2
Evolution of School Health Programs
HISTORICAL OVERVIEW
Schools have been the focus of numerous and varied efforts to promote and secure the health of American children and young people since the colonial era. In its interim statement, the committee reviewed some of the historical aspects of school health programming to provide a context for its definition of a comprehensive school health program (CSHP) and a background for identifying issues to be examined in the committee's study. The following section extends that review. An understanding of the evolution of school health programs gives insight into how educational, political, and societal issues—as well as health issues—have influenced these programs over the years and provides lessons for the future development of school health programs.
School Health Through the Early Twentieth Century
During the colonial period, only limited attention was paid to any aspect of school health. Benjamin Franklin advocated a "healthful situation" and promoted physical exercise as one of the primary subjects in the schools that were developing during his time. Samuel Moody, headmaster of the Dummer Grammar School, which opened in 1763 as the first private boarding school, taught the value of exercise and participated in it himself. Prior to the mid-1800s, however, public education was still in a formative stage and efforts to introduce health into the schools were iso-
lated and sparse. It was not until 1840 that Rhode Island passed legislation to make education compulsory, and other states soon followed (Means, 1975).
School health professionals often state that the ''modern school health era" began in 1850 (Pigg, 1992). In that year, the Sanitary Commission of Massachusetts, headed by Lemuel Shattuck, produced a report that had a significant impact on school health and has become a classic in the field of public health. Shattuck served as a teacher in Detroit and as a member of the school committee in Concord, Massachusetts, where he helped reorganize the public school system. His background led to school programs receiving major attention as a means to promote public health and prevent disease (Means, 1975). The report states the following:
Every child should be taught early in life, that, to preserve his own life and his own health and the lives and health of others, is one of the most important and constantly abiding duties. By obeying certain laws or performing certain acts, his life and health may be preserved; by disobedience, or performing certain other acts, they will both be destroyed. By knowing and avoiding the causes of disease, disease itself will be avoided, and he may enjoy health and live; by ignorance of these causes and exposure to them, he may contract disease, ruin his health, and die. Everything connected with wealth, happiness and long life depends upon health; and even the great duties of morals and religion are performed more acceptably in a healthy than a sickly condition.
Soon after the release of the Shattuck report, the medical and public health sectors began to recognize the role that schools could play in controlling communicable disease with their "captive audience" of children and young people. For example, even though a vaccine had been developed years earlier, smallpox continued to strike well into the latter half of the nineteenth century, due to the constant influx of new immigrants and the mobility of the population. When New York City was faced with an outbreak of smallpox in the 1860s, no mechanism was in place to provide free vaccinations to those who needed them, so the Board of Health turned to the schools. Education officials agreed to permit inspection of school children to determine whether or not they had been vaccinated, and in 1870, smallpox vaccination became a prerequisite to school attendance (Duffy, 1974).
Although the schools of this period had the potential to confront and control communicable disease, no doubt they also contributed to the spread of disease. In the late 1860s and early 1870s, the New York City Board of Health instituted a program of sanitary inspections of all public school twice a year. These inspections revealed a filthy environment and excessive crowding. Modern plumbing was nonexistent, and schools were sometimes overrun by rats. Frequently, more than 100 students occupied
a single small classroom, with two or three children sitting at the same desk. Classrooms lacked ventilation and fresh air, a problem exacerbated by using stoves for heating and gaslights for illumination. These problems continued in New York City even into the early twentieth century, and no doubt the situation was not unique to New York (Duffy, 1974).
The era of school "medical inspection" began in earnest at the end of the nineteenth century (Means, 1975). In 1894, Boston appointed 50 "medical visitors" to visit schools and examine children thought to be "ailing." By 1897, Chicago, Philadelphia, and New York had all started comparable programs, and most of the participating medical personnel provided their services without compensation. The success of these early programs developed into more formalized medical inspection. In 1899, Connecticut made examination of school children for vision problems compulsory. In 1902, New York City provided for the routine inspection of all students to detect contagious eye and skin diseases, and employed school nurses to help the students' families seek and follow through with treatment. In 1906, Massachusetts made medical inspection compulsory in all public schools, a step that ushered in broad-based programs of medical inspections in which school nurses and physicians participated. Legislative mandates became the means of ensuring medical inspections, and legislation continues to this day to be the basis for many elements of school health programs.
Around the turn of the century, the role and advantages of school nurses began to be recognized. In 1902, Lillian Wald demonstrated in New York City that nurses working in schools could reduce absenteeism due to contagious diseases by 50 percent in a matter of weeks (Lynch, 1977). For minor conditions, nurses treated students in school and instructed them in self-care. For major illnesses, nurses visited the homes of children who had been excluded from school because of illness or infection, educated parents on their child's condition, provided information on available medical and financial resources, and urged the parents to have their child treated and returned to school. School nurses began to assume a major role in the daily medical inspection of students, treatment of minor conditions, and referral of major problems to physicians. By 1911, there were 102 cities employing cadres of school nurses. In 1913, New York City alone had 176 school nurses (Means, 1975). This expansion of the role of school nurses freed physicians to spend more time in conducting medical inspections of individual students with recognized needs rather than in inspecting entire classes.
Medical inspections in the early part of the century were no doubt perfunctory and superficial. For example, in New York City in 1904, it was reported that 8,261,733 examinations were given and 515,505 students were treated by school nurses and physicians, yet the total number
of medical inspectors was only 50! Another factor reducing the effectiveness of medical inspections was the Victorian attitude toward exposing the body. As late as 1914, school inspectors were not allowed to touch children, and inspections were done with children fully clothed. In 1915, the New York Board of Education introduced a new requirement that all children entering school must undergo a physical examination without clothing. This requirement met some resistance, with critics declaring it immoral to strip children for medical purposes and asserting that school physical examinations were an intrusion and a "violation of personal liberty, and hence contrary to the principles of a free government" (Duffy, 1974).
The prevalence of tuberculosis in the United States had a significant impact on school health during the early part of the century. Particularly notable was the development and spread of "open-air classrooms"—wide open to the outside air, even in the middle of winter—in all major cities, under the supervision of both medical and education personnel. In 1915, the National Tuberculosis Association enlisted school children in the Christmas Seal drive. A child who bought or sold 10 cents worth of seals was enrolled as a "Modern Health Crusader" and received a certificate with four "health rules." Crusaders also kept a personal record of how well they carried out 11 daily "health chores.''1 In the first year of the program, 100,000 children became "crusaders," and the drive was endorsed by the National Education Association and the National Congress of Parents and Teachers (Means, 1975).
Throughout the late nineteenth century and early twentieth century, the temperance movement also had an influence on school health programs, stressing that children should learn about the effects of alcohol, tobacco, and narcotics on the human system. As a result of this effort, a
majority of states passed legislation mandating such instruction, which was often incorporated into the physiology and hygiene curricula. Physical training—commonly called "gymnastics"—also began to be introduced into schools during this period. The early leaders in the physical education movement had medical degrees, and there was much discussion about the new profession of physical education being a blend of the medical and educational fields. Physical training was often associated with instruction in temperance and hygiene; other topics of focus in the early years of physical education included anthropometrical measurement, gymnastic systems, athletics, folk dancing, and military drill—although military activities fell out of favor around the turn of the century (Lee and Bennett, 1985).
The range of school-linked health services was broad in the early twentieth century, and school-based medical and dental clinics sprang up to provide services, especially to indigent students. These services were sometimes overpromised and touted as a panacea for eliminating school failure and delinquency, providing equal educational opportunity, and reaching parents to make them more responsible citizens. Although free school clinics were frequently denounced by the medical establishment as socialized medicine, dentists tended to support free school dental clinics. Many dentists considered children to be "troublesome patients; moreover, parents demanded lower fees for children's care, and they often refused to pay the dentist's bill for that care" (Tyack, 1992).
The extent of the medical services provided was so broad that sometimes even minor surgery was performed in schools. For example, in New York City in 1906, when the parents of large numbers of children who needed their tonsils and adenoids removed could not afford carfare to the nearest dispensary, several volunteer physicians performed this surgery on 83 children at Public School 75. Unfortunately, a rumor subsequently spread that "school doctors were slitting the throats of school children as a prelude to a general massacre of the Jews," and several riots resulted. These riots were found to be instigated by the "snip doctors," private physicians who performed the same surgery for a fee and resented the schools doing the work for free (Duffy, 1974).
In the period between the 1890s and World War I, the impetus for many health and social services in education came from outside the schools. In the 1890s, schools in Boston and Philadelphia were early pioneers in establishing cooperative programs with philanthropic organizations to provide school lunches to fight malnutrition and hunger and their consequent effect on learning. In many cities, women's clubs provided school meals, transportation, and special classes for sickly or handicapped children, as well as education and recreation programs during the sum-
mer and out-of-school hours. Settlement-house workers developed model programs for social work and for vocational counseling, generally staffed by volunteers or supported by charitable contributions. Visiting teachers, the forerunner of school social workers, worked with families—especially immigrant families—to help them adjust and to find needed resources and worked with educators to help them deal with the greater diversity of students coming into the classroom. Vocational guidance counselors, the forerunners of school guidance counselors, attempted to link students with jobs and to connect the school with the overall economy (Tyack, 1992).
School Health from World War I to the 1960s
World War I marked a turning point in the history of school health programs. Prior to this period, programs had a narrow focus emphasizing inspection, hygiene, negative messages, and didactic instruction about anatomy and physiology. However, the advent of the war made the problems of poverty more visible: malnutrition, poor physical condition, and the abysmal state of the health and welfare of many of the country's children. New health promotion philosophies and movements began to spring up to replace the outmoded methods; these new approaches were based on using motivational psychology and an understanding of behavior. During the years immediately following World War I, the image of modern school health programs began to emerge.
The Influence of Reports and Publications
Following World War I, the Child Health Organization was one of the most active groups devoted to the health of children, and the organization conducted "a nationwide campaign to raise the health standard of the American School Child." This distinguished group began as an outgrowth of the Committee on War Time Problems of Childhood, and its members were leaders in the fields of medicine, education, public health, psychology, and other arts and sciences. The organization's primary focus was on the development of improved health practices, and its approach was enlightened and progressive. Recognizing the motivating effect of stimulating students' interest, the organization promoted a positive approach to health and influencing behavior. It printed and distributed teaching materials for students, provided speakers, and published a large volume of material on school health. In 1922, in collaboration with the U.S. Department of the Interior and the Bureau of Education, the organi-
zation published and widely distributed The Rules of the Health Game 2 (Means, 1975).
In 1918, the Commission on the Reorganization of Secondary Education of the National Education Association (NEA) published the pivotal report The Cardinal Principles of Secondary Education. This report established a new framework for contemporary secondary education in the United States and listed seven main objectives of education: health, command of fundamental processes, worthy home membership, vocation, citizenship, use of leisure, and ethical character (Commission on the Reorganization of Secondary Education, 1981). The NEA had also joined with the American Medical Association (AMA) in 1911 to sponsor what would be for more than a half century one of the most influential groups in the development of school health: the Joint Committee on Health Problems of the National Education Association and the American Medical Association. Prior to 1920, this group published the report Minimum Health Requirements for Rural Schools. The Joint Committee strongly promoted the emerging concept of coordinated effort for health in schools. In a 1927 paper, Health Supervision and Medical Inspection of Schools, the group declared (Means, 1975):
As yet, states have been slow in providing for coordination between the medical service or supervision, the physical education, and health education programs. Such a step is necessary for the proper functioning of any program of health supervision.
