Chapter 4 focuses on the topic of priorities and strategies for strengthening information management systems. Health information and digital health solutions are available to improve day-to-day systems and to prepare for and improve epidemic response. The critical capacity for disease surveillance can also be augmented by both new and existing technology solutions.
HEALTH INFORMATION SYSTEMS
Improving Epidemic Response Using Digital Health Solutions
Kate Wilson, Director of Digital Health Solutions at PATH, focused on possible options for improving epidemic response using digital health solutions. She suggested a shift in focus away from specific products, functions, or solutions and toward how people actually utilize the information and technologies that are available to them. Striving for a broader health information system and improved functional applicability would enhance flexibility: for example, situating a surveillance function within a health information system, rather than implementing a separate surveillance system. Broadly, she called for improved usability in making health information systems designed to be easier and more accessible for their users.
Institutionalizing Digital Health Services
Despite the proliferation of digital health services that have launched over the past 10 years,1 only few—if any—have yet scaled, reported Wilson. She defined a digital health intervention as being at scale when its routine
__________________
1 A reported 728 services were active as of August 2015, with an increase of more than 30 percent in the number of mobile health launches per year between 2005 and 2011 (Sources: The Bill & Melinda Gates Foundation, based on Groupe Speciale Mobile Association [GSMA] Mobile for Development Intelligence data; GSMA Mobile for Development deployment tracker, accessed October 4, 2015).
use is institutionalized by either governments or end users as an approach to delivering health impact. She suggested that the goal of institutionalizing digital health services could parlay into a range of advantages from various stakeholders’ perspectives. For example, most health care providers have already adopted a standards-based suite of digital tools; most major nongovernmental organization (NGO) programs and donors’ health-related investments leverage those nationally endorsed, sustainable tools. For technology providers, products and services become more economically sustainable and for mobile operators, digital health services can drive long-term value creation.
Lessons Learned About Health Information Systems During Previous Outbreaks
Regarding past instructive experiences during an outbreak, Fitter mentioned that after the Ebola virus disease (EVD) outbreak, the U.S. Centers for Disease Control and Prevention (CDC) viral hemorrhagic fever database did not include enough information beyond patients’ names to recognize individual records, given that thousands of affected people had their data input at facilities in different locations. Frankfurter remarked that based on his experiences with EVD response, health information systems were not optimized to be scaled down to the individual level. He explained that while the purpose of informatics is to take individual patient-level data and scale it up for population-level analysis, for smaller organizations it is important to be able to scale down to make decisions on the individual level. He suggested information technology (IT) systems be structured in such a way that makes it easy to go either up or down the chain to broaden or narrow the picture. Greenough commented that following the 2010 earthquake in Haiti, the health information system had the advantage of being able to combine information from more than 50 separate sites, because they all used the same platform. However, he noted that population-based data were important in Haiti, but they also needed to geocode the data, and questioned whether this was a security risk that warranted further consideration.
Suggested Principles for Digital Health Solutions and Investments
Wilson offered a set of guiding principles related to the implementation of digital health solutions and information systems. She described how ensuring sustainability requires partnering with countries to derive a realistic picture of costs that they can sustain in the future and those they would be unable to maintain. In the context of creating country-owned systems built on existing capacities and infrastructure, she suggested that open-source
products should be adapted, built on, and informed by related products, thus being structured and tailored to be optimal for each country. She further called for attention to the misrepresentation that the developed world can do a better job of implementing projects than the developing world can, remarking that in fact, the developing world is often more innovative in their use of these types of products.
Wilson emphasized that health information systems should be interoperable, in that they work with a country’s previous investments, within its existing infrastructure, and will continue to operate with systems put in place in the future.2 She explained that regardless of the specific system being implemented, it is very important to establish an agreed-upon way to collect and digitize various kinds of data elements at the beginning. Having a standard set of data elements in place can obviate most future problems, because it becomes relatively straightforward to implement different platforms and create a coordinated system (see Box 4-1).
“Systems that are built to be interoperable from the outset and designed to last in the long term have the advantages of enhanced flexibility and repurposing potential.”
