Summary
The nation’s growing recognition of the obesity crisis as a major public health concern for our children and youth has led to an array of diverse efforts aimed at increasing physical activity and promoting healthful eating. These efforts, however, generally remain fragmented and small-scale. Furthermore, there is a lack of systematic tracking and evaluation of childhood obesity prevention interventions. When compared to the strong commitment and heavy infusion of governmental and private-sector resources devoted to other possible major public health concerns, such as infectious disease outbreaks or bioterrorism events, there is a marked underinvestment in the prevention of childhood obesity and related chronic diseases.
Addressing the childhood obesity epidemic is a collective responsibility involving multiple stakeholders and different sectors—including the federal government, state and local governments, communities, schools, industry, media, and families. This was a clear message from the 2005 Institute of Medicine (IOM) report, Preventing Childhood Obesity: Health in the Balance.
Following the release of the Health in the Balance report, the Robert Wood Johnson Foundation asked the IOM to assess progress in childhood obesity prevention actions across a variety of sectors and also to engage in a dissemination effort that would promote the implementation of the 2005 report’s findings and recommendations through three regional symposia. The dual purpose of convening each symposium was to galvanize childhood obesity prevention efforts among local, state, and national decision
makers, community and school leaders, health care providers, public health professionals, and grassroots community-based organizations, as well as to apprise the committee of the experiences and insights of the broad variety of partnerships and activities related to preventing childhood obesity throughout the nation.
To respond to this task, the IOM appointed the Committee on Progress in Preventing Childhood Obesity, comprised of 13 experts in diverse disciplines including nutrition, physical activity, obesity prevention, pediatrics, family medicine, public health, public policy, health education and promotion, community development and mobilization, private-sector initiatives, behavioral epidemiology, and program evaluation. The committee obtained information through a comprehensive literature review, three regional symposia, and two public workshops.
The three regional symposia were held in Wichita, Kansas; Atlanta, Georgia; and Irvine, California; and served to inform the committee about ongoing and innovative promising practices and evaluation approaches that are being used to address the problem and assess the effectiveness of childhood obesity prevention efforts. The crosscutting themes that emerged from all three symposia to support childhood obesity prevention efforts were to forge strategic partnerships, educate stakeholders, increase resources, and empower local schools, communities, and neighborhoods.
This report, Progress in Preventing Childhood Obesity: How Do We Measure Up?, offers four distinct contributions to the childhood obesity discourse. It summarizes the findings of the three regional symposia; provides an evaluation framework that stakeholders can use to assess progress for a range of childhood obesity prevention efforts across different sectors and settings; measures progress for specific recommendations in the Health in the Balance report; and offers new recommendations for leadership and commitment to childhood obesity prevention efforts including an expansion of the nation’s capacity and action in implementing, evaluating, and monitoring childhood obesity prevention initiatives and interventions.
The challenge presented in this report is to take the next steps toward developing a robust evidence base for effective childhood obesity prevention interventions and practices. Given the numerous changes being implemented throughout the nation to improve the dietary quality and extent of physical activity for children and youth, an overarching assessment of progress in preventing childhood obesity necessitates both the tracking of trends across the nation and a more detailed examination of lessons learned through the evaluations of relevant interventions, policies, and programs. Evaluations produce information or evidence that can be used to improve a policy, program, or an intervention in its original setting; refine those that need restructuring and adaptation to different settings and contexts; and revise or discontinue those efforts found to be ineffective. Evaluation is
central to identifying and disseminating effective initiatives—whether they are national or local programs, large- or small-scale efforts.
