8
Information Management
and Integration
As the principal department advisor on all medical and public health issues, the Chief Medical Officer (CMO) must be able to brief the Secretary regarding the health, safety, and readiness of the Department of Homeland Security (DHS) workforce and to advocate for needed investments in prevention and health protection programs to address suboptimal readiness. Requisite to fulfilling this charge is the capability to maintain situational awareness regarding the health and medical status of the DHS workforce and the major health and safety risks that impede readiness. Given the absence of department-level health and safety information management systems, this capability currently does not exist in the Office of Health Affairs (OHA), or anywhere else in the department. This chapter presents the committee’s recommendations for steps DHS can take to establish a systems approach to information management, supported by a robust health information technology and informatics infrastructure, that enables evidence-based decision making, surveillance, accountability, and continuous quality improvement.
INFORMATION AND KNOWLEDGE MANAGEMENT
Obtaining reliable and consistent information is essential to the implementation and sustainment of an integrated workforce health protection program. This capability begins with the development of a set of standard core measures and metrics, linked to the program goals. Such measures and metrics allow for a better understanding of organizational needs and outcomes at all levels. However, the mere collection of data is not enough;
the data must be aggregated, analyzed, and used to monitor the effects of the program and enable continuous improvement. This can be achieved through a focus on information management—a systematic approach involving both technological and informatics capabilities that supports information exchange. Within a large, decentralized organization such as DHS, a centralized system for information management with standardized metrics and measures will support both horizontal (across levels) and vertical (between levels) integration.
Ultimately, the ability to manage information should support a larger organizational goal: the ability to manage knowledge. Knowledge management has been defined as “the process of creating value from an organization’s intangible assets” (Liebowitz, 1999, p. iii). The ability to accomplish this depends on capturing, sharing, and deploying not only data but also the knowledge and intellectual capital that reside in an organization’s people, structures, and relationships (Blue Ridge Academic Health Group, 2000). Just as an infrastructure can be built to support information management, an infrastructure also can be built to support knowledge management. Often referred to as a “knowledge web,” such an infrastructure connects employees with information, knowledge, and each other, helping to reduce redundancies, streamline work processes, optimize resource allocation, and facilitate relationships across a dispersed organization (Blue Ridge Academic Health Group, 2000).
Throughout its information gathering, the committee noted multiple cases in which stovepiped programs and a lack of communication and coordination mechanisms across DHS have resulted in failures of knowledge management. In the most striking example, Customs and Border Protection (CBP) reported that its occupational safety and health office had conducted a cost-benefit analysis of placing medical clinics or practitioners at some of its high-volume stations along the southwest border to help manage employee injuries and illnesses. Ultimately, CBP determined that employee utilization rates would not be high enough to justify the costs (Rupard, 2013). However, the committee subsequently heard that OHA had conducted a similar cost-benefit analysis indicating that significant cost savings could be achieved by having on-site medical care for detainees at high-volume Border Patrol stations (Zapata, 2013); these estimates did not even include collateral benefits to employees. Remarkably, neither office had been aware of the other’s efforts. This example clearly demonstrates the need to establish a knowledge management system that can provide the CMO with the enterprise-level health and medical intelligence needed to address cross-cutting issues and the ability to communicate those efforts across the department.
THE NEED FOR A DHS MEASUREMENT AND EVALUATION FRAMEWORK
In September 2013, the Institute of Medicine’s (IOM’s) Committee on Department of Homeland Security Workforce Resilience released its report containing recommendations for a 5-year strategic plan for the department’s workforce resilience program, DHSTogether. One of the major gaps in the program identified by that committee was the lack of a strategy, framework, and common set of metrics for use in conducting a comprehensive evaluation of workforce readiness and resilience and for evaluating and improving the effectiveness of programs that support a ready and resilient workforce. The findings of the present committee support that conclusion. The committee learned that components routinely gather safety and employee health data, albeit in an uneven and inconsistent manner. However, little of this information is transmitted to OHA. In fact, the only source of data currently received by OHA of which the committee is aware is the centralized electronic patient care record.
In a presentation to the IOM Committee on Department of Homeland Security Workforce Resilience, representatives of the Office of the Chief Human Capital Officer outlined a number of currently available DHS-wide data sources related to workforce health, readiness, and resilience (see Box 8-1). Many of these types of data will be essential to developing a comprehensive understanding of employee health status and needs; however, these data are “not actively integrated or analyzed for the purpose of measuring workforce readiness or resilience” (IOM, 2013, p. 134), and it is unclear whether or how OHA could access them. Injury and illness data (Total Case Rate and Lost Time Case Rate), although reported at least annually to the DHS occupational safety and health program staff in the Office of the Chief Human Capital Officer, as required by the Occupational Safety and Health Administration (OSHA), are not shared routinely with OHA. Attempts to collect medical quality assurance data (e.g., reports of sentinel events, frequency of clinical competency assessments), as authorized by Directive 248-01 on medical quality management, have been unsuccessful; components have begun collecting some of the required data but are not using dashboards provided by the medical quality management staff to share these data with OHA. Minimal data appear to be collected on employee health risks, even at the component level, with the notable exception of the Coast Guard, which mandates a health risk appraisal for all active-duty members.
