1
Setting the Stage for Revising Pregnancy Weight Guidelines: Conceptual Framework
BACKGROUND
Improvement of maternal, fetal, and child health are key public health goals. Over the past four decades, changes in public health trends have challenged the health care sector to provide optimal guidance to women before, during, and after pregnancy so that they can achieve healthy outcomes for both themselves and their newborns. During this time, two reports have contributed to providing this guidance.
The first report, Maternal Nutrition and the Course of Pregnancy (NRC, 1970), developed from concern about high neonatal and infant mortality rates in the United States compared to other developed countries. In that report, the Committee on Maternal Nutrition recognized the positive relationship between gestational weight gain (GWG) and birth weight. The committee also noted the positive association between prepregnancy maternal weight and birth weight and the fact that higher prepregnancy maternal weight reduced the impact of GWG on birth weight. The report advised an average gestational weight gain of 24 pounds (20-25-pound range) and advised against the then-current practice of limiting GWG to 10-14 pounds.
The subsequent Institute of Medicine (IOM) report Nutrition During Pregnancy (IOM, 1990) offered more specific recommendations for weight gain during pregnancy stratified by prepregnancy maternal body mass index (BMI). The report also made specific weight gain recommendations for population subgroups, including adolescents, members of racial and ethnic
groups, women of short stature, and women carrying twins; and detailed historic trends in weight gain recommendations and guidelines. The IOM (1990) recommendations for weight gain during pregnancy have been adopted by or have been influential in many countries. Observational studies have demonstrated that women who enter pregnancy at a normal BMI and gain within the recommended ranges are more likely to have a good birth outcome than women who gain outside the recommended ranges (Taffel et al., 1993; Abrams et al., 2000; Groth, 2006).
In the years since the release of the weight gain recommendations from the IOM (1990) report, however, some dramatic shifts in the demographic and epidemiologic profile of the U.S. population have occurred. Notably, the population of U.S. women of childbearing age has become more diverse; and prepregnancy BMI and excess GWG have increased across all population groups, particularly among minority groups who are already at risk for poor maternal and child health outcomes (Yeh and Shelton, 2005; Kim et al., 2007). These and other factors suggested a need to consider whether a revision of the IOM (1990) pregnancy weight gain guidelines is necessary.
RATIONALE FOR REVISING THE GUIDELINES
General Principles Framing the IOM (1990) Pregnancy Weight Guidelines
The IOM (1990) pregnancy weight guidelines were developed principally in response to concerns about low birth weight infants. Although adverse health outcomes for excess weight gain were considered in the IOM (1990) weight gain guidelines, the recommendations were derived largely from data collected in the 1980 National Natality Survey (Available: http://www.cdc.gov/nchs/about/major/nmihs/abnmihs.htm [accessed March 3, 2009]) and focused on preventing premature births and small-for-gestational age infants.
The IOM (1990) report and a subsequent report, Nutrition During Pregnancy and Lactation: An Implementation Guide (IOM, 1992), identified specific actions practitioners could take to achieve the recommendations in working with patients. They also identified a series of recommendations for epidemiologic, basic, and applied research to enable better estimates of GWG, prepregnancy weight for height, and gestational duration, which affect study design and interpretation.
INDICATORS FOR REVISING THE CONCEPTUAL FRAMEWORK OF THE GUIDELINES
In 1996 an expert work group was convened by the Maternal and Child Health Bureau of the Health Resources and Services Administration
(HRSA), Department of Health and Human Services (HHS), to examine issues relating to maternal weight gain that had been published in the IOM (1990) report. The goal of this group was to determine whether new research provided a basis for practitioners to change guidance for GWG and recommend future directions for research, training, and/or other programmatic initiatives. The group concluded that formal revision of the IOM (1990) weight gain recommendations was not yet warranted; however, reservations were expressed that the recommendations for African American women, young adolescents, and women of short stature were too specific (Suitor, 1997).
Since publication of the IOM reports, Nutrition During Pregnancy (1990), Nutrition During Lactation (1991), and Nutrition During Pregnancy and Lactation: An Implementation Guide (1992), the population of U.S. women of childbearing age has become more diverse. Although low birth weight remains a significant concern during pregnancy, new health concerns have emerged. These include the greater prevalence of women who are overweight or obese entering pregnancy, which puts them at high risk for pregnancy complications. For example, data from the 2003-2004 round of the National Health and Nutrition Examination Survey (NHANES) show that 28.9 percent of women of reproductive age (20-39 years old) were obese (BMI ≥ 30 kg/m2) and 8.0 percent were extremely obese (BMI ≥ 40 kg/m2) (Ogden et al., 2006). Additionally, women are becoming pregnant at an older age and enter pregnancy with chronic conditions such as type 2 diabetes, which also puts them at risk for pregnancy complications and may lead to increased morbidity during their post-pregnancy years (Cleary-Goldman et al., 2005; Joseph et al., 2005; Delpisheh et al., 2008).
