Crisis Standards of Care
A Systems Framework for Catastrophic Disaster Response
Volume 7: Appendixes
Committee on Guidance for Establishing Standards of Care for Use in Disaster Situations
Board on Health Sciences Policy
Dan Hanfling, Bruce M. Altevogt, Kristin Viswanathan, and Lawrence O. Gostin, Editors
INSTITUTE OF MEDICINE
OF THE NATIONAL ACADEMIES
THE NATIONAL ACADEMIES PRESS
Washington, D.C.
|
THE NATIONAL ACADEMIES PRESS |
500 Fifth Street, NW |
Washington, DC 20001 |
NOTICE: The project that is the subject of this report was approved by the Governing Board of the National Research Council, whose members are drawn from the councils of the National Academy of Sciences, the National Academy of Engineering, and the Institute of Medicine. The members of the committee responsible for the report were chosen for their special competences and with regard for appropriate balance.
This study was supported by Contract No. HHSP23320042509XI between the National Academy of Sciences and the Department of Health and Human Services. Any opinions, findings, conclusions, or recommendations expressed in this publication are those of the author(s) and do not necessarily reflect the view of the organizations or agencies that provided support for this project.
Library of Congress Cataloging-in-Publication Data
Crisis standards of care : a systems framework for catastrophic disaster response / Committee on Guidance for Establishing Standards of Care for Use in Disaster Situations, Board on Health Sciences Policy ; Dan Hanfling … [et al.], editors.
p. ; cm.
Includes bibliographical references.
ISBN 978-0-309-25346-8 (hardcover) — ISBN 978-0-309-25347-5 (pdf ) I. Hanfling, Dan.
II. Institute of Medicine (U.S.). Committee on Guidance for Establishing Standards of Care for Use in Disaster Situations.
[DNLM: 1. Disaster Medicine—standards—United States. 2. Emergency
Medical Services—standards—United States. 3. Emergency Treatment—
standards—United States. WA 295]
363.34—dc23
2012016602
Additional copies of this report are available from the National Academies Press, 500 Fifth Street, NW, Keck 360, Washington, DC 20001; (800) 624-6242 or (202) 334-3313; http://www.nap.edu.
For more information about the Institute of Medicine, visit the IOM home page at: www.iom.edu.
Copyright 2012 by the National Academy of Sciences. All rights reserved.
Printed in the United States of America
The serpent has been a symbol of long life, healing, and knowledge among almost all cultures and religions since the beginning of recorded history. The serpent adopted as a logotype by the Institute of Medicine is a relief carving from ancient Greece, now held by the Staatliche Museen in Berlin.
Suggested citation: IOM (Institute of Medicine). 2012.Crisis Standards of Care: A Systems Framework for Catastrophic Disaster Response. Washington, DC: The National Academies Press.
THE NATIONAL ACADEMIES
Advisers to the Nation on Science, Engineering, and Medicine
The National Academy of Sciences is a private, nonprofit, self-perpetuating society of distinguished scholars engaged in scientific and engineering research, dedicated to the furtherance of science and technology and to their use for the general welfare. Upon the authority of the charter granted to it by the Congress in 1863, the Academy has a mandate that requires it to advise the federal government on scientific and technical matters. Dr. Ralph J. Cicerone is president of the National Academy of Sciences.
The National Academy of Engineering was established in 1964, under the charter of the National Academy of Sciences, as a parallel organization of outstanding engineers. It is autonomous in its administration and in the selection of its members, sharing with the National Academy of Sciences the responsibility for advising the federal government. The National Academy of Engineering also sponsors engineering programs aimed at meeting national needs, encourages education and research, and recognizes the superior achievements of engineers. Dr. Charles M. Vest is president of the National Academy of Engineering.
The Institute of Medicine was established in 1970 by the National Academy of Sciences to secure the services of eminent members of appropriate professions in the examination of policy matters pertaining to the health of the public. The Institute acts under the responsibility given to the National Academy of Sciences by its congressional charter to be an adviser to the federal government and, upon its own initiative, to identify issues of medical care, research, and education. Dr. Harvey V. Fineberg is president of the Institute of Medicine.
The National Research Council was organized by the National Academy of Sciences in 1916 to associate the broad community of science and technology with the Academy’s purposes of furthering knowledge and advising the federal government. Functioning in accordance with general policies determined by the Academy, the Council has become the principal operating agency of both the National Academy of Sciences and the National Academy of Engineering in providing services to the government, the public, and the scientific and engineering communities. The Council is administered jointly by both Academies and the Institute of Medicine. Dr. Ralph J. Cicerone and Dr. Charles M. Vest are chair and vice chair, respectively, of the National Research Council.
COMMITTEE ON GUIDANCE FOR ESTABLISHING STANDARDS OF CARE FOR USE IN DISASTER SITUATIONS
LAWRENCE O. GOSTIN (Chair), O’Neill Institute for National and Global Health Law, Georgetown University Law Center, Washington, DC
DAN HANFLING (Vice-Chair), Inova Health System, Falls Church, VA
DAMON T. ARNOLD, Illinois Department of Public Health, Chicago (retired)
STEPHEN V. CANTRILL, Denver Health Medical Center, CO
BROOKE COURTNEY, Food and Drug Administration, Bethesda, MD
ASHA DEVEREAUX, California Thoracic Society, San Francisco, CA
EDWARD J. GABRIEL,* The Walt Disney Company, Burbank, CA
JOHN L. HICK, Hennepin County Medical Center, Minneapolis, MN
JAMES G. HODGE, JR., Center for the Study of Law, Science, and Technology, Arizona State University, Tempe
DONNA E. LEVIN, Massachusetts Department of Public Health, Boston
MARIANNE MATZO, University of Oklahoma Health Sciences Center, Oklahoma City
CHERYL A. PETERSON, American Nurses Association, Silver Spring, MD
TIA POWELL, Montefiore-Einstein Center for Bioethics, Albert Einstein College of Medicine, New York, NY
MERRITT SCHREIBER, University of California, Irvine, School of Medicine
UMAIR A. SHAH, Harris County Public Health and Environmental Services, Houston, TX
JOLENE R. WHITNEY, Bureau of Emergency Medical Services (EMS) and Preparedness, Utah Department of Health, Salt Lake City
Study Staff
BRUCE M. ALTEVOGT, Study Director
ANDREW M. POPE, Director, Board on Health Sciences Policy
CLARE STROUD, Program Officer
LORA TAYLOR, Senior Project Assistant (until January 2012)
ELIZABETH THOMAS, Senior Project Assistant (since February 2012)
KRISTIN VISWANATHAN, Research Associate
RONA BRIER, Editor
BARBARA FAIN, Consultant for Public Engagement
_________________
* Resigned from the committee October 2011.
Reviewers
This report has been reviewed in draft form by individuals chosen for their diverse perspectives and technical expertise, in accordance with procedures approved by the National Research Council’s Report Review Committee. The purpose of this independent review is to provide candid and critical comments that will assist the institution in making its published report as sound as possible and to ensure that the report meets institutional standards for objectivity, evidence, and responsiveness to the study charge. The review comments and draft manuscript remain confidential to protect the integrity of the deliberative process. We wish to thank the following individuals for their review of this report:
Richard Alcorta, Maryland Institute for Emergency Medical Services Systems
Knox Andress, Louisiana Poison Center
Connie Boatright-Royster, MESH Coalition
Susan Cooper, Tennessee Department of Health
Lance Gable, Wayne State University Center for Law and the Public’s Health
Carol Jacobson, Ohio Hospital Association
Amy Kaji, Harbor-UCLA Medical Center
Jon Krohmer, Department of Homeland Security
Onora Lien, King County Healthcare Coalition
Suzet McKinney, The Tauri Group
Peter Pons, Denver Health Medical Center
Clifford Rees, University of New Mexico School of Law
Linda Scott, Michigan Department of Community Health
Robert Ursano, Uniformed Services University School of Medicine
Lann Wilder, San Francisco General Hospital and Trauma Center
Matthew Wynia, American Medical Association
Although the reviewers listed above have provided many constructive comments and suggestions, they were not asked to endorse the conclusions or recommendations nor did they see the final draft of the report before
its release. The review of this report was overseen by Dr. Georges Benjamin, American Public Health Association. Appointed by the Institute of Medicine, he was responsible for making certain that an independent examination of this report was carried out in accordance with institutional procedures and that all review comments were carefully considered. Responsibility for the final content of this report rests entirely with the authoring committee and the institution.
Contents
VOLUME 1: INTRODUCTION AND CSC FRAMEWORK
2 Catastrophic Disaster Response: Creating a Framework for Medical Care Delivery
4 Cross-Cutting Themes: Ethics, Palliative Care, and Mental Health
VOLUME 2: STATE AND LOCAL GOVERNMENT
6 Prehospital Care: Emergency Medical Services (EMS)
7 Hospitals and Acute Care Facilities
VOLUME 5: ALTERNATE CARE SYSTEMS
Alternate care facility A temporary site, not located on hospital property, that is established to provide patient care. It may provide either ambulatory or nonambulatory care. It may serve to “decompress” hospitals that are maximally filled, or to bolster community-based triage capabilities. Has also been referred to as an “alternate care site.”
Clinical care committee Composed of clinical and administrative leaders at a health care institution, this committee is responsible for prioritizing the allocation of critical life-sustaining interventions. The clinical care committee may also be formed at the health care coalition level (e.g., hospital, primary care, emergency medical services agency, public health, emergency management, and others), playing the role of the disaster medical advisory committee at the regional level (see disaster medical advisory committee). May appoint a triage team (see triage team) to evaluate case-by-case decisions.
Contingency surge The spaces, staff, and supplies used are not consistent with daily practices, but provide care that is functionally equivalent to usual patient care practices. These spaces or practices may be used temporarily during a major mass casualty incident or on a more sustained basis during a disaster (when the demands of the incident exceed community resources).
Conventional capacity The spaces, staff, and supplies used are consistent with daily practices within the institution. These spaces and practices are used during a major mass casualty incident that triggers activation of the facility emergency operations plan.
Crisis standards of care The level of care possible during a crisis or disaster due to limitations in supplies, staff, environment, or other factors. These standards will usually incorporate the following principles: (1) prioritize population health rather than individual outcomes; (2) respect ethical principles of beneficence, stewardship, equity, and trust; (3) modify regulatory requirements to provide liability protection for healthcare providers making resource allocation decisions; and/or (4) designate a crisis triage officer and include provisions for palliative care in triage models for scarce resource allocation (e.g., ventilators). Crisis standards of care will usually follow a formal declaration or recognition by state government during a pervasive (pandemic influenza) or catastrophic (earthquake, hurricane) disaster which recognizes that contingency surge
response strategies (resource-sparing strategies) have been exhausted, and crisis medical care must be provided for a sustained period of time. Formal recognition of these austere operating conditions enables specific legal/regulatory powers and protections for health care provider allocation of scarce medical resources and for alternate care facility operations. Under these conditions, the goal is still to supply the best care possible to each patient.
Crisis surge Adaptive spaces, staff, and supplies are not consistent with usual standards of care, but provide sufficiency of care in the setting of a catastrophic disaster (i.e., provide the best possible care to patients given the circumstances and resources available). Crisis capacity activation constitutes a significant adjustment to standards of care.
Disaster medical advisory committee At the state or regional level, evaluates evidence-based, peerreviewed critical care and other decision tools and recommends decision-making algorithms to be used when life-sustaining resources become scarce. May also be involved in providing broader recommendations regarding disaster planning and response efforts. When formed at the regional level, this group may take on the same functions as that of the clinical care committee. Those functions are focused in two distinct areas—medical advisory input and resource allocation decision approval. The state development and implementation templates, at the end of Chapter 5, describe planning and response roles for the State Disaster Medical Advisory Committee (SDMAC).
Emergency Management Assistance Compact (EMAC) The first national disaster-relief compact, the EMAC has been adopted by all fifty states and the District of Columbia. It utilizes a responsive system that connects states with each other and federal government agencies during governor-declared emergencies, allowing them to request and send personnel, equipment, and other resources to the site of disasters.
Emergency response system A formal or informal organization covering a specified geographic area minimally composed of health care institutions, public health agencies, emergency management agencies, and emergency medical service providers to facilitate regional preparedness planning and response.
EMS (emergency medical services) The full spectrum of emergency care from recognition of the emergency, telephone access of the system, provision of prehospital care, through definitive care in the hospital. It often also includes medical response to disasters, planning for and provision of medical coverage at mass gatherings, and interfacility transfers of patients. However, for the purposes of this document, the definition of EMS is limited to the more traditional, colloquial meaning: prehospital health care for patients with real or perceived emergencies from the time point of emergency telephone access until arrival and transfer of care to the hospital.
Health care coalition A group of individual health care assets (e.g., hospitals, clinics, long-term care facilities, etc.) in a specified geographic location that have partnered to respond to emergencies in a coordinated manner. The coalition has both a preparedness element and a response organization that possess appropriate structures, processes, and procedures. During response, the goals of the coalition are to facilitate
situational awareness, resource support, and coordination of incident management among the participating organizations.
Health care institution Any facility providing patient care. This includes acute care hospitals, community health centers, long-term care institutions, private practices, and skilled nursing facilities.
Health care practitioners Includes “health care professionals” and other nonlicensed individuals who are involved in the delivery of health care services.
Health care professionals Individuals who are licensed to provide health care services under state law.
Indicator Measurement or predictor that is used to recognize surge capacity and capability problems within the health care system, suggesting that crisis standards of care may become necessary and requiring further analysis or system actions to prevent overload.
Legal standard of care The minimum amount of care and skill that a health care practitioner must exercise in particular circumstances based on what a reasonable and prudent health care practitioner would do in similar circumstances; during nonemergencies and disasters, they are based on the specific situation.
Medical standard of care The type and level of medical care required by professional norms, professional requirements, and institutional objectives; these standards vary as circumstances change, including during emergencies or crisis events.
Memorandums of Understanding (MOUs) Voluntary agreements among agencies and/or jurisdictions for the purpose of providing mutual aid at the time of a disaster.
Mutual aid agreements (MAAs) Written instruments among agencies and/or jurisdictions in which they agree to assist one another on request by furnishing personnel and equipment. An “agreement” is generally more legally binding than an “understanding.”
Palliative care Care provided by an interdisciplinary team to prevent and relieve suffering and to support the best possible quality of life for patients and their families, regardless of the stage of the disease or the need for other therapies. Palliative care affirms life by supporting the patient and family’s goals for the future, including their hopes for cure or life prolongation, as well as their hopes for peace and dignity throughout the course of illness, the dying process, and death.
Protocol A written procedural approach to a specific problem or condition.
Public health system A complex network of individuals, organizations, and relevant critical infrastructures that have the potential to act individually and together to create conditions of health, including communities, health care delivery systems (e.g., home care, ambulatory care, private practice, hospitals, skilled nursing
facilities, and others), employers and business, the media, homeland security and public safety, academia, and the governmental public health infrastructure.
Region An organizational area defined for the purpose of efficiently coordinating, administering, and facilitating disaster preparedness, response, and recovery activities. The area is typically determined by geographic, jurisdictional, demographic, political, and/or functional service area boundaries. For example, it may be based on areas that are already established for activities conducted by public sector partners (e.g., federal, state, local, or tribal governments), such as existing regions defined by public health, emergency management, EMS, or law enforcement agencies, or for activities conducted by private sector partners, such as existing regions defined for delivering hospital and trauma care. The area may be within a state’s boundaries (i.e., an intrastate region), including spanning substate jurisdictional lines (e.g., county and city lines), may cross state boundaries (i.e., an interstate region), or may be a hybrid (e.g., adjacent counties in bordering states). These factors also may be used to help define the boundaries of health care coalitions.
Regional Disaster Medical Advisory Committee (RDMAC) A designated group of subject-matter experts that can homogenize state and local crisis care clinical guidance when the affected region encompasses areas across state lines. The RDMAC is necessary because state guidance alone may not address the specific needs of an area. While regional guidance can provide greater clarity on applying state guidance in local situations, it must not be inconsistent with it. The RDMAC can also serve as the coordinator of information and process improvement where appropriate. The state development and implementation templates, at the end of Chapter 5, describe planning and response roles for the RDMAC.
Resource sparing The process of maximizing the utility of supplies and material through conservation, substitution, reuse, adaptation, and reallocation.
Scope of practice The extent of a professional’s ability to provide health services pursuant to their competence and license, certification, privileges, or other lawful authority to practice.
SOFA score The Sequential Organ Failure Assessment (SOFA) score is a scoring system to determine the extent of a person’s organ function or rate of failure. The score is based on six different body systems: respiratory, cardiovascular, hepatic, hematopoietic, renal, and neurologic.
State Disaster Medical Advisory Committee (SDMAC) The dedicated body within a state that is responsible, in planning for or during an emergency, for providing clinical and other crisis standards of care (CSC) guidance when prolonged or widespread crisis care is necessary in order to maintain a consistent basis for life-sustaining resource allocation decisions. During a response, the SDMAC should draw on the expertise of its membership and that of other preidentified subject-matter experts to address ongoing issues as crisis care is implemented.
The SDMAC’s guidance should accompany other state declarations or invocations of emergency powers to empower and protect providers during their provision of crisis care. The state development and implementation templates, at the end of Chapter 5, describe planning and response roles for the SDMAC.
Triage The process of sorting patients and allocating aid on the basis of need for or likely benefit from medical treatment. Several types of triage are referenced in this report:
• Primary triage: The first triage of patients into the medical system (it may occur out of hospital), at which point patients are assigned an acuity level based on the severity of their illness/disease.
• Secondary triage: Reevaluation of the patient’s condition after initial medical care. This may occur at the hospital following EMS interventions or after initial interventions in the emergency department. This often involves the decision to admit the patient to the hospital.
• Tertiary triage: Further reevaluation of the patients’ response to treatment after further interventions; this is ongoing during their hospital stay. This is the least practiced and least well-defined type of triage.
Triage team Appointed by the clinical care committee, uses decision tools appropriate to the event and resource being triaged, making tertiary triage using scarce resource allocation decisions. This is similar in concept to triage teams established to evaluate incoming patients to the emergency department requiring primary or secondary triage, usually in a sudden-onset, no-notice disaster event (e.g., explosive detonation).
Trigger Evidence that austere conditions prevail so that crisis standard of care practices will be required. This may occur at an institutional, and often regional, level of response. It suggests the need for the immediate implementation of response pathways that are required to manage a crisis surge response emanating from the disaster situation.
Volume 7 B: Hospital Emergency Operations Plan Crisis Standard of Care Annex1
Policy #:
Date of Adoption:
Activation:
A disaster has occurred that overwhelms the hospital. Resources are inadequate to provide a usual standard of care. Resources are not rapidly available and systematic adaptations must be made to provide the best care possible under the circumstances. Examples may include
• Capacity is overwhelmed and patient care is being provided on cots within the institution
• ICU capacity is overwhelmed due to a pandemic or other event which is not amenable to patient transfer or resource importation
• Burn unit capacity is overwhelmed due to a massive fire/blast event
Notifications:
• Hospital Incident Commander (IC) will notify Regional Hospital Coalition (RHC) and local public health (LPH) of situation and attempt to obtain needed resources—this may include needed supplies, staff, or assistance with patient movement or evacuation to re-balance the standard of care in the area:
o RHC 24/7 phone
o LPH 24/7 phone (or emergency management, depending on availability of LPH)
_________________
1 This template is designed to provide an example of structure of a sample hospital annex to their Emergency Operations Plan which may be used as a discussion document with institutional stakeholders. The plan must be customized to the specifics of the facility and the process for interagency coordination including with local, regional, and state entities.
• If needs cannot be met in the region LPH will
o Notify State Department of Health and/or State Emergency Management.
o Work with RHC to notify other hospitals and healthcare facilities in the regional hospital coalition of a need to activate Crisis Standard of Care plans.
o Notify jurisdictional emergency management and public health of the situation via their metropolitan area coordinators.
o Establish a Multi-Agency Coordination Group including the above agencies and including participating in a Joint Public Information Center to communicate the situation to the public.
Actions:
1. Short-term strategies: Short-term strategies to increase healthcare facility capacity should have been implemented. Reference the Surge Capacity Template of the Surge Capacity Annex. Short-term measures usually do not require a systematic assessment of the standard of care being provided, particularly when they are designed to cope with resource shortages that will be quickly addressed (e.g., within hours to days).
Triage: In the early (reactive) phases of an event triage should be carried out by experienced clinicians (emergency medicine, surgery, etc.) according to the demands of the situation. The IC should be aware of these activities and gather information on what can be done to rebalance resources to needs. In an ongoing event, where the resources will not be available, more proactive (and structured) triage strategies may be needed that will require more of an institutional/regional approach. See long-term strategies below.
The IC, in consultation with appropriate technical specialists and the medical care branch director (critical care, nursing, respiratory care, other sources of specific information), may recommend strategies such as (many of these elaborated in the surge capacity annex to the emergency operations plan)
• Rapid discharge of emergency department and outpatients that can safely continue their care at home.
• Rapid assessment and early discharge of inpatients (surge discharge).
• Transfer of patients to alternate facilities (if they are available)—these may be permanent (longterm care facility) or temporary (alternate care site) locations, or usual health care facilities in an adjacent region/state.
• Cancellation of elective surgeries and procedures, with reassignment of surgical staff and space (e.g., postanesthesia care area, endoscopy suites).
• Reduction of usual use of imaging, laboratory testing, and other ancillary services.
• Expansion of critical care capacity by placing select ventilated patients on monitored/stepdown beds, using pulse oximetry (with high/low rate alarms) in lieu of cardiac monitors, or relying on ventilator alarms (which should alert for disconnect, high pressure, and apnea) for ventilated patients, with spot oximetry checks.
• Call-in of appropriate staff.
• Changes in staff scheduling—may elect to change duration of shifts or alter staffing ratios—however, longer shift duration during an infectious event may be detrimental to staff who may not adhere to protective equipment (e.g., N95 masks, barrier precautions) recommendations when fatigued, or changes in staff assignments (all nurse educators work clinical shifts, etc.).
• Changes in documentation requirements and release from administrative, teaching, and other responsibilities.
• Request for supplemental staff from partner hospitals, clinics (refer to Human Resources disaster credentialing policies and hospital coalition agreements).
• Conversion of single rooms to double rooms or double rooms to triple rooms if possible.
• Designation of wards or areas of the facility that can be converted to negative pressure/isolated from rest of ventilation system for cohorting contagious patients.
• Use of cots and beds in flat-space areas (classrooms, gymnasiums, lobbies) within the hospital for noncritical patient care.
• Communication with staff and public, educate staff about specifics of event and provide just-intime training on specialty patient care (e.g., burns, highly contagious infections, toxic exposures).
• Develop web-based modes of communication and education for staff.
• Provision of behavioral health support for patients and family members.
• Provision of staff support including feeding, behavioral health support, family/pet support and access to supplies (gas, groceries, etc.).
2. Long-term strategies: These are usually employed in a >24h incident which will continue to require a crisis standard of care due to pervasive region-wide demands on resources. Appropriate state declarations should occur to facilitate responses and protect responders. Planning cycles will be implemented by the incident commander. Strategies may include
• Staffing: in addition to usual staff sharing, medical reserve corps, local American Red Cross, public health, public works, schools, or other agencies and state/federal staff may be used as needed.
o Determine need for nonemployee assistance in the facility (provision of non-medical responsibilities, supervision by hospital staff “mentor,” etc.).
o Determine a preference list of providers (e.g., hospital staff first, followed by local hospital staff followed by clinic staff, out-of-state licensed staff, retired staff, medical reserve corps, trainees, non-health care organization staff, and patient family members (e.g., military, Community Emergency Response Team [CERT] members), lay volunteers) that might assist the facility during an event.
o Determine need to use family members to provide patient care/feeding duties.
• Facilitation of home-based care for a larger proportion of patients in cooperation with public health and home care agencies.
• Establish mobile or temporary evaluation and treatment facilities in the community to supplement usual clinic locations. These locations may also be used to screen those with mild symptoms when
medications (e.g., antivirals) are available and must be taken early in the course of illness to be effective.
• Establish guidelines and public messaging directing potential patients how to evaluate symptoms and care for themselves at home, indications for seeking medical evaluation and treatment, whether evaluation and treatment for some conditions can safely be delayed, and locations of available care.
• Close coordination with the Regional Hospital Coalition, Local Public Health, EMS, and emergency management is critical to assure that consistent care is provided within the area.
At this point, the Incident Commander (IC) must incorporate a structured assessment of hospital services and resources for each operational period as part of the Incident Action Plan. The IC should examine the administrative and clinical adaptations needed based on the demands of the event. Administrative, rather than clinical adaptations should be emphasized until no longer possible (e.g., the risk to the patient should be kept to the minimum required given the challenges/demand) (Figure B-1).
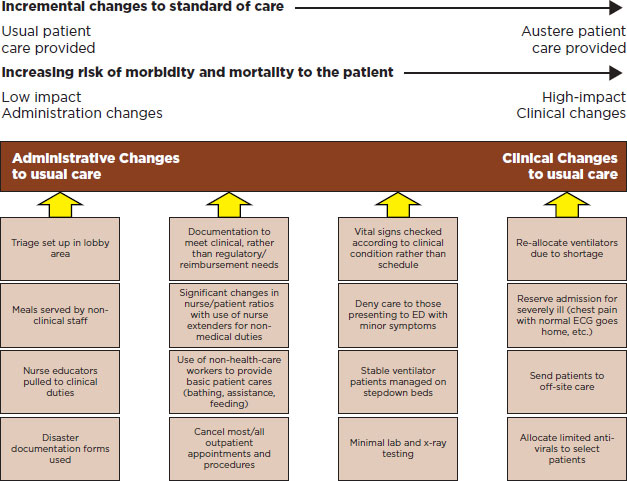
FIGURE B-1
Changes to usual care in relation to demand/severity of effect (from AHRQ—providing mass medical care with scarce resources 2006).
Process for adopting proactive (structured) Crisis Standard of Care:
1. Incident commander (IC) recognizes that systematic clinical changes will be required over days to allocate scarce resources to those most likely to benefit.
2. Planning chief gathers any guidelines, epidemiologic information, resource information, and regional hospital information and schedules meeting or conference call with IC, Medical Care Branch Director, and designees to clinical care committee.
3. Clinical care committee is convened by IC—membership may vary depending on event (full committee may not be required in some situations—technical specialists may be the only members necessary to resolve specific issues or may be added to the committee per IC discretion):
a. Hospital administrator
b. Medical director (Medical Care Branch Director)
c. Hospital attorney (if possible)
d. Critical care
e. Emergency medicine
f. Pediatrics
g. Nursing supervisor
h. Respiratory care supervisor
i. Chair of hospital ethics committee
j. Community representative (if possible—similar to Institutional Review Board role)
k. Ambulatory care (clinics) representative
l. Other—may include lab, radiology, bioelectronics, pharmacy, technical expertise specific to event (infection control, infectious diseases, maternal health/OB, toxicology, radiation safety, pediatrics, burn surgery, etc.)
4. Clinical care committee reviews situation, outside guidance, and regional/state hospital efforts and determines
a. Methods to meet patient care needs (for example, use of noninvasive ventilation techniques, changes in med administration techniques, use of oral medications and fluids instead of intravenous, etc.). These will generally be of limited value in correcting large demand/resource deficits, however. Use pre-event scarce resource guidance (see Minnesota Department of Health scarce resources recommendations) and adapt for the specifics of the event.
b. Additional changes in staff responsibilities to allow specialized staff to redistribute workload (for example, floor nurses provide basic ICU patient care while critical care nurses supervises these nurses and their patients) or would incorporate other health care providers, lay providers, or family members.
c. Mechanism for reassessment of local and regional hospital efforts and strategies (e.g., assignment of liaison officer and establishment of regular communications loop with state/regional multiagency coordination [MAC] groups).
d. Mechanism to summarize recommendations and changes and circulate to all staff and patients/ families (concrete guidelines are important to provide clarity and reduce decision making based upon emotional or subjective factors).
5. Assure that appropriate state declarations have been made, state department of health is aware of situation requiring proactive triage, and any appropriate provider protections have been invoked by the state.
6. Committee reviews options for
a. Location of care (triage of patients to critical care, floor care, off-site care, home based on disease severity).
b. Assignment of resources (which patients will receive resources in limited supply—ventilators, antitoxin, etc., or which will not be offered such interventions when there are competing demands).
7. Committee summarizes recommendations for care for next operational period and determines meeting and review cycles for subsequent periods (e.g., daily meeting, twice daily conference call, etc.) assuring that regional efforts at the MAC level or RHC level are integrated into facility process/timelines.
8. Incident commander approves recommendations and integration into Incident Action Plan. Section chiefs and Command Staff briefed and PIO assures communications to all staff.
9. Information is disseminated to inpatient services, outpatient services, RHC.
Re-allocation of ventilators or critical care resources:
In select situations (pandemic, for example) triage decisions about access to specific, life-critical resources may have to be made when there are not enough devices to accommodate demand. Consideration should be given to whether there is any ability to temporize (bag-valve manual ventilation, for example) until the excess demand passes. Should ongoing triage be necessary, continue with steps below:
1. Current inpatients, patients presenting to the hospital, and their family members are given verbal and printed information (ED patients by the triage nurse in the ED with reinforcement by medical staff, inpatients by their primary nurse or physician) explaining the situation and that resources may have to be reallocated, even once assigned, in order to provide the care to those that will most benefit. A contact point (phone extension) for responding to patient/family questions and concerns should also be included, as should spiritual support contact information.
2. Access controls should be implemented. Consider single entrance to hospital with metal detectors and community law enforcement support.
3. Assure behavioral health branch director planning for staff and patient needs and appoint palliative care unit leader if needed.
4. Clinical care committee should review available guidance and modify according to current knowledge of the specific disease state to provide decision tool for triage team. Triage team membership
should be agreed upon by team. Data collection and decision process should be reviewed and any necessary templates developed.
5. Triage plan for each operational period:
a. Emergency department/Outpatient screening of patients (and denial of service to patients either too sick or too well to be benefited by evaluation / admission) based on current regional resources and regional/state health guidance as well as hospital resources.
b. Patient data—ICU and other affected units will supply data to the triage team as requested not less than daily (for example, laboratory values, vital signs, medication drip information) using template supplied by clinical care committee.
c. Tertiary triage team—Two critical care physicians or one critical care and one infectious disease consider ventilator and other resource allocation decisions acting on data supplied by units/ teams in concordance with decision tool.
i. When two patients have essentially equal levels of illness/prognosis, a “first-come, first-served” policy should be used.
ii. When, according to guidelines or the triage team’s clinical experience, the prognosis is clearly not equal, the patient with a substantially more favorable prognosis shall receive the resource.
iii. The triage team should ask for and receive whatever patient information is necessary to make a decision but should NOT consider subjective assessments of the quality of the patient’s life or value to society and in fact, should ideally be blinded to such information when possible. The treating physician should assure that the patient/family wishes to use the resources if they are available prior to asking the triage team for an opinion.
iv. Triage team should make recommendations to the inpatient division supervisor and document decision making on worksheets and in the patient’s medical record accounting for the decision.
v. Prior to any removal of resources, the bedside caregivers shall assure that no major improvement in clinical condition has occurred since the triage team received their data and notify the team if this has occurred.
6. The inpatient division supervisor should monitor and make final decisions on bed assignments. This individual should have access to
a. ED and other outpatients waiting for beds (both floor and critical care units).
b. Inpatient bed status including pending transfers into/out of critical care areas.
c. Clinical status of patients by unit (improving—able or anticipated to move to floor status or discharge, worsening—may require critical care or may not be eligible for continued treatment). (This requires ongoing contact between the division supervisor and the clinical units to assure that information is up to date and accurate so that good decisions can be made. The inpatient division supervisor will work closely with the Triage Team to determine the best use of beds available.)
7. The process and rationale for resource assignment should be provided to the treating physician and family:
a. Grounds for the decision.
b. An appeals process that allows a period of time (appropriate to the intervention being allocated—for ventilators 15 minutes) for treating physician or family to request reconsideration of the decision if there is objective information available that that patient’s prognosis is more favorable than determined by the triage team based on improving data since the data was last supplied to the triage team.
c. The resource allocation protocol and decisions should be reviewed by the clinical care committee and additional oversight physicians at set periods (e.g., every 24-48 hours) and as needed to assure the best evidence available is being used and that the decisions and the system are operating justly.
8. Palliative care—specific plans for continuation of symptomatic care should be included in guidance to the units, and the inpatient division supervisor will monitor and provide assistance as required.
9. A regional triage team may be utilized according to plans of the RHC in which case the clinical care committee will work with the RHC and any regional medical advisory team (RMAT) to assure continuity with hospital operational plans.
See also: MDH guidance for providing clinical care in resource-scarce situations including ventilator triage criteria (http://www.health.state.mn.us/oep/healthcare/standards.pdf ), the Institute of Medicine report Guidance for Establishing Crisis Standards of Care for Use in Disaster Situations: A Letter Report 2009, and AHRQ’s Providing Mass Medical Care with Scarce Resources 2006.
Volume 7 C: Potentially Scarce Medical Resources by Category
| Category | Specific Resources | Notes |
| Ventilators and components | Staff, circuits, machines | Including adaptive methods such as some anesthesia machines, BiPAP, etc. |
| Extracorporeal membrane oxygenation (ECMO) | Equipment and access catheters, staff | Knowledge of regional capacity for ECMO may be helpful. |
| Oxygen and oxygen delivery devices | Cannulas, masks, bag-valve devices (including pediatric sizes) | Knowledge of hospital system capacity and maximum flow deliveries is helpful in planning. |
| Vascular access devices | Peripheral and central, including pediatric sizes | |
| Intensive care unit | Beds, monitors, pumps, etc. | May use oxygen saturation monitors with high/low rate alarms as surrogate monitoring for tachy/brady dysrhythmias. |
| Health care providers | Particularly emergency medicine, critical care, burn, and surgical/anesthesia staff (nurses and physicians) and respiratory therapistsa | Hospital staff, coalition, regional/state/federal teams.b,c,d,e Must include credentialing/privilegingf and orientation/mentoring as well as accommodations and the management of “volunteer” medical providers that present to the facility.g |
| Hospitals | Due to infrastructure damage or compromise from access problems (flooding, etc.) or failure of critical systems or utilities (oxygen, power, potable water) | Regional coalitions are critical. Temporary field hospitals can provide support, especially in areas with limited healthcare infrastructure. |
| Specialty medications or intravenous fluids | Sedatives/analgesics, sodium bicarbonate, specific antibiotics, antivirals, inotropes, standard intravenous fluids, chemical antidotes (e.g., atropine),h etc. | Intravenous fluid needs can be substantial (e.g., 70 kg patient with 50% burn patient requires 14 liters of fluid in first 24h, thus 10 patients require 140 liters). |
| Blood products | Packed red cells, platelets, fresh frozen plasma Unusual to have regional shortages during disasters, though locally may be limited after a disaster due to access problems.i |
| Renal replacement therapy | Dialysis catheters, water purifiers, dialysis machines | Partnership with hospital and community dialysis providers is encouraged as dialysis networks have robust disaster plans. |
| Surgical equipment | Procedure trays, orthopedic equipment, chest tube and suture trays | May need very large numbers of suture trays, including at alternate care sites. |
| Wound/burn care supplies | Tourniquets, splinting materials, dressings, including burn dressings and wound dressings | Inexpensive, and a priority for MCI preparedness. |
| Medical transportation | Advanced and basic life support ambulances, rotor-wing, fixed wing, wheelchair and ambulatory patient (bus, etc.) transport | Coordination with local EMS and emergency management is critical to establish available resources and coordinate during an incident |
NOTE: BiPAP = bilevel positive airway pressure ventilator; EMS = emergency medical services; MCI = mass casualty incident.
a IOM (Institute of Medicine). 2009. Guidance for Establishing Crisis Standards of Care for Use in Disaster Situations: Letter Report. Washington, DC: The National Academies Press.
b National Disaster Medical System. 2012. Department of Health and Human Services website. http://ndms.dhhs.gov (accessed May 22, 2006).
c HHS (Department of Health and Human Services). 2012. Medical Reserve Corps website. http://www.medicalreservecorps.gov (accessed January 16, 2004).
d Schultz, C. H., and S. J. Stratton. 2007. Improving hospital surge capacity: A new concept for emergency credentialing of volunteers. Annals of Emergency Medicine 49:602-609.
e HHS (Department of Health and Human Services). 2001. The emergency system for advance registration of volunteer health professionals. Washington, DC: HHS, http://www.phe.gov/esarvhp/pages/default.aspx (accessed February 13, 2012).
f Comprehensive Accreditation Manual for Hospitals. 2003. Medical Staff Section MS.5.14.4.1. Disaster Privileging Standard. Oakbrook Terrace, IL: Joint Commission on Accreditation of Healthcare Organizations.
g Cone, D. C., S. D. Weir, and S. Bogucki. 2003. Convergent volunteerism. Annals of Emergency Medicine 41:457-462.
h Kozak, R. J., S. Siegel, and J. Kuzma. 2003. Rapid atropine synthesis for the treatment of massive nerve agent exposure. Annals of Emergency Medicine 41(5):685-688.
i Schmidt, P. J. 2002. Blood and disaster-supply and demand. New England Journal of Medicine 346(8):617-620.
SOURCE: Koenig, K. L., et al. 2011. Crisis standard of care: Refocusing health care goals during catastrophic disasters and emergencies. Journal of Experimental and Clinical Medicine 3(4):159-165. Hick, J. L., D. Hanfling, and S. V. Cantrill. 2011. Allocating scarce resources in disasters: emergency department principles. Annals of Emergency Medicine published online August 22; IOM (Institute of Medicine). 2009. Guidance for Establishing Crisis Standards of Care for Use in Disaster Situations: Letter Report. Washington, DC: The National Academies Press. For more detailed information, see Minnesota Healthcare System Preparedness Program. 2011. Patient Care Strategies for Scarce Resource Situations. St. Paul, MN: Minnesota Department of Health, http://www.health.state.mn.us/oep/healthcare/standards.pdf (accessed February 13, 2012).
| Specific Challenges | Space/Staff/Supply Considerations | Triage Issues | |
| Chemical |
• Mass airway management and ventilatory therapy • Antidotal treatment (atropine, pralidoxime particularly) • Mass decontaminationa |
• Intubation equipment • Antidotes (onsite and community/ SNS) (SNS weblink) • Critical care equipment • “Dry decontamination“ kits (redressing kits) • Chemical PPE and HAZMAT training for staffb |
• Temporizing (bag-valve, other) therapies reasonable while awaiting outside resources • May still have good outcomes in cardiac arrest in organophosphate poisoning, but in mass casualty situation may have to prioritize care to those prior to respiratory arrestc |
| Pandemic |
• PPE use and type required • Vaccine, antiviral, antibiotic supply and use • Critical care capacity • Outpatient care capacity • Alternate care site establishment (early treatment—flu centers, also hospital overflow) • Mechanical ventilation capacity • ECMO criteria and capacity |
• PPE supplies, particularly N95 masks if required • Medications including antivirals, antibiotics, analgesics, paralytics • Outpatient care and inpatient care spaces may be insufficient and require alternate care sites • Ventilators, ECMO supplies, and equipment and staffing plans • Staff illness, family obligations, or reluctance to report may contribute to difficulty with adequate staffingd,e |
• Contingency plans for PPE and medication shortages • Outpatient referral/triage plans (hotlines, phone prescribing, etc.) • Triage criteria and process for life-saving interventions • Triage criteria for emergency care (vs. referral to "flu center" or similar location) |
| Pediatric mass casualty |
• Age-specific sizes of equipment, airway, intravenous access, catheters, operative equipmentf,g • Educational background often acking for pediatric-specific resuscitation and management |
• All facilities should be prepared to stabilize and initially treat pediatric patients • Community plan should concentrate critical patients and those 5 yrs or ess at pediatric facilitiesh • Just-in-time education for staff, initial treatment resources • Consider pediatric technica expert availability (telemedicine or telephone consult—preferably to experts outside affected area) to facilities that have to manage patients out of their usual range of expertise • Facility should plan for managing unaccompanied children (including once medically cleared) and their needs for support |
• Trauma care—see below • Assessment may be difficult due to verbal skills and fear • Physiologic compensation may mask "usual" signs of shock until advanced • EMS triage procedures should emphasize keeping families together when possible (e.g., critically injured child to pediatric center along with parents with minor injuries) |
| Trauma |
Triagei bottlenecks
• Airway and initial interventions • CT and imaging bottlenecksj • Operative bottlenecks • Surgical and trauma supplies |
• All hospitals should be prepared to manage trauma patients and stock adequate supplies according to their role in the community • Consider caching operative supplies (especially major procedure, chest tube, orthopedic trays) • Selective use of CT and other imaging—plan and exercise |
• Basic trauma triage, including knowledge of impact of GCS, age, and multisystem trauma on prognosis • Provide palliative care to those who cannot be offered definitive nterventions • The larger the event, the higher the concentration on targeted, brief interventions with high impact (hemorrhage control, pneumothorax decompression, airway management)k • Limit definitive imaging and procedures (e.g., for example, limit CT to cranial for decreased level of consciousness, perform bailout surgical procedures with temporary closures) • Ultrasound may contribute to rapid assessments of casualtiesl,m,n |
| Burn |
• Lack of burn beds and burn centers • Educational background often acking for burn resuscitation and management • Intravenous fluids, dressings, and analgesics limited • Limited number of burn surgeons and nurseso |
• Burn centers should stock supplies for large-scale burn incidents, ncluding adequate analgesia • All facilities should be prepared to stabilize and initially treat burn patients • Community plan should concentrate critical burns at burn centers (may nvolve redistributing other patient groups) • Just-in-time education for staff • Consider burn technical expert availability (telemedicine or telephone consult—consider experts from another unaffected area) to facilities that have to manage patients out of their usual range of expertise |
• Use knowledge of contributing injuries, inhalational injury, age, and extent of burns when triaging burn patientsp • Provide palliative care to those who cannot be offered definitive nterventions • Provide temporizing measures such as escharotomy and airway management while deferring formal burn dressings initially in favor of sterile sheets and towels |
| Blast/crusl |
• Triage—education on blast/crush njuries may be lacking q • Intravenous fluids and medications may be limited • Surgical bottlenecks Dialysis capacity may be challenged, especially if nfrastructure damaged in community |
• Cache common medications (sodium bicarbonate, narcotic analgesia, antibiotics) needed for blast/crush njuries • Cache equipment such as tourniquets, major procedure trays, external fixators and ortho trays, additional suture trays, ocular trays, ENT trays • Just-in-time education on crush njury and other specific syndromesr • Activate necessary community (and national, if needed) dialysis capacity for event |
• Triage based on knowledge of injuries, contributing underlying disease and age—for blast injuries multiple extremity injuries and low GCS are correlated with poor outcomess,t,u • Assess carefully for subtle penetrating injury and compartment syndrome • Provide temporizing treatments such as hemorrhage contro (including tourniquets when tissue destruction is significant) and analgesia initially |
| Specific Challenges | Space/Staff/Supply Considerations | Triage Issues | |
| Nuclear* |
• Overwhelming acute trauma for hospitals near incident • Overwhelming numbers of acute radiation syndrome (ARS) casualties in subsequent days/ weeksyv • Identification/categorization of ARS casualtieswdifficulty accessing lab testing or results • Shortages of cytokines and blood products (especially platelets during bone marrow failure phase) • Large number of expectant patients from initial trauma, radiation, or combined injuryx |
• Plan with community according to hazard vulnerability for overal response, including evacuation of patients in latent phase of ARS to other jurisdictions with intact nfrastructurey • Identify areas for alternate ambulatory triage sites • Identify equipment for triage areas (tourniquets, bandages early, later antiemetics and antidiarrheals) • Identify sources of radiation illness nformation,z,aa cytokines, other supplies |
• Triage for injured is according to usual trauma prioritiesbb • Vomiting in early hours is non-specific and can be due to many causescc • Use of Absolute Lymphocyte Count (ALC) is optimal for assessment of ARS, but may not be easily availabledd • Victim information (proximity, particulate debris) and symptoms can allow rough classification within a few days after the eventee • All forms of triage likely to be needed with more proactive processes and guidance the farther out from the event both temporally and geographically |
*Note that this section does NOT apply toa radiological dispersal device(RDD) or “dirty bomb,” which should not result in significant radiation illness/injury—see blast section above. Also does not apply to a nuclear plant mishap, which should not tax hospital resources. Both of these situations may require community screening centers and potentiallya mass screening and/or decontamination response on the part of the hospital, but this would mainly be to prevent low-level contamination and reassure patients. REMM(Radiation Emergency Medical Management). 2012. Guidance on diagnosis & treatment for health care providers: download REMM to your computer. Washington, DC: HHS(Department of Health and Human Services), http://www.remm.nlm.gov/download.htm (accessed March 6, 2012); Christodouleas, J. P., R. D. Forrest, C. G. Ainsley, Z. Tochner, S. M. Hahn, and E. Glatstein. 2011. Short-term and long-term health risks of nuclear-power-plant accidents. New England Journal of Medicine 364:2334-2341.
a Macintyre, A. G., G. W. Christopher, E. Eitzen, et al. 2000. Weapons of mass destruction events with contaminated casualties: Effective planning for healthcare facilities. Journal of the American Medical Association 4:261-269.
b OSHA(Occupational Safety and Health Administration). 2005. OSHA best practices for hospital-based first receivers of victims from mass casualty incidents involving the release of hazardous substances. http://www.osha.gov/dts/osha/bestpractices/firstreceivers_hospital.pdf (accessed September 21, 2007).
c Okumura, T., K. Suzuki, A. Fukada et al. 1998. The Tokyo subway sarin attack: Disaster management, part 2: Healthcare facility response. Academic Emergency Medicine 5:618-624.
d Chaffee, M. 2009. Willingness of health care personnel to work ina disaster: An integrative review of the literature. Disaster Medicine and Public Health Preparedness 3(1):42-56.
e Lanzilotti, S. S., D. Galanis, N. Leoni, and B. Craig. 2002. Hawaii medical professionals assessment. Hawaii Medical Journal 61(8):162-173.
f Committee on Pediatric Emergency Medicine. 2007. Preparation for emergencies in the offices of pediatricians and pediatric primary care providers. Pediatrics 120(1):200-212. http://pediatrics.aappublications.org/cgi/reprint/120/1/200 (accessed February 25, 2011).
g Gausche-Hill, M., C. Schmitz, and R. J. Lewis. 2007. Pediatric preparedness of U.S. emergency departments: A 2003 survey. Pediatrics 120:1229-1237.
h Kanter, R. K. 2007. Strategies to improve pediatric disaster surge response: Potential mortality reduction and tradeoffs. Critical Care Medicine 35(12):2837-2842.
i Frykberg, E. K. 2005. Triage, principles and practice. Scandinavian Journal of Surgery 94:272-278.
j Einav, S., L. Aharonson-Daniel, C. Weissman et al. 2006. In-hospital resource utilization during multiple casualty incidents. Annals of Surgery 243:533-540.
k U.S. Army Institute of Surgical Research. 2009. Tactical combat casualty care guidelines. Houston, TX: U.S. Army Institute of Surgical Research. http://www.usaisr.amedd.army.mil/tccc/TCCC%20Guidelines%20091104.pdf (accessed February 25, 2011).
l Lee, B. C., E. L. Ormsby, J. P. McGahan, G. M. Melendres, and J. R. Richards. 2007. The utility of sonography for the triage of blunt abdominal trauma patients to exploratory laparotomy. American Journal of Roentgenology 188(2):415-421.
m Ma, O. J., and J. R. Mateer. 1997. Trauma ultrasound examination versus chest radiography in the detection of hemothorax. Annals of Emergency Medicine 29(3):312-315; discussion 5-6.
n Ma, O. J., J. G. Norvell, and S. Subramanian. 2007. Ultrasound applications in mass casualties and extreme environments. Critical Care Medicine 35(5 Suppl):S275-S279.
o Posner, Z., H. Admi, and N. Menashe. 2003. Ten-fold expansion ofa burn unit in mass casualty: How to recruit the nursing staff. Disaster Management & Response 1(4):100–104.
p Saffle, J. R., N. Gibran, and M. Jordan. 2005. Defining the ratio of outcomes to resources for triage of burn patients in mass casualties. Journal of Burn Care Rehabilitation 26(6):478–482.
q Kluger, Y., K. Peleg, L. Daniel-Aharonson, and A. Mayo. 2004. The special injury pattern in terrorist bombings. Journal of the American College of Surgeons 199:875-879.
r Sever, M. S., R. Vanholder, and N. Lameire. 2006. Management of crush-related injuries after disasters. New England Journal of Medicine 354(10):1052–1063.
s Frykberg, E. R. 2002. Medical management of disasters and mass casualties from terrorist bombings: How can we cope? Journal of Trauma and Acute Care Surgery 53:201-212.
t Peleg, K., L. Aharonson-Daniel, M. Stein et al. 2004. Gunshot and explosion injuries: Characteristics, outcomes, and implications for care of terror-related injuries in Israel. Annals of Surgery 239:311-318.
u Borden Institute, Walter Reed Army Medical Center. 2004. Triage. In Emergency war surgery, 3rd ed. Washington, DC: U.S. Department of Defense. Pp. 3.1-3.17.
v Hick, J. L., D. M. Weinstock, C. N. Coleman, D. Hanfling, S. Cantrill, I. Redlener, J. L. Bader, P. Murrain-Hill, and A. R. Knebel. 2011. Health care system planning for and response toa nuclear detonation. Disaster Medicine and Public Health Preparedness 5(Suppl 1):S73-S88.
w DiCarlo, A. L., C. Maher, J. L. Hick, D. Hanfling, N. Dainiak, N. Chao, J. L. Bader, C. N. Coleman, and D. M. Weinstock. 2011. Radiation injury aftera nuclear detonation: Medical consequences and the need for scarce resources allocation. Disaster Medicine and Public Health Preparedness 5(Suppl 1):S32-S44.
x Hirsch, E. F. 1990. The status of combined injuries. In Treatment of Radiation Injuries, edited by D. Browne. New York: Plenum Press.
y DHS(Department of Homeland Security). 2009. Planning guidance for response toa nuclear detonation. http://www.afrri.usuhs.mil/outreach/pdf/planning-guidance.pdf (accessed September 9, 2009).
z Waselenko, J. K., T. J. MacVittie, W. F. Blakely, N. Pesik, A. L. Wiley, W. E. Dickerson, H. Tsu, D. L. Confer, C. N. Coleman, T. Seed, P. Lowry, J. O. Armitage, and N. Dainiak. 2004. Medical management of the acute radiation syndrome: Recommendations of the Strategic National Stockpile Radiation Working Group. Annals of Internal Medicine 140(12):1037–1051.
aa National Library of Medicine. 2011. Radiation emergency medical management(REMM) Web site. http://www.remm.nlm.gov/ (accessed February 25, 2011).
bb Hick, J. L., D. M. Weinstock, C. N. Coleman, D. Hanfling, S. Cantrill, I. Redlener, J. L. Bader, P. Murrain-Hill, and A. R. Knebel. 2011. Health care system planning for and response toa nuclear detonation. Disaster Medicine and Public Health Preparedness 5:S73-S88.
cc Demidenko, E., B. B. Williams, and H. M. Swartz. 2009. Radiation dose prediction using data on time to emesis in the case of nuclear terrorism. Radiation Research 171:310-319.
dd DiCarlo, A. L., C. Maher, J. L. Hick, D. Hanfling, N. Dainiak, N. Chao, J. L. Bader, C. N. Coleman, and D. M. Weinstock. 2011. Radiation injury after a nuclear detonation: Medical consequences and the need for scarce resources allocation. Disaster Medicine and Public Health Preparedness 5(Suppl 1):S32-S44.
ee Coleman, C. N., R. Casagrande, J. L. Hick et al. 2011. Triage and treatment tools for use ina scarce resources-crisis standards of care setting followinga nuclear detonation. Disaster Medicine and Public Health Preparedness 5(Suppl 1):S111-S121.
In response to a request from the HHS Office of the Assistant Secretary for Preparedness and Response, the Institute of Medicine will convene an ad hoc committee to conduct a phase-two activity on standards of care for use in disaster situations. The committee will focus attention on developing guidance to establish standards of care that should apply to disaster situations—both naturally occurring and man-made—where there are scarce resources. Ethical principles will be incorporated into the standards.
PHASE 2
In September 2009 the Institute of Medicine released Guidance for Establishing Crisis Standards of Care for Use in Disaster Situations: A Letter Report. Building on this letter report the committee will reconvene to conduct a study and issue a report, which will serve as the second phase of this project. The committee is expected to come forward with conclusions and recommendations it determines are necessary and justified based on its analysis. Specifically the committee will
• Identify metrics to assess the development of crisis standards of care protocols by state and local governments, that include elements such as dissemination, development, and implementation.
• Review the impact of its 2009 letter report including progress made by state and local governments and health care organizations in establishing crisis standards of care guidance.
• Develop templates for states, emergency medical services (EMS) systems, hospitals, and individual clinicians to guide decision making when implementing crisis standards of care that can be easily read, understood and executed during an incident. These templates will
o Address the inclusion of all critical components of the emergency response and health care system necessary to plan for and respond to crisis standards of care situations.
o Examine the specific process of declaring a shift to crisis standards of care, focusing on roles and responsibilities of decision makers from the local to the national level, including
![]() The roles and responsibilities of public and private health care systems (e.g., the responsibility of a local VA Medical Center Director vs. regional Veterans Integrated Service Network [VISN] Director), authority and the role of military treatment facilities (MTFs), local, regional and national healthcare system clinical and administrative leadership in private health care systems;
The roles and responsibilities of public and private health care systems (e.g., the responsibility of a local VA Medical Center Director vs. regional Veterans Integrated Service Network [VISN] Director), authority and the role of military treatment facilities (MTFs), local, regional and national healthcare system clinical and administrative leadership in private health care systems;
![]() The role of state EMS authorities in providing medical oversight and coordination of a shift to crisis response for a state’s EMS system, including 911 dispatch and prehospital emergency medical care.
The role of state EMS authorities in providing medical oversight and coordination of a shift to crisis response for a state’s EMS system, including 911 dispatch and prehospital emergency medical care.
o Identify clinical and administrative indicators that govern the transition from conventional surge response and conventional standards of care to crisis surge response and crisis standards of care, and the return to conventional standards of care. Reference and highlight existing clinical protocols and related governance structures that need to be in place to facilitate decision making under crisis standards. These indicators, clinical protocols, and governance structures should be applicable to specific scenarios of both gradual onset as well as no notice incidents, and should pertain to the prehospital, community, and hospital settings.
o Define terms and provide consistent language (e.g., definitions, situational markers) for communicating across jurisdictions and levels of government the status of health care systems related to crisis standards of care.
In addition the committee will develop templates that can be used by state and local governments to guide community engagement. These would be based on a series of focus groups utilizing scenario-based engagement strategies to identify what shifts are tolerable from the community point of view, including the physician, active duty military, and veteran’s communities. In order to accomplish this, the IOM may establish a subcontract with an independent firm (e.g., Keystone Symposia, AmericaSpeaks, Harris Interactive) to assist in the design, organization, and execution of the meetings. The committee will provide the scientific and subject-matter expertise to the contractor to ensure the appropriate objectives are identified and met, e.g., the right questions are asked and the right populations are engaged in the process.
Volume 7 F: Committee Biographies
Lawrence O. Gostin, J.D., LL.D. (Hon.) (Chair), is an internationally acclaimed scholar in law and public health. He is associate dean (Research and Academic Programs) and the Linda D. and Timothy J. O’Neill Professor of Global Health Law at the Georgetown University Law Center, where he directs the O’Neill Institute for National and Global Health Law. Dean Gostin is also a professor of Public Health at the Johns Hopkins University and director of the Center for Law & the Public’s Health at Johns Hopkins and Georgetown Universities—a Collaborating Center of the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC). He is the health law and ethics editor, a contributing writer, and a columnist for the Journal of the American Medical Association. In 2007, the WHO Director General appointed Dean Gostin to the International Health Regulations Roster of Experts and the Expert Advisory Panel on Mental Health. Dean Gostin is a member of the Institute of Medicine (IOM)/National Academy of Sciences, and serves on the Board on Health Sciences Policy and the Committee on Science, Technology, and Law. He has previously chaired committees on health information privacy, genomics, and prisoner research. In the United Kingdom, he was the legal director of the National Association for Mental Health, director of the National Council of Civil Liberties (the U.K. equivalent of the American Civil Liberties Union), and a Fellow at Oxford University. He helped draft the current Mental Health Act (England and Wales) and brought several landmark cases before the European Commission and Court of Human Rights. Dean Gostin has led major U.S. law reform initiatives, including the drafting of the Model Emergency Health Powers Act to combat bioterrorism and the Turning Point Model State Public Health Act. He is also leading a drafting team on developing a Model Public Health Law for WHO.
Dan Hanfling, M.D. (Vice Chair), is special advisor to the Inova Health System in Falls Church, VA, on matters related to emergency preparedness and disaster response. He is a board-certified emergency physician practicing at Inova Fairfax Hospital, Northern Virginia’s Level I trauma center. He serves as an operational medical director for PHI Air Medical Group—Virginia, and has responsibilities as a medical team manager for Virginia Task Force One, an international urban search and rescue team sanctioned by FEMA and USAID. He has been involved in the response to numerous international and domestic disaster events. Dr. Hanfling was integrally involved in the management of the response to the anthrax bioterror mailings, when two cases of inhalational anthrax were successfully diagnosed at Inova Fairfax Hospital. He is clinical professor of Emergency Medicine at George Washington University, contributing scholar at the UPMC
Center for Biosecurity, and adjunct faculty of the George Mason University School of Public Policy, Office of International Medical Policy. Dr. Hanfling received an A.B. in Political Science from Duke University and an M.D. from Brown University. He completed an internship in Internal Medicine at the Miriam Hospital in Providence, RI, and an Emergency Medicine Residency at George Washington/Georgetown University Hospitals.
Damon T. Arnold, M.D., M.P.H., currently serves as the director for Graduate Studies in Public Health at Chicago State University in Illinois. He was the 16th director of the Illinois Department of Public Health from 2007 to 2011. Prior to his current position, Dr. Arnold was the medical director for bioterrorism and preparedness for the Chicago Department of Public Health. During his professional career, he also was medical director for St. Francis Hospital, Blue Island, IL; LTV Steel Company in Indiana; and Mercy Hospital and Medical Center, Chicago. He served in the Army National Guard for 25 years, holds the rank of colonel, and was the guard’s commander of the Joint Task Force Medical Command in Springfield and the Illinois State Surgeon. He had a distinguished military career and received many military awards, including the Legion of Merit, three Army Commendations, and two National Defense Service and Humanitarian Service medals. He has served missions to Iraq, Kuwait, Central America, South America, Africa, and Europe, and participated in relief efforts for Hurricanes Katrina and Rita. He was the American Red Cross Military Hero of the Year for 2007. Dr. Arnold is the former chair of the Association of State and Territorial Health Officials (ASTHO) Preparedness Policy Committee, served as a board member for the American Red Cross of Greater Chicago, and served as the ASTHO Liaison Representative for the CDC Board of Scientific Counselors, Coordinating Office for Terrorism Preparedness and Emergency Response. Dr. Arnold also holds associate professorships at the University of Illinois School of Public Health, the University of Illinois Medical School, and the Southern Illinois Medical School. Dr. Arnold received his M.D. and M.P.H. from the University of Illinois, and has completed several law courses at DePaul University College of Law.
Stephen V. Cantrill, M.D., FACEP, is an emergency physician from Denver who recently retired from serving as the associate director of Emergency Medicine at Denver Health Medical Center for 18 years. He was also the director of the Colorado BNICE Weapons of Mass Destruction (WMD) Training Program at Denver Health for more than 5 years. Dr. Cantrill has lectured nationally and internationally on many topics, including weapons of mass destruction, disasters, and disaster management, and has been involved in disaster management education for more than two decades. He served as the regional medical coordinator for Denver’s participation in Operation TopOff 2000. He has also been involved in weapons of mass destruction training for Colorado and has participated in the planning for multiple mass-gathering events, including the Denver Papal visit and the Denver Summit of Eight world economic conference. He has testified at U.S. Senate Committee hearings on bioterrorism preparedness and was a member of the U.S. Department of Health and Human Services (HHS) National Biodefense Science Board for 4 years. He has recently served as the Principal Investigator on an Agency for Healthcare Research and Quality (AHRQ) regional surge capacity grant and the AHRQ HAvBED national bed availability project. He also served as Principal Investigator on the AHRQ disaster alternate care facility task order. Dr. Cantrill has authored more than 90 publications and has received multiple teaching and clinical excellence awards.
Brooke Courtney, J.D., M.P.H., is regulatory counsel in the Food and Drug Administration’s (FDA’s) Office of Counterterrorism and Emerging Threats. Ms. Courtney was previously director of the Office of Public Health Preparedness and Response at the Baltimore City Health Department, where she oversaw all emergency operations for the agency, coordinated the city’s healthcare coalition, and oversaw medical countermeasure (MCM) stockpiling and dispensing. She was an associate at the Center for Biosecurity, where she researched and published on hospital, public health, and legal preparedness issues and was associate editor of the peer-reviewed journal, Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science. Ms. Courtney has also worked at Pfizer, at the Maryland Health Care Commission, and on international disaster response at the American Red Cross. She is a term member of the Council on Foreign Relations, the 2010 recipient of the Public Health Law Association’s Emerging Leader in Public Health Law award, and lead author of the MCM chapter in Food and Drug Law and Regulation. She received her J.D. and Health Law Certificate from the University of Maryland Carey School of Law and was admitted to practice in the District of Columbia and Maryland. Her M.P.H. is from Yale University.
Asha Devereaux, M.D., M.P.H., is a pulmonary/critical care physician in private practice in Coronado, CA. Dr. Devereaux has 11 years of training and service with the U.S. Navy and formerly served as the Intensive Care Unit (ICU) director on the Isolation Unit of the USNS Mercy Hospital ship. She is currently a Steering Committee Member for the American College of Chest Physicians Disaster Response Network. Dr. Devereaux has spearheaded a national conference on disaster preparedness, has published on the topic, and now serves on the board of the American Lung Association in California and on the Board of Directors of the San Diego American Lung Association. Dr. Devereaux is president of the California Thoracic Society and lead physician advisor of the San Diego Medical Reserve Corps. Dr. Devereaux received her undergraduate education at the University of California, San Diego, followed by an M.D./M.P.H. from Tulane University.
Edward J. Gabriel, M.P.A., AEMT-P,1 is director, Global Crisis Management, for The Walt Disney Company, and is responsible for the development and implementation of global policy, planning, training, and exercises to manage crisis for The Walt Disney Company. He is also responsible for East and West Coast Medical and Emergency Medical Operations and the Walt Disney Studio’s Fire Department. He supports and collaborates with global business units in development and testing of resumption planning, and develops policies and strategies to manage crisis. Mr. Gabriel has been an emergency medical technician (EMT) since 1973 and is a 27-year paramedic veteran of New York City (NYC) Fire Department’s Emergency Medical Service (EMS). He rose through the ranks from EMT to paramedic through lieutenant and retired at the level of assistant chief/division commander. As deputy commissioner for Planning and Preparedness at the New York City Office of Emergency Management, he served as commissioner for all preparedness and planning-related projects and initiatives. During his role with NYC, he was a member of the Federal Bureau of Investigation/NYC Joint Terrorism Task Force, and still sits on the International Advisory Board of the Journal of Emergency Care, Rescue and Transportation. He has worked with the Joint Commission, sitting on the Emergency Preparedness Roundtable as well as the Community Linkages in Bioterrorism Preparedness
_________________
1 Resigned from the committee October 2011.
Expert Panel. He served as a member of the HHS Federal Contingency Medical Facility Working Group and the AHRQ Expert Panel on Mass Casualty Medical Care. Most recently he has worked with the HHS AHRQ expert panel as Principal Author of the prehospital chapter of Providing Mass Medical Care with Scarce Resource: Community Planning Guide. He also worked with the U.S. Department of Defense, General George C. Marshall School of International Studies Program on Terrorism and Security Studies, located in Garmisch-Partenkirchen, Germany, presenting on methodologies for planning and preparedness for international leaders. He is credentialed through the International Association of Emergency Managers as a Certified Emergency Manager and the Disaster Recovery Institute International as a Certified Business Continuity Professional. Mr. Gabriel continues to lecture nationally and internationally on crisis management, business continuity, emergency management, planning and preparedness, WMD, terrorism, and emergency medical topics. Mr. Gabriel holds a B.A. from the College of New Rochelle and an M.P.A. from Rutgers University.
John L. Hick, M.D., is a faculty emergency physician at Hennepin County Medical Center (HCMC) and an associate professor of Emergency Medicine at the University of Minnesota. He serves as the associate medical director for Hennepin County Emergency Medical Services and medical director for Emergency Preparedness at HCMC. He is medical advisor to the Minneapolis/St. Paul Metropolitan Medical Response System. He also serves the Minnesota Department of Health as the medical director for the Office of Emergency Preparedness and medical director for Hospital Bioterrorism Preparedness. He is the founder and past chair of the Minneapolis/St. Paul Metropolitan Hospital Compact, a 29-hospital mutual aid and planning group active since 2002. He is involved at many levels of planning for surge capacity and adjusted standards of care. He traveled to Greece to assist in health care system preparations for the 2004 Summer Olympics as part of a 15-member CDC/HHS team. He is a national speaker on hospital preparedness issues and has published numerous papers dealing with hospital preparedness for contaminated casualties, personal protective equipment, and surge capacity.
James G. Hodge, Jr., J.D., LL.M., is the Lincoln Professor of Health Law and Ethics at the Sandra Day O’Connor College of Law; director, Public Health Law and Policy Program; and Fellow, Center for the Study of Law, Science, and Technology, at Arizona State University (ASU). He is also a senior scholar at the Centers for Law and the Public’s Health: A Collaborative at Johns Hopkins and Georgetown Universities, and the director of the Western Region Office of the Network for Public Health Law and current president of the Public Health Law Association. Prior to joining ASU, he was a professor at the Johns Hopkins Bloomberg School of Public Health; adjunct professor of Law at Georgetown University Law Center; executive director of the Centers for Law and the Public’s Health; and a Core Faculty member of the Johns Hopkins Berman Institute of Bioethics. Through his scholarly and applied work, Professor Hodge delves into multiple areas of public health law, global health law, ethics, and human rights. The recipient of the 2006 Henrik L. Blum Award for Excellence in Health Policy from the American Public Health Association (APHA), he has drafted (with others) several public health law reform initiatives, including the Model State Public Health Information Privacy Act, the Model State Emergency Health Powers Act, the Turning Point Model State Public Health Act (Turning Point Act), and the Uniform Emergency Volunteer Health Practitioners Act. His diverse, funded projects include work on (1) the legal framework underlying the use of volunteer health
professionals during emergencies; (2) the compilation, study, and analysis of state genetics laws and policies as part of a multiyear project funded by the National Institutes of Health; (3) historical and legal bases underlying school vaccination programs; (4) international tobacco policy for WHO’s Tobacco Free Initiative; (5) legal and ethical distinctions between public health practice and research; (6) legal underpinnings of partner notification and expedited partner therapies; and (7) public health law case studies in multiple states. He is a national expert on public health information privacy law and ethics, having consulted with HHS, CDC, FDA, CMS, OHRP, APHA, CSTE, APHL, and others on these privacy issues.
Donna E. Levin, J.D., M.A., is general counsel for the Massachusetts Department of Public Health. Prior to her 1988 appointment, She served as a deputy general counsel and concentrated on several areas of health law, including determination of need, long-term care and hospital regulation, and environmental health. In her current role, she manages the Office of General Counsel and advises the Commissioner of Public Health and senior staff on all legal aspects concerning the implementation of Department responsibilities pursuant to statutory and regulatory authority; major policy initiatives of the Department; and legislation affecting the Department’s interests. Most recently, Ms. Levin has focused on the expansion of newborn screening services in the Commonwealth; the review and analysis of the Massachusetts Law on Genetics and Privacy; implementation of the Health Insurance Consumer Protections Law and the Pharmaceutical and Medical Device Manufacturer Conduct Law; issues of public health authority and response relating to emergency preparedness; and legal oversight of nine Boards of Registration for health professionals. Ms. Levin is a member of the Health Law Section Steering Committee of the Boston Bar Association and an adjunct professor at Suffolk University Law School. She holds a B.A. from the State University of New York at Stony Brook and a J.D. from Northeastern University School of Law.
Marianne Matzo, Ph.D., APRN, BC, FPCN, FAAN, is professor and Ziegler Endowed Chair in Palliative Care Nursing at the College of Nursing and adjunct professor, Department of Geriatric Medicine, at the University of Oklahoma Health Sciences Center. Dr. Matzo is director of the Sooner Palliative Care Institute, through which research is conducted to ensure the delivery of high-quality care and to educate health professionals. She has received research funding from the American Cancer Society and the Oncology Nursing Society to conduct research related to sexual health issues in the palliative care population. She was a 2008 Recipient of the Project on Death in America Nursing Leadership Award in Palliative Care sponsored by the Hospice and Palliative Nurses Foundation. Dr. Matzo is a nationally and internationally recognized palliative care educator having developed and taught educational programs in Japan, Russia, and Serbia. In addition, Dr. Matzo is a three-time winner of the American Journal of Nursing Book of the Year award. Dr. Matzo had published in numerous peer-reviewed publications and is involved in ongoing work in disaster planning for situations in which there are scarce resources.
Cheryl A. Peterson, M.S.N., R.N., is the director of Nursing Practice and Policy at the American Nurses Association (ANA). Prior to that, she was a senior policy fellow for the ANA, responsible for researching and developing association policy related to preparing for and responding to a disaster, whether man-made or natural. Since 1998, Ms. Peterson has been actively involved in disaster planning at the federal level. In addition, she coordinated ANA’s response to the Tsunami disaster in Southeast Asia and to hurricanes dur-
ing the 2005 U.S. hurricane season. Ms. Peterson spent 13 years in the Reserve Army Nurse Corps and in 1990, was deployed during Desert Storm. She also spent 7 years as an active volunteer in the Kensington Volunteer Fire Department (Montgomery County, Maryland). Ms. Peterson received her B.S.N. from the University of Cincinnati and her M.S.N. from Georgetown University.
Tia Powell, M.D., is director of the Montefiore-Einstein Center for Bioethics and of the Einstein-Cardozo Master of Science in Bioethics, and professor of Clinical Epidemiology and Clinical Psychiatry at Albert Einstein College of Medicine. Previously she served as executive director of the New York State (NYS) Task Force on Life and the Law. She was the founding director of Clinical Ethics at Columbia-Presbyterian Hospital in New York City, where she launched the bioethics consultation service. She is a graduate of Radcliffe College of Harvard University, and Yale Medical School. She did her psychiatric internship, residency, and a Fellowship in Consultation-Liaison Psychiatry all at Columbia University, College of P&S, and the NYS Psychiatric Institute. In 2007, she chaired a workgroup that developed NYS guidelines to allocate ventilators during a flu pandemic. She has served as an advisor on the ethics of disasters for a number of committees sponsored by IOM, CDC, and others.
Merritt Schreiber, Ph.D., is the director of Psychological Programs at the Center for Disaster Medical Sciences, and an associate clinical professor of Emergency Medicine at the University of California, Irvine School of Medicine. Previously, Dr. Schreiber was an associate research psychologist in the Department of Community Health Sciences in the University of California, Los Angeles (UCLA) School of Public Health. He was appointed to the HHS Secretary’s Emergency Public Information and Communications Advisory Board, where he helped draft several policy recommendations on the risk communications for our nation and particularly the needs of children and families. Dr. Schreiber was the program manager of the Terrorism/Disaster Branch of the UCLA/National Center for Child Traumatic Stress at the David Geffen School of Medicine at UCLA. He coordinated the NCCTS/TDB Rapid Response Support Team of National Child Traumatic Stress Network for disasters, terrorism, and mass casualty events impacting children and families. He also served as cochair of the Pediatric Emergency Mental Health Taskforce as the American Psychological Association to the HHS/Emergency Medical Services for Children Program. He received a presidential citation from the American Psychological Association for his work with victims’ families after 9/11 and received the Outstanding Humanitarian Contribution Award from the California Psychological Association in 2004. Dr. Schreiber was a first responder to Hurricane Katrina as a reserved commissioned officer with the U.S. Public Health Service and as mental health team lead with California Disaster Medical Assistance Team CA-1 of the U.S. Department of Homeland Security’s National Disaster Medical System. Dr. Schreiber also developed the first known disaster behavioral health rapid triage and incident management system, called PsySTART.
Umair A. Shah, M.D., M.P.H., has served as deputy director and director of Disease Control & Clinical Prevention at Harris County, TX Public Health & Environmental Services (HCPHES)—the county health department serving the third most populous county in the United States—since 2004. Prior to HCPHES, Dr. Shah was an emergency department physician at Houston’s Michael E. DeBakey VA Medical Center
(MEDVAMC), then chief medical officer at the Galveston County Health District. Dr. Shah’s interests include global and refugee health issues; health equity work; health care management; emergency response activities for events such as Tropical Storm Allison and Hurricanes Katrina, Rita, and Ike; novel H1N1; and the devastating earthquakes in Kashmir and Haiti. His global experience also includes previous work at WHO in Geneva. He is involved in numerous national initiatives, including the APHA Injury Control &Emergency Health Services; the National Association of County and City Health Officials’ (NACCHO’s) National Coalition for Health Equity; UCLA’s Preparedness and Emergency Response Research Center Advisory Board; the National Consensus Panel on Emergency Preparedness and Cultural Diversity (sponsored by the HHS); and various activities related to the CDC. Dr. Shah is immediate past chair of the South Asian Public Health Association, currently chairs NACCHO’s Global Health Workgroup, and was recently selected to the prestigious National Public Health Leadership Institute. In addition to national recognition, Dr. Shah is also involved in the local community, serving in leadership roles with Developments in Literacy, the South Asian Chamber of Commerce, and the Harris County Medical Society. He is an adjunct faculty member at The University of Texas School of Public Health and remains on emergency department staff at the MEDVAMC. He is board certified in Internal Medicine, remains active in clinical patient care, and serves as one of the local health authorities for Harris County. Dr. Shah received a B.A. in Philosophy from Vanderbilt University and an M.D. from The University of Toledo Health Science Center, before completing a residency in Internal Medicine, Fellowship in Primary Care/General Medicine, and an M.P.H. (management) at The University of Texas Health Science Center at Houston.
Jolene R. Whitney, M.P.A., is currently the deputy director for the Utah Bureau of Emergency Medical Services and Preparedness, and also serves as the state trauma system program manager. She directs several programs and staff performing various functions related to Trauma System Development (including Stroke and STEMI Chemical Stockpile Emergency Preparedness, Surge Capacity and MCI Planning, ED, Trauma and Prehospital databases, EMS Licensing and Operations, certification and testing processes, Critical Incident Stress Management, National Disaster Medical System, EMS medical disaster resources, and the EMS for Children program. She has worked with the Bureau for more than 30 years. Ms. Whitney earned her M.P.A. from Brigham Young University and her B.S. in Health Sciences, with an emphasis in Community Health Education, from the University of Utah. Ms. Whitney is coauthor of five publications pertaining to domestic violence, preventable trauma mortality in Utah, Western states rural care challenges, and state and hospital surge capacity planning. Ms. Whitney has served on several national committees and teams, which include state EMS system assessments for the National Highway Traffic and Safety Administration (NHTSA) (Michigan, Delaware, Oklahoma, Ohio and Missouri), American College of Surgeons trauma system assessments (Alaska, Arkansas, Colorado, Louisiana, Minnesota, and Texas); Health Resources and Services Administration (HRSA) rural trauma grant reviewer; and contributor to the development of the HRSA model trauma system plan, the National Association of State Emergency Medical Services Officials trauma system planning guide, National Trauma Data Standards, and the NHTSA curriculum for an EMT refresher course. She is the previous past chair for the National Council of State Trauma System Managers/ NASEMSO and served as vice chair for the previous 3 years. She is a member of the American Trauma Society and Utah Emergency Managers Association, and a previous member of the National Association of
State EMS Training Coordinators and the Utah Public Health Association. Ms. Whitney spent 250 hours in the Olympic Command Center, serving as the hospital liaison for the 2002 Winter Olympics in Salt Lake City. Ms. Whitney is currently assisting with the development of UT DMAT-1, has recently been hired as a federal intermittent employee for the team, and serves as the acting Planning Section Chief. She was certified as an EMT in 1979 and became certified as an intermediate EMT in 1983.













