BOX 8-1
Summary of DHS-Wide Data Sources Available to
the Office of the Chief Human Capital Officer*
Workforce demographics on age, gender, geographic location, time with agency, time in service, veteran status, job type, pay level (from the National Finance Center [NFC])
Turnover (from NFC), including intent to leave (from the Federal Employee Viewpoint Survey) and reasons for leaving (from exit surveys—response rates vary, and participation is voluntary; the Transportation Security Administration [TSA] and the Secret Service administer their own)
Sick and annual leave, although detailed information (e.g., types of sick leave) must be requested from component agencies and may be subject to privacy considerations
Federal Employee Viewpoint Survey (FEVS) results (from the Office of Personnel Management [OPM])
Equal employment opportunity (EEO) complaints—icomplaints, 462 reports to the Equal Employment Opportunity Commission (EEOC)
Workers’ compensation (from the Department of Labor’s [DOL’s] Office of Workers’ Compensation, cross-referenced with DHS component systems)
Accidents and injuries, including line-of-duty deaths (from DOL, component systems)
Health and safety program quality and implementation (on-site assessments)
The Office of the Chief Human Capital Officer relies on data calls to DHS component agencies for
- employee assistance program (EAP) reports,
- suicide numbers,
- employee relations cases, and
- cross-referencing for other measures.
________________
*As presented to the Institute of Medicine Committee on Department of Homeland Security Workforce Resilience (IOM, 2013, p. 135).
SOURCE: Green, 2013.
A SYSTEMS APPROACH TO DATA COLLECTION
Although alignment of workforce health protection programs into a single reporting structure under the CMO, as suggested in the committee’s Recommendation 2 (Chapter 6), would help address data sharing among headquarters entities, a systems approach is needed to collect and integrate data from across the department (see Figure 8-1). This type of approach, which entails data collection and analysis at four nested levels (individual, group, component, and department), supports both horizontal and vertical integration. Both forms of integration depend on the establishment of a common set of core metrics, which can be used for comparison across components and enable data aggregation for population-level analyses. Another important aspect of this approach is the consistent collection of data over time for longitudinal analysis (trending) to support continuous improvement.
In the absence of a comprehensive, standardized system with which to measure the performance of DHS’s occupational safety and health, occupational medicine, operational medicine, health promotion, and workers’ compensation programs, it is not possible to determine whether each component agency is managing its safety risk in an acceptable manner and whether occupational health programs are meeting objectives for improving workforce health and readiness. Thus, there is no means of ensuring
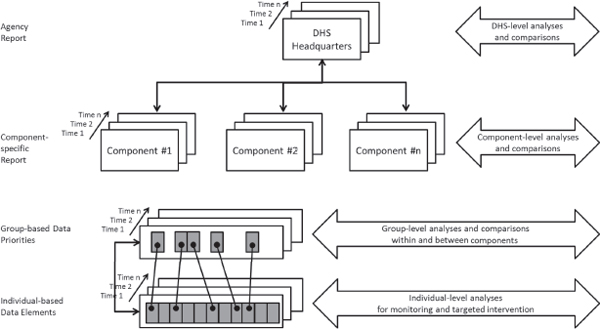
FIGURE 8-1 A systems approach to data management.
SOURCE: Adapted from IOM, 2005.
accountability, and those with responsibilities for workforce health, safety, and readiness are unable to make evidence-based decisions on investments in programs and infrastructure or to assess and improve the quality of programs and services.
Recommendation 10: Collect core metrics for accountability, continuous quality improvement, and readiness assessment.
The Chief Medical Officer, in collaboration with the proposed Component Lead Medical Officers, should develop a common core set of performance and outcome metrics to allow analysis of activities, outcomes, and trends in the areas of workplace safety and health, workforce medical readiness, and quality of medical services. Ongoing monitoring and analysis of these metrics as part of a measurement and evaluation framework are essential to drive continuous improvement and accountability.
In accordance with the recommendation of the IOM Committee on Department of Homeland Security Workforce Resilience to “develop and implement a measurement and evaluation strategy for continuous improvement of workforce readiness and resilience” (IOM, 2013, p. 153), the present committee believes that in developing a common surveillance and analytic framework, DHS also should include workplace safety and health, workforce medical readiness, and the quality of medical services to ensure the health, safety, resilience, and readiness of its workforce. In addition to measures of resilience discussed in that prior IOM report, DHS, using a systems approach as discussed above, should identify and collect the following types of metrics:
- Occupational safety and health metrics, including both leading (process) and lagging (outcome) indicators, should be used to identify and track progress toward the mitigation of health and safety hazards. An example of a leading indicator recommended by the committee is safety climate survey scores, which have been linked with employee compliance with and participation in health and safety programs (Clarke, 2006; Johnson, 2007; Payne et al., 2009; Zohar, 1980).
