7
Socioecological Perspectives: The Environmental Level
|
Key Messages Noted by Participants
|
One critical question from the socioecological perspective is whether the environment is a mediating factor between food insecurity and obesity, said Katherine Alaimo, associate professor in the Department of Food Science and Human Nutrition at Michigan State University, who moderated the session on the environmental level. “Regardless of whether or not there is a causal pathway between food insecurity and overweight we know that [they can] coexist,” she said. “There is a possibility that one of the reasons why both of these things exist is because of [influences from] the environ-
ment.” Three speakers addressed this topic at the workshop, focusing specifically on the availability, quality, and marketing of food.
THE FOOD ENVIRONMENT IN COMMUNITIES
Obesogenic environments are becoming more common, said Angela Odoms-Young, assistant professor in the Department of Kinesiology and Nutrition at the University of Illinois at Chicago. The least expensive food options are typically high in calories and low in nutrients. Households with limited resources tend to spend less on food overall and less on healthful foods such as fruits and vegetables (Alaimo et al., 2001; Drewnowski and Specter, 2004; Hartline-Grafton et al., 2009; Ludwig and Pollack, 2009; Larson and Story, 2010a).
Some evidence suggests that food-insecure families may be more susceptible to obesogenic environments for a variety of reasons including the ways in which food assistance is distributed, maternal stress, and disruptive family routines (Anderson and Whitaker, 2010; Gundersen et al., 2010). In addition, race/ethnicity, poverty, household structure, and location (such as living in a rural or urban area or in the Midwest or South) all interact with both food insecurity and obesity in complicated ways (Kendall et al., 1996; Blanchard and Lyson, 2002; Powell et al., 2007; Nord et al., 2008; Sharma et al., 2009; Chen and Escarce, 2010; Grow et al., 2010; Ogden et al., 2010).
Surprisingly, Odoms-Young said, relatively few studies have looked at the ways in which the environment, food insecurity, and obesity are interconnected. She discussed several possible mechanisms that could tie together these three phenomena as a guide to future research.
Energy-Dense Foods
The first mechanism is the high availability of energy-dense food options and the low cost of less healthful options. People living in low-income areas and communities of color tend to have less access to outlets that carry more healthful food options and greater access to stores with less healthful options (Cheadle et al., 1991; Morland et al., 2002a, 2002b; Laraia et al., 2004; Lewis et al., 2005; Zenk et al., 2005). Odoms-Young cited one study that looked at the relationship between food pantry clients and the food environment in Pomona, California, which demonstrated that these families had lower access to stores that carried more healthful food options and that only 9 percent lived within walking distance of the pantry (Algert et al., 2006). In this study, 83 percent of food pantry clients were within walking distance of stores with limited or no produce, generally small to midsized convenience marts, while 41 percent of the food pantry clients did not live within walking distance of a store carrying a variety of fresh produce.
Odoms-Young described studies she has conducted in Chicago and Detroit in neighborhoods with reduced access to healthful foods. As one person surveyed in Chicago said, “You go all the way out to the suburbs where the white people live at and you find everything…. It’s even a better variety in [chain supermarkets] when you go to their stores. There’s a difference.” Another person interviewed in Detroit said, “You’ve got to go out in the suburbs now to get some decent food. And therefore, it’s not available for us in this community. By the time you get to that store and get some fresh fruits and vegetables, you’re going to pass about 30 fast-food joints and about 100 liquor stores.” In these cases, added Odoms-Young, the stress of living in neighborhoods perceived to be substandard may further contribute to obesity.
Dietary energy density tends to be inversely associated with dietary quality and cost, so that people eating more calorie-dense foods are eating less healthful and cheaper foods, regardless of socioeconomic status (Monsivais and Drewnowski, 2009; Townsend et al., 2009). These dietary patterns are in turn associated with obesity. For example, Powell et al. (2010) found that a 10 percent increase in the price of fruits and vegetables was associated with a 0.7 percent increase in child body mass index (BMI). The impact of prices on BMI was stronger in both magnitude and significance for children of low compared to high socioeconomic status (SES).
