PAPER CONTRIBUTION L
Behavioral and Psychosocial Intervention to Modify Pathophysiology and Disease Course
Andrew Baum
BEHAVIOR, STRESS, AND DISEASE
Evidence of behavioral influences in disease outcomes is growing and comes from many diverse sources. This paper considers summaries of this rapidly growing literature focusing on studies of cardiovascular disease, cancer, and HIV disease/AIDS (Figure 1). Other diseases and serious medical conditions are also considered briefly.
Stress and Cardiovascular Disease
The effects of stress on the pathophysiology of heart disease, hypertension, stroke, and other cardiovascular disorders are broad and increasingly well documented. Stress appears to contribute directly to atherosclerotic processes by which blood vessels become increasingly narrow and unable to adapt to changing circulatory demands (e.g., Smith and Gallo, 1994; Kopp, 1999). Among the effects of stress on the circulatory system are increases in damage to vessel walls and lining, increases in fat deposits in injured intimal areas and lipid pro-
|
Dr. Baum is director, Behavioral Medicine and Oncology and professor of psychiatry and psychology, University of Pittsburgh Cancer Institute, Pittsburgh Mind-Body Center, Departments of Psychiatry and Psychology, University of Pittsburgh. This paper was prepared for the symposium on “Capitalizing on Social Science and Behavioral Research to Improve the Public's Health,” the Institute of Medicine and the Commission on Behavioral and Social Sciences and Education of the National Research Council, Atlanta, GA, February 2–3, 2000. |
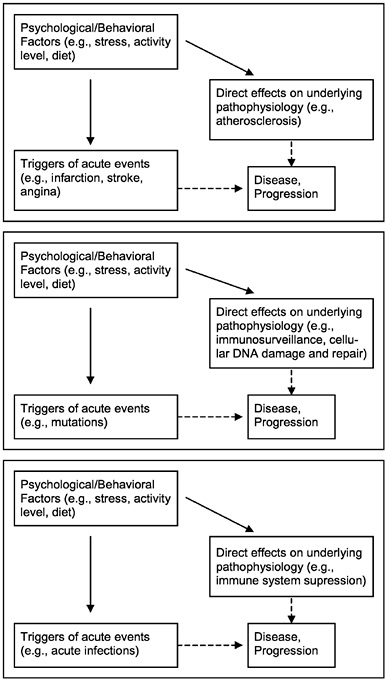
FIGURE 1 Schematic drawings of the basic relationships between stress or behaviors and diseases discussed in this chapter. The first describes simple relationships between behavioral variables and cardiovascular disease, the second considers behavioral influence and cancer, and the third depicts simple relationships between behavior and HIV disease.
files in general, and increases in plaque associated with repair and overgrowth of these injury sites in blood vessels (Schneiderman, 1983; Foreyt and Poston, 1996). Though far more complex than can be portrayed here, atherosclerosis is a lifelong process of gradual narrowing of arteries and veins, in part because of this repeated pattern of vessel damage, repair, and growth of plaque.
In coronary heart disease, factors such as diet, tobacco use, and stress modify the vessels that provide nutrients to the heart and periphery and demand for delivery of nutrients. Sharp increases in demand in an organism with occluded coronary arteries can precipitate cardiovascular events such as infarction, angina, or arrhythmias (e.g., Kamarck and Jennings, 1991). Stress also affects platelets and other clotting factors in the blood that can increase the likelihood of troublesome or dangerous clot formation, pulmonary embolism, or other untoward events (Markovitz and Matthews, 1991; Allen and Patterson, 1995). Finally, these factors can increase blood pressure in several different ways (e.g., Barnes et al., 1997). Some influences on blood pressure are directly related to stress, as is the case, for example, for beta-adrenergic receptor density (Dimsdale et al., 1994). Other effects are more broadly caused by a number of biobehavioral processes, and differences in the magnitude of acute blood pressure and heart rate changes associated with stress appear to be a risk factor for hypertension and coronary heart disease (e.g., Manuck and Krantz, 1984; Manuck et al., 1997). However, evidence is mixed, with some studies suggesting that acute stress-related effects on blood pressure are related to hypertension and some finding little or no evidence of such a relationship (Fredrikson and Matthews, 1990; Picketing and Gerin, 1990). Overall increases in blood pressure associated with chronic stress may also contribute to hypertension (Blumenthal et al., 1995).
Direct evidence that stress and other behavioral factors cause cardiovascular dysfunction or disease is increasingly conclusive, but the data are not complete. This is due in part to the nature of these diseases and their development over one's lifetime. Because the development of disease is a very long term process, it is difficult if not impossible to monitor all potential contributors to pathophysiologic disease processes or to pinpoint specific instances of stress-related plaque formation or blood pressure adjustment. However, general patterns are very clear and intermediate events or changes in a bodily system that are highly correlated with disease outcomes (such as elevated blood pressure or intimal narrowing of coronary arteries) are reliably observed as a function of stress. Animal studies, in which investigators can observe or control major stressors and can exert greater experimental control (including the possibility of genetic comparability or manipulation), offer some of the best evidence of stress effects on cardiovascular diseases (e.g., Manuck et al., 1983). Animal studies clearly suggest that stress can accelerate pathogenesis of coronary heart disease and hypertension and can evoke cardiac events (Smith and Gallo, 1994). Although not all studies agree that stress
can cause cardiovascular problems, there is certainly enough evidence to warrant further study and intervention (e.g., Elliott, 1995).
As an example, consider a series of experimental and observational studies of cynomolgous monkeys by Manuck and colleagues. This species shares many characteristic cardiovascular properties with humans, and many aspects of their behavior also resemble or parallel human social activity (e.g., Kaplan et al., 1982). When these animals have been exposed repeatedly to disruption of their social environments, they have exhibited greater evidence of coronary heart disease (Manuck et al., 1986). When unfamiliar animals are introduced into a stable group of monkeys, the result is a destabilization of the social hierarchy that had been established. This destabilizing influence is a powerful social stressor for the monkeys, and they respond to it by becoming more aggressive and more prone to cardiovascular disease (Manuck et al., 1986). Periodic reorganization of social groups has been used to generate chronic stress as animals repeatedly experience unstable social conditions, and this manipulation has permitted detailed observation of the impact of social dominance, diet, and stress on the development of cardiovascular disease (Kaplan et al., 1984). Dominant monkeys in unstable conditions exhibited the most extensive signs of heart disease, but these effects were dramatically increased by high-cholesterol diets (Manuck et al., 1986).
Interestingly, when females were studied, dominant animals showed few signs of atherosclerosis but subordinate females showed more evidence of atherosclerosis and elevated cortisol as well as ovarian dysfunction (Kaplan et al., 1996). Further stress was associated with endothelial injury through sympathetic activation (the effect was reduced by beta-adrenergic blockage), suggesting that stress-related central nervous system arousal can initiate as well as exacerbate arterial damage (Skantze et al., 1998).
Epidemiological studies of large samples of people who were thought to vary in level of chronic stress provide the most general evidence of stress effects on cardiovascular disease. For example, longitudinal studies of civil servants in the United Kingdom found that lower-status occupations thought to be more stressful were associated with higher rates of cardiovascular disease (Marmot, 1994). Several other explanations for such an effect are possible, but stress remains a viable explanation for many effects attributed to socioeconomic status (SES) (e.g., Baum et al., 1999). Other large-scale studies have found robust correlations between stress and cardiovascular outcomes, although these relationships are frequently complicated by moderating variables such as SES, social support or social integration, and personality variables (e.g., Mellors et al., 1994). For example, hostility and Type A behavior have been associated with cardiovascular disease or related intermediate outcomes in several studies (e.g., Suarez and Williams, 1990; Bennett and Carroll, 1990a; Rosenman, 1991; Houston et al., 1992), presumably because of the effects of these personality or behavioral styles on biological processes regulating atherosclerosis or other as-
pects of cardiovascular pathophysiology. Depression also appears to be related to some cardiovascular outcomes (Freedland et al., 1992; Musselman et al., 1998), and several studies have related low social support or poor social integration to disease (e.g., Uchino et al., 1996; Knox and Uvnaes-Moberg, 1998). All of these studies suggest that stress, together with a number of other psychosocial or behavioral variables, affects cardiovascular disease enough to represent targetable variance in disease risk management (Niaura and Goldstein, 1992).
Another complicating factor in studies of stress and cardiovascular risk is the fact that many other behavioral influences on cardiovascular disease, such as diet, active versus sedentary life-style, tobacco use, and coronary-proven behaviors are correlated with stress (e.g., Eysenk, 1990, 1991; Shekelle et al., 1991; Krantz et al., 1996). Smoking, consumption of high-fat diets, sedentary behavior, and hostile, competitive behaviors are independently correlated with cardiovascular outcomes but are also reliably influenced by stress. Smoking contributes to a range of outcomes and appears to be influenced by stress, as is exercise or other behavioral factors that may affect cardiovascular health (e.g. Krantz et al., 1996). Separating direct effects of stress on physiological activity from those effects of stress-induced smoking, sleep problems, or other potential behavioral pathogens is difficult but necessary if we are to most effectively target disease processes for intervention (Matarrazo, 1980).
Most of these studies look at one or more conditions thought to be stressful and statistically isolate relationships between these conditions and cardiovascular disease. For example, among women, stress associated with having several roles (e.g., employment, educational attainment) appears to increase risk for cardiovascular disease (Baum and Grunberg, 1991; Brezinka and Kittel, 1996). Job stress, particularly when demand is high and control is low, has also been linked to cardiovascular disease (e.g., Johnson et al., 1996; Kasl, 1996; Theorell and Karasek 1996; Peter and Siegrist, 1997; Weidner et al., 1997). Several studies find associations between mood or distress and hypertension, coronary artery disease, or other disorders (e.g., Carney et al., 1995; Kubzansky et al., 1998; Everson et al., 1998; Barrick, 1999; Jacob et al., 1999). Personality variables related to hostility, optimism, and coping and social variables such as support that typically buffer the effects of stress are also associated with the development of disease, disease events, and recovery outcomes (e.g., Eaker, 1989; Fontana et al., 1989; Johnson et al., 1989; Orth-Gomer and Unden, 1990). In general, research shows a broadly characterized effect of life-style behaviors and stress on cardiovascular disease and health (Kringlen, 1986; Krantz et al., 1988).
Stress and Cancer
Like heart disease, cancer is a slowly developing disease that features gradual pathophysiological activity and disease events that may have specific triggers. Also like cardiovascular disease, cancer may be influenced by behavioral factors
at several different stages. However, cancer is also different from cardiovascular disease in several ways. First, the underlying pathophysiology is difficult to identify or measure, so detection and intervention during this long recruitment stage are difficult or impossible. In addition, the immune system appears to have direct surveillance responsibilities in cancer defense and some of the most important medical advances in treatment are those that boost immunological defenses or help the immune system identify and target malignant or premalignant cells. Adding to this is the fact that cancer is not a single disease nor does it attack only one or a few systems. Cancer is best thought of as a group of more than 100 diseases that all feature dysfunctional controls on cell proliferation.
Cancer begins with mutations that occur in a cell or small cluster of cells, and progresses and becomes malignant through several other mutations in these same cells. These mutations are a function of increasing genomic instability due to age, exposure to mutagenic agents, or other factors, and are reflected in greater and greater relaxation of inhibitions on cell proliferation. In other words, each mutation makes the likelihood of uncontrolled cell growth and proliferation more likely and affected cells begin to grow in uncontrolled fashion. This instability is also related to repair rates or capabilities of cells throughout the body to repair mutations or flush them out. Mutations or more basic damage to DNA that could contribute to further mutation or instability is ordinarily repaired through a variety of cellular repair processes or eliminated through apoptotic activity (which leads cells to destroy themselves). In some cases, repair mechanisms are inhibited, damage is increased, and/or apoptotic controls are reduced, allowing mutations to be reproduced and further increasing proliferation of abnormal cells. Recent theory in immunology posits several mechanisms for immune system surveillance and defense against developing tumors; natural killer (NK) cells, for example, can conjugate or bind with tumor cells, create pores in the tumor cell membrane, and inject substances that can initiate apoptosis in tumor cells. Immune defenses against tumor cells depend on accurate identification of tumor cells and rapid elimination of them. Anything that interferes with these processes may inhibit overall tumor rejection and enhance cancer development.
There is some evidence that stress can contribute to the onset of cancer, including a considerable amount of circumstantial evidence of such links, mostly in the form of correlations between stressors and cancer diagnosis. Most studies that address stress or other behavioral factors in the etiology of cancer do not find large effects of these variables, for many reasons. The most important, perhaps, is the issue of timing and matching disease-related events to stressful episodes or other life experiences. If one is interested in the relationship between stress and cancer etiology, it is necessary to identify stressors characterizing a fairly long, extended period during which the disease develops. Unfortunately, we cannot detect early development of most cancers and cannot specify the length of the recruitment period. In some cases, a nascent breast cancer, for example, may be detectable after 5 years of development, in other cases, this developing tumor
may grow for 10 years before it is detected. Correlating stressful life events or other stressors with possible disease processes that cannot be identified readily over such long periods of time is a difficult task and is likely to yield moderate to weak correlations due to “noise” or nuisance variance associated with other events or other illnesses generated during these extended periods. Large, long term prospective studies in high-risk populations involving collection of biomarkers of disease development are needed, to accomplish this in a meaningful and interpretable manner; such studies would be very expensive, and time consuming, and are presently not feasible given the state of biomarker research and scientific funding. As a result, we are left with suggestive studies indicating that psychosocial variables are related to cancer incidence and progression (Spiegel et al., 1996). For example, loss experienced within a 7-year period preceding diagnosis of cancer was associated with this diagnosis (e.g., Ramirez et al., 1989). Cancer is a stressful disease and treatments for it are stressful as well. Increasing stress, together with economic costs and loss of self-esteem, confer a substantial burden for many patients (Schulz et al., 1995). There are also many animal studies that suggest a link between stress and tumor growth or rejection of neoplasms (e.g., Sklar and Anisman, 1981; Kerr et al., 1999).