- Workers’ compensation metrics should be used primarily to evaluate the past performance of health protection programs and target future risk reduction efforts (e.g., by site or by hazard type).1
- Occupational medicine metrics should be used to help maintain and track the fitness-for-duty status of employees and should clearly link occupational medicine programs to mission readiness.
- Operational medicine metrics should include process and quality measures, and they also should demonstrate the value of having medical support available to those engaged in DHS operations, highlighting the impact of operational medicine programs on mission capability.
- Health promotion metrics should include aggregated, deidentified population health data and utilization rates, and they should be used to inform the creation and continuance of health promotion programs (see Box 8-2 for unique opportunities to collect such data at DHS).
- Workforce readiness metrics should be used to provide an overarching picture of workforce health and readiness to complete the mission. This will require component agencies to define the requirements for readiness.2
Common Core Metrics
The committee was asked to identify metrics that could be used for evidence-based quality improvement. A challenge associated with this task was the lack of information provided to the committee on the health risks (disease and injury) that are shared across DHS. Before such commonalities can be identified, the major health and safety hazards must be understood within the components. Since few metrics are being aggregated at the headquarters level, it is unclear what information is being collected and analyzed by individual components. Some, such as the Transportation Security Administration (TSA) and, more recently, CBP, have conducted thorough investigations to determine root causes for high injury rates. Such analyses should be conducted by all DHS components so that targeted mitigation
__________________
1It is important that occupational injury and illness incidence rates and workers’ compensation data not be used to evaluate the performance of individual employees or managers, nor should incentives be related to these metrics. Such evaluations and incentives invite individuals to suppress reporting of injuries and illnesses, thus diminishing the usefulness of these data for both evaluation and injury and illness surveillance purposes.
2As discussed in Chapter 4, to the committee’s knowledge, only the Coast Guard has defined requirements for individual readiness (based on alignment with Department of Defense policy), which can be monitored for individuals but also aggregated to measure the proportion of the component workforce that is classified as medically ready.
BOX 8-2
Measuring Employee Health at DHS
Data with which to monitor employee health and support federal workplace health promotion programs can be difficult to generate. Although the Office of Personnel Management has begun to collect health care utilization data from group insurance carriers, such data currently are not made available to federal agencies. Health risk assessments are another common source of health risk data. Although such assessments are mandated by military organizations, including the Coast Guard, as part of readiness assessments, civilian government employees cannot be required to participate. As a result, low response rates are a problem in civilian federal agencies offering health risk assessments, raising questions about the cost-effectiveness of such programs and the representativeness of the data thus procured.
Department of Homeland Security (DHS) does, however, have a ready source of employee health data that currently is not being fully exploited. Because of the security- and safety-sensitive nature of their jobs, a large proportion of the DHS workforce is required to submit to preplacement and, in some cases, periodic medical examinations. Such evaluations are a valuable source of population health data if processes, such as deidentification, are instituted to aggregate the data appropriately. For outsourced medical examinations, requirements for the provision of such data can be written into contracts and interagency agreements. For example, the Federal Air Marshal Service (FAMS), which uses Federal Occupational Health (FOH) for its mandatory medical exams, provides FOH with queries for extracting population health information; FOH then generates reports with deidentified aggregated data based on those queries. FAMS is planning to use these data to guide its new employee health and wellness program.
mechanisms can be put in place. Once component agencies have a better understanding of their major health risks, shared challenges can be identified and used to develop a robust set of core metrics. Common reporting standards/metrics would enable OHA and the DHS occupational safety and health program management staff to track the effectiveness of quality improvement activities and to provide more effective support (e.g., advising on best practices) and oversight of component efforts.
