1
Introduction
Although improvement in workplace safety was recently hailed as one of the 20th century’s outstanding achievements in public health (Centers for Disease Control and Prevention, 1999) (Figure 1-1), it is nevertheless true that even in the waning years of the century, 20 American workers died each day as a result of occupational injuries, for a total of 6,000 deaths per year. More than 16,000 suffer nonfatal injuries on the job every day, for a total of 6 million injuries per year (Bureau of Labor Statistics, 1998a). The incidence of occupational illness is more difficult to estimate, but a recent thorough and methodologically sound attempt placed the number of new cases in 1992 at 860,000 and the number of deaths from occupational disease that year alone at 60,000 (Leigh et al., 1997). The best current estimate of the costs of these job-related injuries ($145 billion) and illnesses ($26 billion) is much higher than those for AIDS and Alzheimer’s disease and are on par with the costs of cancer or of all circulatory diseases (Leigh et al., 1997).
The U.S. Congress passed the Occupational Safety and Health Act of 1970 (OSHAct) to assure “every working man and woman in the United States safe and healthful working conditions.” This mandate gave rise to the Occupational Safety and Health Administration (OSHA) and also established the National Institute for Occupational Safety and Health (NIOSH). Over the last 30 years NIOSH has implemented a training program to address a provision of the OSHAct that mandates an “adequate supply of qualified professionals to carry out the purposes of the Act.” NIOSH extramural funds support a $10 to $15 million training program
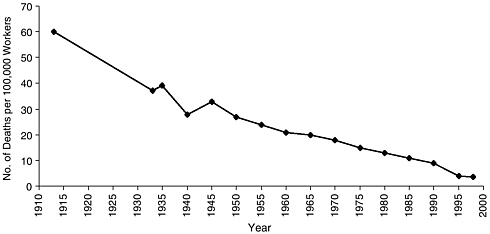
FIGURE 1-1 Deaths per 100,000 workers due to injury, 1913 to 1998. (Data for death rates from injury for the years between 1913 and 1933 were not available. Because of adoption of the Census of Fatal Occupational Injuries to include deaths of any worker regardless of age (previous years surveyed only persons over the age of 16 who were gainfully employed), numbers of deaths and death rates from 1992 to the present are not comparable to those for earlier years). SOURCES: Corn (1992), National Safety Council (1999).
(approximately 9 percent of the institute’s occupational safety and health [OSH] budget) that comprises a network of 15 regional Education and Research Centers (ERCs) located at leading universities in 14 states and approximately 40 individual training project grants in 25 states and Puerto Rico. Every year, approximately 500 students graduate from NIOSH-supported programs with backgrounds in occupational medicine, occupational health nursing, industrial hygiene, and safety. Many current leaders and OSH advocates have received training from NIOSH-funded programs. According to a 1996 report by the inspector general of the U.S. Department of Health and Human Services (Office of Inspector General, 1996), about 90 percent of ERC graduates pursue careers in OSH in private industry, labor, government agencies, medicine, and academia.
The work environment has changed since the OSHAct was passed more than 30 years ago. Work injuries and illnesses that were unrecognized at that time now contribute greatly to the present OSH burden. New information about ergonomics and the association between work organization and job stress mean that there is a newly recognized need for personnel qualified in carrying out interventions that will prevent adverse health outcomes related to these factors. Worker demographics are changing, with more women, minorities, and people with disabilities being in the workforce. Older workers (those over 50 years of age) and
younger workers (those under 18 years of age) also play important roles in the workforce. Individuals in these populations have risk factors that may need to be addressed differently from those risk factors among individuals in the general population. For example, are older workers more adversely affected by shiftwork? The U.S. workplace itself has also evolved as the U.S. economy has moved rapidly from a manufacturing-based to a service-based economy and is now developing into one centered on information and information technology. In addition, there have been profound changes in the way in which work is organized. Distributed work arrangements, flexible matrix- and team-based organizational structures, and nonstandard work arrangements have become commonplace, challenging the competencies of current occupational safety and health professionals.
In terms of delivery of OSH services, industry-supplied OSH resources may no longer play as large a role as they once did. As companies downsize, OSH staff may be outsourced or eliminated altogether. The OSH role may be assumed by other staff who do not have training in OSH or by a person with training in a combination of disciplines. Other important changes are occurring in health care delivery generally, with an increased emphasis on managed care and other means of reducing costs. The evolving role of the occupational physician has not been explored in this new delivery system, nor have the roles of primary care physicians, nurse practitioners, or other health professionals who may be treating workers.
