3
Recent Health Trends In The Native American Population
T. Kue Young
Introduction
The health of Native Americans has undergone substantial changes in the second half of the twentieth century. In broad terms, the recent epidemiologic history of Native American populations can be characterized by several key features: the decline but persistence of infectious diseases, stabilizing at a level still higher than that of the non-Native population; the rise in chronic diseases, especially diabetes; and the overwhelming importance of the so-called social pathologies—violence, unintentional injuries, and the ill effects of alcohol and drug abuse. The rise of chronic diseases also characterizes various indigenous populations around the world that are undergoing rapid sociocultural changes. Such diseases collectively have also been called ''Western" diseases (Trowell and Burkitt, 1981).
The long-term temporal changes in the pattern of health and disease of a population have been termed epidemiologic or health transition. One particular conception of that transition, originally proposed by Omran (1971, 1977, 1983), consists of three stages: the age of pestilence and famines, the age of receding pandemics, and the age of degenerative and man-made diseases. The pace of the transition differs among populations. Omran distinguishes among the classical or western model, exemplified by western Europe and North America; the accelerated model, characterized by Japan and eastern Europe; and the delayed model, which encompasses most developing countries. Other researchers (Olshansky
and Ault, 1986) have added a fourth stage—the age of delayed degenerative diseases—to account for the phenomena observed in the industrialized countries of a decline in mortality from such causes as heart disease and later age at death among the elderly.
The concept of epidemiologic transition has gained some currency in the population and health literature, and a variety of case studies from around the world have attempted to fit available health statistics to the theory. Furthermore, the theory has found applications in the area of health policy and planning, particularly in the context of developing countries (Gribble and Preston, 1993; Jamison et al., 1993; Mackenbach, 1994; Phillips, 1994). Several authors have specifically investigated the applicability of the theory to some Native American populations, for example, the Navajo (Broudy and May, 1983; Kunitz, 1983) and Canadian Indians (Young, 1988). Such attempts are difficult and infrequent, however, because they require the reconstruction of historical time series of mortality/morbidity rates. It is interesting to speculate whether the Native American population has diverged sufficiently from the broader North American experience to merit a separate model, or merely is experiencing a time lag of several decades, or fits better the model for developing countries. However, this issue is of less public health importance than discerning the major health trends to inform the planning and targeting of intervention programs.
This paper does not review the extensive literature on Native American health; a comprehensive review is available elsewhere (Young, 1994). Rather, the focus here is on broad trends based on U.S. data, especially those published by the U.S. Indian Health Service (IHS) (1990a, 1990b, 1994a, 1994b) on the population it serves. The following questions are addressed:
- What are the changes in Native American mortality/morbidity since the mid-1950s?
- Do Native Americans differ from non-Natives in their disease patterns?
- Are there regional and tribal differences within the Native American population?
- What are the determinants of the current patterns?
Before discussing these questions, we examine some methodological issues involved in the use and interpretation of Native American health data. This is followed by sections addressing overall health trends among Native Americans, relative risks of dying from various diseases, regional variations, and health determinants. A final section presents conclusions.
Methodological Issues
In the calculation of rates of occurrence of various events of interest among the Native American population (e.g., mortality, incidence, prevalence, health service use), there are problems associated with both the numerator and denominator. In the United States, the IHS began publishing data on Indians it served starting in 1955, the year it was formed. The IHS provides an important source of time-series data on some health indicators for a substantial proportion of the Native American population nationally. The IHS population, however, should not be equated with the total population of Native Americans in the United States. Data that are truly national in scope are sparse.
The issue of the number of Native Americans in the United States is a topic of major concern that is discussed elsewhere. Generally, there are two main sources of these data: the U.S. census (data based on self-identification) and the IHS (data based on eligibility for and use of service). The IHS in fact uses two populations: a service population, which is ultimately derived from the census, and a user population, based on the agency's own patient registration system.
The IHS estimates the service population by counting those Native Americans identified by the census who reside in geographical areas—on or near reservations—in which the IHS has responsibilities. The service population, which may or may not use IHS services, is used primarily for vital statistics. Service population data for intercensal years are estimated by a smoothing technique; with each new revision to decennial census counts, previously estimated intercensal populations are adjusted accordingly. Rates for 1981-89 differ among the 1991, 1992, 1993, and 1994 Trends in Indian Health reports as a result of revisions of the intercensal estimates using two versions of the 1990 census counts of Native Americans and a revision of the 1980 census itself (Indian Health Service, 1994a).
The IHS user population comprises Indian patients who have obtained direct or contract health services from the IHS or tribally operated facilities at least once during the past 3 years and thus are registered in the Patient Registration System. This population serves as the denominator for rates of morbidity and healthcare utilization.
