Commentary
A Progress Report on Computer-Based Patient Records in Europe
Jan H. van Bemmel, Astrid M. van Ginneken, and Johan van der Lei
After more than two decades of pioneering efforts, in both the United States and Europe, a new era in the use of computer-stored patient data has clearly begun. The proliferation of inexpensive personal computers and workstations, the development of more user-friendly interfaces, the standardization of network technology, the original release of this report 6 years ago, and the stimulation of health care telematics (i.e., network communications) in Europe have contributed significantly to this growing interest. Equally important, developers of systems have acquired much experience since they first attempted to develop electronic patient records, and their subsequent attempts have become more successful and gained momentum.
In this commentary we discuss some recent developments in computer-based patient records (CPRs) in Europe and review some CPR developments in Europe that fall within the Framework Programs on Research and Development of the European Union. Specifically, we review European developments in CPRs for primary care, clinical care (i.e., hospital care), and shared care. We also address the use of CPR data beyond patient care and two barriers to CPR development: protection of patient confidentiality and standards development for data.
The Current State of CPRs in Europe
Computer-based information systems are now abundant in a large percentage of European hospitals as well as in primary care settings. Systems support general tasks such as patient administration, scheduling, and billing, as well as specific tasks such as in the clinical laboratory, radiology, or the catheterization laboratory. Hospital information systems are primarily administration oriented
and seldom contain patient record data other than, for example, laboratory results, drug prescriptions, or diagnostic codes. Some systems store patient data, but none of them fully replaces the paper-based patient record. Many existing systems are not connected or are only loosely interconnected in networks. CPRs are being developed as part of a hospitalwide network (Degoulet et al., 1991; Van Mulligen et al., 1994; Scherrer et al., 1995) or as stand-alone or interconnected applications, such as in primary care (Westerhof et al., 1987; Branger et al., 1992; van der Lei et al., 1993). Increasingly, systems are being interconnected by electronic data interchange.
The field of hospital information systems in Europe consists, on the one hand, of mainly homemade systems (e.g., Bakker, 1984; Scherrer et al., 1995) sometimes supporting a group of hospitals and, on the other, of systems offered by industry, mainly of U.S. origin. A wide variety of information systems are operational on different platforms. Information systems in Europe reflect the differences in health care organizations which arise from the different historical developments, legislation, education, and languages among European countries. Therefore, systems developed in one European country are rarely installed in another country. This is also why the European hospital information system industry, with few exceptions, is virtually absent from the global market.
The differences in health care structures of different European countries might pose less of a problem for patient-centered approaches, such as CPRs. In all countries, patient care itself is quite similar. Europe has succeeded early at its attempts at CPR development and has since made considerable progress in the use of CPRs, especially in the primary care setting (van der Lei et al., 1991a; Millman et al., 1995). On the basis of these successes, several collaborative projects were started in health care; these were financially subsidized in part by the European Union (EU, 1994). Three developments related to CPRs in Europe deserve attention: the use of CPRs in the primary care setting, in hospitals, and for shared care (i.e., collaboration between care providers). In addition, in the area of standardization in health care, the European Union plays a pivotal role on a global scale as well (De Moor, 1993).
Network technology and communication (in Europe the latter is called telematics) are now prominent developments in information technology and have a large impact on health care (Branger et al., 1992; EU, 1994). By using standard communication networks and standard software (De Moor, 1993), data interchange between the four levels of health care delivery (i.e., the region, the institution, the clinical department or outpatient clinic, and the individual physician, nurse, or patient) is more efficient. A fully operational exchange of patient data between systems, with proper authorization, is one of the present challenges in European health care.
The data in CPRs are not begging to be used for electronic data exchange, research, and shared care. The use of CPRs for purposes other than direct patient care has been associated with several problems (van der Lei et al., 1991a; Vlug
and van der Lei, 1995). These limitations are, for instance, the lack of a common terminology for patient data collection, or the use of different modes for the CPR systems. As the knowledge gained from experience accumulates, CPR developers learn important lessons, particularly the need to develop structured patient records based on a clear conceptual model. If CPR systems are not based on a conceptual model, and if the data in CPRs are not well structured, it will not be possible to use CPR data for different goals, nor will it be possible for such data to be exchanged between health care providers to support shared care. Therefore, if CPR systems are to be used for these other goals, care providers should realize that it is not sufficient that the systems merely support their own practice or clinic, but they should take care that patient data can be exchanged over the entire health care domain and be used, for instance, to support clinical research, decision making, the assessment of the quality of care, or management and planning.
A variety of CPR applications and projects have been completed or are ongoing including those supported through Framework Programs on Research and Development of the European Union. They concern computer-based records for primary care, in hospitals, and for shared care, as well as the use of data in CPRs for research, assessment of the quality of care, and decision support. Other projects focus on what the Institute of Medicine (IOM) Committee on Improving the Patient Record classified as barriers to CPR development: privacy and confidentiality and standardization of terminologies and data-exchange formats.
Several developments related to CPRs in Europe are discussed below, including the status of CPRs in the primary care settings, in hospitals, and in shared care (i.e., collaboration between care providers). The final sections consider more specific uses of CPR data and remaining barriers to wider use of the computer-based patient record.
CPR Systems in Primary Care
In some European countries, especially The Netherlands (van der Lei et al., 1993) and the United Kingdom (Millman et al., 1995), there has been a rapid increase in the use of information systems by general practitioners (GPs) in primary care (Figure 1). CPRs are incorporated into these information systems and are quickly replacing existing paper-based records. The use of CPRs by GPs in particular is rapidly increasing. At the beginning of 1996 it was estimated that more than 90 percent of all GPs in The Netherlands and the United Kingdom used information systems in their practices. About 50 percent of Dutch GPs had implemented a CPR system for the support of patient care and about 25 percent of GPs had a paperless office.
