5
Expenditures and Financing for Oral Health Care
Understanding how oral health services are financed in the United States is critical to the access question. Financing for oral health care greatly influences where and whether individuals receive care. At the individual level, dental coverage and socioeconomic factors play a significant role in access to oral health care. That is, individuals who have private dental coverage or can afford care, either through private insurance or through out-of-pocket expenditures, are generally able to obtain care. On the other hand, individuals who lack dental coverage, who have minimal dental coverage, and/or those of limited financial means experience significant barriers to care. Financing also has a powerful influence on providers’ practice patterns. For example, low reimbursement by public programs, such as Medicaid and the Children’s Health Insurance Program (CHIP), are often cited as a disincentive to providers’ willingness to participate in these publicly funded programs. Finally, state and federal spending on oral health has a tremendous impact on what oral health services are available and to whom. This begins at the level of support for dental schools and continues in the form of subsidies for residency programs, reimbursement policies of public insurance programs, mandated benefits, and additional financial incentives. For example, the federal government makes considerable investments in improving the distribution of oral health care professionals in urban and rural areas while states are authorized under federal law to determine the rate of Medicaid reimbursement for oral health services provided.
This chapter provides an overview of the various sources and mechanisms of financing for oral health care in the United States and describes the
influences that these expenditures have on access to oral health care among vulnerable and underserved populations.
Health care costs and spending have been rapidly increasing in the United States in recent years. In 2009, overall health expenditures were $2.5 trillion, including the cost of hospital care, physician and dental services, home health care, nursing home services, prescription drugs, medical equipment and supplies, and public health direct services (CMS, 2010b). This translates to more than $8,000 per person and accounted for 17.6 percent of the national gross domestic product (CMS, 2010b). Growth in national health expenditures is expected to increase by 6.1 percent between 2009 and 2019 (CMS, 2010c). In contrast, expenditures for dental services in the United States in 2009 were $102.2 billion, approximately 5 percent of total spending on health care (CMS, 2010b). While medical and dental spending both have been rising, the growth in medical expenditures has far outpaced the growth in dental expenditures.
The reported national expenditure levels undercount the total spent on improving oral health. Estimates represent only the costs associated with direct services delivered by dentists in traditional practice settings. Spending on public health initiatives (e.g., water fluoridation and public education campaigns) and oral health services delivered in medical care settings are not included in estimates of overall expenditures. For example, there are approximately 3.6 million craniofacial cases (e.g., diabetes-related conditions, oral cancers, and injuries) treated in medical care settings each year, and the total costs for these treatments exceed several billion dollars (Snowden et al., 2003).
Average Annual Dental Expenses
In 2007, the average annual expense for individuals who had any dental expenses was $643 (Rohde, 2010). Individual expenses varied by age, income, race and ethnicity, and insurance status (see Figure 5-1). Annual dental expenses also varied by source of insurance. The average annual dental expense for individuals with private dental insurance was $662. Among individuals with public dental insurance (e.g., Medicaid or CHIP), the average annual dental expense was $370 (AHRQ, 2009). Individuals with higher incomes had higher annual dental expenses. The average annual dental expense for “high-income” individuals (<400 percent of the federal poverty level [FPL]) was $710. Among “poor” individuals (≤100 percent FPL), the average annual dental expense was $428 (AHRQ, 2009). This difference in expenses may reflect the ability of individuals with higher
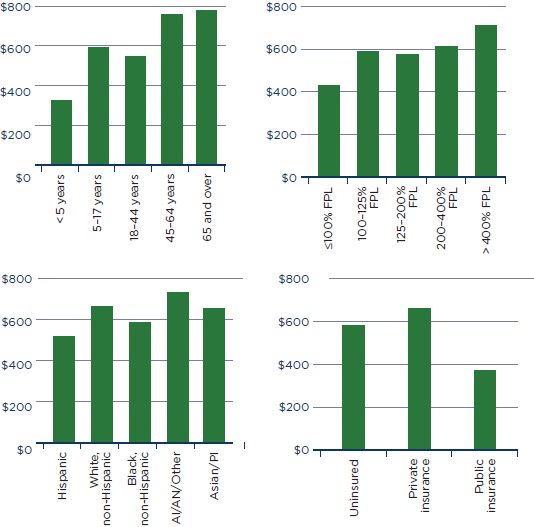
FIGURE 5-1
Mean annual dental expenses by age, income, race/ethnicity, and insurance status, United States, 2007.
NOTE: AI/AN = American Indians/Alaska Natives;
FPL = federal poverty level; PI = Pacific Islander.
SOURCE: AHRQ, 2009.
incomes to pay for and use dental care. Finally, older adults (individuals 65 and over) had the highest average annual dental expenses at $776. By contrast, children and adolescents (individuals under age 18) had the lowest average annual dental expenses (AHRQ, 2009).
In 2007, the source of payments for dental care (e.g., private insurance, out-of-pocket, or public insurance) varied among individuals who had any
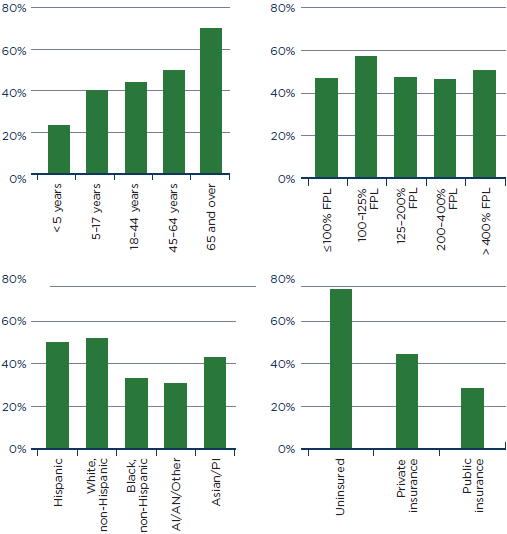
FIGURE 5-2
Percent of total annual dental expenses paid out of pocket by age, income, race/ethnicity, and insurance status, United States, 2007.
NOTE: AI/AN = American Indians/Alaska Natives;
FPL = federal poverty level; PI = Pacific Islander.
SOURCE: AHRQ, 2009.
dental expenses. For example, the percentage of annual dental expenses paid out of pocket varied by age, race and ethnicity, income, and insurance status (see Figure 5-2). As would be expected, uninsured individuals pay the highest percentage—nearly three quarters—of their annual dental expenses out of pocket (74.7 percent) compared to individuals with private insurance and those with public insurance (44.3 percent and 28.5 percent,
respectively) (AHRQ, 2009). Older adults (individuals 65 and over) had the highest percent of total annual dental expenses paid out of pocket than any other age group (70.3 percent). By contrast, children, who are more likely to have public insurance that includes dental coverage, had the lowest percent of total annual dental expenses paid out of pocket than any other age group (23 percent). Working age adults (individuals between 18 and 64 years of age), who are more likely to have employer-based dental coverage, had lower costs than older adults (AHRQ, 2009). The lack of dental coverage in Medicare and the lack of employee-based dental coverage translate into higher out-of-pocket dental expenses for older adults (Manski et al., 2010a).
Dental Coverage
There is strong evidence that dental coverage is positively tied to access to and utilization of oral health care (AHRQ, 2010; Decker, 2011; Sohn et al., 2007), although whether or not this relationship is causal is not clear. For example, it may be that those with greater demand for dental care are the ones most likely to purchase dental coverage. This suggests it is not clear if more coverage leads to greater use or greater demand leads to the purchase of dental coverage (and then greater use). The tie is clear, though: In 2007, 52 percent of adults with private dental coverage had at least one dental visit, compared to 31 percent of those without private dental coverage and 22 percent of uninsured individuals (Manski and Brown, 2010). Moreover, children who have dental coverage, through public programs (e.g., Medicaid or CHIP) or private insurance, use preventive care more routinely than their counterparts who lack coverage (Lewis et al., 2007). Studies using quasi-experimental designs to assess the impact of dental coverage on access and utilization indicate that, once children acquire coverage through a public program, they are significantly less likely to have unmet needs for dental care. For example, after enrolling in CHIP, unmet needs for oral health care decline among adolescents (Klein et al., 2007). Another study found that, after enrolling in CHIP, children with special health care needs had significantly improved access to a broad range of health care services, including dental care (Kenney, 2009). Overall, uninsured children are at least twice as likely as children with dental coverage to have unmet need for oral health care (Damiano et al., 2003; Feinberg et al., 2002; Fox et al., 2003; Kenney, 2007; Lave et al., 2002; McBroome et al., 2005; Mofidi et al., 2002; Szilagyi et al., 2004; Trenholm et al., 2005; Wang et al., 2007).
Millions of Americans lack dental coverage. Recent data from several sources underscore this deficiency among children, adults, and older adults:
• An estimated 130 million U.S. adults and children lack dental coverage (based on enrollment in private dental plans) (NADP, 2009).
• Over 40 percent adults ages 21-64 lack private dental coverage (see Figure 5-3) (Manski and Brown, 2010).
• Approximately 70 percent of adults age 65 and older, lack any kind of dental coverage—public or private (Manski and Brown, 2007).
• Over 22 percent of children ages 1-17 lack dental coverage (Liu et al., 2007).
What Do Dental Plans Cover?