In this paper, national estimates of mortality rates from various causes are derived primarily from the IHS Trends series, unless otherwise noted. For vital rates, the IHS receives Native American data from the National Center for Health Statistics (NCHS), extracted from records submitted electronically by state health agencies. There is a further complication in that vital rates prior to the 1992 Trends report were not based strictly on the IHS service population, but on the total Native American population in the "reservation states," i.e., states that contain Indian reservations (or
legally equivalent entities) and in which the IHS has responsibility. Thus Native Americans living in counties or cities not on or near a reservation but in the same state are included. The reservation state-based vital rates tend to be lower than the "true" IHS service population-based rates. For this paper, vital rates for 1955 to 1972 were obtained from the 1990 Trends report, which still used the reservation state method, whereas data for 1973 to 1990 were obtained from the 1994 Trends report, which used the IHS service population. However, while the subtle difference between the two data series should be recognized, it does not affect the overall conclusions to be drawn about long-term trends.
Another methodological issue arises from the considerable underreporting of Native American status that has been shown to occur with birth and death certificates. This is a phenomenon that varies widely among states/IHS areas; the problem is most serious for the California, Oklahoma, and Portland, Oregon areas (Centers for Disease Control and Prevention, 1993). (Note that California data are not included in any of the figures/tables in this paper.)
To illustrate the problem, a study that linked infant death records nationally with their birth records showed that more than a third of the deaths classified as Native American at the time of birth were coded as belonging to other races on the death certificates. The infant mortality rate would have increased from 9.8 to 14.4 per 1,000 if the improved race data drawn from this linkage had been used (Hahn et al., 1992). In a national study that linked deaths at all ages to the census, only 74 percent of deaths among individuals who had self-identified themselves as Native American in the census were found to be coded as such on their death certificates; this discrepancy could result in an underestimation of the death rate by 22 percent (Sorlie et al., 1992). Similar discordances were found in linkage studies conducted in specific regions. Examples are a study of infant deaths in Washington State that linked birth and death certificates (Frost and Shy, 1980) and a later study that linked deaths at all ages with the IHS patient registry (Frost et al., 1994). As noted above, the IHS patient registry includes Native Americans who actually use some IHS services and hence are bona fide Native Americans according to legal/bureaucratic criteria. This study also found that Native American status was more likely to be coded correctly for alcohol-related deaths than for diseases such as cancer. Concordance was highest for "full-blooded" Native Americans, and lowest for those with less than one-quarter Native American "blood quantum" (Frost et al., 1994).
Many regional/tribal studies of disease incidence rely on special disease registries. Identification of Native American status in such local registries has also been shown to be incomplete and inaccurate, particularly when it is validated through linkage with the IHS patient registry.
Examples include the Oregon Injury Registry (Sugarman et al., 1993); the Puget Sound Surveillance, Epidemiology and End Results cancer registry (Frost et al., 1992); and the Pacific Northwest Renal Network registry of end-stage renal disease (Sugarman and Lawson, 1993). In the Los Angeles County AIDS registry, only 6 cases had been identified as Native Americans by January 1, 1989; however, when community organizations providing support services to AIDS victims were surveyed, at least 60 Native American cases were identified (Lieb et al., 1992).
The population with which Native Americans are most often compared is the national "all-races" population of the United States, although sometimes specific subgroups such as blacks, whites, Asians, and Hispanics may be compared. It should be noted that the Native American population is younger than the U.S. national population. In the 1990 census, the median age of Native Americans was 26 years, compared with 33 years nationally, and 39 percent of the Native American population was under the age of 20, compared with 29 percent nationally. In most IHS publications, age-standardized rates (by the direct method) are usually provided, with the 1940 U.S. population as the standard. Because of the smaller size of the Native American population, 3-year moving averages are used, whereas single-year data for the U.S. all races population are reported.
Despite the above deficiencies and limitations of existing data sources, it is still possible to discern broad trends in the health and disease status of the Native American population. Indeed, one has the choice of basing planning and policy decisions on imperfect existing data or on no data at all.
Overall Trends
There is little doubt that the overall health status of Native Americans has substantially improved. Between 1940 and 1990, life expectancy at birth among Native Americans increased by 17.8 years to 69.1 years among men and by 25.6 years to 77.5 years among women. The gap between Native Americans and whites (both sexes combined) narrowed from 13.2 to 2.9 years (Indian Health Service 1990a, 1994a, 1994b). Figure 3-1 compares the infant mortality rate of Native Americans and the U.S. national population since 1955. The substantial decline and convergence is evident, although the low rate shown for Native Americans may have to be adjusted upward to account for under enumeration of Native American infant deaths.
Figure 3-2 shows, in semi-logarithmic scale, trends in age-standardized mortality rates from six causes: tuberculosis, gastroenteritis, cancer, motor vehicle accidents, homicide, and suicide. These six causes were
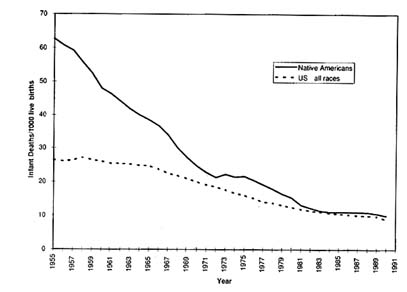
FIGURE 3-1 Trends in infant mortality rates: Native Americans and U.S. all-races national population. SOURCES: 1955-1972 data from Indian Health Service (1990a); 1973-1990 data from Indian Health Service (1994a).