Similar figures apply to the United Kingdom (Millman et al., 1995). This is directly related to the fact that in both the United Kingdom and The Netherlands, GPs are the ''gatekeepers" in health care. Most GPs run a practice by themselves or with a small number of colleagues. In contrast, specialists work in large institutions
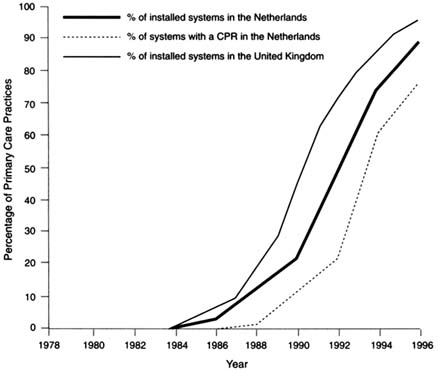
FIGURE 1 Growth of installed information systems and computer-based patient records in primary care in The Netherlands (100% represents 6,500 general practitioners [GPs]) and England and Wales (where 100% represents 9,000 GPs) as a function of time. The values for 1996 are extrapolations. Not indicated is the growing number of primary care systems that are electronically connected to other health care systems (see also the text and Figure 3).
in more complex settings, involving many more departments and personnel. Furthermore, GPs keep less extensive records so that data entry is less time-consuming and less detailed.
The actual situation in The Netherlands offers a good example of both the success and the potential use of CPRs (van der Lei et al., 1993). This can be attributed to four factors: (1) the role of GPs, (2) physician training, (3) the structure of health care, and (4) population-based care.
Role of GPs
From the outset, professional organizations of GPs have played an active role in setting guidelines for information systems in general practice and in assessing
the systems available in the market. This active role was started in the early 1980s, when they identified the basic needs of GPs for using systems in their practices and set the first broad guidelines for systems tailored specifically for primary care. Furthermore, these organizations announced to industry that they would recommend to their members that they use only those systems that would meet their requirements. In this way, a de facto standard was established. Since then, systems requirements are refined and extended every 2 to 3 years, and vendors must submit their systems for reevaluation by professional organizations. This iterative way of refining guidelines and assessing systems gives potential buyers of systems a basis on which to judge the available information systems. It also gives vendors clear-cut standards for their products. During the last 15 years, the definition of standards started with requirements for patient administration and evolved into standards for diagnostic coding (in all systems the International Classification for Primary Care has been implemented [Lamberts and Wood, 1987]), drug prescriptions (all systems use the same national thesaurus for drugs), and the type of data to be contained in a basic CPR and requirements for electronically interchanging patient data between different systems in the primary care setting, that is, from one GP's system to that of another.
Training
The success of information systems is largely determined by physicians' expectations. Education at medical faculties of universities prepares physicians in the use of computer-based information systems and patient records. Early on, students get acquainted with how to use computers for the documentation of patient data in CPRs. Professional organizations have also ensured that postgraduate training of GPs conveys a realistic set of expectations. These expectations must be realistic, because if they are too high they lead to disillusionment, and if they are too low they may impede the introduction of systems. The training emphasizes that the proper use of systems and CPRs reduces administrative workload, increases the accuracy of billing (no accountable patient data are lost), and enables the production of referral letters, the use of electronic data interchange, and the tracking of certain categories of patients.
Potential users should realize that, certainly at the beginning, investments must be made. The investments must be expressed not only in financial terms but also in time and personal efforts. For instance, for a typical practice of about 2,300 patients, it takes about 2 years for all patient data to be entered into the system's CPR. This data transcription from paper to computer is most often done at the time that patients come for a consultation, since the majority of patients pay a visit to their GP once every 2 years. A GP who is just starting to use a CPR system needs an extra 2 to 3 minutes during the consultation. The GP's assistant enters data related to all administrative operations, such as patient admission and patient scheduling, but the GP enters the patient care-related data into the CPR.
Structure of Health Care
The factors described above are related to the role and training of GPs in using CPRs and may be useful for other countries. A third factor, however, is strongly related to the structure of health care in The Netherlands, which in many ways is comparable to that in the United Kingdom and Scandinavian countries. Patients in The Netherlands and the United Kingdom have a single GP who coordinates their health care, acting as a gatekeeper to other specialists; the latter report back to the GP. Several projects are now under way to use electronic data interchange for this GP-specialist communication (see the section on "CPR Systems for Shared Care," page 32). Thus, in principle, the GP coordinates the health care-related data for a single patient over the patient's lifetime and is requested by other specialists to share that information. The GP's role as coordinator eases the introduction of CPR systems because the demands of care are easier to meet when the data are available in electronic form. This factor may be increasingly relevant in the United States as managed care and capitated reimbursement continue to penetrate the health care delivery market.
Population-Based Care
A fourth reason for the success of the acceptance of CPRs in the primary care setting is the fact that Dutch general practice is population-based care, in contrast to institution- or physician-based care. The Dutch primary care system can be characterized as providing services that are responsive to the needs both of the individual patients and the population at large. Such a population-based orientation creates demands that are easier to satisfy when CPRs are introduced. For instance, CPRs with properly coded data greatly facilitate the creation of a gender-age register to report on statistics in primary care or active case finding (e.g., for periodic cervical smears or cardiovascular risk assessments). The availability of CPRs facilities studies on the use and effects of drugs in the population and postmarketing drug surveillance (see the section on "Use of CPR Data," page 34).
CPR Systems in Hospitals
Electronic information technology has been introduced in all hospitals in Europe. This is no longer restricted to special areas of care, such as radiology or the laboratory. In principle, the available technology allows central and monolithic hospital information systems to be transformed into hospitalwide networks with "intelligent" workstations or personal computers throughout the hospital, from the consultation room to close to the bedside. This transformation is just beginning, however. At present, graphical workstations and network technology
are the latest developments in the computer industry. Client-server protocols ease the integration of systems and distribution of processing tasks (Degoulet et al., 1991; Van Mulligen et al., 1994; Nowlan et al., 1994). In principle, workstations offer an environment in which, from the user's perspective, all applications running either locally or through a network act as a single integrated system. Several institutions are developing health care workstations that enable the integration of patient data scattered throughout different systems (Degoulet et al., 1991; Van Mulligen et al., 1994; van Bemmel et al., 1996a). In principle, such systems offer to the clinician on one computer screen patient data, images, and biological signals, regardless of the computer on which they are stored or the system on which they are processed.
