these diets are at work, perhaps in combination with fiber, in lowering the risk for these chronic diseases.
Can Too Much Fiber Be Bad?
Some health experts have raised the concern that high-fiber diets may make it difficult for the body to absorb important minerals from the digestive system. This does not appear to happen, however. For example, vegetarians eating high-fiber diets have normal levels of iron, zinc, copper, and selenium in their bodies. Similarly, the levels of iron, calcium, and magnesium are the same in people with diabetes who eat a high-fiber diet and in those who eat the average U.S. diet. The conclusion seems to be that there is little evidence that high-fiber diets alone will produce a mineral deficiency in people who otherwise consume a balanced diet.
You should be aware, however, that switching abruptly from a low-fiber diet to one high in fiber may make you feel bloated and nauseous and may cause flatulence. This is particularly true if the increased fiber comes from wheat bran and guar gum. These effects are temporary, though, and diminish after a few weeks. On the plus side, a high-fiber diet reduces constipation and contributes to more regular bowel movements. You are likely to be more comfortable if you gradually increase your intake of fiber-rich foods.
One final word on fiber—do not start taking fiber supplements based on what you have read here. There is an impressive amount of evidence showing the beneficial effects of eating a diet containing a large amount of fruits and vegetables (i.e., fiber-containing foods), and relatively low levels of meat and fatty products. We do not know, yet, whether the benefits of such a diet are the result of the large amounts of fiber and carbohydrates, low amounts of fat, other protective factors in plants, a combination of the three, or some other dietary factor. Therefore, although it is desirable to eat a diet containing fiber-rich foods, it is not necessary to take fiber supplements unless specifically advised to do so by your doctor.
Chapter 8
VITAMINS, MINERALS, AND CHRONIC DISEASES
Vitamins and minerals are a diverse group of substances that play an enormous number of roles in the body. Compared to proteins, carbohydrates, and fats, the body needs very small amounts of these nutrients to remain in good working order, and yet eating too little or too much of them can be physically devastating.
Today, it is rare for people in the United States to suffer from severe vitamin or mineral deficiencies; those disorders, such as rickets and pellagra, are not the subject of this chapter. Instead, we are more likely to consume too much of some minerals and not quite enough of other minerals and vitamins. One of the goals of the Eat for Life guidelines, in fact, is to ensure that you get adequate amounts of these nutrients as part of your usual eating pattern. Therefore by simply following the Eat for Life guidelines, you will be eating foods that provide you with sufficient vitamins and minerals. This chapter reviews the evidence linking slight deficiencies or excesses of vitamins and minerals to a number of chronic diseases.
VITAMINS
In this section only those vitamins thought to have some connection with chronic disease are discussed.
Vitamin A
The body gets vitamin A from two different sets of chemicals—retinoids and carotenoids. Vitamin A itself is the compound retinol. It and the similar compounds belonging to the retinoid family occur only in foods of animal origin, such as liver, butter, milk, and egg yolks.
The body can also make vitamin A from select members of the carotenoid family of compounds, which are present in dark-green, leafy vegetables and in yellow and orange vegetables and fruits. The most common carotenoid is beta-carotene. Enzymes in the small intestine split beta-carotene (and certain closely related carotenoids) to produce vitamin A.
Food labels and nutritional tables state the "vitamin A activity" in a particular product or food. This value, stated in international units (I.U.), reflects how much vitamin A in total—vitamin A, other retinoids, and carotenoids that yield the vitamin—the body gets from that product. Another unit for measuring vitamin A activity is the retinol equivalent (RE). The relationship between REs and I.U.s of vitamin A depends on the form of the vitamin. For example, 1 RE equals 3.33 I.U. of retinol or 10 I.U. of beta-carotene.
