8
Dental Schools, the Profession, and the Public
Chapter 7 considers dental schools in their universities and academic health centers. This chapter shifts the view to the profession and the public. It focuses on two issues—institutional accreditation and professional licensure. The next chapter considers a third related topic of public importance, the supply of dental personnel and services.
Accreditation and licensure involve, respectively, private standard-setting activities and government regulations whose primary explicit purpose is to protect the public from poorly trained, incompetent, or unethical dental practitioners. Individually and together, these two processes account for many of the tensions between dental schools and the profession. When dental school deans were asked what recommendations from this committee would have greatest positive impact, changes related to accreditation and licensure headed the list.
Accreditation and licensure are components of a broad social strategy to ensure the quality of dental care. In examining the patient care mission of dental schools, Chapter 6 discussed basic concepts of quality assurance and improvement. Other quality-related mechanisms, for example, risk management strategies required by malpractice insurers, are not considered in this report, nor are a variety of other regulations and quasi-regulatory practices such as those intended to control communicable diseases, protect workers, and inform consumers. These regulations may involve substantial costs for practitioners and schools.
Chapter 2 briefly reviews the historical context of accreditation and licensure, highlighting the controversies that have marked their birth and development. This chapter examines current issues and debates. The background paper by Guarino provides additional information.
Accreditation
The accreditation of U.S. dental educational programs is a private function with a public purpose. As expressed in the mission statement adopted by the Commission on Dental Accreditation in 1989, the purpose of accreditation is "to ensure the quality of dental and dental-related education" (CDA, 1993a). If effective, accreditation
- protects the public welfare by ensuring that dental school graduates are appropriately prepared to provide oral health services;
- ensures students that their educational program meets basic educational standards;
- guards public funds from use in support of inferior programs; and
- assists educational programs in achieving—and improving on—minimum standards.
In theory, accreditation is voluntary. In practice, it has become a virtual requirement for schools because graduation from an accredited school is a prerequisite for dental licensure in most states, although some states have special provisions for licensing those who have graduated from foreign dental schools. The debates about accreditation focus on whether it is effective, whether its benefits outweigh its costs, how its ratio of benefits to costs can be improved, whether it hinders innovation and flexibility, and whether it is unduly dominated by narrow vested interests. These debates take place in the context of larger debates about the proper role of accreditation and the dozens of organizations that accredit various educational institutions and other service organizations such as hospitals and home care agencies (CDA, 1993b; Wolff, 1993; Weiss, 1994). The typical university faces dozens of accrediting organizations. Not only do these accreditation processes impose significant costs, but they may be viewed as a form of self-interested lobbying on behalf of the disciplines in question. Beyond the educational arena, questions about the independence of credentialing organizations and their effectiveness in ensuring quality are a staple of the debate over procedures for ensuring the quality of care in hospitals and other health care organizations [IOM, 1990e).
Structure and Process
Organizations
A single organization, the Commission on Dental Accreditation (CDA), is responsible for accrediting dental education programs. Through five committees, it accredits programs in general dentistry education, dental specialty education, and allied dental education. The latter category includes dental hygiene, dental assisting, and dental laboratory technology programs. In addition to predoctoral programs in general dentistry, the CDA examines two advanced education in general dentistry programs and advanced programs in the eight recognized dental specialties. In total, the CDA accredits approximately 1,300 education programs (Table 8.1).
Although autonomous, the commission is an agency of the American Dental Association (ADA), which houses, staffs, and funds it. Its membership breaks down as follows: four members each from the ADA, the American Association of Dental Examiners (AADE), and the American Association of Dental Schools (AADS); two members from the general public; two from recognized dental specialty organizations (as a group); and one member each from the dental student body, the American Dental Hygienists' Association, the American Dental Assistants' Association, and the National Association of Dental Laboratories.
The Commission on Dental Accreditation formulates and revises accreditation standards, establishes procedures for applying those standards, and determines accreditation status for individual pro-
TABLE 8.1
Number of Programs Accredited by Commission on Dental Accreditation
|
No. of Accredited Programs: |
|
|
54 |
Predoctoral dental programs |
|
421 |
Specialty programsa |
|
325 |
General practice residency/advanced general dentistry programs |
|
233 |
Dental assisting programs |
|
212 |
Dental hygiene programsa |
|
41 |
Dental laboratory technology programs |
|
1,286 |
Total number of programs accredited as of January 1994 |
|
a Includes accreditation eligible programs. SOURCE: CDA, 1994a-c. |
|
grams. It appoints consultants to assist with these activities and maintains a formal process for the appeal of its decisions. Accreditation decisions are based on periodic on-site reviews. and regularly collected quantitative data that are intended to assess both the educational process and its outcomes (graduate dentists).
The commission and its accrediting programs are recognized by two national organizations, the U.S. Department of Education (USDOE), a government agency, and the Commission on Recognition of Postsecondary Accreditation (CORPA), a newly established private group.
The USDOE recognizes accrediting organizations that meet specified criteria that reflect the interest of Congress in ensuring the quality of educational programs supported by federal funds. One of the government's major concerns has been high default rates on student loans, particularly in some technical and vocational areas.