Yet, although the technical issues involved in the integration of various systems were slowly being solved, the absence of a conceptual model for a CPR was increasingly becoming a stumbling block, particularly as the amount of available data increased. Thus emerged a trend in which a technical infrastructure (the platform for the CPR) takes care of the communication with the numerous systems available in the hospital, including legacy systems, such as a laboratory system, a picture archiving and communication system (PACS), or an electrocardiogram (ECG) interpretation system. CPRs are developed at the core of this integration platform. This distinction is not trivial. When developing the platforms, questions such as how an existing legacy system should be embedded are addressed on a technical level. On the level of CPR development, questions relate, for example, to how the data will be presented to the user in a consistent manner or what additional data the physician must record are addressed.
Platforms for CPRs
Both the Helios (Degoulet at al., 1991) and the Hermes (Van Mulligen et al., 1994) integrated clinical workstations offer an environment for systems integration. Communication between applications is automatically performed by the workstation and follows ISO1 standards (ISO, 1987). Instead of having one large central database of patient data, all existing databases and applications are left unchanged and patient data are combined by the workstation on demand. This has two advantages over one large integrated database. First, data can remain distributed and stored at places that are most convenient (i.e., close to where the data are collected and used). Second, commercially available applications can be used for data processing without modifying them.
The Hermes workstation was initially developed to support clinical data analysis, but its architecture has also been extended to support patient care. It is
integrated with the generic CPR system ORCA2 (van Ginneken, 1996). Hermes is also able to integrate with legacy systems by encapsulation.
The Helios workstation, similar to Hermes in many respects, also integrates alphanumeric data (text), images, and biological signals. The Helios platform is being used as one of the building blocks of a new generation of hospital information systems. The Hermes approach, originally developed on a Unix platform, has now migrated to a Windows NT/95 environment, forming the basis for the European project I4C (van Bemmel et al., 1996), as explained below.
Integrated CPRs
As an example of the introduction of a CPR in a clinical department, we briefly describe the European project I4C (Integration and Communication for the Continuity of Cardiac Care). Although I4C is intended to support cardiology, it uses a generic CPR, ORCA, which is also applicable to other departments. In this way, the CPR used in the I4C project can be used by many other clinical departments (van Ginneken et al., 1995; van Ginnekin and Stam, 1995), because it contains a variety of patient data: patient history, physical examination findings, laboratory test results, images, biological signals, and so forth. Real-time data, such as from the catheterization laboratory, are also intended to be incorporated into the CPR. Data are meant to be used by more than one physician (e.g., the cardiologist often must coordinate his or her treatment with that of other specialists in the hospital or with GPs in primary care).
Figure 2 presents the CPR structure that forms the basis for the I4C project, together with its branches to other systems in the hospital or elsewhere. Patient record data, as well as images such as echocardiograms and coronary angiograms, or signals such as ECGs or blood pressure curves are collected, stored, and presented by using the workstation.
The I4C project in principle is intended to support cardiac care, from prevention and treatment to follow-up and rehabilitation. This is accomplished by: (a) consistently recording patient data in the CPR; (b) accessing diagnostic and therapeutic information; (c) accessing patient data, images, and biological signals wherever they are stored and irrespective of where the inquiry originates; and (d) collecting well-defined reference sets of patient data.
Data are to be used not only for patient care, research, and education but also for the assessment of the quality of care and for management and planning. The fourth issue is similar to the data collection that resulted from the European CSE3 project that preceded I4C (Willems et al., 1991). The project is carried out by centers in The Netherlands—which provides coordination—the United Kingdom, France, Germany, Italy, and Greece.
CPR Data Entry
For a CPR to have benefits, the data in that record need to be structured and coded, at least to a certain degree. Obtaining structured and coded data, however, has proved to be a significant hurdle. Physicians are accustomed to paper records. How physicians use these records has been the subject of several European projects (e.g., Nygren and Henriksson, 1992). From such investigations it became apparent that physicians are far more likely to use computers to consult the data in present patient records than to enter patient data. This is not surprising: Data entry requires more effort from the physician than browsing through the record. Some researchers have argued that direct input by physicians will have to wait for radical improvements of the human-machine interface, such as speech input. Experience in a number of countries where GPs are particularly using CPRs (e.g., The Netherlands, the United Kingdom, and Sweden) has shown, however, that physicians will accept the limitations of the current human-machine interaction.
Views of CPR data for patient care, decision support, scientific data analysis, or assessment of quality of care require patient data to be highly structured and unambiguous. It is difficult to fulfill these requirements with narrative (textual) data (e.g., Moorman et al., 1994). Ideally, therefore, patient data should be acquired directly from the physician in a structured format and, preferably, should also be entered by the physician. To accomplish this, different approaches to data entry have received attention: form-driven data entry, natural language processing, and structured data entry. The last two methods are also the focus of several research projects in Europe (Nowlan and Rector, 1991; Baud et al., 1992; Moorman et al., 1994).