Food Marketing
The marketing of foods is another mechanism that could create differences between higher-income and lower-income communities. Yancey et al. (2009) showed that living in an upper-income neighborhood, regardless of the residents’ predominant ethnicity, is generally protective against exposure to most types of obesity-promoting outdoor advertising, including fast food, sugar-sweetened beverages, sedentary entertainment, and transportation advertisements. Food advertising coverage was greatest in low-income Latino neighborhoods, and fast-food advertisement coverage differed by neighborhood income but not ethnicity. The most advertisements for sugar-sweetened beverages were found in low-income African-American neighborhoods. Even though there was less advertising coverage in upper-income than in low-income African-American neighborhoods, it was similar to the coverage levels in low-income white and Latino neighborhoods.
Odoms-Young and her colleagues have done a study with low-income African-American families of how food marketing and environmental factors affect consumption (Odoms-Young et al., 2010). Low-income and food-insecure families can be very sensitive to discount-oriented marketing, she said. In her study, many families received information about food
products from store circulars and other types of community promotions. Many families reported that marketing efforts for unhealthful foods were most intensive at the time people received food benefits. As one person said, “So you’d about spent all your stamps on the junk food, cause you ain’t even got to the meat and stuffs. You are still over here in this one aisle. But there is how it is. All the pop stacked up against the wall right there, you got your box of cookies, big box of cookies over here.”
Violence
Community violence plays a role in food choices. In some locations where people access food, violence and other illegal activities are frequent. People may not go at night to certain stores to avoid robberies or other forms of crime.
Unfair Treatment
Zenk et al. (2010) have shown that greater everyday unfair treatment and an acute experience of unfair treatment in the past year were positively associated with greater consumption of comfort foods in the presence of a convenience store in the neighborhood. In contrast, for those with a large grocery store in the neighborhood, greater everyday unfair treatment and neighborhood physical environment stress were negatively related to comfort food intake.
Low-Resource Environments as a Source of Stress
Negotiating a low-resource environment can be a major source of stress. Odoms-Young reported that another interviewee in her study said, “That’s the thing that kills us most because most of us don’t watch what we eat you know…. Most of us in this area are stressed beyond belief. Because they are trying to make ends meet, they’re trying to figure out how they’re going to feed their families or how are they going get their kids to school next week off the $54 paycheck they just got. So you know high blood pressure is a big thing and diabetes is another big thing because of, again, we don’t watch what we eat and we don’t exercise properly.”
Research Considerations
In conclusion, said Odoms-Young, the evidence suggests that the environment affects the relationship between food insecurity and obesity. She said that more research is needed on the following:
-
The cost of food, marketing, and community stressors
-
The varying impact of social, economic, and geographic factors
-
The relationship of the food environment to obesity among families that are not food insecure, including high-income families
THE FOOD ENVIRONMENT IN SCHOOLS
The Food Trust, which was founded in 1992, is an organization of about 85 people based in Philadelphia that seeks to increase access to affordable, nutritious food. “Are children, especially those at risk of hunger, eating the right amount of the right kinds of foods to maintain a healthful diet?” This question speaks to the quantity, frequency, and quality of the food that children eat, said Allison Karpyn, director of research and evaluation for The Food Trust.
Eating Opportunities During the School Day
Students have a variety of opportunities to eat at school. Reimbursable school meals include breakfast, lunch, twilight meals (after-school meals provided by the Child and Adult Care Food Program), and snacks, and summer meals when school is not in session. Competitive foods—so called because they compete with the foods provided by schools—include vending machine items, foods from school stores, rewards from teachers, and foods made available at class parties and fundraisers. Foods brought into schools from outside include those prepared at home, bought from stores, and purchased at fast-food restaurants.
For the average child, on a school day 26 percent of daily energy is obtained and consumed at school, according to national survey data (Briefel et al., 2009a). If a child participates in the National School Lunch Program (NSLP), the proportion increases to 35 percent. If a child participates in both the NSLP and the School Breakfast Program (SBP), the figure is 47 percent.
Food Assistance Programs in Schools
Among the children who are certified for reimbursable school meals, more than 40 percent are from families that earn less than $10,000 a year. “This is a striking statistic for me,” said Karpyn. “We are talking about a number of families that come from very low incomes.”
Karpyn displayed a typical breakfast menu (Figure 7-1) and lunch menu (Figure 7-2) for Philadelphia’s public schools. Children get an average of about 400 calories from breakfast and 560 calories from lunch. About 31 million children participated in the NSLP in 2009, which represents about
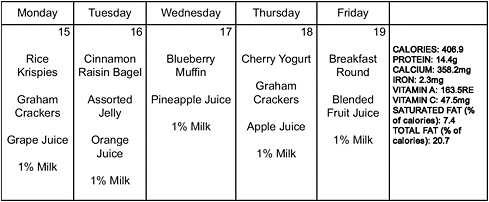
FIGURE 7-1 A typical school breakfast menu for Philadelphia public schools.
