7
Implementation and Models of Care
for Veterans Who Have
Chronic Multisymptom Illness
As previously described, nearly all veterans who have chronic multisymptom illness (CMI) have comorbid illnesses—illnesses that are themselves multisymptomatic and that overlap with CMI in complex and highly variable ways. The most common chronic condition in the United States, and probably the world, is multimorbidity (Tinetti et al., 2012), and this is especially true for patients who have CMI. Even though there may be evidence-based treatments for one or more of these conditions, the committee believes that a treatment plan consisting simply of the sum of these practice guidelines will be altogether inadequate and is ill-advised. An integrated approach to care is required. There is a fundamental difference between managing a disease or a condition and caring for a person who has one or more conditions—just as there is a fundamental difference between a clinical practice guideline (CPG) and a personal care plan. Anecdotal evidence suggests that simply adhering to multiple CPGs often is not effective for managing chronic conditions with multiple morbidities such as CMI and can result in incomplete care and decrease patient satisfaction, and increase the likelihood of overtreatment and adverse side effects. Each personal care plan will be peculiar to the individual veteran (although crafted from the therapeutic elements outlined in Chapters 4 and 5), will change, and will almost always be complex and detailed. A clinician caring for a veteran who has CMI faces a daunting and time-consuming task that cannot always be accomplished in the course of an ordinary primary care visit and can hardly be implemented by a single clinician; it generally takes a team approach and specific expertise. Special consideration must be
given to the resources and the organization—the system of care—that are marshaled for the management of CMI patients.
This chapter presents a patient-centered management approach for veterans who have CMI. It begins by describing some of the current capabilities of the Department of Veterans Affairs (VA) for managing the health of veterans. It identifies inadequacies of existing VA models of care for veterans who have CMI and recommends a general approach to the management of such veterans. The chapter next describes models of care used by other organizations to manage CMI patients. Building on information presented in Chapter 6, it ends with a discussion of how information about managing CMI might be disseminated to VA clinicians and patients.
Veterans use the full array of health care benefits and systems for their care: the Veterans Health Administration (VHA); TRICARE, the Department of Defense (DOD) health care program for active-duty, reserve, and retired armed forces personnel; Medicare; and private care. Fewer than 20% of all veterans receive their health care exclusively in VHA facilities, about one-third of veterans use Medicare benefits, and almost half use both (Hynes et al., 2007; Petersen et al., 2010; Stroupe et al., 2005; West et al., 2008). The distribution among the health care system of veterans who have CMI is not known, nor is there any difference in the pathway of care between veterans of the 1991 Gulf War and veterans of the Iraq and Afghanistan wars (Operation Iraqi Freedom, Operation New Dawn, and Operation Enduring Freedom).
More than 8 million veterans are enrolled in VHA (Walters, 2011). In FY 2009, the number of pre–September 2001 Gulf War–era veterans receiving health care through VHA was 571,656 (VA, 2011d).1 That number represents 8.7% of the total Gulf War–era veteran cohort. Of the pre–September 2001 Gulf War–era veterans receiving care from VHA, 145,832 were deployed to the Persian Gulf and 110,487 of the deployed personnel were active participants in the Gulf War. Inpatient care in VHA facilities was used by 24,578 pre–September 2001 Gulf War–era veterans in FY 2009, and outpatient care was used by 540,802 Gulf War–era veterans in the same year. About 55% of veterans of the Iraq and Afghanistan wars (834,463 veterans) have used VHA health care services since October 2001
_____________
1For this case, Gulf War–era veterans are defined as military personnel who served on active duty during August 2, 1990–September 10, 2001. Not all Gulf War–era veterans were deployed to the Persian Gulf or were Gulf War participants.
(VA, 2012a). Among those Iraq and Afghanistan war veterans who have sought care at VHA facilities, about 94% have used only outpatient services and about 6% have been hospitalized at least once (VA, 2012a).
VHA has substantial experience in treating patients who have chronic illnesses. Its patients have a higher prevalence of the eight most common chronic health conditions than do patients who are using TRICARE and private plans (Gibson et al., 2009), not including CMI. As indicated above, information is not available on the number of veterans who have CMI and receive their care from VHA or elsewhere.
Postdeployment Patient-Aligned Care Team Program
Gulf War veterans have begun to enter the VHA system by being assigned to a postdeployment patient-aligned care team (PD-PACT) (Hunt, 2012). A PD-PACT serves as a veteran’s medical home in VHA. The move to a medical-home model is relatively recent in VHA and implementation is ongoing (Reisinger et al., 2012). VHA’s implementation of this model of care compares favorably with implementation in most civilian practices and systems, in which the transition to patient-centered medical homes is still in the early stages of implementation. VHA has established principles and guidelines for the implementation of PACTs, educated its clinicians about the principles, and assigned champions to lead the implementation effort (VA, 2012j). It is important to note that this pathway to care did not exist when military personnel were returning from the 1991 Gulf War and entering the VHA system. The 1991 Gulf War veterans are now being served by PD-PACTs, but their enrollment rates have been highly variable among settings (VA, 2012e). The plan is for assignment to a PD-PACT to begin after a postdeployment comprehensive health examination and a postdeployment disability determination. At some sites, the wait time for the two steps is extremely long, sometimes more than a year. That is frustrating for veterans, who sometimes seek care elsewhere; it also compromises PACT primary care clinicians’ ability to render high-quality care.
Each PD-PACT is overseen by a project manager. Other team members can include primary care clinicians, nursing-care managers, mental health clinicians, social workers, and others who have expertise in such subjects as brain injury and physical rehabilitation. The number, specialty types, relative availability, and extent of integration into the primary care team of specialty-team members vary widely from clinic to clinic; VHA currently assigns behavioral-health clinicians to PACTs in VA medical centers (VAMCs) and outpatient clinics that have more than 5,000 primary care patients, and many smaller clinics also have behavioral clinicians on PACT teams. A veteran being cared for is considered a member of the team. The goal of the PD-PACT model is to provide comprehensive, integrated care,
including follow-up health care, education, and training (Reisinger et al., 2012). Postdeployment integrated care services are in place in 79% of VAMCs and 35% of community-based outpatient clinics (Hunt, 2012), but the extent to which these teams actually function as teams and contain all the necessary expertise is highly variable. Under ideal circumstances, PD-PACT members work together as a coherent team, but many PD-PACT members operate as consultants without a continuing commitment to patients’ care plans and without close communication with other PACT members. Some 84% of VAMCs have clinical experts who can provide clinical guidance for veterans in the context of their continuing primary care (Hunt, 2012).
Educational Materials
VHA provides extensive educational materials to patients and their families about such topics as environmental exposures, associated adverse health outcomes, and techniques for self-management of symptoms. For example, materials are available on controlled-breathing techniques (VA, 2009a), complementary and integrative medicine (VA, 2011b), using exercise to manage chronic pain and fatigue (VA, 2011c), and medically unexplained symptoms (VA, 2011e). Materials also are produced for clinicians (for example, a resource guide on helping patients self-manage their symptoms) (VA, 2009c).
Clinical Practice Guidelines
VHA has a CPG for the management of veterans who have symptoms that remain unexplained after appropriate medical assessment (VA and DOD, 2001b).2 In addition, VHA has developed CPGs for a number of relevant conditions, including postdeployment health and common comorbidities and conditions that have overlapping symptoms, such as major depressive disorder, posttraumatic stress disorder, traumatic brain injury, and chronic pain (Chou et al., 2007; VA and DOD, 2001a, 2009a,b,c, 2010a,b). The CPG on medically unexplained symptoms provides a general approach for managing CMI patients. For example, the key points made in the CPG (VA and DOD, 2001b) are to
• Obtain a thorough medical history, physical examination, and medical record review.
_____________
2VA has plans to update its 2001 CPG on medically unexplained symptoms (personal communication, C. Cassidy, Office of Quality and Safety, Department of Veterans Affairs, March 19, 2012).
• Minimize low-yield diagnostic testing.
• Identify treatable causes (conditions) for the patient’s symptoms.