—Kate Wilson, Director of Digital Health Solutions, PATH
Wilson outlined a set of characteristics that, in her opinion, should ideally apply to every digital health investment. The initiative should be triggered and selected according to the health system’s needs, and then mandated and delivered by the Ministry of Health. It should be underpinned by committed, realistic long-term funding and robust program management so solutions have time and support to iterate, evolve, and integrate into existing systems and practices, she continued. It should be designed to conform to agreed-upon standards, but also created with the participation and input of the end users and long-term implementers.
Potential Levers for Implementing Effective Health Information Systems
Paul Biondich, Research Scientist at Regenstrief Institute, Inc., suggested that once stakeholders agree on the “destination” for an effective health information system and develop the roadmap for reaching it, there are two concurrent streams that can accelerate the process—catalyzing national digi-
__________________
2 She noted that the United States provides an example of what not to do, because its health system has multiple platforms that do not allow for interoperability (i.e., the U.S. Department of Veterans Affairs compared to another electronic medical records system).
tal health investments and investing in cross-market levers for scaling. He outlined seven components implicated in each of those two streams:
- Case for action
- Leadership
- Effective product
- Viable economic model
- Supportive policy, regulation, and standards
- Effective program management
- Human capacity
For each component, he offered examples of near- and longer-term potential country investments, as well as near- and longer-term possible cross-market investments for scaling digital health interventions (see Tables 4-1 and 4-2).
HEALTH INFORMATION SYSTEMS: HIGHLIGHTED OPPORTUNITIES
Biondich reported on three suggestions that arose out of the discussion around building health information systems and leveraging existing capacity within various countries.
TABLE 4-1 Potential Country Investments for Scaling Digital Health Interventions
| Near-Term Investments | Longer-Term Investments | |
| Case for Action | Develop rigorous total cost of ownership (TCO) models and collect consistent health impact data on each implementation | Sponsor national advocacy and education efforts on the impact seen from digital health investments |
| Leadership | Require government and donor coordination before allocating investments | Invest in design and implementation of country-led strategies |
| Effective Product | Direct investments toward making products inter-operable with existing infrastructure | Evaluate more rigorously each project against agreed performance levels and health outcomes |
| Viable Economic Model | Identify the “gives” and “gets” for each product before rollout by stakeholder | Require that each rollout identifies a viable long-term business model after catalytic financing ends |
| Supportive Policy, Regulation, and Standards | Support national development of eHealth architecture and implementation plans | Provide incentives to adopt agreed standards and policy frameworks to national governments |
| Effective Program Management | Require new investments to have dedicated program management staff through national rollout | Capture and share best program management practices within a country |
| Human Capacity | Sponsor greater local university and entrepreneurs’ participation from the outset | Embed national informatics capacity in projects versus using overseas staff |
SOURCE: Wilson presentation, August 6, 2015.
TABLE 4-2 Potential Cross-Market Investments for Scaling Digital Health Interventions
| Near-Term Investments | Longer-Term Investments | |
| Case for Action | Create better advocacy toolkits to educate national leaders and donors | Develop modeling tools to demonstrate return on digital health investments |
| Leadership | Call for a global action plan for digital health investments | Convene stakeholders to develop the action plan and oversee implementation |
| Effective Product | Direct investment toward a smaller pipeline of best-in-class cross-cutting platform | Cultivate private-sector technology firms to invest in digital health platforms |
| Viable Economic Model | Develop financial forecasting tools that any country can use to consider TCO and return on investment of new digital health tools | Develop innovative financing mechanisms (e.g., demand aggregation) |
| Supportive Policy, Regulation, and Standards | Continue more inclusive development of shared standards and best practices frameworks | Negotiate aggregated licenses for standards and agree on global standards for developing world (e.g., WHO/ITU for NCDs) |
| Effective Program Management | Capture and sharing of best practices in more digestible, practical forms | Investment directed toward most effective models for implementing digital health |
| Human Capacity | Sponsor regional peer networks and specialized capacity programs targeted toward practitioners | Develop the next cadre of eHealth leaders through university-level health informatics programs in emerging markets |
NOTE: ITU = International Telecommunication Union; NCD = noncommunicable disease; TCO = total cost of ownership; WHO = World Health Organization.