From a regulatory standpoint, OSHA has added standards over the years that require “qualified,” “designated,” or “competent” persons to ensure enforcement at the work site, but there has been no agreement on the training that will enable personnel to meet these designations. OSHA also mandates training of workers in more than 100 standards but does not speak to the quantity, quality, or efficacy of that training. Few if any standards call for training of employers or managers responsible for workplace safety and health.
Because of these workforce, workplace, and OSH care changes, NIOSH’s traditional focus on training of industrial hygienists, occupational physicians, occupational nurses, and safety professionals may no longer be sufficient. Evolving demands on the OSH professional in meeting the challenges of the new workplace may call for a much broader perspective than that taken in the past, including an expanded emphasis on such fields as epidemiology, ergonomics, health communication, the behavioral sciences, health care cost control, and management.
There is thus an urgent need to examine the numerous factors changing the modern workplace, derive the implications of these trends for OSH, and make corresponding changes in the education and training of
OSH professionals, management and union officials, and the workers themselves. Moreover, national guidelines are required to inform universities, industries, and other public health agencies of the personnel requirements needed to ensure worker safety and health. Accordingly, NIOSH, with support from OSHA, the National Institute of Environmental Health Science (NIEHS), and the U.S. Department of Veterans Affairs, approached the Institute of Medicine (IOM) for a needs assessment that would characterize the current U.S. workforce and work environment and forecast the demand, need, and supply of qualified OSH professionals.* The goal of the assessment would be to identify gaps in occupational safety and health training programs in the United States that can be filled by either public or private programs and identify the critical curricula and skills needed to meet these evolving OSH concerns.
CHARGE TO THE COMMITTEE
The charge to the committee from the sponsors was fourfold, calling for analyses of both the adequacy of the current OSH workforce and training and adjustments that might be required in the future because of changes in the workforce, the workplace, the organization of work, and health care delivery.
-
Assess the demand and need for OSH professionals as well as the adequacy of the OSH professional supply by sampling members of the OSH community (industry, small business, labor, academia, professional organizations, health providers, contract services, and governmental agencies). This assessment would determine the number and type of personnel currently employed; their professional duties, skills, abilities, and knowledge; and shortfalls in these categories.
-
Analyze changes in the workforce and work environment that are affecting the roles of OSH professionals now, and how they are likely to affect these roles over the next decade.
-
Identify gaps in current OSH education and training. For example, determine whether training programs provide an appropriate number of personnel and a matrix of knowledge, skills, and abilities at appropriate levels. Determine which disciplines and skills will be most effective in addressing OSH needs over the next decade.
-
Identify the critical curricula and skills needed to meet these evolving OSH concerns.
LEGISLATIVE AND REGULATORY BACKGROUND
Laws and regulations have played a major role in the great improvement in worker health and safety alluded to in the opening lines of this report. Appendix C provides the names and dates of some of the most significant events in the history of OSH. The process has been a cumulative one, however, so this section will summarize the major provisions of the most recent and far-reaching of these laws, the OSHAct of 1970 (the Mine Occupational Safety and Health Act, as amended in 1977, is very similar but is limited to a single industry) and the common features of state workers’ compensation (WC) laws. Workers, employers, and occupational safety and health professionals are affected by many more industry-specific laws and regulations, but these two affect all of these individuals and are thus the starting place for OSH education and training.
The Occupational Safety and Health Act of 1970
The OSHAct was a far-reaching piece of legislation that went far beyond spawning the NIOSH training programs mentioned above. It authorizes the Secretary of Labor to set mandatory OSH standards for businesses, conduct inspections to see that they are being observed, and apply sanctions for violations of the standards. Coverage extends to all businesses except the self-employed, farms that employ only members of the immediate family, and a few specific industries such as mining, nuclear power, and civil aviation that are regulated by other federal agencies. It does not cover over 8 million employees of federal, state, and local governments, including public schools, public healthcare facilities, and correctional institutions. Federal agencies, although not generally subject to inspection by OSHA, are required to comply with standards consistent with those issued to the private sector, and they must self-inspect annually. Like private-sector employers, they must also record and analyze injury and illness data and provide training to protect employees from on-the-job hazards. OSHA is the federal agency responsible for promulgating and enforcing the standards that employers must meet, but the OSHAct does allow states to assume that role within their own borders, and 25 states have done so to date. States seeking authority to establish their own OSH programs must submit a detailed plan to OSHA for approval, which depends upon convincing OSHA that the state program will be at least as effective as the federal program (states must add or modify their standards whenever OSHA adds or modifies the federal standards). Once approved, OSHA funds up to 50 percent of the state program. Further use of the term “OSHA” in this chapter should be taken to mean OSHA or OSHA-approved state programs.