• Determine if the patient can be classified as having chronic multi-symptom illness (CMI) (that is, has two or more symptom clusters: pain, fatigue, cognitive dysfunction, or sleep disturbance).
• Negotiate treatment options and establish collaboration with the patient.
• Provide appropriate patient and family education.
• Maximize the use of nonpharmacologic therapies:
— Graded aerobic exercise with close monitoring.
— Cognitive behavioral therapy.
• Empower patients to take an active role in their recovery.
The guidelines are useful and appropriate, and VHA has published its method for disseminating and implementing its CPGs in VHA clinics (Nicholas et al., 2001; VA and DOD, 2011).
VHA has also published a study guide (not a full CPG) for clinicians on caring for veterans of the 1991 Gulf War (VA, 2011a). It includes information on exposures of concern to veterans of the 1991 Gulf War and instructions for conducting an exposure assessment of veterans. It also contains a section on undiagnosed and unexplained illnesses, including information about CMI.
Specialty Care Access Network
Although VHA has 153 medical centers and more than 900 outpatient clinics nationwide, not all veterans have easy access to VHA facilities (Reisinger et al., 2012). Accordingly, VHA developed a specialty care access network (SCAN) to bring specialty care to veterans who live in rural and other underserved areas, generally areas that do not have VAMCs (VA, 2012e). SCAN is modeled after Project ECHO (Extension for Community Healthcare Outcomes), a program developed by the University of New Mexico Health System. The mission of Project ECHO is to develop the capacity to treat chronic, common, and complex diseases in rural and underserved areas safely and effectively and to monitor outcomes (Arora et al., 2011). The program works by bringing ECHO network specialists with the medical expertise necessary for the condition being addressed into otherwise isolated primary care practices. After an initial in-person orientation, a team meets weekly via video conference to present and discuss patients and to formulate care plans. The program fits well into the medical home model by augmenting comprehensiveness, improving continuity and coordination of care, and enhancing quality and safety of care. An important element of the ECHO program is teaching and implementing concepts of team management of patients (Katzman, 2012).
VHA adopted the SCAN-ECHO program in 2010 and contracted with Project ECHO to leverage technology and use case-based learning to educate its primary care physicians in chronic pain management and other specialty care topics. Eleven regional VAMCs are using the SCAN-ECHO program. In addition, VAMCs in Denver, Colorado; Richmond, Virginia; Cleveland, Ohio; Albuquerque, New Mexico; greater Los Angeles, California; Salem, Massachusetts; Portland, Oregon; and New Haven, Connecticut, are now replicating the Project ECHO chronic pain program, and clinicians in their regions are calling in each week for consultations related to pain management (VA, 2012e).
War-Related Illness and Injury Study Centers
Under a congressional mandate, VA established war-related illness and injury study centers (WRIISCs) in 2001 to serve combat veterans who had unexplained illnesses (Lincoln et al., 2006). Three WRIISCs are operating in East Orange, New Jersey; Palo Alto, California; and Washington, DC. The WRIISCs are multidisciplinary centers of excellence to which veterans who are severely afflicted with CMI can be referred. They also are charged with conducting research on CMI and its constituent symptoms and with creating and disseminating educational materials for veterans, their families, and clinicians (Lincoln et al., 2006; VA, 2012l).
Veterans may be referred to a WRIISC by their clinicians. Referrals generally come about because a veteran has a complex medical history of no known etiology, treatments have resulted in little or no symptom improvement, deployment-related environmental exposures may have occurred, or the veteran is not improving and further local expertise is unavailable (Reinhard, 2012). Veterans in a WRIISC are evaluated by a multidisciplinary team that conducts a comprehensive health assessment and formulates a comprehensive personal care plan aimed at managing symptoms and improving functional health; the plan is implemented in the WRIISC and given to the referring clinicians (Lincoln et al., 2006). As of 2012, the WRIISCs’ clinical programs have conducted health assessments of about 1,000 veterans (Reinhard, 2012).
Patient-Centered Medical Care and the Office of Cultural Transformation
VHA has established an office of Patient Centered Care and Cultural Transformation (Petzel, 2012; VA, 2012g,h). The goal of the office is to develop personal, patient-centered models of care for veterans who receive their health care at VHA facilities. There will be greater focus on providing team-based care and integrative approaches throughout VHA. The office seeks to address the “full range of physical, emotional, mental, social, spiritual, and environmental influences” on veterans (VA, 2012g).
Summary of Models of Care in the
Department of Veterans Affairs Health Care System
VHA has developed extensive infrastructure and support for veterans who have CMI and the clinicians who care for them: multispecialty teams, practice guidelines, training and educational materials for clinicians and patients, access to consultants when they are not available locally, support for such elements of implementation as practice champions, the basic structure of a system of stepped care, and more. The infrastructure is remarkable and far outstrips the corresponding elements of the civilian health care system, which is generally much less developed. All those efforts notwithstanding, however, veterans who have CMI will remain seriously underserved, and their clinicians will remain unable to serve them adequately, until additional measures are put into place. Clinical guidelines for chronic conditions are extraordinarily difficult to implement, and their implementation follows a set of rules and principles that are just now becoming understood. CPGs assume a degree of uniformity of presentation and severity and the availability of time, training, and personnel that are not always available even in the most dedicated and highest-quality settings. But the patients present with highly variable and ever-changing symptom constellations—with a spectrum of severity ranging from just barely symptomatic to profoundly disabled—in a highly variable and constantly changing clinical environment. Thus, the treatment burden of and need for care coordination is not uniform among clinical settings. Finally, and most important, even in settings where it is possible to bring a high degree of standardization, the team members themselves—their seniority, previous experiences, personalities, team “chemistry,” and response to the particular local leaders—constitute a source of irreducible variation that must be taken into account in the implementation process. Local practice coaches and other local resources are almost always necessary for successful implementation. The issue of implementation will be addressed after a description of the veterans’ experience of care.
GULF WAR VETERANS’ EXPERIENCE OF CARE
Patient Satisfaction
Despite the extensive efforts devoted to improving care for veterans who have CMI, some Gulf War veterans have expressed frustration and anger about what they consider to be subpar care from VHA (public comments to the committee, December 17, 2011, and February 1, 2012; Furey, 2012). Often, they do not believe that VHA clinicians take their symptoms
seriously, and they get the impression that the clinicians believe that their health problems are mental in origin.
Gulf War veterans report less satisfaction with waiting-room time, copayment or costs, courtesy of office staff, and clinician time than World War II veterans (Harada et al., 2002). Differences in several other variables were not significant—number of days waited for an appointment, how easy it is to get around a facility, clinician skill, and overall satisfaction. Harada et al. (2002) found that veterans who used both VHA and non-VHA facilities (“dual users”) were less satisfied overall with their outpatient care than were veterans who used only VHA or only non-VHA facilities.
In a study that compared veterans’ satisfaction with types of clinicians in VHA facilities, satisfaction scores increased as the numbers of nurse practitioners increased (Budzi et al., 2010). Veterans are more satisfied with nurse-practitioners who were trained in particular skills, such as paying attention to and providing for the patient’s educational needs, individualized care, and active listening.
Health status is significantly associated with patient satisfaction in veterans who use VHA outpatient care (Ren et al., 2001). Mental health status correlates more strongly with patient satisfaction than does physical health status. In general, veterans who are healthier are more likely to be satisfied with their care. Satisfaction can be both a consequence and a determinant of health status; in the study by Ren et al. (2001), health status seemed to be more of a determinant of patient satisfaction than the reverse.
Veterans who had chronic illnesses and experienced greater satisfaction with VHA were less likely to seek care elsewhere after discharge from active duty (Stroupe et al., 2005). Greater dissatisfaction at baseline led to a greater probability that veterans would later go outside the VHA system, thereby seeding the civilian primary care sector with unhappy veterans who had CMI. Veterans older than 65 years old are more likely to use non-VHA health care facilities than younger veterans; this may be due to the older veterans’ Medicare eligibility.
Female veterans reported scores similar to those of male veterans on most dimensions of outpatient satisfaction with VHA facilities after adjustment for a number of demographic attributes (Wright et al., 2006).
