|
BOX 3.1 Amelia and her family live in a suburb of Chicago.1 She is 60 and has been married for 35 years. Amelia has worked at part-time jobs in retail stores most of her life while caring for her children and now her grandchildren. Her husband Bob worked in a tire company all of his life, where he made foreman before retiring at 65. His company had provided health insurance coverage for him and the family throughout his life, and Bob had always expected they would still be providing coverage for him when he retired. Unfortunately, however, about 10 years ago the company realized that it could no longer afford to provide health insurance to retirees and their families. The business had just gotten too competitive and costs had to be cut somewhere. It was a real shock when Bob and Amelia realized that, while Bob would automatically go on Medicare, Amelia would be without any kind of coverage until she turned 65. In addition, when they found out the gaps in Medicare coverage, they realized they would have to get an insurance supplement for Bob, who has a history of heart problems. Amelia, too, has a health problem—she has suffered from situational depression for more than a year, since their eldest son was killed in a car crash. Otherwise she has been healthy. While they were not worried much about the depression, which was under control with treatment, they also knew that anything could happen at Amelia’s age. When Amelia applied independently for insurance, several companies rejected her, offered limited benefits that would exclude the mental health treatments and drugs she needs, or increased the premium. Amelia was able to get an offer of private insurance. However her health history meant that the price was high relative to their limited income, especially in combination with the $180 a month Bob was paying for a Medicare supplement with prescription coverage. Bob and Amelia spend a lot of time at the kitchen table with the calculator, trying to figure out whether they should spend some of their retirement savings to purchase coverage for Amelia at $400 a month or whether that would jeopardize their future income too seriously. On top of the premium, insurance for Amelia would require her to pay an annual deductible of up to $500 and a $20 copayment for each office visit. It is not an easy choice to make.2 An opportunity for Amelia to “buy-in” to Medicare would probably be a better deal, but it remains an idea whose time has not yet come. |
3
Insurance Transitions over the Family Life Cycle
The Committee noted in its first report, Coverage Matters, that U.S. insurance arrangements function like a sieve, with many holes through which individuals and whole families may slip. This chapter focuses on the transitions in a family’s life cycle where this slippage is most likely to occur (see Box 3.2).
Many of these transitions and their insurance consequences could affect anyone and some are essentially unavoidable. These transition points, which sometimes threaten continuous insurance coverage, represent targets of opportunity for policy action. Some of the transitions indicate where families bump up against the rules of coverage set by private insurers and public programs.
In this chapter, three kinds of transitions are particularly relevant:
-
Age: As individuals within families age, their health insurance status may change because of rules in public programs and private plans.
-
Employment status: How and where family members are employed may affect the family’s insurance status.
-
Marital status: Family issues relating to marriage, divorce, widowhood, single parenting, cohabiting, and separating may affect coverage.
There is considerable overlap among these three types of changes in status when one considers how each may influence coverage. For example, a child may reach age 19, get a job, and get married all around the same time. Decisions for each change may be interrelated and each can have insurance implications. In the following pages, each kind of transition is described and their interactions are discussed.
|
BOX 3.2 How Family Members Gain, Maintain, and Lose Coverage Transitions related to the age, employment, and marital status of family members may influence the chances to gain or maintain health insurance coverage for themselves and for their whole family. Some of the transitions expand opportunities for coverage, while others narrow the options or even lead to the loss of coverage. Below is an overview of the transitions discussed in this chapter. How Family Members Gain or Maintain Coverage Age
Employment
Marital Status
How Family Members Lose Coverage Age
Employment
|
Marital Status
|
The dynamic processes that create transitions mean that some individuals move back and forth between having and not having health insurance. Table 3.1 shows how these transitions relate to the social characteristics of individuals and to who has health insurance for all of the year, who has no health insurance for the entire year, and who has health insurance for at least one month during the calendar year. For example, widowed or divorced individuals are almost twice as likely to have been uninsured for the previous year (18.2 percent) as are people who were married all year (9.8 percent). Similarly, those with a family income below 100 percent of the federal poverty level (FPL) are twice as likely to be uninsured during part of the year (20.3 percent) as are those with incomes above 200 percent FPL (9.9 percent). When these individuals are grouped into families and considered as a unit, the number of people affected by the experience of uninsurance within the family is enlarged and the points of transition can come more frequently.