EVALUATION FRAMEWORK
The committee uses the term evaluation to represent the systematic assessment of the quality and effectiveness of a policy, program, or initiative. It is an effort to determine whether and how an intervention has important and consequential outcomes. Many types of evaluations can contribute to the knowledge base by identifying promising practices and helping to establish causal relationships between interventions and various outcomes. Evaluation can also enhance our understanding of the intrinsic quality of the intervention and of the critical context where factors can moderate or mediate an intervention’s effect in particular ways. The committee emphasizes that program evaluations of varying scope and size, at all levels and within and across all sectors, play a vital role in addressing the childhood obesity epidemic. Evaluation fosters collective learning, supports accountability and responsibility, reduces uncertainty, guides improvements and innovations in policies and programs, determines cost-effectiveness, and helps to leverage change in society.
Evaluations are conducted for multiple stakeholders and the findings broadly shared and disseminated. These audiences include policy makers, funders, and other elected and appointed decision makers; program developers and administrators; program managers and staff; and program participants, their families, and communities. Moreover, these diverse evaluation audiences tend to value evaluation for different reasons. The committee emphasizes the need for a collective commitment to evaluation by those responsible for funding, planning, implementing, and monitoring childhood obesity prevention efforts.
Although resources are limited, evaluation should be incorporated as an essential component of the program planning and implementation process rather than as an optional activity. Government agencies, foundations, and other funders of childhood obesity programs and interventions should incorporate evaluation requirements, as is current practice by many agencies and organizations. Similarly, program planners and those who implement policy changes should view evaluation as an integral part of their efforts. If something is valuable enough to invest time, energy, and resources, then it is also worthy of the investment necessary to carefully document the success of the effort.
All childhood obesity prevention policies and interventions deserve some type of evaluation. Evaluations can range in scope and complexity from comparisons of pre- and post-intervention counts of the number of
individuals participating in a program to methodologically sophisticated evaluations with comparison groups and research designs. All types of evaluation can make an important contribution to the evidence base upon which to design policies, programs, and interventions.
The translation of evaluation and research findings into promising practices constitutes the primary means for accelerating national efforts to reverse the childhood obesity epidemic. Since the need for effective evaluation is ongoing, both the capacity and quality of evaluation will be positively influenced by a steadfast national commitment to support obesity prevention efforts and the rapid translation and dissemination of evaluation and research findings—across the geographical landscape—to stakeholders involved in obesity prevention efforts in states and communities. Furthermore, the social and cultural diversity within the United States precludes assumptions about the transferability of interventions from one sub-population to another and should therefore be assessed.
Changing stakeholder perceptions about evaluation—from considering it a daunting task of questionable value to a manageable and highly useful endeavor to inform their efforts—can be facilitated by considering four key evaluation questions to guide childhood obesity prevention policies, programs, and interventions (Box S-1). Although these questions are relevant to obesity prevention strategies and actions across all sectors, not every evaluation can be expected to address all of the questions. Rather, the relevance of the four evaluation questions depends on the type of obesity prevention intervention and the available evaluation resources and technical expertise.
|
BOX S-1 Questions to Guide Childhood Obesity Prevention Policies and Interventions
|
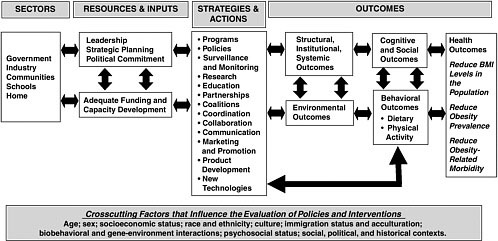
Experienced evaluators have long acknowledged the importance of identifying and understanding the key contextual factors (e.g., environmental, cultural, normative, and behavioral) that influence the potential impact of an intervention. The evaluation framework that the committee developed offers a depiction of the resources and inputs, strategies and actions, and a range of outcomes that are important to childhood obesity prevention. All are amenable to documentation, measurement, and evaluation (Figure S-1).