SOURCE: School District of Philadelphia, 2010. See http://www.phila.k12.pa.us/ (accessed January 26, 2011).
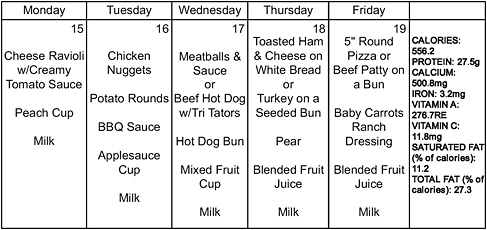
FIGURE 7-2 A typical school lunch menu for Philadelphia public schools.
SOURCE: School District of Philadelphia, 2010. See http://www.phila.k12.pa.us/ (accessed January 26, 2011).
60 percent of school-aged children in America, at a cost of about $10 billion. About 11 million participated in the SBP, representing a cost of about $3 billion. Among children eligible for free and reduced-price meals, 79 percent of those who are eligible for a free meal on average each day actually take a lunch, while 71 percent of those eligible for a reduced-price lunch do so.
Participation in the NSLP went up 13 percent from 2000 to 2008 (School Nutrition Association, 2009), while the SBP saw an increase in participation of 40 percent over the same period. However, the effectiveness
in reaching low-income students with the SBP varies greatly among cities, from 98 percent in Portland, Oregon, to about 29 percent in New York City and Chicago (Levin et al., 2007).
Participation in the SBP is associated with lower BMI, although the effect size is small (Gleason et al., 2009). Other researchers, such as Millimet et al. (2010), have found null or modestly beneficial effects and cite evidence of nonrandom selection into the SBP as a problem with such studies. Overall, said Karpyn, although some changes in the program are desirable, “it looks like school breakfast is basically a good thing.”
Participation in the NSLP, in contrast, appears to have a null or possibly detrimental connection to BMI, according to Millimet et al. (2010). However, some researchers have found positive influences on dietary intakes, such as reduced intake of sugar-sweetened beverages and increased intake of fruits and vegetables (Briefel et al., 2009b). Data from the National Health and Nutrition Examination Survey (NHANES) show that some children who are participating in the NSLP are eating more nutrient-dense lunches, including more milk, fruits, and vegetables (Cole and Fox, 2008).
Competitive Foods
According to a nationwide study of the food consumed at school, home, and other locations, about 17 percent of the calories public school children consumed consisted of foods brought into school from outside (Briefel et al., 2009a). About 50 percent of the children studied in a Philadelphia-based project shopped at least once a day in corner stores, about 40 percent shopped twice a day, and at each purchasing opportunity they bought about 350 calories and spent about a dollar on food (Borradaile et al., 2009).
Larson and Story (2010b) have found that limiting access to competitive foods improves diets. In Philadelphia, the top 10 purchased items include bottled water, Doritos, blow pops, gum, Cheetos, and—at number 1—Hugs, which are 8-ounce sugar-sweetened beverages (Borradaile et al., 2009). Vending machines, school stores, and snack bars remain very prevalent in schools and are largely exempt from federal standards. School wellness policies may regulate such food outlets, but these policies generally are not enforced. Schools have competing priorities, because food sales generate revenue.
Models for Improving School Eating
In Philadelphia, The Food Trust worked with the School District of Philadelphia and a number of collaborators on the School Nutrition Policy Initiative. A taskforce of 40 people representing different sectors has established school health and wellness councils. All schools completed a
School Health Index and a School Health Action Plan. Social marketing, food guidelines, and nutrition education were at the center of the initiative. Teachers received 10 hours of nutrition training, and family members and the community were involved. Over a 2-year period, 15 percent of students became overweight in the control schools versus 7.5 percent in the schools where the interventions were implemented (Foster et al., 2008). However, the initiative did not have an effect on the remission of obesity (i.e., moving individuals from overweight or obesity to a normal weight).
Another program that has led to changes in schools is the Healthy Corner Store Initiative. The Food Trust has worked with hundreds of corner stores to change their product mix and promote more healthful products. A school-based program also has been instituted to educate students about how to improve their purchasing patterns in corner stores.