Comparing “uninsured” with “insured” at a given point in time overlooks the fact that many families may have members uninsured for short or long periods that cannot be detected simply by knowing their current insurance status.1 A lack of continuity in health insurance coverage can adversely affect access and health outcomes (IOM, 2001; 2002a).
Gaps in health care coverage are more common for lower-income families than for wealthier families. On average, those under age 65 with coverage through public programs are more likely to be uninsured at some time during the year than
TABLE 3.1 Transitional Points and Health Insurance Status of the Population Under Age 65, 1996
are those with private health coverage (19 percent and 7 percent, respectively) (Monheit et al., 2001b). Only 75 percent of those with public coverage maintain it for the full year compared to 92 percent of those with private coverage (Monheit et al., 2001b). African-American males are somewhat more likely to retain public coverage for the full year than are Hispanic males, and the uninsured rate for the whole year is higher for Hispanics than for other ethnic groups. For some families, the annual or more frequent recertification process for Medicaid and the State Children’s Health Insurance Program (SCHIP) may pose a barrier to maintaining coverage. For some immigrant families, public coverage is not an option.
The remainder of this chapter focuses on the age, employment, and marital transitions that affect the insurance status of individuals and the gaps in coverage they experience.
AGE ISSUES AFFECTING INSURANCE PATTERNS WITHIN FAMILIES
Finding: The structure of public health insurance programs and the cutoff age for dependents’ eligibility in private insurance plans make it more likely that children will become uninsured as they grow up.
The probability that a person will be without health insurance varies with age and the type of family in which he or she lives. From the consumer’s perspective, the most important age for insurance purposes is 65, the point at which almost everyone qualifies for and is enrolled in Medicare. Through this federal program, basic coverage is ensured for the rest of the person’s life and is not directly influenced by any of the age, employment, marital status, or health-related transitions that can affect coverage for younger individuals. However, for families with at least one member younger than age 65, aging may cause the loss of coverage. A family member’s transitions can precipitate not only his or her own but also other family members’ loss of coverage
Children and Public Programs
Families with Medicaid or SCHIP coverage for their children may face tightened income eligibility limits as their children get older (see Appendix B). Thus, within a family, only younger children may be covered. Depending on how close a family’s income is to the limit, an infant could lose Medicaid coverage when he or she reaches a first birthday. For example, in Florida the infant would be covered with a family income up to 185 percent FPL, children between the ages of 1 and 6 are covered if family income is less than 133 percent FPL, and children between ages 6 and 18 are covered if family income is not over 100 percent FPL. Figure 3.1 shows that the likelihood of having public insurance gradually decreases for children through age 17 (see Appendix C, Table C.2). There is a drop of almost 6 percentage points in public coverage of young adults aged 18–20, but the almost
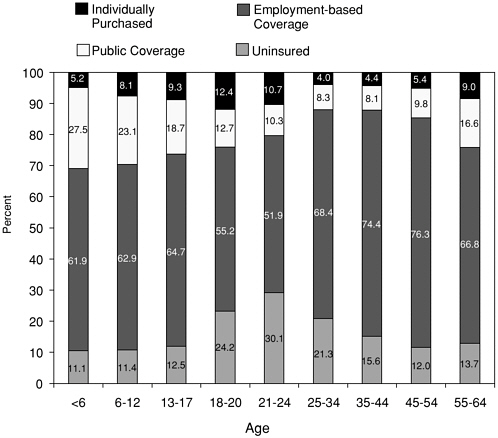
FIGURE 3.1 Health insurance status, by age
NOTE: Percentages may not total 100 percent because individuals may receive coverage from more than one source.