The types of dental services covered by dental plans vary widely among private plans and between various public plans. Currently, there is no standard set of essential oral health benefits. For example, one plan may include “comprehensive” care such as routine diagnostic and preventive services, X-rays, restorative services, and oral surgery, while another may cover more limited services such as emergency care only. A recent survey of employersponsored health plans of the benefits typically covered by employers based on data from the National Compensation Survey provides an overview of employment-based dental benefits (see Box 5-1). Some of the variation in services covered is driven by employer and consumer choice. Dental benefits available to employees may be based upon their employers’ selection of low-cost dental benefit packages or benefits packages that appeal to
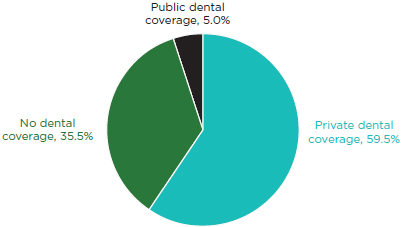
FIGURE 5-3
Percentage of adults 21-64 according to dental coverage status: U.S. civilian noninstitutionalized population, 2007.
SOURCE: Manski and Brown, 2010.
BOX 5-1
Summary of Employment-Based Dental Benefits
A recent report from the Department of Labor on selected medical benefits provided the following summary of employment-based dental benefits based on data from the National Compensation Survey (NCS):
Plans typically grouped dental services into categories, such as preventive services (typically exams and cleanings), basic services (typically fillings, dental surgery, periodontal care, and endodontic care), major services (typically crowns and prosthetics), and orthodontia. Cost sharing for dental services typically involved an annual deductible—the median was $50 per person. After meeting the deductible, dental plans often paid a percent of covered services up to a maximum annual benefit. The median percent paid by the plan was 100 percent for preventive services, 80 percent for basic services, and 50 percent for major services and orthodontia. The median annual maximum was $1,500; a separate maximum applicable to orthodontic services also had a median value of $1,500.
SOURCE: BLS, 2011.
their higher paid workers. Alternatively, consumers may purchase or select employer-based coverage (when available) that provides a range of desired benefits and/or choice of providers. The dental benefits included in public plans are determined by federal law and/or state decisions. (A discussion of what is covered in public plans is included later in the chapter.) Each of the factors described above contribute to the tremendous variation in dental coverage.
How Is Dental Coverage Unique?
The usual premise for buying insurance is to cover unpredictable and rare events. This is the impetus behind purchasing health care, home, and car insurance. But this logic does not neatly fit most dental care. In general, dental care does not meet the criteria for casualty insurance that “the event or expense insured against (1) is relatively rare for the individual person but occurs at known rates for groups, (2) is very costly, and (3) cannot generally be controlled by the insured” (IOM, 1980). In fact, most people need or use oral health care at least annually.
Dental coverage is similar to health coverage in one notable way: the availability of a significant tax subsidy has led employers to offer dental coverage. Thus, most private dental coverage is employer provided, subsi-
dized through the tax system. However, dental coverage typically requires higher percentage co-payments than health insurance.
The IOM report Public Policy Options for Better Dental Health (Public Policy Options) concluded that, despite the unique attributes of dental coverage, it is in the nation’s best interest to cover dental services; the reasons provided by the committee over 30 years ago remain largely the same today:
• Use of oral health care is highly correlated with income, education, and occupational status.
• Effective preventive measures exist.
• The overall structure of dental benefit coverage does not adequately promote preventive services, often resulting in delayed treatment.
Finally, the Public Policy Options committee concluded that “welldesigned public and private dental health insurance would be useful for achieving important objectives in dental health and that this advantage outweighs the inapplicability of some of the traditional insurance principles to dental care benefits.” Specifically, the committee determined that dental coverage could, among other things, improve access to dental care delivery systems (IOM, 1980).
Variation in Coverage Rates by Race/Ethnicity
Dental coverage varies significantly by race and ethnicity (Flores and Tomany-Korman, 2008; Manski and Brown, 2007, 2008, 2010; Zuckerman et al., 2004). For example, data from the 2004 Household Component of the Medical Expenditure Panel Survey showed that among individuals of all ages, white non-Hispanics were more likely to have private dental coverage than black non-Hispanic and Hispanic individuals (who were more likely to have public dental coverage) (Manski and Brown, 2007). Data from the 2006 Health and Retirement Study showed that among older adults, nonHispanic blacks were more likely to have dental coverage (56.8 percent) than non-Hispanic whites (46.7 percent) and Hispanics (42.4 percent) (Manski et al., 2010b).
Dental care is financed primarily through private sources, including individual out-of-pocket payments and private coverage (see Table 5-1). For more than 50 years, these two sources have financed over 90 percent of all dental expenditures (CMS, 2010b). Americans spend billions of dollars out of pocket for dental services each year. In 2008, dental services accounted
TABLE 5-1
National Dental Expenditures, by Source of Funds, 2003-2009 (in $ billions)
| Year | Total | Private Out-of-Pocket |
Private Health Insurance |
Public Medicare |
Medicaid | Other Health Insurance Programs |
| 2003 | 76.0 | 33.7 | 37.4 | 0.1 | 3.7 | 0.8 |
| 2004 | 81.8 | 36.0 | 40.5 | 0.1 | 4.0 | 0.9 |
| 2005 | 86.8 | 38.3 | 42.9 | 0.1 | 4.2 | 1.0 |
| 2006 | 91.4 | 40.3 | 45.1 | 0.1 | 4.4 | 1.1 |
| 2007 | 97.3 | 42.7 | 47.8 | 0.2 | 4.8 | 1.5 |
| 2008 | 102.3 | 44.9 | 49.1 | 0.2 | 5.8 | 1.7 |
| 2009 | 102.2 | 42.5 | 50.0 | 0.3 | 7.1 | 1.9 |
SOURCE: CMS, 2010b.
for 22 percent of all out-of-pocket health care expenditures, ranking second only to prescription drug expenditures (BLS, 2010a).
Variation in Coverage Rates by Employment and Income
Variations in dental coverage have been observed by employment status and income level. For example, data from the 2008 National Health Interview Survey showed that the percentage of individuals with private dental coverage increased as income levels increased (Bloom and Cohen, 2010). Similarly, higher-paid workers are also more likely to have access to and participate in stand-alone dental plans (Barsky, 2004; Ford, 2009). The availability of dental coverage through one’s employer is associated with the size of the establishment; that is, the larger the number of employees overall, the greater the likelihood that stand-alone dental plans will be available to employees (Barsky, 2004; Ford, 2009). Employers can add a separate oral health product to their overall coverage package, but often they do not. In 2006, 56 percent of all employers offered health insurance but only 35 percent offered dental coverage (Manski and Cooper, 2010). Employees are more likely to be offered options for medical insurance than dental coverage, and a higher percentage of employees will take advantage of available dental benefits as compared with the percentage of employees who take advantage of available medical benefits (80 percent vs. 75 percent) (BLS, 2010b). As noted earlier, with the exception of coverage of
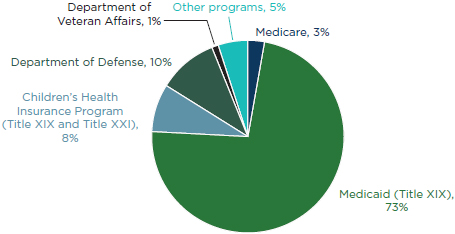
FIGURE 5-4
Public expenditures for dental services by program, 2009.
SOURCE: CMS, 2010b.
rare events, dental coverage differs from the typical insurance model; thus, employer-based dental coverage might be viewed as a fringe benefit that subsidizes oral health care utilization.
Access to dental care depends on a variety of factors; however, chief among these is having a provider available and having the ability to pay for services (either through insurance, direct out-of-pocket payments, or subsidies) (Borchgrevink et al., 2008; Fisher and Mascarenhas, 2007; GAO, 2000; Hughes et al., 2005). In 2009, public subsidies or direct payments for dental services from public programs totaled $7.4 billion or less than 1 percent of national expenditures for dental services (CMS, 2010b). The overwhelming majority (73 percent) of these public expenditures for direct services or coverage came from Medicaid (CMS, 2010b) (Figure 5-4).
Medicaid and CHIP
Medicaid
Medicaid is a federal-state entitlement program for medical assistance to low-income children and pregnant women, persons over age 65, and those with disabilities who meet income and resource requirements; at the state’s discretion, certain persons who are considered medically needy
based on their high medical costs may also be covered. The vast majority of state Medicaid programs now purchase at least some medical care services through contracts with managed care plans (CMS, 2009).
Medicaid’s Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) service provides a comprehensive child health benefit, which requires states to fund well-child health care, diagnostic services, and medically necessary treatment services to Medicaid-eligible children ages birth to age 21 (CMS, 2005a). Under federal EPSDT law, states must cover any Medicaid-covered (i.e., allowed under the federal Medicaid statute) service that is necessary to prevent, correct, or ameliorate a child’s physical health, which includes oral health (CMS, 2005b). Dental coverage is required for all Medicaid enrolled children under age 21 (CMS, 2011b). This is a comprehensive benefit, including preventive, diagnostic, and treatment services. At a minimum, these services must include relief of pain and infections, restoration of teeth, and maintenance of dental health. In contrast, states are not required to provide coverage for adults. For adults, states must only cover medical and surgical services furnished by a dentist to the extent those services can be performed under state law by either a doctor of medicine or a dentist. Beyond this, states’ coverage of routine dental benefits for adults varies widely among the states, with a number of states limiting the benefit to emergency coverage (see Figure 5-5).