A meta-analysis of 46 studies linking mood and anxiety disorders, childhood environment, personality, coping, and stress with the development of breast cancer yielded small but significant effects for denial or repressive coping, separation and loss experiences, and stressful life events (McKenna et al., 1999). The authors concluded that there was evidence of a moderate association between these psychological variables and breast cancer, but the size of these relationships was interpreted as equivocal support for the notion that stress contributes to development of the disease (McKenna et al., 1999). However, a more limited review and meta-analysis of research on breast cancer and stressful life events did not find evidence of an association between negative events and the onset of breast cancer (Pettigrew et al., 1999). Given the considerations discussed briefly above, however, it is possible or likely that methodological limitations made it unlikely that stronger effects could be found. The observed modest effect sizes provide some evidence of a connection between stress and coping on the one hand and cancer development on the other and may actually underestimate one's risk.
There is some evidence that stress or other behaviors affect damage and repair processes in individual cells. As noted earlier, cells can experience damage from any number of sources, including radiation, some toxins, sun exposure, tobacco and tobacco smoke, and some chemicals. The extent to which damage is experienced and the rate at which damage is repaired are critical in early events characterizing the development of cancer and would appear to be a viable mechanism underlying the effects of behavioral processes on cancer pathophysiology. An early study (Kiecolt-Glaser et al., 1985) found that stress was associated with slower repair of x-ray-induced DNA damage, and subsequent
studies found evidence of stress-related suppression of DNA repair enzymes in rats (Glaser et al., 1985). Studies of medical students comparing high-stress examination periods with lower-stress periods also yielded evidence of inhibited apoptotic activity following cell damage and decreased RNA expression of genetic tumor regulation in stressed medical students (Tomei et al., 1990; Glaser et al., 1993). Although not extensive, these data suggest that stress can interfere with basic cellular processes that could constitute a pathway to the development of new cancers or the enhancement of existing tumor growth.
Investigators have reported considerably more evidence that stress, coping, and other behavioral or psychosocial variables affect the course of cancer. Stress has been associated with relapse and recurrence of cancer in several studies (e.g., Spiegel et al., 1998). The extent to which the original diagnosis of cancer was stressful did not predict recurrence of breast cancer in one study but chronic stress assessed before cancer diagnosis was made was a strong predictor of relapse (e.g., De Brabander and Gertis, 1999). Other studies have also shown associations between stress or other biobehavioral factors and cancer recurrence or progression (e.g., Levy et al., 1985, 1989, 1990; Ramirez et al., 1989). Animal studies show this relationship even more clearly and suggest immunological mediation of some of these effects (e.g., Ben-Eliyahu et al., 1991, 1999). Because of the central role of immune system activity in defense against tumors, studies showing relationships between stress and immune system activity among cancer patients are particularly important, suggesting that stress-related immune system changes and tumor growth or metastasis of tumor cells are related (Tejwani et al., 1991; Ishihara et al., 1999). Moreover, investigation of immune system variables that might be modifiable should have an important impact on the course of cancer.
There is growing evidence of stress effects on immune system activity mediated principally by central and sympathetic nervous system activity and neuroendocrine systems (e.g., O'Leary, 1990; Felten and Felten, 1991). As noted, the immune system plays several roles in cancer defense, including immunosurveillance functions that involve immune system activity directed at locating and eliminating new or developing tumors and controlling metastases (e.g., Herberman, 1991). Natural killer cells, cytotoxic T lymphocytes, and other effectors in the system can detect tumor cells and in most cases conjugate or adhere to them to produce killing. These processes are mediated by a number of other activities, factors, and cells, suggesting that a broad look at immune system mediation of stress effects on cancer course is necessary. Evidence suggests that behavioral intervention in healthy populations or in groups with other immune system-related diseases are useful in supporting or boosting a number of aspects of immune function (e.g., Hall and O'Grady, 1991; McGrady et al., 1992).
There is also evidence that these relationships hold in studies of people who have cancer. For example, anticipating surgery shortly after the diagnosis of cancer or other stressors associated with cancer or cancer treatment may sup-
press natural killer cell activity and thereby inhibit defense against micrometastases or spread of cancer cells (e.g., Van der Pompe et al., 1998). A good deal of evidence of stress-related effects on NK cells has been reported (e.g., McKinnon et al., 1989; Kiecolt-Glaser and Glaser, 1992; Cohen et al., 1993; Schedlowski et al., 1993; Delahanty et al., 1996; Ironson et al., 1997;) and many of these effects are also apparent in cancer patient populations (e.g., Levy et al., 1985; Van der Pompe et al., 1998; Gerits and De Brabander, 1999). Cancer surgery has also been associated with suppressed NK cell lysis of tumor cells, interferon production, and lymphocyte proliferation to mitogen challenge (Andersen et al., 1998). Studies have found endocrine sequelae of stress in cancer patients that are associated with immune system regulation in healthy populations, including elevated resting levels of cortisol and attenuated hypothalamic-pituitary-adrenal reactivity to acute stressors (e.g., Van der Pompe et al., 1996). To make a long and growing story short, evidence strongly suggests that stress and other behaviors or biobehavioral processes can affect cancer course and likely do so through effects on cellular repair mechanisms and on immune system surveillance.
Stress and HIV Disease
HIV disease and AIDS are also different from cardiovascular disease in many ways. They refer to the chronic disease established by infection with the human immunodeficiency virus, a relatively new retrovirus that lives in and destroys components of the immune system. Earlier we noted that advances in sanitation, public health, and drug development had greatly limited the dangers of infectious illnesses and had eradicated most of them as major sources of disease and disability. HIV disease and AIDS are an exception to this trend, having emerged in the past 25 years as a major threat to life and well being. The virus is resistant to traditional antiviral therapies. It is spread through intimate sexual contact or in blood or blood products and is therefore commonly contracted as a result of sexual activity or intravenous drug use. It is lymphotropic, being drawn to and living in lymphocytes that are integral components of the immune system. Once established, it replicates itself many times over and destroys its host cell, releasing new viral particles to search for additional host cells. Historically, we have gauged the disease's progress by monitoring helper T lymphocytes, which appear to be a preferred and/or primary host for the HIV. Advancing disease ordinarily causes a precipitous decline in the numbers of helper cells and a corresponding inhibition of immunocompetence.
While HIV disease is initiated when the virus is introduced into the body and infection established, it can pass through many stages before reaching its end stage, AIDS. Often it passes through a period of latency or greatly reduced activity. Several viruses similarly become latent once establishing infection, and herpes viruses are reactivated periodically when immune or neural control of them is reduced or eliminated. Unlike these viruses, however, latency and
reactivation of HIV do not appear to be recurrent, episodic phenomena. Once the HIV is activated or is able to overcome immune system defenses that hold it in check, it systematically compromises the immune system and affects a range of other functions. Criteria for AIDS have varied as classification schemes for the disease have been proposed and revised, but generally AIDS refers to the point at which the immune system has been so compromised that the patient becomes susceptible to opportunistic infections—diseases or disorders that are not as prevalent or dangerous when the immune system is intact.
Behavioral issues have been particularly important in studying and dealing with the HIV/AIDS epidemic. First, HIV infection is associated with behaviors such as sexual activity and drug use, and infection can generally be prevented through a combination of abstinence, monogamy, contraception, and use of clean, uninfected needles. Most attention from the behavioral science community has been in this area of prevention, with program development in teaching people to use “safer sex,” distribution of bleach and/or clean needles to intravenous (IV) drug users, and so on. Less attention has been paid to whether behavioral factors affect the HIV and progression of disease once infection has been established. However, there are now sufficient data to establish a plausible case for such influences.
Like cardiovascular disease and cancer, HIV disease has a variable course and progresses through latency or as it overwhelms immune defenses at widely variable rates. Some people who have been infected with HIV may remain healthy and free from opportunistic infection for many years, but others decline more rapidly and become symptomatic soon after infection (e.g., Munoz et al., 1989; Phair et al., 1992). This variable course has been attributed to differences in viral strains, host immune resistance, and psychosocial variables such as stress (e.g., Levy, 1991; Kemeny, 1994; Cole et al., 1996). Early in the study of HIV disease and AIDS, scientists interested in the effects of stress or behavior on immune status and function began to theorize about application of this work to HIV progression (Soloman, 1987; Solomon et al., 1991). Noting that HIV disease could be discussed in the context of interactions between the central nervous system and the immune system, these theorists argued that anything that perturbed or altered the ability of the immune system to defend the organism could affect the speed of spread of HIV and hasten the development of AIDS.
Early data suggested that several variables might be involved, most notably stress, coping, social support, and emotional or autonomic reactivity (Solomon et al., 1991). Since then data have accumulated suggesting that stress and coping are significant predictors of progression of HIV disease (e.g., Goodkind et al., 1992; Remiea et al., 1992; Reed, 1994; Schlebush and Cassidy, 1995; Mulder et al., 1999). Coping and self-efficacy appear to mediate stressful effects of being HIV seropositive, reducing distress and stress-related immune system fluctuations (e.g., Antoni et al., 1995; Benight et al., 1997). Major stressors may cause exacerbations or intensification of disease processes or symptoms in several
diseases (e.g., Lutgendorf et al., 1995), and variation in stress hormones appears to be related to differences in rates of HIV infection (e.g., Antoni et al., 1991). Depression is also known to affect immune status and function but is not necessarily associated with progression of HIV disease (Lyketsos et al., 1996; Miller et al., 1997). Finally, there is some evidence that psychological inhibition confers negative effects on several basic bodily processes and that gay man with HIV infection appear to progress more rapidly when they report concealing their sexual orientation (Cole et al., 1996).
Interpretation of these studies is complicated by their correlational nature and the complexities of the disease and its social context. For example, social or stress-related changes associated with HIV disease may be both a cause and an effect of disease progression. In a study of 925 Australians living with HIV disease or AIDS, disease progression predicted employment status (Ezzy et al., 1999). Half of those leaving work reported that declining health was the reason, and since unemployment appears to be stressful one could expect that losing work might further contribute to disease progression. This same reasoning complicates the appropriate interpretation of studies of depression and HIV/AIDS. For example, Siegel and her colleagues found that gay and bisexual men with HIV or AIDS were at greater risk for psychological distress than would be expected if they did not have the disease and that risk increased as their disease progressed (Siegel et al., 1996). The results of this clearly indicated that adjustment problems associated with HIV disease were an important source of distress but could not specify whether these adjustment problems were a product of disease progression or fed back to affect disease course.
An interesting avenue of investigation has been studies of inhibition and stress as predictors of disease course. As noted earlier, psychological inhibition, defined as either voluntary or involuntary constraint of discussion or disclosure about a stressful or important event or fact, can also affect well being (e.g., Pennebaker et al., 1987). Many people living with HIV are gay or bisexual, and some of these people may be reluctant to disclose their sexual identities or lifestyles. It is possible, then, that the concealment of one's sexual preferences is stressful and that men who do not disclose such information are at risk for more serious disease. This is similar to the findings of a study by Cole and his associates (Cole et al., 1996) that followed HIV-seropositive but asymptomatic men for 9 years. Time to critical levels of helper lymphocytes, AIDS, and AIDS-related mortality were related to the degree to which homosexual activities were concealed (Cole et al., 1996). These effects may have been due to coping style differences associated with disclosure rather than to the effects of psychological inhibition (e.g., Ostrow, 1996), but the importance of these findings is broader than the specific mechanisms involved.
There are not many studies that specifically measure the mediating effects of immune system activity when evaluating effects of stress on HIV disease progression. There is evidence that changes in several immune parameters that
are affected by behavioral variables predict disease progression, including numbers of helper lymphocytes, loss of antibody response, and other immune system variables (Fernandex-Cruz et al., 1990). Bereavement is a significant stressor for people living with HIV since intimate partners or close friends may also have HIV disease and may die of AIDS-related complications. In a study of 78 bereaved and nonbereaved people with HIV, there was a significant increase in immune system activation but a decrease in T cell proliferation after the death of an intimate friend (Kemeny et al., 1995). Studies like this are rare but no matter how daunting the complexities underlying psychosocial moderation of HIV disease may be, definitive studies of stress or other behavioral factors as factors in the progression of HIV and AIDS should be possible. Data suggest, for example, that stress predicts physical symptoms of AIDS but does not predict progression of HIV disease or related immunological changes (e.g., Rabkin et al., 1991; Perry et al., 1992). Complicated characteristics of the virus and of different “strains” of the HIV are important and not well understood, as are long term effects of new treatment regimens for HIV and AIDS (e.g., Hall, 1988; Levy, 1993). Because HIV disease and AIDS are diseases that are centrally immunological and involve suppression of immune responses that are also suppressed by stress, it remains likely that behavioral influences on immune status constitute modifiable variance in disease progression.
