F Integrating Our Primary Care and Public Health Systems: A Formula for Improving Community and Population Health
William E. Welton, M.H.A.
Theodore A. Kantner, M.D.
Sheila Moriber Katz, M.D., M.B.A.
Mr. Welton is Acting Dean of the School of Public Health at the Medical College of Pennsylvania and Hahnemann University in Philadelphia, Pa., Dr. Kantner is the Chairman of the Department of Family Medicine at the University and Deputy Director of its Robert Wood Johnson sponsored Generalist Physician Initiative, and Dr. Katz is the Senior Associate Dean of the Proposed School of Public Health and former Dean of the Hahnemann University School of Medicine. The authors express their appreciation to Mary Neighbour for editorial assistance provided.
Introduction
As we redefine the role of primary care in a health system rapidly reorienting to a market-oriented managed care paradigm, we must understand and re-explore the current and future relationship between population-based or public health services and personal medical services at the primary care level. This question is no less than that of ensuring our ability as a society to ensure and improve the health of our diverse populations in a dynamically changing delivery, financing, and accountability environment.
This question is of increasing importance as private employers move ever more aggressively, developing managed care programs to decrease costs, to improve overall accountability for performance, and to improve service quality and access. The significance is even further emphasized as government-sponsored health programs at the federal, state, and local levels (e.g., Medicare, Medicaid, Federal Employees Health Benefits Program, CHAMPUS, as well as numerous state and local employee health benefit and worker's compensation programs) move just as aggressively to adopt managed care concepts. Increasingly, pragmatic
analysis requires a rethinking of traditional notions and paradigms of population (public) health.
This paper identifies current issues and offers suggestions for integrating concepts to support functional and practical improvement while ensuring population health maintenance and improvement and reasonable access to services in a context of controlled long-term per capita cost. To ensure these desired outcomes, we must expand our vision to encompass both population-based and primary medicine and health care services as a single integrated system; we must work to remove barriers to its formation; we must develop new operating paradigms to ensure its high-quality performance; and we must develop programs to focus its objectives and ameliorate its excesses.
This paper identifies and highlights significant requirements and challenges for leadership within the public health and primary care communities, and for educational and research leadership among academicians serving and supporting those communities. In the final analysis, many of these challenges must also be addressed and changes supported by visionary leaders within our political and health care delivery systems, if such integrated community health systems are to be created and their potential achieved.
In short, we must view both public health and primary care as two interacting and mutually supportive components of an increasingly complex integrated community health system, having the single common goal of improving the health of a community and its diverse populations.
Background: Public Health And Primary Care
We noted with interest the relative paucity of published material directly addressing the intersection and interaction of population-based programs and services (public health) and primary care programs and services. It is significant that many of the seminal documents on the subject are in the form of special reports and studies commissioned by the Institute of Medicine (IOM), a small number of private foundations, and, more recently, the U.S. Public Health Service (USPHS). In short, the subject is rarely dealt with directly but more often is dealt with obliquely, perhaps indicating a need for new concepts to guide our thinking.
Relatively few of the small number of writings identified were written from the perspective of public health. Most were written from the perspective(s) of preventive medicine and family medicine (mostly community-oriented primary care [COPC]). Few were identified in the internal medicine and pediatric literature. In general, the COPC concept has not spread broadly throughout the world of primary care medical practice since being the subject of a 1984 IOM study (1). The COPC practice model appears to be most apparent in staff-model health maintenance organizations (HMOs) and in a relatively small number of academic community-based practices. This report and concept have been important in
guiding our developing thoughts on the appropriate roles and relationships of both public health and primary care, however.
Over the past two decades, our understanding of public health and primary health care has gone through a number of important transitions. It is important to acknowledge, at this juncture, that public health and primary health care have each developed as distinct and largely unrelated (somewhat competitive) cultures over the past 80 years. It may now be important to develop a more integrated view of the two, however, because these distinct cultures are increasingly being forced to operate together as a result of a series of broader market reforms. Increasingly, these market reforms emphasize the development of competitive managed care programs and strategies to organize and provide integrated health care and preventive services at controlled cost and quality to defined populations, including most of those formerly cared for directly by local and state health departments. This can be seen by the increasingly rapid transition of Medicaid populations to a broad range of managed care programs over the past decade. In this context it is also important to acknowledge the seeming preference of our political system to seek market-oriented solutions to complex health care problems.
As a result, the public health of the past will increasingly become the population health of the future and the primary care of the past will increasingly become the clinical and preventive primary care and community-based medicine of the future. The combination of the two—working more closely (if not always in absolute harmony) in partnership with each other, with integrated health delivery systems, and with market-oriented financing systems to improve the health of the same populations—is increasingly likely to evolve toward the integrated community health system of the future.
In 1994 the IOM began its most recent exploration of primary care by clarifying its use of the term as one that "focuses on the delivery of personal health services" (2). This focus builds on the IOM's earlier conceptualization of COPC:
[By 1984 the notion of] community oriented primary care … [had evolved as] … "a strategy whereby the elements of primary health care and of community medicine are systematically developed and brought together in a coordinated practice" [Abramson and Kark, 1983, p. 22]. [It was also] the provision of primary care services to a defined community , coupled with systematic efforts to identify and address the major health problems of that community through effective modifications in both the primary care services and other appropriate community health programs [italics added] (1, p. 2; 2, p. 12).
IOM's most recent formal definition of primary care combines concepts contained in both paragraphs, above:
the provision of integrated, accessible health care services by clinicians who are accountable for addressing a large majority of personal health care needs, developing a sustained partnership with patients, and practicing in the context of family and community (2, p. 15).
During the period preceding this report, significant attention has also been given to developing a clearer understanding of the role of ''public health" in our pluralistic, diverse, and often fragmented society. In 1988, the IOM published its report The Future of Public Health (3), which has provided significant guidance to the development of public health since that time. The study committee's core recommendations included the following: "the mission of public health (is defined) as fulfilling society's interest in assuring conditions in which people can be healthy" and "the core functions of public health agencies at all levels of government are assessment, policy development, and assurance" (3, p. 7). Additional implementation recommendations were made in areas involving the creation of the appropriate statutory authority, reorganizing all health functions into a single cabinet-level agency (separate from income maintenance functions) at the state level, definition of clear lines of public accountability for public health down through the local level, and strengthening public health ties to the related areas of mental health, environmental health, social services, and care of the indigent (3, pp. 8–13).
From a conceptual point of view the report outlines the basic public health functions of government as shown in Figure F-1.
Assessment involves the systematic collection and analysis of information on the health of the community; assurance involves ensuring that necessary services are provided to achieve agreed-upon (population health) goals; evaluation reviews the results of prior actions (or inactions) relative to previously determined policy goals and/or quality standards; and policy development is intended to guide the operation of the health system and resource allocation for its support,
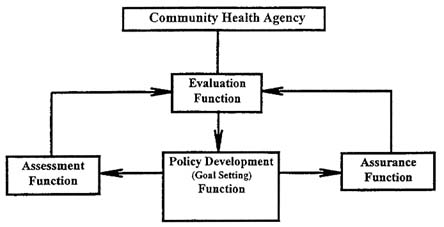
FIGURE F-1 Functions of public health.
SOURCE: Adapted from Institute of Medicine (1988), with modifications and clarifications suggested by the authors.
while taking a strategic approach in the context of a democratic political process (3, p. 8).