CORPA was created after its predecessor organization, the Commission of Postsecondary Accreditation, dissolved in 1993. The debate surrounding this event highlighted questions about whether accreditation is a "reliable indicator of an institution's quality or accountability" (Wolff, 1993, p. B1). The new organization, CORPA, has a seven-member governing body. A Committee on Recognition will review accrediting organizations before granting recognition. CORPA has adopted many procedures of its predecessor organization including its provisions for recognition, calendar of recognition, and required interim reports and deferrals. The Commission on Dental Accreditation has accepted the invitation of CORPA to become a member.
Process
Dental accreditation is unlike medical accreditation in two major respects. First, the Commission on Dental Accreditation differs from the Liaison Committee on Medical Education, the comparable body for medical education, in that it accredits postgraduate programs. In medicine, the Accreditation Council for Graduate Medical Education accredits residency training programs using 23 Residency Review Committees for each of the recognized medical specialties.
Second, CDA also accredits programs in dental hygiene, dental assisting, and dental laboratory technology. Programs for some other allied health professions, for example, occupational therapy and physical therapy, are accredited by independent bodies. Until July 1994, the Committee on Allied Health Education and Ac-
creditation, an umbrella organization, accredited programs in 25 fields (e.g., medical laboratory technology and medical record administration). A successor organization, the Commission for the Accreditation of Allied Health Education Programs, is expected to include 40 organizations and 17 of its predecessor's accreditation review committees.
The process of dental accreditation is complex and time consuming, designed to involve all major parties. In overview, the major steps for the accreditation of D.D.S. or D.M.D. programs include the following:
- Development of standards
Selection of expert panels (and consultants)
Development of draft standards
Review by interested parties followed by revisions
Open hearing followed by revisions
Preliminary publication for comment followed by revisions
Approval by entire commission
Publication and distribution
Effective date
Updating as indicated
- Cyclic accreditation of each school (every seven years)*
Self-study (initiated one year prior to site visit)
Site visit
Preliminary decision and report
Review by site visit team and revisions
Review by school and response
Consideration of responses and any changes in school
Hearing and appeal processes
Final decision
- Monitoring
Annual survey of all schools
Reports, revisits, and reevaluation of conditionally or provisionally approved schools
As of May 1993, the CDA specified 250 standards [or ''must'' statements) for dental schools in eight broad areas: administration, financial resources and facilities, faculty and staff, students, curriculum, patient care and clinic management, research, and outcomes. The curriculum area is the most extensive. The stan-
dards and their accompanying discussion (which includes many "should" statements that do not constitute standards) vary greatly in specificity (CDA, 1993a). In addition to the commission's 27-page listing of accreditation standards, the self-study manual and other supporting material provide further detailed descriptions of the documentation that is needed to demonstrate compliance with the standards.
Given the breadth of the commission's responsibilities for dental school accreditation, it is not surprising that the typical site visit involves a large team of visitors. In contrast to the usual four-person survey team for medical accreditation, the average survey team for a dental school has fifteen members including five consultants for the predoctoral program and one consultant for each advanced education or allied education program. The AADS estimates that accreditation costs an individual school from more than $200,000 to more than $300,000 including the self-study, site visit, and response (AADS, 1993c). Most of the cost involves faculty time.
Accreditation Decisions
The Commission on Dental Accreditation has established three categories of accreditation results: approval, conditional approval, and provisional approval. The first category applies to programs judged to have achieved or to have exceeded published requirements, and it implies that a program has no serious deficiencies or weaknesses. Conditional approval applies to programs that have identified deficiencies or weaknesses that are considered correctable within a set period of time. This category allows an institution's graduates to meet requirements associated with state licensure and board certification. Provisional accreditation likewise allows an institution to meet these requirements, but it indicates that a program has a number of serious deficiencies and that significant improvement in the program must occur within one year.
In 1994, fifty-three programs were fully approved, and one was provisionally accredited (CDA, 1994a). The commission makes public an institution's overall accreditation status. Confidentiality is, however, maintained for most information including the self-study documents, site visit reports, institutional responses to site visits, progress reports, surveys, exit interviews, on-site communications, and proceedings of meetings.
Issues and Debates
The criticisms of dental school accreditation are both substantive and procedural (see, for example, AADS, 1993c; Hutchison, 1993; Pew Health Professions Commission, 1993; ten Pas, 1993). In the committee's survey, a majority of dental school deans expressed concern that government regulatory agencies or other outside forces were influencing the accreditation process or affecting the independence of the CDA. In addition, 14 disagreed and 12 were neutral on the statement that the current process helps ensure entry-level competency. Ten deans did not agree that candidates for state licensure should be graduates of accredited programs.
Accreditation has been such a significant concern to dental educators that the AADS has planned a major study of accreditation (House of Delegates Resolution 24-93-H). Nonetheless, as critical as dental educators have been of aspects of the accreditation process, it is important to note that the AADS itself has conceded that "if one were to start over to design an accrediting body for dental education, . . the basic features of that accrediting body . . . might not be all that dissimilar from what exists currently" (AADS, 1993c, p. 27). Even a purely internal program of quality assurance and improvement would make many similar demands on schools for information, analysis, and faculty participation.