CONCEPTUAL BASES FOR BEHAVIORAL INTERVENTIONS
Simply stated, theories underlying behavioral intervention to modify disease course are based on the assumptions that behavioral or psychosocial influences on disease course are modifiable and that reducing negative influences will slow disease progression or minimize recurrence of disease following treatment. The simplest forms of this theory are inherent in prevention-oriented campaigns that urge people to quit smoking, eat healthy foods, or exercise. Tobacco use, poor diets, and sedentary life-styles all appear to contribute directly to development and persistence of cardiovascular disorders, cancers, and other chronic illnesses. These behaviors as well as stress and other factors (e.g., alcohol use, drug abuse, and obesity) affect basic biological processes, including lipid profiles, insulin resistance, immune function, and sympathetic or hemodynamic tone. These basic processes mediate a number of important pathophysiological outcomes and affect tumor rejection, atherosclerosis, resistance to viral infection, and blood pressure (e.g., Baum and Posluszny, 1999). Modifying behavioral input at the start of these causal sequences is thought to reduce disease outcomes by altering mediating biological conditions.
The logic for this kind of approach is appealing and has received at least circumstantial support. The studies reviewed in the first section of this chapter provide a considerable empirical base for these efforts. A number of behaviors
and biobehavioral processes appear to affect key events in the etiology of cardiovascular disease and cancer and in the development and progression of HIV disease. How these behaviors or processes can best be modified and the extent to which one or another system or condition mediates disease risk or outcome is less clearly specified by the literature. Cessation or prevention of smoking or other tobacco use is unarguably an important public health objective, but how best to accomplish this or how its negative effects are conveyed has not been addressed convincingly. Further, how these behaviors are influenced by stress, or how stress reduction affects them; is often not part of basic prevention or behavior change interventions nor is this clearly delineated. Stress interferes with early detection and surveillance, appears to affect diet and exercise, is a cause of smoking or drug use relapse after cessation, and is a factor in other instances of health-related behavior modification (e.g., Baum and Posluszny, 1999). The best ways to intervene and help people reduce stress, cope with uncertainty, manage side effects, comply with difficult treatments, and the like are not yet established. What has become clear is that modification of these “health-impairing” behaviors and processes is an important goal, that comprehensive programs appear to be well suited for this effort, and that an emphasis on substituting “health-enhancing” behaviors for less healthy activities is important as well.
As suggested by this, interventions remain eclectic and loosely centered on one or another basic approach to stress management, psychoeducation, support provision, and/or behavior change. Many are considered cognitive-behavioral approaches and share emphasis on relaxation training, coping, and appraisal. These approaches work to (1) reduce negative mood and “excess” arousal associated with stress, (2) enhance knowledge of coping so that people can deal with stress more effectively, and (3) modify appraisals of stressors and/or their environmental contexts to reduce the extent to which stress is experienced. These objectives are derived directly from research and theory on cognitive-behavioral therapy, the efficacy of reducing arousal or teaching relaxation, and theories of stress and coping (e.g., Mason, 1975; Leventhal, 1980; Turk et al., 1983; Lazarus and Folkman, 1984). Broader or more comprehensive approaches add one or more other components or focal points, with some success. Some, for example, add aerobic exercise as an adjunct to relaxation (to help disperse arousal and ameliorate mood) which also has a direct benefit (e.g., enhanced cardiovascular or metabolic tone, and fitness). Other interventions may focus instruction in coping or problem solving on a particular problem or problem behavior, using it to illustrate appraisal and coping issues and providing basic knowledge about disease processes.
Many overarching models of health and behavior are relevant to this effort, including those describing three basic pathways between psychosocial or behavioral variables and health or treatment outcomes (e.g., Krantz et al., 1985; Baum and Posluszny, 1999). Behavioral variables or stressors may have direct effects on biological systems involved in pathobiology and may affect other behaviors
that in turn have direct effects on these same biological systems or may affect “sick” behavior or how people behave when they are ill. Andersen et al. (1994) proposed a biobehavioral model that included these general pathways and specifically focused on adjustment to cancer, citing “ample evidence…that adults experiencing other long term stressors experience…important biological effects, such as persistent down regulation of elements of the immune system and adverse health outcomes ” (p. 389). Their model summarizes and organizes a great deal of research and proposes several mechanisms linking psychosocial and behavioral variables with biological processes and treatment outcomes.
Arguing that cancer itself poses a great many sources of stress and that this burden can affect disease course, Andersen and her colleagues suggest that behavioral systems such as compliance and health behaviors are affected by and contribute to direct effects of stressors on central and peripheral nervous system activity, endocrine activity, and immune system functions. Many of these sources of stress are persistent and last well beyond the completion of treatment, including social stigmatization, irrevocable changes in sexual or reproductive function, loss of stamina, economic loss, and diminished cognitive capabilities (e.g., Cella and Tross, 1986; Wingard et al., 1991; Kaplan, 1992; Yellen et al., 1993). These sources of stress, working with other stressors and psychological trauma associated with cancer diagnoses, can affect local and metastatic disease by influencing a range of behavioral and biological variables (e.g., Baum and Posluszny, in press).
The model proposes specific behavioral pathways that may affect disease course, citing evidence that stress can contribute to appetitive disturbances common in cancer patients, sleep disturbances, self-medication with alcohol and other drugs, tobacco use, and sedentary behaviors (Andersen et al., 1994). Nearly 40% of cancer patients report problems with loss of appetite or inability to eat, and cancer patients or survivors appear more likely than healthy people or people who have never had cancer to report sleep difficulties (e.g., Cella and Tross, 1986; Wellisch et al., 1989). The detailed analysis of these and other health behaviors as well as direct effects of cancer treatments on these behaviors describes a compelling framework within which to view psychosocial and biobehavioral mediation of disease course. Importantly, it also specifies a range of intervention targets for stress reduction and enhancement of treatment outcomes.
Theories underlying intervention for medical populations are far more complex and extensive than can be considered here (see Figure 2 for an example). Disease-specific models for other syndromes have been developed, research on mechanisms underlying hypothesized effects has continued to expand, and we are learning more about modifiable behavioral variance in disease course as these developments continue. For now, it is sufficient to note that these models offer a number of intervention targets and suggest a range of approaches and strategies. Evaluation of existing knowledge about intervention effects can be
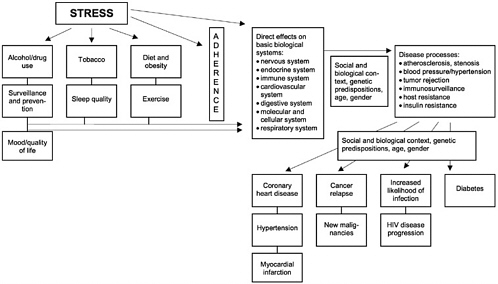
FIGURE 2 A model of processes underlying efforts to intervene to modify disease course. Stress and a wide range of health-impairing or health-protective behaviors interact to produce effects on basic bodily systems that can contribute to pathophysiology. Stress also exerts direct effects on those systems, on mood and quality of life, and on attempts to modify health-impairing or protective behaviors to prevent or detect early disease. These, in turn, also affect pathophysioloical processes. Stress affects adherence and success of behavior change efforts, which also affect biological processes. Effects of these bodily changes are translated into variable disease processes by differences in initial fitness or systemic state, use of chemopreventive regimens, age, and other factors, affecting a number of important disease outcomes.
viewed in the context of these models, and they serve an important organizing function as well.
INTERVENTIONS AND STRESS REDUCTION FOR CHRONIC ILLNESSES
Based on these data and developing theoretical models of health and behavior, a number of interventions for disease prevention and control have been implemented and evaluated. Clearly, intervention can occur at several different points in the process; early on, healthy behaviors can be established and reinforced and the earliest development of disease slowed or stopped. Early detection and surveillance efforts are important in identifying risk profiles and more readily treated early manifestations of disease. Interventions for patients and families designed to reduce stress, buffer immune and endocrine activity from effects of stress or treatment, and otherwise reduce or eliminate behavioral contributions to advancing disease are all warranted by the emerging literatures on these topics. Intervention across the entire course of illnesses, from early asymptomatic stages through more complex advanced stages and need for palliation, seems justified. At the same time, behavioral and psychosocial factors that predict participation in and adherence to interventions add another important dimension to this effort (e.g., Naeslund et al., 1993). The present discussion focuses primarily on comprehensive stress management interventions as they affect cardiovascular disease, cancer course, and the development of AIDS.
STRESS MANAGEMENT AND CARDIOVASCULAR DISEASE
Although there would seem to be numerous avenues of approach to intervention to reduce behavioral effects on the development of cardiovascular disease, there have not been extensive investigations of these interventions beyond smoking cessation, nutrition management, and fitness programs. As we have suggested, interventions directed at smoking or other tobacco use would go a long way to reducing morbidity and mortality from cardiovascular disease, cancer, and many other illnesses. However, interventions to reduce or deflect stress and/or alter life-style have been less frequent. Stress management interventions should, if our reasoning holds, reduce or deflect some of the conditions that regulate or contribute to the pathophysiology of heart disease, stroke, hypertension, and other cardiovascular disorders.
Some studies find evidence supporting the notion that behavioral interventions can reduce risk for cardiovascular disease by reducing physiological developments that predispose or trigger these disorders. For example, stress management interventions can reduce the hostility, competitiveness, and time urgency associated with Type A behavior; can lower serum cholesterol; and can reduce blood pressure (Bennett and Carroll, 1990b).
A meta-analysis of studies of intervention to modify Type A behavior suggested that after intervention, participants reduced Type A behavior scores by about half a standard deviation and the probability of 3-year mortality or heart attack corresponded to a 50% reduction in risk (Nunes et al., 1987). Distress and psychiatric disorders associated with the diagnosis of cardiovascular disease, including hostility, are reduced by regular clinic visits, again suggesting personality-based dynamics in risk for cardiovascular disease (Mann, 1984). Type A behavior may also influence the efficacy of intervention designed to enhance relaxation responses independent of hostility or time urgency. Progressive muscle relaxation training was evaluated among Type A men with borderline hypertension (Haaga et al., 1994). The intervention was intended to modify acute reactivity to challenges rather than hostility or anger. The relaxation training was effective in reducing reactivity and had mild effects on anger or hostility (Haaga et al., 1994).
As late as 1985, Type A behavior was considered to be a major source of risk for heart disease and other cardiovascular disorders (e.g., Matthews and Haynes, 1986). Since then, a focus on the more toxic components of this behavior pattern, most notably hostility (e.g., Dembrosky et al., 1989), has redefined this literature and retargeted some intervention efforts. However, evidence remains that Type A behavior has some predictive value in estimating risk for coronary heart disease, that interventions can reduce biological underpinnings of this behavioral style, and that modification of these and related behaviors still has potential for reducing postinfarction morbidity and mortality (Bennett, 1994).
Stress management programs often focus on relaxation but can be broader in scope. Programs involving both relaxation and more cognitive elements can reduce risk and intermediate outcomes that predict disease progression or contribute to atherosclerosis (e.g., Steptoe, 1989). More intensive interventions appear to be more effective than less involving ones, as was the case in a study of stress management among police recruits (McNulty et al., 1984). An intervention consisting of ten 90-minute sessions dealing with stress management was associated with lower catecholamine levels than was a loosely-organized program of occasional lectures (McNulty et al., 1984). Relaxation training has been associated with lower levels of cortisol, prolactin, and urinary catecholamines (Gallois et al., 1984). Behavioral procedures that are effective in treating circulatory disorders such as Raynaud's disease also provide evidence of the value of these efforts in modifying basic underlying biological causes of disease, in this case beta-adrenergic stimulation in the peripheral circulatory system (Freedman, 1987). Biofeedback-assisted stress management can also reduce muscle tension and cortisol responses that contribute to high blood pressure (McGrady et al., 1987).
The most frequent target of interventions to reduce cardiovascular disease have been directed at hypertension. Primary management of hypertension has typically been pharmacological, administering drugs to reduce heart rate, pre-
serve blood volume, or otherwise alter activity by the heart and vasculature. However, nonpharmacological, behavioral approaches to reducing blood pressure and risk for stroke or other disorders have increased dramatically since 1975 (e.g., Shapiro, 1983). Several studies suggest that stress management interventions that effectively reduce blood pressure or blood pressure responsiveness to challenge are useful in treating hypertension (e.g., Jacob et al., 1987; Irvine and Logan, 1991). One, combining education about stress and hypertension with relaxation training and problem solving, showed that those receiving the intervention were more likely to achieve a significant reduction in resting blood pressure and to maintain normotensive readings (Garcia-Vera et al., 1997). Increases in problem-solving skills were correlated with reductions in blood pressure among intervention participants but not among waiting list control participants (Garcia-Vera et al., 1998). Enhanced problem solving partially mediated the effects of the intervention on blood pressure, swamping effects associated with relaxation training or education. Similarly, a study of 41 hypertensive, African American men suggested that coping skills training reduced blood pressure and distress (Bosley and Allen, 1989). Participants in the skill-building group exhibited larger decreases in systolic blood pressure and in state anxiety than did control participants.
The efficacy of relaxation training in reducing blood pressure has been shown as well (e.g., Irvine et al., 1986; Albright et al., 1991; Broota et al., 1995). A 4-year study of relaxation and behavior change to reduce cardiovascular disease risk found poor long term adherence to the program (only 17% of the intervention group reported that they still engaged in regular relaxation after 4 years), but blood pressure reductions were greater among this group than among participants who had never practiced regular relaxation or had stopped using relaxation exercises within 30 months of the intervention sessions (Steptoe et al., 1987). Other studies also suggest that continued practice of relaxation exercises is important in blood pressure control (Hoelscher, 1987). The effects of these relaxation-oriented interventions are broad and include effects on blood pressure, cortisol, aldosterone, and plasma catecholamines (McGrady et al., 1987).
