6
Cardiovascular Health Promotion Early in Life
The risk factors for cardiovascular disease (CVD) in adults are now well established. However, emerging evidence highlights the importance of exposures and experiences throughout the life course, beginning as early as the prenatal period, on the subsequent development of CVD. As a result, there are opportunities for intervention during the early years of life that can form a crucial component of the global effort to reduce the burden of CVD. This chapter describes the determinants of CVD that have origins early in life, followed by a discussion of the effects of childhood health promotion and prevention initiatives on later CVD risk.
This chapter, consistent with the scope of this report as described in Chapter 1, focuses on the accumulation starting early in life of risk for coronary heart disease and stroke This is not intended to underemphasize the importance of treating and preventing congenital heart diseases and other cardiovascular diseases in childhood, including prevention and treatment of streptococcal infections to prevent rheumatic heart disease, which exacts a high toll on children in low and middle income countries and was discussed in more detail in Chapter 2.
In addition, although the emerging epidemiological evidence is compelling for the importance of childhood and adolescence in the development of risk for CVD, this chapter is not intended to imply that attention should be drawn away from much-needed intervention approaches to reduce risk in adults. Indeed, there is not sufficient low and middle income country evidence on intervention effectiveness, health impact, or cost-effectiveness analyses to conclude that childhood prevention alone is a top priority for widespread implementation.
Rather, the aim of this chapter is to highlight several important messages. First, although evidence has not fully elucidated the onset of risk in early childhood, well-documented trends on youth tobacco use and childhood obesity present an immediate obstacle to achieving future reductions in CVD disease burden. Second, those already working in child health globally should take chronic disease prevention into consideration where there are relatively feasible and evidence-based interventions available in order to achieve not only short-term child outcomes but also to promote lifelong health. Third, the impact of health promotion and health education in children on adult CVD outcomes as well as the effectiveness of active CVD prevention programs in early childhood, youth, and adolescence in low and middle income countries are areas to be emphasized for further intervention research.
A summary framework of opportunities to promote lifelong heart health during development and to engage the next generation in the fight against CVD and related chronic diseases is illustrated in Figure 6.1.
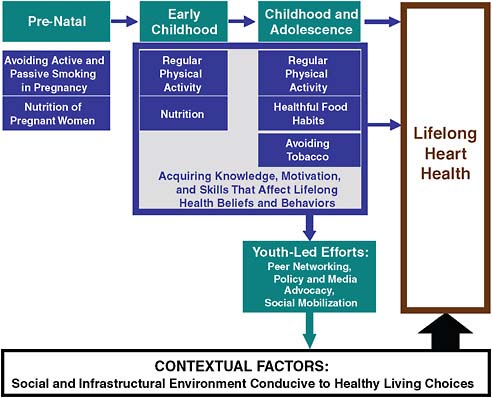
FIGURE 6.1 Growing toward heart health: Influences and opportunities into adulthood.
ASSOCIATION BETWEEN EARLY LIFE FACTORS AND SUBSEQUENT RISK FOR CVD
Prenatal, Infancy, and Early Childhood
There is growing recognition in developing and developed countries, based on recent data emanating from prospective cohort studies, of the importance of the fetal and early childhood periods in the onset of CVD later in life (Aboderin et al., 2002; Victora et al., 2008; Walker and George, 2007; WHO, 2009). The influences during this period include maternal factors during pregnancy, such as smoking, obesity, and malnutrition, and factors in infancy and early childhood, such as breastfeeding, low birth weight, and undernutrition, especially when coupled with rapid weight gain later in childhood.
Maternal smoking during pregnancy has been linked to CVD-related risk factors. It has been consistently associated with increased childhood obesity independent of other risk factors (Oken et al., 2008). This raises the concern that the increasing trend of smoking among young women in the developing world, described in Chapter 2, could contribute to increased prevalence of childhood obesity and obesity-related diseases in those populations.
A number of studies have examined the effects of maternal obesity on the body weight of their children; however, the evidence is inconsistent. Two cohort studies in the United States found that excessive weight gain or maternal obesity during pregnancy was associated with overweight and obesity in the children at ages 3 and 4 years (Gillman et al., 2008; Whitaker, 2004). Similarly, a cohort study in Finland found that mothers’ body mass index (BMI) was positively associated with their sons’ BMI in childhood (Eriksson et al., 1999). However, the recent Avon Longitudinal Study of Parents and Children (ALSPAC) study in the United Kingdom found no association between maternal BMI and child BMI (Davey Smith, 2008; Davey Smith et al., 2007). Furthermore, several researchers have expressed methodological concerns about the retrospective cohort studies that have been used thus far to assess the relationship between maternal and child BMI, asserting that such studies cannot account for confounding variables such as postnatal eating habits of children with obese parents (Davey Smith, 2008).
Another factor that appears to influence risk for long-term cardiovascular health is breastfeeding. Breastfeeding has been found to not only reduce childhood morbidity and mortality but also to be weakly protective against obesity later in life (Bhutta et al., 2008; Gluckman et al., 2008). However, the promotion of breastfeeding must be considered in coordination with other global health efforts so as not to encourage the spread of
some infectious diseases, including HIV, which can be transmitted through breast milk.
A link to adult CVD risk has also been made for maternal malnutrition, low birth weight, and undernutrition in infancy, especially when followed by rapid weight gain. These have been associated with increased risk of CVD and diabetes in adulthood (Barker and Bagby, 2005; Caballero, 2005; Gluckman et al., 2008; Prentice and Moore, 2005). In what is known as the developmental origins theory of CVD, disruptions to the nutritional, metabolic, and hormonal environment at critical stages of development (in utero and in the first years of life) are hypothesized to lead to permanent “programming” of the body’s structure, physiology, and metabolism that translate into pathology and disease, including CVD, later in life (Barker, 1997, 1998, 2007). The exact physiological mechanisms through which this programming occurs are not yet fully elucidated; however, there is evidence that fetal and early postnatal undernutrition can cause metabolic, anatomic, and endocrine adaptations that affect the hypothalamic-pituitary-adrenal axis, lipoprotein profiles, and end organ glucose uptake, among other processes (Prentice and Moore, 2005).
Support for the developmental origins theory of CVD comes from a number of retrospective, and more recently prospective, cohort studies in various populations. Studies in the United Kingdom, the United States, Finland, and India found that fetal undernutrition (as measured by low birth weight, small birth size, ratio of birth length to weight, or ratio of head circumference to weight at birth), followed by a rapid catch-up growth from childhood to early adolescence was significantly associated with the later development of CVD in both men and women (Barker et al., 2005; Eriksson et al., 1999; Forsen et al., 1999; Osmond and Barker, 2000; Stein et al., 1996). Early undernutrition followed by catch-up growth during childhood has also been associated with subsequent hypertension and type 2 diabetes (Barker, 1998; Osmond and Barker, 2000). More recently, Stein et al. (2005) reviewed nutritional studies from China, India, Guatemala, Brazil, and the Philippines and found that growth failure between conception and age 2 years and accelerated weight gain from childhood to adolescence were associated with significantly increased risk of diabetes and CVD in adulthood. In another developing country cohort, a longitudinal study of more than 3,000 children in South Africa also found that the combination of low birth weight and rapid growth in childhood was associated with an increased risk of obesity and risk factors for type 2 diabetes (Crowther et al., 1998; Richter et al., 2007). This emerging data on the effects of rapid weight gain after early undernutrition have prompted some researchers to suggest a shift from the original “fetal origins” hypothesis to an “accelerated postnatal growth hypothesis” of CVD (Singhal et al., 2003, 2004).
Some researchers have expressed reservations about interpreting the available data in this area due to concerns that much of the research to date has not sufficiently accounted for the confounding impact of the social and economic environment during early childhood (Davey Smith, 2007, 2008). In addition, although there is a growing body of evidence exploring the effects of undernutrition in infancy followed by rapid catch-up growth later in childhood on CVD, diabetes, obesity, and metabolic disease in adulthood, evidence is mixed on the effects of rapid growth between birth and age 2 years (Victora et al., 2008). Singhal et al. (2004) found that rapid weight gain within the first 2 weeks after birth was associated with adverse cardiovascular effects later in life. On the other hand, several recent reviews and meta-analyses of studies examining early undernutrition found rapid weight gain between birth and age 2 years was associated with lower morbidity and mortality in low and middle income countries (Black et al., 2008; Victora et al., 2008).
The emerging evidence on the association between low birth weight followed by rapid growth in childhood and subsequent risk for CVD raises important considerations for addressing global CVD because low birth weight and exposure to undernutrition in utero and in infancy are common in many developing countries (Caballero, 2009; Kelishadi, 2007). For example, the 2005-2006 National Family Health International Survey in India found that more than 40 percent of children under age 3 were underweight (International Institute of Population Studies, 2005-2006). In addition, the coexistence of these high rates of undernutrition in utero and early childhood with the potential for overnutrition in later childhood and adulthood may accelerate the epidemics of obesity and CVD in populations that undergo rapid nutrition transitions (Victora et al., 2008). Identifying the most prudent strategy for nourishing low birth weight and stunted infants while neither compromising their childhood health nor increasing their risk for cardiovascular and metabolic complications later in life will be an important area of future research.
Childhood and Adolescence
The acquisition and accumulation of risk for CVD continues in childhood and adolescence (Celermajer and Ayer, 2006; Freedman et al., 2001; Strong et al., 1999). Unhealthful lifestyle practices such as consumption of high calorie and high fat foods, tobacco use, and physical inactivity begin in childhood, introducing major behavioral risks for CVD. Childhood adversity also influences adult cardiovascular health. In addition, there is also an emerging body of evidence on the presence of biological risk factors in children and youth, including pathophysiological processes associated with heart disease that can be seen as early as childhood.
Childhood Obesity and CVD Risk
Childhood obesity is associated with multiple risk factors for CVD, which are amplified in the presence of overweight and persist from childhood into adulthood. These risk factors include hyperlipidemia, high blood pressure, impaired glucose tolerance and high insulin levels, as well as metabolic syndrome. It has been estimated that 60 percent of overweight children possess at least one of these risk factors that can lead to CVD in adulthood (Freedman et al., 1999). This is especially important in terms of implications for global CVD because, as will be described later in this chapter, the prevalence of childhood obesity is increasing in developing countries (WHO, 2008b).
The Bogalusa Heart Study, conducted in the United States in a community near New Orleans, examined the natural history of CVD among children and young adults (Berenson, 2002; Freedman et al., 2001). Repeated cross-sectional and longitudinal studies with participants aged 5 to 38 years suggested that overweight children and adolescents are more likely to become obese adults. A large prospective cohort study from Denmark also found that higher BMI during childhood is associated with an increased risk of coronary heart disease (CHD) in adulthood and that the elevated risk associated with childhood obesity increases with the age of the child (Baker et al., 2007).
Several studies in developed countries have reported that the prevalence of hypertension is significantly higher in obese children as compared to normal-weight children (Guillaume et al., 1996; Rosner et al., 2000; Sorof and Daniels, 2002). Obese children are at a three-fold higher risk of developing hypertension compared to nonobese children, and the risk continues to increase with higher BMI values (Sorof and Daniels, 2002). Similar findings have been reported in studies across developing countries. Verma et al. (1994) found that the prevalence of hypertension was 13.7 percent in obese children as compared to 0.4 percent in nonobese children in Punjab, India.
Childhood obesity is associated with impaired glucose tolerance (Sinaiko et al., 2001) and diabetes mellitus (Rocchini, 2002; Sinha et al., 2002) among children and adolescents. Over the years it has been observed that the upsurge in the prevalence of obesity among children and adolescents has been paralleled by an increasing prevalence of diabetes mellitus. This finding is significant, especially in developing countries such as India and China, which have the highest number of persons with diabetes in the world (Hossain et al., 2007). Sinha et al. (2002) found 25 percent of children (4-10 years) and 21 percent of adolescents (11-18 years) to have impaired glucose tolerance in the United States.
Metabolic syndrome is associated with childhood obesity, as estab-
lished by several studies in developed (Cook et al., 2003; Cruz et al., 2004) as well as developing countries (Agirbasli et al., 2006; Csabi et al., 2000; Kelishadi, 2007). Singh et al. (2007) estimated the prevalence of metabolic syndrome using the National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP III) criterion in adolescents aged 12-17 years in Chandigarh, India, to be 4.2 percent with no gender differences. Moreover, the study also estimated that 11.5 percent of the overweight adolescents and 1.9 percent of those who were of normal weight met the criterion of metabolic syndrome, suggesting a significant difference. Similar findings have been noted in studies conducted in other low and middle income countries (Agirbasli et al., 2006; Csabi et al., 2000; Kelishadi, 2007).