The Commission on Dental Accreditation has, in recent years, made numerous changes in its processes and standards. It has, for example, shifted the accreditation cycle from ten to seven years. The organization has been recognized for its efforts by USDOE, particularly in the area of calibrating its processes, committees, and consultants.
Effectiveness and Quality
A major issue in the debate about accreditation is the lack of evidence that it is effective in identifying substandard schools or improving educational quality and, concomitantly, that it protects students from deficient education or the public from deficient dental care. The problem of evidence has at least two parts: (1) linking educational programs to outcomes, in particular, competency of graduates, and (2) identifying educational processes, methods, or structures (e.g., faculty organization, data systems, accounting procedures) that are desirable in and of themselves.
The high rates of failure on regional examinations, cited below in the discussion of licensure, are invoked in critiques of the
accreditation process as well as in critiques of the dental schools themselves. The argument is that if accreditation were ensuring a basic level of quality overall, failure rates should be lower in general and no school should see half or more of its licensure applicants failing regional clinical examinations. This argument assumes the validity and reliability of the licensure examinations, which are questioned later in this chapter.
Of the 54 dental schools, 53 are accredited without qualification. As noted earlier, detailed accreditation results are not published. Committee members—based on their own involvement in the process—seconded complaints made during site visits and other meetings that substandard programs were allowed to continue despite identified (but not public) deficiencies that are both serious and persistent. The CDA does not encourage closure of schools that do not improve, arguing that such a strategy would be "contrary to the spirit of accreditation" (CDA, 1993b, p. 5). This position is consistent with the commission's mission statement and with the models of continuous quality improvement now widely endorsed (if not successfully applied) in U.S. industry and health care. Such a position is, arguably, inconsistent with enforcing a minimum standard of quality to protect students and the public generally, a process that may require more decisive action for institutions with persistent problems.
Cost and Benefit
Overall, critics of the current accreditation process argue that its costs in time, money, and aggravation are excessive for its positive results. The aggravation factor is highlighted colorfully in the remark that "we will not make it into the 21st Century without killing each other off unless ... we find the correct manner to re-look at accreditation" (Formicola, 1993, p. 214). The cost of the process is indicated by an estimate from the dental school of the University of Maryland that the direct and indirect costs of its 1981 site visit exceeded $200,000 (Linthicum and Moreland, 1981).
The Commission on Dental Accreditation recognizes that the accreditation process makes heavy demands on institutions, and this committee commends its efforts to streamline the process and reduce its costs. The organization hopes to increase the use of electronic data transfer to collect information more quickly and inexpensively. The commission also is helping to develop materials that individual schools can use in assessing student competency and outcomes.
Innovation and Flexibility
Dental accreditation has been criticized for being inflexible, overly prescriptive, insufficiently independent of dental society leadership, and too focused on process and structure. It is said, thus, to stifle innovation. Further, the current system is criticized as being too little concerned with outcomes. It places excessive burdens on satisfactory schools while inadequately protecting students and the public from unsatisfactory programs. Even if accreditation results were valid, the confidentiality of accreditation results for specific dental schools raises questions about how well the process can protect students and the public.
In response to the argument that accreditation standards and processes are inflexible and stifle innovation, the Commission on Dental Accreditation argues that its standards are designed to allow for considerable flexibility. Its work to devise outcome assessments reflects its interest in methods for better evaluating innovative as well as traditional educational programs. Dental schools have, in fact, initiated a number of innovative programs over the years independently and with the assistance of organizations such as the Pew Foundation (Barker and O'Neil, 1989, 1992). The committee heard, however, that some of the schools had faced opposition from accreditors that had created time-consuming and stressful delays in implementing program innovations. For example, efforts to give students some leeway from the traditional "lockstep" curriculum by instituting special focus tracks encountered concerns that the tracks amounted to early specialization, which is restricted under current standards stating that "specialization must not be permitted until the student has achieved a standard of minimal clinical competency in all areas necessary to the practice of general dentistry."
Governance and Representation
Accreditation is, like various other professional standard-setting processes, sometimes criticized as a self-serving mechanism for professional control and protection from competition. For example, a recent suit against the accrediting activities of the American Bar Association (ABA) charged that the ABA process imposed "costly and unnecessary standards that protect the financial interests of professors, law librarians and standardized-test services" (Slade, 1994, p. A19). That the Commission on Dental Accreditation operates under the auspices of the ADA raises ques-
tions about its autonomy in an area characterized by considerable tension between elements of organized dentistry and dental schools.
The issue of independence is also an acute concern for allied dental personnel. The argument can be made that accreditation by an organization dominated by dentists protects dentists as much as it ensures the appropriate education of allied personnel. Allied dental groups and those involved with dental specialties also question their representation and influence in the process of accrediting allied and specialty programs. The committee heard oral and written testimony citing the lack of a separate, impartial, arm's-length accreditation commission. Only one hygienist sits on the Commission on Dental Accreditation, most of whose other members are dentists. The CDA committee that is responsible in the first instance for drafting accreditation standards for dental hygiene programs currently includes four hygienists, one public member, and three dentists (a dentist is always the chair). Site visit teams for dental hygiene programs generally have a majority of hygienists. Previous reviews of standards for dental hygiene did not address the changes requested by dental hygiene professionals, for example, required coursework in gerontology (ADHA, 1993).
