9
Global Health Leadership
“Medical diplomacy must be made a significantly larger part of our foreign and defense policy. . . . America has the best chance to win the war on terror and defeat the terrorists by enhancing our medical and humanitarian assistance to vulnerable countries.”
—Former Secretary of Health and Human Services Tommy Thompson (2005 Boston Globe editorial)
Throughout this report the committee has reiterated the need to understand the changing landscape of health, which is strongly influenced by globalization, climate change, increased travel and trade, and increased life expectancies around the globe. Despite these global changes, history has proven that advancing foreign policy and national security can be achieved through and by health. Global health itself has long been used as a tool to advance foreign policy interests, including security and influence (Feldbaum and Michaud, 2010). The scope of global health in diplomacy was greatly expanded with the creation of the World Health Organization (WHO) in 1948, and since then, by the advent of the International Sanitary Regulations in 1951 (with subsequent updates to become the International Health Regulations [IHR] in 1969 and 2005). The involvement of the United States in the creation of the Global Fund to Fight AIDS, Tuberculosis and Malaria (Global Fund) in 2002, the rollout of The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) in 2003, and the development of the Global Health Security Agenda (GHSA) in 2014, shows the continuing need for a U.S. role in global health diplomacy has not abated.
To maintain the status of the United States as a global health leader and ensure safety for its people, the committee argues it will be essential to stay engaged and involved in international agencies, collaborations, and partnerships. A strong connection to the many multilateral organizations involved in global health and development is critical to maintain situational awareness and a keen recognition of when a small-scale problem could erupt into a global emergency. Consider the example of the involvement of U.S. diplomats in the international response in Nigeria in 2003. At the time
northern Nigerian states banned polio immunization campaigns, which lead to a global outbreak and ended hopes of eradicating the disease in that decade (Kaufmann and Feldbaum, 2009). Though it was difficult for U.S. health officials to understand the diplomatic tools they had, together with the Global Polio Eradication Initiative and the United Nations (UN), U.S. diplomats were able to raise the issue on multiple state visits to the Middle East. Furthermore, by working through the U.S. Embassy in Nigeria, the U.S. was able to influence other countries to put pressure on Nigeria to restart the vaccination campaign (Kaufmann and Feldbaum, 2009). This is just one example demonstrating the benefits of taking a strategic approach to U.S. efforts in global health diplomacy.
This chapter opens with a review of the definitions and needs for global health governance, including the recent calls for reform of WHO following the 2014–2015 Ebola outbreak in West Africa, and newly established multilateral organizations. Next, it offers suggestions for the U.S. approach to global health diplomacy, including coordinated roles for the U.S. Department of State and the U.S. Department of Health and Human Services, and then describes how health could be integrated into the foreign service system. Finally, this chapter discusses the creation of a workforce pipeline to support this proposed approach, and closes with conclusions and recommendations.
GLOBAL HEALTH ARCHITECTURE AND GOVERNANCE
The international architecture for global health governance is complex, cross-cutting, and often driven by political motives. Many definitions of global governance put interdependence in the center (Kickbusch and Szabo, 2014), perhaps illustrating the reasons that global health governance has become so challenging and important in the last few decades. Kickbusch and Szabo (2014) explain the complex interplay of global health governance along three political spaces (see Figure 9-1). Though global health governance refers to institutions with an explicit health mandate, such as WHO, it is now well understood that global governance for health extends to organizations that may have direct or indirect effects on health, such as the UN and its agencies, including the UN International Children’s Emergency Fund (UNICEF), UN Population Fund, and UN Development Programme; the World Trade Organization; or the World Bank (Kickbusch and Szabo, 2014). Finally, governance for global health refers to mechanisms and institutions that contribute to global health governance and governance for global health, including regional strategies for global health (Kickbusch and Szabo, 2014).
Kickbusch and Szabo argue that just as public health challenges can no longer be effectively addressed only within the health sector and at the
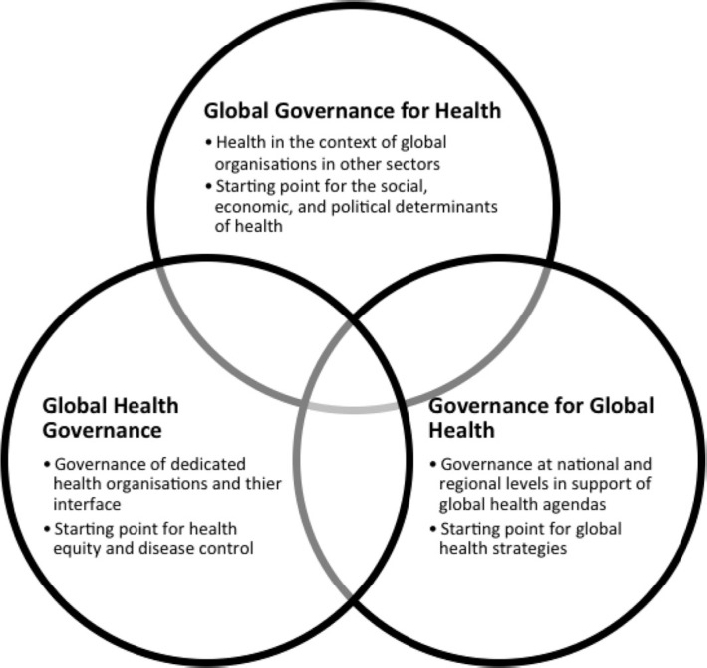
SOURCE: Kickbusch and Szabo, 2014.
national level, WHO can no longer be the sole manager of these types of intergovernmental health challenges. Despite many criticisms, there is still a need for WHO, its strong convening power to coordinate the many new global health players, and its ability to set norms and standards in global health care (The PLOS Medicine Editors, 2007). Yet, the response to the 2014 Ebola outbreak demonstrated that the current state of global health governance is not adequate to manage and respond to the health needs of all countries, and that there is an urgent need for reform.
