2
Why Educational Attainment Is Crucial to Improving Population Health
The two major premises underlying all of the discussions in this workshop were that education is an important determinant of health and that any successful effort to improve health at a population level will depend on improving the overall education level of the American public. In the workshop’s first keynote presentation, Steven Woolf, director of the Center on Society and Health and professor of family medicine and population health at Virginia Commonwealth University, reviewed the evidence base for the strong relationship between education and health. He also discussed a strategy for getting the public health and education policy communities working together toward common goals.
“It is clear that education is a big deal in terms of public health outcomes, and it is appropriate for the Roundtable on Population Health Improvement to make this a priority topic,” Woolf said at the start of his presentation. The data show, for example, that by age 25, U.S. adults without a high school diploma can expect to live 9 fewer years than college graduates. Similarly, those individuals with less than a high school education are almost twice as likely to die in a given year as those with a professional degree, and even those who have completed college with a bachelor’s degree are 26 percent more likely to die than those with professional degrees (Ross et al., 2012) (see Figure 2-1). Woolf noted that evidence accumulated since the 1960s indicates that the impact of educational attainment on health appears to be growing. “This is not a static problem,” he said, “and in our knowledge economy, the difference in health between educated and non-educated Americans has progressively
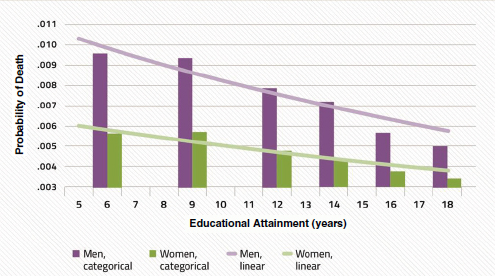
FIGURE 2-1 All-cause mortality risk for men and women by years of education.
NOTE: Data derived from regression modeling.
SOURCE: Woolf presentation, June 5, 2014, adapted from Ross et al., 2012, Virginia Commonwealth University Center on Society and Health.
widened.” Woolf added that while this appears to be a problem in all industrialized countries, it is especially so in the United States. The data also show that while there are steadily increasing benefits to getting more education, there is a major jump in the health benefits—what Woolf described as a “step-like benefit”—associated with high school graduates also graduating from college (see Figure 2-2).
What the data are showing, Woolf said, is that people who do not graduate from high school are experiencing an increase in mortality rates while everyone else is experiencing a decline in mortality. This is partly a selection phenomenon, he said. “The people who don’t graduate from high school over time are becoming a more select population of sicker people because of the movement of the rest of society into the more educated population,” Woolf said.1 This trend is particularly true for white Americans and especially white women (see Figure 2-3). In 2008, white men with fewer than 12 years of education had the same life expectancy as U.S. men born in 1972, while white women with this level
_____________________________
1 As it becomes rarer for people to not finish high school, the increasingly small percentage of individuals who do not finish are becoming more unlike the rest of the population—and, in particular, the ones who do not finish high school now are at significantly higher risk for health problems than those who did not finish high school several decades ago.
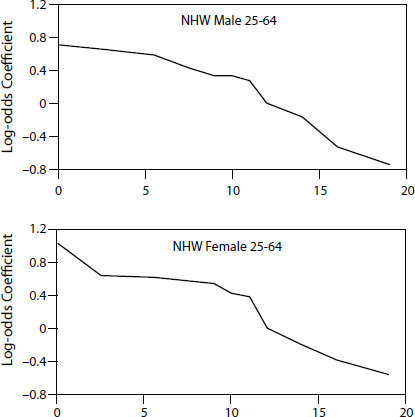
FIGURE 2-2 The relationship between education and health shows clear step-like behavior at 12 years of formal education.
NOTES: Enlarged markers indicate high school diploma and bachelor’s degree attainment. NHW = non-Hispanic white.
SOURCE: Woolf presentation, June 5, 2014, adapted from Montez et al., 2012, Virginia Commonwealth University Center on Society and Health.
of education had the same life expectancy as U.S. women born in 1964 (Olshansky et al., 2012).
The link between education and health is not confined to death rates, Woolf said; it applies to the prevalence of major diseases as well. “If you look at any number of health metrics, you again see this graded relationship in terms of education,” he said. For example, self-reports of fair or poor health are some five-fold higher in high school dropouts than among those with a bachelor’s degree or higher (see Figure 2-4). Similar trends are seen for most other major diseases, he said (see Table 2-1). The numbers show that there is “nothing we do in clinical medicine at the bedside
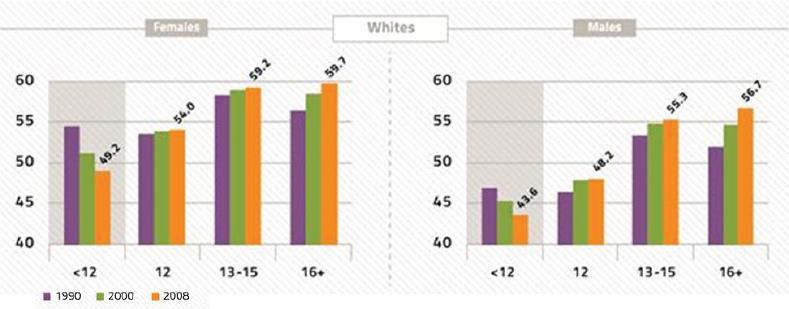
FIGURE 2-3 Life expectancy at age 25 years by educational attainment level in years from 1990, 2000, and 2008.
SOURCE: Woolf presentation, June 5, 2014, adapted from Olshansky et al., 2012, Virginia Commonwealth University Center on Society and Health.
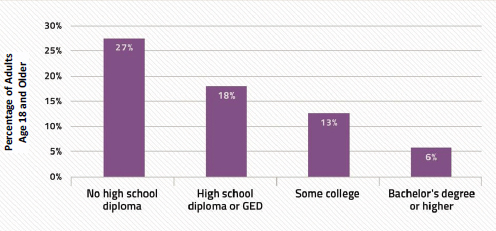
FIGURE 2-4 Self-reports of fair or poor health.
SOURCE: Woolf presentation, June 5, 2014, adapted from Schiller et al., 2012, Virginia Commonwealth University Center on Society and Health.
TABLE 2-1 Prevalence of Diseases Among Adults Age 18 or Older, 2011
| Disease | Less Than a High School Diploma (%) | High School Diploma or GED (%) | Some College (%) | Bachelor’s Degree or Higher (%) |
| Coronary heart disease | 10.2 | 7.5 | 7.4 | 5.4 |
| Stroke | 4.7 | 3.4 | 2.7 | 1.7 |
| Emphysema | 3.3 | 2.5 | 1.9 | 0.7 |
| Asthma (current) | 8.1 | 8.3 | 8.6 | 7.1 |
| Chronic bronchitis | 5.1 | 5.2 | 5.0 | 2.3 |
| Diabetes | 15.1 | 10.5 | 9.6 | 6.5 |
| Ulcers | 9.8 | 7.4 | 8.0 | 5.0 |
| Kidney disease | 3.8 | 2.2 | 2.1 | 0.7 |
| Liver disease | 2.4 | 1.4 | 1.5 | 0.8 |
| Chronic joint symptoms | 35.0 | 33.3 | 34.6 | 25.2 |
| Hearing trouble | 18.8 | 19.3 | 18.1 | 13.5 |
| Vision trouble | 14.0 | 10.4 | 9.5 | 6.3 |
| No teeth | 16.2 | 9.6 | 7.1 | 3.6 |
NOTE: GED = general education diploma.
SOURCE: Woolf presentation, June 5, 2014, adapted from Schiller et al., 2012, Virginia Commonwealth University Center on Society and Health.
or in the exam room that achieves differences in the numbers that we’re seeing,” Wolf said. “Education is that big of a deal.”
Given the overwhelming data showing the major impact that educational attainment has on health and mortality, Woolf said, the question becomes: How can the health and education communities use this evidence in a pitch to those who can do something about it? As an example, he said, if a goal is to reduce admissions to emergency rooms, policy makers need to understand that mental health issues are the leading conditions that are contributing to those admissions, and that psychosocial wellness and education are closely associated with mental health outcomes. People with less wellness and less education are at a sharply higher risk for mental health problems. If the goal is to slow down the alarming increase in mortality rates among American women—mortality rates for women have increased in 42 percent of U.S. counties since the 1990s (see Figure 2-5)—then the link between this phenomenon and educational attainment has to be a critical piece of the argument on what kind of actions the country needs to take, Woolf said.
How is a person’s education related to his or her health? Woolf said that there are three broad categories of possible relationships (see Figure 2-6). First, education has a number of downstream benefits that may lead to improved health, including a higher income, lower odds of being unemployed or having a job that does not provide health insurance, various social and psychological benefits that arise from the social environ-
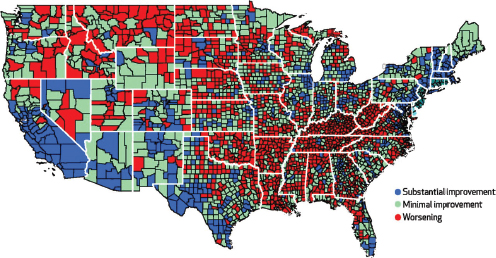
FIGURE 2-5 The change in female mortality rates from 1992–1996 to 2002–2006 in U.S. counties.
SOURCE: Woolf presentation, June 5, 2014, citing Kindig and Cheng, 2013.
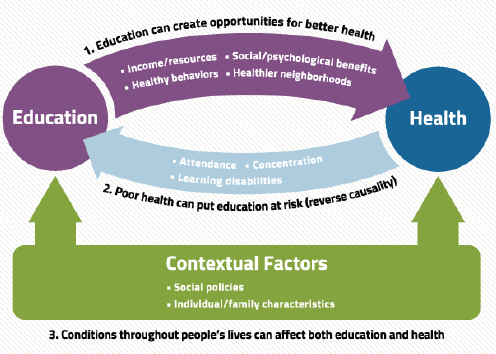
FIGURE 2-6 Exploring the link between education and health.
SOURCE: Woolf presentation, June 5, 2014, Virginia Commonwealth University Center on Society and Health.
ment at school, and the cognitive and social skills that are acquired in high school and college. Other downstream benefits include the resources and knowledge to adopt healthier behaviors and the resources to live in healthier neighborhoods. Second, some suggest that there is a selection phenomenon at work, with people who are less healthy being less likely to succeed and advance in their education so that the people who do end up going farther in school are healthier; in this case better health would lead to more education rather than the reverse. Woolf said that while there is a body of evidence suggesting that education affects health more than the other way around, it is still important to try to improve the health and wellness of students so they can succeed in school. The third possibility is that various contextual factors—what an epidemiologist would call confounding variables—affect both education and health. The list of contextual factors would include adverse childhood events that can affect brain development and social, emotional, and cognitive development as well as childhood health and nutrition, parental and maternal health, stress, immigrant status, gender, and socioeconomic status. He noted that data show a clear link between adverse childhood events and increased
odds of adult diseases, including obesity, diabetes, heart disease, cancer, stroke, chronic lung disease, and depression.
Woolf reported that an animated discussion had been prompted at the previous day’s National Institutes of Health (NIH)-sponsored workshop by questions about how to measure the independent effect of education by adjusting for particular variables and contextual factors. This is more than just an academic question, he said; addressing these contextual factors in terms of social and economic policy, jobs, unemployment, and community development should concern policy makers beyond those interested solely in education reform and health care reform. The challenge, he said, is to think of this problem as a whole and not as isolated components. Education is a system; it is a package deal. Education comes with a set of interrelated variables, such as race and ethnicity and income, and this is true at any particular moment in time in the life course and also in the early years that put a child on the path to a successful education. Any strategy for achieving success must also be a package deal, Woolf said. It has to look at the whole system—the whole set of issues together.
In the last part of his presentation, Woolf turned to the subject of “silos” and the need to improve the connection not just between those who are concerned about health and education but also between these people and those who are interested in jobs and social issues. As examples of the education and health silos, he cited two reports: Rising Above the Gathering Storm published in 2007 by the National Academy of Sciences, the National Academy of Engineering, and the Institute of Medicine (IOM), which came from the education silo, and the U.S. Health in International Perspective, published by the National Research Council and the IOM, from the health silo. Both reports paint a dire picture, one of them of the educational system and the other of the nation’s health status, yet neither of the two communities has thought enough about the role of the other in helping with their respective agendas.
In an attempt to break down these silos, Woolf and his colleagues at the Center on Society and Health have conducted the Education and Health Initiative, part of the center’s Connecting the Dots portfolio. The education and health aspect of this initiative is aimed specifically at raising awareness among policy makers in education and health about the health implications associated with educational attainment—the subject of this workshop—and at helping researchers in these communities develop the tools to communicate their findings in a way that is responsive to their target audiences. Accomplishing the latter requires that each community understand the issues that policy makers in the other community are facing and to then use that understanding to develop better research questions. “This is a different model of research than the current model
of investigator-initiated research, which is driven by the intellectual questions that interest academics,” Woolf said.
Other important components of silo-busting are stakeholder engagement and strategic communication. “We need to package evidence in a way that is compelling and convincing to policy makers,” Woolf said, acknowledging that this is a particularly weak skill in today’s public health community. Target audiences include not only policy makers at the federal, state, and local levels, but also national organizations, health care systems, businesses and employers, foundations, the media, and other disciplines in academia. In the education policy area, for example, Connecting the Dots has reached out to a wide range of public and private sector organizations. Each of these organizations, Woolf said, already has its own agendas and sets of talking points, but Connecting the Dots is providing the organizations with an additional line of argument that these organizations have reported is valuable to them. “The resources that we are able to provide are very helpful,” he said. “I am here to tell you that this cross-sector dialogue works very well.”
As an example, Woolf cited the business community’s positive response to the message that educational attainment has a direct impact on the health care costs that are becoming an increasing burden for companies. Subsequently, reforming the nation’s education system will have significant effects on the companies’ “bottom line” beyond the effects related to the companies’ need for an educated and skilled workforce. As evidence that this message is having an effect, Woolf said that the Virginia Chamber of Commerce’s recent blueprint for the newly elected governor cited population health and wellness and improved education among the eight domains on which it will focus.
One issue that often gets raised in discussions with policy makers is that given today’s focus on the short term, the returns on investment from childhood programs take too long to interest government or business leaders. In answer to that concern, Woolf said that not only are there significant returns on investments in improving adult health, but an increasing amount of evidence shows that investments in health made in early childhood start paying off at an early age. He cited the work of Laurie Miller Brotman (a subsequent speaker in the workshop), which shows that early childhood investments have a positive impact on body mass index that can be seen in children as young as 8 years old. To its credit, Woolf said, the business community understands this connection, and businesses are participating in initiatives around the country that are making significant investments in early childhood. He said he is also encouraged by the financial industry’s engagement in early childhood through novel investment instruments such as social impact bonds.
Woolf and his colleagues have identified a model for strategic com-
munication that divides the target audience into three categories. The first category comprises those who have the lowest level of awareness and who have not yet “connected the dots.” For that group, the best message is a simple one: Health and education are linked. The second category includes those who understand that there is a link between education and health but think that it is not a big deal and that reforming health care and health behaviors is more important. Quantification using compelling data is more important with this group. The third category would be the “choir,” those who know that there is a critical connection between education and health and who now want an evidence-based action plan. For individuals and organizations in this group, it is important to show what works and how to prioritize effective strategies.
Recognizing this segmentation, Woolf and his collaborators have started developing materials to engage each of these audiences. One example is a YouTube video with the message that education matters more than ever to health. This video received 10,000 views in the first week it was available, which Woolf said is a big number in public health media. Another approach is to create layered issue briefs that enable members of each of the three types of audiences to get the information they need at a level they can understand and use.
Woolf then turned to the subject of stakeholder engagement. Among the stakeholders who must be engaged are members of the community, and in particular, the vulnerable populations in the community who know firsthand about these issues. Stakeholders other than the affected population also need to be engaged. Woolf said that he and his colleagues worked for 1 year to build relationships with health and education organizations to develop partnerships for reaching out to the broad range of stakeholders. “Education and teacher organizations that I never heard of before are distributing our materials, along with the public health networks that I am more accustomed to,” he said. “I think this kind of cross-sector partnership and collaboration is the key if we are really going to connect the dots.” As a final comment, Woolf said that although, as his model emphasizes, there is a tremendous need for collaboration in this area, federal agencies and funders are still stuck in their silos. For example, research about education and health has no natural government home because funders like NIH view education as outside their purview.
Robert Kaplan started the discussion by noting that the charters that govern what federal agencies can and cannot do have a great deal to do with keeping those agencies in silos. For example, the National Science Foundation is not allowed to fund work in health care or undergraduate
education and NIH is not permitted to fund educational research. The Agency for Healthcare Research and Quality, where Kaplan works, is not supposed to be concentrating on public health, but rather only with health services delivery. Kaplan then recounted a plea from the director of a government science agency. At the June 4 meeting sponsored by NIH, this director said that people outside of government have to get the message out that collaboration across these disciplines is essential to fully address the nation’s challenges in both education and health. Woolf added that the status quo of the bureaucracy will allow for only incremental change. “The plea I would make to the Population Health Roundtable,” he said, “is that the agenda for the Roundtable can only be achieved through transformational change.” Woolf added that one thing he has learned through his interactions with Congress is how important it is to have an “elevator speech”—that is, a 1-minute summary of important points.
Debbie Chang of Nemours asked Woolf to list some of the bold steps that he would like to see the Roundtable take. Woolf said the first thing would be for members of the Roundtable to make a call for transformational change. Another opportunity is for the Roundtable to highlight the idea that building closer ties between the health and education fields will benefit both communities as well as other groups, such as those in community development and finance. “Helping to have a cross-sector conversation, being a facilitator and catalyst for bringing these communities together, and helping them recognize where they share aligned incentives is a real opportunity for the Roundtable,” he said.
Marthe Gold of the City College of New York asked Woolf if he had any ideas on how to build support for this movement at the grassroots level and to help local groups take steps to improve the educational experience at the community level. Woolf said the same thing that is needed at the national level—cross-sector dialog—is important at the community level. As an example, he said, Connecting the Dots has started an initiative that involves getting residents in public housing together with the local housing authority, a developer, public health leadership, the leadership of the local health systems that serve that community, and the Urban Institute to think about how to apply evidence-based strategies to improve population health in public housing.
Concerning the education community, Woolf noted that Brotman would be speaking later in the workshop about an initiative in New York City that involves all the schools in Brooklyn. In Richmond, Woolf’s Center is bringing representatives of the local school system together with leaders of the three main health systems to work with each other in the area of early childhood development. Woolf said that this conversation involves an intentional effort to align incentives around education.
Kaplan added that these conversations ultimately have to be at the local level because federal education policy has so little impact on what states and school districts do.
George Isham commented that slides in both the Woolf and Kaplan presentations concerning the link between education level and mortality would make a good 1-minute elevator speech, and he asked Woolf what else he would include in a concise pitch to policy makers. Woolf replied that there is no blanket message. “We need to do the equivalent of market research and go to audiences and figure out what they need,” he said, acknowledging that this is not something that researchers are particularly good at doing. “We need to take the resources that we have in our field and make a more serious investment in learning from the communication sciences, advertising, and marketing.” Woolf noted that Washington University in St. Louis and the University of Texas at Austin have notable efforts for doing just that.
Woolf did say that there are different communication tools that would be useful for the three categories of audiences that he described in his presentation. For the first audience, where the goal is simply to raise awareness, social media and other new technologies can convey messages quickly and in a visually interesting way, and the field needs to learn how to exploit those capabilities to connect with this type of audience. For the second audience, infographics of the type that appears in the Washington Post or New York Times can be valuable tools because of their ability to condense large amounts of data and present them in a visually rich manner. His group has just started experimenting with this approach, he said. For the third audience, market research is critical because of the sophistication level of this group. “It is critically important to know exactly what they want to know,” Woolf said.
In response to a question from Terry Allan of the National Association of County and City Health Officials and the Cuyahoga County Board of Health about community development and healthy neighborhoods, Woolf said that a number of communities around the country have exciting cross-sector collaborations that are ongoing, many of which have been stimulated by community transformation grants from the Centers for Disease Control and Prevention. He noted that communities with vulnerable populations already see education as the way to break the cycle of persistent poverty that exists in many U.S. cities, and now they are starting to see education as the path for revitalizing neighborhoods and improving the health of the community. He also said, in response to a question from Isham, that the business community is coming to appreciate the connection between education, early childhood development, and the health of its employees.