Natural Language Processing
Natural language processing intends to automatically extract coded medical data from free text. European research in this area has mainly been done by Baud and colleagues in Geneva (1992). The basic advantage of natural language processing is that physicians do not have to alter the way in which they express their findings or document their decisions. Only when its application domain is strictly
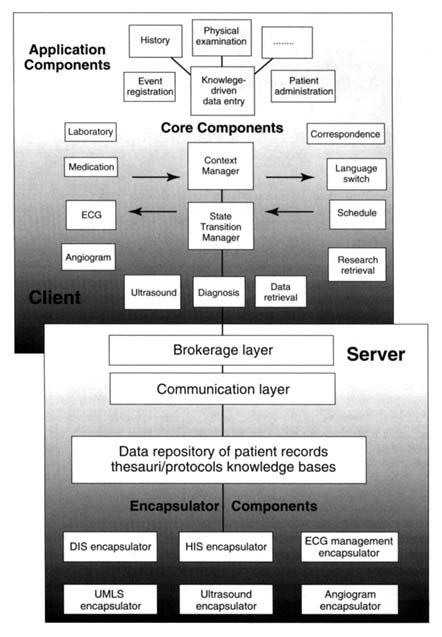
FIGURE 2 Example of the integration of a computer-based patient record (CPR) (ORCA; van Ginneken, 1996) in a clinical network of information systems being developed in the European project I4C (van Bemmel et al., 1996), in which centers from six countries collaborate. At the core of the CPR (called the client here) are three generic core components: the state transition manager, the context manager, and knowledge-driven data entry. The first two deal with all data acquisition, storage, and presentation and communication with the application components of the CPR system and the legacy systems elsewhere in the hospital. Communication is controlled by a brokerage layer and a communication layer, which are part of a group of servers. The broker follows protocols such as those agreed upon by the Common Object Request Broker Architecture (CORBA) Group (OMG, 1996); the communication layer provides data exchange via Electronic Data Interchange for Finance, Administration, Commerce, and Trade (EDIFACT) or HL-7. In the data repository, CPR data and knowledge bases are stored, together with coding systems and thesauruses for diagnoses and drugs. The six systems at the bottom are examples of "legacy systems" from which data (e.g., from a departmental or hospital information system), images (e.g., from an angiogram server), or biological signals (e.g., from an ECG management system) are to be transported to the CPR for presentation or processing. Integration with the legacy systems is provided by encapsulation (Van Mulligen et al., 1994).
confined can natural language processing offer advantages. A fundamental disadvantage of natural language processing is that the data-capturing process itself cannot be influenced and improved. Data that the physician has not written or spoken remain unknown. Freedom of expression is inherent to free text (Moorman et al., 1994). Therefore, it is difficult to impose structure on data that are used as input for natural language processing.
Structured Data Entry
Another way of data entry is context sensitive and is adaptable to different clinical domains. It is called structured data entry and consists of forms whose content is knowledge driven. In a structured data entry-oriented European project, the forms are structured, but their contents can continuously be adapted to accommodate the user's requirements and personal preferences (Moorman et al., 1994). In addition to a knowledge model, it contains a predefined vocabulary and specifications on how the terms of the vocabulary may be combined into meaningful expressions. The knowledge base keeps track of the individual physician's definitions of expressions with a nontrivial meaning, such as "the heart is normal" or "gastroenteritis complaints." When such expressions are used for the first time, the system will prompt the physician-user for an explicit description. Upon later use of such expressions, the system will store its explicit substitute. In this way, efficiency and completeness can be reconciled.
Structured data entry is also an efficient tool for enhancing data completeness and testing for data reliability (Whiting-O'Keefe et al., 1985; Wyatt, 1994).
Graphics and voice input may also serve to enhance the capabilities of structured data entry.
CPR Systems for Shared Care
An environment in which patient record data can be electronically interchanged regionally (Figure 3) is a necessary condition for a shared care environment (Branger et al., 1992, 1994; Branger and Duisterhout, 1995). Local and regional networks are increasingly used for the exchange of patient data between health care institutions. They are also used for communication with, for example, health insurance bodies, governmental organizations, libraries, and research institutions. Orders and payments are exchanged by electronic data interchange, databases are consulted remotely, and laboratory data or referral letters are mailed electronically. Communication between specialists and GPs is also increasingly taking place via telecommunication. In some instances specialists and general practitioners communicate directly with a patient in the patient's home, for example, patients with pacemakers, undergoing hemodialysis, or receiving palliative care. For some purposes, remote medical consultation (telemedicine) is also envisaged. Several regional shared-care networks are under development in Europe within the Framework Programs for Research and Development in health care telematics, as will be discussed below. Such regional networks are a logical extension of networks within hospitals.
With the existence of a computer-based shared care environment, new applications for patient-centered care have arisen, such as:
- GPs are able to send a patient's data to the hospital to obtain results or diagnostic advice instead of referring the patient.
- Patients' hospital stays are shorter and specialists may offer teleconsultation services.
- Outpatient clinics increasingly function as diagnostic screening and ambulatory care centers. Patients are referred to these clinics only when specific diagnostic tests or interventions must be performed.
- Patient admission and scheduling are greatly facilitated, resulting in better planning and decreased waiting times for examinations.
In the next two sections we provide two examples of European projects involving the use of CPR data for shared care. The first describes the project CoCo, concerning the coordination and continuity of health care (Bernstein and Jensen, 1994). The second describes a project that deals with the exchange of data in health care by smart cards, in this case, Diabcard (Schaefer and Sembritzki, 1996).
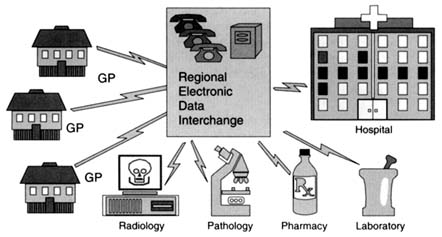
FIGURE 3 Regional electronic data interchange network to support shared care. General practitioners (GPs) in primary care are interconnected with other health care providers, such as the clinical laboratory, pharmacies, pathology laboratories, radiology departments, and departments in the hospital. Usually, such an electronic data interchange network makes use of public telephone lines or special lines (e.g., ISDN). In Europe, growing numbers of such networks are in development as part of European projects, such as the CoCo project (see text).
CoCo
The intention of the European project CoCo (Coordination and Continuity in Health Care) is to establish large-scale interconnected regional health care information networks, with the purpose of improving the coordination and continuity of health care (Bernstein and Jensen, 1994; van Bemmel et al., 1996). It uses available CPR-based systems and telecommunication infrastructures in the participating countries, European EDIFACT4 standards, and electronic mail techniques. The project will not interfere with regional regulations and will not impose new rules on the users of the networks. A major effort is dedicated to ensuring that the project will be implemented in a coordinated and standard way. The practical guidelines and the experiences with the collaboration within CoCo should also be usable for other applications in Europe. CoCo has two goals:
- Establishment of networks for the regional exchange of health care information. Each region will establish running networks that will allow for communication between all the major actors in health care: GPs, laboratories, radiology departments, hospitals, pharmacies, regional and national authorities, and social services and home care providers.