Although the process of issuing a new standard is long and cumbersome, to ensure that all interested parties can be heard, there are hundreds of standards covering a wide range of hazardous materials, equipment, procedures, and working conditions. These standards require employers to protect employees in a variety of ways: from design and maintenance of the workplace and equipment to training of the worker to perform his or her job safely. General Industry Standards apply to materials and conditions common to many industries (for example, toxic chemicals, fire protection, electrical safety, material handling, and general environmental controls). Other standards may be highly specific applications to limited aspects of particular industries (scaffolding, fall protection, or surface transportation of explosives or bloodborne pathogens, for example).
OSHA is authorized to enter and inspect workplaces to enforce these standards. Such inspections cover both record-keeping (employers are required to keep standardized records of injuries and illnesses, and many standards require documentation of exposure assessments, medical surveillance, training, and other activities relevant to OSH) and firsthand examination of the work site, including consultation with employees.
OSHA and its 25 state partners have had some undeniable successes. Since 1970, the overall workplace injury death rate has been cut in half. OSHA’s cotton dust standard virtually eliminated brown lung disease in the textile industry; and OSHA’s lead standard reduced lead poisoning in battery plant and smelter workers by two-thirds. OSHA inspections may be an important part of that success: according to a recent study, in the 3 years following an OSHA inspection that results in penalties, injuries and illnesses drop on average by an average of 22 percent. Overall injury and illness rates have declined in the industries where OSHA has concentrated its attention yet have remained unchanged or have actually increased in the industries where OSHA has had less of a presence. The last of those observations assumes real importance when one notes that OSHA resources allow inspection of less than 2 percent of U.S. workplaces every year. The Mine Safety and Health Administration, in contrast, inspects each U.S. mine at least four times yearly (Institute of Medicine, 1998).
The OSHAct went beyond regulation and enforcement by also charging the Secretary of Labor with establishing and supervising education and training programs for employers and employees. These programs covered recognition and prevention of unsafe or unhealthful working conditions. In addition, the Secretary of Health, Education, and Welfare (now the Secretary of Health and Human Services) was charged with conducting “educational programs to provide an adequate supply of qualified personnel to carry out the purposes of this [OSH] Act” and “informational programs on the importance and proper use of safety and
health equipment.” OSHA has assumed the lead in OSH training of workers and managers, and NIOSH has focused on degree programs and continuing education in occupational medicine, occupational health nursing, industrial hygiene, and occupational safety. Although its effectiveness has been questioned (for example, Hale [1984] and Tan et al. [1991]), health and safety training of workers has generally been acknowledged to be an important component in prevention of work-related injuries and illnesses (Office of Technology Assessment, 1985: Keyserling, 1995; Cohen and Colligan, 1998). Both agencies’ programs are described in more detail in Chapter 7.
Workers’ Compensation
Workers’ Compensation (WC) is no-fault insurance for occupational injuries and illnesses. Beginning in the first decade of the 20th century, each of the 50 states and the District of Columbia have passed “workers’ comp” laws that vary widely in coverage and benefits but that, in general, provide employers immunity from lawsuits in exchange for payments to the affected worker or dependent survivor. Immunity can be waived in cases in which the employer is not in compliance with relevant OSHA standards (in practice, it usually takes gross negligence or criminal activity on the part of the employer), so the laws serve as an incentive for employers to comply with OSHA standards. In addition, since premiums are determined in part by the numbers and sizes of claims, employers should have a financial interest in safe working conditions.