Calls for WHO Reform
The 2014 Ebola outbreak exposed major vulnerabilities in the WHO emergency response capabilities and leadership structure, such as poor IHR
compliance, lack of technical capacity, unstable financing and lack of accountability (Moon et al., 2017). To address those vulnerabilities, several commissions were convened in the year after the height of the outbreak to discuss areas of WHO governance and outbreak response improvement.1 Each of the commissions emphasized the need for reforms in WHO outbreak response and global governance (Gostin et al., 2016).
The Ebola response was hindered by poor coordination at global, national, and subnational levels; therefore, the commissions recommended that outbreak preparedness at all levels be refocused as the core of WHO’s work. Overall, the commissions recommended the creation of a Centre for Emergency Preparedness and Response to integrate and strengthen WHO’s preparedness, response, and humanitarian activities (Gostin et al., 2016). With the understanding that WHO has cut nearly two-thirds of its emergency response unit, this new governing body would fill a much-needed gap that will declare public health emergencies of international concern (PHEICs) and coordinate responses more quickly. The commissions also recommended WHO lead the assessments of countries’ implementation of the core capacities outlined in the IHR (Gostin et al., 2016). While nations must be held responsible for developing their own infrastructure to respond to emerging health threats, the commissions argued that WHO must coordinate global preparedness and hold nations accountable for its maintenance.
The legitimacy and ability of WHO to respond in an outbreak are contingent on strong governance at all levels. Described as suffering from a “crisis of confidence,” WHO was asked to make a number of reforms by the commissions to ensure it remains a global leader in health (Gostin et al., 2016). Specifically, the commissions recommended that to prepare for outbreaks, WHO should partner with countries to ensure they have the technical support required to implement the core capacities necessary to comply with IHR, with the ultimate goal of having every government develop and publish concrete plans to achieve these core capacities by 2020 (Gostin et al., 2016). Additionally, the commissions recommended that WHO take the role of watchdog in ensuring that restrictions on travel and trade set by nations during outbreaks are justified, so that countries experiencing outbreaks are not unjustly punished (Moon et al., 2017). Possible solutions, including “naming and shaming” countries that impose unjusti-
___________________
1 Commissions for WHO reform included (1) the World Health Organization (WHO) Ebola Interim Assessment Panel (WHO Interim Assessment); (2) the Harvard University and the London School of Hygiene & Tropical Medicine’s Independent Panel on the Global Response to Ebola (Harvard/LSHTM); (3) the Commission on a Global Health Risk Framework for the Future (CGHRF) convened by the U.S. National Academy of Medicine; and (4) the United Nations High-Level Panel on the Global Response to Health Crises (UN Panel) (Gostin et al., 2016).
fied restrictions or encouraging the creation of enforcement mechanisms for the enactment of travel and trade restrictions (Moon et al., 2017), would allow WHO to take on an aggressive role of being the authoritative voice in times of PHEICs. Finally, the commissions recommended that WHO reform its internal structure through better management of human resources, increased transparency and accountability through a freedom of information policy, creation of an inspector general role, and marshaling of more effective leadership (Moon et al., 2017).
Up to the release of this report, the work to implement the recommended changes has begun, but is far from finished, and the success of these reforms is contingent on sustainable funding. Multiple assessments and commissions have called for improved funding for WHO (Gostin et al., 2016; Ebola Interim Assessment Panel, 2015); to ensure that countries have the capacity to implement and maintain the IHR, WHO has leveraged additional funding to help countries that need assistance. The Group of Seven (G7) has committed to assisting 76 countries at the 2015 and 2016 summits (Moon et al., 2017). The United States has committed $1 billion for building capacities in 31 countries, largely through the GHSA. South Korea has pledged an additional $100 million to support the GHSA in 13 countries. Additionally, in an effort to find better methods to mobilize both domestic resources and development assistance, the World Bank has “sought funding to assist at least 25 countries with pandemic preparedness plans in its latest financing round and established an international working group on financing preparedness in November 2016” (Moon et al., 2017, p. j281). Despite the financial support for improvements, no formal programs or new guidelines have been announced for travel and trade restrictions for those that do not follow the IHR, and “WHO has not initiated any major institutional reforms since the Ebola outbreak” (Moon et al., 2017, p. j283). While the improvements in financing and engagement from member countries is encouraging, ensuring reforms that improve transparency will be of vital importance for the organization to continue to be the lead authority in global health.
Finding: WHO performs essential functions for the global community, including the setting of international standards, such as the International Health Regulations, and the provision of technical advice and guidance to national health authorities.
Finding: Multiple calls have been made for management and operational reforms of WHO to improve future responses to public health emergencies of international concern.
Strong and Promising International Organizations
While many countries look to WHO as an authoritative leader in global health, several other multilateral organizations and partnerships that have been created in the last 15 years now play extremely important roles in global health governance. Organizations such as the Global Fund and Gavi, the Vaccine Alliance, have constituency-based models of governance and narrowly defined missions that enable more flexibility and support to accomplish their goals.