- Establishment of links between the regions through CoCo Link. Coco Link ensures coordination between the regions to facilitate a common methodology, to start concerted developments, and to use standardized communication in all regions. For instance, it will provide guidelines, it is responsible for developing an electronic test bed that can be used to EDIFACT solutions, and it will also establish networks between networks.
Many countries within the European Union, such as Denmark (coordination), The Netherlands, the United Kingdom, Ireland, Spain, and Greece, participate in CoCo. There is also an extension to Canada. A typical application within CoCo is shared care provided to patients with breast cancer. In this setting, GPs in primary care, internists, surgeons and radiotherapists in secondary care collaborate with nurses in home care, covering the entire period from the first patient visit to the GP up to chemotherapy or surgery and, eventually, palliative care. All care providers have access to the same CPR; nurses in the home care setting use portable computers to exchange data with the system in the clinic.
Diabcard
In Germany, health insurance cards are regulated by law. During 1993 and 1994, more than 70 million smart cards (chip cards) were issued to German citizens, and about 165,000 read-write stations were installed in, for instance, practices, hospitals, and emergency rooms. The insurance cards are primarily used for administrative purposes, but debate is ongoing about the use of these smart cards as carriers of patient data. The German project Diabcard, which has also been extended to other European countries, uses smart cards for the storage and exchange of data for patients suffering from diabetes (Schaefer and Sembritzki, 1996). Other projects, such as for patients with cancer, are also being introduced in the German health care system. Standardization of the health care data on such cards is of utmost importance.
Use of CPR Data
Once patient data are available from CPRs in primary care centers and hospitals, the data can be harvested. We briefly discuss here a project dealing with critiquing a physician's care (van der Lei et al., 1991; van der Lei and Musen, 1991; van Bemmel, 1993). Another European project intends to integrate treatment protocols with CPR systems. It is oriented toward the support of clinical oncology. The third project deals with the assessment of care by using large collections of CPR data harvested from operational CPR systems in the primary care setting. This project is directed toward the postmarketing surveillance of drugs (Vlug and van der Lei, 1995).
Critiquing a Physician's Care
Automated review of CPRs is expected to limit errors in the delivery of care and to control costs. Two projects, carried out with GPs in The Netherlands, have investigated whether CPRs contain sufficient information to support direct care by assessing CPR data and generating critiques and decision support. In the first project (HyperCritic [van der Lei et al., 1991; van der Lei and Musen, 1991]), a system of critiquing the treatment of hypertension was developed. The second project (AsthmaCritic [Kuilboer and van der Lei, 1997]) covers the area of chronic obstructive respiratory diseases. Both systems rely on CPRs for patient data. HyperCritic was assessed in a research project, and we summarize here some of the main outcomes (van der Lei et al., 1991).
The critiquing systems generate comments in two stages. First, CPR data are automatically interpreted to review the actions of the GP at a given visit (e.g., starting a new drug, continuing treatment with a drug, or replacing one drug with another). Second, each action is assessed. The system searches the CPR for conditions that contraindicate that action (e.g., contraindications to specific drugs), determines whether the preparations required for the action have been performed, determines whether the GP has performed the routine monitoring required by the action, and searches for any undesirable condition that might have resulted from the action. Review of the CPR requires detailed knowledge of drugs, such as customary dosages, contraindications, side effects, interactions, workup requirements, and criteria for judging the efficacy of the treatment. Computer-based critiquing of patient care was compared with peer review-based critiquing in the area of mild hypertension. The comparisons revealed the following:
- Automated assessment of CPR data by the computer-based critiquing system could compete successfully with peer review.
- The system was not able to reproduce some comments of experts. This was the result of insufficient CPR data, the lack of sufficient medical consensus, or omissions in the knowledge base of the critiquing system.
On the basis of the outcomes of this and other studies reported in the literature, the following can be concluded:
- Systems for the assessment of patient care should be able to acquire patient data automatically from the CPR.
- Ideally, the care assessment system should be functionally integrated with the CPR system.
Integration of Protocols with CPR Systems
In many patient care areas, protocols are used to increase both the efficiency and the quality of care. In principle, such protocols are not limited to certain hospitals, regions, or countries. This was the reason for starting a large European project on the use of protocols in health care (both in the clinic and in the primary care setting) called Prompt (Lagouarde et al., 1996; van Bemmel et al., 1996), which was based on the earlier European project Dilemma (Thomson, 1995). The project has been established by centers from the United Kingdom (which performs the coordination), France, and The Netherlands and intends to integrate these protocols with CPRs and to deliver and evaluate a set of tools for supporting the use of protocols. The initial focus of the project is oncology; this is now followed by a focus on the primary care and shared care settings.
The clinical objective is to install systems for supporting the treatment of cancer in specialty hospitals in the participating countries. Applications will be based on state-of-the-art therapeutic protocols. By the end of the project it is anticipated that the technology should be ready to be installed in centers in other countries as well. The following are other objectives of Prompt:
- extensions to each hospital system, to support GPs, interconnected by regional networks for shared care;
- initiation of comprehensive studies of the effects of the protocols on clinical outcomes; and
- generic versions of the protocols for other clinical disciplines.
Review of CPR Databases
It is expected that CPRs will increasingly be used to improve the quality of care in practices, departments, and institutions as well as, for instance, to support postmarketing surveillance studies. Pressure from law enforcement bodies, third-party payers, peer review organizations, hospitals, and physicians and patients themselves may lead to this use of automated review of CPRs. We briefly discuss a large ongoing project on the assessment of drug prescriptions in the population (Vlug and van der Lei, 1995; Visser et al., 1996). The project that is reported runs in The Netherlands, but similar projects have been started in other European countries (e.g., Germany and the United Kingdom).