They are also manifest when applied to hypertensive patients for whom pharmacologic interventions have not been effective (Jacob et al., 1992) or as a sole treatment for hypertension (Irvine and Logan, 1991). In the latter study, relaxation decreased blood pressure and also reduced alcohol consumption (which was associated with high blood pressure) (Irvine and Logan, 1991).
Efforts to intervene with hypertensives have also focused on modifying acute blood pressure reactivity to challenge or stressful stimuli (e.g., Haaga et al., 1994). These efforts often combine modification of personality, behavior patterns, and/or emotional reactions to stress and challenge. One study found that relaxation training significantly lowered blood pressure reactivity to a laboratory stressor and that this effect was dependent on endogenous opioid activity (McCubbin et al., 1996). When opioid activity was blocked with naltrexone,
effects of relaxation training were reversed. Other interventions address emotional reactivity or style, as did a successful application of relaxation therapies to borderline hypertension and heart rate (Davison et al., 1991). A comprehensive evaluation of stress management training and Type A management training designed to reduce anger, hostility, and acute blood pressure reactivity found that both interventions reduced resting blood pressure and reactivity to the Type A assessment interview (Bennett et al., 1991). The Type A management intervention was better at modifying anger, hostility, and blood pressure reactivity, suggesting that the emotions that accompany this behavior pattern are a key component of heightened reactivity.
Although large-scale prospective evaluations of comprehensive cardiovascular risk reduction interventions using biological markers of disease progression have generally not been reported, several studies using broad interventions to slow disease progress or otherwise reduce the likelihood of disorders or cardiovascular events have been done. For example, cardiovascular risk reduction programs that are aimed at simultaneous alteration of several risk-enhancing behaviors are associated with beneficial changes in several intermediate outcomes linked with coronary heart disease (Lovibond et al., 1986). Interventionbased changes were maintained for a year and included weight loss of about 20 pounds (on average), 5–10% reductions in blood pressure, 33% reductions in serum cholesterol, and an overall decrease in risk for coronary heart disease.
Psychoeducational programs for coronary heart disease patients (combining education with stress management and general risk behavior reduction) also appear to be important adjuncts to conventional medical care. A study of a behavioral intervention for life-style change among angioplasty patients achieved significant reductions in smoking, exercise, diet, weight reduction, chest pain, and aerobic capacity (King et al., 1999). Meta-analysis of intervention programs, including 37 studies, suggests that there are impressive benefits from these interventions, with reductions of overall cardiac mortality of more than a third and a 29% decrease in recurrent myocardial infarction (Dusseldorp et al., 1999). Significant reductions in blood pressure, cholesterol, body weight, and smoking as well as changes in exercise and diet were also noted. These interventions did not reliably affect anxiety or depression, suggesting that they were not operating through mood enhancement. Finally, and perhaps most importantly, those interventions that had the largest effects on mediating or intervening conditions such as blood pressure, smoking, or exercise also had the most substantial effects on mortality and morbidity (Dusseldorp et al., 1999).
This growing literature strongly suggests that behavioral management of cardiovascular disease processes is an important way to reduce risk of heart attack, hypertension, stroke, or other disorders. Clearly, broad approaches that emphasize education, reduction in behaviors that confer risk, and reduction in stress or stress reactivity are called for to combat the nation's number one cause of death. Education is not sufficient by itself (Suminski et al., 1999), and programs that provide education, skill training, risk behavior intervention, problem-
solving experiences, and relaxation appear best suited to the task. The major behavioral interventions for hypertension, including relaxation, biofeedback, weight loss, diet modification, exercise, and reduction of alcohol use, can reduce risk of cardiovascular disease or events such as infarction or stroke (Dusseldorp et al., 1999). Treatment of depression may enhance conditions ranging from myocardial ischemia, platelet activation, and hyperactivity and improves survival and quality of life (Musselman et al., 1998). The promise of these interventions and the health and cost benefits of behavioral management of chronic illness strongly suggest that investigation and use of such approaches to public health problems like cardiovascular disease are warranted (e.g., Johnston, 1987; Sobel, 1995; Lorig et al., 1999).
Stress Reduction and Cancer
There are now a number of studies of interventions for cancer patients directed at reducing stress and providing context for coping with cancer. Only a few have examined putative mechanisms by which stress might affect cancer course or outcomes, and only a handful have been able to examine effects on recurrence or survival. However, the results of several of these early efforts and intermediate outcome data from ongoing trials are encouraging and suggest that behavioral or psychosocial interventions are an effective means of reducing modifiable variance in cancer mortality.
As noted earlier, the idea that stress affects the nature and course of cancer and/or response to treatment has been popular for some time, and a variety of early efforts at intervention were reported (e.g., Richardson et al., 1990; Andersen, 1992). However, it was the publication of the results of an intervention with advanced-stage breast cancer patients by Spiegel and his associates (e.g., Spiegel et al., 1989) and of an intervention with melanoma patients by Fawzy and his colleagues (Fawzy et al., 1990, 1993) that sparked the current storm of interest in this approach to cancer care. The Spiegel study found evidence of dramatic gains in survival due to an intensive, year-long psychosocial intervention that addressed social support needs as well as existential stressors and other aspects of advanced-stage breast cancer (Spiegel et al., 1989). Fawzy and colleagues found smaller but equally robust gains in survival for melanoma patients with a different but related intervention focusing on stress, coping, and problem solving (Fawzy et al., 1990, 1993). The study included immunological measures and found predicted changes in some indices of immunity, but did not find that these immune system changes mediated survival gains. These findings caught some by surprise, and the clear demonstration of prolonged survival and enhanced quality of life was encouraging and strongly suggested an impact of different intervention approaches on aspects of cancer progression and patient well-being.
Since the appearance of these studies, several investigators have initiated intervention studies. Many are with breast cancer patients (e.g., Helgeson et al., 1999), but this approach is being broadened to include other cancers at a variety
of stages (e.g., Baum et al., 1995). Meta-analyses and critical reviews of this growing literature suggest that psychosocial or psychotherapeutic interventions and differences in social support or social integration can contribute to psychological adjustment and well-being as well as disease course and immune status (Frischenschlayer et al., 1992; Meyer and Mark, 1995; Helgeson and Cohen 1996). For example, Helgeson and her colleagues have compared a psychoeducational intervention for primary-stage breast cancer patients with an intervention concentrating on social support and one dealing with both approaches simultaneously (Helgeson et al., in press). These three interventions were also compared with a control group, and both the psychoeducational and the combined interventions were associated with better adjustment and less distress than the social support intervention or control condition. This major trial produced convincing evidence of the value of these interventions (Helgeson et al., in press). Interestingly, the social support intervention was not associated with better life quality and functioning over the first 6 months after the intervention was complete, raising the strong possibility that different stages of disease with different prognoses are best met with different intervention approaches (Helgeson et al., in press). These possibilities are currently being evaluated in a newly initiated trial at the Pittsburgh Mind-Body Center of Carnegie-Mellon University and the University of Pittsburgh.
Other ongoing trials in Pittsburgh and at Ohio State University, as well as several other sites, are evaluating the generality of interventions to other cancers, some of the immunologic and endocrine mediators of intervention effects on disease, and relative impacts of group and individually delivered interventions. Data from these studies are not yet available, but preliminary evaluations of some of the data are encouraging (e.g., Andersen et al., 1998; Andersen, personal communication, 1999; Helgeson, personal communication, 1999). The further development and study of these interventions as well as interventions, to reduce stress and facilitate psychological adjustment among people at high risk for cancer, seem warranted (e.g., Glanz and Lerman, 1992; Baum and Andersen, in press).
Of particular interest in this literature are studies of interventions that include measures of putative psychological and biological mechanisms underlying observed benefits of these programs (Levy and Wise, 1989). Several ongoing studies have included endocrine and immune measures in their evaluation phases (e.g., Cruess et al., in press), and data are being collected to determine, for example, whether gains in survival and well-being are related to immune system activity, better cell repair and tumor rejection, enhanced adherence to and tolerability of medical treatments, or other phenomena that may be altered or enhanced by psychotherapeutic interventions. Initial reports of intervention for melanoma patients (Fawzy et al., 1990) indicated that six 90-minute intervention sessions were associated with enhanced mood and acute increases in numbers of CD8 T lymphocytes and in numbers and cytotoxicity of natural killer cells 6 months after the intervention. Later reports indicated the same general pattern of result over a longer period of time, with immune system gains corre-
lated with the magnitude of decreases in anxiety and depression (Fawzy et al., 1993). Greater NK cell cytotoxicity was associated with less recurrence (Fawzy, 1994). Other investigations have also found evidence of immune system change that is associated with psychosocial or behavioral interventions. Cancer patients receiving biofeedback training and psychoeducation exhibited lower levels of arousal, lower cortisol levels, and better immune status than did untrained controls (Gruber et al., 1993). Relaxation training, education, and coping skills training also reduced levels of stress hormones and increased overall numbers of lymphocytes among breast cancer patients (Schedlowski et al., 1984). Two months of relaxation training for ovarian cancer patients who were receiving chemotherapy were associated with more lymphocytes and higher white blood cell counts (Lekander et al., 1997). These promising data offer evidence of the impact of behavioral interventions on potential immune mediators of disease course. More focused work on the effects of these interventions on regulatory functions and specific antitumor activities is in progress.
Increased interest and commitment to prevention and surveillance for new or recurrent cancer may also be associated with better adjustment (e.g., Schulz et al., 1995; Charles et al., 1996; Moyer and Salovey, 1996). Interventions focusing on intact families and/or spouses of cancer patients have also been described (e.g., Keller et al., 1996). Other mechanisms by which these interventions may help to achieve better cancer control are related to mental health and associated behaviors, to life-style changes that minimize nonstress conditions contributing to cancer course, and to more effective risk management and reduction (e.g., Gritz, 1991; Glanz and Lerman, 1992; Ganz et al., 1993; Spiegel, 1995; Miller et al., 1996; Spiegel and Kato, 1996, Van der Pompe et al., 1996; Redd, 1997).
To summarize, psychosocial intervention has been an active adjunct to medical care for cancer patients, particularly over the past 10 –15 years. Some evidence of enhanced survival and of immune system effects of these interventions suggests that they accrue benefits, in part, by deflecting pathophysiological processes and either slowing or delaying disease progression or contributing to remission of the illness (e.g., Spiegel et al., 1989; Richardson et al., 1990; Fawzy et al., 1993; Garssen and Goodkind, 1999). Although we will know much more in the next 5 years about how these interventions work and how well they deflect disease course or bolster well-being, available data are sufficient to support widespread, broad-based application of interventions for early- and later-stage cancer patients and their families (e.g., Dreher, 1997; Spiegel et al., 1998).
Psychosocial Intervention and HIV/AIDS
One reason for the lack of large, definitive natural history studies of stress, immunity, and HIV disease is that interventions directed at sources of variance in stress and immune status have already returned encouraging results. Understandably, investigators and funding agencies may be less interested in con-
ducting careful, large-scale, prospective investigations of unintervened subjects and reluctant to propose studies that do not include an intervention component. However, data from these interventions are far from definitive, and the rush to intervene may still be premature.
Early studies of stress management interventions yielded mixed results. One attempt to intervene featured stress management training and efforts to enhance safer sex practices in asymptomatic HIV-seropositive men (Coates et al., 1989). The intervention was successful in reducing some risky sexual behaviors but did not affect immune system status. On the other hand, 10-week stress management and aerobic exercise interventions for men at risk for HIV and AIDS was effective in buffering effects of stress associated with notification of HIV serostatus (LaPerriere et al., 1990; Schneiderman et al., 1992). Notification that they were HIV seropositive was associated with stress and suppression of natural killer cell activity and cell proliferation. The intervention reduced some of these effects.
Several interventions have been shown to affect quality of life and psychological distress (Lutgendorf et al., 1995; Vaughan and Kinnier, 1996; Pomeroy et al., 1997; Belcher et al., 1998; Kelly, 1998). The vast majority of interventions, as noted earlier, were more prevention-oriented and aimed at reducing risk for infection (Baum and Nesselhof, 1988; Fisher et al., 1996; Ford et al., 1996). For the most part, however, these interventions have not addressed mechanistic components, nor have they been broadly conceived to cover the long-range progression of disease. One, designed to improve coping following AIDS-related bereavement is a case in point. The intervention, which provided social support, permitted and encouraged emotional expression, and identified and reviewed AIDS-related problems and coping strategies, was associated with reduced distress (Sikkema et al., 1995). Presumably this reduction in distress could affect immune status and/or disease progression, but these measures were not targets of the study.
There are other behavioral factors that affect immunity in ways that could contribute to HIV disease progression, but evidence is insufficient to draw firm conclusions. Many of these factors are also affected by stress: alcohol use, for instance, is affected by stress (Breslin et al., 1995) and may be linked to HIV disease, but evidence is too inconsistent to permit us to conclude that alcohol is a cofactor in infection or a modulator of progression (e.g., Dingle and Oei, 1997).