Also since publication of the IOM (1990) report and the subsequent 1991 and 1992 reports, research on GWG has demonstrated that weight patterns (underweight and overweight) and total weight gain have short-and long-term consequences for the health of the mother. For example, prepregnancy BMI above normal values (19.8-26 kg/m2) is associated with preeclampsia, gestational diabetes mellitus (GDM), cesarean delivery (Doherty et al., 2006; Abenhaim et al., 2007), and failure to initiate and sustain breastfeeding (Hilson et al., 1997; Li et al., 2003; Kugyelka et al., 2004). Increased maternal BMI and GWG have also been associated with higher fat mass in infants and subsequent overweight in children (Hillier et al., 2007; Oken et al., 2007).
Collectively, these trends (e.g., the greater prevalence of overweight and obese women entering pregnancy) and newer research (e.g., on the consequences of excess GWG) have prompted new concern about the appropriateness of existing guidelines for GWG and whether the guidelines support optimal outcomes for mother, infant, and child. Specifically there have been concerns about the implications of the IOM (1990) recommen-
dations for (1) the health of the mother, particularly for women who are overweight, underweight, older, adolescent, or short in stature; (2) infant and child health; and (3) other metabolic processes that may affect the in utero environment.
Another concern that has frequently been raised by researchers and practitioners is the difference between BMI categories used in the IOM (1990) report and those used in the report Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults from the National Heart, Lung, and Blood Institute (NHLBI, 1998) in cooperation with the National Institute of Diabetes and Digestive and Kidney Diseases, which are based on a report from the World Health Organization (1995). This is a problem for practitioners as well as for researchers. Most importantly, despite the effort made to publicize the recommendations of the IOM (1990) report, including the development of a guide to assist the medical profession to implement these guidelines (IOM, 1992), many health care providers have not used these guidelines and many women have not followed them (Abrams et al., 2000).
SETTING THE STAGE FOR REVISING THE GUIDELINES
In response to such concerns, the Maternal and Child Health Bureau of HHS requested that the National Research Council and the IOM convene a workshop in May 2006. The purpose of this workshop was to review trends in maternal weight; explore emerging research findings related to the complex relationship of the biological, behavioral, psychological, and social interactions that affect maternal and pregnancy weight on maternal and child health outcomes; and discuss interventions. The following specific questions were addressed by the workshop:
-
What research and databases describe the distribution of maternal weight (prior to, during, and after pregnancy) among different populations of women in the United States?
-
What research and databases inform understanding of the effects of different weight patterns (including underweight and overweight) during pregnancy on maternal and child health outcomes?
-
What research has been conducted to describe the individual, community, and health care system factors that impede or foster compliance with recommended GWG guidelines?
-
What opportunities exist for Title V maternal and child health programs to build on this knowledge to help childbearing women achieve and maintain recommended weight?
-
What future research and data collection efforts could improve the efforts of Title V programs to support women from different racial
-
and ethnic backgrounds in their efforts to comply with recommended weight guidelines and to improve their maternal health?
The summary report from that workshop, Influence of Pregnancy Weight on Maternal and Child Health (NRC-IOM, 2007), includes a review of U.S. trends in maternal weight (before, during, and after pregnancy) among different populations of women. The workshop report also includes a discussion of the determinants of GWG; the relationships among maternal weight, GWG, and the health of women and children; interventions in health care and community settings that help women achieve appropriate weight levels during and after pregnancy; and emerging themes that warrant further examination in future studies. Taken together, the workshop and its summary report reinforce the need to reexamine recommendations for GWG, especially in light of the current obesity epidemic, and to highlight ways to encourage their adoption.
THE COMMITTEE’S TASK
Sponsors1 asked the IOM’s Food and Nutrition Board and the Division of Behavioral and Social Sciences and Education Board on Children, Youth, and Families to review and update the IOM (1990) recommendations for weight gain during pregnancy and recommend ways to encourage their adoption through consumer education, strategies to assist practitioners, and public health strategies.