Early epidemiologic studies of diet and cancer focused on foods with vitamin A activity but did not distinguish between the retinoids and the carotenoids. For example, studies found that cigarette smokers who eat a large amount of foods containing vitamin A activity were less likely to develop lung cancer than people who did not eat such foods. Later, researchers showed that it was the carotenoids, and not vitamin A or other retinoids, that exerted the protective effect. Because of the results, doctors are now trying to determine the
effect of dietary beta-carotene supplements on lung cancer. The results of these experiments will be some time in coming.
Similar tests are under way in which scientists want to determine if beta-carotene can prevent other cancers from developing. These experiments were prompted by studies showing that people who ate foods rich in beta-carotene had lower rates of a variety of cancers, including those of the stomach, cervix, bladder, mouth, larynx, and esophagus. None of these studies were particularly convincing, however, and so we must await the results of further research before we proclaim beta-carotene an all-around cancer preventative.
Retinol and other retinoids have been shown to be protective against experimentally induced cancers in several animal species. The role of retinoids in the prevention or treatment of human cancer is being tested in studies being conducted in a number of different locations.
Vitamin C
Vitamin C (also known as ascorbic acid), perhaps more than any other vitamin, has long been a favorite of those claiming that certain nutrients can prevent cancer and other chronic diseases. The problem with most studies of vitamin C as a cancer preventative is that foods rich in vitamin C also contain other nutrients—fiber, vitamin A, and vitamin E, for example—that may have a protective effect as well.
What researchers have found so far is that vitamin-C-containing foods, and possibly vitamin C itself, may protect against some cancers. The strongest evidence for such a protective effect is with stomach cancer; the evidence for cancer of the esophagus is not as convincing.
Vitamin C may also play a role in preventing atherosclerosis, although, again, the studies conducted so far have not been particularly convincing. One study found that people with atherosclerosis had low levels of vitamin C in their blood
stream, implying that these people were not getting enough of the vitamin in their diets. In another study, volunteers under age 25 who took 1-gram (g) supplements of vitamin C [well above the recommended levels] each day experienced a drop in their serum cholesterol levels. Older volunteers did not show a consistent change in cholesterol level when they took the vitamin C supplement.
On the whole, the evidence presented above does not warrant taking large doses of vitamin C as a supplement. Nevertheless, it is a good idea to include plenty of food rich in vitamin C in your diet.
Vitamin D
Vitamin D's main purpose is to increase the amount of calcium in the body and thus increase the amount of calcium that goes into bones. The vitamin does this in several ways. First, it boosts the intestine's ability to absorb calcium from digested food. In addition, vitamin D improves the kidneys' capacity to recycle calcium that might otherwise pass from the blood stream into the urine.
Thus it is not surprising that scientists have been looking for a connection between inadequate consumption of vitamin D and two bone diseases, osteoporosis and osteomalacia. Osteoporosis is a disease in which the bones lose mass (both minerals and bone matrix), eventually leading to fractures in older people. Osteomalacia is a disorder of adults in which bones become soft because the ratio of mineral to the protein component of bone decreases. This disease is known as rickets when it occurs in children.
In countries with limited sunlight, or where the people dress in a fashion that reduces exposure to sunlight, there is a higher incidence of osteomalacia and rickets than in places where the inhabitants get plenty of sunshine (or vitamin D from food). Northern China, Great Britain, Scandinavia, countries
in the Middle East, and other Muslim countries are among those in which osteomalacia is relatively common.
With osteoporosis the situation is more complicated. It is true that women with osteoporosis have lower levels of vitamin D in their blood than women who do not have the disease. However, efforts to treat osteoporosis with the active form of vitamin D have had mixed results. On the one hand, people who receive the treatment show higher levels of calcium in their blood stream, suggesting that their intestines are more efficient at absorbing calcium from food sources. But despite the higher calcium levels in their blood, the treated group's bones do not contain any more calcium than the bones of people with osteoporosis who are not treated with the vitamin.
Vitamin E
Countless newspaper and magazine stories have touted vitamin E supplements as an effective cancer preventive. However, study after study has failed to find any connection between the amount of vitamin E people eat and their risk for cancer. A few studies have found, however, that if selenium consumption is low, then an inadequate amount of vitamin E can increase the risk of breast and lung cancer.