Claims arising from work-related injuries often stem from obvious one-time events where neither the existence of the injury nor the fact that it is work-related is in doubt (a whaler gets his foot tangled in a harpoon line, is dragged into the water and drowns). In other cases, one or both of these criteria (an injury has occurred, and it occurred as a result of employment) are difficult to establish. For example, low back pain is a very common complaint that often cannot be substantiated with objective medical evidence, and injuries like carpal tunnel syndrome are characterized by a gradual onset that may leave room for doubt about whether a specific case is truly occupational in nature. Occupational illnesses can be even more difficult to assess, and only a fraction of cases of work-related disease are thought to be covered by workers’ compensation. Occupational diseases are seldom the result of a single identifiable incident, and many, like cancer, may be diagnosed only many years after exposure to the causative agent. A solution adopted in many states was to establish a list or schedule of recognized occupational diseases associated with certain trades, materials, or processes. This has generally been abandoned as
too limiting, and replaced by a case-specific judgment on whether the illness arose out of the activities of work.
The benefits paid include compensation not only for the explicit costs of medical treatment, including rehabilitation if necessary, but also for the loss of income incurred, which on average is about 50 to 60 percent of the total benefit. Funeral and burial costs are covered in fatal cases, and there is generally some schedule of payment for permanent disabilities independent of any attendant loss of income. The National Academy of Social Insurance (Mont et al., 1999) estimates that approximately $40 billion in benefits was paid out annually in 1993 through 1996, the last year for which they have data, although other estimates are as much as $70 billion to $100 billion (Leone and O’Hara, 1998). A number of studies suggest that WC is underutilized, however, with as much as 30 to 60 percent of work-related fatalities not found in WC records (Cone et al., 1991; Stout and Bell, 1991; Leigh et al., 1997). Parker et al. (1994) found that 67 percent of eligible injuries were not reported to the WC system. Reasons proposed for this underutilization include workers’ ignorance of their rights, workers’ desire to be “team players,” and fear of retaliation from the employer, who has a financial stake in minimizing claims.
The Americans with Disabilities Act
The Americans with Disabilities Act (ADA) was signed into law on July 26, 1990, with the intent of protecting from discrimination the millions of disabled Americans in the workforce or those who are seeking to enter the workforce. A disabled person is defined as an individual who has a physical or mental impairment that substantially limits one or more of his or her major life activities, has a record of such an impairment, or is regarded as having such an impairment. ADA consists of five different titles, the most important being Title I, which prohibits employing entities from discriminating against a qualified, disabled individual in any aspect of employment. Titles II, III, and V of ADA address the need for construction to allow disabled individuals access to public areas and services, as well as to private businesses and recreational establishments (Rogers, 1994). Title IV mandates that various forms of telecommunications services be offered to those individuals with hearing impairments. The U.S. Department of Justice (DOJ) has been given the authority to issue regulations and to offer expertise, technical assistance, and enforcement for Titles II and III of ADA. DOJ is also responsible for calibrating state and municipal codes for building construction and building alterations so that they adhere to ADA standards (U.S. Department of Justice, 1999).
As a result of the new responsibilities associated with adherence to ADA, OSH personnel have assumed a greater presence and new roles in
the workplace (Rogers, 1994). For example, OSH personnel are increasingly important to the recruitment process. To avoid inadvertent discrimination against prospective employees, employing entities must provide accurate job descriptions, which should include input from OSH personnel. Furthermore, when employing entities assess candidates for a new position, the assessment of the position by an OSH expert may be one of the factors that determines the prospective employee’s fitness to complete essential job functions. In assessing a job, OSH personnel consider the general work environment, tools associated with the position, stressors, and other elements that affect essential job functions.
Other roles that OSH personnel play as a result of ADA lie in the areas of reasonable accommodation and WC. Reasonable accommodation provides those disabled persons who are qualified for a particular position with the means to overcome workplace barriers, be they physical, communicative, scheduling, or simple prejudice. Occupational safety personnel and ergonomists, by providing suggestions for reasonable accommodations, become important figures in helping disabled individuals and the employing organizations in overcoming physical barriers. In regard to financial compensation, medical examinations by occupational medicine physicians and occupational health nurses aid in determining not only whether the cause of an injury was work related but also whether an employee has been temporarily or permanently disabled and when and in what capacity he or she is fit to return to work. As a result of ADA, OSH personnel have increased their presence in the workplace, particularly in the areas of recruitment, reasonable accommodation, and financial compensation.