SOURCE: Fronstin, 2001.
12 percentage-point increase in their uninsured rate results from a larger drop-off (more than 9 percentage points) in private coverage, too.
For Medicaid, eligibility based solely on family income usually ends at age 19, although states have the option to cover youth through age 21. Within their SCHIPs, most states also cover youth through their nineteenth birthdays. Generally, for people beyond their nineteenth birthday, Medicaid requires more than just a low income to qualify. Most commonly, low-income people above age 18 who are disabled or who are pregnant are able to maintain or gain Medicaid eligibility.
Dependency Coverage Ends
The age at which young people often leave home (18–24) coincides with the age at which the risk of traumatic injury is the highest and the risk of being without health insurance is the greatest (see Figure 3.1). Among those aged 13 to 17, most of whom are still part of their parents’ households, 12.5 percent are without health insurance. In the next older group, those ages 18 to 20, the risk of being without health insurance almost doubles, to 24.2 percent. The uninsured rate jumps to more than 30 percent for people aged 21–24, the highest rate observed for any age group.
The large increase in young people losing coverage beginning at age 19 is a result of how both private insurers and public programs define eligible family members. The rules for private insurance vary somewhat. Workers who elect family coverage from their employer usually find that children above some age can no longer be included as part of the family’s health insurance unit except under specific circumstances. Many employment-based plans set that limit at age 19 but may make exceptions for full-time students. The Federal Employees Health Benefits Program (FEHBP), the single largest employment-based health plan in the United States covering 9 million federal workers, their dependents, and retirees, takes another approach. The FEHBP has a cutoff age of 22 and permits children with a disability that prevents them from living independently to continue coverage as part of their parent’s family plan (Office of Personnel Management, 2001). While children age 18 and older may continue to live with their parents or return to their parents’ home (there are more than 21 million people who have reached their majority living with their parents), they are more likely to be without health insurance than they had been previously. Twenty-five percent of children who live with their parents and are age 18 and older are without health insurance, nearly twice the share who are under age 18 (Census Bureau, 2000b).
A majority of those who graduate from high school continue in some form of training or higher education. This increases their chances of maintaining private insurance coverage. One-third of the 18 million young adults ages 19 to 23 are full-time students (Quinn et al., 2000). More than half of the 6 million full-time students have health insurance as dependents through their parents’ family coverage. Another fifth have coverage through plans organized by their educational institution and an additional eighth have coverage through other means. The remaining one-fifth are uninsured.
As young people obtain more education, form new families, and become more attached to the labor market, the share without health insurance drops, to 21.3 percent among 25–34-year-olds. Young people follow various paths in leaving their parents’ homes, including marriage, childbearing and rearing, education, and joining the labor force. Leaving home may mean living as a household of one or with roommates. While these young people may have a separate residence from their parents, they continue to look to their parents for many needs, often including
health insurance.2 Depending on the rules defining when a child can no longer be a dependent, the parents may or may not be able to provide that coverage through the family’s insurance plan. In any case, should the independent young adult be in need of health care, the family may feel some responsibility to help financially if it can.
EMPLOYMENT ISSUES AFFECTING FAMILIES
Finding: The link between health insurance and employment for most families creates many opportunities for loss of coverage. In order to obtain or maintain coverage, family work choices may be constrained. Work choices for families enrolled in public insurance may also be constrained because of the income ceilings for eligibility.
Employment can have a positive effect on coverage by making an insurance plan available to family members in addition to the employee as a benefit of the job. Alternatively, a job that increases family income but that does not offer affordable or any health insurance coverage can have a negative effect on coverage by precluding a family’s eligibility for public coverage. It is important to remember that most of those without insurance are in working families, but many jobs do not offer coverage. Transitions into and out of the work force, as well as the terms of participation, affect coverage. Decisions whether to work full-time, part-time or not at all, to change jobs, or to retire from a job each have implications for a family’s eligibility for private or public health insurance. A critical literature review of more than 50 studies provides evidence of the impact that insurance has on work-related choices (Gruber and Madrian, 2002). These transitions highlight many of the gaps in the current insurance system through which individuals and families may lose coverage or remain uninsured.