Recognizing that DHS and its component agencies will ultimately be in the best position to determine which metrics will be of most value to the department after conducting analyses such as those described above, the committee identified a number of metrics relevant to DHS that should, at a minimum, be included in this effort (see Table 8-1). These metrics should be collected as noted and trended annually to identify improved or deteriorating performance and to set goals for achieving superior performance. If such data are to be used to compare performance across components,
TABLE 8-1 Suggested Core Metrics for Tracking Departmental and Component Health, Safety, and Readiness
| Function | Metric | Purpose |
| Occupational safety and health |
• Occupational Safety and Health Administration (OSHA) recordable incident rate per year • Lost Time Case Rate |
• To assist in identifying workplace hazards and assessing the effectiveness of safety interventions • To assist in identifying workplace hazards and assessing the effectiveness of safety interventions |
|
• Safety climatea index scores by site |
• To gauge workforce perception of workplace safety and health as a leading indicator of injury risk |
|
|
• Number of seriousb hazards identified and corrected |
• To serve as a leading indicator of occupational safety and health program effectiveness |
|
|
• Percentage of job series with current job safety analysisc |
• To serve as an indicator of supervisory commitment to job safety and health |
|
| Workers’ compensation |
• Temporary/total disability daysd per 1,000 workers per year |
• To assist in evaluating mission readiness |
|
• Medical and indemnity costd per $100 payroll |
• To provide incentives to prevent and respond quickly to workplace hazards |
|
| Operational medicine |
• Number of employee treatment encounters outside of the conventional workspace per 1,000 operational person days and per 1,000 training days |
• To assist in determining trends in medical readiness and mission safety |
|
• Percent of deployed personnel receiving predeployment assessments |
• To gauge fitness for duty of deployed personnel |
|
|
• Number of employees who return to duty during the same shift per 100 injured employees |
• To assess the effectiveness of on-location medical intervention and to demonstrate the value of operational medicine programs to line leadership |
|
|
• Percentage of operations that have an effective after-action plan |
• To serve as a leading indicator for assessing operational readiness |
| Function | Metric | Purpose |
| Occupational medicine |
• Percent of required job-related health assessments performed per year |
• To serve as a leading indicator to ensure the capability to carry out essential job tasks and reduce injuries and illnesses |
|
• Percent of deploying personnel receiving preventive medicine guidance |
• To serve as a process measure for assessing the implementation of a preventive medicine program |
|
| Health promotion |
• Influenza immunizations per 1,000 employees per yeare |
• To reduce absenteeism related to influenza |
| Workforce readiness |
• Number of employees per 100 who are identified as not mission readyf |
• To monitor and provide operational leadership with information on the current state of workforce operational readiness |
|
• Readiness assessments per 100 workers with more than 7 lost workdays |
• To serve as a leading indicator for assessing operational readiness |
|
|
• Median and mean disability days per employee identified as not mission ready |
• To assess operational readiness |
|
|
• Provision of modified work per 100 workers with more than 7 lost workdays |
• To assess operational readiness and measure the success of return-to-work programs |
aSafety climate scales examine employee perceptions of safety in the workplace, with research supporting a strong link between safety climate and employee compliance with and participation in safety programs (Clarke, 2006; Johnson, 2007; Payne et al., 2009; Zohar, 1980).
b“The word serious as used in serious hazard, serious violation, or serious condition means a hazard, violation or condition such that there is a substantial probability that death or serious physical harm could result” (Occupational Safety and Health Act of 1970, 91st Congress, S.2193 [December 29, 1970]).
cThe Occupational Safety and Health Administration (OSHA) (2002) recommends conducting job hazard analyses to determine and establish proper work procedures and to eliminate and prevent hazards.
dRecommended Employer Measures of Productivity, Absence and Quality (EMPAQ) metric (NBGH, 2013).
eCDC (2013) recommends tracking influenza immunizations and assessing their effect on productivity.
fBased on a component-developed definition of mission readiness.
some of the metrics (e.g., OSHA recordable injuries, temporary/total disability days per 1,000 workers) should be analyzed in a manner consistent with the risk entailed in the entity. For example, DHS components whose employees perform hazardous tasks would have higher accident frequency and lost time injury rates than components whose employees perform less hazardous tasks. To adjust for this difference, a weighting factor should be applied to the data to allow fair cross-organizational comparison.
Data Collection Tools and Accountability
A systems approach to data collection, as described above, necessitates standardized data collection tools. Scorecards and other global assessment tools have been used extensively in private industry (e.g., Procter & Gamble, Johnson & Johnson) to collect data from business units and aggregate them in a way that enables trending for individual business units and monitoring of organization-level outcomes for benchmarking purposes. These auditing tools, which include process and outcome measures that have been established a priori (like those described in Table 8-1), also enable decentralized organizations to hold heads of component business units accountable for compliance with global standards and policies (IOM, 2005). In the implementation of a common surveillance and analytic framework, DHS should develop a global assessment tool for the purpose of performance monitoring and accountability.
ENABLING HEALTH SYSTEM INTEGRATION AND CONTINUOUS IMPROVEMENT THROUGH INFORMATION MANAGEMENT SYSTEMS
The ability to transform data into actionable information is a critical capability. A number of achievements in informatics and health information technology (HIT) can serve as a foundation for this capability. Over the past two decades, for example, the Department of Veterans Affairs (VA) has transformed the quality and safety of patient care at its numerous clinics and hospitals through the implementation of its electronic health record system, VISTA. The VA is now using the data from these records to perform system evaluations and institute quality improvements. A study by the Center for Information Technology Leadership showed that between 1997 and 2007, estimated cost savings from the VA’s investment in HIT exceeded $3 billion (Byrne et al., 2010).