Access to Care
On discharge from the active-duty military, a portion of veterans (8.57 million of a total of about 22.23 million in FY 2011) enroll in the VA health care system (VA, 2012d). To balance demand with resources, VHA uses health care enrollment priority groups (see Box 7-1). The threshold for enrollment changes on the basis of available resources.
The amount of time it takes veterans to get an appointment to visit a VHA clinician varies widely from one clinic to another. Harada et al. (2002) reported that one of veterans’ highest points of dissatisfaction with VHA was the wait time for an appointment. In 2010, nearly all primary care appointments at VHA facilities occurred within 30 days of the desired date (Walters, 2011). In 2011, the standard for primary care appointments was changed to 14 days, which was already the standard for mental health appointments. Data were not available to describe whether VHA has been able to meet the 14-day standard. However, a review by the VA Office of the Inspector General (VA-OIG) found that many veterans waited more than 14 days past their desired appointment date for their mental health appointments (VA, 2012k). In addition, the VA-OIG determined that the “VHA overstated its success in providing veterans new and follow-up appointments for treatment within 14 days.” The principal reasons for wait times to exceed the established standard were inconsistent application of procedures by VHA schedulers and too few mental health clinicians on staff.
Location of VHA facilities affects veterans’ access to care. VHA has over 1,000 facilities, including VAMCs and outpatient clinics, but they are geographically dispersed, and not every veteran has easy access to one (Reisinger et al., 2012). For example, 43% of veterans live in rural areas that may not be readily served by VHA facilities (Walters, 2011). A VA review on interventions to improve access to care found that as distance from a VHA facility increased there was decreased use of outpatient services and that the greatest decrease occurred for distances up to 60 miles from the facility (Kehle et al., 2011). The relationship between facility distance from home and care use was consistent for physical health and mental health appointments. VHA is developing strategies to bring health care to rural veterans through such means as mobile health clinics, telehealth programs, and health care partnerships (Walters, 2011).
In its review, VA evaluated whether integration of primary care and mental health care would increase veterans’ access to mental health services (Kehle et al., 2011). Both integrating mental health services into primary care clinics and offering primary care in mental health clinics showed promise, but more research on these models is needed.
Veterans have access to their medical records through the VA’s My HealtheVet system (VA, 2012i). Furthermore, they can download their medical records and read, print, or save them to a computer using the Blue Button program (VA, 2012b). Veterans can self-enter several types of information in My HealtheVet, including personal health indicators (such as blood pressure, weight, and heart rate), emergency contact information, names of health care providers, laboratory test results, family health history,
BOX 7-1
Department of Veterans Affairs (VA) Health Care Enrollment Priority Groups
Group 1: Veterans with VA-rated service-connected disabilities 50% or more disabling; and veterans determined by VA to be unemployable due to service-connected conditions.
Group 2: Veterans with VA-rated service-connected disabilities 30% or 40% disabling.
Group 3: Veterans who are Former Prisoners of War (FPOWs); veterans awarded a Purple Heart medal; veterans whose discharge was for a disability that was incurred or aggravated in the line of duty; veterans with VA-rated service-connected disabilities 10% or 20% disabling; veterans awarded special eligibility classification under Title 38, U.S.C. ![]() 1151, “benefits for individuals disabled by treatment or vocational rehabilitation”; and veterans awarded the Medal of Honor.
1151, “benefits for individuals disabled by treatment or vocational rehabilitation”; and veterans awarded the Medal of Honor.
Group 4: Veterans who are receiving aid and attendance or housebound benefits from VA; and veterans who have been determined by VA to be catastrophically disabled.
Group 5: Non-service-connected veterans and noncompensable service-connected veterans rated 0% disabled by VA with annual income and/or net worth below the VA national income threshold and geographically-adjusted income threshold for their resident location; veterans receiving VA pension benefits; and veterans eligible for Medicaid programs.
Group 6: World War I veterans; Compensable 0% service-connected veterans; veterans exposed to ionizing radiation during atmospheric testing or during the occupation of Hiroshima and Nagasaki; Project 112/Shipboard Hazard and Defense (SHAD) participants; veterans exposed to the defoliant Agent Orange while serving in the Republic of Vietnam between 1962 and 1975; veterans of the Gulf War that served between August 2, 1990, and November 11, 1998; veterans who served in a theater of combat
operations after November 11, 1998, as follows: (a) currently enrolled veterans and new enrollees who were discharged from active duty on or after January 28, 2003, are eligible for the enhanced benefits for 5-years post-discharge; (b) veterans discharged from active duty before January 28, 2003, who apply for enrollment on or after January 28, 2008, are eligible for this enhanced enrollment benefit through January 27, 2011. Note: At the end of this enhanced enrollment priority group placement time period, veterans will be assigned to the highest Priority Group their unique eligibility status at that time qualifies them for.
Group 7: Veterans with gross household income below the geographi-cally adjusted income threshold for their resident location and who agree to pay co-pays.
Group 8: Veterans with gross household income above the VA national income threshold and the geographically adjusted income threshold for their resident location and who agree to pay co-pays.
a. Veterans eligible for enrollment: Noncompensable 0% serviceconnected and: Subpriority a: Enrolled as of January 16, 2003, and who have remained enrolled since that date and/or placed in this subpriority due to changed eligibility status; Subpriority b: Enrolled on or after June 15, 2009, whose income exceeds the current VA National Income Thresholds or VA National Geographic Income Thresholds by 10% or less.
b. Veterans eligible for enrollment: Nonservice-connected and: Subpriority c: Enrolled as of January 16, 2003, and who have remained enrolled since that date and/or placed in this subpriority due to changed eligibility status; Subpriority d: Enrolled on or after June 15, 2009, whose income exceeds the current VA National Income Thresholds or VA National Geographic Income Thresholds by 10% or less.
c. Veterans not eligible for enrollment: Veterans not meeting the criteria above: Subpriority e: Noncompensable 0% service-connected; and Subpriority g: Nonservice-connected.
SOURCE: VA, 2012f.
and military health history. Military service information, such as service dates and deployment periods, is also included in veterans’ records.
Disability Compensation for Undiagnosed Illnesses
The diagnoses that Gulf War veterans receive have a direct effect on their ability to obtain disability compensation. In 1995, compensation for service-connected chronic disabilities due to undiagnosed illnesses was established (38 CFR Sec. 3.317). The original regulation specified that the illness had to be manifested during the Gulf War or during the 2 years after conclusion of service. The regulation was amended three times to extend the manifestation period and clarify the intent of the regulation; the last change was published in 2011 (76 F.R. 250 [December 29, 2011]). In addition to an undiagnosed illness, the regulation allows compensation for a medically unexplained CMI that is defined by a cluster of signs or symptoms.
Because of the complexity of the disability patterns and the law governing Gulf War disability rating policy, VA produced a training letter for regional Veterans Benefits Administration (VBA) personnel, explaining the rules for disability compensation for undiagnosed illness and a medically unexplained CMI (VA, 2010). The letter and additional materials are sent to examiners to explain how to evaluate Gulf War veterans’ chronic disabilities more effectively (VA, 2012e). The training letter should eliminate some of the confusion surrounding VA’s disability-compensation policy; however, a veteran must receive a qualifying diagnosis before applying for disability compensation.
VA and DOD administer a joint pre-discharge program so that service members can file claims for disability compensation up to 180 days before separation or retirement from military service (VA, 2012c). Three components make up the pre-discharge program: the Benefits Delivery at Discharge program (BDD), Quick Start, and the Integrated Disability Evaluation System (IDES). BDD allows service members to apply for disability compensation from VA before separation or retirement (VA, 2008). To receive VA disability compensation within the goal of 60 days after separation, veterans must submit their claims 60–180 days before release from active duty. The goal of the Quick Start program also is to give service members the opportunity to apply for disability compensation from VA while still on active duty (VA, 2009b). However, unlike the BDD program, it is targeted to service members who have fewer than 60 days remaining on active duty, full-time reserve or National Guard members, and others who do not meet the BDD criteria requiring availability of all evaluations before discharge. The goals of the IDES program are to provide “a single disability exam conducted to VA standards that will be used by both Departments [VA and DOD], a single disability rating completed by VA that is binding
upon both Departments, and expeditious payment of VA benefits within 30 days of a service member’s separation from service” (Rooney, 2012b; VA, 2012c). The IDES program includes a medical examination, but the program is administrative and independent of clinical care and treatment (Rooney, 2012b). Under the IDES program, the wait time for veterans to receive disability compensation from VA and DOD has decreased from an average of 240 days in 2007 (before implementation of the IDES program) to an average of 50 days in 2012 (Rooney, 2012a).