Childhood Adversity and CVD Risk
Stressful or traumatic circumstances in childhood also appear to increase the risk of CVD later in life. The Adverse Childhood Experiences study found that adults exposed to adversities such as abuse, household dysfunction (defined as the presence of alcohol or substance abuse, mental illness, or criminal behavior in the house), or neglect during childhood were significantly more likely to smoke, be physically inactive, be severely obese, and be depressed or angry, all risk factors for CVD. There was a dose–response relationship between the number of childhood exposures to adverse experiences and the number of risk factors for chronic disease later in life (Dong et al., 2004; Felitti et al., 1998). In a further analysis of the study data, Dong et al. (2004) found a similar graded relationship between the number of childhood adverse experiences and risk of ischemic heart disease in adulthood.
In addition to adverse experiences, growing up poor has also been linked to an increased risk of developing and dying from CVD. A review of prospective and cross-sectional studies in high income countries reported that the vast majority found an association between poor socioeconomic circumstances in childhood and greater risk of CHD, angina, stroke, and atherosclerosis in adulthood. This association was independent of the economic circumstances of study participants in adulthood (Galobardes et al., 2006).
Initiation of Tobacco Use
Tobacco use initiated in childhood or adolescence is another factor that leads to early vascular dysfunction and later adult CVD. There are an array of biological, social, environmental, and interpersonal factors that influence experimentation and maintenance of tobacco use among youth. Nicotine is a highly addictive substance. Cigarettes and other forms of tobacco act as
carriers of nicotine, which affects the brain by reinforcing behavior, altering mood and creating a need that did not exist prior to drug exposure (Oates et al., 1988). Once youth start using tobacco, many of them become addicted to nicotine. After reaching the brain, nicotine stimulates the reward pathways in the brain and stimulates the release of dopamine, which is a neurotransmitter associated with addiction (Glover et al., 2003). The brains of children and adolescents, which are still in developmental stages, are highly susceptible to nicotine addiction (Difranza et al., 2002). The number of cigarettes and the duration of smoking that is necessary for making a person addicted are lower in adolescents than in adults. A study by Difranza et al. (2002) showed that some adolescents begin to experience loss of control over their smoking within weeks of smoking the first cigarette.
The U.S. Surgeon General’s report of 1994, Preventing Tobacco Use Among Young People, described four broad categories of psychosocial risk factors that are linked to the initiation of the habit of smoking: sociodemographic, behavioral, personal, and environmental (U.S. Department of Health and Human Services, 1994). The specific sociodemographic factors associated with tobacco use are low socioeconomic status, male gender, low parental education, and single-parent households (Buttross and Kastner, 2003; Tyas and Pederson, 1998). Various behavioral and personal factors are poor academic achievement, low self-esteem, and peer influences (Buttross and Kastner, 2003; Tyas and Pederson, 1998). Environmental influences include smoking by parents, siblings, and peers; absence of rules prohibiting smoking at home (Buttross and Kastner, 2003; Tyas and Pederson, 1998); and the influence of films, television, and media campaigns (Prokhorov et al., 2006). Although these factors leading to initiation of tobacco use have been widely studied in developed countries, the evidence from youth in developing countries remains relatively sparse.
Early CVD Pathology in Childhood
Many of the risk factors described above have been shown to be related to surrogates for CVD pathophysiology that can already be observed in childhood, such as increased left ventricular mass, left ventricular systolic dysfunction, and higher arterial thickness in overweight children (Johnson et al., 1999; Laird and Fixler, 1981; Sorof et al., 2003). Although the predictive value of elevated C-reactive protein (CRP) and raised intima media thickness (IMT) are still under debate, it is worth noting that these have been demonstrated in obese children, along with impaired endothelial function of arteries as well as arterial stiffness and calcification (Celermajer and Ayer, 2006). BMI measured in childhood has been shown to be significantly associated with carotid IMT measured in adulthood. The Bogalusa Heart
Study suggested that low-density lipoprotein (LDL) cholesterol and BMI in childhood are independent risk factors for increased carotid IMT in young adulthood, whereas the Cardiovascular Risk in Young Finns study suggested that systolic blood pressure, LDL cholesterol, smoking, and BMI measured at 12-18 years predict adult IMT (Li et al., 2003; Raitakari, 2003).
The Pathobiological Determinants of Atherosclerosis in Youth Study study also suggested that atherosclerosis, which is a major pathological cause of coronary artery disease, has its origins in childhood (Strong et al., 1999). Fatty streaks in children are associated with risk factors such as dyslipidemia, hypertension, cigarette smoking, and diabetes mellitus (Celermajer and Ayer, 2006). Berenson (2002) suggested that fatty streaks start appearing in the aorta and other arteries as early as 3 years of age, and high maternal cholesterol levels in the ante-natal period contribute to their formation. Fatty streaks and raised lesions in the arteries, especially the aorta and coronary and carotid arteries, increase rapidly in prevalence and extent during the 15- to 34-year age span.
In summary, the evidence cited here clearly suggests that the behavioral and biological risk factors for CVD in adulthood frequently start appearing in childhood and adolescence. The risk factors are genetic, environmental, and behavioral and track from childhood to adulthood leading to premature CVD in adulthood. Hence, efforts for the prevention of CVD should begin right from childhood and adolescence when lifestyle habits are being formed, especially with respect to diet and physical activity, as well as during the prenatal period with respect to maternal nutrition and health.
GLOBAL TRENDS IN MAJOR DETERMINANTS OF CVD RISK EARLY IN LIFE
An understanding of the trends fueling the growing burden of childhood risk factors for chronic diseases is imperative if a reversal is to be brought about through public policy and programs. The following sections offer a brief overview of the global trends in the major determinants of CVD risk in children and youth.
Trends in Tobacco Use in Children and Adolescents
As described in Chapter 2, tobacco use is a growing worldwide epidemic (Reddy and Gupta, 2004). It is a risk factor for many chronic diseases and is the single most important preventable cause of death in the world today (WHO, 2008a). The most susceptible time for initiating tobacco use is during adolescence and early adulthood, before the age of 18 years (U.S.
Department of Health and Human Services, 1994), and the prevalence of tobacco use is increasing among children and adolescents. Due to this increasing prevalence, tobacco use is often referred to as a “pediatric disease” or a “pediatric epidemic” (Committee on Environmental Health et al., 2009; Perry et al., 1994). In India, for example, an estimated 5500 adolescents start using tobacco every day, joining the 4 million young people under the age of 15 years who already regularly use tobacco (Rudman, 2001).
The Global Youth Tobacco Survey (GYTS) provides some insight into global trends in tobacco consumption among youth. GYTS is a school-based survey of students aged 13-15 years that was undertaken at 395 sites in 131 countries. GYTS reported that, globally, about 10 percent of adolescents currently use tobacco in any form (Asma, 2009). Nearly 25 percent of them try their first cigarette before the age of 10 years, and 19 percent are susceptible to initiating smoking during the next year (Global Youth Tobacco Survey Collaborative Group, 2002).
The GYTS estimates also revealed differences within a country or a region, thereby showing how national estimates can obscure within-country differences and highlighting the need to look at subnational data. For example, India had both the highest and lowest rates of current use of any tobacco product (62.8 percent in Nagaland and 3.3 percent in Goa) (Global Youth Tobacco Survey Collaborative Group, 2002). These variations revealed by the GYTS indicate that tobacco-reduction strategies targeting youth will need to be adapted to local contexts with careful consideration paid to the unique factors influencing differential burden in each country, such as geographic regions or ethnic groups. In South Africa, for example, factors associated with race may play an important role in influencing adolescents’ decision to smoke (Panday et al., 2007a, 2007b). Adolescents in different ethnic groups had different responses to the importance of information provided on the pros and cons of smoking, contextual factors, and preexisting self-efficacy (Panday et al., 2005). More research regarding the nuances of adapting approaches to local culture and context is an important priority if the global health community hopes to reduce the startlingly high rates of tobacco use among the world’s youth.
Lastly, the GYTS data provide information about the exposure of children to environmental tobacco smoke. Almost half of the students (44 percent) reported that they were exposed to tobacco smoke at home and greater than 6 in 10 students (52 percent) reported being exposed to tobacco smoke in public places (Warren et al., 2006). This is of particular concern given the causal association that has been established between exposure to secondhand smoke and the prevalence of impaired vascular function, metabolic abnormalities, and chronic debilitating conditions (Peto et al., 1996).
As an example of the status of tobacco use on a national scale, the
National Youth Risk Behavior Survey, conducted with more than 10,000 school children in South Africa in 2002, revealed that 31 percent of students had smoked, and passive tobacco smoke exposure levels ranged from 56-84 percent (Reddy et al., 2003). In addition, since the study looked at a wide variety of potential risk factors, including violence-related intentional and unintentional injuries, mental health and wellness indicators, and nutrition and physical activity levels, it provided a more complete, well-rounded picture of adolescent risk behaviors, reinforcing the need to look more closely at the complex interactions that contribute to youth health status (Reddy et al., 2003). However, as it was the first study of its kind in that country, few conclusions on temporal trends can be drawn. If the study were to be repeated regularly, it could provide information on the impact of a number of national-level policy initiatives implemented in order to bring more focus onto youth and adolescent health.
Trends in Childhood Obesity
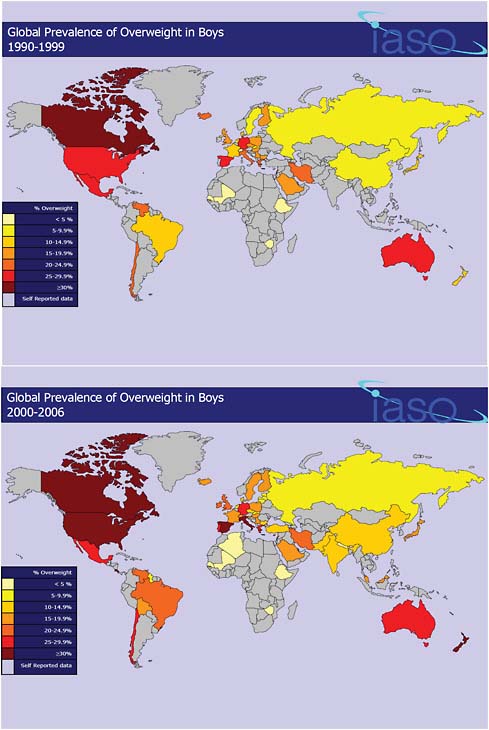
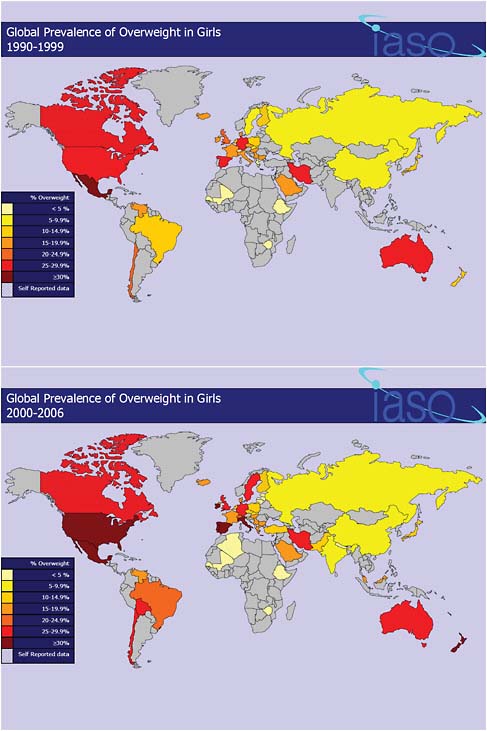
The total global prevalence of overweight in children between the ages of 5 and 17 years is 10 percent, varying from under 2 percent in SubSaharan Africa to more than 30 percent in the United States (Bhardwaj et al., 2008). Although still highest in high income countries, the epidemic of childhood obesity has spread from the United States and other developed countries to low and middle income countries, especially in urban areas (Prentice, 2006). Figures 6.2 and 6.3 provide an illustration—compiled by the International Association for the Study of Obesity (IASO)—of worldwide trends in the prevalence of overweight among boys and girls, respectively, over the past two decades. While the data is not age-standardized across countries or directly comparable across years, the figures suggest a trend of growing prevalence of overweight among children in an increasing number of developing countries.