Within this overall construct we can seek further clarification of the role of public health and its division of effort with primary care medicine in the increasingly important area of prevention as suggested by the Partnership for Prevention in 1993 (4). That report identified three essential elements of prevention: clinical preventive services, community-based health promotion and disease prevention, and public policy for health promotion and disease prevention. In many ways the area of prevention is the critical link between traditional notions of public health and personal and community health (4). In this paper we will assume that the responsibilities for providing and/or facilitating clinical preventive services reside principally within the primary care personal service arena. In this paper we will also assume that the principal responsibility for providing and/or ensuring the provision and coordination of community-based health promotion and disease prevention and public policy for health promotion resides principally within the public arena.
Emphasis is given to the importance of these elements and is eloquently emphasized by Lashof (5) and Schauffler (6) in their papers. We endorse the importance of these points and include them as a matter of definition and clarification in the model(s) set forth throughout this paper in the following manner. For the purposes of this paper, IOM's concepts of assessment and assurance (3) (Figure F-1) will be assumed to incorporate the appropriately determined public functions associated with community-based health promotion and disease prevention. Additionally, the policy development function will be assumed to incorporate the appropriately determined public policy functions required to support health promotion and disease prevention programs. It is significant that Schauffler goes further to propose the development of a new form of community-based organization, community-based health promotion and disease prevention. Such a public-private organization would be separate from the health department, would be based on collaborative and partnership principles within and across the community, and would assume significant responsibility for overseeing community-based programs of health promotion and disease prevention and for providing appropriate linkages between the world of primary and preventive services and public health policy (6).
A more recent and somewhat more functionally oriented definition of public health is provided in the 1994 USPHS Report for a Healthy Nation: Returns on Investment in Public Health (7). According to the report, public health (7, p. 1):
Prevents epidemics
Protects the environment, workplaces, housing, food, and water
Promotes healthy behaviors
Monitors the health status of the population
Mobilizes community action
Responds to disasters
Assures the quality, accessibility, and accountability of medical care
Reaches out to link high-risk and hard-to-reach people to needed services
Researches to develop new insights and innovative solutions
Leads the development of sound health policy and planning
Over the past two decades, the definitional refinements for primary care and for public health have taken place, for the most part, independently of each other. To date, there does not appear to be a single integrated definition that has as its explicit purpose the integration of the two into a single system with the common goal of improving the health of populations through a team approach.
This general issue was recently recognized by Joyce Lashof in 1991:
Bringing public health and primary care together is essential for the economically disadvantaged, but it is also increasingly important to all communities. What is lacking in this effort, however, is the organizational and financial mechanisms necessary to implement this approach on a larger scale (8).
Additionally, Thomas Rundall recently recognized the issue in the broader context of medicine and public health in his discussion of the need to seek their more effective integration (9):
[T]he effectiveness of our future system for improving the health of our citizens depends greatly on the reform and [effective] integration of our nation's public health and medical care systems … [where] "effective" means successfully achieving the functions the system is designed to perform … (and) functional integration ("unity or harmony within a system based upon the interdependence of specialized parts"—Theodorson and Theodorson, Modern Dictionary of Sociology, 1969). … The benefits to our nation's health of proceeding in this way, however, are enormous. As we move into the twenty-first century, an integrated system of public health and medical care services is our nation's best hope not only for improving the health of all of our citizens, but also for closing the "health gap" between socioeconomically disadvantaged groups and the rest of the population.
These definitional refinements have paralleled significant changes in our national health care system, as seen through the passage of the HMO Act of 1973 (and subsequent amendments), OBRA 1991 (diagnosis-related group reimbursement for hospitals), and subsequent legislation defining physician payment in terms of the Resource-Based Relative Value Scale. These major legislative initiatives, occurring in combination with the increasingly aggressive adoption of managed care programs by large employers and governmental programs, have begun to force a practical integration of personal and preventive services and the development of population-based management and assurance systems to support this integration. Unfortunately, as we will see, this often happens without utilizing our traditional public health systems, thus leading to additional confusion and
inefficiency, with an inherent loss of effectiveness in achieving the larger goal of improving the health of the population.
Since the creation of Medicare and Medicaid in 1966, the focus of the nation's health and budgetary policy makers has increasingly turned to issues of cost-containment. Over the same period, the focus of the nation's major industries and employers has turned to issues of international competitiveness and cost control focusing on controlling the rapidly rising cost of health care. State and local governments are facing increasingly constrained resources to support rapidly rising health care costs and the competing needs of more effective social, educational, and crime prevention programs. Overall, the demands have increasingly focused on preventing premature death and disability and on achieving greater value for resources expended.
In 1993 McGinnis and Foege published a landmark study identifying the actual causes of death in the United States (10). In that study the authors concluded that
Approximately half of all deaths that occurred among U.S. residents in 1990 could be attributed to the factors identified [tobacco, 19 percent; diet/activity patterns, 14 percent; alcohol, 5 percent; microbial agents, 4 percent; toxic agents, 3 percent; firearms, 2 percent; motor vehicles, 1 percent; illicit use of drugs, 1 percent]. Despite their approximate nature these estimates … hold implications for program priorities … (and) … they compel examination of the way the United States tracks its health status.
This conclusion underscores the fact that most of these deaths are behaviorally mediated and are therefore potentially preventable. They "are by definition premature and are often preceded by impaired quality of life … the public health burden imposed by these contributors offers both a mandate and guidance for shaping health policy priorities" (10).
In a similar vein the 1994 USPHS Report for a Healthy Nation: Returns on Investment in Public Health (7) noted
An appropriate investment in public health will lead to substantial future savings in medical care. … The fulfillment of public and personal health objectives will increasingly require close collaboration between the changing medical care and public health systems … even a reformed medical care system cannot mount the appropriate actions to address many of the conditions responsible for death and disability in the United States today.
In his 1994 book Medicine's Dilemmas: Infinite Needs Versus Finite Resources (11), William L. Kissick observes these needs from the medical care perspective, providing the following insights:
The golden rule of health care in our society is that everyone deserves the finest health care attainable, provided someone else pays. … In health care it is possible to spend more but get less value, if value is measured as health status for the population. … Increasing quality or access adds value, but then so does
lowering costs if what we seek is cost-effectiveness. Costs, like access and quality and, for that matter, health itself, are relative (11, pp. 2, 14).
The foregoing assessment, of course, begs the issue of the interacting and interdependent "systems" relationship of public (population) health and primary care. Increasingly, public health leaders are calling for an integrated view of population and personal health. Of special note is Philip Lee's delivery of the 1994 Shattuck Lecture to the Massachusetts Medical Society (12), in which he observed
Today, perhaps the best linkage between the personal health care system and the public health system is in the area of clinical preventive services. While clinical preventive services provide one very significant link, applying the population based perspective of public health to the personal health care system in its totality is the next necessary step. … In spite of the intellectual underpinnings and the syntheses of ideas integrating public health and personal health care, public policy has continued to separate public health from the personal health care system, However, if we want to achieve the goals of increasing the span of healthy life for Americans and reducing the health disparities among Americans at an affordable cost, our nation must adopt … an approach that accentuates and promotes a close working relationship between the personal care and public health systems (12).
All of these factors force us to refocus on the practical questions of the prevention-effectiveness and cost-effectiveness of our somewhat idealized "integrated health care system," as distinguished from its medical and acute care subsystems with which we are more familiar today.