The committee was asked to address the following tasks:
-
Review evidence on the relationship between weight gain patterns before, during, and after pregnancy and maternal and child health outcomes, with particular attention to the prevalence of maternal obesity racial/ethnic and age differences, components of GWG, and implications of weight during pregnancy on postpartum weight retention, maternal and child obesity, and later child health.
-
Within a life-stage framework consider factors in relation to GWG that are associated with maternal health outcomes such as lactation
-
performance, postpartum weight retention, cardiovascular disease, metabolic processes including glucose and insulin-related issues, and risk of other chronic diseases; for infants and children, in addition to low birth weight, consider early developmental impacts and obesity-related consequences (e.g., mental health, diabetes).
-
Recommend revisions to the existing guidelines, where necessary, including the need for specific pregnancy weight guidelines for underweight, normal weight, and overweight and obese women and adolescents and women carrying twins or higher-order multiples.
-
Consider a range of approaches to promote appropriate weight gain, including:
-
individual (behavior), psychosocial, community, health care, and health systems;
-
timing and components of interventions; and
-
ways to enhance awareness and adoption of the guidelines, including interdisciplinary approaches, consumer education to men and women, strategies to assist practitioners to use the guidelines, and public health strategies.
-
-
Identify gaps in knowledge and recommend research priorities.
Approach to the Task
The committee approached its task by gathering information from existing scientific literature, including a systematic review of the literature by the Agency for Healthcare Research and Quality (AHRQ) (Viswanathan et al., 2008) as well as additional studies not included in the AHRQ review (see Appendix E for literature reviewed). The committee also gathered information from presentations by recognized experts in three workshops (see Chapter 9), consulted with additional experts in relevant fields, and commissioned four new data analyses. Contributions made to the committee by consultants are noted throughout the report. The information-gathering activities laid the groundwork for the committee’s work of deliberating on issues relevant to the task and formulating a strategy to address the scope of work. This task was not regarded by the committee as a formal systematic, evidence-based review, as the full range of literature did not lend itself to this type of task. Rather, because of the wide-ranging and large literature on this subject, the committee relied on its collective expertise to determine how much weight to give to all of the sources of information at its disposal.
The committee worked from the perspective that pregnancy-related weight begins before conception and continues through the first year postpartum and affects both the mother and her child. In consideration of
Task 1, given the magnitude and complexity of the task, the committee determined that it was unable to address maternal weight history before entering pregnancy other than to take prepregnant BMI into account. Whenever possible, the committee sought and presented data on outcomes associated with GWG by racial/ethnic groups. This was done in the spirit of documenting disparities across racial/ethnic groups that the committee anticipated would reflect the strong socioeconomic differentials and not biological differences across these groups. This assumption is grounded in the fact that ethnicity is, by definition, a sociocultural construct and that race, as it is defined in the United States, has been shown to be a social and not a biological construct (Goodman, 2000).
It is noteworthy that the committee was not charged with evaluating either the safety or effectiveness of the IOM (1990) guidelines. However, observational studies clearly indicate that gaining within the 1990 guidelines is associated with better pregnancy outcomes (and, presumably, greater safety) than gaining outside of them (Taffel et al., 1993; Abrams et al., 2000; Gross, 2006). Moreover, the safety and effectiveness of a set of guidelines is a function of many factors, including adoption and use of the guidelines by the health care team, acceptance and actual use of the guidelines by their target audience, barriers the target audience might experience in achieving the guidelines and, finally, whether those who actually meet the guidelines have better outcomes.
CONCEPTUAL FRAMEWORK
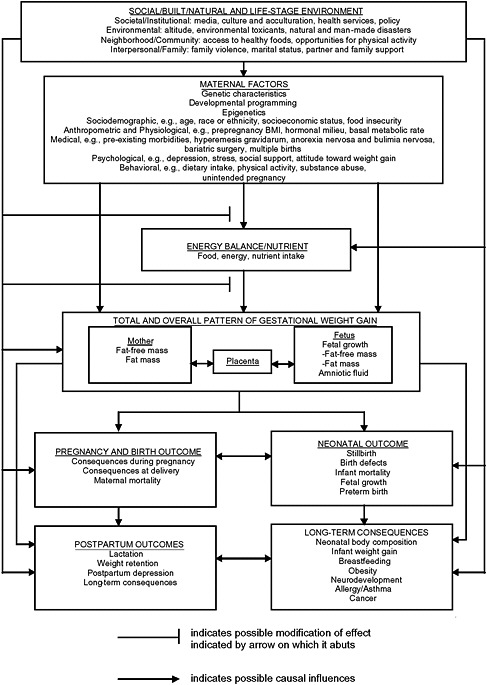
To inform its review of the literature and to guide the organization of this report, the committee reevaluated the conceptual framework utilized in the IOM (1990) report (see Figure 1-1) to account for advances in scientific understanding of the determinants and consequences of GWG. However, it retained the same general scientific approach and epidemiologic conventions used previously and discussed in detail in the IOM (1990) report. Several changes in the conceptual framework are noteworthy. The committee chose to highlight the importance of numerous environmental factors as determinants that lead to GWG. It is recognized that some of these act through maternal factors to influence GWG and its consequences, while others may affect those consequences by other routes.
