Chapter 2 presents the committee’s framework for workforce health protection and identifies key functions of an integrated health protection infrastructure. The two pillars of this framework reflect the two medical requirements for mission readiness: (1) a workforce that is medically ready, and (2) the capability to provide medical support to the workforce during planned and contingency operations. The committee noted significant variability in the implementation and resourcing of occupational health and operational medicine programs across the Department of Homeland Security (DHS). This observation suggests a role for the centralized health and medical authorities at DHS to improve mission readiness by establishing a more uniform and unified approach to workforce health protection. This chapter provides the committee’s recommendations for how DHS can align critical workforce health protection functions that support mission readiness through global policies and standards that set clear expectations.
THE NEED FOR FUNCTIONAL ALIGNMENT
When the Chief Medical Officer (CMO) position was created at DHS, the vision was to appoint a medical leader who could unify the department’s fragmented health and medical system. The Delegation to the Assistant Secretary for Health Affairs and Chief Medical Officer granted the CMO the oversight authority needed to achieve that vision. Despite that vested authority, however, in the absence of accountability processes, the CMO has to date been largely unsuccessful in garnering sufficient support
from component leadership to achieve a unified health system. Throughout the course of this study, the committee noted multiple examples of components taking independent approaches to health protection functions, with varying levels of success. Although components require flexibility to tailor programs to their operational realities, care must be taken to ensure that core requirements are still being met. A continued lack of consistency among critical health and medical programs creates liability risks (legal and monetary) for DHS, including but not limited to
- equal employment opportunity suits if medical standards are not adequately defensible in a court of law,
- liability associated with adverse events if medical providers are not appropriately credentialed,
- liability associated with failure to provide detainees and others for whom DHS has assumed responsibility with adequate and timely medical care, and
- workers’ compensation liabilities associated with unsafe or unhealthful workplaces and inadequate processes for preventing or limiting disability.
Going forward, the Office of Health Affairs (OHA) needs to find a means to ensure that critical health protection functions are aligned across the department in such a manner that all component programs are resourced and appropriately implemented to meet core requirements set by the CMO. The coordination mechanisms recommended in Chapter 6 can support this objective by providing a means of obtaining component support. However, it is still the CMO’s responsibility to set clear expectations through global policies, standards, and programs.
ENSURING THE MEDICAL READINESS OF THE DHS WORKFORCE
To meet mission requirements effectively, DHS needs to build a workforce protection capability that maximizes the number of DHS personnel who are medically ready, or free of health-related conditions that would impede their ability to participate fully in or support operations. Discussions of readiness in civilian organizations tend to focus on fitness for duty. However, a comprehensive strategy for supporting readiness needs to go beyond fitness-for-duty evaluations and address the full employment life cycle. The strategy needs to focus not only on the health and capability of employees, but also on the safety of both job processes and the work environment and the interactions among these three elements (see Figure 7-1). Occupational safety and health and occupational medicine programs, including health promotion programs, work hand in hand to prevent employees from
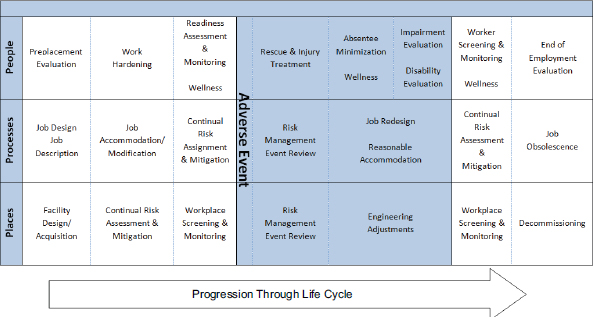
FIGURE 7-1 A life-cycle approach to achieving mission readiness through workforce health protection.
SOURCE: Lang, 2007.
departing from a state of readiness, while disability management programs facilitate reestablishment of readiness. Although not depicted in Figure 7-1, the life-cycle approach should also address special needs related to deployment (e.g., pre- and postdeployment assessments).