Transitions into the Work Force
Young adults who do not pursue full-time education move into the work force at a younger age than those who choose postsecondary education, and they are much less likely to obtain the kind of job that brings health insurance with it. Compared to the 19 percent of young people age 19 to 23 who are in school fulltime and are without health insurance, a much larger share of those not pursuing full-time schooling is without health insurance, 43 percent of men and 35 percent of women (Quinn et al., 2000). Racial minorities are less likely to be full-time students than are whites, and those not in school full-time are even more likely to
be uninsured: 47 percent of African-American men ages 19 to 23 who are not in school full-time are without health insurance, as are 62 percent of men of Hispanic descent. Much of this may be due to higher unemployment and part-time or part-year employment among minority men.
The transition from school to work for young adults may be direct and fulltime or may combine work with part-time schooling. Either route is likely to mean that the new worker holds a job for a shorter period than those who have been in the work force longer, that the work is more likely to be part-time rather than full-time, that it is more likely to be with a small employer, and that it is more likely to have lower pay. For older workers, all of these factors—longer job tenure, employment by larger employers, and higher wages—increase the likelihood that they will be able to maintain employment-based health insurance over time.
To Work (Full-Time) or Not
Families with two wage-earners may have two chances to obtain employmentbased health insurance. Coverage of one spouse through an employer may influence the other spouse’s decisions about whether to work, for what firm, and how much to work. When husbands are not insured through their jobs, their wives are much more likely to work, to work more hours, and to work in jobs that offer health insurance (Gruber, 2000). In families where one spouse has employment-based coverage, the probability that the other spouse works full-time is 6 to 12 percent lower than if the spouse did not have employment-based coverage. The effect is specific to the likelihood of working full-time; part-time work, which is less likely to bring health benefits than full-time work, is unaffected (Buchmueller and Valletta, 1999).
To Change Jobs or Not
Another labor market decision that may be shaped by the availability of health insurance is the decision to change jobs. An extensive literature review documents a phenomenon known as “job lock,” or reduced mobility between jobs, that stems from fear that a new job will bring a disruption in health insurance (Gruber and Madrian, 2002). Families with spouses who both work may avoid job lock if both have access to employment-based coverage with similarly generous benefits and affordable premiums. One study found that the job mobility of husbands is 25 to 32 percent lower when their wives do not have employment-based health insurance and the mobility of wives is 49 percent lower when their husbands do not have health insurance compared to their counterparts with insured spouses (Buchmueller and Valletta, 1996). The federal Health Insurance Portability and Accountability Act (HIPAA), designed to minimize the occurrence of job lock, is discussed below. The studies noted by the Committee are based mainly on data from the period before HIPAA became law.
HIPAA
The Health Insurance Portability and Accountability Act, which became law in 1996, protects health insurance coverage for workers and their families when they change or lose their jobs. It limits the use of preexisting condition exclusions from coverage by health insurance and guarantees, in most cases, that health insurance can be renewed regardless of health condition. It does not limit preexisting condition exclusions for those who have not had health insurance, nor does it limit the premium charged for the insurance (Health Care Financing Administration, 2002).
Work and Public Insurance Programs
Single-parent families have only one opportunity to obtain employmentbased coverage through the employment of an adult family member. Some working parents who do not have employment-based insurance are covered by public programs and may lose their own and their children’s coverage if their earnings exceed the state-set level. For some, the possible loss of coverage may be a factor in deciding whether to work or to change employment and may be a deterrent to increasing earnings above the eligibility level because comparable coverage may not be available or affordable even with the increase in income.