The evaluation outcomes selected will depend on the nature of the intervention, the timeline of the program or intervention, and the resources available to program implementers to collect, analyze, and interpret outcomes data. The timeline of the intervention often determines whether the evaluation can assess progress toward a short-term outcome (e.g., increasing participation in an after-school intramural sports team), an intermediate-term outcome (e.g., changes to the built environment that promote regular physical activity for children and youth) or a long-term outcome (e.g., a reduction in BMI levels of children participating in a new program). Outcomes can also be categorized based on the nature of the change: (1) structural, institutional, and systemic outcomes; (2) environmental outcomes; (3) population or individual-level cognitive and social outcomes; (4) behavioral outcomes (e.g., dietary and physical activity behaviors); and (5) health outcomes (Figure S-1).
The evaluation framework also illustrates the range of inputs and outcomes while giving careful consideration to the following factors:
-
The interconnections and quality of interactions within and among the multiple sectors involved in childhood obesity prevention initiatives.
-
The adequacy of support and resources for policies and programs.
-
The contextual appropriateness, relevance, and potential power of the planned policy, intervention, or action.
-
The multiple outcomes (e.g., structural, institutional, systemic, environmental, behavioral for individuals and the population, and health outcomes).
-
The potential impact of interventions on adverse or unanticipated outcomes, such as stigmatization.
-
The indicators used to assess progress made toward each outcome. Selecting the best indicators will depend on the purpose for which they are intended and the resources available to program staff to collect, analyze, and interpret relevant data.
A variety of crosscutting factors influence program experiences and the evaluation process, thereby requiring consideration at every stage of the evaluation framework for both individuals and populations. These include
age, sex, socioeconomic status, and race/ethnicity; culture, immigration status and acculturation; bio-behavioral and gene-environment interactions; psychosocial status; and social, political, and historical contexts. Context refers to the set of factors or circumstances that surround a situation or event and give meaning to its interpretation. All of these factors should be taken into account when designing, monitoring, and evaluating obesity prevention initiatives as depicted in Figure S-1.
The committee has identified several relevant criteria that can be used to judge the design and quality of interventions and encourages funders and program planners to consider the following actions:
-
Include diverse perspectives and attend to the sub-populations in the greatest need of prevention actions—particularly underserved, low-income, and high-risk populations that experience health disparities;
-
Use relevant empirical evidence relevant to the specific context when designing and implementing the intervention;
-
Identify similar or potentially synergistic efforts and make important cross-sectoral linkages and sustained collaborations; and
-
Link structural, environmental, and behavioral changes in individuals and populations relevant to childhood obesity prevention.
CONCLUSIONS
The committee developed five broad conclusions (Box S-2) based on its assessment of progress in preventing childhood obesity that serve as the foundation for the report’s recommendations and implementation actions discussed in the report.
RECOMMENDATIONS FOR ASSESSING PROGRESS
Reflective of the collective and interrelated responsibility of multiple sectors and stakeholders to create a healthy marketplace and media environment, healthy communities, healthy school environments, and healthy home environments, the committee developed four recommendations for this report. The committee’s recommendations are relevant across five major sectors—government, industry, communities, schools, and home. The first recommendation underscores the importance of promoting leadership and commitment to treat childhood obesity prevention as an urgent national priority. The remaining three recommendations serve as the basis for evaluation activities within and across the sectors, accounting for interdependencies and dynamic changes that will affect obesity prevention actions. More details about the implementation of the recommendations for each sector are discussed throughout the report and collated in Appendix E.
|
BOX S-2 Conclusions
|
These recommendations collectively call our attention to the urgent need to provide more and better information to improve peoples’ lives through evaluation. Stakeholders in each sector are urged to identify and mobilize adequate resources for the evaluation of obesity prevention interventions for children and youth. The recommendations also advance an evaluation process that meaningfully engages diverse stakeholders in the evaluation design and process and that legitimizes the multiplicity of stakeholder perspectives, notably including program recipients along with funders, administrators, and professional staff.
There will be a greater likelihood of success when public, private, and voluntary organizations purposefully combine their respective resources, strengths, and comparative advantages to ensure a coordinated and sustained long-term effort. Evaluations will contribute to building a strong and diverse evidence base upon which promising and best practices can be identified, scaled up, and institutionalized across different settings and sectors.