Health Information Management at DHS
In considering the requirements for health information management within DHS, it is necessary to address two related but clearly different requirements that parallel the issues already discussed with regard to operational medicine services versus occupational health and safety. In support of operational medicine services, a system with characteristics most consistent with a traditional electronic health record is required so that treatment provided to anyone receiving care from DHS providers can be documented. This system would support further care of the patient, enable ongoing quality assurance, and provide complete medical records for legal purposes. The second requirement is a longitudinal health record to support occupational health, including readiness assessment. This record is, by definition, not a complete electronic health record, as it should be used only to document those health issues that are relevant to employment, addressing primarily capabilities specifically relevant to duties and deployments. There will likely be some overlap between these records as employees become patients in operational settings, but the two types of records are not synonymous. DHS’s ongoing exploration efforts demonstrate recognition of these two separate needs.
To address the latter need, OHA has initiated an acquisition process for a department-wide electronic Health Information System (eHIS). Despite repeated requests, however, the committee had difficulty obtaining information on DHS’s strategic approach to health information management using the proposed system. As of this writing, funding for the system has not been approved. OHA is still assessing feasibility and capabilities and has contracted for an evaluation of existing systems to determine the cost-effectiveness of agency-wide implementation. A working group comprising representatives from OHA, the Office of the Chief Human Capital Officer, and other DHS components identified the following mission and capability needs for the eHIS3:
- ensure that staff are medically suitable for their assigned or volunteered duties (e.g., job and environment);
- provide for the execution of an efficient DHS-wide fitness-for-duty and limited-duty program;
- enable efficient dispensing, tracking, and follow-up for medical countermeasures;
- lower occupational health costs across the department; and
__________________
3E-mail communication, I. Hope, DHS OHA, to A. Downey, Institute of Medicine, regarding DHS mission needs capabilities identified-mission needs statement, March 27, 2013.
- unify and standardize occupational health and workforce health protection activities across the department.
If funding for the eHIS is approved, data integrated using the system may include preemployment medical history information, fitness-for-duty examination reports, position descriptions with physical requirements, and medical restrictions for work-related injuries. Such information could be used for multiple purposes, including adjudication of workers’ compensation claims and tracking of medical readiness.
OHA has already acquired an electronic patient care record (ePCR) system to address the first requirement described above. All DHS components with emergency medical services (EMS)/paramedic personnel have been given access to the system and the opportunity to be trained in its use. Allowing DHS to consolidate all patient records, the ePCR system already has been adopted by a number of operational medicine units, including those in Immigration and Customs Enforcement (ICE) and the Federal Air Marshal Service (FAMS), as well as some within CBP and the Federal Emergency Management Agency (FEMA). By spring 2014, all DHS components, including the Coast Guard, are expected to have adopted the system. A function to be added to the ePCR system is a personnel management module that will track credentialing of EMS/paramedic providers. Although the ePCR can be loaded on mobile devices, a lack of hardware to support that function means that paper records remain a part of the patient encounter process, and this information must be transferred to the electronic system later, creating opportunities for error. The ePCR system enables OHA to query aggregate patient encounter data from across the department for both surveillance (e.g., volume and types of encounters) and quality assurance (run review) purposes. However, it is unclear what role the ePCR investment plays in a comprehensive HIT/informatics strategy or how patient record information (for DHS employees) will be integrated with the eHIS should that system be implemented in the future.
At the individual component level, the Coast Guard, working with the VA and the Office of the National Coordinator for Health Information Technology, is building an integrated health information system (IHiS) based on the commercial Epic electronic health record system for traditional clinical care environments. Its functionalities will include ambulatory care, urgent care, dental care, physical therapy, optometry, behavioral health, occupational health, immunizations, audiology, radiology, pharmacy, laboratory, and a patient portal (McCann, 2012). In addition to individual case management capabilities, the IHiS will enable disease management capabilities that can then broaden into data analysis for public health initiatives. The IHiS will consolidate many of the electronic reporting systems currently used by the Coast Guard for medical readiness reporting and deployment
health-related information. The Department of State also will be adopting the Coast Guard’s IHiS. The only other component currently adopting an electronic health record is ICE, which recently awarded a contract for such a system to support comprehensive medical services management for detainees. It is not clear whether this system will also be used to track the health records of ICE employees.
Information technology systems for occupational safety and health vary considerably across DHS, and there is no department-wide system that allows safety and workers’ compensation data to be aggregated at the headquarters level. Some components use spreadsheets to track this information, while others, such as TSA, have sophisticated safety information systems that track reported injury/illness and workers’ compensation claims, as well as leading indicators such as information from safety inspections and job hazard analyses.