Policy and Practice Considerations
Karpyn listed changes in policy and practice that could have an effect on child obesity:
-
Enforce wellness policies
-
Make breakfast part of the school day
-
Include meal participation rates on school report cards
-
Increase the reimbursement rate
-
Provide universal free meals
-
Reevaluate procurement practices to improve available foods
-
Provide integrated nutrition education
-
Establish school wellness councils
-
Create standards and accountability for competitive foods
-
Engage in farm-to-school programming
-
Continue working with corner stores
Research Considerations
Karpyn also listed the following research considerations:
-
What strategies are most effective in upgrading the food consumed from school lunch lines? Possibilities include increases in reimbursement rates, strategic procurement, educational interventions, farm-to-school programs, and taste testing.
-
In what ways do food marketing, merchandizing, and product placement influence purchasing and consumption in schools and at stores?
-
How does the availability of competitive food affect participation in food assistance programs in schools?
-
What can cross-disciplinary studies reveal about diet, educational achievement, and behavioral outcomes?
-
How can taxpayers be engaged in the support of research and the implementation of research-based policies?
Karpyn concluded by calling to task politicians who blame the hungry for their condition. “We have ignored for too long the pervasive attitude of pointing blame back at the individuals who are struggling. We haven’t done enough to engage the taxpayers to talk about what is in it for them, why this is a societal issue, and why we need to be responsible as taxpayers.”
FOOD-INSECURE NEIGHBORHOODS
In the final presentation of the session on environmental factors, Diego Rose, professor in the Department of Community Health Sciences at Tulane University, challenged the argument that environments impact the relationships between food insecurity and obesity, unless one considers a neighborhood or an environment itself as being food insecure. This viewpoint might alter our understanding of the coexistence of poverty, food insecurity, and obesity.
Store Access and Food Consumption
Rose reviewed studies linking neighborhood access to stores and consumption, beginning with the work done by Morland and colleagues (2002a) that linked the presence or absence of a supermarket in a census tract to fruit and vegetable consumption among African Americans. Similarly, Blanchard and Lyson (2003) demonstrated a relationship between residence in a food desert and decreased fruit and vegetable intake.
In the United Kingdom, Wrigley et al. (2002) showed that the opening of a new supermarket leads to increased fruit and vegetable intake. Laraia et al. (2004) and Rose and Richards (2004) also showed that improved access to a supermarket leads to improved diets and increased fruit intake, respectively, findings confirmed by Moore et al. (2008). “What those studies show is that there is a connection between [access to] stores and consumption.”
Rose put these findings into the context of a consumer choice model (Figure 7-3). In traditional models, food purchases are determined by the prices of goods, household income, and tastes and preferences, which are often modeled with proxies such as age, ethnicity, or education. Rose focused instead on food cost, which includes the price for food and how much
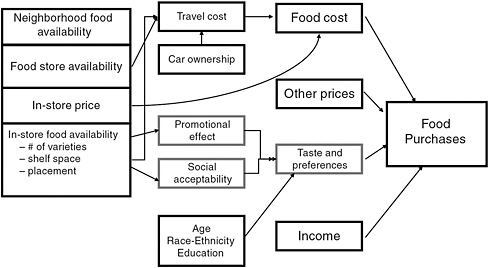
FIGURE 7-3 Food purchases depend on a number of factors in addition to food availability and price.
SOURCE: Rose et al., 2010. Adapted from Journal of Nutrition (2010; 140:1170-1174), © 2010 American Society for Nutrition.
it costs to travel to a store. This depends on such factors as the distance to a store, what is offered in a store, and whether a person owns a car. The variety of products, shelf location, and marketing also can affect preferences through promotional effects and social acceptability.
Food purchases are in turn related to consumption and obesity, which would require additional boxes to the right of his model, said Rose. For example, Morland et al. (2006) have linked the presence of supermarkets in a census tract to a decreased prevalence of obesity and the presence of convenience stores to increased obesity. Powell and colleagues (2007) have connected chain supermarket density to decreased BMI and convenience store density to increased BMI. Smaller-scale studies, such as Lopez (2007) and Rose et al. (2009), have produced similar results. In a national longitudinal study, Sturm and Datar (2005) found that the higher the price for fruits and vegetables in area stores, the higher was the BMI for first-through third-grade students.