As discussed in Chapter 4, mechanisms for assessing, promoting, and sustaining medical readiness vary widely across DHS, and few standards and overarching policies have been promulgated by the CMO to ensure consistency and interoperability. Dr. J. D. Polk, former acting CMO at DHS, told the committee that a gun carrier in Immigration and Customs Enforcement (ICE) and a gun carrier in Customs and Border Protection (CBP) can be doing the same job but be held to different standards (Polk, 2013). This can be a point of contention among unions, and ultimately it may compromise the defensibility of the standards. A common life-cycle framework for approaching workforce health and resilience would provide a mechanism for ensuring that a set of disparate components can achieve the appropriate mission readiness outcomes. A life-cycle approach integrates a fragmented system and typically has the following characteristics:
- clear and explicit guidelines and expectations regarding operation and performance,
- a common approach for monitoring job-related mission readiness, and
- a proactive framework for enhancing or restoring workforce readiness.
Existing injury/illness prevention, fitness-for-duty, health promotion, medical case management, and workers’ compensation programs should be integrated within this life-cycle approach.
Recommendation 7: Develop a common employment life-cycle-based framework for achieving mission readiness.
The Chief Medical Officer should establish a common approach to identifying and mitigating limitations on individual readiness, to be implemented by the components and adapted as necessary. Such an approach should include
- developing health-related functional standards (including specific medical standards when mission-critical) for job series that are common across multiple component agencies, allowing flexibility for reasonable modification where justified by unique duty requirements within components;
- monitoring, assessing, and promoting individual readiness across the entire employment life cycle, from entry into the workforce to the time of separation or retirement; and
- reestablishing readiness, to the extent feasible, when individuals are identified as having limitations.
Job performance requirements1 will drive the evaluation of readiness; it follows, then, that the frequency and content of job-related health and fitness evaluations should be consistent for similar job series across the department. Job-related health, fitness, and resilience should be evaluated at multiple points across the employment life cycle:
- preemployment or preplacement, to ensure that candidates meet physical and medical job requirements and to establish baselines for health and fitness;
- periodically, to ensure that employees continue to meet physical and medical job requirements and to enable the early identification of conditions that may limit individual readiness;2
- when triggered by injury, illness, and/or noted declines in job performance, to assess whether employees still meet physical and
__________________
1Derived from a job task analysis validated by an occupational health professional.
2Periodic screening assessments may be voluntary or mandatory based on job requirements, and when mandatory, can be age-adjusted based on risk. Periodic assessments also should be used as opportunities to discuss health promotion and health risk mitigation strategies to prevent departure from a state of readiness.
-
medical job requirements and, if not, to assess their capacity to return to a state of readiness following appropriate interventions; and
- before and after deployment to sites of contingency operations, to determine the appropriateness of deploying an individual with a given health and physical capability status based on expected working conditions, and to assess the need to reestablish readiness upon return.
A Comprehensive Medical Evaluation and Clearance Process
As described to the committee by Phillip Spottswood (2013), Medical Policy and Programs Specialist at the Office of Personnel Management, a comprehensive medical evaluation and clearance program to support medical readiness would include the following elements (see Figure 7-2):
- a preplacement (postoffer) fitness-for-duty evaluation, including a medical history, to evaluate employees against approved medical standards and physical requirements and to establish baseline information that can be used to control workers’ compensation costs;
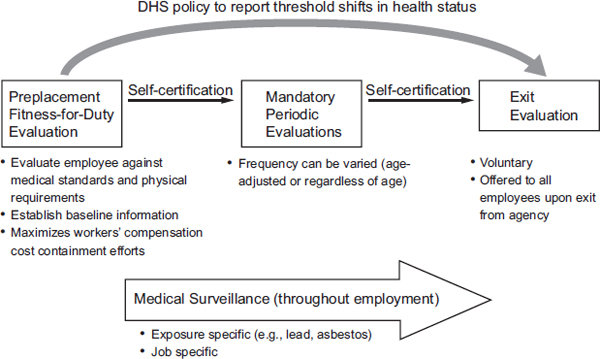
FIGURE 7-2 A comprehensive fitness-for-duty evaluation and clearance program.