A series of studies conducted at the University of Miami provides the most comprehensive picture of psychosocial intervention for people with HIV infection or AIDS. These studies consider a broad application of cognitive behavioral stress management techniques to populations of HIV-seropositive men. The interventions were typically evaluated in randomized, wait list control trials, and a range of outcomes tapping mood, psychological adjustment, mental health, and stress were assessed. Findings have been consistent and dramatic, suggesting that this intervention approach is associated with enhanced mood (less anxiety, anger, or depression), less perceived stress, lower production or excretion of
stress hormones (norepinephrine, cortisol) and testosterone, and “better” immune function (more cytotoxic T cells, lower latent viral antibody titers) when compared with wait list controls (e.g., Lutgendorf et al., 1995; Antoni et al., 2000; Cruess et al., in press). These effects appear to be relatively stable over time and provide compelling evidence of the pervasive influences of biobehavioral processes on HIV disease and of the ameliorative impact of intervention in this population.
An important issue that requires at least brief consideration reflects recent developments in treatment of HIV with protease inhibitors and combination therapies. These treatment modalities have had good success and a substantial impact on the treatment and toll of HIV and AIDS. They represent real progress in medical efforts to stop HIV and its spread through the body. These new therapies were introduced in the mid-1990s and appear to be effective in inhibiting viral replication and disease progression. However, even with the availability of effective treatments, the prevention of infection remains the most effective approach. Further, as Schneiderman and Antoni (in press) have suggested, these drugs have unpleasant side effects, often involve complex regimens that make adherence difficult, and may not be available to everyone who needs them. Interventions that address these issues as well as more conventional targets such as stress and psychological adjustment are of greater significance than those that target only systemic resistance. Since issues such as adherence will ultimately influence the effectiveness of therapy and whether desired treatment outcomes are achieved, they are key targets for behavior modification, shaping, and support (e.g., Schneiderman and Antoni, in press).
CONCLUSIONS
Research clearly suggests that behavioral and social phenomena contribute to health and illness and that interventions designed to modify these factors can improve overall health and well-being. Although we have focused on stress as a general source of variability in disease course and as an influence on health-impairing and health-enhancing behaviors, there are many important influences on these processes, ranging from SES and cultural variables to behavioral inhibition and coping styles. There are also many intervention approaches that may be effective in modifying adverse outcomes, including ways to alter disclosure and inhibition profiles, modify consequences of lower SES, and “ legislate” behavioral changes that can enhance health. The most important conclusions that one can reach at this juncture suggest that behavioral and social influences on disease and disease course are pervasive, that these influences represent modifiable variance that can be altered to reduce overall morbidity and mortality, and that interventions directed at these relationships between behavior and disease can sharply reduce health care costs and improve quality of life and well-being.
These conclusions are consistent with those reached in the Healthy People 2010 document recently released by the U.S. Department of Health and Human
Services (DHHS). The latest in a series of initiatives released periodically by DHHS and the Surgeon General, this report continues a trend that has seen behavioral and life-style factors and disease prevention play an increasingly important role in setting and achieving national health objectives. These goals must address the complexities introduced by changing population demographics such as age and cultural diversity, changing health care economics, and the revolutions in technology and informatics that have characterized the past 20 years and will likely dominate the next 20 years. These issues clearly affect the value and yield of interventions such as those described in this paper, and the broad sources of influence that are often targets of these interventions will advance our knowledge and health practices toward the 2010 objectives. The realistic promise of dramatic decreases in morbidity and mortality that can be achieved through modification of behavioral contributions to disease processes is increasingly within reach.
The importance of cultural diversity, SES, and other population variables cannot be overlooked in discussing these interventions. However, the differences in effectiveness, acceptability, or dynamics of interventions to affect disease-related behavior and stress have generally not varied or examined gender, ethnicity, or age of target participants. One would expect that factors such as gender, age, national origin, and ethnicity could influence receptivity to and appropriateness of psychotherapeutic interventions. In general, gender-, age-, and culturally appropriate intervention programs are best-suited to modifying behavioral variance in disease course, and it is likely that inappropriately generalized approaches could fail to effect positive changes or add to patients' burden of stress. Yet, there are few studies evaluating these issues and none that compare approaches directly across population groups. It has been assumed, for example, that women respond more positively to group interventions and social support than do men, and a variety of theoretical justifications can support such predictions. Comparisons are sparse, in part because the majority of these studies are for breast cancer, and early results from prostate cancer interventions suggest that men also respond well to these approaches. Similarly, there are now data suggesting that women find individual psychoeducational interventions effective and beneficial as well. Age and ethnicity are also important potential mediators but have not received direct attention, and issues related to discrimination, prejudice, and the burdens of minority status in the United States have not been directly addressed either. Extension of this research and clinical literature to systematically evaluate possible differences across population groups will be an important addition over the next decade.
The significance of evolving research on and implementation of interventions that are designed to modify behavioral contributions to disease processes is not limited to its enormous potential for disease control. It is also important as a means of advancing basic research on stress and other biobehavioral aspects of health and illness. Research in these areas is usually correlational or quasiexperimental, and this has imposed limits on how conclusive or applicable findings have been. To some extent, interventions offer the possibility of conducting ex-
perimental in addition to correlational studies of disease progression. Under normal circumstances, one has no control over who is exposed to stress, when exposure occurs, or who develops diseases or progresses more rapidly. As a result, most human studies of psychological or behavioral mediation of cancer course are essentially prospective or retrospective correlations between reported experiences and measures of disease outcomes. Interventions to reduce stress or alter other behavioral conditions or characteristics, when randomized and appropriately applied, constitute a manipulation that permits stronger evaluation of the contribution of stress to disease outcomes. Not surprisingly, evidence of psychosocial mediation of cancer course has been more convincing in studies of psychotherapeutic interventions than in natural history studies that rely on observed associations between psychological variables and disease outcomes (Garssen and Goodkin, 1999). Extending this effort will provide greater insight into disease etiology and progression as well as help to identify promising methods of intervention to reduce these pathophysiologic processes.
REFERENCES
Albright, G.L., Andreassi, J.L., and Brockwell, A.L. ( 1991). Effects of stress management on blood pressure and other cardiovascular variables. International Journal of Psychophysiology, 11 (2), 213–217.
Allen, M.T., and Patterson, S.M. ( 1995). Hemoconcentration and stress: A review of physiological mechanisms and relevance for cardiovascular disease risk. Biological Psychology, 31(1), 1–27.
Andersen, B.L. ( 1992). Psychological interventions for cancer patients to enhance the quality of life. Journal of Consulting and Clinical Psychology, 60(4), 552–568.
Andersen, B.L., Farrar, W.B., Golden-Kreutz, D., Kutz, L.A., MacCallum, R., Courtney, M.E. and Glaser, R. ( 1998). Stress and immune responses after surgical treatment for regional breast cancer. Journal of the National Cancer Institute, 90(1), 30–36.
Andersen, B.L., Kiecolt-Glaser, J.K., and Glaser, R. ( 1994). A biobehavioral model of cancer stress and disease course. American Psychologist, 49(5) 389–404.
Antoni, M.H., LaPerriere, A., Schneiderman, N., and Fletcher, M.A. ( 1991). Stress andimmunity in individuals at risk for AIDS. Stress Medicine, 7(1), 35–44.
Antoni, M.H., Esterling, B.A., Lutgendorf, S., Fletcher, M., Schneiderman, N. ( 1995). Psychosocial stressors, herpesvirus reactivation and HIV-1 infection . Stein, M., Baum, A., et al. (Eds). Chronic diseases. Perspectives in behavioral medicine (pp. 135–168). Mahwah, NJ, USA: Lawrence Erlbaum Assoc., Inc.
Barrick, C.B. ( 1999). Sad, glad, or mad hearts? Epidemiological evidence for a causal relationship between mood disorders and coronary artery disease. Journal of Affective Disorders, 53(2), 193–201.
Barnes, V., Schneider, R., Alexander, C., Staggers, F. ( 1997). Stress, stress reduction, and hypertension in African Americans: An updated review. Journal of the National Medical Association, 89(7) 464–476.
Baum, A and Andersen, B (eds) Psychosocial interventions for cancer. Washington DC: APA Books (in press).
Baum, A., Garofalo, J.P., and Yali, A.M. ( 1999). Socioeconomic status and chronic stress: Does stress account for SES effects on health? Annals of the New York Academy of Sciences, 896, 131–144.
Baum, A., and Grunberg, N.E. ( 1991). Gender, stress, and health. Health Psychology, 10(2), 80–85.
Baum, A., Herberman, H., and Cohen, L. ( 1995). Managing stress and managing illness: Survival and quality of life in chronic disease. Journal of Clinical Psychology in Medical Settings, 2(4), 309–333
Baum, A., and Nesselhof, S.E. ( 1988), Psychological research and the prevention, etiology, and treatment of AIDS. American Psychologist, 43(11), 900–906.
Baum, A. and Posluszny, D.M. ( 1999). Health Psychology: Mapping the biobehavioral contributions to health and illness. Annual Review of Psychology, 50, 137–163.
Baum, A. and Posluszny, D.M. (In press). Cancer and traumatic stress. In A.Baum and B.Andersen (Eds.). Psychosocial Interventions for Cancer. Washington, DC: APA Books.
Belcher, L., Kalichman, S., Topping, M., Smith, S., Emshoff, J., Norris, F., and Nurss, J. ( 1998). Randomized trail of a brief HIV risk reduction counseling intervention for women. Journal of Consulting and Clinical Psychology, 66(5), 856–861.
Ben-Eliyahu, S., Yirmiya, R., Liebeskind, J.C., Taylor, A.N., and Gale, R.P. ( 1991). Stress increases metastatic spread of a mammary tumor in rats: evidence for mediation by the immune system. Brain, Behavior, and Immunity, 5(2), 193–205.
Ben-Eliyahu, S., Page, G.G., Yirmiya, R., and Shakhar, G. ( 1999). Evidence that stress and surgical interventions promote tumor development by suppressing natural killer cell activity. International Journal of Cancer, 80(6), 880–888.
Bennett, P. ( 1994). Should we intervene to modify Type A behaviors in patients with manifest heart disease? Behavioral and Cognitive Psychotherapy, 22(2), 125–145.
Bennett, P., and Carroll, D. ( 1990a). Type A behaviors and heart disease: Epidemiological and experimental foundations. Behavioral Neurology, 3(4), 261–277.
Bennett, P., and Carroll, D. ( 1990b). Stress management approaches to the prevention of coronary heart disease. British Journal of Clinical Psychology. 29(1), 1–12.
Bennett, P., Wallace, L., Carroll, D., and Smith, N. ( 1991). Treating Type A behaviors and mild hypertension in middle-aged men . Journal of Psychosomatic Research 35(2–3), 209–223.
Benight, C.C., Antoni, M.H., Kilbourn, K., Ironson, G., Kumar, M.A., Fletcher, M.A., Redwine, L., and Baum, A. ( 1997). Coping self-efficacy buffers psychological and physiological disturbances in HIV-infected men following a natural disaster. Health Psychology, 16(3), 248–255.
Bennett, P. ( 1994). Should we intervene to modify Type A behaviors in patients with manifest heart disease? Behavioral and Cognitive Psychotherapy, 22(2), 125–145.
Blumenthal, J.A., Thyrum, E.T., and Siegel, W.C. ( 1995). Contribution of job strain, job status and marital status to laboratory and ambulatory blood pressure in patients with mild hypertension . Journal of Psychosomatic Research, 39(2), 133–144.
Bosley, F., and Allen, T.W. ( 1989) Stress Management training for hypertensives: Cognitive and physiological effects. Journal of Behavioral Medicine 12(1), 77–89.
Breslin, F.C., O'Keeffe, Burrell, L., Ratliff-Crain, J., and Baum, A. ( 1995). The effects of stress and coping on daily alcohol use in women. Addictive Behaviors, 20(2), 141–147.
Brezinka, V., and Kittel, F. ( 1996). Psychosocial factors of coronary heart disease in women: A review . Social Science and Medicine, 42(10), 1351–1365.
Broota, A., Varma, R., and Singh, A. ( 1995). Role of relaxation in hypertension. Journal of the Indian Academy of Applied Psychology, 21(1), 29–36.
Carney, R.M., Rich, M.W., and Jaffe, A.S. ( 1995). Depression as a risk factor for cardiac events in established coronary heart disease: A review of possible mechanisms. Annals of Behavioral Medicine, 17(2), 142–149.
Cella, D.F., and Tross, S. ( 1986). Psychological adjustment to survival from Hodgkin's disease. Journal of Consulting and Clinical Psychology, 54(5), 616–622.
Charles, K., Sellick, S.M., Montesanto, B., and Mohide, E.A. ( 1996). Priorities of cancer survivors regarding Psychosocial needs source . Journal of Psychosoical Oncology, 14(2), 57–72.
Coates, T.J., McKusick, L., Kuno, R., and Stites, D.P. ( 1989). Stress reduction for men with HIV. Advances, 6(3), 7–8.
Cohen, L., Delahanty, D., Schmitz, J.B., Jenkins, F.J., and Baum, A. ( 1993). The effects of stress on natural killer cell activity in healthy men. Journal of Applied Biobehavioral Research, 1(2), 120–132.
Cole, S.W., Kemeny, M.E., Taylor, S.E., Visscher, B.R., and Fahey, J.L. ( 1996). Accelerated course of human immunodeficiency virus infection in gay men who conceal their homosexual identity. Psychosomatic Medicine, 58(3), 219–231.
Cruess, D.G., Antoni, M.H., McGregor, M.S., Kilbourn, K.M., Boyers, A.E., Alferi, S.M., Carver, C.S., and Kumar, M. (In press). Cognitive Behavioral Stress Management Reduces Serum Cortisol by Enhancing Positive Contributions among Women Being Treated for Early-Stage Breast Cancer.