For example, among school-going children and adolescents in India (rural and urban) aged 10-18 years, the prevalence of overweight was 1.7 percent in boys and 0.8 percent in girls in the year 2007 (WHO Global InfoBase, 2008). In the Middle East, Kuwait has among the highest prevalence of overweight (30 percent in boys; 31.8 percent in girls) and obesity (14.7 percent in boys; 13.1 percent in girls) among children and adolescents (10-14 years) (Al-Isa, 2004; Kelishadi, 2007). Figure 6.4 shows the prevalence of overweight and obesity among boys and girls aged 6-18 years in developing countries, demonstrating the high prevalence in the Middle East and Central and Eastern Europe. Among younger children, obesity is not a major public health issue in Asia and Sub-Saharan Africa, but in countries of Latin America, the Caribbean, the Middle East, North Africa, and Cen-
tral and Eastern Europe, its prevalence in children below 5 years of age is as high as that in the United States (Martorell et al., 2000).
Some of the most common factors to which the growing prevalence of obesity has been attributed are increasing affluence among populations and their increasing urbanization (Misra and Khurana, 2008). However, the most important determinants that have recently been widely studied are nutrition and physical activity transitions. These have direct implications on the energy imbalance of populations and are widely accepted as the cause for an increase in obesity and chronic diseases.
The present global population is in the midst of a unique phenomenon in which it is not uncommon for both undernutrition and obesity to coexist in the same populations, and indeed even in the same household. Undernutrition, with its associated communicable diseases and micronutrient deficiencies like anemia, has been the hallmark of the low and middle income countries of Africa, Latin America, and South Asia for decades. In India, for instance, between the years of 2005 and 2006, 40 percent of all children under the age of 3 years were underweight, 22 percent of newborns were born with low birth weight, and 55.3 percent of women and 69.5 percent of children were anemic (International Institute of Population Studies, 2005-2006). In one survey in South Africa, 9 percent of students were found to
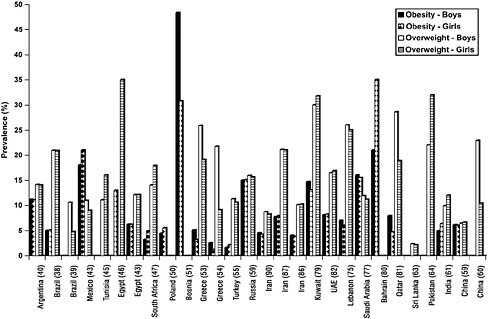
FIGURE 6.4 Prevalence of overweight and obesity among children aged 6-18 years in developing countries.
SOURCE: Kelishadi, 2007.
be either underweight or wasting, while at the same time 16.9 percent were found to be either overweight or obese (Reddy et al., 2009).
Policy makers are faced with a conundrum of sorts in addressing the dietary risks that contribute to the growing prevalence of obesity in developing countries while ensuring that the diets of children are both calorically adequate and nutritionally appropriate. As mentioned previously, there is emerging evidence that undernourishment followed by rapid weight gain in infancy is associated with increased risk of cardiovascular disease later in life. Thus it is possible that well-intentioned interventions targeting undernutrition, such as infant feeding initiatives, school meal programs, and free meals for family members may lead to an increase in adiposity among its target populations. For example, an evaluation of a school feeding program in Chile found that more than 50 percent of the children under the age of 6 years were reported to be obese (Kain et al., 1998). There is a growing need for efforts in maternal and child health and global food programs aimed at reducing malnutrition among children to take into account these potential negative impacts when developing their programmatic nutritional guidance and policies for the distribution of food products. With careful coordination, programs such as Save the Children’s “Survive to 5” initiative (2010) can successfully address the challenges of reducing child hunger while not unintentionally increasing their future risk of cardiovascular disease. Such programs will thereby support not only shorter-term childhood outcomes but also promote future lifelong health.
In addition to changes in nutrition, perceived unsafe neighborhoods, limited open spaces, and inappropriate sports infrastructure can contribute to declines in physical activity, another key determinant of obesity and CVD risk. For example, the rates of participation in organized sport and physical education classes in Australia and the United Kingdom have decreased substantially in school-going children (Dollman et al., 2005). Although data on physical activity among children is generally sparse in developing countries, a 2002 national survey in South Africa found that 37.5 percent of school children in grades 8-11 were physically inactive, classified as not engaging in moderate or vigorous physical activity at least 3 or 5 days per week, respectively (Reddy et al., 2003). Sedentary leisure-time pursuits are also increasing, with more children turning to indoor entertainment. For example, in the United States, children aged 8-18 years watch an average of more than 3 hours of television daily (Roberts and Foehr, 2004). The ownership of televisions has increased dramatically in some developing countries such as China (Popkin and Gordon-Larsen, 2004), but there is limited data from developing countries on hours of television watched by children in particular. In South Africa, 25.2 percent of school-aged children were found to spend more than 3 hours per day watching television or playing computer or videogames (Reddy et al., 2003).
Trends in Marketing That Influence Tobacco Use and Nutrition
A common, although mistaken, belief about chronic diseases is that they arise out of irresponsible personal lifestyle decisions made by individuals—this is only partially true. This tendency to blame the individual for faulty lifestyle choices, and hence onset of disease, has in part led to the current situation of inadequate response from the international public health community to combat the burden. However, broader environmental and socioeconomic determinants are also at play, which lie far from the control of the individual (Yach et al., 2004). Marketing—which has the principal aim of persuasion, pushing a passive observer into becoming an active consumer of a product or service—has the potential of magnifying exposure to CVD risk factors. Marketing related to CVD risk factors is part of the broader social determinants underlying behavioral and lifestyle changes occurring among children and young adults that increase their risk for developing CVD later in life.
Children and teenagers may be disproportionately vulnerable to the effects of marketing. Children under the age of 8 years lack the level of cognitive sophistication required to understand the true persuasive motive of advertising, which has led psychologists and child development experts to view this age group as vulnerable to the effects of the marketing of potentially unhealthy products (John, 1999). While the ability to process advertisements develops by age 8 years, preadolescents (8- to 10-year-olds) do not necessarily process the information they get from ads critically (Strasburger, 2001). Moreover, adolescents, going through a physically and emotionally trying period, might be easily swayed by advertisements focusing on issues related to identity, peer culture, emotions, and sexuality (Story and French, 2004). In addition, children are targeted due to their indirect influence over household food purchases, their direct spending on food and beverages, as well as their potential as future adult consumers (Story and French, 2004). Studies have found that the amount of time spent watching TV predicts the number of times children ask for products at the grocery store, with a majority of the products being the ones advertised on TV (Arnas, 2006; Galst and White, 1976; Taras et al., 1989). One of the main aims of such advertising is to get children to convince their parents to buy their products, what marketers call “pester power” or “nag factor” (Center for Science in the Public Interest, 2003). Thus aggressive marketing of unhealthful products can be seen as a part of the larger socioeconomic environment that compels the youth to adopt lifestyles that are detrimental to their health.
One of the biggest concerns in marketing has been the impact of tobacco advertising on children and adolescents. Tobacco campaigning is often targeted at younger age groups and has tremendous potential to affect their perceptions of smoking, glossing over its harmful effects, and giving
them the image of social acceptability, thereby encouraging them to try smoking early in life. Because smoking is highly addictive, any attempt to try smoking at an early age can lead to serious addictions lasting late into adulthood. Several studies have demonstrated that cigarette retail marketing increases the likelihood of youth smoking uptake (Slater et al., 2007), receptivity to tobacco promotion among adolescents increases their chances of progressing from experimentation to established smoking (Choi et al., 2002), and exposure and receptivity to tobacco advertising are highly associated with tobacco use among schoolchildren (Arora et al., 2008).
It has been argued that the role played by marketing in accelerating the tobacco epidemic has parallels in the current obesity epidemic that is affecting increasingly younger populations today (Chopra and Darnton-Hill, 2004). The food industry in the west, and now even in the developing world, relies heavily on marketing to promote global brands. In the United States, for instance, the food industry spends $30 billion on direct advertising, more than any other industry in the country (Chopra and Darnton-Hill, 2004), and the prime target population is children and adolescents. According to one of the most recent reports on food advertising on television aimed at children, published by the Henry J. Kaiser Family Foundation (2007), 2- to 7-year-olds are exposed to 4,400, 8- to 12-year-olds to 7,600, and 13- to 17-year-olds to 6,000 food ads per year. These ads are not for nutritious foods; according to the former report, 50 percent of all ad time during children’s shows is for food, out of which 34 percent are for candies and snacks, 28 percent are for cereal, 10 percent are for fast food, and only 4 and 1 percent, respectively, are for dairy products and fruit juices. The report found that there were no ads for fruits and vegetables during children’s television shows. With market liberalization and globalization, the effects of promotional marketing have reached all corners of the developing world. This is clearly demonstrated by global fast food and soft drink companies, which have been expanding internationally at a rapid pace. Of particular interest is a marketing strategy used by these companies, termed “glocal” marketing, the main thrust of which is to create demand by replacing traditional food consumption habits with their products, and then to increase demand by applying global marketing principles. Even in these local markets, their prime target populations are children and teenagers (Hawkes, 2002).
Several studies have shown the influence food advertising can have on children’s food choices. Gorn and Goldberg (1982) experimentally manipulated the kind of ads seen by children attending a camp for a month and found that the ones that had been exposed to fruit commercials most often chose orange juice as a beverage, while the ones exposed to candy commercials picked the least amount of fruits and juice as snacks. Children and adolescents are bombarded with food advertisements and promotions
from various channels. While the television is the most common mode of promotion in the United States for food products, multiple other channels are used, including in-school advertising, the Internet, product placements, kids’ clubs, branded toys, and cross-promotions, (i.e., utilizing cartoon and movie characters, musicians, and athletes) (Story and French, 2004). Other indirect forms of marketing used include public-relations marketing, service-related marketing, sports sponsorship, and philanthropy (Hawkes, 2002). This multichannel targeting amplifies the effect of marketing on the food habits of children.
Conclusion 6.1: Accumulation of cardiovascular risks begins early in life, and strong evidence supports the value of starting cardiovascular health promotion during pregnancy and early childhood and continuing prevention efforts throughout the life course. Maternal and child health programs and other settings that already serve children in low and middle income countries offer an opportunity to provide care that takes into account not only shorter-term childhood outcomes but also long-term healthful behavior and reduction of chronic disease risk.
INTERVENTION APPROACHES AND OPPORTUNITIES
School-Based Programs
In places where school attendance is compulsory or attendance rates are high the school environment presents a particularly ideal location for health promotion interventions, because on school days, these children spend nearly half of their waking hours in school. However, the sizeable variations in both primary and secondary school attendance rates must be taken into account when considering the potential effectiveness and prioritization of school-based initiatives. While 80 percent of boys and 77 percent of girls reportedly attend primary schools in developing countries, in the least developed nations only 65 percent of males and 63 percent of females attend school. The lowest percentages are seen in West and Central Africa, while the highest are in Latin America and the Caribbean and the Commonwealth of Independent States. However, within each of these regions, there exists additional variation at the country level. When looking at secondary school—the ages at which youth are most susceptible to risk behavior development—those numbers drop to 48 percent male and 43 percent female, respectively, for developing and 26 percent male and 24 percent female, respectively, for least developed nations (UNICEF, 2008).
In addition, evaluations of school-based programs must be interpreted with caution. The lack of blinding of study personnel and inherent biases
associated with self-reported data, selection of school sites, and even objective data collection may lead to an overestimation of treatment effects. Also, these programs have not operated or been evaluated over time and on a large scale, so the long-term benefits as well as any potential harmful effects of these interventions merit additional study. In addition, it is important to note that the data from low and middle income settings is extremely limited. Regardless of these limitations, the increasing popularity of these types of interventions makes it imperative to examine the benefits of programs that promote everything from increased physical activity and reduced tobacco use to youth empowerment.