NOTE: It is understood that evaluations should be consistent with employment law.
SOURCE: Adapted from Spottswood, 2013.
- mandatory periodic fitness-for-duty evaluations that can be age-adjusted or independent of age, with requirements to self-certify regarding job-related health status on an annual basis;
- a departmental policy requiring employees to report threshold shifts in health status;
- medical surveillance throughout the employment period that is both job and exposure specific; and
- a voluntary exit evaluation offered to all employees upon separation.
Framework Implementation
Standards Development
Given the committee’s lack of information on the various component operational requirements, it was not possible to formulate specific recommendations regarding medical and physical ability standards. As discussed in Chapter 6, the committee believes that Component Lead Medical Officers (CLMOs) should be engaged in the recommendation and validation of such standards (see Recommendation 5 on the Medical and Readiness Committee). Soliciting component buy-in throughout the standards development process will prevent the kinds of problems experienced with past efforts to develop DHS-wide standards (Leffer, 2013). Standards development processes are discussed in detail in Chapter 3, and one model approach is provided in the committee’s case study on the Department of the Interior (see Box 3-5).
Readiness Assessment
Fitness-for-duty evaluations should be functionally based and focus on physical capabilities necessary to establish readiness for a given position, based on documented fitness-for-duty requirements in a given agency. Employee health should be examined only as it relates to those requirements. Although components need flexibility in the implementation of readiness assessment processes, DHS should consider standardizing or setting minimum requirements for some aspects of implementation. The quality of readiness assessments may vary considerably depending on how they are conducted (Garbe, 2013). For example, consistency is improved when assessments are conducted internally or through a centralized contract or agreement (Garbe, 2013), as opposed to allowing individuals to choose their own examining physicians for readiness assessments. The Federal Bureau of Investigation (FBI) takes this approach, using vendors contracted through the central occupational medicine services officer to administer examinations, but reviewing results and making determinations internally (Wade, 2013).
BOX 7-1
Special Considerations Regarding Fitness
for Duty for Contracted Personnel
As a special consideration in addressing fitness for specific duties, especially deployments, the committee takes note of the extensive use of contractors in many aspects of Department of Homeland Security (DHS) operations. The government’s role in the occupational health of contractor personnel has been an ongoing issue throughout the federal government, but it takes on special importance in DHS, where contractors often play an important role in critical incident response. DHS needs to actively engage other government entities in ensuring that these issues are addressed, but at a minimum, the Office of Health Affairs should provide specific minimum occupational health criteria for inclusion in various support contracts to ensure that contracted organizations address such critical issues as appropriate immunizations, requirements for meeting certain fitness-for-deployment standards, and mechanisms for obtaining necessary care during critical incident response before assigning personnel to contracted critical support positions. The Department of Defense has addressed health requirements for contracted personnel, particularly those who deploy with active-duty military personnel, through clear policies (32 CFR 158.7; DoD, 2006). Such policies could serve as models for DHS.
Special considerations regarding fitness for duty for contracted personnel are described in Box 7-1.
Early Intervention and Disability Management to Reestablish Readiness
One of the main objectives of the life-cycle approach is the early identification of any health-related conditions that impede employees’ ability to carry out the responsibilities of their position fully and safely and mitigation of such limitations so as to return those employees to a state of mission readiness. Therefore, a critical requirement is the capacity to follow up on limitations identified through screening assessments. To build and sustain this capacity, components should establish early intervention and injury/illness case management programs that operate in close coordination with fitness-for-duty, injury/illness prevention, and workers’ compensation programs.
Medical case managers should be established in components, or subcomponents as appropriate, to provide continuity of service, allow for deeper understanding of jobs and job requirements, and build understanding and trust between employees and case managers. Special attention
may be needed to ensure that employees injured on and off the job receive coaching regarding best practices in medical management to ensure their timely return to duty. Where feasible, case managers should be assigned to specific geographic locations.
Case management at the subcomponent level may be warranted when subcomponents have their own medical standards that injured employees must meet before returning to duty. For those employees who must meet medical standards, nurse case managers who are familiar with those standards can help avoid delays in medical clearance processes (Lewandowski and Weeks, 2013). In such cases, efficiencies may be realized by having medical program staff responsible for fitness-for-duty evaluations also serve as nurse case managers. If nurse case managers for disability management are separate from occupational health staff, the two groups will need to work together closely after occupational injuries to return employees to work as quickly as possible while still ensuring compliance with medical standards.
Regardless of whether medical case management programs are established internally or outsourced, care must be taken to ensure their integration into the component medical infrastructure. Workers’ compensation reporting systems and occupational safety and health reporting/tracking systems need to be coupled so that trends/issues/problems can be identified rapidly and corrected, thus preventing additional injuries and illnesses (and/or enabling early recognition of nefarious acts such as use of weapons of mass destruction). Such integration may not occur if case management programs are led from workers’ compensation offices that are isolated from safety and medical program offices.
MEDICAL SUPPORT FOR OPERATIONS
All federal employees are entitled to safe and healthful places and conditions of employment.3 Federal agencies are equally responsible for workers operating in the field and those stationed in more conventional workspaces. Operational medicine programs are a means by which occupational health and medical services are made available to workers in the field and are essential to mission readiness. The dependence of the mission on a robust capability to provide medical support to the workforce during operations sets DHS apart from most other federal agencies and imposes unique requirements for a workforce health protection infrastructure.
OHA has achieved commendable progress toward the integration of emergency medical services (EMS) across DHS. The approach to integration
__________________
3As required by the Occupational Safety and Health Act of 1970 and Executive Order 12196.
is well described in the DHS Emergency Medical Services Strategic Framework (DHS, 2012). Working collaboratively with nine DHS component agencies through the Emergency Medical Services Training and Education Advisory Committee, OHA has developed a centralized EMS system plan, has established standards of care through baseline basic life support and advanced life support protocols, and has acquired software for department-wide patient care reporting and tracking of EMS provider credentials. OHA also is working with the Emergency Medical Services Training and Education Advisory Committee on the development of a central EMS policy document. As a result of these efforts, improvements in efficiency, interoperability, consistency, and information sharing have been realized. Interoperability is of notable importance given the potential for joint DHS operations in support of state and local EMS assets in the event of a disaster.
Despite these laudable achievements, a comprehensive program for operational medical support needs to go beyond EMS to include the capability to address the preventive and ambulatory medical care needs of those conducting DHS operations (Heck and Pierluisi, 2001). Like a corporation that sends its employees to regions of the world with limited or low-quality medical resources, DHS has a responsibility to ensure that members of its workforce operating in remote, austere areas and those who, for security reasons, cannot readily access local medical resources have access to comprehensive medical services. Beyond moral and legal responsibilities, the lack of access to basic preventive and responsive medical services to mitigate serious medical events (e.g., infectious disease outbreaks and injuries) in field situations can result in preventable illness or injury, lost productivity, and logistical challenges that lead to mission failure.
The medical and operational needs related to those in DHS care or custody also need to be addressed by a comprehensive DHS operational medicine program. The provision of timely and quality medical treatment to those in DHS care or custody is a legal responsibility of the agency,4 and failure to meet this requirement may expose the department to liability. Beyond liability concerns, inadequate resources to address these needs can substantially impact DHS operations. In some components, for example, the requirement for DHS law enforcement officers to escort detainees to a distant emergency department for even minor injuries and illnesses is costly in terms of both treatment for detainees and the impact on operations of the temporary unavailability of those officers. In 2011, emergency department visits for CBP detainees in the southwest border region alone cost DHS $13 million (Zapata, 2013). At the four busiest stations (out of 139), emergency department visits cost DHS $2.5 million and an estimated
__________________
4Federal courts have held that pretrial medical care, whether in prison or other custody, is required by the Fourteenth Amendment (Wagner v. Bay City, 227 F.3d 316 [5th Circuit 2000]).
90,000 lost agent hours accounting for an additional $3.9 million of agent time (Zapata, 2013).
The diversity of operational and mission requirements among DHS’s component agencies prohibits a one-size-fits-all approach to the establishment of a departmental operational medicine capability. Components and subcomponents need flexibility to develop operational medicine programs that meet the requirements of their unique operating conditions. The Border Patrol’s austere medicine training and protocols program (described in Chapter 4) is an example of the expansion of operational medicine capability beyond that of conventional EMS based on a unique component need. The Office of Field Operations, also within CBP but operating primarily at ports of entry, requires a different medical force capability to deal with the large number of obstetric emergencies encountered regularly (Seifarth, 2013). Yet despite this inherent variability, the committee believes the CMO should set minimum core requirements for operational medicine programs to ensure the timeliness and quality of services, consistent with the practice of other public safety agencies.
Recommendation 8: Establish a comprehensive operational medicine capability to ensure consistent, high-quality medical support during operations.
The Chief Medical Officer (CMO), with input from the Medical and Readiness Committee, should establish a coordinated, department-wide operational medicine capability to ensure that timely and effective preventive and responsive medical services are available to all component employees and others under Department of Homeland Security (DHS) control during routine, planned, and contingency operations. To achieve this capability, the CMO should
- ensure that all DHS and outsourced providers of medical support for operations are appropriately educated and trained, and routinely evaluated through centralized credentialing, baseline training requirements, and a standardized competency assessment process;
- develop baseline treatment protocols to be applied by all component medical providers, and authorize component-specific treatment exceeding the baseline;
- develop, mandate, and maintain uniform reporting methods and system performance criteria for all operational medicine activities across the department to ensure the quality of medical care rendered to all patients;
- identify and provide programmatic support to address significant deficiencies in human (staffing levels and skill sets) and physical resources required to ensure that the medical support needs of the workforce and their non-DHS charges are met; and
- delegate component-level implementation and oversight5of operational medical support to the Component Lead Medical Officers.
The CMO should build on the accomplishments of the DHS Emergency Medical Services Training and Education Advisory Committee and the DHS EMS System Plan to develop a comprehensive operational medicine capability that allows flexibility for adaptation at the component (and subcomponent) level while establishing core requirements. The CMO has overall agency responsibility for medical policy development and standards setting and should assess compliance with policy and protocol and the quality of care rendered to all patients according to prospectively determined outcome measures. However, given the variability in operating conditions among components, it will be critical that the CMO delegate specific execution of the operational medicine program to the CLMOs proposed in Recommendation 4 (see Chapter 6), who would be responsible for overseeing the implementation of DHS standards and policies in the context of their component’s unique requirements. To ensure that CLMOs receive the necessary level of support from their component agencies, the Secretary should hold component agency heads accountable for the effectiveness of such programs and their compliance with department-wide policies and standards.
Medical support for all routine, planned, and contingency operations, including those activities in which care of persons in custody is anticipated, should be explicitly addressed through the medical elements of an overall component operational plan. Such plans, informed by medical threat assessments, would enable the CMO to assess the capacity of components to provide timely and effective medical support during operations. The CMO should delegate responsibility for reviewing medical elements of all component operational plans to the CLMOs to ensure adequate resourcing of day-to-day and surge operations with medical personnel trained and equipped in a manner appropriate to the mission. Where deficiencies in resourcing are identified, OHA should work with components to develop plans for addressing them, considering opportunities to leverage telemedicine and other
__________________
5The committee noted extensive contractor involvement in the direction of medical operations in some components. The role of contractors in the direction and oversight of medical operations should be delineated more clearly following analysis by the DHS General Counsel to ensure compliance with legal requirements set by the Federal Acquisition Regulations regarding inherently governmental functions.
existing and new technologies.6 The Southwest Border Initiative described to the committee provides an example of how OHA can add value by offering programmatic support to address resource deficiencies. That initiative, if funded, would place medical service providers at four high-volume Border Patrol processing stations, potentially saving DHS more than $7 million in unnecessary emergency department visit costs (Zapata, 2013).
The committee heard on several occasions that securing adequate funding for operational medicine programs is a chronic challenge (Ross, 2013; Stair, 2013; Tang, 2013; Wilson, 2013). Metrics that highlight the impact of operational medicine programs on mission capability and success are critical to engendering support from top leadership. As appropriate, the CMO should set benchmarks for components to demonstrate that programs are operating effectively and efficiently. Recommended metrics for performance measurement7 include
- number of treatment encounters conducted outside of conventional workspace;
- type of activity during which treatment was required (i.e., training vs. operational mission);
- classification of person receiving treatment (i.e., DHS employee, subject in custody, third party);
- dispositional indications of severity:
o number requiring hospital treatment or admission,
o number with vital signs meeting criteria indicating a threat to life,*
o number exhibiting injuries defined by protocol as incompatible with life,* and
o number of employees not returned to duty on the same shift;
- dispositional indications of value added:
o number of employees returned to duty on the same shift,
o number of subjects in custody remanded to processing after treatment,* and
o number of third-party patients treated and released.*
Because of the wide variation among their missions, each of the major operating components has specific needs that are best served by support
__________________
6Resources of this type are already in operation within the Coast Guard and Immigration Health Services.
7Indicators requiring enhanced review as sentinel events indicative of increased risk to the department are designated by an asterisk.
programs tailored to its operational functions. For this reason, the committee does not recommend that the management and execution of health, safety, and medical programs be centralized as a departmental shared service. However, some common services should be centralized to promote efficiency and interoperability while ensuring the necessary level of service quality. These include
- services that may be shared for purposes of efficiency of operations, including services not organic to the mission of the organization that can be outsourced;8 and
- services that should be shared to optimize patient outcomes through the application of best practices and to enable effective assessments through the use of common measures and criteria. (Mandated provision of these services centrally also can help ensure that a component cannot apply undue command influence to the process or impede the process through resource restrictions.)
In medicine there are critical areas that time, experience, and public opinion have shown to be highly visible and that require the development and consistent application of common procedures, criteria, and metrics to assist senior management in assessing outcomes and the effectiveness of resource allocations against outcomes. An example for which this has been found nearly universally true is credentialing of health care providers. The basic qualifications for an emergency physician, for example, are well established nationally, but they do require assessment by medical professionals experienced in the understanding of an individual physician’s record, in a dispassionate manner, separate from the hiring process. A common process for obtaining, consolidating, reviewing, and adjudicating health care providers’ credentials can help ensure that any provider within the department meets at least a minimum standard.
OHA has a key role in supporting components’ collective efforts to carry out the DHS mission and, in so doing, in contributing to the “one DHS” concept. Mission support programs and services represent significant investments, and in the current financially constrained operating environment in which programs must compete for funds, strategic allocation of resources and demonstration of program effectiveness are essential. DHS has been criticized for making acquisition decisions on a program-by-program and component-by-component basis (GAO, 2012). The committee found examples of such practices during its information-gathering process.
__________________
8Personnel security investigations are an example of a service that some, though not all, agencies find are most cost-effectively outsourced either to a different government agency that specializes in this work or to an appropriately qualified contractor.
For example, occupational health and medical services are procured at the component and sometimes the local site level, resulting in hundreds of independent contracts and interagency agreements, with little in the way of technical oversight to ensure service quality (Kosh-Suber, 2012). By taking a functional, cross-component perspective, OHA has an opportunity to add value in this area. Centralizing common critical services would enable alignment of component mission needs with department-level goals. Although OHA has made some progress in this area (e.g., centralized credentialing of prehospital medical providers), a more formalized approach for obtaining buy-in from components should be used to accelerate the process of establishing centralized health, safety, and medical services.
Recommendation 9: Centralize common services to ensure quality and to achieve efficiencies and interoperability.
To ensure that health, safety, and medical programs at the component level are effective, efficient, and of high quality, the Office of Health Affairs should develop and deliver certain health-related services common to all components. Centralized common services, to be recommended by the proposed Medical and Readiness Committee and approved by the Chief Medical Officer, should be adopted and implemented by the components unless a component-developed business case demonstrates otherwise. These actions would facilitate integration, department-wide efficiencies, and evaluation against common objectives using common standards and metrics.