Recommendation 1: Government, industry, communities, schools, and families should demonstrate leadership and commitment by mobilizing the resources required to identify, implement, evaluate, and disseminate effective policies and interventions that support childhood obesity prevention goals.
-
Federal, state, and local governments should each establish a high-level task force to identify priorities for action, coordinate public-sector efforts, and establish effective interdepartmental collaborations.
-
Industry should use the full range of available resources and tools to create, support, and sustain consumer demand for products and opportunities that support healthy lifestyles including healthful diets and regular physical activity.
-
Community stakeholders should establish and strengthen the local policies, coalitions, and collaborations needed to create and sustain healthy communities.
-
School boards, administrators, and staff should elevate the priority that is placed on creating and sustaining a healthy school environment and advance school policies and programs that support this priority.
-
Families, parents, and caregivers should commit to promoting healthful eating and regular physical activity to create a healthy home environment.
Recommendation 2: Policy makers, program planners, program implementers, and other interested stakeholders—within and across relevant sectors—should evaluate all childhood obesity prevention efforts, strengthen the evaluation capacity, and develop quality interventions that take into account diverse perspectives, that use culturally relevant approaches, and that meet the needs of diverse populations and contexts.
-
Federal and state government departments and agencies should consistently evaluate the effects of all actions taken to prevent childhood obesity and strengthen the evaluation capacity, paying particular attention to culturally relevant evaluation approaches.
-
Industry should partner with government, academic institutions, and other interested stakeholders to undertake evaluations to assess its progress in preventing childhood obesity and promoting healthy lifestyles.
-
Community stakeholders should strengthen evaluation efforts at the local level by partnering with government agencies, foundations, and academic institutions to develop, implement, and
-
support evaluation opportunities and community-academic partnerships.
-
Schools and school districts should strengthen evaluation efforts by partnering with state and federal agencies, foundations, and academic institutions to develop, implement, and support evaluations of all relevant school-based programs.
-
Parents and caregivers, as the policy makers in the household, should assess their family’s progress in achieving positive lifestyle changes.
Recommendation 3: Government, industry, communities, and schools should expand or develop relevant surveillance and monitoring systems and, as applicable, should engage in research to examine the impact of childhood obesity prevention policies, interventions, and actions on relevant outcomes, paying particular attention to the unique needs of diverse groups and high-risk populations. Additionally, parents and caregivers should monitor changes in their family’s food, beverage, and physical activity choices and their progress toward healthier lifestyles.
-
Government at all levels should develop new surveillance systems or enhance existing surveillance systems to monitor relevant outcomes and trends and should increase funding for obesity prevention research.
-
The U.S. Congress, in consultation with industry and other relevant stakeholders, should appropriate adequate funds to support independent and periodic evaluations of industry’s efforts to promote healthier lifestyles.
-
Community stakeholders and relevant partners should expand the capacity for local-level surveillance and applied research and should develop tools for community self-assessment to support childhood obesity prevention efforts.
-
Schools and school districts should conduct self-assessments to enhance and sustain a healthy school environment, and mechanisms for examining links between changes in the school environment and behavioral and health outcomes should be explored.
-
Parents and caregivers should monitor their families’ lifestyle changes; and government, foundations, and industry should support applied research that examines family interventions in real-world settings.
Recommendation 4: Government, industry, communities, schools, and families should foster information-sharing activities and disseminate evaluation and research findings through diverse communication chan-
nels and media to actively promote the use and scaling up of effective childhood obesity prevention policies and interventions.
-
Government at all levels should commit to the long-term support and dissemination of childhood obesity prevention policies and interventions that have been proven to be effective.
-
Industry should collaborate with the public sector and other relevant stakeholders to develop a mechanism for sharing proprietary data and a sustainable funding strategy that can inform and support childhood obesity prevention interventions.
-
Community stakeholders should partner with foundations, government agencies, faith-based organizations, and youth-related organizations to publish and widely disseminate the evaluation results of community-based childhood obesity prevention efforts.