In recognition of the importance of targeting youth for health promotion activities, WHO has recently launched the Global School Health Initiative with the goal of increasing the number of “Health-Promoting Schools” worldwide (WHO, 2010a). Of the five identified components of a health-promoting school, the focus on nutrition and food safety programs and opportunities for physical education and recreation directly address two of the key determinants of CVD in youth (WHO, 2010a). In addition to the Global School Health Initiative, the newly formed Mega Country Health Promotion Network has also included a school health component into its mission. Current priorities include the development of a “School-Based Multi-Risk Information Surveillance System,” the development and implementation of pilot programs targeting youth tobacco use, and increasing collaboration effort between members (WHO Mega Country Health Promotion Network, 2001). The annual meetings of both the Global School Health Initative and the Mega Country Health Promotion Network also provide potential opportunities for the kinds of regional dissemination and partnerships that are discussed further in Chapter 8.
School-Based Tobacco Prevention Programs
School-based tobacco prevention is a frequently used mechanism to target youth. Experience in developed countries using school-level interventions for tobacco control has been mixed In recent reviews of school-based smoking prevention, Flay (2009a, 2009b) concludes that these programs can have significant long-term effects if they:
-
include 15 or more sessions over multiple years;
-
include some sessions in high school;
-
use the social influence model and interactive delivery methods;
-
include components on norms, commitment not to use, intentions not to use, and training and practice in the use of refusal and other life skills; and
-
use peer leaders in some role.
Flay estimated that this type of school-based program can reduce smoking onset by 25 to 30 percent, and school plus community programs can reduce smoking onset by 35 to 40 percent by the end of high school.
The findings were based on programs in developed countries due to lack of rigorous research on school-based smoking prevention in developing countries, although some school-based programs in middle income countries (South Africa, China, Thailand, Taiwan, India, and Pakistan) were identified in the review (Flay, 2009b). Elements of successful approaches to smoking prevention can potentially be adapted to be effective in developing countries. However, it can be challenging to adapt a successful school-based program for use with populations in different contexts, especially in other cultures and in varying levels and types of school system infrastructure. It is important to implement with fidelity, to monitor implementation, and to evaluate outcomes. Therefore, the effectiveness and implementation of such adaptation needs to be the subject of research so that the benefits of school-based smoking prevention can be evaluated objectively in low and middle income settings (Flay, 2009a).
Experience in India suggests that multicomponent intervention is effective in delaying onset and reducing tobacco use among youth. An Indo-U.S. collaborative endeavor between the University of Texas and Health Related Information Dissemination Amongst Youth (HRIDAY) is a model of collaboration between researchers in developed and developing countries in adapting and replicating the experience of U.S.-school-based smoking prevention intervention in schools in India. Project HRIDAY was a school-based cluster randomized trial in India of 30 public and private elementary schools. The study showed that an intervention that included information provision, interactive classroom activities, and roundtable discussions reduced experimentation, intentions to use tobacco, and offers of tobacco among the intervention schools (Reddy et al., 2002). Another multicomponent group randomized intervention trial designed and implemented in Indian schools was Project MYTRI (Mobilizing Youth for Tobacco Related Initiatives in India). After a rigorous 2-year tobacco use prevention intervention, students in the intervention schools were significantly less likely than controls to exhibit an increase in cigarette or bidi smoking. They were also less likely to intend to smoke or chew tobacco in the future (Perry et al., 2009). These experiences are now being applied to conduct Project ACTIVITY (Advancing Cessation of Tobacco in Vulnerable Indian Tobacco Consuming Youth), a group randomized trial to test the efficacy of a comprehensive, community-based tobacco control intervention among disadvantaged youth (10-19 years) living in low income communities of Delhi, India (Dell Center for Healthy Living, 2010).
Contrastingly, a recent attempt to “translate” existing school-based smoking prevention programs from the United States and Australia to the
cultural context of South Africa was less successful. Resnicow et al. (2008) conducted a clustered randomized controlled trial of two new school-based approaches, the Life Skills Training model, shown to be effective with inner-city and urban youth in the United States, and the Harm Minimization strategy, which showed significant positive results in an experimental trial in Western Australia, and compared each to the standard tobacco use education. Following the intervention, the two new approaches did not differ significantly in their effect on preventing the initiation of tobacco use among youth. However, significant differences were seen in the approaches between boys and girls, indicating an important area for further study given the rising rates of female tobacco use in many countries (Resnicow et al., 2008). Thus, while many school-based programs currently underway in developed countries have the potential to be effective in developing-country settings, cultural, economic, and social differences may limit the transfer-ability of these efforts. More research is needed regarding what aspects of prevention programs are sensitive to cultural variations and which adaptation strategies may be most effective when bringing an existing program to new environments.
School-Based Childhood Obesity, Physical Activity, Nutrition, and CVD Prevention Programs
In the face of the almost pandemic increase in the rates of chronic diseases over the past decade, the need to improve nutrition and increase physical activity is very apparent. In recent times, many interventions have used schools as the vehicle of change because the school culture is seen as one that fosters and supports physical activity and health. Several school-based obesity prevention and health promotion programs have been successfully implemented and evaluated in high income countries, but published efforts from low and middle income countries are scarce.
Several studies in high income countries have demonstrated some effectiveness in reducing risk among children through efforts to improve nutrition as well as to promote physical activity. These interventions have included components such as school self-assessment; nutrition education; nutrition policy for school meals; social marketing; student involvement and empowerment; curricular enhancements that focus on decreased television viewing, reduced consumption of soft drinks and foods high in total and saturated fat, increased fruit and vegetable intake, and increased moderate and vigorous physical activity; parent outreach; and home-based activities. Thus, there are models of programs that have been effective at changing behavioral risk factors and, in some cases, preventing or reducing overweight and obesity (Foster et al., 2008; Gortmaker et al., 1999; Luepker et al., 1996; Veugelers and Fitzgerald, 2005).
Programs more narrowly focused on increasing physical activity have a somewhat more robust evidence base. It is theorized that a physically active childhood would increase the likelihood of maintaining an active lifestyle throughout adult life, which in turn would enhance adult well-being and reduce the risk of chronic diseases in adulthood (Dobbins et al., 2009; Freedson, 1992). From a health perspective, therefore, it appears logical to encourage youth to engage in regular activity. Several interventions for promoting physical activity and fitness in schools have been evaluated in high income country settings using strategies such as changes in the school physical environment; changes in school curriculum to increase time spent on physical activity, particularly on vigorous physical activity during physical education classes; and provision of play equipment and activity cards (Dobbins et al., 2009).
There is convincing evidence that physical education (PE)-based strategies are effective for increasing and maintaining physical activity in school children. The strategies include increasing frequency of PE (e.g., four times per week), increasing PE duration, increasing activity levels during PE classes, and delivering PE using specialists or trained teachers (Naylor and McKay, 2009). In addition to PE, another strategy is to change the school’s physical environment to be more conducive to physical activity in children. Some studies have indicated that improving playgrounds in schools, providing play equipment to schools, or incorporating activity breaks into the elementary school classroom can have positive effects on improving physical activity levels among students, but few studies have rigorously evaluated these approaches (Naylor and McKay, 2009).
In some cases, interventions have been comprised of a combination of multiple components. These approaches combine health education curricula and school environment with other approaches to improve nutrition and physical activity among children. Strategies to engage parents, as well as community-based strategies, mass media, and policy development have formed a part of some interventions. These combined interventions are typically incorporated into a broader program for obesity or chronic disease prevention. Evidence suggests that longer duration, multicomponent interventions are more effective in bringing about a positive change (Dobbins et al., 2009).
Although evidence from low and middle income countries is scarce, there have been a few studies designed to encourage physical activity in middle income countries. Liu et al. (2008) evaluated the effect of the Happy 10 program (incorporating two 10-minute activity breaks into classes) on the promotion of physical activity and obesity control in two primary schools in Beijing. This pilot study showed significantly improved physical activity levels and increased energy expenditure in the intervention group.
The prevalence of overweight and obesity was significantly reduced in the intervention group compared to the control school.
Jiang et al. (2007) conducted a 3-year multicomponent intervention program in 2,425 children (1,029 children in intervention schools and 1,396 children in control schools) in Beijing. The program involved schools and families and emphasized both nutrition and physical activity The program showed significantly reduced prevalence of overweight and obesity in intervention schools compared to the control schools.
Kain et al. (2004) assessed the impact of a 6-month multicomponent intervention on primary schoolchildren in Chile through changes in adiposity and physical fitness. The intervention included nutrition education for children and parents, “healthier” kiosks, 90 minutes of additional physical activity weekly, a behavioral physical activity program designed to teach children about the benefits of physical activity and an active lifestyle, and active recess. The study showed improved physical fitness in both boys and girls and significantly reduced adiposity only in boys.
In summary, there is sufficient evidence to support the potential effectiveness of school-based promotion programs for children in a limited number of settings that are reasonably analogous to the high income country settings in the program models described here and that have sufficient capacity and motivation for long-term sustainability. However, as described for many of the intervention approaches here and in Chapter 5, more evidence from interventions in low and middle income countries is greatly needed. Even if programs are successful on a small scale, it is not known what it will take to diffuse and implement programs on a large scale in developing countries. Demonstration programs need to be developed and evaluated in low and middle income countries before widespread implementation at scale would be justified.
Youth-Focused Policy Initiatives
Tobacco Control
There have been a number of initiatives both at the international and government levels to control the increasing use of tobacco products in both the developed and developing worlds. The World Health Organization’s (WHO’s) Tobacco Free Initiative was launched for tobacco control through research, policy, surveillance, capacity building, and global communications (WHO, 2010b). Events like World No Tobacco Day have become extremely popular in creating awareness about the harmful effects of tobacco. The Framework Convention for Tobacco Control (FCTC), described in Chapter 5, is a major public health treaty that was adopted by the World Health Assembly in 2003. Among its provisions is an explicit mention of
banning the sale of tobacco products to legal minors, and although it has provisions that are applicable for all ages, its principles are particularly targeted to youth, the most vulnerable group to initiate tobacco use (WHO, 2003).
However, despite the adoption of the FCTC, tobacco control programs in low and middle income countries have been limited in their implementation and variable in their success. In addition, the tobacco industry has developed methods to counteract or dilute the effects of policy changes, and young adolescents may be particularly susceptible to these actions as they begin to explore the adult world (Shafey et al., 2009). This is exemplified by India’s experience. The government of India adopted a comprehensive legislation for controlling tobacco use known as the Cigarette and Other Tobacco Products Act (COTPA) in 2003. This act, along with other provisions, banned the sale of all tobacco products to youth younger than 18 years and within 100 yards of educational institutions (Reddy et al., 2006). However, taxation of tobacco products was not included in COTPA, and recent taxation measures have continued the practice of exempting (or minimally taxing) bidis and chewable forms of tobacco on the grounds that these tobacco products are often consumed by the poor (Reddy and Gupta, 2004). The tobacco industry also responded to COTPA; for example, one tobacco company placed air-conditioned mobile lounges for smokers outside major attractions, such as sports stadiums and shopping malls, in four major cities in India (Reddy et al., 2006). In 2007, the government of India, in compliance with the FCTC and COTPA, launched the National Tobacco Control Program (NTCP) to build capacity of the states to effectively implement the tobacco control laws and also to bring about greater awareness about the ill effects of tobacco consumption. Under the NTCP, Tobacco Control Cells were set up in selected states in India to provide technical support to plan, coordinate, and monitor all activities related to tobacco control at the state level (Volunteer Health Association of India, 2009).
Recent progress in combating youth tobacco use has also been seen in the Philippines. The 2003 installment of the GYTS reported that current cigarette use declined significantly, from 32.6 percent (2000) to 21.8 percent (2003) for boys and from 12.9 percent (2000) to 8.8 percent (2003) in girls. The use of other forms of tobacco also experienced a precipitous decline in both adolescent boys and girls between 2000 and 2003, from 18.3 to 10.9 percent and 9.5 to 5.7 percent, respectively. Finally, the proportion of never smokers who reported being likely to initiate smoking within the next year was 13.8 percent in 2003, almost half as many who reported this likelihood in 2000 (26.5 percent). These declines both followed and coincided with a number of major changes in tobacco control policies in the Philippines. While many factors likely contributed to this decline, one significant piece of policy legislation passed in 1999 was the Philippines Clean
Air Act, which limited smoking indoors by enacting smoke-free indoor air laws. Building on this momentum, in 2003 the Youth Smoking Cessation Program led to the establishment of smoke-free campuses. In addition, the Tobacco Regulatory Act, also enacted in 2003, continues these efforts by increasing public education, banning all tobacco advertising, strengthening warning labels on tobacco products, and prohibiting the sale of tobacco to minors (Miguel-Baquilod et al., 2005).