Davison, G.C., Williams, M.E., Nezami, E., Bice, Traci, L., et al. ( 1991). Relaxation, reduction in angry articulated thoughts, and improvements in borderline hypertension and heart rate. Journal of Behavioral Medicine, 14(5), 453–468.
De Brabander, B., and Gertis, P. ( 1999). Chronic and acute stress as predictors of relapse in primary breast cancer patients. Patient Education and Counseling, 37(3), 265–272.
Delahanty, D.L., Dougall, A.L., Craig, K.L., Jenkins, F.J., and Baum, A. ( 1997). Chronic stress and natural killer cell activity after exposure to traumatic death. Psychosomatic Medicine, 59(5), 467–476.
Dembroski, T.M., MacDougall, J.M., Costa, P.T., and Grandits, J.A. ( 1989). Components of hostility as predictors of sudden death and myocardial infarction in the Multiple Risk Factor Intervention Trail. Psychosomatic Medicine, 51, 514–522.
Dimsdale, J.E., Mills, P., Patterson, T., Ziegler, M., et al., ( 1994). Effects of chronic stress on beta-adrenergic receptors in the homeless . Psychosomatic Medicine 56(4), 290–295.
Dingle, G.A. and Oei, T.P. ( 1997). Is alcohol a cofactor of HIV and AIDS? Evidence from immunological and behavioral studies. Psychological Bulletin, 122(1), 56–71.
Dreher, H. ( 1997). The scientific and moral imperative for broad-based psychological interventions for cancer. Advances, 13(3), 38–49.
Dusseldorp, E., van Elderen, T., Maes, S., Meulman, J., and Kraaij, V. ( 1999). A metaanalysis of psychoeducational programs for coronary heart disease . Health Psychology, 18(5), 506–519.
Eaker, E.D., ( 1989). Psychosocial factors in the epidemiology of coronary heart disease in women. Psychiatric Clinics of North America, 12(1), 167–173.
Elliott, S.J. ( 1995). Psychosocial stress, women and heart health: A critical review. Social Science and Medicine, 40(1), 105–115.
Everson, S.A., Goldberg, D.E., Kaplan, G.A., Julkunen, J., and Salonen, J.T. ( 1998). Anger expression and incident hypertension. Psychosomatic Medicine, 60(6), 730–735.
Eysenck, H.J. ( 1990) Type A behavior and coronary heart disease: The third stage. Journal of Social Behavior and Personality, 5(1), 25–44
Ezzy, D., deVisser, R., and Bartos, M. ( 1999). Poverty, disease progression and employment among people living with HIV/AIDS in Australia. AIDS Care, 11(4), 405–414.
Fawzy, F.I. ( 1994). Immune effects of a short-term intervention for cancer patients. Advances, 10(4), 32–33.
Fawzy, F.I., Cousins, N., Fawzy, N.W., Kemeny, M.E., et al ( 1990). A structured psychiatric intervention for cancer patients: I. Changes over time in methods of coping and affective disturbance. Archives of General Psychiatry, 47(8), 720–725.
Fawzy, F.I., Kemeny, M.E., Fawzy, N.W., Elashoff, R., et al. ( 1990). A structured psychiatric intervention for cancer patients: II. Changes over time in immunological measures. Archives of General Psychiatry, 47(8), 729–735.
Fawzy, F.I., Fawzy, N.W., Hyun, C.S., Elashoff, R., Guthrie, D., Fahey, J.L., and Morton, D.L. ( 1993). Malignant melanoma: Effects of an early structured psychiatric intervention, coping, and affective state on recurrence and survival 6 years later . Archives of General Psychiatry, 50(9), 681–689.
Felten, D.L., and Felten, S.Y. ( 1991). Brain-immune signaling: Substrate for reciprocal immunological signaling of the nervous system. Frederickson, R.C., McGaugh, J.L., et al. (Eds). Peripheral signaling of the brain: Role in neural-immune interactions and learning and memory. Neuronal control of bodily function: Basic and clinical aspects, Vol 6 (pp 3–17). Lewiston, NY, USA: Hogrefe and Huber Publishers.
Fernandez-Cruz, E., Desco, M., Garcia Montes, M., Longo, N, et al. ( 1990). Immunological and serological markers predictive to progression to AIDS in a cohort of HIV-infected drug users. AIDS, 4(10), 987–994.
Fisher, J.D., Fisher, W.A., Misovich, S.J., Kimble, D.L., and Malloy, T.E. ( 1996). Changing AIDS risk behavior: Effects of an intervention emphasizing AIDS risk reduction information, motivation, and behavioral skills in a college student population. Health Psychology, 15(2), 114–123.
Fontana, A.F., Kerns, R.D., Rosenberg, R.L., and Colonese, K.L. ( 1989). Support, stress, and recovery from coronary heart disease: A longitudinal causal model. Health Psychology, 8(2), 175–193.
Ford, K., Wirawan, D.N., Fajans, P., Meliawan, P., et al. ( 1996). Behavioral interventions for reduction of sexually transmitted disease/HIV transmission among female commercial sex workers and clients in Bali, Indonesia. AIDS, 10(2), 213–22.
Foreyt, J.P., and Poston, W.S. ( 1996) Reducing risk for cardiovascular disease. Psychotherapy, 33(4), 576–586.
Freedland, K.E., Carney, R.M., Lustman, P.J., Rich, M.W., et al. ( 1992). Major depression in coronary artery disease patients with versus without a prior history of depression. Psychosomatic Medicine, 54(4), 416–421.
Freedman, R.R. ( 1987) Long term effectiveness of behavioral treatments for Raynaud's disease. Behavior Therapy, 18(4), 387–399.
Fredrikson, M., and Matthews, K.A. ( 1990). Cardiovascular responses to behavioral stress and hypertension: A meta-analytic review. Annals of Behavioral Medicine, 12(1), 30–39.
Frischenschlager, O., Broemmel, B., and Russinger, U. ( 1992). The effectivity of psychosocial care of cancer patients: A critical review of empirical studies. Psychotherapie Psychosomatik Medizinische Psychologie, 42(6), 206–213.
Gallois, P., Forzy, G., and Dhont, J.L. ( 1984). Hormonal changes induced by relaxation. Encephale, 10(2), 79–82.
Ganz, P.M., Hirji, K., Sim, M., Schag, C.A., et al. ( 1993). Predicting psychosocial risk in patients with breast cancer. Medical Care, 31(5), 419–431.
Garcia-Vera, M.P., Labrador, F.J., and Sanz, J. ( 1997). Stress-management training for essential hypertension: A controlled study. Applied Psychophysiology and Biofeedback, 22(4), 261–283.
Garcia-Vera, M.P., Labrador, F.J., and Sanz, J. ( 1998). Psychological changes accompanying and mediating stress-management training for essential hypertension. Applied Psychophysiology and Biofeedback, 23(3), 159–178.
Garssen, B., and Goodkin, K. ( 1999). On the role of immunological factors as mediators between psychosocial factors and cancer progression. Psychiatry Research, 85(1), 51–61.
Gerits, P., and De Brabander, B ( 1999). Psychosocial predictors of psychological, neurochemical and immunological symptoms of acute stress among breast cancer patients. Psychiatry Research, 85(1), 95–103.
Glanz, K., and Lerman, C. ( 1992). Psychosoical impact of breast cancer: a critical review. Annals of Behavioral Medicine, 14(3), 204–212.
Glaser, R., Kennedy, S., Lafuse, W.P., Bonneau, R.H., Speicher, C., Hillhouse, J., and Kiecolt-Glaser, J.K. ( 1990). Psychological stress-induced modulation of interleukin 2 receptor gene expression and interleukin 2 production in peripheral blood leukocytes. Archives of General Psychiatry, 47(8), 707–712.
Glaser, R., Thorn, B.E., Tarr, K.L., Kiecolt-Glaser, J.K., and D'Ambrosio, S.M. ( 1985). Effects of stress on methyltransferase synthesis: an important DNA repair enzyme. Health Psychology, 4(5), 403–412.
Goodkin, K., Fuchs, I., Feaster, D, Leeka, J., et al. ( 1992). Life stressors and coping style are associated with immune measures in HIV-1 infection: A preliminary report. International Journal of Psychiatry in Medicine, 22(2), 155–172.
Gritz, E.R. ( 1991). Smoking and smoking cessation in cancer patients. British Journal of Addiction, 86(5), 549–554.
Gruber, G.L., Hersch, S.P., Hall, N.R., Waletzky, L.R., Kunz, J.F., Carpenter, J.K., Kverno, K.S., and Weiss, S.M. ( 1993). Immunological responses of breast cancer patients to behavioral interventions . Biofeedback and Self-Regulation, 18(1), 1–22.
Gulick, R.M., ( 1998). HIV Treatment strategies: Planning for the long term. Journal of the American Medical Association, 279(12), 957–959.
Haaga, D.A., Davison, G.C., Williams, M.E., Dolezal, S.L., et al. ( 1994). Mode-specific impact of relaxation training for hypertensive men with Type A behavior pattern. Behavior Therapy, 25(2), 209–223.
Hall, N.R. ( 1988). The virology of AIDS. American Psychologist, 43(11), 907–913.
Hall, N.R.S., and O'Grady, M.P. ( 1991). Psychological interventions and immune function. Ader R., Felten, D.L., and Cohen N. (Eds): Psychoneuroimmunology, ed 2, (pp 1067–1080) New York, Academic Press.
Helgeson, V., and Cohen, S. ( 1996). Social support and adjustment to cancer: reconciling descriptive, correlational, and intervention research. Health Psychology, 15(2), 135–148.
Helgeson, V., Cohen, S., Schulz, R., and Yasko, J. ( 1999). Education and peer discussion group interventions and adjustment to breast cancer. Archives of General Psychiatry, 56(4), 340–347.
Helgeson, V.S., Cohen, S., Schulz, R., and Yasko, J. (In press). Group support interventions for people with cancer: Benefits and hazards. Baum, A., and Andersen B. (Eds). Psychosocial Intervention for Cancer. Washington, D.C. APA Books.
Helgeson, V.S., Cohen, S., Schulz, R, and Yasko, J. (In press). Group support interventions for women with cancer: Who benefits from what?
Herberman, R.B. ( 1991). Sources of confounding in immunologic data. Reviews of Infectious Diseases, 13, 84–86.
Hoelscher, T.J. ( 1987). Maintenance of relaxation-induced blood pressure reductions: The importance of continued relaxation practice. Biofeedback and Self Regulation, 12(1), 3–12.
Houston, B.K., Chesney, M.A., Black, G.W., Gates, D.S., et al. ( 1992). Behavioral clusters and coronary heart disease risk. Psychosomatic Medicine, 54(4), 447–461.
Ironson, G., Wynings, C., Schneiderman, N., Baum, A., Rodriguez, M., Greenwood, D., Benight, C., Antoni, M., LaPerriere, A., Hui-Sheng, H., Klimas, N., and Fletcher, M.A. ( 1997) Posttraumatic stress symptoms, intrusive thoughts, loss, and immune function after Hurricane Andrew. Psychosomatic Medicine, 59, 128–141.
Irvine, M.J., Johnston, D.W., Jenner, D.A., and Marie, G.V. ( 1986). Relaxation and stress management in the treatment of essential hypertension . Journal of Psychosomatic Research, 30(4), 437–450.
Irvin, M.J., and Logan, A.G., ( 1991). Relaxation behavior therapy as sole treatment for mild hypertension . Psychosomatic Medicine, 53(6), 587–597.
Ishihara, Y., Matsunaga, K., Iijima, H., Fujii, T., Oguchi, Y., and Kagawa, J. ( 1999). Time-dependent effects of stressor application on metastasis of tumor cells in the lung and its regulation by an immunomodulator in mice . Psychoneuroendocrinology, 24(7), 713–726.
Jacob, R.G., Thayer, J.F., Manuck, S.B., Muldoon, M.F., Tamres, L.K., Williams, D.M., Ding, Y., and Gatsonis, C. ( 1999). Ambulatory blood pressure responses and the circumplex model of mood: A 4-day study. Psychosomatic Medicine, 61(3), 319–333.
Jacob, R.G., Shapiro, A.P., O'Hara, P., Portser, S., et al. ( 1992). Relaxation therapy for Hypertension: Setting-specific effects. Psychosomatic Medicine, 54(1), 87–101.
Jacob, R.G., Wing, R.R., and Shapiro, A.P. ( 1987). The behavioral treatment of hypertension: Long term effects. Behavior Therapy, 18(4), 325–352.
Johnson, J.V., Hall, E.M., and Theorell, T. ( 1989). Combined effects of job strain and social isolation on cardiovascular disease morbidity and mortality in a random sample of the Swedish male working population. Scandinavian Journal of Work, Environment and Health, 15(4), 271–279.
Johnson, J.V., Stewart, W., Hall, E.M., Fredlunc, P., et al. ( 1996). Long term psychosocial work environment and cardiovascular mortality among Swedish men. American Journal of Public Health, 86(3), 324–331.
Johnston, M., Wakeling, A., Graham, N., and Stokes, F. ( 1987). Cognitive impairment, emotional disorder and length of stay of elderly patients in a district general hospital. British Journal of Medical Psychology, 60(2), 133–139.
Kamarck, T.W., and Jennings, J.R. ( 1991). Biobehavioral factors in sudden cardiac death. Psychological Bulletin, 109(1), 42–75.