With the decoupling of Medicaid and public assistance eligibility in 1996, however, and increases in upper income limits for children to participate in Medicaid and SCHIP, parents who no longer qualify for Medicaid themselves may still retain Medicaid eligibility for their children. The variation among states in the extent to which Medicaid eligibility has been expanded has created a natural experiment: how much more would single parents work if their children could still participate in Medicaid? An evaluation of these expansions over the 1980s, prior to the decoupling mentioned above, found that for each increase of 25 percent of the poverty threshold in the Medicaid eligibility standard for children, labor force participation by single parents rose by 3.3 percent (Yelowitz, 1995). Single parents were more willing to work if their children could retain Medicaid coverage.
One factor that may constrain the work behavior of a family receiving public assistance is the presence of a disabled child. There are two limited but suggestive studies of this effect. Families with a disabled child that receive public assistance face a double challenge in moving from welfare to work. First, the child’s disabilities may make it more difficult to both care for the child and work; helping a disabled child with activities of daily living, medical treatments, and frequent visits to the doctor can require full-time attention by the parent. Second, earnings beyond some level threaten Medicaid eligibility for both the parents and children. (One might term this the “welfare lock,” a counterpart to job lock, rooted in concern that going to work would endanger a child’s Medicaid eligibility.) Families caring for disabled children are substantially less likely to exit welfare than are families with children who are not disabled (Brady et al., 1998).
A random, stratified sample phone survey of welfare recipients and their families (Aid to Families with Dependent Children [AFDC]) in selected California counties in 1995 found 12 percent of the children had some disability or chronic illness, including 7 percent with a severe disability or chronic illness (Meyers et al., 1998).3 About 20 percent of AFDC families were caring for such children, defined in the survey as children with a disabling or chronic condition that required the child to need a lot more help than other children. Roughly half the children classified in the survey as having severe illness received Supplemental Security Income (SSI), which automatically brings with it Medicaid eligibility. Since SSI provides the child with Medicaid eligibility on his or her own, the parents could move to work, potentially working enough hours at a high enough wage that they would lose their own Medicaid benefits, but the child would remain eligible for Medicaid. Parents whose children did not receive SSI faced loss of both their and their children’s Medicaid when moving to work. Parents in families that received AFDC were more likely to work and leave welfare when their disabled children received SSI than AFDC families whose disabled children were not SSI recipients.
Risk of Job Loss and Layoffs
The loss of a job can result in the loss of employment-based insurance not only for the worker but also for all family members. At a time when family income is significantly if not drastically reduced, families may face difficult choices about purchasing health insurance or taking the risk of being uninsured. A recent survey shows that working-age adults going without insurance for even brief periods have problems getting to see a doctor, filling a prescription, or paying their medical bills, problems similar in magnitude to those of adults who have been uninsured over the long term (Duchon et al., 2001).
Even in stable economic periods, the normal turnover in jobs can put families at risk of being uninsured. Based on statistical modeling, economists have estimated that for every percentage point rise in the unemployment rate, about 1.2 million people become uninsured. This implies that 85 people become uninsured when 100 people lose their jobs (Gruber and Levitt, 2001). During the economic downturn with mass layoffs in the last half of 2001, Congress turned its attention to the plight of workers losing their insurance coverage because of job loss. It attempted to expand an existing program, the Consolidated Omnibus Budget Reconciliation Act of 1986 (COBRA) and proposed alternative approaches to protect former workers and their families, but did not reach political agreement on the best approach.4
COBRA
Part of the Consolidated Omnibus Budget Reconciliation Act facilitates coverage for certain workers who lose employment-based health insurance because of a job change or loss or a related family transition. Generally, persons who lose coverage for work-related reasons are guaranteed access to their former coverage for 18 months. An estimated two-thirds of all workers would qualify for COBRA assistance. However, for workers with incomes below $20,000 this falls to only 40 percent, and for Hispanic workers to 50 percent because they are more likely to work at jobs that are not covered by the law (Doty and Schoen, 2001). Those workers who are eligible under COBRA must pay both the employer and the employee share of their insurance premium (and up to 2 percent more for administrative costs) if they wish to continue coverage. Under COBRA, workers who leave their jobs, or experience a reduction in hours worked below the level that would qualify them for health benefits, may continue in their employer’s plan. Those who lose coverage for family-related reasons are guaranteed access for 36 months, for example, if a spouse becomes entitled to Medicare or following divorce.