It is ironic that almost 70 years later, coordination of these programs is still considered lacking.
Early in the 1920s, the NEA–AMA Joint Committee on Health Problems in Education reported the results of a nationwide survey of the status of health education in 341 city schools. The findings are particularly interesting in light of the current U.S. Public Health Service's Healthy People 2000, which calls for this goal: "Increase to at least 75 percent the
proportion of the nation's elementary and secondary schools that provide planned and sequential kindergarten through grade 12 quality school health education" (U.S. Department of Health and Human Services, 1991). In the 1920s, more than 73 percent of the surveyed schools taught health directly under the name of "health" or "hygiene,'' while 108 cities reported correlating content in their health curriculum to such other subjects as language, civics, reading, physical education, general science, and art. Daily inspection for health habits was reported by 69 percent of the 341 cities, and nearly 30 percent of elementary schools reported having organized student clubs for the promotion of health (Means, 1975).
In 1928, the Sixth Yearbook of the Department of Superintendents of the National Education Association outlined the following content guidelines for health education (Means, 1975):
-
Mental hygiene must be emphasized and protected.
-
The establishment of health habits depends upon the pupil's understanding something of the function of his own body.
-
A discussion of the causes of disease merits a place in the secondary school program.
-
A thorough study of nutrition should be placed in the upper grades.
-
Posture should be emphasized.
-
The hygiene of the home should be taught.
-
Sex hygiene cannot be overlooked.
School health became the focus of a variety of agencies and professional organizations between the 1930s and 1960s, and many important documents emphasizing a range of health issues were published during this period. Nationally and at state levels, maternal and child health agencies sponsored numerous conferences to improve school health services by linking them to other community health efforts. Particularly significant health education reports include Suggested School Health Policies, published by the National Committee on School Health Policies of the National Conference for Cooperation in Health Education, and Health Appraisal of School Children, published by the NEA–AMA Joint Committee on Health Problems in Education. Other agencies and organizations publishing important reports on school health during this period included the U.S. Public Health Service, the U.S. Office of Education, the American Association of School Administrators, and various affiliates of the National Education Association (Means, 1975).
School health services research was also under way during this period and resulted in the publication of reports on such topics as staffing patterns for school health services, effective strategies for referral and
follow-up of students with positive screening results, and the beneficial impact of nursing services on school attendance.
The Nature of School Health Programs from World War I to the 1960s
Between 1918 and 1921, almost every state enacted laws related to health education and physical education for school children (Kort, 1984). During the following decades, the health education curriculum became stabilized and more fully developed. Topics such as nutrition, personal health habits, diseases, exercise, alcohol and tobacco, family health, and sex education became common. The importance of the cooperation of schools with other community agencies and of parental involvement became increasingly acknowledged. The significance of the health of the teaching force became recognized, both so that the teachers would be able to cope with the demands of the job and so that they could better serve as role models of health and vigor for the students (Means, 1975).
Safety problems and conditions that surfaced during World War I stimulated the scientific study of safety and the introduction of safety into the school environment and curriculum. Fire drills began to be prescribed, and safety instruction included such topics as fire prevention, traffic safety, and bicycle safety. Increasingly, safety education became integrated into classroom health education (with the exception of driver training, which developed later and is often organized and staffed separately).
When many of the World War I draftees failed their physical examinations, there was a move to require physical education "without military features" in schools in an attempt to improve the physical condition of children and young people (Lee and Bennett, 1985). Similarly, when many World War II draftees were found to suffer from nutritional deficiencies, the federal government in 1946 passed the National School Lunch Act to provide funds and surplus agricultural commodities to assist schools in serving nutritious hot lunches to school children. It was not until 1966, however, that a pilot school breakfast program was established, and the program was not made permanent until 1975.
School-based medical inspections and screening continued into the 1930s, but typically there was a lack of follow-up to correct defects. In an attempt to remedy the situation, in 1936, in New York City Board of Education set aside a day as Health Day, during which teachers checked children's height, weight, vision, hearing, and teeth. Teachers then had the responsibility for trying to get any defects corrected (Duffy, 1974). Unfortunately, the teachers' work duplicated the efforts of the Health Department. In response, New York City devised the Astoria Plan, an experimental program designed to coordinate all school health services and eliminate duplication; this plan is discussed in the next section.
During this period, the NEA–AMA collaboration defined the role of schools in providing health services. Health services should focus on the prevention of health problems through conducting screening activities, establishing a healthful environment, providing for immediate care in the instance of problems, and referring children to professionals and facilities that could handle more complex health problems. Many school systems had physicians coordinating the health service programs. It was assumed that most students had family doctors for primary care services, and the appropriate role of schools was to inform parents of problems and advise them when it was necessary to take their children to the doctor. Although collaboration between the medical and educational sectors occurred throughout this period, clearly boundaries were also being established to limit the range of health services that should be available in schools (Lynch, 1977; Walker et al., 1990).
This philosophy of discouraging the delivery of primary health services in the schools was the basis for the traditional configuration of school health services between the 1920s and the 1970s (Walker et al., 1990). Although health education was considered an important and legitimate function of the school, when it came to providing services the school acted primarily as a link between students and the community's health services resources. Typically, a school nurse and/or aide, sometimes under the supervision of a part-time physician, was responsible for first aid, immunization, screening, referral, recordkeeping, and follow-up. Over the years, these school-based health services became institutionalized into the educational bureaucracy and were often no longer under the purview of the medical community. As a result, school health policy and the responsibilities of school health personnel became increasingly prescribed by those with an education background rather than health training (Lynch, 1977).
These decades saw a continual decline in the diagnostic and treatment aspect of school health services. A 1930 White House Conference on Child Health and Protection called for the elimination of treatment in schools and for school physicians and nurse supervisors to increase contact with physicians in private practice. School dentistry during this period changed from restorative treatment to dental health education and inspection. The 1948 National School Health Bill, which was designed to provide federal aid to school health, was defeated partly because of the opposition of the medical profession whose members feared that funds would be provided for services to students who would otherwise have paid private practitioners (Solloway et al., 1995). It was not until the 1960s that concern for the health and welfare of children and young people led to a reconsideration of the possibility of delivering diagnostic and treatment services at the school site. A classic report appearing in the 1970s
signified the return to more substantial health services in schools (Leeds et al., 1980).
Research and Experimentation
The period around World War I saw the beginning of many research studies and demonstration projects in school health (Means, 1975). One of the earliest was the Locust Point Demonstration, which was launched in 1914 in Locust Point, a highly underprivileged section of Baltimore, under the direction of a school physician, school nurse, and school principal. The program's team approach was successful in improving the health of children and teachers, and the project attracted visitors from near and far to learn about the new methods and approaches. Another early demonstration conducted in 1917 in Framingham, Massachusetts, was primarily concerned with tuberculosis prevention and resulted in increased school appropriations for health education and physical education; the project was financed by the Metropolitan Life Insurance Company and carried out by the National Tuberculosis Association.
A number of school health demonstration projects and studies were carried out during the 1920s, 1930s, and 1940s. These included such examples as the School Health Study of the American Child Health Association (begun in 1926); the Ohio Research Study (1929–1932); the Cattaragus County Studies (begun in 1931); the School-Community Health Project, funded by the W.K. Kellogg Foundation (begun in 1942); and the California School-Community Health Project (launched in 1944).
One of the most intensive research efforts was the Astoria Plan, carried out in the Astoria Health District of New York City from 1936 to 1940, which was supported by the American Child Health Association, Metropolitan Life Insurance Company, Milbank Memorial Fund, and the U.S. Children's Bureau. Directed by the public health leader Dorothy B. Nyswander, the study had five objectives: (1) to determine whether prevailing methods used to discover children needing medical or dental care were satisfactory and, if not, to find what methods could be substituted; (2) to make inquiries into the nature of the cumulative health records of the children examined; (3) to find out just how the teacher, nurse, and physician were working together; (4) to find out the ways in which the staff made use of its time; (5) and to find out how physicians and nurses, immured in old practices, could be educated to new ways of work and thought (Means, 1975).
Under the Astoria Plan, services became more streamlined and efficient. Routine but cursory annual physical examinations were replaced by detailed examinations when the child first entered school and thereafter only when the conferring teacher and nurse deemed it necessary. The
nurse and teacher would periodically discuss the health condition of each student, and physicians were freed to give attention to those children who most needed help. Parents were included in the nurse–teacher conference, thus ensuring follow-up treatment, and emphasis was placed on having at least one parent present during any physical examination. In one of the program's major accomplishments, education and prevention began to be recognized as being just as important as diagnosing defects and disease. A possible downside was the burden placed on teachers to recognize student health problems and report them to the school nurse and parents.
By 1941, the Astoria Plan was institutionalized throughout New York City, and Solving School Health Problems, which described the details and outcomes of research on the plan, was released in 1942 (Means, 1975).
National Conferences and Collaboration
Since World War I, several White House Conferences have been convened that relate directly to school health issues. These include the Conference on Child Welfare (1919); the White House Conference on Child Health and Protection (1930); the White House Conference on Children in a Democracy (1940); the Mid-Century White House Conference on Children and Youth (1950); the Golden Anniversary Conference on Children and Youth (1960); the White House Conference on Food, Nutrition, and Health (1969); and the White House Conference on Children and Youth (Children's Conference, December 1970, and Youth Conference, February 1971). Each of these landmark conferences resulted in specific recommendations and suggested programs related to school health services, health instruction, and a healthy school environment (Means, 1975).
Throughout this period, numerous other important national conferences devoted to school health have occurred (Means, 1975). In 1947, for example, the American Medical Association, through its Bureau of Health Education, inaugurated a continuing series of conferences that brought together leaders from medicine, allied health professions, and education to focus on school health work. The first national conference on undergraduate and graduate professional preparation in school health education was held in 1948, which has been followed by a variety of other conferences on the preparation of educators. This attention culminated in the development by the Association for the Advancement of Health Education (AAHE) of the current National Council for the Accreditation of Teacher Education guidelines on the preparation of health education specialists, and in the development of guidelines on the health education preparation of elementary teachers by AAHE and the American School Health Association. In 1950, standards for school health services were
reviewed and revised by the American Public Health Association, the American Nurses Association, and the American School Health Association.
School Health from the 1960s to the Present
With the advent of the Great Society programs in the 1960s, the education and health scene experienced another major change. The Great Society and War on Poverty programs marked a new level of federal involvement in the schools and made new health and social services funds available. Relevant legislation passed in the 1960s and 1970s included Head Start, Medicaid, the Elementary and Secondary Education Act, the Community Health Center Program, the Education for All Handicapped Children Act, and the Child Nutrition Act that established the School Breakfast Program and the Nutrition Education and Training Program, and permanently authorized reimbursements for school lunches served to needy students.