The Starting Point: A Systems Model For Clinical And Preventive Services
If one accepts the notion that public health and primary care are two facets of a complex system influencing personal, population, and community health status, the next steps are to synthesize a model for such a system and to identify areas for specific intervention and improvement to move our health care system to higher levels of effectiveness. The beginnings for such a synthesis have been suggested by Thompson et al. (13) in their article "Primary and Secondary Prevention Services in Clinical Practice: Twenty Years' Experience in Development, Implementation, and Evaluation." In that article, the authors describe their own and their HMO's experience with primary and clinical preventive services and provide their recommendations for the effective implementation of an integrated population health and primary care model. Their overall conclusion is that
Systematic population-based approaches to the development and provision of clinical preventive services targeting the one-to-one level of primary care and multiple infrastructure levels of care are forging a synthesis of clinical medicine
and public health approaches. This approach will become pervasive as clinical information systems improve, risk information is captured routinely, and practitioners gain skills in the art of risk behavior change and population-based care (13).
The key elements and concepts of their general model are summarized below. Critical elements for an ideal preventive care provision model are as follows (13):
- Population-based planning.
- Directed toward major causes of morbidity and mortality, epidemiologically determined. This includes the epidemiology of "needs" (the diseases and the risks) and the epidemiology of the "wants" (the desires of the enrollees).
- Evidence for intervention effectiveness.
- Functioning at multiple levels, including one-to-one level of primary care, infrastructure level, organization level, and external community.
- Prospective and automated to the maximum extent feasible.
- Health is a by-product of a shared endeavor between practitioners and patients; informed discussion and consent are maximized.
Criteria used to examine primary and secondary prevention issues are as follows:
- Condition (disease/risk factor) is important.
- The disease or risk factor has a recognizable presymptomatic stage.
- Reliable methods for detecting the disease or factor exist (considering the sensitivity, specificity, and positive predictive values of the screening test).
- Modifications of the risk factor therapy in the presymptomatic disease stage reduces morbidity and mortality more than after symptoms appear.
- Facilities to address the identified risk factor or condition exist.
- The cost and potential benefits of implementing a state-of-the-art approach have been considered.
Thompson et al. (13) have used these concepts to develop an intervention model, summarized in Figure F-2, which specifies three groups of factors necessary to support behavioral change in health professionals and necessary to achieve effective integration of primary and preventive medical services when the professionals deliver those services from an integrated population and individual or personal health perspective. These factor groups include those that predispose a health professional to make a necessary behavioral change in his or her practice (predisposing factors), those that make necessary behavioral change possible (enabling factors at the community level, organization level, and practice environment level), and those that reward and strengthen behavioral change (reinforcing factors).
The model goes on to define an integrated professional and behavioral system supporting effective and efficient delivery of personal health services (primary
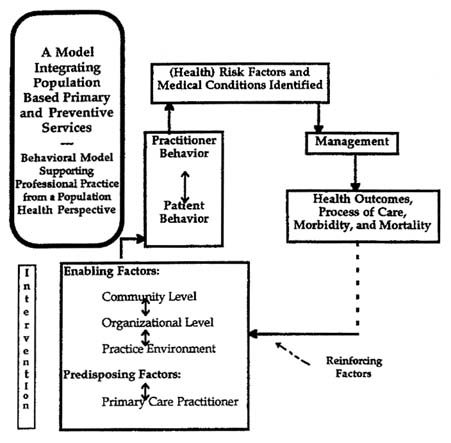
FIGURE F-2 A model integrating population-based primary and preventive services. SOURCE: Adapted from Thompson et al. (1995).
and preventive care) in a population health context (an enrolled [defined] HMO population). The model has been developed and evaluated over a period of 20 years and has produced impressive results including
a 32% decrease in late stage breast cancer (1989 to 1990); 89 percent of 2-year-olds with complete immunizations (1994); decrease in adult smokers from 25% to 17% (1985 to 1994); and an increase in bicycle safety helmet use among children from 4% to 48% along with a 67% decrease in bicycle-related head injuries (1987 to 1992) (13).
Although the work makes a significant theoretical and practical contribution to our understanding of the integration and actual delivery of population health and primary care concepts and its application to an organized primary care practice
population, it begs the question of how this, or any model(s) of population-focused clinical and preventive services, can and should fit into an even broader and more integrated "systems" model supporting improvement of the health of the broader community.
Moving from the delivery model of clinical and preventive services within a staff model HMO, one might logically ask how this differs from the COPC model. The medical practice, as described, does not appear to be organized as a COPC model, although one could say that the staff model HMO is an ideal model for providing community-oriented medical care (COMC).
At the primary care level itself, the COPC concept and model attempt to extend the population-based clinical and preventive oriented primary care practice model described above by
- Defining and characterizing (a) "community" for which it has assumed responsibility to provide health care.
- Through local research the practice identifies the community's health problems.
- Modifying the (service) program in light of problems defined above.
- Monitoring the impact of the program's modification (14).
At this point one could simply conclude that community-oriented primary care is an excellent idea if the population of interest is clearly defined, if the medical practice is organized appropriately, if the financial incentives are appropriately aligned, if the policy support and community service coordination exist, if the staffing is affordable, and if the professionals are appropriately trained.
As noted earlier, the COPC model has not expanded its practice base substantially in this country beyond a relatively small number of academia-based urban practices and a number of staff-model HMOs (which place an increasing emphasis on the integration and delivery of clinical and preventive services at the primary care practice level). Observations on the state of the experiences of the COPC movement to date and shedding some light on its state are provided as follows:
A critical review of COPC applications in the United States shows that despite investigators' use of epidemiologic methods to identify important local health problems, the lack of a supportive policy environment has hampered local efforts to address these problems.
[T]he gap between knowledge about local problems and the power to achieve responsive policies has received scant attention in the COPC literature. While the efforts of COPC leaders deserve praise, optimism about the success of piecemeal approaches to local problems is less warranted than one might suppose. The situation is not likely to improve unless consistent and responsive national (state, and local) policies are put in place to support local actions (14).
Additionally, the W.K. Kellogg Foundation sponsored a demonstration project to begin 13 COPC rural practices in cooperation with the National Rural Health Association from 1989 to 1992. The Kellogg experience is summarized as follows:
the evaluation findings support previous reports in the literature of substantial impediments to the integration of COPC into primary care physician practices
for practices to play a substantial role in the COPC process, they may need to rethink their mission in very fundamental ways
another important finding relates to the (substantial) time and resources required to carry out the different elements in the COPC process
the experience of the demonstration also suggests that communities, with the support of local practices, can accomplish many COPC objectives, although this goal requires modification of COPC as it is generally conceptualized (15, pp. 489–501).
Despite substantial efforts to demonstrate its applicability and utility COPC has encountered significant obstacles to its spread, including the lack of generalized adoption as the practice and training model of choice across all primary care specialties (or at least more than family medicine alone); we should note that no one has suggested that the COPC model is inappropriate, simply suggest that the barriers to its effective implementation appear to have been too great to ensure widespread, rapid expansion to date.
Although there has been somewhat limited success of the COPC movement, one must conclude that there is still no viable model for integrating the population-based primary care practice effectively into a single population-based integrated community health care system at the general population level of the broader community, with the exception of the community-accountable and community-oriented staff model HMO, committed to the provision of COMC. Unfortunately, these models are few and far between.
Moving Toward An Integrated Community Health System: Understanding Public Health And Primary Care Interactions
In general, there does not appear to be an effective and integrated working partnership between public health practitioners and community-based primary care practitioners in the local community. This, we believe, is not very surprising for two main reasons: (a) the historical cultures of public health and primary care medicine have not placed a value on building and maintaining this relationship and (b) the historical paradigms are shifting dramatically to one of managing the per capita cost and outcomes of enrolled populations under conditions of financial risk and market competitiveness. These two observations present both a
large problem and a large opportunity for the public health and primary care communities, both of which bear significant shared responsibility for the health of populations within the community.