Although DHS is moving toward an enterprise approach to HIT, the committee did not find evidence that the department is fully aware of the informatics capability required to maximize the potential of an integrated health information management system. Two OHA staff members are trained in nursing informatics, and a third is familiar with the use of clinical informatics systems for medical quality assurance processes. However, this informatics capability does not appear to be represented at the component level, with the exception of the Coast Guard, which has a Chief Medical Information Officer. The lack of health informatics expertise across DHS may help to explain the lack of success of the Medical Quality Management (MQM) program. Headquarters MQM staff have been working with components to establish systems and processes that will enable structured/standardized data collection, reporting, and analysis for purposes of continuous quality improvement. Yet components, which rely primarily on outsourced medical service providers, appear not to have the personnel or expertise necessary to adopt such practices and have yet to use the MQM-provided dashboards for these purposes.
Building a Robust DHS Health and Safety Information Management Capability
Across DHS, health information and communication technology is viewed primarily as a strictly tactical resource. This perspective is too narrow to meet the current and future mission requirements of the various DHS components. The fields of medical and public health informatics and their application to clinical and public health programs are critical to DHS going forward. Components are engaged with clinical care, preventive medicine, and occupational medicine to varying degrees, but the development of health information management applications, data repositories,
and communications capabilities is spotty at best. Integration through health information management will not be achieved until this capability exists throughout the department.
Recommendation 11: Establish a health and safety informatics and information technology infrastructure.
The Health, Safety, and Medical Council should charter a Health and Safety Informatics and Information Technology Governance Board to develop and oversee the implementation of a strategic plan for building a health and safety informatics and information technology infrastructure. The Governance Board should be led by a Chief Medical Information Officer designated by the Chief Medical Officer (CMO) and should include representatives from the offices of the CMO and the Chief Information Officer, as well as each of the components. The strategic plan should be reviewed and approved by the CMO; the Health, Safety, and Medical Council; and department leadership.
The Governance Board should be supported by an operational-level Steering Committee to manage the implementation of the strategic plan, and both the Governance Board and the Steering Committee should be supported by appropriate experts in health and safety informatics and information technology from within DHS and other federal agencies. Lead agencies from which to seek expert guidance might include, but are not limited to, the National Library of Medicine, the Office of the National Coordinator for Health Information Technology, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute.
An informatics and information technology capability is essential for implementation of the measurement and evaluation framework described in Recommendation 10, and Recommendation 11 is meant to complement efforts currently under way at DHS. Building on the work already accomplished by a DHS eHIS working group, the proposed strategic plan should provide the blueprint for a robust health and safety informatics and information technology infrastructure incorporating medical, public health, and consumer informatics capabilities, and it should be consistent with the overarching DHS information technology strategy. Elements of the plan should include
- a workforce strategy for relevant informatics and information technology personnel, including requisite responsibilities;
- a knowledge management structure within each unit and, where relevant, across the department; and
- a business case analysis demonstrating the return on investment.
Key features of the development and implementation of this plan should include
- engagement of front-line providers and other current stakeholders knowledgeable in informatics and information technology systems to identify needs, available resources, desired future capabilities, and alignment with DHS strategic objectives;
- assurance, through ongoing engagement with the DHS Chief Information Officer, that the DHS health information strategy and all systems are developed in a manner consistent with the department’s overall information strategy and integrated with departmental efforts/systems wherever appropriate;
- an expert advisory board to offer feedback and strategic advice over time until no longer needed;
- ongoing evaluation of any unintended consequences of and barriers to implementation, and the development of strategies for resolving these issues; and
- designation, as a collateral duty initially, of a Chief Medical Information Officer to serve as a point person in OHA.
Although the committee believes that DHS should move to an electronic health information system, it does not have the necessary information to recommend the adoption of a single DHS-wide system over other alternatives. It may be that there is no single system that could meet all the needs of an organization as complex as DHS. Rather, the committee sees the need for an intellectual and technological infrastructure that can move to functional interoperability as the system matures and the agency gets a better sense of what can be achieved.
Considerations for Interoperability and Data Integration
With the exception of the Coast Guard, DHS provides little in the way of health care to employees outside of medical support as part of an operational medicine program. Consequently, its information management needs center on occupational safety and health data sources. Commercial occupational health management software, in contrast to more traditional electronic health records, is designed to facilitate the integration of occupational safety, health, industrial hygiene, environmental, and ergonomics
data into a single system to enable surveillance and risk management, as well as standardized data management, across the enterprise.
Regardless of the type of system ultimately adopted, DHS will need to address data integration at both the individual and population levels. At the individual level, records from diverse sources (e.g., medical treatment, absenteeism, fitness for duty, workers’ compensation claims) need to be linked to provide a better view of the “whole individual.” In the long term, this approach will enable targeted, evidence-based interventions to address individual employee health, which may be more effective than more general population health promotion measures (Bunn et al., 2010). Aggregation of individual data to the population level (in a deidentified form) will allow DHS to develop a global view of the health status of its employee population, identifying and monitoring progress toward mitigation of major health risks.