SOURCE: Wilson presentation, August 6, 2015.
National Data Use and Health Information Systems Capacity Development
To build effective health information systems, multiple participants emphasized the importance of educating all health care and support workers, not only in how to use those systems but also in how to implement, configure, and customize them. Doing so involves combining two forms of capacity building: “strength at source” and “strength at scale.” The former refers to long- and short-term training for workers already in the field and outside of traditional educational circumstances, for example, in the form of vocational training in fundamentals of information fluency. Biondich
cited examples of workers in the field who have not had the opportunity to use information to influence their care delivery, and that when it does become a routine part of their practice, it has the knock-on positive effects downstream of improving the quality of information and how it is gathered. “Strength at scale” in the context of this type of capacity development, according to Biondich, would involve working within countries’ educational systems to embed health information systems training, health informatics, and data use skills within their curriculums on two tiers: health professional organizations and universities, as well as vocational training centers and polytechnic organizations. A further objective offered by multiple participants would be to create a peer-learning network among countries to build a common curriculum and to govern the priorities of the content that is developed.
Several other participants also suggested incentivizing and educating health care workers to use health information systems. Fitter noted that increased transparency of data can actually serve as motivation for people to use the system. Greenough suggested that developing the capacity to rapidly analyze data could also serve as an incentive for users to continue to use the technology.
Strategic Reuse of Common Open Technology Platforms
A second topic of discussion was the strategic reuse of common open technology platforms, reported Biondich. George Kesse of Mpharma noted that during a disease outbreak, it often happens that various partners arrive with a collection of specific information systems to support the response to that outbreak. However, after the outbreak, when the partners leave, the country is left to maintain those information systems in the absence of both context and adequate local capacity, leaving “yet another tool that needs to be locally maintained and sustained.” Biondich advised that if countries had common, freely available, standards-based, open platforms for health information systems, it would prevent the duplication of effort, reduce costs, and support local sustainability. Having internationally standardized, adaptable, and open platforms for data collection across all levels (including the local level) would allow a country to build a platform on its current infrastructure and then locally customize and optimize it for the country’s specific needs. Furthermore, Biondich speculated that these types of open platforms are by nature easier to build capacity around, as well as being potentially more flexible and responsive to outbreaks that emerge. Systems that meet certain qualities could then be strategically reused.
Systematizing a common platform is a complex adaptive problem that necessitates a multidisciplinary approach, cautioned Biondich. Partners involved would range from communities developing common open plat-
forms, to funders of health delivery activities, to workers on the ground, to the Ministries of Health. On the local level, resources required would be local representation within the governance of the open platforms, as well as local engineering support for technologies and training related to the common components. Appropriate documentation would make product consumption easier for new users, and financial support would be needed to sustain growth. Biondich argued that common platforms reduce the proliferation of redundant systems and encourage sustainability because they are collectively resourced public goods. These effects could further impact improved information sharing and surveillance activities within and between countries and regions.
Architectures Based on “Readily Malleable” Routine Information Systems
Biondich explained that a readily malleable routine information system (RIS) is one that allows for adaptation during emergency circumstances. Its foundational components are readily available for emergent outbreaks, coupled with a self-regulating RIS that is capable of serving as a signal detector and triggering itself during potentially emergent infectious events, thus reducing the timespan for alerts. It is an “urban plan” that facilitates leadership during emergency conditions and fosters ministry coordination toward reuse of common components and competencies. The aim of a malleable system is that in circumstances of disease outbreak, it allows for working with and within the existing environment, tools, infrastructure, and capacities rather than bringing in an entirely new system. The community is incorporated as a partner in the health system and the capacity for rapid analysis of data is enhanced.
DISEASE SURVEILLANCE SYSTEMS
The crucial role of effective disease surveillance—both within and between outbreak periods—was a key topic of discussion throughout the workshop. Nguku and Nasidi of the Nigerian CDC characterized disease surveillance as the “backbone of disease control.”