-
Schools should partner with government, professional associations, academic institutions, parent-teacher organizations, foundations, communities, and the media to publish and widely disseminate the evaluation results of school-based childhood obesity prevention efforts and related materials and methods.
-
Government (federal, state, and local), communities, families, and the media should disseminate and widely promote the evaluation results of effective family- and home-based childhood obesity prevention efforts.
NEXT STEPS
Each of the recommendations is further expanded in the report, in which the committee recommends specific implementation actions that should be taken by government, industry, communities, schools, and parents and caregivers at home to ensure that there are adequate resources and a focus on strengthening the evaluation of childhood obesity prevention policies and interventions. Given the range of actions that are needed to move forward in preventing childhood obesity, the committee has identified immediate next steps that it deems essential priority actions in the near future.
Government
The federal, state, and local governments are actively engaged in childhood obesity prevention efforts. However, as noted above, the levels of funding and resources invested in these efforts and their evaluation are not commensurate with the seriousness of this public health problem. Government at all levels should provide coordinated leadership for the prevention of obesity in children and youth.
A critical next step for the federal government is to establish a high-level task force on childhood obesity prevention, as recommended in the Health in the Balance report (IOM, 2005), and underscored in this report. The committee recommends that the president request that the secretary of the U.S. Department of Health and Human Services (DHHS) to convene this high-level task force and the task force include as members the secretaries or senior officials of DHHS and the U.S. Departments of Agriculture, Education, Transportation, Housing and Urban Development, Interior, Defense, and other relevant departments and agencies. The purpose of the task force would be to ensure coordinated budgets, policies, and requirements for obesity prevention programs and to establish effective interdepartmental collaboration and priorities for action.
Furthermore, the federal government should provide a sustained commitment and long-term investment in childhood obesity prevention initiatives found to be effective (such as the VERB™ campaign) and those that are vital to measuring progress (such as national surveillance efforts to track trends in the obesity epidemic).
Surveillance systems—such as the National Health and Nutrition Examination Survey, the School Health Policies and Programs Study, the Youth Media Campaign Longitudinal Survey, the Youth Risk Behavior Surveillance System, and the National Household Transportation Survey—should be expanded to include relevant obesity-related outcomes. Surveillance systems that monitor the precursors of dietary and physical activity behaviors, such as changes in policies and the built environment, need to be expanded or developed.
Additionally, monitoring systems for USDA programs such as the Special Supplemental Nutrition Program for Women, Infants, and Children, the Food Stamp Program, and the school meals programs should be developed that assess a range of obesity-related outcomes for children and youth.
State and local governments should also demonstrate leadership on this issue and commit resources and policies that lead to actions that implement and evaluate changes in schools and communities.
Industry
Certain segments of relevant industries, including the food, beverage, restaurant, food retail, leisure and recreation, physical activity and fitness, and entertainment industries have responded constructively to the childhood obesity epidemic. However, other corporations in these industries are not yet engaged in obesity prevention; and other segments of the industry, such as the fitness, spectator sports, and transportation sectors, have not shown adequate involvement in obesity prevention actions. Nevertheless, careful and independent evaluations are needed to determine if industry is
making a sufficient investment, sustained commitment, and whether those initiatives proposed by industry will be effective and contribute to desirable outcomes.
Industry and the public health community should work toward nurturing and strengthening partnerships that support obesity prevention efforts. To expand the federal research capacity to study the ways in which marketing influences children’s and adolescents’ attitudes and behaviors, industry is encouraged to provide data on pricing strategies, consumer food purchases, and consumption trends from proprietary retail scanner systems, household scanner panels, household consumption surveys, and marketing research. The collaborative work should examine the quality of the data, consider reducing the cost to make the data accessible, and establish priorities for applying the information to promote healthful diets and physical activity.