Licensure
Licensure provides dentists and dental hygienists with legal authority to practice. Initial licensure involves an extensive set of requirements including written and clinical examinations. Continued licensure is largely a matter of filing forms and paying fees, although most states also require documentation of attendance at continuing education courses. Continued competency is not routinely assessed, but egregious errors or misconduct can bring discipline from state licensing bodies.
Dental licensure is distinctive in two respects. First, the requirement for a state or regional clinical examination distinguishes dentistry and dental hygiene from most other health professions. Physicians, for example, take national written examinations but face no clinical examination at either the national or the state level. In medicine, the last clinical examination element—suturing pig carcasses—was dropped 30 years ago (Foti, 1992). Some nonhealth professionals, for example, lawyers and engineers, may face special state or local examinations related to particular state laws or to geophysical conditions (e.g., earthquake zones).
Second, dental licensure is distinctive in requiring clinical examinations that use live patients who may be subjected to irre-
versible treatments. Some medical specialty organizations, in their certification examinations, use individuals trained to simulate patient problems. Candidates are evaluated on their interviewing, diagnosis, and treatment planning skills, but they do not actually treat these "patients." In optometry, the National Board of Examiners in Optometry (NBEO) began in 1989 to administer a "live performance examination," which is now accepted by 24 states (NBEO, 1993). (Many state optometry boards continue to administer their own clinical examinations.) The NBEO examination involves no therapeutic or irreversible interventions and appears to subject patients to very minor risks from the diagnostic procedures. The board recruits the patients for the examinations, which are held in a small number of cities. In addition, some states require allied professionals in audiology and related fields to demonstrate skills using live patients, but no therapeutic or irreversible procedures are required (S. Larson, American Speech Language Hearing Association, personal communication, July 1994).
Structure and Process
General Licensure
In the United States, licensure is a state responsibility, generally one that is delegated to an appointed board supported by a staff of government employees. Boards vary in the extent to which they include other oral health professionals. Some include representatives of the general public. The National Practitioner Data Bank and the American Association of Dental Examiners collect information on disciplinary actions against dentists taken by state boards, hospitals, or professional organizations.
For a dentist, initial licensure in a state typically requires the following: (1) graduation from an accredited U.S. dental school; (2) successful completion of a two-part national written examination; (3) successful completion of written and clinical examinations administered by the state or other designated organization (e.g., a regional board); and (4) a "jurisprudence" examination to check familiarity with specific state practice law. Other requirements (e.g., criminal background checks) may also be imposed.
All states accept the national written examination conducted by the Joint Commission on National Dental Examinations, which operates under the auspices of the ADA. This examination consists of two parts: Part I tests knowledge of the basic biomedical sciences; Part II tests knowledge of dental sciences. To take Part II, a candidate must have passed the first part of the examination.
Twelve states require their own clinical examinations. The other 38 states and the District of Columbia accept the results of one or more of four regional examination boards. The regional boards and the states that recognize their examinations are listed in Table 8.2.
TABLE 8.2
States Participating in Regional Dental Testing Agencies, January 1994
Once an individual is licensed in a single state, the procedures for obtaining a license in other states vary considerably (USDHHS, OIG, 1993). More than half the states permit credentialing under some circumstances; that is, they allow individuals currently licensed in another state to become licensed without a new state or regional clinical examination. These states may, however, require that a previous written or clinical examination be taken within the preceding five years and that the candidate have been in active practice for a specific period prior to applying for credentials. The credentialing process may also include interviews, background checks, evidence of continuing education, letters of reference, reviews of patient case reports, and other requirements. Some state boards have never exercised their credentialing authority. A few states require "reciprocity," that is, they accept credentials only from states that do likewise (AADE, 1992).
In an effort to promote agreement on licensing requirements for out-of-state dentists, the ADA and AADE convened a national conference in 1992. One result was a paper on guidelines for valid and reliable examinations (ADA and AADE, 1992). These guidelines set forth a conceptual and methodological framework for analysis and included data from the ADA's 1990 Survey of Dental Services, a 1990 examination of the clinical content of licensure examinations, and special surveys of dental schools and testing agencies. The recommendations from this conference have influenced the efforts of two of the four regional licensing boards to develop a common clinical examination (AADE, 1993b). In addition, the ADA issued a general set of guidelines for credentialing requirements (ADA, 1992a).
Specialty Licensure
Although all states license general dentists, only 16 license specialists (ADA, 1993d; see background paper by Guarino),1 Most of these 16 states administer their own specialty examination, and all require specialists to have a general dentistry license as
well. States that license by credentials may accept general or specialty licenses from other states. States that do not have specialty examinations or licensure by credentials require specialists coming from other states to pass their general clinical licensure examination. Practicing specialists who pass a general dentistry examination are subsequently precluded by law from practicing general dentistry.2
In addition, eight specialty areas recognized by the ADA have formal, voluntary certification processes. (As described earlier, the Commission on Dental Accreditation oversees accreditation of advanced specialty education programs.) The recognized specialties are dental public health, endodontics, oral and maxillofacial surgery, oral pathology, orthodontics, pediatric dentistry, periodontics, and prosthodontics. The ADA has established rules and monitoring procedures for the recognition of specialties and for the certifying boards associated with them. Certification generally requires graduation from an accredited program of advanced specialty education, a specified number of years of practice experience in the specialty area, and passage of an examination, which may include an oral examination and a clinical component.