Neighborhood Food Availability and Consumption
Focusing solely on store access, however, misses the point that not all stores offer the same products. A number of studies have used in-store surveys to study the foods available in a neighborhood and the connection
to consumption. For example, Cheadle et al. (1991) found an association between shelf space for low-fat milk, meats, and high-fiber breads and people’s consumption of those products in 12 communities in California and Hawaii. Fisher and Strogatz (1999) and Edmonds and colleagues (2001) also looked at the links between the foods being offered in stores and restaurants and consumption. Franco et al. (2009) used the Nutrition Environment Measures Survey (NEMS) to develop a score of diet quality in the store and looked at consumption, finding a relationship between low diet quality and low availability of healthful foods.
Rose and his colleagues found associations in four census tracts in New Orleans between the shelf space allotted to vegetables and vegetable consumption (Bodor et al., 2008). In another study of 103 tracts in southeastern Louisiana, the shelf space allotted to energy-dense snacks was linked with greater BMI (Rose et al., 2009). “If you measure the chips, cookies, candies, and sodas and add it all up within a kilometer of where people live, there is an association with body mass index.”
School Food Environments
Rose also discussed the consumption of food in schools. In a study of the NSLP, Gordon and Fox (2007) found that participants in the program had a higher consumption of calories than nonparticipants. However, their lunches tended to include more nutrients along with more calories, and participants in the program had lower consumption of competitive foods.
Several studies have looked at the availability of vending machines and consumption. Kubik et al. (2003) found a negative association between the availability of vending machine snacks and fruit and vegetable consumption in Minnesota middle schools. In Washington State middle schools, the availability of sugar-sweetened beverages in vending machines was positively associated with consumption (Johnson et al., 2009). Rovner and colleagues (2011), based on a national sample from 2006 and 2007, found that vending machines with fruits, vegetables, and candies each showed a positive association with consumption.
Research Considerations
In summary, said Rose, neighborhood studies show associations between food environments, dietary intake, and weight. However, most of these studies are cross-sectional. Future research needs to look at interventions or panel studies to determine causality, particularly regarding the effects of prices on consumption and obesity, he said.
GROUP DISCUSSION
Moderator: Katherine Alaimo
During the group discussion period, points raised by participants included the following:
Shopping Destinations
Adam Drewnowski observed that research also needs to look at where people actually shop, not just at the characteristics of the stores in a neighborhood. Many people do not shop in their immediate neighborhood. In Seattle, where people tend to shop by car, they may go to a supermarket considerably farther away than the one nearest their homes. “We need to have data on destinations, not just distance.”
Karpyn noted that Amy Hillier at the University of Pennsylvania is doing qualitative and quantitative work on how people shop. When people are using their WIC (Special Supplemental Nutrition Program for Women, Infants, and Children) vouchers, they tend to go to the nearest corner store because they are not price sensitive, she said. With SNAP (Supplemental Nutrition Assistance Program) benefits, they may go to a supermarket. “I agree with you. It is very complicated.”
Modes of Transportation to Shopping
Odoms-Young pointed out that many studies are not able to capture all of the places where people shop. Her studies have shown that some people are walkers and some are riders, and not all riders have cars. In the latter case, people may need to exchange something for rides, which involves social costs. For example, if someone is coming to another person’s home to do informal work, that person may be able to get a ride to or from home or a store. People also have access to food from other people’s homes and from food pantries, not just from stores.
Store Layout
Rose described a proposed study that would convert shelf space at corner stores from junk food to fruits and vegetables and determine the effects. To prepare for the study, he and his colleagues asked a random sample of 100 people from the neighborhoods selected for the study about everything consumed in the previous 24 hours and where it was purchased. They found that 75 percent of the people did not use the corner store. Of the 25 percent who did, the items targeted for intervention by the study
were a minor dietary factor (which led to changes in the study design). The major source of calories from corner stores was the lunch counter in the back preparing sandwiches and other foods.
Programs for Very Young Children
Alexandra Adams mentioned the importance of preschool and home day care environments. These programs tend to use different food reimbursement programs than do schools, which can affect consumption.