ORGANIZATION OF THE REPORT
This report is organized into eight chapters in which the committee describes what is known about GWG, with particular attention to demographic and other factors associated with weight gains that fall above or
below recommended levels; identifies data gaps; and makes recommendations based on the committee’s findings.
The report begins, in this chapter, by introducing the reasoning for a reexamination of pregnancy weight guidelines, based on data that have been gathered since the publication of Nutrition During Pregnancy (IOM, 1990).
Trends in GWG since the time of the IOM (1990) report are considered in Chapter 2, with particular attention to weight gain in racial or ethnic subgroups of the U.S. population. The information reviewed in this chapter helped guide the committee’s recommendations for assisting women in achieving the new GWG guidelines presented in Chapter 7.
The composition and components of GWG are addressed in Chapter 3. Since the IOM (1990) report was prepared, the importance of the placenta in the dialogue between the mother and fetus has become more apparent. The information reviewed in Chapter 3 not only provides a foundation for understanding the variation among women in the amount, pattern, and composition of GWG, but also it helped the committee to identify gaps in scientific understanding of the determinants and consequences of GWG.
The determinants of GWG are discussed in Chapter 4. As with the information covered in Chapter 2, the committee used this information when developing its recommendations—not just recommendations pertaining to specific weight gain amounts but also, and particularly, recommendations for how these guidelines should be implemented (e.g., what types of interventions would most likely work and under what circumstances). When considering the determinants of GWG, the committee chose to distinguish between maternal factors that are fixed at conception (e.g., age, racial or ethnic group, parity) and those that could potentially be modified during the gestation period (e.g., smoking, drug use, medical conditions that could be treated).
The consequences of GWG are discussed in Chapters 5 and 6. Chapter 5 focuses on maternal outcomes and Chapter 6 on offspring outcomes. The conceptual framework upon which the committee based its deliberations draws attention not just to outcomes in the perinatal and postpartum periods but also to those that occur much later in the lives of mothers and their children.
The new guidelines and the committee’s strategy for developing them are discussed in Chapter 7. Approaches to implementation of the new guidelines are discussed in Chapter 8. Additional recommendations for research are presented at the end of each chapter. The data reviewed in the chapters is tabulated in accompanying appendixes.
REFERENCES
Abenhaim H. A., R. A. Kinch, L. Morin, A. Benjamin and R. Usher. 2007. Effect of prepregnancy body mass index categories on obstetrical and neonatal outcomes. Archives of Gynecology and Obstetrics 275(1): 39-43.
Abrams B., S. L. Altman and K. E. Pickett. 2000. Pregnancy weight gain: still controversial. American Journal of Clinical Nutrition 71(5 Suppl): 1233S-1241S.
Cleary-Goldman J., F. D. Malone, J. Vidaver, R. H. Ball, D. A. Nyberg, C. H. Comstock, G. R. Saade, K. A. Eddleman, S. Klugman, L. Dugoff, I. E. Timor-Tritsch, S. D. Craigo, S. R. Carr, H. M. Wolfe, D. W. Bianchi and M. D’Alton. 2005. Impact of maternal age on obstetric outcome. Obstetrics and Gynecology 105(5 Pt 1): 983-990.
Delpisheh A., L. Brabin, E. Attia and B. J. Brabin. 2008. Pregnancy late in life: a hospital-based study of birth outcomes. Journal of Women’s Health (Larchmt) 17(6): 965-970.
Doherty D. A., E. F. Magann, J. Francis, J. C. Morrison and J. P. Newnham. 2006. Prepregnancy body mass index and pregnancy outcomes. International Journal of Gynaecology and Obstetrics 95(3): 242-247.