Medicaid coverage can improve access to medical and dental care; however, health status, age, race and ethnicity, gender, routine source of dental care, amount of reimbursement, and availability of providers all factor into the impact of coverage (Dasanayake et al., 2007; Edelstein and Chinn, 2009; Jablonski et al., 2005; Johnson et al., 2005; Kenney, 2009; Pourat and Finocchio, 2010; Rowley et al., 2006; Shiboski et al., 2005; Snyder, 2009). There are variations in the patterns of utilization for preventive, treatment, emergency, and specialty dental services associated with Medicaid populations compared to privately insured populations (Sweet et al., 2005).
At the same time, low provider participation in the Medicaid program has a direct and generally negative impact on access to oral health care for Medicaid beneficiaries (GAO, 2009, 2010; Lewis et al., 2009; Milgrom et al., 2010; Ramírez et al., 2011; Shortridge and Moore, 2009). For example, 74 percent of pediatricians cite the lack of dentists who accept Medicaid as a “moderate to severe barrier for 0-3-year-old Medicaid-insured patients to obtain dental care” (Lewis et al., 2009). In addition, a recent study in Illinois found that a child with public dental coverage (Medicaid/CHIP) was significantly less likely to obtain an appointment for an urgent oral injury than a child with the same injury with private dental coverage (Bisgaier et al., 2011). This effect was found even among Medicaid/CHIP-enrolled practices. Increases in Medicaid reimbursement, discussed later in this
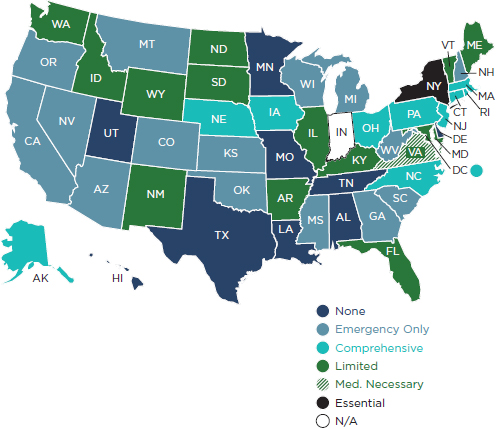
FIGURE 5-5
Medicaid adult dental benefits by state, 2009.
SOURCE: ASTDD, 2010.
chapter, have been shown by some studies to increase dentist participation (Griffin et al., 2007; Helgeson, 2005). Other approaches (e.g., training, administrative support, and quality improvement techniques) also have been shown to increase dentists’ participation in Medicaid, particularly for children’s services (Hughes et al., 2005). Multidimensional, strategically planned initiatives that include provider outreach, increased financing, and consumer education show particular promise (Greene-Mclntyre et al., 2003; Kobayashi et al., 2005; Shirk, 2010; Taichman et al., 2009). As described in Chapter 3, state Medicaid programs are increasingly electing to reimburse primary medical care providers and dental hygienists for preventive oral health services, including the application of fluoride varnish, performing oral examinations, and providing anticipatory guidance (AAP, 2010; ADHA, 2010).
Children’s Health Insurance Program (CHIP)
CHIP is a federal-state grant program that provides resources to states to expand health coverage to uninsured, low-income children up to age 19 and pregnant women. Unlike Medicaid, it is not an entitlement, but it does help states provide publicly subsidized health coverage to uninsured children in households earning up to 200 percent FPL (and with federal approval, well above that level). Following its enactment in 1997, millions of children received coverage for medical care and a portion of those were covered for dental care under CHIP (Rosenbach et al., 2003; VanLandeghem et al., 2003). CHIP plans either offer eligibility for children under Medicaid or create a separate children’s health insurance approach managed by the state (and typically operated by private insurance companies). Non-Medicaid approaches must be equivalent to one of the so-called benchmark benefits packages (e.g., Federal Employees Health Benefits Program [FEHBP], Blue Cross/Blue Shield, or the state employee benefit plan). If CHIP is part of Medicaid, then benefits must be comparable, including EPSDT dental benefits.
The Children’s Health Insurance Program Reauthorization Act (CHIPRA) enacted in February 2009 requires all states to provide dental coverage under CHIP, including “coverage of dental services necessary to prevent disease and promote oral health, restore oral structures to health and function, and treat emergency conditions.”1 States can meet this requirement in separate CHIP programs by providing dental coverage equivalent to one of three benchmark dental benefit packages: (1) the plan under FEHBP selected most frequently by employees seeking dependent coverage; (2) the state employee benefit plan selected most frequently by employees seeking dependent coverage; or (3) the commercial dental plan in the state that has the largest non-Medicaid enrollment of dependents (Paradise, 2008). In addition, states were given the option to offer a stand-alone or dental-only supplemental coverage to families whose children meet income eligibility requirements for CHIP and have private, employer-sponsored medical insurance but lack dental coverage.
CHIPRA also included provisions related to the dissemination of dental education materials, data reporting on dental access and quality, and requirements to post lists of participating dental professionals. For example, HHS’s Insure Kids Now website was designed to provide families with more timely and accessible information about the participating providers in their communities and whether these providers are accepting new patients. However, a recent study by the Government Accountability Office
______________
1Children’s Health Insurance Program Reauthorization Act of 2009, Public Law 3, 111th Cong., 1st sess. (February 4, 2009).
(GAO) highlighted the significant deficiencies in the website’s lists of dental professionals participating in Medicaid or CHIP including incomplete and inaccurate information (e.g., disconnected phone numbers, providers not accepting new patients, and providers no longer in practice) (GAO, 2010). In response to this report, HHS is taking steps to improve the Insure Kids Now website.
Factors That Influence Provider Participation in Medicaid and CHIP
According to the 2000 GAO report Factors Contributing to Low Use of Dental Services by Low-Income Populations, the primary reason individuals enrolled in Medicaid are unable to locate and use needed services is limited dentist participation in Medicaid (GAO, 2000). A recent report identified three main reasons given by dentists for not seeing more Medicaid patients: low reimbursement rates, administrative requirements, and patient-related issues (e.g., missed appointments) (Borchgrevink et al., 2008). The following sections provide a brief overview of how reimbursement rates and program-related administrative requirements influence provider participation in Medicaid. Patient-related issues are addressed in Chapter 4.
Low reimbursement rates Medicaid reimbursement rates are generally lower than dentists’ usual and customary fees (GAO, 2000; Shirk, 2010). This is often cited as a disincentive to providers’ willingness to participate in these publicly funded programs (Damiano et al., 1990; GAO, 2000; Lang and Weintraub, 1986; McKnight-Hanes et al., 1992; Venezie et al., 1997). For example, a recent state-by-state comparison of average retail fees and Medicaid reimbursement rates for oral evaluation revealed that, overall, Medicaid reimbursement rates were about 55 percent of the average retail fees ($18.00 vs. $33.00) (Shirk, 2010) (see Figure 5-6). While this comparison illustrates substantial variations by state, it should be noted that health care providers negotiate with insurers to determine discounts to retail fees. Since individuals without insurance have no one to negotiate such discounts on their behalf, they typically pay the full retail fee for services. Therefore, the only individuals who would be billed at the commercial rate would be the estimated 130 million U.S. adults and children who lack dental coverage. Furthermore, final negotiated rates depend on individual agreements; the larger the size of the insurer, the deeper discounts they may be able to negotiate. The impact of Medicaid reimbursement rates has also been observed in other health professions. For example, one study found a strong and significant correlation between low Medicaid reimbursement rates and low participation in Medicaid by pediatricians (Berman et al., 2002).
Before the recent economic downturn, a number of states had increased reimbursement rates for dentists in an effort to encourage broader partici
pation of dentists in publicly funded programs and increase access to care. However, as states began to look for ways to address budgets shortfalls, many made cuts to dental reimbursement rates. In FY 2010, 13 states made cuts to dental rates, and seven more states adopted cuts to dental rates in FY 2011 (Smith et al., 2010).
Increases in reimbursement rates have shown promise in increasing dentists’ participation in publicly funded programs (Borchgrevink et al., 2008; Eklund et al., 2003; Hughes et al., 2005; Mayer et al., 2000). A recent study found that both dentist participation in Medicaid and the number of Medicaid patients treated increased in states that implemented reimbursement rate increases (Borchgrevink et al., 2008). Moreover, the study found that dentists who were already enrolled in Medicaid began treating more Medicaid patients following the rate increases. Finally, in one state, both the number of providers and the geographic distribution of providers expanded following the increase in reimbursement rates. As a result, the average distance that children had to travel for care in the participating counties served decreased from 24.5 miles to 12.1 miles (Borchgrevink et al., 2008). (See the Innovations in Financing section later in this chapter for examples of enhanced Medicaid payment strategies.)
Efforts to improve access through financing strategies will necessarily be multifaceted and will be one component of broader efforts to improve access. For example, studies have demonstrated that increasing reimbursement rates alone is not sufficient in improving access to care. Without more comprehensive actions (including case management and streamlined enrollment and billing processes), barriers to oral health care persist (Borchgrevink et al., 2008).
Administrative requirements The administrative processes and requirements associated with Medicaid are frequently cited as a barrier to provider participation (ADA, 2004; GAO, 2000). In particular, dentists point to excessive paperwork, complex billing and preauthorization requirements, difficult eligibility-verification processes, slow payments, denials of submitted claims, and complicated provider enrollment as procedural obstacles to providing care to Medicaid patients (ADA, 2004; GAO, 2000; Greenberg et al., 2008). This corresponds with research in other health professions. For example, a nationally representative survey of U.S. physicians in direct patient care found that after inadequate reimbursement (84 percent of respondents), billing requirements and paperwork (70.4 percent of respondents) and delayed reimbursement (64.8 percent of respondents) were the most frequently reasons provided for limiting the number of Medicaid patients they see (Cunningham and May, 2006). Many states have taken measures to reduce administrative burdens as a strategy to improve provider participation in public programs. (See the Innovations in Financing section later in
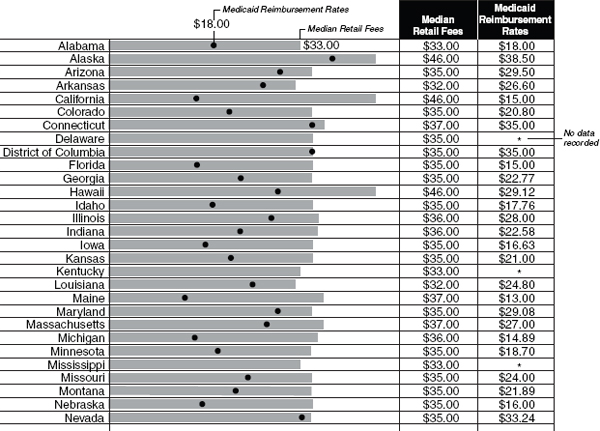
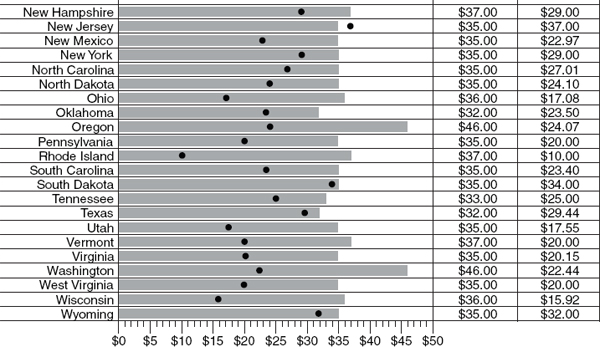
FIGURE 5-6
Median retail fees and Medicaid reimbursement rates for children’s periodic oral evaluation, by state.
SOURCE: Used with permission by the National Health Policy Forum, from “Oral Health Checkup: Progress in Tough Fiscal Times?” Figure 5-2 (Issue Brief No. 836, March 29, 2010).
this chapter for examples of how states are reducing administrative burdens associated with Medicaid.) These actions, in conjunction with rate increases and other supportive strategies (e.g., increased education and outreach to beneficiaries), can have a significant effect on increasing provider participation and patient utilization rates (Borchgrevink et al., 2008; GAO, 2009; Greenberg et al., 2008; Wysen et al., 2004).
Medicare
Medicare coverage is available to most Americans 65 and over,2 regardless of income, and persons with disabilities. Medicare has several parts. Part A covers hospital and other institutional care for all who receive Social Security benefits, without a premium. Part B covers physician and certain other clinical services for those who elect to enroll and pay a premium. Most Medicare beneficiaries have both Part A and Part B coverage. In addition, Medicare Part D provides coverage for prescription drugs through private plans for those who wish to enroll.
The Medicare statute explicitly excludes coverage for what is generally known as dental care, specifically, “for services in connection with the care, treatment, filling, removal, or replacement of teeth or structures directly supporting the teeth.”3 Coverage is not determined by the value or the necessity of the dental care but by the type of service provided and the anatomical structure on which the procedure is performed. Medicare will not cover most dental care. For example, Medicare will not cover routine checkups, cleanings, fillings, or dentures.
The Centers for Medicare and Medicaid Services (CMS) has approved dental coverage in special situations that relate directly to medical needs. Currently, Medicare will pay for dental services that are an integral part either of a covered procedure (e.g., reconstruction of the jaw following accidental injury or removal of a facial tumor). Medicare also pays for extractions done in preparation for radiation treatment for diseases involving the jaw, which may be appropriate for patients with extensive periodontal disease and dental abscesses, but not for others who can be treated with less drastic interventions. Medicare will also reimburse for oral examinations, but not treatment, preceding kidney transplantation or heart valve replacement, under certain circumstances (i.e., such examination would be covered under Part A if performed by a dentist on the hospital’s staff or under Part B if performed by a physician) (CMS, 2010a; IOM, 2000; Patton et al., 2001).
______________
2 Individuals who have not worked at all or have not worked enough to be eligible for Social Security are not eligible for Medicare.
3 Section 1862(a)(12) of the U.S. Social Security Act.
As increasing numbers of baby boomers (individuals born between 1946 and 1964) become eligible for Medicare, considerable attention is being paid to how these aging adults will pay for and obtain oral health care (Ferguson et al., 2010; Manski et al., 2010a; Moeller et al., 2010). The relative size of this cohort—approximately 78 million in 2009—coupled with increases in longevity will create an unprecedented demand for oral health care for older adults.
Increasing access to oral health care is important, but improving oral health will require efforts that reach well beyond the dentist’s office. Public health and community projects across the country are evidence of the important role of state and local health departments in promoting oral health, linking people to needed services, and developing population-based prevention programs. Such oral public health programs include efforts to reduce smoking, expand access to fluoridated water, and to educate the public about personal oral hygiene and prevention (ASTDD, 2011). Monitoring and surveillance are also key roles for oral public health. Table 5-2 provides an overview of additional public investments in oral health.
Maternal and Child Health Block Grant Program
Title V of the Social Security Act is a permanently authorized discretionary grant program that is viewed as a part of the oral health safety net for uninsured and underinsured women and children, including pregnant women and children with special health care needs.4 Title V authorized the creation of the Maternal and Child Health (MCH) programs to promote and improve the health of all mothers and children. Title V operates as a federal-state partnership that requires a 75 percent match, that is, every $4 of federal money must be matched by $3 of state or local funds (HHS, 2008). Because oral health is an MCH priority area, Title V plays an important role in financing oral health care for vulnerable and underserved populations (see Box 5-2 for MCH Oral Health Goals). For example, in 2009, 32 states—or 63 percent—reported “oral health” as a priority need for preventive and primary care for pregnant women, mothers, infants, children, and children with special health care needs (HRSA, 2010). In addition, a recent survey of states found that Title V was the second most common source of funding for school-based health centers (SBHCs) for the 2004-2005 school year ($7.2 million) (Schlitt et al., 2008). As described
______________
4 United States Code, §701-710, subchapter V, chapter 7, Title 42.
TABLE 5-2
Federal and State Funding Sources for Oral Health Services, Infrastructure, and Research
| Source | Appropriations, Grants, and Programs | |
| Congress | Periodic federal legislation includes funding for oral health programs | |
| State/local government | State-sponsored Dental Loan Repayment Programs; Community Support Grants; Funding for State Oral Health Sections, Bureaus, and Programs |
|
| Centers for Disease Control and Prevention (CDC) |
State-based Oral Disease Prevention Programs Preventive Health and Health Services (PHHS) Block Grants Prevention Research Centers Program (PRCs) |
|
| National Center for Health Statistics (NCHS) |
National Health Interview Survey (NHIS) and National Health and Nutrition Examination Survey (NHANES) include data on oral health status and access to services |
|
| Health Resources and Services Administration (HRSA) | ||
| Maternal and Child Health Bureau (MCHB) | Maternal and Child Health Services Block Grants (Title V) | |
| Bureau of Health Professions (BrHP) | National Health Service Corps (NHSC) Loan Repayment Program; Residency Training in General, Pediatric, and Public Health Dentistry; Dental Public Health Residency Training; and State Oral Health Workforce Grants |
|
| HIV/AIDS Bureau | Ryan White Comprehensive AIDS Resources Emergency (CARE) Act Funds; Community-Based Dental Partnership Program |
|
| Bureau of Primary Health Care (BPHC) | New Access Points Grants; Expanded Medical Capacity Grants; Service Expansion Grants | |
| Office of Rural Health Policy (ORHP) | Rural Health Care Services Outreach Grants | |
| Indian Health Service (IHS) | The Early Childhood Caries Initiative; Oral Health Promotion/Disease Prevention Awards | |
| Centers for Medicare and Medicaid Services (CMS) |
Medicaid reimbursement for: case management; services for children with special health care needs; school-based oral health services; selected administrative activities related to outreach, enrollment, and coordination of services; and referrals |
|
| U.S. Department of Agriculture (USDA) | Women, Infants, Children (WIC) Early Intervention for Oral Health Programs | |
| Administration for Children and Families (ACF) | Head Start Oral Health Initiative | |
SOURCES: CDC, 2011a,b,c; Center for Oral Health, 2010; CMS, 2011a; HHS/ACF/OHS, 2011; HRSA, 2011d.
BOX 5-2
Maternal and Child Health Oral Health Goals
• Improve the health infrastructure and systems of care for all, especially underserved, vulnerable, and special needs population to ensure access to comprehensive, high-quality oral health services.
• Improve oral health status and outcomes (and their measurements) in seeking to eliminate health disparities.
• Improve the quality of oral health services (preventive and curative) for all, especially underserved, vulnerable, and special needs populations.
• Promote oral health through building public-private partnerships, including strengthening the dental public health infrastructure.
SOURCE: HHS, 2008.
in Chapter 4, SBHCs offer significant potential to increase access to oral health care among children.
The two major funding categories within the Title V MCH Block Grant program—formula grants and discretionary grants—and examples of oral health activities within both categories are described below.
Title V Block/Formula Grants
Title V Block/Formula Grants can be used to support direct health care services, enabling services (e.g., case management, transportation, outreach, and education), population-based services (e.g., surveillance), and infrastructure-building services (e.g., training and standards development). These broadly defined service areas and the design of the block grants inherently provide states with flexibility in how funds are used. For example, states that deem oral health as a priority have an existing source of annual funding from which to build. On the other hand, MCH block grants are a limited source of federal funds, and states may prioritize other critical maternal and child health issues over oral health. In 2010, Title V appropriations to states were $662 million, 85 percent—or $563 million—of which were set aside for formula block grants (HRSA, 2011a). However, the FY 2012 HRSA budget proposes over $6 million in overall cuts to the MCH block grants (HRSA, 2011d). HRSA maintains the Title V Information System website with “snapshots” of activities in the 59 states and jurisdictions that receive block grant funds from MCH (HRSA, 2011c). This website includes detailed annual reports from each state on programs
and expenditures. However, oral health is not a line item on the budget and expenditure data forms and only some states include specific expenditures on oral health in their budget narratives. This makes estimating the exact amount spent on oral health care through MCH block grants difficult to determine. Data from the 2009 National Health Expenditure Accounts estimated that MCH spent 30 million dollars (11 million federal and 19 million state/local) on dental services (CMS, 2010b).
Title V Discretionary Grants
In addition to block grants, MCH supports oral health activities through Special Projects of Regional and National Significance (SPRANS) grants and Community Integrated Service Systems discretionary grants. These discretionary funds have been used to support a broad range of programs including school-based dental sealant programs, pediatric oral health leadership and leadership training programs, and infrastructure development within states and communities. The grants are intended to provide flexibility to states, communities, and institutions and promote innovation in addressing issues of timely importance that may not easily be accomplished through the formula block grants or through other federal/state programs. In 2010, the HRSA appropriation language included $4.9 million in SPRANS set aside as funds for oral health (HRSA, 2011a). However, the FY 2012 HRSA budget eliminated the SPRANS set-aside grants for oral health (HRSA, 2011d). HRSA maintains the Maternal and Child Health Bureau’s Discretionary Grant Information System with program and performance measure data for these annual grants (HRSA, 2011b). For example, Iowa used Title V funding to develop a dental voucher program to increase access to oral health care for low-income, uninsured, and underinsured children. The program, which provides oral health screenings, examinations, and sealants to children in school-based settings, uses dental hygienists working under public health supervision. In 2005, the Iowa dental voucher program provided more than 25,000 services (e.g., screenings and fluoride varnish applications) and over 10,000 sealants (Association of Maternal and Child Health Programs, 2011).
THE PATIENT PROTECTION AND AFFORDABLE CARE ACT
The Patient Protection and Affordable Care Act (ACA) included numerous provisions to expand dental coverage, increase the number of oral health care professionals, and invest in oral health prevention and public health activities. Box 5-3 highlights key provisions of the ACA specifically related to dental coverage and the financing of oral health care. It also highlights selected provisions for oral public health initiatives, infrastruc-
BOX 5-3
Key Financing and Coverage Provisions for Oral Health Care in ACA
Dental coverage for children—Requires that all Qualified Health Plans offered under the Health Insurance Exchange provide coverage for an essential health benefits package, including oral care for children.
Stand-Alone Dental Plans—Allows stand-alone dental plans (i.e., those not offering medical and dental coverage) to participate in the Health Insurance Exchange.
Dental Coverage in Medicare Advantage—Requires Medicare Advantage Plans to use rebates to pay for dental coverage and other services.
MACPAC and Payments to Dental Professionals—Requires the Medicaid and CHIP Payment and Access Commission (MACPAC) to review and report to Congress on the process for updating payments to dental professionals, payment methodologies, and how the processes and methodologies relate to access and quality of care for Medicaid and CHIP beneficiaries.
Key Public Health, Infrastructure, and Research Provisions for Oral Health Care in ACA
Funding for Workforce Training—Establishes a separate appropriations line item for training of general, pediatric, and public health dentists and appropriates $30 million for FY 2010 to train the oral health workforce. Expands Title VII to create a “dental cluster” with a provision to support development of dental workforce training programs.
ture, and research grants that are likely to have an impact on access to oral health services for vulnerable and underserved populations. While these provisions may help expand access to care for vulnerable and underserved populations, it is unknown whether they will be fully funded.
INNOVATIONS IN FINANCING AND COVERAGE
The following sections provide descriptions of an array of financing and coverage innovations being used to improve access to oral health care. These examples include enhanced Medicaid payments, streamlined
Dental Faculty Loan Repayment Program—Establishes a dental faculty loan repayment program for faculty engaged in primary care dentistry, including general dentistry, pediatric dentistry, and public health dentistry.
Grants for Alternative Dental Health Care Providers Demonstration Projects—Authorizes grants to establish demonstration programs to “train or employ” alternative dental health care providers.
Funding for Oral Health Public Education Campaign—Requires a 5-year, evidence-based public education campaign to promote oral health, including a focus on early childhood caries, prevention, oral health of pregnant women, and oral health of at-risk populations.
Dental Caries Disease Management Grants—Establishes a grant program to demonstrate the effectiveness of research-based dental caries disease management.
Grants for School-based Dental Sealant Programs—Requires that all states, territories, and Indian tribes receive grants for school-based dental sealant programs.
Cooperative Agreements to Improve Oral Health Infrastructure—Requires the CDC to enter into cooperative agreements with states, territories, and Indian tribes to improve public health infrastructure related to oral health.
SOURCE: Children’s Dental Health Project, 2010.
administrative processes, supportive activities, and integrating medical and oral health coverage. In some cases, these innovations are too new to have robust outcomes data for impact on access to care or oral health status, especially in the long term, and therefore the committee does not intend to imply it is recommending these approaches. In addition, these examples are not exhaustive of all of the strategies being used across the nation. Instead, they serve to illustrate the range of ideas and opportunities for improving how oral health care is financed and covered in order to improve access to care for vulnerable and underserved populations.
Enhanced Medicaid Payments
North Carolina Medicaid Waiver
North Carolina has developed a unique arrangement with the CMS to provide enhanced Medicaid payments to state-supported patient care facilities. These supplemental Medicaid payments have resulted in the development of a large network of 120 fixed and 16 mobile county-run dental clinics and an innovative clinical education model at a new School of Dental Medicine (SODM) at East Carolina University. As discussed in Chapter 3, this new clinical educational program is expected to significantly reduce dental access disparities in some of the poorest areas of the state.
In 1997 North Carolina obtained a CMS Medicaid waiver that allows enhanced payments to state-supported facilities that provide care to Medicaid patients. As a result:
1. Clinics bill fee-for-service for covered benefits provided to Medicaidenrolled patients. On an annual basis, clinics determine the actual cost of providing services to Medicaid patients and submit the difference between actual costs and payments to the state Medicaid program.
2. The state pays the university 64 percent of the difference between actual and reimbursed costs. The money comes from CMS and reflects the fact that CMS pays 64 percent of Medicaid program costs in North Carolina.
As an example, assume the allowable cost for dental services is $2.0
million, and total reimbursement to the SODM under fee-for-service reimbursement is $1.75 million. Thus, the unreimbursed allowable amount is $250,000. Medicaid reimburses the unreimbursed costs to the extent of the federal Medicaid participation rate which is currently 64 percent. Accordingly, the school receives an additional settlement of $160,000. There is usually a 12-month period between submitting and receiving the additional funds (Bailit et al., 2010).
Minnesota Critical Access Dental Payment Program (CADPP)
In 2001, the Minnesota legislature established the Critical Access Dental Payment Program (CADPP) to offer increased reimbursement (through add-on payments) to providers that care for patients enrolled in the Minnesota Health Care Program (MHCP). MHCP provides health care coverage through three publicly funded health care programs: the Medical Assistance (MA) program, the General Assistance Medical Care (GAMC) program,
TABLE 5-3
Minnesota Fee-for-Service Payment to Charge Ratio, 2000-2006
| 2000 | 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | |
| CADPP providers | n/a | n/a | 0.62 | 0.61 | 0.61 | 0.58 | 0.51 |
| Non-CADPP providers | 0.50 | 0.48 | 0.50 | 0.50 | 0.49 | 0.46 | 0.43 |
NOTE: n/a = not applicable.
SOURCE: Morales and Reisdorf, 2008.
and MinnesotaCare. While all three programs provide a dental benefit, only 44 percent of MA enrollees, 36 percent of GAMC enrollees, and 51 percent of MinnesotaCare enrollees visited a dentist in 2006 (Morales and Reisdorf, 2008).
A 2008 study of the program’s impact on access showed that while a higher payment to charge ratio could be achieved with the CADPP designation in fee-for-service programs (see Table 5-3), providers continued to state that they could not afford to participate in the program.
The evaluation found that while the number of MHCP participants increased during the study period, the percent of continuously enrolled individuals receiving dental care remained stable while the rate of visits increased slightly. The researchers indicated a “growing concern for the creation of Medicaid dental mills” in which providers might deliver multiple procedures in order to maximize profitability. Overall, the researchers concluded that
As measured by the overall number of enrollees obtaining dental services, the CADPP has demonstrated that add-on payment rates have not led to an increase in dental access for MHCP enrollees. Regardless of this finding, the program should continue to serve as a viable means of sustaining dental practices that see high volumes of MHCP enrollees and provide high quality evidence based care.
In addition, the researchers recommended further exploration into the effect of streamlining of administrative processes as well as payment rates.
Enhanced Medicaid Payments and Streamlined Administration
In 2000 the State of Michigan enrolled Medicaid-eligible children from 22 rural counties (increased to 59 counties in subsequent years) in a Delta Dental of Michigan plan called Healthy Kids Dental (HKD) (Eklund et al., 2003). Delta set fees (adjusted annually for inflation) for HKD children the same as for privately insured patients, used the same administrative
processes for filing claims, and so forth, but did not charge patients any out-of-pocket expenses. In 5 years (2005), HKD utilization rates for those enrolled for 12 months increased to 53 percent, compared to the traditional Medicaid program (35 percent), but they were not as high as the privately insured (64 percent) (Eklund et al., 2003). The existing dental workforce was able to provide care to another 100,000 children (200,000 eligible).
Streamlined Administration and Supportive Activities
A recent CMS report features state-level efforts to improve the provision of Medicaid dental services through innovative practices (CMS, 2011a). For example, in Alabama, outreach to increase provider participation includes on-site assistance to dentists in completing Medicaid application forms; Maryland uses electronic funds transfer to improve the timeliness of reimbursement to providers; and Maryland and Virginia use a single contractor to administer their dental programs to reduce the paperwork providers and their office staff must complete; and Virginia reduced the prior authorizations needed for dental services (CMS, 2011a). The CMS report notes “states and providers interviewed say that these simplifications are extremely important to maintaining and increasing provider participation” (CMS, 2011a).
Integrating Medical and Oral Health Coverage
In Massachusetts, Blue Cross Blue Shield (BCBSMA) provides integrated medical and oral health coverage with the aim of improving overall health outcomes and removing cost barriers to oral health care among its vulnerable beneficiaries. Beneficiaries with diabetes, coronary artery disease (CAD), oral cancer, and women who are pregnant that have both medical and dental coverage are automatically enrolled in a program that provides “enhanced dental benefits.” These individuals are eligible to receive additional services (such as cleanings or periodontal maintenance every 3 months) at no additional cost, based on their condition.
According to BCBSMA claims data, this approach has lowered medical costs among participants with diabetes and CAD. For example, BCBSMA claims data from 2007 showed that beneficiaries with CAD and diabetes who received periodontal services had lower overall monthly costs than those who received no dental care or preventive dental services alone (Lewando, 2010). BCBSMA claims data from 2009 showed that beneficiaries with CAD and diabetes who received dental prophylaxis and/or periodontal treatment had lower per-member-per-month medical costs than beneficiaries who did not receive treatment ($487 and $67, respectively) (Lewando, 2010). While this approach is not specifically designed to increase access, it is an example of an innovative cost-savings strategy
targeted at vulnerable populations. Furthermore, it supports the committee’s guiding principles that oral health care is an essential component of comprehensive health care and that oral health promotion and disease prevention are essential to any strategies aimed at improving access to care.
As described in Chapter 1, the committee encountered considerable shortcomings in the research on expenditures and financing for oral health care during its review of the evidence. The committee made every effort to include the most up-to-date research published in peer-reviewed journals on these subjects. On the surface, it may appear that some of the references are dated. However, the committee determined that, in some cases, the strongest evidence on oral health financing and coverage was found in studies that have not been replicated in recent years. In other cases, newer data have been collected (through surveys such as NHANES and MEPS), but they have not been fully analyzed. Because the committee was not equipped to or charged with analyzing these data, it has cited the most current published analyses.
In addition to the lack of recent data in key areas, the committee was constrained by the somewhat limited analyses of data that exist on oral health coverage and financing. In general, the committee found few studies that provide detailed analyses of oral health financing by specific variables of interest or that analyzed complex relationships. For example, analyses of the different categories of dental coverage by subpopulations would provide a more complete picture of the impact of coverage on access and utilization and move beyond simple comparisons. In lieu of more detailed analyses, the committee relied on the strongest evidence available in the literature.
Finally, by reviewing and synthesizing the evidence, this chapter underscores the overall deficiencies in research on oral health financing. The committee hopes that this examination will help generate additional research questions and provide direction for future research.
The committee noted the following findings and conclusions:
• Financing for oral health care greatly influences where and whether individuals receive care.
• Per capita out-of-pocket spending for dental services is proportionally much greater than for medical services.
• Dental coverage is positively tied to access to and utilization of oral health care.
• Comprehensive dental benefits are federally required for all Medicaid-enrolled children, and all states are required to provide comparable dental coverage to children enrolled in CHIP.
• However, access to dental care continues to be a problem for children in Medicaid and CHIP.
• Medicaid benefits are not required for adults in every state, and among those states that offer dental coverage for adult Medicaid recipients, the benefits are typically limited to emergency coverage.
• Medicaid cannot properly address access to oral health services if it excludes oral health benefits.
• Low provider participation in the Medicaid program has a direct and generally negative impact on access to dental care for Medicaid beneficiaries.
• Medicare does not cover routine checkups, cleanings, fillings, or dentures for older adults.
• The federal government and states make considerable investments in dental coverage (e.g., Medicaid and CHIP), oral health services, infrastructure, and research. These investments, however, are insufficient in providing dental coverage and improving access to care for vulnerable and underserved populations.
AAP (American Academy of Pediatrics). 2010. Fluoride information by state. http://www.aap.org/commpeds/dochs/oralhealth/fluoride.cfm (accessed March 15, 2011).
ADA (American Dental Association). 2004. State and community models for improving access to dental care for the underserved—a white paper. Chicago, IL.
ADHA (American Dental Hygienists’ Association). 2010. States which directly reimburse dental hygienists for services under the Medicaid program. http://www.adha.org/governmental_affairs/downloads/medicaid.pdf (accessed March 12, 2011).
AHRQ (Agency for Healthcare Research and Quality). 2009. Dental services—Mean and median expenses per person with expense and distribution of expenses by source of payment: United States, 2007. http://www.meps.ahrq.gov/ (accessed March 15, 2011).
AHRQ. 2010. 2009 National healthcare disparities report. Rockville, MD: U.S. Department of Health and Human Services.
Association of Maternal and Child Health Programs. 2011. State profile: Iowa maternal and child health block grant 2011. http://www.amchp.org/Advocacy/BLOCK-GRANT/2011PROFILES/Iowa.pdf (accessed March 16, 2011).
ASTDD (Association of State and Territorial Dental Directors). 2010. Synopses of state dental public health programs: Data for FY 2008-2009. http://www.astdd.org/docs/StateSynopsisReport2010SUMMARY.pdf (accessed April 5, 2011).
ASTDD. 2011. Best practice approach reports. http://www.astdd.org/best-practice-approach-reports (accessed March 17, 2011).
Bailit, H., J. D’Adamo, and T. Beazoglou. 2010 (unpublished). Report to the Oral Health Access Committee: State case studies: Improving access to dental care for the underserved.
Barsky, C. B. 2004. Incidence benefits measures in the national compensation survey. Monthly Labor Review 127(8):21-28.
Berman, S., J. Dolins, S. F. Tang, and B. Yudkowsky. 2002. Factors that influence the willingness of private primary care pediatricians to accept more Medicaid patients. Pediatrics 110(2 I):239-248.
Bisgaier, J., D. B. Cutts, B. L. Edelstein, and K. V. Rhodes. 2011. Disparities in child access to emergency care for acute oral injury. Pediatrics, doi:10.1542/peds.2011-0011.
Bloom, B., and R. A. Cohen. 2010. Dental insurance for persons under age 65 years with private health insurance: United States, 2008. Hyattsville, MD: National Center for Health Statistics.
BLS (Bureau of Labor Statistics). 2010a. Consumer out-of-pocket health care expenditures in 2008. http://www.bls.gov/opub/ted/2010/ted_20100325_data.htm (accessed January 9, 2011).
BLS. 2010b. Employee benefits survey: Health care benefits, March 2010. http://www.bls.gov/ncs/ebs/benefits/2010/benefits_health.htm (accessed December 28, 2010).
BLS. 2011. Selected medical benefits: A report from the Department of Labor to the Department of Health and Human Services. http://www.bls.gov/ncs/ebs/sp/selmedbensreport.pdf (accessed May 23, 2011).
Borchgrevink, A., A. Snyder, and S. Gehshan. 2008. The effects of Medicaid reimbursement rates on access to dental care. Washington, DC: National Academy for State Health Policy.
CDC (Centers for Disease Control and Prevention). 2011a. Division of oral health state-based programs. http://www.cdc.gov/oralhealth/state_programs.index.htm (accessed November 17, 2011).
CDC. 2011b. Prevention research centers. http://www.cdc.gov/prc (accessed November 17, 2011).
CDC. 2011c. Preventive health and health services block grant funding by health program areas, fiscal year: 2010. http://www.cdc.gov/phhsblockgrant/funding/blockgrant10.htm (accessed November 17, 2011).
Center for Oral Health. 2010. WIC programs. http://www.centerfororalhealth.org/programs/wic-programs (accessed January 31, 2011).
Children’s Dental Health Project. 2010. Oral health provisions in the Patient Protection and Affordable Care Act. http://www.cdhp.org/system/files/FINAL%20HCR%20Senate%20Bill%20Summary%20-%203%2023%2010.pdf (accessed March 17, 2011).
CMS (Centers for Medicare and Medicaid Services). 2005a. Early and periodic screening, diagnostic, and treatment benefit overview. https://www.cms.gov/MedicaidEarlyPeriodicScrn/01_Overview.asp#TopOfPage (accessed March 16, 2011).
CMS. 2005b. Early and periodic screening, diagnostic, and treatment benefits. https://www.cms.gov/MedicaidEarlyPeriodicScrn/02_Benefits.asp#TopOfPage (accessed March 16, 2011).
CMS. 2009. 2009 Medicaid managed care enrollment report. https://www.cms.gov/MedicaidDataSourcesGenInfo/04_MdManCrEnrllRep.asp (accessed March 16, 2011).
CMS. 2010a. Medicare dental coverage: Overview. http://www.cms.hhs.gov/MedicareDentalCoverage (accessed November 22, 2010).
CMS. 2010b. National health expenditure accounts. https://www.cms.gov/nationalhealthexpenddata/02_nationalhealthaccountshistorical.asp (accessed February 22, 2011).
CMS. 2010c. National health expenditure projections 2009-2019. https://www.cms.gov/NationalHealthExpendData/downloads/NHEProjections2009to2019.pdf (accessed February 22, 2011).
CMS. 2011a. Innovative state practices for improving the provision of Medicaid dental services. Baltimore, MD.
CMS. 2011b. Overview Medicaid dental coverage. https://www.cms.gov/MedicaidDentalCoverage/ (accessed March 16, 2011).
Cunningham, P. J., and J. H. May. 2006. Medicaid patients increasingly concentrated among physicians. Washington, DC: Center for Studying Health System Change.
Damiano, P. C., E. R. Brown, J. D. Johnson, and J. P. Scheetz. 1990. Factors affecting dentist participation in a state Medicaid program. Journal of Dental Education 54(11):638-643.
Damiano, P., J. Willard, E. Momany, and J. Chowdhury. 2003. The impact of the Iowa S-SCHIP program on access, health status, and family environment. Ambulatory Pediatrics 3:263-269.
Dasanayake, A. P., Y. Li, et al. 2007. Challenges faced by minority children in obtaining dental care. Journal of Health Care for the Poor and Underserved 18(4):779-788.
Decker, S. L. 2011. Medicaid payment levels to dentists and access to dental care among children and adolescents. Journal of the American Medical Association 306(2):187-193.
Edelstein, B. L., and C. H. Chinn. 2009. Update on disparities in oral health and access to dental care for America’s children. Academic Pediatrics 9(6):415-419.
Eklund, S. A., J. L. Pittman, and S. J. Clark. 2003. Michigan Medicaid’s healthy kids dental program: An assessment of the first 12 months. Journal of the American Dental Association 134(11):1509-1515.
Feinberg, E., K. Swartz, A. Zaslavsky, J. Gardner, and D. K. Walker. 2002. Family income and the impact of a Children’s Health Insurance Program on reported need for health services and unmet health need. Pediatrics 109(2):E29.
Ferguson, D. A., B. J. Steinberg, and T. Schwien. 2010. Dental economics and the aging population. Compendium of Continuing Education in Dentistry 31(6):418-420, 422, 424-425.
Fisher, M. A., and A. K. Mascarenhas. 2007. Does Medicaid improve utilization of medical and dental services and health outcomes for Medicaid-eligible children in the United States? Community Dentistry and Oral Epidemiology 35(4):263-271.
Flores, G., and S. C. Tomany-Korman. 2008. Racial and ethnic disparities in medical and dental health, access to care, and use of services in U.S. children. Pediatrics 121(2): e286-e298.
Ford, J. L. 2009. The new health participation and access data from the National Compensation Survey. http://www.bls.gov/opub/cwc/cm20091022ar01p1.htm (accessed December 27, 2010).
Fox, M., J. Moore, R. Davis, and R. Heintzelman. 2003. Changes in reported health status and unmet need for children enrolling in the Kansas Children’s Health Insurance Program. American Journal of Public Health 93(4):579-582.
GAO (Government Accountability Office). 2000. Factors contributing to low use of dental services by low-income populations. Washington, DC: U.S. General Accounting Office.
GAO. 2009. State and federal actions have been taken to improve children’s access to dental services, but gaps remain. Washington, DC: U.S. Government Accountability Office.
GAO. 2010. Efforts under way to improve children’s access to dental services, but sustained attention needed to address ongoing concerns. Washington, DC: U.S. Government Accountability Office.
Greenberg, B. J. S., J. V. Kumar, and H. Stevenson. 2008. Dental case management: Increasing access to oral health care for families and children with low incomes. Journal of the American Dental Association 139(8):1114-1121.
Greene-Mclntyre, M., M. Finch, and J. Searcy. 2003. Smile Alabama! Initiative: Interim results from a program to increase children’s access to dental care. Journal of Rural Health 19(5):407-415.
Griffin, S. O., K. A. Jones, S. Lockwood, N. G. Mosca, and P. A. Honoré. 2007. Impact of increasing Medicaid dental reimbursement and implementing school sealant programs on sealant prevalence. Journal of Public Health Management and Practice 13(2):202-206.
Helgeson, M. J. 2005. The Minnesota oral health care solutions project: Implications for people with special needs. CDA Journal 33(8):641-649.
HHS (Department of Health and Human Services). 2008. State MCH-Medicaid coordination: A review of Title V and Title XIX interagency agreements (2nd ed). ftp://ftp.hrsa.gov/mchb/IAA/State_MCH_Medicaid_Coord.pdf (accessed April 5, 2011).
HHS/ACF (Administration for Children and Families)/OHS (Office of Head Start). 2011. Head Start dental home initiative. http://eclkc.ohs.acf.hhs.gov/hslc/tta-system/health/Health/Oral%20Health (accessed November 17, 2011). HRSA (Health Resources and Services Administration). 2010. MCHB discretionary grant information system.https://perfdata.hrsa.gov/mchb/mchreports/search/program/prgsch02_result.asp (accessed March 31, 2011).
HRSA (Health Resources and Services Administration). 2011a. Fiscal year 2011 justification of estimates for appropriations committees. http://www.hrsa.gov/about/budgetjustifica-tion/budgetjustification11.pdf (accessed April 5, 2011).
HRSA. 2011b. Maternal and Child Health Bureau discretionary grant information system reports. https://perfdata.hrsa.gov/MCHB/DGISReports/default.aspx (accessed March 17, 2011).
HRSA. 2011c. Maternal and Child Health Bureau: TVIS snapshots. https://perfdata.hrsa.gov/mchb/TVISReports/Snapshot/SnapShotMenu.aspx (accessed March 17, 2011).
HRSA. 2011d. Fiscal year 2011 justification of estimates for appropriations committees.http://www.hrsa.gov/about/budget/budgetjustification2012.pdf (accessed May 11, 2011).
Hughes, R. J., P. C. Damiano, M. J. Kanellis, R. Kuthy, and R. Slayton. 2005. Dentists’ participation and children’s use of services in the Indiana dental Medicaid program and SCHIP: Assessing the impact of increased fees and administrative changes. Journal of the American Dental Association 136(4):517-523.
IOM (Institute of Medicine). 1980. Public policy options for better dental health. Washington, DC: National Academy Press.
IOM. 2000. Extending Medicare coverage for preventive and other services. Washington, DC: National Academy Press.
Jablonski, R. A., C. L. Munro, M. J. Grap, and R. K. Elswick. 2005. The role of biobehavioral, environmental, and social forces on oral health disparities in frail and functionally dependent nursing home elders. Biological Research for Nursing 7(1):75-82.
Johnson, J. T., E. G. Turner, K. F. Novak, and A. L. Kaplan. 2005. Factors associated with comprehensive dental care following an initial emergency dental visit. Journal of Dentistry for Children 72(2):78-80.
Kenney, G. 2007. The impacts of the State Children’s Health Insurance Program on children who enroll: Findings from ten states. Health Services Research 42(4):1520-1543.
Kenney, M. K. 2009. Oral health care in CSHCN: State Medicaid policy considerations. Pediatrics 124(Supp. 4):S384-S391.
Klein, J. D., L. P. Shone, P. G. Szilagyi, A. Bajorska, K. Wilson, and A. W. Dick. 2007. Impact of the state children’s health insurance program on adolescents in New York. Pediatrics 119(4):e885-e892.
Kobayashi, M., D. Chi, S. E. Coldwell, P. Domoto, and P. Milgrom. 2005. The effectiveness and estimated costs of the access to baby and child dentistry program in Washington state. Journal of the American Dental Association 136(9):1257-1263.
Lang, W. P., and J. A. Weintraub. 1986. Comparison of Medicaid and non-Medicaid dental providers. Journal of Public Health Dentistry 46(4):207-211.
Lave, J. R., C. R. Keane, C. J. Lin, and E. M. Ricci. 2002. The impact of dental benefits on the utilization of dental services by low-income children in western Pennsylvania. Pediatric Dentistry 24(3):234-240.
Lewando, R. 2010. Periodontal disease and chronic diseases: Emerging science and programs: BCBSMA Total Health Solutions. Presentation to the National Oral Health Conference, April 27, 2010. http://www.nationaloralhealthconference.com/docs/presentations/2010/Robert%20Lewando%20-%20Periodontal%20Disease.pdf (accessed May 12, 2011).
Lewis, C., W. Mouradian, R. Slayton, and A. Williams. 2007. Dental insurance and its impact on preventative dental care visits for U.S. children. Journal of the American Dental Association 138(3):369-380.
Lewis, C. W., S. Boulter, M. A. Keels, D. M. Krol, W. E. Mouradian, K. G. O’Connor, and R. B. Quinonez. 2009. Oral health and pediatricians: Results of a national survey. Academic Pediatrics 9(6):457-461.
Liu, J., J. C. Probst, A. B. Martin, J.-Y. Wang, and C. F. Salinas. 2007. Disparities in dental insurance coverage and dental care among U.S. children: The National Survey of Children’s Health. Pediatrics 119(Supp. 1):S12-S21.
Manski, R. J., and E. Brown. 2007. Dental use, expenses, private dental coverage, and changes, 1996 and 2004. Rockville, MD: Agency for Healthcare Research and Quality.
Manski, R. J., and E. Brown. 2008. Dental coverage of children and young adults under age 21, United States, 1996 and 2006. Statistical brief #221. Rockville, MD: Agency for Healthcare Research and Quality.
Manski, R. J., and E. Brown. 2010. Dental coverage of adults ages 21-64, United States, 1997 and 2007. Rockville, MD: Agency for Healthcare Research and Quality.
Manski, R. J., and P. F. Cooper. 2010. Characteristics of employers offering dental coverage in the united states. Journal of the American Dental Association 141(6):700-711.
Manski, R. J., J. Moeller, H. Chen, P. A. St. Clair, J. Schimmel, L. Magder, and J. V. Pepper. 2010a. Dental care expenditures and retirement. Journal of Public Health Dentistry 70(2):148-155.
Manski, R. J., J. Moeller, J. Schimmel, P. A. St. Clair, H. Chen, L. Magder, and J. V. Pepper. 2010b. Dental care coverage and retirement. Journal of Public Health Dentistry 70(1):1-12.
Mayer, M. L., S. C. Stearns, E. C. Norton, and R. G. Rozier. 2000. The effects of Medicaid expansions and reimbursement increases on dentists’ participation. Inquiry 37(1):33-44.
McBroome, K., P. C. Damiano, and J. C. Willard. 2005. Impact of the Iowa S-SCHIP program on access to dental care for adolescents. Pediatric Dentistry 27(1):47-53.
McKnight-Hanes, C., D. R. Myers, and J. C. Dushku. 1992. Method of payment for children’s dental services by practice type and geographic location. Pediatric Dentistry 14(5):338-341.
Milgrom, P., R. S.-Y. Lee, C. E. Huebner, and D. A. Conrad. 2010. Medicaid reforms in Oregon and suboptimal utilization of dental care by women of childbearing age. Journal of the American Dental Association 141(6):688-695.
Moeller, J. F., H. Chen, and R. J. Manski. 2010. Investing in preventive dental care for the Medicare population: A preliminary analysis. American Journal of Public Health 100(11):2262-2269.
Mofidi, M., R. Slifkin, V. Freeman, and P. Silberman. 2002. The impact of a state children’s health insurance program on access to dental care. Journal of the American Dental Association 133(6):707-714.
Morales, M. and C. Reisdorf. 2008. Minnesota health care programs: Critical Access Dental Program—results and recommendations. St. Paul, MN: Minnesota Department of Human Services.
NADP (National Association of Dental Plans). 2009. Dental benefits improve access to dental care. http://www.nadp.org/Libraries/HCR_Documents/nadphcr-dentalbenefitsimproveac-cesstocare-3-28-09.sflb.ashx (accessed January 10, 2011).
Paradise, J. 2008. Dental coverage and care for low-income children: The role of Medicaid and SCHIP. Washington, DC: Kaiser Family Foundation.
Patton, L. L., B. A. White, and M. J. Field. 2001. Extending Medicare coverage to medically necessary dental care. Journal of the American Dental Association 132(9):1294-1299.
Pourat, N., and L. Finocchio. 2010. Racial and ethnic disparities in dental care for publicly insured children. Health Affairs 29(7):1356-1363.
Ramírez, M., K. P. Ahluwalia, and J. A. Teresi. 2011. Correlates of dental visits among community-residing Latino elders: A public health alert. Gerodontology 28(1):12-18.
Rohde, F. 2010. Dental expenditures in the 10 largest states, 2007. Rockville, MD: Agency for Healthcare Research and Quality.
Rosenbach, M., M. Ellwood, C. Irvin, C. Young, W. Conroy, B. Quinn, and M. Kell. 2003. Implementation of the state children’s health insurance program: Synthesis of state evaluations. Washington, DC: Mathematica Policy Research Inc.
Rowley, S. T., B. Sheller, B. J. Williams, and L. Mancl. 2006. Utilization of a hospital for treatment of pediatric dental emergencies. Pediatric Dentistry 28(1):10-17.
Schlitt, J. J., L. J. Juszczak, and N. H. Eichner. 2008. Current status of state policies that support school-based health centers. Public Health Reports 123(6):731-738.
Shiboski, C. H., M. Cohen, K. Weber, A. Shansky, K. Malvin, and R. M. Greenblatt. 2005. Factors associated with use of dental services among HIV-infected and high-risk uninfected women. Journal of the American Dental Association 136(9):1242-1255.
Shirk, C. 2010. Oral health checkup: Progress in tough fiscal times? Washington, DC: National Health Policy Forum.
Shortridge, E. F., and J. R. Moore. 2009. Use of emergency departments for conditions related to poor oral healthcare: Implications for rural and low-resource urban areas for three states. Journal of Public Health Management and Practice 15(3):238-245.
Smith, V., K. Gifford, E. Ellis, R. Rudowitz, and L. Snyder. 2010. Hoping for economic recovery, preparing for health reform: A look at Medicaid spending, coverage and policy trends. Washington, DC: Kaiser Family Foundation.
Snowden, C. B., T. R. Miller, A. F. Jensen, and B. A. Lawrence. 2003. Costs of medically treated craniofacial conditions. Public Health Reports 118(1):10-17.
Snyder, A. 2009. Increasing access to dental care in Medicaid: Targeted programs for four populations. Washington, DC: National Association for State Health Policy.
Sohn, W., A. Ismail, A. Amaya, and J. Lepkowski. 2007. Determinants of dental care visits among low-income African-American children. Journal of the American Dental Association 138(3):309-318.
Sweet, M., P. Damiamo, E. Rivera, R. Kuthy, and K. Heller. 2005. A comparison of dental services received by Medicaid and privately insured adult populations. Journal of the American Dental Association 136(1):93-100.
Szilagyi, P. G., A. W. Dick, J. D. Klein, L. P. Shone, J. Zwanziger, and T. McInerny. 2004. Improved access and quality of care after enrollment in the New York State Children’s Health Insurance Program (SCHIP). Pediatrics 113(5):e395-e404.
Taichman, L. S., W. Sohn, S. Lim, S. Eklund, and A. Ismail. 2009. Assessing patterns of restorative and preventive care among children enrolled in Medicaid, by type of dental care provider. Journal of the American Dental Association 140(7):886-894.
Trenholm, C., E. Howell, D. Hughes, and S. Orzol. 2005. The Santa Clara County Healthy Kids Program: Impacts on children’s medical, dental, and vision care. Mathematica Policy Research Report, http://www.mathematica-mpr.com/publications/PDFs/santaclara.pdf (accessed May 10, 2011).
VanLandeghem, K., J. Bronstein, and C. Brach. 2003. Children’s dental care access in Medicaid: The role of medical care use and dentist participation. Rockville, MD: Agency for Healthcare Research and Quality.
Venezie, R., W. Vann Jr., S. Cashion, and R. Rozier. 1997. Pediatric and general dentists’ participation in the North Carolina Medicaid program: Trends from 1986 to 1992. Pediatric Dentistry 19(2):114-117.
Wang, H., E. C. Norton, and R. G. Rozier. 2007. Effects of the State Children’s Health Insurance Program on access to dental care and use of dental services. Health Services Research 42(4):1544-1563.
Wysen, K. H., P. M. Hennessy, M. I. Lieberman, T. E. Garland, and S. M. Johnson. 2004.
Kids get care: Integrating preventive dental and medical care using a public health case management model. Journal of Dental Education 68(5):522-530.
Zuckerman, S., J. Haley, Y. Roubideaux, and M. Lillie-Blanton. 2004. Health service access, use, and insurance coverage among American Indians/Alaska Natives and whites: What role does the Indian Health Service play? American Journal of Public Health 94(1):53-59.




