Lessons from Surveillance Response to West Africa EVD Outbreak
Fitter contextualized the discussion of disease surveillance systems by detailing the problems that arose in response to the West Africa EVD outbreak. The Integrated Disease Surveillance and Response (IDSR)3 frame-
__________________
3 For more on the IDSR framework, see http://www.cdc.gov/globalhealth/healthprotection/ghsb/idsr/what/objectives.html (accessed October 20, 2015).
work, designed to strengthen health systems’ core capacities for surveillance and response, was adopted by Guinea, Liberia, and Sierra Leone, but it was not fully implemented in any of those countries. Fitter noted that prior to the outbreak, the countries’ health systems lacked the surveillance capacities for detection, reporting, supervision, and feedback mechanisms such that “as the outbreak engulfed the national health systems and hundreds of health organizations responded, the people and tools which comprised ‘the system’ could not keep up and became increasingly disorganized.”
The affected West African countries’ telecommunications, transportation, laboratory, and clinical infrastructures were too weak or compromised to facilitate the necessary outbreak response. Workforces lacked sufficient training or capacities to collect, manage, or disseminate information, despite the thousands of community health workers and volunteer responders who were engaged. Many of those responders were working across multiple domains, Fitter said: different laboratories were under different technical oversight, and providers from different groups were running various treatment units. A case-reporting surveillance tool was put in place but its efficacy was hampered by its length, incomplete data entry, and untrained staff. Alternate data sources and systems were put into place (e.g., decedent registries, call centers, logbooks and spreadsheets, and surveys) but a robust unique identification system bridging all services was still lacking. However, Fitter highlighted some of the innovations that did arise: mobile data collection for surveys, contact tracing, geocoding, supervision, and technical assistance; and cloud hosting for central data storage and integration, case and laboratory registries, and analysis.
Lessons from Uganda’s IDSR Strategy
Aceng provided an overview of Uganda’s integrated disease surveillance and response strategy, adopted in 2000, as an example of an effective day-to-day system that can respond to emergency situations. The strategy mirrors the health system’s structure in its coordinated levels of response and responsibilities instigated from the community or village through the district, regional, and national levels. At each level, there are designated surveillance “focal persons” who routinely receive and disseminate information from health facilities and community health workers, on the basis of which they carry out investigations on priority diseases and report accordingly through the health management information system. With the support of the U.S. CDC, they have also initiated a field epidemiology training program to build a pool of epidemiologists to support surveillance efforts.
A set of standardized clinical and community case definitions was also developed to improve community health workers’ ability to detect atypical
outbreaks. Information on any unusual occurrences or atypical outbreaks is remitted to the epidemiologist surveillance division of the Ministry of Health and the chair of the National Task Force. Verified information triggers further investigations, higher-level action, and daily task force meetings. Aceng identified contact tracing as another key component of the strategy, carried out by a team of surveillance officers deployed during outbreaks. Each officer is assigned a specific set of contacts (no more than 30 people) to follow daily for 3-6 weeks and report back on to the surveillance committee. Officers are provided with transportation and mobile communication support to facilitate their contact tracing work.
During interoutbreak periods, the ongoing surveillance system remains in place, she said, and the task force meets on a monthly basis to review disease surveillance data and continually updates epidemic preparedness and response plans with respect to the situation on the ground. There is constant communication between staff at each level of the health system regarding the current situation, and with the support of the World Health Organization (WHO), Uganda has also been working with its neighboring countries to strengthen cross-border communication and improve outbreak response. Aceng noted that the system relies strongly on radio announcements coupled with a mobile phone alert and call center system to keep people informed and to alert surveillance officers to early signs of potential problems. Community guidelines in various languages inform people about when and where they should call the toll-free alert service. Fitter noted that such alert call centers often receive calls unrelated to surveillance alerts or become overwhelmed. Aceng responded that they address this through an alert system management structure by having one officer receive and filter all calls, passing those deemed necessary of immediate response to a second officer. The center may receive up to 4,000 calls per day, and responds immediately to about 20 of those. She noted that this alert system runs continuously even between outbreaks and generates valuable tracking information even in the interepidemic periods.