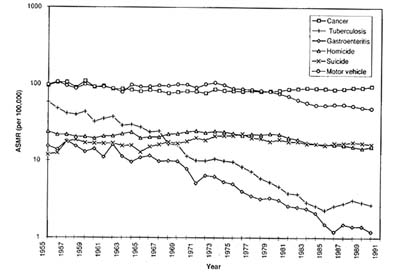
FIGURE 3-2 Trends in age-standardized mortality rates for selected causes among Native Americans. SOURCES: 19551972 data from Indian Health Service (1990a); 1973-1990 data from Indian Health Service (1994a).
selected because of the availability of data, as well as general trends they illustrate.
The most dramatic decline in mortality is for the two infectious diseases—tuberculosis and gastroenteritis—which are now insignificant causes of death among Native Americans. Of the six causes shown, cancer and motor vehicle accidents are the most important contributors to mortality, while suicide and homicide occupy an intermediate position. It should be noted that all three causes of injury, especially motor vehicle accidents, have shown some decline since the early 1970s, whereas the rate for cancer has remained relatively unchanged.
It should be cautioned that trend data are subject to variation in coding rules and practices over the years. Between 1955 and 1990, three different revisions of the International Classification of Diseases (ICD)—the seventh, eighth, and ninth—were in use. Moreover, ascription of a death to a specific diagnosis is often based solely on clinical impression and unsubstantiated by medical record or autopsy confirmation. The deficiencies of death certificates as a source of mortality information are well recognized in epidemiologic research (e.g., Kirchner et al., 1985; Israel et al., 1986).
Relative Risks
The risk of dying from various diseases among Native Americans relative to the total U.S. population can be determined from the age-standardized mortality rates of selected causes for the two populations. Native Americans experience excessive risk for most conditions listed in Table 3-1, with the exception of cardiovascular diseases and cancer.
As the rates of mortality from infectious diseases have declined substantially among both populations, the enormous gap between the two populations has also narrowed (Figure 3-3). However, this should not be interpreted to mean that infectious diseases are no longer a threat to the health of Native Americans. Unfortunately, with the exception of notifiable diseases such as tuberculosis, on which reasonably accurate statistics on the incidence of new active cases are kept, there is a general lack of national data on disease incidence. Figure 3-4 shows incidence data for tuberculosis, indicating that although a substantial decline in incidence has occurred, the gap between Native Americans and the national population is still wide. Moreover, many regional and local studies have demonstrated that Native Americans are still at high risk for such infections as meningitis, acute respiratory infections, viral hepatitis, sexually transmitted diseases, and intestinal infections (reviewed in Young, 1994).
Figure 3-5 shows the trends in age-standardized mortality rates for two chronic diseases, diabetes and cancer. In terms of mortality risk
TABLE 3-1 Age-Standardized Mortality Rates for Selected Causes: Native Americans (1989-91) and Total U.S. Population (1990)
among Native Americans relative to the total U.S. population, the two diseases are very different: elevated for diabetes and reduced for cancer. It has been recognized since the pioneering work of West (1974) that diabetes is a "new" disease among Native Americans, having developed from a rarity before World War II to an "epidemic" in recent years. Mortality from diabetes does not convey the excessive burden of this disease among most Native American tribes. Many glucose tolerance surveys have been conducted among Native Americans over the years (Gohdes, 1995), and estimates of prevalence of the disease can be derived from IHS patient care data (Valway et al., 1993). A national estimate of self-reported diabetes is also available from the Survey of American Indians and Alaska Natives, a special component of the 1987 National Medical Expenditures Survey, which covered Native Americans residing in IHS service areas who self-identified as being eligible for IHS services. The estimated age-adjusted prevalence of diabetes among Native Americans was 11 percent in men and 13 percent in women, more than twice the rates of the total U.S. population (Johnson and Taylor, 1991). A detailed review of diabetes among Native Americans is provided by Narayan in this volume.
A chronic disease of increasing concern among Native Americans is end-stage renal disease (ESRD). While the etiology of ESRD is varied,
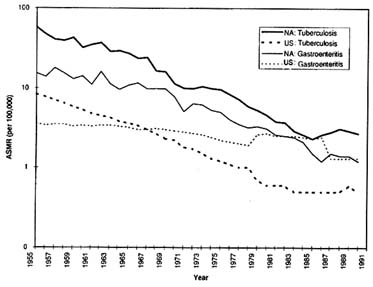
FIGURE 3-3 Trends in age-standardized mortality rates for tuberculosis and gastroenteritis: Native Americans and total U.S. population (semilogarithmic scale). SOURCES: 1955-1972 data from Indian Health Service (1990a); 1973-1990 data from Indian Health Service (1994a).
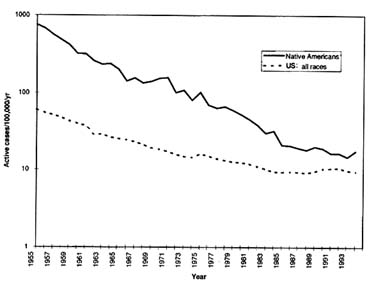
FIGURE 3-4 Trends in incidence of active tuberculosis: Native Americans and total U.S. population. SOURCES: 1955-1978 data from Indian Health Service (1979); other years from unpublished data from National Center for Health Statistics.
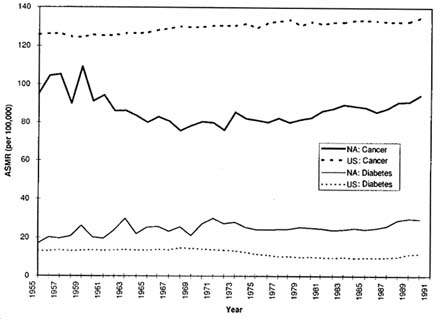
FIGURE 3-5 Trends in age-standardized mortality rates of diabetes and cancer; Native Americans and total U.S. population. SOURCES: 1955-1972 data from Indian Health Service (1990a); 1973-1990 data from Indian Health Service (1994a).
diabetes is an important cause. A national survey using Medicare data indicated that the incidence of ESRD was three times higher among Native Americans than among whites, and the incidence of ESRD due specifically to diabetes was six times higher (Newman et al., 1990).
Incidence data support the lower mortality risk for cancer among Native Americans relative to the total U.S. population. In a meta-analysis of seven published epidemiological studies on Native Americans in four U.S. states and two Canadian provinces from the mid-1950s to early 1980s, a low incidence was found when all cancer sites were combined. There are a few sites, however, for which Native Americans are at increased risk: kidney in men and gallbladder and cervix in women. On the other hand, Native Americans have a reduced risk of the most common cancers in the total U.S. population, such as lung, breast, and colon (Mahoney and Michalek, 1991). Similar findings were obtained from a national study using IHS hospital discharge data (Nutting et al., 1993).
Table 3-1 indicates that the risk of death from heart disease and stroke is slightly lower among Native Americans than among the total U.S. population, after adjustment for age. Incidence data are not readily available,
as there are no registries of myocardial infarction, stroke, or other cardiovascular disorders on a national scale. The hospital discharge rates for IHS facilities do offer one measure of morbidity for cardiovascular diseases, and indicate a lower rate than that shown by U.S. national data (Welty and Coulehan 1993). Self-reported prevalence data are available from the Survey of American Indians and Alaska Natives (Table 3-2); however, these data do not truly represent the risk of disease as cross-sectional data can capture only survivors of rapidly progressing and sometimes fatal diseases. A review of NCHS data on stroke shows that Native Americans had lower mortality rates than both blacks and whites between 1980 and 1990. Moreover, the trend has also been declining (Gillum, 1995).
Injuries, both intentional (homicide and suicide) and unintentional (accidents), constitute the second largest group of causes of mortality (after cardiovascular diseases) among Native Americans. While a decline in the past two decades can be observed, there is still a substantial gap as compared with the national population (Figures 3-6 and 3-7). Young adults are at highest risk for death from motor vehicle accidents, drowning, and firearm accidents, while falls and house fires disproportionately affect the elderly. One national survey of mortality from childhood injuries during 1980-85 showed that overall, the risk among Native Americans was 1.8 times that of the total U.S. population. For individual causes, the relative risks were 2.2 for motor vehicle occupant accidents, 3.9 for
TABLE 3-2 Prevalence (%) of Selected Self-Reported Chronic Diseases from the Survey of American Indians and Alaska Natives, 1987
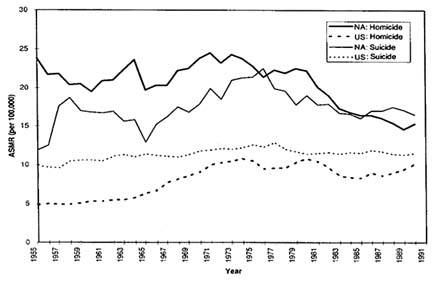
FIGURE 3-6 Trends in age-standardized mortality rates of homicide and suicide; Native Americans and total U.S. population. SOURCE: 1955-72 data from Indian Health Service (1990a); 1973-1990 data from Indian Health Service (1994a).
pedestrian accidents, 1.7 for drowning, 3.5 for poisoning, and 2.6 for aspiration (Waller et al., 1989).
Regional Variations
The preceding sections address disease and injury rates among Native Americans nationally. While Native Americans do share common experiences as a group, particularly as compared with the dominant North American society, they live in different ecological zones; have different genetic lineages; have different historical experiences; lead different life-styles; and maintain different values, customs, and traditions. All of these factors have some impact on the distribution of disease and injury, and indeed, substantial regional variations can be observed for almost all indicators.
Administratively, the IHS divides the United States into various areas, each of which serves a tribally mixed population, with the exception of the Navajo Area. Certain groups, however, are found mainly in one area, such as Eskimo and Aleuts in Alaska, various tribes belonging to the
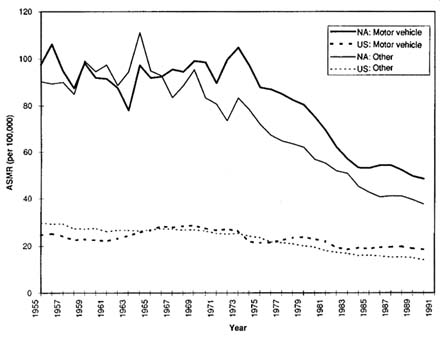
FIGURE 3-7 Trends in age-standardized mortality rates of unintentional injuries, Native Americans and total U.S. population. SOURCES: 1955-1972 data from Indian Health Service (1990a); 1973-1990 data from Indian Health Service (1994a).
Northwest Coast culture in the Portland Area, and Siouan-speaking tribes in the Aberdeen Area. On the other hand, the Nashville Area, for example, covers the entire eastern United States from Maine to Louisiana. Nevertheless, in the absence of data disaggregated into tribes, language families, or culture areas, the IHS administrative divisions provide a readily available perspective on geographic variation.
Figures 3-8, 3-9, and 3-10 show the variation in mortality rates by IHS region for selected infections, chronic diseases, and injuries, respectively. Where prevalence or incidence data exist, they tend to correspond to the regional variation in mortality, for example, in diabetes (Valway et al., 1993) and cancer (Nutting et al., 1993). For diabetes, the Alaska Area has the lowest rates, a reflection of its large Eskimo (Inuit) population. While the rates have increased in recent years, the circumpolar Eskimo in Russia, Alaska, Canada, and Greenland continue to be at substantially lower risk for diabetes than other American Indians (Young et al., 1992). At the other extreme are the Pima, who have the world's highest known prevalence of the disease and have been monitored extensively over the past
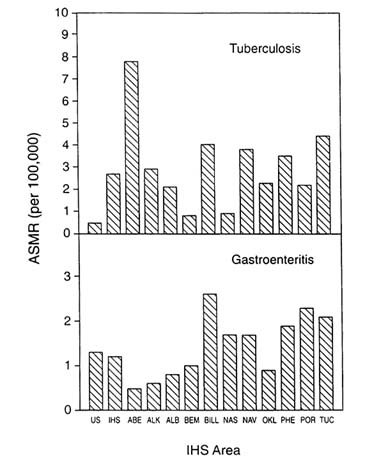
FIGURE 3-8 Regional variation in age-standardized mortality rates for selected infectious diseases, 1989-1991. SOURCE: Indian Health Service (1994b).
three decades (Knowler et al., 1990). With regard to cancer, the Eskimo are at high risk for certain sites, especially nasopharynx and liver (Lanier et al., 1989), contributing to the overall high cancer mortality and incidence rates of the Alaska Area.
The Navajo Area tends to have low mortality rates for cardiovascular disease. A relatively low risk of ischemic heart disease has been observed for some years among the Navajo and Apache, members of the Athapaskan language family who migrated to the Southwest from the northern reaches of the continent around the tenth century (and whose kin today largely inhabit the subarctic boreal forests of Alaska and northern
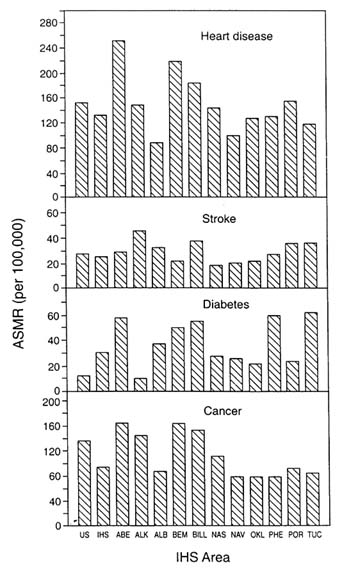
FIGURE 3-9 Regional variation in age-standardized mortality rates for selected chronic diseases, 1989-1991. SOURCE: Indian Health Service (1994b).
Canada). A study among the Navajo based on clinical records confirmed the low incidence of the disease in the mid-1980s, although even this group seems to be ''catching up" (Klain et al., 1988).
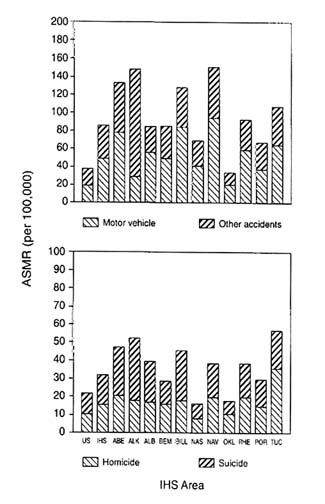
FIGURE 3-10 Regional variation in age-standardized mortality rates for injuries, 1989-1991. SOURCE: Indian Health Service (1994b).
Health Determinants
While individual diseases and health conditions have their unique causes or risk factors, there are some common factors which are responsible, by and large, for the observable pattern of health and disease. Some of these determinants relate to individual physiology and genetics, some to individual life-styles and health practices; and still others to socioeconomic status, community infrastructure, and environmental quality.
Native Americans provide an excellent case study of how genetics and environment interact to affect health status and the distribution of disease. For the chronic diseases, especially diabetes, there is strong evidence that genetic susceptibility is an important factor, and theories such as the "thrifty gene" (Neel, 1982) have been proposed to explain the explosive emergence of these diseases among Native Americans. The metabolic mechanisms are complex and not completely elucidated. From an evolutionary perspective, the diabetic genotype probably conferred a survival advantage under harsh, "feast-or-famine" conditions, but became a liability with an increasingly sedentary life-style and the assurance of a continuous and ample food supply, resulting in obesity and diabetes. There are also alternative theories (e.g., Ritenbaugh and Goodby, 1989; Szathmary, 1990) that can be applied more appropriately to Native American groups in the arctic and subarctic with a hunting tradition and a low-carbohydrate diet. The co-occurrence of gallbladder disease, obesity, and diabetes observed among diverse Native American populations led to the proposal of a ''New World Syndrome" of disorders that are likely to be genetically based and mediated through the metabolism of lipids (Weiss et al., 1984).
Historically, the high incidence of and mortality from infectious diseases among Native Americans have contributed to the view that such diseases as tuberculosis are "racial." It has since been recognized that conditions in the social environment probably play the leading etiologic role (Kushigemachi et al., 1984). However, the pendulum has again swung the other way, and recent research on ethnic differences in disease susceptibility and the molecular basis of host resistance suggests that there is a role for genetics in infectious diseases after all (Skamene, 1994).
While genetics are likely to contribute least to injuries among causes of mortality and morbidity, genetically determined enzyme differences affecting alcohol metabolism between Native Americans and other populations have been recognized (Reed, 1985), although the evidence is not consistent. It is also important to note that even if metabolic differences do exist, they are not sufficient to explain the high risk of alcohol abuse and its health effects in terms of accidents and violence among Native Americans populations.
An important factor among the determinants of health is individual health risk behaviors, which have increasingly become the focus of health promotion. Such behaviors as smoking, diet and nutrition, alcohol and drug use, safety knowledge and practices, sexual behavior, and physical activity are implicated in diverse health problems. For Native Americans, national data on health determinants are far more limited than data on health outcomes such as mortality. Surveys such as the Survey of American Indians and Alaska Natives provide useful data on smoking habits;
obesity; and the use of preventive health services, such as screening for hypertension and for cervical and breast cancer (Lefkowitz and Underwood, 1991). Such data are not encouraging: Native Americans smoke more, are more overweight, and use preventive services less often.
Another source of national survey data on health determinants is the Behavioral Risk Factor Surveillance System, a telephone survey conducted since 1984 by the Centers for Disease Control in collaboration with state health departments. Data have been reported on 1,055 Native Americans between 1985 and 1988, covering such areas as seatbelt nonuse, drinking, drinking and driving, high blood pressure, sedentary life-style, cigarette smoking, use of smokeless tobacco, and obesity. In general, the sex-specific prevalences for Native Americans compared with whites do not differ by more than 4 percent, except for current smoking (substantially higher among Native Americans in all regions except the Southwest, where it is lower), and obesity (substantially higher among Native American women). Interestingly, regional differences among Native Americans are similar in magnitude to the regional differences among whites (Sugarman et al., 1992). A recent update on the prevalence of smoking showed that 33 percent of Native American men and 27 percent of women are smokers (Centers for Disease Control and Prevention, 1992). Regionally based data on cardiovascular risk factors, including serum lipids, hypertension, obesity, physical activity, and smoking, can be found in a recent review (Ellis and Campos-Outcalt, 1994).
Broader socioeconomic and environmental factors, such as income, education, housing, and employment, affect health through a variety of pathways. Thus overcrowding and inadequate sanitation promote the acquisition and transmission of respiratory, intestinal, and skin infections; low education and low income affect food choices and nutritional status and contribute to the development of chronic diseases; and unemployment engenders family breakdown and increases the likelihood of violence and injuries. According to the 1990 census, Native Americans nationally continue to be at a disadvantage in terms of a variety of indicators, as summarized in Table 3-3.
It should be emphasized that Native American health must be examined and understood in its historical and political context, beyond the mere cataloging of isolated, individual determinants and outcomes. The evolution of health and disease among Native Americans has been termed an "unnatural history" (Campbell, 1989), and resolution of the major health problems of Native Americans requires redressing the underlying social, cultural, and political causes of those problems.
TABLE 3-3 Selected Socioeconomic Indicators from the 1990 Census: Native Americans and Total U.S. Population
|
Indicator |
Native Americans |
U.S. Population |
|
% families maintained by female householder without husband |
27 |
17 |
|
% adults 25 years + with high school graduation |
66 |
75 |
|
% adults 16 years+ in the labor force |
62 |
65 |
|
% employed persons 16 years + in managerial and professional occupations |
18 |
26 |
|
Median family income |
$21,750 |
$35,225 |
|
% individuals below poverty level |
3 |
13 |
|
SOURCE: Bureau of the Census, 1993. |
||
Conclusions
The health of Native Americans is undergoing both quantitative and qualitative changes. While the absolute burden of mortality and morbidity has decreased substantially in the decades since World War II, the relative contributions of various diseases and health conditions have also changed. Whether one calls this an "epidemiologic transition" in the sense intended by the theory's original proponents—as well as the associated issues of what stage of the transition currently characterizes Native Americans and whether they should constitute a model distinct from that which characterizes developing countries—is not as important as the utility of the theory in advancing our ability to monitor and predict trends. Clearly, planning for future health interventions must be based on how the current burden of illness will evolve (Rhoades et al., 1987). On a theoretical level, the data are insufficient, particularly at a national level, to characterize more clearly "health" beyond mortality. Among Native Americans, one must also proceed beyond the descriptive to the analytic to help understand and explain why the Native American pattern of health has changed and is continuing to do so. This will be a challenge to demographers and epidemiologists interested in Native Americans.