Because not much research has been conducted nor has much been written on the subject of this paper, we initiated discussions with a range of primary care and preventive medicine practitioners and educators and with public health practitioners and educators locally.1 Most recently, this collaboration took the form of a roundtable discussion focusing on the relationship and relative roles of primary care and public health. The resulting insights are, we believe, sufficiently significant to suggest a direction for future investigation, synthesis, and policy evaluation in this important area. The observations and conclusions of the panel are important in that they provide early practical insight into a somewhat murky area. The conclusions may not be generalizable to all communities, but on the basis of other, similar discussions, we believe that the observations will provide guidance for others.
For background information, a summary of primary care and public health perspectives is presented below, organized by general areas of concern.
Primary Care Practitioner Perspective: General Comments
There is a conceptual gap between the primary care physician and the public health professional:
- Primary care physicians are providing care to individual patients and families.
- They do not routinely stay in touch with the local health department.
- Reportable diseases are generally reported through clinical laboratories.
- Incidence and prevalence of diseases of significance to the primary care practitioner and his (her) individual practice community are often not reportable (e.g. asthma, diabetes, coronary heart disease, etc.).
- Often, therefore, the local health department does not communicate information of practical importance to the primary care practitioner's practice.
- Neither group seems to talk about the same subject, community, or population at the same time.
- Many times it seems that each interrupts the other's work flow and, in fact, makes that work even more difficult and less efficient than it already is.
It is, therefore, often difficult to believe that both are focusing on a common objective: improving the health of the same population.
Primary Care and Public Health Professionals in the Community
Both primary care practitioners and public health professionals are often marginalized in the broader health community. Knowledge-based, research-driven traditional medicine often focuses on finding and applying improved technical solutions to difficult technical problems and has attracted significant funding and public support, so it has become the focus of medical education and professional esteem. Neither primary care nor public health professionals have that focus. Both will need to recognize that they must build the better organizational, informational, and systems solutions of the future—as a team, however. These solutions will, of course, involve creation of a more efficient and effective population-focused health delivery system, integrated with more effective systems and methods for delivering primary and preventive services to individuals in a systems context.
Primary care physicians and public health professionals will need to understand that they often have much in common with each other as they develop the necessary systems solutions to difficult organization problems and as they provide the necessary leadership in these important areas to their communities and to their colleagues within the specialty medical community.
Integration of Public Health and Medicine in Education and in Practice
Integration of public health and primary care through a shared population perspective has been neither a primary focus nor an inherent value in either the primary care or public health educational and practice cultures. In practice, over many decades, neither public health nor primary care professionals have concentrated on constructing systems of mutual benefit aimed at supporting the work of the other. Both seem to have defined their own roles and methods independently of the other.
Achieving integration in community-based ambulatory medical practice requires resources (time, staff, easy and comprehensive information access, etc.) and organization that most practitioners do not have and cannot afford. Economic drawbacks to integration often make it simpler to continue to do what has been done before.
Integration of services and functions at the health department often appears nonexistent, and the system often appears to be completely compartmentalized. The shift toward a holistic outlook has already begun in primary care, but it has not yet begun in public health. Public health is still very fragmented, which is
frustrating to generalist primary care physicians. Public health appears to be a series of subspecialties as well.
If the focus of both primary care medicine and public health move to a common and synchronized educational base and operate with and from common information and support systems, providing benefit for both and for their common patients, clients, and constituents within the same population(s), we will begin to eliminate this fragmentation.
Clinical Decision Making, Public Health, Primary Care, and Managed Care
A large concern of primary care physicians has to do with the de facto determination of health policy and standards of medical practice through individual health plan or HMO reimbursement policies. Ultimately, physicians are likely to be influenced by what they are paid for. Who is determining these policies and who is accountable to the public interest for the quality of their decision-making? Who resolves policy conflicts among payers in favor of the public interest? The practicing physician and the patients are often caught in the middle. Generally, the payer with the most muscle or the one who gets there first will determine de facto clinical standards through early reimbursement policies. Perhaps the determination of general standards and the monitoring of performance against those standards of payers, professionals, and institutions should be a role of tomorrow's public health professionals, ensuring population health.
Information to Support Population Health Improvement, Health System Efficiency, and Health System Effectiveness
The increasingly rapid move to managed care in most larger metropolitan markets is forcing the management perspective of health systems, managers, and physicians to the population level. Information is the currency necessary to manage a population's health status efficiently and effectively. Population-based information is absolutely essential to define standards, to monitor performance against those standards, and to ensure public accountability over time. Managed care systems are playing the leadership role today, and state and local health departments are often sitting on the sidelines.
The community and its health providers often operate in a Tower of Babel because no one is standardizing record-keeping and information systems. This situation helps no one, particularly patients. Many providers feel that the state and local health departments or affiliated and newly formed nonprofit organizations chartered and operating in the public interest should be playing a community-wide role in leading this development. There are related roles in standardizing information systems across health plans and integrated health delivery systems and in supporting patients and families over time as they change health plans and
move through their life cycles. This sort of information tracking will be increasingly important as the population ages and as management of chronic disease and the prevention of disability become increasingly important. In short, a kinship and potential for shared perspective and values exist between public health in this context and primary care practitioners.
Information to Ensure Market Function and Health Plan Accountability
Just as broad-based population health information is essential for ensuring the quality of care—currently and longitudinally—to populations and communities, it is also essential to improve market function and the public accountability of health plans offered in the market. In short, there are issues of consumer protection that are of great consequence. If, as a matter of policy, our society continues its movement to an even greater emphasis on competitive markets for health plans, and if one of the effects of such a policy is to deemphasize the traditional public and community accountability of the not-for-profit hospital system (deemphasizing their historical community accountability role through increased reliance on nationally owned insurance-driven health plans), who will step in at the local level to assure quality and access? Many believe that this role will be increasingly important for state and local health departments or community health agencies affiliated with the health departments. It is likely to require both a major shift in perspective and a Manhattan Project to develop community standards for community health information systems, however.
Public Health, Community Services, and Primary Care
The complexity of problems seen by primary care practitioners is growing, and many problems require coordination of a complex array of community-based social, educational, support, and transportation services. It is not uncommon for primary care practitioners to interact with utility companies to ensure that a patient's home will have heat. Public health can help primary care in this area by attempting to coordinate community-based medical support, social, educational, and transportation services with the primary care community. Even simple and inexpensive steps in this area are likely to show significant improvement at the patient, family, and individual practice levels. Coordination and standardization of information flows across all of these boundaries will only help patients of primary care practitioners who are also citizens of the community (and who also vote for the mayor or governor).
Community-Oriented Primary Care, Public Health, and the Primary Care Practitioner
Today, 10 years after the publication of the IOM study on COPC, it is interesting to note the relatively small number of primary care practices and graduate medical education training programs serving a relatively small number of mostly underserved urban communities. At the same time it is significant to note a growing number of influential multispecialty group practices and staff model HMOs around the country (Kaiser, Henry Ford, Group Health Cooperative, Harvard Community Health Plan, etc.) that are increasingly incorporating COPC—like clinical and preventive patient services and management models and strategies into their primary care practices. Perhaps the message is that the focus must be broad medically, community-wise, policy-wise, educationally, and financially. This stands to reason since communities are complex and diverse themselves.
One additional note at this point must take into account the focal emphasis on COPC in a portion of the family medicine community and its relative absence in the internal medicine and pediatrics communities. Rhetorically, how can we move to COPC unless the primary care disciplines standardize training and practice models and integrate those standardized models appropriately with current systems of economic incentives and organizational design and accountability?