Food Use in Homes
Adams also mentioned that people may use WIC to feed their entire families, not just their children, which could have adverse consequences on some children. Finally, she emphasized not just whether food is available in the home but how it is used. For example, is anyone able to cook food? “A lot of the families that I work with of all ethnicities have really low cooking skills. Because of that, they value getting prepared foods that are more expensive, or they value being able to go out to fast foods.” The role of cooking skills is an important target for research, she said, because simply increasing the availability of food will not necessarily lead to greater use of that food.
REFERENCES
Alaimo, K., C. M. Olson, and E. A Frongillo, Jr. 2001. Low family income and food insufficiency in relation to overweight in U.S. children: Is there a paradox? Archives of Pediatrics and Adolescent Medicine 155(10):1161-1167.
Algert, S. J., A. Agrawal, and D. S. Lewis. 2006. Disparities in access to fresh produce in low-income neighborhoods in Los Angeles. American Journal of Preventive Medicine 30(5):365-370.
Anderson, S. E., and R. C. Whitaker. 2010. Household routines and obesity in US preschoolaged children. Pediatrics 125(3):420-428.
Blanchard, T., and T. Lyson. 2002. Access to low cost groceries in nonmetropolitan counties: Large retailers and the creation of food deserts. Ithaca, NY: Cornell University.
Blanchard, T., and T. Lyson. 2003. Retail concentration, food deserts, and food-disadvantaged communities in rural America. Final Report for Food Assistance Grant Program, Southern Rural Development Center. Mississippi State University: Economic Research Service, U.S. Department of Agriculture.
Bodor, J. N., D. Rose, T. A. Farley, C. Swalm, and S. K. Scott. 2008. Neighbourhood fruit and vegetable availability and consumption: The role of small food stores in an urban environment. Public Health Nutrition 11(4):413-420.
Borradaile, K. E., S. Sherman, S. S. Vander Veur, T. McCoy, B. Sandoval, J. Nachmani, A. Karpyn, and G. D. Foster. 2009. Snacking in children: The role of urban corner stores. Pediatrics 124(5):1293-1298.
Briefel, R. R., A. Wilson, and P. M. Gleason. 2009a. Consumption of low-nutrient, energy-dense foods and beverages at school, home, and other locations among school lunch participants and nonparticipants. Journal of the American Dietetic Association 109(2).
Briefel, R. R., M. K. Crepinsek, C. Cabili, A. Wilson, and P. M. Gleason. 2009b. School food environments and practices affect dietary behaviors of US public school children. Journal of the American Dietetic Association 109(2).
Cheadle, A., B. M. Psaty, S. Curry, E. Wagner, P. Diehr, T. Koepsell, and A. Kristal. 1991. Community-level comparisons between the grocery store environment and individual dietary practices. Preventive Medicine 20(2):250-261.
Chen, A. Y., and J. J. Escarce. 2010. Family structure and childhood obesity, Early Childhood Longitudinal Study—Kindergarten Cohort. Preventing chronic disease 7(3).
Cole, N., and M. K. Fox. 2008. Diet quality of American young children by WIC participation status: Data from the National Health and Nutrition Examination Survey, 1999-2004. Document No. PR08-67. Washington, DC: Abt Associates, Inc. and Mathematica Policy Research.
Drewnowski, A., and S. E. Specter. 2004. Poverty and obesity: The role of energy density and energy costs. American Journal of Clinical Nutrition 79(1):6-16.
Edmonds, J., T. Baranowski, J. Baranowski, K. W. Cullen, and D. Myres. 2001. Ecological and socioeconomic correlates of fruit, juice, and vegetable consumption among African-American boys. Preventive Medicine 32(6):476-481.
Fisher, B. D., and D. S. Strogatz. 1999. Community measures of low-fat milk consumption: Comparing store shelves with households. American Journal of Public Health 89(2):235-237.
Foster, G. D., S. Sherman, K. E. Borradaile, K. M. Grundy, S. S. Vander Veur, J. Nachmani, A. Karpyn, S. Kumanyika, and J. Shults. 2008. A policy-based school intervention to prevent overweight and obesity. Pediatrics 121(4).
Franco, M., A. V. Diez-Roux, J. A. Nettleton, M. Lazo, F. Brancati, B. Caballero, T. Glass, and L. V. Moore. 2009. Availability of healthy foods and dietary patterns: The Multi-Ethnic Study of Atherosclerosis. American Journal of Clinical Nutrition 89(3):897-904.