References
Broudy, D.W., and P.A. May 1983 Demographic and epidemiologic transition among the Navajo Indians. Social Biology 30:1-16.
Bureau of the Census 1993 We the First Americans. Washington, DC: Racial Statistics Branch, Population Division.
Campbell, G.R. 1989 The changing dimension of Native American health: A critical understanding of contemporary Native American health issues. American Indian Culture and Research Journal 13(3 & 4):1-20.
Centers for Disease Control and Prevention 1992 Cigarette smoking among American Indians, Alaska Natives—Behavioral Risk Factor Surveillance System, 1987-1991. Journal of the American Medical Association 268:3052, 3055.
1993 Classification of American Indian race on birth and infant death certificates—California and Montana. Morbidity and Mortality Weekly Reports 42:220-223.
Ellis, J.L., and D. Campos-Outcalt 1994 Cardiovascular disease risk factors in Native Americans: A literature review. American Journal of Preventive Medicine 10:295-307.
Frost, F., and K.K. Shy 1980 Racial differences between linked birth and infant death records in Washington State. American Journal of Public Health 70:974-976.
Frost, F., V. Taylor, and E. Fries 1992 Racial misclassification of Native Americans in a Surveillance, Epidemiology and End Results registry. Journal of the National Cancer Institute 84:957-962.
Frost, F., K. Tollestrup, A. Ross, E. Sabotta, and E. Kimball 1994 Correctness of racial coding of American Indians and Alaska Natives on the Washington State death certificate. American Journal of Preventive Medicine 10:290-294.
Gohdes, D. 1995 Diabetes in North American Indians and Alaska Natives. Pp. 683-701 in Diabetes in America, 2nd ed. National Diabetes Data Group. NIH Pub. No. 95-1468. Bethesda, MD: National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases.
Gillum, R.F. 1995 The epidemiology of stroke in Native Americans. Stroke 26:514-521.
Gribble, J.N., and S. Preston, eds. 1993 The Epidemiological Transition: Policy and Planning Implications for Developing Countries. Committee on Population, National Research Council. Washington, DC: National Academy Press.
Hahn, R.A., J. Mulinare, and S.M. Teutsch 1992 Inconsistencies in coding of race and ethnicity between birth and death in U.S. infants: A new look at infant mortality, 1983-1985. Journal of the American Medical Association 267:259-263.
Indian Health Service 1979 Illness Among Indians and Alaska Natives, 1970 to 1978. Rockville, MD.
1990a Trends in Indian Health 1990. Rockville, MD.
1990b Regional Differences in Indian Health 1990. Rockville, MD.
1994a Trends in Indian Health 1994. Rockville, MD.
1994b Regional Differences in Indian Health 1994. Rockville, MD.
Israel, R.A., H.M. Rosenberg, and L.R. Curtin 1986 Analytical potential for multiple cause-of-death data. American Journal of Epidemiology 124:161-179.
Jamison, D.T., W.H. Mosley, A.R. Measham, and J.L. Bobadilla, eds. 1993 Disease Control Priorities in Developing Countries. New York: Oxford University Press.
Johnson, A., and A. Taylor 1991 Prevalence of Chronic Diseases: A Summary of Data from the Survey of American Indians and Alaska Natives. Pub. No. 91-0031. Rockville, MD: Agency for Health Care Policy and Research.
Kirchner, T., J. Nelson, and H. Burdo 1985 The autopsy as a measure of accuracy of the death certificate. New England Journal of Medicine 313:1263-1269.
Klain, M., J.L. Coulehan, V.C. Arena, and R. Janett 1988 More frequent diagnosis of acute myocardial infarction among Navajo Indians. American Journal of Public Health 78:1351-1352.
Knowler, W.C., D.J. Pettit, M.F. Saad, and P.H. Bennett 1990 Diabetes mellitus in the Pima Indians: Incidence, risk factors and pathogenesis. Diabetes Metabolism Reviews 6:1-27.
Kunitz, S.J. 1983 Disease Change and the Role of Medicine: The Navajo Experience . Berkeley, CA: University of California Press.
Kushigemachi, M., L.J. Schneiderman, and E. Barrett-Connor 1984 Racial differences in susceptibility to tuberculosis: Risks of disease after infection. Journal of Chronic Diseases 37: 853-62.
Lanier, A.P., L.R. Bulkow, and B. Ireland 1989 Cancer in Alaska Indians, Eskimos and Aleuts, 1969-83: Implications for etiology and control. Public Health Reports 104:658-664.
Lefkowitz, D., and C. Underwood 1991 Personal Health Practices: Findings from the Survey of American Indians and Alaska Natives. Pub. No. 91-0034. Rockville, MD: Agency for Health Care Policy and Research.
Lieb, L.E., G.A. Conway, M. Hedderman, J. Yao, and P.R. Kerndt 1992 Racial misclassification of American Indians with AIDS in Los Angeles County. Journal of AIDS 5:1137-1141.