Kaplan, G.A. ( 1992). Health and aging in the Alameda County Study. Schaie, K.W., Blazer, D.G., et al (Eds). Aging, health behaviors, and health outcomes. Social structure and aging, (pp 69–88). Hillsdale, NJ, USA: Lawrence Erlbaum Assoc., Inc.
Kaplan, J.R., Manuck, S.B., Clarkson, T.B., Lusso, P.M., and Taub, D.B. ( 1982). Social status, environment and atherosclerosis in cynomolgus monkeys . Arteriosclerosis, 2, 359–368.
Kaplan, J.R., Adams, M.R., Clarkson, T.B., Koritnick, D.R. ( 1984). Psychosocial influences on female “protection” among cynomolgus macaques. Atherosclerosis, 53, 283–295.
Kaplan, J.R., Adams, M.R., Clarkson, T.B., Manuck, S.B., Shively, C.A., and Williams, J.K. ( 1996). Psychological factors, sex differences, and atherosclerosis: Lessons from animal models. Psychosomatic Medicine, 58, 598–611.
Kasl, S.V. ( 1996). The influence of the work environment on cardiovascular health: A historical, conceptual, and methodological perspective. Journal of Occupational Health Psychology, 1(1), 42–56.
Kiecolt-Glaser, J.K., Stephens, R.E., Lipetz, P.D., Speicher, C.E., and Glaser, R. ( 1985). Distress and DNA repair in human lymphocytes. Journal of Behavioral Medicine, 8(4), 311–320.
Keller, M., Henrich, G., Sellschopp, A., and Beutel, M. ( 1996). Between distress and support: Spouses of cancer patients. Baider, L., Cooper, C.L., et al (Eds). Cancer and the family (pp 187–223). Chichester, England UK: John Wiley and Sons.
Kelly, J.A. ( 1998). Group psychotherapy for persons with HIV and AIDS-related illnesses . International Journal of Group Psychotherapy, 48(2), 143–162.
Kemeny, M.E. ( 1994). Psychoneuroimmunology of HIV infection. Psychiatric Clinics of North America, 71(1), 55–68.
Kemeny, M.E., Weiner, H., Duran, R., Taylor, S.E., et al. ( 1995). Immune system changes after the death of a partner in HIV-positive gay men. Psychosomatic Medicine, 57(6), 547–554.
Kerr, L.R., Wilkinson, D.A., Emerman, J.T., and Weinberg, J. ( 1999). Interactive effects of psychosocial stressors and gender on mouse mammary tumor growth. Physiology and Behavior, 66(2), 277–281.
Kiecolt-Glaser, J.K., and Glaser, R. ( 1992). Psychoneuroimmunology: can psychological interventions modulate immunity? Journal of Consulting and Clinical Psychology, 60(4), 569–575.
King, M., Speck, P., Thomas, A. ( 1999). The effect of spiritual beliefs on outcome from illness. Social Science and Medicine, 48(9), 1291–1299.
Knox, S.S., and Uvnaes-Moberg, K. ( 1998). Social isolation and cardiovascular disease: An atherosclerotic pathway? Psychoneuroendocrinology, 23(8), 877–890.
Kop, WJ. ( 1999). Chronic and acute psychological risk factors for clinical manifestations of coronary artery disease. Psychosomatic Medicine, 61(4), 476–487.
Krantz, D.S., Contrada, R.J., Hill, D.R., and Friedler, E. ( 1988). Environmental stress and biobehavioral antecedents of coronary heart disease. Journal of Consulting and Clinical Psychology, 56(3), 333–341.
Krantz, D.S., Grunberg, N.E, and Baum, A. ( 1985). Health psychology. In: Annual review of psychology. Vol. 36. Palo Alto, CA: Annual Reviews, Inc. (p. 349–383).
Krantz, D.S., Kop, W.J., Antiago, H.T., and Gottdiener, J.S. ( 1996). Mental stress as a trigger of myocardial ischemia and infarction. Cardiology Clinics, 14(2), 271–287.
Krantz, D.S., Schneiderman, N., Chesney, M.A., McCann, B.S., et al. ( 1989). Biobehavioral research on cardiovascular disorders. Health Psychology, 8(6), 737–746.
Kringlen, E. ( 1986). Psychosocial aspects of coronary heart disease. Acta PsychiatricaScandinavica, 74(3), 225–237.
Kubzansky, L.D., Kawachi, I., Weiss, S.T., and Sparrow, D. ( 1998). Anxiety and coronary heart disease: A synthesis of epidemiological, psychological, and experimental evidence. Annals of Behavioral Medicine, 20(2), 47–58.
LaPerriere, A., Schneiderman, N., Antoni, M.H., and Fletcher, M.A. ( 1990). Aerobic exercise training and psychoneuroimmunology in AIDS research . Temoshok, L, Baum, A., et al (Eds). Psychosocial perspectives on AIDS: Etiology, prevention, and treatment, (pp. 259–286). Hillsdale, NJ, USA: Lawrence Erlbaum Associates, Inc.
Lazarus, R.S. and S. Folkman. ( 1984). Stress, appraisal, and coping. Springer. New York
Lekander, M., Furst, C.J., Rotstein, S., Hursti, T.J., and Fredrikson, M. ( 1997). Immune effects of relaxation during chemotherapy for ovarian cancer . Psychotherapy and Psychosomatics, 66, 185–191.
Leventhal, H. ( 1980). Toward a comprehensive theory of emotion. Berkowitz, L. (Ed): Advances in Experimental Social Psychology (pp 140–208). Academic Press.
Levy, S.M. ( 1991). Behavioral and immunological host factors in cancer risk. McCabe, P.M., and Schneiderman, N., et al (Eds). Stress, coping, and disease. Stress and coping. Hillsdale, NJ, USA. Lawrence Erlbaum Associates, Inc.
Levy, S.M., Cottrell, M.C., and Black, P.H. ( 1990). Psychological and immunological associations in men with AIDS pursuing a macrobiotic regimen as an alternative therapy: A pilot study. Brain, Behavior and Immunity, 3(2), 175–182.
Levy, S.M., Herberman, R.B., Maluish, A.M., Schlien, V., and Lippman, M. ( 1985). Prognostic risk assessment in primary breast cancer by behavioral and immunological parameters. Health Psychology, 4(2), 99–113.
Levy, S.M. ( 1990). Psychosocial risk factors and cancer progression: Mediating pathways linking behavior and disease. Craig, K.D., Weiss, S.M., et al (Eds). Health enhancement, disease prevention, and early intervention: Biobehavioral perspectives (pp. 348–369). New York, NY, USA: Springer Publishing Co., Inc.
Levy, S.M., and Wise, B.D. ( 1989). Psychosocial risk factors, natural immunity, and cancer progression: Implications for intervention. Johnston, M., and Marteau, T., et al. (Eds). Applications in health psychology (pp. 141–155). New Brunswick, NJ, USA: Transaction Publishers.
Lorig, K.R., Sobel, D.S., Stewart, A.L., Brown, B.W., Bandura, A., Ritter, P., Gonzalez, V.M., Laurent, D.D., and Holman, H.R. ( 1999). Evidence suggesting that a chronic disease self-management program can improve health status while reducing hospitalization. Medical Care, 37(1), 5–14.
Lovibond, S.H., Birrell, P.C., and Langeluddecke, P. ( 1986). Changing coronary heart disease risk-factor status: The effects of three behavioral programs. Journal of Behavioral Medicine 9(5), 415–437.
Lutgendorf, S., Antoni, M.H., Schneiderman, N., Ironson, G., Fletcher, M.A. ( 1995). Psychosocial interventions and quality of life changes across the HIV spectrum. Dimsdale, J.E., and Baum, A. (Eds). Quality of life in behavioral medicine research. Perspectives in behavioral medicine (pp. 205–239). Hillsdale, NJ, USA: Lawrence Erlbaum Associates, Inc.
Lyketsos, C.G., Hoover, D.R., and Guccione, M. ( 1996). Depression and survival among HIV-infected persons. Journal of the American Medical Association, 275(1), 35–36.
Mann, A.H. ( 1984). Hypertension: Psychological aspects and diagnostic impact in a clinical trial. Psychological Medicine, Mono Suppl 5, 35.
Manuck, S.B., Kaplan, J.R., and Clarkson, T.B. ( 1983). Social instability and coronary artery atherosclerosis in cynomolgus monkeys. Neuroscience and Biobehavioral Reviews, 74(4), 485–491.
Manuck, S.B., and Krantz, D.S. ( 1984). Psychophysiologic reactivity in coronary heart disease. Behavioral Medicine Update, 6(3), 11–15.
Manuck, S.B., Adams, M.R., McCaffery, J.M., and Kaplan, J.R. ( 1997) Behaviorally elicited heart rate reactivity and atherosclerosis in ovariectomized cynomolgus monkeys (Macaca fasciculairs). American Heart Association, Inc.
Manuck, S.B., Kaplan, J.R., and Matthews, K.A. ( 1986). Behavioral antecedents of coronary heart disease and atherosclerosis . Arteriosclerosis, 6, 2–14
Markovitz, J.H. and Matthews, K.A. ( 1991). Platelets and coronary heart disease: Potential psychophysiologic mechanisms. Psychosomatic Medicine, 53(6), 643–668.
Marmot, M. ( 1994). Work and other factors influencing coronary health and sickness absence . Work and Stress, 8(2), 191–201.
Mason, J.W., ( 1975). A historical view of the stress field. Journal of Human Stress, 1, 22–36.
Matarazzo, J.D. ( 1980). Behavioral health and behavioral medicine: Frontiers for a new health psychology. American Psychologist, 35(9), 807–817.
Matthews, K.A., and Haynes, S.G. ( 1986). Type A behavior patterns and coronary disease risk: Update and critical evaluation. American Journal of Epidemiology, 123(6), 923–960.
McCubbin, J.A., Wilson, J.F., Bruehl, S., Ibarra, P., et al. ( 1996). Relaxation training and opioid inhibition of blood pressure response to stress. Journal of Consulting and Clinical Psychology, 64(3), 593–601.
McGrady, A., Conran, P., Dickey, D., Garman, D., Farris, E., and Schumann-Brezezinski, C. ( 1992). The effects of biofeedback-assisted relaxation on cellmediated immunity, cortisol, and white blood cell count in healthy adult subjects. Journal of Behavioral Medicine, 15, 343–354.
McGrady, A.V., Woerner, M., Bernal, G.A., and Higgins, J.T. ( 1987). Effect of biofeedback-assisted relaxation on blood pressure and cortisol levels in normotensives and hypertensives. Journal of Behavioral Medicine, 10(3), 301–310.
McGrady, A., Turner, J.W., Fine, T.H., and Higgins, J.T. ( 1987). Effects of biobehaviorally-assisted relaxation training on blood pressure, plasma renin, cortisol, and aldosterone levels in borderline hypertension. Clinical Biofeedback and Health: An International Journal, 10(1), 16–25.
McKenna, M.C., Zevon, M.A., Corn, B., and Rounds, J. ( 1999). Psychosocial factors and the development of breast cancer: A meta-analysis . Health Psychology, 18(5), 520– 531.
McKinnon, W., Weisse, C.S., Reynolds, C.P., Bowles, C.A. and Baum, A. ( 1989). Chronic stress, leukocyte subpopulations, and humoral response to latent viruses. Health Psychology, 8(4), 389–402.
McNulty, S., Jefferys, D., Singer, G., and Singer, L. ( 1984). Use of hormone analysis in the assessment of the efficacy of stress management training in police recruits. Journal of Police Science and Administration, 12(2), 130–132.
Mellors, V., Boyle, G.J., and Roberts L. ( 1994). Effects of personality, stress and life-style on hypertension: An Australian twin study. Personality and Individual Differences, 16(6), 967–974.
Meyer, T.J., Mark, M.M., ( 1995). Effects of psychological interventions with adult cancer patients: A meta-analysis of randomized experiments. Health Psychology, 14(2),101–108.
Miller, G.E., Kemeny, M.E., Taylor, S.E., Cole, S.W., and Visscher, B.R. ( 1997). Social relationships and immune processes in HIV seropositive gay and bisexual men. Annals of Behavioral Medicine, 19(2), 139–151.
Miller, S.M., Mischel, W., O'Leary, A., and Mills, M. ( 1996). From human papilloma virus (HPV) to cervical cancer: Psychosocial processes in infection, detection, and control. Annals of Behavioral Medicine, 18(4), 219–228.
Moyer, A., and Salovey, P. ( 1996). Psychosocial sequelae of breast cancer and its treatment. Annals of Behavioral Medicine, 18(2), 110–125.
Mulder, C.L., deVroome, E.M., van Griensven, G.J., Antoni, M.H., and Sandfort, T.G. ( 1999). Avoidance as a predictor of the biological course of HIV infection over a 7-year period in gay men. Health Psychology, 18(2), 107–113.
Munoz, A., Wang, M.C., Bass, S., Taylor, J.M., Kingsley, L.A., Chmiel, J.S., and Polk, B.F. ( 1989). Acquired immunodeficiency syndrome (AIDS)-free time after human immunodeficiency virus type 1 (HIV-1) seroconversion in homosexual men. Multicenter AIDS Cohort Study Group. American Journal of Epidemiology, 130(3), 530–539.
Musselman, D.L., Evans, D.L., and Nemeroff, Charles B. ( 1998). The relationship of depression to cardiovascular disease: epidemiology, biology, and treatment. Archives of General Psychiatry, 55(7), 580–592.
Naeslund, G.K., Fredrikson, M., and Holm, L. ( 1993). Psychosocial factors associated with participation and nonparticipation in a diet intervention program. Journal of Psychosocial Oncology, 19(4), 93–107.