As multiple infectious disease outbreaks have immediately threatened global health security in the past several years, newer partnerships have been formed just since 2014, including the Coalition for Epidemic Preparedness Innovation (CEPI) and the GHSA. CEPI, supported by the governments of Germany, Japan, and Norway, the Bill & Melinda Gates Foundation, and the Wellcome Trust, is initially investing $540 million to finance and coordinate the development of new vaccines to protect against infectious diseases (CEPI, 2017). While new, CEPI has shown strong commitment from supporters through engagement and funding, and holds promise for accelerating capacity building and critical medical product development. Because GHSA was launched as a partnership by the United States, and has received positive feedback thus far on its progress, the committee has included more detailed examples of its successes.
Global Health Security Agenda
As introduced in Chapter 3, the U.S. government undertakes a significant number of activities within GHSA, but the agenda is a global one. Currently, GHSA has a membership of 55 countries, as well as WHO, the World Organisation for Animal Health, and the Food and Agriculture Organization of the UN (GHSA, 2016), and has endorsements from the G7 and Group of 20 (HHS, 2017). Furthermore, the GHSA’s unique operating style allows the United States to maintain a leadership role in global health security while encouraging shared responsibility with partner countries through its 10-country steering group (GHSA, 2016). This work is also supported by a roundtable of several private-sector partners that strives to mobilize industry to help countries prepare for emergencies and strengthen health systems. The Private Sector Roundtable also aims to be a clearinghouse for industry to respond to health emergencies in collaboration with governments and multilateral stakeholders (GHSA, n.d.). The roundtable has even set up working groups aligning with member capabilities across the action packages, including Supply Chain and Logistics; Policy Development and Advocacy; Workforce Development; Partnerships, Technology and Analytics; and Antimicrobial Resistance.
Because of its convening of multisectoral actors and coordination at both the White House and in-country levels, GHSA has shifted the U.S. government health security approach from a fragmented strategy—a characterization of many global health programs—to a more coherent and cohesive one. In bringing multiple organizations and sectors to the table, including the United States, GHSA provides a different, more innovative approach to answering the world’s global health security issues through comprehensive assessments and technical assistance. Additionally, in part because of increased accountability and partnership, the abilities of countries to prevent, detect, and respond to outbreaks have improved. For example, the United States has strengthened the public health laboratory and surveillance systems in Uganda, in addition to supporting the creation of a public health emergency operating centers (EOCs). The first test of this occurred in March 2016 when an outbreak of yellow fever was contained by the Uganda Ministry of Health through the quick activation of the EOC and improved lab capacity (GHSA, 2017). In 2015 alone, GHSA was able to produce measurable improvements in national capacities to prevent, detect, and respond to infectious disease threats: 9 countries established or strengthened mechanisms to limit animal-to-human spillover; 17 countries participated in Field Epidemiology Training Programs (FETPs); and 12 countries activated EOCs (GHSA, 2017).
The United States can capitalize on this momentum for global health security. By continuing to provide technical and financial assistance and collaborate with partners to help countries assess and improve their national health security capacities, together the world can more effectively contain outbreaks, as well as promote evidence-based plans for limiting the global spread of disease (Nuzzo and Shearer, 2017).
Finding: Many international agencies, organizations, and partnerships are now critical parts of the global health architecture and also carry out essential global functions.
U.S. APPROACH TOWARD GLOBAL HEALTH DIPLOMACY
American foreign policy has long been the “three-legged stool” of defense, development, and diplomacy. Though the defense leg has been the main driver, it will continually be important for the United States to be able to tell its story in ways that do not include military force. The military needs civilian partners in the battle against extremism. This idea of soft power—the ability to attract others without force or coercion through development efforts, including in health—is supported by a rationale that it reinforces American values, improves how the United States is viewed by the rest of the world by promoting peace and prosperity, and contributes
to U.S. security at home by building stability abroad (Armitage and Nye, 2007). Consider the example of the falling of the Berlin Wall, where U.S. diplomacy shared a central role in bringing an end to the cold war, and encouraging American values of free speech and democratic governance to citizens in other countries (Kuo, 2016). This can also be applied to fighting terrorism. A RAND study in 2008 examined more than 600 terrorist groups since 1968 and found that the majority of them have ended because they either joined the political process or because key members were arrested or killed by local police and intelligence (Jones and Libicki, 2008). The RAND authors found that rarely has military force been the reason for the ending of terrorist groups. Many opportunities like this still exist to protect American interests through development and soft-power diplomacy initiatives, and if the United States fails to act through the other two legs of the foreign policy stool, other countries are likely to fill this role instead.
In the last few decades, China has quietly increased many of its health and development programs around the world, asserting itself as a powerful and committed leader both through bilateral programs and taking a leadership role in multilateral organizations. China’s flexibility and lack of conditionality in its aid programs has generated large amounts of good will and political capital in the world (Armitage and Nye, 2007). Furthermore, China has sent more than 15,000 doctors to Africa and has treated nearly 180 million African patients, which has helped to ensure its long-term foreign policy interests in energy and food security (McGiffert, 2009). Additionally, Cuba has sent medical staff and medical diplomats to about 70 countries and provided free medical training in return for various benefits, including oil from Venezuela (Fieinsilver, 2009). How countries spend their money overseas directly reflects their priorities. People on the receiving end understand this notion, and in turn often base their opinions on these aid and development decisions, setting the stage for how various wealthy countries are viewed globally (Armitage and Nye, 2007).