Predictive Modeling
Predictive modeling involves building scenarios for analyzing and strengthening response systems across best- to worst-case scenarios, explained Campbell. The objective is to build sufficient capacity to respond effectively to all such scenarios. Reporting on the discussion of this topic among participants in the focus group, Campbell suggested that the first steps are better understanding of the challenge of disease outbreak response, learning from how other sectors respond to disasters, and predicting what to anticipate at various time points as the response matures. These analytical steps inform the plans for deployment strategies, competency and
capacity building, necessary skills, and operational logistics that are needed to underpin an effective response.
Building effective predictive models would benefit from in-kind contributions from leading technology specialists, suggested Campbell. Another key component is global consensus building based on lessons learned from other outbreaks; depending on scale of consensus achieved, recommendations could be presented to countries and regions to make sure that they are appropriately planning for an all-hazards approach with partners and appropriate national ownership.
Real-Time Data Analysis and Evidence
To improve modeling and monitor performance, real-time data analysis is fundamental; Campbell noted that continual improvement of modeling practices (and their underlying assumptions) depends on continuing data monitoring and reporting. Remarking that there is already a requirement for daily operational reporting in disaster management, he suggested that daily information sharing and reporting could be brought into disease management by institutionalizing real-time operational science and monitoring and evaluation practices. In addition to partnering with government, WHO, the United Nations (UN), and relevant specialists to do so, the private sector could be engaged for components such as IT mapping. He cautioned that implementing this strategy would require new considerations about data transparency and must emphasize data sharing from the outset (i.e., discouraging the tendencies protect data or be the first to publish it). Fowler noted that getting data early is important for generating case report forms that can be both standardized and generalizable. However, it is also worthwhile to consider the unintended consequences of continual requests for data monitoring and reporting of case counts and laboratory information. Once an outbreak has been established, the value of constant reporting could be weighed against using those same resources for other elements of a response. For assessment to inform the dynamic improvement of care, Rubinson called for it to be geared toward providing accurate assessments of functional status rather than only counting patients and deaths, for example. Additionally, making sure that countries susceptible to the outbreak are reporting indicators in a standardized manner, such as suspected cases or confirmed cases, can help to show the true picture of an outbreak’s magnitude.
Key Gaps in Existing Surveillance Systems
Several participants highlighted gaps and challenges in existing systems, with the view to discussing strategies for capacity building and system strengthening. Some of the gaps Fitter highlighted included
- Building capacity in order to understand where the problem is and put the right resources in the right places
- Integrating surveillance training into broader health care education to enable the workforce to monitor systems, manage technology, translate information, and all other key components of surveillance
- Linking training, education, and research to promote the acquisition of information and outbreak tracking
Fitter also raised the issue of funding for training the workforce to carry out surveillance, and the challenge of convincing funders outside of the public health community about the importance of long-term surveillance training and capacity-building programs. Wilson suggested presenting health impact as contingent on reciprocal information sharing for a sustainable system and packaging them together; she noted that while an IT system is largely routinized, strategies and human connections are more challenging. Ellora Guhathakurta, Planning, Monitoring, and Evaluation Officer with the UN Development Programme, agreed regarding the strategy of linking a system’s long-term capacity to the sustainability of its surveillance system.
Remarking that acquisition of resources and funding is a challenge in all countries, Aceng called for sensitizing all decision makers to the dangers of epidemics and urged governments to invest in the control of epidemics by having funding available and protected for immediate use in times of emergency. Omaswa of the African Centre for Global Health and Social Transformation (ACHEST) also commented that the appropriate channeling of funds into surveillance, and the alleviation of dependency upon donors, is critical to institutional capacity building in low- and middle-income countries (LMICs), and institutional capacity will require a universal preparedness approach focusing on all causes of mortality and morbidity. He explained that essential care provision can compete for funding in budgetary allocations and called for improved leadership within decision-making structures to ensure that surveillance is part of a basic health care package.
DISEASE SURVEILLANCE SYSTEMS: HIGHLIGHTED OPPORTUNITIES
Multiple participants highlighted several key areas for improvement in disease surveillance systems and sketched possible strategies for addressing them.