Gleason, P. M., R. Briefel, A. Wilson, and A. H. Dodd. 2009. School meal program participation and its association with dietary patterns and childhood obesity. Contractor and cooperator report no. 55. Washington, DC: Mathematica Policy Research.
Gordon, A., and M. K. Fox. 2007. School Nutrition Dietary Assessment Survey-III: Summary of findings. Washington, DC: USDA Food and Nutrition Service.
Grow, H. M. G., A. J. Cook, D. E. Arterburn, B. E. Saelens, A. Drewnowski, and P. Lozano. 2010. Child obesity associated with social disadvantage of children’s neighborhoods. Social Science & Medicine 71(3):584-591.
Gundersen, C., D. Mahatmya, S. Garasky, and B. Lohman. 2010. Linking psychosocial stressors and childhood obesity. Obesity Reviews DOI: 10.1111/j.1467-789X.2010.00813.x.
Hartline-Grafton, H. L., D. Rose, C. C. Johnson, J. C. Rice, and L. S. Webber. 2009. Energy density of foods, but not beverages, is positively associated with body mass index in adult women. European Journal of Clinical Nutrition 63(12):1411-1418.
Johnson, D. B., B. Bruemmer, A. E. Lund, C. C. Evens, and C. M. Mar. 2009. Impact of school district sugar-sweetened beverage policies on student beverage exposure and consumption in middle schools. Journal of Adolescent Health 45(3 SUPPL.).
Kendall, A., C. M. Olson, and E. A. Frongillo. 1996. Relationship of hunger and food insecurity to food availability and consumption. Journal of the American Dietetic Association 96(10):1019-1024.
Kubik, M. Y., L. A. Lytle, P. J. Hannan, C. L. Perry, and M. Story. 2003. The association of the school food environment with dietary behaviors of young adolescents. American Journal of Public Health 93(7):1168-1173.
Laraia, B. A., A. M. Siega-Riz, J. S. Kaufman, and S. J. Jones. 2004. Proximity of supermarkets is positively associated with diet quality index for pregnancy. Preventive Medicine 39(5):869-875.
Larson, N., and M. Story. 2010a. Food insecurity and risk for obesity among children and families: Is there a relationship? A research synthesis. Princeton, NJ, and Minneapolis, MN: Robert Wood Johnson Foundation Healthy Eating Research.
Larson, N., and M. Story. 2010b. Are “competitive foods” sold at school making our children fat? Health Affairs 29(3):430-435.
Levin, M., J. Adach, R. Cooper, L. Parker, and M. Saltzman. 2007. School breakfast in America’s big cities: Successes and shortfalls. Washington, DC: Food Research and Action Center.
Lewis, L. B., D. C. Sloane, L. M. Nascimento, A. L. Diamant, J. J. Guinyard, A. K. Yancey, and G. Flynn. 2005. African Americans’ access to healthy food options in South Los Angeles restaurants. American Journal of Public Health 95(4):668-673.
Lopez, R. P. 2007. Neighborhood risk factors for obesity. Obesity 15(8):2111-2119.
Ludwig, D. S., and H. A. Pollack. 2009. Obesity and the economy from crisis to opportunity. Journal of the American Medical Association 301(5):533-535.
Millimet, D. L., R. Tchernis, and M. Husain. 2010. School nutrition programs and the incidence of childhood obesity. Journal of Human Resources 45(3):640-654.
Monsivais, P., and A. Drewnowski. 2009. Lower-energy-density diets are associated with higher monetary costs per kilocalorie and are consumed by women of higher socioeconomic status. Journal of the American Dietetic Association 109(5):814-822.
Moore, L. V., A. V. Diez Roux, J. A. Nettleton, and D. R. Jacobs. 2008. Associations of the local food environment with diet quality—A comparison of assessments based on surveys and geographic information systems. American Journal of Epidemiology 167(8):917-924.
Morland, K., S. Wing, and A. D. Roux. 2002a. The contextual effect of the local food environment on residents’ diets: The Atherosclerosis Risk in Communities Study. American Journal of Public Health 92(11):1761-1767.
Morland, K., S. Wing, A. Diez Roux, and C. Poole. 2002b. Neighborhood characteristics associated with the location of food stores and food service places. American Journal of Preventive Medicine 22(1):23-29.
Morland, K., A. V. Diez Roux, and S. Wing. 2006. Supermarkets, other food stores, and obesity: The Atherosclerosis Risk in Communities Study. American Journal of Preventive Medicine 30(4):333-339.