In 2009, the number of pre–September 2001 Gulf War–era veterans who had service-connected undiagnosed illnesses and received health care through VHA was 18,002, or nearly 0.3% of the total Gulf War–era cohort (VA, 2011d), compared with 2,980 in 2000 and 4,439 in 2005.3
Data are available on the numbers of pre–September 2001 Gulf War– era veterans who have been granted disability compensation for their undiagnosed illnesses. In FY 2009, the number was 24,409 (VA, 2011d), and that was substantially higher than in previous years—for example, it was 6,109 in FY 2000 and 7,322 in FY 2005. Because not all veterans receive their health care through VHA, it is not possible to determine whether the veterans who are identified as having an undiagnosed illness in the VHA system overlap with the veterans who are receiving disability compensation through VBA.
VA has estimated that a higher percentage of veterans of the Iraq and Afghanistan wars (about 45%) have applied for disability compensation compared to veterans of the 1991 Gulf War (about 20%) (Hickey, July 18, 2012). The average number of medical conditions claimed by the Iraq and Afghanistan war veterans is 8.5. Information was not found on the categories of medical conditions for which the veterans of the Iraq and Afghanistan wars are receiving disability compensation.
AN APPROACH TO ORGANIZING SERVICES FOR CARE OF
VETERANS WHO HAVE CHRONIC MULTISYMPTOM ILLNESS
As noted above, VA, in conjunction with DOD, has already committed in principle to expeditious completion of a disability examination for soldiers who are leaving active duty (Rooney, 2012b; VA, 2012c). However, the disability examination process is independent of clinical care and treatment. A PACT team will be incapable of properly managing a veteran who
_____________
3VA (2011b) defines an undiagnosed illness as “a chronic disability which manifested either during active military, naval, or air service in the Southwest Asia theater of operations during the Gulf War, or to a degree of 10 percent or more not later than December 31, 2011. Additionally, the disability cannot be attributed to any known clinical diagnosis by history, physical examination, and laboratory tests.”
has CMI or any of its common comorbidities without a comprehensive health assessment and without a definitive disability determination. A comprehensive health assessment is a prerequisite for producing a comprehensive personal care plan, for engaging the patient as a partner in managing the care plan, and for determining the resources that will be needed for the particular veteran’s team to execute the care plan. It is patently impossible to accomplish that in the context of a PACT clinic under ordinary operating conditions. In the absence of a comprehensive health assessment, a veteran who has CMI cannot receive high-quality care. With respect to the disability determination, maximum symptom resolution and functional capacity cannot be reached until pending disability dispositions are resolved. Disability is a fluid phenomenon and must be reassessed periodically, but this is not an acceptable argument for deferring disability determination beyond the time when a PACT primary care clinician is expected to initiate a comprehensive personal care plan. Thus, without a comprehensive health assessment and a disability determination, a PACT cannot provide an adequate medical home and a veteran cannot get high-quality care.
The postseparation comprehensive health assessment is useful not only for initiating care but for making initial triage decisions. VHA already has in place a basic setup for a stepped care system for veterans who have CMI. Most CMI patients can and should be managed in an ordinary PACT setting with appropriate adjustments as discussed below. In larger settings, such as VAMCs, there may be a sufficient concentration of CMI patients and a sufficient concentration of interested clinicians to justify the development of a dedicated CMI-PACT or CMI clinic days in a particular PACT made up of interested and expert primary care clinicians, behavioral health clinicians, pain specialists, neurologic consultants, physical rehabilitation clinicians, multiple care coordination and measurement-based management resources, patient-education experts, and others as needed. A needs assessment would show what expertise is necessary and what adjustments are necessary in the clinical constitution of the CMI-PACT team. It is known from experience with, for example, pediatric special-needs clinics that a fully adequate concentration of dedicated human resources, functioning well as a team, is expensive but cost-effective in managing patients who have complex conditions (McAllister et al., 2007; Murphy et al., 2011). Disability care coordination organizations, which coordinate care for people with disabilities who often have multiple, complex physical health, mental health, and psychosocial comorbidities, have also demonstrated the effectiveness of a team approach (Mastal et al., 2007; Palsbo and Ho, 2007; Palsbo et al., 2006). A CMI-PACT team might require six or eight full-time-equivalent clinical professionals, or even more, for the comprehensive and orderly management of 1,000 veterans who have active CMI and its associated comorbidities. Such a clinic may be useful as a consultation center for
less severely affected patients whose continuing care is managed in more distant, less well resourced PACTS. Perhaps 5–10% of veterans who have CMI might benefit from such a referral. A more extremely affected subset, perhaps 0.5%–1.0%, might need referral to a center of excellence, such as a WRIISC, where deep expertise is available and state-of-the-art modalities are being developed. The criteria for stepping care up to the next level of intensity will generally include difficulty of managing or failure to manage symptoms adequately, but the criteria would be specified, and the transition needs to be managed so that continuity of care is achieved, consistency is maintained, and communication between sites of care is ensured. Many lapses in quality occur during transitions of care to different settings, so VHA should monitor closely and periodically evaluate the adequacy of communication and the coordination of care among settings when care is stepped.
As noted above, most veterans who have CMI can be managed in a PACT, but care in this setting will fail unless the PACT can adjust the visit schedule to accommodate extended, complex visits; access the specific team members and clinical expertise needed to follow the care plan, including nonclinic care and follow-up; and master the implementation strategies necessary to incorporate the multitude of relevant CPGs, to master team-based care, to navigate the delicate territory between team-based care and developing an accountable personal relationship with patients, and to incorporate self-management strategies into the fabric of the personal care plan. VHA has many of those elements already available and ready to be organized into a system that can render excellent care to veterans who have CMI.
Perhaps the most important of those preconditions is VHA’s commitment to make the time available to the primary care team to address the multiple issues that these patients are dealing with. No matter how deep and available the expertise of team members and no matter how successfully implementation is carried out, the primary care team will fail unless it has enough time. Studies of somatizing patients have shown that they can consume substantially more resources than those used by comparable patients who are not so afflicted (Bermingham et al., 2010; Burton et al., 2012; Konnopka et al., 2012; Reid et al., 2002). Clinic visits themselves take longer because many symptoms are interacting with one another in unique and ever-changing ways that require frequent adjustments in the care plan. Multiple team members will need time together to integrate their varied expertise into a coherent and internally consistent plan. It takes time to negotiate competing priorities and to set priorities among and sequence interventions, for example, to work out how a course of cognitive behavioral therapy can be fit into a physical rehabilitation program and how to adjust the timing of several medications. Much PACT-based care can be
rendered without a visit, by using the telephone, computer, smart telephone, or other modalities; it takes time to plan, record, communicate, and integrate a care plan that is executed through these modalities. And it takes time to learn to function as a team, to maintain team-based care skills, and to meet together as a team to assign responsibilities for elements of the plan.
VHA can be viewed as the largest health education and health professional training institution in the nation, and it has active interprofessional team training programs in palliative care and geriatrics; it has recently extended interprofessional team-based training into a small number of primary care settings (VA, 2011f). VHA has begun routinely incorporating behavioral health and complementary medicine professionals into PACT teams, as have DOD and civilian patient-centered medical homes (PCMHs). Those laudable efforts should be dramatically expanded so that all PACTs consist of teams whose members have been systematically trained to work together and are given time to do so. Preclinic huddles, team meetings to hammer out complex care plans, joint interprofessional training, communication to consolidate the multiple “touches” that various team members have made in executing a care plan, and, above all, time dedicated to developing and maintaining healthy team dynamics are prerequisites of successful team-based care. Such an investment will pay more than it costs in reduced hospitalizations, emergency department visits, consultant charges, and diagnostic testing. An occasional averted hospitalization will buy a year’s worth of care management and behavioral health consultation.