Corporate responsibility can be demonstrated by sharing marketing research findings, to the greatest extent possible, which will assist the public health sector to develop, implement, and evaluate more effective childhood obesity prevention policies, programs, and interventions. Data sharing will need to balance many considerations including transparency, public accessibility, the demands of the competitive marketplace, and legal issues. In certain cases, it may be appropriate for the data to be released after a time lag to keep the public informed with relatively recent data. The committee recommends that the public and private sectors engage in a collaborative process that will assist relevant stakeholders to share proprietary data for the public good.
Communities
Communities vary widely in the extent and nature of the resources available to be used in changing the built and social environments to facilitate physical activity and access to foods and beverages that contribute to a healthful diet. A number of state and local governments, foundations, nonprofit and youth-related organizations, faith-based organizations, and community coalitions are demonstrating innovative and collaborative approaches to childhood obesity prevention. However, there is much that remains to be learned, translated, and disseminated, particularly from effective evidence-based interventions that continue even when seed funding and external resources are no longer available.
The committee identified two immediate next steps for communities. The development of a validated community self-assessment tool, such as a community health index, will help communities identify their strengths and gaps in designing and evaluating childhood obesity-prevention efforts, rang-
ing from local programs and evaluation capacity to the local physical and built environments, and the extent of community involvement.
Congress should appropriate funds for CDC, in partnership with the Department of Transportation, the Department of the Interior, and other relevant federal agencies, private-sector and nonprofit organizations, and community stakeholders to develop this type of well-validated tool that can be used in economically and culturally diverse communities. Additionally, the National Association of County and City Health Officials, in partnership with government agencies and other nonprofit and voluntary health organizations, should develop a means of compiling and sharing community-based evaluation results, lessons learned, and community action plans as well as provide links to resources, templates, and evaluation tools. A web-based database or repository of published and unpublished literature, case studies, and promising intervention websites is needed.
Schools
Schools are the current focus of many childhood obesity prevention efforts, particularly changes to the school food and beverage environment. Less attention has been paid to increasing physical activity in schools, although this issue seems to be gaining momentum. As is true for community efforts, wide variations in the extent of the efforts and resources available for investment in obesity prevention by individual schools, school districts, and state agencies are observed. Federal law requires that schools receiving federal funds for school meals must develop school wellness policies by the fall of 2006, which has stimulated school-based health promotion and obesity prevention efforts across the country. Additionally, teachers, food service personnel, school administrators, and state and federal agency staff have developed many creative and innovative approaches to improve students’ diets and to increase physical activity, but these need to be evaluated. The committee encourages states and school districts to bolster their physical education and physical activity requirements and standards, as should preschool, child-care, and after-school programs. Accountability mechanisms are needed for state school nutrition and physical activity standards that include increased transparency and dissemination of school-by-school reports on success in meeting these standards. Furthermore, federal and state leadership is needed to provide adequate and sustained resources to implement changes relevant to obesity prevention in the school environment. Not only are political will and leadership needed to improve school nutrition and physical activity opportunities, but it is critically important that adequate and sustained funding be provided to reinforce these priorities so that attention to this issue does not result in un-funded mandates.
Home
Many families across the country are aware of their role in preventing childhood obesity and are actively making changes towards a healthier lifestyle, while others are not yet engaged in change. A next step for parents, caregivers, children, and adolescents is to periodically assess the home environment and ask the following questions: Are the foods and beverages that are available and prepared in the home healthful and served in reasonable portions? Is physical activity emphasized and a family priority? Do families have established rules or guidelines limiting leisure screen time? Incremental changes are valuable and signal that progress is occurring.
Conclusion
A succinct assessment of the nation’s progress in preventing childhood obesity is not feasible given the diverse and varied nature of America’s communities and population. However, it can be said that awareness of obesity has been raised, actions have begun, coordination and prioritization of limited resources are critical, and evaluation of interventions within and across all sectors is essential. A long-term commitment to create a healthy environment for our children and youth is urgently needed. This commitment will require widespread changes in social norms, institutions, and practices beyond those that directly involve children and youth.