Issues and Debates
With few exceptions, even strong critics of current policies for dental licensure recognize a legitimate public interest in having a formal process for granting people the right to practice dentistry based on some evidence of competency. Where defenders and critics divide is on what constitutes evidence of competency, who should judge it, how often it should be demonstrated, and whether live patients should be used in examinations (see, for example, Friedland and Valachovic, 1991; ADA, 1992c; AADS, 1993c; ADA, 1993c; Dugoni, 1993; Gaines, 1993; Hutchison, 1993; USDHHS, OIG, 1993; and the background paper by Guarino). Other disagreements focus on the effects licensure has on the educational process, the mobility of practitioners, and the geographical availability of services.
In addition to the criticisms discussed further below, specialty organizations also criticize requirements that specialists obtain
general dentistry licenses even when they do not plan to practice general dentistry and are, in fact, legally precluded from doing so. For example, the committee heard testimony that ''it is senseless to require a . . . specialist to perform dental procedures on a licensing examination which he or she has not done in the past twenty years and has no intention of doing so in the future'' (AAO, 1993, p. 25). In the same vein, "how is the public interest protected when a specialist is examined in an area of care he/she will not practice" (AAOMS, 1993).
Evidence of Competency
On the issue of what constitutes public evidence of competency, the major dividing line is between those who believe that a freestanding clinical examination is necessary and those who believe that competency is adequately demonstrated by a combination of dental school graduation, passage of national written examinations, and completion of a year in a certified residency program (AMA, 1994). This latter approach is termed the medical model, although some details vary from state to state. The content of the national written examinations is the subject of ongoing discussion and critique, but few seriously challenge the continued use of these tests for dental licensure.
Those who support a separate clinical examination in dentistry typically argue that, at a minimum, (1) a dental school diploma is no guarantee of competency; (2) a written examination is an insufficient measure of competency; (3) residency programs are too variable for residency experience to serve as an adequate measure of competency; and (4) public safeguards in medicine, such as hospital procedures for granting practice privileges and hospital peer review, are less generally applicable to dentists. To the committee, supporters of the clinical examination also cited legal and financial pressures on dental schools that might compromise their ability to ensure the competency of their graduates. As evidence of problems, they cite the initial failure rates on regional board examinations displayed in Figure 8.1 for the 1993 Northeast Regional Examination Board (NERB) examinations.
In addition, in testimony to this committee the Central Regional Dental Testing Service (CRDTS) expressed concern that the limited clinical experience of dental students was showing up in their examinations as poor test results. CRDTS also pointed to poor results in the discipline of periodontics and urged better faculty training in assessment methodologies.
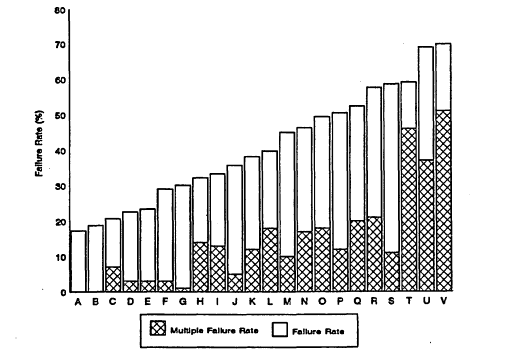
Figure 8.1
Overall failure rate on Northeast Regional Examination Boards by school.
Source: Northeast Regional Board of Dental Examiners, Inc., 1993.
In contrast, critics of current licensure arrangements argue that the clinical licensure examination is itself a flawed measure of competency. The examination (1) is intrinsically too narrow in scope to constitute a valid assessment of an applicant's ability to provide comprehensive patient care proficiently; (2) subjects applicants to capricious or at least highly subjective and unreliable evaluations despite procedures to calibrate the evaluations of individual examiners; and (3) varies in content across states and regions in ways that cannot be justified by documented regional differences in patient needs or effective practice. A uniform national examination (discussed further below) would answer the third criticism but would not by itself overcome other criticisms. As long as live patients are used in an examination, variations in the testing "material" will make it particularly difficult to standardize and monitor assessments.
To critics, the inadequacy of the clinical examination—not the schools—is revealed every year in the variable failure rates from
region to region and state to state. To Damiano et al. (1992, p. 72), this variability suggests that "factors other than the ability of the candidates influence exam outcomes." Deans and faculty complain that "extremely competent applicants frequently" fail initial clinical examinations (Hutchison, 1993). The fact that most of those who fail eventually pass, without any required remedial work, reinforces concerns about the inadequacies of the examinations. Other criticisms, as described below, focus not on the validity of the clinical examination but on ethical shortcomings in using live patients.
Although state, regional, and national examining organizations have made efforts to improve the validity and reliability of examinations, fundamental problems remain. Too little is known about the outcomes of dental practice and variations in that practice. As in medicine and other health professions, this knowledge gap raises questions about the content of professional education and performance assessments of all kinds.
Locus of Responsibility
Those who reject the medical model for licensure may still differ on the question of who should judge competency. One subgroup argues that a state-level judgment of clinical competency is required. The other supports a uniform regional if not national clinical examination and generally supports a credentialing process for licensed dentists who move to a new state.
As heard by this committee, the stated "public interest" arguments for a state-level examination are that (1) regional examinations as designed, as administered, or both cannot be trusted as a measure of competency; (2) the National Practitioner Data Bank, other clearinghouses, and dental boards in other states cannot be trusted to identify incompetent practitioners; and (3) special state circumstances require state-specific measures of competency. On occasion, the committee heard that some state examiners have a stake in working closely and cooperatively with dental schools in the state to ensure that students are prepared to pass the examination.
The committee also heard more dubious arguments for state clinical examinations. One is that "we've always done it this way, and it is too much trouble to ask state boards to give up this power." The other is that "we will be overrun by out-of-state dentists attracted by our lifestyle or economy." The latter argument is rarely stated officially for legal reasons. The case law on
licensure recognizes protection of the public as a rationale for regulation but rejects protection from competition as a basis for policy (Stromberg, 1992; see background paper by Guarino, 1994). Nonetheless, it is telling that requirements for state clinical examinations are concentrated in southern and western states such as Florida and California that have mild climates and fast-growing populations.
Live Patient Examination
Many critics of the clinical examination focus their harshest criticism on the continued use of live patients. These criticisms cite such problems as (1) inappropriate delays in treatment because patient problems are "saved" for the examination rather than treated promptly; (2) unnecessary or duplicative X rays and other evaluative procedures; (3) incomplete and otherwise inappropriate patient care that violates the normal expectation of competent, comprehensive, and continuous care, especially when patients undergo irreversible procedures or must return after the procedure to another state; and (4) recruitment under questionable circumstances (e.g., for money, without true informed consent). Further, in exposing patients to such risks or harms, the clinical examination inevitably involves applicants and examiners in unethical practices. It also subjects participants, including sponsors, evaluators, and applicants, to unacceptable legal risks. These problems are intensified when patients are recruited for examinations that require travel to a distant site, a frequent situation for dentists seeking licensure in a new state.
State and regional examiners have been moving to limit their use of live patients in the clinical examination. Still, many defend the practice on grounds that typodonts or manikins do not adequately represent "real-world circumstances" either physiologically or behaviorally. Indeed, concern about the sterility and artificiality of written examinations has led medical specialty groups to consider how "standardized patients" (often actors) might be used to assess diagnosis and treatment planning skills for purposes of specialty certification. Although no changes have occurred in the examinations required for initial medical licensure in the United States, an ''objective structured clinical examination" using standardized patients has been tested in Canada for possible inclusion in national licensure requirements. The rationale is that it is important to evaluate "behavioral performance . . . by observing 'what is being done' rather than finding out if the practitioner 'knows how to do it''' (Martini, 1988, p. 1057).
Educational Process
Clinical licensing examinations (both regional and state) are said to undermine dental education by distorting the curriculum, stifling innovation, and complicating faculty recruitment. Schools understandably want their students to pass the examinations; thus, to varying degrees, faculty "teach to the examination." One result is that procedures that are covered on the examination may receive more attention than warranted by their relevance to current patient needs and may thereby divert time from other, more relevant topics. To the extent that a school feels that it must prepare students for more than one examination, the problem is multiplied.
The committee often heard that clinical examinations still focus too much on prosthetic exercises that very few dentists currently perform themselves. The schools must devote extra curriculum time to procedures that could otherwise be allocated for new or more common services. Until and unless each state or regional clinical examination is revised to reflect new and more effective technologies, schools may make uncomfortable compromises in the curriculum. For example, the gold-foil procedure (a kind of restoration) was long criticized as an "out-of-date" requirement. This procedure has finally been eliminated entirely or made optional in state and regional examinations, but only after years of lobbying—and largely wasted curriculum time.
Faculty recruitment may also be complicated by state licensure requirements. In a case discussed during a visit to one university, an oral surgeon recruited from another region failed to pass the general dentistry clinical examination administered by the state board. Once he finally passed the exam, he was then barred from practicing general dentistry because he was a specialist. The clinical examination requirement in such cases appears both burdensome and irrelevant to the public interest.
Those who defend the clinical examination typically argue that critics overstate their case and that little would change in the curriculum if the clinical examination were eliminated. That is, teaching to the exam probably enters into the rigidity of curriculum as only one factor among many, including accreditation, faculty self-interest, alumni pressure, and the financial cost of change. To the extent that the examinations are off-target, educators and examiners could work together to improve them.
Continued Competency
Although most states have requirements for continuing education, none, according to the U.S. Department of Health and Human Services, Office of Inspector General (1993, p. 9), requires "any assessment of what a dentist actually learned from a course." Some states examine competency of licensed, out-of-state dentists on a one-time basis by requiring them to be reexamined through a state clinical examination or requiring reexamination if a past examination dates back more than five years. None of these states, however, requires periodic reexamination for in-state dentists.
Those who favor periodic assessment of competency argue that state boards do not satisfactorily monitor continued competency and that required continuing education is inadequate because courses are too variable in content and impact. (Issues related to continuing education are discussed in Chapter 4.) Within dentistry, the American Association of Oral and Maxillofacial Surgery has adopted a recertification process that is scheduled to begin in 1998 (AAOMS, 1993).