As evidenced through previous chapter discussions about globalization, the growing economies of many low- and middle-income countries, and the proliferation of private-sector players in the global health sphere, there is a clear need to change the way the United States engages in foreign policy and development assistance. Specifically, as countries mobilize domestic resources, develop health systems, structure fiscal policies, and build surveillance systems, the U.S. government could transition away from the provision of bilateral aid toward the sharing of technical assistance. Doing so will allow the United States to maintain close relationships with partner countries and an awareness of health issues they face, while allowing funds typically allocated to foreign aid to be spent on other global goods. However, there are a limited number of countries in this position, and those low-income countries will still depend on donor governments like the United States for foreign
aid until they can advance their economies. These countries, sometimes also afflicted by conflict or poor governance, can also be a source of insecurity and instability for global health, so a continued commitment of direct aid will still be critical. Currently, a number of U.S. agencies, including the U.S. Department of State and U.S. Department of Health and Human Services, coordinate global health interests abroad. But there is a need to better coordinate the activities of these agencies, with long-term strategic vision and cross-cutting approaches in order to maximize efforts and efficiency.
Finding: The role of the United States in global diplomacy has proven useful in events ranging from the fall of the Berlin Wall to the resuming of Nigeria’s polio vaccination campaign.
Finding: Other countries, such as China and Cuba, have increased their participation in global health and development around the world, positively affecting how they are viewed globally.
The Role of the U.S. Department of State
The U.S. Department of State is the primary agency responsible for foreign affairs, and global health is interwoven into its structure and activities in both its regional bureaus and functional bureaus. Table 9-1 provides an overview of the functional bureaus and their offices, which explicitly conduct activities that relate to global health. The Office of International Health and Biodefense is the primary office responsible for global health issues (U.S. Department of State, 2017b),2 but the other offices listed offer pockets of knowledge and work in a variety of domains that include biological weapons control and nonproliferation, biosecurity, GHSA, finance, and migration (ISAB, 2016). Given the range of offices within the U.S. Department of State that work on global health, it is apparent that the department considers global health a vital, cross-cutting issue. However, the strengths within these bureaus on global health are not mirrored by similar strengths at U.S. embassies, which often lack personnel with global health expertise.
A Sustainable Career Track
Almost every U.S. embassy has foreign service officers (FSOs) that are assigned to work on global health issues, with some selected to become
___________________
2 The Office of International Health and Biodefense leads the U.S. Department of State’s efforts for pandemic response, and ensures that global health issues, such as emerging infectious diseases, global health security and antimicrobial resistance, are incorporated into U.S. foreign policy.
| Undersecretary for Economic Growth, Energy, and the Environment | Undersecretary for Arms Control and International Security | Undersecretary of Civilian Security, Democracy, and Human Rights | Undersecretary for Political Affairs | ||||
|---|---|---|---|---|---|---|---|
| Bureau of Economic and Business Affairs | Bureau of Oceans and International Environmental and Scientific Affairs | Bureau of Arms Control, Verification and Compliance | Bureau of International Security and Nonproliferation | Bureau of Democracy, Human Rights, and Labor | Bureau of Population, Refugees, and Migration | Regional Bureaus | Bureau of International Organizations |
| Office of International Finance and Development | Office of International Health and Biodefense | Office of Chemical and Biological Weapons | Office of the Biological Policy Staff | ||||
| Office of Cooperative Threat Reduction | |||||||
| Office of Missile, Biological, and Chemical Nonproliferation | |||||||
| Office of Threat Reduction | |||||||
environment, science, technology, and health (ESTH) officers. Although health is a component of ESTH officers’ portfolios (ISAB, 2016), it is not the strongest part of their training (NASEM, 2015). Not only do ESTH officers receive inadequate health training (a mere 1.5 hours in global health at the Foreign Service Institute) (ISAB, 2016), there is a sentiment that ESTH postings are outside the mainstream FSO career track. Due to the up-or-out promotion system within the U.S. Department of State (OIG, 2002), FSOs reportedly lack interest to pursue such postings (NASEM, 2015). In embassies that lack ESTH officers, the health portfolio is managed by economic officers.3 The neglect of global health in the Foreign Service career track system (which includes consular, economic, management, political, and public diplomacy) (U.S. Department of State, 2017a) means that the U.S. Department of State’s workforce lacks the requisite skills for sustainable approaches to global health, which can result in the development of ad hoc solutions and policy.
Although the lack of this specific workforce capacity is not always evident, it comes into sharp focus in the midst of a large-scale global health event. Consider the example of the U.S. response to the 2014–2015 Ebola outbreak in West Africa, where the U.S. Department of State formed an Ebola coordination unit using “ambassadorial leadership and staff borrowed from across the department” (ISAB, 2016, p. 20). The unit was comprised almost entirely of FSOs, but only two had a background in science. This issue was also notable in an analysis of the previously mentioned polio vaccination response in Nigeria in 2003, where public health professionals were found to lack the skills needed to approach ministries of foreign affairs. Similarly, diplomats required greater training on the role of health in foreign policy (Kaufmann and Feldbaum, 2009). If more staff members had public health or global health backgrounds, stronger alliances could have been built during the relief effort (Chen, 2015). These ad hoc, stand-alone groups, like the now-defunct Avian Influenza Action Group, do not allow for learning or the development of institutional knowledge for future events because they often disband immediately after the crisis ends (ISAB, 2016).
Strategizing for Downstream Effects
While many global health programs are measured in terms of direct health outcomes and perhaps cost-effectiveness, appropriately designed programs can also have multiple downstream effects on other sectors of society. These downstream effects can affect poverty, education, or employment, and in turn provide diplomatic advantages for the donor government (Feldbaum
___________________
3 Personal communication Matthew Brown, NIH, November 9, 2016.
and Michaud, 2010; Kevany, 2015). PEPFAR is one of the most robust and well-known U.S. global health programs, has had measured success in several nonhealth areas, as discussed in Chapter 4, and is overseen by the Office of Global AIDS Coordinator at the U.S. Department of State. This position also leads the Office of Global Health Diplomacy (OGHD) at the U.S. Department of State, though since its creation in 2013, the OGHD has not been as targeted and effective with its efforts as many had hoped. Moving forward, OGHD could offer an opportunity for the United States to be more strategic about its soft power development and diplomacy initiatives, and to align them with the ongoing critical investments in health across the U.S. government that have been made in the last decade. If adequately funded, a central office such as OGHD could guide U.S. global health policy through a more coherent approach, and elevate the issues of health and development worldwide while giving them greater credence within the U.S. government. Importantly, part of the success of the PEPFAR program and the whole-of-government approach is the important work that is implemented by other government agencies such as the U.S. Agency for International Development (USAID) and the U.S. Centers for Disease Control and Prevention (CDC). With their technical competence and established in-country networks, these two organizations significantly contribute to the health diplomacy of the United States. If the health programs were designed and measured for indicators beyond just health outcomes, their use and knowledge generation could be attractive to foreign policy experts and decision makers (Kevany, 2015). Accordingly, having FSOs with global health expertise would be important to complement the work of implementing agencies, and support the U.S. Department of State’s day-to-day functioning and its responses to health emergencies as they occur. Building on lessons learned from the failed Global Health Initiative (described in Chapter 1), in order for this to be successful OGHD would require funding, accountability, and authority.
The Role of the U.S. Department of Health and Human Services
The U.S. Department of Health and Human Services (HHS) and its agencies, such as CDC, the U.S. Food and Drug Administration, and the National Institutes of Health (NIH), also play a vital role in global health, including global health diplomacy. These agencies are responsible for U.S. health program implementation, technical advisory actions, and health workforce training programs. HHS also engages at a high level of diplomacy with partner countries by using a specialized cadre of workers known as health attachés, the definition and roles of which are presented in Box 9-1 (Brown et al., 2014).
Health attachés, though officially working at U.S. embassies abroad, are typically on-loan from HHS agencies. Often populated by employees
with field experience serving from CDC or NIH, placement and support of health attachés is coordinated by the HHS Office of Global Affairs (OGA) (HHS, 2016b), which acts as the central leadership for all of HHS’s global activities (Bliss, 2014). As a result, health attachés report to OGA at the headquarters level,4 but they also report directly to the U.S. ambassador of the embassy to which they are assigned (U.S. Department of State and USAID, 2010). The United States currently has six health attachés posted in Brazil, China, India, Mexico, South Africa, and Switzerland. While the first five support U.S. embassies in direct country to country relationships, the health attaché posted in Geneva, Switzerland, offers support to the U.S. mission to the UN (HHS, 2016b).
Health attachés have played a critical role at U.S. missions. A notable example was the bilateral negotiation that took place between the United States and China during the 2003 Severe Acute Respiratory Syndrome outbreak. The health attaché posted in Beijing brokered a memorandum of understanding between the Chinese Ministry of Health and HHS to form the U.S.–China Collaboration of Emerging and Reemerging Infections (U.S. Department of State, 2010).5 Although the agreement itself was positive for health-related outcomes at the time, the ongoing relationship that was developed served as a platform for collaboration in the subsequent H5N1 and Ebola epidemics. During the H5N1 pandemic in 2005, this agreement enabled smoother sharing of information, and during the Ebola outbreak in 2014, the agreement clarified roles each country would play in the response (in which China built a treatment center in Liberia and a 60-bed hospital
___________________
4 Personal communication with Matthew Brown, NIH, January 5, 2017.
5 Personal communication Matthew Brown, NIH, November 9, 2016.
in Sierra Leone).6 This partnership has since been renewed for 5 years in 2015 (Huang, 2016).
Creating an International Workforce
Despite the clear value of the expertise brought by health attachés, there is limited placement of health attachés at U.S. missions. This is partly because of inadequate funding, as the annual cost of placement can be close to $500,000 per year.7 Yet more importantly, the limited placement of health attachés is due to a lack of appropriately experienced personnel to draw from—resulting from limitations in how HHS can hire for overseas positions. For new employees or outside hires, HHS uses term appointments to hire and deploy personnel abroad. While this in itself is not a problem, the lack of a global health career track in HHS and the temporary, ad hoc nature of the available positions makes these positions one-off and not attractive to a talented pool of candidates. At the conclusion of their term, employees often leave the U.S. government to seek a career in global health elsewhere, taking with them critical cross-cultural, management, leadership, and scientific skills that can take years or decades to acquire. However, HHS’s workforce abroad has expanded between 2000 and 2015 from less than 50 to more than 500 in more than 70 countries. Despite this expansion though, HHS has an average standing vacancy rate of more than 30 percent for its overseas positions.8 As a result, many positions go unfilled or have large gaps between incumbents, which create deficits in HHS’s ability to ensure the safety and security of the U.S. population.9 Furthermore, due to the lack of a predictable and unified process of rotating HHS employees in and out of overseas positions, the department is unable to maintain institutional knowledge of overseas operations and is not flexible enough to meet its expanding global mandate.10
HHS has acknowledged this weakness, and in an American Journal of Tropical Medicine and Hygiene editorial, Nils Daulaire (former Assistant Secretary for OGA) stated that OGA is working to “establish a global health career track within HHS to formalize career opportunities and training for our staff working in global health, both domestically and internationally” (Daulaire, 2012). In August 2015, a pilot project was conducted with support from HHS Idea Lab to develop the Global Bidding and Assignment System (GBAS), a specialized system for department-wide recruitment,
___________________
6 Personal communication Matthew Brown, NIH, November 9, 2016.
7 Personal communication with David Hohmann, formerly Office of Global Affairs (HHS), November 8, 2016.
8 Personal communication with Matthew Brown, NIH, November 9, 2016.
9 Personal communication with Matthew Brown, NIH, March 28, 2017.
10 Personal communication with Matthew Brown, NIH, March 28, 2017.
assessment, bidding, and deployment for overseas positions (HHS, 2016a). More than 200 HHS employees applied to GBAS and 90 were selected to be matched to U.S. missions. As of November 2016, 23 percent of the selected HHS employees seeking overseas placements have been matched and are in the process of being deployed.11 However, as of the release of this report, GBAS has not been renewed or taken to scale.
Finding: The limited number of noncareer health appointments currently available abroad is an ad hoc system. It does not facilitate institutional knowledge across events or a promising career track for global health professionals.
A PLACE FOR HEALTH IN FOREIGN SERVICE
Between the U.S. Department of State and HHS, the U.S. government has an inadequate workforce to meet its global health needs. Owing to the neglect of global health in the Foreign Service career track system and limited knowledge of health by ESTH officers, the U.S. Department of State is unable to address global health in a concerted fashion across its embassies. Similarly, because of the inability to consistently deploy employees overseas, HHS is unable to build institutional knowledge on vital global health matters or develop a workforce that has global health experience. The latter is problematic as it limits the number of individuals with appropriate competencies that HHS can draw from to appoint health attachés and other needed positions. With the ever-changing landscape of global health, and the constant array of threats that have the potential to affect the health of Americans, a constant standing workforce deployed abroad that is well versed in global health would benefit the United States. Current efforts to address this issue, which include courses and certificates in diplomacy and science and technology, are not able to address competency issues in the workforce in a scalable and real-world fashion. Furthermore, current mechanisms to inject global health expertise into the U.S. Department of State, such as the limited noncareer appointments, while useful in filling workforce deficiencies for programs like PEPFAR (U.S. Department of State, 2017c) are short-term solutions and fail to address the loss of institutional knowledge and the need for the creation of a true global health career track.12
Establishing a global health career track in the U.S. Department of State would address the workforce deficiencies described above. However, this would require a strong commitment by State to build global health as a career path and elevate it as a critical issue. This could happen simi-
___________________
11 Personal communication with Matthew Brown, NIH, November 9, 2016.
12 Personal communication with Matthew Brown, NIH, January 9, 2017.
larly to how the U.S. Department of State elevated economic diplomacy by increasing training in economics, establishing a chief economist, and creating a role of an Undersecretary for Economic Growth, Energy, and the Environment—as was described in the 2010 Quadrennial Diplomacy and Development Review (U.S. Department of State and USAID, 2010). Creating a global health track would first involve establishing a skill code for public health in the Foreign Service and more thoroughly introducing global health into the School of Professional and Area Studies, perhaps by creating a dean at the Foreign Service Institute.13 This would establish a solid foundation for global health within the Foreign Service, but it would need to be supplemented by designating positions for global health at all levels within the department to align with the promotion system. Though this would be resource intensive, it could lead to a sustainable and proactive approach to addressing global health issues throughout the world within the U.S. Department of State’s purview.
Enabling Knowledge Sustainment
Because it will take time for the U.S. Department of State to establish the global health career track, an integrated system with HHS and the U.S. Department of State would enable HHS employees (who have a full depth of expertise in health-related issues, such as disease surveillance and research) to populate positions in the U.S. Department of State as the track gets developed, and can lead to cooperation during outbreaks and global health emergencies in the future. An amendment of the Foreign Service Act by Congress to authorize HHS to use the Foreign Service Personnel System14 would also be a first step to developing a foreign service arm of HHS. As the U.S. Department of State itself has called for more collaboration and workforce mobility between it and other departments and agencies to foster a whole-of-government approach to diplomacy (U.S. Department of State and USAID, 2010), allowing HHS to access the Foreign Service Personnel System could help to foster this collaboration. Additionally, during public health emergencies, this foreign service arm designation would facilitate a rapid injection of knowledgeable people from HHS into the U.S. Department of State to meet temporary needs (U.S. Department of State and USAID, 2010), providing the U.S. government much needed agility and a more cohesive approach to responding to urgent threats.
The need for a Foreign Service arm of HHS, namely at CDC, was echoed by multiple respondents from this committee’s information gather-
___________________
13 Personal communication with Matthew Brown, NIH, February 6, 2017.
14 This would be similar to that of the Foreign Agricultural Service and the Foreign Commercial Service.
ing solicitation (described in Chapter 1). With CDC’s leading role in GHSA and the clear effects of emerging infectious disease threats on national security, it is evident that the current ad hoc approach is insufficient and such an arm is needed. By using the Foreign Service Personnel System, HHS can enable employees to pursue a career in global health in the short term. In the long term, this would systematically build a global health workforce—a necessary prerequisite for HHS to develop a pool from which to draw future health attachés to support U.S. embassy missions.
Creating the Workforce Pipeline
To create a sustainable U.S. workforce with these types of health and foreign diplomacy skills, it is important to think about the education and skills needed. Universities are already creating environments that support interdisciplinary education and research and blending majors to ensure cross-sector thinking and interaction. This is particularly relevant to the field of global health, with nearly 250 North American universities now offering global health education. This reflects the growing interest from American students in global health as well as a trend of funding agencies turning to universities as problem solvers for global health. These networks of interdisciplinary collaboration and culture of reciprocity make universities great environments for innovation. Pushing the feedback loop even further are entities like USAID’s Higher Education Solutions Network, which is using this built expertise to help solve global health problems. These universities are prime locations to start integrating diplomacy skills and leadership into global health curricula in a manner that reflects the necessary shared competencies (Brown et al., 2016). As centers of learning already supported by international partners (Hosseini Divkolaye et al., 2016), they can create a strong and dedicated workforce for the United States’ global health diplomacy.
SUMMARY AND RECOMMENDATION
The developments described throughout this report have created an environment for a centralized and comprehensive strategy for global health diplomacy. For the United States to continue to be a leader in global health, as well as adequately protect U.S. citizens at home and abroad, continued engagement in the international global health architecture is paramount. Though there are many calls for management and operational reforms in WHO (Gostin et al., 2016), the functions that it performs will continue to be essential for global health security and prosperity. Additionally the increased number of other multilateral organizations focused on health, either directly or indirectly, provides an opportunity to synergize efforts to-
ward achieving aligned global health goals more sustainably and efficiently (Nuzzo and Shearer, 2017).
The United States can maintain a health presence in countries in today’s interconnected world while sustainably beginning to phase down direct aid programs. In the absence of a health career track in the Foreign Service, the demand for U.S. health expertise in host countries cannot be sustainably filled and those that are deployed often lack diplomacy skills. Similarly, during an international health emergency, the U.S. Department of State does not have historical experience and appropriate health knowledge networks to draw from, leading to ad hoc groups being formed for each new event that are much less effective than they could be (Chen, 2015; Kaufmann and Feldbaum, 2009).
Conclusion: While the committee agrees on the need for management and operational reform for the World Health Organization (WHO), it also recognizes that the organization is underfunded and that many functions it performs are essential. In addition, many other United Nations agencies and international organizations and partnerships formed in the last few decades are crucial in providing support around the world. The success of all these entities will help the U.S. government accomplish its global health goals and maximize its returns on investments.
Conclusion: Important priorities for the U.S. government, such as global health security, reduction of child mortality, research and development to create new tools and improve program delivery, and achievement of the goal of an AIDS-free generation, will depend on continued engagement with and strengthening of these established and emerging multilateral institutions.
Conclusion: With the changing landscape of global health, the U.S. government has an opportunity to be more strategic in its programs and diplomacy. There is a need for better bidirectional communication and partnership between health and diplomacy professionals.
Recommendation 14: Commit to Continued Global Health Leadership
To protect itself from global threats, benefit from successes achieved in global health programs, and maintain a strong research and development pipeline, the United States should commit to maintaining its leadership in global health and actively participating in global health governance, coordination, and collaboration. To
this end, the U.S. Department of State and the U.S. Department of Health and Human Services (HHS) should do the following:
- Use their influence to improve the performance of key United Nations agencies and other international organizations important to global health, particularly the World Health Organization (WHO). WHO is in need of greater resources to address the health challenges of the 21st century, and many of its priorities align with those of the U.S. government. However, U.S. government financial contributions to WHO should come with a requirement that the organization adopt and implement the much-needed management reforms identified in recent reports.
- Remain involved in and firmly committed to innovative global partnerships that further U.S. global health goals, such as the highly successful Gavi, the Vaccine Alliance, and the Global Fund to Fight AIDS, Tuberculosis and Malaria, as well as promising new entities such as the Global Health Security Agenda and the Global Financing Facility.
- Implement a more strategic approach to achieving global health goals. This new approach should include the commitment of the U.S. Department of State to creating a global health career track and congressional action to enable the establishment of a cadre of global health experts within HHS through an amendment to the Foreign Service Act. This would create the environment necessary to expand the health attaché program, particularly in middle-income countries.
REFERENCES
Armitage, R. L., and J. S. Nye Jr. 2007. CSIS Commission on Smart Power: A smarter, more secure America. Washington, DC: Center for Strategic and International Studies.
Bliss, K. E. 2014. Global health within a domestic agency: The transformation of the Office of Global Affairs at HHS. Washington, DC: Center for Strategic and International Studies.
Brown, M., J. Bergmann, T. Mackey, Q. Eichbaum, L. McDougal, and T. Novotny. 2016. Mapping foreign affairs and global public health competencies: Towards a competency model for global health diplomacy. Global Health Governance 10(2):3-49.
Brown, M. D., T. K. Mackey, C. N. Shapiro, J. Kolker, and T. E. Novotny. 2014. Bridging public health and foreign affairs: The tradecraft of global health diplomacy and the role of health attachés. Science and Diplomacy 3(3).
CEPI (Coalition for Epidemic Preparedness Initiative). 2017. CEPI: New vaccines for a safer world. http://cepi.net/sites/default/files/CEPI_2pager_03_Feb_17.pdf (accessed March 1, 2017).
Chen, J. F. 2015. Reinstituting the ESTH cone within the US foreign service. Journal of Science Policy and Governance 7(1).
Ebola Interim Assessment Panel. 2015. Report of the Ebola Interim Assessment Panel. Geneva, Switzerland: World Health Organization.
Daulaire, N. 2012. The importance of the global health strategy from the U.S. Department of Health and Human Services. The American Journal of Tropical Medicine and Hygiene 87(3):382-384.
Feldbaum, H., and J. Michaud. 2010. Health diplomacy and the enduring relevance of foreign policy interests. PLOS Medicine 7(4):e1000226.
Fieinsilver, J. 2009. Cuban medical diplomacy. In The Cuba Reader: History, Culture, Politics, edited by A. Chomsky, P. M. Smorkaloff and B. Carr. Durham, NC: Duke University Press. Pp. 590-594.
GHSA (Global Health Security Agenda). 2016. Membership. https://www.ghsagenda.org/members (accessed December 15, 2016).
GHSA. 2017. Advancing the Global Health Security Agenda: Progress and early impact from U.S. investment. Washington, DC: Global Health Security Agenda.
GHSA. n.d. Global Health Security Agenda Private Sector Roundtable: Mobilizing industry for action. https://www.ghsagenda.org/docs/default-source/default-document-library/ghsa-private-sector-roundtable-508.pdf (accessed February 20, 2017).
Gostin, L. O., O. Tomori, S. Wibulpolprasert, A. K. Jha, J. Frenk, S. Moon, J. Phumaphi, P. Piot, B. Stocking, V. J. Dzau, and G. M. Leung. 2016. Toward a common secure future: Four global commissions in the wake of Ebola. PLOS Medicine 13(5):e1002042.
Huang, Y. 2016. China’s healthcare sector and U.S.-China health cooperation. Paper presented at the Hearing on China’s 13th Five-Year Plan. Washington, DC: U.S.-China Economic and Securty Review Commission.
HHS (U.S. Department of Health and Human Services). 2016a. Health attachés. https://www.hhs.gov/about/agencies/oga/global-health-diplomacy/health-attaches/index.html (accessed December 15, 2016).
HHS. 2016b. Global Bidding & Assignment System: Filling overseas global public health vacancies with a specialized system for global recruitment. https://www.hhs.gov/idealab/projects-item/global-bidding-assignment-system (accessed December 15, 2016).
HHS. 2017. Global health security. https://www.hhs.gov/about/agencies/oga/global-health-security/index.html?language=es (accessed February 2, 2017).
Hosseini Divkolaye, N. S., M. H. Radfar, F. Seighali, and F. M. Burkle. 2016. When health diplomacy serves foreign policy: Use of soft power to quell conflict and crises. Disaster Medicine and Public Health Preparedness 10(5):724-727.
ISAB (International Security Advisory Board). 2016. Report on international security and foreign policy implications of overseas disease outbreaks. Washington, DC: International Security Advisory Board, U.S. Department of State.
Jones, S. G., and M. C. Libicki. 2008. How terrorist groups end: Lessons for countering al qa’ida. Arlington, VA: RAND Corporation.
Kaufmann, J. R., and H. Feldbaum. 2009. Diplomacy and the polio immunization boycott in northern Nigeria. Health Affairs 28(4):1091-1101.
Kevany, S. 2015. Diplomatic advantages and threats in global health program selection, design, delivery and implementation: Development and application of the Kevany Riposte. Globalization and Health 11(1):22.
Kickbusch, I., and M. M. C. Szabo. 2014. A new governance space for health. Global Health Action 7(1):25307.
Kuo, M. A. 2016. U.S.-China relations: Public diplomacy and soft power. The Diplomat, December 5. http://thediplomat.com/2016/12/us-china-relations-public-diplomacy-and-soft-power (accessed January 15, 2017).
McGiffert, C. 2009. Chinese soft power and its implications for the United States: Competition and cooperation in the developing world: A report of the CSIS Smart Power Initiative. Washington, DC: Center for Strategic & International Studies.
Moon, S., J. Leigh, L. Woskie, F. Checchi, V. Dzau, M. Fallah, G. Fitzgerald, L. Garrett, L. Gostin, D. L. Heymann, R. Katz, I. Kickbusch, J. S. Morrison, P. Piot, P. Sands, D. Sridhar, and A. K. Jha. 2017. Post-Ebola reforms: Ample analysis, inadequate action. British Medical Journal 356:j280-j288.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2015. Diplomacy for the 21st century: Embedding a culture of science and technology Throughout the Department of State. Washington, DC: The National Academies Press.
Nuzzo, J. B., and M. P. Shearer. 2017. International engagement is critical to fighting epidemics. Health Security 15(1):33-35.
OIG (Office of the Inspector General). 2002. Memorandum audit report: U.S. Department of State’s Foreign Service “up-or-out” promotion system. Washington, DC: Office of Inspector General, U.S. Department of Health and Human Services.
The PLOS Medicine Editors. 2007. How is who responding to global public health threats? PLOS Medicine 4(5):e197.
U.S. Department of State. 2010. Momorandum of understanding for the collaborative program on emerging and re-emerging infectious diseases between the Department of Health and Human Services of the United States of America and the Ministry of Health of the People’s Republic of China. Washington, DC: U.S. Department of State.
U.S. Department of State. 2016. Department of State organization chart: November 2016. https://www.state.gov/r/pa/ei/rls/dos/99484.htm (accessed February 10, 2017).
U.S. Department of State. 2017a. Career tracks for foreign service officers. https://careers.state.gov/work/foreign-service/officer/career-tracks (accessed February 2, 2017).
U.S. Department of State. 2017b. International health and biodefense. https://www.state.gov/e/oes/intlhealthbiodefense (accessed February 2, 2017).
U.S. Department of State. 2017c. Limited non-career appointments (LNAs). https://careers.state.gov/work/foreign-service/lna (accessed February 2, 2017).
U.S. Department of State. n.d. What we do. https://www.state.gov/whatwedo (accessed April 10, 2017).
U.S. Department of State and USAID (U.S. Agency for International Development). 2010. Leading through civilian power: The first quadrennial diplomacy and development review. Washington, DC: U.S. Department of State.






