Recognizing that the CMO, in consultation with the proposed CLMOs, would best be able to determine which services, if centralized, would improve in both efficiency and quality, the committee did not wish to be prescriptive in this area and offers the following only as examples of services that the CMO might wish to consider centralizing:
- medical quality management, including credentialing, maintenance of certification, and licensure;
- health information management capabilities as outlined in Recommendation 11 in Chapter 8;
- health professions education and training;
- medical logistics, including purchasing and distribution;
- public health services and consultations (e.g., immunization programs, travel medicine, risk communication, wellness programs); and
- requirements development and technical oversight for contracts, interagency agreements, and memorandums of understanding with
outside entities providing health and medical services to DHS and its components.
Instead of attempting to develop a comprehensive list of services that should be centralized, the committee proposes that the CMO use the following criteria to develop a prioritized list of candidate services/programs that would appropriately be delivered with a centralized approach:
- The service is well defined and well circumscribed.
- It is not an operational aspect of the component’s mission but is required in support of the mission. This latter determination could be made by either component leadership or DHS headquarters.
- OHA can develop a DHS-wide set of criteria, standards, and procedures for the provision of the service using a combination of those that are nationally accepted and those that are DHS-specific as required to meet particular departmental needs.
- Law or public opinion expects the success of the service to be demonstrable against standards.
The following are additional desirable but not required features:
- The service can be fairly costed on a standardized unit basis for the purposes of component chargeback.
- The service is not unique to DHS, and there is a track record of its being provided in a shared manner to diverse components of other organizations.
Members of the proposed Medical and Readiness Committee, as representatives of component heads, should review and prioritize services on the list and suggest additional services not anticipated by OHA. As centralized services are developed, OHA should establish parallel assessment and accountability metrics for use across the department. Such metrics could be used in performance evaluations of component heads to ensure that components are held accountable for demonstrating the achievement of an effective and efficient program.
It should be noted that the committee does not mean to imply that OHA is the only entity that could execute a shared or centralized health-related function. If there are functions that one component, or even another government agency, already operates in an exemplary manner, DHS could choose to have that agency execute this function for the entire department (or for those components opting in) using a center of excellence model (see Figure 6-1 in Chapter 6).
DHS (Department of Homeland Security). 2012 DHS emergency medical services system plan. Washington, DC: DHS.
DoD (Department of Defense). 2006. DoD instruction:Deployment Health. DoDI 6490.03. Washington, DC: DoD.
GAO (U.S. Government Accountability Office). 2012. DHS requires more disciplined investment management to help meet mission needs. GAO-12-833. Washington, DC: GAO.
Garbe, B. 2013. Department of the Interior medical clearance programs. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Heck, J. J., and G. Pierluisi. 2001. Law enforcement special operations medical support. Prehospital Emergency Care 5(4):403-406.
Kosh-Suber, J. 2012. DHS health care quality committee. Washington, DC: DHS.
Lang, W. L. 2007. Office of component services. Washington, DC: DHS.
Leffer, M. 2013. FOH Office of Health and Safety Deployments: Department of Homeland Security. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Lewandowski, C. T., and D. Weeks. 2013. Overview of the Federal Air Marshal Service medical program. Presentation at IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 5, August 27, Washington, DC.
Polk, J. D. 2013. The charge to the committee. Presentation at IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 1, March 5, Washington, DC.
Ross, D. 2013. National Park Service operational and emergency medical services. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Seifarth, W. 2013. Operational medical at DHS. Presentation at IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Spottswood, P. 2013. Medical evaluation and clearance programs. Presentation at IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 1, March 5, Washington, DC.
Stair, R. 2013. Operational medicine at DHS: Secret Service. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Tang, N. 2013. Academic model of medical direction and operational support for law enforcement. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Wade, D. 2013. Medical structures and functions in the FBI. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Wilson, D. 2013. Operational medicine at DHS: Office of Border Patrol. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
Zapata, I. 2013. FY2015-FY2019 Southwest Border Health Initiative business case. Presentation to IOM Committee on DHS Occupational Health and Operational Medicine Infrastructure: Meeting 2, June 10-11, Washington, DC.
