In the face of resistance from the tobacco industry and its continued attempts to market their products, proactive steps need to be taken that can protect children and adolescents from exposure to tobacco products. A significant step in this direction has been taken with the initiation of the WHO FCTC, described previously. Antitobacco advertising, for example, can be effective in deterring children and preadolescents from taking up the habit in the first place (Penchmann, 2001; Wakefield et al., 2003). While evidence regarding the role of antitobacco advertising in encouraging young adults to quit the habit is inconclusive, antitobacco marketing, combined with other strategies to restrict tobacco use, can be an effective strategy in reducing the impact of tobacco promotion.
Restricting Food Marketing
There is a continued need for the international public health community, learning from the experience with the tobacco industry, to develop a sustained, global response to the aggressive marketing of potentially unhealthful food products, aimed pointedly at children and adolescents. Marketing restrictions, curtailing advertising of such products in children’s television, and the banning of in-school marketing, accompanied by the promotion of healthful foods such as fruits and vegetables, are some examples of steps that can be and have been taken to this end. Although studies on the effectiveness of marketing restrictions is inconclusive, the Institute of Medicine examined the issue in the United States and determined that the totality of the evidence available indicates that television marketing to children under the age of 11 years does affect the dietary preferences and patterns of youth (IOM, 2006). Support for the reasonableness of marketing restrictions given the available evidence has also been articulated in other recent policy-oriented reviews (Hastings et al., 2006; IOM, 2006). This guidance must be considered with caution when addressing similar challenges in developing countries due to potential differences in advertising type and exposure levels, but it does support both measured action and additional research into effective activities to promote better nutrition.
Since 2004, a number of countries have employed a variety of strategies to limit food marketing to children. Product advertisements are largely dominated by promotion of the “big five”: pre-sugared breakfast cereals,
soft drinks, confectionary, savory snacks, and fast food retailers (Hastings et al., 2006). Television commercials have dominated marketing efforts in the past, but there is emerging evidence that alternative branding mechanisms, most notably for the fast food industry, are growing in importance in developing countries (Hastings et al., 2006). While statutory regulations are the most common attempt at marketing restrictions, it is in fact self-regulation by the private sector and advertising corporations that are playing the largest part in limiting advertising to children (Hawkes, 2007).
Many developed and some developing countries limit the amount or duration of advertisements permitted to air during children’s television programming, from 5 minutes in Spain to 15 minutes in Venezuela. In 2006 in Brazil, the ministry of health drafted proposed legislation directly restricting and in some cases proscribing food-related advertising to children. Additionally, India has recently developed an inter-ministerial committee to review questionable television advertisements and more routinely enforce the previously established Cable Television Act Rules. Despite these promising steps, specific targeting of food products in statutory regulation remains extremely rare in both developed and developing countries (Hawkes, 2007).
Self-regulation, both by advertising agencies and individual companies, is by far the most common regulatory mechanism used in the European Union and is employed to a lesser extent in South-East Asia, New Zealand and Australia, and some African nations. The International Chamber of Commerce published a Framework for Responsible Food and Beverage Communications that focuses on reducing food and drink marketing approaches that are misleading to children, and a similar set of principles were endorsed by the Confederation of the Food and Drink Industries of the European Union (Hawkes, 2007). In addition, the International Food and Beverage Alliance’s (IFBA’s) Global Policy and Pledge Programs, which require participants to only market nutritionally sound products to youth, was recently expanded to Brazil, South Africa, Russia, and Thailand (International Food and Beverage Alliance, 2009). Since 2008, the IFBA reports greater than 99 percent compliance with the Pledge Programs by companies in participating countries (International Food and Beverage Alliance, 2009) Progress at monitoring and enforcing these self-regulation mechanisms in low and middle income countries has been more inconsistent and ranges from almost no action in South Africa to the very responsive Indian Advertising Standards Council (Hawkes, 2007).
There has been limited evidence demonstrating whether or not efforts to regulate food marketing will result in a positive health impact. Nonetheless, there is a strong rationale for these efforts, and the increasing prevalence of voluntary commitments by private companies and associations provides the potential for the cardiovascular disease prevention community
to forge partnerships with the private sector and makes this a feasible area for further implementation, as described further in Chapter 8. Thus, while the pursuit of stronger regulation of food marketing to children may not be a nation’s first priority, the presence of a growing global movement and the fact that many food and beverage companies have already taken the initiative to begin instituting self-imposed limits presents an opportunity for the global CVD community to encourage progress in this effort. In addition, enhanced efforts in policy research in this area—in collaboration with the child obesity field—would make a significant contribution to health promotion.
Youth-Focused Awareness and Advocacy
Mass Media
An important aspect of interventions for CVD prevention is health promotion through mass media campaigns. Because habits related to diet and physical activity begin to be established at an early age, and because adolescents and young adults are particularly susceptible to experimenting with alcohol and tobacco use, targeting campaigns focused on these risk factors of younger age groups is a rational strategy (IOM, 2006).
There are several examples of national-level mass media campaigns that have been successful in achieving greater awareness of the importance of healthful dietary habits and physical activity in leading a healthy life. One such example is the Australian government’s two-pronged mass media strategy, with one campaign addressing the importance of healthful eating (the Go for 2&5® campaign), and the other addressing the importance of incorporating more physical activity into children’s lives (the Get Moving campaign). Both campaigns targeted parents of 0- to 17-year-olds, along with children and youth aged 5-17 years. The main aims of the campaigns were to increase awareness of, improve attitudes toward, and change intentions to increase healthful eating and physical activity in the lives of the target audience. The campaigns adopted multiple elements to communicate its message, including television, radio, and print commercials; shopping center and shopping cart advertisements; media partnership activities; a campaign website; an information line; and distribution of other reading material. In an evaluation of the campaigns, Elliot and Walker (2007) found both aspects of the campaigns to be successful in generating awareness, increasing knowledge, and enhancing more positive attitudes toward healthful eating and physical activity. Although they didn’t find these to translate into improved behavior to a considerable extent, they did find a trend toward the right direction, which, given a more sustained and long-term campaign, could have been more substantial. Thus, the duration for
which a mass media campaign should run to bring about significant change at the population level is an important consideration when developing such campaigns.
A systematic review of mass media campaigns in the United States and Norway for prevention of smoking among youth illustrates this point (Sowden and Arblaster, 2000). Out of the six studies that met the inclusion criteria, Sowden found that only two significantly reduced smoking behavior among young people; both of these studies were of longer duration and of greater intensity than the others. In addition, both successful campaigns were based on sound theories and included extensive formative research.
Carrying out adequate formative research before developing a campaign is extremely important. The success of one campaign doesn’t necessarily translate into successful implementation in all other settings. The success of mass media campaigns is greatly contingent on the characteristics and requirements of the target population, and educational levels, socioeconomic backgrounds, and cultural backdrops go a long way in determining whether such a campaign will generate results in the desired direction. Thus it is important to tailor social marketing efforts to the needs and constraints of particular contexts and peoples before anticipating a successful outcome.
Another use of the media is through direct educational programming. Sesame Workshop, for example, is a nonprofit educational organization that develops educational content delivered in a variety of ways—including television, radio, books, magazines, interactive media, and community outreach. Taking advantage of all forms of media and using those that are best suited to deliver a particular curriculum, it efficiently reaches millions of children, parents, caregivers, and educators—locally, nationally, and globally. Sesame Workshop uses a collaborative, research-intensive approach to the development of programs and activities. Its offerings strive to reflect both a deep understanding of children’s developmental needs and the best ways to address those needs in order to engage children in a way that maximizes learning (Cole, 2009; Sesame Workshop, 2010).
Health and wellness is one of the key themes of Sesame Workshop, including programs to foster health habits and life skills that are active in 18 developed and developing countries. One of these programs is “Healthy Habits for Life” in Colombia, which addresses the need for nutrition and exercise learning and aims to instill healthful behaviors in children. An impact evaluation for this program is currently underway with researchers from the Children’s Heart Foundation (Bogotá) and Mount Sinai Medical Center (New York); the results are expected in mid-2010 (Cole, 2009).
Youth-Driven Advocacy
Youth Advocacy for CVD Over the past decade, a number of youth-driven initiatives have targeted reduction in CVD risk factors and demonstrated the potential power in the energy and enthusiasm of young people. In the United States, for example, Kick Butts Day (KBD) is annual event for youth advocacy, leadership, and activism for tobacco control from the Campaign for Tobacco Free Kids (CTFK). This event is now in its 15th year. Youth advocacy groups can register on the KBD website. Each year, a date is decided when KBD events are organized across the United States, with resources and merchandise provided to the participating youth groups by CTFK. In addition, CTFK also facilitates media mobilization to garner media attention for the various events that are organized. This concerted youth advocacy effort organizes support for specific tobacco control policies at the national and local level, which teaches young people about the process of policy initiatives while pursuing tangible end goals (Campaign for Tobacco Free Kids, 2010).
The Global Youth Action on Tobacco (GYAT) Network was founded in 2006 during a pre-conference youth advocacy training workshop organized by Essential Action and CTFK in conjunction with the 13th World Conference on Tobacco or Health (WCTOH). The participants for this workshop included youth health advocates from 30 countries. Contact is maintained through e-connectivity, allowing members to share experiences with advocacy events focused on targeting the tobacco industry (Global Youth Action on Tobacco Network, 2009).
Another organization that can serve as a model for youth-driven advocacy in low and middle income countries is Youth For Health (Y4H). Y4H is a network comprised of nearly 220,000 youth health advocates from 45 countries across the globe. Y4H was launched during the first Global Youth Meet on Health (GYM 2006), a unique global health conclave with participation from 280 youth from 35 countries. GYM 2006 was organized by HRIDAY, a nongovernemtnal organization based in Delhi, India, engaged in awareness, advocacy, and research related to health promotion (HRIDAY–SHAN, 2006). The deliberations during GYM 2006 highlighted the need for a sustained network of global youth to take the battle forward in their respective countries while having a common platform to monitor progress and share knowledge, which led to the Y4H movement. The group aims to connect young people from around the world, forming a global alliance of national, regional, and global partnerships that can collectively promote common causes. These include advocating for tobacco control, healthful diets, regular physical activity, environmental protection, gender equality, women’s health, and reduction of alcohol and drug abuse (HRIDAY–SHAN, 2006).
A dedicated forum facilitates sharing of experiences and undertaking concerted global action on health promotion by encouraging youth advocates to start in their own communities or countries and present their views to legislatures and other policy makers (Youth For Health, 2009). For example, Y4H activists from Argentina, Chile, Colombia, Mexico, and Uruguay worked together to draft an antitobacco manifesto in September 2007, and in South Africa Y4H members have called for stricter tobacco control policies. They presented their views in front of the South African Parliamentary Committee reviewing the Tobacco Act. In Georgia, a “HeartWeek” event was organized by Georgia Against Tobacco and Drugs (an organization formed by the Georgian Y4H delegates), where youth sport competitions were held to raise awareness about physical activity and its connections with heart health. More than 100 children aged 8-12 years (including 3 with diabetes and 4 with heart problems) from Georgia, Armenia, and Azerbaijan participated in these events (Youth For Health, 2009).
At the global level, an electronic signature campaign on Global Health Promotion for Youth with a focus on tobacco control, initiated by Y4H members and endorsed by more than 225,000 youth and adults worldwide, was presented by Y4H members to the Secretary General of the United Nations (UN) on October 24, 2007 (UN Day) at the UN Headquarters in New York. Y4H representatives discussed action areas of Y4H activities with the Secretary General and Special Adviser to the Secretary General on Gender Issues and Advancement of Women. In addition, in 2009, Y4H helped organize the Global Youth Meet on Tobacco Control (GYM 2009), a pre-conference to the 14th WCTOH. GYM 2009 was attended by 140 participants from 27 countries who discussed tobacco control issues (HRIDAY–SHAN, 2006).