PREVIOUS STUDIES OF THE OSH WORKFORCE
Several previous studies have attempted to estimate the size and nature of the OSH workforce or some part thereof and of its adequacy for the task of minimizing occupational injuries and illnesses. The largest and oldest of these is a nationwide survey of more than 3,000 nonagricultural organizations and firms and all 112 known educational institutions that provide a degree or certificate in an OSH-related field (National Institute for Occupational Safety and Health, 1978). A smaller survey study commissioned by NIOSH in 1985 (Cox and Johnston, 1985) solicited descriptive information and summary data on graduates from all identifiable OSH academic programs at U.S. colleges and universities. Additional components of the Cox and Johnston (1985) study were telephone interviews with 40 employers of OSH professionals and questionnaire data from 500 recent OSH graduates. In 1987, IOM convened a committee that identified a number of barriers that prevent primary care physicians from
adequately diagnosing and treating occupationally and environmentally related diseases and published the committee’s report the following year (Institute of Medicine, 1988). Follow-up reports by Castorina and Rosenstock (1990) and IOM (1991) identified a shortage of occupational and environmental physicians and offered specific measures to remedy the shortfall.
The 1978 Nationwide Survey of the OSH Workforce
The relevant universe of workplaces for the 1978 survey study’s estimates of the 1977 OSH workforce included all firms that employ 100 or more individuals in mining, construction, manufacturing and transportation, communication and utilities and all firms that employ 500 or more individuals in the trade and service industries and in non-OSH related state and local government agencies. Survey instruments collected data on each firm and its OSH operations, on each of the firm’s OSH-related positions, and on the background and activities of each of the firm’s identified OSH personnel. A total of 3,300 firms responded representing a return rate of approximately 50 percent.
On the basis of the data from the survey, the study’s authors estimated that approximately 85,000 employees spent at least 50 percent of their time in OSH-related activities. However, only about two-thirds of their positions were full-time. Manufacturing employed the greatest number of OSH employees, accounting for 44 percent of the total number of OSH employees, followed by trades, services, non-OSH related government organizations, and loss-prevention insurance carriers. Almost half of the OSH workforce (44 percent) was employed in a safety-related position (injury prevention). Nurses comprised an additional 11 percent, physicians comprised 1 percent, industrial hygienists and fire protection experts each comprised 6 percent, and radiation safety specialists comprised 2 percent of the identified OSH workforce. Twenty-four percent of the OSH workforce fell in the “general” category because although they spent 50 percent of their time on OSH-related activities, their work was spread over two or more basic areas. Overall, about 58 percent of OSH employees’ time was spent on the prevention and treatment of injuries. Twenty-two percent of their time was spent on the prevention and treatment of illnesses, and about 20 percent of their time was spent on fire prevention. The OSH employees themselves reported a mean age of 42, an average of about 7 years of tenure in their current job, and just short of 15 years of formal education (i.e., less than a baccalaureate degree). Employers, asked about their expectations for new hires, anticipate only 4 years experience on average and were looking for bachelor’s degrees for only one-third of
their new hires and graduate degrees for only 3 percent of their new hires (1 percent would presumably be physicians).
The study’s second major product was a set of predictions about demand for OSH employees in 1980, 1985, and 1990. These were produced by a model based on industry employment projections by the Bureau of Labor Statistics. One of the two published predictions assumed that the distribution and concentration of OSH employees would remain unchanged (status quo model), so the number of OSH employees would grow at the same rate as the rate of growth of the industries that employed them in 1977. A second prediction assumed that government regulations would lead to an increased concentration of OSH employees and used a panel of technical advisers to make estimates about the industries and specialties most likely to be affected (accelerated model). The two forecasts for the 1990 OSH workforce were for 104,000 in the status quo model and 110,000 in the accelerated model. This translates to a demand for roughly 3,000 new hires annually in the late 1980s.
The final segment of the report looked at the expected supply of OSH personnel from four sources: educational institutions, insurance carriers, government, and industry. A total of 956 OSH related degrees (including 208 2-year associate degrees) were awarded by the 88 institutions responding to the NIOSH request for data. This number was up sharply from the 1970 total of 144, and the responding schools anticipated a continuing increase to a level of 2,200 by 1990. Inquiries to loss prevention insurance carriers indicated that 50 percent of all new hires were trained internally—300 to 500 per year. The only federal government source included was the National Mine Health and Safety Academy, which in 1978 graduated 200 to 250 individuals annually (the OSHA Training Institute and other federal training programs were considered primarily continuing education and not primary sources of supply). It proved impossible for the report’s authors to estimate the extent of formal and informal training being carried out by private firms, but they speculated that reliance on in-house training had diminished steadily since the passage of the OSHAct of 1970 and would continue to do so. Their total projected annual supplies for 1977 and 1990 were 1,426 and 2,504, respectively. The report concluded that demand equaled supply for industrial hygienists but that demand exceeded supply for safety personnel, occupational health nurses, occupational health physicians, and OSH generalists.