Postmarketing surveillance examines the beneficial and adverse side effects of drugs on human health from the time that these drugs are marketed. Postmarketing surveillance consists of two stages: a hypothesis generation stage in which an effect or side effect is suspected and a hypothesis verification stage in which the hypothesis is tested. Hypothesis generation is typically based on the spontaneous reporting of potential side effects by physicians. Studies have indicated, however, that this spontaneous reporting leaves much to be desired. For
instance, Classen and colleagues (1991) studied the prescription of drugs in cases in which the drug prescription was changed, increased, or stopped. It was shown that computerized monitoring of adverse drug events in hospitals by using computer-stored patient data offers many advantages over the voluntary reporting of such events.
An extensive project that analyzes prescriptions in primary care to support the postmarketing surveillance of drugs is under way in The Netherlands. To test a hypothesis, large populations need to be monitored. Reports of patient contacts with GPs are anonymously sent to a research database. The data in that database are subsequently used to conduct postmarketing surveillance studies (Vlug and van der Lei, 1995). The Dutch authorities responsible for drug safety are investigating the potential use of this type of database. Preliminary results indicate that the CPRs can be used as a way to track large numbers of patients and that use of CPRs will allow researchers to build longitudinal databases (Visser et al., 1996). At the end of 1996, about 250,000 patients were followed longitudinally; this number will increase to about 1.5 million in the next few years.
Addressing Barriers
Privacy and Confidentiality
Now that CPR data are becoming available for the different goals mentioned in the introduction to this commentary, it is of great importance to protect these data, to guard the privacy of patients, and to protect the professional interests of health care providers (van Bemmel, 1992; Barber et al., 1996). Many parties (employers, insurance companies, etc.) are interested in permanent patient data, 5 and these data should be extremely well protected in CPR systems. In Europe there may be more sensitivity toward the improper use of patient data than elsewhere; this sensitivity could even impede the introduction of CPRs in some countries, and for some purposes could hamper the use of CPR data for goals other than patient care. In the different European countries, privacy laws control health care data, but privacy laws also exist in Europe as a whole. European law supersedes the laws of the individual countries. The right to privacy has been anchored in the Treaty for the Protection of Human Rights and Fundamental Freedom
(Treaty of Rome, 1954) and in European law (EU, 1995). Yet, it will be difficult to totally prevent the improper use of data stored in CPRs.
Because modern health care often requires shared care instead of care by a single physician only, the individual physician is no longer capable of personally guaranteeing the privacy of a patient's data. For that reason, after implementing regulations related to ensure the secrecy of patient data, modern societies must ensure the right to privacy. This means that in the different countries written regulations related to requests for personal data, including patient data, are required. These regulations should be supervised by a privacy committee and should contain descriptions of the purpose of the data registration that is maintained. It also should describe when data can be provided to third parties, and the right of all persons concerned to inspect, alter, and destroy their own data. In principle, these regulations do not concern data that have been made anonymous.
It is of utmost importance that in all (future) CPR systems proper measures be taken to protect the privacy of patients and their data. This issue is also the subject of discussions at the EU level, for example, in the standardization committees established for health care informatics and telematics. Some of the standardization activities related to CPRs are summarized in the following section.
Standardization
As discussed above, it is essential that standards for the acquisition, storage, and exchange of patient data be available. In health care this pertains to both administrative data and patient data. On the basis of the experiences over the past decade, a technical committee (TC 251 [De Moor and van Maele, 1996]) falling under CEN (Comité Europeén de Normalisation, the ''European Committee for Standardization") was established. This committee defines preliminary standards and compiles reports on the standards to be introduced in the different countries of the European Union (De Moor, 1993; De Moor and van Maele, 1996). For instance, the ability to link systems via standard interfaces is widely recognized as a necessity. Especially in Europe, where data cross regional and national boundaries, agreement on how to exchange patient data is urgent. Directly and indirectly, such standards will contribute to the quality and efficiency of patient care.
From the long list of preliminary standards that have been or are being elaborated by Technical Committee 251, a few examples specifically dealing with data in CPRs are provided in the following sections (De Moor, 1996).
Electronic Health Care Record Architecture
Work on defining the basic architecture for data contained in an electronic health care record has begun. Standardization is necessary if patient data are to be exchanged between different health care professionals. It is also necessary so that patients can travel or move from one region or country in Europe to another. The
architecture should enable physicians to use CPRs that are adapted to their own requirements and should therefore support a variety of formats. The aim of this standardization effort is not to specify the CPR system as such but to bring structure to the data stored in such records.
Coding Systems for Drugs
Standardization of coding systems for drugs concerns prescribing drugs and the effects of drugs on patients. A conceptual model for the correct labeling of drugs is foreseen within Technical Committee 251. The standard covers the identification of generic drug products as well as the drugs themselves. A coding system itself, however, is not intended.
Syntax for Health Care Data Interchange
Electronic messages in health care can be coded in many different ways. Therefore, consensus is required on the exchange formats for health care data between different systems. This has many advantages, because the systems' vendors can then handle the different data formats. The standard intends to define and adopt syntaxes for this exchange of information.
Exchange of Medical Images and Related Data
The medical image exchange standard concerns the exchange of high-volume data such as images or similar data. The Technical Committee 251 standard has adopted the industrial DICOM6 3.0 standard for medical images, enabling the possibility of standardized storage and global exchange of such images, which is important for supporting, for example, teleradiology or similar services.
User Identification
As open systems are gradually installed in hospitals and regional networks become operational, it will be important to prevent patient data from being used illegally. To ensure the proper use of patient data, it is necessary to positively identify authorized users. Software systems should therefore make use of automatic procedures for user identification, for example, by the use of passwords and different technical measures. Smart cards are other means of positive user identification (e.g., fingerprints or face recognition are possible techniques that could be standardized and that may eventually replace the more vulnerable passwords).
Conclusion
Significant progress has been made in Europe toward the primary recommendation of the IOM Committee on Improving the Patient Record's report over the past 6 years. Several factors account for the success to date. First, in those countries where CPRs are most prevalent, the health care delivery system or structure relies on a gatekeeper model and emphasizes primary health care and the health of the population. Thus, there is a recognized need for individual and aggregate patient data and a willingness to invest at both macro- (i.e., government) and microlevels (i.e., a practitioner) to make such data available. Second, CPR development projects are ideal for the EU insofar as they offer benefits both within and across countries and collaboration in their development may well speed up visible success. The evidence of political support and support by the medical professional organizations for CPRs sends a strong message to system developers and users, as well as to the general public.
Third, the emerging focus on conceptual models that build upon rather than are driven by the technology is a significant breakthrough in CPR development and will likely result in systems that can be adopted throughout Europe. Ultimately, this conceptual focus, which is also evident in the United States, may increase the ability of generic CPR systems to be transported globally. Fourth, collaboration between end-users and developers in system specification is a critical element of a sound CPR development process, aiding both the developers and users of the systems. Finally, the readiness of users with realistic expectations eases the implementation and increases the likelihood that CPRs will be used to their full potential. Thus, the education of health professionals is an important strategy in speeding CPR diffusion.
Like in the United States, important challenges remain to be addressed for CPR developers. First, continued support of CPR development efforts by supra-regional and national organizations is absolutely essential. Second, the issues surrounding the operational exchange of patient data must be fully explored and addressed. Third, protecting the confidentiality of patient data in the information age is a global issue that must be a priority in all countries and will ultimately require greater collaboration among countries as the technologies that support CPRs continue to evolve and are exploited in ways that we have not yet identified. Fourth, flexible, user-adaptable generic models for the generation of CPRs are needed to overcome the great variety in specialized care, the differences in culture among various clinics, and particularly in Europe, among countries.
References
ACR-NEMA (American College of Radiology and National Electrical Manufacturers Association). 1985. Digital Imaging and Communications Standard 300-1985. Washington, D.C.: NEMA Standards Publications.
Baud, R.H., A.M. Rassinoux, and J.-R. Scherrer. 1992. Natural language processing and semantical representation of medical texts. Methods of Information in Medicine 31(2):117–125.
Bakker, A. R. 1984. The development of an integrated and cooperative hospital information system. Medical Informatics 9:135–142.
Barber, B., A. Treacher, and K. Louwerse. 1996. Toward Security in Medical Telematics. Studies in Health Technology and Informatics, No. 27. Amsterdam: IOS Press.
Bernstein, K., and H. B. Jensen. 1994. Managing change in developing communication systems for integrated care; the Funen model. Pp. 266–269 in Proceedings of Medical Informatics Europe 1994, eds. P. Barahona, M. Veloso, and J. Bryant. Lisbon: Medical Informatics Europe.
Branger, P. J., J. C. van der Wouden, B. R. Schudel, E. Verboog, J. S. Duisterhout, J. van der Lei, and J. H. van Bemmel. 1992. Electronic communication between providers of primary and secondary care. British Medical Journal 305:1068–1070.
Branger, P. J., A. van't Hooft, J. S. Duisterhout, and J. van der Lei. 1994. A standardized message for supporting shared care. Pp. 473–477 in Proceedings of the 18th Annual Symposium for Computer Applications in Medical Care, ed. J. G. Ozbolt. (Special issue of the Journal of the American Medical Informatics Association 1994:473–477.)
Branger, P. J., and J. S. Duisterhout. 1995. Communication in health care. Methods of Information in Medicine 34:244–252.
Classen, D. C., S. L. Pestotnik, R. S. Evans, and J. P. Burke. 1991. Computerized surveillance of adverse drug events in hospital patients. Journal of the American Medical Association 266:2847–2851.
Degoulet, P., J. Coignard, F. C. Jean, et al. 1991. The Helios European project on software engineering. Pp. 125–137 in Software Engineering in Medical Informatics, eds. T. Timmers and B. I. Blum. Amsterdam: Elsevier Science.
De Moor, G. J. E. 1993. Standardization in medical informatics. Pp. 61–66 in 1993 Yearbook of Medical Informatics, eds. J. H. van Bemmel and A. T. McCray. Stuttgart: Schattauer Verlag.
De Moor, G. J. E., and G. van Maele, eds. 1996. Standards in Healthcare Informatics and Telematics. Brussels: CEN/TC 251.
EU (European Union). 1994. European Union DG XIII Work Programme on Health Telematics. Brussels: Commission of the European Communities.
EU. 1995. European Union Directive 95/46/EC of the European Parliament and of the Council of 24 October 1995 "On the Protection of Individuals with Regard to the Processing of Personal Data and on the Free Movement of such Data." Journal of the European Communities 38:L281/31–50.
ISO (International Standards Organization). 1987. Electronic Data Interchange for Administration, Commerce and Transport (EDIFACT), Application Level Syntax Rules, IS 9735.
Kuilboer, M. M., and J. van der Lei. 1997. Exploring the role of a critiquing system: A simulation. Journal of the American Medical Association in press.
Lagouarde, P., R. Thomson, J.-L. Renaud-Salis, et al. 1996. The PROMPT electronic health care record. In Proceedings of Medical Informatics in Europe 1996, ed. P. McNair. Amsterdam: IOS Press.
Lamberts, H., and M. Wood, eds. 1987. International Classification of Primary Care. Oxford, England: Oxford University Press.
Millman, A., N. Lee, and A. Brooke. 1995. Computers in General Practice. Parts I, II, and III . British Medical Journal 311:800–802, 864–867, and 938–941.
Moorman, P. W., A. M. van Ginneken, J. van der Lei, and J. H. van Bemmel. 1994. A model for structured data entry based on explicit descriptional knowledge. Methods of Information in Medicine 33(5):454–463.
Nowlan, W. A., and A. L. Rector. 1991. Medical knowledge representation and predictive data entry. Pp. 105–116 in Proceedings of Symposium on Artificial Intelligence in Medicine Europe,ed. M. Stefanelli. Heidelberg: Springer-Verlag.
Nowlan, W. A., A. L. Rector, T. W. Rush, and W. D. Solomon. 1994. From terminology to terminology servers. Pp. 150–154 in Proceedings of the 18th Annual Symposium for Computer Applications in Medical Care, ed. J. G. Ozbolt. (Special issue of the Journal of the American Medical Informatics Association 1994:150–154.)
Nygren A., and P. Henriksson. 1992. Reading the medical record. I. Analysis of physicians' ways of reading the medical record. Computer Methods and Programs in Biomedicine 39:1–12.
OMG. 1996. The Common Object Request Broker: Architecture and Specification (V2.0). X/Open Publ.
Schaefer, O. P., and J. Sembritzki. 1996. German patient cards and the impact on interoperability. Pp. 137–139 in Proceedings Toward an Electronic Patient Record '96, ed. P. Waegemann. Newton, Mass.: Medical Records Institute.
Scherrer, J.-R., C. Louis, and F. Borst. 1995. Diogene 2, a distributed hospital information system with an emphasis on its medical information content. Pp. 86–97 in 1995 IMIA Yearbook of Medical Informatics, eds. J. H. van Bemmel and A. T. McCray. Stuttgart: Schattauer Verlag.
Thomson, R. 1995. DILEMMA, decision support in primary are, oncology and shared care. Pp. 208–217 in Health in the New Communication Age , eds. M. F. Laires, M. J. Ladeira, and J. P. Christensen. Amsterdam: IOS Press.
Treaty for the Protection of Human Rights and Fundamental Freedom. Rome, 1954.
van Bemmel, J. H. 1992. Protection of medical data. Pp. 51–59 in Cryptography and Data Protection. Proceedings of the Royal Netherlands Academy of Arts and Sciences, Vol. 38, eds. J. H. van Lint and R. Tijdeman. Amsterdam: North-Holland.
van Bemmel, J. H. 1993. Criteria for the acceptance of decision support systems by clinicians—lessons from ECG interpretation systems. Pp. 7–10 in Proceedings of Symposium on Artificial Intelligence in Medicine Europe, eds. S. Andreassen and J. Wyatt. Amsterdam: IOS Press.
van Bemmel, J. H., J. Fox, and K. Bernstein. 1996. Multimedia shared patient records—European experiences. Pp. 164–168 in Proceedings Toward an Electronic Patient Record '96, ed. P. Waegemann. Newton, Mass.: Medical Records Institute.
van der Lei, J., M. A. Musen, E. van der Does, A. Man in 't Veld, and J. H. van Bemmel. 1991a. Review of physician decision making using data from computer-stored medical records. Lancet 338:1504–1508.
van der Lei, J., and M. A. Musen. 1991b. A model for critiquing based on automated medical records. Computers and Biomedical Research 24:344–378.
van der Lei, J., J. S. Duisterhout, H. Westerhof, W. Boon, P. V. M. Cromme, and J. H. van Bemmel. 1993. The introduction of computer-based patient records in the Netherlands. Annals of Internal Medicine 119:1036–1041.
van Ginneken, A. M., J. van der Lei, and P. W. Moorman. 1993. Toward unambiguous representation of patient data. Pp. 69–73 in Sixteenth Annual Symposium on Computer Applications in Medical Care, ed. M. E. Frisse. New York: McGraw-Hill.
van Ginneken, A. M., H. Stam, and P. W. Moorman. 1995. A multi-strategy approach for medical records of specialists. Pp. 290–294 in Proceedings of MEDINFO 95, eds. R. A. Greenes, H. E. Peterson, and D. J. Protti. Vancouver, B.C.: Coach Publishing.
van Ginneken, A. M., and H. Stam. 1995. Can one patient record accommodate the diversity of specialized care? Pp. 406–410 in Proceedings of the 19th Symposium on Computer Applications in Medical Care, ed. R. M. Gardner. Philadelphia: Hanley & Belfus.
van Ginneken, A. M. 1996. Structured data entry: ORCA combines the strength of two models. In Proceedings of the 20th Symposium on Computer Applications in Medical Care. Philadelphia: Hanley & Belfus.
van Mulligen, E. M., T. Timmers, J. Brand, et al. 1994. Hermes: A health care workstation integration architecture. International Journal of Biomedical Computing 34:267–275.
Visser, L. E., A. E. Vlug, J. van der Lei, and B. H. Ch. Stricker. 1996. Cough due to ace inhibitors: A case-control study using automated general practice data. European Journal of Clinical Pharmacology 49:439–444.
Vlug, A. E., and J. van der Lei. 1995. Postmarketing surveillance with computer-based patient records. Pp 327–330 in Proceedings of the 8th World Congress on Medical Informatics, MEDINFO 95, eds. R. A. Greenes, H. E. Peterson, and D. J. Protti. Vancouver, B.C.: Coach Publishing.
Westerhof, H. P., W. M. Boon, P. V. M. Cromme, and J. H. van Bemmel. 1987. ELIAS: Support of the Dutch general practitioner. Pp 1–10 in Present Status of Computer Support in Ambulatory Care, eds. P. L. Reichertz, R. Engelbrecht, and U. Picollo. New York: Springer-Verlag.
Whiting-O'Keefe, Q. E., D. W. Simborg, W. V. Epstein, and A. Warger. 1985. A computerized summary medical record system can provide more information than the standard medical record. Journal of the American Medical Association 254(9):1185–1192.
Willems, J. L., C. Abreu-Lima, P. Arnaud, J. H. van Bemmel, et al. 1991. The diagnostic performance of computer programs for the interpretation of electrocardiograms. New England Journal of Medicine 325:1767–1773.
Wyatt, J. C. 1994. Clinical data systems. Part 3: Development and evaluation. Lancet 344:1682–1688.
| This page in the original is blank. |
