Lessons from Youth Advocacy on HIV/AIDS Examples of youth advocacy efforts for cardiovascular disease in developing countries are limited, but lessons can be learned from some successful youth movements in the global HIV/AIDS community. For example, the Global Youth Coalition on HIV/AIDS (GYCA) was started by young people following the 2004 International AIDS Conference in Bangkok, Thailand. Now, with partnerships and support from the Joint United Nations Programme on HIV/AIDS (UNAIDS), the United Nations Population Fund (UNFPA), and other multinational NGOs, the GYCA operates programs in 150 countries through diverse initiatives ranging from the distribution of small grants to “outstanding young leaders” to participation in international summits (Global Youth Coalition on HIV/AIDS, 2010). Groups also network among themselves, allowing them to share best practices and advocacy tools. Because the entire program is led by young people, it not only provides op-
portunities for members to make a positive impact on their community, but also establishes connections between the next generation of HIV advocates and leaders. This is just one of the many efforts driven by the efforts of young people around the world in the fight against HIV/AIDS that can be examined for lessons learned.
In summary, the opportunity to capitalize on the momentum of youth advocacy in global health to increase awareness of the importance of cardiovascular health presents promising potential for the global CVD community. If efforts are to be successful and sustained, it will be critical to both push young people interested in heart health to think globally and to encourage young people already acting on the global health stage to recognize that cardiovascular disease is a fundamental component of youth wellness.
CHALLENGES TO IMPLEMENTING YOUTH-BASED PROGRAMS IN LOW AND MIDDLE INCOME COUNTRIES
Despite great progress in identifying increasing trends in the acquisition of risk early in life, data on the incidence and prevalence of CVD risk factors in youth remain very limited. More data is clearly needed to prioritize avenues for program implementation and intervention research, yet the best methods to pursue information specific to children and adolescents remain unclear. The Global Youth Tobacco Survey and South African Youth Risk Behavioral Survey are stand-alone efforts focused entirely on issues pertaining to children and adolescents, specifically targeting those groups through schools and other venues. Efforts such as these have the advantage of using questions, survey and interview strategies, and analytical models that are tailored to the needs of youth and produce a more comprehensive picture of the targeted risk behaviors in that age group. However, in order to accomplish surveys such as these, additional resources must be committed, and in some cases perhaps diverted away from existing surveillance efforts. Alternatively, the disaggregation of results of already established or ongoing surveillance efforts by age may also provide a relevant data picture with fewer additional resources required. The greater potential feasibility of this option in developing countries warrants further investigation into what survey methodologies might be most effective when youth are one of the many target populations. Regardless of which approach is ultimately selected, as discussed in Chapter 4, efforts must be made to ensure that local country and community capacity to conduct both the survey and analysis is strengthened. This is essential to ensuring the sustainability of such efforts, a critical need in order to reveal extended temporal trends that can identify whether youth-focused initiatives are ultimately having any impact on health status.
In addition to the need for better data on CVD risk factors in children and youth, evidence from youth-focused interventions targeted at these risk factors in low and middle countries is also quite limited. There are some promising findings, especially in the area of tobacco reduction. Other intervention approaches with some success in developed countries offer models for adaptation. However, many of these possible models did not operate over long periods of time and on a large scale. The issue of what it will take to adapt, diffuse, implement, and maintain programs on a large scale in low and middle income countries needs to be addressed. One particularly important potential barrier to adopting cardiovascular health promotion programs targeting children and youth in schools and other settings is whether there exist reasonable incentives for non-health organizations to create and maintain such programs. For schools, the advantages of implementing such programs are not often straightforward. For example, physical activity may be central in some schools, but the engagement and participation of schools are not guaranteed, especially if there is a competition for resources that would otherwise be dedicated to their primary academic mission. They may not commit limited resources to programs over the long term if the incentives for doing so are weak and the interventions are complex to implement, manage, and maintain. Thus, it is necessary to consider the long-term viability of such efforts as the programs may dissipate even if there is early enthusiasm, especially in developing countries where resources may be limited. Additionally, in order for many school-based interventions to be implemented, especially at a large scale, there may need to be interaction and cooperation between different divisions of the national government, such as the health and education sectors. The degree to which each of these independent agents work together varies in developing countries, and thus effort may be required to assist different sectors in coordinating their actions where appropriate and feasible. This coordination with the education sector is thus a critical component of the broader messages in this report supporting intersectoral and whole-of-government approaches to address CVD and related chronic diseases.
CONCLUSION
Accumulation of cardiovascular risk begins early in life, and evidence on rising rates of childhood obesity and youth smoking in low and middle income countries as well as emerging evidence on the effects of early nutrition on later cardiovascular health support the value of starting cardiovascular health promotion during pregnancy and early childhood and continuing prevention efforts throughout the life course. Maternal and child health (MCH) programs offer an opportunity to provide care that takes into account not only shorter-term childhood outcomes but also
future lifelong health. In particular, emerging evidence on the effects of early nutrition on later cardiovascular health means that the CVD and MCH communities need to work together more closely to ensure that food and nutrition programs for undernourished children do not inadvertently contribute to long-term chronic disease risk. This could be accomplished through future coordination with multinational organizations that provide both service and programmatic guidance such as the United Nations World Food Program, United States Agency for International Development, Oxfam America, and Save the Children, as well as through direct consultation with local governments where possible. Increased efforts are needed to identify ways in which emergency and long-term food provision can be accomplished without unnecessarily increasing CVD risk or significantly increasing existing program costs.
The available evidence on the impact of cardiovascular health promotion and CVD prevention initiatives in childhood and adolescence is limited and of variable quality, especially in low and middle income country settings. Approaches with some success on a small scale that have emerging potential for developing countries include education initiatives targeted to children, school-based programs, and programs targeted to take advantage of the potential for adolescents and young adults to serve as powerful advocates for change. This foundation provides an opportunity to develop, evaluate, and implement child- and youth-based programs to prevent the development of CVD in later life.
REFERENCES
Aboderin, I., A. Kalache, Y. Ben-Shlomo, J. W. Lynch, C. S. Yajnik, D. Kuh, and D. Yach. 2002. Life course perspectives on coronary heart disease, stroke and diabetes: Key issues and implications for policy and research. Geneva: World Health Organization.
Agirbasli, M., S. Cakir, S. Ozme, and G. Ciliv. 2006. Metabolic syndrome in Turkish children and adolescents. Metabolism: Clinical and Experimental 55(8):1002-1006.
Al-Isa, A. N. 2004. Body mass index, overweight and obesity among Kuwaiti intermediate school adolescents aged 10-14 years. European Journal of Clinical Nutrition 58(9):1273-1277.
Arnas, Y. 2006. The effects of television food advertisement on children’s food purchasing requests. Pediatrics International 48(2):138-145.
Arora, M., S. Reddy, M. H. Stigler, and C. L. Perry. 2008. Associations between tobacco marketing and use among urban youth in India. American Journal of Health Behavior 32(3):283-294.
Asma, S. 2009. Global tobacco surveillance system. Presentation at the Public Information Gathering Session for the Institute of Medicine Committee on Preventing the Global Epidemic of Cardiovascular Disease, Washington, DC.
Baker, J. L., L. W. Olsen, and T. I. A. Sørensen. 2007. Childhood body-mass index and the risk of coronary heart disease in adulthood. New England Journal of Medicine 357(23):2329-2337.
Barker, D. J. 1997. The fetal origins of coronary heart disease. Acta Paediatrica Supplement 422:78-82.
Barker, D. J. P. 1998. In utero programming of chronic disease. Clinical Science 95(2): 115-128.
Barker, D. J. P. 2007. The origins of the developmental origins theory. Journal of Internal Medicine 261(5):412-417.
Barker, D. J. P., and S. P. Bagby. 2005. Developmental antecedents of cardiovascular disease: A historical perspective. Journal of the American Society of Nephrology 16(9): 2537-2544.
Barker, D. J. P., C. Osmond, T. J. Forsen, E. Kajantie, and J. G. Eriksson. 2005. Trajectories of growth among children who have coronary events as adults. New England Journal of Medicine 353(17):1802-1809.
Berenson, G. S. 2002. Childhood risk factors predict adult risk associated with subclinical cardiovascular disease. The Bogalusa Heart Study. American Journal of Cardiology 90(10C):3L-7L.
Bhardwaj, S., A. Misra, L. Khurana, S. Gulati, P. Shah, and N. K. Vikram. 2008. Childhood obesity in Asian Indians: A burgeoning cause of insulin resistance, diabetes and sub-clinical inflammation. Asia Pacific Journal of Clinical Nutrition 17(Suppl 1):172-175.
Bhutta, Z. A., T. Ahmed, R. E. Black, S. Cousens, K. Dewey, E. Giugliani, B. A. Haider, B. Kirkwood, S. S. Morris, H. P. S. Sachdev, and M. Shekar. 2008. What works? Interventions for maternal and child undernutrition and survival. Lancet 371(9610):417-440.
Black, R. E., L. H. Allen, Z. A. Bhutta, L. E. Caulfield, M. de Onis, M. Ezzati, C. Mathers, and J. Rivera. 2008. Maternal and child undernutrition: Global and regional exposures and health consequences. Lancet 371(9608):243-260.
Buttross, L. S., and J. W. Kastner. 2003. A brief review of adolescents and tobacco: What we know and don’t know. American Journal of the Medical Sciences 326(4):235-237.
Caballero, B. 2005. A nutrition paradox—underweight and obesity in developing countries. New England Journal of Medicine 352(15):1514-1516.
Caballero, B. 2009. Early undernutrition and risk of CVD in the adult. Presentation at Public Information Gathering Session for the Institute of Medicine Committee on Preventing the Global Epidemic of Cardiovascular Disease, Washington, DC. Campaign for Tobacco Free Kids. 2010. Kick butts day. http://kickbuttsday.org (accessed February 19, 2010).
Celermajer, D. S., and J. G. Ayer. 2006. Childhood risk factors for adult cardiovascular disease and primary prevention in childhood. Heart 92(11):1701-1706.
Center for Science in the Public Interest. 2003. Pestering parents: How food companies market obesity to children. http://www.cspinet.org/pesteringparents (accessed August 23, 2009).
Choi, W. S., J. S. Ahluwalia, K. J. Harris, and K. Okuyemi. 2002. Progression to established smoking: The influence of tobacco marketing. American Journal of Preventive Medicine 22(4):228-233.
Chopra, M., and I. Darnton-Hill. 2004. Tobacco and obesity epidemics: Not so different after all? British Medical Journal 328(7455):1558-1560.
Cole, C. 2009. Plaza sésamo healthy habits for life: Colombia. Presentation at Public Information Gathering Session for the Institute of Medicine Committee on Preventing the Global Epidemic of Cardiovascular Disease, Washington, DC.
Committee on Environmental Health, Committee on Substance Abuse, Committee on Adolescence, and Committee on Native American Child Health. 2009. Tobacco use: A pediatric disease. Pediatrics 124:1474-1487.
Cook, S., M. Weitzman, P. Auinger, M. Nguyen, and W. H. Dietz. 2003. Prevalence of a metabolic syndrome phenotype in adolescents: Findings from the third National Health and Nutrition Examination Survey, 1988-1994. Archives of Pediatrics and Adolescent Medicine 157(8):821-827.
Crowther, N. J., N. Cameron, J. Trusler, and I. P. Gray. 1998. Association between poor glucose tolerance and rapid post natal weight gain in seven-year-old children. Diabetologia 41(10):1163-1167.
Cruz, M. L., M. J. Weigensberg, T. T. K. Huang, G. Ball, G. Q. Shaibi, and M. I. Goran. 2004. The metabolic syndrome in overweight hispanic youth and the role of insulin sensitivity. Journal of Clinical Endocrinology and Metabolism 89(1):108-113.
Csabi, G., K. Torok, D. Molnar, and S. Jeges. 2000. Presence of metabolic cardiovascular syndrome in obese children. European Journal of Pediatrics 159(1-2):91-94.
Davey Smith, G. 2007. Life-course approaches to inequalities in adult chronic disease risk: Boyd Orr lecture. Proceedings of the Nutrition Society 66(2):216-236.
Davey Smith, G. 2008. Assessing intrauterine influences on offspring health outcomes: Can epidemiological studies yield robust findings? Basic and Clinical Pharmacology and Toxicology 102(2):245-256.
Davey Smith, G., C. Steer, S. Leary, and A. Ness. 2007. Is there an intrauterine influence on obesity? Evidence from parent-child associations in the Avon Longitudinal Study of Parents and Children (ALSPAC). Archives of Disease in Childhood 92(10):876-880.