Riboflavin
For over 30 years, scientists have suspected that low levels of riboflavin may increase the risk of developing cancer of the esophagus. Although no definite connection has ever been made, a number of studies suggest that low levels of riboflavin may allow alcohol or substances in chewing tobacco to promote cancer of the esophagus. So, if you drink alcoholic beverages or chew tobacco, make sure your diet contains some riboflavin-rich foods.
Vitamins and Alcoholism
One of the most consistent findings in research on vitamins is that alcoholics are often deficient in many of these nutrients, including vitamins B6 and B12, thiamin, riboflavin, niacin, and folacin. In fact, alcoholism is probably the number one cause of most cases of multivitamin deficiency in the United States.
In many instances, vitamin deficiencies are tied to the liver damage that develops after years of heavy drinking. In other cases, alcohol damages the intestines' ability to absorb vitamins from the digested food. And then there is the problem of alcoholic malnutrition: alcoholics tend to get a large share of their calories from alcohol, and they do not eat enough of other foods. As a result, their consumption of many vitamins is very inadequate.
MINERALS
Food contains dozens of minerals in varying amounts. Some of these are known to be essential nutrients. Others are toxic, although in amounts that greatly exceed the amount consumed in a normal U.S. diet. And then there are those that just happen to be present in the foods we eat, serving no apparent purpose but doing no apparent harm. Every once in a while, new research shows that some mineral in this latter group is, in fact, essential in very small amounts, or perhaps toxic in amounts larger than we consume ordinarily.
The discussion in this section skips those minerals in which there is no strong connection between consumption and disease as well as those minerals, such as lead and cadmium, that are toxic in large amounts but are not related to chronic diseases at the levels found in food.
Calcium
For many people in the United States, getting enough calcium is a constant challenge. In general, dairy products are very good sources of calcium. In fact, it is difficult to get adequate levels of this mineral without eating these foods.
Low calcium intake is almost certainly connected to osteoporosis. Human bones reach their maximum mass at about age 25 to 30, so it is imperative that children, teenagers, and young adults eat calcium-rich foods. To achieve peak bone mass, the Committee on Diet and Health recommended that adolescents and young adults 11 to 25 years of age consume about 1200 mg of calcium per day. Once bones reach their maximum mass, they stabilize for the next 10 to 20 years, and the need for this mineral drops to 800 mg/day. Then, between ages 35 and 45, bones start losing their calcium (even if the diet is high in calcium), a process that accelerates in women immediately before and after menopause.
If calcium intake is low during childhood and adolescence, bones will not develop to the fullest extent possible, which later in life could translate into weaker bones and eventually osteoporosis. In a survey of women in 12 countries, researchers found a direct relationship between high calcium consumption and low risk for osteoporosis. Women in Finland consumed the largest amount of calcium—about 1300 mg/day—and had the lowest number of fractures. In contrast, among Japanese women, who ate the lowest amount of calcium—a mere 400 mg/day—fractures were the most common.
One way of countering bone loss as we age might be to take calcium supplements. However, tests conducted to date have been disappointing. In fact, the most effective way for women at risk for developing osteoporosis to avoid this disorder is to receive estrogen treatment after menopause, which virtually stops bone loss completely. For women who cannot
or will not take estrogen therapy, calcium plus vitamin D supplementation may slow bone loss to a degree.
Fluoride
In the late 1930s, scientists began studies that would lead to one of the most significant advances in public health. These researchers were investigating whether there was a relationship between the fluoride content of water and the prevalence of tooth decay. There was, and since 1949 communities across the country have added fluoride to drinking water, helping to produce a dramatic reduction in the number of cavities we now develop.