The Institute for Healthcare Improvement (IHI) breakthrough collaborative series offers a useful model for promoting and maintaining organizational change from a continuous quality-improvement perspective by facilitating the emergence of a “learning network.” A continuous quality-improvement approach communicates that change is continuous and sustained and provides evidence about the degree of change within the organization. IHI has recommended the Plan Do Study Act (PDSA) cycle with specific and clear goals for changing practices and assessing whether a change is an improvement (see Figure 7-1). The approach also acknowledges that change and improvement are not immediate or one-shot and that they take time. The idea that mistakes can be identified and corrected is built into the cycle. Continuous quality improvement also allows for incorporation of new models of care, such as integrative medicine and optimal healing environments, into the PACT care process when they are needed (IOM, 2009; Jonas and Chez, 2004). Periodic program evaluation is essential to determine whether the process put onto paper and disseminated throughout VHA is being applied (Walter et al., 2010).
VA clinicians have already demonstrated the capacity to use PDSA methods for quality improvement. The model should be applied to the care of patients who have CMI.
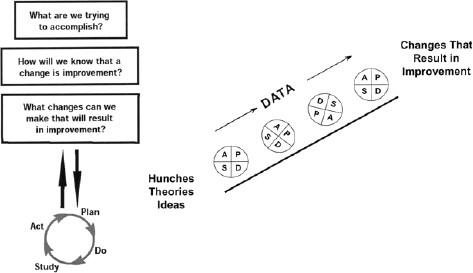
FIGURE 7-1 Institute for Healthcare Improvement Plan Do Study Act model.
SOURCE: Reproduced with permission from IHI (Institute for Healthcare Improvement).
Dissemination and implementation of new guidelines require a long-term perspective and the creation of a clinical-care environment in which continuous change in systems of care is the norm. Organizational-level change demands changes in procedures or systems, active communication and marketing of innovation, training, measurement and monitoring, and engagement of key stakeholders (Ruzek and Rosen, 2009).
Implementation science is an emerging field; it is turning out to be highly technical and surprisingly distinct from clinical science in its methods and outcomes. Implementation of multiple guidelines for management of chronic conditions is difficult, requiring complex teamwork by staff who are otherwise fully engaged in caring for patients in distress. Successful implementation has its own measures of success that are distinct from clinical outcomes. It is difficult to implement change in clinics that are highly stressed, that are seriously understaffed, or that operate under rigid directives that discourage flexible problem solving. Successful implementation is a highly local process—best practices do not all look the same—that requires an accurate appraisal of initial conditions and the application of active problem-solving skills. For example, one clinic may reprogram an appointment clerk to become the telephone-based part of the care-management system, and another may be able to use a dedicated care manager for this task. At the heart of successful implementation is the capacity to find workarounds; to sequence elements according to local strengths,
opportunities, constraints, and preferences; and especially to address unexpected difficulties and unintended consequences. It is also necessary to collect data systematically on processes of care, on how to effect process change when necessary, on the results of changes with respect to intermediate outcomes, on what works and what does not, and on unintended consequences of changes. The implementation team must be prepared not only to collect information but to reflect on its implications and to act on it with the next process-adjustment cycle. Practice redesign requires a series of linked incremental steps—it is not accomplished in one step. The PDSA method described above has been used successfully in a variety of primary care settings to improve practice.
Implementation work that uses the PDSA method has a unique approach. If changes in disease-specific outcomes are used as the principal measure of success, valuable progress can occur. The road to improved disease state is long and difficult—it is actually many roads—and is beset with so many problems that it requires an approach to dealing with many unexpected problems. Progress needs to be measured by success in solving operational and functional problems that appear one after another, not just in improved disease outcomes. An improved disease state will appear only after a long run of successful interim problem-solving steps.
Many primary care practice redesign organizations (such as TransforMed, HealthTeamWorks, and the Institute for Clinical Systems Improvement) have learned that practice coaches are highly useful (or indispensable) to practices as they begin their redesign efforts. Thus, implementation teams should include health coaches, integrative-medicine practitioners, and other local practice resources that can help practices to work out local changes and solutions to the problem of implementing multiple CPGs for their own unique patient-panel demands under variable local conditions.
The value of learning collaboratives or learning communities must be stressed. Practices, coaches, and other forms of technical support are valuable, but local practice teams often benefit most from the experience of their peers in similar circumstances, and periodic meetings in which ideas and solutions can be exchanged will pay handsome dividends.
Thus, implementation success depends on teams that work well together, that practice active creative problem solving, that maintain flexibility, and that persist in the face of failure—that demonstrate resilience, the ability to learn and improve. Progress toward complete implementation of a guideline is measured in terms of successfully solving one after another the small problems that arise in the course of PDSA work. Use of metrics can lead to improved care and ultimately lead to healthier patients and better outcomes.
A practice that is ready for successful redesign cannot be understood by looking only at workflow; it must also be assessed for active, flexible
problem solving. Over time, such a practice can be expected to have shaped workflow to solve the problems of the particular patients in the panel with the particular resources at hand.
SELECT MODELS OF CARE USED BY OTHER ORGANIZATIONS
As noted above, most veterans receive some of or all their care outside the VHA system of clinics in the civilian sector. Civilian settings are more variable and generally less well resourced, and their clinicians are generally less able to devote the time needed to manage CMI and its attendant comorbidities properly in the context of a busy daily practice. Stepped care is much harder in the civilian setting, because specialty resources are less available. Perhaps most important, primary care clinicians in the civilian setting are less familiar with the characteristics of CMI in veteran populations and therefore less adept at creating the complex personal care plans described above. Nevertheless, PCMHs are rapidly appearing in this sector, and the practice-redesign efforts necessary to produce PCMHs will benefit veterans who have CMI and are seeking care—particularly if VHA can extend its resources to these practices. A civilian PCMH that is rendering care to veterans who have CMI would benefit from the following:
• Notification from VHA of the names, disability status, comprehensive health assessment, and other medical care records of the veterans under care, as allowed under the Health Insurance Portability and Accountability Act.
• VHA CPGs applicable to the specific patients, particularly those related to time allocations and team expertise.
• Recommended care-team membership for the patients.
• Access, via telehealth or other ECHO-like variations, to specific team members who have the expertise necessary for the management of the patients, such as neurologists adept at managing traumatic brain injury or acupuncturists adept at pain management.
• Access to consultation with or referral to VAMCs, WRIISCs, and other resources that may benefit veterans as specific problems arise that cannot be managed adequately in the civilian PCMH.
DISSEMINATING EVIDENCE-BASED GUIDELINES THROUGH
THE DEPARTMENT OF VETERANS AFFAIRS SYSTEM
The flow of evidence-based information (EBI)—knowledge transfer— through a system to influence policy and practice has become a major topic of focus in the era of evidence-based medicine. It is particularly important when the sheer volume of research data appears to have only slight
influence on clinician-practice behaviors. As a result, research has shifted attention from mere generation of guidelines to concerns about their dissemination and implementation (Grimshaw and Russell, 1993; Thomas et al., 1999). Knowledge transfer, some suggest, may occur in three stages: diffusion, dissemination, and implementation (Lomas, 1993). The stages are characterized by increasing specificity, targeting, and customization, leading, in theory, to the adoption of new information that changes practice and policy. Successful models of knowledge transfer do not yet exist (French et al., 2012), but recent work is offering some useful insights into the processes that potentially would help in disseminating EBI, such as practice guidelines. It is instructive to elucidate the three stages and the distinctions among them before discussing the relevance of knowledge transfer in treating for CMI by clinicians in the VA health system.
Diffusion is a passive process that involves spread of EBI with little attention to specificity in defining the target audience or to the customization of the information itself. Publication of studies in professional journals or coverage of scientific studies in the mass media may garner a widespread audience for the message (Viswanath et al., 2008) but may or may not attract the attention of clinicians and patients unless they are already attuned to the topic. Although print media may remain an important source for some physicians and patients, few physicians read medical journals for the latest scientific findings, given the sheer amount of published literature, busy schedules, and possible lack of suitability in how the information is presented (Lomas, 1993; Thomas et al., 1999). Patient-related factors may also act as barriers to using EBI (Thomas et al., 1999).