Federal COBRA exempts employers with fewer than 20 employees, and it does not apply to the federal government and some church-related employers. These exemptions, along with the fact that many workers do not have access to employment-based insurance, explain why many workers and their dependents are not protected during job and family transitions. Of those workers unemployed in 1999, only 7 percent actually took advantage of COBRA coverage (Zuckerman et al., 2001). For many workers, particularly those with low wages, the cost of the full premium (more than $2,700 for an individual plan or $7,000 for a family plan, on average) would be prohibitive (Kaiser-HRET, 2001). Although the majority of lower-income workers would not be eligible for COBRA, if the premiums were affordable, millions of other workers and their families could continue group health coverage.
Retirement
Retirement is the employment-related decision that most strongly affects insurance status for older persons. The economics literature also shows that retirement decisions are strongly influenced by the availability of insurance after retirement (Gruber and Madrian, 2002). Nearly all Americans become eligible for Medicare, although a majority retire before reaching age 65. Between ages 55 and 65, labor force participation by men declines from 81 percent to 33 percent (Burkhauser et al., 1996). Employment-based insurance is particularly important for adults in late middle age because they are at greater risk of having health problems and opportunities to purchase insurance individually can be limited and too costly (IOM, 2002a). This expense may deter workers from retiring before they become eligible for Medicare. On the other hand, some workers may suffer
from debilitating health conditions that make it difficult for them to continue work even though they are not yet eligible for full retirement benefits or Medicare. The uninsured rates for men and women are about even—more than 13 percent—for those workers aged 60–64 (Monheit et al., 2001a).
Some firms offer retiree health insurance, but the percentage of firms doing so has been declining since the 1980s and varies substantially by the size of the firm. Two-thirds of all large firms (more than 200 workers) offered retirees coverage in 1988, but that is down to one-third now and only 3 percent of small businesses still offer it (Kaiser-HRET, 2001). Among firms still offering such coverage, the cost sharing for the employee has been increasing, and these increases are expected to continue (Freudenheim, 2002; Kaiser-HRET-Commonwealth, 2002).
Retirement at or after age 65 can result in a married couple with an older, retired spouse insured through Medicare and an uninsured younger spouse. Women tend to be the younger spouse and are more likely dependent upon their husband’s coverage than the reverse (Lambrew, 2001a; Monheit et al., 2001a). Working women aged 55–59 are more likely to be uninsured than are working men, reversing the pattern seen in younger adults, when men are more likely to be uninsured. Among women who are younger than their husbands, 10 percent become uninsured when their husbands begin Medicare eligibility (Lambrew, 2001a). Because women are more likely to have chronic conditions than are men in this age group, their opportunities for purchasing independent insurance may be more limited by higher premiums and restrictions on benefits, if they are offered coverage at all (National Center on Women and Aging, 2001).
MARITAL ISSUES AFFECTING FAMILIES
Finding: Marriage increases the chances of having employmentbased health insurance for the whole family. Getting separated or divorced or being widowed may increase the risk that family members lose their employment-based coverage.
Decisions about marriage, cohabitation, having children, and divorce are intimate family choices that may include consideration of health insurance issues, and the decisions may affect the family’s coverage. In addition, the death of a spouse or parent may also change the insurance status of surviving family members.
Marriage
Marriage brings the opportunity to obtain health insurance coverage through one’s spouse’s employer, if it is offered. If both spouses work, they might obtain health insurance coverage from either employer. These factors contribute both to persons in married households being more likely to have health insurance and to health insurance being more common in families with two workers compared to those with one. Married adults are more likely to have health insurance than
those who are not married, and children who live in families headed by a married couple are more likely to have health insurance than are children who live in single-parent families. Among children in married-couple families, 10 percent were uninsured in 2000, compared to 15 percent of children in single-parent families (Census Bureau, 2001a).