Using Existing Technologies and/or Knowledge in Innovative Ways
Wilson expressed concern about focusing too heavily on new technology innovation, calling for a shift away from thinking about existing
technologies as innovations just because they are being utilized differently. Citing examples raised by other participants, such as the use of SMS for alert systems and the use of satellites in Nigerian polio surveillance, she commented that neither SMS nor satellite imagery are innovative new technologies,4 but they are being applied differently to strengthen systems and communication coordination. She remarked that while such ideas can be good and useful, emphasis should be placed on mechanisms that can use standardized, common technologies and to generate opportunities for innovative thinking in reapplying them to build an interoperable infrastructure. To illustrate, she suggested using standardized, existing technology to channel alerts into a national-level infrastructure, or to capture unique registration and identification data such as biometrics or fingerprints.
Participants discussed the challenges associated with the ability to disseminate the correct information, using the right resources, to the targeted people in such a way that results in actionable impact and a response that is both reactive and preemptive. To do so would require identifying which standardized technologies and reporting systems should be used in order to create a well-utilized system, with which stakeholders at all levels are aware and familiar. Myers suggested that using the same system for day-to-day communications as well as alert systems would be a way to help ensure user familiarity and comfort. Other participants proposed that the salient use of social media could provide a useful platform for disseminating correct and timely information. Multiple participants suggested that a promising way forward could be to integrate the existing technology infrastructure by ensuring it is linked together, institutionalized, and interoperable on a community, district, and national level. The aim in doing so is to build more cost-effective, sustainable systems that countries can take ownership of to improve their surveillance capacities.
Promoting Country Ownership of Institutionalized Surveillance Systems
A related topic discussed was the idea of building on existing capacities to allow countries to take ownership of institutionalized surveillance systems by instilling accountability and the abilities to self-audit, self-regulate, and report. Multiple participants noted that a challenge faced by efforts to establish more country-level autonomy is the lack of adequate supervision and management for reciprocal information acquisition, training, and reporting on the country and international levels. To address this, Agyepong of the University of Ghana suggested fostering better interagency collaboration (for example, among agricultural, vet-
__________________
4 Ardalan cautioned that innovation is a relative concept that depends on the particular circumstances of each country, that is, what may be new in some areas may not be in others.
erinary, and health services) to address the lack of cohesion among agencies. In the context of governments leveraging their positions with private industries to better link into existing infrastructures, Kimball contributed the idea of turning over actions such as census collections and surveys to in-country private industries. Tomori called for equipping people at all levels to gather and analyze information on an ongoing basis, rather than retroactively. Many participants noted that this could provide a feedback mechanism, cultivate open and reciprocal communication, and foster trust; an associated benefit might be that if people at all levels are contributing data, the function and impact of surveillance programs can be measured on a broader scale.
Similar to donor issues mentioned in Chapter 2, funding issues represent further challenges to promoting country ownership of surveillance processes. Kimball suggested expanding the funding timeline—for example, from 2 years to 5 years—because sustained and longer-term funding would help countries to more clearly grasp how to deliver services effectively, and to better understand their assets and how best to manage them. Guhathakurta, Fitter, and other participants highlighted the issue of dependency on donor funding that is employed to effect short-term changes that are neither sustainable nor appropriately institutionalized. Warning that donor money can fall into a trap of unintentionally forcing dependency, they suggested a broad strategy of turning over skills and resources to in-country investors and participants. As an example, Rwanda took an innovative approach in requiring all donors to channel funds in support of their Vision 2020 strategy and to rebuild government systems, institutions, and processes by investing in them. It maintained the right to decline aid that was not aligned with the national strategy or had high transaction costs or conditionalities (Farmer, 2015). As Fitter reported, routing donor money into mechanisms that result in institutionalized, sustainable, country-owned surveillance systems could promote countries’ abilities to self-regulate and maintain accountability to all stakeholders.