Dissemination is more deliberate flow of information toward a defined target audience, and the information itself is more customized. Examples include evidence reviews, practice guidelines, and consensus statements.
Implementation goes beyond reaching the intended audience, clinicians. The new information is actually used to change practice behaviors. Given its more ambitious goal, implementation is facilitated by a sharper focus on addressing organizational barriers to the adoption of EBI (Ramanadhan et al., 2012). Localization and customization of EBI will go a long way in facilitating implementation. Appropriate incentives and sanctions may help in this phase. Implementation of guidelines for treatment of veterans who have CMI was discussed in detail earlier in this chapter.
Channels or sources on which physicians rely for EBI, the nature of the information and messages that appeal to them, and the conditions that improve or hinder their capacity to use EBI define the target audience and guide the methods used to approach them. Diffusion and dissemination, in theory, could create awareness about new developments or consensus guidelines but do not necessarily address the day-to-day reality of the clinicians in VHA. They are, however, critical in creating the necessary
“readiness for change” in practice behaviors. Change in practice behaviors requires “enabling factors” that address barriers that deter implementation (Lomas, 1993). Behavior change is most likely when environmental changes accompany dissemination of EBI. System changes and support systems will also reinforce changed practice behaviors and may enable their maintenance.
CLINICIANS’ BEHAVIOR CHANGE: SYSTEM
AND INTERPERSONAL DETERMINANTS
The role of clinicians is critical in any adoption of health care innovations, and much of the adoption and maintenance of innovations requires change in clinicians’ behaviors (Gunter and Whittal, 2010). The literature of a variety of fields—including communication, sociology, marketing, psychology, and business—offers useful pointers to understanding how practice behaviors could potentially be changed.
• Peer networks, such as the learning communities described above, have a profound influence on adoption of new behaviors and skills (Bernstein et al., 2009; IOM, 2012; Ramanadhan et al., 2010). Peers could potentially introduce new information, norms, and skills in a network and thereby facilitate the adoption of EBI. Some peers could model new behaviors and skills, making learning of new skills smoother. A network of peers in which communication and informal transfer are routine may lead to the emergence of “learning organizations” in which acquisition of new information, skills, and behaviors can be made routine.
• Opinion leaders and champions, particularly in local health centers, may carry considerable weight in the community of clinicians, facilitating behavior changes and making adoption of new practices acceptable (Moore et al., 2004). One study of knowledge transfer of evidence-based technology that included screening, brief intervention, and referral to treatment conducted in emergency departments found that having local staff as champions made a big difference in adoption and maintenance of a new practice (Bernstein et al., 2009).
• The role of leadership is critical in overcoming barriers to implementation as it ensures quality control, endorsement, priority setting, and the creation of an overall climate of innovation support (Yano et al., 2012).
• Behaviors that are substantive departures from existing practices could be more difficult to change; in a similar vein, complex interventions in contrast to simpler interventions are difficult to implement
and less likely to be adopted (McGovern et al., 2004; Rogers, 1995).
• Organizational constraints—such as inflexible rules, lack of incentives, and potential for negative sanctions—can deter EBI-based changes in practice.
• New methods for connecting EBI to practice, such as appropriate methodology, could link evidence to practices better in the context of the reality of clinical variation.
The advent of information and communication technologies has enabled the development of decision-support systems that facilitate the adoption of recommendations. Decision-support systems, particularly ones that draw on such electronic health records as those used by VA, may provide patient-specific information to a clinician when needed in a manner that is user-friendly. These systems are especially effective when they are user-friendly, easily available, and part of a physician’s work flow (Thomas et al., 1999). Thomas et al. (1999) argued that such design considerations as easier navigation, clear indexing, and forgiving interfaces enhance the utility of communication technologies to facilitate behavior change.
As asserted earlier, customization is a critical element in facilitating adoption of innovations. A recommended innovation should be flexible, easy to try out, and customizable to local conditions, and it should have some advantage over current practices (Rogers, 1995). Customization demands careful audience segmentation and designing of intervention components that meet the needs of segments of the audience. In one study, VA tried a social marketing approach to disseminate a new model of collaborative care to treat depression (Luck et al., 2009). In the model, the intervention targeted not just the physicians but other staff, such as local leaders, frontline staff, and managers; it focused on cultural change in the larger organization. Marketing was also reported to be a critical determinant in the national dissemination of a new model to promote collaborative care for depression in the VA system (Smith et al., 2008). Those efforts, in theory, reduce resistance from people in an organization to adopt innovations and ease the change in clinician behaviors.
VHA faces extraordinary challenges in caring for the burgeoning population of veterans who have CMI. It is possible to meet the challenges with adequate clinician education and support, organization and preparation of care teams that fit the needs of the veterans, establishment of implementation protocols that lead to continuous quality improvement, dissemination of these successes to other clinical teams and settings that are struggling
with similar problems, and extension of VHA resources to civilian settings, where most veterans receive their care.
Arora, S., S. Kalishman, D. Dion, D. Som, K. Thornton, A. Bankhurst, J. Boyle, M. Harkins, K. Moseley, G. Murata, M. Komaramy, J. Katzman, K. Colleran, P. Deming, and S. Yutzy. 2011. Partnering urban academic medical centers and rural primary care clinicians to provide complex chronic disease care. Health Affairs 30(6):1176-1184.
Bermingham, S. L., A. Cohen, J. Hague, and M. Parsonage. 2010. The cost of somatisation among the working-age population in England for the year 2008-2009. Mental Health in Family Medicine 7(2):71-84.
Bernstein, E., D. Topp, E. Shaw, C. Girard, K. Pressman, E. Woolcock, and J. Bernstein. 2009. A preliminary report of knowledge translation: Lessons from taking screening and brief intervention techniques from the research setting into regional systems of care. Academic Emergency Medicine 16(11):1225-1233.
Budzi, D., S. Lurie, K. Singh, and R. Hooker. 2010. Veterans’ perceptions of care by nurse practitioners, physician assistants, and physicians: A comparison from satisfaction surveys. Journal of the American Academy of Nurse Practitioners 22(3):170-176.
Burton, C., K. McGorm, G. Richardson, D. Weller, and M. Sharpe. 2012. Healthcare costs incurred by patients repeatedly referred to secondary medical care with medically unexplained symptoms: A cost of illness study. Journal of Psychosomatic Research 72(3):242-247.
Chou, R., A. Qaseem, V. Snow, D. Casey, J. T. Cross Jr., P. Shekelle, and D. K. Owens. 2007. Diagnosis and treatment of low back pain: A joint clinical practice guideline from the American College of Physicians and the American Pain Society. Annals of Internal Medicine 147:478-491.
French, S. D., S. E. Green, D. A. O’Connor, J. E. McKenzie, J. J. Francis, S. Michie, R. Buchbinder, P. Schattner, N. Spike, and J. M. Grimshaw. 2012. Developing theory-informed behaviour change interventions to implement evidence into practice: A systematic approach using the theoretical domains framework. Implementation Science 7(38).
Furey, P. 2012 (unpublished). Analysis of the Social Media Discussion of Chronic Multi-Symptom Illness in Veterans of the Iraq and Afghanistan Wars. Analysis commissioned by the Committee on Gulf War and Health: Treatment of Chronic Multisymptom Illness, Institute of Medicine, Washington, DC.
Gibson, T. B., T. A. Lee, C. S. Vogeli, J. Hidalgo, G. S. Carls, K. Sredl, S. DesHarnais, W. D. Marder, K. B. Weiss, T. V. Williams, and A. E. Shields. 2009. A four-system comparison of patients with chronic illness: The military health system, Veterans Health Administration, Medicaid, and commercial plans. Military Medicine 174(9):936-943.
Grimshaw, J. M., and I. T. Russell. 1993. Effect of clinical guidelines on medical practice: A systematic review of rigorous evaluations. Lancet 342(8883):1317-1322.