The share of young people who are married has been shrinking. The rate at which people marry has declined during much of the period since World War II. Among women ages 20 to 24 who are white or African American, the percentage who had ever married dropped by 32 points from 1975 to 1998 (Teachman et al., 2000). Approximately one in four 20–24-year-olds, of either sex and all races, was married in 1998.
The relatively high uninsured rate for young adults reflects both the declining marriage rate and the increasing age at first marriage. As young people age they tend to marry and increasingly they gain coverage through their spouse. Of those aged 19 to 23, 15 percent are married and 3 percent have coverage through a spouse’s employer. Those rates increase to 68 percent married and 18 percent obtaining coverage through a spouse among those from age 30 to age 64 (Quinn et al., 2000).
Cohabitation
Lower rates of marriage and later ages of first marriage might be related to cohabitation, which may affect health insurance because members of cohabiting couples are not as likely as are married ones to obtain health insurance as a dependent of their partner. Only one in five workers in the private sector works for an employer that offers coverage to nontraditional partners such as same-sex and unmarried heterosexual couples (Kaiser-HRET, 2001).
Young adults are more likely to cohabit than are members of older age groups, although cohabitation is increasing among all age groups (Bumpass and Sweet, 1989; Chevan, 1996). A total of 4.1 million couples were regarded as cohabiting as of 1997, which represents an increase of 46 percent since 1990 (Casper and Cohen, 2000). Among families headed by cohabiting couples, about half include children. Cohabiting couples make up one-fourth of all stepfamilies (Bumpass et al., 1995). Children in these stepfamilies are unlikely to have health insurance coverage through their parent’s partner’s employer, although they may retain coverage through their absent parent.
Most employment-based insurance plans technically exclude an unmarried couple from dependent coverage, although insurance may be offered to the worker alone (Kaiser-HRET, 2001). It is unclear where cohabiting people fit in Figure 2.1, which depicts different family types, because of the variety of ways that people respond to the census survey. Some couples may consider themselves married and respond as such, so they would be noted in either the two-parent or the married-without-children categories. Other cohabiting couples might be in the “living with non-relatives” category.
Separation, Divorce, and Children
Decisions of parents to divorce or to separate affect the likelihood that their children will have health insurance. Children in one-parent families, including those where parents are divorced, separated, or never marry, are less likely to have health insurance than are children in two-parent families. The lower rate of health insurance coverage in single-parent families reflects, in part, lower incomes on average in single-parent households.
As adults increasingly spend fewer years in marriage, more children live in families without two married parents. Nearly half of white children and two-thirds of African-American children are likely to spend part of their lives before age 18 in a single-parent household (Bumpass and Sweet, 1989).
Marriage confers some insurance advantage on children, even after separation or divorce. Almost half of children in ever-married single-parent families had private health insurance, often provided through the employment of either the parent in the household or the absent parent, compared to one-fifth among children in never-married single-parent families (Weinick and Monheit, 1999).
Children living apart from a parent may obtain coverage through the absent parent as a consequence of a legal or informal child support agreement or award. Overall, 24 percent of noncustodial parents provide health insurance for their children (Grall, 2000). This share reflects both the proportion of noncustodial parents who have jobs that allow for dependent coverage and the share of child support awards that include health insurance. Health insurance for children through a noncustodial parent was most common where a child support award or agreement was in place and the award or agreement included health insurance. In these 4.6 million cases with agreements to provide health insurance, custodial parents reported that the absent parent provided health insurance 44 percent of the time. Having health insurance from noncustodial parents was about equally likely where there was an agreement or award that was silent on health coverage (13.5 percent) and where there was no agreement (15 percent). Among the 21 million children eligible for child support, the federal government reports that approximately 15 percent are uninsured (Medical Child Support Working Group, 2000).