The 1985 Cox and Johnston Report on the Impact of OSH Training and Education Programs
NIOSH commissioned a study on the impact of OSH training and education programs (Cox and Johnston, 1985) to evaluate the effective-
ness of the training programs that it had instituted to alleviate perceived shortages in trained OSH personnel. It sought to determine the nature and number of academic programs in OSH, estimate the current and projected numbers of graduates from those programs, and obtain feedback from both recent graduates and a small sample of employers about the value of the academic preparation.
The study identified 241 academic programs in OSH, at 136 U.S. institutions. NIOSH-supported ERCs accounted for 83 of the 241 programs, and another 34 programs received non-ERC-related support from NIOSH. Programs that combined industrial hygiene and safety were most common (n = 75), followed by industrial hygiene programs (n = 73) and safety programs (n = 62), occupational medicine programs (n = 16) and occupational health nursing programs (n = 15). Thirty-five programs offered associate degrees or certificates (20 in industrial hygiene and safety and 12 in safety); 71 programs offered baccalaureate degrees; 87 offered master’s degrees (35 in industrial hygiene, 19 in safety, 20 in industrial hygiene and safety, and 13 in occupational health nursing). Doctoral degrees were offered by 33 programs (18 in industrial hygiene), and the 15 occupational medicine programs were post doctoral.
In 1979-1980 and again in 1981-1982, these programs produced about 1,600 graduates, with about 950 at the associate or baccalaureate level. Almost half of the graduate-level degrees were granted by institutions associated with ERCs. A sample of 500 ERC graduates reported ease in gaining suitable employment, a high level of job satisfaction, and a reasonable match between academic preparation and job requirements. Employers (n = 40) reported some shortage of occupational health nurses and occupational medicine graduates, a reasonable balance of supply and demand for industrial hygienists, and a possible surplus of occupational safety graduates.
The 1988 IOM Report on the Role of the Primary Care Physician in Occupational and Environmental Medicine
Growing recognition of adverse health effects associated with exposure to toxic substances at home, at work, and in the general community, and the limited capacity of most physicians to deal with those effects, led IOM to form a committee to seek ways to foster more active and effective participation of primary care physicians in preventing and treating occupationally and environmentally related health problems. The committee recommended improved information sources, preferably a single access point for pertinent clinical information, improved availability of clinical consultation, primarily through increased numbers of trained specialists, and changes in the reimbursement system both to increase the adequacy
and speed of payment for treatment and also to reward prevention efforts (Institute of Medicine, 1988). IOM further recommended that the field of occupational and environmental medicine (OEM) be better represented on medical school faculties and in medical school curricula, that residency programs for internal medicine and family practice devote more time to experience in OEM, and that these areas receive greater representation in the examinations of the various state and local boards for certification and licensing.
The 1991 IOM Report Addressing the Physician Shortage in Occupational and Environmental Medicine
A second IOM committee commissioned a quantitative estimate of the need for and supply of physicians with clinical training in OEM, reiterated the recommendations of the 1988 study, and elaborated on the methods by which those recommendations might be implemented. The needs estimate is fully described in a paper by Castorina and Rosenstock (1990). In that critical review of previously published estimates of the need for and supply of physicians with clinical training in OEM, the authors call for 1 to 3 OEM specialists at each of the 127 U.S. medical schools, 1 to 1.5 community-based OEM specialists per 100,000 population, and 1 to 3 board-certified OEM physicians in each of 57 state and 505 local public health agencies. They also assert that approximately 1 percent of primary care physicians should have special competence in OEM. Their resulting estimate of a need for 3,100 to 4,700 board-certified OEM specialists and 1,500–2,000 primary care physicians with special competence in OEM is far higher than their estimate of the supply (1,200 to 1,500).
Central to that IOM committee’s suggestions for addressing this shortage was the vision of three levels of specialization. OEM specialists, who would be board certified in occupational medicine, would be employed as full-time university faculty, in a public health agency, in industry, or as a consultant to any of those institutions. OEM clinicians, who would be board certified in internal medicine or family practice but with a Certificate of Added Qualifications in OEM, would work primarily in community hospitals and clinics as clinical faculty and in industry. Primary care physicians, who would be board certified in internal medicine or family practice but who would have additional awareness of OEM issues via implementation of the initiatives outlined in the 1988 IOM report, would continue to be the first contact with the medical system for most patients.