Gunter, R. W., and M. L. Whittal. 2010. Dissemination of cognitive-behavioral treatments for anxiety disorders: Overcoming barriers and improving patient access. Clinical Psychology Review 30(2):194-202.
Harada, N. D., V. M. Villa, and R. Andersen. 2002. Satisfaction with VA and non-VA outpatient care among veterans. American Journal of Medical Quality 17(4):155-164.
Hickey, A. A. 2012 (July 18). Statement of Allison A. Hickey, Under Secretary for Benefits, Veterans Benefits Administration (VBA), U.S. Department of Veterans Affairs (VA). In House Committee on Oversight and Government Reform, Subcommittee on National Security, Homeland Defense, and Foreign Operations. http://oversight.house.gov/wp-content/uploads/2012/07/7-18-12-Hickey-Testimony.pdf (accessed September 29, 2012).
Hunt, S. C. 2012 (unpublished). VA Approaches to the Management of Chronic Multi-Symptom Illness in Gulf War I Veterans. Presentation at the Third Committee Meeting, April 12, 2012, Irvine, CA.
Hynes, D. M., K. Koelling, K. Stroupe, N. Arnold, K. Mallin, M. W. Sohn, F. M. Weaver, L. Manheim, and L. Kok. 2007. Veterans’ access to and use of Medicare and Veterans Affairs health care. Medical Care 45(3):214-223.
IOM (Institute of Medicine). 2009. Integrative Medicine and the Health of the Public: A Summary of the February 2009 Summit. Washington, DC: The National Academies Press.
IOM. 2012. Best Care at Lower Cost: The Path to Continuously Learning Health Care in America. Washington, DC: The National Academies Press.
Jonas, W. B., and R. A. Chez. 2004. Toward optimal healing environments in health care. Journal of Alternative and Complementary Medicine 10:S1-S6.
Katzman, J. 2012. Making connections: Using telehealth to improve the diagnosis and treatment of complex regional pain syndrome, an underrecognized neuroinflammatory disorder. Journal of Neuroimmune Pharmacology. Published online October 2, 2012.
Kehle, S. M., N. Greer, I. Rutks, and T. J. Wilt. 2011. Interventions to Improve Veterans’ Access to Care: A Systematic Review of the Literature. Health Services Research &Development Service, Department of Veterans Affairs, Washington, DC.
Konnopka, A., R. Schaefert, S. Heinrich, C. Kaufmann, M. Luppa, W. Herzog, and H. H. Konig. 2012. Economics of medically unexplained symptoms: A systematic review of the literature. Psychotherapy & Psychosomatics 81(5):265-275.
Lincoln, A. E., D. A. Helmer, A. I. Schneiderman, M. Li, H. Copeland, M. K. Prisco, M. T. Wallin, H. K. Kang, and B. H. Natelson. 2006. The war-related illness and injury study centers: A resource for deployment-related health concerns. Military Medicine 171(7):577-585.
Lomas, J. 1993. Diffusion, dissemination, and implementation: Who should do what? Annals of the New York Academy of Sciences 703:226-237.
Luck, J., F. Hagigi, L. E. Parker, E. M. Yano, L. V. Rubenstein, and J. E. Kirchner. 2009. A social marketing approach to implementing evidence-based practice in VHA QUERI: The TIDES depression collaborative care model. Implementation Science 4:64.
Mastal, M. F., M. E. Reardon, and M. English. 2007. Innovations in disability care coordination organizations: Integrating primary care and behavioral health clinical systems. Professional Case Management 12(1):27-36.
McAllister, J. W., E. Presler, and W. C. Cooley. 2007. Practice-based care coordination: A medical home essential. Pediatrics 120(3):e723-e733.
McGovern, M. P., T. S. Fox, H. Y. Xie, and R. E. Drake. 2004. A survey of clinical practices and readiness to adopt evidence-based practices: Dissemination research in an addiction treatment system. Journal of Substance Abuse Treatment 26(4):305-312.
Moore, K. A., R. H. Peters, H. A. Hills, J. B. LeVasseur, A. R. Rich, W. M. Hunt, M. S. Young, and T. W. Valente. 2004. Characteristics of opinion leaders in substance abuse treatment agencies. American Journal of Drug and Alcohol Abuse 30(1):187-203.
Murphy, N. A., P. S. Carbone, Council on Children With Disabilities, and American Academy of Pediatrics. 2011. Parent-provider-community partnerships: Optimizing outcomes for children with disabilities. Pediatrics 128(4):795-802.
Nicholas, W., D. O. Farley, M. E. Vaiana, and S. Cretin. 2001. Putting Practice Guidelines to Work in the Department of Defense Medical System. Santa Monica, CA: RAND Corporation.
Palsbo, S. E., and P. S. Ho. 2007. Consumer evaluation of a disability care coordination organization. Journal of Health Care for the Poor and Underserved 18(4):887-901.
Palsbo, S. E., M. F. Mastal, and L. T. O’Donnell. 2006. Disability care coordination organizations: Improving health and function in people with disabilities. Lippincott’s Case Managment 11(5):255-264.
Petersen, L. A., M. M. Byrne, C. N. Daw, J. Hasche, B. Reis, and K. Pietz. 2010. Relationship between clinical conditions and use of Veterans Affairs health care among Medicare-enrolled veterans. Health Services Research 45(3):762-791.
Petzel, R. A. 2012. What does the future look like for VA healthcare? U.S. Medicine: the Voice of Federal Medicine, http://www.usmedicine.com/outlook/what-does-the-future-look-like-for-va-healthcare.html (accessed September 28, 2012).
Ramanadhan, S., J. Weicha, S. Gortmaker, K. M. Emmons, and K. Viswanath. 2010. Informal training in staff networks to support dissemination of health promotion programs. American Journal of Health Promotion 25(1):12-18.
Ramanadhan, S., J. Crisostomo, J. Alexander-Molloy, E. Gandelman, M. Grullon, V. Lora, and K. Viswanath. 2012. Perceptions of evidence-based programs among community-based organizations tackling health disparities: A qualitative study. Health Education Research 27(4):717-728.
Reid, S., S. Wessely, T. Crayford, and M. Hotopf. 2002. Frequent attenders with medically unexplained symptoms: Service use and costs in secondary care. British Journal of Psychiatry 180:248-253.
Reinhard, M. J. 2012 (unpublished). Complementary and Alternative Medicine (CAM) and Chronic Multi-symptom Illness. Presentation at the Second Committee Meeting, February 29, 2012, Washington, DC.
Reisinger, H. S., S. C. Hunt, A. L. Burgo-Black, and M. A. Agarwal. 2012. A population approach to mitigating the long-term health effects of combat deployments. Preventing Chronic Disease 9:E54.
Ren, X. S., L. Kazis, A. Lee, W. Rogers, and S. Pendergrass. 2001. Health status and satisfaction with health care: A longitudinal study among patients served by the Veterans Health Administration. American Journal of Medical Quaityl 16(5):166-173.
Rogers, E. M. 1995. Diffusion of Innovations. 4th ed. New York: The Free Press.
Rooney, J. A. 2012a. Testimony Before the Senate Committee on Veterans Affairs. Hearing on Seamless Transition: Review of the Integrated Disability Evaluation System. 112th Cong. 2nd Sess. May 23, 2012. http://veterans.senate.gov/hearings.cfm?action=release.display&release_id=5a948325-1c39-4251-81a7-a724f9b58c15 (accessed September 28, 2012).
Rooney, J. A. 2012b. Directive-Type Memorandium (DTM) 11-015—Integrated Disability Evaluation System (IDES). Washington, DC: Department of Defense.
Ruzek, J. I., and R. C. Rosen. 2009. Disseminating evidence-based treatments for PTSD in organizational settings: A high priority focus area. Behaviour Research and Therapy 47(11):980-989.
Smith, J. L., J. W. Williams, R. R. Owen, L. V. Rubenstein, and E. Chaney. 2008. Developing a national dissemination plan for collaborative care for depression: QUERI series. Implementation Science 3.