Nord, M., M. Andrews, and S. Carlson. 2008. Household food security in the United States, 2007. Economic Research Report No. 66. Washington, DC: Economic Research Service.
Odoms-Young, A., S. Zenk, L. Holland, A. Watkins, J. Wroten, N. Oji-Njideka, S. Ellis, I. Davis, C. Dallas, M. Fitzgibbon, R. Jarrett, M. Mason, A. Webb, and D. Sharp. 2010. Family food access report: When we have better, we can do better. Chicago, IL: University of Illinois at Chicago and Chicago Department of Public Health Englewood Neighborhood Health Center.
Ogden, C. L., M. D. Carroll, L. R. Curtin, M. M. Lamb, and K. M. Flegal. 2010. Prevalence of high body mass index in U.S. children and adolescents, 2007-2008. Journal of the American Medical Association 303(3):242-249.
Powell, L. M., F. J. Chaloupka, and Y. Bao. 2007. The availability of fast-food and full-service restaurants in the United States. Associations with neighborhood characteristics. American Journal of Preventive Medicine 33(4 SUPPL.).
Powell, L. M., E. Han, and F. J. Chaloupka. 2010. Economic contextual factors, food consumption, and obesity among U.S. adolescents. Journal of Nutrition 140(6):1175-1180.
Rose, D., and R. Richards. 2004. Food store access and household fruit and vegetable use among participants in the US Food Stamp Program. Public Health Nutrition 7(8):1081-1088.
Rose, D., P. L. Hutchinson, J. N. Bodor, C. M. Swalm, T. A. Farley, D. A. Cohen, and J. C. Rice. 2009. Neighborhood food environments and body mass index. The importance of in-store contents. American Journal of Preventive Medicine 37(3):214-219.
Rose, D., J. N. Bodor, P. L. Hutchinson, and C. M. Swalm. 2010. The importance of a multidimensional approach for studying the links between food access and consumption. Journal of Nutrition 140(6):1170-1174.
Rovner, A. J., T. R. Nansel, J. Wang, and R. J. Iannotti. 2011. Food sold in school vending machines is associated with overall student dietary intake. Journal of Adolescent Health 48(1):13-19.
School Nutrition Association. 2009. The pressure cooker: School meals face rising costs and participation. National Harbor, MD: School Nutrition Association.
Sharma, A. J., L. M. Grummer-Strawn, K. Dalenius, D. Galuska, M. Anandappa, E. Borland, H. Mackintosh, and R. Smith. 2009. Obesity prevalence among low-income, preschool-aged children: United States, 1998-2008. Morbidity and Mortality Weekly Report 58(28):769-773.
Sturm, R., and A. Datar. 2005. Body mass index in elementary school children, metropolitan area food prices and food outlet density. Public Health 119(12):1059-1068.
Townsend, M. S., G. J. Aaron, P. Monsivais, N. L. Keim, and A. Drewnowski. 2009. Less-energy-dense diets of low-income women in California are associated with higher energy-adjusted diet costs. American Journal of Clinical Nutrition 89(4):1220-1226.
Wrigley, N., C. Guy, and M. Lowe. 2002. Urban regeneration, social inclusion and large store development: The Seacroft development in context. Urban Studies 39(11):2101-2114.
Yancey, A. K., B. L. Cole, R. Brown, J. D. Williams, A. Hillier, R. S. Kline, M. Ashe, S. A. Grier, D. Backman, and W. J. McCarthy. 2009. A cross-sectional prevalence study of ethnically targeted and general audience outdoor obesity-related advertising. Milbank Quarterly 87(1):155-184.
Zenk, S. N., A. J. Schulz, B. A. Israel, S. A. James, S. Bao, and M. L. Wilson. 2005. Neighborhood racial composition, neighborhood poverty, and the spatial accessibility of supermarkets in metropolitan Detroit. American Journal of Public Health 95(4):660-667.
Zenk, S. N., A. J. Schulz, G. Mentz, B. A. Israel, and M. Lockett. 2010. Do obesogenic neighborhood food environments exacerbate effects of psychosocial stressors on ‘comfort’ food intake? Presented at the International Society of Behavioral Nutrition and Physical Activity Conference, Minneapolis, MN.
