Primary Care Office Practice and Public Health
The primary care office is a bad place for a primary care physician to do public health. The proper tools are not available, and physicians do not have the denominator data necessary to analyze the information (even if they were trained to do it). Primary care physicians need a public health entity that has the necessary resources and the willingness to collect information relevant to his/her practice and to communicate the information it has on a timely basis to support the primary care practitioner. At the same time the local health department is often not structured to meet the public health needs of the primary care physician. As noted earlier, this leads to lack of meaningful and/or timely communication between the two groups. We need to view the two groups as part of a single system and members of a collaborative team with common objectives—improving population and community health, sharing the same information systems, and serving the same patients and populations at the same time.
Primary Care, Public Health, and Mental Health
Many of the same comments stated above apply to the mental health system's support of primary care practice as well. It is estimated that as much as 30 to 40
percent of family relations are affected by some kind of mental health, behavioral, or substance abuse problem over time. Additionally, mental health and substance abuse problems are often dealt with in discrete, but uncoordinated systems of care (community mental health centers, employee assistance programs, worker's compensation, automobile insurance, and so forth). Rarely do these systems of care interact effectively with the primary care medical care system. Perhaps the local health department could play an integrating, standardizing, and coordinating role in these areas as well. The concept here is not dissimilar to the earlier discussion about managed care.
Public Health, Primary Care, and Organizational Issues
As noted earlier, public health departments must increasingly fulfill the role of ensuring population and community health. We also noted the reality of society's movement to a health care system and service environment increasingly characterized by managed care provided in a competitive market context. In fulfilling its responsibilities to ensure the health of populations, the public health department of the future will increasingly need to play a coordinating, standardizing, and monitoring role relative to the vast array of personal health and community-based social services. This will be necessary to ensure access to populations by increasing the efficiency and effectiveness of local markets for health care services.
To accomplish this critical and mission-related objective, public health departments (or some other appropriate community health agency) assuming responsibility for ensuring access and service must assure the appropriate function of the health care market as well. One of the most important functions to be accomplished in this regard will be to ensure the standardization and availability of information to health providers and managed care organizations and to consumers—individuals, employers, and government program sponsors. To accomplish this critical function it will be particularly important for public health departments or other designated community health agencies to establish strong operational relationships with managed care organizations and with emerging integrated delivery systems, many of which are combining hospitals and primary care physicians in the same organizational structures.
These operational relationships must be based on standardized information exchange and a strong emphasis on communications. Many of these emerging systems have broader resource bases than solo or small-group primary care practices, and it may therefore be easier in many cases to emphasize the development of primary care and public health communications relationships between the health department and the medical directors of these emerging organizations. In communities where there are significant medical and nursing training activities in the area of primary care, as well as training activities in public health, it may also be important to develop ongoing communications systems, as well as to standardize
training program emphasis on primary care and preventive health services within the community.
By developing these roles and relationships it will also be easier and quicker to establish standards and to conduct health services research, to determine more efficient and effective information flows and organizational forms to improve population and community health.
Finally, significant opportunities exist for health departments, schools of public health, and schools of medicine to collaborate with each other and with these emerging systems of care—sharing in research and in training for the future. These partnerships, and those with managed care organizations and emerging integrated health delivery systems, will be critical to ensure the future health of populations and communities. Unless these relationships are properly developed and managed by health departments, on the basis of a realistic local assessment of local market conditions for health services and its future direction, major opportunities for improving population and community health will almost certainly be lost.
The above observations seem to have a single common denominator. All represent significant discontinuities at the critical interface between the traditional population- and community-based services of public health and the emerging personal care system required to provide the base of integrated clinical and preventive services—in a population and community context—essential to maintain and/or improve population and community health in this period of transition to a more market-oriented health economy. All seem to result from decades of separation of education, practice, research, professional culture, perspective, and accountability structures for the health professionals and organizations that must now increasingly work in partnership and in common organizational structures to succeed in achieving common objectives.
The implications of these observations are profound for both public health and medicine—education, practice, and research—as we approach the 21st century. In the next section, we will explore these implications and suggest a number of future directions for both public health and primary care.
Improving Community Health Through an Integrated Community Health System
We have concluded that there is a need to visualize a health care system that includes a number of elements acting as a regularly interacting or interdependent group of elements forming a unified whole, with the overall goal being to improve the long-term health of population(s). The health care system must accept significant (but not necessarily total) responsibility for this. If we accept the fact that our existing and compartmentalized independent systems of primary care and population health are not achieving this objective either efficiently or effectively, if at all, we must now begin to suggest an alternative model for the future.
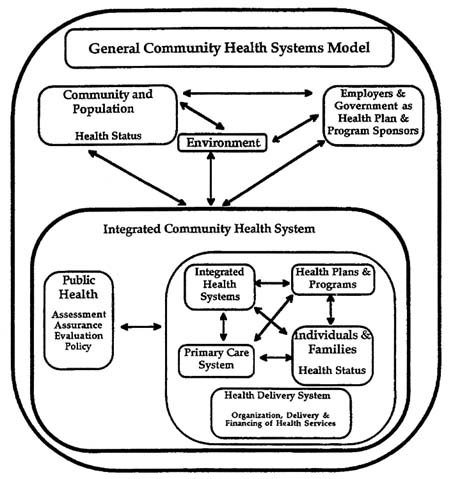
FIGURE F-3 General community health systems model.
Figure F-3 suggests the key elements, their conceptual interrelations, and their fundamental interactions within a general community health systems model.
Although Figure F-3 is somewhat complex, we believe it is generally accurate in portraying what is an inherently complex set of roles, responsibilities, relationships, interrelationships, and interactions. Perhaps this observation is important for policy makers, since it is clear that we, as a society, have not designed or accepted such a ''system" to achieve our "clearly defined objectives" efficiently. This observation, of course, begs the significant policy question of: (1) whether we should wish to; (2) the economic question of whether we must (in order to continue to obtain reasonable services at affordable cost); and (3) the
significant legal and political questions of whether we can, and under what circumstances and constraints. In any event, the development of a community health systems perspective may be the single most important conceptual reorientation necessary to ensure population and community health over time.
In evaluating such a systems concept and assuming the objective of "fulfilling society's interest in fulfilling conditions in which people can be healthy" (3, p. 7), it is important to define essential organizational requirements for optimal system performance. These may be summarized as follows:
- Objectives must be clearly defined to achieve population health status targets.
- System operating elements and critical relationships among elements must be clearly defined; responsibilities must be defined, agreed upon, and accepted; performance measurement systems defined (for the system as a whole and for each element of the system); and incentive systems must be designed to ensure that individual and system objectives are met.
- Information systems, record-keeping systems, and information access policies must be designed and standardized to support the operation and outcomes evaluation of all elements of the system individually and to support the operation and outcomes evaluation of the system as a whole.
- Population-based assessment, education, and resource services must be available as and when necessary to support the discharge of system element responsibilities. Assessment and resource services must be related to the populations for which individual practitioners and other operating elements of the system have direct responsibility.
- Ongoing programs of quality assessment must be established, as must programs of continuing improvement, including continuing education of individuals, families, community organizations, school systems, employers, health plans, and providers.
- To ensure that such a system operates effectively, it is essential to have appropriately trained personnel. Some of the training will occur within the system through the ongoing performance improvement process.
Ultimately, these integrated community health systems must depend on the educational establishment to train a broad range of health professionals (not only primary care physicians) appropriately to work in such a systems environment. In addition to any basic technical skills, educational programs must emphasize such elements as systems thinking and future orientation, how to achieve effectiveness through interdisciplinary teams, integration of diverse skills and information elements as a basis for critical analysis, organization and management skills (at varying levels of sophistication), and continuous evaluation and improvement skills.
