For the most part, the VA and the IHS work independently of one another. However, they have a formal Memorandum of Agreement that addresses how they should work cooperatively to serve veterans of mutual interest. In this session, a panel of experts discussed the approach to telehealth within each of these agencies, and the challenges and opportunities that emerge with collaboration. The following sections reflect the individual speaker’s comments and reflections.
U.S. DEPARTMENT OF VETERANS AFFAIRS1
Adam Darkins, M.D., M.P.H.M., FRCS
U.S. Department of Veterans Affairs
The issue of telehealth is not about whether it will happen, but how it will happen. The VA is recognized as a national leader in telehealth, and defines several modalities within telehealth, including home telehealth, clinical video teleconferencing, S&F telehealth, teleradiology, secure messaging, and mobile health. The VA uses off-the-shelf technologies, and has a dedicated national telehealth training center for their staff. Additionally, they use standardized business processes because of the need for interoperability. Developing telehealth services should be based on a demonstrable patient need, and the VA introduced telehealth primarily in the interest of
______________
1 Data presented in this section belong to the VA. Personal communication, A. Darkins, U.S. Department of Veterans Affairs, August 17, 2012.
providing care to veterans. The reasons for doing telehealth include reducing costs, increasing quality, and improving access. Therefore, the VA’s vision of telehealth is that it should be veteran focused, forward looking, and results oriented.
Telehealth Modalities in the VA
Home Telehealth
The value of home telehealth is based in the care of people with chronic conditions. There is no evidence the traditional outpatient clinic is the most effective way to care for individuals with long-term chronic conditions. The VA uses home telehealth (e.g., video, mobile devices) to provide noninstitutional care across the health care continuum: for chronic care management, acute care management, and health promotion and disease prevention. As shown in Figure 11-1, the census for VA patients receiving home telehealth has grown steadily. In FY 2003, about 800 patients were cared for with home telehealth. By the end of FY2012, the VA estimates 92,000 patients will receive home telehealth services annually.
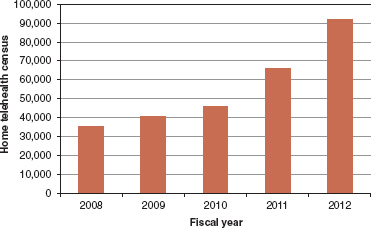
FIGURE 11-1 VA home telehealth patient census, FY2008-2011 and projected FY2012.
SOURCE: Reprinted with permission from Adam Darkins (2012).
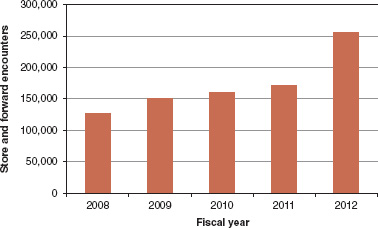
FIGURE 11-2 VA store and forward encounters, FY2008-2011 and projected FY2012.
SOURCE: Reprinted with permission from Adam Darkins (2012).
Store and Forward Telehealth
In the VA, S&F telehealth is mainly used for teleimaging for diabetic retinopathy and for teledermatology. Both of these serve a demonstrable patient need. About 20 percent of the 5.6 million veterans in the United States have diabetes, and screening for diabetic retinopathy is a way to prevent avoidable blindness. Additionally, many VA organizations, particularly those in rural areas, have difficulty finding dermatology services. The VA is also exploring how to use this technology into wound care. Figure 11-2 shows the growth in S&F encounters. In 2005, about 1,500 patients were managed by S&F telehealth; by the end of FY2012, this number is estimated to be around 256,000.
Clinical Video Telehealth
Clinical video telehealth replicates the face-to-face consultation (e.g., between provider and patient, provider to provider) and eliminates the need to travel for certain services. The VA primarily uses this for real-time videoconferencing between VA medical centers and community-based outpatient clinics. It is mostly used for the delivery of mental health services and specialty consultations (e.g., telecardiology, teleneurology, tele-amputation care, teleaudiology, telepathology). In the past year, the VA has been moving
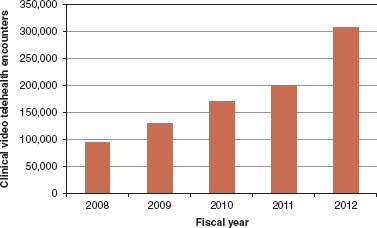
FIGURE 11-3 VA clinical video telehealth encounters, FY2008-2011 and projected FY2012.
SOURCE: Reprinted with permission from Adam Darkins (2012).
into tele-ICU. Over the past 7 years, the VA has built a dedicated national network for clinical video telehealth. This network includes 4,000 video endpoints within the VA system (e.g., hospitals, clinics), with everyone using Internet protocol (IP) video. The VA is also extending IP video into home care. As seen in Figure 11-3, the VA has had tremendous growth in the use of clinical video telehealth.
Impact
In 2011, clinical video telehealth, home telehealth, and S&F telehealth together accounted for care at more than 150 VA medical centers and 750 community-based outpatient clinics to 380,865 patients. Thirty-seven percent of the patients were in rural areas and 3 percent were in highly rural areas. For FY12, the VA estimates that 480,000 veterans (approximately 9 percent of the veteran population) will have been served by one of these telehealth modalities, and that in FY13, the number will rise to 820,000, or about 15 percent of the veteran population.
Outcomes assessments show reductions in bed days for home telehealth programs (53 percent) and clinical video telehealth for mental health care (25 percent). In terms of patient satisfaction, home telehealth programs have a mean score of 86 percent and S&F telehealth has a mean score of 92
percent. The VA pays for a certain amount of travel costs, and assessments show an average savings of $34.45 per video consultation and $38.81 per consultation for S&F. In previous years, savings associated with the home telehealth program (above all other costs, including the cost of the program) ranged from $1,238 to $1,999 per annum per patient.
Telemental Health
Mental health care is a major reason for implementing telehealth. In FY2011, 146 hospitals provided 55,000 patients in 531 community-based outpatient clinics with 140,000 telemental health visits. Home telemental health programs provided care to more than 6,700 patients for conditions such as depression and posttraumatic stress disorder. A review of more than 98,600 patients who received clinic-based telemental health care between 2006 and 2010 showed a 25 percent reduction in hospitalization. A review of 1,041 mental health patients before and after enrollment in home telemental health services by the VA in 2011 showed a 30 percent reduction in admissions in their first 6 months of care as compared to a similar period of time before enrollment.
Meeting Challenges and Ensuring Quality
Two challenges facing the VA are not unique to the VA: training often is not part of the health professions’ curricula, and there are no outside resources to train VA providers on the use of telehealth. Currently, more than 60 requirements exist to establish a telehealth program, and they are often beyond the competency of most individual VA staff (e.g., privileging, information technology compatibility). Furthermore, the Joint Commission does not survey telehealth specifically, but will encounter telehealth during their reviews.
To meet these and other challenges, and to ensure the quality of their programs, the VA has three telehealth training centers that develop and provide standardized training and resource materials. Additionally, a quality management team provides biannual reviews of each Veterans Integrated Service Network (VISN) for integration of telehealth standards with Joint Commission requirements for hospital- and home-based care. The VA also has national databases, reports, and analyses for metrics of performance and quality of telehealth programs at the levels of the local VA medical center, the VISN, and nationwide. The VA also has national contracts and contract support for telehealth technologies, including service and warranties to ensure equipment quality and safety, and collaborates with national clinical experts to develop standards of care for telehealth care. Lastly, the
VA collaborates and coordinates with stakeholders to ensure comprehensive infrastructure for telehealth.
National Telehealth Training Centers
The mission of the telehealth training centers is the right training, in the right place, and at the right time. Because of the size of the VA network, it is important that people are trained in a standardized way. The emphasis is on virtual training (98 percent of the training is provided virtually) and strategic partnerships with the Employee Education System. These centers provide the training, tools, and resources to
- successfully plan, deploy, and manage telehealth programs;
- standardize organizational, clinical, technical, and business infrastructures;
- assess programs to identify clinical needs that telehealth can address;
- improve and expand the delivery of care via telehealth to ensure the efficiency, quality, and sustainability of services; and
- integrate with existing programs.
Through the third quarter of FY12, the VA has had 150 training courses or forums available from the three centers. The clinical video telehealth training center has trained more than 4,000 staff through more than 600 events. The S&F training center has trained more than 3,200 unique staff through more than 250 training events, and the home telehealth national training center has trained more than 2,500 staff through 800 events.
Training innovations include clinical practice forums, integrated telehealth master preceptor programs, interactive meeting rooms, new and improved methods of training, out options for super users, the use of video to capture the human element, scenario-based instruction evaluation, the use of animation, and rapid response training.
Mark Carroll, M.D.
Flagstaff Medical Center
Where are we trying to go in telehealth? The widespread adoption of telehealth seems to be an important and major goal. Why is this so difficult,
______________
2 Dr. Carroll indicated that while he worked for the IHS for 20 years, his comments did not necessarily reflect those of the agency.
and are we approaching it in the right way? The easy answer is that the problem is all about reimbursement, and that telehealth payment should be equivalent to in-person care. However, perhaps the widespread adoption of telehealth is not really the goal. Instead, the real goal is quality, as conceptualized by the triple aim of the Institute for Healthcare Improvement: experience of care, cost, and population health (IHI, 2012). So, the real question is how can telehealth innovation help achieve the triple aim?
The IHS includes more than 600 facilities, some full-time and some part-time, across the country. These facilities include hospitals, health centers, Alaskan village clinics, and health stations. Most of these facilities are under tribal self-governance. Partnerships and collaborations are critical, and tribal governance is an important part of that. Indian health care is mainly rural, but it also occurs in urban environments. A differentiating point for IHS as compared to other federal systems of care (e.g., the VA) is that more than half of annual operating budgets of many IHS facilities is from third party billing, so business models matter.
Telehealth is not new to the IHS. In the 1970s, the STARPAHC project was jointly sponsored by the IHS; NASA; the Department of Health, Education, and Welfare (predecessor to HHS); and the Papago Tribe. In the project, health care providers traveled in a van to deliver health care via “two-way television,” radio, and remote telemetry, applying some of the same basic precepts of care that we talk about today.
New Service Models
Since that time, many new tools have been embraced with the development of new service models. However, one model does not fit all. Some of the models are driven by necessity, such as the complete lack of access to specific specialty care. Many of the models for these new services rely on new partnerships, including ones that seem unfamiliar. For example, Coconino County in northern Arizona is the second largest county in the United States, and it sits adjacent to the Navajo nation and the Hopi nation. Currently, shared models are being developed for psychiatry and other services. Some models add very robust efficiencies. For example, the use of S&F consultation across the state of Alaska has resulted in dramatic improvements in speed of reply. However, efficiencies cannot be reached in some places because the models are not integrated into the care systems. This depicts the care approach and the culturally appropriate plan-do-study-act cycle in the Chinle Service Unit on the Navajo reservation. New types of innovation that do not work in this type of model and depiction are not easily integrated. Many models require new commitments. For example, the IHS ran telenutrition services from northern Arizona in Indian health sites in multiple states for years, resulting in thousands of interactions. When the
commitment went away, so did the ability to continue that model of care. Most models are not successful without a lot of effort. In another example, the IHS uses the Joslin Vision Network for a teleophthalmology program for retinopathy screening. The program improves access to screening and it improves access to laser treatment for diabetic patients already cared for in the clinic. The costs are lower, and the screening and care is better than in-person exams. This took a long time to get up to speed, and while eye screening rates across the IHS have improved by 20 percent in the facilities that have embraced this program, there is still much room for improvement.
Diffusion of Innovations
In Diffusion of Innovations (Rogers, 1962), Rogers highlighted issues relevant to telehealth. Many care models using telehealth do not diffuse the same way, yet these models are still isolated in specific categories (e.g., real time, S&F, remote monitoring). A different stratification system may be needed to distinguish telehealth innovations by their ability to diffuse easily rather than by the modality. For example, first there are innovations that can integrate more easily into conventional models of care because fundamental process and payment changes are not required. Teleradiology may be an example of that. Next are innovations that require important, but non-fundamental, changes within a closed health care system. Examples may include the use of telehealth within the Kaiser health system and the VA. Finally, there are the telehealth innovations that require fundamental changes, especially for open systems, systems that are collaborative in nature, and not within particular organizations. An example is chronic care coordination after hospital discharge.
Telehealth-enabled care is not necessarily the same as in-person care. They are different models of care and should not necessarily be reimbursed in the same way. Instead, new models of reimbursement are needed care. For some care models, there is no in-person option, and so reimbursing the same way across video makes sense. For some care models, a new tool (i.e., telehealth) does not necessarily bring added value. However, there is a growing evidence base for certain models that shows that telehealth care is just as good as conventional care; and sometimes it is better. We need to remember that not all of telehealth is exactly the same.
Relationships and Connectedness
In research, we need to consider the value of relationships and connectedness in some of these new care models. Part of the purpose of innovation in health care is to activate certain intermediate behaviors and activities, such as self-efficacy, self-management, and medication compli-
ance to achieve the triple aim. Relationship supports (e.g., social supports, behavioral health screenings, health coaching) are critical to this activation.
A 2010 study of patients hospitalized for heart failure concluded that telemonitoring did not improve outcomes (Chaudhry et al., 2010). However, important details might affect that interpretation. For example, this multisite trial was based on an earlier single-site trial that resulted in a 44 percent reduction in the rate of readmission, and was associated with significant cost savings. In the attempt to scale the model, a single skilled nurse case manager (who had one-on-one conversations with the responsible physician) was replaced with an automated monitoring system. Therefore, an alternate conclusion is that the non-relationship based model did not work.
Learning from that, Care Beyond Walls and Wires, a collaborative project in northern Arizona among private industry, the IHS, community health centers, and the Flagstaff Medical Center, is built on the need for relationships. This model uses tools like smartphones and a 3G signal so patients who live in remote areas can stay in communication with health care coordinators, especially after a hospital discharge. At the heart of this and other telehealth models is the relationship and regular communication between the patient and the care provider.
Concluding Remarks
Carroll reflected that changing care models is a daunting task, and challenges health care teams and policy makers alike. To facilitate these changes, telehealth innovations need to be stratified differently so that we can identify and learn from the different obstacles to diffusion. Also, more collaboration is needed in open health systems to work toward achieving better experience of care, lower costs, and improved population health. Different health organizations have different business drivers and motivators. Because of that, more study is needed on the role of connectedness in regional partnerships to improve transitional care for patients. Finally, care model change on a larger scale can be supported by focusing on key locations such as IHS facilities and community health centers, where national projects to study the effects of systematic uses of telehealth innovation can lead to policy and legislative changes.
CRITICAL RELATIONSHIPS IN TELEHEALTH WITH
AMERICAN INDIANS AND ALASKAN NATIVES
Jay H. Shore, M.D., M.P.H.
U.S. Department of Veterans Affairs;
University of Colorado Denver
Telehealth is not about the technology itself, but is a bridge to the relationship with the patient needed to provide care. In a lot of ways, the most important treatment we give is the healing relationship between the patient and a provider. As seen in Figure 11-4, that relationship is the core of telehealth care, but that does not happen without a series of relationships that need to occur to allow a provider to see a patient in a rural community. In fact, although that relationship is critical, it is not the most important relationship for successful telehealth clinics. In rural populations, the most important relationship is often the relationship between the provider and the community, because without it the service will not exist. Embedded in that are organization-to-organization relationships, and particularly for native patients; this relates to eligibility across multiple systems. For example,
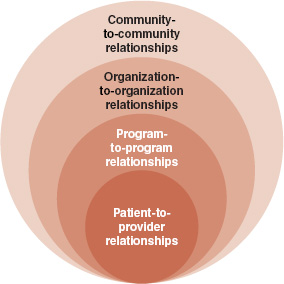
FIGURE 11-4 Multiple relationships of telehealth care.
SOURCE: Reprinted with permission from Jay H. Shore (2012).
evidence shows that native patients in particular use various systems of care; so, native veterans might get primary care from the IHS, and then choose to get specialty mental health care from the VA. Finally, in specific programs, there are internal and external relationships that need to occur for successful clinical interaction.
Mental health has a unique fit for telehealth in that most of mental health care can be accomplished in some form over videoconferencing. This has been shown in the growing literature over the past decades, across age groups, populations, and treatments, although even more research is still needed. Particularly in the past 5 years, the emerging technologies of direct in-home video conferencing, mobile health, and Web-based care have been changing how providers interact with patients. Telehealth and telemental health are especially relevant for native communities with geographic barriers to access, as well as cultural and institutional barriers that may prevent them from accessing care. RCTs are certainly needed to demonstrate that these treatments are as rigorous as any other treatment, but more nuanced approaches are also needed to understand this tool of technology and how it interacts in relationships. Each type of technology has strengths and weaknesses. There are appropriate pairings of technology with diseases and populations, but we do not necessarily understand in a systematic way how to make those pairings.
Patient-Provider Relationships
Good data show that there are some situations where telehealth may be more effective than face-to-face visits. For example, Shore related that in working with female natives with a history of domestic violence or post-traumatic stress disorder, the women often say it is easier to begin working with an unknown provider over video because in the initial visits, the distance helps facilitate a feeling of safety. As the relationship builds over subsequent sessions, the need for this feeling of safety through distance lessens as the patient develops trust with the provider. Counterpoints to that distance include the loss of cues and the perception of emotional distance. RCTs in telemental health show equal outcomes, but there are some hints of an impact on the patient-provider relationship and the clinical process. We do not know how that translates and how that ultimately impacts clinical outcomes. Telemental health clinicians will say it is different than seeing someone face-to-face. The good clinicians and systems understand that and make adaptations.
There are many different adaptations to bridge patient-provider gaps, such as provider contextual training. Providers are often from urban areas, and may not have spent much time in rural communities, so they may feel disconnected when caring for remote patients by video. Unless these provid-
ers make real efforts to understand the patient’s environment and the issues impacting the patient in terms of community events, they may lose touch with what is going on contextually. Cultural and clinical facilitators are also useful. For example, the tribal outreach worker is a native veteran who lives in the community, does scheduling, builds rapport, and helps bring in patients who traditionally may have been reluctant to get care from federal health care systems. Veterans without a history of care for mental health issues may come for care for the first time not because of a stranger coming over video from an urban location, but because of the community member involved in the clinic. That is one adaptation at the patient-provider level. Additional adaptations include collaboration with traditional healers and family members.
Program-Program Relationships
Telehealth requires multiple internal and external collaborations among programs that may not come together in the traditional course of health care (e.g., primary care providers and information technology specialists). These programmatic areas may also have different languages, cultures, structures, models, and philosophies. The need to work together compels an increased level of coordination, continuity, and consistency in care, and leads to more holistic approaches. It also requires new models of care integration and health care team configuration. The conceptualization of health care teams has not kept pace with the technologies and the models that are delivering these technologies.
Organizational Relationships
Providing care may also involve multiple organizational collaborations. For example, one of Shore’s clinics has six different partners: two VAs, a university site, the IHS, and two tribal partners. The cooperation and coordination of multiple systems of care is possible and, at times, highly desirable. Whereas one institution might not have all of the necessary resources, this cooperation provides more options for patients and increases care coordination. Also, with multiple systems, there may be better collective sources of funding. However, challenges include the identification of the correct configuration of partners. In addition, the technologies in the different organizations need to be able to interact, and managing multiple compliance and regulatory issues across systems can also be very challenging. Other sensitive issues include the designation of the primary funder and determination of who will pay for which programs or services. Organizational collaborations often start off based on individual relationships, and are critical in native communities. Overall, success depends on systematiz-
ing the right communication and collaboration processes that work within the local context, so that when the champions and other individuals move on, the infrastructure remains.
Concluding Remarks
Shore concluded that we need to do a better job of investigating, exploring, and codifying models that are successful at each relationship level in order to understand the importance of the impact of the relationships— how they are successful or how they do not work. We also need to understand how technology affects the process of health care, either positively or negatively. Finally, we need to learn more about appropriate adaptations to make sure that the development of telehealth services and networks focuses on enhancing the quality of and access to care in order to fulfill the promise of telehealth, especially for American Indians and Alaskan Natives.
Moderator: Spero M. Manson, Ph.D.
University of Colorado Denver
An open discussion followed the panelists’ presentations. Manson began the session by noting the speakers’ emphasis on relationship building not just at the provider-patient level, but throughout the hierarchy of relationships that underpin health care. He added that these relationships relate directly to the success of health care services in both the short and long terms. Audience members were then able to give comments and ask questions of the panelists. The following sections summarize the discussion session.
Reducing Federal Silos
One participant asked how to facilitate more successful collaboration among federal agencies and reduce silos. Carroll stated that recognition of the differences in the organizations and systems (including their missions) is critical. He noted that the IHS and the VA have a Memorandum of Understanding that allows for the exchange of information, tools, and experiences, but the respective missions of the organizations have guided the focus of their collaborations on service for native veterans. Carroll stated that better understanding of why certain models diffuse well in some systems and not others can serve as guideposts to steer expectations of diffusion because not all systems will work the same way. For example, there have been some great programs that work well within closed systems, but
are challenged when translated into systems that require interactive partnerships. Shore added that growth is needed both from the “top down” and the “bottom up.” He cited the Memorandum of Understanding as an example of growth from the top. He added that the best IHS-VA collaborative successes occur when individuals at the local level look for how to use national processes to serve veterans. He noted that this, in turn, often leads to changes at the structural level.
Darkins responded that reducing silos is not merely about agreeing to work together, but that developing networks and standardized processes has real challenges, including issues of privacy and confidentiality. He suggested that telehealth could be defined as a multimedia patient record. Without the ability to exchange information, he said, the utility of video alone is relatively limited because telehealth is really about decision making for patients, and so successful collaboration is about building communities that link different systems. Darkins further noted that building a standardized process even within one system of care is challenging, adding that the VA is no different from other organizations when it comes to funding. He stated that the VA does not mandate the use of telehealth, nor is there centralized funding, so the values to growing these programs are largely access and local savings. For example, he said, it took nearly 5 years to build the data to support home telehealth.
One participant stated that NASA would be a good collaborative partner for the IHS and VA for the sharing of electronic medical record modules.
Linking Data Sources
One participant asked if federal data might be made available for use by the private sector, especially to do point-in-time evaluations. Darkins agreed, stating that linking data is the challenge of health care systems worldwide. He noted that the VA is working toward how information can be shared like this. Carroll also agreed, adding that the VA has been involved in information system development for many decades, and is interested in the bidirectional and contiguous exchange of data.
Involvement of Decision Makers
Manson asked how each system of care has educated and involved key decision makers, especially within the local community. Shore stated that the involvement of both the VA system leadership and the tribal leadership have been critical to his work. He said that in each community where they set up telemental health services, they have discussions with the tribal council and engage that leadership, as well as the local VA leadership. He agreed that support of the local and regional leadership is critical to success.
He added that engaging leaders at the national level is key to expanding models to other locations. Manson agreed, stating that generating an early series of small but effective models can inform other advocacy levels. For example, Manson and Shore discussed the role of the VA in supporting the development and further adoption of local models of care that were based on existing tribal relationships. Darkins stated that population health is really the driver for the development of telehealth. Perhaps there will be collaborations at the state level to allow for telecommunications resources to be pooled and used in different ways to serve multiple organizations. However, he said, there are many complexities, including privacy and confidentiality, to making this happen.
One participant asked how to get CMS to accept the work and data of the VA and IHS as evidence for coverage decisions. Carroll answered that the IHS has been working with CMS on these issues. He noted that the IHS also has tremendous data to share on outcomes, process, and costs related to the use of telehealth for national coverage determinations for telehealth. Carroll noted that a U.S. Senate bill had previously been proposed to authorize Medicare telehealth reimbursement for community health centers and Indian health sites. Darkins stated that CMS has been actively supporting telehealth development with many pilot programs. He added that telehealth is not being carried out in a standardized way across the United States, and that creating standardized systems for telehealth within the VA is a key to success. Darkins stated that CMS bases investment decisions on effectiveness, and they will determine if and when there is sufficient evidence to support the development of larger telehealth networks, and which, if any, of the models they believe can be transferred.
Cultural Competency
One participant raised the issue of the importance of cultural competency to the patient-provider relationship. Shore responded that in each community he and his team have served, they have tried to establish either a formal or an informal network with traditional healers. He said they have had ceremonies and blessings for the use of videoconferencing. They also will refer patients interested in traditional healers for sweat lodges to help with posttraumatic stress disorder, and that occasionally, those healers (with the patient’s permission) will come in to discuss the patient’s treatment. Shore stressed that this demonstrates to the individual patient that his or her perspective on health care and treatment is being considered, and it is an indication to the community that the individual provider and the larger health care organization are considering the community needs. Shore further asserted that demonstration of collaboration and partnership at the community level is critical to relationships.
