Dell Center for Healthy Living. 2010. Project ACTIVITY (Advancing Cessation of Tobacco In Vulnerable Indian Tobacco Consuming Youth). http://www.sph.uth.tmc.edu/DellHealthyLiving/default.aspx?id=3995 (accessed June 4, 2010)
DiFranza, J. R., J. A. Savageau, N. A. Rigotti, K. Fletcher, J. K. Ockene, A. D. McNeill, M. Coleman, and C. Wood. 2002. Development of symptoms of tobacco dependence in youths: 30 month follow up data from the Dandy Study. Tobacco Control 11(3):228-235.
Dobbins, M., K. De Corby, P. Robeson, H. Husson, and D. Tirilis. 2009. School-based physical activity programs for promoting physical activity and fitness in children and adolescents aged 6-18. Cochrane Database Syst Rev(1):CD007651.
Dollman, J., K. Norton, and L. Norton. 2005. Evidence for secular trends in children’s physical activity behaviour. British Journal of Sports Medicine 39(12):892-897; discussion 897.
Dong, M., W. H. Giles, V. J. Felitti, S. R. Dube, J. E. Williams, D. P. Chapman, and R. F. Anda. 2004. Insights into causal pathways for ischemic heart disease: Adverse childhood experiences study. Circulation 110(13):1761-1766.
Elliott, D., and D. Walker. 2007. Evaluation of the national ‘get moving’ compaign. Australian Government Department of Health and Ageing, Commonwealth of Australia, Canberra.
Eriksson, J. G., T. Forsen, J. Tuomilehto, P. D. Winter, C. Osmond, and D. J. P. Barker. 1999. Catch-up growth in childhood and death from coronary heart disease: Longitudinal study. British Medical Journal 318:7181.
Felitti, V. J., R. F. Anda, D. Nordenberg, D. F. Williamson, A. M. Spitz, V. Edwards, M. P. Koss, and J. S. Marks. 1998. Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults: The adverse childhood experiences (ACE) study. American Journal of Preventive Medicine 14(4):245-258.
Flay, B. R. 2009a. The promise of long-term effectiveness of school-based smoking prevention programs: A critical review of reviews. Tobacco Induced Diseases 5(1):7.
Flay, B. R. 2009b. School-based smoking prevention programs with the promise of long-term effects. Tobacco Induced Diseases 5(1):6.
Forsen, T., J. G. Eriksson, J. Tuomilehto, C. Osmond, and D. J. P. Barker. 1999. Growth in utero and during childhood among women who develop coronary heart disease: Longitudinal study. British Medical Journal 319(7222):1403-1407.
Foster, G. D., S. Sherman, K. E. Borradaile, K. M. Grundy, S. S. Vander Veur, J. Nachmani, A. Karpyn, S. Kumanyika, and J. Shults. 2008. A policy-based school intervention to prevent overweight and obesity. Pediatrics 121(4):e794-e802.
Freedman, D. S., W. H. Dietz, S. R. Srinivasan, and G. S. Berenson. 1999. The relation of1999. The relation of overweight to cardiovascular risk factors among children and adolescents: The Bogalusa heart study. Pediatrics 103(6):1175-1182.
Freedman, D. S., L. K. Khan, W. H. Dietz, S. R. Srinivasan, and G. S. Berenson. 2001. Relationship of childhood obesity to coronary heart disease risk factors in adulthood: The Bogalusa Heart Study. Pediatrics 108(3):712-718.
Freedson, P. S. 1992. Physical activity among children and youth. Canadian Journal of Sport Sciences 17(4):280-283.
Galobardes, B., G. D. Smith, and J. W. Lynch. 2006. Systematic review of the influence of childhood socioeconomic circumstances on risk for cardiovascular disease in adulthood. Annals of Epidemiology 16(2):91-104.
Galst, J. P., and M. A. White. 1976. The unhealthy persuader: The reinforcing value of television and children’s purchase-influencing attempts at the supermarket. Child Development 47(4):1089-1096.
Gillman, M. W., S. L. Rifas-Shiman, K. Kleinman, E. Oken, J. W. Rich-Edwards, and E. M. Taveras. 2008. Developmental origins of childhood overweight: Potential public health impact. Obesity 16(7):1651-1656.
Global Youth Action on Tobacco Network. 2009. GYAT network. http://www.gyatnetwork.org/ (accessed March 9, 2010).
Global Youth Coalition on HIV/AIDS. 2010. Global youth coalition on HIV/AIDS. http://www.youthaidscoalition.org/ (accessed February 18, 2010).
Global Youth Tobacco Survey Collaborative Group. 2002. Tobacco use among youth: A cross country comparison. Tobacco Control 11(3):252-270.
Glover, E. D., P. N. Glover, and T. J. Payne. 2003. Treating nicotine dependence. American Journal of the Medical Sciences 326(4):183-186.
Gluckman, P. D., M. A. Hanson, A. S. Beedle, and D. Raubenheimer. 2008. Fetal and neonatal pathways to obesity. In Frontiers of hormone research. Vol. 36. Edited by M. Korbonits. Basel: Karger. Pp. 61-72.
Gorn, G., and M. Goldberg. 1982. Behavioural evidence of the effects of televised food messages on children. Journal of Consumer Research 9:200-205.
Gortmaker, S. L., K. Peterson, J. Wiecha, A. M. Sobol, S. Dixit, M. K. Fox, and N. Laird. 1999. Reducing obesity via a school-based interdisciplinary intervention among youth: Planet health. Archives of Pediatrics and Adolescent Medicine 153(4):409-418.
Guillaume, M., L. Lapidus, F. Beckers, A. Lambert, and P. Björntorp. 1996. Cardiovascular risk factors in children from the Belgian province of Luxembourg: The Belgian Luxembourg Child Study. American Journal of Epidemiology 144(9):867-880.
Hastings, G. L., M. Stead, L. McDermott, A. Forsyth, A. M. MacKintosh, M. Rayner, C. Godfrey, M. Caraher, and K. Angus. 2003. Review of research on the effects of food promotion to children. Glasgow: Centre for Social Marketing.
Hastings, G., L. McDermott, K. Angus, M. Stead, and S. Thompson. 2006. The extent, nature and effects of food promotion to children: A review of the evidence. Geneva: World Health Organization.
Hawkes, C. 2002. Marketing activities of global soft drink and fast food companies in emerging markets: A review. In Globalization, diets and noncommunicable diseases. Geneva: World Health Organization.
Hawkes, C. 2007. Marketing food to children: Changes in the global regulatory environment 2004-2006. Geneva: World Health Organization.
Henry J. Kaiser Family Foundation. 2007. Food for thought: Television food advertising to children in the United States. Washington, DC: Henry J. Kaiser Family Foundation.
Hossain, P., B. Kawar, and M. El Nahas. 2007. Obesity and diabetes in the developing world—a growing challenge. New England Journal of Medicine 356(3):213-215.
HRIDAY–SHAN. 2006. HRIDAY–SHAN website. http://www.hriday-shan.org/ (accessed February 19, 2010).
IASO (International Association for the Study of Obesity). 2008a. About: Global prevalence of overweight in boys. http://www.iotf.org/database/documents/GlboalBoytrendsv2pdf.pdf (accessed December 9, 2009).
IASO. 2008b. About: Global prevalence of overweight in girls. http://www.iotf.org/database/documents/GlobalGirltrendspdf.pdf (accessed December 8, 2009).
International Food and Beverage Alliance. 2009. IFBA update since November, 2008. Presentation presented to the World Health Organization on August 31, 2009. Geneva, Switzerland.
International Institute of Population Studies. 2005-2006. National family health survey 3. Mumbai, India: International Institute of Population Studies.
IOM (Institute of Medicine). 2006. Food marketing to children and youth: Threat or opportunity? Washington, DC: The National Academies Press.
Jiang, J., X. Xia, T. Greiner, G. Wu, G. Lian, and U. Rosenqvist. 2007. The effects of a 3-year obesity intervention in schoolchildren in Beijing. Child: Care, Health and Development 33(5):641-646.
John, D. R. 1999. Consumer socialization of children: A retrospective look at twenty-five years of research. Journal of Consumer Research 26(3):183-213.
Johnson, M. C., L. J. Bergersen, A. Beck, G. Dick, and B. R. Cole. 1999. Diastolic function and tachycardia in hypertensive children. American Journal of Hypertension 12(10 I):1009-1014.
Kain, J., F. Vio, and C. Albala. 1998. Childhood nutrition in Chile: From deficit to excess. Nutrition Research 18(11):1825-1837.
Kain, J., R. Uauy, Albala, F. Vio, R. Cerda, and B. Leyton. 2004. School-based obesity prevention in Chilean primary school children: Methodology and evaluation of a controlled study. International Journal of Obesity and Related Metabolic Disorders 28(4): 483-493.
Kelishadi, R. 2007. Childhood overweight, obesity, and the metabolic syndrome in developing countries. Epidemiologic Reviews 29:62-76.
Laird, W. P., and D. E. Fixler. 1981. Left ventricular hypertrophy in adolescents with elevated blood pressure: Assessment by chest roentgenography, electrocardiography, and echocardiography. Pediatrics 67(2):255-259.
Li, S., W. Chen, S. R. Srinivasan, M. G. Bond, R. Tang, E. M. Urbina, and G. S. Berenson. 2003. Childhood cardiovascular risk factors and carotid vascular changes in adulthood: The Bogalusa Heart Study. Journal of the American Medical Association 290(17):2271-2276.
Liu, A., X. Hu, G. Ma, Z. Cui, Y. Pan, S. Chang, W. Zhao, and C. Chen. 2008. Evaluation of a classroom-based physical activity promoting programme. Obesity Reviews 9(Suppl 1):130-134.
Luepker, R. V., C. L. Perry, S. M. McKinlay, P. R. Nader, G. S. Parcel, E. J. Stone, L. S. Webber, J. P. Elder, H. A. Feldman, C. C. Johnson, et al. 1996. Outcomes of a field trial to improve children’s dietary patterns and physical activity. The child and Adolescent Trial for Cardiovascular Health. Catch Collaborative Group. Journal of the American Medical Association 275(10):768-776.
Martorell, R., L. K. Khan, M. L. Hughes, and L. M. Grummer-Strawn. 2000. Overweight and obesity in preschool children from developing countries. International Journal of Obesity 24(8):959-967.
Miguel-Baquilod, M., B. Fishburn, J. Santos, N. R. Jones, and C. W. Warren. 2005. Tobacco use among students age 13-15 years—Phillipines, 2000 and 2003. Morbidity and Mortality Weekly Report 54(4):94-97.
Misra, A., and L. Khurana. 2008. Obesity and the metabolic syndrome in developing countries. Journal of Clinical Endocrinology and Metabolism 93(11 Suppl 1):S9-S30.
Naylor, P. J., and H. A. McKay. 2009. Prevention in the first place: Schools a setting for action on physical inactivity. British Journal of Sports Medicine 43(1):10-13.
Oates, J. A., A. J. J. Wood, and N. L. Benowitz. 1988. Drug therapy: Pharmacologic aspects of cigarette smoking and nicotine addiction. New England Journal of Medicine 319(20):1318-1330.
Oken, E., E. B. Levitan, and M. W. Gillman. 2008. Maternal smoking during pregnancy and child overweight: Systematic review and meta-analysis. International Journal of Obesity 32(2):201-210.
Osmond, C., and D. J. P. Barker. 2000. Fetal, infant, and childhood growth are predictors of coronary heart disease, diabetes, and hypertension in adult men and women. Environmental Health Perspectives 108(Suppl 3):545-553.
Panday, S., S. P. Reddy, R. A. Ruiter, E. Bergstrom, and H. de Vries. 2005. Determinants of smoking cessation among adolescents in South Africa. Health Education Research 20(5):586-599.
Panday, S., S. P. Reddy, R. A. Ruiter, E. Bergstrom, and H. de Vries. 2007a. Determinants of smoking among adolescents in the Southern Cape-Karoo Region, South Africa. Health Promotion International 22(3):207-217.
Panday, S., S. P. Reddy, R. A. Ruiter, E. Bergstrom, and H. de Vries. 2007b. Nicotine dependence and withdrawal symptoms among occasional smokers. Journal of Adolescent Health 40(2):144-150.
Parliament of the Republic of India. The cigarettes and other tobacco products (prohibition of advertisement and regulation of trade and commerce, production, supply and distribution) amendment bill, 2007. 62. (2007).