Parenthetically, the adoption of these educational outcome objectives will
mean significant change for educational institutions and programs, for those bodies that accredit them, and, finally, for the educators, themselves.
As an old Vermonter once said, "If you don't know where you're go'in, any road'll get you there." It's a tall order for change, but a necessary one to achieve the long-term results in population health maintenance and/or improvement that we all desire.
We submit that the key elements of an integrated model have already surfaced, in pieces. They simply have not been linked, integrated, or properly supported, however. Specifically, we refer to the functions of public health as outlined in Figure F-1 and the integrated system of primary and preventive care (P&PC) for clinical and preventive services outlined in Figure F-2. When the two are combined with each P&PC and the community health agency focuses on monitoring and supporting the health improvement of the same specific populations—in an information environment defined and supported through an integrated community health information network and in a context within which the health status impacts of improvements in environmental and occupational health policy and programs are understood and integrated (even if these policies and programs are not, as is most often the case, under the control of the health department)—a model for an integrated community health system emerges, as outlined in Figure F-4.
We note that such a system does not require a merged financial, business, or operating organization. It simply organizes and standardizes the market environment within which population-based providers will function. To this end it also standardizes technical, educational, marketing, and evaluative information flows within the market, thus leading to higher levels of public accountability and more efficient market function. Note that this model emphasizes accountability to the community for the overall functioning of the market for health insurance and for the results in terms of population health improvement, provider coordination, and consistency of public expectations.
With such a system in place and with proper attention paid to policy objectives and public accountability, its ultimate operation can only be positive relative to the dilemma presented by the "iron triangle" of cost containment, quality, and access noted by Kissick (Figure F-5).
Finally, the perspective of all systems elements is moved to the population(s) served within the community through its various health plans. Once the system is organized from the population perspective, health status expectations and accountabilities are established, the infrastructure providing universal provider access to standardized information on a real-time or other timely basis is in place, and the capitated reimbursement mechanisms and per capita performance measurements and operating systems are developed and aligned, the overall system should begin to work much more effectively than today's system does to improve the health of the community and its populations.
Although it is important to begin our overall recommendations with a general
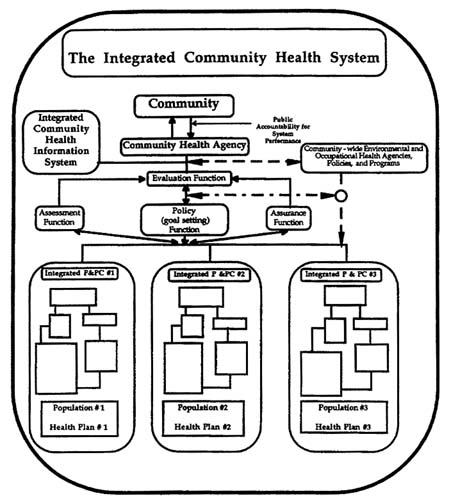
FIGURE F-4 The integrated community health system.
model, we are under no illusions regarding the difficulty of realigning the system to produce this result. We would simply note that if society as a whole and our political and commercial systems, specifically, want the nation's (public and population) health system to produce the results that can be achieved through a simultaneous and synergistic reorganization of the public health and primary care systems—operating in a capitated and competitive market context—we will need to move in this direction.
As public and purchaser dissatisfaction with increasing health costs and the
FIGURE F-5 Cost containment, access, and quality.
diminishing value per dollar spent on health care or on taxes required to support publicly sponsored health care programs increase, changes of this kind are more likely to occur. This will be exacerbated by an increasing public recognition and understanding of the importance of environmental and occupational health programs on personal, family, and community health status. These feelings are likely to occur and intensify over time, because an increasingly unstable combination of popular dissatisfaction, political pressure, and increasing purchaser concern will create an environment forcing more and more dramatic systemic change.
Future Directions And Issues For Consideration For Health Policy, Public Health, And Primary Care: Moving To Tomorrow's Integrated Community Health Systems
Although it is important to create a vision for the future, it is also important to offer suggestions for the present. Many of these suggestions, of course, come directly from observations presented earlier.
- Legislators (federal, state, and local) and health departments (local and
- state) should move from a categorical focus to a population focus. This simple move would do more to reorient the entire health system than many other steps that could be taken.
- Health departments and affiliated community-accountable not-for-profit entities should assume leadership roles in the development of community health information networks (CHINs). They should also assume responsibility for the standardization of data transfers and automated record information required for entry into the CHIN.
- Health departments should develop a service perspective and mentality to serve the primary care system, integrated health provider networks, and emerging managed care organizations. Specifically, many of the difficulties noted earlier had to do with the lack of communication, the difficulty of communicating, and the categorical nature of health department responsibility assignment versus population- or community-focused responsibility assignment.
With personnel assigned to serve populations, the providers (hospitals and medical providers) and the health plans serving those same populations and focusing on the same populations and communities, there is a much higher likelihood of improved health outcomes for little or no additional expenditure of funds. - Health departments working collaboratively with providers and health plans should make greater efforts to coordinate community services affecting community health status (e.g., health aspects of social and educational services) and to offer this as a service to primary care providers within the community and to managed care plans. The net effect of this action would be to support the community and population service responsibilities of providers and health plans and to support the community served by the health department.
- Although health departments should take the lead in ensuring the development of publicly accountable CHINs, it will be important to develop the networks in such a way as to facilitate and encourage the functioning of the competitive market for health insurance and competition on the basis of cost, quality (including service), and access among competing health plans and providers. From a public policy standpoint, this should have the effect of improving quality and reducing cost over the long run. This strategy will also support cultural values of entrepreneurism, pluralism, and independence on the one hand, while it will provide necessary public accountability and market facilitation services on the other.
- Just as federal and state legislators and state and local health departments can move to a population and community perspective on their own volition, such a move would be facilitated by coordinated decisions of federal agencies responsible for assessment programs (Centers for Disease Control and Prevention [CDC] the Environmental Protection Agency, etc.) and for program organization and reimbursement (Health Care Financing Administration, CHAMPUS, etc.) to change their views to a population and community perspective, building the capabilities of the state and local health department infrastructure and policy
- apparatus to assume the population-based management and information network management responsibilities suggested above. It should be noted that a relatively "simple and coordinated" federal policy decision of this sort will accelerate reorientation of the entire public health and primary care systems.
- A simpler step to assist health departments to reorient their perspective would be for CDC to require state and local health departments to report statistics by population segments aligned by logical primary care markets and service areas. Aligning the statistical perspective of markets and service areas, disease prevention and control, and primary care will ultimately realign the perspectives and ongoing communications patterns of population health and primary care professionals. Noted, at this point, is the fact that multiple health plans and primary care systems will likely serve each primary care market area. In spite of this fact, however, the alignment of health statistics will be of greater assistance to all involved in problem identification, solution implementation, and ongoing assurance activities.
- Health departments should build collaborative service relationships with managed care plans and integrated health delivery networks to provide population- and community-focused continuing education programs in the areas of prevention to primary care providers within their networks. This action taken in concert with several of the actions noted above should build positive relationships and improve primary care system communications.
- In defining the "primary care system" we must be certain to include a broad base of community-based practitioners, all of whom provide some aspects of "primary care'' to a community's residents. These will include dentists, physical therapists, nurse practitioners and midwives, pharmacists, sports medicine physicians, visiting nurses and other home care professionals, and psychologists, among others. Of course, some of these practitioners practice in association with primary care physicians; others do not. In any event, communityand population-based primary care information systems and coordination systems must ultimately capture the activities of these practitioners if the picture of our "community primary care system" is to be complete.
- Most of the primary care physicians consulted complained of the significant amount of time "wasted" in processing paperwork. On the other hand, the public health system requires high-quality, timely, and complete information to discharge its community assessment, evaluation, assurance, and policy roles appropriately. With proper attention to the development of standards for record-keeping and for electronic information transfers and with the role of facilitating the development of such systems, it is likely that the efficiency and effectiveness of the primary care system would be improved significantly. The assessment, evaluation, policy, and assurance functions of the health departments would be improved substantially as well.
- As populations throughout the nation diversify in terms of language and culture, primary care practitioners need assistance in serving those populations.
- This is particularly true from a community health education perspective and from a cultural sensitivity perspective. With public health and primary care practitioners aligning their perspectives on the same populations, it is more likely that these important issues will be addressed more effectively.
- Health departments and primary care providers cannot align their perspectives on populations and ignore issues of mental health, behavioral issues, and substance abuse issues. Although the mental health system often functions independently of both, it must be effectively integrated with the primary care system if the health of populations is to improve.
- Health departments should develop a service focus by placing high-quality, population-related, and timely surveillance and environmental data on electronic data systems easily available to primary care providers. By providing them with more and more relevant services, long-term communications and relationships should be enhanced.
- The federal and state governments, health departments, schools of public health, schools of medicine, managed care plans, and integrated provider networks should place a greater emphasis on organizational research, health services research, information systems research, and health policy research to improve the population health system. Without such a commitment to improving the organization and financing of the delivery system, we will not be able to move as swiftly to improve primary care system functionality.
- Governing authorities involved with the accreditation of primary care residency training programs (specifically, family medicine, internal medicine, and pediatrics), working in partnership with interested private foundations and with public health leaders, should develop recommendations for a standardized model for training primary care physicians (including training in population health concepts and skills) and for encouraging schools of public health to train population health professionals in the skills and methods previously outlined to support the community practices of primary care physicians. Both should be trained in team settings to work collaboratively and longitudinally to improve the health of the populations commonly served.
Additionally, arrangements must be made to train and/or retrain existing primary care providers in the elements of population-based and preventive medicine. Overall, the training and retraining needs of health professionals will be significant, and they will be critical to the ultimate success of the program, as ultimately defined. The importance of adopting such principles by the Council on Graduate Medical Education and other accrediting bodies for graduate and continuing education of primary health professionals cannot be overemphasized. - A significant practical and policy question involves the mechanisms which must be contemplated to move to the type of model suggested herein, particularly considering the extremely powerful market forces involved and the extraordinarily powerful local and state political positions of large health plans. It seems to us that change of this magnitude must be facilitated nationally, perhaps
by setting national data transfer standards, assignment of certain monitoring and assessment responsibilities under federal health care programs (Medicare, Medicaid, Federal Employee Health Benefits Program, and CHAMPUS) to state and local health departments or specially chartered community benefit organizations, etc. In short, the federal government can use its market power to define the structure of the future system and its accountability mechanisms. If the federal programs define the need for these changes in a clear, coordinated, and consistent way across all markets, the markets and their supporting structures will change, and will do so in a relatively short period of time.
Most of the suggestions presented above call for fundamental change at the individual program or health department level. This arises from the dramatic changes in the markets for health services and in the significant restructuring, already under way, of our primary care provider, health plan and integrated community health delivery systems. Transformation of their structure, perspective, and financing affects public health by creating an even greater imperative for a conceptual reorientation in that area. Both public health and primary care providers must therefore seek and move together to a new paradigm in which both are collaborators and teammates, developing and operating from the common perspective of the population(s) that the two of them jointly serve. In this light they also must serve each other, if the health of their population(s) is to improve.
One overarching and additional important observation must be made at this juncture, however. The preceding suggestions tend to assume that all citizens have required access to the necessary clinical and preventive services through organized plans of care. Unfortunately, this is not the case, and the situation appears to be worsening as the nation's employer-based health insurance system encounters the stresses and strains of international competition. One is led to an unavoidable conclusion. If we accept the premises inherent in this paper, we must also move to ensure appropriate access to clinical and preventive services for all. This conclusion begs the question of the responsibility for financing such access, which could occur at each, or a combination thereof, of the federal, state, county, city, and community levels of jurisdiction on either a publicly funded or voluntarily funded (or a combination of both) basis.
Although it may seem that a number of new roles are being suggested for government and it may, in fact, be the case, many feel that government is the only entity that can rationalize the market and the rules of the game. In short the roles suggested are for rulemaker, honest broker, standardizer, market facilitator, and community quality ensurer. All of these roles are essential if public health and primary care are to improve the health of populations. Government in some form (or affiliated, publicly accountable entities) may be the necessary vehicle to ensure population health. It is important to note above all that this paper conceptualizes a clear separation between the appropriate role of government in the
foregoing facilitation capacities and the appropriate role of government as a payer and, if necessary, as a provider.
If the changes suggested herein are adopted or largely adopted in communities, we will have effectively moved to COPC. We have concluded that the COPC model requires the following elements to ensure widespread adoption and success:
- Access to and support of local and state health policy structures and mechanisms, with broad support of national health policy.
- Broad bases of organizational support to provide and fund necessary staff support, including more highly organized forms of medical practice (e.g., comprehensive primary care group or multispecialty group practice forms of organization).
- Capitated revenue flows to align incentives and to support development of clinical and preventive service structures.
- Access to comprehensive, automated information flows and structures, integrating to the maximum extent information regarding community health issues, risk factors and risk behaviors, and longitudinal clinical information.
- Greater integration of primary care training supporting the COPC model or at the minimum the integrated clinical and preventive services model.
The importance of the availability of good information to support population (county) based primary care was noted by Lashof, above, and additionally by Barbara Starfield:
The development of technology for collecting and processing information will certainly facilitate achievement of the initial steps in COPC. Improved medical technology will expand the definition of health needs; as existing problems are solved, new challenges at another level of need will emerge. Community-oriented care may not be achieved everywhere, or to the same degree in all places. But the concept is now appropriate for consideration as the challenges of the twenty-first century approach. (16, pp. 194-195).
The changes suggested herein are simple and complex at the same time. Mutual changes to a population perspective, service orientation, organizational structure, communications skills and patterns, and rapid movement to a modern information technology base to support population health improvement will lead us where we need to go. Several of these issues were addressed by Joyce Lashof in her 1991 Plenary Address to the AHCPR Conference on Primary Care Research:
spectrum of community health problems is more difficult initially but in the long run far simpler than developing separate programs for each risk factor and disease. … We must experiment with new models that break out of the categorical mode, and we must develop the methodologies for evaluating the impact of programs on the health of populations … the development of a true partnership
between public health and primary care remains an unrealized goal. Yet such a partnership is essential if we are to achieve the goals of Healthy People in the Year 2000 (8) to mount a county-wide effort to integrate medical care and public health across the
The question is, of course, familiar—will we have the leadership vision and fortitude, the management skills, and political will to move there and in time?
Finding Our Way: The Leadership Challenge
Throughout this paper we have suggested the need for a paradigm shift to improve the health of populations by restructuring the relationship between public health and primary care, as the nation's health care system itself is in the process of restructuring. In fact, we have suggested ways in which the population health system (the public health and primary care team) can work together to assist communities (society) in fulfilling their interest in ensuring conditions in which people can be healthy. This is, of course, the mission suggested by IOM in 1988 (3). Having said this, however, we must acknowledge both the degree and completeness of the change required for state and local public health departments to support our evolving market-oriented structure, particularly in the case of those populations categorically supported for the past 50 years and for those populations for which public health has been the "provider of last resort."