Not only did the committee offer the suggestion of a Certificate of Added Qualifications to create OEM Clinicians but it also proposed an alternative, streamlined approach to certification of full-fledged OEM specialists that would shorten training by a year.
METHODS OF THE PRESENT IOM STUDY
In 1999 IOM assembled a committee of scientists and medical practitioners in accordance with the established procedures of the National Academies, including an examination of possible biases and conflicts of interest and provision of opportunity for public comment. A roster with brief biographies of the committee members is provided in Appendix A.
A wide variety of sources were used to assemble the data and information necessary to respond to the charge. A list of some of the individuals who assisted the committee in this effort is provided on page xiii. An initial organizational and data-gathering meeting of the committee in March 1999 provided an overview of several important organizations and education and training programs within the federal government—NIOSH, OSHA, NIEHS, and U.S. Department of Veterans Affairs. At a subsequent meeting, in May 1999, the committee heard about the training and utilization of OSH professionals in additional federal agencies, namely the U.S. Department of Defense and the U.S. Department of Energy. That meeting also featured briefings from representatives of the major OSH professional associations: the American Industrial Hygiene Association (AIHA), the American College of Occupational and Environmental Medicine (ACOEM), the American Society of Safety Engineers (ASSE), and the American Association of Occupational Health Nurses (AAOHN). The committee also heard from the National Safety Council and representatives of business (Organization Resource Counselors, Inc.), labor (New York State Public Employees Federation, American Federation of Labor-Congress of Industrial Organizations) and the insurance industry (Liberty Mutual). Follow-up with the speakers provided more detailed information and points of contact for additional questions. The sponsors’ project officers shared information on education and training from their files or put committee members in touch with the offices that had relevant data, and the committee members themselves contributed both personal contacts and specific information from their own files and experience. The World Wide Web provided much information about additional organizations and OSH training, and the following databases were accessed and searched: the National Center for Education Statistics database, National Center for Health Statistics Data Warehouse, the Federal Research in Progress database, the Federal Conference Papers database, Medline, MedStar, and HSRProj. The committee relied heavily on published and Internet-accessible data from the Bureau of Labor Statistics for projections of changes in the workforce and trends in occupational injuries and illnesses. The committee’s discussion of distance learning (Chapter 8) was greatly enhanced by a commissioned paper on that topic written for the committee by Tim Stephens, the director of the Center for
Distance Learning at the University of North Carolina at Chapel Hill. This paper, and other written materials presented to the committee, are maintained by the Public Access Office of the National Research Council Library. Appointments to view these materials may be made by telephoning the library at (202) 334-3543 or by electronic mail to nrclib@nas.edu.
Because time, expense, and contract specifications ruled out collection of original survey data on both the supply of and the demand for OSH professionals, the committee drew on membership data from the leading OSH professional societies for its analysis of the current OSH workforce. AAOHN and the American Board of Occupational Health Nursing, ACOEM, AIHA, ASSE, and the Employee Assistance Professional Association all provided copies of membership demographics and recent member surveys on relevant topics. Other quantitative information describing the current OSH workforce came from the Internet sites of the Board of Certified Safety Professionals, the American Conference of Government Industrial Hygienists, the Human Factors and Ergonomics Society, and the Society for Industrial-Organizational Psychology.
ORGANIZATION OF THIS REPORT
Following this introductory chapter, Chapter 2 describes the current OSH professional workforce. Four chapters then describe current and anticipated trends in the general workforce, the workplace, the organization of work, and the delivery of health care. Chapter 3 explores the changing demographics of the United States and its possible effects on health and safety in the workplace. Chapter 4 examines the changing nature of work in the United States in the information age and the implications of those changes for occupational injuries and illnesses. Chapter 5 takes up the globalization of work in the 1990s and its consequences for workers and OSH professionals. In Chapter 6 the committee reviews a decade of changes in health care delivery in the United States, offers some thoughts on possible trends for the next decade, and points out the implications of those trends for the training of OSH personnel. Chapter 7 describes the current education and training programs that produce these OSH professionals. Chapter 8 analyzes the growing popularity of alternatives to campus-based, classroom instruction (e.g., “distance learning”) and their application to the education and training of OSH personnel. The final chapter presents a brief summary and the committee’s overall conclusions and recommendations.