Mackenbach, J.P. 1994 The epidemiologic transition theory [editorial]. Journal of Epidemiology and Community Health 48:329-331.
Mahoney, M.C., and A.M. Michalek 1991 A meta-analysis of cancer incidence in United States and Canadian Native population. International Journal of Epidemiology 20:323-327.
Neel, J.V. 1982 The thrifty gene revisited. Pp. 283-293 in J. Kobberling and R. Tattersall, eds., The Genetics of Diabetes Mellitus. New York: Academic Press.
Newman, J.M., A.A. Marfin, P.W. Eggers, and S.D. Helgerson 1990 End stage renal disease among Native Americans, 1983-86. American Journal of Public Health 80:318-319.
Nutting, P.A., W.L. Freeman, D.R. Risser, S.D. Helgerson, R. Paisano, J. Hisnanick, S.K. Beaver, I. Peters, J.P. Carney, and M.A. Speers 1993 Cancer incidence among American Indians and Alaska Natives, 1980 through 1987. American Journal of Public Health 83:1589-1598.
Olshansky, S.J., and A.B. Ault 1986 The fourth stage of the epidemiologic transition: The age of delayed degenerative diseases. Milbank Quarterly 64:355-391.
Omran, A.R. 1971 The epidemiological transition: A theory of the epidemiology of population change. Milbank Memorial Fund Quarterly 49:509-538.
1977 A century of epidemiologic transition in the United States. Preventive Medicine 6:30-51.
1983 The epidemiologic transition theory: A preliminary update. Journal of Tropical Pediatrics 29:305-316.
Phillips, D.R. 1994 Does epidemiological transition have utility for health planners? [editorial]. Social Science and Medicine 38:vii-x.
Reed, T.E. 1985 Ethnic differences in alcohol use, abuse and sensitivity: A review with genetic interpretation. Social Biology 32:195-209.
Rhoades, E.R., J. Hammond, T.K. Welty, A.O. Handler, and R.W. Amler 1987 The Indian burden of illness and future health interventions. Public Health Reports 102:361-8.
Ritenbaugh, C., and C. Goodby 1989 Beyond the Thrifty Gene: Metabolic implications of prehistoric migration into the New World. Medical Anthropology 11: 227-36.
Skamene, E. 1994 The Bcg gene story. Immunobiology 191: 451-60.
Sorlie, P.D., E. Rogot, and N.J. Johnson 1992 Validity of demographic characteristics on the death certificate. Epidemiology 3:181-184.
Sugarman, J.R., C.W. Warren, L. Oge, and S.D. Helgerson 1992 Using the Behavioral Risk Factor Surveillance System to monitor Year 2000 Objectives among American Indians. Public Health Reports 107:449-456.
Sugarman, J.R., and L. Lawson 1993 The effect of racial misclassification on estimates of end-stage renal disease among American Indians and Alaska Natives in the Pacific Northwest, 1988 through 1990. American Journal of Kidney Diseases 21:383-386.
Sugarman, J.R., R. Soderberg, J.E. Gordon, and F.P. Rivara 1993 Racial misclassification of American Indians: Its effect on injury rates in Oregon, 1989 through 1990. American Journal of Public Health 83:681-684.
Szathmary, E.J.E. 1990 Diabetes in Amerindian populations: The Dogrib studies. Pp. 75-103 in A. Swedlund and G. Armelagos, eds., Health and Disease of Populations in Transition. New York: Bergin and Garvey.
Trowell, H.C., and D.P. Burkitt, eds. 1981 Western Diseases: Their Emergence and Prevention. Cambridge, MA: Harvard University Press.
Valway, S., W. Freeman, S. Kaufman, T. Welty, S. Helgerson, and D. Ghodes 1993 Prevalence of diagnosed diabetes among American Indians and Alaska Natives, 1987. Diabetes Care 16 (Suppl 1):271-276.
Waller, A.E., S.P. Bakes, and A. Szocka 1989 Childhood injury deaths: national analysis and geographic variations. American Journal of Public Health 79:310-315.
Weiss, K.M., R.E. Ferrell, and C.L. Hanis 1984 A New World Syndrome of metabolic diseases with a genetic and evolutionary basis. Yearbook of Physical Anthropology 27:153-178.
Welty, T.K., and J.L. Coulehan 1993 Cardiovascular disease among American Indians and Alaska Natives. Diabetes Care 16 (Suppl 1):277-83.
West, K.M. 1974 Diabetes in American Indians and other native populations of the New World. Diabetes 23:841-855.
Young, T.K. 1988 Health Care and Cultural Change: The Indian Experience in the Central Subarctic. Toronto: University of Toronto Press.
1994 The Health of Native Americans: Toward a Biocultural Epidemiology . New York: Oxford University Press.
Young, T.K., C.D. Schraer, E.V. Shubnikoff, E.J. Szathmary, and Y.P. Nikitin 1992 Prevalence of diagnosed diabetes in circumpolar indigenous populations. International Journal of Epidemiology 21:730-736.
| This page in the original is blank. |
