Penchmann, C. 2001. Changing adolescent smoking prevalence. In Smoking and tobacco control monograph no 14. NIH Pub. No. 02-5086. Bethesda, MD: National Cancer Institute.
Perry, C. L., M. Eriksen, and G. Giovino. 1994. Tobacco use: a pediatric epidemic. Tobacco Control 3(2):97-98.
Perry, C. L., M. H. Stigler, M. Arora, and K. S. Reddy. 2008. Prevention in translation: Tobacco use prevention in India. Health Promotion Practice 9(4):378-386.
Perry, C. L., M. H. Stigler, M. Arora, and K. S. Reddy. 2009. Preventing tobacco use among young people in India: Project MYTRI. American Journal of Public Health 99(5): 899-906.
Peto, R., A. D. Lopez, J. Boreham, M. Thun, C. Heath Jr., and R. Doll. 1996. Mortality from smoking worldwide. British Medical Bulletin 52(1):12-21.
Popkin, B. M., and P. Gordon-Larsen. 2004. The nutrition transition: Worldwide obesity dynamics and their determinants. International Journal of Obesity and Related Metabolic Disorders 28(Suppl 3):S2-S9.
Prentice, A. M. 2006. The emerging epidemic of obesity in developing countries. International Journal of Epidemiology 35(1):93-99.
Prentice, A. M., and S. E. Moore. 2005. Early programming of adult diseases in resource poor countries. Archives of Disease in Childhood 90(4):429-432.
Prokhorov, A. V., J. P. Winickoff, J. S. Ahluwalia, D. Ossip-Klein, S. Tanski, H. A. Lando, E. T. Moolchan, M. Muramoto, J. D. Klein, M. Weitzman, and K. H. Ford. 2006. Youth tobacco use: A global perspective for child health care clinicians. Pediatrics 118(3): e890-e903.
Raitakari, O. T., M. Juonala, M. Kahoen, L. Taittonen, T. Laitinen, N. Maki-Torkko, M. J. Jarvisalo, M. Uhari, E. Jokinen, T. Ronnemaa, H. K. Akerblom, J. S. A. Viikari. 2003. Cardiovascular risk factors in childhood and carotid artery intima-media thickness in adulthood: The Cardiovascular Risk in Young Finns Study. Journal of the American Medical Association 290(17):2277-2291.
Reddy, K. S., and P. C. Gupta. 2004. Report on tobacco control in India. New Delhi, India: Ministry of Health & Family Welfare, Government of India, CDC, and WHO.
Reddy, K. S., M. Arora, C. L. Perry, B. Nair, A. Kohli, L. A. Lytle, M. Stigler, and D. Prabhakaran. 2002. Tobacco and alcohol use outcomes of a school-based intervention in New Delhi. American Journal of Health Behavior 26(3):173-181.
Reddy, K. S., C. L. Perry, M. H. Stigler, and M. Arora. 2006. Differences in tobacco use among young people in urban India by sex, socioeconomic status, age, and school grade: Assessment of baseline survey data. Lancet 367(9510):589-594.
Reddy, S. P., S. Panday, D. Swart, C. C. Jinabhai, S. L. Amosun, S. James, K. D. Monyeki, G. Stevens, N. Morejele, N. S. Kambaran, R. G. Omardien, and H. W. Van den Borne. 2003. Umthenthe uhlaba usamila: The South African Youth Risk Behavior Survey 2002. Cape Town: South African Medical Research Council.
Reddy, S. P., K. Resnicow, S. James, N. Kambaran, R. Omardien, and A. D. Mbewu. 2009. Underweight, overweight and obesity among South African adolescents: Results of the 2002 national youth risk behaviour survey. Public Health and Nutrition 12(2):203-207.
Resnicow, K., S. P. Reddy, S. James, R. Gabebodeen Omardien, N. S. Kambaran, H. G. Langner, R. D. Vaughan, D. Cross, G. Hamilton, and T. Nichols. 2008. Comparison of two school-based smoking prevention programs among South African high school students: Results of a randomized trial. Annals of Behavioral Medicine 36(3):231-243.
Richter, L., S. Norris, J. Pettifor, D. Yach, and N. Cameron. 2007. Cohort profile: Mandela’s children: The 1990 birth to twenty study in South Africa. International Journal of Epidemiology 36(3):504-511.
Roberts, D. F. and U. G. Foehr. 2004. Kids and media in America. Cambridge: Cambridge University Press.
Rocchini, A. P. 2002. Childhood obesity and a diabetes epidemic. New England Journal of Medicine 346(11):854-855.
Rosner, B., R. Prineas, S. R. Daniels, and J. Loggie. 2000. Blood pressure differences between blacks and whites in relation to body size among US children and adolescents. American Journal of Epidemiology 151(10):1007-1019.
Rudman, A. 2001. India inhales. USA: Bullfrog Films.
Save the Children. 2010. Survive to 5. http://www.savethechildren.org/programs/health/child-survival/survive-to-5 (accessed March 9, 2010).
Sesame Workshop. 2010. Inside the Workshop. http://www.sesameworkshop.org/insidetheworkshop (accessed June 4, 2010).
Sinaiko, A. R., D. R. Jacobs Jr., J. Steinberger, A. Moran, R. Luepker, A. P. Rocchini, and R. J. Prineas. 2001. Insulin resistance syndrome in childhood: Associations of the euglycemic insulin clamp and fasting insulin with fatness and other risk factors. Journal of Pediatrics 139(5):700-707.
Singh, R., A. Bhansali, R. Sialy, and A. Aggarwal. 2007. Prevalence of metabolic syndrome in adolescents from a north Indian population. Diabetic Medicine 24(2):195-199.
Singhal, A., M. Fewtrell, T. J. Cole, and A. Lucas. 2003. Low nutrient intake and early growth for later insulin resistance in adolescents born preterm. Lancet 361(9363):1089-1097.
Singhal, A., T. J. Cole, M. Fewtrell, J. Deanfield, A. Lucas, A. Singhal, T. J. Cole, M. Fewtrell, J. Deanfield, and A. Lucas. 2004. Is slower early growth beneficial for long-term cardiovascular health? Circulation 109(9):1108-1113.
Sinha, R., G. Fisch, B. Teague, W. V. Tamborlane, B. Banyas, K. Allen, M. Savoye, V. Rieger, S. Taksali, G. Barbetta, R. S. Sherwin, and S. Caprio. 2002. Prevalence of impaired glucose tolerance among children and adolescents with marked obesity. New England Journal of Medicine 346(11):802-810.
Slater, S. J., F. J. Chaloupka, M. Wakefield, L. D. Johnston, and P. M. O’Malley. 2007. The impact of retail cigarette marketing practices on youth smoking uptake. Archives of Pediatrics and Adolescent Medicine 161(5):440-445.
Sorof, J., and S. Daniels. 2002. Obesity hypertension in children: A problem of epidemic proportions. Hypertension 40(4):441-447.
Sorof, J. M., A. V. Alexandrov, G. Cardwell, and R. J. Portman. 2003. Carotid artery intimalmedial thickness and left ventricular hypertrophy in children with elevated blood pressure. Pediatrics 111(1):61-66.
Sowden, A. J., and L. Arblaster. 2000. Mass media interventions for preventing smoking in young people. Cochrane Database of Systematic Reviews (2):CD001006.
Stein, A. D., A. M. Thompson, A. Waters, A. D. Stein, A. M. Thompson, and A. Waters. 2005. Childhood growth and chronic disease: Evidence from countries undergoing the nutrition transition. Maternal and Child Nutrition 1(3):177-184.
Stein, C. E., C. H. D. Fall, K. Kumaran, C. Osmond, V. Cox, and D. J. P. Barker. 1996. Fetal growth and coronary heart disease in south India. Lancet 348(9037):1269-1273.
Story, M., and S. French. 2004. Food advertising and marketing directed at children and adolescents in the U.S. International Journal of Behavioral Nutrition and Physical Activity 1(1):3.
Strasburger, V. C. 2001. Children and TV advertising: Nowhere to run, nowhere to hide. Journal of Developmental and Behavioral Pediatrics 22(3):185-187.
Strong, J. P., G. T. Malcom, C. A. McMahan, R. E. Tracy, W. P. Newman, 3rd, E. E. Herderick, and J. F. Cornhill. 1999. Prevalence and extent of atherosclerosis in adolescents and young adults: Implications for prevention from the Pathobiological Determinants of Atherosclerosis in Youth Study. Journal of the American Medical Association 281(8):727-735.
Swart, D., S. Panday, S. P. Reddy, E. Bergstrom, and H. de Vries. 2006. Access point analysis: What do adolescents in South Africa say about tobacco control programmes? Health Education Research 21(3):393-406.
Taras, H. L., J. F. Sallis, T. L. Patterson, P. R. Nader, and J. A. Nelson. 1989. Television’s influence on children’s diet and physical activity. Journal of Developmental and Behavioral Pediatrics 10(4):176-180.
Tyas, S. L., and L. L. Pederson. 1998. Psychosocial factors related to adolescent smoking: A critical review of the literature. Tobacco Control 7:409-420.
UNICEF (United Nations Children’s Fund). 2009. State of the world’s children 2009: Maternal and newborn health. New York: UNICEF.
U.S. Department of Health and Human Services. 1994. Preventing tobacco use among young people: A report of the surgeon general. Atlanta, GA: Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, U.S. Department of Health and Human Services, Public Health Service.
van Sluijs, E. M. F., A. M. McMinn, and S. J. Griffin. 2007. Effectiveness of interventions to promote physical activity in children and adolescents: Systematic review of controlled trials. British Medical Jornal 335(7622):703.
Verma, M., J. Chhatwal, and S. M. George. 1994. Obesity and hypertension in children. In Indian Pediatrics 31(9):1065-1069.
Veugelers, P. J., and A. L. Fitzgerald. 2005. Effectiveness of school programs in preventing childhood obesity: A multilevel comparison. American Journal of Public Health 95(3):432-435.
Victora, C. G., L. Adair, C. Fall, P. C. Hallal, R. Martorell, L. Richter, and H. S. Sachdev. 2008. Maternal and child undernutrition: Consequences for adult health and human capital. Lancet 371(9609):340-357.
Volunteer Health Association of India. 2009. Tobacco control in India: What have we achieved till date? New Delhi: Volunteer Health Association of India.
Wakefield, M., B. Flay, M. Nichter, and G. Giovino. 2003. Effects of anti-smoking advertising on youth smoking: A review. Journal of Health Communication 8(3):229-247.
Walker, S., and S. George. 2007. Young@heart. USA: Fox Searchlight Pictures.
Warren, C. W., N. R. Jones, M. P. Eriksen, and S. Asma. 2006. Patterns of global tobacco use in young people and implications for future chronic disease burden in adults. Lancet 367(9512):749-753.
Whitaker, R. C. 2004. Predicting preschooler obesity at birth: The role of maternal obesity in early pregnancy. Pediatrics 114(1):e29-e36.
WHO (World Health Organization). 2003. WHO Framework Convention on Tobacco Control. Geneva: World Health Organization.
WHO. 2008a. WHO report on the global tobacco epidemic, 2008: The mpower package. Geneva: World Health Organization.
WHO. 2008b. Childhood overweight and obesity. http://www.who.int/dietphysicalactivity/childhood/en/ (accessed December 12, 2008).
WHO. 2009. Aging and life course. Geneva: World Health Oranization.
WHO. 2010a. Global school health initiative. http://www.who.int/school_youth_health/gshi/en/ (accessed March 9, 2010).
WHO. 2010b. Tobacco free initiative. http://www.who.int/tobacco/en/index.html (accessed March 9, 2010).
WHO Global InfoBase. 2008. Overweight & obesity (BMI) country data. Geneva: World Health Organization.
WHO Mega Country Health Promotion Network. 2001. Recommendations from the fourth annual meeting of the school health component of the WHO mega country health promotion network. Paris: World Health Organization.
Yach, D., C. Hawkes, C. L. Gould, and K. J. Hofman. 2004. The global burden of chronic diseases: Overcoming impediments to prevention and control. Journal of the American Medical Association 291(21):2616-2622.
Yajnik, P. C., and C. S. Yajnik. 2009. Predictive equations for body fat in Asian Indians. Obesity 17(5):935-936.
Youth For Health. 2009. Y4H. http://www.y4h.hriday-shan.org (accessed February 19, 2010).