The federal government first took steps in 1984 to increase the share of absent parents who included their children in employment-based coverage both to increase coverage for children and to minimize Medicaid enrollment by children who could be privately covered. (This is an early example of federal efforts to prevent the substitution of public insurance programs for private coverage, a phenomenon described as “crowd out”). Legislation required states to include provisions for health coverage in their child support guidelines and to pursue private coverage where the noncustodial parent could obtain it at a reasonable cost. By 1998, 93 percent of support orders had provisions requiring medical support. Compliance went up 18 percentage points from 1989 to 1998 (Medical Child Support Working Group, 2000).
Evidence of increased compliance might be seen in the reported increased share of private coverage for children in single-parent families that came from someone outside the household, presumably the absent parent, between the 1987 and 1996 rounds of the Medical Expenditure Panel Survey (MEPS) (Weinick and Monheit, 1999). Coverage from outside the household for children with never-married parents increased from 4 percent to 12 percent and to 21 percent for children of ever-married parents. However, the absolute level of private coverage remained the same, which suggests some combination of custodial parents being less likely to have jobs that bring coverage for dependent children, and custodial parents moving children to the absent parent’s coverage.
Divorce and Women
Divorce diminishes the probability that an individual will have health insurance through his or her spouse’s employer. Because more women than men are covered through their spouses’ job (26 percent of women and 11 percent of men), women are more likely to suffer an insurance loss through divorce (Lambrew, 2001a). The rate of divorce showed a pronounced increase from 1968 to 1980 with less change since then (Teachman et al., 2000).
When spouses divorce, loss of health insurance is part of a broader decline in economic status among women (Hoffman and Duncan, 1988; Weir and Willis, 2000; National Center on Women and Aging, 2001). Among women between 35 and 64 years of age, divorced women are about twice as likely to lack health insurance as married women, and divorced women are more likely to be uninsured than widows or women who have never been married (Berk and Taylor, 1983).
Widowhood
Although both men and women can be widowed, widowhood is more common among women than among men and is more likely to mean a loss of health insurance for women than it is for men. Eighty-three percent of those widowed by age 65 are women. The probability of widowhood increases with age. Widows and widowers comprise 4 percent of people aged 50–55 and 16 percent of those aged 62–64, an increase of 400 percent (Weir and Willis, 2000).
Widows are more likely to be without health insurance than married persons of the same age. With one-quarter of widows aged 51–61 not having health insurance, they are almost twice as likely to be uninsured as married women in the same age group (Weir and Willis, forthcoming). For women, widowhood carries adverse economic effects (Weir and Willis, 2000). Widowhood does not provide any exception to the general rule that initial eligibility for Medicare begins at age 65.
SUMMARY
Given the many transitional events that affect the life of a family and its chances to gain or lose health insurance, it is not surprising that so many families lack full coverage. When the choice of a spouse or job or the date of retirement can affect health coverage for oneself and others within the family, family decisions become more complex. Even families with the best of intentions and making the most rational choices cannot ensure that all of their members will be able to get and maintain coverage. Many of the factors affecting coverage are beyond the immediate control of the family, are unpredictable, and have no apparent rationale. Not all workers have a choice of a job with affordable employee and dependent coverage. Not all lower-income families are fortunate enough to live in a state with expansive public programs.
A common thread runs through most of the family transitions that result in the loss of coverage. Often, uninsurance results from a combined loss of income and loss of access to employment-based coverage.
The nature of these family transitions make it easier to understand the patterns discussed in the preceding chapter—why single-parent families are at greater risk of uninsurance and why, within the same family, children may be covered and parents not. The following chapters look at the impacts on families of not having all members insured. Nevertheless, it is also important to keep in mind that 81 percent of all families with children do have coverage for all their members. If they are lucky, they will be able to maintain that coverage until they all reach Medicare age.


















