data using an API. To implement the task force recommendations,9 HL7 International’s Argonaut Project began to create a straightforward set of resources in JavaScript format that are easy to use and in the same format as non–health care industries. This became the FHIR implementation guide, which now contains about 150 resources, including one on scheduling.
Several speakers described technical products or services relevant to patient scheduling. Graham Gardner from Kyruus explained that the company’s goal is to route patients in order to align with clinicians’ strengths, in real time and at scale. Its system was developed using the travel industry as a model, with a focus on solving the supply–demand mismatch that exists in health care, with new and community care providers having up to 20–40 percent of the slots open each week. Kyruus is a tool for health care systems that allows the user to search for clinicians online across EHRs using criteria such as gender, subspecialty, and location. The system is based on an aggregation of data from multiple sources, enriched with a library of 20,000 search terms that include popular misspellings, and developed into an app that allows patients and schedulers to route patients to available clinicians, he said.
Adeel Yang described Medumo as focused on patient navigation, with the goal of ensuring that patients get to their appointments on time and fully prepared. Medumo has three pillars; it is (1) patient centric, providing multichannel and multilingual communication options that may include caregivers to meet patients where they are; (2) clinician centric, improving workflow and supporting rather than replacing staff; and (3) data centric, using data to drive behavioral changes for patients and to support clinicians. Yang pointed out that the majority of Americans own a cell phone—95 percent as of 2018—includ-ing 77 percent with a smartphone (among Americans age 65 or older, 85 percent own cell phones including 46 percent with smartphones, and 67 percent use the Internet). He also highlighted a shift in communication between patients and clinicians from primarily written and oral communication in the past to digital portals, text messaging, and apps in the present to automated communication using artificial intelligence (AI) in the future. He stated that machine learning informed by psychology can drive behavioral changes and suggested that communication strategies should be comprehensive, allow stakeholders to communicate with each other, and provide thoughtful automation for clinicians. Yang provided a few examples of how Medumo has been used, such as assessing care acuity before a procedure to improve resource utilization, and reducing appointment cancellations using timed, targeted reminder messages consistent with patient preferences.
Spencer Cross from Change Healthcare spoke about driving patient access through coordinated digital experiences. The goal of Change Healthcare is to use technology to turn data from health care workflow systems into meaningful patient communication that improves the patient experience. The system coordinates across multiple technologies and systems to provide notifications, communication, and services to interact with patients in a more streamlined, continuous fashion across the health care system. For example, Change Healthcare has created a “Yelp-like” consumer-driven directory that allows patients to search for health care providers using a matching algorithm. In a communication campaign, it worked with a radiology practice to identify patients needing follow-up to encourage them to schedule future appointments.
Oliver Kharraz said that Zocdoc is a scheduling and inventory management tool that enables patients to self-schedule appointments. It serves 6 million patients per month to help them access open appointment slots, including last-minute appointments due to cancellations and no-shows. Patient search results show clinicians with available appointments that meet their search terms and accept their insurance. The system started with a small vocabulary but has “learned” based on the search terms entered, he said, adding that Zocdoc has a singular focus on the patient experience and uses the percent of patients who would recommend it as its primary metric. Kharraz emphasized the importance of designing a system for the patient, while also delivering value for the clinician and health care system.
Halamka asked the panelists for suggestions to create a good care experience in cases in which veterans might be seen across multiple locations. Yang suggested obtaining patient communication preferences and automatically applying them across the VA system. Gardner suggested creating a single care provider inventory with options to sort and filter. Halamka noted that in emergency situations, it would be ideal for a health care provider to be able to search for patients’ medical records across all EHR systems.
Halamka also asked panelists if they thought symptom-based scheduling using voice-activated systems will be coming soon. Yang noted that several companies are already working on such a tool. Cross said that the APIs exist, but that health care and scheduling system data still need to be integrated into a format that voice-activated technology can use. Gardner noted that the use of sophisticated AI technology for automated digital scheduling opens space for people who need human assistance, highlighting that there will still be a need for people to perform some functions.
Regarding data governance and standards, Halamka noted that Carequality provides a common interoperability framework that enables exchange among health data sharing networks, and that CommonWell Health Alliance provides infrastructure in the form of a master index and locator guide for health data.
___________________
9 JASON Report Task Force. Final Report. October 15, 2014. https://www.healthit.gov/sites/default/files/facas/Joint_HIT_JTF%20Final%20Report%20v2_2014-10-15.pdf (accessed June 21, 2019).
WRAP-UP DISCUSSION
The final session of the workshop featured reflections on participants’ key takeaways from the meeting. Suggestions made by individual participants during the workshop are highlighted in Box 2. ◆◆◆
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Melissa Maitin-Shepard; Katiria Ortiz; and Sharyl Nass as a factual summary of what occurred at the workshop. The statements made are those of the rapporteurs or individual workshop participants and do not necessarily represent the views of all workshop participants; the planning committee; or the National Academies of Sciences, Engineering, and Medicine.
*The National Academies of Sciences, Engineering, and Medicine’s planning committees are solely responsible for organizing the workshop, identifying topics, and choosing speakers. The responsibility for the published Proceedings of a Workshop—in Brief rests with the rapporteurs and the institution. The planning committee comprises Kenneth W. Kizer,Chair, University of California, Davis, Schools of Medicine and Nursing; John Halamka, Harvard Medical School; Joe Kimura, Atrius Health; Amanda Lazar, University of Maryland; Eva K. Lee, Georgia Institute of Technology; Mark Murray, Mark Murray & Associates, LLC; and Rachel Weber, HealthcareIE LLC.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Adrian Atizado, Disabled American Veterans; Suzanne R. Bakken, Columbia University; James C. Benneyan, Northeastern University; and Joe Kimura, Atrius Health. Lauren Shern, National Academies of Sciences, Engineering, and Medicine, served as the review coordinator.
SPONSORS: This workshop was sponsored by the U.S. Department of Veterans Affairs.
For additional information about the workshop, visit http://nationalacademies.org/hmd/Activities/HealthServices/KeyOperationalCharacteristicsandFunctionalitiesStateArtPatientSchedulingSystem/2019-MAY-16.aspx.
STAFF: Sharyl Nass, Carol Sandoval, and Annalee Gonzales, Board on Health Care Services, Health and Medicine Division; Jon Eisenberg and Katiria Ortiz, Computer Science and Telecommunications Board, Division on Engineering and Physical Sciences, National Academies of Sciences, Engineering, and Medicine.
Suggested Citation: National Academies of Sciences, Engineering, and Medicine. 2019. Key operational characteristics and functionalities of a state-of-the-art patient scheduling system: Proceedings of a workshop—in brief. Washington, DC: The National Academies Press. https:doi.org/10.17226/25556.
Health and Medicine Division

Copyright 2019 by the National Academy of Sciences. All rights reserved.