In the future, periodic reviews of competency may become increasingly feasible and acceptable with the growth of sophisticated electronic communication and computer-based patient records. Such assessments would have to be relatively unobtrusive and inexpensive as well as valid. (See discussion of the Dental Interactive Simulations Corporation below.) To the extent that assessments are designed to help improve performance rather than punish poor practice, they are more likely to be welcomed.
Dentist Mobility and Access to Care
Clearly, dentists in many parts of the United States view clinical examination requirements for out-of-state dentists as a barrier to mobility. Some also cite the potential adverse effect on access to care (Pew Health Professions Commission, 1993). The Inspector General of the U.S. Department of Health and Human Services reported instances in which state licensure requirements discouraged National Health Service Corps dentists from staying in underserved areas (USDHHS, OIG, 1993). However, the Inspector General's 1993 report stated that "we found no data, nor any studies, to indicate that licensure-by-credentials policies have much overall bearing on the access to dental services in underserved areas" (p. 10). Other factors such as isolation, family preferences, and earnings potential appear more significant.
Issues in the Licensure of Dental Hygienists
Most of the issues raised above also are raised with respect to hygienists. Dental hygienists too are concerned about the variability of state licensure requirements, reliability and validity problems with clinical examinations, and the appropriateness of using live patients during examinations. In addition, the scope of practice permitted under state laws has provoked considerable controversy among hygienists. Most of the controversy focuses on provisions regarding supervision. A sizable minority of states requires that dentists directly supervise certain hygienists' services (i.e., they must be physically present). This limits the opportunity for hygienists to provide routine hygiene services in nonoffice settings such as nursing homes. At least nine states forbid the employment of more than two hygienists in a dental office (ADHA, 1993). A 1993 analysis by the staff of the Federal Trade Commission suggested that such restrictions should be examined for their anticompetitive effects (Wise, 1993).
In principle, training, competency, and patient or societal needs should inform practice acts; in actuality, they are heavily shaped by economic interests of the dominant professional groups. Critics of licensing policies for dental hygiene note that the majority of state boards members are dentists (IOM, 1989a). On a few state licensing boards, the dental hygiene member or members may vote only on matters relating to hygiene, whereas the public or consumer member has full voting privileges (ADHA, 1994).
Options
In the course of its study, the committee identified three options for improving the current process of entry-level dental licensure. They were to Ill continue the current system with incremental steps to remedy deficiencies; (2) intensify efforts currently under way to move toward a uniform national clinical examination accepted by all states and away from unreasonable restrictions on professional mobility; or (3) adopt the medical model and eliminate the state or regional clinical examination.
The line between incremental and major changes is not precise. For purposes of this discussion, incremental change focuses primarily on continued efforts to improve the validity, reliability, and relevance of competency assessments for a variety of educational, quality improvement, and other purposes. To call these efforts incremental is not to imply that they are unimportant.
Major change would involve at least two additional steps. First, the use of live patients would be reduced and eventually eliminated. Second, a uniform clinical examination would be accepted by all state licensing authorities.3 This step would be an extension of those that led to the regional examination organizations.
One initiative that would support both incremental and major change is a technology-oriented effort to improve competency assessments organized by the Dental Interactive Simulations Corporation or DISC (Foti, 1992). The product of the effort is also called DISC. Members of the nonprofit corporation include the AADE, AADS, ADA, CRDTS, NERB, Southern Regional Testing Association, and Western Regional Examination Board. Notable for their absence are the state boards of California, Florida, and North Carolina, which do not participate in regional examination boards.
DISC proposes a "computer software program that uses high-quality images and video to represent real patients . . [with extensive] intraoral images. . . [and links] to a knowledge base that would support instant [information] retrieval, cross-referencing, glossaries, images, animations, and motion video features" (Foti, 1992, p. 5) The simulated patients could be "questioned," "treatments" could be ordered, and consequences evaluated. All candidates being assessed would be evaluated on their handling of the same case. Patient variability would not complicate examination findings, although reliable evaluation of results would still be an issue. The difficult search for complex or special patients as test subjects would be avoided.4
If the technology and processes on which these and other initiatives are based prove valid, reliable, and acceptable to both
regulators and educators, it is likely that dental schools will be employing much the same technology and procedures to evaluate student competency during the course of their predoctoral education. This should narrow the gulf between examiners and educators and should facilitate movement toward the medical model, perhaps in a form that brings examiners into the schools.
Those who would eliminate clinical exams and adopt the medical model were supported by the Pew Health Professions Commission, which recommended that "graduates should be granted entry-level licensure based upon graduation from an accredited dental school, successful completion of the national board examinations, and completion of a postdoctoral training program" (Pew Health Professions Commission, 1993, p. 54). That commission also endorsed relicensure and recertification based on continued competency.
The options for relicensure involve two distinct issues (1) the treatment of dentists relocating from one state to another and (2) the assessment of continued competency for all practitioners. For relocating dentists, the options are essentially to continue the current system or to persuade all states to adopt some form of credentialing including background checks and similar requirements but not a repeated clinical examination. For all dentists, the options are, again, to continue the present system or to move toward some periodic reassessment of competency as some specialty groups are doing.