Engaging and Educating All Sectors in Disease Surveillance
Participants including Awunyo-Akaba, Myers, Greenough, and Tomori emphasized the key role of community health workers, NGOs, and civil society, traditional rulers, and religious leaders in disease surveillance, and suggested ways to more effectively engage them in that system. Building on ideas presented in the discussion on promoting country ownership of surveillance, several participants remarked that community trust could be fostered by interdisciplinary information sharing; for example, veterinary students and medical students could collaborate and contribute to understanding manifestations of certain zoonotic diseases.
Greenough noted that surveillance systems often break down because the people at the local level, who are conducting the groundwork of data gathering and due diligence, do not receive back the relevant, aggregate information from decision makers and analysts. Fitter responded by highlighting the importance of increased, bidirectional reporting and information sharing, with respect to both health care actors and the population at large; he shared that information is collected more effectively when everyone involved understands why it needs to be collected. With respect to communities in particular, several participants suggested that better transparency surrounding the benefits of strong surveillance systems (and the consequences of poor ones) would help to strengthen a community’s trust of health care workers, NGOs, and government entities such as Ministries of Health. Several participants pointed to the related topic of better and earlier training and education about public health concepts for communities, health care workers (including veterinary students and pharmacists), NGOs, and civil societies in order to further facilitate improved and sustainable surveillance systems. These participants suggested that integrating public health and health care in training would allow for the implementation of institutionalized best practices. Fitter also noted that based upon basic analyses of IDSR, health care sites often suffer from lack of supervision and would benefit from more constant feedback to enhance trust.
Another suggestion was to facilitate better understanding and awareness of important considerations that could help make communities, health care workers, and other community-level actors more astute to the kinds of disease they should expect, and to be more sensitive to detecting them in specific circumstances. Aceng noted that in Uganda, for example, their alert system focuses on different diseases during different seasons. During the season when bats are returning to caves, they provide public alerts about avoiding them to prevent zoonotic transmission. During the dry season, the alert system focuses on spreading awareness about meningitis. Burkina Faso sends similar seasonal meningitis alerts to physicians, Fitter added.
Strengthening Routine Day-to-Day Surveillance Systems Between Outbreaks
The crosscutting principle of capitalizing on interoutbreak periods to strengthen surveillance systems in various contexts was also highlighted. One area of discussion focused in particular on the importance of strengthening routine day-to-day surveillance systems, echoing some of the advantages that were ascribed to strengthening routine information systems. Fitter characterized routine reporting and laboratory surveillance systems as foundational building blocks of an everyday system that is capable of detecting and responding effectively to outbreaks. Figure 4-1 illustrates
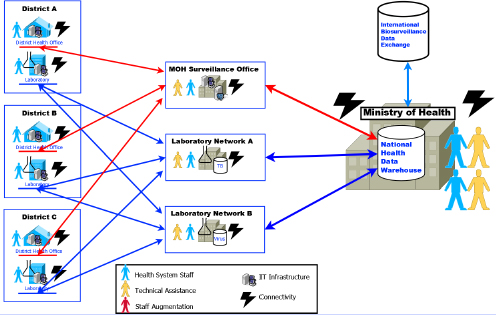
NOTE: IT = information technology; MoH = Ministry of Health.
SOURCE: Fitter presentation, August 5, 2015.
how those components combine to facilitate data integration and use in an expanding health data network.
With a routine surveillance system embedded within a national health information system architecture, Fitter further described how the system can expand to increase capacity when the number of suspect cases increases, allowing for the incident management system to be activated earlier in an outbreak. According to the Global Health Security Agenda (CDC, 2015a), a national surveillance strategy should be both IDSR-based and International Health Regulations–compliant, combining routine indicator- and event-based surveillance across human and animal health systems for early outbreak detection and rapid response.5 Implemented in a step-wise fashion and facilitated by routine progress monitoring, the strategy encompasses disease-specific protocols and an information communication technology infrastructure that encompasses a workforce trained in surveillance, an integrated surveillance and laboratory national health data warehouse, and data exchange that is interoperable across local, national, and international platforms.
__________________
5 See http://www.cdc.gov/globalhealth/security/actionpackages/real-time_surveillance.htm (accessed November 9, 2015).
This page intentionally left blank.


