Niaura, R., and Goldstein, M.G. ( 1992). Psychological factors affecting physical condition: Cardiovascular disease literature review: II. Coronary artery disease and sudden death and hypertension. Psychosomatics 33(2), 146–155.
Nunes, E.V., Frank, K.A., and Kornfeld, D.S. ( 1987). Psychologic treatment for the TypeA behavior pattern and for coronary heart disease: A meta-analysis of the literature. Psychosomatic Medicine, 49(2), 159–173.
O'Leary, A. ( 1990). Stress, emotion, and human immune function. Psychological Bulletin, 108, 363–382.
Orth-Gomer, K., and Unden, A. ( 1990). Type A behavior, social support, and coronary risk: Interaction and significance for mortality in cardiac patients. Psychosomatic Medicine, 52(1), 59–72.
Ostrow, D.G. ( 1996). The search for the elusive psychosocial modulators of human immunodeficiency virus disease progression. Psychosomatic Medicine, 58(3), 232–233.
Pennebaker, J.W., Hughes, C.F., and O'Heeron, R.C. ( 1987). The psychophysiology of confession: Linking inhibitory and psychosomatic processes. Journal of Personality and Social Psychology, 52(4), 781–793.
Perry, S.W., Fishman, B., Jacobsberg, L., Frances, A.J. ( 1992) Relationships over 1 year between lymphocyte subsets and psychosocial variables among adults with infection by human immunodeficiency virus . Archives of General Psychiatry, 49(5), 396–401.
Peter, R., and Siegrist, J. ( 1997). Chronic work stress, sickness absence and hypertension in middle managers: General or specific sociological explanations? Social Scienceand Medicine, 45(7), 1111–1120.
Petticrew, M., Fraser, J.M. and Regan, M.F. ( 1999). Adverse life-events and risk of breast cancer: A meta-analysis. British Journal of Health Psychology, 4(1), 1–17.
Phair, J.P., Farzadegan, H., Chmiel, J., Munoz, A., Detels, R., Saah, A. and Kaslow, R. Progression of HIV-infection: markers or determinants. Transactions of the American Clinical and Climatoloigcal Association, 104, 123–128, discussion 129–129.
Pickering, T.G., and Gerin, W. ( 1990). Cardiovascular reactivity in the laboratory and the role of behavioral factors in hypertension: A critical review. Annals of Behavioral Medicine, 12(1), 3–16.
Pomeroy, E.C., Rubin, A., Van Laningham, L., and Walker, R.J. ( 1997). “Straight talk”: The effectiveness of a psychoeducational group intervention for heterosexuals with HIV/AIDS. Research on Social Work Practice, 7(2), 149–164.
Rabkin, J.G., Williams, J.B., Remien, R.H., Goetz, R., et al. ( 1991). Depression, distress, lymphocyte subsets, and human immunodeficiency virus symptoms on two occasions in HIV-positive homosexual men. Achieves of General Psychiatry, 48(2), 111–119.
Ramirez, A.J., Craig, T.K., Watson, J.P., Fentiman, I.S., North, W.R., and Rubens, R.D. ( 1989). Stress and the relapse of breast cancer. British Medical Journal, 298, 291–293.
Reed, G.M., Kemeny, M.E., Taylor, S.E., Wang, H.J., et al. ( 1994). Realistic acceptance as a predictor of decreased survival time in gay men with AIDS. Health Psychology, 13(4), 299–307.
Redd, W.H. ( 1997). Behavioral intervention in cancer treatment. Baer, D.M., Elsie, M., et al. (Eds). Environment and behavior (Pp. 155–162). Boulder, CO, USA: Westview Press.
Remien, R.H., Rabkin, J.G., Williams, J.B., and Katoff, L. ( 1992). Coping strategies and health beliefs of AIDS longterm surivors. Psychology and Health, 6(4), 335–345.
Richardson, J.L., Zarnegar, Z., Bisno, B., and Levine, A. ( 1990). Psychosocial status atinitiation of cancer treatment and survival . Journal of Psychosomatic Research, 34(2), 189–201.
Rosenman, R.H. ( 1991). Type A behavior pattern and coronary heart disease: The hostility factor? Stress Medicine, 7(4), 245–253.
Schedlowski, M., Jacobs, R., Alker, J., Proehl, F., et al. ( 1993). Psychophysiological, neuroendocrine and cellular immune reactions under psychological stress. Neuro-psychobiology, 28(1–2), 87–90.
Schulz, R., Williamson, G.M., Knapp, J.E., Bookwala, J., et al. ( 1995). The psychological, social, and economic impact of illness among patients with recurrent cancer. Journal of Psychosocial Oncology, 13(3), 21–45.
Schlebusch, L., and Cassidy, M.J. ( 1995). Stress, social support and biopsychosocial dynamics in HIV-AIDS. South African Journal of Psychology, 25(1), 27–30.
Schneiderman, N., ( 1983). Animal Behavior Models of Coronary Heart Disease. Krantz, D.S., Baum, A., and Singer, J.E. (Eds) Handbook of Psychology and Health Vol. III Cardiovascular Disorders and Behavior, (pp. 19–56). Hillsdale, N.J.: Lawrence Erlbaum Assoc., Inc
Schneiderman, N., Antoni, M.H., Ironson, G., LaPeriere, A., et al. ( 1992). Applied psychological science and HIV-1 spectrum disease. Applied and Preventive Psychology, 1(2), 67–82.
Shapiro, A.P. ( 1983). Krantz, D.S., Baum, A., Singer, J.E. (Eds) The Non-Pharmacologic Treatment of Hypertension. Handbook of Psychology and Health Vol. III Cardiovascular Disorders and Behavior, (pp 277–294). Hillsdale, N.J.: Lawrence Erlbaum Assoc., Inc.
Shedlowski, M., Jung, C., Shimanski, G., Tewes, V., and Schmoll, H.J. ( 1994). Effects of behavioral intervention on plasma cortisol and lymphocytes in breast cancer patients: an exploratory study. Psycho Oncology, 3, 181–187.
Shekelle, R.B., Vernon, S.W., Ostfeld, A.M. ( 1991). Personality and coronary heart disease. Psychosomatic Medicine 53(2), 176–184.
Siegel, K., Karus, D., Epstein, J., and Raveis, V.H. ( 1996). Psychological and psychosocial adjustment of HIV-infected gay/bisexual men: Diseases stage comparisons. Journal of Community Psychology, 24(3), 229–243.
Sikkema, K.J., Kalichman, S.C., Kelly, J.A., and Koob, J.J. ( 1995). Group intervention to improve coping with AIDS-related bereavement: model development and an illustrative clinical example. AIDS Care, 7(4), 463–475.
Skantze, H.B., Kaplan, J., Pettersson, K., Manuck, S., Blomqvist, N., Kyes, R., Williams, K., and Bondjers, G. ( 1998). Psychosocial stress causes endothelial injury in cynomolgus monkeys via • beta-adrenoceptor activation. Atherosclerosis, 136, 153–161.
Sklar, L.S., and Anisman, H. ( 1981). Stress and Cancer. Psychological Bulletin, 89(3), 369–406.
Sobel, D.S. ( 1995). Rethinking medicine: Improving health outcomes with cost-effective psychosocial interventions. Psychosomatic Medicine, 57(3), 234–244.
Solomon, G.F., ( 1987). Psychoneuroimmunologic approaches to research on AIDS. Annals of the New York Academy of Sciences, 496, 628–636.
Solomon, G.F., Kemeny, M.E., and Temoshok, L. ( 1991). Psychoneuroimmunologic aspects of human immunodeficiency virus infection . Ader, R., Felten, D.L. et al (Eds). Psychoneuroimmunology (2nd Ed) (pp. 1081–1113). San Diego, CA, USA: Academic Press, Inc.
Suarez, E.W., and Williams, R.B. ( 1990). The relationships between dimensions of hostility and cardiovascular reactivity as a function of task characteristics. Psychosomatic Medicine, 52(5), 558–570.
Smith, T.W., and Gallo, L.C. ( 1994). Psychosocial influences on coronary heart disease. Irish Journal of Psychology, 15(1), 2–26.
Spiegel, D. ( 1995) Psychosocial influences on cancer survival. Stein, M., and Baum, A. (Eds). Chronic diseases. Perspectives in behavioral medicine (pp 223–223). Mahwah, NJ, USA: Lawrence Erlbaum Associates, Inc.
Spiegel, D. ( 1996). Cancer and depression. British Journal of Psychiatry—Supplement, 30, 109–116.
Spiegel, D., Bloom, J.R., Kraemer, H.C., and Gottheil E. ( 1989). Effect of psychosocial treatment on survival of patients with metastatic breast cancer. Lancet, 2(8668), 888–891.
Spiegel, D., and Kato, P.M. ( 1996). Psychosocial influences on cancer incidence and progression. Harvard Review of Psychiatry 4(1), 10–26.
Spiegel, D., Sephton, S.E., and Sites, D.P. ( 1998). Effects of psychosocial treatment in prolonging cancer survival may be mediated by neuroimmune pathways. McCann, S.M., and Lipton, J.M. (Eds) Annals of the New York Academy of Sciences, Vol. 840: Neuroimmunomodualtion: Molecular aspects, integrative systems, and clinical advances. Annals of the New York Academy of Sciences, Vol. 840. (pp 674–683). New York, NY USA: New York Academy of Sciences.
Steptoe, A.( 1989). Psychophysiological interventions in behavioral medicine. Turpin, G. (Ed.). Handbook of Clinical Psychophysiology. Chi Chester: John Wiley.
Steptoe, A., Patel, C., Marmot, M., and Hunt, B. ( 1987). Frequency of relaxation practice, blood pressure reduciton and the general effects of relaxation following a controlled trial of behavior modification for reducing coronary risk. Stress Medicine, 3(2), 101–107.
Suminski, R.R., Anding, J., Smith, D.W., Zhang, J.J., Utter, A.C., and Kang, J. ( 1999). Risk and reality: The association between cardiovascular disease risk factor knowledge and selected risk-reducing behaviors. Family and Community Health 21(4), 51–62.
Tejwani, G.A., Gudehithlu, K.P., Hanissian, S.H., Gienapp, I.E., Whitacre, C.C., and Malarkey, W.B. ( 1991). Facilitation of dimethylbenz [a] anthracene-induced rat mammary tumorigenesis by restraint stress: role of beta-endorphin, prolactin and naltrexone . Carcinogenesis, 12(4), 637–641.
Theorell, T., and Karasek, R.A. ( 1996). Current issues relating to psychosocial job strain and cardiovascular disease research. Journal of Occupational Health Psychology 1(1), 9–26.
Tomei, L.D., Kiecolt-Glaser, J.K., Kennedy, S., and Glaser, R. ( 1990). Psychological stress and phorbol ester inhibition of radiation-induced apoptosis in human peripheral blood leukocytes. Psychiatry Resource, 33, 59–71.
Turk, D.C., Meichenbau, D., and Genest, M.(Eds) ( 1983). Pain and Behavioral Medicine A Cognitive-Behavioral Perspective. New York: The Guilford Press.
Uchino, B.N., Cacioppo, J.T., and Keicolt-Glaser, J.K. ( 1996). The relationship between social support and physiological processes: A review with emphasis on underlying mechanisms and implications for health. Psychological Bulletin, 119(3), 488–531.
Van der Pompe, G, Antoni, M., Visser, A., and Garssen, B. ( 1996). Adjustment to breast cancer: The psychobiological effects of psychosocial interventions. Patient Education and Counseling, 28(2), 209–219.
Van der Pompe, G., Antoni, M.H., and Heijnen, C.J. ( 1996). Elevated basal cortisol levels and attenuated ACTH and cortisol responses to a behavioral challenge in women with metastatic breast cancer . Psychoneuroendocrinology, 21(4), 361–374.
Van der Pompe, G., Antoni, M.H., and Heijnen, C.J. ( 1998). The effects of surgical stress and psychological stress on the immune function of operative cancer patients. Psychology and Health, 13(6), 1015–1026.
Van der Pompe, G., Antoni, M.H., Visser, A., and Heijnen, C.J.( 1998). Effect of mild acute stress on immune cell distribution and natural killer cell activity in breast cancer patients. Biological Psychology, 48(1), 21–36.
Vaughn, S.M., and Kinnier, R.T. ( 1996). Psychological effects of a life review intervention for persons with HIV disease. Journal of Counseling and Development, 75(2), 115–123.
Weidner, G., Boughal, T., Connor, S.L., Pieper, C., et al., ( 1997). Relationship of job strain to standard coronary risk factors and psychological characteristics in women and men of the Family Heart Study. Health Psychology, 16(3), 239–247.
Wellisch, D.K., Wolcott, D.L. Pasnau, R.O., Fawzy, F., et al., ( 1989). An evaluation of the psychosocial problems of the homebound cancer patient: Relationship of patient adjustment to family problems. Journal of Psychosocial Oncology, 71, 55–76.
Wingard, J.R., Curbow, B., Baker, F., Zabora, J., and Piantadosi, S. ( 1992). Sexual satisfaction in survivors of bone marrow transplantation. Bone Marrow Transplantation, 9(3), 185–190.
Yellen, S.B., Cella, D.F., and Bonomi, A. ( 1993). Quality of life in people with Hodgkin's disease. Oncology (Huntington), 7(8), 41–45.







