Stroupe, K. T., D. M. Hynes, A. Giobbie-Hurder, E. Z. Oddone, M. Weinberger, D. J. Reda, and W. G. Henderson. 2005. Patient satisfaction and use of Veterans Affairs versus non– Veterans Affairs healthcare services by veterans. Medical Care 43(5):453-460.
Thomas, K. W., C. S. Dayton, and M. W. Peterson. 1999. Evaluation of Internet-based clinical decision support systems. Journal of Medical Internet Research 1(2):E6.
Tinetti, M. E., T. R. Fried, and C. M. Boyd. 2012. Designing health care for the most common chronic condition–multimorbidity. Journal of the American Medical Association 307(23):2493-2494.
VA (Department of Veterans Affairs). 2008. Benefits Delivery at Discharge (BDD): A Joint VA-DOD Initiative. VA Pamphlet 21-08-1.
VA. 2009a. Controlled Breathing Techniques. War Related Illness and Injury Study Center. Palo Alto, CA.
VA. 2009b. Quick Start. http://www.vba.va.gov/predischarge/quickstart.htm (accessed September 29, 2012).
VA. 2009c. Self-Management: Giving Veteran Patients Tools to Take Control of Their Own Health—A Resource for Health Care Providers. War Related Illness and Injury Study Center. East Orange, NJ.
VA. 2010 (unpublished). Training letter 10-01: Adjudicating Claims Based on Service in the Gulf War and Southwest Asia. http://www.ngwrc.org/docs/VAtl10-01.pdf (accessed September 28, 2012).
VA. 2011a. Caring for Gulf War I Veterans. http://www.publichealth.va.gov/docs/vhi/caring-for-gulf-war-veterans-vhi.pdf (accessed March 11, 2013).
VA. 2011b. Complementary and Integrative Medicine: A Resouce for Veterans, Service Members and Their Families. War Related Illness and Injury Study Center. East Orange, NJ.
VA. 2011c. Excercise to Help Manage Chronic Pain and/or Fatigue: A Resource for Veterans, Service Members, and Their Families. War Related Illness and Injury Study Center. East Orange, NJ.
VA. 2011d. Gulf War Era Veterans Report: Pre-9/11 (August 2, 1990 to September 10, 2001). Washington, DC: Department of Veterans Affairs. http://www.va.gov/vetdata/docs/SpecialReports/GW_Pre911_report.pdf (accessed September 28, 2012).
VA. 2011e. Medically Unexplained Symptoms: A Resource for Veterans, Service Members, and Their Families. War Related Illness and Injury Study Center. East Orange, NJ.
VA. 2011f. VA Centers of Excellence in Primary Care Education. http://www.va.gov/oaa/rfp_coe.asp (accessed September 19, 2012).
VA. 2012a. Analysis of VA Health Care Utilization Among Operation Enduring Freedom (OEF), Operation Iraqi Freedom (OIF), and Operation New Dawn (OND) Veterans. http://www.publichealth.va.gov/docs/epidemiology/healthcare-utilization-report-fy2012-qtr2.pdf (accessed September 12, 2012).
VA. 2012b. Blue Button. http://www.va.gov/BLUEBUTTON/index.asp (accessed October 24, 2012).
VA. 2012c. Chapter 10 transition assistance. In Federal Benefits for Veterans, Dependents and Survivors. http://www.va.gov/opa/publications/benefits_book/benefits_chap10.asp (accessed November 29, 2012).
VA. 2012d. Department of Veterans Affairs Statistics at a Glance. http://www.va.gov/vetdata/docs/Quickfacts/Stats_at_a_glance_FINAL.pdf (accessed September 19, 2012).
VA. 2012e. Gulf War Veterans’ Illnesses Task Force Report. http://www.va.gov/opa/publications/2011_GWVI-TF_Report.pdf (accessed September 28, 2012) VA. 2012f. Health Benefits Priority Groups Table. http://www.va.gov/healthbenefits/resources/priority_groups.asp (accessed November 19, 2012).
VA. 2012g. Health Care: Patient Centered Care. http://www.va.gov/health/newsfeatures/20120827a.asp (accessed November 19, 2012).
VA. 2012h. Improving Quality of Care. http://www.qualityandsafety.va.gov/qualityofcare/improving-quality-of-care.asp (accessed November 19, 2012).
VA. 2012i. My HealtheVet. https://www.myhealth.va.gov/index.html (accessed October 24, 2012).
VA. 2012j. Patient Aligned Care Team (PACT). http://www.va.gov/primarycare/pcmh/ (accessed September 28, 2012).
VA. 2012k. Review of Veterans’ Access to Mental Health Care. VA Office of Inspector General, Veterans Health Administration. http://www.va.gov/oig/pubs/VAOIG-12-00900-168.pdf (accessed September 28, 2012).
VA. 2012l. War Related Illness and Injury Study Center: What We Do. http://www.warrelatedillness.va.gov/WARRELATEDILLNESS/about-us/what-we-do.asp (accessed September 28, 2012).
VA and DOD (Department of Defense). 2001a. Clinical Practice Guideline for Post-Deployment Health Evaluation and Management, Version 1.2. http://www.healthquality.va.gov/pdh/PDH_cpg.pdf (accessed September 28, 2012).
VA and DOD. 2001b. Clinical Practice Guideline for the Management of Medically Unexplained Symptoms: Chronic Pain and Fatigue. http://www.healthquality.va.gov/mus/mus_fulltext.pdf (accessed September 28, 2012).
VA and DOD. 2009a. Clinical Practice Guideline for the Management of Substance Use Disorders (SUD). http://www.healthquality.va.gov/sud/sud_full_601f.pdf (accessed September 28, 2012).
VA and DOD. 2009b. Clinical Practice Guideline: Management of Concussion/Mild Traumatic Brain Injury. http://www.healthquality.va.gov/mtbi/concussion_mtbi_full_1_0.pdf (accessed September 28, 2012).
VA and DOD. 2009c. Clinical Practice Guideline: Management of Major Depressive Disorder (MDD). http://www.healthquality.va.gov/MDD_FULL_3c.pdf (accessed September 28, 2012).
VA and DOD. 2010a. Clinical Practice Guideline For Management of Post-Traumatic Stress. http://www.healthquality.va.gov/ptsd/PTSD-FULL-2010a.pdf (accessed September 28, 2012).
VA and DOD. 2010b. Clinical Practice Guideline: Management of Opioid Therapy for Chronic Pain. http://www.healthquality.va.gov/COT_312_Full-er.pdf (accessed September 28, 2012).
VA and DOD. 2011. Manual for Facility Clinical Practice Guideline Champions. https://www.qmo.amedd.army.mil/general_documents/Champion_Manual.pdf (accessed September 28, 2012).
Viswanath, K., K. D. Blake, H. I. Meissner, N. G. Saiontz, C. Mull, C. S. Freeman, B. Hesse, and R. T. Croyle. 2008. Occupational practices and the making of health news: A national survey of US health and medical science journalists. Journal of Health Communication 13(8): 759-777.
Walter, J., I. D. Coulter, A. Adler, P. D. Bliese, and R. Nicholas. 2010. Program evaluation of total force fitness in the military. Military Medicine 175(8):103-109.
Walters, T. 2011 (unpublished). Institute of Medicine Committee on Gulf War and Health: Treatments for Multi-Symptom Illness, December 12, 2011, Washington, DC.
West, A. N., W. B. Weeks, and A. E. Wallace. 2008. Rural veterans and access to high-quality care for high-risk surgeries. Health Services Research 43(5):1737-1751.
Wright, S. M., T. Craig, S. Campbell, J. Schaefer, and C. Humble. 2006. Patient satisfaction of female and male users of Veterans Health Administration services. Journal of General Internal Medicine 21 (Suppl 3):S26-S32.
Yano, E. M., L. W. Green, K. Glanz, J. Z. Ayanian, B. S. Mittman, V. Chollette, and L. V. Rubenstein. 2012. Implementation and spread of interventions into the multilevel context of routine practice and policy: Implications for the cancer care continuum. Journal of the National Cancer Institute Monograph (44):86-99.




