Title I of the Elementary and Secondary Education Act tripled the number of school nurses, and a new nursing role—the school nurse practitioner—began to emerge in the late 1960s. At that time, issues of diagnosis and treatment in nontraditional health facilities surfaced, and the prevailing belief was that such activities were not permissible in schools by any primary care provider, including physicians. However, a state-by-state survey released in 1972 and sponsored by the Robert Wood Johnson Foundation failed to uncover any legislation that would prohibit the delivery of these services in schools. As a result, the clinical functions of school nurses were expanded to include primary care services with the nurses working in close collaboration with physicians. The introduction of school nurse practitioners into schools resulted in reaching students in need of primary care, an increase in problem resolution rates, and greater accuracy in excluding students from school for illness and injury (Hilmar and McAtee, 1973; Kohn, 1979; Silver et al., 1976).
The most significant school health education initiative of the 1960s was the School Health Education Study. This study defined health as a dynamic, multidimensional entity and outlined 10 conceptual areas of focus that over the years have often been translated into 10 instructional content areas. These conceptual areas include such themes as human growth and development, personal health practices, accidents and disease, food and nutrition, mood-altering substances, and the role of the family in fulfilling health needs. The primary publication from this initiative, School Health Education Study: A Summary Report, provided the basis for most of the current legislation on school health education (Sliepcevich, 1964). Numerous additional publications resulted from nearly 10 years of
this activity, including curriculum designs and teacher–student resource guides that address the 10 instructional content areas of health education across all grade levels.
The new social morbidities of children and young people began to increase in visibility beginning in the 1950s and 1960s. Mental, social, and emotional health became issues, and schools began to attempt to deal with delinquency, narcotic addiction, and the inability of students to adjust to the regular school environment. The 1960 White House Conference on Children and Youth had youths participating for the first time; the conference was profoundly concerned with drug abuse, increases in the incidence of venereal diseases, illegitimate births, and inadequate opportunities for youth employment (University of Colorado, Office of School Health, 1991).
Although the Great Society programs of the 1960s and 1970s brought an influx of funding for school health, many of these programs focused largely on disadvantaged and special populations. As these programs grew, the perceived importance of school health for mainstream students may have begun to decline. In addition, with the publication of A Nation at Risk (Goldberg and James, 1983) and the emergence of the "back to the basics" movement during the early 1980s, the role of health and physical education in the curriculum also came under question. Should these courses be considered part of the core curriculum or did they intrude on and distract from "academics"?
Since the mid- to late-1980s, however, there has been a resurgence of concern for the health and welfare of children and families, with renewed focus on the potential for schools to address health and social problems. Examples of recent significant activities in school health include the following:
-
the School-Based Adolescent Health Care Program, begun in 1986 by the Robert Wood Johnson Foundation, which catalyzed the rapid proliferation of school-based clinics;
-
the establishment in 1987 of the National Commission on Children, a bipartisan group created by public law "to serve as a forum on behalf of the children of the Nation;" the commission published its seminal report, Beyond Rhetoric, in 1991 (National Commission on Children, 1991);
-
the creation of the Division of Adolescent and School Health (DASH) of the Centers for Disease Control and Prevention (CDC) in 1988, and the associated increase in funding of school health initiatives and demonstration projects;
-
the launching of the U.S. Public Health Service's Healthy People 2000 initiative, which includes a set of nearly 300 national health promotion and disease prevention objectives to be achieved by the year 2000.
-
One-third of these objectives can be influenced significantly or achieved in or through the schools (McGinnis and DeGraw, 1991);
-
the National Education Goals, a bipartisan effort begun at a national governors' summit in 1989; among their directives, the goals call for (National Education Goals Panel, 1993, 1994) students to start school with the healthy minds, bodies, and mental alertness necessary for learning; the development of safe and disciplined school environments that are free of drugs and alcohol, including the development of comprehensive K–12 drug and alcohol prevention education programs in every school district; access for all students to physical education and health education to ensure that students are healthy and fit; and increased parental partnerships with schools in order to promote the social, emotional, and academic growth of children;
-
the organization in the early 1990s of a federal Interagency Committee on School Health and a National Coordinating Committee on School Health;
-
significant reports during the late 1980s and early 1990s on the health status of children and young people from organizations such as the American Medical Association, the National Association of State Boards of Education, the National School Boards Association, the Office of Technology Assessment of the U.S. Congress, the Carnegie Corporation, and the Council of Chief State School Officers (Lavin et al., 1992); numerous reports from the Maternal and Child Health Bureau, especially in relation to students with special health care needs, have also provided valuable assistance to school health planners (much of this material can be accessed through local and state health department maternal and child health offices);
-
the issuance by the American Medical Association in 1992 of Guidelines for Adolescent Preventive Services (GAPS), which calls for all adolescents aged 11 to 21 to have an annual preventive services visit to a physician who will address both the biomedical and the psychosocial aspects of health, with emphasis on health guidance and screening for risky behaviors such as sexual activity, substance abuse, eating disorders, learning difficulties, abuse, and emotional problems (American Medical Association, 1992);
-
since the beginning of 1994, a number of national conferences and reports have focused on the importance of improving access to comprehensive health and social services for children and families as a means of improving the health, welfare, and educational achievement of children; 3
-
recent legislation contains new provisions encouraging access to comprehensive services through school-based and school-linked approaches; 4
-
the formation of the National Nursing Coalition for School Health, with representatives from the American School Health Association, the American Nurses Association, the National State School Nurse Consultants Association, the American Public Health Association, and the National Association of School Nurses; in 1994 the coalition convened a national conference to examine future issues and priorities in school nursing (National Nursing Coalition for School Health, 1995);
-
the establishment of the Healthy Schools, Healthy Communities initiative by the U.S. Public Health Service's Maternal and Child Health Bureau and the Bureau of Primary Health Care, to support and strengthen school-based health centers;
-
the organization of the National Assembly on School-Based Health Care in 1995 (Adolescent Medicine, 1995); this group is establishing standards for school-based health centers and developing strategies for expanding and financing school-based health services; and
-
the development of national standards in many fields related to school health, including health education (Joint Committee on National Health Education Standards, 1995), physical education (National Association for Sport and Physical Education, 1995), school nursing (Proctor et al., 1993), and school foodservice and nutrition practices (American School Food Service Association, 1995).
What Have We Learned from the History of Health Programs in the Schools?
Today, some observers question whether school health programs and school-accessed comprehensive services for families go well beyond the intended function of the schools. A review of history shows, however, that for more than a century, schools been called on to play an important role in addressing health and social needs due to their strategic ability to reach children and families. The potential for schools to provide more
than mere academic preparation continues to be rediscovered, and today's renewed efforts in school health could be regarded as not new in concept but simply updated to reflect the needs of the times. There is a parallel, for example, between today's HIV (human immunodeficiency virus) and AIDS (acquired immunodeficiency syndrome) instruction and yesteryear's curriculum in physiology and hygiene, today's school-based clinics and yesteryear's medical inspections, and today's family services programs and yesteryear's of visiting teachers home visits to immigrants in urban tenements.
History also shows that controversy is not new to school health programs. Today's issues of local control of education and resistance to well-intended mandates imposed from above were also prominent a century ago. For example, at the turn of the twentieth century when the New York State Legislature proposed a bill to provide for sanitation, ventilation, and fire protection in schoolhouses in cities with populations of more than 5,000, the bill was easily defeated with charges that "it smacked of interference and paternalism in local affairs" (Duffy, 1974). These charges are echoed today as some individuals and communities resist directives about school health programs imposed from above, especially directives pertaining to such controversial aspects of programs as sex education or mental health counseling.
Other conflicts mirroring contemporary issues have surfaced periodically over the years. The New York free lunch program of the early twentieth century was criticized for the "hysterical sentimentality" over needy children, and later budgetary cuts led to farming out the lunch program to concessionaires whose sole motivation was making a profit. When free dental care for New York children was advocated in the early 1900s, the New York Times argued that this tendency toward "free everything" would only lead to socialism. Some considered the mandatory inspections of children at the turn of the century immoral and a violation of personal liberty. The debate about the proper role of the schools in providing primary care, begun in the 1920s during the period of the NEA–AMA collaboration, continues into this era of managed care.
The problems that confronted school health programs a hundred or more years ago—disease, physical defects, poor sanitation, inadequate nutrition, poverty, parental illiteracy, exploitation of children—were as critical in their time as current problems are today. However, yesterday's problems lent themselves more readily to well-defined permanent solutions—immunizations, eyeglasses, better personal health habits and nutrition, improved sanitary conditions, child labor laws. In contrast, many of today's new social morbidities are amorphous, chronic rather than acute, mental as much as physical. Individual behavior and societal norms have replaced disease pathogens and sanitation as major contributors to
health problems, and solutions are not clear-cut. The schools of yesteryear were not expected to solve the health and social problems of the day by themselves; the medical, public health, social work, legislative, and philanthropic sectors all pitched in. Given the scope and complexity of the health problems of today's children and young people, it is again likely that schools will not be able to provide solutions without the cooperation and support of families, community institutions, the health care enterprise, and the political system.
THE COMPREHENSIVE SCHOOL HEALTH PROGRAM
School health programming has evolved into today's concept of a comprehensive school health program. As the Institute of Medicine (IOM) committee began its study, it became clear that there were many descriptions about what a comprehensive school health program is and what outcomes it is expected to produce. In its interim statement, the committee considered these issues, and the following sections extends that discussion.
Goals and Desired Outcomes
The committee believes that the overarching goals of a comprehensive school health program are to enable all students to achieve and maintain an optimal state of health and well-being, reach their full academic potential, and develop into healthy productive adults who take personal responsibility for their own health.
In its interim statement (IOM, 1995), the committee described the following set of optimal outcomes for CSHPs—a vision of what these programs might be able to achieve. These optimal outcomes are categorized into three general areas: (1) student outcomes, (2) programmatic and organizational outcomes, and (3) community outcomes.
Student Outcomes
Students will assume personal responsibility for avoiding behaviors that compromise physical, social, and emotional well-being and for engaging in health-promoting behaviors. Students' health needs—preventive, emergency, acute, and chronic—will be addressed to allow students to reach the highest possible level of educational achievement and personal health. Particular attention will be given to the health component of Individualized Education Plans of students with special health care needs who require special education and related services.
Programmatic and Organizational Outcomes
The relationship between health status and educational achievement will be evident in the policies and programs of the school. The school's health emphasis will be integrated across all activities. Linkages among program components, disciplines, and participating agencies will be clearly defined and regularly evaluated. Individual and group health problems will be identified and managed with appropriate prevention, assessment, intervention or referral, and follow-up measures. Services will be organized to provide appropriate and timely responses to emergency, acute, and chronic health problems. The school's education and health programs will be continually reexamined and reformed as necessary to enhance student health, performance, and achievement.
Community Outcomes
The community will be actively involved in determining the design of a school health program and in supporting and reinforcing the goals of the program. This design will include assurance that schools are safe, with an environment conducive to learning and health promotion, and that policies and procedures are in place to enhance the use of schools as a community resource for health. All health-related programs delivered by the school and by community members through the schools will enhance the health status of the students and result in an improvement of the health and quality of life of the community.