Ultimately such a vision and the required reorientation of existing large bureaucratic structures, a task analogous to turning a huge, lumbering oil tanker in a very short distance, is unachievable without four vital resources: political vision combined with appropriate amounts of courage, and willing and appropriately trained personnel and committed leadership supported by adequate resources. To this end the challenges for the nation's schools of public health, medicine, nursing, and allied health professions have never been greater. Just as it is necessary for public health and primary care practitioners to form a population health team, it will be necessary for these professional schools to form their own educational teams to teach population health and to reorient their perspectives and those of their colleagues within the university. The task is daunting, but essential.
Although critically important, the subject of resources may be easily addressed, in the relative and conceptual senses. If the suggestions outlined earlier relative to using existing federal program resources to define system requirements in the areas suggested herein are used, many, if not most, of the required resources to support the reorientation can be provided efficiently through that method. It will take a change of this sort and magnitude, however, to accomplish the task.
The subject of leadership deserves special attention, however, and may turn out to be the most significant question of all. We were particularly taken with a recent report from the Milbank Memorial Fund "Leadership in Public Health"
(17). In that report Molly Coye, William Foege, and William Roper each discuss different aspects of public health leadership and conclude that public health leadership must, in many ways, reinvent itself. Perspectives must be changed to become more global and to measure effectiveness over longer periods of time and to develop new systems and strategic thinking skills, as well as organizational and political skills, team management, and motivational skills (18). This is a tall order for any profession.
We share their concerns, yet we would submit that leadership development to support population health improvement paradigms is critical for primary care and public health professionals alike if our nation's ambitious, long-term goals are to be achieved and its substantial long-term challenges are to be met. In this regard, it will be most important to create a common vision of a system such as we have proposed and a clear understanding of their individual roles and of their shared and collaborative roles within such a system required to achieve its single objective improving the health of populations.
The Integrated Community Health System: Clinical And Preventive Personal Health Services Provided In A Community Context From An Integrated Perspective
The recommendations of this paper challenge all of us to adapt our thinking to the market-based and community health-oriented realities of the years ahead. Whether or not any of us agree with such an evolution, the challenge for all will ultimately be how we will work collaboratively to make such a system work to improve the health of populations and communities. At the same time all will have to work collaboratively to ensure appropriate access to service.
The move to an integrated system of care such as that suggested in this paper is not without significant risks and difficulties. We suspect that the perspectives of population health professionals and personal health professionals will continue to exhibit tensions vis á vis priorities and resource allocation. To a large degree this is healthy. It is healthiest, however, when these perspectives operate within the same organizational and accountability structure—whatever that may be. It is also healthiest when these tensions are acknowledged as being appropriate to reach the best result for the populations and communities served—and when those populations and communities have a significant voice in guiding the decision processes of the organizational structures within which these critical decisions are made.
Increasingly, we will see the tensions evolving between the publicly accountable and voluntary components of our community health systems and the investor-owned (and non-community-oriented) elements serving our community health needs. We believe that these tensions can be appropriately managed to produce a positive health result for the community. We also believe, however,
that we may have to seek or develop new organizational methods and public-private political structures to balance the competing requirements of community and shareholder accountability. It is entirely possible that the growing complexity of our communities, combined with the increasing recognition of the need to develop new ways to bridge the public-private chasm will lead us in the directions of exploring Schauffler's Community Based Health Promotion and Disease Prevention (CBHPDP) partnership concept, referenced earlier (6).
In any event, Schauffler recognizes the complexity of organizing the complete spectrum of community-accountable population-based and personal services required to create an environment within which health can be assured. Thus, a community, in the context of CBHPDP, is defined by its people, institutions organization, and locality.
Many of our communities are experiencing growing economic, cultural, and ethnic diversity; significant inequities in health status have accompanied this diversity. As a result, it is imperative that we recognize the important role communities must play if we are to improve and maintain the health status of our population. Two choices are available: (1) we can continue down the current path and support models that fragment care and focus only on the individual as the unit of prevention interventions, thereby risking an increase in the health status gaps that exist between the most advantaged and disadvantaged subgroups of our population; or (2) we can build a model for the twenty-first century that recognizes the diversity of our communities by developing a multidisciplinary, intersectoral approach that encourages and supports the significant role communities can and must play in promoting health and preventing disease (6, p. 9).
The difficulty of achieving this result and of reconciling the tensions described above between the community-accountable and non-community-accountable components of our integrated health system must not be underestimated. Ultimately, this is a problem that must be solved through our political system—local, regional, state, and national.
As we survey the path suggested in this paper, we ask, will it be risky to move in the direction(s) suggested? Ultimately, we also ask, will it be even more risky to make no movement at all?
References
1. IOM. Community Oriented Primary Care: A Practical Assessment, Vol. 1. The Committee Report. Washington, D.C.: National Academy Press, 1984.
2. IOM. Defining Primary Care: An Interim Report. Washington, D.C.: National Academy Press, 1994.
3. IOM. The Future of Public Health. Washington, D.C.: National Academy Press, 1988.
4. Partnership for Prevention. Prevention Is Basic to Health Reform: A Position Paper from an Expert Panel. Washington, D.C.: Partnership for Prevention, March 1993.
5. Lashof, J. Public Health and Prevention. Presented at Public Health Agencies and Managed Care: Partnerships for Health Conference, Atlanta, Ga., 1994.
6. Schauffler, H. H. Health Promotion and Disease Prevention in Health Care Reform . American Journal of Preventive Medicine 10(5)(Suppl.), 1994.
7. USPHS. For A Healthy Nation: Returns on Investment in Public Health . M. Gold and S. Teutsch, project co-directors. Washington, D.C.: U.S. Government Printing Office, 1994.
8. Lashof, J. Public Health and Primary Care. Pp. 323–330 in AHCPR Conference Proceedings: Primary Care Research: Theory and Methods, M. Grady, ed., Publication No. (PHS) 91-0011. Rockville, Md.: U.S. Department of Health and Human Services, 1991.
9. Rundall, T.G. The Integration of Public Health and Medicine. Frontiers of Health Services Management 10:3–24, 1994.
10. McGinnis, J.M. and Foege, W.H., "Actual Causes of Death in the United States." Journal of the American Medical Association 270:2207–2212, 1993.
11. Kissick, W. L. Medicine's Dilemmas: Infinite Needs Versus Finite Resources. New Haven, Ct.: Yale University Press, 1994.
12. Lee, P.R. Re-Inventing Public Health, Shattuck Lecture, Massachusetts Medical Society, 1994 Annual Meeting. Boston, Mass., May 21, 1994.
13. Thompson, R.S., Taplin, S.H., McAfee, T.A., Mandelson, M.T., and Smith, A.E. "Primary and Secondary Prevention Services in Clinical Practice: Twenty Years' Experience in Development, Implementation, and Evaluation. Journal of the American Medical Association 273:1130–1135, 1995.
14. Waitzkin, H. And Hubbell, F.A. Truth's Search for Power in Health Policy: Critical Applications to Community Oriented Primary Care and Small Area Analysis. Medical Care Review 49:161–189, 1992.
15. Kukulka, G., Christianson, J.B., Moscovice, I.S., and DeVries, R. Community Oriented Primary Care: Implementation of a National Rural Demonstration. Archives of Family Medicine 3:495–501, 1994.
16. Starfield, B. Primary Care: Concept, Evaluation, and Policy. New York, N.Y.: Oxford University Press, 1992.
17. Coye, M.J., Foege, W.H., and Roper, W.L. Leadership in Public Health. New York, N.Y.: Milbank Memorial Fund, 1994.

