To address data integration at the systems level, DHS needs to consider interoperability with vendor and legacy component data management systems. It is important to note that some component agencies, including TSA and the Coast Guard, have already invested heavily in systems for health information management. In addition to integrating data sources internally, the proposed strategic plan should address mechanisms for integrating data collected by vendors providing outsourced health services (e.g., preplacement and fitness-for-duty evaluations; clinical services, including vaccinations; medical surveillance; and nurse case management). For example, Federal Occupational Health (FOH) has initiated an acquisition process for its own occupational health management system to integrate patient data (e.g., medical clearance, medical surveillance, vaccination status) with administrative information. Components contracting with FOH will have access to their own data within the planned system, but OHA will need to consider how such data can be collected into a DHS-wide system if integration is to be successful. Likewise, the vendor for the forthcoming DHS medical case management program is tasked with providing its own information technology solution, and it is unclear how these data will be integrated into the proposed DHS eHIS.
Perhaps the greatest challenge today is the integration of quality and safety dimensions into the informatics and information technology enterprise. This is a national challenge not limited to DHS, but success in this area will pay major dividends (see IOM, 2011).
Building an Informatics Capability
In addition to HIT specialists, DHS will need internal personnel with core competencies in clinical and public health informatics if it is to successfully transform information management to support health maintenance;
fitness-for-duty evaluation; and management of injuries, illnesses, and disabilities across the spectrum of DHS workforces and missions. Informatics specialists will need to be integrated with those charged with managing quality and safety to realize improvements in communications and coordination; standardization, harmonization, and interoperability; and efficiency.4 The change called for will not be a minor one for a department as complex and diverse as DHS. DHS will need to undertake three related cultural and organizational transitions with respect to informatics and HIT:
- a shift from viewing information technology as a “fix” to recognizing the opportunities provided by informatics expertise as an ongoing strategic resource;
- a shift from viewing informatics and HIT leadership as overseeing a peripheral support group to seeing them as key players in conducting strategic planning, designing solutions, and advising departmental leadership; and
- a shift from relying on information technology staff to be both informaticians and information technologists to making a sustained investment in both information technology and informatics specialists.
These transitions will require medical and nursing officers who not only recognize the importance of informatics but also are trained in clinical informatics to support direct patient applications, as well as in public health informatics to support both individual health and wellness programs and population health monitoring and evaluation. In light of current staffing, external consultants will be needed initially to augment the currently insufficient informatics expertise within the department. However, DHS should initiate an education and training program as part of a workforce strategy designed to ensure that sufficient expertise will be available internally to meet general workforce requirements for clinical and public health informatics, as well as to build expertise in informatics areas specific to DHS missions (e.g., telemedicine for care of detainees at border areas, fitness-for-duty health programs monitored via electronic health records throughout the world). Continuing education will be needed as well to maintain cutting-edge knowledge and skills as technology and expectations continue to evolve. Newer educational technologies should be considered for addressing aspects of this challenge (Blue Ridge Academic Health Group, 2013).
__________________
4See Blue Ridge Report 12, October 2008, available for free download at http://www.whsc.emory.edu/blueridge/publications/archive/blue_ridge_report_12_2008.pdf (accessed August 21, 2013).
Ultimately, Chief Medical and/or Chief Nursing Information Officers should be prominently located in the organizational charts of each of the components, and a coordinating council should be established to enable these leaders to interact with one another and jointly with line leadership within DHS. Engagement of senior DHS leaders should be undertaken through intermittent briefings to ensure that sufficient financial and staffing resources are allocated to the effort.
Implementation Challenges
Although ultimately beneficial, the implementation of an electronic health and safety information management system will be costly and disruptive in the near term, as evidenced by the continued delays and challenges encountered by the Coast Guard with implementation of its IHiS 2 years after awarding the initial contract to Epic (Janda, 2011). However DHS proceeds with the implementation of future systems, the Coast Guard’s recent experience should be leveraged to identify lessons learned and opportunities for efficiency that may help DHS in those efforts.
Given the up-front investment costs and implementation challenges, the decision on the best approach going forward will require a series of business cases for each component, followed by a business case addressing whether common systems would be most effective across the department. The benefits of an electronic health record may be obvious for the Coast Guard and the detainee health services unit within ICE, both of which have longitudinal health services missions such that the loss of paper records as a consequence of patients moving within the system could result in missed diagnoses or other inappropriate care. For other components, however, an electronic health record could actually increase expenses for various reasons that could be explored in a business case. The committee did not have the manpower or time to develop these cost-analysis business cases, and it notes that OHA and other entities are in the process of doing so; the committee fully supports these efforts.
Oversight of the Implementation of Information Management Systems
To address the kinds of challenges discussed above, the proposed strategic plan should outline roles and responsibilities, as well as coordination mechanisms, for an oversight and coordination structure in the spirit of the Government Accountability Office (GAO)-described integrated enterprise governance structure illustrated earlier in this report (see Figure 6-1 in Chapter 6). This structure would suggest, and the committee recommends, two groups. The charge for the first group, at the level of a portfolio governance board, would be to establish policies and procedures needed to
achieve an integrated, first-rate informatics and HIT operation over time. This group would need to include representation from key stakeholders (a senior staff representative from each component) to ensure buy-in for recommended policies. The second group, at the level of a steering committee, would provide oversight of operations, including needs, implementation, and ongoing operational effectiveness (e.g., data management considerations). This group would need to consist of informaticians, users, and health information technicians close to the front lines. Because informatics and HIT continue to evolve, the committee believes DHS should create a Health Information and Informatics Advisory Group consisting of experts from across government that would work iteratively with leaders of both the governance board and the steering committee. The goal of these interrelated groups would be to meet the operational and management information and communication needs of individual components while exploiting opportunities for collective benefit where appropriate. All of these efforts need to be undertaken from the perspective of a value-driven learning health system, in which continuous learning supports evidence-based practices and continuous improvement (IOM, 2012).
Blue Ridge Academic Health Group. 2000. Into the 21st century: Academic health centers as knowledge leaders. Charlottesville: University of Virginia Health System.
Blue Ridge Academic Health Group. 2013. Health professions education: Accelerating innovation through technology. Atlanta, GA: Blue Ridge Academic Health Group.
Bunn, III, W. B., H. Allen, G. M. Stave, and A. B. Naim. 2010. How to align evidence-based benefit design with the employer bottom-line: A case study. Journal of Occupational and Environmental Medicine 52(10):956-963.
Byrne, C. M., L. M. Mercincavage, E. C. Pan, A. G. Vincent, D. S. Johnston, and B. Middleton. 2010. The value from investments in health information technology at the U.S. Department of Veterans Affairs. Health Affairs 29(4):629-638.
CDC (Centers for Disease Control and Prevention). 2013. Workplace health—evaluation—adult immunization. http://www.cdc.gov/workplacehealthpromotion/evaluation/topics/immunization.html (accessed November 22, 2013).
Clarke, S. 2006. The relationship between safety climate and safety performance: A meta-analytic review. Journal of Occupational Health Psychology 11(4):315.
Green, A. 2013. Data resources for resilience: DHS OCHCO. Presentation at IOM Committee on DHS Workforce Resilience: Meeting 2, February 4-5, Washington, DC.
IOM (Institute of Medicine). 2005. Integrating employee health: A model program for NASA. Washington, DC: The National Academies Press.
IOM. 2011. Health IT and patient safety: Building safer systems for better care. Washington, DC: The National Academies Press.
IOM. 2012. Best care at lower cost: The path to continuously learning health care in America. Washington, DC: The National Academies Press.
IOM. 2013. A ready and resilient workforce for the Department of Homeland Security: Protecting America’s front line. Washington, DC: The National Academies Press.
Janda, T. A. 2011. Becoming more than just a new EHR. The Uniformed Family Physician 4(4): 30-32. http://epubs.democratprinting.com/publication/?i=80240&p=30 (accessed December 13, 2013).
Johnson, S. E. 2007. The predictive validity of safety climate. Journal of Safety Research 38(5):511-521.
Liebowitz, J. 1999. Preface, “Knowledge management: Fact or fiction?” In Knowlege management handbook, 1st ed., edited by J. Liebowitz. Boca Raton, FL: CRC Press.
McCann, E. 2012. Coast Guard awards $17 million contract for health information system. Healthcare IT News. http://www.healthcareitnews.com/news/coast-guard-awards-17-million-contract-health-information-system (accessed November 12, 2013).
NBGH (National Business Group on Health). 2013. About workers’ compensation. http://www.empaq.org/metrics/workers_comp.cfm (accessed November 22, 2013).
Payne, S. C., M. E. Bergman, J. M. Beus, J. M. Rodríguez, and J. B. Henning. 2009. Safety climate: Leading or lagging indicator of safety outcomes? Journal of Loss Prevention in the Process Industries 22(6):735-739.
Rupard, D. 2013. Occupational safety and health at DHS: CBP. Presentation at IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Zapata, I. 2013. FY2015-FY2019 Southwest Border Health Initiative business case. Presentation at IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Zohar, D. 1980. Safety climate in industrial organizations: Theoretical and applied implications. Journal of Applied Psychology 65(1):96.






