The Need for a Definition
Early in its study, the committee encountered a variety of terminologies to describe school health programs and realized that there was not a single universally adopted model or definition for the term comprehensive school health program. According to recent common usage, a CSHP refers to an overall school health program, of which school health education and school health services are each components. However, some use the term ''comprehensive school health education" to refer to an overall program and consider school health services to be a component of comprehensive school health education. (For example, the commissioned paper by Mary Ann Pentz in Appendix A.) Others use the term "school health services" to describe an overall program and consider health education to be a component of school health services. (For example, see the list of Maine integrated services in Appendix G-1 and Solloway et al., 1995).
For the sake of consistency, the committee determined that it was necessary to establish its own working definition of the term comprehen-
sive school health program to serve as the basis for further work. In developing that definition, the committee examined previous models and definitions of school health programs that have evolved into today's concept of a CSHP. The provisional definition and relevant background information on previous models were presented in the committee's interim statement, and the following section reviews and expands on that discussion.
Previous Definitions and Models of School Health Programs
The Three-Component Model
The three-component model is considered the traditional model of school health programs. Originating in the early 1900s and evolving through the 1980s, this model, as shown in Table 2-1, defines a school health program as consisting of the following three basic components:
-
health instruction, accomplished through a comprehensive health education curriculum that focuses on increasing student understanding of health principles and modifying health-related behaviors;
-
health services, focused on prevention and early identification and remediation of student health problems; and
-
a healthful environment, concerned with the physical and psychosocial setting and such issues as safety, nutrition, foodservice, and a positive learning atmosphere.
The Eight-Component Model
In the 1980s, the three-component model was expanded to include additional components (Allensworth and Kolbe, 1987; Kolbe, 1986). According to this model, a comprehensive school health program contains the following eight essential components:
-
Health education consists of a planned, sequential, K–12 curriculum that addresses the physical, mental, emotional, and social dimensions of health.
-
Physical education is a planned, sequential, K–12 curriculum promoting physical fitness and activities that all students could enjoy and pursue throughout their lives.
-
Health services focuses on prevention and early intervention, including the provision of emergency care, primary care, access and referral to community health services, and management of chronic health conditions. Services are provided to students as individuals and in groups.
-
Nutrition services provides access to a variety of nutritious and
TABLE 2-1 Three-Component Model of the School Health Program
-
appealing meals, an environment that promotes healthful food choices, and support for nutrition instruction in the classroom and cafeteria.
-
Health promotion for staff provides health assessments, education, and fitness activities for faculty and staff, and encourages their greater commitment to promoting students' health by becoming positive role models.
-
Counseling, psychological, and social services include school-based interventions and referrals to community providers.
-
Healthy school environment addresses both the physical and the psychosocial climate of the school.
-
Parent and community involvement engages a wide range of resources and support to enhance the health and well-being of students.
The CDC's Division of Adolescent and School Health has promoted the eight-component model, which has received widespread attention and adoption by many states in recent years. Some states have even developed their own logo to depict the model; New Mexico, for example, represents the eight components as leaves of a yucca plant, the state flower, as shown in Figure 2-1.
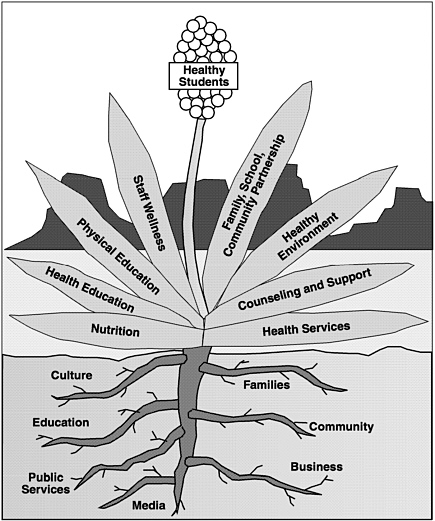
FIGURE 2-1 Eight-component model. SOURCE: New Mexico HealthierSchools: A Model of Comprehensive School Health, State of New Mexico.
Related Models and Definitions
In recent years, additional models, definitions, and descriptions of school health programs have emerged that build upon previous models. Several examples are discussed below.
-
Nader (1990) has proposed that the school is one locus of a broad range of health and educational activities that are carried out by a diverse group of health and educational personnel based both in the community and in the school. This model emphasizes that the school, community, and family or friends are the three important systems supporting children's health status and educational achievement. Further, the media—including educational, electronic, and print media—play a prominent role in influencing health-related behaviors. This model is shown in Figure 2-2. According to this model, the first steps in developing a CSHP
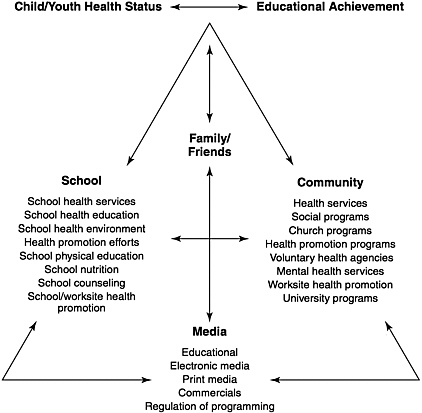
FIGURE 2-2 Family-school-community model. SOURCE: Nader, 1990. Reprinted with permission. American School Health Association, Kent, Ohio.
-
are to establish community linkages and carry out a community needs and resources assessment. These steps will then lead to the implementation and expansion of school health services, school health education, and a healthful school environment.
-
The ACCESS model—Administration, Community, Curricula, Environment, School, Services—regards the school as an institution that is a microcosm of society where students spend much of their developmental years (Stone, 1990). This model calls for five "keystones" or interrelated areas, with interactive pathways between the areas, as shown in Figure 2-3.
-
According to this model, the administration and community keystones are overarching and should be developed first to provide an administrative structure and base of support for the other areas. The environmental keystone should be developed next, for it sets a tone for students and school personnel. Once these three areas have been developed, the remaining areas of curricula and services can be added with optimal effect, for then there will be consistency between what is learned in the classroom and what takes place outside the classroom. Another distinguishing feature of this model is that the word "promotion" has been added to its title to give "school health promotion program," to reflect more accurately the nature of the program and of the public health movement in this country.
-
The Illinois Department of Health has recently developed a model of a CSHP as part of its long-range plan for school health (Edwards, 1992). This model consists of six critical elements: (1) management, (2) health promotion and education, (3) school health services, (4) healthy and safe environment, (5) integration of school and community programs, and (6) specialized services for students with special needs. This model is shown in Figure 2-4.
-
The distinguishing characteristics of this model include the importance of the management role in coordinating and integrating the other critical elements, and the emphasis on students with special health care needs.
-
Allensworth (1993) has described a CSHP by what it does, rather than by listing what it contains. According to this model, a comprehensive school health program focuses on priority behaviors that interfere with learning and long-term well-being; fosters the development of a supportive foundation of family, friends, and community; coordinates multiple programs within the school and community; uses interdiscipli-
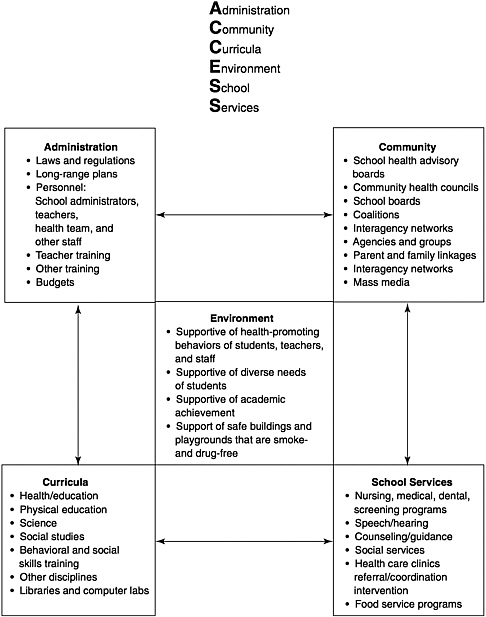
FIGURE 2-3 ACCESS model. SOURCE: Stone, 1990. Reprinted with permission. American School Health Association, Kent, Ohio.
-
nary and interagency teams to coordinate the program; uses multiple intervention strategies to attain programmatic goals; promotes active student involvement; solicits active family involvement; provides staff development; and accomplishes health promotional goals via a program planning process.
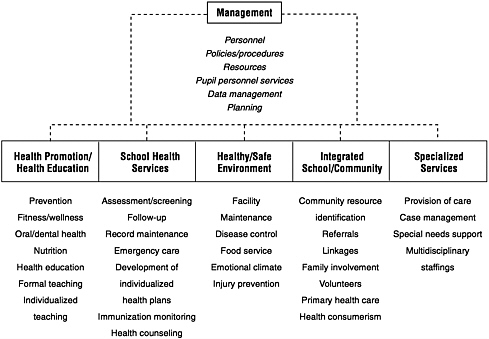
FIGURE 2-4 Illinois Department of Health model. SOURCE: Wallace et al., 1992. Reprinted with permission from Third Party Publishing, Oakland, California.
-
International models of school health programs often include the school as an element of a country's primary health care system (Edwards, 1992). Although each country's approach to primary health care may vary, school programs throughout the world typically include components of preventive, promotive, curative, and rehabilitative services. Another prominent feature in many countries is the strong collaboration between the school nurse and the physician, with both health professionals often available to the school, on either a full- or a part-time basis.
In 1992, the European Network of Health Promoting Schools was initiated "to foster and sustain innovation, disseminate models of good practice, and make opportunities for health promotion in schools more equitably available throughout Europe" (Hirsch, 1995). The network of school health educators is a joint project of the World Health Organization, the Council of Europe, and the Commission of the European Communities and is active in 34 countries. Each participating school develops programs that include health education, a health-promoting environment, and linkages with families and community resources. Collaboration at all levels is emphasized, and best practices are shared and disseminated through cross-border workshops and major international meetings.
The prominent role of the school in many international health efforts is facilitated by two conditions that exist in many countries but not in the United States: health care is an entitlement, and the educational system is nationalized.
Full-Service Schools
A recent model in the evolution of school health programs is the full-service school (Dryfoos, 1994). A full-service school is the center for collocating—locating together in one place—a wide range of health, mental health, social, and/or family services into a one-stop, seamless institution. The exact nature and configuration of services and resources offered will vary from place to place, but services should thoroughly address the unique needs of each particular school and community—hence the title "full-service schools."
According to this model, a full-service school provides a quality education for students that includes individualized instruction, team teaching, cooperative learning, a healthy school climate, alternatives to tracking, parental involvement, and effective discipline. The school and/or community agencies provide comprehensive health education, health promotion, social skills training, and preparation for the world of work.
A distinguishing feature of this model is the broad spectrum of services to be provided at the school site by community agencies. Some examples of these various services include health services such as health and dental screening and services, nutrition counseling, and weight management; mental health services such as individual counseling, crisis intervention, and substance abuse treatment and follow-up; and family welfare and social services such as family planning, childcare, parent literacy, employment training, legal services, recreational and cultural activities, basic services for housing, food, and clothing.
Definition of the Joint Committee on Health Education Terminology
In 1990, the Association for the Advancement of Health Education convened a committee of delegates from the Coalition of National Health Organizations5 and the American Academy of Pediatrics. The charge to
this Joint Committee on Health Education Terminology was to review and update earlier terminology and to provide definitions for new terms currently used in the health education field. The Joint Committee defined a CSHP as follows (Joint Committee on Health Education Terminology, 1991):
A comprehensive school health program is an organized set of policies, procedures, and activities designed to protect and promote the health and well-being of students and staff which has traditionally included health services, healthful school environment, and health education. It should also include, but not be limited to, guidance and counseling, physical education, food service, social work, psychological services, and employee health promotion.
The Committee's Provisional Definition
After review of previous models and definitions, the committee proposed the following provisional definition of a CSHP, which was presented in its interim statement (IOM, 1995):
A comprehensive school health program is an integrated set of planned, sequential, school-affiliated strategies, activities, and services designed to promote the optimal physical, emotional, social, and educational development of students. The program involves and is supportive of families and is determined by the local community based on community needs, resources, standards, and requirements. It is coordinated by a multidisciplinary team and accountable to the community for program quality and effectiveness.
Each term printed in bold was further described and discussed in the interim statement. A brief summary of that discussion follows:
Comprehensive means inclusive, covering completely and broadly, and refers to a broad range of components. It should be emphasized, however, that programs and services actually delivered at the school site may not provide complete coverage by themselves but are intended to work with and complement the efforts of families, primary sources of health care, and other health and social service resources in the community to produce a continuous and complete system to promote and protect students' health.
Integrated means formed, coordinated, or blended into a functioning or unified whole. It is assumed that when the various elements of CSHPs are integrated, they mutually reinforce and support each other, producing a whole that is greater than the sum of its separate parts in meeting the health needs of students and fostering student health literacy.
Planned implies a deliberate design, a detailed formulation of a program of action. Planning involves developing an orderly arrangement of program strategies, activities, and services, after careful consideration of needs and resources, in order to meet the needs of students and their families. The planning process should involve a broad range of stakeholders and should begin with local needs and resources assessment. Planning should also include ongoing evaluation and means for continuous program improvement.
Sequential implies a deliberate ordering or succession of program elements, so that each successive event builds upon previous student experience and is compatible with a student's developmental status.
School-affiliated refers to activities that take place at the school site (school based), that take place off-site but are associated with the school (school linked), or that have any other connection with the schools.
Strategies, activities, and services refer to approaches, methods, actions, and interventions for the purpose of accomplishing program goals and objectives. Strategies are the overall approach or network of related methods and processes, carefully designed to achieve desired goals. Activities and services are those specific and concrete actions carried out as part of a strategy.
Development refers to the process of growth, advancement, and maturation. Optimal development implies setting children on a course of growth and maturation that will lead to a healthy adulthood.
Involve means to engage as a participant, to include. Supportive of families implies helping, assisting, or advocating, to keep families as a key foundation, with family defined in its broadest context as a unit consisting of one or more children plus parent(s), guardian, or other care provider(s). Involving the family implies that the family has knowledge about the CSHP and participates in community deliberations to determine needs and to design program strategies, activities, and services. When properly designed and sensitive to community concerns, CSHPs provide family support by reinforcing community values and providing access to health and social services, both for students and possibly for other family members.
Determine means to come to a decision by investigation, reasoning, or calculation, to settle or decide by choosing among alternatives or possibilities.
The local community refers to the wide range of stakeholders—parents, students, educators, health and social service personnel, insurers, business and political leaders, and so forth—at the particular site where the program will be implemented.
Needs refer to the lack of something desirable or useful and to conditions requiring relief or remediation. Resources refer to the strengths and
available sources of relief or recovery upon which the community can draw in meeting identified needs. Standards and requirements involve both professional and legal criteria and community ethics, mores, and values.
Coordinated means brought into combined action to cause separate elements to function in a smooth concerted manner. Coordination implies a formal relationship and blurring of boundaries between coordinating partners, although partners can still retain their identity and affiliation to their profession.
Multidisciplinary team involves individuals with different backgrounds, skills, and knowledge working together. Even in a small or isolated school, it should be possible to find two or more individuals with different disciplinary backgrounds to coordinate the program and link it to the community.
Accountable means that those involved in the program are responsible and answerable to the community and that they must provide information on program implementation, outcomes, and financial matters to allow for informed decisionmaking.
Quality refers to the degree of competence and excellence of the program; effectiveness has to do with producing the desired result: improved health and educational outcomes. Quality and effectiveness are interrelated in CSHPs—the existence of one implies the presence of the other.
The Definition Revisited
With the benefit of knowledge and insight gained during the course of its study, the committee reexamined its original provisional definition of a CSHP and determined that it was still valid and useful. The definition is flexible, not overly prescriptive, and emphasizes what the committee believes are the crucial features of a CSHP—family and community involvement, multiple interventions, integration of program elements, and collaboration across disciplines. The various definitions and models of CSHPs are not separate and distinct, and considerable commonality exists among them. The committee believes that there is no single ''best" definition or model for a CSHP but that programs must be tailored to meet each community's needs, resources, perspectives, and standards. It is important to move beyond definitions and models to examine essential program elements and approaches for program design and implementation. The remainder of this chapter provides a brief overview of key program elements found in virtually all program models.
Key Elements of a Comprehensive School Health Program
Community Participation and Focus
The essential foundation for any successful CSHP is built from the involvement of a wide range of community stakeholders—parents, students, educators, health and social service personnel, insurers, and business and political leaders. This involvement can be effectively organized and channeled through the formation of some type of "community school health coordinating council." The first step under the leadership of the council should be to assess the priority health-related needs and problems of children and young people in that community. Are they related to poor dietary habits and physical fitness, stress, violence, substance abuse, risky sexual behavior, deteriorating family conditions, lack of access to medical care, or other factors? Next, an assessment should be made of resources available to deal with these needs. Chances are that many resources already exist and merely need to be reconfigured, rejuvenated, or made more accessible. To provide focus, it is important to identify at the onset a few key indicators that will be monitored to track program impact—perhaps improved attendance or academic achievement, increased physical fitness scores, decreased teen pregnancy or drug abuse, fewer hospital emergency room visits, or an increase in the number of families with a medical "home."
Once the foundation of community support and the program focus have been established, the actual program will certainly consist of a collection of program elements or components, which ideally should work in an integrated fashion to address identified community needs. As mentioned previously, all program models share many common components. The committee does not believe it fruitful to attempt to rank components in order of importance or to prioritize which should be implemented first. Each community may have different priorities, and furthermore, the resources and infrastructure for many of these components are already in place. All that may be needed is a reinvigoration and refocusing of current efforts—and the development of linkages and mutual support among the component parts.
The most prominent program components found in virtually every recent model of school health program are described below. The following discussion is intended simply to provide a brief overview, not an exhaustive analysis. Each of these components has its own wide literature 6 that should be consulted for an in-depth understanding of that component.
|
6 |
Guidelines for Comprehensive School Health Programs from the American School Health Association (1994) gives a concise summary of each of the components of the eight-component model. Excerpts from this document are found in Appendix B. The following documents are also suggested as an introduction to the various components and as a source of references to the primary literature and research in these fields: • The Guidelines documents from the CDC: At the time of writing of this report, guidelines for tobacco prevention programs had been released (CDC, 1994). Guidelines for school health programs to promote healthy eating and guidelines for school and community health programs to promote physical activity among youth were scheduled to be released in 1997, and guidelines for school health education were under development. • Principles and Practices of Student Health, edited by Wallace et al. (1992), is a three-volume compendium of papers on all aspects of student health programs. • School Health: Policy and Practice was issued by the Committee on School Health, American Academy of Pediatrics (1993). • The School Health Challenge is a document from ETR Associates (Cortese and Middleton, 1994). • In addition, CDC's DASH is supporting the development of a series of papers, under the direction of the Education Development Center, that examine in depth each of the individual components of the eight-component model and how the components fit together to make an integrated program. Drafts are expected to be available for discussion in late 1997, and a monograph containing all papers is expected to be released in the fall of 1997. |
School Environment
Physical Environment. School buildings and grounds should be clean, safe, and secure. Regulations from the Occupational Safety and Health Administration and others must be followed in ensuring a safe and healthful environment. Building design should ensure adequate ventilation, lighting, noise abatement, and heating and cooling, with provisions for complying with federal Americans with Disabilities Act mandates. Environmental hazards—such as asbestos, lead, and radon—must be given attention, and school sources of pollution—science laboratories, art classes, shop and vocational classes—should be governed by appropriate policies and receive constant vigilance. Safety and sanitation measures are established, understood, and followed. Emergency disaster plans are in place and emergency drills are held periodically. Policies are in place to ensure safe transportation practices that address such transportation modes as cars, buses, bicycles, skateboards, and walking. Staff and students are made aware of safety, first aid, and infection control equipment and procedures. Buildings, equipment, and grounds are kept clean, in good repair, and free of hazards that foster infection and handicaps.
As a result of the 103d Congress considering 66 bills that referenced the "school environment" and 51 that were directed at the goal of "safe schools," the Office of Technology Assessment of the U.S. Congress was asked to prepare the report Risks to Students in Schools (Office of Technol-
ogy Assessment, 1995). This document describes regulations and risks pertaining to environmental hazards, such as asbestos and lead; exposure to infectious agents, such as influenza virus and disease-causing bacteria; unintentional injuries, such as sports and playground accidents; and intentional injuries, such as homicide and fighting.
Policy and Administrative Environment. Rules and regulations are established to promote the physical, psychological, and social health of students. Health and safety promotion is prominent. A smoke-, drug-, weapon-, and violence-free environment is enforced, with clear and reasonable penalties. Extracurricular sports and physical fitness activities are promoted for all students, and healthful foods are sold in the school lunch, school breakfast, and a la carte options in the school cafeteria, as well as through vending machines, school events, or fund-raising drives. Schedules are designed not merely to improve efficiency but also to reduce stress; for example, class release times may be staggered to minimize crowding in halls and avoid unnecessary sources of conflict, and lunch periods may be scheduled to provide adequate time to enjoy healthful meals. When appropriate, students have input in establishing policies and discipline procedures, and discipline is administered in a fair and evenhanded manner. A consistent process is in place for reporting, analyzing, and preventing injuries and health problems.
Psychosocial Environment. Students and staff function in a supportive atmosphere that encourages open communication, respects individual differences, and promotes each student's reaching full academic and social potential. The diverse needs of individual students are addressed, and families are kept informed and involved. There is a collaborative rather than adversarial spirit among students and staff, and a sense that everyone is pulling together toward the same goals. A cooperative, not overly competitive, atmosphere exists in academic instruction. Expectations are high, but students are not left to flounder or fall through the cracks. Academic assistance is easily available and actively promoted for those students needing additional help. Faculty and staff take the initiative to look for and help resolve student problems that may affect learning, morale, and well-being. Policies related to provision of services for at-risk students, such as free and reduced-price meals, are made in ways that do not stigmatize recipients. A crisis response system is established to support students in the event of violence, suicide, disaster, or other incident.
The psychosocial environment has been shown to have a significant impact on student achievement and functioning. It has been speculated that in some situations, a healthful psychosocial environment may be as
important—or even more important—than classroom health education in keeping students away from drugs, alcohol, violence, risky sexual behavior, and the rest of today's new social morbidities (Carnegie Council on Adolescent Development, 1995). Studies have also shown that families of students can be reached and can benefit from an improved school psychosocial environment (Comer, 1988).
Many authorities believe that for all children and young people to have a chance to succeed, significant changes are required in the environment in which students are educated and in the way schools are structured. In quality schools, the staff has high expectations for all students, student receive support and nurturing, and students are involved in significant and worthwhile activities. Schools are responsive to a wide range of students' needs and interests, and meaningful involvement of families is sought and supported. Change in the school structure and climate is seen as the ultimate intervention to insure the long-term "health" of students. Examples of endeavors promoting these principles include the following:
-
The School Development Program, founded by James Comer of the Yale University Child Study Center, focuses on school-based management and parental involvement to improve the education of disadvantaged students (Comer, 1984, 1988). Each participating school is governed by an elected School Advisory Council that includes the principal, teachers, teacher aides, and parents. A mental health team, comprising the school psychologist and other support personnel, provides direct services to children and advises school staff and parents. A parent is employed to work in each classroom on a part-time basis, and parents are encouraged to volunteer as teacher aides and librarians, publish newsletters, and organize social activities. A social skills curriculum has been developed that integrates the teaching of basic skills with teaching of "mainstream" arts and social skills. According to Comer, the strength of this project is its focus on the entire school rather than on any one particular aspects, and its attention to institutional change rather than to individual change.
-
Success for All, initiated by Robert Slavin and colleagues at the Johns Hopkins University, restructures the entire school to do "everything" necessary to ensure that all students will be performing at grade level by the end of third grade (Slavin et al., 1992). Interventions include a half-day preschool and full-day kindergarten, a family support team, an effective reading program with reading tutors, individual academic plans based on frequent assessments, a full-time program facilitator and coordinator, training and support for teachers, and a school advisory committee that meets weekly. The family support team works full-time in each school and consists of social workers, attendance workers, and a parent liaison
-
worker. The team provides parenting education and support assistance for day-to-day problems such as nutrition, getting glasses, attendance, and problem behaviors. Family support teams are also responsible for developing linkages with community resources.
-
Turning Points, led by the Carnegie Council on Adolescent Development, focuses on early adolescence, a critical and pivotal developmental period (Carnegie Council on Adolescent Development, 1989). The project is based on the premise that a serious mismatch exists between the organization and curriculum of most middle grade schools and the intellectual and emotional needs of young adolescents, which results in increased alienation, substance abuse, absenteeism, and school dropouts. The project is restructuring a set of middle schools with the following characteristics. There will be "Schools-Within-a-School" that has students and teachers grouped together in teams, with every student known well by at least one adult. There will be a core academic program that emphasizes critical thinking, citizenship values, a healthy life-style, and responsible and ethical behavior. Cooperative learning will be used, and tracking will be eliminated. The staff will be expert in teaching young adolescents, and the staff will be empowered to make decisions and create the environment necessary for students to succeed. Emphasis will be placed on health and fitness as a means to improve academic performance, and every school will have a health coordinator, access to health care and counseling, and a health-promoting environment. Finally, families and the community will be involved with the operation of the school.
Health Promotion for Staff. Staff health promotion frequently receives low priority among school health issues, and research on its impact is scarce. A few studies, however, have shown that staff health promotion programs are feasible and produce improvement in morale, absenteeism, perceptions of well-being, attitudes toward personal health, and even quality of classroom instruction. (Belcastro and Gold, 1984; Falck and Kilcoyne, 1984; Jamison, 1993; Maysey, 1988) Another benefit of staff health promotion may be a decrease in group health insurance costs.
Healthy People 2000 calls for employee health promotion for all worksites (U.S. Department of Health and Human Services, 1991). Employers are encouraged to provide physical activity and fitness programs, nutrition education and weight management programs, blood pressure and cholesterol education and control activities, stress management, policies limiting smoking, and aggressive prevention and intervention programs for drug and alcohol abuse. The Health Insurance Association of America has outlined reasons why health promotion for school employees is a particularly strategic investment (Allensworth et al., 1994). For example, health promotion would have a significant impact on overall
health care costs; reduce absenteeism and hiring of substitute teachers, improving instruction for students; improve employee morale by demonstrating a commitment to their well-being; create a "multiplier effect" as staff become positive role models for students and reinforce consistent CSHP health-enhancing messages; take advantage of existing school-based facilities and resources; and encourage the school to develop "open-door" policies and become the focus for community-wide health promotion activities.
Education
The two educational components of CSHPs are physical education and health education. In addition, health topics may be integrated into other curricular areas. The following is a brief overview of these educational components; Chapter 3 provides a more in-depth discussion.
Physical Education. Physical education involves a planned, sequential, developmentally appropriate, K–12 curriculum that provides cognitive and affective content and physical activity. Content areas include motor skills; physical fitness; rhythm and dance; games; team, dual, and individual sports; tumbling and gymnastics; and aquatics. Most states mandate the minimum time per week spent in physical education and the number of years that students must be enrolled.
While debate continues over whether the essential purpose of physical education is to teach motor skills or promote fitness, the concept of health-related fitness is emerging to bridge the gap between skills and fitness7 (Simons-Morton, 1992). The focus in physical education is shifting away from competitive sports and athletic performance to cultivating an interest and sense of self-efficacy in physical activities that students can enjoy and pursue throughout adulthood.
Physical activity in youth is associated with higher levels of health and physical fitness, greater resistance toward cigarette and alcohol use, and possibly enhanced academic achievement and cognitive functioning. Physical activity levels tend to decline steadily during adolescence, especially among girls, although how physical activity tracks into an adult life-style is not well understood. It is established, however, that merely engaging in physical activity during youth will not protect against risks brought on by a sedentary life-style as an adult; physical activity must be
sustained throughout adulthood. A sedentary life-style in adults is associated with higher risk for coronary heart disease, hypertension, non-insulin-dependent diabetes mellitus, and certain cancers; evidence also suggests that physical activity may reduce risks for osteoporosis and obesity and relieve symptoms associated with anxiety and depression (CDC, 1997).
Health Education. Health education consists of a planned, sequential, developmentally appropriate K–12 curriculum that deals with the physical, mental, emotional, and social dimensions of health, provided by qualified teachers prepared to teach the subject. The goal of health education is to empower students with the necessary knowledge and skills to maintain and improve their health, adopt healthful behaviors, avoid health-threatening behaviors, and become health literate consumers and decisionmakers. The CDC's School Health Policies and Programs Study (SHPPS)8 examined the most commonly required topics in health education across the country; these findings are shown in Table 3-10 (see Chapter 3). SHPPS found that a large majority of schools require instruction in such areas as the prevention of alcohol and other drug use, HIV and other sexually transmitted diseases, and tobacco use; dietary behaviors and nutrition; human growth and development; and human sexuality.
Issues in health education are complicated, and national consensus is slow to emerge on the position of health education in the overall curriculum. Questions continue to be raised about what topics should be taught in health education, who should teach them and when, how conflicts over controversial topics can be resolved, and what outcomes can reasonably be expected and measured. These questions are considered in Chapters 3 and 6.
Other Curricular Areas. Other subject matter areas—home economics, science, mathematics, language arts, social studies, visual and performing arts, vocational education—can use health-related topics to reinforce the school health message and also capture student interest in these other subjects. Health topics seem relevant to students, whereas other academic
subjects may seem abstract and remote.9 Science is a logical area to connect with health because most health practices and health problems have a scientific basis. The National Science Education Standards call for students to understand science in its personal and social perspectives, including science in health. These standards contain extensive references to health, including basic body functions, cardiovascular fitness, nutrition, sexuality, the scientific basis for disease, problems with substance abuse, accident prevention and safety, risks and personal decisionmaking (National Research Council, 1996).
Science is not the only subject that can be enhanced and made more relevant using health topics. In mathematics, elementary students can collect and use the information on nutrition labels to devise a well-rounded diet for themselves, and secondary students can examine the mathematical models for the spread of contagious disease. Language arts classes can analyze the persuasive effects of the media on health behaviors or write letters to politicians and the media about student health concerns. Visual and performing arts classes, including dance, drama, music, and visual arts, can encourage students to enhance mental health through expression of personal feelings; awareness of health issues can be promoted through student expression and interpretation in these various art media. Social studies classes can explore how nutrition and disease shaped history, discuss the advantages and disadvantages of prohibition and current implications for controlling other substances, or debate the ethics of withholding health care and other benefits to those suffering from conditions caused by deliberately engaging in risky behavior.
It should be emphasized that the inclusion of health topics in other curricular areas should enhance, but not replace, the health education curriculum.
Services
Presented below is a brief summary of the types of services typically found in school health programs. These services represent a complex area, and issues of concern include determining the appropriate range and configuration of school-based services, interaction between the school and other community providers, qualifications and training of service deliv-
ery personnel, scientific validity of mandated services, financing, evaluation, and controversial aspects of certain services. Chapter 4 focuses on services, and these issues are discussed in greater depth there.
Health Services. Health services are designed to evaluate, protect, and promote student health. SHPPS has described school health services as a "coordinated system that ensures a continuum of care from school to home to community health care provider and back" (Small et al., 1995). The goals and program elements of school health services vary at the state, community, school district, and individual school levels, but some common elements exist across the country. A recent national school health survey, A Closer Look, reported on the most frequently provided health services in schools (Davis et al., 1995). The results are shown in Table 4-1 (see Chapter 4). Two health services are provided almost universally by school districts—first aid and administration of medications. Other commonly provided services include screenings—height, weight, vision, and hearing—and services mandated by law for children with disabilities and special needs.
School health services are provided by nurses, physicians, dentists, and other allied health personnel in settings ranging from a health aide's office in the school to a full-blown school-based clinic providing a wide range of primary care services. Depending on the community, certain basic health services may be considered the responsibility of the school system, such as the provision of school nurses or health aides. However, more extensive ventures—school-based clinics, for example—are often initiated and managed in cooperation with the school by groups outside education, such as a health department, community clinic, or hospital.
Counseling, Psychological, and Social Services. These services promote the mental, emotional, and social health of students and deal with problems that interfere with teaching and learning. Services include individual or group assessment, interventions, and referrals. School staff and families of students may also receive these services, and services for special education students are an important focus.
These services bridge the gap between the school's academic program and the mental and emotional health of students and their families. Professionals in these fields work closely with each other and with school health personnel, teachers and administrators, families, and community agencies. They frequently serve as brokers in linking community health and social service resources to the school site.
In this era of emphasis on academic standards and limited financial resources, counseling, psychological, and social services are sometimes seen as outside the mainstream and are threatened by cutbacks. However,
these services address today's new social morbidities that prevent students from achieving at their highest potential, and the extent of the problems may not be recognized. It is estimated that 12 to 20 percent of our nation's children and adolescents suffer from one or more diagnosable mental disorders, and many others are at risk due to violent neighborhoods, parental abuse or neglect, and risky and dangerous behavior (IOM, 1994). In fact, it has been suggested that fully 40 percent of all students are in ''very bad educational shape" and "at risk of failing to fulfill their physical and mental promise" (Hodgkinson, 1993). It is also important to realize that all students—not simply low-income or low-achieving students—are vulnerable to mental and emotional problems. A recent national survey of high-achieving high school students indicated that more than 50 percent report violence at their school, 29 percent have considered committing suicide, 81 percent report that it is easy to get alcohol and 77 percent say alcohol is very common at parties, 25 percent have engaged in sexual intercourse, and 11 percent have tried marijuana. More than 30 percent of these high-achieving students say their home life is less than "happy and close most of the time" (Who's Who Among American High School Students, 1994). Given this context, it has been proposed that counseling, psychological, and social services receive increased emphasis in school reform and restructuring, as an essential "enabling" component to address factors that interfere with students' learning and performance (Adelman, in press).
Nutrition and Foodservice. The school foodservice not only provides nutritious and appealing meals but also helps students develop lifelong healthful eating habits. Evidence shows that dietary behaviors tend to stay constant over time, and poor eating habits established in childhood tend to persist through adulthood (CDC, 1996). A poor diet contributes to the development of four of the nation's ten leading causes of death: coronary heart disease, stroke, diabetes, and certain types of cancer. Other detrimental conditions associated with diet are hypertension, obesity, osteoporosis, and poor oral health. Also, the number of overweight children and adults has increased significantly in the last decade, and eating disorders and unsafe weight loss methods have become more prevalent as well.
Nutrition education is critical at all levels, even in early childhood and elementary schools, in order that students develop healthful dietary habits and understand the influence of nutrition on health. Nutrition education should be part of classroom health education, and nutrition should be introduced into other subjects such as science, physical education, and home economics. In providing a variety of nutritious and appealing meals, the school foodservice serves as a laboratory to reinforce the lessons learned in the classroom.
Research has shown that children's cognitive, behavioral, and physical performance are impaired by poor nutrition (Center on Hunger, Poverty, and Nutrition Policy, 1993; CDC, 1996). School meals that meet U.S. Department of Agriculture (USDA) dietary guidelines play a significant role in providing good nutrition. The School Nutrition Dietary Assessment Study (Burghart and Devaney, 1995) found that students who ate the school lunch had higher intakes of key nutrients than students who made other choices. A study of low-income elementary students found that participation in the school breakfast program led to increased standardized test scores and decreased absenteeism and tardiness (Meyers et al., 1989).
The concept of foodservice is not limited to the reimbursable school meal program for which the USDA establishes nutrition standards. High-quality local standards are needed for all food available on the school campus—including food sold through vending machines and special events—and for the environment in which these foods are made available to students. Although the immediate goal of the school foodservice may be the provision of student meals, the ultimate goals are providing education and establishing lifelong healthful dietary habits.
Comprehensive Family Services. Access may be provided through the school to a wide range of health and social services for students and their families, especially in disadvantaged communities. Examples of services include health and dental care, adult literacy programs, employment training, family counseling, child care, legal services, recreation and culture, and provision of basic needs in housing, food, and clothing. Providing access to services through the school does not necessarily require an increase in overall budgets for these services. Typically, many of these services already exist but in a fragmented manner, and families often find the system difficult to access and navigate. Collocating and coordinating comprehensive services through a familiar neighborhood institution such as the school has been found to improve access, increase efficiency, and facilitate follow-up (Wagner et al., 1994). Comprehensive school-affiliated family services are increasingly considered to be an important means for reaching families and for improving academic, health, and social outcomes for students10 (American Academy of Pediatrics, 1994a, 1994b;
Bruininks et al., 1994; U.S. Department of Education and U.S. Department of Health and Human Services, 1993; U.S. Department of Education, 1995). Although seeming ambitious, comprehensive school-affiliated family services are not a new idea; many schools were providing access to a similar range of services in poor urban and rural areas a century ago (Tyack, 1992).
Integration of Comprehensive School Health Programs with Community Health Efforts
Early in its study, the IOM committee sensed that school programs working in isolation are likely to have limited effect without community support and reinforcement. To examine this premise further, a paper on integrating school and community health efforts was commissioned; the paper is found in its entirety in Appendix A. (Note that in this paper the author uses the terminology "comprehensive school health education" to refer to what the committee has called a "comprehensive school health program.") The paper reviews the results of selected studies on school-based programs, community programs, and programs integrating the efforts of schools and communities. Examples of community participation and mechanisms for interfacing the school and community are also discussed. Results suggest that combined school-community programs yield higher levels of participation, implementation, and dissemination; greater effects on the more serious levels of health risk (e.g., on daily smoking compared to monthly smoking); and effects on parents as well as youth, perhaps longer effects than are currently obtainable from most school programs alone. The author notes that in the programs analyzed, the assumption of the need for integrating school and community efforts has usually been based on practical considerations and common wisdom rather than on theory or empirical evidence. The author also points out knowledge gaps and the limitations of existing studies, and suggests directions for future research.
Integration of the Elements of a Comprehensive School Health Program
Integration—the blending of program components into a unified whole—is an elusive concept. A single standard process for achieving and recognizing "integration of components" does not exist, because each situation is unique. Integration might be considered a topic that is "hard to define, but you recognize it when you see it." Consider the following simple example pertaining to nutrition that illustrates the practical meaning of the term integration:
Lessons on nutrition in the health education classroom are supported
by a school foodservice that serves healthful, well-balanced meals and labels the nutritional content of cafeteria selections to increase nutrition awareness. Classroom lessons are also strengthened by school policies requiring that foods available through vending machines, special events, and fund-raising drives meet a high standard of nutrition. School nurses and counselors promote awareness about weight management and eating disorders, and provide assistance for students and staff with problems in this area. Students with special conditions, such as diabetes, have dietary provisions prescribed by a physician and arranged by the school nurse and foodservice or by a community dietitian if the school lacks the required expertise. Physical education instructors help students understand the relationship between caloric intake and energy expenditure and between nutrition quality and physical stamina and performance. Nutrition-related topics also enhance instruction in other subject matter areas, such as science, mathematics, and social studies. Community-wide campaigns promote nutrition awareness so that healthy eating habits acquired in school will be reinforced outside school; restaurant and fast-food outlets promote healthful choices, and grocery stores publicize healthful selections and provide recipes and tips for healthful family meal planning.
The conventional wisdom is that when the various elements of a CSHP are integrated, they will mutually reinforce and support each other and produce a whole that is greater than the sum of its separate parts. The concept and desired outcomes of integration are simple to recite, but integration is a difficult and sophisticated process to implement and measure—"the reality lags far behind the vision" (Education Development Center, 1995). While exemplary individual program components exist in many schools and various states and communities are making progress in establishing CSHPs, truly comprehensive and integrated programs do not yet appear to be widespread.11 Although individual program components have been studied separately and many are reasonably well understood, the committee could find no record of systematic research on the integration of multicomponent programs. There is a dearth of scientific analysis of what exactly constitutes integration of components, whether integration actually enhances the effects of separate components, and what the most effective strategies are for achieving integration and measuring its impact. This lack of evidence is not surprising, given the scarcity and complexity of programs and limited program resources. Research
on the process and effectiveness of individual components—a particular health education curriculum, health services intervention, or modification of school environment—is difficult enough; even more so is the study of any synergism among them.
Since individual programs are idiosyncratic and not easily replicable, research and evaluation that attempt to detect the effects of integration per se or to detect the specific contribution of individual or various combinations of factors to the overall program are not likely to be fruitful. The pragmatic approach to integration of program components at the local level is to make certain that each individual component is designed to address identified needs and implemented according to effective practices, and that systematic and regular communication occurs among all stakeholders. Then, if indicators are moving in the right direction at the desired rate, this should be sufficient evidence for a community to declare that its program is effective. Additional issues and dilemmas involved in evaluating comprehensive integrated programs are discussed further in Chapter 6.
SUMMARY
Schools have a long history of providing health education, services, and outreach to families. A vision of what schools might be able to do to promote health, education, and family well-being has led to the concept of a CSHP. Although exemplary individual program components exist in many schools, truly comprehensive and integrated programs are not yet widespread. Various models for CSHPs exist, but most of the basic elements or components tend to be similar. There is no "best" model or standard algorithm for establishing a program—it must be specifically tailored to fit each particular community. Active community involvement is key, and the integration of school programs with other community efforts appears to produce more positive results than school or community programs operating in isolation.
REFERENCES
Adelman, H.S. In press. Restructuring Education Support Services: Toward the Concept of the Enabling Component. Kent, Ohio: American School Health Association.
Adolescent Medicine. 1995. 20(10):1–4.
Allensworth, D.D. 1993. Expansion of comprehensive school health: What works. Paper presented at the Institute of Medicine Workshop, Integrating Comprehensive School Health Programs in Grades K-12, Washington, D.C., May.
Allensworth, D.D., and Kolbe, L.J. 1987. The comprehensive school health program: Exploring an expanded concept. Journal of School Health 57(10):409–411.
Allensworth, D.D., Wolford Symons, C., and Olds, R.S. 1994. Healthy Students 2000: An Agenda for Continuous Improvement in America's Schools. Kent, Ohio: American School Health Association.
American Academy of Pediatrics, Committee on School Health. 1993. School Health: Policy and Practice. Elk Grove Village, Ill.: American Academy of Pediatrics.
American Academy of Pediatrics. 1994a. Principles to Link By: Integrating Education, Health, and Human Services for Children, Youth, and Families . Report of the Consensus Conference. Washington, D.C.
American Academy of Pediatrics. 1994b. Statement by the Task Force on Integrated School Health Services. Pediatrics 94(3):400–402.
American Medical Association. 1992. Guidelines for Adolescent Preventive Services. Chicago: American Medical Association, Department of Adolescent Medicine.
American School Food Service Association. 1995. Keys to Excellence: Standards of Practice for School Food Service and Nutrition. Alexandria, Va.: American School Food Service Association.
American School Health Association. 1994. Guidelines for Comprehensive School Health Programs. Kent, Ohio: American School Health Association.
Belcastro, A., and Gold, R. 1984. Teacher stress and burnout: Implications for school health personnel. Journal of School Health 53(7)404–407.
Bruininks, R.H., Frenzel, M., and Kelly, A. 1994. Integrating services: The case for better links to schools. Journal of School Health 64(6):242–248.
Burghart, J., and Devaney, B., eds. 1995. The school nutrition dietary assessment study. American Journal of Clinical Nutrition 61:1(Suppl.).
Carnegie Council on Adolescent Development. 1989. Turning Points: Preparing American Youth for the 21st Century. Washington, D.C.: Carnegie Corporation.
Carnegie Council on Adolescent Development. 1995. Personal communication with Turning Points Evaluator.
Center on Hunger, Poverty, and Nutrition Policy. 1993. Statement on the Link between Nutrition and Cognitive Development in Children. Medford, Mass.: Tufts University School of Nutrition.
Centers for Disease Control and Prevention. 1994. Guidelines for school health programs to prevent tobacco use and addiction. Morbidity and Mortality Weekly Report 43(RR–2):1–18.
Centers for Disease Control and Prevention. 1997. Guidelines for school and community health programs to promote physical activity among youth. Morbidity and Mortality Weekly Report.
Centers for Disease Control and Prevention. 1996. Guidelines for school health programs to promote healthy eating. Morbidity and Mortality Weekly Report 45(RR-9).
Collins, J.L., Small, M.L., Kann, L., Pateman, B.C., Gold, R.S., and Kolbe, L.J. 1995. School health education. Journal of School Health 65(8):302–311.
Comer, J.P. 1984. Improving American Education: Roles for Parents. Hearing Before the Select Committee on Children, Youth, and Families. Washington, D.C.: U.S. Government Printing Office.
Comer, J.P. 1988. Educating poor minority children. Scientific American 259(5):42–48.
Commission on the Reorganization of Secondary Education. 1981. Cardinal Principles of Secondary Education. Bulletin #35. Washington, D.C.: Bureau of Education.
Cortese, P., and Middleton, K., eds. 1994. The Comprehensive School Health Challenge. Santa Cruz, Calif.: Education, Training, and Research Associates.
Davis, M., Fryer, G.E., White, S. and Igoe, J.B. 1995. A Closer Look: A Report of Select Findings from the National School Health Survey 1993–1994 . Denver, Colo.: Office of School Health, University of Colorado Health Sciences Center.
Dryfoos, J.G. 1994. Full-Service Schools: A Revolution in Health and Social Services for Children, Youth, and Families. San Francisco, Calif.: Jossey-Bass.
Duffy, J. 1974. A History of Public Health in New York City, 1866–1966 . New York: Russell Sage Foundation.
Education Development Center. 1995. The Status of School Health: Annex 1 to the Working Paper of the World Health Organization Expert Committee on Comprehensive School Health Education and Promotion. Newton, Mass.: Education Development Center.
Edwards, L.H. 1992. Organizational models for school health. In Principles and Practices of Student Health, Volume Two: School Health, H.M. Wallace, K. Patrick, G.S. Parcel, and J.B. Igoe, eds. Oakland, Calif.: Third Party Publishing.
Falck, V., and Kilcoyne, M. 1984. A health promotion program for school personnel. Journal of School Health 54(6):239–242.
Goldberg, M., and James, H. 1983. A nation at risk: the report of the National Commission on Excellence in Education. Phi Delta Kappan 65(1):14–18.
Hilmar, N.S., and McAtee, P. 1973. The school nurse practitioner and her practice: A study of nurses in elementary schools . Journal of School Health 43(7):431–441.
Hirsch, D. 1995. Health-Promoting Schools: From Ideas to Action. Frontiers in Education: Schools as Health Promoting Environments. Review of conference held in Geneva, Switzerland, February, 1995, jointly sponsored by the Johann Jacobs Foundation and the Carnegie Corporation.
Hodgkinson, H.L. 1993. American education: The good, the bad, and the task. Phi Delta Kappan 74:619–623.
Institute of Medicine. 1994. Reducing Risks for Mental Disorders. Washington, D.C.: National Academy Press.
Institute of Medicine. 1995. Defining a Comprehensive School Health Program: An Interim Statement. Washington, D.C.: National Academy Press.
Jamison, J. 1993. Health education in schools: A survey of policy and implementation. Health Education Journal 52(2):59–62.
Joint Committee on Health Education Terminology. 1991. Report of the 1990 Joint Committee on Health Education Terminology. Journal of Health Education 22(2):99–108.
Joint Committee on National Health Education Standards. 1995. National Health Education Standards: Achieving Health Literacy. Atlanta, Ga.: American Cancer Society.
Kohn, M.A. 1979. School Health Services and Nurse Practitioners: A Survey of State Laws. Washington, D.C.: Center for Law and Social Policy.
Kolbe, L.J. 1986. Increasing the impact of school health promotion programs: Emerging research perspectives. Journal of Health Education 17(5):47–52.
Kort, M. 1984. The delivery of primary health care in American public schools, 1890–1980. Journal of School Health 54(11):453–457.
Lavin, A.T., Shapiro, G.R., and Weill, K.S. eds. 1992. Creating an Agenda for School-Based Health Promotion: A Review of Selected Reports . Boston: Harvard School of Public Health.
Lee, M., and Bennett, B. 1985. Centennial articles. Journal of Physical Education, Recreation and Dance Centennial Issue 56(4):19–27.
Leeds, S., Heneson-Walling, R., and Shwab, J. eds. 1980. EPSDT: A Guide for Educational Programs. Washington, D.C.: U.S. Government Printing Office.
Lynch, A. 1977. Evaluating school health programs. In Health Services: The Local Perspective, A. Levin, ed. New York: Academy of Political Science; Proceedings of the Academy of Political Science 32(3):89–105.
Maysey, D.L. 1988. School worksite wellness programs: A strategy for achieving the 1990 goals for a healthier America. Health Education Quarterly 15(1):53–62.
McGinnis, J.M., and DeGraw, C. 1991. Healthy Schools 2000: Creating partnerships for the decade. Journal of School Health 61(7):292–297.
Means, R.K. 1975. Historical Perspectives on School Health. Thorofare, N.J.: Charles B. Slack.
Meyers, A.F., Sampson, A.D., Weitzman, M., Rogers, B.L., and Kayne, H. 1989. School breakfast program and school performance. American Journal of Diseases and Children 143:1234.
Nader, P.N. 1990. The concept of comprehensiveness in the design and implementation of school health programs. Journal of School Health 60(4):133–138.
National Association for Sport and Physical Education. 1995. Moving into the Future: National Standards for Physical Education: A Guide to Content and Assessment. St. Louis, Mo.: Mosby.
National Commission on Children. 1991. Beyond Rhetoric: A New American Agenda for Children and Families. Washington, D.C.: U.S. Government Printing Office.
National Education Goals Panel. 1993. The National Education Goals Report: Building a Nation of Learners, Volume One: The National Report . Washington, D.C.: U.S. Government Printing Office.
National Education Goals Panel. 1994. The National Education Goals Report: Building a Nation of Learners. Washington, D.C.: U.S. Government Printing Office.
National Nursing Coalition for School Health. 1995. School health nursing services: Exploring national issues and priorities. Journal of School Health 65(9):370–389.
National Research Council. 1996. National Science Education Standards . Washington, D.C.: National Academy Press.
Office of Technology Assessment, Congress of the United States. 1995. Risks to Students in School. OTA–ENV–633. Washington, D.C.: U.S. Government Printing Office, September.
Pate, R.R., Small, M.L., Ross., J.G., Young, J.C., Flint, K.H., and Warren, C.W. 1995. School physical education. Journal of School Health 65(8):312–318.
Pateman, B.C., McKinney, P., Kann, L., Small, M.L., Warren, C.W., and Collins, J.L. 1995. School food service. Journal of School Health 65(8):327–332.
Pigg, R.M. 1992. The school health program: Historical perspectives and future prospects . In Principles and Practices of Student Health, Volume Two: School Health, H.M. Wallace, K. Patrick, G.S. Parcel, and J.B. Igoe, eds. Oakland, Calif.: Third Party Publishing.
Proctor, S.T., Lordi, S.L., and Zarger, D.S. 1993. School Nursing Practice Roles and Standards. Scarborough, Maine: National Association for School Nurses.
Ross, J.G., Einhaus, K.E., Hohenemser, L.K., Greene, B.Z., Kann, L., and Gold R.S. 1995. School health policies prohibiting tobacco use, alcohol and other drug use, and violence. Journal of School Health 65(8): 333–338.
Silver, H.K., Igoe, J.B., and McAtee, P. 1976. The school nurse practitioner: Providing improved health care to children. Pediatrics 58(4):580–584.
Simons-Morton, B.G. 1992. Health-related physical education. In Principles and Practices of Student Health, Volume Two: School Health, H.M. Wallace, K. Patrick, G.S. Parcel, and J.B. Igoe, eds. Oakland, Calif.: Third Party Publishing.
Slavin, R.E., Madden, N.A., Karweit, N.L., Dolan, L.J., and Wasik, B.A. 1992. Success for All: A Relentless Approach to Prevention and Early Intervention in Elementary Schools. Arlington, Va.: Educational Research Service.
Sliepcevich, E. 1964. School Health Education Study: A Summary Report. Washington, D.C.: School Health Education Study.
Small, M.L., Majer, L.S., Allensworth, D.D., Farquhar, B.K., Kann, L., and Pateman, B.C. 1995. School health services. Journal of School Health 65(8):319–326.
Solloway, M.R., Pine, Y., and Anderson, E. 1995. Health supervision and school health services for children. In Child Health Supervision , M.R. Solloway and P.P. Budetti, eds. Arlington, Va.: National Center for Education in Maternal and Child Health.
Stone, E.J. 1990. ACCESS: Keystones for school health promotion. Journal of School Health (60)7:298–300.
Tyack, D. 1992. Health and social services in public schools: Historical perspectives. The Future of Children: School Linked Services, R.E. Behrman, ed. Los Altos, Calif.: Center for the Future of Children, David and Lucille Packard Foundation 2(1):19-31.
U.S. Department of Education. 1995. School-Linked Comprehensive Services for Children and Families: What We Know and What We Need to Know. Washington, D.C.: U.S. Department of Education, SAI 9503025.
U.S. Department of Education and U.S. Department of Health and Human Services. 1993. Together We Can: A Guide for Crafting a Profamily System of Education and Human Services. Washington, D.C.: U.S. Government Printing Office.
U.S. Department of Health and Human Services, Public Health Service. 1991. Healthy People 2000: National Health Promotion and Disease Prevention Objectives. DHHS Publication No. (PHS) 91-50213, Washington, D.C.: U.S. Government Printing Office.
University of Colorado Health Sciences Center, Office of School Health. 1991. The Community Health Nurse in the Schools. Denver, Colo.: University of Colorado Health Sciences Center.
Wagner, M., Golan, S., Shaver, D., Newman, L., Wechsler, M., Kelley, F. 1994. A Healthy Start for California's Children and Families: Early Findings from a Statewide Evaluation of School-Linked Services . Menlo Park. Calif.: SRI International.
Walker, D.K., Butler, J.A., and Bender, A. 1990. Children's health care and the schools. In Children in a Changing Health System: Assessments and Proposals for Reform, M.J. Schlesinger and L. Eisenberg, eds. Baltimore: Johns Hopkins University Press.
Wallace, H.M., Patrick, K., Parcel, G.S., and Igoe, J.B., eds. 1992. Principles and Practices of Student Health, Volume Two: School Health . Oakland, Calif.: Third Party Publishing.
Who's Who Among American High School Students. 1994. Twenty-Fifth Annual Survey of High Achievers. Views on Education, Social and Sexual Issues, Drugs. Lake Forest, Ill.: Educational Communications. Health, State of New Mexico.
















