Goodman A. H. 2000. Why genes don’t count (for racial differences in health). American Journal of Public Health 90(11): 1699-1702.
Groth S. 2006. Adolescent gestational weight gain: does it contribute to obesity? MCN; American Journal of Maternal Child Nursing 31(2): 101-105.
Hillier T. A., K. L. Pedula, M. M. Schmidt, J. A. Mullen, M. A. Charles and D. J. Pettitt. 2007. Childhood obesity and metabolic imprinting: the ongoing effects of maternal hyperglycemia. Diabetes Care 30(9): 2287-2292.
Hilson J. A., K. M. Rasmussen and C. L. Kjolhede. 1997. Maternal obesity and breast-feeding success in a rural population of white women. American Journal of Clinical Nutrition 66(6): 1371-1378.
IOM (Institute of Medicine). 1990. Nutrition During Pregnancy. Washington, DC: National Academy Press.
IOM. 1991. Nutrition During Lactation. Washington, DC: National Academy Press.
IOM. 1992. Nutrition During Pregnancy and Lactation: An Implementation Guide. Washington, DC: National Academy Press.
Joseph K. S., A. C. Allen, L. Dodds, L. A. Turner, H. Scott and R. Liston. 2005. The perinatal effects of delayed childbearing. Obstetrics and Gynecology 105(6): 1410-1418.
Kim S. Y., P. M. Dietz, L. England, B. Morrow and W. M. Callaghan. 2007. Trends in prepregnancy obesity in nine states, 1993-2003. Obesity (Silver Spring) 15(4): 986-993.
Kugyelka J. G., K. M. Rasmussen and E. A. Frongillo. 2004. Maternal obesity is negatively associated with breastfeeding success among Hispanic but not Black women. Journal of Nutrition 134(7): 1746-1753.
Li R., S. Jewell and L. Grummer-Strawn. 2003. Maternal obesity and breast-feeding practices. American Journal of Clinical Nutrition 77(4): 931-936.
NHLBI (National Heart, Lung, and Blood Institute). 1998. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. National Institutes of Health Publication 98-4083. Washington, DC: National Institutes of Health.
NRC (National Research Council). 1970. Maternal Nutrition and the Course of Pregnancy. Washington, DC: National Academy Press.
NRC-IOM. 2007. Influence of Pregnancy Weight on Maternal and Child Health. Workshop Report. Committee on the Impact of Pregnancy Weight on Maternal and Child Health. Board on Children, Youth, and Families, Division of Behavioral and Social Sciences and Education and Food and Nutrition Board, Institute of Medicine. Washington, DC: The National Academies Press.
Ogden C. L., M. D. Carroll, L. R. Curtin, M. A. McDowell, C. J. Tabak and K. M. Flegal. 2006. Prevalence of overweight and obesity in the United States, 1999-2004. Journal of the American Medical Association 295(13): 1549-1555.
Oken E., E. M. Taveras, K. P. Kleinman, J. W. Rich-Edwards and M. W. Gillman. 2007. Gestational weight gain and child adiposity at age 3 years. American Journal of Obstetrics and Gynecology 196(4): 322 e321-e328.
Suitor C. W. 1997. Maternal Weight Gain: A Report of an Expert Work Group. Arlington, VA: National Center for Education in Maternal and Child Health.
Taffel S. M., K. G. Keppel and G. K. Jones. 1993. Medical advice on maternal weight gain and actual weight gain. Results from the 1988 National Maternal and Infant Health Survey. Annals of the New York Academy of Sciences 678: 293-305.
Viswanathan M., A. M. Siega-Riz, M.-K. Moos, A. Deierlein, S. Mumford, J. Knaack, P. Thieda, L. J. Lux and K. N. Lohr. 2008. Outcomes of Maternal Weight Gain, Evidence Report/Technology Assessment No. 168. (Prepared by RTI International-University of North Carolina Evidence-based Practice Center under contract no. 290-02-0016.) AHRQ Publication No. 08-E-09. Rockville, MD: Agency for Healthcare Research and Quality.
WHO (World Health Organization). 1995. Physical status: the use and interpretation of anthropometry. Report of a WHO Expert Committee. World Health Organization Technical Report Series 854: 1-452.
Yeh J. and J. A. Shelton. 2005. Increasing prepregnancy body mass index: analysis of trends and contributing variables. American Journal of Obstetrics and Gynecology 193(6): 1994-1998.
Website: