The committee was charged with identifying measures of quality for the Leading Health Indicators (LHIs), and in this chapter it provides a starter set of measures identified by developing detailed versions of the logic models introduced in Chapter 1 for four of the LHI topic areas: tobacco; environmental quality (the air quality LHI); obesity, nutrition, and physical activity; and maternal, infant, and child health.
As noted earlier, the committee believes that the purpose of measurement is threefold. Assessment can be conducted simply for the purpose of monitoring and reporting about the health of a population; this can be done to provide a comparison with other jurisdictions or nations, or to mobilize interested parties. Measures can be used in the work of quality improvement, whether organization-wide or in a specific program. And measures can be used for accountability, for example, to report back to funders, partners, legislators, and communities. More extensive discussion of the three purposes of measurement is provided in the Institute of Medicine (IOM) report For the Public’s Health: The Role of Measurement in Action and Accountability (2011a, p. 3, et seq.).
In addition to the criteria outlined in Chapter 2, several other issues are important when selecting measures of quality. The level of measurement is important, for example. Some of the LHIs are national in scope and dependent on national-level data, but they may be of secondary importance in some local jurisdictions. One of the challenges in measurement is the paucity of truly granular health data at the local level and the capability to access and analyze the data that are available. A variety of novel strategies for data collection and analysis are needed to expand the data sources available to local public health planners and their system partners. Data relevant to health are also available from non-health sources, such as police records and school data, as well as other non-
traditional sources such as Google Maps for parks and Chamber of Commerce and trade groups for businesses and tax revenues. As one example of evolution in analytical capabilities, Srebotnjak and colleagues (2010) developed a novel methodology to estimate health trends (e.g., diagnosed diabetes) in counties and other small population areas. Their modeling approach allows health officials and researchers to use Behavioral Risk Factor Surveillance System (BRFSS) data for small-area estimation and validation. Advances in information and communication technology offer novel opportunities for data generation, such as crowd-sourcing data collection and analysis to support health improvement (e.g., through health behavior change) in the community (see, for example, Piniewski et al., 2011). A real-life application is offered by the experience with Global Positioning System (GPS)-equipped inhalers (i.e., the Asthmapolis sensor and mobile application system that produces “timely, comprehensive and objective data on the burden of asthma”1 but also supports remote monitoring of broncho-dilator use; see Van Sickle et al. [2013]). There are several challenges in creating novel data sources, including balancing business potential with public use, and addressing concerns about real and perceived threats to privacy, technical obstacles related to gleaning useful information from “big” data, and the cost of establishing and sustaining long-term data generation and analysis efforts. However, the potential of disruptive innovation to dramatically increase access to population health data is undeniable.
The committee did not conduct a systematic and comprehensive review of all potential measures related to the LHIs for several reasons. Such an undertaking would require time and resources (including a wider range of expertise) to research all effective interventions for a given outcome, and to identify and evaluate all candidate measures. The committee also believes that describing a framework and process for a continually updated set of measures could be of more lasting value than identifying a static set of measures. Finally, many measures of quality relate to the specific interventions implemented and are context specific. For this reason, too, describing a process seemed more useful than providing specific examples that would result from applying that process.
As discussed earlier, the LHIs are heterogeneous, and organizing them to support quality improvement is not a straightforward process. There are at least three ways to conceptually organize the Healthy People 2020 LHIs other than the alphabetical order presented in the Healthy People publications. They may be organized roughly according to the
___________________
1 Available at http://asthmapolis.com/public-health (accessed June 26, 2013).
ecological model,2 based on the type of “determinant” of health/level in the ecological model they occupy. They may be divided by locus of intervention (clinical/individual vs. population-based), al-though some LHIs fall somewhere in between. LHIs do not fit neatly into one level of the ecological model, and may be altered by interventions at both the individual and at the population level. Finally, the LHIs may be organized according to the committee’s logic model provided above: resources and capacity, interventions, healthy conditions, and healthy outcomes, with a focus on the latter two categories, which can “house” most of the LHIs (see Figure 3-1).
Table 3-1 provides a list of the LHIs organized according to the logic model (and shown in bold type), and showing areas for potential measures of quality related to the LHIs. The non-bolded entries represent non-LHI measures that are directly linked to an LHI (e.g., an intermediate outcome linked to the LHIs representing an ultimate health outcome) or found along the pathway that includes an LHI (e.g., morbidity from childhood disease is an ultimate outcome linked to the LHI childhood vaccines). The entries marked with an asterisk represent measures that are endorsed by the National Quality Forum (NQF), that met the criteria for inclusion in the County Health Rankings, or that met other criteria such as face validity in the case of measures that emerge from the evidence-based interventions recommended by the Guide to Community Preventive Services (population-based interventions) and the U.S. Preventive Services Task Force (USPSTF) (for interventions in the clinical

FIGURE 3-1 Health outcome logic model.
___________________
2 The ecological model is a diagram adapted from Dahlgren and Whitehead (1991) by an IOM committee and in Healthy People 2020 planning by the Department of Health and Human Services (HHS) to show the array of determinants of health, or the ecology of health, beginning with individual level factors at the center (biology/genetics), then on to behavior, family, social networks, and communities, followed by broad policies pertaining to the determinants of health (education, income, etc.) at the state and national level (see HHS, 2008; IOM, 2003a).
setting). The table is not intended to be comprehensive or exhaustive, but the committee hopes that it illustrates a step in the process of identifying measures of quality related to the LHI. A subsequent step would be the application of the criteria outlined in Chapter 2.
TABLE 3-1 The LHIs (in Bold Typeface) Organized According to the Logic Model and Showing Areas for and Examples of Potential Measures of Quality (in Regular Typeface)
| Resources and Capacity; Interventions | Healthy Conditions | Outcome |
| Females receiving reproductive health services (FP-7.1) |
Infant deaths (MICH-1.3) Preterm births (MICH-9.1) |
|
| Childhood vaccines (IID-8) | ||
| Students graduating with a regular diploma 4 years after starting 9th grade (AH-5.1)*a
|
TABLE 3-1
| Resources and Capacity; Interventions | Healthy Conditions | Outcome |
| Persons living with HIV who know their serostatus (HIV-13) | ||
| Adolescents (12-17 years old) using alcohol or any illicit drugs (SA-13.1) | Fatal injuries (IVP-1.1) | |
| Adults engaging in binge drinking (SA-14.3) | ||
| Air Quality Index (EH-1) Daily particulate matter days (PM2.5)* |
||
| Adults who smoke (TU-1.1)* | ||
| Suicides (MHMD-1) Adolescents experiencing major depressive episodes (MHMD-4.1) |
TABLE 3-1
| Resources and Capacity; Interventions | Healthy Conditions | Outcome |
| Homicides (IVP-29) | ||
| Persons using the oral health care system (OH-7) |
||
| Persons with a usual primary care provider (AHS-3) | ||
| Persons with medical insurance (AHS-1.1) |
||
| Adults with hypertension under control (HDS-12) |
TABLE 3-1
| Resources and Capacity; Interventions | Healthy Conditions | Outcome |
| Adults receiving colorectal cancer screening (C-16) | ||
| Adults meeting physical activity guidelines (PA-2.4) |
NOTE: Items marked with an asterisk (*) represent measures that are endorsed by NQF, met the criteria for inclusion in the County Health Rankings, or met other criteria (e.g., face validity in the case of measures that emerge from the evidence-based interventions recommended by the Guide to Community Preventive Services [population-based interventions] and the U.S. Preventive Services Task Force [for interventions in the clinical setting]).
a “The averaged freshman graduation rate measures the percentage of public high school students who graduate on time with a regular diploma” (Department of Education, National Center for Education Statistics, 2012, http://nces.ed.gov/programs/coe/analysis/2012-section5.asp [accessed June 1, 2013]).
TABLE 3-1
b Tworek et al., 2010.
c See Henschel et al., 2012, for a review of published studies of air pollution interventions which showed that improving air quality is associated with improved health outcomes (decreased respiratory and cardiovascular morbidity and mortality).
d Baxley and Miller, 2006.
e Fleegler et al., 2013, found that “a higher number of firearm laws in a state was associated with a lower rate of firearm fatalities in the state” controlling for a range of factors, but also concluded that additional research is needed to examine the nature of the association.
f OH-1.1: Reduce (by 10%, from 33.3% to 30.0%) the proportion of young children aged 3 to 5 years with dental caries experience in their primary teeth; OH-3.1: Reduce (by 10%, from 27.8% to 25%) the proportion of adults aged 35 to 44 years with untreated dental decay; OH-3.2: Reduce (by 10%, from 17.1% to 15.4%) the proportion of older adults aged 65 to 74 years with untreated coronal caries; and OH-3.3: Reduce (by 10%, from 37.9% to 34.1%) the proportion of older adults aged 75 years and older with untreated root surface caries.
g “The DGAs (2005 Dietary Guidelines for Americans) provide science based guidelines for food policy, food benefits, and nutrition education provided through the Federal nutrition assistance programs. The 2005 DGA Advisory Committee Report stated that ‘greater consumption of fruits and vegetables (5-13 servings or 2½-6½ cups per day depending on calorie needs) is associated with a reduced risk of stroke and perhaps other cardiovascular diseases, with a reduced risk of cancers in certain sites (oral cavity and pharynx, larynx, lung, esophagus, stomach, and colon-rectum), and with a reduced risk of type 2 diabetes (vegetables more than fruit). Moreover, increased consumption of fruits and vegetables may be a useful component of programs designed to achieve and sustain weight loss’” (USDA, 2008).
h Guide to Community Preventive Services, 2004.
The committee considered the quality improvement needs at all geographic levels, with the recognition that as one localizes quality improvement it becomes more important to have measures most relevant to the interventions chosen (which are intrinsically more process-oriented or structurally oriented) and which are more likely to be measurable and changeable at local levels. To reconcile these somewhat different objectives, the committee suggests that a well-developed portfolio of measures will have a core set of standard measures to be used at all levels (national, state, local), and a menu of additional options (largely process measures appropriate to specific settings) to be used as needed at the local level.
The priority areas or drivers of improvement of quality in public health identified in the work of the OASH (Honoré and Scott, 2010) are metrics and information technology; evidence-based practices, research, and evaluation; systems thinking; sustainability and stewardship; policy;
and workforce and education. As with the quality characteristics, these drivers cannot be linked directly to LHIs, but instead refer to the system’s underlying structural inputs illustrated by the Resources and Capacity box in Figure 3-1. For public health agencies, these may be linked with domains and measures employed in the Public Health Accreditation Board voluntary accreditation process. The drivers also seem somewhat related to the notion of foundational capabilities (part of a minimum package of public health services) proposed by a recent IOM report (2012). Those capabilities include the research infrastructure, information systems, and skills and workforce development for policy analysis and communication. That committee recommended that the minimum package, including the foundational capabilities, be used to establish new and robust approaches to demonstrating accountability, including linking funding inputs to outcomes in order to demonstrate value to funders and the public.
Below, the committee provides a “starter set” of measures of quality that could be considered in the development of a robust portfolio of measures for the nation, and for state and local jurisdictions. The committee used two approaches.
- The committee found that many of the LHIs included or led to one or more measures that can be used to measure quality (see Table 3-1).
- The committee developed case studies that applied the report’s health outcome logic model to the LHI topic areas of
a. tobacco use;
b. nutrition, physical activity, and obesity;
c. environmental quality; and
d. maternal, infant, and child health.
Finding 3-1: The committee finds that
a. Many of the Leading Health Indicators are measures of health outcomes or of conditions that can directly affect health outcomes and are, therefore, measures of the quality of the multisectoral health system.
b. The LHIs that meet the definition above of a quality measure can be used for assessment, improvement, and accountability. To be used thus, they must be relevant and measurable at the national, state, and local levels.
c. The LHIs reflect conditions or outcomes that directly contribute to the Healthy People 2020 foundation measures (e.g., general health status, health-related quality of life) and the ecologic model that underlies it.
The committee has developed concrete illustrations of the functioning of the logic model for four LHI topics and also more detailed explanation of activities for each LHI topic to help in the selection of metrics. Each case study lists the LHIs under the topic, provides a brief digest of the evidence and causal pathway(s) to which the LHI is an endpoint (ultimate outcome) or an intermediate outcome, provides a detailed logic model to illustrate the possible measures under Healthy Conditions and Health Outcomes, depicts the likely relationships among them, and offers both a list of possible measures and a shorter list of candidate measures (endorsed by NQF; based on evidence from the Guide to Community Preventive Services, the USPSTF, or equivalent, and for which data sources are available). The 1997 IOM report Improving Health in the Community: A Role for Performance Monitoring provides additional lists of potential measures organized by topic.
The detailed examples and their associated logic models provide an overview of resources, interventions, conditions, and outcomes that are related to specific and important health determinants and outcomes, and highlight the importance of the LHIs as components of these models. By explicitly describing these relationships, these models provide ideas for potential measures for assessing (1) the effectiveness of resources, programs, and actions on conditions that promote health, and (2) the impact of these conditions on outcomes. As the committee’s Recommendation 1-1 states, these conditions and outcomes are a reflection of the quality of the multisectoral health system. Similar models can be developed for other health determinants (or healthy conditions) and outcomes related to other Leading Health Indicators, or to other Healthy People objectives. These models can also facilitate the development of more detailed and quantitative systems models, such as Prevention Impacts Simulation Model (PRISM) and Population Health Model (POHEM), described earlier in this report, that can identify which components of these models make greater potential contributions to improved health conditions and outcomes. As mentioned above, evidence from studies and meta-analyses, such as those of the Guide to Clinical Preventive Services and Guide to Community Preventive Services, and practical knowledge sup-
port some of the logical relationships and connections in these models, but evidence to support—or refute—other relationships is sorely needed. Thus, another use of these models is to highlight relationships supported by scientific evidence that can already serve as the foundation for measures of health system quality, while also identifying other relationships in need of further study.
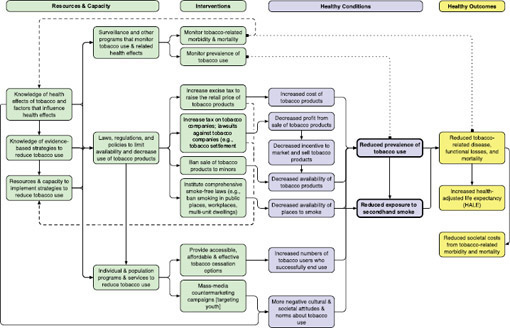
By way of illustration, the committee used the tobacco model to identify potential measures of quality. Outcome-related quality measures can be generated from “tobacco-related disease, functional losses, and mortality.” Obvious examples include lung cancer incidence and mortality, and the prevalence of and mortality from chronic obstructive pulmonary disease, to which tobacco use is a major contributor. There are several potential healthy condition-related quality measures that are suggested by the model. “Prevalence of tobacco use” is most closely related to outcomes and is the most obvious choice for a quality measure. The seven conditions shown that directly affect “prevalence of tobacco use” could next be reviewed for those which have the greatest potential impact, the best supporting scientific evidence for their effectiveness, and available data to track them (see Recommendation 2-2). Depending on need, one or more of these seven conditions could be selected to monitor performance of the health system. Most of the process measures in the model are supported by evidence and recommended by either the Clinical Guide or the Community Guide. Again, these require review using the selection criteria described in Recommendation 2-2. Because these actions and processes can be implemented at the state and local level, selecting one or more of them as the basis for a measure of state or local health system performance could provide more immediate feedback to local public health practitioners and stakeholders than relying on quality measures of conditions and outcomes, which change over a much longer time frame.
The case studies gave the committee an opportunity to consider the nine characteristics of public health quality and the six drivers of public health quality improvement as they relate primarily to the Resources and Capacity component of the logic model. As discussed in Chapter 1, in general, the nine characteristics cannot be directly linked with quality measures, since they primarily describe the system itself (e.g., population-centered, transparent, health-promoting) and the interventions undertaken to address health issues (a program or process or policy may be risk-reducing, or may be a manifestation of the system’s vigilance, or efficiency). Below, the committee provides tobacco use as an example for applying the nine characteristics of quality and the six drivers. Addi-
tionally, decision makers can maintain a focus on quality by asking themselves if an intervention being considered is consistent with the nine characteristics, or if it reveals something about the system that resonates with the nine characteristics. For example, in the case of the tobacco LHI, one would expect interventions in use or under consideration to be congruent with one of more of the following:
- effective: based on evidence about what works to decrease tobacco use and its initiation, and showing system (or an agency’s) capacity to identify and implement effective interventions;
- efficient: cost-effective, providing value on investment, demonstrating the capacity to invest wisely;
- equitable: reaching the appropriate target population, paying attention to vulnerable populations;
- health-promoting: ensuring that interventions to decrease tobacco use increase the probability of healthy conditions (including healthy behaviors) and outcomes;
- population-centered: intended to protect and promote health and healthy (e.g., smoke-free) environments for everyone;
- proactive: timely and responsive to emerging data and issues, and even able to predict and prepare (e.g., for legislative or regulatory challenges);
- risk-reducing: having identified areas of risk, this would reflect on the capacity of those implementing interventions to mitigate the probability of negative outcomes or protect against risk;
- transparent: for example, engaging the community, communicate openly about objectives and strategies, and make data and information widely available; and
- vigilant: include such activities as surveillance and simulation modeling to inform about what works and to what extent it is working.
The drivers of quality (population health metrics and information technology; evidence-based practices, research, and evaluation; systems thinking; sustainability and stewardship; policy; and public health workforce and education) are consistent with the foundational capabilities of public health described in the 2012 IOM report For the Public’s Health: Investing in a Healthier Future. These drivers refer to system elements that are needed for all topics and hence they are described here rather than for each case study to reduce redundancy. For example, systems
thinking, policy, and workforce considerations apply to most health improvement efforts, whether in tobacco use reduction or in decreasing pre-term births. Below, the committee discusses how the six drivers provide a clear starting point for improving quality in public health in the area of tobacco use. Specifically, health departments (and some of their partners in communities) will need
- The data and information technology capabilities to understand the extent and nature of tobacco use in their communities. This could be achieved independently, for large and better-resourced health departments, or through various collaborative arrangements for smaller health departments. This is also essential for information exchange with health care providers in the community. Gathering data about providers who implement the National Committee for Quality Assurance (NCQA) measure of asking about tobacco use at every patient encounter and providing counseling when needed could contribute considerably to improving tobacco use behaviors in their community and to public health officials’ understanding of how comprehensively an effective intervention is being delivered.
- The ability to conduct or access research and evaluation in order to enable evidence-based practice in tobacco use prevention and reduction. Quality measures in this area could be informed by building on an already robust evidence base.
- Systems thinking that recognizes the complex and reinforcing network of causes and effects that influences tobacco use. Factors contributing to smoking and other tobacco use behavior include social norms; the existence of adequate laws and policies and their enforcement, the availability of counseling and other smoking-cessation supports, health insurance coverage of smoking-cessation services including access to pharmacologic products (nicotine replacement therapy and others); and multiple actors who can influence tobacco use, such as the mass media, employers, local governments, and schools. Smoking, in turn, is a factor in the causal trajectories of cardiovascular disease, many cancers, respiratory diseases, and other health outcomes. Similarly to other LHIs, tobacco use is a health issue that involves many areas of society, including government, schools, workplaces, community organizations, and the mass and entertainment media. The ability to mobilize and sustain effective multisector
partnerships requires a skillset considerably linked with systems thinking.
- Sustainability and stewardship that have relevance to how interventions are crafted, for example, dedicating tobacco tax revenues to tobacco use prevention (rather than going to general revenues) and requiring the inclusion of nicotine replacement therapy in insurance coverage. Stewardship also offers an opportunity to talk about the health system and mutual accountability of diverse contributors for changes that improve health (see IOM, 2011a).
- Policy-development capabilities, including legal counsel and other expert staff who can advise local or state government about changes in policies, regulations, and laws to extend and sustain public health successes; this includes doing the research and health impact assessments, developing the legal framework, getting community support, engaging in advocacy, etc.
- Workforce and education, in particular, the need for public health department and community organization staff who are trained in policy analysis and development and in communication (including social marketing, the use of social media, etc.).
Resources and capabilities analogous to those described above are needed for improvement efforts related to most of the LHI topics.
Tobacco
There are two Leading Health Indicators under the LHI topic Tobacco Use: adults who are current cigarette smokers (TU-1.1) and adolescents who smoked cigarettes in the past 30 days (TU-2.2). (The Environmental Quality topic includes the related LHI “Children aged 3 to 11 years exposed to secondhand smoke” [TU-11.1].)
The committee applied the Health Outcome Logic Model to the topic of Tobacco Use. This included reviewing the evidence base on effective interventions, such as clinical services, programs, laws, and policies among other system inputs, the healthy conditions needed to decrease poor tobacco use–related outcomes, and finally, the intermediate and ultimate outcomes of decreased tobacco use. The committee identified a set of quality measures, and also explained how consideration of the six drivers of improvement of quality in public health would influence action to reduce tobacco use.
First, the committee reviewed how tobacco interventions and programs relate to health outcomes. A scan of the literature showed a strong evidence base for interventions that reduce or prevent the initiation of tobacco use. Recommendations on effective tobacco control interventions have been provided by the USPSTF, the Guide to Community Preventive Services, the Cochrane Collaboration, and others. Ending the Tobacco Epidemic, a 2010 HHS strategic plan, reviewed three additional authoritative sources on tobacco control programs (HHS, 2010). The common findings across all these sources are that the most effective programs are comprehensive, sustained, and accountable, and the HHS plan found that five specific types of interventions collectively reduce tobacco use: mass-media counter-marketing campaigns targeting youth; the adoption of comprehensive smoke-free laws; the availability of affordable tobacco-cessation options; excise tax increases that raise the retail price of tobacco products; and restrictions on advertising and promotion (HHS, 2010). Research has also shown that even when a population-level intervention has only modest effects on tobacco use behavior, the public health impact can be large (National Cancer Institute, 2000).
Second, the committee reviewed the literature on some of the inputs, such as system resources and capacity, programs, and policies. Examples include evidence that taxes and other policies are effective and may even bring in revenue and evidence that greater spending by states on specific types of tobacco interventions leads to the desired health outcomes, which are reductions in tobacco use, reductions in health conditions that result from tobacco use, and ultimately, increased healthy life expectancy. Research has shown that states and localities that have made substantial investments in comprehensive tobacco control programs have realized faster decreases in cigarette sales and smoking prevalence (HHS, 2010).
In its search for quality measures that could be used for the Tobacco Use LHIs, the committee found that NQF has endorsed a set of tobacco use measures. Most are for use in the clinical setting, and only two seem suited to the level of the total population: children who are exposed to secondhand smoke inside the home (a measure from the Maternal and Child Health Bureau of the Health Resources and Services Administration [HRSA]) and adult smoking prevalence (a measure from the Centers for Disease Control and Prevention [CDC]). However, there are no endorsed measures of population or community-level factors that influence tobacco use, such as the prevalence of smoke-free laws in a state or community (such as laws that ban smoking in multi-unit rental housing, a
factor that could play a role in child exposure to environmental tobacco smoke).
Making the best use of evidence about the effectiveness of many policy-based interventions to prevent and reduce tobacco use by both adolescents and adults requires a certain level of capacity within health departments, which are, according to the IOM Committee on Public Health Strategies to Improve Health, “a source of knowledge and analysis on community and population health” (the assessment and policy development functions of public health) and “a steward of the community’s health, assuring that policies and services needed for a healthy population are in place” (the policy development and assurance functions of public health) (IOM, 2012). Each community, state, or measure-endorsing entity could use the logic model described below to generate a portfolio of measures for comparison and improvement in the area of tobacco use. The logic model (see Figure 3-2, page 62) can also be used to assess local resources and capacities to implement interventions to reduce or prevent tobacco use.
Tobacco Use: Example Measures of Quality
Measures of Healthy Outcomes (Outcome Measures)
Lung cancer mortality
Prevalence of chronic obstructive pulmonary disease
Measures of Healthy Conditions (Intermediate Outcome Measures)
Percentage of adults who smoke
Unit price of tobacco products
Availability of tobacco products
Availability of smoking cessation programs
Insurance coverage for nicotine replacement therapy
Availability of policies regulating tobacco use in multi-unit housing
Percentage of active smokers trying to quit (Farkas et al., 1996)
Percentage of workplaces covered by smoke-free workplace policies
Measures of Interventions (Process) or Resources (Structure)
Comprehensive smoke-free laws
Mass-media counter marketing campaigns, especially targeting youth
Excise tax on tobacco products
Accessible, affordable, and effective tobacco cessation programs
The following measures are endorsed by NQF (measure steward provided in parentheses):
- Medical assistance with smoking and tobacco use cessation (NCQA)
- Screening and cessation interventions (American Medical Association [AMA] Convened Consortium for Performance Improvement)
- Adult current smoking prevalence (CDC)
- Risky behavior assessment or counseling by age 13 years (NCQA)
- Screening for abdominal aortic aneurysm in adult male smokers (ActiveHealth Management)
Nutrition, Physical Activity, and Obesity
There are four LHIs under the LHI topic Nutrition, Physical Activity, and Obesity: adults who meet guidelines on physical activity (aerobic and muscle strengthening), obese adults, obese children, and adequate vegetable intake in persons 2 years of age and older. These are process measures along the trajectory to the outcomes of premature mortality, such as from cardiovascular disease, complications of diabetes, and cancer.
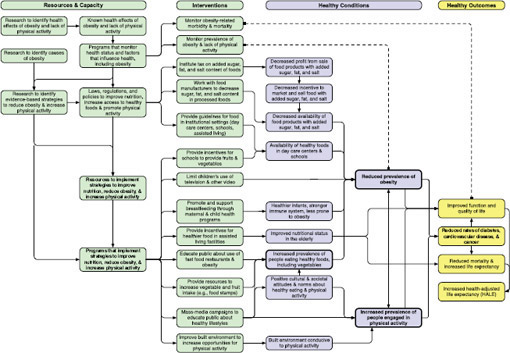
The evidence base in these related areas is growing rapidly, but it is not as robust as the evidence on interventions to reduce tobacco use; considerable gaps remain. Thus, the obesity model (and others) provided can be used to select potential quality measures, but it can also be used to identify components and relationships needing additional research. For example, several actions and processes depicted in the obesity model have face validity as potential quality measures, but lack scientific evidence about their effectiveness because of limited research. Even some of the conditions depicted in the model as contributing to “reduced prevalence of obesity” lack adequate scientific evidence about their effectiveness. The obesity example and model, therefore, provide fewer potential quality measures, particularly for processes and conditions, and
highlight the need for additional research. At this time, quality measures for this topic area might be limited to “prevalence of obesity,” for which there is good evidence about its impact on specific diseases and functional status, and outcomes with a direct link to obesity, such as diabetes, cardiovascular disease, and mobility.
Obesity is an area where multiple determinants of health are involved, and the causal pathways are extremely complex. In addition to individual level factors, such as genetics, there are behavioral factors that include nutrition and physical activity (and two of the LHIs measure these), and a wide range of factors in the built and social environment. The built and social environment factors include the availability and affordability of healthy foods, especially fruit and vegetables, in the community and in schools; the availability and quality of a public transportation system (associated with increased walking); and the quality of the built environment, including the density of fast food outlets, the availability of green spaces such as parks and walking or bike trails, and the existence of complete streets that allow safe access to pedestrians of varying physical ability and to bicycles (i.e., those with sidewalks, bike lanes, wheelchair ramps, and signals appropriate for people with vision impairments) (Gustat et al., 2012; McCormack and Shiell, 2011; Saelens and Handy, 2008). Socioeconomic status and race/ethnicity are linked in complex ways to the environmental characteristics just described, for instance, families and communities that live in or near poverty are more likely to live in environments that are less health-promoting. Social norms also play an important role in shaping public perception of eating and physical activity behaviors and environments, as they have in the case of tobacco use. Some process measures related to the LHI obesity have been identified, but additional research is needed to develop and validate relevant process measures or measures of intermediate outcomes and health conditions, such as walkability indices (Christian et al., 2011). Research on aspects of the built environment and the information environment (e.g., advertising) is ongoing. It will be important to establish whether menu labeling policies have an effect on consumer behavior and some early affirmative evidence is emerging (Krieger et al., 2013).
The logic model described below (see Figure 3-3, page 65) could be used by organizations identifying measures of quality (or a measure-endorsing entity) in the area of nutrition, physical activity, and obesity. The logic model can also be used to assess local resources and capacities to implement interventions to improve nutritional status and physical activity, and to reduce obesity.
Nutrition, Physical Activity, and Obesity: Example Measures of Quality
Measures of Outcome
Mortality rate from disease with obesity as a risk factor
Percent of overweight and obese adults
Percent of overweight and obese children
Expected quality of life in the population
Number of disability days due to obesity related disease
Number of quality nutrition programs available
Measures of Healthy Conditions (e.g., Intermediate Outcomes)
Number of adults with regular physical activity
Number of child hours watching television (or hours of screen time)
Number of adults following nutritional guidelines
Amount of calorie intake in diets
Number of hours children are active during school days
Number of months children were breastfed
Measures of Resources (Structure) or Interventions (Process)
Number of programs that promote physical activity for children
Availability of fresh fruits and produce
Nutritious meals available in school, day care, and assisted-living housing
Space available for physical activity in child care and school facilities
Menu labeling regulations
Average calories per meal purchased at chain restaurants
The following measures have been endorsed by NQF (measure steward provided in parentheses):
- Child overweight or obesity status based on parental report of body mass index (Maternal and Child Health Bureau, HRSA)
- Weight assessment and counseling for nutrition and physical activity for children and adolescents (NCQA)
Environmental Quality
There are two LHIs under Environmental Quality: (1) LHI 7: Air Quality Index (AQI) exceeding 100 (EH-1) and (2) LHI 8: Children aged 3 to 11 years exposed to secondhand smoke (TU-11.1). The set of objectives under the Environmental Quality topic includes the subtitles Outdoor Air Quality, Water Quality, Toxics and Waste, Healthy Homes and Healthy Communities, and Infrastructure and Surveillance. The objectives under Healthy Homes and Healthy Communities cover radon, mold, pesticides, and lead. This is an area where measures of the built environment, based on the evolving evidence base on effective interventions, would be useful in the future. Examples could include walkability, the proportion of the population close to public transit, the density of green and recreational spaces, etc. The LHIs in this area are limited and are only proxies for a broader range of environmental quality issues.
A review of the literature substantiates the associations between air pollution and poor health outcomes (for example, Henschel et al., 2012). Air Quality Index (AQI) “reports five most common ambient air pollutants that are regulated under the Clean Air Act: ground-level ozone, particle pollution (or particulate matter), carbon monoxide, sulfur dioxide, and nitrogen dioxide” (EPA, 20123). Although the AQI data (collected through the Environmental Protection Agency’s monitoring networks) are of high quality, the AQI has considerable geospatial limitations. For example, rural areas are generally not well represented. Also, given the placement of monitors (away from sources of high air pollution), the data collected may not be informative about the cumulative burden of air pollution in a certain area (California Department of Public Health, 2010).
The Guide to Community Preventive Services has recommended multi-trigger and multi-component interventions for asthma control, which would suggest that a composite measure of asthma-aggravating aspects of the environment could be helpful (housing quality in a given area, combined with air quality, and other factors). For air quality, an environmental quality index that can be used for rural and urban areas would be most useful at the local level. At the federal and state level, metrics such as proportion of vehicles that meet a miles-per-gallon threshold could be used.
The logic model provides an illustration of some of the potential areas for measurement related to the AQI indicator. (Children’s exposure to secondhand smoke is covered to some extent in the Tobacco Use logic
___________________
3 See http://www.epa.gov/o3healthtraining/aqi.html (accessed June 27, 2013).
model earlier in this chapter.) The available literature shows that the AQI is not the only available indicator in this area. The environment is one area where the local, state, and federal needs for quality measures (and the ability to act) may diverge greatly. In other words, the system inputs for environmental quality can be expanded beyond just air quality to also include water, housing, transportation, land use, and food, although data availability and measures may vary widely in each domain. For example, the built environment is an important determinant of health and of great local relevance, but it is harder to identify suitable measures of the built environment. There are several reasons for this. First, although the association between the built environment and health outcomes has support in the literature, the evidence base regarding effective interventions is incomplete and evolving. The Community Guide does provide recommendation on several types of interventions on the built environment (e.g., community scale urban design and land use) that are likely to have effects on physical activity.
In the area of indoor air quality, specifically, children’s exposure to secondhand smoke (SHS) (the second LHI in this topic), the UK National Institute for Clinical Excellence has found review-level evidence of effectiveness for the several classes of interventions (Taylor et al., 2005). A Cochrane review has also found sufficient evidence of effectiveness for legislative bans on smoking in workplaces and other indoor spaces, with evidence of great effectiveness of bans in hospitals (Callinan et al., 2010). Little evidence is available on policies banning smoking in multi-unit housing, although such policies have been enacted in some jurisdiction on the assumption that they could potentially lower SHS exposure for children.
NQF has endorsed one measure pertinent to secondhand smoke exposure of children inside the home. This is a measure developed by the Maternal and Child Health Bureau of HRSA.
Each community, state, or measure-endorsing entity could use the logic model described below to generate a portfolio of measures for comparison and improvement in the area of environmental quality. The logic model can also be used to assess local resources and capacities to implement interventions to improve air quality.
Air Quality: Example Measures of Quality
The list below provides a partial set of potential measures. Figure 3-4 illustrates how the logic model can be applied to this LHI topic.
Measures of Outcome
Mortality due to respiratory complications
Asthma incidence in children
Inhaler use (as proxy for frequency of asthma attacks)
Hospital visits for asthma attacks
Emergency visits with respiratory related complications
Measures of Healthy Conditions (e.g., Intermediate Outcome)
Concentration of air pollutants in the air
Number of clean air days
Indoor air quality at home and workplace
Mass transit system coverage and use
Measures of Resources (Structure) or Interventions (Process)
Implementation of pollution reduction technology
Proportion of vehicles on the road that meet Corporate Average Fuel Economy (CAFE) standards
The following are measures that have been endorsed by NQF (measure steward provided in parentheses). They pertain largely to the clinical care setting and to a far lesser extent to the population level.
- Asthma Emergency Department Visits (Alabama Medicaid Agency)
- Relative Resource Use for People with Asthma (NCQA)
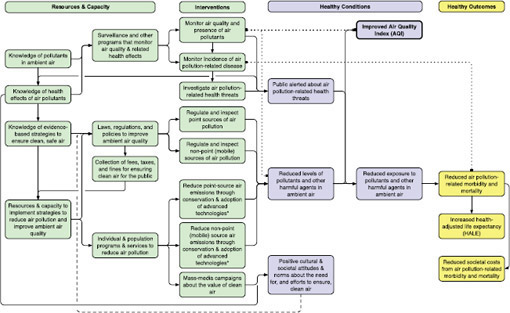
FIGURE 3-4 Applying the logic model to the LHI topic Environmental Quality (Air Quality Index LHI only).*
* Examples of reducing point source emissions include reduces power consumption through conservations measures; replacement of coal and other fossil fuel power generation with water-, wind-, and solar-based power generation; and use of low-sulfur coal, and scrubbers to reduce pollutants in power plant emissions. Examples of reducing mobile sources of air pollution include improvements in fuel efficiency through Corporate Average Fuel Economy standards and reductions in diesel fuel—related emissions through the use of low-sulfur diesel fuel and particulate filters.
Maternal, Infant, and Child Health
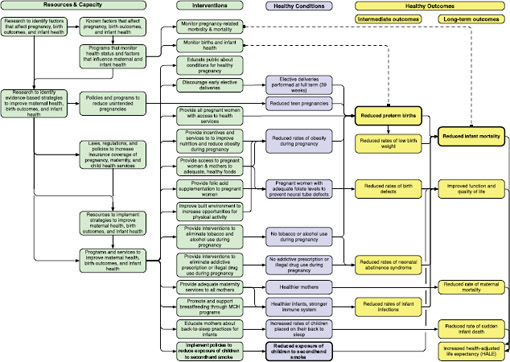
The two LHIs under this topic are LHI 11, infant deaths (MICH-1.3) and LHI 12, preterm births (MICH-9.1). Infant mortality is one of the four LHIs that is also an ultimate health outcome. Preterm birth is an intermediate outcome in the causal network that ends with infant death and is strongly associated with poor birth outcomes and development. According to 2010 data, 11.99 percent of American babies are born before 37 weeks of gestation (Martin et al., 2012). Although the preterm birth rate has decreased slightly every year for the past several years, the United States continues to lag behind its peers and ranked 130th out of 184 countries in a recent World Health Organization report (WHO et al., 2012). The U.S. infant mortality rate in 2009 was 6.39 deaths per 1,000 births. A report from the Organisation for Economic Co-operation and Development (OECD) showed that between 2005 and 2009 the United States had the highest infant mortality of 17 peer nations, and that it ranked 31st among 40 OECD countries (OECD, 2011). Within the United States, ethnic and racial disparities in neonatal and infant mortality are deep and persist across levels of educational attainment (Mathews and McDorman, 2012). In 2008, infant mortality among non-Hispanic blacks was 12.67 per 1,000 live births, compared to 5.52 among non-Hispanic whites (Mathews and MacDorman, 2012). Moreover, despite considerable decreases in infant mortality across all socioeconomic groups between 1969 and 2001, socioeconomic deprivation remains associated with higher neonatal and postneonatal mortality (Singh and Kogan, 2007).
Infant deaths may serve as a quality measure because they are a reflection of the ability of the health system (broadly conceived to include public health, health care delivery, social services, and others) to influence factors linked with infant survival at various points in the causal network. Reviewing the literature on infant deaths, including the extensive information provided in Healthy People 2020, the committee found that the top causes include, in order: birth defects, prematurity and low birth weight, and Sudden Infant Death Syndrome (SIDS) (Heron, 2012).
Given this broad and interrelated array of causal factors, a variety of system resources and capacity are relevant to both infant mortality and preterm birth. For example, access to health care services is an important factor in preventing preterm birth, but insurance coverage of maternity services is not enough. More than half of women who receive Medicaid coverage of pregnancy and birth lose that coverage within 60 days of giving birth (Johnson, 2012). The loss of coverage has serious conse-
quences for women with medical risks who had previous adverse pregnancy outcomes such as preterm birth or low birth weight, in part because of the likelihood that they will have similar poor outcomes with subsequent births.
A range of social, physical environmental, and economic conditions and changes in behavioral risk factors relate to infant mortality and pre-term birth. However, there are considerable gaps in the evidence base. The existing evidence-based interventions to address one or more of the causes of infant mortality and preterm birth include: folic acid supplementation, tobacco use cessation counseling, tobacco use interventions used in combination (excise taxes, campaigns, education) and worksite programs to control and reduce obesity (Community Preventive Services Task Force, 2013). In addition to those lifestyle factors, preterm birth and infant death are also related to teenage and unintended pregnancy, socio-economic status, educational status of the parents, sleep position, obesity, nutritional status, and infections in the mother, including sexually transmitted diseases (STDs). Clinical interventions that have been effective in addressing causes of infant mortality related to preterm birth include appropriate use of surfactant for preterm neonates experiencing respiratory distress.
A perinatal conceptual risk framework has been proposed, which involves recognizing that although many of the existing interventions occur at the level of the most proximal determinants—risk factors for poor pregnancy outcomes—the foundations for those poor outcomes are laid much earlier in life (Johnson et al., 2006; Misra et al., 2003). Such a life-course framework calls for undertaking strategies at the population and individual levels that intervene much earlier in life, years before a woman conceives, as well as during the interconception periods, with the intent of influencing such factors as nutritional status, tobacco use, and sexual behavior, among many others. Such an array of interventions would require changes in policies, including reorientation of federal and state investments, and the implementation of evidence-based interventions on many fronts. Several recent efforts have sought to improve infant health and survival, including the Association of State and Territorial Health Officials Healthy Babies Initiative, which has carried out efforts to improve birth outcomes in a number of states (ASTHO, 2012); the Peer-to-Peer State Medicaid Learning Project, operated by CDC and the Commonwealth Fund (Johnson, 2012), and the Strong Start for Mothers and Newborns Initiative, which is a joint effort of CMS, HRSA, and the Administration on Children and Families. The Strong Start initiative aims to reduce preterm birth and improve infant and ma-
ternal outcomes through two strategies: the reduction of elective deliveries before 39 weeks, and the testing of approaches to reducing prematurity among Medicaid and Children’s Health Insurance Program recipients at risk of premature birth.
Maternal, Infant, and Child Health: Example Measures of Quality
The list below provides a partial set of potential measures. Figure 3-5 (page 75) illustrates how the logic model can be applied to this LHI topic.
Measures Related to Healthy Outcomes
Infant mortality rate
Percent of overweight and obesity in pregnant women and women of childbearing age
Number of stillbirths and miscarriages
Number of preterm births
Number of children with congenital conditions
Percent of early elective deliveries
Measures Related to Healthy Conditions
Prevalence of infant exposure to environmental tobacco smoke in the home (HHS, 2006)
The existence of laws related to indoor air quality, such as municipal ordinances prohibiting or restricting smoking in multi-family housing (Environmental Law Institute, 2013)
Prevalence of back-to-sleep practices (data from Pregnancy Risk Assessment Monitoring System);
Rate of elective deliveries occurring prior to 39 weeks (objective of the National Priorities Partnership)
The rate of overweight and obesity in women of childbearing age and in pregnant women
Percentage of women of childbearing age receiving family planning services
Percent of pregnant women receiving prenatal care Number of women that adhere to dietary and nutritional guidelines during pregnancy
Percentage of women smoking during pregnancy
Percentage of women who consume alcohol during pregnancy
Percentage of teenage pregnancies
Percentage of unwanted pregnancies
Percentage of women breastfeeding a minimum of 12 months (American Academy of Pediatrics) or 2 years (World Health Organization)
Percentage of infants and children exposed to secondhand smoke Percentage of vaccinated (up to date) infants and children Percentage of mothers following nutritional guidelines Percentage of infants visiting the emergency room
Measures Related to Resources and Interventions
Availability of prenatal care
Availability of family planning services
The following are measures that have been endorsed by NQF (measure stewards provided in parentheses). They pertain largely to the clinical care setting and to a far lesser extent to the population level (e.g., AHRQ).
- Percentage of low-birth-weight births (CDC)
- Low-birth-weight rate (AHRQ)
- Healthy-term newborn (California Maternal Quality Care Collaborative)
- Prenatal and postpartum care (NCQA)
- Infant under 1,500 g not delivered at appropriate level of care (CA Maternal Quality Care Collaborative)
- SIDS counseling
- Exclusive breast milk feeding during the newborn’s entire hospitalization (Joint Commission)
- Frequency of ongoing prenatal care (NCQA)
- Prenatal and postpartum care—timeliness of prenatal care and postpartum care at 21 and 56 days after delivery (NCQA)
Given the role of smoking in influencing several factors that lead to infant death, quality measures related to tobacco use may be useful.
- Medical assistance with smoking and tobacco use cessation (three-component—advice to quit, discussion of medications, discussion of strategies for cessation) (NCQA)
- Percentage of patients aged 18 years and older who were screened for tobacco use at least once during the 2-year measurement period and who received tobacco cessation counseling intervention if identified as a tobacco user (AMA-convened Physician Consortium for Performance Improvement)
- The HRSA Maternal and Child Health Bureau measures children exposed to secondhand smoke inside their homes (fits under Healthy Conditions).