Findings and Recommendations
Accreditation
Although the current process for accrediting dental education programs has many positive features, it is in need of significant revision. The accreditation process is too expensive, too focused on procedural details, and too inhospitable to educational innovation. Although the specifics of accreditation assessment are not made public, the committee believes that the process tolerates some inferior educational programs. The standards may be too low or their application may be too permissive or both.
Accreditation reform should focus on standards and methods (1) that will identify and improve those schools that are not educating their students effectively or ethically and (2) that will not allow persistently poor performance. At the same time, excessively detailed assessments of structures and processes should be trimmed.
Improvements in methods of assessing educational outcomes are as central to accreditation reforms as they are to improvements in predoctoral education, entry-level licensure, and assessment of continued competency. Thus, cooperation and coordination among responsible organizations in each of these arenas should be established to avoid conflicting strategies and costly duplication of effort. Improvements in the processes for collecting information-particularly those based on electronic transfer of data—likewise will produce multiple benefits and should be coordinated.
The committee understood and sympathized with concerns expressed about self-regulation, but it believed that the major alternative—a federal accreditation process—would not, on balance, solve (and, in fact, might worsen) most current problems including costliness, inflexibility, and questionable effectiveness. The committee, however, does believe it prudent that dental accreditors and educators be prepared to respond constructively to reasonable demands for increased public accountability and information. The committee supported the goal of better information for the public, but members were split about recommending extensive disclosure of accreditation results. Most believed that the current process needed improvement first. Some believed that disclosure would promote defensiveness and work against cooperative and candid analyses of educational deficits and strategies for correcting them.
The committee agreed that after steps are taken to improve the validity and reliability of licensure and accreditation processes, the AADS, AADE, and CDA should investigate the relationships among accreditation results, school-wide pass rates on national written examinations and on regional or state clinical licensure examinations, student grades, and graduates' subsequent performance in practice. They should then review current policies limiting public disclosure of institution-level information about student performance on licensure examinations and should study the advantages and disadvantages of making more accreditation information public.
To protect students and the public from inferior educational programs and to reduce administrative burdens and costs, the committee recommends that the Commission on Dental Accreditation involve concerned constituencies in a sustained effort to:
- expand the resources and assistance devoted to schools with significant deficiencies, and decrease the burden imposed on schools that meet or exceed standards;
- increase the emphasis on educational outcomes rather than on detailed procedural requirements; and
- develop more valid and consistent methods for assessing clinical performance for purposes of student evaluation, licensure, and accreditation.
Licensure
The dental community has begun important steps to improve the validity, reliability, relevance, and fairness of competency assessments for dental professionals. Many of the deficiencies or uncertainties that characterize licensure processes also characterize evaluations within dental schools and health care organizations. Further improvements in assessment methodologies will benefit both dental education and practice. One major problem in assessing current licensure processes is the lack of research on their effectiveness in protecting patients from inept practitioners.
Although states can be criticized for occasional parochialism and inefficiency, they are a reasonable locus of responsibility for professional regulation. The relevant task is not to construct a new national licensure system but rather to minimize deficiencies in the present system and to involve all major parties in the process of change.
In the view of this committee, the most important deficiencies are concentrated in a few areas: the use of live patients in clinical licensure examinations; variations in the content and relevance of clinical examinations; unreasonable barriers to movement of dentists and dental hygienists across state lines; inadequate means of assessing competency after initial licensure; and practice acts that unreasonably restrict the use of appropriately trained allied dental personnel. In addressing these problems, the committee suggests that a task force of the relevant organizations of dental examiners, educators, consumers, and others should be created to devise demonstration projects to test alternative regulatory policies and mechanisms. Possible anticompetitive features of current statutes and regulations should also be examined carefully.
To improve the current system of state regulation of dental professionals, the committee recommends that the American Association of Dental Examiners, American Association of Dental Schools, professional associations, and state and regional boards work closely and intensively to
- develop valid, reliable, and uniform clinical examinations and secure acceptance of the examinations by all state
- licensing boards as replacements for state or regional clinical examinations and as complements to current National Dental Board Examinations;
- accelerate steps to eliminate examinations using live patients and replace them with other assessment methods, such as the use of ''standardized patients" for evaluating diagnosis and treatment planning skills and simulations for evaluating technical proficiency;
- strengthen and extend efforts by state boards and specialty organizations to maintain and periodically evaluate the competency of dentists and dental hygienists through recertification and other methods;
- remove barriers to the movement of dental personnel among states by developing uniform criteria for state licensure except in areas where variation is legitimate (e.g., dental jurisprudence); and
- eliminate statutes and regulations that restrict dentists from working with allied dental personnel in ways that are productive and consistent with their education and training.
Summary
Debates about accreditation and licensure are among the most divisive in dentistry. Greater agreement on reliable and valid methods for assessing clinical competency in all settings would reduce tensions as would greater agreement on the clinical skills that need assessment. Both would pave the way for state acceptance of uniform clinical examinations and for less procedurally oriented accreditation standards.


