How good is fluoride at preventing cavities? Children who live for a few years in a community with optimal fluoride levels in drinking water have up to 60 percent fewer cavities. Despite the unparalleled success of fluoridation, more than 45 percent of the U.S. population still drinks water with less than optimal levels of fluoride. To address this need, the American Dental Association, the American Academy of Pediatrics, and the American Academy of Pediatric Dentistry have issued guidelines, shown in Figure 8.1, for giving children fluoride supplements.
If you think you or your children do not receive an adequate amount of fluoride in your drinking water, see your physician. It is important not to take too much fluoride because this can actually damage teeth.
Iron
Iron is an essential element, present in all body cells. It is part of the hemoglobin found in red blood cells, where its main function is to carry oxygen in the blood stream. It is also an important component of certain enzymes. Good food sources of iron include red meats, poultry, fish, whole and enriched grain products, and dark-green leafy vegetables.
Iron-deficiency anemia is the most obvious disorder related
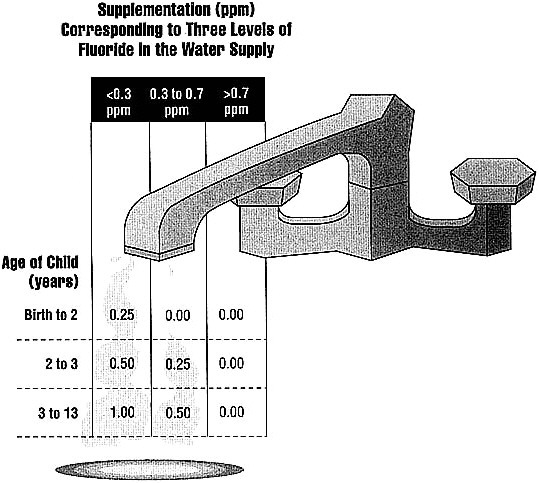
FIGURE 8.1 Recommended daily fluoride supplements for children in three age categories, based on fluoride concentration in the water supply.
SOURCE: Recommendations by the Council on Dental Therapeutics of the American Dental Association, by the Committee on Nutrition of the American Academy of Pediatrics, and by the American Academy of Pediatric Dentistry.
to iron. It is also the most common and widespread nutritional disease in the world, though its overall prevalence in the United States is low compared with its prevalence in the rest of the world. Poor nutrition in infants and small children and blood loss and pregnancy in adults are the most frequent causes of iron deficiency. You might also be depriving yourself of iron if you do not eat many calories in the first place.
Women are particularly vulnerable to this cause of iron deficiency because they eat less food than men to begin with, but their requirements for iron are greater because they lose iron during menstruation. This may be one of the few cases where taking supplements is warranted, though you should do so only on the advice of your physician.
Potassium
The evidence is clear that for people with high blood pressure, potassium is one dietary factor that exerts a beneficial effect. This is partly because potassium lowers blood pressure and partly because it also protects against stroke and damage to blood vessels when blood pressure is high.
Several studies have shown that groups of people who eat low-potassium diets have an increased incidence of high blood pressure and heart disease. In addition, diets high in potassium and low in sodium can lower blood pressure. An intake of 3.5 g/day of potassium is associated with lower blood pressure and fewer deaths from strokes. All you have to do to get to this level of potassium is eat the five or more servings of fruit and vegetables a day recommended in the Eat for Life guidelines.
Sodium
Sodium is an essential nutrient, but the amount consumed by most people—mostly in the form of salt (sodium chloride)—well exceeds the amount needed for normal body function. Although the average adult needs no more than several hundred milligrams of sodium a day, surveys show that people consume between 4 and 5.8 g (4000 to 5800 mg) a day.
Although researchers have been studying the relationship of sodium to high blood pressure since the turn of the century, there is still some controversy about the importance of salt in regulating blood pressure. Many studies have shown, for example, that the higher a culture's average salt consumption, the higher the average blood pressure.
The controversy concerns what happens when individual people consume more or less salt—the effect on blood pressure varies tremendously. People differ greatly in their sensitivity to salt. In some, blood pressure is affected to a large extent by the amount of salt they eat. But other people can












